Interval cancers in BreastScreen Aotearoa
|
|
|
- Cecilia Mason
- 5 years ago
- Views:
Transcription
1 in BreastScreen Aotearoa Richard Taylor Madeleine Wall Stephen Morrell Independent Monitoring Group School of Public Health and Community Medicine University of New South Wales for BreastScreen Aotearoa June
2 EXECUTIVE SUMMARY Introduction breast are diagnosed after a mammographic screen with a normal result but before the next scheduled screen. This report presents information on 2-year interval breast from the BreastScreen Aotearoa (BSA) mammographic screening programme for , and comparisons with a previous report (for ) and published results from other services. Methods Identification of interval breast was carried out through the matching of BreastScreen Aotearoa data with New Zealand Cancer Registry (NZCR) data using the National Health Index (NHI) numbers of women screened by BSA from 1 January 1999 to 31 December cancer rates are calculated as the number of detected within 12, and 0-24 months following negative screens. breast cancer rates per 10,000 women screened were calculated for 45 49, 50 54, 55 59, 60 64, and 65 years. Programme sensitivity is defined as the number of screen-detected expressed as a proportion of total cancer incidence (screen detected plus interval ) in women screened. Confidence intervals (95%) are provided. Results. For , 678 interval occurred in the first year following a negative mammogram, an interval cancer rate of 6.3 per 10,000 screens; 1,346 interval were detected in the second year following a negative mammogram, an interval cancer rate of 12.6 per 10,000 screens. The trend in <12 month interval declined from 7.3 in 1999 to ~6 per 10,000 screens in For month and all interval the secular trend showed a sharper decline from 1999 to 2002, and plateaued thereafter. cancer rates are in line with comparable screening programmes internationally. For <12 month interval, none of the BSA Lead Providers differed significantly from the NZ BSA programme overall; for and 0-24 month interval, BSC had significantly lower interval cancer rates. Programme sensitivity. 4,979 breast were detected by screening from 1,074,959 screens during Programme sensitivity for <12 month interval was 88%, and 79% for month interval which is in line with comparable screening programmes internationally. No Lead Provider differed significantly from NZ overall with regard to <12 month interval. BSC had significantly higher programme sensitivity for month interval from initial and subsequent screens, and for 0-24 months for subsequent and all screens. Conclusion BSA has achieved comparable interval cancer rates and programme sensitivity as comparable international programmes and there are minimal differences between Lead Providers, especially for the <12 months intervals which can reflect missed. 2
3 1. INTRODUCTION breast are diagnosed after a mammographic screen with a normal result but before the next scheduled screen. Consistently low interval cancer rates correlate with significant reductions in breast cancer mortality in screened populations 1 ; consequently interval cancer rates are used as a key indicator of the effectiveness of screening programmes. breast can be classified by diagnosis: after the initial (prevalent) or a subsequent (incident) screen; in the first or subsequent year after a normal mammogram; by age and period (both indexed to the date of the screen). In some studies interval breast have been categorised by characteristics of the mammographic process: missed (present but not recognised at a screen), occult (mammographically invisible) and true (those that developed to become mammographically visible after a screen). The distribution of in these categories is reported to be about 30% missed, 10% occult and 60% true, 1-3 although the proportion of these vary with screening interval and method of mammogram review. BreastScreen Aotearoa Providers regularly categorise interval in this way for radiologists quality improvement and to provide objective information to women with interval. Stratification of interval breast by occurrence in the first or second year after a normal mammogram is important. Those that occur in the first year are more likely to be missed by the mammographic process, whereas those that occur in the second or subsequent year are more likely to be true interval. This must be qualified by the rate at which the cancer progresses from incidence to clinical indication, which in the case of cancer of the breast is known to vary with age: breast in the elderly progress at much slower rates than those in younger women, largely due to hormonal influences. 1 Stratification of interval breast by age at screen thus is also important. Rates of interval in the first year after a normal mammogram are likely to decrease with increasing age, whereas in subsequent years after a normal mammogram the reverse is more likely. The purpose of this report is to present information on 2-year interval breast from the BreastScreen Aotearoa (BSA) mammographic screening programme for , and to compare this with a previous BSA interval cancer report (for ) and published results from other services. 2. METHODS 2.1 Screening The study population consists of women who attended for mammography screening at BSA during BSA has offered government funded biennial mammography screening for all New Zealand (NZ) women aged years since 1999, and for women aged between 45 and 69 years since mid Women who attend for screening undergo bilateral two-view mammography and all films are read independently by two radiologists. If agreement cannot be reached concerning a recommendation of either routine re-screen or recall for assessment, a 3
4 final recommendation is made based on either a consensus opinion of two or more radiologists, or the recommendation of a third radiologist, or both. 2.2 The definition of primary cancer of the breast used for this report includes invasive cancer, and excludes ductal carcinoma in situ (DCIS), lobular carcinoma in situ (LCIS) and Paget s disease of the nipple without an underlying invasive breast cancer (Table 1). are defined as cases of primary breast cancer diagnosed up to 24 months after a normal screening mammogram, or after an abnormal screening mammogram and a normal assessment by a BreastScreen Aotearoa provider. This definition includes invasive diagnosed at early review (that is, at a repeat assessment 6 months or more after an equivocal assessment visit). Table 1. Case definition for invasive breast cancer Histopathology High-grade DCIS with or without necrosis Invasive cribriform Invasive duct not otherwise specified Invasive lobular classical Invasive lobular variant Invasive medullary Invasive mucinous Invasive tubular Lobular carcinoma in situ LCIS Mixed Invasive ductal/lobular Non-high grade DCIS with necrosis Non-high grade DCIS without necrosis Other DCIS Other primary invasive malignancy Included No Yes Yes Yes Yes Yes Yes Yes No Yes No No No Yes 2.3 Matching of BSA and NZCR data Identification of interval breast was carried out through the matching of BreastScreen Aotearoa data with New Zealand Cancer Registry (NZCR) data. The National Screening Unit (NSU) provided NZ Ministry of Health Analytical Services an extract containing National Health Index (NHI) numbers of women who were screened by BSA from 1 January 1999 to 31 December The NHI number is a unique 7-character identification number assigned to a healthcare user by the NHI database. NHI numbers uniquely identify healthcare users, and allow linking between 4
5 different data collections. The master NHI of each BSA-screened woman was matched by NZ Ministry of Health Analytical Services against the master NHI of all breast cancer registrations from the NZ Cancer Registry. Following a positive match, Analytical Services then appended breast cancer registration data to the matched NHI. This data was returned to NSU and loaded into a database. The number of months between the screen and diagnosis date was calculated and added to the database. All that were detected outside of 25 months were automatically excluded later in the matching process and those diagnosed between 24 and 25 months after the index screen were manually checked then excluded. Histopathology codes were mapped to DCIS, LCIS or Invasive morphological types. In the data set returned by Analytical Services, BSA-detected were identified and removed excluding those diagnosed by BSA on extended assessment (early review). Cancers detected after 31 December 2009 were also removed. All fields from the Cancer Registry that were sent as alpha or numerical codes were mapped to the appropriate descriptions and loaded into the database. Date-of-birth mismatches between the NSU BSA database and the NZCR data were identified and flagged in the database. Details of verified interval previously identified by NZCR and BSA Lead Providers were also matched and entered in to the database. A list of women with provisional interval was created under the guidance of the Clinical Advisor. The Clinical Advisor then manually reviewed each record and excluded duplicated records, and data entry and matching errors. The remaining list, complete with all variables, was sent to the appropriate BSA Lead Providers. BSA Lead Providers were asked to check the data contained in their spreadsheet against their own records and enter the following where required: (a) the final diagnosis for each screening record; (b) agree or disagree that a record was an interval cancer according to the rules in an accompanying BSA interval cancer definitions sheet; (c) provide reasons why a record was not an interval; and (d) the correct date of birth where there was a date-of-birth mismatch. BSA Lead Providers were also able to send the NSU details of interval that were not recorded by the NZCR. The returned spreadsheets were then reviewed by the Clinical Advisor against the following definitions and either included or excluded as interval : Inclusions: Women who were diagnosed with cancer up to 24 months after a normal BSA screen or normal BSA assessment. Cancers in women placed on extended assessment (early recall), where the diagnosis by the BSA programme was delayed 6 months or more after an assessment recommendation (16 women). 5
6 Women with multiple synchronous or metachronous interval, had only the cancer with the highest modified Nottingham Prognostic Index included (41 cases). Exclusions: Local recurrence or regional or systemic metastases from a previously treated cancer (4 women). Cancers diagnosed outside the programme, after a correct recommendation by BSA for assessment. These included: 12 women who refused to return to BSA for assessment and 49 women who opted for private rather than BSA assessment. Cancers diagnosed as Paget s disease of the nipple without evidence of an underlying intra-mammary carcinoma (1 case). Cancers from a non-breast primary metastatic to the breast (e.g. secondary lymphoma). Cancers on the Cancer Registry diagnosed from cytology only with no recorded follow-up malignant histology. 15 cases were identified, of which 10 had subsequent benign surgical open biopsy of the purported malignant lesion performed by BSA providers. Cancers on the Cancer Registry diagnosed by clinical examination alone with no histology (4 cases identified). Cancers notified to the Cancer Registry from death certificate only with no definitive primary. Cancer metastases from an unknown primary with indeterminate histology (13 women). Because of inconsistent reporting and ascertainment of symptoms, the presence or absence of symptoms was not used as a criterion to determine whether a cancer diagnosed either within or outside the BSA programme was an interval cancer. The BSA Lead Providers forwarded details of 62 additional that were not already on the Lead Provider interval spreadsheets. 3 of these had been diagnosed overseas and were therefore not on the NZCR. In order to maintain consistency with the NZCR, these were not included as interval. 7 were additional interval and are included in the report 10 of the additional were recurrences of previously treated and were excluded 15 were diagnosed more than 24 months after the index screen 1 cancer was in a woman screened after December 2007 and will be included in the next interval cancer report. 26 reported by the BSA Lead Providers had no pathology information to allow accurate categorisation. Although these were excluded from the current analysis, the National Screening Unit is seeking further information to ensure improved accuracy of future interval cancer reports and to inform the Cancer Registry. The interval cancer dataset was sent in a secure file to the BSA Independent Monitoring Group for analysis and reporting. 6
7 Table 2. Exclusions from interval cancer Reason Excluded Number Recurrence 4 Cancer diagnosed months after normal screen 62 Cancer diagnosed >25 months after normal screen 18 Recalled by BSA but cancer diagnosed outside BSA 49 Recalled by BSA but refused assessment 12 Diagnosed by BSA but cancer diagnosis not recorded 14 Incorrect index screening date 3 Incorrect NHI 9 Paget s disease of the nipple 1 No (or indeterminate) histology Cancer Rates cancer rates are calculated as the number of detected within 12, and 0-24 months following negative screens. As numbers of screen-detected are known, the denominators for interval are calculated as the number of screens minus the number of detected through screening in a given screening year, age group or area. Numbers of screen-detected make little difference to estimates if all screens are used instead as the denominator. In this report, interval are reported as rates per 10,000 women screened but are calculated as above, and thus women screened in this case is shorthand for women with a normal screen. breast cancer rates per 10,000 women screened were calculated for the following age groups at the time of screening: 45 49, 50 54, 55 59, 60 64, and 65 years. cancer rates are presented for the screening years , both as annual rates and as aggregate rates for this period. For age-group comparisons, interval cancer rates were aggregated for the most recent screening quinquennium ( ) in order to ensure sufficient numbers, and are shown graphically for comparison. cancer rates in this report are calculated as cohort rates. That is, interval occurring in women with negative screening mammography in a given year are cumulated for the following 12 months, the subsequent year (12-24 months) and for the full 2-year interval (0-24 months) following the screening year. Consequently, the total interval cancer rates reported here are the sum of the first and second year rates, and are not the same measure as those reported in the previous BSA interval cancer report modelled on the BreastScreen monitoring reports from the Australian Institute of Health and Welfare (AIHW) which effectively use an average of annual rates for first and second year screens. 7
8 2.5 Programme Sensitivity Programme sensitivity is defined as the number of screen-detected expressed as a proportion of total cancer incidence (screen detected plus interval ) in women screened. Sensitivity was calculated for the BSA programme for each age group as specified above. Temporal trends are shown by initial, subsequent and all screens, but for BSA Lead Provider are shown only for all screens, because of small numbers. 2.5 Statistical methods For age-specific interval cancer rates, confidence intervals were calculated as score intervals according to a method developed by Vollset which addresses the issue of confidence intervals calculated by the exact method being too conservative (wide). 5,6 8
9 3. RESULTS (MAIN FEATURES) 3.1 For the screening years , 678 interval occurred in the first year following a negative mammogram, representing an interval cancer rate of 6.3 per 10,000 screens (Table 3); 1,346 interval were detected in the second year following a negative mammogram, representing an interval cancer rate of 12.6 per 10,000 screens (Table 4). The total interval for was 2,024. occurring in the first 12 months (aggregated for ) decrease with increasing age, from 7.5 in year women to 5.0 per 10,000 screens in 65 year women for all screens (Figure 1). cancer rates in the subsequent months for all screens showed no significant age trend. The secular trend for screening years 1999 to 2007 for <12 month interval declined from 7.3 to ~6 per 10,000 screens. For month and all interval the secular trend showed a sharper decline from 1999 to 2002, and plateaued thereafter (Figure 2). 3.2 Programme sensitivity 4,979 breast were detected by screening from 1,074,959 screens during (Tables 5 & 6). Programme sensitivity for <12 month interval was 88% (Table 5), and 79% for month interval (Table 6). Programme sensitivity (aggregated for ) increases with age for <12, and 0-24 months interval (Figure 3). Programme sensitivity decreased somewhat after 2001 for initial screens, but this was counteracted to an extent by increased sensitivity for subsequent screens, leaving a slight decreasing trend overall (Figure 4). 3.3 BSA Lead providers For <12 month interval, none of the BSA Lead Providers differed significantly from the NZ BSA programme overall (Figure 5); for and 0-24 month interval, BSC had significantly lower interval cancer rates. For programme sensitivity, no lead provider differed significantly from NZ overall with regard to <12 month interval (Figure 6). Reflecting interval cancer differences, BSC had significantly higher programme sensitivity for month interval from initial and subsequent screens and 0-24 month interval from subsequent and all screens. Two BSA Lead Providers, BSC and BSSL, showed decreasing secular trends in interval cancer rates, 2 others showed early decreases followed by an increase (BSCC, BSM), while BSHC and BSAL showed no discernible trends (Figure 7). Secular trends for BSWN and BSCM cannot be interpreted as these Lead Providers were recent additions to the screening programme. Secular trends in programme sensitivity by BSA Lead Provider appear to be decreasing for BSAL, BSCC, BSHC and BSM, and neutral for BSC, BSSL (Figure 8). While BSWN and BSCM are too recent for meaningful interpretation of trends, stochastic variation along with the small number of time points, warrants caution in interpreting secular trends in programme sensitivity by Lead Provider. 9
10 More detail on individual Lead Providers is in the Appendix. Table 3. First-year ( <12 months) interval breast after an initial or subsequent screen by age-group and screening year, BSA programme, Age group (yr) Initial Screens Subsequent Screens All Screens Rate/10,000 Women Rate/10,000 Women screened (95% CI) screened screened (95% CI) screened Women screened Rate/10,000 screened (95% CI) , ( ) 2 2, ( ) 22 29, ( ) , ( ) 5 4, ( ) 20 24, ( ) , ( ) 1 3, ( ) 13 21, ( ) ( ) (0.0-1,936) ( ) All , ( ) 8 11, ( ) 55 75, ( ) , ( ) 4 3, ( ) 24 34, ( ) , ( ) 3 5, ( ) 19 24, ( ) , ( ) 4 4, ( ) 13 20, ( ) ( ) (0.0-2,039) ( ) All , ( ) 11 13, ( ) 56 79, ( ) , ( ) 6 16, ( ) 18 36, ( ) , ( ) 17 21, ( ) 19 29, ( ) , ( ) 19 20, ( ) 19 26, ( ) (0.0-1,431) ( ) ( ) All , ( ) 42 58, ( ) 56 93, ( ) , ( ) 17 20, ( ) 31 39, ( ) , ( ) 16 25, ( ) 21 30, ( ) , ( ) 10 22, ( ) 11 26, ( ) (0.0-4,899) (0.0-1,758) (0.0-1,486) All , ( ) 43 69, ( ) 63 96, ( ) , ( ) 8 19, ( ) 24 38, ( ) , ( ) 22 30, ( ) 23 34, ( ) , ( ) 16 26, ( ) 17 29, ( ) (0.0-3,903) (0.0-1,135) ( ) All , ( ) 46 77, ( ) , ( ) ( ) (0.0-9,701) ( ) , ( ) 17 23, ( ) 28 40, ( ) , ( ) 21 33, ( ) 25 36, ( ) , ( ) 16 26, ( ) 19 28, ( ) , ( ) 3 13, ( ) 3 14, ( ) All 19 24, ( ) 57 97, ( ) , ( ) , ( ) (0.0-1,287) 12 21, ( ) , ( ) 10 21, ( ) 19 37, ( ) , ( ) 17 33, ( ) 19 36, ( ) , ( ) 19 28, ( ) 21 30, ( ) , ( ) 12 21, ( ) 12 23, ( ) All 25 43, ( ) , ( ) , ( ) , ( ) ( ) 28 34, ( ) , ( ) 9 23, ( ) 20 38, ( ) , ( ) 20 38, ( ) 20 41, ( ) , ( ) 21 30, ( ) 25 32, ( ) , ( ) 12 22, ( ) 12 24, ( ) All 42 55, ( ) , ( ) , ( ) , ( ) 12 10, ( ) 33 42, ( ) , ( ) 18 29, ( ) 29 42, ( ) , ( ) 18 35, ( ) 20 38, ( ) , ( ) 22 31, ( ) 23 33, ( ) , ( ) 15 25, ( ) 15 27, ( ) All 35 52, ( ) , ( ) , ( ) , ( ) 13 10, ( ) 74 99, ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) 42 83, ( ) 42 90, ( ) All , ( ) , ( ) 678 1,074, ( ) 1 Includes year women who screened 10
11 Table 4. Second-year (12 to <24 months) interval breast after an initial or subsequent screen by age-group and screening year, BSA programme, Age group (yr) Initial Screens Subsequent Screens All Screens Rate/10,000 Women Rate/10,000 Women screened (95% CI) screened screened (95% CI) screened Women screened Rate/10,000 screened (95% CI) , ( ) 6 2, ( ) 52 29, ( ) , ( ) 5 4, ( ) 42 24, ( ) , ( ) 2 3, ( ) 29 21, ( ) ( ) (0.0-1,936) ( ) All , ( ) 13 11, ( ) , ( ) , ( ) 5 3, ( ) 52 34, ( ) , ( ) 8 5, ( ) 39 24, ( ) , ( ) 8 4, ( ) 33 20, ( ) ( ) (0.0-2,039) ( ) All , ( ) 21 13, ( ) , ( ) , ( ) 17 16, ( ) 42 36, ( ) , ( ) 29 21, ( ) 40 29, ( ) , ( ) 28 20, ( ) 36 26, ( ) (0.0-1,431) ( ) ( ) All , ( ) 74 58, ( ) , ( ) , ( ) 19 20, ( ) 35 39, ( ) , ( ) 30 25, ( ) 39 30, ( ) , ( ) 27 22, ( ) 30 26, ( ) (0.0-4,899) (0.0-1,759) (0.0-1,486) All , ( ) 76 69, ( ) , ( ) , ( ) 23 19, ( ) 43 38, ( ) , ( ) 35 30, ( ) 43 34, ( ) , ( ) 33 26, ( ) 36 29, ( ) (0.0-3,903) (0.0-1,135) ( ) All , ( ) 91 77, ( ) , ( ) ( ) (0.0-6,576) ( ) , ( ) 36 23, ( ) 60 40, ( ) , ( ) 36 33, ( ) 39 36, ( ) , ( ) 33 26, ( ) 34 28, ( ) , ( ) 14 13, ( ) 16 14, ( ) All 32 24, ( ) , ( ) , ( ) , ( ) (0.0-1,287) 33 21, ( ) , ( ) 22 21, ( ) 48 37, ( ) , ( ) 33 33, ( ) 36 36, ( ) , ( ) 34 28, ( ) 34 30, ( ) , ( ) 32 21, ( ) 33 23, ( ) All 63 43, ( ) , ( ) , ( ) , ( ) ( ) 52 34, ( ) , ( ) 19 23, ( ) 30 38, ( ) , ( ) 45 38, ( ) 51 41, ( ) , ( ) 36 30, ( ) 38 32, ( ) , ( ) 18 22, ( ) 21 24, ( ) All 72 55, ( ) , ( ) , ( ) , ( ) 17 10, ( ) 48 42, ( ) , ( ) 35 29, ( ) 50 42, ( ) , ( ) 45 35, ( ) 50 38, ( ) , ( ) 32 31, ( ) 34 33, ( ) , ( ) 40 25, ( ) 46 27, ( ) All 59 52, ( ) , ( ) , ( ) , ( ) 19 10, ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) , ( ) All , ( ) , ( ) 1,346 1,074, ( ) 1 Includes year women who screened 11
12 Figure 1. by 5-year age group years, initial and subsequent screens, aggregated, with 95% confidence intervals 12
13 Figure 2. occurring in first year (<12 months) and second year (12-24 months) following initial or subsequent screens occurring in , women aged years, with 95% confidence intervals 13
14 Table 5. First-year ( <12 months) programme sensitivity (%) after an initial or subsequent screen by age-group and screening year, Age group (yr) Initial Screens Subsequent Screens All Screens Sensitivity Screen Sensitivity Screen (95% CI) detected (95% CI) detected Screen detected Sensitivity (95% CI) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) 215 1, ( ) ( ) ( ) 186 1, ( ) ( ) ( ) 161 1, ( ) ( ) ( ) ( ) All ( ) 413 2, ( ) 678 4, ( ) 14
15 Table 6. Second-year (12 to <24 months) programme sensitivity (%) after an initial or subsequent screen by age-group and screening year, Age group (yr) Initial Screens Subsequent Screens All Screens Sensitivity Screen Sensitivity Screen (95% CI) detected (95% CI) detected Screen detected Sensitivity (95% CI) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) All ( ) ( ) ( ) ( ) ( ) ( ) ( ) ( ) 412 1, ( ) ( ) ( ) 379 1, ( ) ( ) ( ) 304 1, ( ) ( ) ( ) ( ) All ( ) 804 2, ( ) 1,346 4, ( ) 15
16 Figure 3. Programme sensitivity by age years, by interval in first and second year following initial or subsequent screen, with 95% confidence intervals,
17 Figure 4. Programme sensitivity (%) by first and subsequent screens in relation to interval in the first year (<12 months) and second year (12-24 months) following screens occurring in , with 95% confidence intervals 17
18 Figure 5. cancer rates by BSA Lead Provider, by first and second year interval and by initial and subsequent screens, with 95% confidence intervals, % CI for BSA (all Lead Providers) 18
19 Figure 6. Programme sensitivity by BSA Lead Provider, by first and second year interval and by initial and subsequent screens, with 95% confidence intervals, % CI for BSA (all Lead Providers) 19
20 Figure 7. Trends in interval cancer rates by BSA Lead Provider, , with 95% confidence intervals 20
21 Figure 8. Trends in programme sensitivity by BSA Lead Provider, , with 95% confidence intervals 21
22 4. COMPARISONS WITH PREVIOUS INTERVAL CANCER REPORT Estimates of interval cancer rates are slightly higher in the present report than those reported previously for the years , and programme sensitivity estimates correspondingly are lower. For instance, in the first BSA interval cancer report, 4 45 interval for the screening year 1999 were reported occurring 12 months subsequently, compared to 55 interval in the present report. occurring in the second year following screening in 1999 were reported originally as 114, compared to 123 in this report. For , 198 first year (<12 months) and 419 second year (12-24 months) interval were recorded in the first BSA interval cancer report, 4 compared with 241 first year (<12 months) and 469 second year (12-24 months) intervals for the same period in this report. The higher numbers in the present report are due to the more exhaustive process in ascertaining interval. For , the additional 33 first year (0-12 months) interval found represented a 17% increase, and the 49 second year (12-24 months) interval a 12% increase. The total of 82 extra interval found for represented a 13% increase overall. 22
23 5. INTERNATIONAL COMPARISONS cancer rates reported from trials and by various population based mammography screening programmes enable comparison and assessment of BSA in relation to trial conditions and to programmes operating as part of routine health services. cancer rates for BSA are not significantly different to those of comparable programmes in the UK, the Netherlands and Australia (Table 7). Table 7. BSA interval cancer rates (per 10,000) compared with other national mammography screening programmes, by first year (<12 months) and second year (12-<24 months) interval Programme/trial Target age-group (yr) NZ Period (Index screening year) cancer rate <12 months Initial: 6.8 ( ) Subsequent: 6.1 ( ) All: 6.3 ( ) Initial: 6.9 ( ) Subsequent: 5.9 ( ) All: 6.2 ( ) cancer rate 12-<24 months Initial: 13.8 ( ) Subsequent: 11.9 ( ) All: 12.6 ( ) Initial: 12.8 ( ) Subsequent: 11.8 ( ) All: 12.1 ( ) Screening Programme NHS (UK) April March 2003 All: 5.5 ( ) All: 11.3 ( ) East Anglia (UK) Subsequent: 5.2 ( ) Subsequent: 12.8 ( ) Scotland Initial: 4.8 ( ) Initial: 12.1 ( ) Dublin (Ireland) Initial: 10.1 ( ) Initial: 10.6 ( ) Subsequent: 6.8 ( ) Subsequent: 11.1 ( ) Turin (Italy) Initial: 5.6 ( ) Initial: 10.0 ( ) Netherlands Initial: 6.6 ( ) Subsequent: 5.9 ( ) All: 6.4 ( ) Initial: 11.3 ( ) Subsequent: 12.0 ( ) All: 11.5 ( ) Australia NSW 12, Victoria 12, Queensland South Australia Western Australia Initial: 6.9 ( ) Initial: 11.9 ( ) Subsequent: 7.0 ( ) Subsequent: 12.5 ( ) Initial: 5.5 ( ) Initial: 13.3 ( ) Subsequent: 6.7 ( ) Subsequent: 12.5 ( ) Initial: 7.2 ( ) Initial: 12.8 ( ) Subsequent: 9.6 ( ) Subsequent: 14.3 ( ) Initial: 6.4 ( ) Initial: 9.9 ( ) Subsequent: 7.3 ( ) Subsequent: 11.5 ( ) Initial: 5.9 ( ) Initial: 12.0 ( ) Subsequent: 6.6 ( ) Subsequent: 12.2 ( ) Initial: 6.5 ( ) Initial: 12.8 ( ) Initial: 7.2 ( ) Initial: 10.0 ( ) Subsequent: 6.9 ( ) Subsequent: 13.5 ( ) Initial: 5.6 ( ) Initial: 19.0 ( ) Subsequent: 7.0 ( ) Subsequent: 12.7 ( ) Initial: 7.5 ( ) Initial: 17.4 ( ) Subsequent: 7.1 ( ) Subsequent: 14.0 ( ) Initial: 5.9 ( ) Initial: 11.9 ( ) Subsequent: 7.1 ( ) Subsequent: 14.2 ( ) Initial: 3.5 ( ) Initial: 9.4 ( ) Subsequent: 6.7 ( ) Subsequent: 12.0 ( ) Initial: 4.0 ( ) Initial: 4.6 ( ) Subsequent: 5.9 ( ) Subsequent: 12.9 ( ) Initial: 4.8 ( ) Initial: 14.2 ( ) Subsequent: 6.6 ( ) Subsequent: 11.3 ( ) Initial: 2.4 ( ) Initial: 19.1 ( ) Subsequent: 5.9 ( ) Subsequent: 10.8 ( ) Trial Sweden (Two County) All: 3.2 ( ) All: 6.4 ( ) Edinburgh Subsequent: 2.0 ( ) Subsequent: 7.1 ( ) BSA programme sensitivity is also similar to other programmes, with estimates close to those for Australia (Table 8). 23
24 Table 8. BSA programme sensitivity (%) compared with other national mammography screening programmes, by first year (<12 months), second year (12-<24 months) interval Programme/trial Target age-group Period (index screening Sensitivity Sensitivity (yr) year) <12 months 12-<24 months Initial: 89.0 ( ) Subsequent: 87.3 ( ) Initial: 79.8 ( ) Subsequent: 77.9 ( ) NZ All: 88.0 ( ) All: 78.7 ( ) Initial: 87.7 ( ) Initial: 79.4 ( ) Subsequent: 87.6 ( ) All: 87.6 ( ) Subsequent: 77.8 ( ) All: 78.3 ( ) Screening Programme Dublin (Ireland) Initial: 74.7 ( ) Initial: 73.8 ( ) Subsequent: 64.4 ( ) Subsequent: 52.6 ( ) Turin (Italy) Initial: 84.9 ( ) Initial: 75.8 ( ) Netherlands Initial: 88.2 ( ) Subsequent: 83.6 ( ) All: 87.4 ( ) Initial: 81.4 ( ) Subsequent: 71.3 ( ) All: 79.5 ( ) Australia Initial: 90.4 ( ) Initial: 78.2 ( ) Subsequent: 86.0 ( ) Subsequent: 69.9 ( ) Initial: 92.5 ( ) Initial: 79.9 ( ) Subsequent: 86.3 ( ) Subsequent: 70.2 ( ) Initial: 86.3 ( ) Initial: 78.9 ( ) Subsequent: 78.5 ( ) Subsequent: 70.7 ( ) NSW 12, Initial: 90.8 ( ) Initial: 79.6 ( ) Subsequent: 85.6 ( ) Subsequent: 71.1 ( ) Initial: 91.4 ( ) Initial: 80.6 ( ) Subsequent: 86.5 ( ) Subsequent: 72.4 ( ) Initial: 85.9 ( ) Initial: 68.6 ( ) Victoria 12, Initial: 89.4 ( ) Initial: 78.3 ( ) Subsequent: 84.2 ( ) Subsequent: 64.7 ( ) Initial: 91.8 ( ) Initial: 74.6 ( ) Subsequent: 85.1 ( ) Subsequent: 67.0 ( ) Queensland Initial: 92.2 ( ) Initial: 74.8 ( ) Subsequent: 86.6 ( ) Subsequent: 69.6 ( ) Initial: 92.7 ( ) Initial: 80.2 ( ) Subsequent: 86.1 ( ) Subsequent: 66.9 ( ) South Australia Initial: 94.7 ( ) Initial: 85.4 ( ) Subsequent: 87.4 ( ) Subsequent: 72.7 ( ) Initial: 94.0 ( ) Initial: 88.6 ( ) Subsequent: 88.7 ( ) Subsequent: 71.6 ( ) Western Australia Initial: 92.7 ( ) Initial: 78.9 ( ) Subsequent: 87.3 ( ) Subsequent: 74.0 ( ) Initial: 96.6 ( ) Initial: 79.3 ( ) Subsequent: 87.9 ( ) Subsequent: 74.2 ( ) Trial Sweden (Two County) All: 82.1 ( ) All: 79.9 ( ) 24
25 REFERENCES 1. Tabár L, Fagerberg G, Duffy SW, Day NE, Gad A, Grontoft O. Update of the Swedish two-county program of mammographic screening for breast cancer. Radiol Clin North Am 1992;30(1): Field S, Michell MJ, Wallis MG, Wilson AR. What should be done about interval breast? BMJ 1995;310(6974): Frisell J, Eklund G, Hellstrom L, Somell A. Analysis of interval breast carcinomas in a randomized screening trial in Stockholm. Breast Cancer Res Treat 1987;9(3): Begg S, Page A, Arnett K, Taylor R. in BreastScreen Aotearoa Final. BreastScreen Aotearoa, Vollset SE. Confidence intervals for a binomial proportion. Stat Med. 1993;12: Agresti A, Coull BA. Approximate is better than exact for interval estimation of binomial proportions. Am Stat. 1998;52: Bennett RL, Sellars SJ, Moss SM. in the NHS breast cancer screening programme in England, Wales and Northern Ireland. British Journal of Cancer. 2011;104: Day N, McCann J, Camilleri-Ferrante C, et al. Monitoring interval in breast screening programmes: the east Anglian experience. Quality Assurance Management Group of the East Anglian Breast Screening Programme. J Med Screen 1995;2: Everington D, Gilbert FJ, Tyack C, Warner J. The Scottish breast screening programme's experience of monitoring interval. J Med Screen 1999;6: Tornberg S, Codd M, Rodrigues V, Segnan N, Ponti A. Ascertainment and evaluation of interval in population-based mammography screening programmes: a collaborative study in four European centres. J Med Screen 2005;12: Fracheboud J, de Koning HJ, Beemsterboer PM, Boer R, Verbeek AL, Hendriks JH, et al. in the Dutch breast cancer screening programme. Br J Cancer 1999;81(5): Australian Institute of Health and Welfare BreastScreen Australia Monitoring Report Cancer series no. 63. Cat. no. CAN 60. Canberra: AIHW. 13. Taylor R, Page A, Bampton D, Estoesta J, Rickard M. Age-specific interval breast in New South Wales and meta-analysis of studies of women aged years. J Med Screen 2004;11: Kavanagh AM, Mitchell H, Farrugia H, Giles GG. Monitoring interval in an Australian mammographic screening programme. J Med Screen 1999;6: Alexander FE, Anderson TJ, Brown HK, et al. The Edinburgh randomised trial of breast cancer screening: results after 10 years of follow-up. Br J Cancer 1994;70:
26 APPENDIX Table A1. First-year (<12 months) interval breast after an initial or subsequent screen by age-group and BreastScreen Lead Provider, BSA programme, Age group (yr) Initial Screens Subsequent Screens All Screens Rate/10,000 Women Rate/10,000 Women screened (95% CI) screened screened (95% CI) screened Women screened Rate/10,000 screened (95% CI) BSAL , ( ) ( ) 6 8, ( ) , ( ) 19 32, ( ) 56 80, ( ) , ( ) 26 46, ( ) 38 69, ( ) , ( ) 18 37, ( ) 26 55, ( ) , ( ) 2 11, ( ) 2 12, ( ) All , ( ) , ( , ( ) BSC , ( ) 1 1, ( ) 7 10, ( ) , ( ) 6 16, ( ) 25 35, ( ) , ( ) 15 23, ( ) 21 32, ( ) , ( ) 12 19, ( ) 13 25, ( ) ( ) 4 9, ( ) 4 9, ( ) All , ( ) 38 69, ( ) , ( ) BSCC , ( ) 2 1, ( ) 9 12, ( ) , ( ) 11 19, ( ) 27 43, ( ) , ( ) 22 28, ( ) 28 39, ( ) , ( ) 17 24, ( ) 27 33, ( ) ( ) 4 11, ( ) 4 12, ( ) All , ( ) 56 86, ( ) , ( ) BSCM , ( ) ( ) 3 5, ( ) , ( ) 1 3, ( ) 3 7, ( ) ( ) 2 6, ( ) 3 7, ( ) ( ) 2 5, ( ) 3 5, ( ) ( ) 1 3, ( ) 1 4, ( ) All , ( ) 6 19, ( ) 13 30, ( ) BSHC , ( ) 2 1, ( ) 7 8, ( ) , ( ) 8 16, ( ) 11 28, ( ) , ( ) 14 23, ( ) 15 25, ( ) ( ) 20 20, ( ) 20 21, ( ) ( ) 5 6, ( ) 5 6, ( ) All , ( ) 49 69, ( ) 58 90, ( ) BSM , ( ) 4 2, ( ) 12 15, ( ) , ( ) 18 24, ( ) 36 48, ( ) , ( ) 33 38, ( ) 42 45, ( ) , ( ) 27 36, ( ) 30 41, ( ) ( ) 6 15, ( ) 6 16, ( ) All , ( ) , ( ) , ( ) BSSL , ( ) 4 2, ( ) 24 27, ( ) , ( ) 25 42, ( ) 48 82, ( ) , ( ) 25 52, ( ) 37 68, ( ) , ( ) 26 42, ( ) 35 55, ( ) , ( ) 16 19, ( ) 16 21, ( ) All 64 94, ( ) , ( ) , ( ) BSWN , ( ) ( ) 6 11, ( ) , ( ) 3 6, ( ) 10 11, ( ) , ( ) 2 10, ( ) 2 11, ( ) ( ) 6 8, ( ) 7 9, ( ) ( ) 4 6, ( ) 4 7, ( ) All 14 19, ( ) 15 32, ( ) 29 52, ( ) 1 Includes year women who screened 26
Interval Cancers in BreastScreen Aotearoa
 Interval Cancers in BreastScreen Aotearoa 2008 2009 Released 2018 nsu.govt.nz Citation: National Screening Unit. 2018. Interval Cancers in BreastScreen Aotearoa 2008 2009. Wellington: Ministry of Health.
Interval Cancers in BreastScreen Aotearoa 2008 2009 Released 2018 nsu.govt.nz Citation: National Screening Unit. 2018. Interval Cancers in BreastScreen Aotearoa 2008 2009. Wellington: Ministry of Health.
Ascertaining and reporting interval cancers in BreastScreen Aotearoa: A protocol NATIONAL SCREENING UNIT (NSU) MINISTRY OF HEALTH
 Ascertaining and reporting interval cancers in BreastScreen Aotearoa: A protocol NATIONAL SCREENING UNIT (NSU) MINISTRY OF HEALTH Dr. Simon Baker National Screening Unit Ministry of Health October 2005
Ascertaining and reporting interval cancers in BreastScreen Aotearoa: A protocol NATIONAL SCREENING UNIT (NSU) MINISTRY OF HEALTH Dr. Simon Baker National Screening Unit Ministry of Health October 2005
BREASTSCREEN AOTEAROA INDEPENDENT MONITORING REPORT:
 BREASTSCREEN AOTEAROA INDEPENDENT MONITORING REPORT: TREATMENT OF WOMEN WITH BSA DETECTED CANCERS (WOMEN SCREENED JANUARY 5-DECEMBER 6) Dr Andrew Page Kathryn Arnett Professor Richard Taylor School of
BREASTSCREEN AOTEAROA INDEPENDENT MONITORING REPORT: TREATMENT OF WOMEN WITH BSA DETECTED CANCERS (WOMEN SCREENED JANUARY 5-DECEMBER 6) Dr Andrew Page Kathryn Arnett Professor Richard Taylor School of
Cohort and Case Control Analyses of Breast Cancer Mortality: BreastScreen Aotearoa
 Cohort and Case Control Analyses of Breast Cancer Mortality: BreastScreen Aotearoa 1999-2011 by Stephen Morrell, 1 Richard Taylor, 1 David Roder, 2 Bridget Robson 3 1. School of Public Health and Community
Cohort and Case Control Analyses of Breast Cancer Mortality: BreastScreen Aotearoa 1999-2011 by Stephen Morrell, 1 Richard Taylor, 1 David Roder, 2 Bridget Robson 3 1. School of Public Health and Community
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report 29 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 29 Produced by: BreastScreen Victoria Coordination Unit Level, 3 Pelham Street, Carlton South Victoria
BreastScreen Victoria Annual Statistical Report 29 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 29 Produced by: BreastScreen Victoria Coordination Unit Level, 3 Pelham Street, Carlton South Victoria
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report CONTENTS FIGURES AND TABLES... Figures... Tables... 3 INTRODUCTION... 5 SECTION MAXIMISING PARTICIPATION... 6 Program acceptance... 6 Eligibility... 6 Inviting
BreastScreen Victoria Annual Statistical Report CONTENTS FIGURES AND TABLES... Figures... Tables... 3 INTRODUCTION... 5 SECTION MAXIMISING PARTICIPATION... 6 Program acceptance... 6 Eligibility... 6 Inviting
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report 005 Produced by: BreastScreen Victoria Coordination Unit Level, Pelham Street, Carlton South Victoria 05 PH 0 9660 6888 FX 0 966 88 EM info@breastscreen.org.au
BreastScreen Victoria Annual Statistical Report 005 Produced by: BreastScreen Victoria Coordination Unit Level, Pelham Street, Carlton South Victoria 05 PH 0 9660 6888 FX 0 966 88 EM info@breastscreen.org.au
The Australian BreastScreen workforce: a snapshot
 Original article Volume 59 (1) 2012 The Australian BreastScreen workforce: a snapshot S Moran British Diploma of Diagnostic Radiography H Warren Forward Bsc (Hons), Phd Medical Radiation Science Hunter
Original article Volume 59 (1) 2012 The Australian BreastScreen workforce: a snapshot S Moran British Diploma of Diagnostic Radiography H Warren Forward Bsc (Hons), Phd Medical Radiation Science Hunter
Trends in stage-specific breast cancer incidence and overdiagnosis in NSW
 Trends in stage-specific breast cancer incidence and overdiagnosis in NSW Presented by Dr Gemma Jacklyn Sydney School of Public Health @gemmajacklyn Authors Gemma Jacklyn, Kevin McGeechan, Les Irwig, Nehmat
Trends in stage-specific breast cancer incidence and overdiagnosis in NSW Presented by Dr Gemma Jacklyn Sydney School of Public Health @gemmajacklyn Authors Gemma Jacklyn, Kevin McGeechan, Les Irwig, Nehmat
- The University of. - Student. Western Australia, Crawley, Western Australia
 Title: Is Step Down Assessment of Screen Detected Lesions as Safe as Workup at a Metropolitan Assessment Centre? Authors Author name Degrees/ Fellowships Position Institution Phone Email Jade P Hughes
Title: Is Step Down Assessment of Screen Detected Lesions as Safe as Workup at a Metropolitan Assessment Centre? Authors Author name Degrees/ Fellowships Position Institution Phone Email Jade P Hughes
Cite this article as: BMJ, doi: /bmj f (published 8 March 2005)
 Cite this article as: BMJ, doi:10.1136/bmj.38398.469479.8f (published 8 March 2005) Model of outcomes of screening mammography: information to support informed choices Alexandra Barratt, Kirsten Howard,
Cite this article as: BMJ, doi:10.1136/bmj.38398.469479.8f (published 8 March 2005) Model of outcomes of screening mammography: information to support informed choices Alexandra Barratt, Kirsten Howard,
Effect of NHS breast screening programme on mortality from breast cancer in England and Wales, : comparison of observed with predicted mortality
 Effect of NHS breast screening programme on mortality from breast cancer in England and Wales, 1990-8: comparison of observed with predicted mortality R G Blanks, S M Moss, C E McGahan, M J Quinn, P J
Effect of NHS breast screening programme on mortality from breast cancer in England and Wales, 1990-8: comparison of observed with predicted mortality R G Blanks, S M Moss, C E McGahan, M J Quinn, P J
What is the most appropriate breast-cancer screening interval for women aged 45 to 49 years in New Zealand?
 Vol 118 No 1221 ISSN 1175 8716 What is the most appropriate breast-cancer screening interval for women aged 45 to 49 years in New Zealand? Simon Baker, Madeleine Wall, Ashley Bloomfield Abstract Aim To
Vol 118 No 1221 ISSN 1175 8716 What is the most appropriate breast-cancer screening interval for women aged 45 to 49 years in New Zealand? Simon Baker, Madeleine Wall, Ashley Bloomfield Abstract Aim To
Table of contents. Page 2 of 40
 Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
BreastScreen Victoria Annual Statistical Report
 BreastScreen Victoria Annual Statistical Report 2010 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 2010 Produced by: BreastScreen Victoria Coordination Unit Level 1, 31 Pelham Street, Carlton South
BreastScreen Victoria Annual Statistical Report 2010 BREASTSCREEN VICTORIA: ANNUAL STATISTICAL REPORT, 2010 Produced by: BreastScreen Victoria Coordination Unit Level 1, 31 Pelham Street, Carlton South
Summary of the BreastScreen Aotearoa Mortality Evaluation
 Summary of the BreastScreen Aotearoa Mortality Evaluation 1999 2011 Released 2015 nsu.govt.nz Citation: Ministry of Health. 2015. Summary of the BreastScreen Aotearoa Mortality Evaluation 1999 2011. Wellington:
Summary of the BreastScreen Aotearoa Mortality Evaluation 1999 2011 Released 2015 nsu.govt.nz Citation: Ministry of Health. 2015. Summary of the BreastScreen Aotearoa Mortality Evaluation 1999 2011. Wellington:
Public Health Agency NORTHERN IRELAND BREAST SCREENING PROGRAMME ANNUAL REPORT & STATISTICAL BULLETIN QUALITY ASSURANCE REFERENCE CENTRE
 Public Health Agency Improving Your Health and Wellbeing NORTHERN IRELAND BREAST SCREENING PROGRAMME ANNUAL REPORT & STATISTICAL BULLETIN 2010-2011 QUALITY ASSURANCE REFERENCE CENTRE August 2012 1 2 Contents
Public Health Agency Improving Your Health and Wellbeing NORTHERN IRELAND BREAST SCREENING PROGRAMME ANNUAL REPORT & STATISTICAL BULLETIN 2010-2011 QUALITY ASSURANCE REFERENCE CENTRE August 2012 1 2 Contents
BARC/2013/E/019 BARC/2013/E/019. AUDIT OF MAMMOGRAPHY PERFORMED IN OUR HOSPITAL by Surita Kantharia Medical Division
 BARC/2013/E/019 BARC/2013/E/019 AUDIT OF MAMMOGRAPHY PERFORMED IN OUR HOSPITAL by Surita Kantharia Medical Division BARC/2013/E/019 GOVERNMENT OF INDIA ATOMIC ENERGY COMMISSION BARC/2013/E/019 AUDIT OF
BARC/2013/E/019 BARC/2013/E/019 AUDIT OF MAMMOGRAPHY PERFORMED IN OUR HOSPITAL by Surita Kantharia Medical Division BARC/2013/E/019 GOVERNMENT OF INDIA ATOMIC ENERGY COMMISSION BARC/2013/E/019 AUDIT OF
Title: Breast Screen Reader Assessment Strategy (BREAST): UK Collaboration
 Susan Williams CoRIPS Research Grant 147 5000 awarded Title: Breast Screen Reader Assessment Strategy (BREAST): UK Collaboration Principle Aim The principal aim of the study is to evaluate the performance
Susan Williams CoRIPS Research Grant 147 5000 awarded Title: Breast Screen Reader Assessment Strategy (BREAST): UK Collaboration Principle Aim The principal aim of the study is to evaluate the performance
Screen detection of ductal carcinoma in situ and subsequent incidence of invasive interval breast cancers: a retrospective population-based study
 Screen detection of ductal carcinoma in situ and subsequent incidence of invasive interval breast cancers: a retrospective population-based study Stephen W Duffy, Amanda Dibden, Dimitrios Michalopoulos,
Screen detection of ductal carcinoma in situ and subsequent incidence of invasive interval breast cancers: a retrospective population-based study Stephen W Duffy, Amanda Dibden, Dimitrios Michalopoulos,
Mammo-50 Eligibility Queries
 Mammo-50 Eligibility Queries Are patients who have received either neo-adjuvant or adjuvant chemo, radiotherapy or been part of another trial, ie OPTIMA, FAST FORWARD excluded from entry? Any patients
Mammo-50 Eligibility Queries Are patients who have received either neo-adjuvant or adjuvant chemo, radiotherapy or been part of another trial, ie OPTIMA, FAST FORWARD excluded from entry? Any patients
The aim of screening mammography is to detect malignant breast cancer. Performance of screening mammography in organized programs in Canada in 1996
 Performance of screening mammography in organized programs in Canada in 1996 Dana Paquette, * Judy Snider, * Françoise Bouchard, * Ivo Olivotto, Heather Bryant, Kathleen Decker, Gregory Doyle, for the
Performance of screening mammography in organized programs in Canada in 1996 Dana Paquette, * Judy Snider, * Françoise Bouchard, * Ivo Olivotto, Heather Bryant, Kathleen Decker, Gregory Doyle, for the
BreastScreen-based mammography screening in women with a personal history of breast cancer, Western Australian study
 Research Nehmat Houssami MB BS, FAFPHM, PhD, Principal Research Fellow and Associate Professor (Research) 1 Janette J Tresham BSc(Agric), Data Manager 2 Lin Fritschi MB BS, FAFPHM, PhD, Professor 3 Liz
Research Nehmat Houssami MB BS, FAFPHM, PhD, Principal Research Fellow and Associate Professor (Research) 1 Janette J Tresham BSc(Agric), Data Manager 2 Lin Fritschi MB BS, FAFPHM, PhD, Professor 3 Liz
BreastScreen Aotearoa Annual Report 2015
 BreastScreen Aotearoa Annual Report 2015 EARLY AND LOCALLY ADVANCED BREAST CANCER PATIENTS DIAGNOSED IN NEW ZEALAND IN 2015 Prepared for Ministry of Health, New Zealand Version 1.0 Date November 2017 Prepared
BreastScreen Aotearoa Annual Report 2015 EARLY AND LOCALLY ADVANCED BREAST CANCER PATIENTS DIAGNOSED IN NEW ZEALAND IN 2015 Prepared for Ministry of Health, New Zealand Version 1.0 Date November 2017 Prepared
Rare Breast Tumours. 1. Breast Tumours. 1.1 General Results. 1.2 Incidence
 Rare Breast Tumours 1. Breast Tumours 1.1 General Results Table 1. Epithelial Tumours of Breast: Incidence, Trends, Survival Flemish Region 2001-2010 Incidence Trend Survival Females EAPC Relative survival
Rare Breast Tumours 1. Breast Tumours 1.1 General Results Table 1. Epithelial Tumours of Breast: Incidence, Trends, Survival Flemish Region 2001-2010 Incidence Trend Survival Females EAPC Relative survival
Breast Cancer Screening and Diagnosis
 Breast Cancer Screening and Diagnosis Priya Thomas, MD Assistant Professor Clinical Cancer Prevention and Breast Medical Oncology University of Texas MD Anderson Cancer Center Disclosures Dr. Thomas has
Breast Cancer Screening and Diagnosis Priya Thomas, MD Assistant Professor Clinical Cancer Prevention and Breast Medical Oncology University of Texas MD Anderson Cancer Center Disclosures Dr. Thomas has
Association of symptoms and interval breast cancers in the mammography-screening programme: population-based matched cohort study
 www.nature.com/bjc ARTICLE Epidemiology Association of symptoms and interval breast cancers in the mammography-screening programme: population-based matched cohort study Deependra Singh 1,, Joonas Miettinen
www.nature.com/bjc ARTICLE Epidemiology Association of symptoms and interval breast cancers in the mammography-screening programme: population-based matched cohort study Deependra Singh 1,, Joonas Miettinen
BREAST CANCER SCREENING:
 BREAST CANCER SCREENING: controversies D David Dershaw Memorial Sloan Kettering Cancer Center New York, NY Areas of general agreement about mammographic screening Screening mammography has been demonstrated
BREAST CANCER SCREENING: controversies D David Dershaw Memorial Sloan Kettering Cancer Center New York, NY Areas of general agreement about mammographic screening Screening mammography has been demonstrated
HEALTH TECHNOLOGY ASSESSMENT IN PRACTICE: EVALUATION OF THE COSTS AND BENEFITS OF SCREENING FOR BREAST CANCER IN THE CZECH REPUBLIC
 HTA in Real-Time HEALTH TECHNOLOGY ASSESSMENT IN PRACTICE: EVALUATION OF THE COSTS AND BENEFITS OF SCREENING FOR BREAST CANCER IN THE CZECH REPUBLIC SVOBODNÍK A. 1, KLIMEŠ D. 1, BARTOŇKOVÁ H. 2, DANEŠ
HTA in Real-Time HEALTH TECHNOLOGY ASSESSMENT IN PRACTICE: EVALUATION OF THE COSTS AND BENEFITS OF SCREENING FOR BREAST CANCER IN THE CZECH REPUBLIC SVOBODNÍK A. 1, KLIMEŠ D. 1, BARTOŇKOVÁ H. 2, DANEŠ
Current Status of Supplementary Screening With Breast Ultrasound
 Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Current Status of Supplementary Screening With Breast Ultrasound Stephen A. Feig, M.D., FACR Fong and Jean Tsai Professor of Women s Imaging Department of Radiologic Sciences University of California,
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Carcinoma mammario: le istologie non frequenti. Valentina Guarneri Università di Padova IOV-IRCCS
 Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
Carcinoma mammario: le istologie non frequenti Valentina Guarneri Università di Padova IOV-IRCCS Histological diversity of breast adenocarcinomas Different histological types are defined according to specific
Multiple Primary and Histology Site Specific Coding Rules BREAST. FLORIDA CANCER DATA SYSTEM MPH Breast Site Specific Coding Rules
 Multiple Primary and Histology Site Specific Coding Rules BREAST 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways to view the Multiple l Primary/Histology
Multiple Primary and Histology Site Specific Coding Rules BREAST 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways to view the Multiple l Primary/Histology
The value of the craniocaudal mammographic view in breast cancer detection: A preliminary study
 The value of the craniocaudal mammographic view in breast cancer detection: A preliminary study P D Trieu 1, Prof. P C Brennan 1, Dr. W Lee 2, Dr. E Ryan 1, Dr. W Reed 1, Dr. M Pietrzyk 1 1. Medical Image
The value of the craniocaudal mammographic view in breast cancer detection: A preliminary study P D Trieu 1, Prof. P C Brennan 1, Dr. W Lee 2, Dr. E Ryan 1, Dr. W Reed 1, Dr. M Pietrzyk 1 1. Medical Image
Life expectancy in the United States continues to lengthen.
 Reduced Mammographic Screening May Explain Declines in Breast Carcinoma in Older Women Robert M. Kaplan, PhD and Sidney L. Saltzstein, MD, MPH wz OBJECTIVES: To examine whether declines in breast cancer
Reduced Mammographic Screening May Explain Declines in Breast Carcinoma in Older Women Robert M. Kaplan, PhD and Sidney L. Saltzstein, MD, MPH wz OBJECTIVES: To examine whether declines in breast cancer
Cancer screening: Breast
 Cancer control in NSW: 2016 Cancer screening: Breast Introduction In NSW, breast cancer accounted for 27.4 per cent of all new cancer cases in women, and 14.6 per cent of all cancer mortality in women
Cancer control in NSW: 2016 Cancer screening: Breast Introduction In NSW, breast cancer accounted for 27.4 per cent of all new cancer cases in women, and 14.6 per cent of all cancer mortality in women
Cite this article as: BMJ, doi: /bmj (published 13 January 2005)
 Cite this article as: BMJ, doi:10.1136/bmj.38313.639236.82 (published 13 January 2005) in Copenhagen after introduction of mammography screening: cohort study Anne Helene Olsen, Sisse H Njor, Ilse Vejborg,
Cite this article as: BMJ, doi:10.1136/bmj.38313.639236.82 (published 13 January 2005) in Copenhagen after introduction of mammography screening: cohort study Anne Helene Olsen, Sisse H Njor, Ilse Vejborg,
Uptake of breast cancer screening in older women
 Age and Ageing 2000; 29: 131 135 Uptake of breast cancer screening in older women NIA I. EDWARDS, DEE A. JONES 1 University Department of Geriatric Medicine, Glan Clwyd Hospital, Rhyl, Denbighshire, North
Age and Ageing 2000; 29: 131 135 Uptake of breast cancer screening in older women NIA I. EDWARDS, DEE A. JONES 1 University Department of Geriatric Medicine, Glan Clwyd Hospital, Rhyl, Denbighshire, North
NORTHERN IRELAND BREAST SCREENING PROGRAMME ANNUAL REPORT & STATISTICAL BULLETIN
 Improving Your Health and Wellbeing NORTHERN IRELAND BREAST SCREENING PROGRAMME ANNUAL REPORT & STATISTICAL BULLETIN 211-212 QUALITY ASSURANCE REFERENCE CENTRE August 213 1 2 Contents Page Summary 4 Introduction
Improving Your Health and Wellbeing NORTHERN IRELAND BREAST SCREENING PROGRAMME ANNUAL REPORT & STATISTICAL BULLETIN 211-212 QUALITY ASSURANCE REFERENCE CENTRE August 213 1 2 Contents Page Summary 4 Introduction
Mammographic imaging of nonpalpable breast lesions. Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand
 Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Mammographic imaging of nonpalpable breast lesions Malai Muttarak, MD Department of Radiology Chiang Mai University Chiang Mai, Thailand Introduction Contents Mammographic signs of nonpalpable breast cancer
Breast pathology. 2nd Department of Pathology Semmelweis University
 Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
Breast pathology 2nd Department of Pathology Semmelweis University Breast pathology - Summary - Benign lesions - Acute mastitis - Plasma cell mastitis / duct ectasia - Fat necrosis - Fibrocystic change/
ACRIN 6666 Therapeutic Surgery Form
 S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
Comparative pathology of breast cancer in a randomised trial of screening
 Br. J. Cancer (1991), 64, 18-113 '." Macmillan Press Ltd., 1991 Br. J. Cancer (1991), 64, 18 113 Comparative pathology of breast cancer in a randomised trial of screening T.J. Anderson', J. Lamb', P. Donnan2,
Br. J. Cancer (1991), 64, 18-113 '." Macmillan Press Ltd., 1991 Br. J. Cancer (1991), 64, 18 113 Comparative pathology of breast cancer in a randomised trial of screening T.J. Anderson', J. Lamb', P. Donnan2,
TARGETS To reduce the age-standardised mortality rate from cervical cancer in all New Zealand women to 3.5 per or less by the year 2005.
 Cervical Cancer Key points Annually, around 85 women die from, and 230 women are registered with, cervical cancer. The decline in both incidence and mortality rates for cervical cancer has accelerated
Cervical Cancer Key points Annually, around 85 women die from, and 230 women are registered with, cervical cancer. The decline in both incidence and mortality rates for cervical cancer has accelerated
Audit. Public Health Monitoring Report on 2006 Data. National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons.
 National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons Audit Public Health Monitoring Report on 2006 Data November 2009 Prepared by: Australian Safety & Efficacy Register of
National Breast & Ovarian Cancer Centre and Royal Australasian College of Surgeons Audit Public Health Monitoring Report on 2006 Data November 2009 Prepared by: Australian Safety & Efficacy Register of
Interval cancers in the Dutch breast cancer screening
 Article no. bjoc.1999.0786 Interval cancers in the Dutch breast cancer screening programme J Fracheboud 1, HJ de Koning 1, PMM Beemsterboer 1, R Boer 1, ALM Verbeek 3, JHCL Hendriks 4, BM van Ineveld 2,
Article no. bjoc.1999.0786 Interval cancers in the Dutch breast cancer screening programme J Fracheboud 1, HJ de Koning 1, PMM Beemsterboer 1, R Boer 1, ALM Verbeek 3, JHCL Hendriks 4, BM van Ineveld 2,
BR 1 Palpable breast lump
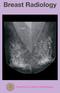 BR 1 Palpable breast lump Palpable breast lump in patient 40 years of age or above MMG +/- spot compression or digital breast tomosynthesis over palpable findings Suspicious or malignant findings (BIRADS
BR 1 Palpable breast lump Palpable breast lump in patient 40 years of age or above MMG +/- spot compression or digital breast tomosynthesis over palpable findings Suspicious or malignant findings (BIRADS
GUIDELINES FOR MONITORING BREAST CANCER SCREENING PROGRAM PERFORMANCE THIRD EDITION
 Report from the Evaluation Indicators Working Group GUIDELINES FOR MONITORING BREAST CANCER SCREENING PROGRAM PERFORMANCE THIRD EDITION Public Health Agency of Canada Acknowledgments We would like to acknowledge
Report from the Evaluation Indicators Working Group GUIDELINES FOR MONITORING BREAST CANCER SCREENING PROGRAM PERFORMANCE THIRD EDITION Public Health Agency of Canada Acknowledgments We would like to acknowledge
Mammography and Other Screening Tests. for Breast Problems
 301.681.3400 OBGYNCWC.COM Mammography and Other Screening Tests What is a screening test? for Breast Problems A screening test is used to find diseases, such as cancer, in people who do not have signs
301.681.3400 OBGYNCWC.COM Mammography and Other Screening Tests What is a screening test? for Breast Problems A screening test is used to find diseases, such as cancer, in people who do not have signs
European Commission Initiative on Breast Cancer (ECIBC) MEETING OF MONITORING SUBGROUP Ispra, 14 September 2016 (10:00-17:00) Minutes
 EUROPEAN COMMISSION DIRECTORATE GENERAL JOINT RESEARCH CENTRE Directorate F Health, Consumers and Reference Materials Unit F1 Health in Society European Commission Initiative on Breast Cancer (ECIBC) MEETING
EUROPEAN COMMISSION DIRECTORATE GENERAL JOINT RESEARCH CENTRE Directorate F Health, Consumers and Reference Materials Unit F1 Health in Society European Commission Initiative on Breast Cancer (ECIBC) MEETING
Certifications and training for mammography screening services and professionals in Norway
 Certifications and training for mammography screening services and professionals in Norway Solveig Hofvind Cancer Registry of Norway Thursday May 31, 2018, 15:40-16:00 Rome, Italy Health costs per inhabitants,
Certifications and training for mammography screening services and professionals in Norway Solveig Hofvind Cancer Registry of Norway Thursday May 31, 2018, 15:40-16:00 Rome, Italy Health costs per inhabitants,
Cytyc Corporation - Case Presentation Archive - March 2002
 FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
FirstCyte Ductal Lavage History: 68 Year Old Female Gail Index: Unknown Clinical History: Negative Mammogram in 1995 6 yrs. later presents with bloody nipple discharge Subsequent suspicious mammogram Suspicious
NHSCSP proposals for cervical screening intervals. Comments and recommendations of Council of the British Society for Clinical Cytology
 NHSCSP proposals for cervical screening intervals Comments and recommendations of Council of the British Society for Clinical Cytology The following paper is written on behalf of BSCC Council to express
NHSCSP proposals for cervical screening intervals Comments and recommendations of Council of the British Society for Clinical Cytology The following paper is written on behalf of BSCC Council to express
Audit Report. Breast Cancer Quality Performance Indicators. Patients diagnosed during Published: December 2015 NORTH OF SCOTLAND PLANNING GROUP
 NORTH OF SCOTLAND PLANNING GROUP Breast Cancer Managed Clinical Network Audit Report Breast Cancer Quality Performance Indicators Patients diagnosed during Published: December 2015 Mr Douglas Brown NOSCAN
NORTH OF SCOTLAND PLANNING GROUP Breast Cancer Managed Clinical Network Audit Report Breast Cancer Quality Performance Indicators Patients diagnosed during Published: December 2015 Mr Douglas Brown NOSCAN
CLINICAL SIGNIFICANCE OF BENIGN EPITHELIAL CHANGES
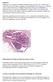 Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
Papillomas. Papillomas are composed of multiple branching fibrovascular cores, each having a connective tissue axis lined by luminal and myoepithelial cells ( Fig. 23-11 ). Growth occurs within a dilated
National Cervical Screening Programme. Annual Report 2014
 National Cervical Screening Programme Annual Report 2014 Report prepared February 2017 Revised May 2017 Finalised June 2017 Report prepared by Megan Smith, Leanne Rumlee and Karen Canfell. Cancer Research
National Cervical Screening Programme Annual Report 2014 Report prepared February 2017 Revised May 2017 Finalised June 2017 Report prepared by Megan Smith, Leanne Rumlee and Karen Canfell. Cancer Research
Programme Report
 Programme Report 2015-2016 Contents Introduction from the Head of Screening, National Screening Service 2 Highlights of 2015-2016 4 Programme report 5 References 19 Introduction from the Head of Screening,
Programme Report 2015-2016 Contents Introduction from the Head of Screening, National Screening Service 2 Highlights of 2015-2016 4 Programme report 5 References 19 Introduction from the Head of Screening,
Atypical proliferative lesions diagnosed on core biopsy - 6 year review
 Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
Atypical proliferative lesions diagnosed on core biopsy - 6 year review Dr Angela Harris, Dr Julie Weigner & Dr Ricardo Vilain NSW Health Pathology Pathology North, Hunter Anatomical Pathology & Cytology
United Kingdom and Ireland Association of Cancer Registries (UKIACR) Performance Indicators 2018 report
 United Kingdom and Ireland Association of Cancer Registries (UKIACR) Performance Indicators 2018 report 20 June 2018 UKIACR Performance Indicators 2018 report 1 Contents Introduction... 3 Commentary for
United Kingdom and Ireland Association of Cancer Registries (UKIACR) Performance Indicators 2018 report 20 June 2018 UKIACR Performance Indicators 2018 report 1 Contents Introduction... 3 Commentary for
Medical Audit of Diagnostic Mammography Examinations: Comparison with Screening Outcomes Obtained Concurrently
 Katherine E. Dee 1,2 Edward A. Sickles 1 Received July 3, 2000; accepted after revision September 12, 2000. Presented in part at the annual meeting of the American Roentgen Ray Society, Washington, DC,
Katherine E. Dee 1,2 Edward A. Sickles 1 Received July 3, 2000; accepted after revision September 12, 2000. Presented in part at the annual meeting of the American Roentgen Ray Society, Washington, DC,
I.2 CNExT This section was software specific and deleted in 2008.
 CANCER REPORTING IN CALIFORNIA: ABSTRACTING AND CODING PROCEDURES FOR HOSPITALS California Cancer Reporting System Standards, Volume I Changes and Clarifications 8th th Edition Revised May 2008 SECTION
CANCER REPORTING IN CALIFORNIA: ABSTRACTING AND CODING PROCEDURES FOR HOSPITALS California Cancer Reporting System Standards, Volume I Changes and Clarifications 8th th Edition Revised May 2008 SECTION
National Breast Cancer Audit next steps. Martin Lee
 National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
Audit Report. Breast Cancer Quality Performance Indicators. Patients diagnosed during Published: February 2018
 Breast Cancer Managed Clinical Network Audit Report Breast Cancer Quality Performance Indicators Patients diagnosed during 2016 Published: February 2018 Mr Douglas Brown NOSCAN Breast Cancer MCN Clinical
Breast Cancer Managed Clinical Network Audit Report Breast Cancer Quality Performance Indicators Patients diagnosed during 2016 Published: February 2018 Mr Douglas Brown NOSCAN Breast Cancer MCN Clinical
IL Balance Sheet dei programmi di screening mammografici dell Unione Europea
 Seminario di studio LA SORVEGLIANZA EPIDEMIOLOGICA DELLO SCREENING DEI TUMORI DELLA MAMMELLA NELLA REGIONE EMILIA-ROMAGNA Bologna, 18 marzo 2013 IL Balance Sheet dei programmi di screening mammografici
Seminario di studio LA SORVEGLIANZA EPIDEMIOLOGICA DELLO SCREENING DEI TUMORI DELLA MAMMELLA NELLA REGIONE EMILIA-ROMAGNA Bologna, 18 marzo 2013 IL Balance Sheet dei programmi di screening mammografici
GENERAL COMMENTS. The Task Force Process Should be Fully Open, Balanced and Transparent
 December 9, 2013 Submitted Electronically United States Preventive Services Task Force c/o Dr. Robert Cosby Agency for Healthcare Research and Quality 540 Gaither Road Rockville, MD 20850 RE: USPSTF Draft
December 9, 2013 Submitted Electronically United States Preventive Services Task Force c/o Dr. Robert Cosby Agency for Healthcare Research and Quality 540 Gaither Road Rockville, MD 20850 RE: USPSTF Draft
Diseases of the breast (2 of 2) Breast cancer
 Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
Diseases of the breast (2 of 2) Breast cancer Epidemiology & etiology The most common type of cancer & the 2 nd most common cause of cancer death in women 1 of 8 women in USA Affects 7% of women Peak at
Study Design of Randomized Controlled Clinical Trials of Breast Cancer Screening
 Study Design of Randomized Controlled Clinical Trials of Breast Cancer Screening Eugenio Paci, Freda E. Alexander* Evaluation of population screening must be based on a randomized clinical trial (RCT)
Study Design of Randomized Controlled Clinical Trials of Breast Cancer Screening Eugenio Paci, Freda E. Alexander* Evaluation of population screening must be based on a randomized clinical trial (RCT)
Breast Density. Information for Health Professionals
 Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
Breast Density Information for Health Professionals BreastScreen NSW provides free screening mammography to asymptomatic women aged 50-74 every two years, with the aim of diagnosing breast cancer at an
Introduction to Breast Density
 Introduction to Breast Density A/Prof Wendy Ingman Breast Biology & Cancer Unit Ethical and Legal Considerations in Breast Density Workshop 2018 In this presentation My interest in breast density What
Introduction to Breast Density A/Prof Wendy Ingman Breast Biology & Cancer Unit Ethical and Legal Considerations in Breast Density Workshop 2018 In this presentation My interest in breast density What
Screening Mammography for Women Aged 40 to 49 Years at Average Risk for Breast Cancer
 Ontario Health Technology Assessment Series 2007; Vol. 7, No. 1 Screening Mammography for Women Aged 40 to 49 Years at Average Risk for Breast Cancer An Evidence-Based Analysis January 2007 Medical Advisory
Ontario Health Technology Assessment Series 2007; Vol. 7, No. 1 Screening Mammography for Women Aged 40 to 49 Years at Average Risk for Breast Cancer An Evidence-Based Analysis January 2007 Medical Advisory
BREAST PATHOLOGY. Fibrocystic Changes
 BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
BREAST PATHOLOGY Lesions of the breast are very common, and they present as palpable, sometimes painful, nodules or masses. Most of these lesions are benign. Breast cancer is the 2 nd most common cause
Cancer in the Northern Territory :
 Cancer in the Northern Territory 1991 21: Incidence, mortality and survival Xiaohua Zhang John Condon Karen Dempsey Lindy Garling Acknowledgements The authors are grateful to the many people, who have
Cancer in the Northern Territory 1991 21: Incidence, mortality and survival Xiaohua Zhang John Condon Karen Dempsey Lindy Garling Acknowledgements The authors are grateful to the many people, who have
TRIAL SYNOPSIS LORIS. The Low Risk DCIS Trial. Chief Investigator. Miss Adele Francis
 TRIAL SYNOPSIS LORIS Chief Investigator The Low Risk DCIS Trial Miss Adele Francis ISRCTN No. 27544579 Sponsor University of Birmingham, United Kingdom Trial Design Objectives of Feasibility Study A multi-centre,
TRIAL SYNOPSIS LORIS Chief Investigator The Low Risk DCIS Trial Miss Adele Francis ISRCTN No. 27544579 Sponsor University of Birmingham, United Kingdom Trial Design Objectives of Feasibility Study A multi-centre,
Summary. Chapter 7. Breast cancer and screening
 Chapter 7 Breast cancer and screening World-wide burden Breast cancer is the commonest cancer among women in both high-income and low-income countries, accounting for 22% of the 4.7 million new cases of
Chapter 7 Breast cancer and screening World-wide burden Breast cancer is the commonest cancer among women in both high-income and low-income countries, accounting for 22% of the 4.7 million new cases of
Diagnostic Dilemmas of Breast Imaging
 Diagnostic Dilemmas of Breast Imaging Common Causes of Error in Breast Cancer Detection By: Jason Cord, M.D. Mammography: Initial Imaging The standard for detection of breast cancer Screening mammography
Diagnostic Dilemmas of Breast Imaging Common Causes of Error in Breast Cancer Detection By: Jason Cord, M.D. Mammography: Initial Imaging The standard for detection of breast cancer Screening mammography
Breast imaging in general practice
 Breast series CLINICAL PRACTICE Breast imaging in general practice Nehmat Houssami, MBBS, FAFPHM, FASBP, PhD, is Associate Clinical Director, NSW Breast Cancer Institute, Westmead Hospital, Honorary Senior
Breast series CLINICAL PRACTICE Breast imaging in general practice Nehmat Houssami, MBBS, FAFPHM, FASBP, PhD, is Associate Clinical Director, NSW Breast Cancer Institute, Westmead Hospital, Honorary Senior
Quantification of the effect of mammographic screening on fatal breast cancers: The Florence Programme
 British Journal of Cancer (2002) 87, 65 69 All rights reserved 0007 0920/02 $25.00 www.bjcancer.com Quantification of the effect of mammographic screening on fatal breast cancers: The Florence Programme
British Journal of Cancer (2002) 87, 65 69 All rights reserved 0007 0920/02 $25.00 www.bjcancer.com Quantification of the effect of mammographic screening on fatal breast cancers: The Florence Programme
Telephone: Learning objectives
 BreastScreen WA Breast Cancer Screening Investigation of a New Breast Symptom Dr Eric Khong, Liaison GP Telephone: 13 20 50 Learning objectives Increased understanding of the availability, benefits and
BreastScreen WA Breast Cancer Screening Investigation of a New Breast Symptom Dr Eric Khong, Liaison GP Telephone: 13 20 50 Learning objectives Increased understanding of the availability, benefits and
BCSC Glossary of Terms (Last updated 09/16/2009) DEFINITIONS
 Screening mammography scrmam_c BCSC Glossary of Terms (Last updated 09/16/2009) DEFINITIONS The radiologist s indication for exam is the primary determinant of whether a mammogram is screening or diagnostic.
Screening mammography scrmam_c BCSC Glossary of Terms (Last updated 09/16/2009) DEFINITIONS The radiologist s indication for exam is the primary determinant of whether a mammogram is screening or diagnostic.
Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol
 Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Krishnan et al. BMC Cancer (2017) 17:859 DOI 10.1186/s12885-017-3871-7 RESEARCH ARTICLE Mammographic density and risk of breast cancer by tumor characteristics: a casecontrol study Open Access Kavitha
Advanced Course on Multimodality Detection and Diagnosis of Breast Diseases
 BREAST SEMINAR Advanced Course on Multimodality Detection and 3D image of the breast tissue Invited speaker LÁSZLÓ TABÁR, MD,FACR (Hon) Falun, Sweden Nov 22-23, 2014 ATHENS, Greece Royal Olympic Hotel
BREAST SEMINAR Advanced Course on Multimodality Detection and 3D image of the breast tissue Invited speaker LÁSZLÓ TABÁR, MD,FACR (Hon) Falun, Sweden Nov 22-23, 2014 ATHENS, Greece Royal Olympic Hotel
TMIST: Frequently Asked Questions
 TMIST: Frequently Asked Questions Key Topics for Site Investigators and Staff This document answers frequently asked questions about the Tomosynthesis Mammographic Imaging Screening Trial (TMIST/EA1151);
TMIST: Frequently Asked Questions Key Topics for Site Investigators and Staff This document answers frequently asked questions about the Tomosynthesis Mammographic Imaging Screening Trial (TMIST/EA1151);
Increasing the uptake of. breast screening. Supporting the PHO Performance Programme. 32 BPJ Issue 33
 Increasing the uptake of breast screening Supporting the PHO Performance Programme 32 BPJ Issue 33 Achieving breast screening targets Significant improvements are being made in the rate of screening for
Increasing the uptake of breast screening Supporting the PHO Performance Programme 32 BPJ Issue 33 Achieving breast screening targets Significant improvements are being made in the rate of screening for
BREAST MRI. Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School
 BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
BREAST MRI Elizabeth A. Rafferty, M.D. Avon Comprehensive Breast Center Massachusetts General Hospital Harvard Medical School BREAST MRI Any assessment of the breast parenchyma requires the administration
SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT
 SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT BREAST CANCER 2016 COMPARATIVE AUDIT REPORT Mr Glyn Neades Chair SCAN Breast Group and Consultant Surgeon, NHS Fife & NHS Lothian Mr Ahmed
SOUTH EAST SCOTLAND CANCER NETWORK (SCAN) PROSPECTIVE CANCER AUDIT BREAST CANCER 2016 COMPARATIVE AUDIT REPORT Mr Glyn Neades Chair SCAN Breast Group and Consultant Surgeon, NHS Fife & NHS Lothian Mr Ahmed
Interpretation of Breast Pathology in the Era of Minimally Invasive Procedures
 Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Shahla Masood, M.D. Professor and Chair Department of Pathology and Laboratory Medicine University of Florida College of Medicine Jacksonville Medical Director, UF Health Breast Center Chief of Pathology
Icd 10 code for breast cancer stage 2
 Icd 10 code for breast cancer stage 2 The Borg System is 100 % Icd 10 code for breast cancer stage 2 Approximate Synonyms. Angiosarcoma of bilateral female breasts; Angiosarcoma of left female breast;
Icd 10 code for breast cancer stage 2 The Borg System is 100 % Icd 10 code for breast cancer stage 2 Approximate Synonyms. Angiosarcoma of bilateral female breasts; Angiosarcoma of left female breast;
LOBULAR CARCINOMA IN SITU: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE
 : WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
: WHAT DOES IT MEAN? THE SURGEON'S PERSPECTIVE Benjamin O. Anderson, M.D. Director, Breast Health Clinic Professor of Surgery and Global Health, University of Washington Joint Member, Fred Hutchinson Cancer
HTA commissioned call
 HTA commissioned call BACKGROUND 2002 NICE Guidance for Early Breast Cancer Discharge asymptomatic patients from hospital follow-up by 3 years. 2007 Questioning specialists attitudes to breast cancer follow-up
HTA commissioned call BACKGROUND 2002 NICE Guidance for Early Breast Cancer Discharge asymptomatic patients from hospital follow-up by 3 years. 2007 Questioning specialists attitudes to breast cancer follow-up
BreastScreen Queensland Gold Coast Service. General Practice Nurses Forum Thursday 4 May 2017
 BreastScreen Queensland Gold Coast Service General Practice Nurses Forum Thursday 4 May 2017 BreastScreen Queensland Gold Coast Service General Practice Nurses Forum Thursday 4 May 2017 BreastScreen in
BreastScreen Queensland Gold Coast Service General Practice Nurses Forum Thursday 4 May 2017 BreastScreen Queensland Gold Coast Service General Practice Nurses Forum Thursday 4 May 2017 BreastScreen in
Breast Tomosynthesis. What is breast tomosynthesis?
 Scan for mobile link. Breast Tomosynthesis Breast tomosynthesis is an advanced form of mammography, a specific type of breast imaging that uses low-dose x-rays to detect cancer early when it is most treatable.
Scan for mobile link. Breast Tomosynthesis Breast tomosynthesis is an advanced form of mammography, a specific type of breast imaging that uses low-dose x-rays to detect cancer early when it is most treatable.
Breast Pathology. Breast Development
 Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
Breast Pathology Lecturer: Hanina Hibshoosh, M.D. Reading: Kumar, Cotran, Robbins, Basic Pathology, 6th Edition, pages 623-635 Breast Development 5th week - thickening of the epidermis - milk line 5th
National Drug and Alcohol Treatment Waiting Times Report
 Publication Report National Drug and Alcohol Treatment Waiting Times Report October December 2016 Publication Date 28 March 2017 A National Statistics Publication for Scotland Contents Introduction...
Publication Report National Drug and Alcohol Treatment Waiting Times Report October December 2016 Publication Date 28 March 2017 A National Statistics Publication for Scotland Contents Introduction...
Histological Type. Morphological and Molecular Typing of breast Cancer. Nottingham Tenovus Primary Breast Cancer Study. Survival (%) Ian Ellis
 Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Morphological and Molecular Typing of breast Cancer Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology, Nottingham University Hospitals NHS Trust Histological Type
Mammography. What is Mammography?
 Scan for mobile link. Mammography Mammography is a specific type of breast imaging that uses low-dose x-rays to detect cancer early before women experience symptoms when it is most treatable. Tell your
Scan for mobile link. Mammography Mammography is a specific type of breast imaging that uses low-dose x-rays to detect cancer early before women experience symptoms when it is most treatable. Tell your
ARTICLE. Epidemiology of melanoma in situ in New Zealand: Sam Rice, Lifeng Zhou, Richard Martin ABSTRACT
 Epidemiology of melanoma in situ in New Zealand: 2008 2012 Sam Rice, Lifeng Zhou, Richard Martin ABSTRACT AIM: The incidence of melanoma in situ varies throughout the world. It is associated with excellent
Epidemiology of melanoma in situ in New Zealand: 2008 2012 Sam Rice, Lifeng Zhou, Richard Martin ABSTRACT AIM: The incidence of melanoma in situ varies throughout the world. It is associated with excellent
Cancer in Australia: Actual incidence data from 1991 to 2009 and mortality data from 1991 to 2010 with projections to 2012
 bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2013; 9: 199 213 doi: 10.1111/ajco.12127 ORIGINAL ARTICLE Cancer in Australia: Actual incidence data from 1991 to 2009 and mortality data from 1991
bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2013; 9: 199 213 doi: 10.1111/ajco.12127 ORIGINAL ARTICLE Cancer in Australia: Actual incidence data from 1991 to 2009 and mortality data from 1991
Breast Cancer Diagnosis, Treatment and Follow-up
 Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Screening and Breast Cancer Survival in Aboriginal and Torres Strait Islander Women of Australia
 RESEARCH COMMUNICATION Breast Screening and Breast Cancer Survival in Aboriginal and Torres Strait Islander Women of Australia David Roder 1,2, Fleur Webster 3 *, Helen Zorbas 1, Sue Sinclair 4 Associate
RESEARCH COMMUNICATION Breast Screening and Breast Cancer Survival in Aboriginal and Torres Strait Islander Women of Australia David Roder 1,2, Fleur Webster 3 *, Helen Zorbas 1, Sue Sinclair 4 Associate
Mammography. What is Mammography? What are some common uses of the procedure?
 Mammography What is Mammography? Mammography is a specific type of imaging that uses a low-dose x-ray system to examine breasts. A mammography exam, called a mammogram, is used to aid in the early detection
Mammography What is Mammography? Mammography is a specific type of imaging that uses a low-dose x-ray system to examine breasts. A mammography exam, called a mammogram, is used to aid in the early detection
