Induction of tolerance to parental parathyroid grafts using allogeneic thymus tissue in patients with DiGeorge anomaly
|
|
|
- Adam Barber
- 5 years ago
- Views:
Transcription
1 Induction of tolerance to parental parathyroid grafts using allogeneic thymus tissue in patients with DiGeorge anomaly Ivan K. Chinn, MD, a and M. Louise Markert, MD, PhD a,b Durham, NC DiGeorge anomaly can affect both thymic and parathyroid function. Although athymia is corrected by allogeneic thymus transplantation, treatment options for hypoparathyroidism have been unsatisfactory. Parathyroid transplantation offers the potential for definitive cure but remains challenging because of graft rejection. Some allogeneic parathyroid grafts have functioned in adult recipients in the context of immunosuppression for renal transplantation. Other efforts have attempted to reduce the allogenicity of the parathyroid grafts through manipulation of the parathyroid tissues before transplantation (by using encapsulation or special culture techniques). Recently, we demonstrated the efficacy of parental parathyroid transplantation when combined with allogeneic thymus transplantation in an infant with complete DiGeorge anomaly. The recipient developed tolerance toward the parathyroid donor. The parathyroid graft has functioned for 5 years after transplantation without the need for continued immunosuppression or calcium supplementation. We observed that matching of the allogeneic thymus graft to the parathyroid donor HLA class II alleles that are unshared with the recipient appears to be associated with the induction of tolerance toward the parathyroid graft. Further work is needed to determine the optimal means for using combined allogeneic thymus and parental parathyroid transplantation to correct hypoparathyroidism in patients with both complete and partial DiGeorge anomaly. (J Allergy Clin Immunol 2011;127: ) Key words: DiGeorge anomaly, parathyroid, thymus, tolerance induction, transplantation DiGeorge anomaly arises from abnormal embryologic development of the third and fourth pharyngeal pouches and the fourth pharyngeal arch, resulting in congenital defects involving (to varying degrees) the heart, parathyroid glands, and thymus. 1,2 A hemizygous deletion at 22q11.2 can be found in approximately half of patients with DiGeorge anomaly; in other cases the diagnosis can be made based on the clinical phenotype. 3 From a the Department of Pediatrics, Division of Allergy and Immunology, and b the Department of Immunology, Duke University Medical Center. Supported by the American Academy of Allergy, Asthma & Immunology 2006 Third- Year Fellow-in-Training Research and 2008 Senior Allergy/Immunology Fellow Transition Awards and National Institutes of Health grants R01 AI , R21 AI , M03 RR 30 (General Clinical Research Center, National Center for Research Resources), T32 AI A2, and 2 K12 HD M. L. M. is a member of the Duke Comprehensive Cancer Center. Disclosure of potential conflict of interest: I. K. Chinn and M. L. Markert receive research support from the National Institutes of Health. Received for publication January 20, 2011; revised March 25, 2011; accepted for publication March 30, Available online April 21, Reprint requests: Ivan K. Chinn, MD, Box 3068, Duke University Medical Center, Durham, NC chinn001@mc.duke.edu /$36.00 Ó 2011 American Academy of Allergy, Asthma & Immunology doi: /j.jaci Abbreviations used MLC: Mixed lymphocyte culture PTH: Parathyroid hormone Infants with DiGeorge anomaly who demonstrate fewer than 50 naive (CD45RA 1 CD62L 1 ) T cells/mm 3 or naive T-cell percentages of less than 5% of total T cells in the peripheral blood have athymia and meet criteria for the definition of complete DiGeorge anomaly. 3 This condition affects approximately 1% of infants with DiGeorge anomaly and leads to a primary immunodeficiency that is usually fatal because of infection by 2 years of age. Thymus transplantation with postnatal cultured allogeneic non HLA-matched thymus tissue provides immunoreconstitution that significantly improves survival. 3 In the recipients, host bone marrow derived thymocyte precursors migrate to the donor thymus graft and develop into genetically host mature T cells. By 6 to 12 months after transplantation, naive T cells appear in the circulation; the T cells proliferate normally to mitogens and have diverse T-cell receptor repertoires. The recipients develop tolerance toward the thymus donors and do not require longterm immunosuppression. 4 Although athymia can be corrected with thymus transplantation, the parathyroid defect in patients with DiGeorge anomaly remains a significant yet poorly addressed issue. Parathyroid deficiency has previously been identified in 17% to 60% of patients with DiGeorge anomaly. 5 In our own series of 60 infants with complete DiGeorge anomaly who received allogeneic thymus grafts, 48 (80%) have required calcium or vitamin D supplementation before thymus transplantation to prevent hypocalcemia. Hypocalcemia from primary hypoparathyroidism places children with DiGeorge anomaly at risk for seizures, which can lead to decreased mental capacity. Calcium supplementation itself can result in serious complications, including severe skin burns from intravenous infiltration, nephrocalcinosis, ectopic calcifications, and death. In addition, when children with DiGeorge anomaly and hypoparathyroidism undergo periods of physiologic stress, such as during infections, they often develop hypocalcemia despite ongoing calcium supplementation. Replacement of parathyroid hormone (PTH) could directly address the primary defect. However, exogenous replacement with recombinant human PTH presents a relatively poor option for treatment because of the associated potential risk for bone malignancies. 6 Allogeneic parathyroid transplantation would theoretically provide physiologic replacement of PTH without the risks associated with calcium and PTH supplementation. ALLOGENEIC PARATHYROID TRANSPLANTATION Observations in animal models Animal models have yielded important insights regarding factors that contribute to rejection of, as opposed to tolerance 1351
2 1352 CHINN AND MARKERT J ALLERGY CLIN IMMUNOL JUNE 2011 toward, allogeneic parathyroid grafts. Not long after the MHC antigens were discovered, it was demonstrated that the degree of histocompatibility between the recipients and donors plays a significant role in determining long-term parathyroid graft survival. 7 This understanding has resulted in efforts to reduce recipient allorecognition toward mismatched parathyroid graft MHC antigens. Various strategies have been tested in both animal models and human recipients (discussed in the following section). Of interest, in one approach Goss et al 8 were able to demonstrate 50% indefinite survival of allogeneic parathyroid grafts in calcium-deficient rats after engrafting the parathyroid tissues within the endogenous recipient thymuses and administering a single dose of antilymphocyte serum. This finding revealed the potential for using the thymus to protect parathyroid grafts from rejection caused by mismatched MHC antigens. Allogeneic parathyroid transplantation in human subjects Early attempts to perform allogeneic parathyroid transplantation met limited success. Allogeneic parathyroid transplantation was reported as early as the beginning of the 20th century. 9 A review of parathyroid allotransplantation published in 1963 was not encouraging because recipients did not demonstrate long-term graft function. 9 However, in 1967, Amos and Bach reported the discovery of human MHC antigens (HLA). 10 As the understanding evolved concerning how these antigens contribute to graft rejection, investigators began to develop strategies to overcome HLA mismatches between recipients and parathyroid graft donors. The most commonly used approaches include parathyroid transplantation within the context of immunosuppression for renal allografts, encapsulation of the parathyroid tissues, and culture of the parathyroid tissues before transplantation. Persistent parathyroid graft function has been observed when allogeneic parathyroid tissues are transplanted into patients who have received renal allografts. The first case was reported in 1973; the recipient was given an allogeneic parathyroid graft within 2 months of allogeneic renal transplantation, as summarized by Torregrosa et al. 11 The patient was receiving immunosuppression at the time of parathyroid transplantation to prevent rejection of the renal graft. The immunosuppression was maintained indefinitely, allowing the parathyroid graft to function for more than 21 months after transplantation. In 1979, Wells et al similarly performed parathyroid allotransplantation after allogeneic renal transplantation. 11 The parathyroid graft function was lost when acute rejection of the renal graft developed in the recipient. Since that time, multiple other cases have been reported in which renal allograft recipients were given allogeneic parathyroid transplants. 11 In almost all cases that have demonstrated parathyroid graft function beyond 2 years after transplantation, the patients were maintained on long-term immunosuppression. As a possible exception, Zeng discontinued immunosuppression in 9 patients after 2 years. The clinical data suggested persistent parathyroid graft function in the patients up to 6 years after transplantation, although PTH data were not provided. 11 Thus transplant surgeons have been able to take advantage of the fact that renal allograft recipients require indefinite immunosuppression after transplantation to perform subsequent transplantation of allogeneic parathyroid tissues. Although the parathyroid grafts can function for as long as 13 years 11 after transplantation by using this approach, the recipients fail to develop tolerance to the parathyroid grafts, and persistent parathyroid graft function has not been demonstrated in the absence of the immunosuppression. In efforts to overcome the need for immunosuppression, other investigators have attempted to encapsulate the parathyroid graft tissues to limit exposure of any mismatched parathyroid HLA antigens to the recipient immune system. Initial experiments used alginate, a potential carcinogen. Later work transitioned to the use of a different form of sodium alginate. In 1997, Hasse et al reported the first use of alginate-encapsulated allogeneic parathyroid tissues in human recipients (see brief review by Torregrosa et al 11 ). The allografts were well tolerated and demonstrated normal parathyroid function without the need for immunosuppression, although long-term follow-up data are not available. Long-term function of encapsulated allogeneic parathyroid grafts might be complicated by the development of fibrosis for unclear reasons. 12 Meanwhile, the need to extensively manipulate the parathyroid graft tissues before transplantation increases the risk for environmental contamination or loss of viability of the tissues. Thus although encapsulation shows promise, further work is required to optimize its use in human recipients. Other investigators have sought to extend the survival and function of allogeneic parathyroid grafts without long-term immunosuppression by culturing the parathyroid tissues before transplantation. In normal healthy parathyroid tissue, HLA class I antigens are expressed in 23% of parenchymal cells and 62% of stromal cells; HLA class II antigens are not expressed in parenchymal cells but are ubiquitously expressed in the stromal cells. 13 Culturing the parathyroid tissues in vitro or in vivo before transplantation significantly reduces the expression of the HLA antigens through unclear mechanisms, although loss of passenger donor leukocytes might play a role. 13,14 Feind et al reported the first series of human in vitro cultured allogeneic parathyroid graft recipients. 11 The investigators were not able to demonstrate graft function through 6 months after transplantation. Several subsequent reports of cultured allogeneic parathyroid transplantation without immunosuppression have emerged. Sollinger et al cultured irradiated parathyroid allografts in vivo (in nude mice) before placing the tissues into human recipients. 11 The recipients demonstrated PTH production without immunosuppression but continued to require calcium supplementation after transplantation. The largest series of cultured parathyroid allotransplantation was reported in 2007 by Nawrot et al. 14 Dissected parathyroid tissues were cultured in vitro and transplanted into 85 recipients. The optimal culture period was 6 weeks, and reduction of parathyroid tissue HLA expression was demonstrated. Four of 85 recipients had parathyroid graft function that persisted beyond 24 months after transplantation. Thus cultured allogeneic parathyroid transplantation remains an unsatisfactory treatment option for hypoparathyroidism at this time. COMBINED ALLOGENEIC THYMUS AND PARENTAL PARATHYROID TRANSPLANTATION We recently used parental parathyroid transplantation in combination with allogeneic thymus transplantation to treat 4 infants with congenital athymia and primary hypoparathyroidism from complete DiGeorge anomaly. 15 Although 1 subject received immunosuppression because of the diagnosis of atypical complete DiGeorge anomaly, 3 all immunosuppression was discontinued in the recipient by 6 months after transplantation. The other 3
3 J ALLERGY CLIN IMMUNOL VOLUME 127, NUMBER 6 CHINN AND MARKERT 1353 subjects did not receive posttransplantation immunosuppression. The surgical procedures were tolerated well by the recipients and donors. One subject died at 9.6 months after transplantation from respiratory failure related to congenital rib defects. The remaining 3 recipients have done well clinically, aside from the development of autoimmune hypothyroidism in 2 of the 3 survivors. Results All recipients demonstrated thymus and parathyroid graft function after transplantation. 15 Two of the 3 survivors developed alloreactivity toward their parathyroid donors in mixed lymphocyte cultures (MLCs) and lost parathyroid graft function. 15 The third survivor, however, has demonstrated continued parathyroid graft function at 5 years after transplantation together with persistent recipient tolerance toward the parathyroid donor in MLCs. 15 Matching of the allogeneic thymus tissue to the parental parathyroid graft for HLA class II alleles not shared between the parathyroid donor and the recipient appeared to be required for the development of recipient tolerance toward the parathyroid donor and long-term parathyroid graft function. The 2 subjects who received parathyroid grafts that had HLA class II alleles not shared with either the recipient or the thymus donor rejected their parathyroid grafts. On the other hand, in the subject who developed tolerance toward the parathyroid donor and long-term parathyroid graft function, all of the HLA class II alleles for the parathyroid graft matched with either the recipient or the thymus graft. A model for tolerance The abrogation of alloreactivity toward allogeneic parathyroid grafts may be mediated through central or peripheral tolerance mechanisms. 16 In central tolerance, developing T cells are negatively selected within the thymus and deleted if they demonstrate strong reactivity toward intrathymically presented antigens. In peripheral tolerance, a variety of mechanisms exist to suppress self-reactive T cells that are not eliminated within the thymus. These mechanisms include suppression by regulatory T cells, anergy, and activation-induced cell death. Regulatory T cells maintain tolerance by inhibiting the activity of self-reactive T cells through contact-mediated or cytokine-mediated processes. Regulatory T cells can be stimulated or induced by so-called tolerogenic dendritic cells. 17 In anergy self-reactive T cells are functionally inactivated but not deleted. Lack of costimulatory signaling is believed to play a role in inducing anergy. The inactivated T cells can escape anergy in vitro through the combination of IL-2 supplementation, engagement of their T-cell receptors, and costimulation. Finally, in activation-induced cell death T cells that demonstrate strong affinity for self-antigens not only become functionally inactivated but also undergo apoptosis. In combined allogeneic thymus and parental parathyroid transplantation, several of these mechanisms might play important roles in promoting the development of recipient tolerance toward the parathyroid grafts. The work by Goss et al 8 showed that placement of the parathyroid tissues, including the parathyroid MHC antigens, within the thymus can induce recipient tolerance toward the parathyroid grafts. In allogeneic thymus transplantation, microchimerism develops within the thymus graft, consisting of thymus donor medullary thymic epithelial cells and recipient antigen-presenting cells (eg, dendritic cells). Thus if all of the parathyroid donor HLA class II alleles are shared with either the thymus graft or the recipient, the HLA class II antigens of the parathyroid graft will be expressed within the thymus graft, producing a model similar to the one created by Goss et al. The mechanisms by which expression of the parathyroid donor HLA class II alleles within the thymus graft leads to tolerance toward the parathyroid graft remain incompletely understood. Negative selection within the thymus graft likely deletes recipient alloreactive T cells that recognize the parathyroid donor HLA class II antigens shared with and expressed by the medullary thymic epithelial cells and recipient antigen-presenting cells. This hypothesis remains difficult to test directly. In our studies appropriate matching appeared to induce anergy in some T cells of the recipient who developed tolerance to the parathyroid donor that were capable of rejecting the parathyroid graft. 15 Regulatory T cells did not appear to be required to suppress alloreactivity by the subject toward the parathyroid donor when tested at 17 months after transplantation, 15 but our more recent assessments suggest that the role of regulatory T cells cannot be completely excluded (unpublished data). We have not excluded a possible role for activation-induced cell death. Other considerations It remains unclear why the presence of HLA class I mismatches between the parathyroid donor, recipient, and thymus donor did not appear to create a barrier to tolerance induction. It is known that the alloreactivity observed in MLCs comes from HLA class II differences. 18 Thus HLA class I mismatches alone might be insufficient for the generation of significant allorecognition responses in certain conditions, 19 such as in parental parathyroid transplantation. In this manner our results are similar to findings in a registry of cardiac transplant recipients that showed a significant effect of HLA class II, but not class I, mismatches on long-term outcomes after transplantation. 20 We observed the development of autoimmune hypothyroidism in 2 recipients: in 1 of the 2 subjects who rejected the parathyroid graft and in the recipient who developed tolerance to the parental parathyroid. The etiology for this finding remains unclear. In reviewing all subjects who have received allogeneic thymus grafts without parathyroid transplantation at our institution, we identified 38 who have survived beyond 1 year. Thirteen of the 38 recipients have developed autoimmune thyroid disease (unpublished data). 3 The appearance of thyroid disease in 2 subjects who received combined allogeneic thymus and parental parathyroid transplantation is not statistically greater in prevalence and thus is not likely to have been caused by parathyroid transplantation. Other potential explanations for our observations remain under consideration. The recipients each received a single parental parathyroid gland. As a result, no significant dose differences should account for the disparate outcomes. On the other hand, graft failure due to failure to vascularize or other factors cannot be excluded in the subjects who lost parathyroid function. In addition, loss of parathyroid function due to rejection of parathyroid tissue specific proteins, such as PTH or the calciumsensing receptor, remains possible. However, our MLC data argue that allorecognition is a key mechanism of graft rejection and that tolerance toward the parathyroid donor HLA antigens is required for persistent parathyroid graft function. FUTURE WORK Further efforts will be needed to optimize the approach for combined allogeneic thymus and parathyroid transplantation.
4 1354 CHINN AND MARKERT J ALLERGY CLIN IMMUNOL JUNE 2011 First, our proposed matching strategy needs to be confirmed with additional transplants or in animal models. Next, if matching of the allogeneic thymus graft to the parathyroid donor HLA class II alleles that are unshared with the recipient is required for the induction of tolerance toward the parathyroid graft, allogeneic thymus tissues might need to be cryopreserved for transplantation. Protocols would need to be developed to create and use these tissue banks. Finally, for combined allogeneic thymus and parental parathyroid transplantation to work as a therapy in patients with partial DiGeorge anomaly, an immune-conditioning or ablation protocol will need to be developed that will allow the allogeneic thymus tissue to be accepted by the recipient so that it can promote, in turn, tolerance toward the parathyroid graft. The fact that complete DiGeorge anomaly recipients of allogeneic thymus transplants do not reject their grafts when host T cells develop demonstrates that tolerance toward the thymus grafts is an achievable goal. 4 Our model for combined allogeneic thymus and parathyroid transplantation suggests other potential avenues for future research that could be focused on creating intrathymic donor and recipient HLA chimerism. According to our paradigm, placement of parathyroid donor HLA class II antigens directly within the thymus should result in tolerance to the parathyroid allograft without the need to match the parathyroid to the thymus or the recipient. Thus in recipients with complete DiGeorge anomaly recipients, a completely mismatched parathyroid allograft could be wrapped within the thymus tissue and transplanted within the same quadriceps incision. For other patients who have endogenous thymus tissue, parathyroid donor bone marrow cells or HLA class II peptides could be injected intrathymically together in combination with heterotopic parathyroid transplantation. The induction of tolerance after allopeptide injection into endogenous thymic tissue has been reported in animal models. 21 This approach might be difficult in patients who have thymic hypoplasia or who have significant replacement of the thymic tissue with adipose tissue. As an alternative technique to intrathymic injection, patients could receive bone marrow transplantation from the donor of the allogeneic parathyroid graft. In this approach the parathyroid donor bone marrow cells would presumably generate dendritic cells to populate the endogenous thymus tissue, inducing tolerance to the parathyroid graft. Such a method would be similar to efforts in combined bone marrow and tissue transplantation for other solid organs, such as the heart, lungs, or kidneys, that have been studied by multiple other investigators over the past several years. 21 Combined bone marrow and renal cotransplantation has been reported in human subjects with mixed success. 16,21 Posttransplantation analyses have focused on bone marrow chimerism, and it remains unclear how well these evaluations gauge intrathymic chimerism. As a final option, recipients could be infused with dendritic cells from the parathyroid donor or from the recipient that have been primed with parathyroid donor HLA class II peptides. Circulation of the dendritic cells into the thymus would then lead to the induction of tolerance. The successful use of allopeptidepulsed immature dendritic cells to induce tolerance to cardiac, pancreatic islet, and renal allografts has been described in animal models but will need to be further studied in human subjects. 21 Finally, adjunctive therapies should be considered to support and enhance the induction of tolerance to allogeneic parathyroid grafts by cotransplanted thymus tissue in patients with DiGeorge anomaly. Recipient regulatory T cells can be collected, expanded ex vivo, and then reinfused. This process is being developed for bone marrow transplant recipients but has not yet been reported in human solid organ transplantation. 22 Alternately, recipient regulatory T cells can be induced in vivo with rapamycin. 16,21 As a third method for promoting regulatory T cell mediated suppression of graft rejection, tolerogenic dendritic cells can be generated in vitro and infused into the recipients. This technique has only recently been examined for use in transplantation. 17 Another adjunctive therapy might include costimulatory blockade to induce anergy. This approach is being tested in human renal 21 and hepatic 16 transplantation recipients and has been complicated by reports of thromboembolic events. Finally, methods may be explored to silence HLA class II expression in the allogeneic parathyroid tissues by using small molecules. Continued technological advances could make this approach more promising in future years. CONCLUSIONS Efforts have increased over the last 20 years to offer the possibility of successful parathyroid allotransplantation. Combined allogeneic thymus and parental parathyroid transplantation holds promise for the treatment of primary hypoparathyroidism due to DiGeorge anomaly, especially complete DiGeorge anomaly. Further work is needed to identify the optimal means for manipulating the thymus to enhance its ability to induce tolerance to parathyroid grafts. REFERENCES 1. DiGeorge AM. Discussion of Cooper MD, Peterson RDA, Good RA. A new concept of cellular basis of immunity. J Pediatr 1965;67: M uller W, Peter H, Wilken M, Juppner H, Kallfelz HC, Krohn HP, et al. The Di- George syndrome. I. Clinical evaluation and course of partial and complete forms of the syndrome. Eur J Pediatr 1988;147: Markert ML, Devlin BH, Alexieff MJ, Li J, McCarthy EA, Gupton SE, et al. Review of 54 patients with complete DiGeorge anomaly enrolled in protocols for thymus transplantation: outcome of 44 consecutive transplants. Blood 2007;109: Chinn IK, Devlin BH, Li Y-J, Markert ML. Long-term tolerance to allogeneic thymus transplants in complete DiGeorge anomaly. Clin Immunol 2008;126: Sullivan KE. Chromosome 22q11.2 deletion syndrome: DiGeorge syndrome/ velocardiofacial syndrome. Immunol Allergy Clin North Am 2008;28: Vahle JL, Sato M, Long GG, Young JK, Francis PC, Engelhardt JA, et al. Skeletal changes in rats given daily subcutaneous injections of recombinant human parathyroid hormone (1-34) for 2 years and relevance to human safety. Toxicol Pathol 2002;30: Naji A, Barker CF. The influence of histocompatibility and transplant site on parathyroid allograft survival. J Surg Res 1976;20: Goss JA, Nakafusa Y, Flye MW. Prolonged intrathymic parathyroid allograft survival. Transplant Proc 1994;26: Jacob SW, Dunphy JE. Successful parathyroid transplantation: a review of the literature. Am J Surg 1963;105: Bach FH, Amos DB. Hu-1: major histocompatibility locus in man. Science 1967; 156: Torregrosa NM, Rodrıguez JM, Llorente S, Balsalobre MD, Rios A, Jimeno L, et al. Definitive treatment for persistent hypoparathyroidism in a kidney transplant patient: parathyroid allotransplantation. Thyroid 2005;15: Tibell A, Rafael E, Wennberg L, Nordenstr om J, Bergstr om M, Geller RL, et al. Survival of macroencapsulated allogeneic parathyroid tissue one year after transplantation in nonimmunosuppressed humans. Cell Transplant 2001;10: Bjerneroth G, Juhlin C, Rastad J, Akerstrom G, Klareskog L. MHC class I and II antigen expression on parathyroid cells and prospects for their allogeneic transplantation. Transplantation 1993;56: Nawrot I, Wozniewicz B, Tolloczko T, Sawicki A, Gorski A, Chudzinski W, et al. Allotransplantation of cultured parathyroid progenitor cells without immunosuppression: clinical results. Transplantation 2007;83:
5 J ALLERGY CLIN IMMUNOL VOLUME 127, NUMBER 6 CHINN AND MARKERT Chinn IK, Olson JA, Skinner MA, McCarthy EA, Gupton SE, Chen D-F, et al. Mechanisms of tolerance to parental parathyroid tissue when combined with human allogeneic thymus transplantation. J Allergy Clin Immunol 2010;126: Seyfert-Margolis V, Feng S. Tolerance: is it achievable in pediatric solid organ transplantation? Pediatr Clin North Am 2010;57: Liu W, Li XC. An overview on non-t cell pathways in transplant rejection and tolerance. Curr Opin Organ Transplant 2010;15: Jeras M. The role of in vitro alloreactive T-cell functional tests in the selection of HLA matched and mismatched haematopoietic stem cell donors. Transpl Immunol 2002;10: Li XC, Raghavan M. Structure and function of major histocompatibility complex class I antigens. Curr Opin Organ Transplant 2010;15: Kaczmarek I, Deutsch M-A, Rohrer M-E, Beiras-Fernandez A, Groetzner J, Daebritz S, et al. HLA-DR matching improves survival after heart transplantation: is it time to change allocation policies? J Heart Lung Transplant 2006; 25: Griesemer AD, Sorenson EC, Hardy MA. The role of the thymus in tolerance. Transplantation 2010;90: Safinia N, Sagoo P, Lechler R, Lombardi G. Adoptive regulatory T cell therapy: challenges in clinical transplantation. Curr Opin Organ Transplant 2010;15:
The Thymus as The Primary Site of T-cell Production
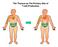 The Thymus as The Primary Site of T-cell Production Thymus Histology Lobulated organ with outer cortex and inner medulla C M Ordered Microenvironments Support T-cell Development CD4-CD8- precursors CD4+CD8+
The Thymus as The Primary Site of T-cell Production Thymus Histology Lobulated organ with outer cortex and inner medulla C M Ordered Microenvironments Support T-cell Development CD4-CD8- precursors CD4+CD8+
T Cell Development. Xuefang Cao, MD, PhD. November 3, 2015
 T Cell Development Xuefang Cao, MD, PhD November 3, 2015 Thymocytes in the cortex of the thymus Early thymocytes development Positive and negative selection Lineage commitment Exit from the thymus and
T Cell Development Xuefang Cao, MD, PhD November 3, 2015 Thymocytes in the cortex of the thymus Early thymocytes development Positive and negative selection Lineage commitment Exit from the thymus and
Immunology Lecture 4. Clinical Relevance of the Immune System
 Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Immunology Lecture 4 The Well Patient: How innate and adaptive immune responses maintain health - 13, pg 169-181, 191-195. Immune Deficiency - 15 Autoimmunity - 16 Transplantation - 17, pg 260-270 Tumor
Lecture outline. Immunological tolerance and immune regulation. Central and peripheral tolerance. Inhibitory receptors of T cells. Regulatory T cells
 1 Immunological tolerance and immune regulation Abul K. Abbas UCSF 2 Lecture outline Central and peripheral tolerance Inhibitory receptors of T cells Regulatory T cells 1 The immunological equilibrium:
1 Immunological tolerance and immune regulation Abul K. Abbas UCSF 2 Lecture outline Central and peripheral tolerance Inhibitory receptors of T cells Regulatory T cells 1 The immunological equilibrium:
SEVENTH EDITION CHAPTER
 Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
Judy Owen Jenni Punt Sharon Stranford Kuby Immunology SEVENTH EDITION CHAPTER 16 Tolerance, Autoimmunity, and Transplantation Copyright 2013 by W. H. Freeman and Company Immune tolerance: history * Some
TRANSPLANT IMMUNOLOGY. Shiv Pillai Ragon Institute of MGH, MIT and Harvard
 TRANSPLANT IMMUNOLOGY Shiv Pillai Ragon Institute of MGH, MIT and Harvard Outline MHC / HLA Direct vs indirect allorecognition Alloreactive cells: where do they come from? Rejection and Immunosuppression
TRANSPLANT IMMUNOLOGY Shiv Pillai Ragon Institute of MGH, MIT and Harvard Outline MHC / HLA Direct vs indirect allorecognition Alloreactive cells: where do they come from? Rejection and Immunosuppression
FOCiS. Lecture outline. The immunological equilibrium: balancing lymphocyte activation and control. Immunological tolerance and immune regulation -- 1
 1 Immunological tolerance and immune regulation -- 1 Abul K. Abbas UCSF FOCiS 2 Lecture outline Principles of immune regulation Self-tolerance; mechanisms of central and peripheral tolerance Inhibitory
1 Immunological tolerance and immune regulation -- 1 Abul K. Abbas UCSF FOCiS 2 Lecture outline Principles of immune regulation Self-tolerance; mechanisms of central and peripheral tolerance Inhibitory
LONG TERM OBSERVATION AFTER CULTURED HUMAN PARATHYROID CELLS ALLOTRANSPLANTATION WITHOUT IMMUNOSUPPRESSION
 LONG TERM OBSERVATION AFTER CULTURED HUMAN PARATHYROID CELLS ALLOTRANSPLANTATION WITHOUT IMMUNOSUPPRESSION Nawrot I, Tołłoczko T, Szmidt J, Woźniewicz B, Migaj M, Górski A, Sawicki A, Zawitkowska T, Pietrasik
LONG TERM OBSERVATION AFTER CULTURED HUMAN PARATHYROID CELLS ALLOTRANSPLANTATION WITHOUT IMMUNOSUPPRESSION Nawrot I, Tołłoczko T, Szmidt J, Woźniewicz B, Migaj M, Górski A, Sawicki A, Zawitkowska T, Pietrasik
Central tolerance. Mechanisms of Immune Tolerance. Regulation of the T cell response
 Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. Mechanisms of Immune Tolerance ACTIVATION (immunity) SUPPRESSION (tolerance)
Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. Mechanisms of Immune Tolerance ACTIVATION (immunity) SUPPRESSION (tolerance)
Mechanisms of Immune Tolerance
 Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. ACTIVATION (immunity) SUPPRESSION (tolerance) Autoimmunity Immunodeficiency
Immunoregulation: A balance between activation and suppression that achieves an efficient immune response without damaging the host. ACTIVATION (immunity) SUPPRESSION (tolerance) Autoimmunity Immunodeficiency
Dr. Yi-chi M. Kong August 8, 2001 Benjamini. Ch. 19, Pgs Page 1 of 10 TRANSPLANTATION
 Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Benjamini. Ch. 19, Pgs 379-399 Page 1 of 10 TRANSPLANTATION I. KINDS OF GRAFTS II. RELATIONSHIPS BETWEEN DONOR AND RECIPIENT Benjamini. Ch. 19, Pgs 379-399 Page 2 of 10 II.GRAFT REJECTION IS IMMUNOLOGIC
Immunological Tolerance
 Immunological Tolerance Introduction Definition: Unresponsiveness to an antigen that is induced by exposure to that antigen Tolerogen = tolerogenic antigen = antigen that induces tolerance Important for
Immunological Tolerance Introduction Definition: Unresponsiveness to an antigen that is induced by exposure to that antigen Tolerogen = tolerogenic antigen = antigen that induces tolerance Important for
Chapter 13. DiGeorge Syndrome
 Chapter 13 DiGeorge Syndrome DiGeorge Syndrome is a primary immunodeficiency disease caused by abnormal migration and development of certain cells and tissues during fetal development. As part of the developmental
Chapter 13 DiGeorge Syndrome DiGeorge Syndrome is a primary immunodeficiency disease caused by abnormal migration and development of certain cells and tissues during fetal development. As part of the developmental
Transplantation. Immunology Unit College of Medicine King Saud University
 Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
Transplantation Immunology Unit College of Medicine King Saud University Objectives To understand the diversity among human leukocyte antigens (HLA) or major histocompatibility complex (MHC) To know the
One Day BMT Course by Thai Society of Hematology. Management of Graft Failure and Relapsed Diseases
 One Day BMT Course by Thai Society of Hematology Management of Graft Failure and Relapsed Diseases Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital
One Day BMT Course by Thai Society of Hematology Management of Graft Failure and Relapsed Diseases Piya Rujkijyanont, MD Division of Hematology-Oncology Department of Pediatrics Phramongkutklao Hospital
Development of B and T lymphocytes
 Development of B and T lymphocytes What will we discuss today? B-cell development T-cell development B- cell development overview Stem cell In periphery Pro-B cell Pre-B cell Immature B cell Mature B cell
Development of B and T lymphocytes What will we discuss today? B-cell development T-cell development B- cell development overview Stem cell In periphery Pro-B cell Pre-B cell Immature B cell Mature B cell
5/1/13. The proportion of thymus that produces T cells decreases with age. The cellular organization of the thymus
 T cell precursors migrate from the bone marrow via the blood to the thymus to mature 1 2 The cellular organization of the thymus The proportion of thymus that produces T cells decreases with age 3 4 1
T cell precursors migrate from the bone marrow via the blood to the thymus to mature 1 2 The cellular organization of the thymus The proportion of thymus that produces T cells decreases with age 3 4 1
Objectives. Abbas Chapter 11: Immunological Tolerance. Question 1. Question 2. Question 3. Definitions
 Objectives Abbas Chapter 11: Immunological Tolerance Christina Ciaccio, MD Children s Mercy Hospitals and Clinics February 1, 2010 To introduce the concept of immunologic tolerance To understand what factors
Objectives Abbas Chapter 11: Immunological Tolerance Christina Ciaccio, MD Children s Mercy Hospitals and Clinics February 1, 2010 To introduce the concept of immunologic tolerance To understand what factors
Immune Regulation and Tolerance
 Immune Regulation and Tolerance Immunoregulation: A balance between activation and suppression of effector cells to achieve an efficient immune response without damaging the host. Activation (immunity)
Immune Regulation and Tolerance Immunoregulation: A balance between activation and suppression of effector cells to achieve an efficient immune response without damaging the host. Activation (immunity)
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
- Transplantation: removing an organ from donor and gives it to a recipient. - Graft: transplanted organ.
 Immunology Lecture num. (21) Transplantation - Transplantation: removing an organ from donor and gives it to a recipient. - Graft: transplanted organ. Types of Graft (4 types): Auto Graft - From a person
Immunology Lecture num. (21) Transplantation - Transplantation: removing an organ from donor and gives it to a recipient. - Graft: transplanted organ. Types of Graft (4 types): Auto Graft - From a person
IMMUNOBIOLOGY OF TRANSPLANTATION. Wasim Dar
 IMMUNOBIOLOGY OF TRANSPLANTATION Wasim Dar Immunobiology of Transplantation Overview Transplantation: A complex immunologic process Contributions Innate Immunity Adaptive immunity T Cells B Cells HLA Consequences
IMMUNOBIOLOGY OF TRANSPLANTATION Wasim Dar Immunobiology of Transplantation Overview Transplantation: A complex immunologic process Contributions Innate Immunity Adaptive immunity T Cells B Cells HLA Consequences
Histocompatibility antigens
 Histocompatibility antigens Tuesday 09 November 2010 Telegraph UK Livers grown in the laboratory could eventually solve organ transplant shortage. Made-to-measure organs for transplantation are a step
Histocompatibility antigens Tuesday 09 November 2010 Telegraph UK Livers grown in the laboratory could eventually solve organ transplant shortage. Made-to-measure organs for transplantation are a step
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Immunologic Features 22q11.2DS. Chiraag S. Patel, MD
 Immunologic Features 22q11.2DS Chiraag S. Patel, MD Objectives Genetics and DiGeorge Syndrome Thymus Immune cells (T-, B-, and NK cells) 22q11.2DS-associated disorders autoimmune and allergic diseases
Immunologic Features 22q11.2DS Chiraag S. Patel, MD Objectives Genetics and DiGeorge Syndrome Thymus Immune cells (T-, B-, and NK cells) 22q11.2DS-associated disorders autoimmune and allergic diseases
Transplant Booklet D Page 1
 Booklet D Pretest Correct Answers 4. (A) is correct. Technically, performing a hematopoietic stem cell transplant is one of the simplest transplantation procedures. The hematopoietic stem cells are infused
Booklet D Pretest Correct Answers 4. (A) is correct. Technically, performing a hematopoietic stem cell transplant is one of the simplest transplantation procedures. The hematopoietic stem cells are infused
Darwinian selection and Newtonian physics wrapped up in systems biology
 Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
XIV. HLA AND TRANSPLANTATION MEDICINE
 XIV. HLA AND TRANSPLANTATION MEDICINE A. Introduction 1. The HLA system includes a complex array of genes and their molecular products that are involved in immune regulation and cellular differentiation.
XIV. HLA AND TRANSPLANTATION MEDICINE A. Introduction 1. The HLA system includes a complex array of genes and their molecular products that are involved in immune regulation and cellular differentiation.
Cellular Pathology of immunological disorders
 Cellular Pathology of immunological disorders SCBM344 Cellular and Molecular Pathology Witchuda Payuhakrit, Ph.D (Pathobiology) witchuda.pay@mahidol.ac.th Objectives Describe the etiology of immunological
Cellular Pathology of immunological disorders SCBM344 Cellular and Molecular Pathology Witchuda Payuhakrit, Ph.D (Pathobiology) witchuda.pay@mahidol.ac.th Objectives Describe the etiology of immunological
Recommended reading: Abbas et al. 5th edition, chapters 7 and 10; Janeway and Travers, 5th edition, chapter 7.
 Harvard-MIT Division of Health Sciences and Technology HST.176: Cellular and Molecular Immunology Course Director: Dr. Shiv Pillai 10/05/05; 11 AM Shiv Pillai T Lymphocyte Development Recommended reading:
Harvard-MIT Division of Health Sciences and Technology HST.176: Cellular and Molecular Immunology Course Director: Dr. Shiv Pillai 10/05/05; 11 AM Shiv Pillai T Lymphocyte Development Recommended reading:
The Lymphatic System and Body Defenses
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Lymphatic System and Body Defenses 12PART B Adaptive Defense System: Third Line of Defense Immune
CHAPTER 9 BIOLOGY OF THE T LYMPHOCYTE
 CHAPTER 9 BIOLOGY OF THE T LYMPHOCYTE Coico, R., Sunshine, G., (2009) Immunology : a short course, 6 th Ed., Wiley-Blackwell 1 CHAPTER 9 : Biology of The T Lymphocytes 1. 2. 3. 4. 5. 6. 7. Introduction
CHAPTER 9 BIOLOGY OF THE T LYMPHOCYTE Coico, R., Sunshine, G., (2009) Immunology : a short course, 6 th Ed., Wiley-Blackwell 1 CHAPTER 9 : Biology of The T Lymphocytes 1. 2. 3. 4. 5. 6. 7. Introduction
FIT Board Review Corner March 2016
 FIT Board Review Corner March 2016 Welcome to the FIT Board Review Corner, prepared by Sarah Spriet, DO, and Tammy Peng, MD, senior and junior representatives of ACAAI's Fellows-In-Training (FITs) to the
FIT Board Review Corner March 2016 Welcome to the FIT Board Review Corner, prepared by Sarah Spriet, DO, and Tammy Peng, MD, senior and junior representatives of ACAAI's Fellows-In-Training (FITs) to the
T Lymphocyte Activation and Costimulation. FOCiS. Lecture outline
 1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
The development of T cells in the thymus
 T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
T cell maturation. T-cell Maturation. What allows T cell maturation?
 T-cell Maturation What allows T cell maturation? Direct contact with thymic epithelial cells Influence of thymic hormones Growth factors (cytokines, CSF) T cell maturation T cell progenitor DN DP SP 2ry
T-cell Maturation What allows T cell maturation? Direct contact with thymic epithelial cells Influence of thymic hormones Growth factors (cytokines, CSF) T cell maturation T cell progenitor DN DP SP 2ry
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Autoimmune Diseases File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_autoimmune_diseases
Corporate Medical Policy Hematopoietic Stem-Cell Transplantation for Autoimmune Diseases File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_stem-cell_transplantation_for_autoimmune_diseases
Synergistic combinations of targeted immunotherapy to combat cancer
 Synergistic combinations of targeted immunotherapy to combat cancer Myung Ah Lee, M.D., Ph. D Division of Medical Oncology, Hepato-biliary pancreatic cancer center Seoul St. Mary s hospital, The Catholic
Synergistic combinations of targeted immunotherapy to combat cancer Myung Ah Lee, M.D., Ph. D Division of Medical Oncology, Hepato-biliary pancreatic cancer center Seoul St. Mary s hospital, The Catholic
T Cell Differentiation
 T Cell Differentiation Ned Braunstein, MD MHC control of Immune Responsiveness: Concept Whether or not an individual makes an immune response to a particular antigen depends on what MHC alleles an individual
T Cell Differentiation Ned Braunstein, MD MHC control of Immune Responsiveness: Concept Whether or not an individual makes an immune response to a particular antigen depends on what MHC alleles an individual
Mucosal Immune System
 Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Exam Format 100 points - 60 pts mandatory; 40 points where 4, 10 point questions will be chosen Some open-ended questions, some short answer. Kuby question Cytokines Terminology How do cytokines achieve
Tolerance 2. Regulatory T cells; why tolerance fails. Abul K. Abbas UCSF. FOCiS
 1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
A Tolerance Approach to the Transplantation of Vascularized Tissues
 A Tolerance Approach to the Transplantation of Vascularized Tissues The 9th New Jersey Symposium on Biomaterials Science and Regenerative Medicine October 29-31, 2008 David H. Sachs, M.D. Harvard Medical
A Tolerance Approach to the Transplantation of Vascularized Tissues The 9th New Jersey Symposium on Biomaterials Science and Regenerative Medicine October 29-31, 2008 David H. Sachs, M.D. Harvard Medical
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
GUIDELINES FOR IRRADIATED BLOOD COMPONENTS
 GUIDELINES FOR IRRADIATED BLOOD COMPONENTS 1. Policy Statement 2. Definitions 1.1 Blood transfusion services shall have a policy which indicates recipients who are to receive irradiated blood components.
GUIDELINES FOR IRRADIATED BLOOD COMPONENTS 1. Policy Statement 2. Definitions 1.1 Blood transfusion services shall have a policy which indicates recipients who are to receive irradiated blood components.
Immunology. Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency
 Immunology Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency Transplant Immunology Transplantation is the process of moving cells, tissues or organs from one site to another
Immunology Anas Abu-Humaidan M.D. Ph.D. Transplant immunology+ Secondary immune deficiency Transplant Immunology Transplantation is the process of moving cells, tissues or organs from one site to another
CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells
 CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells Karin Pfisterer, Karoline M Lipnik, Erhard Hofer and Adelheid Elbe-Bürger Journal of Investigative Dermatology (2015)
CD90 + Human Dermal Stromal Cells Are Potent Inducers of FoxP3 + Regulatory T Cells Karin Pfisterer, Karoline M Lipnik, Erhard Hofer and Adelheid Elbe-Bürger Journal of Investigative Dermatology (2015)
T Cell Development II: Positive and Negative Selection
 T Cell Development II: Positive and Negative Selection 8 88 The two phases of thymic development: - production of T cell receptors for antigen, by rearrangement of the TCR genes CD4 - selection of T cells
T Cell Development II: Positive and Negative Selection 8 88 The two phases of thymic development: - production of T cell receptors for antigen, by rearrangement of the TCR genes CD4 - selection of T cells
MECHANISMS OF CELLULAR REJECTION IN ORGAN TRANSPLANTATION AN OVERVIEW
 MECHANISMS OF CELLULAR REJECTION IN ORGAN TRANSPLANTATION AN OVERVIEW YVON LEBRANCHU Service Néphrologie et Immunologie Clinique CHU TOURS ANTIGEN PRESENTING CELL CD4 + T CELL CYTOKINE PRODUCTION CLONAL
MECHANISMS OF CELLULAR REJECTION IN ORGAN TRANSPLANTATION AN OVERVIEW YVON LEBRANCHU Service Néphrologie et Immunologie Clinique CHU TOURS ANTIGEN PRESENTING CELL CD4 + T CELL CYTOKINE PRODUCTION CLONAL
Robert B. Colvin, M.D. Department of Pathology Massachusetts General Hospital Harvard Medical School
 Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Robert B. Colvin Transplantation: Friendly organs in a hostile environment Robert B. Colvin,
Harvard-MIT Division of Health Sciences and Technology HST.035: Principle and Practice of Human Pathology Dr. Robert B. Colvin Transplantation: Friendly organs in a hostile environment Robert B. Colvin,
Hematopoietic Stem Cells, Stem Cell Processing, and Transplantation
 Hematopoietic Stem Cells, Stem Cell Processing, and Joseph (Yossi) Schwartz, M irector, Hemotherapy and Stem Cell Processing Facility Bone Marrow Can Cure: Leukemia Lymphoma Multiple Myeloma Genetic iseases:
Hematopoietic Stem Cells, Stem Cell Processing, and Joseph (Yossi) Schwartz, M irector, Hemotherapy and Stem Cell Processing Facility Bone Marrow Can Cure: Leukemia Lymphoma Multiple Myeloma Genetic iseases:
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology
 Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Attribution: University of Michigan Medical School, Department of Microbiology and Immunology License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Harnessing tolerance mechanisms with monoclonal antibodies Prof. Herman Waldmann
 Harnessing tolerance mechanisms Herman Waldmann Sir William Dunn School of Pathology, Oxford University, UK 1 1. Transplantation 2 Lymphocyte depletion strategies to minimise drug immunosuppression in
Harnessing tolerance mechanisms Herman Waldmann Sir William Dunn School of Pathology, Oxford University, UK 1 1. Transplantation 2 Lymphocyte depletion strategies to minimise drug immunosuppression in
HLA and antigen presentation. Department of Immunology Charles University, 2nd Medical School University Hospital Motol
 HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
HLA and antigen presentation Department of Immunology Charles University, 2nd Medical School University Hospital Motol MHC in adaptive immunity Characteristics Specificity Innate For structures shared
Examples of questions for Cellular Immunology/Cellular Biology and Immunology
 Examples of questions for Cellular Immunology/Cellular Biology and Immunology Each student gets a set of 6 questions, so that each set contains different types of questions and that the set of questions
Examples of questions for Cellular Immunology/Cellular Biology and Immunology Each student gets a set of 6 questions, so that each set contains different types of questions and that the set of questions
Allotransplantation of Cryopreserved Parathyroid Tissue for Severe Hypocalcemia in a Renal Transplant Recipient
 American Journal of Transplantation 2010; 10: 2061 2065 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2010; 10: 2061 2065 Wiley Periodicals Inc. C 2010 The Authors Journal compilation C 2010 The American Society of Transplantation and the American Society of Transplant
Defensive mechanisms include :
 Acquired Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated immunity Humoral immunity Two mechanisms 1) Humoral
Acquired Immunity Defensive mechanisms include : 1) Innate immunity (Natural or Non specific) 2) Acquired immunity (Adaptive or Specific) Cell-mediated immunity Humoral immunity Two mechanisms 1) Humoral
Summary of T32 Research Joshua Weiner June 2015
 Summary of T32 Research Joshua Weiner June 2015 Project 1: Regulatory T Cell (Treg) Expansion Xenotransplantation could help make up the difference in the numbers of organs needed for transplantation and
Summary of T32 Research Joshua Weiner June 2015 Project 1: Regulatory T Cell (Treg) Expansion Xenotransplantation could help make up the difference in the numbers of organs needed for transplantation and
CHAPTER 3 LABORATORY PROCEDURES
 CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
CHAPTER 3 LABORATORY PROCEDURES CHAPTER 3 LABORATORY PROCEDURES 3.1 HLA TYPING Molecular HLA typing will be performed for all donor cord blood units and patients in the three reference laboratories identified
T cell manipulation of the graft: Yes
 T cell manipulation of the graft: Yes J.H. Frederik Falkenburg Department of Hematology L M U C Allogeneic Hematopoietic Stem Cell Transplantation (SCT) for non-malignant disorders: no need for anti-tumor
T cell manipulation of the graft: Yes J.H. Frederik Falkenburg Department of Hematology L M U C Allogeneic Hematopoietic Stem Cell Transplantation (SCT) for non-malignant disorders: no need for anti-tumor
T cell development October 28, Dan Stetson
 T cell development October 28, 2016 Dan Stetson stetson@uw.edu 441 Lecture #13 Slide 1 of 29 Three lectures on T cells (Chapters 8, 9) Part 1 (Today): T cell development in the thymus Chapter 8, pages
T cell development October 28, 2016 Dan Stetson stetson@uw.edu 441 Lecture #13 Slide 1 of 29 Three lectures on T cells (Chapters 8, 9) Part 1 (Today): T cell development in the thymus Chapter 8, pages
Autoimmunity & Transplantation. Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel:
 Autoimmunity & Transplantation Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Recognize
Autoimmunity & Transplantation Dr. Aws Alshamsan Department of Pharmaceu5cs Office: AA87 Tel: 4677363 aalshamsan@ksu.edu.sa Learning Objectives By the end of this lecture you will be able to: 1 Recognize
Advancing Opportunities To Prevent Type 1 Diabetes
 Advancing Opportunities To Prevent Type 1 Diabetes Dr. Allison Green Centre for Immunology and Infection Hull York Medical School York University Type 1 Diabetes Insulin deficiency destabilizes regulation
Advancing Opportunities To Prevent Type 1 Diabetes Dr. Allison Green Centre for Immunology and Infection Hull York Medical School York University Type 1 Diabetes Insulin deficiency destabilizes regulation
S. No Topic Class No Date
 S. No Topic Class No Date 1 Introduction 2 3 4 5 6 7 Fundamentals of Immunology Definitions and basic terms Types of immunity Organs of immune system Cells of immune system Innate immunity PAMPs PRRs Phagocytosis
S. No Topic Class No Date 1 Introduction 2 3 4 5 6 7 Fundamentals of Immunology Definitions and basic terms Types of immunity Organs of immune system Cells of immune system Innate immunity PAMPs PRRs Phagocytosis
Immune Tolerance. Kyeong Cheon Jung. Department of Pathology Seoul National University College of Medicine
 Immune Tolerance Kyeong Cheon Jung Department of Pathology Seoul National University College of Medicine Immune tolerance Unresponsiveness to an antigen that is induced by previous exposure to that antigen
Immune Tolerance Kyeong Cheon Jung Department of Pathology Seoul National University College of Medicine Immune tolerance Unresponsiveness to an antigen that is induced by previous exposure to that antigen
Ron Shapiro, MD, Abdul S. Rao, MD, D. Phil., Paulo Fontes, MD, Adrianna Zeevi, Ph.D., Mark Jordan, MD, Velma P. Scantlebury, MD,
 Kidney IBone Marrow Transplantation Ron Shapiro, MD, Abdul S. Rao, MD, D. Phil., Paulo Fontes, MD, Adrianna Zeevi, Ph.D., Mark Jordan, MD, Velma P. Scantlebury, MD, Carlos Vivas, MD, H. Albin Gritsch,
Kidney IBone Marrow Transplantation Ron Shapiro, MD, Abdul S. Rao, MD, D. Phil., Paulo Fontes, MD, Adrianna Zeevi, Ph.D., Mark Jordan, MD, Velma P. Scantlebury, MD, Carlos Vivas, MD, H. Albin Gritsch,
Disruption of Healthy Tissue by the Immune Response Autoimmune diseases: Inappropriate immune response against self-components
 Chapter 13 Disruption of Healthy Tissue by the Immune Response Autoimmune diseases: Inappropriate immune response against self-components Humoral imm 胞外 胞內 CMI: CD8 T Self Ag Self(Auto) antigen (encoded
Chapter 13 Disruption of Healthy Tissue by the Immune Response Autoimmune diseases: Inappropriate immune response against self-components Humoral imm 胞外 胞內 CMI: CD8 T Self Ag Self(Auto) antigen (encoded
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
Before beginning the practice test, please read this announcement:
 Before beginning the practice test, please read this announcement: As mentioned in the UCF SI Wordpress site and in class, I will not be able to hold a review session for this test due to my personal schedule.
Before beginning the practice test, please read this announcement: As mentioned in the UCF SI Wordpress site and in class, I will not be able to hold a review session for this test due to my personal schedule.
Tolerance and Cancer: Mechanisms of Tumor Evasion and Strategies for Breaking Tolerance Markus Y. Mapara and Megan Sykes
 VOLUME 22 NUMBER 6 MARCH 15 2004 JOURNAL OF CLINICAL ONCOLOGY B I O L O G Y O F N E O P L A S I A Tolerance and Cancer: Mechanisms of Tumor Evasion and Strategies for Breaking Tolerance Markus Y. Mapara
VOLUME 22 NUMBER 6 MARCH 15 2004 JOURNAL OF CLINICAL ONCOLOGY B I O L O G Y O F N E O P L A S I A Tolerance and Cancer: Mechanisms of Tumor Evasion and Strategies for Breaking Tolerance Markus Y. Mapara
Role of NMDP Repository in the Evolution of HLA Matching and Typing for Unrelated Donor HCT
 Role of NMDP Repository in the Evolution of HLA Matching and Typing for Unrelated Donor HCT Stephen Spellman, MBS Director, Immunobiology and Observational Research Assistant Scientific Director CIBMTR,
Role of NMDP Repository in the Evolution of HLA Matching and Typing for Unrelated Donor HCT Stephen Spellman, MBS Director, Immunobiology and Observational Research Assistant Scientific Director CIBMTR,
Overview B cell development T cell development
 Topics Overview B cell development T cell development Lymphocyte development overview (Cont) Receptor diversity is produced by gene rearrangement and is random Includes specificities that will bind to
Topics Overview B cell development T cell development Lymphocyte development overview (Cont) Receptor diversity is produced by gene rearrangement and is random Includes specificities that will bind to
Priming the Immune System to Kill Cancer and Reverse Tolerance. Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics
 Priming the Immune System to Kill Cancer and Reverse Tolerance Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics Learning Objectives Describe the role of the immune system in cancer
Priming the Immune System to Kill Cancer and Reverse Tolerance Dr. Diwakar Davar Assistant Professor, Melanoma and Phase I Therapeutics Learning Objectives Describe the role of the immune system in cancer
Principles of Adaptive Immunity
 Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Principles of Adaptive Immunity Chapter 3 Parham Hans de Haard 17 th of May 2010 Agenda Recognition molecules of adaptive immune system Features adaptive immune system Immunoglobulins and T-cell receptors
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/20522 holds various files of this Leiden University dissertation. Author: Stevanović, Sanja Title: Exploiting HLA-class II disparity for anti-tumor immunity
Cover Page The handle http://hdl.handle.net/1887/20522 holds various files of this Leiden University dissertation. Author: Stevanović, Sanja Title: Exploiting HLA-class II disparity for anti-tumor immunity
Tumor Immunity and Immunotherapy. Andrew Lichtman M.D., Ph.D. Brigham and Women s Hospital Harvard Medical School
 Tumor Immunity and Immunotherapy Andrew Lichtman M.D., Ph.D. Brigham and Women s Hospital Harvard Medical School Lecture Outline Evidence for tumor immunity Types of tumor antigens Generation of anti-tumor
Tumor Immunity and Immunotherapy Andrew Lichtman M.D., Ph.D. Brigham and Women s Hospital Harvard Medical School Lecture Outline Evidence for tumor immunity Types of tumor antigens Generation of anti-tumor
Adaptive (acquired) immunity. Professor Peter Delves University College London
 Adaptive (acquired) immunity Professor Peter Delves University College London p.delves@ucl.ac.uk Haematopoiesis Haematopoiesis Lymphocytes = adaptive response Recognition of pathogens by adaptive cells,
Adaptive (acquired) immunity Professor Peter Delves University College London p.delves@ucl.ac.uk Haematopoiesis Haematopoiesis Lymphocytes = adaptive response Recognition of pathogens by adaptive cells,
T Cell Activation, Costimulation and Regulation
 1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
LESSON 2: THE ADAPTIVE IMMUNITY
 Introduction to immunology. LESSON 2: THE ADAPTIVE IMMUNITY Today we will get to know: The adaptive immunity T- and B-cells Antigens and their recognition How T-cells work 1 The adaptive immunity Unlike
Introduction to immunology. LESSON 2: THE ADAPTIVE IMMUNITY Today we will get to know: The adaptive immunity T- and B-cells Antigens and their recognition How T-cells work 1 The adaptive immunity Unlike
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16
 COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
Haplo vs Cord vs URD Debate
 3rd Annual ASBMT Regional Conference for NPs, PAs and Fellows Haplo vs Cord vs URD Debate Claudio G. Brunstein Associate Professor University of Minnesota Medical School Take home message Finding a donor
3rd Annual ASBMT Regional Conference for NPs, PAs and Fellows Haplo vs Cord vs URD Debate Claudio G. Brunstein Associate Professor University of Minnesota Medical School Take home message Finding a donor
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep
 The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
The Immune System: Innate and Adaptive Body Defenses Outline PART 1: INNATE DEFENSES 21.1 Surface barriers act as the first line of defense to keep invaders out of the body (pp. 772 773; Fig. 21.1; Table
Self Tolerance and MHC Restriction. Dr. Issa Abu-Dayyeh
 Self Tolerance and MHC Restriction Dr. Issa Abu-Dayyeh How do we teach B and T cells not to recognise self antigens as dangerous? How do we restrict T cells to recognise only Ags presented on a self MHC
Self Tolerance and MHC Restriction Dr. Issa Abu-Dayyeh How do we teach B and T cells not to recognise self antigens as dangerous? How do we restrict T cells to recognise only Ags presented on a self MHC
Trends in Hematopoietic Cell Transplantation. AAMAC Patient Education Day Oct 2014
 Trends in Hematopoietic Cell Transplantation AAMAC Patient Education Day Oct 2014 Objectives Review the principles behind allogeneic stem cell transplantation Outline the process of transplant, some of
Trends in Hematopoietic Cell Transplantation AAMAC Patient Education Day Oct 2014 Objectives Review the principles behind allogeneic stem cell transplantation Outline the process of transplant, some of
Tumors arise from accumulated genetic mutations. Tumor Immunology (Cancer)
 Tumor Immunology (Cancer) Tumors arise from accumulated genetic mutations Robert Beatty MCB150 Mutations Usually have >6 mutations in both activation/growth factors and tumor suppressor genes. Types of
Tumor Immunology (Cancer) Tumors arise from accumulated genetic mutations Robert Beatty MCB150 Mutations Usually have >6 mutations in both activation/growth factors and tumor suppressor genes. Types of
ASH 2011 aktualijos: MSC TPŠL gydyme. Mindaugas Stoškus VULSK HOTC MRMS
 ASH 2011 aktualijos: MSC TPŠL gydyme Mindaugas Stoškus VULSK HOTC MRMS #3042. Yukiyasu Ozawa et al. Mesenchymal Stem Cells As a Treatment for Steroid-Resistant Acute Graft Versus Host Disease (agvhd);
ASH 2011 aktualijos: MSC TPŠL gydyme Mindaugas Stoškus VULSK HOTC MRMS #3042. Yukiyasu Ozawa et al. Mesenchymal Stem Cells As a Treatment for Steroid-Resistant Acute Graft Versus Host Disease (agvhd);
Introduction. Introduction. Lymphocyte development (maturation)
 Introduction Abbas Chapter 8: Lymphocyte Development and the Rearrangement and Expression of Antigen Receptor Genes Christina Ciaccio, MD Children s Mercy Hospital January 5, 2009 Lymphocyte development
Introduction Abbas Chapter 8: Lymphocyte Development and the Rearrangement and Expression of Antigen Receptor Genes Christina Ciaccio, MD Children s Mercy Hospital January 5, 2009 Lymphocyte development
PROBLEMS WITH THE IMMUNE SYSTEM. Blood Types, Transplants, Allergies, Autoimmune diseases, Immunodeficiency Diseases
 PROBLEMS WITH THE IMMUNE SYSTEM Blood Types, Transplants, Allergies, Autoimmune diseases, Immunodeficiency Diseases Antigens on red blood cells determine whether a person has type A, B, AB, or O blood
PROBLEMS WITH THE IMMUNE SYSTEM Blood Types, Transplants, Allergies, Autoimmune diseases, Immunodeficiency Diseases Antigens on red blood cells determine whether a person has type A, B, AB, or O blood
Transplantation Immunology
 Transplantation Immunology Mitchell S. Cairo, MD Professor of Pediatrics, Medicine and Pathology Chief, Division, Pediatric Hematology & Blood & Marrow Transplantation Children s Hospital New York Presbyterian
Transplantation Immunology Mitchell S. Cairo, MD Professor of Pediatrics, Medicine and Pathology Chief, Division, Pediatric Hematology & Blood & Marrow Transplantation Children s Hospital New York Presbyterian
Transplantation Immunology
 Transplantation Immunology MHC Restricted Allograft Rejection Mitchell S. Cairo, MD Professor of Pediatrics, Medicine and Pathology Chief, Division, Pediatric Hematology & Blood & Marrow Transplantation
Transplantation Immunology MHC Restricted Allograft Rejection Mitchell S. Cairo, MD Professor of Pediatrics, Medicine and Pathology Chief, Division, Pediatric Hematology & Blood & Marrow Transplantation
Tolerance 2. Regulatory T cells; why tolerance fails. FOCiS. Lecture outline. Regulatory T cells. Regulatory T cells: functions and clinical relevance
 1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
1 Tolerance 2. Regulatory T cells; why tolerance fails Abul K. Abbas UCSF FOCiS 2 Lecture outline Regulatory T cells: functions and clinical relevance Pathogenesis of autoimmunity: why selftolerance fails
Mesenchymal Stem Cells
 Mesenchymal Stem Cells Science and therapeutic applications Dirk Büscher (Former VP-R&D Cellerix) GRIFOLS SA May 10 th, 2010 EMA 1 Discovery and Definition of Mesenchymal Stem Cells MSC must be plastic-adherent
Mesenchymal Stem Cells Science and therapeutic applications Dirk Büscher (Former VP-R&D Cellerix) GRIFOLS SA May 10 th, 2010 EMA 1 Discovery and Definition of Mesenchymal Stem Cells MSC must be plastic-adherent
5/9/2018. Bone marrow failure diseases (aplastic anemia) can be cured by providing a source of new marrow
 5/9/2018 or Stem Cell Harvest Where we are now, and What s Coming AA MDS International Foundation Indianapolis IN Luke Akard MD May 19, 2018 Infusion Transplant Conditioning Treatment 2-7 days STEM CELL
5/9/2018 or Stem Cell Harvest Where we are now, and What s Coming AA MDS International Foundation Indianapolis IN Luke Akard MD May 19, 2018 Infusion Transplant Conditioning Treatment 2-7 days STEM CELL
IMMUNOTHERAPY FOR CANCER A NEW HORIZON. Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust
 IMMUNOTHERAPY FOR CANCER A NEW HORIZON Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust ASCO Names Advance of the Year: Cancer Immunotherapy No recent
IMMUNOTHERAPY FOR CANCER A NEW HORIZON Ekaterini Boleti MD, PhD, FRCP Consultant in Medical Oncology Royal Free London NHS Foundation Trust ASCO Names Advance of the Year: Cancer Immunotherapy No recent
A Review of Guidelines and Evidence for the Use of Irradiated Blood Products in Solid Tumor, Chemotherapy Patients. Chris Kim 11/29/12
 A Review of Guidelines and Evidence for the Use of Irradiated Blood Products in Solid Tumor, Chemotherapy Patients Chris Kim 11/29/12 Background Prevention of TAGVHD Irradiation: induces DNA crosslinks,
A Review of Guidelines and Evidence for the Use of Irradiated Blood Products in Solid Tumor, Chemotherapy Patients Chris Kim 11/29/12 Background Prevention of TAGVHD Irradiation: induces DNA crosslinks,
Primer on Tumor Immunology. International Society for Biological Therapy of Cancer. C. H. June, M.D. November 10, 2005
 Primer on Tumor Immunology International Society for Biological Therapy of Cancer C. H. June, M.D. November 10, 2005 Outline: Primer on Tumor Immunology T Cell Receptors T Cell Biology Tumor immunology
Primer on Tumor Immunology International Society for Biological Therapy of Cancer C. H. June, M.D. November 10, 2005 Outline: Primer on Tumor Immunology T Cell Receptors T Cell Biology Tumor immunology
Antigen capture and presentation to T lymphocytes
 Antigen capture and presentation to T lymphocytes What T lymphocytes see Innate Immunity Immediately available or Very broad specificity rapidly recruited Adaptive Immunity Rare and naïve cells require
Antigen capture and presentation to T lymphocytes What T lymphocytes see Innate Immunity Immediately available or Very broad specificity rapidly recruited Adaptive Immunity Rare and naïve cells require
