Inter-hospital Geriatrics Meeting August 2014 The Watery Curse
|
|
|
- Lawrence Bailey
- 5 years ago
- Views:
Transcription
1 Inter-hospital Geriatrics Meeting August 2014 The Watery Curse Speaker: Dr. KK Yam (QMH) Supervisor: Dr. Patrick Chiu
2 Patient s history F/95 Lives with daughter & maid ADL partially dependent. Walks with stick (indoor); Wheelchair (outdoor)
3 Medical history & medications HT Aspirin AF Pantoprazole CHF Frusemide CVA (Lt cerebellar infarct) Duodenal ulcers Perindopril Diltiazem Uterine prolapse
4 Admission in Dec 2012 Presented with fever and dysuria MSU culture grew E. Coli sensitive to cefuroxime Given cefuroxime for 1 week and symptoms resolved Dec Jan Feb Mar Apr May UTI
5 Admission in Jan 2013 Presented with fever & cough CXR: RMZ consolidation ST: no dysphagia Treated as pneumonia with Augmentin for 1 week Dec Repeated CXR showed resolution of consolidation Jan Feb Mar Apr May UTI Pneumonia
6 Re-admission after 2 days Developed profuse watery diarrhea 2 days later With small amount of fresh blood in stool Colicky central abdominal pain No vomiting No recent contact / travel history / raw food Dec Jan Feb Mar Apr May UTI Pneumonia
7 Physical examination Mildly dehydrated Vital signs stable and afebrile Abdomen: mild tenderness over peri-umbilical region, soft with hyperactive bowel sounds PR: brownish stool Other systems unremarkable
8 Differential diagnoses Drug related: Augmentin Infective: viral GE, bacterial dysentery, C.difficile associated diarrhea Malignancy: Colorectal tumour Other causes of colitis
9 Investigations WCC and differential counts normal Hb 11.5 Electrolytes, renal, liver & serum amylase - unremarkable Albumin 29 g/l. CEA normal AXR unremarkable
10 Stool investigations Clostridium difficile culture & its cytotoxin - positive Other bacterial culture negative Norovirus study negative Clinical Impression Clostridium difficile associated diarrhea (CDAD)
11 A review on C. Difficile associated infection Microbiology /pathophysiology Epidemiology Risk factors Presentation and Diagnosis
12 C. difficile associated diarrhea (CDAD) % of all Antibiotic-associated diarrhea - A spectrum of diseases of different severity 1. C. difficile associated diarrhea (CDAD) with colitis 2. Pseudomembranous colitis 3. Fulminant colitis Different manifestations and endoscopic findings Mild disease Severe disease
13 C. Difficile Difficult clostridium" Microbiology Anaerobic, gram-positive, spore-forming, toxin-producing bacillus Spores are resistant to drying, temperature & many antiseptic solutions. Toxin A (enterotoxin) causes inflammation leading to intestinal fluid secretion, mucosal injury, directly activates neutrophils Toxin B (cytotoxin) essential for the virulence of C. difficile, approximately 10 times more potent than toxin A for mediating colonic mucosal damage
14 Pathophysiology Colonization of C. Difficile (pre-existing / spores via fecal oral route) Plus Disruption of normal intestinal flora by antimicrobial therapy Evasion of immunity & C. difficile multiplies 2 toxins that bind to receptors on intestinal epithelial cells Inflammation and diarrhea
15 A review on C. Difficile associated infection Microbiology /pathophysiology Epidemiology Risk factors Presentation and Diagnosis
16 Carrier state 3% of healthy adults carry this organism 16-35% in hospitalized adults 50% in institutionalized elderly Saima Aslam, Richard J Hamill, Daniel M Musher; Treatment of Clostridium difficileassociated disease: old therapies and new strategies; Lancet Infect Dis 2005; 5:
17 Epidemiology Increase in incidence since 2000 US National Hospital Discharge Survey CDI-associated hospitalizations 31 / in / in / in 2005 An approximate 25% annual increase each year since 2000 Associated with the rise of BI/NAP1/027 strain Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No 9
18 Hypervirulent strains Characterized by higher than usual toxin A and B production Presence of a third toxin, binary toxin (unknown effects) Designated as BI/NAP1/027 Associated with lower clinical cure rates, increased recurrence rates, increase mortality rate Jennifer R. O Connor et al. Clostridium difficile Infection Caused by the Epidemic BI/NAP1/027 Strain. GASTROENTEROLOGY 2009;136:
19 Prognosis in age >=80 70 patients with C. difficile infection (1/1 31/12/06) Mean age = 84.0 (range 80-94). 41.1% were male. Treatment failure 27.7% 90-day mortality 17.1%. 90-day mortality in hospitalized patients: 21.8%. 4.3% developed toxic megacolon. Reference: Eric D. Cober, Preeti N. Malani; Clostridium Difficile Infection in the Oldest Old Clinical Outcomes in Patients Aged 80 and Older; JAGS; 57: , 2009
20 Mortality due to Clostridium difficile infection 27 studies with cases of CDI great heterogeneity in the methods for reporting mortality The overall associated mortality to be at least 5.99% within 3 months of diagnosis (mostly due to severe diseases) Higher mortality is associated with advanced age, being 13.5% in patients over 80 years J.A. Karas a,*, D.A. Enoch b, S.H. Aliyu; A review of mortality due to Clostridium difficile infection; Journal of Infection (2010) 61, 1e8.
21 Predictors of fatal outcome Poor comorbidity status High WCC counts (>20 asso. with 18% mortality) Low diastolic BP Clinical signs of sepsis Renal and pulmonary dysfunction Haig Dudukgian et al; C. difficile colitis-predictors of fatal outcome; J Gastrointest Surg (2010) 14:
22 Situation in HK Situation in Queen Mary Hospital Between Sept 2008 to Dec 2008, 723 stool samples (496 patients) were collected for detection of C difficile cytotoxin. 37 samples (5.1%) demonstrate a positive result for the cytotoxin assay. Hypervirulent NAP-1/027 Strain Detected in 1 out of 37 stool samples +ve for C. difficile cytotoxin in Queen Mary Hospital in 2008 (Sept to Dec). Reference: Clostridium difficile ribotype 027 arrives in Hong Kong; Letters to the Editor/ International Journal of Antimicrobial Agents 34 (2009)
23
24 A review on C. Difficile associated infection Microbiology /pathophysiology Epidemiology Risk factors of Clostridium Difficile associated disease (CDAD) Presentation and Diagnosis
25 4 Main Risk factors of (CDAD) 1: Antimicrobial use Clindamycin (RR=9), penicillins (Augmentin RR=22), cephalosporins (Rocephin RR=36), and fluoroquinolones (associated with the hypervirulent strain BI/NAP1/027 ) 2: Hospital admission Risk is proportional to duration of hospital stay Risk increases with increased exposure to antibiotics 3: Age > 65 years confers a relative risk > 10 4: Impaired immunity Reference: (1) Haihui Huang et al. Antimicrobial resistance in Clostridium difficile. International Journal of Antimicrobial Agents 34 (2009) (2) A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No 9 Saima Aslam, Richard J Hamill, Daniel M Musher; Treatment of Clostridium difficile-associated disease: old therapies and new strategies; Lancet Infect Dis 2005; 5: (3),(4) Kelly C, LaMont J. N Engl J Med 2008;359:
26 Hospital admission If we use the same antibiotics CDI complicated 0.5%-1% of hospital admissions CDI complicated <0.02% antimicrobial usage in the community Why? Exposure to toxigenic C difficile or its spores, everywhere inside the hospital environment Reference: Saima Aslam, Richard J Hamill, Daniel M Musher; Treatment of Clostridium difficile-associated disease: old therapies and new strategies; Lancet Infect Dis 2005; 5:
27 Impaired immunity Kelly C, LaMont J. N Engl J Med 2008;359:
28 A review on C. Difficile associated infection Microbiology /pathophysiology Epidemiology Risk factors Presentation and Diagnosis of Clostridium difficile associated disease (CDAD)
29 Clinical presentations Onset of diarrhea during or after antimicrobial usage (Disease onset can be delayed by 2 months or rarely 3 months) Mild disease Fever (28%), abdominal discomfort (22%) and neutrophilia (50%) indicating colitis Hypoalbuminemia Unexplained leukocytosis in hospitalized patients (even in the absence of diarrhea) may reflect underlying C. difficile infection; diarrhea often develops in the next one to two days Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No 9
30 Clinical presentations Severe disease / Fulminant colitis (10%) Abdominal pain - severe lower quadrant / diffuse; Peritonism may indicate bowel perforation Diarrhea - may be less prominent (atonic colon) Systemic manifestation - shock & high fever Metabolic acidosis On AXR: Toxic megacolon (4.3): colonic dilatation >7 cm in its greatest diameter accompanied by severe systemic toxicity Reference: Eric D. Cober, Preeti N. Malani; Clostridium Difficile Infection in the Oldest Old Clinical Outcomes in Patients Aged 80 and Older; JAGS; 57: , 2009
31 Diagnosis of CDAD Diarrhoea Diarrhoea (> 3 unformed stools per 24 hr for > 2 days) PLUS Toxin A/B in the stool OR Toxigenic C. difficile detected by stool culture OR Pseudomembranes seen in the colon Reference: Harrison s principles of Internal Medicine 16th edition
32 Diagnosis of CDAD Possibilities CDAD? Remarks Both Toxin and Culture -ve Both Toxin and Culture +ve No Yes Toxin +ve only Yes Contamination usually unlikely Culture +ve only Depends on clinical situation -Labile toxins may be lost -Carrier stage because culture in most lab does not distinguish between toxigenic and nontoxigenic strains References: -Uptodate.com -QMH microbiologists
33 Indications Endoscopy? High clinical suspicion for C. difficile with negative laboratory assays. Prompt C. difficile diagnosis needed before laboratory results can be obtained Failed to respond to antibiotic therapy Atypical presentation with ileus or minimal diarrhea Findings: Shallow ulcerations on the intestine mucosal surface Pseudomembranes: raised yellow or white plaques up to 2 cm in diameter, scattered over the colorectal mucosa Pathognomonic for C. difficile infection
34 Role of CT abdomen? CT abdomen shows marked thickening of colonic wall Usually done for suspected colonic perforation Or to rule out other diagnosis including ischemic bowel
35 Back to our patient
36 Progress Dx to have CDAD due to positive cytotoxin in stool Started on a 5 days course of Flagyl 500 mg tds po by parent team Symptoms improved and discharged. Dec Jan Feb Mar Apr May UTI Pneumonia C.Difficile infection
37 Admission in Feb 2014 LUT symptoms and fever Urine culture grew E.Coli (sensitive to cefuroxime) Prescribed with cefuroxime USG kidneys for recurrent UTI - only a few renal cysts Dec Jan Feb Mar Apr May UTI Pneumonia C.Difficile infection UTI
38 Admission in Mar 2014 Presented with watery diarrhoea for 2 days No fever, soft abdomen with hyperactive bowel sounds WCC normal, Liver and renal biochemistries unremarkable, Albumin 22 g/l AXR showed no dilated bowel shadow Dec Jan Feb Mar Apr May UTI Pneumonia C.Difficile infection UTI
39 Progress Stool C/ST grew Aeromonas, Clostridium difficile and its cytotoxin +ve Tx: Ciprofloxacin 500 mg BD po for 5 days. oral vancomycin 125 mg Q6H for 2 weeks (1 st recurrence of CDAD) Diarrhea subsided Dec Jan Feb Mar Apr May UTI Pneumonia C.Difficile infection UTI C.Difficile infection
40 Admission in May 2014 Dec Presented with watery diarrhea again. No intake of antibiotics in between PE: no signs of acute abdomen: soft with hyperactive bowel sounds WCC normal, Liver and renal biochemistries unremarkable, Albumin 22 g/l Jan Feb Mar Apr May Jun UTI Pneumonia C.Difficile infection UTI C.Difficile infection
41 Progress C. Difficile and its cytotoxin were +ve (2nd recurrence). Dec Jan Feb Mar Apr May Jun UTI Pneumonia C.Difficile infection UTI C.Difficile infection (First recurrence) C.Difficile infection (Second recurrence)
42 A review on C. Difficile associated infection Microbiology /pathophysiology Epidemiology Risk factors Presentation and Diagnosis Management (initial and recurrent disease)
43 Treatment of Initial Infection mild disease Stopped the inciting antibiotics 25% of patients have resolution of diarrhea within 48 hrs However, stopping the inciting antibiotic may not be practical clinically! Contact precautions and hand hygiene (soap better than alcohol based agent) Avoid anti-motility agents e.g. imodium linked to toxic megacolon / delay toxins excretion Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359:
44 Treatment of Initial Infection mild disease Regime: Oral metronidazole, 500 mg every 6 hours for 10 to 14 days - in frail patients - in patients whose inciting antimicrobials cannot be discontinued safely because of intercurrent infection The Society for Healthcare Epidemiology of America recommends initiating empirical therapy for C. difficile immediately after specimen procurement for patients with more severe symptoms consistent with CDI A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359: The Society for Healthcare Epidemiology of America
45 Treatment of Initial Infection - severe disease Regime: Oral vancomycin, 125 mg every 6 hours for 10 to 14 days Oral vancomycin also indicated for - metronidazole contraindications or intolerance - inadequate response to metronidazole treatment - proven metronidazole resistance strains - pregnancy - age <10 yo
46 Treatment of Initial Infection - severe disease Consulted surgeons: Peritoneal signs / suspicion of acute abdomen Severe ileus Toxic megacolon Implications: monitor IO, AXR closely
47 How to define severe infection? No consensus Predictors of fatal outcome Poor comorbidity status High WCC counts (>20 asso. with 18% mortality) Low diastolic BP Clinical signs of sepsis Renal impairment Presence of pseudomembranous colitis on endoscopy
48 Rationale of use of flagyl? Response Rates to Vancomycin and Metronidazole Therapy, According to the Severity of C. difficile Infection Oral vancomycin is generally reserved as 2 nd line to minimize the emergency of vancomycin resistant strains Kelly C, LaMont J. N Engl J Med 2008;359:
49 Comparison of minimal inhibitory conc (MICs) and resistance rates of C. difficile isolates from different countries Most isolates are still susceptible to vancomycin and metronidazole (MTZ) Haihui Huang et al; Antimicrobial resistance in Clostridium difficile; International Journal of Antimicrobial Agents 34 (2009)
50 Recurrent C. Difficile Infection
51 Risk factors for recurrence History of recurrence Age Use of additional / multiple antimicrobials Inadequate protective immune response Inadequate treatment Infection by hypervirulent strains Proton pump inhibitor use during incident CDI ICU stay / Long hospital stay Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359: Saima Aslam, Richard J Hamill, Daniel M Musher; Treatment of Clostridium difficile-associated disease: old therapies and new strategies; Lancet Infect Dis 2005; 5:
52 Mechanism of recurrence Poorly understood Rarely related to antimicrobial resistance Impaired immunity Could be re-infection by the same strain or infection by a new strain Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359:
53 Recurrence of C. Difficile Infection Typically occurs 1-2 weeks after stopping metronidazole or vancomycin. Recurrence rates following treatment with metronidazole or vancomycin are 20%. 2nd recurrence: > 40% risk of recurrence. 3rd recurrence: > 60% risk of recurrence. Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359:
54 Management of 1 st recurrence Same as for initial episode. Metronidazole [Flagyl] 500 mg tds po for 10 to 14 days. Vancomycin 125 mg QID po for 10 to 14 days. Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359:
55 Management of 2 nd recurrence Vancomycin in TAPERED and PULSED doses (response rate 86% ): 125 mg QID po for 14 days 125 mg BD for 7 days 125 mg daily for 7 days 125 mg every 2 days for 8 days [4 doses] 125 mg every 3 days for 15 days [5 doses] Prolonged metronidazole therapy is not advocated because of risk of peripheral neuropathy Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359:
56 Management of 3rd recurrence Vancomycin 125 mg QID po for 14 days and then Rifaximin 400 mg BD for 14 days (not available in HA formulary). Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359:
57 Back to our patient again
58 2 nd recurrence in our patient Tx: Started on Pulsed and Tapered dose of vancomycin. Still persistent watery diarrhea after around 1.5 weeks of treatment Impression: refractory disease Dec Jan Feb Mar Apr May Jun UTI Pneumonia C.Difficile infection UTI C.Difficile infection (First recurrence) C.Difficile infection (Second recurrence)
59 Most respond after 1 week of Tx
60 Management of refractory disease / not responding to initial agent(s) Change oral metronidazole to oral vancomycin Add IV Metronidazole 500 mg Q8H i.v. (IV vancomycin is not useful) Vancomycin enema usage of rectal tube with instillation of vancomycin (500 mg vancomycin into 1L of normal saline at 1-3 ml/min to maximum of 2 gram in 24 hrs). Reference: QMH microbiologists
61 Summary of Tx for CDAD Initial Management First recurrence Second recurrence Third recurrence Refractory and multiple recurrences For all Strict Contact precaution consider stopping the inciting antibiotics Mild Po Flagyl for days Same as initial Pulsed vancomycin -Vancomycin enema -intrgastric vancomycin -rifaximin -add iv flagyl Consider novel agents Severe Po Vancomycin for days Same as initial Pulsed vancomycin -Vancomycin enema - intrgastric vancomycin -rifaximin -add iv flagyl +/- intensive care +/- intensive care +/- intensive care
62 Novel therapy for refractory disease / multiple recurrences
63 Novel therapy 1. New antibiotics 2. Probiotics 3. IVIG 4. Monoclonal antibodies 5. Fecal Microbiota Transplantation
64 New antibiotics Fidaxomicin was approved in 2011 for treatment of CDI by USA FDA New class of narrow spectrum antibiotics Selective eradication of C. difficile with minimal disruption to the bacteria that make up the normal healthy intestinal flora A 20 tab pack costs upwards of Not a/v in HA formulatory
65 Probiotics Probiotics (S. Boulardii, lactobacillus species) Insufficient evidence for prophylactic measures Insufficient evidence to recommend probiotic therapy as an adjunct to antibiotic therapy for colitis or alone in the treatment of colitis. May consider in refractory or recurrent diseases Risks do present (reports of fungemia) Reference: - Pillai, Anjana. Nelson, Richard L; Probiotics for treatment of Clostridium difficile-associated colitis in adults; Cochrane Database of Systematic Reviews. 1, Gareth C Parkes, Jeremy D Sanderson, Kevin Whelan; The mechanisms and effi cacy of probiotics in the prevention of Clostridium diffi cile-associated diarrhoea; Lancet Infect Dis 2009;9:
66 IVIG as an option for recurrent infection IVIG 400 mg/kg once every 3 weeks for 2 or 3 doses case series for patients with relapsing or severe C. difficile colitis No RCT yet Reference: A 76-Year-Old Man With Recurrent Clostridium difficile-associated Diarrhoea; JAMA, March 4, 2009 Vol 301 No Kelly C, LaMont J. N Engl J Med 2008;359:
67 Monoclonal antibodies Against C. difficile toxins A (CDA1) and B (CDB1). The antibodies were administered together as a single infusion in symptomatic CDAD patients in addition to antibiotics (VAN or MTZ) rate of recurrence of C. difficile infection was lower among patients treated with monoclonal antibodies (7% vs. 25%; 95% confidence interval, 7 to 29; P<0.001). Lowy I et al. N Engl J Med 2010;362:
68 Time to Recurrence of Clostridium difficile Infection Lowy I et al. N Engl J Med 2010;362:
69 Fecal Microbiota Transplantation An RCT published in the NEJM Jan 2013 Excellent efficacy in treatment of recurrent / refractory C.difficile infection 94% vs 31% cure rate by vancomycin Study is terminated prematurely because unethical NOT to offer this treatment to all patients in the study Accepted by patients? Van Nood E et al; "Duodenal Infusion of Donor Feces for Recurrent Clostridium difficile". N Engl J Med368 (5):
70 Back to our patient
71 Our patient Started on IV Metronidazole for 2 weeks (Microbiologist s suggestion) Diarrhoea improved Dec Jan Feb Mar Apr May Jun Jul Aug UTI Pneumonia C.Difficile infection UTI C.Difficile infection (First recurrence) C.Difficile infection (Second recurrence)
72 Our patient Well until now after the 2 nd recurrence (which was treated with oral vancomycin and IV flagyl) Dec Jan Feb Mar Apr May Jun Jul Aug UTI Pneumonia C.Difficile infection UTI C.Difficile infection (First recurrence) C.Difficile infection (Second recurrence) Discharged
73 Conclusions Geriatrics patients possess many risk factors for C. Difficile infection Judicious use of antibiotics AND hand hygiene are important to prevent the disease Adequate treatment of C. Difficile infection is important to reduce recurrence Consult surgeons in case of severe disease Outcome is poorer in older adults Existence of hypervirulent strain
74 Thank you
Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review
 Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review October 18, 2010 James Kahn and Carolyn Kenney, MSIV Overview Burden of disease associated
Diagnosis, Management, and Prevention of Clostridium difficile infection in Long-Term Care Facilities: A Review October 18, 2010 James Kahn and Carolyn Kenney, MSIV Overview Burden of disease associated
ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE
 ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE The diagnosis of CDI should be based on a combination of clinical and laboratory findings. A case definition for the usual
ENGLISH FOR PROFESSIONAL PURPOSES UNIT 3 HOW TO DEAL WITH CLOSTRIDIUM DIFFICILE The diagnosis of CDI should be based on a combination of clinical and laboratory findings. A case definition for the usual
9/18/2018. Clostridium Difficile: Updates on Diagnosis and Treatment. Clostridium difficile Infection (CDI) Clostridium difficile Infection (CDI)
 Clostridium Difficile: Updates on Diagnosis and Treatment Elizabeth Hudson, DO, MPH 9/25/18 Antibiotic-associated diarrhea and colitis were well established soon after widespread use of antibiotics In
Clostridium Difficile: Updates on Diagnosis and Treatment Elizabeth Hudson, DO, MPH 9/25/18 Antibiotic-associated diarrhea and colitis were well established soon after widespread use of antibiotics In
Division of GIM Lecture Series Case Presentation David A. Erickson, M.D October 9th, 2013
 Division of GIM Lecture Series Case Presentation David A. Erickson, M.D October 9th, 2013 Financial Disclosures No financial disclosures Objectives Review a case of recurrent Clostridium difficile infection
Division of GIM Lecture Series Case Presentation David A. Erickson, M.D October 9th, 2013 Financial Disclosures No financial disclosures Objectives Review a case of recurrent Clostridium difficile infection
Case 1. Which of the following would be next appropriate investigation/s regarding the pts diarrhoea?
 Case 1 21 yr old HIV +ve, Cd4-100 HAART naïve Profuse diarrhoea for 3/52. Stool MC&S ve Which of the following would be next appropriate investigation/s regarding the pts diarrhoea? Repeat stool MC&S Stool
Case 1 21 yr old HIV +ve, Cd4-100 HAART naïve Profuse diarrhoea for 3/52. Stool MC&S ve Which of the following would be next appropriate investigation/s regarding the pts diarrhoea? Repeat stool MC&S Stool
Clostridium difficile Infection (CDI) Management Guideline
 Clostridium difficile Infection (CDI) Management Guideline Do not test all patients with loose or watery stools for CDI o CDI is responsible for
Clostridium difficile Infection (CDI) Management Guideline Do not test all patients with loose or watery stools for CDI o CDI is responsible for
Clostridium Difficile Infection in Adults Treatment and Prevention
 Clostridium Difficile Infection in Adults Treatment and Prevention Definition: Clostridium Difficile colonizes the human intestinal tract after the normal gut flora has been altered by antibiotic therapy
Clostridium Difficile Infection in Adults Treatment and Prevention Definition: Clostridium Difficile colonizes the human intestinal tract after the normal gut flora has been altered by antibiotic therapy
CLOSTRIDIUM DIFICILE. Negin N Blattman Infectious Diseases Phoenix VA Healthcare System
 CLOSTRIDIUM DIFICILE Negin N Blattman Infectious Diseases Phoenix VA Healthcare System ANTIBIOTIC ASSOCIATED DIARRHEA 1978: C diff first identified 1989-1992: Four large outbreaks in the US caused by J
CLOSTRIDIUM DIFICILE Negin N Blattman Infectious Diseases Phoenix VA Healthcare System ANTIBIOTIC ASSOCIATED DIARRHEA 1978: C diff first identified 1989-1992: Four large outbreaks in the US caused by J
Stony Brook Adult Clostridium difficile Management Guidelines. Discontinue all unnecessary antibiotics
 Stony Brook Adult Clostridium difficile Management Guidelines Summary: Use of the C Diff Infection (CDI) PowerPlan (Adult) Required Patient with clinical findings suggestive of Clostridium difficile infection
Stony Brook Adult Clostridium difficile Management Guidelines Summary: Use of the C Diff Infection (CDI) PowerPlan (Adult) Required Patient with clinical findings suggestive of Clostridium difficile infection
Clostridium difficile Infection: Diagnosis and Management
 Clostridium difficile Infection: Diagnosis and Management Brian Viviano D.O. Case study 42 year old female with history of essential hypertension and COPD presents to ED complaining of 24 hours of intractable,
Clostridium difficile Infection: Diagnosis and Management Brian Viviano D.O. Case study 42 year old female with history of essential hypertension and COPD presents to ED complaining of 24 hours of intractable,
The Epidemiology of Clostridium difficile DANIEL SAMAN, DRPH, MPH RESEARCH SCIENTIST ESSENTIA INSTITUTE OF RURAL HEALTH
 The Epidemiology of Clostridium difficile DANIEL SAMAN, DRPH, MPH RESEARCH SCIENTIST ESSENTIA INSTITUTE OF RURAL HEALTH Some history first Clostridium difficile, a spore-forming gram-positive (i.e., thick
The Epidemiology of Clostridium difficile DANIEL SAMAN, DRPH, MPH RESEARCH SCIENTIST ESSENTIA INSTITUTE OF RURAL HEALTH Some history first Clostridium difficile, a spore-forming gram-positive (i.e., thick
EDUCATIONAL COMMENTARY CLOSTRIDIUM DIFFICILE UPDATE
 EDUCATIONAL COMMENTARY CLOSTRIDIUM DIFFICILE UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click
EDUCATIONAL COMMENTARY CLOSTRIDIUM DIFFICILE UPDATE Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click
Updated Clostridium difficile Treatment Guidelines
 Updated Clostridium difficile Treatment Guidelines Arielle Arnold, PharmD, BCPS Clinical Pharmacist Saint Alphonsus Regional Medical Center September 29 th, 2018 Disclosures Nothing to disclose Learning
Updated Clostridium difficile Treatment Guidelines Arielle Arnold, PharmD, BCPS Clinical Pharmacist Saint Alphonsus Regional Medical Center September 29 th, 2018 Disclosures Nothing to disclose Learning
Clostridium Difficile Associated Disease. Edmund Krasinski, Jr., D.O., F.A.C.G. Southwest Conference on Medicine 2011
 Clostridium Difficile Associated Disease Edmund Krasinski, Jr., D.O., F.A.C.G. Southwest Conference on Medicine 2011 Introduction Which of the following is more common in community hospitals in the Southeast
Clostridium Difficile Associated Disease Edmund Krasinski, Jr., D.O., F.A.C.G. Southwest Conference on Medicine 2011 Introduction Which of the following is more common in community hospitals in the Southeast
Clostridium difficile: Can you smell the new updates?
 Clostridium difficile: Can you smell the new updates? Sunish Shah, Pharm.D. PGY-2 Infectious Disease Pharmacy Resident Yale-New Haven Hospital sshah1741@mail.usciences.edu Learning objectives Recognize
Clostridium difficile: Can you smell the new updates? Sunish Shah, Pharm.D. PGY-2 Infectious Disease Pharmacy Resident Yale-New Haven Hospital sshah1741@mail.usciences.edu Learning objectives Recognize
Clostridium difficile CRISTINA BAKER, MD, MPH INFECTIOUS DISEASE PARK NICOLLET/HEALTH PARTNERS 11/9/2018
 Clostridium difficile CRISTINA BAKER, MD, MPH INFECTIOUS DISEASE PARK NICOLLET/HEALTH PARTNERS 11/9/2018 Disclosures None Objectives Highlight important changes in the management of Clostridium difficile
Clostridium difficile CRISTINA BAKER, MD, MPH INFECTIOUS DISEASE PARK NICOLLET/HEALTH PARTNERS 11/9/2018 Disclosures None Objectives Highlight important changes in the management of Clostridium difficile
Literature Scan: Antibiotics for Clostridium difficile Infection. Month/Year of Review: May 2015 Date of Last Review: April 2012
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Bezlotoxumab (Zinplava) as Adjunct Treatment for Clostridium difficile. Janel Liane Cala, RPh Medical Center Hospital
 Bezlotoxumab (Zinplava) as Adjunct Treatment for Clostridium difficile Janel Liane Cala, RPh Medical Center Hospital Objectives Review pathophysiology, risk factors, prevention, and treatment options of
Bezlotoxumab (Zinplava) as Adjunct Treatment for Clostridium difficile Janel Liane Cala, RPh Medical Center Hospital Objectives Review pathophysiology, risk factors, prevention, and treatment options of
A Pharmacist Perspective
 Leveraging Technology to Reduce CDI A Pharmacist Perspective Ed Eiland, Pharm.D., MBA, BCPS (AQ-ID) Clinical Practice and Business Supervisor Huntsville Hospital System Huntsville Hospital 881 licensed
Leveraging Technology to Reduce CDI A Pharmacist Perspective Ed Eiland, Pharm.D., MBA, BCPS (AQ-ID) Clinical Practice and Business Supervisor Huntsville Hospital System Huntsville Hospital 881 licensed
ABSTRACT PURPOSE METHODS
 ABSTRACT PURPOSE The purpose of this study was to characterize the CDI population at this institution according to known risk factors and to examine the effect of appropriate evidence-based treatment selection
ABSTRACT PURPOSE The purpose of this study was to characterize the CDI population at this institution according to known risk factors and to examine the effect of appropriate evidence-based treatment selection
Clostridium DifficileInfection & Readmissions: An ounce of prevention is worth a pound of cure
 Clostridium DifficileInfection & Readmissions: An ounce of prevention is worth a pound of cure Brian S. Zuckerbraun, MD, FACS Henry T. Bahnson Professor of Surgery University of Pittsburgh Chief, Trauma
Clostridium DifficileInfection & Readmissions: An ounce of prevention is worth a pound of cure Brian S. Zuckerbraun, MD, FACS Henry T. Bahnson Professor of Surgery University of Pittsburgh Chief, Trauma
March 3, To: Hospitals, Long Term Care Facilities, and Local Health Departments
 March 3, 2010 To: Hospitals, Long Term Care Facilities, and Local Health Departments From: NYSDOH Bureau of Healthcare Associated Infections HEALTH ADVISORY: GUIDANCE FOR PREVENTION AND CONTROL OF HEALTHCARE
March 3, 2010 To: Hospitals, Long Term Care Facilities, and Local Health Departments From: NYSDOH Bureau of Healthcare Associated Infections HEALTH ADVISORY: GUIDANCE FOR PREVENTION AND CONTROL OF HEALTHCARE
! MQ is a 44 year old woman that I first saw in Sept ! In MVA in Jan 2003 requiring spinal surgery
 Case MQ is a 44 year old woman that I first saw in Sept 2006 UPDATE ON CLOSTRIDIUM DIFFICILE DISEASE Richard A. Jacobs, M.D.,PhD In MVA in Jan 2003 requiring spinal surgery Subsequently developed fecal
Case MQ is a 44 year old woman that I first saw in Sept 2006 UPDATE ON CLOSTRIDIUM DIFFICILE DISEASE Richard A. Jacobs, M.D.,PhD In MVA in Jan 2003 requiring spinal surgery Subsequently developed fecal
DISCLAIMER: ECHO Nevada emphasizes patient privacy and asks participants to not share ANY Protected Health Information during ECHO clinics.
 DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
DISCLAIMER: Video will be taken at this clinic and potentially used in Project ECHO promotional materials. By attending this clinic, you consent to have your photo taken and allow Project ECHO to use this
Update on Clostridium difficile infection.
 Update on Clostridium difficile infection. K. Honein Gastroenterologist, HDF Associate Professor Head of Medicine Department St Joseph University-Beirut. Introduction Gram+anaerobic bacillus responsible
Update on Clostridium difficile infection. K. Honein Gastroenterologist, HDF Associate Professor Head of Medicine Department St Joseph University-Beirut. Introduction Gram+anaerobic bacillus responsible
GUIDELINE FOR THE MANAGEMENT OF ANTIBIOTIC- ASSOCIATED DIARRHOEA IN ADULTS
 GUIDELINE FOR THE MANAGEMENT OF ANTIBIOTIC- ASSOCIATED DIARRHOEA IN ADULTS Version 3.0 Date ratified May 2008 Review date May 2010 Ratified by NUH Antibiotic Guidelines Committee NUH Drugs and Therapeutics
GUIDELINE FOR THE MANAGEMENT OF ANTIBIOTIC- ASSOCIATED DIARRHOEA IN ADULTS Version 3.0 Date ratified May 2008 Review date May 2010 Ratified by NUH Antibiotic Guidelines Committee NUH Drugs and Therapeutics
Fecal Microbiota Transplantation in C. diff. colitis Benefits and Limitations
 January 27th 2017, 8th Gastro Foundation Weekend for Fellows; Spier Hotel & Conference Centre, Stellenbosch Fecal Microbiota Transplantation in C. diff. colitis Benefits and Limitations Gerhard Rogler,
January 27th 2017, 8th Gastro Foundation Weekend for Fellows; Spier Hotel & Conference Centre, Stellenbosch Fecal Microbiota Transplantation in C. diff. colitis Benefits and Limitations Gerhard Rogler,
Patient Safety Summit 2014
 Patient Safety Summit 2014 The War on C Diff Mark Mellow, MD + C Diff The Organism Gram + bacillus Anaerobic Spore forming Intestinal flora (up to 35% hospitalized patients, 3% of healthy adults) Leading
Patient Safety Summit 2014 The War on C Diff Mark Mellow, MD + C Diff The Organism Gram + bacillus Anaerobic Spore forming Intestinal flora (up to 35% hospitalized patients, 3% of healthy adults) Leading
Clostridium Difficile Infection: Applying New Treatment Guidelines and Strategies to Reduce Recurrence Rate
 Clostridium Difficile Infection: Applying New Treatment Guidelines and Strategies to Reduce Recurrence Rate Objectives Summarize the changing epidemiology and demographics of patients at risk for Clostridium
Clostridium Difficile Infection: Applying New Treatment Guidelines and Strategies to Reduce Recurrence Rate Objectives Summarize the changing epidemiology and demographics of patients at risk for Clostridium
Probiotics for Primary Prevention of Clostridium difficile Infection
 Probiotics for Primary Prevention of Clostridium difficile Infection Objectives Review risk factors for Clostridium difficile infection (CDI) Describe guideline recommendations for CDI prevention Discuss
Probiotics for Primary Prevention of Clostridium difficile Infection Objectives Review risk factors for Clostridium difficile infection (CDI) Describe guideline recommendations for CDI prevention Discuss
Clostridium difficile
 Clostridium difficile Care Homes IPC Study Day Sue Barber Infection Prevention & Control Lead AV & Chiltern CCG s Clostridium difficile A spore forming Bacterium. Difficult to grow in the laboratory hence
Clostridium difficile Care Homes IPC Study Day Sue Barber Infection Prevention & Control Lead AV & Chiltern CCG s Clostridium difficile A spore forming Bacterium. Difficult to grow in the laboratory hence
Labeled Uses: Treatment of Clostiridum Difficile associated diarrhea (CDAD)
 Brand Name: Dificid Generic Name: fidaxomicin Manufacturer 1,2,3,4,5 : Optimer Pharmaceuticals, Inc. Drug Class 1,2,3,4,5 : Macrolide Antibiotic Uses 1,2,3,4,5 : Labeled Uses: Treatment of Clostiridum
Brand Name: Dificid Generic Name: fidaxomicin Manufacturer 1,2,3,4,5 : Optimer Pharmaceuticals, Inc. Drug Class 1,2,3,4,5 : Macrolide Antibiotic Uses 1,2,3,4,5 : Labeled Uses: Treatment of Clostiridum
Clostridium difficile
 Clostridium difficile Alex Aspinall MD, PhD, FRCPC Clinical Assistant Professor, University of Calgary Division of Gastroenterology and Hepatology, South Health Campus www.seacourses.com 1 Learning Points
Clostridium difficile Alex Aspinall MD, PhD, FRCPC Clinical Assistant Professor, University of Calgary Division of Gastroenterology and Hepatology, South Health Campus www.seacourses.com 1 Learning Points
Clostridium difficile Infection (CDI)
 18.09.10 월요집담회 Clostridium difficile Infection (CDI) R4 송주혜 Clostridium difficile infection (CDI) Anaerobic gram (+), spore-forming, toxin(tcda&tcdb)-producing bacillus Transmitted among humans through
18.09.10 월요집담회 Clostridium difficile Infection (CDI) R4 송주혜 Clostridium difficile infection (CDI) Anaerobic gram (+), spore-forming, toxin(tcda&tcdb)-producing bacillus Transmitted among humans through
SMT19969: A Selective Therapy for C. difficile Infection
 SMT19969: A Selective Therapy for C. difficile Infection One Bug, One Drug 25 th September 2012 SMT19969: A Selective Therapy for CDI SMT19969 is a novel antibiotic for the specific treatment of Clostridium
SMT19969: A Selective Therapy for C. difficile Infection One Bug, One Drug 25 th September 2012 SMT19969: A Selective Therapy for CDI SMT19969 is a novel antibiotic for the specific treatment of Clostridium
Los Angeles County Department of Public Health: Your Partner in CDI Prevention
 Los Angeles County Department of Public Health: Your Partner in CDI Prevention Dawn Terashita, MD, MPH Acute Communicable Disease Control Los Angeles County Department of Public Health dterashita@ph.lacounty.gov
Los Angeles County Department of Public Health: Your Partner in CDI Prevention Dawn Terashita, MD, MPH Acute Communicable Disease Control Los Angeles County Department of Public Health dterashita@ph.lacounty.gov
Fecal Microbiota Transplantation (FMT): Current Concepts in Clostridium difficile and beyond
 Fecal Microbiota Transplantation (FMT): Current Concepts in Clostridium difficile and beyond Amir Patel, MD Assistant Professor of Medicine Froedtert Hospital and the Medical College of Wisconsin I have
Fecal Microbiota Transplantation (FMT): Current Concepts in Clostridium difficile and beyond Amir Patel, MD Assistant Professor of Medicine Froedtert Hospital and the Medical College of Wisconsin I have
Modern approach to Clostridium Difficile Infection
 Modern approach to Clostridium Difficile Infection Pseudomembranous Colitis: Principles for diagnosis and treatment Aggelos Stefos Internist, Infectious diseases Specialist Department of Medicine and Research
Modern approach to Clostridium Difficile Infection Pseudomembranous Colitis: Principles for diagnosis and treatment Aggelos Stefos Internist, Infectious diseases Specialist Department of Medicine and Research
DISCLOSURE Relevant relationships with commercial entities Wyeth (received advisory board & speaker honoraria) Potential for conflicts of interest wit
 GASTROENTERITIS DISCLOSURE Relevant relationships with commercial entities Wyeth (received advisory board & speaker honoraria) Potential for conflicts of interest within this presentation fidaxomicin (which
GASTROENTERITIS DISCLOSURE Relevant relationships with commercial entities Wyeth (received advisory board & speaker honoraria) Potential for conflicts of interest within this presentation fidaxomicin (which
Terapia dell infezione da Clostridium difficile. Massimo Coen I Div Mal Inf AO L Sacco
 Terapia dell infezione da Clostridium difficile Massimo Coen I Div Mal Inf AO L Sacco Disease Severity Mild CDI 3 5 BM/day WBC 15,000/mm 3 Defining CDI Disease Severity Mild abdominal pain due to CDI Moderate
Terapia dell infezione da Clostridium difficile Massimo Coen I Div Mal Inf AO L Sacco Disease Severity Mild CDI 3 5 BM/day WBC 15,000/mm 3 Defining CDI Disease Severity Mild abdominal pain due to CDI Moderate
Lifting the lid on a difficile problem part 2 (Clinical) Evidence Based Practice. Problem in evolution (1) Problem in evolution (1) Interventions (2)
 Lifting the lid on a difficile problem part (Clinical) Dr Philip T Mannion Consultant Microbiologist, Rhyl Evidence Based Practice Antibiotic prescribing guidance Isolation policy Hand hygiene (soap and
Lifting the lid on a difficile problem part (Clinical) Dr Philip T Mannion Consultant Microbiologist, Rhyl Evidence Based Practice Antibiotic prescribing guidance Isolation policy Hand hygiene (soap and
CDI The Impact. Disclosures. Acknowledgments. Objectives and Agenda. What s in the Name? 11/14/2012. Lets Talk Numbers
 Disclosures No conflict of interest to declare Acknowledgments Objectives and Agenda Society for Healthcare Epidemiology of America (SHEA) and the Infectious Diseases Society of America (IDSA) Guidelines
Disclosures No conflict of interest to declare Acknowledgments Objectives and Agenda Society for Healthcare Epidemiology of America (SHEA) and the Infectious Diseases Society of America (IDSA) Guidelines
Corporate Medical Policy Fecal Microbiota Transplantation
 Corporate Medical Policy Fecal Microbiota Transplantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: Fecal_microbiota_transplantation 7/2014 11/2017 11/2018 11/2017 Description
Corporate Medical Policy Fecal Microbiota Transplantation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: Fecal_microbiota_transplantation 7/2014 11/2017 11/2018 11/2017 Description
Fecal transplantation as a treatment option for recurrent Clostridium difficile infection
 Fecal transplantation as a treatment option for recurrent Clostridium difficile infection Josbert Keller Department of Gastroenterology Haga Teaching Hospital, The Hague Case: 81 yrs, CVA, recurrent UTI,
Fecal transplantation as a treatment option for recurrent Clostridium difficile infection Josbert Keller Department of Gastroenterology Haga Teaching Hospital, The Hague Case: 81 yrs, CVA, recurrent UTI,
... Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment.
 Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
Definition Inflammatory disorder of the colon that occurs as a complication of antibiotic treatment. " Epidemiology Humans represent the main reservoir of Clostridium difficile, which is not part of the
GI Bacterial Infections (part-2)
 GI Bacterial Infections (part-2) Mohammed Abdulla Mehdi FIBMS (internal medicine), FIBMS (G&H) Clostridium difficile infection C. difficile is the most commonly diagnosed cause of antibioticassociated
GI Bacterial Infections (part-2) Mohammed Abdulla Mehdi FIBMS (internal medicine), FIBMS (G&H) Clostridium difficile infection C. difficile is the most commonly diagnosed cause of antibioticassociated
Clinical Review Criteria Fecal Microbial Transplant for Treatment of C. Difficile Infection Fecal GI Infusion Fecal Capsule (G3 OpenBiome)
 Clinical Review Criteria Fecal Microbial Transplant for Treatment of C. Difficile Infection Fecal GI Infusion Fecal Capsule (G3 OpenBiome) Criteria Codes Revision History Kaiser Foundation Health Plan
Clinical Review Criteria Fecal Microbial Transplant for Treatment of C. Difficile Infection Fecal GI Infusion Fecal Capsule (G3 OpenBiome) Criteria Codes Revision History Kaiser Foundation Health Plan
Patient presentation
 Update: Clostridium difficile Colitis David H. Kerman, MD Assistant Professor of Clinical Medicine Director, Fellowship Program Division of Gastroenterology University of Miami Miller School of Medicine
Update: Clostridium difficile Colitis David H. Kerman, MD Assistant Professor of Clinical Medicine Director, Fellowship Program Division of Gastroenterology University of Miami Miller School of Medicine
Management of Clostridium Difficile: Total Colectomy versus Colon Sparing Surgery
 Management of Clostridium Difficile: Total Colectomy versus Colon Sparing Surgery Rahul Narang, MD Colon and Rectal Surgery Assistant Professor of Surgery No Disclosure Clostridium Difficile Colitis: Treatments,
Management of Clostridium Difficile: Total Colectomy versus Colon Sparing Surgery Rahul Narang, MD Colon and Rectal Surgery Assistant Professor of Surgery No Disclosure Clostridium Difficile Colitis: Treatments,
Clostridium difficile infection (CDI) Week 52 (Ending 30/12/2017)
 Clostridium difficile infection (CDI) Week 52 (Ending 30/12/2017) What is Clostridium difficile? Clostridium difficile is a Gram-positive anaerobic spore forming bacillus. It is ubiquitous in nature and
Clostridium difficile infection (CDI) Week 52 (Ending 30/12/2017) What is Clostridium difficile? Clostridium difficile is a Gram-positive anaerobic spore forming bacillus. It is ubiquitous in nature and
Atypical Presentation of Clostridium Difficille Infection (CDI).
 Article ID: WMC004648 ISSN 2046-1690 Atypical Presentation of Clostridium Difficille Infection (CDI). Peer review status: No Corresponding Author: Dr. Syed A Gardezi, CT1, Medicine,NevillHall Hospital
Article ID: WMC004648 ISSN 2046-1690 Atypical Presentation of Clostridium Difficille Infection (CDI). Peer review status: No Corresponding Author: Dr. Syed A Gardezi, CT1, Medicine,NevillHall Hospital
FIS 2013, Birmingham
 Fidaxomicin: CDDFT Case Studies Dr Deepa Nayar County Durham and Darlington Foundation Trust FIS 2013, Birmingham This meeting has been initiated and funded by Astellas Pharma Ltd. County Durham and Darlington
Fidaxomicin: CDDFT Case Studies Dr Deepa Nayar County Durham and Darlington Foundation Trust FIS 2013, Birmingham This meeting has been initiated and funded by Astellas Pharma Ltd. County Durham and Darlington
What s New for Clostridium difficile John Lynch MD MPH Harborview Medical Center University of Washington
 What s New for Clostridium difficile 2013 John Lynch MD MPH Harborview Medical Center University of Washington Pathogenic Mechanisms of Diarrhea Toxins: Preformed: S aureus, C perfringens, B cereus Formed
What s New for Clostridium difficile 2013 John Lynch MD MPH Harborview Medical Center University of Washington Pathogenic Mechanisms of Diarrhea Toxins: Preformed: S aureus, C perfringens, B cereus Formed
Learning Goals. Clostridium difficile. Historical Context. Historical Context 6/27/2012
 Learning Goals Clostridium difficile Justin L. Sewell, MD, MPH Assistant Clinical Professor of Medicine University of California San Francisco San Francisco General Hospital Understand the epidemiology,
Learning Goals Clostridium difficile Justin L. Sewell, MD, MPH Assistant Clinical Professor of Medicine University of California San Francisco San Francisco General Hospital Understand the epidemiology,
more intense treatments are needed to get rid of the infection.
 What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
What Is Clostridium Difficile (C. Diff)? Clostridium difficile, or C. diff for short, is an infection from a bacterium that can grow in your intestines and cause bad GI symptoms. The main risk of getting
Star Articles in Review
 Star Articles in Review CDDW/CASL Meeting Toronto, February 10, 2014 Christina M. Surawicz, MD MACG Professor of Medicine Division of Gastroenterology Department of Medicine University of Washington Disclosure
Star Articles in Review CDDW/CASL Meeting Toronto, February 10, 2014 Christina M. Surawicz, MD MACG Professor of Medicine Division of Gastroenterology Department of Medicine University of Washington Disclosure
Clostridium difficile infections: Drug treatment re-evaluated
 Clostridium difficile infections: Drug treatment re-evaluated Kimberly D. Leuthner, PharmD University Medical Center of Southern Nevada August 11, 2016 Random Fact: The human body has 10 13 human cells
Clostridium difficile infections: Drug treatment re-evaluated Kimberly D. Leuthner, PharmD University Medical Center of Southern Nevada August 11, 2016 Random Fact: The human body has 10 13 human cells
Journey to Decreasing Clostridium Difficile and the Unexpected Twist. Jackie Morton, Infection Prevention Cortney Swiggart, Medication Safety Officer
 Journey to Decreasing Clostridium Difficile and the Unexpected Twist Jackie Morton, Infection Prevention Cortney Swiggart, Medication Safety Officer 4/13/2018 Objectives Discuss the organism and clinical
Journey to Decreasing Clostridium Difficile and the Unexpected Twist Jackie Morton, Infection Prevention Cortney Swiggart, Medication Safety Officer 4/13/2018 Objectives Discuss the organism and clinical
Disclosure. Objectives. Assessment Questions. History. Clinical Case 2/27/2015. Clostridium difficile update and new therapies
 Disclosure Clostridium difficile update and new therapies Corey Frederick, PharmD PGY-2 Pharmacy Resident, Infectious Diseases Jackson Memorial Hospital Miami, Florida I do not have a vested interest in
Disclosure Clostridium difficile update and new therapies Corey Frederick, PharmD PGY-2 Pharmacy Resident, Infectious Diseases Jackson Memorial Hospital Miami, Florida I do not have a vested interest in
ACG Clinical Guideline: Diagnosis, Treatment, and Prevention of Clostridium difficile Infections
 ACG Clinical Guideline: Diagnosis, Treatment, and Prevention of Clostridium difficile Infections Christina M. Surawicz, MD 1, Lawrence J. Brandt, MD 2, David G. Binion, MD 3, Ashwin N. Ananthakrishnan,
ACG Clinical Guideline: Diagnosis, Treatment, and Prevention of Clostridium difficile Infections Christina M. Surawicz, MD 1, Lawrence J. Brandt, MD 2, David G. Binion, MD 3, Ashwin N. Ananthakrishnan,
! Macrolide antibacterial. Fidaxomicin (Dificid ) package labeling. Optimer Pharmaceuticals, Inc. May 2011.
 Disclosure! I have no conflicts of interest related to this presentation Nina Naeger Murphy, Pharm.D., BCPS Clinical Pharmacy Specialist Infectious Diseases MetroHealth Medical Center Learning Objectives!
Disclosure! I have no conflicts of interest related to this presentation Nina Naeger Murphy, Pharm.D., BCPS Clinical Pharmacy Specialist Infectious Diseases MetroHealth Medical Center Learning Objectives!
Clostridium difficile Essential information
 Clostridium difficile Essential information Clostridium difficile Origins Clostridium difficile (C. diff) is a Gram positive, spore forming, anaerobic bacterium with a rod structure. It was first identified
Clostridium difficile Essential information Clostridium difficile Origins Clostridium difficile (C. diff) is a Gram positive, spore forming, anaerobic bacterium with a rod structure. It was first identified
Probiotics: Their Role in Medicine Today. Objectives. Probiotics: What Are They? 11/3/2017
 Probiotics: Their Role in Medicine Today Viki Barr Pharm.D., BCPS AQ ID Assistant Professor, Pharmacy Practice Rosalind Franklin University of Medicine and Science Clinical Pharmacist, Infectious Diseases
Probiotics: Their Role in Medicine Today Viki Barr Pharm.D., BCPS AQ ID Assistant Professor, Pharmacy Practice Rosalind Franklin University of Medicine and Science Clinical Pharmacist, Infectious Diseases
HEALTHCARE- ASSOCIATED INFECTIONS: A FOCUS ON Clostridium difficile
 OBJECTIVES HEALTHCARE- ASSOCIATED INFECTIONS: A FOCUS ON Clostridium difficile Identify and describe the pathophysiology of C. diff. Identify and describe current therapies in treatment of C. diff Identify
OBJECTIVES HEALTHCARE- ASSOCIATED INFECTIONS: A FOCUS ON Clostridium difficile Identify and describe the pathophysiology of C. diff. Identify and describe current therapies in treatment of C. diff Identify
500,000 29,000. New 2015 Data. Lessa et al, N Eng J Med 2015: 34.2% of CDI cases were considered community-acquired
 Cost-effective Treatment of Clostridium difficile Infection in the ICU Kevin W. Garey, PharmD, MS. Professor and Chair University of Houston College of Pharmacy New 2015 Data 500,000 29,000 Lessa et al,
Cost-effective Treatment of Clostridium difficile Infection in the ICU Kevin W. Garey, PharmD, MS. Professor and Chair University of Houston College of Pharmacy New 2015 Data 500,000 29,000 Lessa et al,
Long-Term Care Updates
 Long-Term Care Updates April 2017 Bezlotoxumab to Prevent Recurrent Infection By Amy Wilson, PharmD and Zara Risoldi Cochrane, PharmD, MS, FASCP Introduction The Gram-positive bacteria is a common cause
Long-Term Care Updates April 2017 Bezlotoxumab to Prevent Recurrent Infection By Amy Wilson, PharmD and Zara Risoldi Cochrane, PharmD, MS, FASCP Introduction The Gram-positive bacteria is a common cause
Diarrhoea on the AMU. Dr Chris Roseveare
 Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
Diarrhoea on the AMU Dr Chris Roseveare The Society for Acute Medicine, Spring Meeting, Radisson Blu Hotel, Dublin 3-4 May 2012 Acute diarrhoea in developed countries adult populations Mainly a primary
Managing Clostridium Difficile: An Old Bug With
 932 The Red Section see related editorial on page x Managing Clostridium Difficile: An Old Bug With New Tricks Stephen M. Vindigni, MD, MPH 1,2 and Christina M. Surawicz, MD 1 Am J Gastroenterol (2018)
932 The Red Section see related editorial on page x Managing Clostridium Difficile: An Old Bug With New Tricks Stephen M. Vindigni, MD, MPH 1,2 and Christina M. Surawicz, MD 1 Am J Gastroenterol (2018)
Updates to pharmacological management in the prevention of recurrent Clostridium difficile
 Updates to pharmacological management in the prevention of recurrent Clostridium difficile Julia Shlensky, PharmD PGY2 Internal Medicine Resident September 12, 2017 2017 MFMER slide-1 Clinical Impact Increasing
Updates to pharmacological management in the prevention of recurrent Clostridium difficile Julia Shlensky, PharmD PGY2 Internal Medicine Resident September 12, 2017 2017 MFMER slide-1 Clinical Impact Increasing
Incidence of and risk factors for communityassociated Clostridium difficile infection
 University of Iowa Iowa Research Online Theses and Dissertations 2010 Incidence of and risk factors for communityassociated Clostridium difficile infection Jennifer Lee Kuntz University of Iowa Copyright
University of Iowa Iowa Research Online Theses and Dissertations 2010 Incidence of and risk factors for communityassociated Clostridium difficile infection Jennifer Lee Kuntz University of Iowa Copyright
Xifaxan. Xifaxan (rifaximin) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.34 Subject: Xifaxan Page: 1 of 6 Last Review Date: December 8, 2017 Xifaxan Description Xifaxan (rifaximin)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.34 Subject: Xifaxan Page: 1 of 6 Last Review Date: December 8, 2017 Xifaxan Description Xifaxan (rifaximin)
Clostridium Difficile colitismore
 Clostridium Difficile colitismore virulent than ever ECHO- February 18, 2016 Charles Krasner, M.D. UNR School of Medicine Sierra NV Veterans Affairs Hospital Growing problem of pseudomembranous colitis
Clostridium Difficile colitismore virulent than ever ECHO- February 18, 2016 Charles Krasner, M.D. UNR School of Medicine Sierra NV Veterans Affairs Hospital Growing problem of pseudomembranous colitis
Fecal Microbiota Transplantation
 Protocol Fecal Microbiota Transplantation (20192) Medical Benefit Effective Date: 10/01/14 Next Review Date: 07/18 Preauthorization Yes Review Dates: 07/14, 07/15, 07/16, 07/17 Preauthorization is required.
Protocol Fecal Microbiota Transplantation (20192) Medical Benefit Effective Date: 10/01/14 Next Review Date: 07/18 Preauthorization Yes Review Dates: 07/14, 07/15, 07/16, 07/17 Preauthorization is required.
C. difficile: The Changing Epidemiology Evaluations Clostridium difficile Thank You to our Sponsors
 C. difficile: The Changing Epidemiology Ghinwa Dumyati, MD University of Rochester Monroe County Department of Public Health Thank You to our Sponsors Evaluations School of Public Health, University at
C. difficile: The Changing Epidemiology Ghinwa Dumyati, MD University of Rochester Monroe County Department of Public Health Thank You to our Sponsors Evaluations School of Public Health, University at
All POOPed out: fecal microbiota transplant in C. difficile
 All POOPed out: fecal microbiota transplant in C. difficile SUSAN M. KELLIE, MD, MPH PROFESSOR OF INTERNAL MEDICINE DIVISION OF INFECTIOUS DISEASES UNIVERSITY OF NEW MEXICO SCHOOL OF MEDICINE HOSPITAL
All POOPed out: fecal microbiota transplant in C. difficile SUSAN M. KELLIE, MD, MPH PROFESSOR OF INTERNAL MEDICINE DIVISION OF INFECTIOUS DISEASES UNIVERSITY OF NEW MEXICO SCHOOL OF MEDICINE HOSPITAL
Fecal microbiota transplantation: Breaking the chain of recurrent C. difficile infection
 Fecal microbiota transplantation: Breaking the chain of recurrent C. difficile infection Issue Date: June 2013 Vol. 8 No. 6 Author: Amy Marinski, MSN, RN, CCRN, CNL More than 3 million new cases of Clostridium
Fecal microbiota transplantation: Breaking the chain of recurrent C. difficile infection Issue Date: June 2013 Vol. 8 No. 6 Author: Amy Marinski, MSN, RN, CCRN, CNL More than 3 million new cases of Clostridium
Duodenal infusion of donor feces for recurrent Clostridium difficile infection A French experience
 Duodenal infusion of donor feces for recurrent Clostridium difficile infection A French experience Benoit Guery Unité des Maladies Infectieuses CHRU - Faculté de Médecine Lille Conflicts of interest Conferences,
Duodenal infusion of donor feces for recurrent Clostridium difficile infection A French experience Benoit Guery Unité des Maladies Infectieuses CHRU - Faculté de Médecine Lille Conflicts of interest Conferences,
JMSCR Vol 05 Issue 07 Page July 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i7.15 Rapid Diagnosis of Toxigenic Clostridium
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i7.15 Rapid Diagnosis of Toxigenic Clostridium
Treatment Update on Fecal Microbiota Transplantation. Arnab Ray, MD Ochsner Clinic Foundation Gastroenterology Department
 Treatment Update on Fecal Microbiota Transplantation Arnab Ray, MD Ochsner Clinic Foundation Gastroenterology Department Disclosure I serve as a paid medical monitor for Rebiotix Objectives The scope of
Treatment Update on Fecal Microbiota Transplantation Arnab Ray, MD Ochsner Clinic Foundation Gastroenterology Department Disclosure I serve as a paid medical monitor for Rebiotix Objectives The scope of
ADJUVANT TIGECYCLINE FOR SEVERE CLOSTRIDIUM DIFFICILE-ASSOCIATED DIARRHEA
 ADJUVANT TIGECYCLINE FOR SEVERE CLOSTRIDIUM DIFFICILE-ASSOCIATED DIARRHEA Candace Marr, DO Catholic Health System University at Buffalo, NY Kevin Shiley, MD Catholic Health System Buffalo, NY FINANCIAL
ADJUVANT TIGECYCLINE FOR SEVERE CLOSTRIDIUM DIFFICILE-ASSOCIATED DIARRHEA Candace Marr, DO Catholic Health System University at Buffalo, NY Kevin Shiley, MD Catholic Health System Buffalo, NY FINANCIAL
C. difficile Infection: How it all comes out
 C. difficile Infection: How it all comes out Larry Danziger, Pharm.D. Professor of Pharmacy and Medicine College of Pharmacy University of Illinois at Chicago The speaker has no conflicts to disclose.
C. difficile Infection: How it all comes out Larry Danziger, Pharm.D. Professor of Pharmacy and Medicine College of Pharmacy University of Illinois at Chicago The speaker has no conflicts to disclose.
Nicola Petrosillo Istituto Nazionale per le Malattie Infettive Lazzaro Spallanzani, IRCCS Roma. L infezione da C difficile grave o complicata
 Nicola Petrosillo Istituto Nazionale per le Malattie Infettive Lazzaro Spallanzani, IRCCS Roma L infezione da C difficile grave o complicata Bagdasarian N et al. JAMA 2015; 313: 398-408 European Society
Nicola Petrosillo Istituto Nazionale per le Malattie Infettive Lazzaro Spallanzani, IRCCS Roma L infezione da C difficile grave o complicata Bagdasarian N et al. JAMA 2015; 313: 398-408 European Society
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
L infezione da Clostridium difficile (CDI) Quadri clinici e nuovi approcci terapeutici
 L infezione da Clostridium difficile (CDI) Quadri clinici e nuovi approcci terapeutici Roberto Luzzati SC Malattie Infettive, AOU Trieste Presidente :Prof. Enzo Raise Clinical presentation of infection
L infezione da Clostridium difficile (CDI) Quadri clinici e nuovi approcci terapeutici Roberto Luzzati SC Malattie Infettive, AOU Trieste Presidente :Prof. Enzo Raise Clinical presentation of infection
Treatment of Clostridium Difficile Infection in Community Teaching Hospital: A Retrospective Study
 International Journal of Infectious Diseases and Therapy 2018; 3(3): 52-61 http://www.sciencepublishinggroup.com/j/ijidt doi: 10.11648/j.ijidt.20180303.12 ISSN: 2578-9651 (Print); ISSN: 2578-966X (Online)
International Journal of Infectious Diseases and Therapy 2018; 3(3): 52-61 http://www.sciencepublishinggroup.com/j/ijidt doi: 10.11648/j.ijidt.20180303.12 ISSN: 2578-9651 (Print); ISSN: 2578-966X (Online)
New approaches to treating Clostridium difficile Infection
 7:45 8:45 am New Approaches to Treating C. difficile Infection SPEAKER Fred A. Lopez, MD, MACP Presenter Disclosure Information The following relationships exist related to this presentation: Fred A. Lopez,
7:45 8:45 am New Approaches to Treating C. difficile Infection SPEAKER Fred A. Lopez, MD, MACP Presenter Disclosure Information The following relationships exist related to this presentation: Fred A. Lopez,
Clostridium difficile Infection (CDI) Guideline
 Clostridium difficile Infection (CDI) Guideline Site Applicability All VCH PHC acute care and residential sites. Practice Level Physicians basic skill Pharmacists basic skill Nurses (RN, LPN, RPN) basic
Clostridium difficile Infection (CDI) Guideline Site Applicability All VCH PHC acute care and residential sites. Practice Level Physicians basic skill Pharmacists basic skill Nurses (RN, LPN, RPN) basic
When To Do Fecal Microbiota Transplant (FMT) For C. difficile
 When To Do Fecal Microbiota Transplant (FMT) For C. difficile Lawrence J. Brandt, MD, MACG Emeritus Chief, Gastroenterology Montefiore Medical Center Professor of Medicine and Surgery Albert Einstein College
When To Do Fecal Microbiota Transplant (FMT) For C. difficile Lawrence J. Brandt, MD, MACG Emeritus Chief, Gastroenterology Montefiore Medical Center Professor of Medicine and Surgery Albert Einstein College
Sherwood L. Gorbach, MD Professor of Public Health, Medicine, and Microbiology Tufts University School of Medicine
 Sherwood L. Gorbach, MD Professor of Public Health, Medicine, and Microbiology Tufts University School of Medicine Chief Scientific Officer, Optimer Pharmaceuticals, Inc. Conflicts: Chief Scientific Officer,
Sherwood L. Gorbach, MD Professor of Public Health, Medicine, and Microbiology Tufts University School of Medicine Chief Scientific Officer, Optimer Pharmaceuticals, Inc. Conflicts: Chief Scientific Officer,
Revisiting Clostridium Difficile Infection
 CLINICAL VIGNETTE Revisiting Clostridium Difficile Infection Michael A. Pfeffer, M.D., Ruby Shandilya, M.D., and Jeffrey Hsu, M.Eng. Clostridium difficile infection is commonly seen in patients in the
CLINICAL VIGNETTE Revisiting Clostridium Difficile Infection Michael A. Pfeffer, M.D., Ruby Shandilya, M.D., and Jeffrey Hsu, M.Eng. Clostridium difficile infection is commonly seen in patients in the
8/29/2016 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW. LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES
 DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
DIVERTICULAR DISEASE: WHAT EVERY NURSE PRACTITIONER SHOULD KNOW LENORE LAMANNA Ed.D, ANP-C LEARNING OBJECTIVES Define Diverticular Disease Discuss Epidemiology and Pathophysiology of Diverticular disease
Antibiotic Associated Diarrhea (AAD) and Clostridium Difficile Infection (CDI)
 Antibiotic Associated Diarrhea (AAD) and Clostridium Difficile Infection (CDI) Dario Conte, M.D. Gastroenterology and Endoscopy Unit Postgraduate School of Gastroenterology Fondazione IRCCS Ca Granda Ospedale
Antibiotic Associated Diarrhea (AAD) and Clostridium Difficile Infection (CDI) Dario Conte, M.D. Gastroenterology and Endoscopy Unit Postgraduate School of Gastroenterology Fondazione IRCCS Ca Granda Ospedale
The incubation period is unknown. However; the onset of clinical disease is typically 5-10 days after initiation of antimicrobial treatment.
 C. DIFFICILE Case definition CONFIRMED CASE A patient is defined as a case if they are one year of age or older AND have one of the following requirements: A laboratory confirmation of a positive toxin
C. DIFFICILE Case definition CONFIRMED CASE A patient is defined as a case if they are one year of age or older AND have one of the following requirements: A laboratory confirmation of a positive toxin
Long-Term Care Updates
 Long-Term Care Updates April 2018 By Austin Smith, PharmD Candidate and Lindsay Slowiczek, PharmD is the most common healthcare-acquired infection (HAI) in the United States. 1,2 A 2014 prevalence survey
Long-Term Care Updates April 2018 By Austin Smith, PharmD Candidate and Lindsay Slowiczek, PharmD is the most common healthcare-acquired infection (HAI) in the United States. 1,2 A 2014 prevalence survey
New approaches to treating
 9:45 10:45am New Approaches to Treating C Difficile Infection SPEAKER Kalpana Gupta, MD, MPH Presenter Disclosure Information The following relationships exist related to this presentation: Kalpana Gupta,
9:45 10:45am New Approaches to Treating C Difficile Infection SPEAKER Kalpana Gupta, MD, MPH Presenter Disclosure Information The following relationships exist related to this presentation: Kalpana Gupta,
Updates in Fecal Microbial Transplant
 Updates in Fecal Microbial Transplant Dina Kao, MD FRCPC Associate Professor, Gastroenterology University of Alberta Nikhil Pai, MD FAAP FRCPC Assistant Professor, Ped Gastroenterology McMaster University
Updates in Fecal Microbial Transplant Dina Kao, MD FRCPC Associate Professor, Gastroenterology University of Alberta Nikhil Pai, MD FAAP FRCPC Assistant Professor, Ped Gastroenterology McMaster University
Pennington Feb 19, 2015
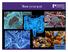 Trust your gut Pennington Feb 19, 2015 Crohn s Disease -an autoimmune disorder that causes inflammation of the intestinal tract along with unpredictable, often incapacitating episodes of abdominal pain
Trust your gut Pennington Feb 19, 2015 Crohn s Disease -an autoimmune disorder that causes inflammation of the intestinal tract along with unpredictable, often incapacitating episodes of abdominal pain
OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA
 OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP and Cleveland
OMED 17 OCTOBER 7-10 PHILADELPHIA, PENNSYLVANIA 29.5 Category 1-A CME credits anticipated ACOFP / AOA s 122 nd Annual Osteopathic Medical Conference & Exposition Joint Session with ACOFP and Cleveland
Management of the Hospitalized IBD Patient. Drew DuPont MD
 Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Management of the Hospitalized IBD Patient Drew DuPont MD Ulcerative Colitis: Indications for Admission Severe ulcerative colitis Frequent loose bloody stools ( 6 per day) Severe cramps Systemic toxicity:
Presenter Disclosure Information
 10:45 11:45am New Approaches to Treating C. Difficile Infection SPEAKER Kalpana Gupta, MD, MPH Presenter Disclosure Information The following relationships exist related to this presentation: Kalpana Gupta,
10:45 11:45am New Approaches to Treating C. Difficile Infection SPEAKER Kalpana Gupta, MD, MPH Presenter Disclosure Information The following relationships exist related to this presentation: Kalpana Gupta,
