E ssential tremor is a commonly diagnosed movement
|
|
|
- Rosalind Hampton
- 5 years ago
- Views:
Transcription
1 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence to: Dr R J Uitti, Department of Neurology, Davis Bldg E- 8, Mayo Clinic Jacksonville, 4500 San Pablo Road, Jacksonville, FL 4, USA; uitti@ mayo.edu Received 1 March 004 In revised form 6 July 004 Accepted 1 August J Neurol Neurosurg Psychiatry 005;76: doi: /jnnp Objectives: To determine the efficacy of bilateral deep brain stimulation (DBS) for management of midline tremor (head, voice, tongue, trunk) in patients with essential tremor. Design: Prospective assessment of tremor at baseline (presurgical), and postoperatively at 1,, and 1 months, and annually thereafter. Methods: A clinical series of individuals undergoing staged, bilateral DBS for treatment of essential tremor. The tremor rating scale was the primary outcome measure. Results: Midline tremor showed significant improvement with stimulation on at nearly every postoperative interval when compared with stimulation off and with baseline tremor. Bilateral stimulation was associated with a significant incremental improvement in midline tremor control compared with unilateral stimulation: average stimulation on percentage change in midline tremor from the unilateral to bilateral period was 81%. Head and voice tremor showed the most consistent improvement. Among those requiring a change in stimulation parameters because of side effects, dysarthria, disequilibrium, motor disturbances, and paraesthesiae were the most common. Dysarthria was more common with bilateral (n = 6; 7%) than with unilateral (n = 0) stimulation. Stimulation parameters remained largely unchanged after the first three months. Nine of 44 leads placed (0%) required subsequent repositioning or replacement. Conclusions: Unilateral thalamic stimulation significantly improves midline tremor, and subsequent bilateral thalamic stimulation offers an additional incremental improvement in midline tremor control. E ssential tremor is a commonly diagnosed movement disorder 1 typically involving high frequency postural and intention tremor. It predominantly affects the distal upper extremities, but may also affect midline structures and functions, including the head, face, voice, and trunk (range 5 4% with various midline tremors). Deep brain stimulation (DBS) of the ventral intermediate (Vim) nucleus of the thalamus has been shown to be effective at reducing disabling tremor in the contralateral distal upper and lower extremities among individuals with essential tremor. 4 In some cases stimulation may also reduce ipsilateral tremor; however, the magnitude of effect is substantially smaller, of marginal clinical significance, 5 and not sustained over the long term (that is, more than 1 months). 6 7 There is increasing evidence that thalamic stimulation also improves midline tremor The ability to control midline tremor tends to be associated with symptom severity such that more severe tremors show the greatest improvement with stimulation, 8 whereas mild tremor shows little or no change. 15 Although several studies have shown that unilateral DBS may improve midline tremor, the most consistent effects occur with bilateral Vim stimulation. 15 Indeed, studies of staged, bilateral DBS have shown that improvement in midline tremor tends to occur primarily after placement of the second lead Unfortunately, potential bias in dropouts, variable data collection, and limited analyses that account for missing data are three methodological concerns that have limited our understanding of midline tremor control with thalamic DBS. Our current study was designed to extend previous research on midline tremor control by including a standardised data collection protocol (that is, at one, three, and 1 months and annually thereafter), an examination of dropout characteristics, and a range of missing data estimation methods to account for missing data. METHODS Participants and procedures A clinical series of 4 consecutive individuals with essential tremor undergoing bilateral thalamic DBS for intractable tremor was considered for study. The diagnosis of essential tremor was made by one neurologist (RJU), based on the Louis criteria. 16 The indication for surgery was disabling tremor despite optimal medical treatment, which involved individual and combination trials of propranolol, primidone, and gabapentin at maximum tolerated doses. All patients discontinued pharmacological antitremor therapy before preoperative tremor assessment. One patient who underwent previous stimulator placement at another institution was excluded from the study. One of the initial individuals was not followed according to the standard protocol (that is, one, three, and 1 months and annually thereafter) until after the placement of the second DBS lead 14 months later. No data were available between the first and second placement, and the patient was therefore not included in the study. One individual had simultaneous bilateral lead placement and was only included in the analyses of bilateral DBS and midline tremor. In all, therefore, individuals were included, representing a subset of the 5 patients previously reported with unilateral and bilateral stimulation. 6 More specifically, the current study is a detailed report of midline tremor control among those individuals with bilateral stimulation. The surgical procedures have been described in detail previously. 17 In brief, a stereotactic target in the Vim was planned with magnetic resonance guidance. In all patients test stimulations were carried out intraoperatively to evaluate tremor relief and side effects. After determining the optimal Abbreviations: DBS, deep brain stimulation; IPG, implantable pulse generator; TRS, tremor rating scale; Vim, ventral intermediate (nucleus) J Neurol Neurosurg Psychiatry: first published as /jnnp on 15 April 005. Downloaded from on 9 September 018 by guest. Protected by copyright.
2 Deep brain stimulation and midline tremor 685 Table 1 Electrode position across various groups Distal electrode Proximal electrode All leads Laterality from PC 14.4 (1.9) 16.6 (.1) Anterior distance from PC 5.9 (.) 11.5 (.6) Distance above () or below (+) AC/PC line 0. (.6) 6. (.5) Leads not requiring repositioning Laterality from PC 14.4 (1.9) 16.6 (.1) Anterior distance from PC 6.0 (.1) 11.6 (.) Distance above () or below (+) AC/PC line 0. (.6) 6. (.5) Leads requiring repositioning Laterality from PC 14. (.4) 16.6 (.7) Anterior distance from PC 5.0 (4.0) 10.6 (4.6) Distance above () or below (+) AC/PC line 0.5 (.5) 6.1 (.5) Values are distances in mm (mean (SD). There were no significant differences across groups. AC, anterior commissure; PC, posterior commissure. position, the stimulation electrode (model 87, Medtronic, Minneapolis, Minnesota, USA) was secured to the skull and connected to the infraclavicular pulse generator under general anaesthesia. Initial stimulation programming occurred the day after surgery and within two weeks after surgery for further stimulator programming. If necessary, stimulation parameters were adjusted for optimal tremor control with minimal side effects. If patients later observed side effects or a loss of tremor control, they returned for further pulse generator adjustment. Initial paraesthesiae, occurring when the stimulator was turned on and subsiding within a few seconds, were not considered side effects. Clinic visits to assess tremor control and side effects were scheduled after the initial lead placement for each side at one, three, and 1 months, and then annually thereafter. Follow up scores were measured with the stimulator switched off and switched on. Typically, the stimulator was deactivated overnight before the patient was examined in the morning. In cases in which the patient did not deactivate the stimulator overnight, it was deactivated for at least one hour before tremor assessment. All scores were recorded before any adjustments were made to the stimulation parameters, thus providing a conservative estimate of efficacy. The tremor rating scale (TRS) 18 is a well established patient and clinician based rating scale of tremor and activities of daily living. The TRS contains 1 items that use a five point Likert scale (0, no tremor/disability; 4, severe tremor/ disability) as well as a global disability item (0, no functional disability; 4, severe disability). The midline tremor total score (possible range 0 to ) was the sum the five tremor location scores: face, tongue, voice, head, and trunk tremor. The types of tremor assessed for each location included resting tremor for the face (possible range 0 to 4), intention tremor for voice (0 to 4), and postural and resting tremor for the tongue, head, and trunk (0 to 8). The activities of daily living (ADL) score (possible range 0 to ) summed eight items involving the ability to carry out day to day tasks (dressing, writing, hygiene, and so on). Statistical procedures The Wilcoxon signed rank test was used for three primary sets of comparisons. First, baseline functioning was compared with both the on and the off stimulation condition at each postoperative interval. Second, the stimulation on versus off condition was compared at each postoperative interval. Third, the unilateral three month on stimulation condition was compared to bilateral on stimulation scores at each postoperative bilateral interval in order to determine whether bilateral DBS offers a significant incremental effect over unilateral DBS. Significance was set at p,0.05; however, three significance levels are reported ( 1 p,0.05, p,0.01, p,0.001) so that results could be evaluated according to various correction methods (for example, Bonferroni). RESULTS Sample characteristics Examination of demographic characteristics indicated that the group was mostly male (n = 1, 55%), with a mean (SD) age of 70. (9.0) years and a tremor duration of 0.0 (14.) years at the time of the first surgery. Left sided brain stimulation was carried out first in the majority of cases (n = 0, 91%). As part of a staged bilateral DBS placement, the mean duration between placement of the first and second lead was days, most being undertaken within five months or less (n = 17; 77%) following initial surgery. The mean time between the initial lead placement and last available follow up was 9 months. Over the course of follow up, seven leads required repositioning owing to loss of effect, and two leads were broken and subsequently replaced. Other surgical procedures included replacement of one implantable pulse generator (IPG) and one DBS system (right side) was explanted because of infection after months. Table 1 presents a summary of the electrode position separated into three groups: all leads combined; leads that did not require repositioning; and leads requiring repositioning. In general, results suggest that most distal lead positions were in one of the usual Vim thalamic locations. Lead position was not significantly different between the leads that did or did not require repositioning. Rather than arbitrarily establishing a cut off date for study inclusion, all available data at the time of analysis were included. Thus individuals were separated into mutually exclusive and collectively exhaustive status groups based on their evaluation status at each postoperative interval. Three status groups were defined several months after the initial lead placement: those whose evaluation was obtained; those whose evaluation was not obtained; and those in whom a second lead was already placed. For the period after placement of the second lead, the five status groups were as follows: those with evaluations not due yet; those with evaluations due and outcome measures obtained; those with evaluations due and outcome measures not obtained; lost to follow up; and deceased. For clarification, the evaluation not due yet group included those who had yet to reach a particular postoperative interval. For example, an individual who was three months out from their second lead placement would be considered in the evaluation not due yet group at the 1 month bilateral postoperative interval. Table presents several summary characteristics including the number of individuals in the various status groups at each postoperative interval, the mean days from the expected date the evaluation was carried out, and the proportion of evaluations due that were actually obtained. Three individuals died of unrelated causes (lung cancer, gunshot wound, and colon cancer). One was considered lost to follow up because of transfer of care. During a structured telephone interview the individual lost to follow up reported continued good tremor control and improvement in activities of daily living with stimulation, and no subsequent device related surgery (for example, lead repositioning, battery replacement). Two sets of comparisons were made to determine whether those available for analysis at each postoperative interval were representative of the overall sample. First, the demographic characteristics (sex, duration of symptoms, and age at first surgery) of those with completed evaluations at each postoperative interval were compared with the overall group J Neurol Neurosurg Psychiatry: first published as /jnnp on 15 April 005. Downloaded from on 9 September 018 by guest. Protected by copyright.
3 686 Putzke, Uitti, Obwegeser, et al Table Summary of data collection at various intervals (n = patients) characteristics at baseline. Second, the demographic characteristics of those with complete versus incomplete evaluations (lost to follow up, evaluation not obtained, deceased) at each postoperative interval were compared to assess differential drop out rates. None of the demographic comparisons examined was significant (p.0.05). Efficacy over time As previously shown, 6 contralateral upper extremity tremor was significantly improved with stimulation on at nearly every postoperative interval when compared with the stimulation off condition and with baseline tremor (fig 1). An additional incremental effect following placement of the second lead was not observed. However, contralateral upper extremity tremor remained consistently controlled with stimulation during the bilateral stimulation period. The extent of midline tremor was evaluated at baseline. Results indicated that 95% of the sample had a score of 1 or more on the TRS midline tremor total score, and 57% had a score of 4 or more. The midline tremor total score showed significant improvement with stimulation on at nearly every postoperative unilateral and bilateral interval when compared with the stimulation off condition and with baseline tremor. Moreover, placement of the second lead was associated with incremental improvement in midline tremor control as compared with unilateral stimulation (the three month postoperative unilateral interval was chosen so as to be outside the window of possible microthalamotomy effects) Contralateral tremor Baseline 1 Month Months 1 Months 4 Months 6 Months Unilateral DBS (period between first and second lead placement) Evaluation obtained 1 (96) 1 (96) 16 (7) 4 (18) 0 (0) 0 (0) Evaluation not obtained 1 (4) 0 (0) 0 (0) 0 (0) (9) 0 (0) Second lead already placed 1 (4) 6 (7) 18 (8) 0 (91) (100) Days from expected date (mean (SD)) 1. (1.0) 4. (.) 14.4 (.5) 11.0 (9.8) Bilateral DBS (period after placement of second lead) Evaluation not due yet 0 (0) 0 (0) (9) 5 () 1 (54) Evaluation obtained 18 (8) 0 (91) 1 (54) 1 (59) 5 () Evaluation not obtained 4 (18) (9) 5 () 0 (0) 1 (4) Deceased 0 (0) 0 (0) (14) (14) (14) Lost to follow up 0 (0) 0 (0) 0 (0) 1 (4) 1 (4) Percentage of evaluations due that were obtained 8% 91% 60% 76% 50% Days from expected date (mean (SD)).4 (.5) 9.9 (1.) 6.0 (101.9) 75.7 (118.4) 4.0 (4.9) Values are n (%) except where indicated Baseline Off stimulation On stimulation Unilateral Mn, Mn Bilateral, at most postoperative bilateral intervals (fig ). Indeed, the average on percentage change from the unilateral to the various bilateral follow up periods was 81% (range 59% to 100%) and the average effect size estimate (the difference between the unilateral and bilateral mean divided by the pooled average standard deviation) was 1. (range 0.77 to 1.95), representing a large effect size difference. Bivariate correlations were calculated between baseline midline tremor score, and the off v on stimulation difference score at each postoperative interval in order to determine the relation between initial tremor severity and treatment effect. (Correlations not generated for the 6 month postoperative bilateral stimulation interval due to small sample size.) With one exception (that is, 1 months postoperative bilateral stimulation, r = 0.1, p = 0.74), the correlation coefficients were all significant (mean r = 0.69; range = 0.57 to 0.8). Analysis of midline tremor at the longest postoperative interval (that is, 6 months post bilateral stimulation) was limited owing to the small sample size (n = 5) and attrition (50%). Intention to treat analyses were carried out in an attempt to account for missing data at the year bilateral stimulation interval. More specifically, all those with evaluations due at the 6 month bilateral interval were included for analysis (that is, those with evaluations obtained and not obtained, deceased, and lost to follow up). A range of liberal to conservative estimates for the total midline tremor score was used for missing data. The most conservative technique was the insert baseline functioning method, followed by Mn 4 Mn 6 Figure 1 Contralateral tremor. 1 p,0.05 v baseline; p,0.01 v baseline; p,0.001 v baseline; *p,0.01 v on stimulation; Àp,0.001 v on stimulation. J Neurol Neurosurg Psychiatry: first published as /jnnp on 15 April 005. Downloaded from on 9 September 018 by guest. Protected by copyright.
4 Deep brain stimulation and midline tremor 687 Midline tremor Off stimulation On stimulation Baseline Unilateral, 1, 1, 1,,, the carry forward the worst stimulation on and off score ; the most liberal estimate of missing data was the carry forward the most recently available stimulation on and off score technique. In all, three comparisons were made for each intent to treat technique: the stimulation on condition at 6 months was compared with both the stimulation off condition and baseline, and the stimulation off condition was compared with baseline. None of the three comparisons was significant using the most conservative approach (p.0.05); two of the three were significant using the next most conservative approach, and all three were significant using the most liberal approach (p,0.05). Mn Table Summary of clinical tremor rating scale (unilateral stimulation) Tremor location Baseline Month 1 Month Head Off stimulation.1 (.1) 1.4 (.0) 1 * 1. (1.6) 1 On stimulation 0.8 (1.) 0.9 (1.1) Voice Off stimulation 1.7 (1.) 1.7 (1.0)À 1.1 (1.1) On stimulation 0.7 (1.0) (1.1) Tongue Off stimulation 0.9 (1.4) 0.6 (1.) 0.4 (0.7) On stimulation 0. (0.4) 1 0. (0.6) Face Off stimulation 0.7 (1.1) 0.6 (0.8)` 0.6 (0.8)* On stimulation 0.1 (0.) 0.1 (0.) 1 Trunk Off stimulation 0.4 (1.0) 0. (1.1) 0.4 (0.7) On stimulation 0.0 (0.0) 0.0 (0.0) Ipsilateral UE tremor Off stimulation 6.4 (.) 6.4 (.5)* 5.8 (.0) On stimulation 5.7 (.) (.9) ADL Off stimulation 18.0 (.) On stimulation 7.1 (5.) 6.4 (6.0) Mn Values are mean (SD). 1 p,0.05 v baseline; p,0.01 v baseline; p,0.001 v baseline; *p,0.05 v on stimulation; Àp,0.001 v on stimulation; `p,0.01 v on stimulation. ADL, activities of daily living; UE, upper extremity. Bilateral, Mn 4 Mn 6 Figure Midline tremor. 1 p,0.05 v baseline; p,0.01 v baseline; p,0.001 v baseline; *p,0.01 v on stimulation; Àp,0.001 v on stimulation; `p,0.05 v on stimulation; 1p,0.05 v on stimulation unilateral month ; ôp,0.01 v on stimulation unilateral month. Table (unilateral stimulation) and table 4 (bilateral stimulation) provide a more detailed summary of the individual items that comprise the TRS midline tremor total score for the stimulation on and off conditions at the various postoperative intervals. Upper extremity ipsilateral tremor and ADL scores are also provided. As can be seen, the most consistent improvement during both unilateral and bilateral stimulation was found for head and voice tremor. Moreover, the bilateral stimulation on condition for head and voice tremor showed a significant incremental improvement over unilateral stimulation through the first 1 months of bilateral stimulation. Small sample size limited power for these analyses at 4 and 6 months after the second DBS placement. It should be noted, however, that effect size estimates (mean of unilateral on stimulation mean minus mean of bilateral on stimulation divided by pooled standard deviation) remained largely the same. Trunk, tongue, and face tremor also showed significant improvement with stimulation, although floor effects and the small number of individuals with these types of tremor limited statistical power. For example, only three individuals at baseline were rated with observable trunk tremor. These three individuals had no observable trunk tremor with stimulation during both the unilateral and bilateral period. Side effects and stimulator settings In all, 5 clinic visits (both scheduled and unscheduled) were made, and 81% (n = 18) involved a change to the stimulator settings for at least one IPG. Of the 18 changes made, the stimulator setting adjustment was required in order to eliminate side effects in 17% (n = 1), to improve tremor control in 68% (n = 14), or both in 8% (n = 15), or else data were missing (7% (n = 1)). The most common self reported problems among those undergoing a stimulation change to eliminate side effects were dysarthria (45%), disequilibrium (41%), motor disturbances (%), and paraesthesiae (%). The side effect profile during unilateral and bilateral stimulation was compared. In order to control for variability in time between the staged procedure, the interval over which side effects were examined was standardised for each patient as the shorter of two periods: either the number of days between the placement of the first and second lead, or the number of days between placement of the second lead and the date of the last available assessment of side effects. Thus intervals of similar length were compared during periods with unilateral and bilateral DBS. McNemar s test J Neurol Neurosurg Psychiatry: first published as /jnnp on 15 April 005. Downloaded from on 9 September 018 by guest. Protected by copyright.
5 688 Putzke, Uitti, Obwegeser, et al Table 4 Summary of clinical tremor rating scale (bilateral stimulation) Tremor location Month 1 Month Year 1 Year Year Head Off stimulation 1.1 (1.) 1` 1.0 (1.) 1` 1. (1.4) 1` 0.8 (1.0) 1 0. (0.5) On stimulation 0.1 (0.) 1 0. (0.4) (0.) 1 0. (0.4) 0.0 (0.0) Voice Off stimulation 1.5 (0.9)À 1.4 (1.)À 1.6 (0.9)` 1. (0.8)* 1.0 (0.8) On stimulation 0.6 (0.8) ô 0. (0.7) ô 0. (0.7) (0.7) 0.0 (0.0) Tongue Off stimulation 0. (0.6) 0. (0.7) (1.0) 0.5 (0.8) 0.0 (0.0) On stimulation 0.1 (0.) (0.0)À 0.0 (0.0) 1 0. (0.5) 0.0 (0.0) Face Off stimulation 0. (0.7) 0. (0.5) (0.0) 0.0 (0.0) 0.0 (0.0) On stimulation 0.1 (0.) (0.0) (0.0) 0.0 (0.0) (0.0) Trunk Off stimulation 0.1 (0.5) 0.1 (0.) 0.0 (0.0) 0.1 (0.) 0.0 (0.0) On stimulation 0.0 (0.0) 0.0 (0.0) 0.0 (0.0) 0.0 (0.0) 0.0 (0.0) Ipsilateral UE tremor Off stimulation 5. (.) 1 À 5. (.5)À 4. (.5) 1` 5.6 (.)` 4.0 (.0) On stimulation 1. (1.) ô 1.0 (1.4) ô 0.6 (0.8) ô 1. (1.) (0.7) ADL Off stimulation On stimulation 4.6 (5.1) 4. (5.7). (4.5) 5.5 (4.4).6 (1.5) Values are mean (SD). 1 p,0.05 v baseline; p,0.01 v baseline; p,0.001 v baseline; *p,0.05 v on stimulation; Àp,0.001 v on stimulation; `p,0.01 v on stimulation; 1p,0.05 v on stimulation; ôp,0.01 v on stimulation unilateral month. ADL, activities of daily living; UE, upper extremity. Table 5 Side effects reported during staged bilateral lead placement over standardised intervals Side effect Unilateral Bilateral Dysarthria 0 (0) 6 (7)* Disequilibrium (9) 5 () Paraesthesiae (14) 1 (5) Motor disturbance 1 (5) (9) Values are n (%). Average standardised interval length = 146 days; total n =. *p = 0.0 v unilateral. for symmetry was used to compare the proportion of individuals experiencing each side effect during unilateral v bilateral stimulation (table 5). Dysarthria was more common after bilateral than after unilateral stimulation (p,0.05). None of the other comparisons was significant. Stimulation parameters were recorded both as part of the standard clinical protocol and during patient initiated visits for parameter adjustments. Stimulator settings closest to the expected standard clinical protocol (that is, 1,, 1, 4, 6 months) were used for analysis. Two sets of analyses were carried out using the Wilcoxon signed rank test. First, the stimulation parameters (amplitude, rate, pulse width) for each DBS system (right and left) were compared between each adjacent postoperative interval (for example, year 1 v year ). Second, stimulation parameters at month 1 were compared with all other intervals for each DBS system. Overall, a total of 18 unique comparisons was made for each stimulation parameter. Tables 6 and 7 present a summary of the stimulation parameters at each postoperative interval for the two DBS systems placed. As can be seen, most of the comparisons were non-significant. Indeed, none of the comparisons was Table 6 Summary of stimulator settings over time, unilateral stimulation Setting Month 1 Month Amplitude First side.6 (0.8).8 (1.1) Second side Rate First side (0.9) 158. (0.8) Second side Pulse width First side 78.5 (19.5) 80.9 (.0) Second side Days from expected date 6.4 (5.9) 7.6 (6.) Values are mean (SD). significant for pulse width. Only two of the 18 paired comparisons were significant for both amplitude and rate (both showing an increase between month 1 and month for the second DBS system). Amplitude at year was higher than at month 1, and rate at year 1 was higher than at month 1. Lastly, change in parameter settings in the first DBS system after surgical placement of the second DBS system was further examined by using the closest evaluation (rather than the evaluation closest to the clinical protocol) just before and after the placement of the second DBS system. This approach served to control for interval length variability between placement of the first and second DBS systems. None of the three comparisons (amplitude, rate, pulse width) showed a difference in the stimulation parameters of the first DBS system after the second DBS system was placed (p.0.05). J Neurol Neurosurg Psychiatry: first published as /jnnp on 15 April 005. Downloaded from on 9 September 018 by guest. Protected by copyright.
6 Deep brain stimulation and midline tremor 689 Table 7 Summary of stimulator settings over time (bilateral stimulation) Setting Month 1 Month Year 1 Year Year Amplitude First side.8 (1.).8 (1.). (1.1).1 (0.9).8 (1.0) Second side.0 (0.7).5 (0.7)*.5 (0.8).8 (0.9)*.4 (0.7) Rate First side 15.4 (7.) (7.0) (1.8) 17.5 (0.4) (19.8) Second side (1.9) 15.5 (6.5)* 16.0 (0.1)* 16.8 (19.4) (19.4) Pulse width First side 9.8 (.0) 96. (8.) 96.9 (1.8) 95.0 (5.0) 97.5 (6.6) Second side 86.8 (19.9) 78.0 (15.) 94.7 (6.4) 87.7 (19.) 97.5 (1.1) Days from expected date 6. (7.1) 10. (10.5) 47.8 (60.0) 6.5 (6.) 40.9 (8.) *p,0.05 v month 1. None of the adjacent pairs was significantly different except as noted between month 1 and month. DISCUSSION Between 5% and 4% of individuals with essential tremor may present with midline tremor. Both unilateral and bilateral thalamic stimulation have been shown to improve this condition. However, methodological limitations have complicated interpretation of the data. The current study was designed to improve the methodological approach of previous research by incorporating additional analytical (missing data estimation methods, examination of drop outs) and design related techniques (results reported according to a standardised clinical protocol). Three main findings emerged. First, unilateral thalamic stimulation was associated with significant improvement in midline tremor when compared both with the off stimulation condition and with baseline tremor The reported follow up period for unilateral stimulation in the current study was relatively short (three months); however, others have shown stable midline tremor control with unilateral stimulation for 1 months or more. 6 1 Second, bilateral stimulation was also associated with a significant improvement in midline tremor when compared both with the off stimulation condition and with baseline tremor. In fact, bilateral stimulation offered an additional incremental effect in midline tremor control over unilateral stimulation. For instance, the average stimulation on percentage change from the unilateral to the various bilateral follow up periods was 81%. Third, the effect of stimulation on midline tremor was stable over time, although results at the longest postoperative interval were limited owing to the small sample size and missing data. In order to further examine the results at the longest postoperative interval, missing data estimation methods were undertaken using a range of liberal to conservative estimates. Results were mixed, with the more liberal intention to treat analysis (carry forward the most recent) confirming midline tremor control, whereas the other two more conservative techniques failed to show consistent statistical support. Thus results at the 6 month bilateral stimulation interval are speculative. The TRS midline tremor total score includes items that assess face, tongue, voice, head, and trunk tremor. The most consistent results were found for head and voice tremor, which were also the most commonly experienced midline tremors (81% and 90% of the sample with a score of 1 or more, respectively, on at least one item). 10 Face, tongue, and trunk tremor were less common in the sample (8%, 47%, and 14% of the sample with a score of 1 or more on at least one item), thus limiting the statistical power to find an effect, but generally showed improvement with stimulation (for example, none of the three individuals with trunk tremor at baseline had observable trunk tremor with stimulation during both the unilateral and bilateral periods). Related to this, the effect of thalamic stimulation on midline tremor tended to increase with symptom severity. More specifically, those with the most severe midline tremor at baseline had the greatest difference between the stimulation on v off condition which may explain, in part, the limited effect between stimulation and midline tremor control found in the European trial that reportedly involved primarily those with mild midline tremor. 15 It should be noted, however, that an attenuated relation between baseline tremor, and on v off difference scores may also be attributed to restricted scaling in the mild tremor range (for example, ceiling effects). Indeed, the psychometric characteristics of the TRS for the various types of midline tremor are limited. Future research on midline tremor would benefit from the development of measures that allow more extensive assessment of the various types and locations of midline tremor. The mechanisms of action are not well understood, but DBS is generally thought potentially to involve any of the following: stimulation of neural tracts, depolarisation block, disruption of neural networks ( neural jamming ), generation of action potentials at the cathode, and build up of neurotransmitters and neuromodulators over time that produce changes to neural network properties. 19 Adverse side effects related to stimulation were generally mild and easily altered by adjusting stimulus parameters. The most common side effects reported were dysarthria, disequilibrium, motor disturbances, and paraesthesiae. Consistent with our previous report, 6 the proportion of individuals who experienced each side effect at least once during the course of DBS was used as the level of analysis, rather than a simple count of each side effect occurrence. This approach limited the impact of over-representation caused by variation in treatment seeking behaviour (for example, report of the same side effect on repeated occasions by one individual). In order to control for interval variability between the first and second lead placement, the length of time over which side effects were compared under the unilateral v bilateral stimulation condition was standardised for each individual as the shorter of two intervals: time between the first and second surgery, or time between the second surgery and the last available follow up. Results showed that dysarthria appeared only after bilateral stimulation. An increase in adverse events after placement of a 11 1 second DBS system has been reported previously, although these were not considered serious adverse events. The proportion of individuals who experienced other side effects was not significantly different between the unilateral and the bilateral stimulation periods. Taken together, the increased benefits of tremor control associated with the J Neurol Neurosurg Psychiatry: first published as /jnnp on 15 April 005. Downloaded from on 9 September 018 by guest. Protected by copyright.
7 690 Putzke, Uitti, Obwegeser, et al placement of a second lead should be weighed against the increased risk of dysarthria. Examination of the stimulator settings at adjacent postoperative intervals for each DBS system (left and right) showed little or no change over long term follow up intervals. Moreover, the stimulation parameters of the initial DBS system did not change after placement of the second stimulator lead. The rate and amplitude of the second stimulator showed some change, mostly over the first three months, levelling off thereafter. Pulse width remained largely unchanged across all postoperative intervals. These findings are consistent with other studies that showed an increase in stimulation parameters only within the first several months after surgery, 0 1 although others have shown evidence of the need for a systematic increase in stimulation parameters 14 to maintain tremor control. An attempt was made to determine whether the results at each postoperative interval were representative. In fact, analyses of the demographic characteristics of those whose midline tremor evaluations were obtained at each postoperative interval showed no difference when compared with those whose evaluations were not obtained, or with the overall sample at baseline. The lack of differences in demographic characteristics served to minimise concerns that selective attrition may have influenced the results, and increased the likelihood that they can be generalised to apply to the overall sample. It should be noted, however, that the small sample size at the longer postoperative intervals limits the power to detect differences. If one considers the nine leads that required reoperation as failures, then the failure rate for tremor control in this series was 0% (9/44). In our experience, lead fractures that had been occurring in the extreme proximal region of the brain electrode (close to the extension lead connector site) happened in this historic cohort but not since we have employed the revised smaller profile connector, which has also shown less propensity to migrate. In all patients, however, long term tremor control was achieved and stimulation tolerance to the extent of preventing tremor control was not observed. Moreover, the vast majority of patients have maintained stable tremor control. Examination of lead position showed no differences between leads that did or did not require repositioning. In general, the benefits of stimulation are thought to outweigh health care provider and patient burden costs related to device maintenance and failure. 4 However, the costs associated with DBS, particularly over the long term, have yet to be clearly determined and will be an important focus of future research. Conclusions Thalamic stimulation is generally an effective approach for management of midline tremor associated with essential tremor. Although unilateral stimulation results in improvement, bilateral stimulation offers a significant further increment in midline tremor control. The results tend to be maintained over time and do not require a systematic increase in stimulation parameters. Adverse affects are generally mild and can be controlled by adjustment to the stimulation parameters. Bilateral stimulation, however, may be associated with modest speech difficulties that can typically be minimised with adjustment in stimulation parameters. ACKNOWLEDGEMENTS We would like to thank Margaret Turk and Audrey Stongosky for their careful work in organising and collecting patient data. Resources for the production of this manuscript were provided, in part, by the Smith Fellowship given to John Putzke. This work was also supported by the Udall Center Grant at Mayo Clinic, Jacksonville, Florida, USA.... Authors affiliations J D Putzke, R J Uitti, Z K Wszolek, Department of Neurology, Mayo Clinic Jacksonville, Florida, USA R E Wharen, A A Obwegeser*, Department of Neurosurgery, Mayo Clinic Jacksonville *Also at Department of Neurosurgery, University Innsbruck, Austria Competing interests: none declared REFERENCES 1 Findley LJ. Epidemiology and genetics of essential tremor. Neurology 000;54:S8 1. Elble RJ. Diagnostic criteria for essential tremor and differential diagnosis. Neurology 000;54:S 6. Benabid AL, Pollak P, Gao DM, et al. Chronic electrical stimulation of the ventralis intermedius nucleus of the thalamus as a treatment of movement disorders. J Neurosurg 1996;84: Obwegeser AA, Uitti RJ, Witte RJ, et al. Quantitative and qualitative outcome measures after thalamic deep brain stimulation to treat disabling tremors. Neurosurgery 001;48: Ondo W, Dat VK, Almaguer M, et al. Thalamic deep brain stimulation: effects on the nontarget limbs. Move Disord 001;16: Putzke JD, Wharen RE, Uitti RJ, et al. Thalamic deep brain stimulation for essential tremor: recommendations for long-term outcome analysis. Can J Neurol Sci 004;1: 4. 7 Kumar R, Lozano AM, Sime E, et al. Comparative effects of unilateral and bilateral subthalamic nucleus deep brain stimulation. Neurology 1999;5: Carpenter MA, Pahwa R, Miyawaki KL, et al. Reduction in voice tremor under thalamic stimulation. Neurology 1998;50: Obwegeser AA, Uitti RJ, Turk MF, et al. Thalamic stimulation for the treatment of midline tremors in essential tremor patients. Neurology 000;54: Taha JM, Janszen MA, Favre J. Thalamic deep brain stimulation for the treatment of head, voice, and bilateral limb tremor. J Neurosurg 1999;91: Ondo W, Almaguer M, Jankovic J, et al. Thalamic deep brain stimulation comparison between unilateral and bilateral placement. Arch Neurol 001;58:18. 1 Pahwa R, Lyons KL, Wilkinson SB, et al. Bilateral thalamic stimulation for the treatment of essential tremor. Neurology 1999;5: Koller WC, Lyons KE, Wilkinson SB, et al. Efficacy of unilateral deep brain stimulation of the VIM nucleus of the thalamus for essential head tremor. Move Disord 1999;14: Kumar K, Kelly M, Toth C. Deep brain stimulation of the ventral intermediate nucleus of the thalamus for control of tremors in Parkinson s disease and essential tremor. Stereotact Funct Neurosurg 1999;7: Limousin P, Speelman JD, Gielen F, et al. Multicentre European study of thalamic stimulation in parkinsonian and essential tremor. J Neurol Neurosurg Psychiatry 1999;66: Louis ED, Ford B, Lee H, et al. Diagnostic criteria for essential tremor: a population perspective. Arch Neurol 1998;55: Obwegeser AA, Uitti RJ, Turk MF, et al. Simultaneous thalamic deep brain stimulation and implantable cardioverter-defibrillator. Mayo Clin Proc 001;76: Fahn S, Tolosa E, Marin C. Clinical rating scale for tremor. In: Jankovic J, Tolosa E, eds. Parkinson s disease and movement disorders. Baltimore: Urban and Schwarzenberg, 199: Benazzouz A, Hallett M. Mechanism of action of deep brain stimulation. Neurology 000;55:S Benabid AL, Benazzouz A, Gao DM, et al. Chronic electrical stimulation of the ventralis intermedius nucleus of the thalamus and of other nuclei as a treatment for Parkinson s disease. Techniques Neurosurg 1999;5: Koller WC, Lyons KE, Wilkinson SB, et al. Long-term safety and efficacy of unilateral deep brain stimulation of the thalamus in essential tremor. Move Disord 001;16: Blond S, Caparros-Lefebvre D, Parker F, et al. Control of tremor and involuntary movement disorders by chronic stereotactic stimulation of the ventral intermediate thalamic nucleus. J Neurosurg 199;77:6 8. Hariz MI, Shamsgovara P, Johansson F, et al. Tolerance and tremor rebound following long-term chronic thalamic stimulation for parkinsonian and essential tremor. Stereotact Funct Neurosurg 1999;7: Tomaszewski KJ, Holloway RG. Deep brain stimulation in the treatment of Parkinson s disease: a cost effectiveness analysis. Neurology 001;57: J Neurol Neurosurg Psychiatry: first published as /jnnp on 15 April 005. Downloaded from on 9 September 018 by guest. Protected by copyright.
I n 1991 Benabid et al introduced deep brain stimulation
 PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
M ultiple sclerosis can be associated with tremor in the
 1392 PAPER Chronic deep brain stimulation for the treatment of tremor in multiple sclerosis: review and case reports H A Wishart, D W Roberts, R M Roth, B C McDonald, D J Coffey, A C Mamourian, C Hartley,
1392 PAPER Chronic deep brain stimulation for the treatment of tremor in multiple sclerosis: review and case reports H A Wishart, D W Roberts, R M Roth, B C McDonald, D J Coffey, A C Mamourian, C Hartley,
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
Outcome of Gamma Knife Thalamotomy in Patients with an Intractable Tremor
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.3.192 J Korean Neurosurg Soc 57 (3) : 192-196, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2015.57.3.192 J Korean Neurosurg Soc 57 (3) : 192-196, 2015 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2015 The Korean Neurosurgical Society Clinical
SUPPLEMENTAL DIGITAL CONTENT
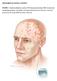 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
Multicentre European study of thalamic stimulation in parkinsonian and essential tremor
 J Neurol Neurosurg Psychiatry 999;66:89 96 89 Department of Clinical and Biological Neurosciences, Joseph Fourier University, Grenoble, France P Limousin MRC HMBU, Institute of Neurology, Queen Square,
J Neurol Neurosurg Psychiatry 999;66:89 96 89 Department of Clinical and Biological Neurosciences, Joseph Fourier University, Grenoble, France P Limousin MRC HMBU, Institute of Neurology, Queen Square,
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy (all ages) NHS England Reference: P
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy (all ages) NHS England Reference: 1736P NHS England INFORMATION READER BOX Directorate Medical Operations and Information
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy (all ages) NHS England Reference: 1736P NHS England INFORMATION READER BOX Directorate Medical Operations and Information
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
UNIFORM QUALITATIVE ELECTROPHYSIOLOGICAL CHANGES IN POSTOPERATIVE REST TREMOR
 UNIFORM QUALITATIVE ELECTROPHYSIOLOGICAL CHANGES IN POSTOPERATIVE REST TREMOR Norbert Kovacs, 1 Istvan Balas, 2 Zsolt Illes 1, Lorant Kellenyi, 2 Tamas P Doczi, 2 Jozsef Czopf, 1 Laszlo Poto 3 and Ferenc
UNIFORM QUALITATIVE ELECTROPHYSIOLOGICAL CHANGES IN POSTOPERATIVE REST TREMOR Norbert Kovacs, 1 Istvan Balas, 2 Zsolt Illes 1, Lorant Kellenyi, 2 Tamas P Doczi, 2 Jozsef Czopf, 1 Laszlo Poto 3 and Ferenc
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech?
 Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Troubleshooting algorithms for common DBS related problems in tremor and dystonia
 Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
A COMPARISON OF THALAMIC STIMULATION AND THALAMOTOMY FOR SUPPRESSION OF SEVERE TREMOR
 A COMPARISON OF THALAMIC STIMULATION AND THALAMOTOMY FOR SUPPRESSION OF SEVERE TREMOR A COMPARISON OF CONTINUOUS THALAMIC STIMULATION AND THALAMOTOMY FOR SUPPRESSION OF SEVERE TREMOR P. RICHARD SCHUURMAN,
A COMPARISON OF THALAMIC STIMULATION AND THALAMOTOMY FOR SUPPRESSION OF SEVERE TREMOR A COMPARISON OF CONTINUOUS THALAMIC STIMULATION AND THALAMOTOMY FOR SUPPRESSION OF SEVERE TREMOR P. RICHARD SCHUURMAN,
Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II
 Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor
 Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor Karen L. Francis, PhD* Waneen W. Spirduso, EdD Tim Eakin, PhD Pamela Z.
Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor Karen L. Francis, PhD* Waneen W. Spirduso, EdD Tim Eakin, PhD Pamela Z.
Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients
 J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
Linköping University Post Print. Patient-specific models and simulations of deep brain stimulation for postoperative follow-up
 inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
PARKINSON S SYMPTOM TRACKER
 PARKINSON S SYMPTOM You can help your doctor make good treatment decisions by tracking your symptoms. A well-kept Symptom Tracker provides a clear picture of when you are taking your medications, when
PARKINSON S SYMPTOM You can help your doctor make good treatment decisions by tracking your symptoms. A well-kept Symptom Tracker provides a clear picture of when you are taking your medications, when
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Activa RC and Activa PC
 Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
Neuromodulation Approaches to Treatment Resistant Depression
 1 Alternative Treatments: Neuromodulation Approaches to Treatment Resistant Depression Audrey R. Tyrka, MD, PhD Assistant Professor Brown University Department of Psychiatry Associate Chief, Mood Disorders
1 Alternative Treatments: Neuromodulation Approaches to Treatment Resistant Depression Audrey R. Tyrka, MD, PhD Assistant Professor Brown University Department of Psychiatry Associate Chief, Mood Disorders
Surgical treatments for essential tremor
 EXPERT REVIEW OF NEUROTHERAPEUTICS, 2018 https://doi.org/10.1080/14737175.2018.1445526 REVIEW Surgical treatments for essential tremor Rodger J. Elble a, Ludy Shih b and Jeffrey W. Cozzens a a Neuroscience
EXPERT REVIEW OF NEUROTHERAPEUTICS, 2018 https://doi.org/10.1080/14737175.2018.1445526 REVIEW Surgical treatments for essential tremor Rodger J. Elble a, Ludy Shih b and Jeffrey W. Cozzens a a Neuroscience
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic surgery
 ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
Patient selection for surgery: Hyperkinetic movement disorders
 Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
Patient selection for surgery: Hyperkinetic movement disorders Alfons Schnitzler, MD, PhD Dept. of Neurology, Movement Disorder and Neuromodulation, Heinrich-Heine-University Düsseldorf, Germany Hyperkinetic
DBS Programming. Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18
 DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE
 11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici
 DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
DBS efficacia, complicanze in cronico e nuovi orizzonti terapeutici TECNICHE DI NEUROMODULAZIONE Invasiva: odeep Brain Stimulation Non Invasiva: o Transcranial Magnetic Stimulation (TMS) o Transcranial
POSTOPERATIVE PATIENT MANAGEMENT
 POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
POSTOPERATIVE PATIENT MANAGEMENT INTRODUCTION Deep brain stimulation of the internal globus pallidus (GPi) or the subthalamic nucleus (STN) effectively reduces parkinsonian motor symptoms and alleviates
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery
 Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Deep Brain Stimulation. Is It Right for You?
 Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes
 Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
University of Groningen. Diagnosis and imaging of essential and other tremors van der Stouwe, Anna
 University of Groningen Diagnosis and imaging of essential and other tremors van der Stouwe, Anna IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
University of Groningen Diagnosis and imaging of essential and other tremors van der Stouwe, Anna IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite
Median-ulnar nerve communications and carpal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Journal of Neurology, Neurosurgery, and Psychiatry, 1977, 40, 982-986 Median-ulnar nerve communications and carpal tunnel syndrome LUDWIG GUTMANN From the Department of Neurology, West Virginia University,
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
Introduction to Neurosurgical Subspecialties: Functional Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Functional Neurosurgery Functional
The Surgical Management of Essential Tremor
 The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
Cortical Brain Computer Interface for Closed-Loop Deep Brain Stimulation
 1 Cortical Brain Computer Interface for Closed-Loop Deep Brain Stimulation Jeffrey A. Herron Ph.D., Margaret C. Thompson, Timothy Brown, Howard J. Chizeck, Sc.D., Jeffrey G. Ojemann, M.D., and Andrew L.
1 Cortical Brain Computer Interface for Closed-Loop Deep Brain Stimulation Jeffrey A. Herron Ph.D., Margaret C. Thompson, Timothy Brown, Howard J. Chizeck, Sc.D., Jeffrey G. Ojemann, M.D., and Andrew L.
Clinical Commissioning Policy Proposition:
 Clinical Commissioning Policy Proposition: Stereotactic Radiosurgery (SRS) for adults with Parkinson's tremor and Familial Essential Tremor Version Number: NHS England B13X06/01 Information Reader Box
Clinical Commissioning Policy Proposition: Stereotactic Radiosurgery (SRS) for adults with Parkinson's tremor and Familial Essential Tremor Version Number: NHS England B13X06/01 Information Reader Box
AT THE FOREFRONT OF MENDING THE BRAIN
 AT THE FOREFRONT OF MENDING THE BRAIN Abbott's neuromodulation portfolio fuels earnings growth while offering lifechanging treatment Many people who are dealt with a diagnosis of Parkinson's disease or
AT THE FOREFRONT OF MENDING THE BRAIN Abbott's neuromodulation portfolio fuels earnings growth while offering lifechanging treatment Many people who are dealt with a diagnosis of Parkinson's disease or
Deep Brain Stimulation Surgery for Parkinson s Disease
 Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
Surgical Options. A History of Surgical Treatment. Patient selection. Essential Tremor (ET)
 Essential tremor (ET) is the most common movement disorder, impacting the lives of an estimated 10 million Americans and millions more worldwide. At this time, there is no cure for ET and only about 50%
Essential tremor (ET) is the most common movement disorder, impacting the lives of an estimated 10 million Americans and millions more worldwide. At this time, there is no cure for ET and only about 50%
Deep Brain Stimulation (DBS) For patients with tremor
 Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
Patient Education Deep Brain Stimulation (DBS) For patients with tremor Please read this handout before reading and signing the form Special Consent for Procedural Treatment. This handout describes how
Indications. DBS for Tremor. What is the PSA? 6/08/2014. Tremor. 1. Tremor. 2. Gait freezing/postural instability. 3. Motor fluctuations
 Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Deep Brain Stimulation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Kaoru Sakatani, Yoichi Katayama, Takamitsu Yamamoto, Susumu Suzuki
 J Neurol Neurosurg Psychiatry 999;67:769 77 769 Neurosurgery, Nihon University School of Medicine, Japan K Sakatani Y Katayama T Yamamoto Neurosurgery, China-Japan Friendship Hospital, China K Sakatani
J Neurol Neurosurg Psychiatry 999;67:769 77 769 Neurosurgery, Nihon University School of Medicine, Japan K Sakatani Y Katayama T Yamamoto Neurosurgery, China-Japan Friendship Hospital, China K Sakatani
Long-term follow up of subthalamic nucleus stimulation in Parkinson s disease
 oped parallel to a progressive cerebral disease. These findings are supported by other recent reports showing that EDS correlates with more advanced PD. 9 The close correlation between persistent and new
oped parallel to a progressive cerebral disease. These findings are supported by other recent reports showing that EDS correlates with more advanced PD. 9 The close correlation between persistent and new
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
S ince the pioneering work of Benabid et and Pollak
 409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
Summary of Selected Spinal Cord Stimulation Studies
 Randomized Controlled Trials Kemler, et al. Effect of for chronic complex regional pain syndrome Type I: five-year final follow-up of patients in a randomized controlled trial. Neurosurg 2008. Kemler,
Randomized Controlled Trials Kemler, et al. Effect of for chronic complex regional pain syndrome Type I: five-year final follow-up of patients in a randomized controlled trial. Neurosurg 2008. Kemler,
The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
 Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
Clinical Neurophysiology 113 (2002) 1 6 www.elsevier.com/locate/clinph The oscillatory activity in the Parkinsonian subthalamic nucleus investigated using the macro-electrodes for deep brain stimulation
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group
 Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
Deep Brain Stimulation (DBS) Surgery for Parkinson s Disease Atkinson Morley Movement Disorders Group This information leaflet contains information about DBS and should answer some of your questions. If
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Parkinson s disease, Essential Tremor and primary dystonia
 Parkinson s disease, Essential Tremor and primary dystonia What is Deep Brain Stimulation and how does it work? Deep Brain Stimulation (DBS) uses one or two surgically implanted medical devices, similar
Parkinson s disease, Essential Tremor and primary dystonia What is Deep Brain Stimulation and how does it work? Deep Brain Stimulation (DBS) uses one or two surgically implanted medical devices, similar
Deep brain stimulation (DBS) of the ventral intermediate
 CLINICAL ARTICLE J Neurosurg 129:290 298, 2018 Intraoperative test stimulation versus stereotactic accuracy as a surgical end point: a comparison of essential tremor outcomes after ventral intermediate
CLINICAL ARTICLE J Neurosurg 129:290 298, 2018 Intraoperative test stimulation versus stereotactic accuracy as a surgical end point: a comparison of essential tremor outcomes after ventral intermediate
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Critical Review: Can sub-thalamic deep brain stimulation (STN-DBS) improve speech output in patients with Parkinson s Disease?
 Copyright 2007, Iulianella, I. Critical Review: Can sub-thalamic deep brain stimulation (STN-DBS) improve speech output in patients with Parkinson s Disease? Iulianella, I. M.Cl.Sc. (SLP) Candidate School
Copyright 2007, Iulianella, I. Critical Review: Can sub-thalamic deep brain stimulation (STN-DBS) improve speech output in patients with Parkinson s Disease? Iulianella, I. M.Cl.Sc. (SLP) Candidate School
Original Policy Date
 MP 7.01.48 Deep Brain Stimulation Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index
MP 7.01.48 Deep Brain Stimulation Medical Policy Section Surgery Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature search/12:2013 Return to Medical Policy Index
Unilateral deep brain stimulation of the subthalamic nucleus for Parkinson disease
 J Neurosurg 106:626 632, 2007 Unilateral deep brain stimulation of the subthalamic nucleus for Parkinson disease JERZY L. SLOWINSKI, PH.D., 1 JOHN D. PUTZKE, PH.D., 2 RYAN J. UITTI, M.D., 2 JOHN A. LUCAS,
J Neurosurg 106:626 632, 2007 Unilateral deep brain stimulation of the subthalamic nucleus for Parkinson disease JERZY L. SLOWINSKI, PH.D., 1 JOHN D. PUTZKE, PH.D., 2 RYAN J. UITTI, M.D., 2 JOHN A. LUCAS,
Name of Policy: Deep Brain Stimulation
 Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
Name of Policy: Deep Brain Stimulation Policy #: 347 Latest Review Date: June 2013 Category: Surgery Policy Grade: B Background/Definitions: As a general rule, benefits are payable under Blue Cross and
(12) Patent Application Publication (10) Pub. No.: US 2006/ A1
 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2006/0058855A1 Gill US 20060058855A1 (43) Pub. Date: Mar. 16, 2006 (54) DEEP BRAIN STIMULATION (76) Inventor: Steven Streatfield
(19) United States (12) Patent Application Publication (10) Pub. No.: US 2006/0058855A1 Gill US 20060058855A1 (43) Pub. Date: Mar. 16, 2006 (54) DEEP BRAIN STIMULATION (76) Inventor: Steven Streatfield
Deep Brain Stimulation
 Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Elias WJ, Huss D, Voss T, et al. A pilot study of focused ultrasound
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Elias WJ, Huss D, Voss T, et al. A pilot study of focused ultrasound
Functional neurosurgery for the treatment of movement. Deep Brain Stimulation REVIEW ARTICLE. Drew S. Kern, MS,* and Rajeev Kumar, MD, FRCPC
 REVIEW ARTICLE Deep Brain Stimulation Drew S. Kern, MS,* and Rajeev Kumar, MD, FRCPC Background: Deep brain stimulation (DBS) for the treatment of neurologic diseases has markedly increased in popularity
REVIEW ARTICLE Deep Brain Stimulation Drew S. Kern, MS,* and Rajeev Kumar, MD, FRCPC Background: Deep brain stimulation (DBS) for the treatment of neurologic diseases has markedly increased in popularity
Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine:
 Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Chapter 19 Peripheral Extracranial Neurostimulation for the treatment of Primary Headache and Migraine: Introduction 1) The occipital nerve is involved in pain syndromes originating from nerve trauma,
Surgical treatment for Parkinson's disease. Citation Hong Kong Practitioner, 1999, v. 21 n. 3, p
 Title Surgical treatment for Parkinson's disease Author(s) Leung, GKK; Hung, KN; Fan, YW Citation Hong Kong Practitioner, 1999, v. 21 n. 3, p. 106-115 Issued Date 1999 URL http://hdl.handle.net/10722/45396
Title Surgical treatment for Parkinson's disease Author(s) Leung, GKK; Hung, KN; Fan, YW Citation Hong Kong Practitioner, 1999, v. 21 n. 3, p. 106-115 Issued Date 1999 URL http://hdl.handle.net/10722/45396
HealthTalks. Deep Brain Stimulation for Parkinson s Disease Patients
 HealthTalks Parkinson s Disease and Wellness Ali Rezai, MD Neurological Institute Director, Center for Neurological Restoration Cleveland Clinic Appointments: 216.444.4720 Deep Brain Stimulation for Parkinson
HealthTalks Parkinson s Disease and Wellness Ali Rezai, MD Neurological Institute Director, Center for Neurological Restoration Cleveland Clinic Appointments: 216.444.4720 Deep Brain Stimulation for Parkinson
Highmark Medical Policy Bulletin
 Highmark Medical Policy Bulletin Section: Miscellaneous Number: Z 7 Topic: Electrical Nerve Stimulation Effective Date: March 3, 2003 Issued Date: November 1, 2003 Date Last Reviewed: 12/2002 General Policy
Highmark Medical Policy Bulletin Section: Miscellaneous Number: Z 7 Topic: Electrical Nerve Stimulation Effective Date: March 3, 2003 Issued Date: November 1, 2003 Date Last Reviewed: 12/2002 General Policy
 www.optimalsp.com.au What may happen to breathing, voice and swallow in PD? Muscles of breathing, voice and speech can be subject to the same disease processes as other muscle groups in PD Slowness, stiffness,
www.optimalsp.com.au What may happen to breathing, voice and swallow in PD? Muscles of breathing, voice and speech can be subject to the same disease processes as other muscle groups in PD Slowness, stiffness,
Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache
 Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
Pain Physician 2011; 14:435-440 ISSN 1533-3159 Case Report Occipital Nerve Stimulation with the Bion Microstimulator for the Treatment of Medically Refractory Chronic Cluster Headache Natalie H. Strand
As clinical experience with deep-brain stimulation (DBS) of
 ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
Outcome of selective ramisectomy for botulinum toxin resistant torticollis
 472 Center for Dystonia, Neurological Institute, Columbia-Presbyterian Medical Center B Ford E D Louis P Greene S Fahn Sergievsky Center, Columbia University, New York, USA E D Louis Correspondence to:
472 Center for Dystonia, Neurological Institute, Columbia-Presbyterian Medical Center B Ford E D Louis P Greene S Fahn Sergievsky Center, Columbia University, New York, USA E D Louis Correspondence to:
O ver the past decade, deep brain stimulation (DBS) has
 1031 PAPER Identification of target areas for deep brain stimulation in human basal ganglia substructures based on median nerve sensory evoked potential criteria F Klostermann, J Vesper, G Curio... See
1031 PAPER Identification of target areas for deep brain stimulation in human basal ganglia substructures based on median nerve sensory evoked potential criteria F Klostermann, J Vesper, G Curio... See
Parkinson's disease before and after a surgical
 J. Neurol. Neurosurg. Psychiat., 1968, 31, 284-290 Simple motor performance of patients with Parkinson's disease before and after a surgical lesion in the thalamus ETIENNE PERRETV From the Montreal Neurological
J. Neurol. Neurosurg. Psychiat., 1968, 31, 284-290 Simple motor performance of patients with Parkinson's disease before and after a surgical lesion in the thalamus ETIENNE PERRETV From the Montreal Neurological
Parkinson's Disease Center and Movement Disorders Clinic
 Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone pdcmdc@bcm.edu www.jankovic.org Essential Tremor Tremor, an oscillatory
Parkinson's Disease Center and Movement Disorders Clinic 7200 Cambridge Street, 9th Floor, Suite 9A Houston, Texas 77030 713-798-2273 phone pdcmdc@bcm.edu www.jankovic.org Essential Tremor Tremor, an oscillatory
Pocket Adaptor Kit FOR SPINAL CORD STIMULATION. Tip Cards
 Pocket Adaptor Kit FOR SPINAL CORD STIMULATION Tip Cards model 74001 (1 4) model 74002 (2 4) The Pocket Adaptor Tip Cards are to be used for educational purposes only. Please refer to the Pocket Adaptor
Pocket Adaptor Kit FOR SPINAL CORD STIMULATION Tip Cards model 74001 (1 4) model 74002 (2 4) The Pocket Adaptor Tip Cards are to be used for educational purposes only. Please refer to the Pocket Adaptor
Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart review
 Mehanna et al. Journal of Clinical Movement Disorders 2014, 1:6 RESEARCH Open Access Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart
Mehanna et al. Journal of Clinical Movement Disorders 2014, 1:6 RESEARCH Open Access Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart
Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri)
 1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
1 Deep Brain Stimulation Surgery Interoperative Magnetic Resonance Imaging (imri) Patient Information Booklet What are the benefits and risks of this treatment for me? Am I a good candidate? What should
Deep brain stimulation: What can patients expect from it?
 MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease
 CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
Parkinsonian rigidity
 J. Neurol. Neurosurg. Pyschiat., 1963, 26, 27 Studies on induced exacerbation of Parkinsonian rigidity The effect of contralateral voluntary activity KEIZO MATSUMOTO, FERDINAND ROSSMANN, TUNG HUI LIN,
J. Neurol. Neurosurg. Pyschiat., 1963, 26, 27 Studies on induced exacerbation of Parkinsonian rigidity The effect of contralateral voluntary activity KEIZO MATSUMOTO, FERDINAND ROSSMANN, TUNG HUI LIN,
Case Report Neuropsychiatric Outcome of an Adolescent Who Received Deep Brain Stimulation for Tourette s Syndrome
 Case Reports in Neurological Medicine Volume 2011, Article ID 209467, 4 pages doi:10.1155/2011/209467 Case Report Neuropsychiatric Outcome of an Adolescent Who Received Deep Brain Stimulation for Tourette
Case Reports in Neurological Medicine Volume 2011, Article ID 209467, 4 pages doi:10.1155/2011/209467 Case Report Neuropsychiatric Outcome of an Adolescent Who Received Deep Brain Stimulation for Tourette
Deep Brain Stimulation. Description
 Subject: Deep Brain Stimulation Page: 1 of 20 Last Review Status/Date: September 2013 Deep Brain Stimulation Description Deep brain stimulation (DBS) involves the stereotactic placement of an electrode
Subject: Deep Brain Stimulation Page: 1 of 20 Last Review Status/Date: September 2013 Deep Brain Stimulation Description Deep brain stimulation (DBS) involves the stereotactic placement of an electrode
Medtronic, Inc.
 Recharging System Quick Guide for Chronic pain www.medtronic.com Medtronic, Inc. 710 Medtronic Parkway Minneapolis, MN 55432-5604 USA Tel: 763-505-5000 Toll-free: 1-800-328-0810 UC201002746a EN 2013 Medtronic,
Recharging System Quick Guide for Chronic pain www.medtronic.com Medtronic, Inc. 710 Medtronic Parkway Minneapolis, MN 55432-5604 USA Tel: 763-505-5000 Toll-free: 1-800-328-0810 UC201002746a EN 2013 Medtronic,
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: MP.108.MH Last Review Date: 05/10/2018 Effective Date: 07/01/2018
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.0108.MH Deep Brain and Dorsal Column (Spinal Cord) This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.0108.MH Deep Brain and Dorsal Column (Spinal Cord) This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst
Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease
 Article Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease Deep-Brain Stimulation for Parkinson's Disease Study Group KRACK, Paul (Collab.)
Article Deep-brain stimulation of the subthalamic nucleus or the pars interna of the globus pallidus in Parkinson's disease Deep-Brain Stimulation for Parkinson's Disease Study Group KRACK, Paul (Collab.)
PNS FOR BACK PAIN IMPROVING PATIENT OUTCOMES
 PNS FOR BACK PAIN IMPROVING PATIENT OUTCOMES New Level-1 evidence The SubQStim Study The Focus SM workflow A recommended and standardised approach for applying PNS based on clinical data BACK PAIN REDUCE
PNS FOR BACK PAIN IMPROVING PATIENT OUTCOMES New Level-1 evidence The SubQStim Study The Focus SM workflow A recommended and standardised approach for applying PNS based on clinical data BACK PAIN REDUCE
