Dysphagia and the MBSS: Disclosures. Instrumental Assessment. The Disorder Guides the Treatment
|
|
|
- Baldwin McDaniel
- 5 years ago
- Views:
Transcription
1 Dysphagia and the MBSS: The Disorder Guides the Treatment Jennifer Jones, PhD, CCC-SLP, BCS-S C/NDT Board Certified Specialist in Swallowing and Swallowing Disorders Certified in Neurodevelopmental Treatment Disclosures My name is Jennifer Jones and I am here to discuss Interpreting the MBSS. I have authored a book As They Grow: Birth To Six, which is in it s 2 nd edition and sold by Talk Tools. I receive royalty when my books are sold by Talk Tools. However, I will be discussing only a minimal amount of information that is presented in that book. I lecture nationally for Talk Tools on the topic of Interpreting the MBSS for Adults and Pediatrics. I do receive financial compensation for those lectures. I am being compensated for my travel expenses by Talk Tools to lecture here today. I have no other financial disclosures. Instrumental Assessment First you must be able to determine what is truly a normal swallow across the age span as viewed on the instrumental assessment 1
2 Normal swallowing includes an integrated interdependent group of complex feeding behaviors emerging from interacting cranial nerves of the brainstem and governed by neural regulatory mechanisms in the medulla, as well as in sensorimotor and limbic cortical systems. (Groher, 1997) Normal and Elderly Prevalence of swallowing impairment increases with age Longer oral and pharyngeal transit times Longer duration of pharyngeal pressures Higher incidences of pharyngeal residue after the swallow Changes in the activity patterns of the suprahyoid muscles (Robbins, Hamilton, Lof, & Kempster, 1992; Nilsson, Ekberg, Olsson, & Hindfeldt, 1996) (Miyaoka et al., 2007) Normal and Elderly Eat less Sense of smell & taste Aguesia / Anosmia absence of taste /smell Hypoguesia / Hyposmia diminished taste / smell Dysguesia / Dysosmia distorted taste / smell (1/3 of elderly report dissatisfaction with taste / smell) Large decrease (~1200 cal.) between years old Eat slower 2
3 Instrumental Assessment MBSS is the most frequently performed instrumental assessment because it permits the determination of: Underlying physiologic or anatomic reasons for the dysphagia Analysis of bolus flow Direction, duration and clearance Bolus response to treatment trials How do we watch an MBSS? Watch the bolus? Watch the structures? What are we looking for? How do we know to stop the study? 3
4 Before the Swallow is Initiated Examine the anatomy for any abnormalities Cervical vertebrae & esophagus are there any bulges Valleculae is the epiglottis there? Tongue base is there a tongue? Airway entrance, larynx, trachea Dentition Velum, tongue, mandible, lips, VP port, hyoid, pharynx, PES, pyriform sinuses, PPW Watch for any movement disorders Normal Swallow As the swallow is initiated Watch the bolus movement Does the bolus move consistently or hesitate? If so, where? How long? Count the delay. Where is the bolus head when the pharyngeal swallow is triggered? Count the delay. Does any bolus enter the airway before, during or after the swallow? 4
5 Physiology and Coordination Labial closure Mandibular motion & mastication efficiency Onset of lingual bolus propulsion Lingual Range of motion & control during: Elevation of bolus to palate Bolus seal against palate A-P (anterior-posterior) propulsion of the bolus Oral Phase Timing Physiology and Coordination Tongue base retraction Velopharyngeal closure soft palate Epiglottic Inversion Initiation of the Pharyngeal Swallow & bolus location relative to timing Pharyngeal constriction stripping wave Laryngeal protection: supraglottic & glottic level Hyolaryngeal motion anterior excursion & elevation Physiology and Coordination Pharyngeal Phase Timing Pharyngo-esophageal opening Coordination of pharyngeal structural movement during swallow Presence or absence of upper airway and/or aerodigestive tract obstruction Movement of bolus through upper 1/3 of esophagus and esophageal clearance 5
6 After the Swallow Residue in the Oral Cavity poor oral tongue movement Residue in Valleculae Reduced tongue base retraction Unilateral pharyngeal paralysis Residue in Pyriform Reduced laryngeal elevation Reduced cricopharygneal opening (PES) Reduced hyolaryngeal excursion Residue on Posterior Pharyngeal Wall (PPW) Reduced pharyngeal wall contraction forward and lateral What You Should Know To treat Dysphagia it is VERY important to know when the aspiration occurred and why it occurred. If you don t have this information then you can NOT adequately treat the patient. When Is the Aspiration? 1. Before 2. During 3. After 6
7 Planning Treatment Remember, not all dysphagia patients have the same problem Therefore, you cannot treat them all the same Review your history Put the pieces of the puzzle together to determine the disorders Make your treatment plan based on the problems the patient is having, NOT only their Medical Diagnosis Goal of Feeding Program Acute medical status MUST be stable Swallowing evaluation must demonstrate: an adequate protective and productive cough reflex and laryngeal elevation during a swallow Be sure if you say NO to NG or G-tube that the patient is receiving adequate oral intake to meet nutritional requirements (consult dietician) Always recommend an oral care program for the patient before & after meal if possible Treatment Techniques Compensatory Treatment (Indirect) circumvents problem using indirect strategies to alter bolus flow Postures, Sensory procedures, Maneuvers, Combine postures and maneuvers, Diet changes Rehabilitative Treatment (Direct) Changing the swallowing physiology to restore fxn and directed at improving neuromuscular control Visual feedback, auditory feedback, sensory therapies, physiotherapeutic exercises (ROM & resistive) (Logemann, 1997; Sate of Colorado Dept of Labor and Employment, 2006) 7
8 Indirect Treatment Strategies 1. Postures 2. Maneuvers 3. Bolus Modifications 4. Sensory Enhancement 5. Other compensatory techniques 6. Diet changes See handout for maneuver/posture summary! Postures 1. Chin down / tuck 2. Head back 3. Head tilt 4. Head rotated / turned 5. Combinations Results: Narrows oropharynx Widens valleculae space Displaces tongue base & epiglottis posteriorly Reduces laryngohyoid distance But, may weaken pharyngeal contraction Chin Down 8
9 Chin Down Indication: improve airway protection Use with a patient who has: Reduced laryngeal vestibule closure Reduced laryngeal closure Reduced tongue base movement Delayed trigger of pharyngeal swallow (Logemann, 1993, Logemann et al., 1994, Rasley et al., 1993, Shanahan et al., 1993) Contraindicated for: neurogenic patients with pharyngeal constrictor weakness pharyngeal delay pyriform pooling cervical spine injuries Chin Down Head back / Chin up Indication: Propel bolus to back of mouth or pharynx Use with a patient who has: Poor anterior-posterior propulsion of the bolus Reduced oral tongue strength Abnormal labial strength / closure Reduced velopharyngeal closure (Logemann, 1998) 9
10 Results: Better oral transport Head back / Chin up Contraindicated for: Patients with poor airway protection Head Tilt Tilt the head to the stronger side by placing the ear over his shoulder Indicated for: Unilateral oral and/or pharyngeal disorder to channel bolus through stronger side of oral cavity and/or pharynx (Logemann, 1998) Head Rotated / Turned Turn head to right/left (weakened side) shoulder while swallowing Indication: reduce post swallow residue and aspiration to close off weaker side of pharynx Use with a patient who has: Unilateral pharyngeal paresis / weakness Unilateral laryngeal weakness Post-radio therapy Reduced CP opening (Logemann et al., 1989, Logemann, 1998, Logemann et al., 1994) 10
11 Results: Isolates damaged side from bolus path redirects bolus to stronger side of pharynx Reduces UES pressure increases opening Increases proportion of bolus swallowed Contraindications: Bilateral pharyngeal paresis Head Rotated / Turned Combinations Chin down and then chin up Reduced oral control Reduced tongue vertical or lateral range of motion Head turn and chin down at the same time Use for best airway protection for patient with reduced laryngeal closure at entrance or cords Airway Protection Maneuvers Requirements: Ability to learn cognition intact Motivation Praxis Respiratory reserve 11
12 Maneuvers 1. Supraglottic 2. Super Supraglottic 3. Mendelsohn 4. Effortful Supraglottic Swallow Inhale, exhale slightly, valve glottis, swallow, clear pharynx, swallow again For Super add bear down / squeeze with swallow Indications: Pharyngeal delay Unilateral pharyngeal wall disorder Bilateral pharyngeal wall disorder Other populations: Head & neck irradiated patients Medullary stroke patients Others with pharyngeal dysfunction Supraglottic Swallow Indications & rationale: Promote earlier airway closure Promote increased subglottal air pressure Improve efficiency of cough Clear residual hypopharyngeal pooling Minimize aspiration before, during and after the swallow Intended to: Reduce aspiration by increasing glottal closure (Logemann et al., 1995; Bisch et al., 1994) 12
13 Supraglottic & Super Supraglottic Contraindications: Vocal fold paralysis = can t hold breath Restrictive lung disease = voluntary breath hold restricted Hx of cardiac arrhythmia or coronary artery disease What procedure tells the patient to: Place your finger on your voice box and feel it rise and fall as you swallow your saliva. This time when you swallow and feel it move up, try to hold it up and not let it fall back down. Hold it up for a count of about three. A.) Supraglottic Swallow B.) Double Swallow C.) Mendelsohn D.) Masako Maneuver Mendelsohn Indicated for: Reduced laryngeal elevation Reduced CP opening Discoordinated swallow Intended to: Improve swallowing coordination Increase UES opening width & duration Increase tongue base retraction Increase laryngeal elevation by increasing hyoid movement Increase anterior laryngeal excursion (Lazarus, Logemann, & Gibbons, 1993; Logemann & Kahrilas, 1990; Kahrilas et al., 1991) 13
14 Effortful Swallow The patient is asked to swallow harder What does that mean? Better description: as you swallow, squeeze hard with all of your muscles and push your tongue into the roof of your mouth. Indicated for: Reduced tongue base retraction Generation of higher intra-oral pressure Reduce valleculae residue Effortful Swallow Physiological changes: Increased tongue-palate pressures Increased duration of swallow Increased tongue base movement Studies show: Increased pressure exerted on the palate and tongue base Increase in tongue base movement Depth of airway penetration decreased Decreased residue (Logemann, 1993; Lazarus et al., 2002; Pouderoux & Kahrilas, 1995) Combine Postures and Maneuvers Supraglottic chin down, head rotated or both Super Supraglottic chin down or head rotated Effortful chin down Mendelsohn head rotated 14
15 Sensory Procedures Other ways to change the swallow: Bolus volume and viscosity Taste, texture and temperature changes To facilitate lingual motion To improve triggering of the pharyngeal swallow Change Bolus Volume Decrease the amount of intake Respiratory issues Poor bolus control Increase the amount of intake Decreased sensation in oral cavity change onset & duration of swallow by changing the bolus larger bolus moves faster increase bolus size = decrease pharyngeal transit times (Bisch et al., 1994; Lazarus et al., 1993; Logemann et al., 1995) Differences with Large Bolus 1. Anterior position of the velum 2. Widening of the PES 3. Increased closure time of the airway Therefore, large bolus would definitely be contraindicated for people with respiratory issues. (e.g. COPD) 15
16 Change of Bolus Viscosity Viscosity levels Thin, nectar, syrup, honey, pudding Up to 28% of residents in long term care receive thickened liquids Cost is $200 / month to drink (Castellanos, 2004) USDA Funded Project Components of taste Sweet, sour, bitter, salty, umami Change of Flavor May want to add materials to existing foods to increase the taste (e.g. spices) A lot of taste manipulation actually involves smell manipulation 16
17 Carbonation / Thin Liquids For patients with mild aspiration or bolus control issues Use carbonated beverages without thickener Reduces swallow time Therefore, reduces the misdirection and poor coordination of the bolus (Bülow, Olsson, & Ekberg, 2003) Other Sensory Procedures Pressure of spoon May trigger response Self-feeding Oral-preparatory assistance Chewing Stimulates saliva and swallow reflex Absence of chewing may also help Enhances taste!! Bolus Hold Double or multiple swallows Alternate liquids & solids Throat clearing Other Techniques 17
18 Pt. is asked to hold the bolus in the mouth until asked to swallow Intra-Oral Bolus Hold This technique teaches oral containment and control, while heightening sensory input of feeling the bolus Good procedure to use with a delayed pharyngeal swallow Double Swallow Simply ask the patient to swallow two times for every bolus taken into the oral cavity Good to use with a patient who has pharyngeal residue Direct Treatment Methods Visual Feedback VFSS Videofluoroscopic Swallow Study FEES Fiberoptic Endoscopic Eval of Swallowing Biofeedback IOPI Madison Oral Strengthening Therapeutic Most Device 18
19 Iowa Oral Performance Instrument (IOPI) hand-held, portable, battery-operated instrument that can accurately measure tongue strength and the relative fatigability useful for diagnostic and therapeutic purposes Madison Oral Strengthening Therapeutic Device Developed by JoAnne Robbins, PhD, Univ of Wisconsin and the VA in Madison She has pioneered research on tongue strengthening exercises - first with the IOPI MOST Device - now developing her own product that is undergoing a lot of research at this time. Direct Treatment Methods Auditory Feedback Cervical Auscultation Sensory Stimulation Thermal application Bolus positioning Electrical Stimulation 19
20 Cervical Auscultation What can we learn about swallow by listening? Easier to recognize sound than describe it Adds to the clinical examination Ongoing monitoring/feedback device Screening tool The Method Use cold mirrors, ice sticks, or lemon glycerin swabs Rub pillars and sides of tongue vigorously Have pt. swallow hard w/ or w/o a bolus All above constitutes one trial Time between trials individualized as is number of stimulations per trial Thermal Application Thermal-Tactile Stimulation Indicated for: Delayed initiation of pharyngeal swallow also no swallow response Mostly use with slowness and aspiration slowness = delay greater than 2 seconds But not always, As we age we need more time to adapt physiologically Therefore, slower swallows may sometimes be safer (Lazzara, Lazarus, & Logemann, 1986; Rosenbek, Roecker, Wood & Robbins, 1996) 20
21 Bolus Positioning Place the bolus on the unimpaired side of the mouth instead of midline The bolus will tend to go to the weak side if it is placed at midline This placement should help facilitate proper movement of the bolus to the pharyngeal area Electrical Stimulation Must have an intact nerve You set up electrodes around the nerve and the current between the electrodes stimulates the nerve Difficult to do because the sensory nerves are closer to the skin than the motor nerves Most muscles that we want to stimulate are very deep and questioned if electrical stimulation will even effect those muscles Electrical Stimulation Protocol the placement of surface electrodes on the neck using one of four different positions, as described by the developers of the technique (Wijting & Freed, 2003). The electrodes are simultaneously activated over the submental and laryngeal regions. The intensity level of the current is increased until the patient reports feeling a sensation of muscles grabbing. This is referred to as reaching motor levels of stimulation. The electrical current remains on, cycling off for 1 second every minute throughout 1 hour of therapy. Meanwhile, the patient is encouraged to repeatedly swallow hard using endogenous saliva. With progress, the patient is upgraded to swallowing ice chips and eventually solid foods. 21
22 Direct Treatment Strategies Exercises Shaker Masako Specific muscles targeted These are designed to give the patient more information to facilitate learning maneuvers These are performed WITHOUT FOOD Suprahyoid Exercises - Shaker Patient is asked to lay on your back and raise your head to look at your shoes, do not raise your shoulders. Intended to: Improve PES opening, anterior laryngeal excursion and reduce backflow aspiration Works to strengthen: Mylohyoid, geniohyoid and anterior belly of digastric Pharyngeal Wall Exercise - Masako Also known as the Tongue holding maneuver Patient is asked to hold tongue between the teeth while swallowing Intended to: Increase contact between tongue base and pharyngeal wall Physiological Effects: Increased anterior movement of posterior pharyngeal wall 22
23 Physiotherapeutic Approaches Muscles of the mouth, suprahyoid and pharyngeal are striated muscles and they need resistive exercise Resistive exercise = strengthening the muscles Range of motion = mobility You should have ROM and resistance exercises for every muscle group that is affected Labial musculature Mandible Intrinsic & extrinsic lingual musculature Suprahyoid muscles Yawning Gargling Masako Pulling tongue back Tongue base exercises Muscle Specific Exercises Lingual (straws, horns, z-vibe) Labial (button pull, tongue dep., straws, horns) Mandible (jaw exerciser, bite blocks, bite tubes) Sara will have a book published soon on Adult Oral Placement Therapy 23
24 Decision Making Process 1. The first step in deciding the disorder: SIGNS AND SYMPTOMS These are obtained with a good: a. history b. clinical examination Decision Making Process 2. Now establish or hypothesize if the signs and symptoms are related to: the swallowing structure (s), to other variables such as poor dentition, vision loss, cognitive impairment, lapses in attention, fatigue, etc. 3. If a sign or symptom seems to be related to abnormality within the swallowing anatomy then establish or hypothesize what structure (s) are involved. Decision Making Process 4. Establish whether the structure itself is involved as in Zenker s, fibrosis, tumor, surgical wound, etc. or whether movement of the structures are impaired or if both are occurring in combination. 5. Establish why the structure(s) or movement(s) are involved. 24
25 Decision Making Process Two possible variables: 1. movement variables: range, rate, timing 2. control variables: strength, tone, coordination Decision Making Process 6. Establish the treatment targets based on: interaction of the various signs (e.g. residual in the pyriform sinuses spills over after the swallow and is aspirated) impact on safety & adequacy pleasure of nutrition and hydration (QOL) Decision Making Process 7. Next, decide if the target (s) and its variables (movement or control) are modifiable YES: then the next step is to pick a method or set of methods (e.g. lingual weakness modifiable with IOPI or other strengthening methodology) NO: (or if effects can be expected to take some time) then the full range of compensations need to be considered. 25
26 Decision Making Process 8. Finally, decide: the intensity and duration of treatment the expected outcomes Neurogenic Mechanical Developmental Categories of Dysphagia See page in resources for examples Neurogenic Dysphagia Swallowing dysfunction due to movement & control variables Due to neurologic disease or insult Results in impaired motor and sensory functions of the oral and pharyngeal phases 26
27 Neurogenic Difficulties - Oral Abnormal oral containment Out of the lips Over the base of the tongue Abnormal / difficult mastication Abnormal / difficult bolus formation Abnormal A-P propulsion of bolus Saliva production (amount & sensation of) Abnormal lingual strength and movement Oral residual (anterior & lateral sulcus, palate, tongue) Neurogenic Difficulties - Pharyngeal Abnormal / Poor tongue base retraction Abnormal / Poor laryngeal elevation NP regurgitation Ineffective airway protection Ineffective airway clearance Abnormal / Poor pharyngeal contraction Diminished displacement of the hyoid bone and/or epiglottis Abnormal opening of the P-E segment Delay triggering the pharyngeal swallow Mechanical Dysphagia Due to muscle loss and loss of the motor and sensory innervations to those muscles. Muscles to perform acts are not intact Results in impaired motor and sensory functions of the oropharyngeal mechanism (similar to neurogenic dysphagia) Most mechanical dysphagia patients have had oral, pharyngeal, laryngeal, or esophageal structures removed or reconstructed during surgery for cancer. 27
28 Mechanical Difficulties - Oral Poor oral containment (anterior & posterior) Abnormal / Difficult mastication Abnormal / Difficult initiation of the swallow Abnormal Saliva production (amount & sensation) Abnormal / Decreased lingual strength Mechanical Difficulties - Pharyngeal Abnormal / decreased laryngeal elevation Abnormal opening of the P-E segment Abnormal / Decreased pharyngeal contraction Increased swallow transit times Ineffective closure to laryngeal vestibule Ineffective closure of the vocal folds 28
29 Complications Dehydration Malnutrition Aspiration pneumonia Asphyxia Loss of pleasurable eating Social difficulties Developmental Dysphagia Central nervous system injuries associated with: Infection Anoxia Trauma Vascular accident Hydrocephalus Mental retardation Cerebral palsy Cranial nerve palsy Muscular disorders (e.g. Myasth. Gravis) Variations May let the patient feed themselves May allow the patient to determine the size of the bolus to see what size they are commonly using May use different types of spoons, cups or straws May alternate liquids & solids 29
30 Effectiveness of Intervention Fatigue Patient motivation Patient alertness, judgment, & distractibility Level of cueing and assistance necessary to perform techniques Ability to repeatedly & consistently perform techniques Language and cultural influences Possible Adverse Reactions Agitation Changes in breathing pattern Changes in level of alertness Changes in color Nausea and vomiting Changes in overall medical status MBSS Report Should Explain Problems by occurrence Sensory vs. motor Symptoms: residue, penetration, aspiration Physiologic / anatomic causes of symptoms Effects of therapy strategies or why therapy not needed / attempted during the study Recommended feeding strategies Recommended therapy procedures & goals 30
31 Description of the Swallow If swallows of all consistencies exhibit the same disorders, this can be indicated at the beginning of the report If the disorders vary by food consistency, the report sequence should be repeated for each food consistency Compensatory Strategies If no effect is seen a simple sentence can be used, such as Postural techniques and supraglottic swallow were unsuccessful in eliminating aspiration. Compensatory Strategies If techniques are successful, the conditions under which the patient can eat successfully should be defined, for ex. With the chin down and head rotated to the left, aspiration is eliminated on all volumes and food consistencies. Recommend eating orally only with the chin down and head rotated. Using the Mendelsohn maneuver, laryngeal movement and cricopharyngeal opening are improved enough so that a spoonful of thin liquid can be given orally in therapy only. 31
32 Recommended Therapy Depends on the nature of the swallowing motility disorders & the underlying cause of the patient s swallowing disorder Tx strategies should focus on the purpose of the therapy, for ex: To improve laryngeal elevation, closure at the airway entrance, or triggering of the pharyngeal swallow Recommend Re-evaluation Depends on the: patient s medical diagnosis, anticipated rate of recovery Prognosis For the neurologic patient in the process of recovery 3-4 weeks is appropriate For a patient w/ a degenerative neurologic condition 3-6 months is adequate unless swallowing worsens Recommend Re-evaluation Typical statement for recommendation of reevaluation Re-evaluation is suggested when clinical improvement is seen. Or Re-evaluation is suggested when swallow degeneration is suggested by... 32
33 Recommendations Oral vs. Non-oral delivery Specific oral intake modifications Therapeutic interventions required during meals Safe feeding / aspiration precautions Positioning Diet consistent with ethnocultural preferences and practices Need for thorough & consistent oral hygiene Dysphagia Treatment Plan consistent with exam findings Other consultations or assessments Identify & Interpret Penetration: cause, timing, & approx. % / severity Aspiration: cause, timing, & approx. % / severity Residue: cause, approx. % and location Sensory Awareness: Reaction to residue Reaction to penetration Reaction to aspiration (e.g. cough, throat clear) Effectiveness of Reaction to: Residue, penetration, aspiration (e.g. reduction of % residue, productive cough, & expectoration of material from airway) Aspiration: Before the Swallow Limited / Uncoordinated Lingual Movement Limited Mandibular Movement Delayed or absent swallow Poor Pharyngeal Motility 33
34 Aspiration: During the Swallow Reduced laryngeal elevation Inefficient / absent closure of laryngeal vestibule (vocal cords) Decreased anterior movement of the hyoid bone Decreased closure of true or false cords Aspiration: After the Swallow Residue in the oral cavity poor oral tongue movement Residue in valleculae Reduced tongue base retraction Unilateral pharyngeal paralysis Residue in pyriform Reduced laryngeal elevation Reduced CP opening Reduced hyolaryngeal excursion Residue on PPW Reduced pharyngeal wall contraction forward and lateral Jennifer Jones PhD, CCC-SLP, BCS-S, C/NDT Board Certified Specialist in Swallowing and Swallowing Disorders Certified in Neurodevelopmental Treatment TalkTools 1852 Wallace School Road, Suite H Charleston, SC Tel: info@talktools.com 34
Daniels SK & Huckabee ML (2008). Dysphagia Following Stroke. Muscles of Deglutition. Lateral & Mesial Premotor Area 6. Primary Sensory
 An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
An Overview of Dysphagia in the Stroke Population Stephanie K. Daniels, PhD Michael E. DeBakey VA Medical Center PM & R, Baylor College of Medicine Communication Sciences and Disorders, University of Houston
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Strategies
 Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
Department of Head and Neck Surgery Section of Speech Pathology & Audiology M.D. Anderson Cancer Center (713) 792-6525 Swallowing Strategies 1) POSTURAL CHANGES: a) Chin Tuck: (1) Delayed onset pharyngeal
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
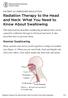 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Feeding and Oral Hygiene: How to Address the Challenges
 Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Feeding and Oral Hygiene: How to Address the Challenges Paige W. Roberts, OTR/L Occupational Therapist Pediatric Feeding Disorders Program Marcus Autism Center Disclaimer: This content is for personal
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing
 PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
PATIENT & CAREGIVER EDUCATION Radiation Therapy to the Head and Neck: What You Need to Know About Swallowing This information describes swallowing problems that can be caused by radiation therapy to the
Main Aspects of the Management of Neurogenic Dysphagia
 Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Main Aspects of the Management of Neurogenic Dysphagia Mario Prosiegel/München German Society of Neurology (DGN) prosiegel@t-online.de DYSPHAGIA October 8-10, 2015 Pavia, Italy Overview Diagnosis Causal
Surgical Effects on Swallowing DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Surgical Effects on Swallowing
 Susan Langmore, PhD, CCC-SLP, BRS-S Professor, BUMC, BU September 27, 2010 DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Incidence of dysphagia after XRT VA study (Wolf; Terrell
Susan Langmore, PhD, CCC-SLP, BRS-S Professor, BUMC, BU September 27, 2010 DYSPHAGIA AFTER TREATMENT FOR HNC: WHAT CAUSES IT? WHAT TREATMENT WORKS? Incidence of dysphagia after XRT VA study (Wolf; Terrell
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Management of oropharyngeal dysphagia
 Management of oropharyngeal dysphagia Course Objectives Know the normal anatomy of swallowing Know the normal physiology of swallowing Enumerate different etiologies of oropharyngeal dysphagia Be able
Management of oropharyngeal dysphagia Course Objectives Know the normal anatomy of swallowing Know the normal physiology of swallowing Enumerate different etiologies of oropharyngeal dysphagia Be able
Swallowing after a Total Laryngectomy
 Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing after a Total Laryngectomy Diane Longnecker, M.S.,CCC-SLP, BCS-S Baylor Institute for Rehabilitation at Baylor University Medical Center Dallas, TX Disclosure Statement No relevant financial
Swallowing Course (RHS )
 Swallowing Course (RHS ) Dr/Mohamed Farahat Ibrahim, M.D., Ph.D. Professor, Consultant Phoniatrician (Communication and Swallowing Disorders) Chairman, Communication and Swallowing Disorders Unit (CSDU)
Swallowing Course (RHS ) Dr/Mohamed Farahat Ibrahim, M.D., Ph.D. Professor, Consultant Phoniatrician (Communication and Swallowing Disorders) Chairman, Communication and Swallowing Disorders Unit (CSDU)
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
Dysphagia Treatment: What are We Doing, and Why?
 Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
Dysphagia Treatment: What are We Doing, and Why? ASHA Convention, 2014; Orlando James L. Coyle, Ph.D., CCC SLP, BCS S University of Pittsburgh jcoyle@pitt.edu 1 Treatment 2 Aims, targets and ingredients
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS
 SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring Patricia Bednarik, MS, CCC-SLP, MSCS
 Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Page 1 MS Learn Online Feature Presentation Swallowing Difficulties in Multiple Sclerosis Featuring, MS, CCC-SLP, MSCS >>Kate Milliken: Welcome to MS Learn Online. I am Kate Milliken. Swallowing is something
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Clinical Swallowing Exam
 Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Clinical Evaluation Template 1 Clinical Exam Name: ID/Medical record number: Date of exam: Referred by: Reason for referral: Medical diagnosis: Date of onset of diagnosis: Other relevant medical history/diagnoses/surgery
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA
 TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Safe swallowing strategies
 Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Learning Guide Safe swallowing strategies 27468 Apply safe swallowing strategies in a health or wellbeing setting Level 3 5 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved.
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
Swallowing disorder, aspiration: now what?
 Swallowing disorder, aspiration: now what? Poster No.: C-0691 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Kavka, M. Kysilko, M. Rocek; Prague/CZ Keywords: Swallowing disorders, Dynamic swallowing
Swallowing disorder, aspiration: now what? Poster No.: C-0691 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Kavka, M. Kysilko, M. Rocek; Prague/CZ Keywords: Swallowing disorders, Dynamic swallowing
Workbook. Apply safe swallowing strategies as a health assistant in an aged care, health or disability context. US Level 4 Credits 4. Name...
 Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
Workbook Apply safe swallowing strategies as a health assistant in an aged care, health or disability context US 27468 Level 4 Credits 4 Name... US 27468 Level 4 Credits 4 All rights reserved. Careerforce
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION. Brenda Sitzmann, MA, CCC-SLP (816)
 FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
FLOOVIDEOFLUOROSCOPIC SWALLOW STUDIES: LOOKING BEYOND ASPIRATION Brenda Sitzmann, MA, CCC-SLP bksitzmann@cmh.edu (816) 302-8037 DISCLOSURES Ms. Sitzmann is speech-language pathologist at Children s Mercy
SWALLOWING: HOW CAN WE HELP
 SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
SWALLOWING: HOW CAN WE HELP Carol Romero-Clark, M.S., CCC-SLP University of New Mexico Hospital Speech Pathology Department November 10, 2017 What happens when you swallow? Mouth (Oral Phase) Your tongue
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation David A. Muir Course Outline Physiology of Swallow
 Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Managing the Patient with Dysphagia
 Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
State of Art & Science for Evaluation of Infants & Children with Signs/Symptoms of Dysphagia. Introduction. Instrumental Swallow Evaluations
 Problem Solving with Instrumental Swallow Evaluations & Management 49 th Annual Mid-South Conference, Feb. 21, 2019 Joan C. Arvedson, PhD, CCC-SLP, BCS-S, ASHA Honors & Fellow jcarved@aol.com & jarvedson@chw.org
Problem Solving with Instrumental Swallow Evaluations & Management 49 th Annual Mid-South Conference, Feb. 21, 2019 Joan C. Arvedson, PhD, CCC-SLP, BCS-S, ASHA Honors & Fellow jcarved@aol.com & jarvedson@chw.org
Dysphagia as a Geriatric Syndrome Assessment and Treatment. Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit
 Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
Dysphagia as a Geriatric Syndrome Assessment and Treatment Ashton Galyen M.A., CCC-SLP St. Vincent Indianapolis Acute Rehabilitation Unit March 16, 2018 Ashton Galyen, M.A., CCC-SLP Master s degree in
Normal and Abnormal Oral and Pharyngeal Swallow. Complications.
 ESPEN Congress Gothenburg 2011 Assessment and treatment of dysphagia What is the evidence? Normal and Abnormal Oral and Pharyngeal Swallow. Complications. Pere Clavé Educational Session. Assessment and
ESPEN Congress Gothenburg 2011 Assessment and treatment of dysphagia What is the evidence? Normal and Abnormal Oral and Pharyngeal Swallow. Complications. Pere Clavé Educational Session. Assessment and
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
Effects of a Sour Bolus on Oropharyngeal Swallowing Measures in Patients With Neurogenic Dysphagia
 Journal of Speech and Hearing Research, Volume 38, 556-563, June 1995 Effects of a Sour Bolus on Oropharyngeal Swallowing Measures in Patients With Neurogenic Dysphagia Jeri A. Logemann Barbara Roa Pauloski
Journal of Speech and Hearing Research, Volume 38, 556-563, June 1995 Effects of a Sour Bolus on Oropharyngeal Swallowing Measures in Patients With Neurogenic Dysphagia Jeri A. Logemann Barbara Roa Pauloski
When Swallowing Becomes Impossible
 University of Tennessee, Knoxville Trace: Tennessee Research and Creative Exchange University of Tennessee Honors Thesis Projects University of Tennessee Honors Program 5-2011 When Swallowing Becomes Impossible
University of Tennessee, Knoxville Trace: Tennessee Research and Creative Exchange University of Tennessee Honors Thesis Projects University of Tennessee Honors Program 5-2011 When Swallowing Becomes Impossible
Analyzing Swallow Studies in Pediatrics
 Analyzing Swallow Studies in Pediatrics About the Speaker Robert Beecher, M.S., CCC-SLP was formerly senior speech-language pahologist at the Children's Hospital of Wisconsin in Milwaukee. He is specialized
Analyzing Swallow Studies in Pediatrics About the Speaker Robert Beecher, M.S., CCC-SLP was formerly senior speech-language pahologist at the Children's Hospital of Wisconsin in Milwaukee. He is specialized
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE
 EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
EATING SAFELY AND TALKING ABOUT IT KIERA N BERGGREN, MA/CCC-SLP, MS 2018 FSHD CONNECT CONFERENCE DISCLOSURES I have no personal financial relationships with commercial interests relevant to this presentation
Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease
 Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease Alexandra E. Brandimore, Ph.D. CCC/SLP MESPA Conference April 13, 2019 No conflicts of interest or disclosure
Airway Protection: Clinical Management of Dysphagia and Dystussia in Neurodegenerative disease Alexandra E. Brandimore, Ph.D. CCC/SLP MESPA Conference April 13, 2019 No conflicts of interest or disclosure
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
SESSION 2: THE MOUTH AND PHARYNX
 SESSION 2: THE MOUTH AND PHARYNX 9 In the pig s digestive tract, food flows in only one direction from mouth to anus.this allows for greatly specialized sections that can act independently of each other.
SESSION 2: THE MOUTH AND PHARYNX 9 In the pig s digestive tract, food flows in only one direction from mouth to anus.this allows for greatly specialized sections that can act independently of each other.
Anatomy of the Airway
 Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
Anatomy of the Airway Nagelhout, 5 th edition, Chapter 26 Morgan & Mikhail, 5 th edition, Chapter 23 Mary Karlet, CRNA, PhD Airway Anatomy The airway consists of the nose, pharynx, larynx, trachea, and
ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION.
 ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Moving Tongues Beyond Frenectomy Grace Sun, DDS FAACD MALD MAGD MICOI Los Angeles ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Accredited Fellow, American Academy
ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Moving Tongues Beyond Frenectomy Grace Sun, DDS FAACD MALD MAGD MICOI Los Angeles ALD 2015 KNOWLEDGE EXPERIENCE APPLICATION Accredited Fellow, American Academy
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
HOMES AND SENIORS SERVICES. APPROVAL DATE: August 1985 REVISION DATE: January 2015 REVIEW DATE: May 2018
 POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
POLICY: Page 1 of 10 Residents who experience signs and symptoms associated with dysphagia will have their nutrition and hydration needs met in a safe, coordinated manner as managed by the interdisciplinary
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP
 DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016
 Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Assessing the Eating Needs of Personal Care Services (PCS) Beneficiaries Effective 12/1/2016 The Freedom to Succeed November 22,2016 Content Introduction Signs and Symptoms Caring for Individuals with
Pharyngeal Effects of Bolus Volume, Viscosity, and Temperature in Patients With Dysphagia Resulting From Neurologic Impairment and in Normal Subjects
 Journal of Speech and Hearing Research, Volume 37, 1041-1049, October 1994 Pharyngeal Effects of Bolus Volume, Viscosity, and Temperature in Patients With Dysphagia Resulting From Neurologic Impairment
Journal of Speech and Hearing Research, Volume 37, 1041-1049, October 1994 Pharyngeal Effects of Bolus Volume, Viscosity, and Temperature in Patients With Dysphagia Resulting From Neurologic Impairment
POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN
 POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN WHAT IS POST POLIO SYNDROME (PPS)? Post-polio syndrome (PPS) is a condition that affects polio survivors years after recovery
POST POLIO SYNDROME (PPS) AND ITS EFFECTS ON SWALLOWING BY: LINDSAY JORDAN WHAT IS POST POLIO SYNDROME (PPS)? Post-polio syndrome (PPS) is a condition that affects polio survivors years after recovery
Long Term Toxicities of Head & Neck Cancer Therapies. Faith Mutale Abramson Cancer Center University of Pennsylvania
 Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
Long Term Toxicities of Head & Neck Cancer Therapies Faith Mutale Abramson Cancer Center University of Pennsylvania Head & Neck Cancer 2-3% of all cancers 1-2% of all cancer deaths Incidence includes:
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
«Einschluckstörungen»
 18. Fortbildungskurs der SGG Brunnen 20.04.2018 «Einschluckstörungen» Troubles de la déglutition Swallowing disorders Dr Valérie Schweizer Unité de Phoniatrie Service ORL et chirurgie cervicofaciale CHUV
18. Fortbildungskurs der SGG Brunnen 20.04.2018 «Einschluckstörungen» Troubles de la déglutition Swallowing disorders Dr Valérie Schweizer Unité de Phoniatrie Service ORL et chirurgie cervicofaciale CHUV
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Management of dysphagia in MS
 Management of dysphagia in MS Marta Renom Speech and Language Therapist CEM-CAT (UNeR) Barcelona INTRODUCTION Normal swallowing Dual function: transporting / protecting airway oral phase pharyngeal phase
Management of dysphagia in MS Marta Renom Speech and Language Therapist CEM-CAT (UNeR) Barcelona INTRODUCTION Normal swallowing Dual function: transporting / protecting airway oral phase pharyngeal phase
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Cover Page The handle http://hdl.handle.net/1887/32744 holds various files of this Leiden University dissertation Author: Heemskerk, Anne-Wil Title: Dysphagia in Huntington s disease Issue Date: 2015-04-15
Swallow-respiratory coordination. Liza Bergström, Leg. logoped.
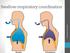 Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
copyrighted material by PRO-ED, Inc.
 CONTENTS Preface xi Chapter 1 Introduction: Definitions and Basic Principles of Evaluation and Treatment of Swallowing Disorders Signs and Symptoms of Dysphagia Screening: Identifying the Patient at High
CONTENTS Preface xi Chapter 1 Introduction: Definitions and Basic Principles of Evaluation and Treatment of Swallowing Disorders Signs and Symptoms of Dysphagia Screening: Identifying the Patient at High
B. Correct! As air travels through the nasal cavities, it is warmed and humidified.
 Human Anatomy - Problem Drill 20: The Respiratory System Question No. 1 of 10 1. Which of the following statements about the portion of the respiratory system labeled in the image below is correct? Question
Human Anatomy - Problem Drill 20: The Respiratory System Question No. 1 of 10 1. Which of the following statements about the portion of the respiratory system labeled in the image below is correct? Question
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
How Speech and Swallowing are Affected with ALS
 Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
Patient Education How Speech and Swallowing are Affected with ALS This handout describes how ALS affects speech and swallowing. For speech issues it covers tips for listeners and speakers and what can
Dysphagia. A Problem Swallowing Foods or Liquids
 Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy
 Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS. Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis
 DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
ESSD. EUGMS-ESSD Working Group on Oropharyngeal Dysphagia. 9 th Congress of the European Union Geriatric Medicine Society (EUGMS)
 ESSD EUGMS-ESSD Working Group on Oropharyngeal Dysphagia 9 th Congress of the European Union Geriatric Medicine Society (EUGMS) ESSD European Society for Swallowing Disorders (ESSD). ESSD Mission. The
ESSD EUGMS-ESSD Working Group on Oropharyngeal Dysphagia 9 th Congress of the European Union Geriatric Medicine Society (EUGMS) ESSD European Society for Swallowing Disorders (ESSD). ESSD Mission. The
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Speech and Swallowing in KD: Soup to Nuts. Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland
 Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Speech and Swallowing in KD: Soup to Nuts Neil C. Porter, M.D. Assistant Professor of Neurology University of Maryland Disclosures I will not be speaking on off-label use of medications I have no relevant
Subdivided into Vestibule & Oral cavity proper
 Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Laryngoscopy Examinations
 Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Laryngoscopy Examinations Laryngoscopy is a visual examination of the back of the throat where the voice box (larynx) and vocal cords are located. The procedure is done by using hand mirrors and a light
Using an Inhaler and Nebulizer
 Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Using an Inhaler and Nebulizer Introduction An inhaler is a handheld device that is used to deliver medication directly to your airways. A nebulizer is an electric or battery powered machine that turns
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Introduction to Standard Esophageal Speech. Texas Laryngectomy Association 2018
 Introduction to Standard Esophageal Speech Texas Laryngectomy Association 2018 Disclosure Objectives At the end of this presentation the participant will be able to: Describe the production of standard
Introduction to Standard Esophageal Speech Texas Laryngectomy Association 2018 Disclosure Objectives At the end of this presentation the participant will be able to: Describe the production of standard
If You Have Head or Neck Cancer
 EASY READING If You Have Head or Neck Cancer What is head and neck cancer? Cancer can start any place in the body. Cancer that starts in the head and neck can have many names. It depends on where the cancer
EASY READING If You Have Head or Neck Cancer What is head and neck cancer? Cancer can start any place in the body. Cancer that starts in the head and neck can have many names. It depends on where the cancer
TECHNICAL SKILLS COMPETENCY
 TECHNICAL SKILLS COMPETENCY Date Education Plan Knowledge Competencies 1. Demonstrates Understanding of rationale for performing FEES a) Identifies indications & contraindications for the procedure, MBS
TECHNICAL SKILLS COMPETENCY Date Education Plan Knowledge Competencies 1. Demonstrates Understanding of rationale for performing FEES a) Identifies indications & contraindications for the procedure, MBS
What are the Challenges? Spreading the Word in NICU. Need for NICU Care: Impact. Baby Trachs: Use of the Passy Muir Valve in the NICU to
 What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
Deciphering Dysphagia with E-Stim 8 March 2015
 Deciphering Dysphagia with E-Stim 8 March 2015 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Sponsored by: HEMAX Health Products Company Limited New Options
Deciphering Dysphagia with E-Stim 8 March 2015 Electrical Stimulation for Muscle Re-education in Swallowing Presented by: Russ Campbell, PT Sponsored by: HEMAX Health Products Company Limited New Options
IVOR LEWIS Esophagogastrectomy
 IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
Respiratory Swallow Coordination in Healthy Individuals
 Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010
 Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Dysphagia Diagnostic Procedures
 The Role of Lingual Pressures In Dysphagia Screening Andrew Kaufman, BS Jackie Hind, MS Georgia Malandraki, PhD JoAnne Robbins, PhD American Speech Language Hearing Association Annual Meeting New Orleans,
The Role of Lingual Pressures In Dysphagia Screening Andrew Kaufman, BS Jackie Hind, MS Georgia Malandraki, PhD JoAnne Robbins, PhD American Speech Language Hearing Association Annual Meeting New Orleans,
Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10
 GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
Effect of posture on swallowing.
 Effect of posture on swallowing. Ahmad H. Alghadir, Hamayun Zafar, Einas S. Al-Eisa, Zaheen A. Iqbal Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, KSA.
Effect of posture on swallowing. Ahmad H. Alghadir, Hamayun Zafar, Einas S. Al-Eisa, Zaheen A. Iqbal Rehabilitation Research Chair, College of Applied Medical Sciences, King Saud University, Riyadh, KSA.
Dysphagia Identification and Management
 Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Dysphagia Identification and Management Presented By Speech-Language Pathologist Developmental Disabilities Administration DC Department on Disability Services Training Objectives After this training session
Temporal and Biomechanical Measurements of Upper Esophageal Sphincter (UES) Opening in Normal Swallowing
 Temporal and Biomechanical Measurements of Upper Esophageal Sphincter (UES) Opening in Normal Swallowing Youngsun Kim School of Hearing, Speech and Language Sciences, College of Health and Human Services,
Temporal and Biomechanical Measurements of Upper Esophageal Sphincter (UES) Opening in Normal Swallowing Youngsun Kim School of Hearing, Speech and Language Sciences, College of Health and Human Services,
Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper. Oral vestibule : is slit like space between.
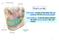 Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Exercise- Based Approaches to Dysphagia Rehabilitation
 Interventions Cichero J, Clavé P (eds): Stepping Stones to Living Well with Dysphagia. Nestlé Nutr Inst Workshop Ser, vol 72, pp 109 117, Nestec Ltd., Vevey/S. Karger AG., Basel, 2012 Exercise- Based Approaches
Interventions Cichero J, Clavé P (eds): Stepping Stones to Living Well with Dysphagia. Nestlé Nutr Inst Workshop Ser, vol 72, pp 109 117, Nestec Ltd., Vevey/S. Karger AG., Basel, 2012 Exercise- Based Approaches
Acknowledgements. To my family and good friends who have cheered me on to the finish.
 THE VALIDITY OF A THREE-PART CRITERIA FOR DIFFERENTIATING BETWEEN DELAYED PHARYNGEAL SWALLOW AND PREMATURE SPILLAGE SECONDARY TO POOR ORO-LINGUAL CONTROL ON VIDEOFLUOROSCOPY A thesis completed in partial
THE VALIDITY OF A THREE-PART CRITERIA FOR DIFFERENTIATING BETWEEN DELAYED PHARYNGEAL SWALLOW AND PREMATURE SPILLAGE SECONDARY TO POOR ORO-LINGUAL CONTROL ON VIDEOFLUOROSCOPY A thesis completed in partial
Standardisation of Videofluoroscopy: Where is it taking us?
 Standardisation of Videofluoroscopy: Where is it taking us? Jodi Allen, Senior Speech and Language Therapist, The National Hospital for Neurology and Neurosurgery If somebody asked you. What do you start
Standardisation of Videofluoroscopy: Where is it taking us? Jodi Allen, Senior Speech and Language Therapist, The National Hospital for Neurology and Neurosurgery If somebody asked you. What do you start
Asma Karameh. -Shatha Al-Jaberi محمد خطاطبة -
 -2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
-2 Asma Karameh -Shatha Al-Jaberi محمد خطاطبة - 1 P a g e Gastrointestinal motilities Chewing: once you introduce the first bolus to the mouth you started what we call chewing reflex appears by muscle
Dysphagia after Stroke. Wendy Busby Stroke Service Dunedin Hospital
 Dysphagia after Stroke Wendy Busby Stroke Service Dunedin Hospital Incidence IN NEW ZEALAND 9,5000 new stroke per year Rate is decreasing More people surviving Major cause of disability in adults Prevalence
Dysphagia after Stroke Wendy Busby Stroke Service Dunedin Hospital Incidence IN NEW ZEALAND 9,5000 new stroke per year Rate is decreasing More people surviving Major cause of disability in adults Prevalence
