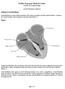
Name of Policy: Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins as a Treatment of Atrial Fibrillation
|
|
|
- Sheila Crawford
- 5 years ago
- Views:
Transcription
1 Name of Policy: Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins as a Treatment of Atrial Fibrillation Policy #: 283 Latest Review Date: June 2014 Category: Medical Policy Grade: A Background/Definitions: As a general rule, benefits are payable under Blue Cross and Blue Shield of Alabama health plans only in cases of medical necessity and only if services or supplies are not investigational, provided the customer group contracts have such coverage. The following Association Technology Evaluation Criteria must be met for a service/supply to be considered for coverage: 1. The technology must have final approval from the appropriate government regulatory bodies; 2. The scientific evidence must permit conclusions concerning the effect of the technology on health outcomes; 3. The technology must improve the net health outcome; 4. The technology must be as beneficial as any established alternatives; 5. The improvement must be attainable outside the investigational setting. Medical Necessity means that health care services (e.g., procedures, treatments, supplies, devices, equipment, facilities or drugs) that a physician, exercising prudent clinical judgment, would provide to a patient for the purpose of preventing, evaluating, diagnosing or treating an illness, injury or disease or its symptoms, and that are: 1. In accordance with generally accepted standards of medical practice; and 2. Clinically appropriate in terms of type, frequency, extent, site and duration and considered effective for the patient s illness, injury or disease; and 3. Not primarily for the convenience of the patient, physician or other health care provider; and 4. Not more costly than an alternative service or sequence of services at least as likely to produce equivalent therapeutic or diagnostic results as to the diagnosis or treatment of that patient s illness, injury or disease. Page 1 of 24
2 Description of Procedure or Service: Radiofrequency ablation using a percutaneous catheter-based approach is widely used to treat supraventricular arrhythmias. Atrial fibrillation frequently arises from an abnormal focus at or near the junction of the pulmonary veins and the left atrium, thus leading to the feasibility of more focused ablation techniques directed at these structures. Catheter-based ablation, using both radiofrequency ablation and cryoablation, is being studied in the treatment of various types of atrial fibrillation. Atrial fibrillation (AF) is the most common sustained cardiac arrhythmia and is associated with considerable morbidity and a decrease in the quality of life. The prevalence of AF is estimated at 0.4% of the general population and increases with age. At present, approximately 2.3 million adults in the U.S. have AF. AF is primarily a disorder of the atrial pacemaker, which initiates the electrical activity leading to coordinated contractions of the atria and ventricles. The underlying mechanism of AF involves interplay between the electrical triggering events and the myocardial substrate that permits propagation and maintenance of the aberrant electrical circuit. The most common focal trigger of AF appears to be located within the cardiac muscle that extends into the pulmonary veins. AF accounts for approximately one-third of hospitalizations for cardiac rhythm disturbances. Symptoms of AF, e.g., palpitations, decreased exercise tolerance, and dyspnea, are primarily related to poorly controlled or irregular heart rate. The loss of AV synchrony results in a decreased cardiac output, which can be significant in patients with compromised cardiac function. In addition, patients with AF are at higher risk for stroke and thromboembolic events, and anticoagulation is typically recommended. AF is also associated with other cardiac conditions, such as valvular heart disease, heart failure, hypertension and diabetes. Although episodes of AF can be converted to normal sinus rhythm using either pharmacologic or electroshock conversion, the natural history of AF is one of recurrence, thought to be related to fibrillation induced anatomic and electrical remodeling of the atria. AF represents a relatively heterogeneous disorder. AF can be subdivided into paroxysmal (selfterminating), persistent (non-self terminating), or permanent. Treatment strategies can be broadly subdivided into rate control, in which only the ventricular rate is controlled and the atria are allowed to fibrillate, or rhythm control, in which there is an attempt to re-establish and maintain normal sinus rhythm. Rhythm control has long been considered an important treatment goal for AF management, although it should be noted that its primacy has recently been challenged by the results of two randomized trials, both of which reported that pharmacologically maintained rhythm control offered no improvement in mortality compared to rate control. In any event, in patients with persistent AF, rhythm control typically involves initial pharmacologic or electronic cardioversion, followed by pharmacologic maintenance of normal sinus rhythm. However, episodes of recurrent AF are typical, and patients may require multiple episodes of cardioversion. Implantable defibrillators, which are designed to detect and terminate an episode of AF, may be an alternative in patients otherwise requiring serial cardioversions. Patients with paroxysmal AF, by definition, do not require cardioversion, but may be treated pharmacologically to prevent further episodes of AF. Treatment of permanent AF, by definition, Page 2 of 24
3 focuses on rate control, using either pharmacologic therapy or ablation of the AV node followed by ventricular pacing. Although AV nodal ablation produces symptomatic improvement, it does entail lifelong anticoagulation (due to the ongoing fibrillation of the atria), loss of AV synchrony, and lifelong pacemaker dependency. Implantable defibrillators are contraindicated in patients with permanent AF. The above treatment options are not considered curative. A variety of ablative procedures have been investigated as potentially curative approaches, or perhaps modifying the arrhythmia such that drug therapy becomes more effective. Ablative approaches focus on interruption of the electrical pathways that contribute to AF, through modifying the triggers of AF and/or the myocardial substrate that maintains the aberrant rhythm. The Maze procedure, an open surgical procedure often combined with other cardiac surgeries (e.g., valve repair) is an ablative procedure involving sequential atriotome incisions designed to create electrical barriers that prevent the maintenance of AF. Since the inception of this technique in the early 1990s, there has been a progressive understanding of the underlying electrical pathways in the heart, such that catheter based radiofrequency procedures have become feasible. Radiofrequency ablation is a widely used technique for a variety of supraventricular arrhythmias where intracardiac mapping identifies a discrete arrhythmogenic focus that is the target of ablation. The situation is more complex for AF, since there is not a single arrhythmogenic focus. However, the recent recognition that triggering foci are commonly located within the myocytes extending into the pulmonary veins creates a potential target for ablation. Three basic strategies have emerged: focal ablation within the pulmonary veins, as identified by electrophysiologic mapping; segmental ostial ablation guided by pulmonary vein potential (electrical approach); or circumferential pulmonary vein ablation (anatomic approach). Circumferential pulmonary vein ablation using radiofrequency energy appears to be the preferred approach at the present time. The procedure also can be done using cryoablation technology. Use of currently available catheters for AF has a steep learning curve because they require extensive guiding to multiple ablation points. One of the potential advantages to cryoablation techniques is that cryoablation catheters have a circular or shaped end point, allowing a one-shot ablation. Other types of radiofrequency catheters, such as Medtronic s radiofrequency-based Pulmonary Vein Ablation Catheter, that incorporate circular or otherwise shaped end points are under investigation. Repeat procedures following an initial radiofrequency ablation are commonly performed if atrial fibrillation recurs or if atrial flutter develops post-procedure. The need for repeat procedures may, in part, depend on clinical characteristics of the patient (age, persistent vs. paroxysmal atrial fibrillation, atrial dilatation, etc.), and the type of initial ablation performed. Repeat procedures are generally more limited than the initial procedure. For example, in cases where electrical reconnections occur as a result of incomplete ablation lines, a touch up procedure is done to correct gaps in the original ablation. In other cases where atrial flutter develops following ablation a "flutter ablation is performed, which is more limited than the original atrial fibrillation ablation procedure. A number of clinical and demographic factors have been associated with the need for a second procedure, including age, length of atrial fibrillation, permanent atrial fibrillation, left atrial size, and left-ventricular ejection fraction. Page 3 of 24
4 Policy: Effective for dates of service on or after May 1, 2014: Transcatheter ablation of arrhythmogenic foci in the pulmonary veins (pulmonary vein isolation) by means of radiofrequency energy or cryoballoon ablation, meets Blue Cross and Blue Shield of Alabama s medical criteria for coverage as a treatment for atrial fibrillation when all the following criteria are met: There is no significant structural heart disease. Individual case consideration will be given to patients with hypertrophic cardiomyopathy (both primary and secondary to hypertension), other forms of left ventricular hypertrophy (LVH), coronary artery disease (CSD), or mild forms of valvular heart disease. Patients have recurrent, symptomatic AF. Patients have failed treatment with two or more antiarrhythmic drugs (or have intolerance of or a contraindication to appropriate antiarrhythmic drug therapy). Patients with Class II or III congestive heart failure and symptomatic AF in whom heart rate is poorly controlled by standard medications, as an alternative to atrioventricular nodal ablation and pacemaker insertion. OR Transcatheter ablation of arrhythmogenic foci in the pulmonary veins does not meet Blue Cross and Blue Shield of Alabama s medical criteria for coverage and is considered investigational as a treatment for all indications except for specific cases of atrial fibrillation as noted above. Effective for dates of service on or after June 1, 2013 and prior to May 1, 2014: Transcatheter ablation of arrhythmogenic foci in the pulmonary veins (pulmonary vein isolation) by means of radiofrequency energy or cryoballoon ablation, meets Blue Cross and Blue Shield of Alabama s medical criteria for coverage as a treatment for atrial fibrillation when all the following criteria are met: 1. There is no significant structural heart disease. Individual case consideration will be given to patients with hypertrophic cardiomyopathy (both primary and secondary to hypertension), other forms of left ventricular hypertrophy (LVH), coronary artery disease (CSD), or mild forms of valvular heart disease. 2. Patients have recurrent, symptomatic AF. 3. Patients have failed treatment with two or more antiarrhythmic drugs (or have intolerance of or a contraindication to appropriate antiarrhythmic drug therapy). OR 4. Patients with Class II or III congestive heart failure and symptomatic AF in whom heart rate is poorly controlled by standard medications, as an alternative to atrioventricular nodal ablation and pacemaker insertion. Page 4 of 24
5 Transcatheter ablation of arrhythmogenic foci in the pulmonary veins does not meet Blue Cross and Blue Shield of Alabama s medical criteria for coverage and is considered investigational as a treatment for all indications except for specific cases of atrial fibrillation as noted above. Effective for dates of service prior to June 1, 2013: Transcatheter ablation of arrhythmogenic foci in the pulmonary veins as a treatment for atrial fibrillation (AF) meets Blue Cross and Blue Shield of Alabama s medical criteria for coverage when the following criteria are met: 1. There is no significant structural heart disease. Individual case consideration will be given to patients with hypertrophic cardiomyopathy (both primary and secondary to hypertension), other forms of left ventricular hypertrophy (LVH), coronary artery disease (CSD), or mild forms of valvular heart disease. 2. Patients have recurrent, symptomatic AF. 3. Patients have failed treatment with two or more antiarrhythmic drugs (or have intolerance of or a contraindication to appropriate antiarrhythmic drug therapy). OR 4. Patients with Class II or III congestive heart failure and symptomatic AF in whom heart rate is poorly controlled by standard medications, as an alternative to atrioventricular nodal ablation and pacemaker insertion. Transcatheter ablation of arrhythmogenic foci in the pulmonary veins does not meet Blue Cross and Blue Shield of Alabama s medical criteria for coverage and is considered investigational as a treatment for all indications except for specific cases of atrial fibrillation as noted above. Transcatheter cryoablation of arrhythmogenic foci in the pulmonary veins as a treatment for atrial fibrillation does not meet Blue Cross and Blue Shield of Alabama s medical criteria for coverage and is considered investigational. Blue Cross and Blue Shield of Alabama does not approve or deny procedures, services, testing, or equipment for our members. Our decisions concern coverage only. The decision of whether or not to have a certain test, treatment or procedure is one made between the physician and his/her patient. Blue Cross and Blue Shield of Alabama administers benefits based on the members' contract and corporate medical policies. Physicians should always exercise their best medical judgment in providing the care they feel is most appropriate for their patients. Needed care should not be delayed or refused because of a coverage determination. Page 5 of 24
6 Key Points: This policy was originally created in 2004 and updated periodically with literature review since that time. The most recent literature search was performed through February 4, Following is a summary of the key literature to date. In patients with paroxysmal or persistent atrial fibrillation (AF), catheter ablation may be considered an alternative to drug therapy. In patients with permanent AF, catheter ablation may be considered an alternative to drug therapy or to atrioventricular (AV) nodal ablation and pacing. For all types of AF, it is possible that catheter ablation may not be curative as a sole treatment but might alter the underlying myocardial triggers or substrate in such a way that subsequent pharmacologic therapy may become more effective. There is ongoing controversy regarding the relative benefits of rhythm versus rate control in AF, which underlies the evaluation of evidence on catheter ablation. Randomized trials of pharmacologic therapies have not demonstrated the superiority of rhythm versus rate control. However, the apparent equivalency of these two strategies with pharmacologic therapy cannot be extrapolated to the rhythm control achieved with ablation. Antiarrhythmic medications used for rhythm control are only partially effective and have serious complications, including proarrhythmic properties, which can be lethal. Therefore, nonpharmacologic strategies for rhythm control have the potential to achieve superior outcomes than have been seen with pharmacologic strategies. A variety of outcomes for treatment of AF may be considered. The mortality and morbidity related to AF, such as cardiovascular mortality, stroke, and heart failure, are the most important clinical outcomes. However, these are uncommon events, and currently available trials are not powered to detect differences in these outcomes. Quality of life (QOL) is also an important outcome, as these measures reflect important manifestations of AF, such as symptoms and reduced exercise tolerance. AF has been shown to be associated with lower QOL scores, and maintenance of sinus rhythm has been associated with higher QOL scores for patients with paroxysmal AF. Recurrence of AF is a more problematic outcome measure, because the intermittent and often transient nature of recurrences makes accurate measurement difficult. This outcome measure has been reported in different ways. For example, the proportion of patients in sinus rhythm at the end of the study, the time to first recurrence, and the number of recurrences within a time period have been reported. A recent publication highlights the difficulties in measuring AF recurrence and recommends a measure of AF burden, defined as the percentage of time an individual is in AF, as the optimal measure of treatment efficacy. However, this parameter requires continuous monitoring over a relatively long period of time, which is inconvenient for patients, resource intensive, and usually not pragmatic in patients who do not already have an implanted pacemaker. Recommendations for outcome assessment in trials of AF treatment were included in the 2006 American College of Cardiology/American Heart Association practice guidelines for the treatment of AF. These guidelines pointed out that the appropriate end points for evaluation of treatment efficacy in patients with paroxysmal or persistent AF have little in common. For Page 6 of 24
7 example, in studies of persistent AF, the proportion of patients in sinus rhythm at the end of follow-up is a useful end point, but this is a less useful measure in studies of paroxysmal AF. Given all these variables, ideally, controlled clinical trials would report a range of outcomes (including QOL) and complications in homogeneous patient groups and compare with the most relevant treatment alternatives, such as pharmacologic therapy; defibrillator therapy; and AV nodal ablation, depending on the classification of AF (paroxysmal, persistent, permanent). RFA for AF The literature review for this policy was originally based on a 2008 TEC Assessment. Six randomized controlled trials (RCTs) met the inclusion criteria for this TEC Assessment. The trials differed in their patient populations, the specific catheter ablation techniques used, and the comparisons made. The trials addressed three distinct indications for catheter ablation: patients with paroxysmal AF, as a first-line treatment option (n=1 trial); patients with symptomatic paroxysmal or persistent AF who have failed treatment with antiarrhythmic drugs (n=4 trials); and patients with symptomatic AF and heart failure who have failed treatment with standard medications for rate control and who would otherwise be considered for AV nodal ablation and pacemaker insertion (n=1 trial). All six trials reported that maintenance of sinus rhythm was improved for the catheter ablation group. Recurrence rates of AF at one year ranged from 11% to 44% for the catheter ablation groups in these trials, compared with 63% to 96% for the medication groups. Four of the six trials reported QOL outcomes. One of these only reported within-group comparisons, as opposed to between-group comparisons. The other three trials reported improvements in QOL associated with catheter ablation. These QOL measures were self-reported, and because both trials were unblinded, there is the possibility of reporting bias due to placebo effect. None of the available trials reported meaningful data on cardiovascular morbidity and mortality associated with AF. The Assessment concluded that radiofrequency catheter ablation is more effective than medications in maintaining sinus rhythm across a wide spectrum of patients with AF and across different variations of catheter ablation. The evidence on QOL is suggestive, but not definitive, of a benefit for patients undergoing catheter ablation. For other outcomes, the evidence did not permit conclusions. It was not possible to estimate the rate of serious complications, such as pulmonary vein stenosis, cardiac tamponade, or atrioesophageal fistula with precision given the limited number of patients in the trials and the continued evolution of the technique. However, the rate of serious complications is expected to be low, likely in the 1% to 5% range. Based on these findings, TEC criteria were met for two indications: patients with symptomatic paroxysmal or persistent AF who have failed treatment with antiarrhythmic drugs and patients with symptomatic AF and heart failure who have failed treatment with standard medications for rate control and who would otherwise be considered for AV nodal ablation and pacemaker insertion. For the first indication, the conclusion followed from the premise that reducing episodes of recurrent AF for this population will reduce or eliminate the symptoms associated with episodes of AF. For the other indication, the single multicenter RCT available was judged sufficient to conclude that catheter ablation improved outcomes compared with the alternative, AV nodal ablation and pacemaker insertion. While this trial was relatively small, it was judged Page 7 of 24
8 to be otherwise of high quality and reported improvements of a relatively large magnitude across a range of clinically important outcome measures, including QOL, exercise tolerance, left-ventricular ejection fraction (LVEF), and maintenance of sinus rhythm. Since the publication of the 2008 TEC Assessment, several additional systematic reviews and meta-analyses of catheter ablation for AF have been published. A Cochrane Review on catheter ablation for paroxysmal and persistent AF was published in This review included seven RCTs of catheter ablation versus medical therapy. Main conclusions were that catheter ablation was superior at reducing the recurrence of AF (risk ratio [RR], 0.27; 95% confidence interval [CI], 0.18 to 0.41) but that there were no differences in mortality (RR=0.50; 95% CI, 0.04 to 5.65), embolic complications (RR=1.01; 95% CI, 0.18 to 5.68), or death from thromboembolism (RR=3.04; 95% CI, 0.13 to 73.4). In 2013, Ganesan et al published results from a systematic review and meta-analysis of studies reporting long-term outcomes after percutaneous catheter ablation for paroxysmal and nonparoxysmal AF. The authors included 19 studies (RCTs, case-control and cohort studies, case series) that reported catheter ablation outcomes at three years or more after the index ablation procedures. Sample sizes in these studies ranged from 39 to 1404, with a total of 6167 patients included overall. For a single procedure, the pooled overall success rate at 12 months post-procedure was 64.2% (95% CI, 57.5% to 70.3%). At late follow-up, the overall singleprocedure success, defined as freedom from atrial arrhythmia at latest follow-up, was 53.1% (95% CI, 46.2% to 60.0%). The pooled overall multiple-procedure long-term success rate was 79.8% (95% CI, 75.0% to 83.8%). The analysis was unable to identify any predictors of shortor long-term recurrence. Reporting of periprocedural complications was heterogeneous across the studies, but complication rates were generally low. Three systematic reviews and meta-analyses comparing RFA with antiarrhythmic drug therapy for AF were published from 2008 to Nair et al included six RCTs comparing RFA with antiarrhythmic drug therapy for AF, five of which were included in the TEC Assessment. Two systematic reviews published in 2008 summarized and synthesized the RCT evidence on catheter ablation versus alternate therapy. These reviews included four of the six trials reviewed for the TEC Assessment. Noheria et al included three of these four RCTs, as well as an additional small RCT of 30 patients not included in the TEC Assessment. Gjesdal et al included five RCTs in their analysis, including the four trials in the Noheria et al systematic review, and one additional trial (included in the TEC Assessment) that compared catheter ablation plus antiarrhythmic drugs with antiarrhythmic drugs alone. All three systematic reviews concluded that catheter ablation was more effective than pharmacologic treatment in maintaining normal sinus rhythm. Nair et al demonstrated a pooled relative risk for AF at one year after procedure of 0.35 compared with antiarrhythmic drug therapy. In combined analysis, Noheria et al reported AF-free survival at one year to be 75.7% in the catheter ablation group compared with 18.8% in the comparison group. The relative risk for maintaining sinus rhythm was 3.73 (95% CI, 2.47 to 5.63) for the catheter-ablation group compared with alternative treatment. Gjesdal et al concluded that the available evidence was of moderate quality and consistent in reporting that AF-free survival was superior for the catheter ablation group. However, due to unexplained heterogeneity, these authors did not perform a combined analysis. Page 8 of 24
9 Since the TEC Assessment, six additional RCTs comparing radiofrequency ablation (RFA) versus pharmacologic treatment have been identified. Wilber et al enrolled 167 patients who had failed at least one antiarrhythmic medication and had at least three AF episodes in the prior six months. Patients were randomly assigned to either catheter ablation or continued drug therapy and followed for nine months. At the end of follow-up, 66% of patients in the ablation group were free of recurrent AF compared with 16% of patients in the medication group. Adverse events related to treatment occurred in 4.9% (5/103) of patients treated with ablation and in 8.8% (5/57) of patients treated with medications. Forleo et al randomly assigned 70 patients with Type 2 diabetes and AF to either RFA or an antiarrhythmic medication. Follow-up was for one year, with the primary outcome being recurrence of AF. At the end of the trial, 42.9% of patients in the medication group were free of AF compared with 80% of patients in the ablation group. There was also a significant improvement in QOL for patients in the ablation group. Adverse events from medications occurred in 17.2% (6/35) patients, whereas complications from ablation occurred in 2.9% (1/35). An RCT of RFA ablation as the initial therapy for paroxysmal AF was published in A total of 294 patients were randomized to initial treatment with catheter ablation or pharmacologic therapy. Patients were followed for up to 24 months for the primary outcomes of burden of AF (percent of time in AF on Holter monitor) at each time point and cumulative burden of AF over all time points. For the individual time points, the burden of AF was lower in the catheter ablation group at 24 months (9% vs 18%, p=0.007), but not at other time points. The cumulative burden did not differ significantly for the catheter ablation group compared with pharmacologic therapy (90th percentile of cumulative burden, 13% vs 19%, p=0.10). The secondary outcome of percent of patients free from AF at 24 months was greater for the catheter ablation group (85% vs 71%, p=0.004), as was the secondary outcome of freedom from symptomatic AF (93% vs 84%, p=0.01). There was one death in the ablation group due to a procedural-related stroke, and there were three patients in the ablation group who developed cardiac tamponade following the procedure. Mont et al conducted an RCT comparing radiofrequency catheter ablation with antiarrhythmic drug therapy among 146 patients with symptomatic persistent AF. Patients were randomized in a 2:1 fashion to catheter ablation (n=98) or antiarrhythmic drug therapy (N=48). Although the study was terminated before the planned sample size of 208 was met due to lower than expected enrollment, at 12 months of follow up, the proportion of patients who were free of sustained episodes of AF was higher in the catheter ablation group than the antiarrhythmic drug therapy group (70.4% vs 43.7%, p=0.002). QOL scores did not significantly differ between the groups. Longer term outcomes were not reported. Several studies have compared catheter ablation with medical therapy for AF in the setting of heart failure. Hunter et al conducted an RCT comparing catheter ablation with medical rate control for patients with persistent AF and symptomatic heart failure, with adequate rate control at the time of enrollment. The study s primary end point was difference between groups in LVEF at six months postprocedure. Fifty patients were randomized, 26 to catheter ablation and 24 to medical management. At six months, 81% of the catheter ablation group was free from Page 9 of 24
10 recurrent AF off antiarrhythmic drugs. LVEF at six months after procedure was 40% (±12%) in the catheter ablation group, compared with 31% (±13%, p=0.015). Catheter ablation was also associated with improvements in health-related QOL. Jones et al reported results from an RCT comparing catheter ablation with medical rate control for patients with symptomatic heart failure, LVEF 35% or less, and persistent AF. Fifty-two patients were randomized, 26 each to catheter ablation or medical rate control. At 12 months after procedure, sinus rhythm was maintained in 88% of the catheter ablation group, with a single-procedure success rate of 68%. For the study s primary outcome, peak oxygen consumption at 12 months after procedure, there was a significant increase in the catheter ablation group compared with the medical management group (+3.07 ml/kg/min; 95% CI, 0.56 to 5.59; p=0.018). Longer-term outcomes The available RCTs mainly report on short-term outcomes up to one year and, therefore, do not evaluate the rate of late recurrences after one year. Longer-term outcomes have been reported by several authors. These studies generally report rates of early recurrence in the range of 20% to 30%, requiring repeat ablations. Rates of longer-term recurrence are lower if early recurrence does not occur, in the range of 1% to 2% per year. Hussein et al reported on 831 patients who were treated in 2005, with a median follow-up of 55 months. During the first year following ablation, 23.8% had a recurrence of AF. During the remaining follow-up, recurrences occurred in 8.9% additional patients. The overall rate of arrhythmia-free and off drugs was 79.4% at 55 months. An additional 10.5% of patients were arrhythmia-free on drugs, for a total rate of 89.9% clinical improvement. In 2013, Bunch et al reported results from a prospective cohort study comparing risk of stroke between patients with AF who had undergone catheter ablation, patients with AF who did not undergo ablation, and patients without a history of AF. A total of 4212 patients with AF who had undergone catheter ablation were age and sex matched in a 1:4 ratio to 16,848 subjects in each of the other groups. The mean follow up time was 3.9 years. At one year postprocedure, significantly more patients with AF who did not undergo ablation had a stroke (3.5%) than those with AF who underwent ablation (1.4%) or had no history of AF (1.4%; p<0.001 for trend). During the follow up period, for all ages and CHADS2 profiles, patients with AF who had ablation had a lower stroke risk than those with AF without ablation. Several smaller studies have also reported longer-term follow-up after radiofrequency catheter ablation. Weerasooriya et al reported five-year follow-up in 100 patients treated with catheter ablation. Recurrences were most common within the first six months, with repeat procedures being common during that period. At one, two, and five years after ablation, arrhythmia-free survival was 87%, 81%, and 63%, respectively. Tzou et al reported long-term follow-up for 123 patients who had a previous successful ablation, defined as free of AF at one year. At three years of follow-up, 85% of patients were still free of AF and off of all medications, and at five years, 71% remained free of AF. The authors estimated a late recurrence rate of approximately 7% per year for patients with an initial successful procedure. In a similar study, Bertaglia et al reported outcomes after six years of follow-up for 229 patients who had a single, successful ablation. At one-year follow-up, 77% of patients (177/229) were free of AF and off of all medications. After a mean additional follow-up of 49.7±13.3 months for these 177 patients, Page 10 of 24
11 58% remained free of AF. Sawhney et al reported five-year success rates in 71 patients who underwent ablation in 2002 or Freedom from symptomatic AF off medications was achieved in 86% of patients at one year, 79% at two years, and 56% at five years. A substantial minority of patients (22.5%) had recurrence at times greater than two years after ablation. A 2013 study by Anselmino et al followed 196 patients who underwent radiofrequency catheter ablation for paroxysmal or persistent AF and had LVEF 50% or less for a mean of 46.2 months. During follow-up, 29.6% of patients required repeat ablation procedures. At the end of follow up, 37.8% had at least one episode of AF, atrial flutter, or ectopic atrial tachycardia. Numerous RCTs of RFA of the pulmonary veins versus medical management report that freedom from AF at one year is higher with RFA compared with medical management. The trials mainly include patients who have failed antiarrhythmic medications, although two trials treat patients with paroxysmal AF as initial treatment. These studies report that most patients undergoing RFA are free of AF at one year. QOL is also improved in these trials for patients undergoing catheter ablation. A smaller number of studies evaluate outcomes longer than one year and report that late recurrences occur up to five years but are uncommon after the first year. Complications from RFA are reported at low rates in the RCTs, but the numbers of patients in these trials are too low to accurately estimate rates of uncommon events. There is a lack of data on clinical outcomes other than freedom from AF. Larger RCTs are underway to evaluate long-term clinical outcomes such as stroke and mortality. Cryoablation of the pulmonary veins A number of studies reported outcomes of ablation using cryoablation. These were mainly case series reporting success rates in the range of that reported for RFA. One small matched analysis compared 20 patients undergoing cryoablation with 20 patients undergoing RFA, matched for age, gender, LVEF, and AF history. Freedom from AF at six months was 55% for the cryoablation group, compared with 45% for the RFA group, a difference that was not significantly different. In 2013, Packer et al reported results of the STOP-AF trial, an RCT of cryoablation versus antiarrhythmic medications. This study enrolled 245 patients with paroxysmal AF who had failed at least one (median, 1.2) membrane-active antiarrhythmic medications. Patients were randomized in 2:1 fashion to either cryoballoon ablation (n=163) or drug therapy (n=82). At one-year follow-up, 69.9% of patients in the ablation group were free of AF versus 7.3% in the medication group. The single-procedure success rate was 57.7%. There was also a significantly greater reduction in symptoms for the ablation group. Seventy-nine percent of the drug treatment group crossed over to cryoablation during 12 months of study follow-up because of recurrent, persistent AF. Cryoablation procedure-related adverse events occurred in five patients (3.1%); major AF events occurred in 3.1% of the cryoablation group compared with 8.5% of the drug-treatment group (non-inferiority p<0.001). Phrenic nerve injury occurred at a rate of 13.5%, with 86% resolved at 12 months. The Mesh Ablator versus Cryoballoon Pulmonary Vein Ablation of Symptomatic Paroxysmal AF (MACPAF) study was a single-center RCT comparing cryoablation with RFA with the HD Mesh Ablator Catheter (Bard, purchased by Boston Scientific in 2013) for AF. The HD Mesh Ablator Catheter, which is not cleared for use in the U.S., is a multielectrode RF catheter that Page 11 of 24
12 involves a mesh electrode that is designed to delivery RF energy to multiple points of contact. Primary short-term results for MACPAF were reported by Koch et al in The study randomized symptomatic paroxysmal AF to catheter ablation with the Arctic Front cryoablation catheter or the HD Mesh Ablator. The study s primary end point was complete isolation of the pulmonary veins at the end of the procedure. Enrollment was initially planned for 108 with symptomatic paroxysmal AF that was inadequately controlled with antiarrhythmic drug treatment. However, at interim analysis, the HD Mesh Ablator demonstrated a lack of efficacy for the primary end point, and the study s data safety monitoring board prematurely terminated the subject. Forty-four patients with drug-resistant paroxysmal AF were randomized at the time the study was terminated and comprise the intention-to-treat analysis cohort. The per-protocol analysis cohort included 32 patients. Three patients withdrew before the catheter procedure; nine additional patents were excluded from analysis due to use of a study noncompliant catheter (n=2), identification of a trigger arrhythmia, which was subsequently ablated (n=1), failure of transseptal puncture (n=1), or ablation occurring after the interim analysis (n=5). For the primary end point, by intention-to-treat analysis, complete pulmonary vein isolation was achieved in 13/23 (56.5%) of patients in the cryoablation group, compared with 2/21 (9.5%) of patients in the mesh ablator group (p=0.001). In the per-protocol cryoablation group, 76.5% of subjects had complete pulmonary vein isolation. Major complications included one case of retroperitoneal hematoma in the cryoablation group and one case of pericardial tamponade requiring drainage in the mesh ablator group. Malmborg et al reported results from an RCT comparing cryoablation with the Arctic Front cryoballoon catheter to RFA with the Pulmonary Vein Ablation Catheter. One hundred ten patients with paroxysmal or persistent AF were randomized, 54 to the cryoablation group and 56 to the RFA group. Complete pulmonary vein isolation was achieved in 98% of the cryoablation group, compared with 93% of the RFA group (p=0.37). At six-month follow-up, freedom from AF (absence of symptoms and no AF episodes on seven-day Holter monitoring or 12-lead electrocardiogram) without antiarrhythmic drug treatment was achieved in 52% of the cryoablation group and 38% of the RFA group (p=0.13). Schmidt et al used data from a prospective German registry of catheter ablation procedures to compare RF with cryoablation for paroxysmal AF. The cohort included 905 patients who underwent cryoablation and 2870 patients who underwent RFA who were enrolled from January 2007 to August The two groups were generally similar, with the exception that patients who underwent RFA were significantly more likely to have valve disease (8.1% vs 3.0%, p<0.001) and an ejection fraction 40% or less (2.4% vs 1.2%, p<0.05). Rates of acute success were similar for the two groups (97.5% for cryoablation vs 97.6% for RFA, p=0.92), as were rates of major procedure-related adverse cardiac and cerebrovascular events (0.4% for cryoablation vs 0.2% for RFA, p=0.15). The overall procedural complication rates were similar for the two groups (4.6% for each group, p=1.0); the rate of postprocedural phrenic nerve palsy was significantly higher for the cryoablation group (2.1% for cryoablation vs 0% for RFA, p=0.15). Long-term follow rates are not reported. A meta-analysis of studies of cryoablation was published in This analysis included the STOP-AF results in abstract form and a total of 22 other nonrandomized studies, primarily case series. Procedural success was reported in over 98% of cases. At one year, the rates of success, Page 12 of 24
13 as defined by no recurrent AF, were 73% (95% CI, 69% to 77%) for paroxysmal AF and 60% (95% CI, 54% to 66%) for persistent AF. Complications were inconsistently reported among the available studies. The most common complication reported was phrenic nerve palsy, which occurred in 6.4% of patients. Other rates of reported complications were pericardial effusion or tamponade (1.5%), groin complications at insertion site (1.8%), stroke (0.3%), and pulmonic stenosis (0.9%). Vogt et al reported longer-term follow up for 605 patients who underwent cryoablation for symptomatic, paroxysmal or persistent AF. Follow-up data beyond 12 months were available for 451 patients (median follow-up, 30 months). Of those with follow up available, 278 (61.6%) were free of AF recurrence with no need for repeat procedures after a three-month blanking period. After one, two, and three repeat procedures, rates of freedom from AF were 74.9%, 76.2%, and 76.9%, respectively. Phrenic nerve palsy was the most common adverse event, occurring in 2% of patients, all of which resolved within three to nine months. There were two periprocedural strokes, and one case each of periprocedural pericardial tamponade and pericardial effusion. Neumann et al reported five-year outcomes after a single cryoablation procedure among 163 patients with symptomatic, drug-refractory paroxysmal AF. Fifty-three percent of subjects were free from recurrent AF, atrial tachycardia, or atrial flutter at five years of follow-up with no additional procedures (after a three-month blanking period). There are ongoing trials of cryoablation versus RFA for AF. The FreezeAF trial is a noninferiority RCT comparing cryoablation with RFA for patients with paroxysmal AF. Enrollment of 244 patients is planned, and patients will be followed for at least one year. The primary outcome is freedom from AF off all drugs. Secondary outcomes include longer-term success rates, procedural data, and cost-effectiveness. The evidence related to cryoablation for AF includes three RCTs and numerous uncontrolled case series. The STOP AF trial, which compared cryoablation with antiarrhythmic medication therapy, reported that cryoablation is superior to medical management, and that rates of freedom from arrhythmia at one year in the cryoablation group are in the range reported with RFA. Nonrandomized studies also report that cryoablation has efficacy in the same range as RFA. However, data from randomized trials directly comparing cryoablation with RFA are limited. Interpretation of the MACPAF study is limited by early termination due to unexpectedly low efficacy of the RFA method used. While the Malmborg et al study is suggestive that cryoablation is comparable with RFA, success in the RFA group was also unusually low. This study is also limited by relatively short-term follow-up (six months) and use of a catheter that is not cleared for use in the U.S. Therefore, the evidence is not sufficient to determine the comparative efficacy of cryoablation compared with RFA. Ongoing RCTs, particularly the FreezeAF trial, are currently addressing this question. Page 13 of 24
14 Repeat procedures Repeated procedures for recurrent AF or atrial flutter were commonly performed in most of the clinical trials included in this policy statement. Of the 10 RCTs reviewed that compared RFA with medical management, only two did not include repeated procedures. In the other five studies, one or more repeated procedures were allowed, and success rates reported generally incorporated the results of up to three procedures. In four studies that reported these data, repeated procedures were performed in 8.2%, 9%, 20%, and 32% of patients randomized to ablation. In their RCT of catheter ablation of AF in patients with heart failure, Hunter et al report that repeat procedures were required in 65.4% of the catheter ablation group. Stabile et al did not report specifics on how many patients actually underwent repeated procedures, but limited data in the publication indicated that up to 30% of treated patients were eligible for repeated procedures. In the Jais et al study, patients underwent a mean of 1.8 procedures per patient and a median of two procedures per patient, indicating that approximately 50% of patients in the ablation group underwent at least one repeated procedure. Because of this high rate of repeated procedures, the results reported in these studies do not reflect the success of a single procedure. Rather, they more accurately estimate the success of an ablation strategy that includes repeated procedures for recurrences that occur within the first year of treatment. Nonrandomized evidence suggests that early reablation increases the success of the procedure, when defined as maintenance of sinus rhythm at one year. There is variability in the protocol for when repeated procedures should be performed. There is also uncertainty concerning other details on repeated procedures, such as how soon after the initial procedure it should be done, the threshold of AF recurrence that should prompt a repeat, and whether medications should be tried before a repeated procedure. Pokushalov et al reported results of an RCT comparing repeat catheter ablation with antiarrhythmic drug therapy for patients with paroxysmal AF who had failed an initial pulmonary vein isolation procedure. After an initial postablation blanking period, 154 patients with symptomatic AF recurrence were randomized to drug therapy (n=77) or repeat ablation (n=77). Patients were followed for three years with an implanted cardiac monitor. At the threeyear follow up, 58% (45/77) of the repeat ablation group were free from AF or atrial tachycardia on no antiarrhythmic drugs, compared with 12% (9/77) of the antiarrhythmic therapy group (p<0.01). In the antiarrhythmic drug group, 43 patients (56%) crossed over to receive repeat ablation; in the repeat ablation group, 21 patients (27%) required antiarrhythmic drug therapy. By intention-to-treat analysis, 65% (50/77) of the repeat ablation group and 45% (35/77) of the drug therapy group were free from AF or atrial tachycardia (p=0.02). Complications Individual clinical trials and case series report relatively low rates of complications, but may be limited in their ability to detect uncommon outcomes due to their small size. In 2013, Gupta et al reported results from a systematic review and meta-analysis of periprocedural complications following catheter ablation for AF. The authors included 192 studies that included at least 100 participants undergoing catheter ablation for symptomatic AF and that reported complications. The total sample size was 83,236 patients. The overall acute complication rate was 2.9% (95% CI, 2.6 to 3.2), with significant heterogeneity across studies. The most common complications Page 14 of 24
15 were vascular complications (1.4%), cardiac tamponade (1.0%), pericardial effusion (0.7%), stroke/transient ischemic attack (TIA) (0.6%), and pulmonary vein stenosis (0.5%). In addition to the complication rates reported in available clinical trials and case series, there have been a number of database studies and postmarketing surveillance that report complications in larger numbers of patients than are in the clinical trials. A representative sample of these studies is discussed next, some of which were included in the Gupta et al review (Shah et al, Dagres et al). Waldo et al reported the results of a U.S. Food and Drug Administration (FDA) directed postmarketing safety study involving 1275 patients from six prospective, multicenter studies of RFA ablation using an open-irrigated catheter. A total of 4.9% (63/1275) of patients experienced any acute serious complication within seven days of the procedure. Vascular access complications were most common, ranging from 0.5% to 4.7% across the six studies. Exacerbations of heart failure occurred in 1.5% of patients, and two patients experienced cardiac tamponade. There were no strokes or TIAs reported after the procedure. Shah et al used data from a California hospital database to evaluate complications in 4156 patients who underwent catheter ablation for AF. Major complications occurred in 5.1% (211/4156) of patients, with approximately half of these (2.6%, 110/4156) consisting of hemorrhage or hematoma at the vascular entry site. The most common cardiac complication was cardiac perforation and/or tamponade, which occurred in 2.5% (104/4156) of patients. Less common rates of serious adverse events included death (0.02%), stroke/tia (0.31%), and pneumothorax/hemothorax (0.1%). Factors that were predictive of complications were female gender, older age, prior hospitalizations for AF, and less hospital experience with ablation. In a study of Medicare beneficiaries, Ellis et al identified 6065 admissions from 168 hospitals in which RFA for AF was performed. The total rate of in-hospital complications was 9.1%, with vascular complications accounting for over half of the total complications at a rate of 5.7%. The mortality rate was 0.4%, and 0.6% of patients suffered a stroke or TIA. Perforation or tamponade occurred in 3.1% of patients and pneumothorax occurred in 0.4% of patients. The presence of chronic obstructive pulmonary disease or unstable angina was associated with a higher risk of complications, while obesity and hyperlipidemia were associated with a lower risk. Age and hospital volume were not significant predictors of risk, but low hospital volume was a significant predictor of in-hospital death. Complications of catheter ablation were reported in a large cohort of 1000 patients undergoing ablation at a high-volume center in Europe. There were no deaths definitely attributable to the procedure, but there were two deaths of uncertain cause within the first 30 days following ablation. Overall, 3.9% of patients had a major complication resulting from the procedure. Tamponade was the most serious life-threatening complication, occurring in 1.3% of patients. Major vascular complications occurred in 1.1%. Thromboembolism, cerebrovascular accident/tia, atrioesophageal fistula, and endocarditis were all reported complications that occurred at a rate of less than 1%. Page 15 of 24
Description. Section: Medicine Effective Date: July 15, 2014 Subsection: Cardiology Original Policy Date: December 7, 2011 Subject:
 Page: 1 of 24 Last Review Status/Date: June 2014 Description Radiofrequency ablation using a percutaneous catheter-based approach is widely used to treat supraventricular arrhythmias. Atrial fibrillation
Page: 1 of 24 Last Review Status/Date: June 2014 Description Radiofrequency ablation using a percutaneous catheter-based approach is widely used to treat supraventricular arrhythmias. Atrial fibrillation
Catheter Ablation as Treatment for Atrial Fibrillation
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Catheter Ablation as Treatment for Atrial Fibrillation Page 1 of 37 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Catheter Ablation as Treatment for Atrial Fibrillation
Catheter Ablation as Treatment for Atrial Fibrillation Page 1 of 37 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Catheter Ablation as Treatment for Atrial Fibrillation
Catheter Ablation as Treatment for Atrial Fibrillation
 Catheter Ablation as Treatment for Atrial Fibrillation Policy Number: Original Effective Date: MM.06.011 09/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 08/29/2018 Section:
Catheter Ablation as Treatment for Atrial Fibrillation Policy Number: Original Effective Date: MM.06.011 09/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 08/29/2018 Section:
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): April 26, 2011 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
Original Issue Date (Created): April 26, 2011 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT
AF Today: W. For the majority of patients with atrial. are the Options? Chris Case
 AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
Catheter Ablation of the Pulmonary Veins as Treatment for Atrial Fibrillation
 Catheter Ablation of the Pulmonary Veins as Treatment for Atrial Fibrillation Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Catheter Ablation of the Pulmonary Veins as Treatment for Atrial Fibrillation Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana,
Catheter Ablation: Atrial fibrillation (AF) is the most common. Another Option for AF FAQ. Who performs ablation for treatment of AF?
 : Another Option for AF Atrial fibrillation (AF) is a highly common cardiac arrhythmia and a major risk factor for stroke. In this article, Dr. Khan and Dr. Skanes detail how catheter ablation significantly
: Another Option for AF Atrial fibrillation (AF) is a highly common cardiac arrhythmia and a major risk factor for stroke. In this article, Dr. Khan and Dr. Skanes detail how catheter ablation significantly
Corporate Medical Policy
 Corporate Medical Policy Catheter Ablation as a Treatment for Atrial Fibrillation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: catheter_ablation_as_a_treatment_for_atrial_fibrillation
Corporate Medical Policy Catheter Ablation as a Treatment for Atrial Fibrillation File Name: Origination: Last CAP Review: Next CAP Review: Last Review: catheter_ablation_as_a_treatment_for_atrial_fibrillation
Catheter Ablation for Cardiac Arrhythmias
 Catheter Ablation for Cardiac Arrhythmias Policy Number: 2.02.01 Last Review: 5/1/2018 Origination: 05/2015 Next Review: 5/1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Catheter Ablation for Cardiac Arrhythmias Policy Number: 2.02.01 Last Review: 5/1/2018 Origination: 05/2015 Next Review: 5/1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Ablation Should Not Be Used as Primary Therapy for Treatment of Patients with Atrial Fibrillation
 Ablation Should Not Be Used as Primary Therapy for Treatment of Patients with Atrial Fibrillation 25 October 2008 Update in Electrocardiography and Arrhythmias Zian H. Tseng, M.D., M.A.S. Assistant Professor
Ablation Should Not Be Used as Primary Therapy for Treatment of Patients with Atrial Fibrillation 25 October 2008 Update in Electrocardiography and Arrhythmias Zian H. Tseng, M.D., M.A.S. Assistant Professor
Κατάλυση παροξυσμικής κολπικής μαρμαρυγής Ποια τεχνολογία και σε ποιους ασθενείς; Χάρης Κοσσυβάκης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 Κατάλυση παροξυσμικής κολπικής μαρμαρυγής Ποια τεχνολογία και σε ποιους ασθενείς; Χάρης Κοσσυβάκης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» Rhythm control antiarrhythmic drugs vs catheter ablation Summary
Κατάλυση παροξυσμικής κολπικής μαρμαρυγής Ποια τεχνολογία και σε ποιους ασθενείς; Χάρης Κοσσυβάκης Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» Rhythm control antiarrhythmic drugs vs catheter ablation Summary
Supplementary Online Content
 Supplementary Online Content Morillo CA, Verma A, Connolly SJ, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line Treatment of Paroxysmal Atrial Fibrillation (RAAFT-2): a randomzied clinical
Supplementary Online Content Morillo CA, Verma A, Connolly SJ, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line Treatment of Paroxysmal Atrial Fibrillation (RAAFT-2): a randomzied clinical
Cigna Medical Coverage Policy
 Cigna Medical Coverage Policy Subject Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of Atrial Fibrillation Table of Contents Coverage Policy... 1 General Background...
Cigna Medical Coverage Policy Subject Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of Atrial Fibrillation Table of Contents Coverage Policy... 1 General Background...
Understanding Atrial Fibrillation
 Understanding Atrial Fibrillation Todd J. Florin, M.D. Table of Contents The Normal Heart...1 What is Atrial Fibrillation...3 Risks of Afib: Stroke...5 Treatment Options...7 Radiofrequency Ablation...9
Understanding Atrial Fibrillation Todd J. Florin, M.D. Table of Contents The Normal Heart...1 What is Atrial Fibrillation...3 Risks of Afib: Stroke...5 Treatment Options...7 Radiofrequency Ablation...9
Comparative Effectiveness of Radiofrequency Catheter Ablation for Atrial Fibrillation Executive Summary
 Number 15 Effective Health Care Comparative Effectiveness of Radiofrequency Catheter Ablation for Atrial Fibrillation Executive Summary Background The Agency for Healthcare Research and Quality commissioned
Number 15 Effective Health Care Comparative Effectiveness of Radiofrequency Catheter Ablation for Atrial Fibrillation Executive Summary Background The Agency for Healthcare Research and Quality commissioned
480 April 2004 PACE, Vol. 27
 Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
What s new in my specialty?
 What s new in my specialty? Jon Melman, MD Heart Rhythm Specialists McKay-Dee Hospital some would say some would say my specialty 1 some would say my specialty First pacemaker 1958 some would say my specialty
What s new in my specialty? Jon Melman, MD Heart Rhythm Specialists McKay-Dee Hospital some would say some would say my specialty 1 some would say my specialty First pacemaker 1958 some would say my specialty
Dipen Shah Cardiology Service, University Hospitals, Geneva Switzerland
 Dipen Shah Cardiology Service, University Hospitals, Geneva Switzerland Disclosures Research Grants: Biosense Webster, St. Jude, Bard, Endosense, Biotronik Speakers Honoraria: Biosense Webster, Endosense,
Dipen Shah Cardiology Service, University Hospitals, Geneva Switzerland Disclosures Research Grants: Biosense Webster, St. Jude, Bard, Endosense, Biotronik Speakers Honoraria: Biosense Webster, Endosense,
Name of Policy: Bi-Ventricular Pacemakers (Cardiac Resynchronization Therapy) for the Treatment of Heart Failure
 Name of Policy: Bi-Ventricular Pacemakers (Cardiac Resynchronization Therapy) for the Treatment of Heart Failure Policy #: 055 Latest Review Date: April 2014 Category: Surgery Policy Grade: A Background/Definitions:
Name of Policy: Bi-Ventricular Pacemakers (Cardiac Resynchronization Therapy) for the Treatment of Heart Failure Policy #: 055 Latest Review Date: April 2014 Category: Surgery Policy Grade: A Background/Definitions:
AF :RHYTHM CONTROL BY DR-MOHAMMED SALAH ASSISSTANT LECTURER CARDIOLOGY DEPARTMENT
 AF :RHYTHM CONTROL BY DR-MOHAMMED SALAH ASSISSTANT LECTURER CARDIOLOGY DEPARTMENT 5-2014 Atrial Fibrillation therapeutic Approach Rhythm Control Thromboembolism Prevention: Recommendations Direct-Current
AF :RHYTHM CONTROL BY DR-MOHAMMED SALAH ASSISSTANT LECTURER CARDIOLOGY DEPARTMENT 5-2014 Atrial Fibrillation therapeutic Approach Rhythm Control Thromboembolism Prevention: Recommendations Direct-Current
Cardiac Arrhythmias. Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company
 Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
Cardiac Arrhythmias Cathy Percival, RN, FALU, FLMI VP, Medical Director AIG Life and Retirement Company The Cardiovascular System Three primary functions Transport of oxygen, nutrients, and hormones to
This overview was prepared in October 2011, and updated in March 2012.
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous balloon cryoablation for pulmonary vein isolation in atrial fibrillation
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of percutaneous balloon cryoablation for pulmonary vein isolation in atrial fibrillation
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Long-Term Outcome and Risks of Catheter Ablation for Atrial Fibrillation
 Long-Term Outcome and Risks of Catheter Ablation for Atrial Fibrillation Carlo Pappone, MD, PhD, FACC EP Director, Villa Maria Hospital Group How many times AF can increase mortality DO MORTALITY REALLY
Long-Term Outcome and Risks of Catheter Ablation for Atrial Fibrillation Carlo Pappone, MD, PhD, FACC EP Director, Villa Maria Hospital Group How many times AF can increase mortality DO MORTALITY REALLY
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
Basics of Atrial Fibrillation. By Mini Thannikal NP-BC Mount Sinai St Luke s Hospital New York, NY
 Basics of Atrial Fibrillation By Mini Thannikal NP-BC Mount Sinai St Luke s Hospital New York, NY Atrial Fibrillation(AF) is a supraventricular tachyarrhythmia characterized by uncoordinated atrial activation
Basics of Atrial Fibrillation By Mini Thannikal NP-BC Mount Sinai St Luke s Hospital New York, NY Atrial Fibrillation(AF) is a supraventricular tachyarrhythmia characterized by uncoordinated atrial activation
Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of Atrial Fibrillation
 Medical Coverage Policy Effective Date... 1/15/2018 Next Review Date... 1/15/2019 Coverage Policy Number... 0469 Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of
Medical Coverage Policy Effective Date... 1/15/2018 Next Review Date... 1/15/2019 Coverage Policy Number... 0469 Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Long-term Preservation of Left Ventricular Function and Heart Failure Incidence with Ablate and Pace Therapy Utilizing Biventricular Pacing
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 976 981 HEART FAILURE RESEARCH ARTICLE Long-term Preservation of Left Ventricular Function and Heart Failure Incidence with Ablate and
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 976 981 HEART FAILURE RESEARCH ARTICLE Long-term Preservation of Left Ventricular Function and Heart Failure Incidence with Ablate and
Kadlec Regional Medical Center Cardiac Electrophysiology
 Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
Definition of electrophysiology study and ablation Kadlec Regional Medical Center Cardiac Electrophysiology Electrophysiology Study and Ablation An electrophysiology, or EP, study is a test of the heart
Management of ATRIAL FIBRILLATION. in general practice. 22 BPJ Issue 39
 Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Management of ATRIAL FIBRILLATION in general practice 22 BPJ Issue 39 What is atrial fibrillation? Atrial fibrillation (AF) is the most common cardiac arrhythmia encountered in primary care. It is often
Is cardioversion old hat? What is new in interventional treatment of AF symptoms?
 Is cardioversion old hat? What is new in interventional treatment of AF symptoms? Joseph de Bono Consultant Electrophysiologist University Hospitals Birmingham Atrial Fibrillation (AF) Affects 2% of the
Is cardioversion old hat? What is new in interventional treatment of AF symptoms? Joseph de Bono Consultant Electrophysiologist University Hospitals Birmingham Atrial Fibrillation (AF) Affects 2% of the
X-Plain Atrial Fibrillation Reference Summary
 X-Plain Atrial Fibrillation Reference Summary Introduction Atrial fibrillation is a common heart condition that affects approximately 2.5 million Americans every year. Atrial fibrillation requires immediate
X-Plain Atrial Fibrillation Reference Summary Introduction Atrial fibrillation is a common heart condition that affects approximately 2.5 million Americans every year. Atrial fibrillation requires immediate
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A AADs. See Antiarrhythmic drugs (AADs) ACE inhibitors. See Angiotensin-converting enzyme (ACE) inhibitors ACP in transseptal approach to
Index Note: Page numbers of article titles are in boldface type. A AADs. See Antiarrhythmic drugs (AADs) ACE inhibitors. See Angiotensin-converting enzyme (ACE) inhibitors ACP in transseptal approach to
ABLATION OF CHRONIC AF
 ABLATION OF CHRONIC AF A PISAPIA ST JOSEPH HOSPITAL MARSEILLE MEET 2008 Atrial Fibrillation The most common significant heart rhythm disturbance Incidence increases with age and the development of structural
ABLATION OF CHRONIC AF A PISAPIA ST JOSEPH HOSPITAL MARSEILLE MEET 2008 Atrial Fibrillation The most common significant heart rhythm disturbance Incidence increases with age and the development of structural
Combined catheter ablation and left atrial appendage closure as a. treatment of atrial fibrillation
 Combined catheter ablation and left atrial appendage closure as a hybrid procedure for the treatment of atrial fibrillation Giulio Molon, MD FACC, FESC, Fellow ANMCO Card Dept, S.Cuore hospital Negrar
Combined catheter ablation and left atrial appendage closure as a hybrid procedure for the treatment of atrial fibrillation Giulio Molon, MD FACC, FESC, Fellow ANMCO Card Dept, S.Cuore hospital Negrar
Jay Simonson, MD, FACC, FHRS Medical Director, Cardiac Electrophysiology Park Nicollet Heart and Vascular Center
 Jay Simonson, MD, FACC, FHRS Medical Director, Cardiac Electrophysiology Park Nicollet Heart and Vascular Center A-Fib Facts Yes, you may be able to blame your parents It is more of a nuisance than a
Jay Simonson, MD, FACC, FHRS Medical Director, Cardiac Electrophysiology Park Nicollet Heart and Vascular Center A-Fib Facts Yes, you may be able to blame your parents It is more of a nuisance than a
Interventional solutions for atrial fibrillation in patients with heart failure
 Interventional solutions for atrial fibrillation in patients with heart failure Advances in Cardiovascular Arrhythmias Great Innovations in Cardiology Matteo Anselmino, MD PhD Division of Cardiology Department
Interventional solutions for atrial fibrillation in patients with heart failure Advances in Cardiovascular Arrhythmias Great Innovations in Cardiology Matteo Anselmino, MD PhD Division of Cardiology Department
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Occlusion de l'auricule gauche: Niche ou réel avenir? D Gras, MD, Nantes, France
 Occlusion de l'auricule gauche: Niche ou réel avenir? D Gras, MD, Nantes, France LAA Occlusion Is there a real future? Background Protect AF Trial Other Studies CAP, ASAP, Prevail Left Atrial Appendage
Occlusion de l'auricule gauche: Niche ou réel avenir? D Gras, MD, Nantes, France LAA Occlusion Is there a real future? Background Protect AF Trial Other Studies CAP, ASAP, Prevail Left Atrial Appendage
Page 1. Current Trends in the Management of Atrial Fibrillation: Left Atrial Appendage Occlusion. Atrial fibrillation: Scope of the problem
 Current Trends in the Management of Atrial Fibrillation: Left Atrial Appendage Occlusion Benjamin A. D Souza, MD, FACC, FHRS Assistant Professor of Clinical Medicine Penn Presbyterian Medical Center Cardiac
Current Trends in the Management of Atrial Fibrillation: Left Atrial Appendage Occlusion Benjamin A. D Souza, MD, FACC, FHRS Assistant Professor of Clinical Medicine Penn Presbyterian Medical Center Cardiac
Treatment of Atrial Fibrillation in Heart Failure
 Stockholm, September 1st 2010 Treatment of Atrial Fibrillation in Heart Failure Rhythm control: Which drugs? Stefan H. Hohnloser J.W. Goethe University Frankfurt, Germany Presenter disclosure information:
Stockholm, September 1st 2010 Treatment of Atrial Fibrillation in Heart Failure Rhythm control: Which drugs? Stefan H. Hohnloser J.W. Goethe University Frankfurt, Germany Presenter disclosure information:
DO YOU HAVE PAROXYSMAL ATRIAL FIBRILLATION?
 DO YOU HAVE PAROXYSMAL ATRIAL FIBRILLATION? Do you have atrial fibrillation ()? Do you think you might have it? If so, the time to take control is now. There are three important things to do. 1. If you
DO YOU HAVE PAROXYSMAL ATRIAL FIBRILLATION? Do you have atrial fibrillation ()? Do you think you might have it? If so, the time to take control is now. There are three important things to do. 1. If you
Invasive and Medical Treatments for Atrial Fibrillation. Thomas J Dresing, MD Section of Electrophysiology and Pacing Cleveland Clinic
 Invasive and Medical Treatments for Thomas J Dresing, MD Section of Electrophysiology and Pacing Cleveland Clinic Disclosures Fellow s advisory panel for St Jude Medical Speaking honoraria from: Boston
Invasive and Medical Treatments for Thomas J Dresing, MD Section of Electrophysiology and Pacing Cleveland Clinic Disclosures Fellow s advisory panel for St Jude Medical Speaking honoraria from: Boston
Arrhythmia 341. Ahmad Hersi Professor of Cardiology KSU
 Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
National Coverage Determination (NCD) for Cardiac Pacemakers (20.8)
 Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Page 1 of 12 Centers for Medicare & Medicaid Services National Coverage Determination (NCD) for Cardiac Pacemakers (20.8) Tracking Information Publication Number 100-3 Manual Section Number 20.8 Manual
Atrial Fibrillation: Rate vs. Rhythm. Michael Curley, MD Cardiac Electrophysiology
 Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Atrial Fibrillation: Rate vs. Rhythm Michael Curley, MD Cardiac Electrophysiology I have no relevant financial disclosures pertaining to this topic. A Fib Epidemiology #1 Most common heart rhythm disturbance
Ambulatory Cardiac Monitors and Outpatient Telemetry Corporate Medical Policy
 Ambulatory Cardiac Monitors and Outpatient Telemetry Corporate Medical Policy File Name: Ambulatory Event Monitors and Mobile Cardiac Outpatient Telemetry File Code: UM.SPSVC.13 Origination: 10/2015 Last
Ambulatory Cardiac Monitors and Outpatient Telemetry Corporate Medical Policy File Name: Ambulatory Event Monitors and Mobile Cardiac Outpatient Telemetry File Code: UM.SPSVC.13 Origination: 10/2015 Last
Mission Statement for our Arrhythmia Care
 Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Mission Statement for our Arrhythmia Care We are dedicated to provide a compassionate and an outstanding care for patients with cardiac arrhythmias. We will be utilizing the cutting edge and the most advanced
Atrial Fibrillation Ablation Recent Clinical Trials That Changed (or not) My Practice
 Atrial Fibrillation Ablation Recent Clinical Trials That Changed (or not) My Practice Walid Saliba, MD, FHRS Director, Atrial Fibrillation Center Director EP laboratory Heart and Vascular Institute Cleveland
Atrial Fibrillation Ablation Recent Clinical Trials That Changed (or not) My Practice Walid Saliba, MD, FHRS Director, Atrial Fibrillation Center Director EP laboratory Heart and Vascular Institute Cleveland
Kadlec Regional Medical Center Cardiac Electrophysiology
 Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
Definition of atrial fibrillation Kadlec Regional Medical Center Cardiac Electrophysiology Atrial Fibrillation Ablation Atrial fibrillation is a heart rhythm disturbance that causes an irregular (and often
ESC Stockholm Arrhythmias & pacing
 ESC Stockholm 2010 Take Home Messages for Practitioners Arrhythmias & pacing Prof. Panos E. Vardas Professor of Cardiology Heraklion University Hospital Crete, Greece Disclosures Small teaching fees from
ESC Stockholm 2010 Take Home Messages for Practitioners Arrhythmias & pacing Prof. Panos E. Vardas Professor of Cardiology Heraklion University Hospital Crete, Greece Disclosures Small teaching fees from
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Catheter Ablation of Atrial Fibrillation
 Cardiology Update 2011 Catheter Ablation of Atrial Fibrillation Laurent Haegeli University Hospital Zurich February 16, 2011 Willem Einthoven and Sir Thomas Lewis The first ECG in 1903 Willem Einthoven
Cardiology Update 2011 Catheter Ablation of Atrial Fibrillation Laurent Haegeli University Hospital Zurich February 16, 2011 Willem Einthoven and Sir Thomas Lewis The first ECG in 1903 Willem Einthoven
Fibrillazione atriale e scompenso: come interrompere il circolo vizioso.
 Alessandria, September 23 th 2017 Fibrillazione atriale e scompenso: come interrompere il circolo vizioso. Professor Fiorenzo Gaita Chief of the Cardiovascular Department Città della Salute e della Scienza
Alessandria, September 23 th 2017 Fibrillazione atriale e scompenso: come interrompere il circolo vizioso. Professor Fiorenzo Gaita Chief of the Cardiovascular Department Città della Salute e della Scienza
Catheter Ablation for Atrial Fibrillation: Patient Selection and Outcomes
 Catheter Ablation for Atrial Fibrillation: Patient Selection and Outcomes Francis Marchlinski, MD Richard T and Angela Clark President s Distinguished Professor Director Cardiac Electrophysiolgy University
Catheter Ablation for Atrial Fibrillation: Patient Selection and Outcomes Francis Marchlinski, MD Richard T and Angela Clark President s Distinguished Professor Director Cardiac Electrophysiolgy University
AF and arrhythmia management. Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire
 AF and arrhythmia management Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire Atrial fibrillation Paroxysmal AF recurrent AF (>2 episodes) that
AF and arrhythmia management Dr Rhys Beynon Consultant Cardiologist and Electrophysiologist University Hospital of North Staffordshire Atrial fibrillation Paroxysmal AF recurrent AF (>2 episodes) that
ATRIAL FIBRILLATION: REVISITING CONTROVERSIES IN AN ERA OF INNOVATION
 ATRIAL FIBRILLATION: REVISITING CONTROVERSIES IN AN ERA OF INNOVATION Frederick Schaller, DO, MACOI,FACP Adjunct Clinical Professor Touro University Nevada DISCLOSURES I have no financial relationships
ATRIAL FIBRILLATION: REVISITING CONTROVERSIES IN AN ERA OF INNOVATION Frederick Schaller, DO, MACOI,FACP Adjunct Clinical Professor Touro University Nevada DISCLOSURES I have no financial relationships
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
About atrial fibrillation (AFib) Atrial Fibrillation (AFib) What is AFib? What s the danger? Who gets AFib?
 Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Understanding AFib Atrial Fibrillation (AFib) About AFib 3 How Your Heart Works 4 Types of AFib 5 Symptoms 5 Risk Factors 5 How is AFib Diagnosed? 6 Treatment 6 What to Ask Your Doctor 7 A normal heartbeat
Atrial Fibrillation 2009
 Atrial Fibrillation 2009 Michael Glikson, MD Director of Pacing & Electrophysiology Leviev Heart Center Sheba medical Center Sheba Medical Center Tel Hashomer The Leviev Heart Center Rhythm vs rate control
Atrial Fibrillation 2009 Michael Glikson, MD Director of Pacing & Electrophysiology Leviev Heart Center Sheba medical Center Sheba Medical Center Tel Hashomer The Leviev Heart Center Rhythm vs rate control
Long-Term ECG Monitoring Using an ILR. Evgeny Pokushalov, MD, PhD
 Long-Term ECG Monitoring Using an ILR Evgeny Pokushalov, MD, PhD Long- Term ECG Monitoring Using an ILR Evgeny Pokushalov, MD, PhD, FESC State Research Ins;tute of Circula;on Pathology, Novosibirsk, Russia
Long-Term ECG Monitoring Using an ILR Evgeny Pokushalov, MD, PhD Long- Term ECG Monitoring Using an ILR Evgeny Pokushalov, MD, PhD, FESC State Research Ins;tute of Circula;on Pathology, Novosibirsk, Russia
Non-Invasive Ablation of Ventricular Tachycardia
 Non-Invasive Ablation of Ventricular Tachycardia Dr Shaemala Anpalakhan Newcastle upon Tyne Hospitals NHS Foundation Trust Freeman Road, Newcastle Upon Tyne, NE7 7DN Contact: shaemala@doctors.org.uk Introduction
Non-Invasive Ablation of Ventricular Tachycardia Dr Shaemala Anpalakhan Newcastle upon Tyne Hospitals NHS Foundation Trust Freeman Road, Newcastle Upon Tyne, NE7 7DN Contact: shaemala@doctors.org.uk Introduction
Scompenso cardiaco e F A : ruolo della ablazione transcatetere. Prof. Fiorenzo Gaita
 Scompenso cardiaco e F A : ruolo della ablazione transcatetere Prof. Fiorenzo Gaita Patients with atrial fibrillation (%) Prevalence of AF in HF Trials 60 50 30% NYHA III-IV NYHA IV 40 NYHA II-III 30 20
Scompenso cardiaco e F A : ruolo della ablazione transcatetere Prof. Fiorenzo Gaita Patients with atrial fibrillation (%) Prevalence of AF in HF Trials 60 50 30% NYHA III-IV NYHA IV 40 NYHA II-III 30 20
Transcoronary Chemical Ablation of Atrioventricular Conduction
 757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
757 Transcoronary Chemical Ablation of Atrioventricular Conduction Pedro Brugada, MD, Hans de Swart, MD, Joep Smeets, MD, and Hein J.J. Wellens, MD In seven patients with symptomatic atrial fibrillation
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation
 The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
The pill-in-the-pocket strategy for paroxysmal atrial fibrillation KONSTANTINOS P. LETSAS, MD, FEHRA LABORATORY OF CARDIAC ELECTROPHYSIOLOGY EVANGELISMOS GENERAL HOSPITAL OF ATHENS ARRHYTHMIAS UPDATE,
CATHETER ABLATION CODING & REIMBURSEMENT GUIDE. Updated September 2018
 CATHETER ABLATION CODING & REIMBURSEMENT GUIDE Updated September 2018 TABLE OF CONTENTS Diagnosis Codes...3 ICD-10-CM Diagnosis Codes Coverage for Catheter Ablation Procedures....4 Medicare Other Payers
CATHETER ABLATION CODING & REIMBURSEMENT GUIDE Updated September 2018 TABLE OF CONTENTS Diagnosis Codes...3 ICD-10-CM Diagnosis Codes Coverage for Catheter Ablation Procedures....4 Medicare Other Payers
Atrial Fibrillation Ablation: in Whom and How
 Update on Consensus Statement on Management of Atrial Fibrillation: EHRA 2012 Atrial Fibrillation Ablation: in Whom and How Update of HRS/EHRA AF/ECAS Ablation Document 2012 Anne M Gillis MD FHRS Professor
Update on Consensus Statement on Management of Atrial Fibrillation: EHRA 2012 Atrial Fibrillation Ablation: in Whom and How Update of HRS/EHRA AF/ECAS Ablation Document 2012 Anne M Gillis MD FHRS Professor
Page: 1 of 22. Open and Thoracoscopic Approaches to Treat Atrial Fibrillation and Atrial Flutter (Maze and Related Procedures)
 7.01.14 Last Review Status/Date: September 2015 Page: 1 of 22 to Treat Atrial Fibrillation and Atrial Description There are a variety of surgical approaches to treat atrial fibrillation (AF) that work
7.01.14 Last Review Status/Date: September 2015 Page: 1 of 22 to Treat Atrial Fibrillation and Atrial Description There are a variety of surgical approaches to treat atrial fibrillation (AF) that work
Innovations in AF Management
 Innovations in AF Management Barry Boilson MD PhD FRCPI boilson.barry@mayo.edu Disclosures Relevant None financial relationship(s) with industry None Off Label Usage None Overview Mechanisms of AF AF as
Innovations in AF Management Barry Boilson MD PhD FRCPI boilson.barry@mayo.edu Disclosures Relevant None financial relationship(s) with industry None Off Label Usage None Overview Mechanisms of AF AF as
National Medical Policy
 National Medical Policy Subject: Policy Number: Catheter Ablation for Atrial Fibrillation NMP175 Effective Date*: May 2010 Update: July 2016 This National Medical Policy is subject to the terms in the
National Medical Policy Subject: Policy Number: Catheter Ablation for Atrial Fibrillation NMP175 Effective Date*: May 2010 Update: July 2016 This National Medical Policy is subject to the terms in the
Biatrial Stimulation and the Prevention of Atrial Fibrillation
 374 September 2001 Biatrial Stimulation and the Prevention of Atrial Fibrillation L. MELCZER Heart Institute, Faculty of Medicine, University of Pécs, Pécs, Hungary I. LORINCZ 1 st Internal Department,
374 September 2001 Biatrial Stimulation and the Prevention of Atrial Fibrillation L. MELCZER Heart Institute, Faculty of Medicine, University of Pécs, Pécs, Hungary I. LORINCZ 1 st Internal Department,
SUPPLEMENTAL MATERIAL
 SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
SUPPLEMENTAL MATERIAL Table S1. Patient Selection Codes, CIED Generator Procedures Code Type Code Description ICD9 Proc 00.51 Implantation of cardiac resynchronization defibrillator, total system [CRT-D]
ESSA HEART AND VASCULAR INSTITUTE APR/MAY/JUNE 2009 CLINICAL LETTER
 CLINICAL LETTER Exciting things are happening at the ESSA Heart and Vascular Institute and the Pocono Medical Center! We are all proud of the stellar team of professionals who are working very hard to
CLINICAL LETTER Exciting things are happening at the ESSA Heart and Vascular Institute and the Pocono Medical Center! We are all proud of the stellar team of professionals who are working very hard to
5/5/2010. World incidence 720, 000 new cases / year. World prevalence 5.55 million AF prevalence increasing with aging of population
 Atrial Fibrillation: Guidelines through clinical cases and 2010 updates Samy Claude ELAYI Cardiac Clinical Pacing and Electrophysiology UK World incidence 720, 000 new cases / year World prevalence 5.55
Atrial Fibrillation: Guidelines through clinical cases and 2010 updates Samy Claude ELAYI Cardiac Clinical Pacing and Electrophysiology UK World incidence 720, 000 new cases / year World prevalence 5.55
SUPPLEMENTARY INFORMATION
 Table S1 Sex- specific differences in rate- control and rhythm- control strategies in observational studies Study region Study period Total sample size Sex- specific results Ozcan (2001) 1 Mayo Clinic,
Table S1 Sex- specific differences in rate- control and rhythm- control strategies in observational studies Study region Study period Total sample size Sex- specific results Ozcan (2001) 1 Mayo Clinic,
THE ISSUE OF RESTITUTION AND MAINTENANCE OF SINUS RHYTHM IN ATRIAL FIBRILLATION
 UNIVERSITY LUCIAN BLAGA SIBIU UNIVERSITY OF MEDICINE VICTOR PAPILIAN SIBIU DOCTORAL THESIS THE ISSUE OF RESTITUTION AND MAINTENANCE OF SINUS RHYTHM IN ATRIAL FIBRILLATION - ABSTRACT - PhD student Mentor
UNIVERSITY LUCIAN BLAGA SIBIU UNIVERSITY OF MEDICINE VICTOR PAPILIAN SIBIU DOCTORAL THESIS THE ISSUE OF RESTITUTION AND MAINTENANCE OF SINUS RHYTHM IN ATRIAL FIBRILLATION - ABSTRACT - PhD student Mentor
AF in the ER: Common Scenarios CASE 1. Fast facts. Diagnosis. Management
 AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
For Personal Use. Copyright HMP 2013
 Original Contribution Early Experience With the Cryoablation Balloon Procedure for the Treatment of Atrial Fibrillation by an Experienced Radiofrequency Catheter Ablation Center Jeffrey Mandell, Frank
Original Contribution Early Experience With the Cryoablation Balloon Procedure for the Treatment of Atrial Fibrillation by an Experienced Radiofrequency Catheter Ablation Center Jeffrey Mandell, Frank
Tehran Arrhythmia Center
 Tehran Arrhythmia Center The Worst Scenario A 4 year old kid High heart rates first noted by parents at 20 months of age. Family physician detected rates as high as 220 bpm at that age. He was visited,
Tehran Arrhythmia Center The Worst Scenario A 4 year old kid High heart rates first noted by parents at 20 months of age. Family physician detected rates as high as 220 bpm at that age. He was visited,
Management strategies for atrial fibrillation Thursday, 20 October :27
 ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
ALTHOUGH anyone who has had to run up a flight of steps or has had a frightening experience is quite familiar with a racing heartbeat, for the more than 2 million Americans who suffer from atrial fibrillation
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES
 UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
UNDERSTANDING ELECTROPHYSIOLOGY STUDIES Testing and Treating Your Heart s Electrical System A Problem with Your Heart Rhythm The speed and pattern of a heartbeat is called the heart rhythm. The rhythm
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
A MULTIDISCIPLINARY APPROACH TO ATRIAL FIBRILLATION: OUR EXPERIENCE WITH THE CONVERGENT PROCEDURE
 A MULTIDISCIPLINARY APPROACH TO ATRIAL FIBRILLATION: OUR EXPERIENCE WITH THE CONVERGENT PROCEDURE Joe Aoun, MD Ioannis Koulouridis, MD, MSc Aleem Mughal, MD Maxwell Eyram Afari, MD Caroline Zahm, MD John
A MULTIDISCIPLINARY APPROACH TO ATRIAL FIBRILLATION: OUR EXPERIENCE WITH THE CONVERGENT PROCEDURE Joe Aoun, MD Ioannis Koulouridis, MD, MSc Aleem Mughal, MD Maxwell Eyram Afari, MD Caroline Zahm, MD John
Catheter Ablation for Cardiac Arrhythmias. Description
 Subject: Catheter Ablation for Cardiac Arrhythmias Page: 1 of 21 Last Review Status/Date: December 2016 Catheter Ablation for Cardiac Arrhythmias Description Catheter ablation is a technique to eliminate
Subject: Catheter Ablation for Cardiac Arrhythmias Page: 1 of 21 Last Review Status/Date: December 2016 Catheter Ablation for Cardiac Arrhythmias Description Catheter ablation is a technique to eliminate
Contemporary Strategies for Catheter Ablation of Atrial Fibrillation
 Contemporary Strategies for Catheter Ablation of Atrial Fibrillation Suneet Mittal, MD Director, Electrophysiology Medical Director, Snyder Center for Atrial Fibrillation The Arrhythmia Institute at The
Contemporary Strategies for Catheter Ablation of Atrial Fibrillation Suneet Mittal, MD Director, Electrophysiology Medical Director, Snyder Center for Atrial Fibrillation The Arrhythmia Institute at The
Catheter ablation is not a class I indication after failed antiarrhythmic drugs
 Catheter ablation is not a class I indication after failed antiarrhythmic drugs Martin Jan Schalij Department of Cardiology Leiden University Medical Center Disclosure: Research grants from: Boston Scientific
Catheter ablation is not a class I indication after failed antiarrhythmic drugs Martin Jan Schalij Department of Cardiology Leiden University Medical Center Disclosure: Research grants from: Boston Scientific
Atrial Fibrillation Procedures Data Summary. Participant STS Period Ending 12/31/2016
 Period Ending 12/31/2016 Number of Cases Preoperative Predominant Atrial Arrhythmia Type Paroxysmal Atrial Fibrillation... - - Persistent Atrial Fibrillation... - - Longstanding Persistent Atrial Fibrillation...
Period Ending 12/31/2016 Number of Cases Preoperative Predominant Atrial Arrhythmia Type Paroxysmal Atrial Fibrillation... - - Persistent Atrial Fibrillation... - - Longstanding Persistent Atrial Fibrillation...
Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks
 Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks Alireza Ghorbani Sharif, MD Interventional Electrophysiologist Tehran Arrhythmia Clinic January 2016 Recurrent ICD shocks are associated
Antiarrhythmic Drugs and Ablation in Patients with ICD and Shocks Alireza Ghorbani Sharif, MD Interventional Electrophysiologist Tehran Arrhythmia Clinic January 2016 Recurrent ICD shocks are associated
TREATING PAROXYSMAL ATRIAL FIBRILLATION WITH CRYOBALLOON ABLATION
 TREATING PAROXYSMAL ATRIAL FIBRILLATION WITH CRYOBALLOON ABLATION ABOUT YOUR AF Atrial fibrillation (AF or Afib) is an irregular heart rhythm that affects the upper chambers (atria) of the heart. This
TREATING PAROXYSMAL ATRIAL FIBRILLATION WITH CRYOBALLOON ABLATION ABOUT YOUR AF Atrial fibrillation (AF or Afib) is an irregular heart rhythm that affects the upper chambers (atria) of the heart. This
Atrial Fibrillaton. Key: RA: right atrium RV: right ventricle PA: pulmonic artery LA: left atrium LV: left ventricle AO: aorta
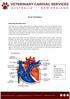 Atrial Fibrillaton How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Atrial Fibrillaton How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Name of Policy: Measurement of Long-Chain Omega-3 Fatty Acids in Red Blood Cell Membranes as a Cardiac Risk Factor
 Name of Policy: Measurement of Long-Chain Omega-3 Fatty Acids in Red Blood Cell Membranes as a Cardiac Risk Factor Policy #: 239 Latest Review Date: July 2010 Category: Laboratory Policy Grade: Active
Name of Policy: Measurement of Long-Chain Omega-3 Fatty Acids in Red Blood Cell Membranes as a Cardiac Risk Factor Policy #: 239 Latest Review Date: July 2010 Category: Laboratory Policy Grade: Active
Long Standing Persistent AF ; CPVI is enough for it
 Long Standing Persistent AF ; CPVI is enough for it Kee-Joon Choi, MD University of Ulsan College of Medicine Asan Medical Center, Seoul, Korea Boston AF Symposium 2012 In a patient undergoing AF ablation
Long Standing Persistent AF ; CPVI is enough for it Kee-Joon Choi, MD University of Ulsan College of Medicine Asan Medical Center, Seoul, Korea Boston AF Symposium 2012 In a patient undergoing AF ablation
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of Atrial Fibrillation
 Medical Coverage Policy Effective Date... 6/15/2018 Next Review Date... 1/15/2019 Coverage Policy Number... 0469 Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of
Medical Coverage Policy Effective Date... 6/15/2018 Next Review Date... 1/15/2019 Coverage Policy Number... 0469 Transcatheter Ablation of Arrhythmogenic Foci in the Pulmonary Veins for the Treatment of
