Repair of Perineal trauma, including 3 rd and 4 th degree tear
|
|
|
- Clyde Shields
- 5 years ago
- Views:
Transcription
1 MATERNITY GUIDELINES Repair of Perineal trauma, including 3 rd and 4 th degree tear Navigation Guidance document in the contents page the Press Ctrl on your keyboard and click on a heading to navigate to that section in this document. Contents 1. Classification of genital trauma Risk factors for OASI (obstetric anal sphincter injury) Training in repair and OASI prevention Prevention of OASI Assessment Perineal repair Episiotomy Repair of 3 rd or 4 th degree tear Identification of injury Prerequisites Procedure Post-operative instructions OASI follow-up Patient information Swab counts Audit and monitoring Record keeping Appendix 1 AN sticker... Error! Bookmark not defined. Appendix 2 - Care pathway for OASI... Error! Bookmark not defined. Appendix 3 OASI Postnatal Management plan... Error! Bookmark not defined. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 1
2 Midwives and obstetricians should be aware that suturing is a major and often traumatic event for women. Approximately 85% of women having a vaginal birth will sustain perineal trauma 1. Classification of genital trauma GRADE OF TEAR First degree Second degree Third degree Grade 3a Grade 3b Grade 3c Fourth degree Button Hole injury Labial injury FEATURES Injury to the perineal skin only Injury to the perineal muscles Injury to the perineal muscles AND disruption to the anal sphincter muscles <50% thickness of EAS (external anal sphincter) torn >50% thickness of EAS torn IAS (internal anal sphincter) also torn Disruption of both the anal sphincters and rectal epithelium A vaginal tear that breaches the anal mucosa but does not involve the muscles of the anal sphincters. Injury to the labia 2. Risk factors for OASI (obstetric anal sphincter injury) First vaginal delivery (including VBAC). Instrumental delivery (forceps without episiotomy has highest rate of OASI). Difficult delivery including: forceps, ventouse, shoulder dystocia, long second stage, oxytocin augmentation. Poor control at point of birth; waterbirth, BBA, no Manual Perineal Protection. Good communication is essential for a slow and controlled delivery. Large baby >4kg, OP position, large HC, post maturity, compound presentation (Hand delivered alongside head). Precipitate/rapid labour. Previous OASI, short perineum, scarred perineum, Asian ethnicity, FGM. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 2
3 Short stature (research shows that short statue under 5f 2/ 158cm is a risk factor for pelvic floor trauma) Advancing maternal age 3. Training in repair and OASI prevention The repair of the perineum is an important part of continuing care of a woman during labour and delivery. The trust and support that develop between a woman and her midwife can make the experience of suturing less traumatic. Women prefer to be sutured by their own midwife. A registered midwife may repair 1st and 2nd degree tears, episiotomies and labial tears. OASI and more complex labial/perineal tears should be undertaken by the obstetric registrar or consultant. All relevant healthcare professionals should attend specific training in perineal / genital assessment and repair, and ensure that they maintain these skills. Suturing workshops are timetabled throughout the year. These can be booked via Practice Development (plh-tr.midwiferypracticedev@nhs.net). The workshops are aimed at midwives, doctors or students, to update, enhance or learn current suturing techniques in perineal and labial trauma. An annual OASI study day run by Plymouth is highly recommended. It is relevant to all members of the obstetric and midwifery staff. It includes the latest research, practical sessions on OASI repair and OASI prevention. This is currently free to local staff and can be booked via Sarah Hooper. It is normally held in July, see posters for more details. 4. Prevention of OASI Prevention techniques should be used for all vaginal deliveries to minimise the risk of OASI due to the catastrophic impact OASI can have on a woman's longer term wellbeing. After 5 years 53% of women who sustain OASI will have some symptoms of anal incontinence (including urgency and incontinence of flatus). At the 34 or 36 week antenatal appointment all women should be given the booklet Perineal tears - Advice for mums-to-be and a signed OASI sticker applied to the birth plan page in her handheld notes. These both highlight to women the risk of OASI and gives simple preventative advice to women (see appendix 1). Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 3
4 The OASI Care Bundle is recommended for all vaginal deliveries (waterbirth exempt). 1.Discuss risk & OASI care bundle 2. Episiotomy, when indicated, at 60 degrees at crowning. 3. Use of manual perineal protection whenever possible. The only instance where it may not be possible to use MPP, is when women are labouring in water or, on a birthing stool, all other positions should allow for the attending clinician to visualise the perineum and use their hands to support it at time of delivery. Posterior shoulder delivered while MPP continues. 4. Perineal examination, including a per rectum examination, carried out following all vaginal deliveries. Thorough & systematic. Antenatally advice should include (all information in booklet Perineal tears-advice for mums-to-be ); Perineal massage from 35 weeks Pelvic floor exercises Brief description of risk factors and preventative techniques Encouraging optimum position of the baby (OA) Birth positions In labour where possible and not compromising the fetus, use the following techniques: Most importantly, a slow and controlled delivery of the head. MPP (manual perineal protection) using specific OASI care bundle technique (see image below). Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 4
5 Continue MPP during delivery of the posterior shoulder. A second assistant may be required to perform MPP during a difficult delivery or instrumental. Using a warm compress on the stretching perineum (this can also relieve discomfort for the woman). Episiotomy when required at a 60 degree angle, ideally with Epi-scissors. Allow natural expulsive efforts rather than forced, instructive pushing. Deliver baby in optimal position - lateral, all fours, semi-recumbent. Avoid squatting, birthing stools and lithotomy where possible. Women choosing a waterbirth should not be dissuaded from using water for analgesia in the 1st stage of labour. If a woman has multiple risk factors for OASI then recommend they deliver out of the pool from the start of the 2nd stage. This is due to the increased risk of an OASI when delivering underwater-probably due to poor visualisation, no MPP and a quicker 2 nd stage. 5. Assessment Systematic assessment including PR examination after every delivery is vital to correctly diagnose trauma. Of those women suffering anal incontinence after childbirth, 50% were found to have an incorrect assessment and an OASI missed. Training in PR examinations is vital for correct diagnosis of OASI. The woman should be referred to a more experienced healthcare professional if uncertainty exists as to the nature or extent of the trauma sustained. All relevant healthcare professionals should attend hands on training in perineal/genital assessment and repair and ensure that they maintain these skills. This is included in the training session mentioned in section 3. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 5
6 Before assessing for genital / perineal trauma, healthcare professionals should: o o o o Explain to the woman what they plan to do and why. Offer analgesia. Ensure good lighting. Position the woman so that she is comfortable and so that the genital structures can be seen clearly (usually lithotomy if in hospital). The timing of this systematic assessment should not interfere with mother infant bonding unless there is bleeding that requires urgent attention. The initial examination should be performed gently and with sensitivity and may be done in the immediate period following birth. Systematic assessment with PR examination should be carried out following all vaginal deliveries including women with apparently an intact perineum and should include: o o o o Further explanation of what is planned, why and consent obtained from the woman to continue. Confirmation by the woman that analgesia is adequate. Visual assessment of the trauma, the structures involved, the apex of the injury and assessment of bleeding. PR examination to assess whether there has been any damage to anal sphincters. Seek advice from more experienced staff if there is an uncertainty about the nature or extent of the trauma. 6. Perineal repair 1 st degree tears do not need to be sutured if the skin is in alignment and there is no bleeding. Difficult trauma should be repaired by an experienced operator in theatre under regional or general anaesthesia. It may be necessary to insert an indwelling catheter to prevent urinary retention. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 6
7 2 nd degree trauma should be sutured in order to improve healing. If a woman chooses not to be sutured, evidence of information and advice given must be documented. Perineal trauma should be repaired using an aseptic technique. Repair of the perineum should be undertaken as soon as possible to minimise the risk of infection and blood loss. Perineal repair should only be undertaken after effective analgesia is ensured either by infiltration with up to 20 ml of 1% lidocaine or topping up the epidural. If the woman reports inadequate pain relief at any point this should be addressed immediately. Please note 19% women reported a lot of pain during suturing and 12% of women reported suturing as the most painful part of childbirth. Good exposure and lighting is essential to see and identify the structures involved. An absorbable synthetic suture material should be used to suture the perineum. Identify the apex of the tear and use a surgical anchor knot to start 1cm above the apex of the tear. The vaginal wall and muscle layer should be repaired using a continuous nonlocked suturing technique and the dead-space deep intramuscularly closed to prevent bleeding and lower the risk of infection. If the skin is neatly opposed after suturing the muscle there is no need to suture it. Where the skin does require suturing, this should be undertaken using a continuous subcuticular technique. Always finish with a surgical knot, ideally not at the fourchette. Good anatomical alignment of the wound should be achieved, and consideration given to the cosmetic result. Rectal examination should be carried out after completing the repair to ensure that suture material has not been accidentally inserted through the rectal mucosa. Rectal non-steroidal anti-inflammatory drugs (e.g. Diclofenac 100 mg) should be offered routinely following perineal repair provided these drugs are not contraindicated. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 7
8 o Contraindications include postpartum haemorrhage, preeclampsia, renal disease, asthma, concurrent use of other NSAIDs. Information should be given to the woman about the extent of the trauma, pain relief, diet, pelvic floor and the importance of good hygiene. After completion of the repair accurately document on p44 of the yellow birth notes, with a drawing if needed, the following: consent, extent of the trauma, method of repair, type and number of sutures and swabs used,. A second signature is required for the swab/needle count (this doesn t need to be a registered health professional ie. HCA but patients and relatives cannot be asked). Community midwives should assess the perineum for signs of infection and wound breakdown with the woman's consent at each postnatal check-up. If any signs of infection are present, antibiotics should be prescribed via the GP (normally coamoxiclav) and a swab taken. Research shows between 1:10-20 wounds breakdown. The wound will then heal by secondary intention which is a much longer and more painful process. 7. Episiotomy Episiotomy should not be performed routinely but only where there are concerns for the fetal well-being or multiple maternal risk factors for OASI. If it is a woman's 1 st vaginal delivery and she requires a forceps delivery then an episiotomy is recommended. Most instrumental deliveries require an episiotomy. Use Epi-scissors whenever they are available. Note- please rinse epi-scissors with tap water after use as bodily fluids can degrade the metal, and if any concerns regarding their sharpness then please attach yellow tag shown below so SDU can hand sharpen. Please see picture below for how to use these scissors- line up the guide with the anus. The hilt of the blade should be at the base of the fourchette. This means the episiotomy with commence just to the right of the fourchette. If the guide is in line with the anus the episiotomy will be at the correct 60 degree angle. If an effective epidural anaesthetic is in place it should be topped up for delivery with the patient upright to get best coverage of the perineal area or the perineum should be infiltrated with local anaesthetic. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 8
9 If a tear is imminent, an episiotomy may be necessary without local anaesthetic. A mediolateral episiotomy at 60 O angle is recommended to avoid an OASI. Ideally this would be using the Epi-scissors as research shows practitioner inaccuracy on eye-balling the degree and length required. Do NOT dispose of these Epi-scissors and make a note of their use in the birth register and birth notes. 8. Repair of 3 rd or 4 th degree tear 8.1 Identification of injury The understanding of normal anal sphincter anatomy, adequate assessment of the obstetric trauma and appropriate repair are essential to maintenance of continence. 8.2 Prerequisites A repair should only be performed by a doctor who is experienced in anal sphincter repair (i.e. has attended a teaching session or course). For 4 th degree tears a Consultant Obstetrician has to be informed and surgical opinion may be sought at the consultant s discretion. A trainee obstetrician may carry out the repair but MUST be SUPERVISED by a Consultant Obstetrician or trained SpR. Repair should be conducted in an operating theatre where there is access to good lighting, appropriate equipment and aseptic conditions. General or epidural/spinal anaesthesia needs to be given prior to the commencement of the procedure. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 9
10 It is important that informed consent is obtained prior to the procedure. This should be recorded in the obstetric notes. 8.3 Procedure The full extent of the injury should be assessed in lithotomy position by vaginal and rectal examination. In the presence of a 4 th degree tear the torn rectal mucosa should be repaired with Polyglactin 3-0 interrupted, surgical knots pointing into the rectal lumen. The IAS should be repaired separately to the EAS with 3-0 PDS (Polydioxanone) or 2-0 Polyglactin (vicryl).using an end-to-end technique only with interrupted or mattress sutures. The two different suture materials have similar outcomes. When the EAS is injured with a partial thickness (i.e. some 3b and all 3a tears) it should be sutured with 3/0 PDS (Polydioxanone) or 2-0 Polyglactin by an end-to-end technique only. If the EAS injury is a full thickness tear the same suture materials as above can be used in either an end-to-end or an overlapping technique with similar outcomes. Surgical knots should be buried to prevent knot migration to the skin. Note there is a deep, superficial and subcutaneous part of the external anal sphincter. Reconstruction of the torn perineal body is essential. Consider using a standard Vicryl suture for repair of the perineal body. A rectal examination should be performed after the repair to ensure that sutures have not been inadvertently inserted through the anorectal mucosa. If a suture is identified it should be removed. Ensure adequate documentation by using page 44 in the intrapartum care (yellow) notes. Complete a proforma for every OASI and a Datix There are packs containing all the necessary paperwork for OASIs in the drawers behind the desk on CDS. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 10
11 8.4 Post-operative instructions Prevention of constipation: To reduce the risk of passing a large bolus of hard stool, which may disrupt the repair, a stool softener must be prescribed (e.g. lactulose) for 10 days. Prevention of infection: See Intravenous antibiotics in theatre (Co-amoxiclav 1.2g IV) and consider up to 3 days of oral co-amoxiclav 625mg TDS. Use alternative antibiotics if the patient has a Penicillin allergy: Mild Penicillin allergy: Cefuroxime 1.5g IV and Metronidazole 500mg IV in theatre (consider oral switch Cefalexin 500mg PO TDS and Metronidazole 400mg TDS for up to 3 days. Severe Penicillin allergy: Teicoplanin 400mg IV, Metronidazole 500mg IV and Gentamicin 240mg IV in theatre. (After this initial dose an individual consultation regarding ongoing management is required. A decision will need to be made regarding ongoing antibiotics as there is no straightforward oral switch for breastfeeding. Patients MAY choose to not continue with antibiotics after being counselled as there is only limited evidence of benefit. If ongoing antibiotics are felt to be necessary then follow with: oral Metronidazole 400mg TDS for up to 3 days and Teicoplanin 400mg IV at 12 hours and 24 hours after the first dose to complete the loading dose and then once every 24 hours to complete up to 3 days and Gentamicin 240mg IV OD (if the gentamicin level at hours after the first dose is <1mg/l to complete up to 3 days). No additional gentamicin levels are required if the renal function is normal. Please note that metronidazole covers anaerobes, Teicoplanin covers Gram positive organisms and gentamicin covers Gram negative organisms. It is not sufficient to only use part of this combined regimen Please clarify the allergy history carefully. You may need to speak to the patient s GP or review their previous hospital records to determine the exact nature of the reaction (were there features of immediate type hypersensitivity or not) and what other antibiotics they have safely received in the past subsequent to the date of the reaction. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 11
12 There is no straightforward oral switch for breastfeeding women with severe penicillin allergy. If it is necessary for antibiotics to continue, please contact microbiology in hours to discuss Pain control: Regular oral analgesia, avoid opiates e.g. codeine or oramorph Bladder care: Insert a Ch 14 Foley catheter with Instillagel and leave on free drainage until patient fully mobile. Measure 2 voids and if small volume will require bladder scan. See bladder care maternity guideline. 8.5 OASI follow-up Appointment to be made for Perineal Follow-up Clinic at 6-8 weeks. This is run by a midwife and physiotherapist. Clinic diary in red folder in notes room on CDS. Appointment to be made before the woman is transferred to the ward. A red top referral for anorectal studies (to be performed 6-9 months post delivery) should be sent to Mr. Oppong s secretary at delivery. If a woman is experiencing anal incontinence or pain at 6-8weeks, referral is made to the specialist joint clinic with both gynae and colorectal specialists present. 9. Patient information Patient information leaflet How to care for my stitches following the birth of my baby should be given for all types of perineal and anal sphincter trauma. Perineal checks must be carried out with consent by the community midwife at every contact. Any deviations from normality or signs of infection with OASI patients should be discussed with the on-call obstetric registrar or consultant. Signs of infection and wound breakdown in the perineum should be prescribed antibiotics via the GP or triage. Be aware that this can be a route of severe infection - look for signs of sepsis and refer appropriately (see Sepsis guideline). Where there are communication or language support needs assistance can be obtained via patient advice and liaison service (PALS) and interpretation services. Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 12
13 10. Swab counts All swabs used in Maternity must be x-ray detectable, not less than 30 cm x 30 cm and have tails (this is the only type of swab available on labour ward). A 2 person swab count must be conducted prior to and following any procedure in which they are used. This must be clearly documented, together with the names and signatures of the persons conducting the swab count, within the birth record or surgical booklet, if procedure undertaken in theatre. Any swabs/vaginal packs deliberately left in the vagina MUST be clearly documented together with a management plan for their removal. 11. Audit and monitoring Audits of OASI are presented to Clinical Effectiveness Committee and Clinical Governance and Risk Management committee. Findings together with recommendations and action plan published in Risk Management (RM) Newsletter for dissemination of information to all staff. Follow-up of rate and cause of returns for women with problems relating to all types of perineal repair is achieved via Datix incident reporting system. Readmission of all women should be reported. This feeds into RM strategy for review. 12. Record keeping It is expected that every episode of care be recorded clearly, in chronological order and as contemporaneously as possible by all healthcare professionals. This is in keeping with standards set by professional colleges, i.e. NMC and RCOG. All entries must have the date and time together with signature and printed name. Documentation with respect to perineal trauma: Ensure adequate documentation by using the perineal repair template in the Birth Notes page 44. Documentation should include: The extent of trauma. Analgesia used for repair Material used Technique used Swab and needle count prior to and on completion of procedure Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 13
14 Documentation of advice given Postnatal documentation A sticker for OASI (see appendix 3) should be placed in the mother s management plan. Alternatively, a handwritten management may be documented for perineal or labial repair. Appendix 1 Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 14
15 Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 15
16 Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 16
17 Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 17
18 Monitoring: Auditable standards: Antenatal- booklet discussing risk and prevention of OASI. And sticker for handheld notes Postnatal OASI Performa and Datix Audit of OASI- identify risk factors and preventative techniques used and follow up care Management of 3 / 4 degree tears Standards of record keeping in relation to all perineal trauma Documented patient information and PIL Audit of documentation and implementation of swab counts Please refer to audit tool, location: Maternity on cl2-file11, Guidelines Reports to: Clinical Effectiveness Committee responsible for action plan and implementation of recommendations from audit Service Line Business Meeting Care group quality assurance committee (QAC) Frequency of audit: continually Responsible person: CDS Manager Training requirements Audit of training needs compliance please refer to TNA policy Annual midwives training OASI prevention/diagnosis session (grand round for Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 18
19 doctors) Suturing workshops Training needs analysis: Please refer to Training Needs Analysis guideline together with training attendance database for all staff Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 19
20 Cross references Maternity Hand Held Notes, Hospital Records and Record Keeping - ity%20hand%20held%20notes%20and%20hospital%20records.pdf?timestamp= Care of urinary bladder - /EXPIRED%20Bladder%20care.pdf?timestamp= Sepsis, infection and prophylaxis in obstetric patients - /Sepsis,%20infection%20and%20prophylaxis%20in%20obstetric%20patients.pdf?tim estamp= References OASI care bundle-laine 2012 Incidence of OASI after training to protect the perineum Episcissors-60 for guided mediolateral episiotomy. July 2015 Medtech innovation briefing [MIB33] NICE recommendations for Intrapartum care for healthy women and their babies. NICE clinical guideline 190; published 2017, updated Feb Royal College of Obstetricians and Gynaecologists (RCOG) Greentop guideline 29. The management of 3 rd and 4 th degree perineal tears. June Royal College of Midwives 2012 Evidence Based Guidelines for Midwifery-Led Care in Labour- suturing the perineum Keighley et al, 2016 The social, psychological, emotional morbidity and adjustment techniques for women with anal incontinence following obstetric Anal Sphincter Injury. BMC pregnancy and childbirth Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 20
21 Author Lizzie Percy, Joseph Clarke, Professor Robert Freeman Work Address Maternity Unit, Derriford Hospital, Plymouth, Devon, PL6 8DH Version 1 OASI prevention including booklet and sticker OASI care bundle- hands on Training workshops in prevention, diagnosis and repair Episcissors Packs Changes Risk factors for OASI Closer observation by community midwives for perineal infection Catheter post OASI can now be removed once patient fully mobile and 2 voids measured as per bladder guideline Antibiotics reduced to stat IV dose in theatre plus considering up to 3 days oral. Audit ongoing with this via follow up clinic Date Ratified July 2018 Valid Until Date July 2023 Repair of Perineal trauma, including 3 rd and 4 th degree tear Page 21
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Clinical Guideline for: The Management of Perineal Trauma following Childbirth
 For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
For Use in: By: For: Division responsible for document: Key words: Name of document author: Job title of document author: Name of document author s Line Manager: Job title of author s Line Manager: Supported
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
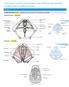 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Guideline for Management and Repair of Perineal Trauma
 Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Guideline for Management and Repair of Perineal Trauma Author: Labour Ward Forum Specialty: Maternity Date Approved: September 2014 Approved by: W&CH Clinical Governance Committee Date for Review: August
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May Dr. Annie Leong MBBS, FRANZCOG, CU
 EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
EPISIOTOMY & PERINEAL TEARS Anatomy &Functionality May 2011 Dr. Annie Leong MBBS, FRANZCOG, CU Restore normal perineal anatomy Achieve good haemostasis Avoid infection and wound breakdown Avoid coital
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Taking care of your perineum before, during and after birth
 Taking care of your perineum before, during and after birth A Parent Information Leaflet Where is is my my perineum and and what what happens happens during childbirth? during childbirth? Your perineum
Taking care of your perineum before, during and after birth A Parent Information Leaflet Where is is my my perineum and and what what happens happens during childbirth? during childbirth? Your perineum
Patient Advice for Third & Fourth Degree Tears
 Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
SUTURING AN EPISIOTOMY/GENITAL LACERATION
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
Hands-on Workshop. Cape Town, South Africa 3 August Chairpersons
 Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Hands-on Workshop www.perineum.net Cape Town, South Africa 3 August 2016 Chairpersons Mr Abdul H Sultan, MB.ChB (Natal), MD, FRCOG Consultant Obstetrician & Urogynaecologist Miss Ranee Thakar, MB.BS, MD,
Risk factors and management of obstetric perineal injury
 Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Risk factors and management of obstetric perineal injury Ruwan J Fernando Abstract Perineal injury sustained during childbirth is a major aetiological factor in the development of perineal pain, sexual
Guidelines on the Management of Complications related to Female Genital Mutilation
 Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE. Our suture portfolio meets all your procedural needs
 UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
UNDERSTANDING EPISIOTOMY C-SECTION AND RECTOCELE Our suture portfolio meets all your procedural needs GYNECOLOGY Episiotomy A surgically planned incision on the perineum and the posterior vaginal wall,
Female Genital Mutilation (circumcision) guideline (GL837)
 Female Genital Mutilation (circumcision) guideline (GL837) Approval Approval Group Job Title, Chair of Committee Date Policy Approval Group Chair, Policy Approval Group July 2018 Maternity & Children s
Female Genital Mutilation (circumcision) guideline (GL837) Approval Approval Group Job Title, Chair of Committee Date Policy Approval Group Chair, Policy Approval Group July 2018 Maternity & Children s
Bladder care postpartum including bladder care for women with epidural analgesia (GL792)
 Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Bladder care postpartum including bladder care for women with epidural analgesia (GL792) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children's Services Clinical Governance Committee
Perineal Trauma Assessment, Repair and Safe Practice
 1. Purpose This document outlines the guideline and the procedure details for the assessment and repair of perineal trauma in postpartum women. Genital tract trauma can occur spontaneously during a vaginal
1. Purpose This document outlines the guideline and the procedure details for the assessment and repair of perineal trauma in postpartum women. Genital tract trauma can occur spontaneously during a vaginal
Number of pages: This policy and procedure guideline applies to all obstetrics and gynecology medical and midwifery staff.
 Saudi Society of Obstetrics and Gynaecology Policy and Procedure Title/Description: REPAIR OF PERINEAL TRAUMA Effective Date: 1st July 2016 1. PURPOSE Department: Obstetrics and Gynecology (Labour & Birth)
Saudi Society of Obstetrics and Gynaecology Policy and Procedure Title/Description: REPAIR OF PERINEAL TRAUMA Effective Date: 1st July 2016 1. PURPOSE Department: Obstetrics and Gynecology (Labour & Birth)
Women & Children's Business Unit Maternity Contraception and Sexual Health
 Women & Children's Business Unit Maternity Contraception and Sexual Health Author/s Contact name Approval process Obstetric Guidelines Group/Associate Medical Director First Issue Date Trust intranet ref:
Women & Children's Business Unit Maternity Contraception and Sexual Health Author/s Contact name Approval process Obstetric Guidelines Group/Associate Medical Director First Issue Date Trust intranet ref:
Pain Relief in Labour Epidurals and Spinals
 Pain Relief in Labour Epidurals and Spinals Information for woman Maternity Services For more information, please contact: Anaesthetics Department Telephone Scarborough: 01723 385202 Telephone York: 01904
Pain Relief in Labour Epidurals and Spinals Information for woman Maternity Services For more information, please contact: Anaesthetics Department Telephone Scarborough: 01723 385202 Telephone York: 01904
Maternity Services. Comment / Changes / Approval. First draft of new guidelines. Comments included after consultation.
 Bladder Care v4.0 Nov 2016 for public website FINAL NOV16 Document Control Title Bladder Care Guideline Author Directorate Women and Children s Version Date Issued Status 0.1 Jun Draft 2009 0.2 July 2009
Bladder Care v4.0 Nov 2016 for public website FINAL NOV16 Document Control Title Bladder Care Guideline Author Directorate Women and Children s Version Date Issued Status 0.1 Jun Draft 2009 0.2 July 2009
Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair
 SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
SOGC CLINICAL PRACTICE GUIDELINE No. 330, December 2015 Obstetrical Anal Sphincter Injuries (OASIS): Prevention, Recognition, and Repair This clinical practice guideline has been prepared by the Urogynaecology
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD
 PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
PROTOCOL FOR BLADDER CARE MANAGEMENT DURING INTRAPARTUM AND POSTNATAL PERIOD Specialty: Obstetrics Date Approved: Revised September 2015 Approved by: Labour Ward Forum Date for Review: September 2018 Overview
Discharge information for patients Fistula plug for anal fistula
 Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
Discharge information for patients Fistula plug for anal fistula Clinical Sciences Building Colorectal Surgery 0161 206 1249 All Rights Reserved 2017. Document for issue as handout.. What is an anal fistula?
Guideline for the Post Operative Management of Women who have received Intrathecal or Epidural Opioid Analgesia for Caesarean Section
 Guideline for the Post Operative Management of Women who have received Intrathecal or Epidural Opioid Analgesia for Caesarean Section Speciality: Maternity Approval Body: Labour Ward Forum Approval Date:
Guideline for the Post Operative Management of Women who have received Intrathecal or Epidural Opioid Analgesia for Caesarean Section Speciality: Maternity Approval Body: Labour Ward Forum Approval Date:
Aneurin Bevan University Health Board Diabetes in Pregnancy: Care Pathway for Management of Diabetes in Pregnancy
 Aneurin Bevan University Health Board Diabetes in Pregnancy: Care Pathway for Management of Diabetes in Pregnancy N.B. Staff should be discouraged from printing this document. This is to avoid the risk
Aneurin Bevan University Health Board Diabetes in Pregnancy: Care Pathway for Management of Diabetes in Pregnancy N.B. Staff should be discouraged from printing this document. This is to avoid the risk
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Perineal Suturing and Surgical Drapes/Gowns
 Date of Search: 11 January 2017 Sources Searched: Medline, Embase, CINAHL, TRIP Database, Cochrane Library Perineal Suturing and Surgical Drapes/Gowns Summary Surgical site infection has been estimated
Date of Search: 11 January 2017 Sources Searched: Medline, Embase, CINAHL, TRIP Database, Cochrane Library Perineal Suturing and Surgical Drapes/Gowns Summary Surgical site infection has been estimated
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
INTRAPARTUM AND POSTNATAL BLADDER CARE
 INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
INTRAPARTUM AND POSTNATAL BLADDER CARE BACKGROUND Urinary retention is uncommon but carries significant morbidity and the risk is increased by a number of factors including epidural analgesia (Teo, et
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
Diabetes Emergency Caesarean section or other unplanned surgery (GL822)
 Diabetes Emergency Caesarean section or other unplanned surgery (GL822) i.e. insulin dependent diabetic having unplanned surgery e.g. a diabetic woman with pre-labour SROM prior to elective Caesarean section.
Diabetes Emergency Caesarean section or other unplanned surgery (GL822) i.e. insulin dependent diabetic having unplanned surgery e.g. a diabetic woman with pre-labour SROM prior to elective Caesarean section.
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases
 CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
CASE REPORT Secondary Repair of Third Degree Perineal Tear Leading to Fecal Incontinence in 2 Cases Vasant Kawade 1 and Abhijit Ambike 2 Professor and Head, Department of OBGY, B.K.L.Walawakarl Rural Medical
GUIDELINE FOR THE POST OPERATIVE MANAGEMENT OF WOMEN WHO HAVE RECEIVED INTRATHECAL OR EPIDURAL OPIOID ANALGESIA FOR CAESAREAN SECTION
 GUIDELINE FOR THE POST OPERATIVE MANAGEMENT OF WOMEN WHO HAVE RECEIVED INTRATHECAL OR EPIDURAL OPIOID ANALGESIA FOR CAESAREAN SECTION Originator: Maternity Services & Anaesthetics Dept Date Approved: January
GUIDELINE FOR THE POST OPERATIVE MANAGEMENT OF WOMEN WHO HAVE RECEIVED INTRATHECAL OR EPIDURAL OPIOID ANALGESIA FOR CAESAREAN SECTION Originator: Maternity Services & Anaesthetics Dept Date Approved: January
Diabetes in pregnancy
 Diabetes in pregnancy Patient information This leaflet provides information about gestational diabetes during pregnancy and delivery. Sometimes women who are not known to have diabetes develop it during
Diabetes in pregnancy Patient information This leaflet provides information about gestational diabetes during pregnancy and delivery. Sometimes women who are not known to have diabetes develop it during
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
Patient Information. Tension Free Vaginal/ Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust
 Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Yorkshire & the Humber Clinical Network. Striving to Reduce Stillbirth Rates and Improve Bereavement Care
 Yorkshire & the Humber Clinical Network Striving to Reduce Stillbirth Rates and Improve Bereavement Care Transforming and Modernising Maternity Care in England London 12 th July 2016 Content Yorkshire
Yorkshire & the Humber Clinical Network Striving to Reduce Stillbirth Rates and Improve Bereavement Care Transforming and Modernising Maternity Care in England London 12 th July 2016 Content Yorkshire
Treating your prolapse
 Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
8 A SIMPLE FISTULA REPAIR, STEP BY STEP
 8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
8 A SIMPLE FISTULA REPAIR, STEP BY STEP The first step is to suture the labia to the thighs and cover the anus with a swab (Figure 31). Figure 31 The labia are sutured to the thighs and the anus is covered
RANZCOG Advanced Training Modules
 RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
RANZCOG Advanced Training Modules Generalist Obstetrics ATM and Generalist Gynaecology ATM The Generalist ATMs in each of Obstetrics and Gynaecology provide a framework for trainees to consolidate and
Pain Relief During Labor and Delivery
 Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Tension-free Vaginal Tape (TVT)
 Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Page 1 of 7 Tension-free Vaginal Tape (TVT) Introduction This leaflet will provide you with basic information about the Tension--free Vaginal Tape (TVT) procedure. What is a TVT? TVT is an operation to
Posterior Vaginal Wall Prolapse Repair And Repair of Perineum
 Posterior Vaginal Wall Prolapse Repair And Repair of Perineum Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together by members of the BSUG
Posterior Vaginal Wall Prolapse Repair And Repair of Perineum Patient Information Leaflet BSUG Patient Information Sheet Disclaimer This patient information sheet was put together by members of the BSUG
Hepatitis B protocol (CG487)
 Hepatitis B protocol (CG487) Approval and Authorisation Approved by Maternity Clinical Guidelines Committee Job Title or Chair of Committee Chair, Maternity Clinical Governance Committee Date 6 th April
Hepatitis B protocol (CG487) Approval and Authorisation Approved by Maternity Clinical Guidelines Committee Job Title or Chair of Committee Chair, Maternity Clinical Governance Committee Date 6 th April
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Integrated Continence Service Policy. January SafeCare Council January Carol Giffin, Continence Advisor
 Policy No: OP51 Version: 1.0 Name of Policy: Integrated Continence Service Policy Effective From: January 2008 Approved by: SafeCare Council January 2008 Next Review Date: January 2010 Reviewed by: Carol
Policy No: OP51 Version: 1.0 Name of Policy: Integrated Continence Service Policy Effective From: January 2008 Approved by: SafeCare Council January 2008 Next Review Date: January 2010 Reviewed by: Carol
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Haemorrhoidectomy. Colorectal Surgery. Patient Information
 Haemorrhoidectomy Colorectal Surgery Patient Information What are haemorrhoids? Haemorrhoids, also know as piles, are soft fleshy lumps just inside the back passage (anus). They have a rich blood supply
Haemorrhoidectomy Colorectal Surgery Patient Information What are haemorrhoids? Haemorrhoids, also know as piles, are soft fleshy lumps just inside the back passage (anus). They have a rich blood supply
BASINGSTOKE AND NORTH HAMPSHIRE NHS FOUNDATION TRUST. Clinical Policy for Peripheral Venous Cannula Insertion and Management (Adults)
 BASINGSTOKE AND NORTH HAMPSHIRE NHS FOUNDATION TRUST Clinical Policy for Peripheral Venous Cannula Insertion and Management (Adults) Reviewed in accordance with The Health and Social Care Act 2008: Code
BASINGSTOKE AND NORTH HAMPSHIRE NHS FOUNDATION TRUST Clinical Policy for Peripheral Venous Cannula Insertion and Management (Adults) Reviewed in accordance with The Health and Social Care Act 2008: Code
Surveillance report Published: 8 June 2017 nice.org.uk. NICE All rights reserved.
 Surveillance report 2017 Antenatal and postnatal mental health: clinical management and service guidance (2014) NICE guideline CG192 Surveillance report Published: 8 June 2017 nice.org.uk NICE 2017. All
Surveillance report 2017 Antenatal and postnatal mental health: clinical management and service guidance (2014) NICE guideline CG192 Surveillance report Published: 8 June 2017 nice.org.uk NICE 2017. All
Epidural analgesia in labour Guideline for care
 This is an official Northern Trust policy and should not be edited in any way Epidural analgesia in labour Guideline for care Reference Number: NHSCT/12/523 Target audience: This policy is directed to
This is an official Northern Trust policy and should not be edited in any way Epidural analgesia in labour Guideline for care Reference Number: NHSCT/12/523 Target audience: This policy is directed to
Pregnancy and childbirth: the effects on pelvic floor muscles
 Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
Page 1 of 9 Pregnancy and childbirth: the effects on pelvic floor muscles 26 February, 2009 Stress incontinence can follow childbirth as pelvic floor muscles are damaged AUTHOR Julia Herbert, MSc, MCSP,
The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units
 Royal College of Obstetricians and Gynaecologists and London School of Hygiene and Tropical Medicine The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units An audit
Royal College of Obstetricians and Gynaecologists and London School of Hygiene and Tropical Medicine The Prevention of Early-onset Neonatal Group B Streptococcal Disease in UK Obstetric Units An audit
Advice for patients following a Slap Repair
 Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Urinary Catheters. Prevalence of Infections
 Urinary Catheterisation Urinary catheterisation is defined as an intervention to enable the emptying of the bladder by insertion of a catheter. Catheters can be short term less than 28 days or long term
Urinary Catheterisation Urinary catheterisation is defined as an intervention to enable the emptying of the bladder by insertion of a catheter. Catheters can be short term less than 28 days or long term
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086)
 Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Seasonal Influenza in Pregnancy and Puerperium Guideline (GL1086) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity
Asthma in Pregnancy, Labour and Postnatal Guidelines
 Asthma in Pregnancy, Labour and Postnatal Guidelines N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet
Asthma in Pregnancy, Labour and Postnatal Guidelines N.B. Staff should be discouraged from printing this document. This is to avoid the risk of out of date printed versions of the document. The Intranet
Focus on Post-Partum Incontinence
 Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
A Comparison Study on Chlorhexidine and Normal Saline for Perineal Wound Cleansing
 A Comparison Study on Chlorhexidine and Normal Saline for Perineal Wound Cleansing Department of Obstetrics & Gynaecology Kwong Wah Hospital Sin Ming TAI, Amy KM YEUNG, Karen KL YU, Pui I LOU, Alice SY
A Comparison Study on Chlorhexidine and Normal Saline for Perineal Wound Cleansing Department of Obstetrics & Gynaecology Kwong Wah Hospital Sin Ming TAI, Amy KM YEUNG, Karen KL YU, Pui I LOU, Alice SY
An operation for anterior vaginal wall prolapse
 n The Leeds Teaching Hospitals NHS Trust An operation for anterior vaginal wall prolapse Information for patients Leeds Centre for Women s Health BSUG (British Society of Urogynaecology) Patient Information
n The Leeds Teaching Hospitals NHS Trust An operation for anterior vaginal wall prolapse Information for patients Leeds Centre for Women s Health BSUG (British Society of Urogynaecology) Patient Information
Post operative voiding dysfunction and the Value of Urodynamics. Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist
 Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Post operative voiding dysfunction and the Value of Urodynamics Dr Salwan Al-Salihi Urogynaecologist Obstetrician and Gynaecologist Learning objectives: v Pathophysiology of post op voiding dysfunction.
Returning to fitness after birth
 Returning to fitness after birth This leaflet is designed for all women, whether you have given birth vaginally or by Caesarean section. During pregnancy your body undergoes many changes to adapt to your
Returning to fitness after birth This leaflet is designed for all women, whether you have given birth vaginally or by Caesarean section. During pregnancy your body undergoes many changes to adapt to your
Posterior vaginal wall prolapse repair and repair of perineum
 INFORMATION FOR PATIENTS Posterior vaginal wall prolapse repair and repair of perineum We advise you to take your time to read this leaflet. If you have any questions please write them down on the sheet
INFORMATION FOR PATIENTS Posterior vaginal wall prolapse repair and repair of perineum We advise you to take your time to read this leaflet. If you have any questions please write them down on the sheet
Screening, Diagnosis and Management of Gestational Diabetes in New Zealand: A Clinical Practice Guideline
 Screening, Diagnosis and Management of Gestational Diabetes in New Zealand: A Clinical Practice Guideline 6 November 2014 Gary Tonkin Today Process to develop the guideline What the guideline recommends
Screening, Diagnosis and Management of Gestational Diabetes in New Zealand: A Clinical Practice Guideline 6 November 2014 Gary Tonkin Today Process to develop the guideline What the guideline recommends
Guidelines for the Manual Evacuation of Faeces
 Rationale Guidelines for the Manual Evacuation of Faeces These guidelines are to provide the required information for designated registered nurses, health care assistants and bank support workers to perform
Rationale Guidelines for the Manual Evacuation of Faeces These guidelines are to provide the required information for designated registered nurses, health care assistants and bank support workers to perform
INTRAVENOUS HYDRALAZINE POLICY
 PURPOSE INTRAVENOUS HYDRALAZINE POLICY The purpose of this policy is to: provide safe and effective care for women establish a local approach to care that is evidence based and consistent inform good decision
PURPOSE INTRAVENOUS HYDRALAZINE POLICY The purpose of this policy is to: provide safe and effective care for women establish a local approach to care that is evidence based and consistent inform good decision
Patient Group Direction for the Supply of Nitrofurantoin MR 100mg capsules
 October 2016 Patient Group Direction for the Supply of Nitrofurantoin MR 100mg capsules This Patient Group Direction (PGD) is a specific written instruction for the supply and/or administration of nitrofurantoin
October 2016 Patient Group Direction for the Supply of Nitrofurantoin MR 100mg capsules This Patient Group Direction (PGD) is a specific written instruction for the supply and/or administration of nitrofurantoin
Coping with a difficult birth experience and where to get help
 Coping with a difficult birth experience and where to get help I had flashbacks of the final delivery for weeks afterwards and couldn t stop thinking about it I blame myself for not having a good birth,
Coping with a difficult birth experience and where to get help I had flashbacks of the final delivery for weeks afterwards and couldn t stop thinking about it I blame myself for not having a good birth,
Pregnancy, birth and postnatal information for women who have epilepsy
 Pregnancy, birth and postnatal information for women who have epilepsy This leaflet is for pregnant women with epilepsy. It explains what complications may occur, how your pregnancy will be monitored because
Pregnancy, birth and postnatal information for women who have epilepsy This leaflet is for pregnant women with epilepsy. It explains what complications may occur, how your pregnancy will be monitored because
Pain Relief Options for Labor. Providing you with quality care, information and support
 Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
Pain Relief Options for Labor Providing you with quality care, information and support What can I expect during my labor and delivery? As a patient in the Labor and Delivery suite at Lucile Packard Children
RECTAL INJURY IN UROLOGIC SURGERY. Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences.
 RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
RECTAL INJURY IN 27 UROLOGIC SURGERY Inadvertent rectal injury from a urologic procedure is often subtle but has serious postoperative consequences. With good mechanical bowel preparation plus antibiotic
2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL)
 E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
E10d 2012/13 NHS STANDARD CONTRACT FOR ACUTE, AMBULANCE, COMMUNITY AND MENTAL HEALTH AND LEARNING DISABILITY SERVICES (MULTILATERAL) SECTION B PART 1 - SERVICE SPECIFICATIONS Service Specification No.
A Clinical Guideline for Bladder Care in Labour and Postnatally
 For Use in: Maternity department By: Clinical staff caring for women during pregnancy, labour and postnatally For: Obstetric patients Division responsible for document: Division 3- Women and Children s
For Use in: Maternity department By: Clinical staff caring for women during pregnancy, labour and postnatally For: Obstetric patients Division responsible for document: Division 3- Women and Children s
Urethral Bulking to treat Stress Urinary Incontinence. Patient Information Leaflet
 Urethral Bulking to treat Stress Urinary Incontinence Patient Information Leaflet About this leaflet The information provided in this leaflet should be used as a guide. There may be some variation in how
Urethral Bulking to treat Stress Urinary Incontinence Patient Information Leaflet About this leaflet The information provided in this leaflet should be used as a guide. There may be some variation in how
in pregnancy Document Review History Version Review Date Reviewed By Approved By
 GYNAECOLOGY/ ANTENATAL CARE WIRRAL WOMEN & CHILDREN S HOSPITAL Guideline No: Hepatitis B management in pregnancy VERSION 1 AMENDMENTS MADE: N/A DATE OF ISSUE: May 2012 DATE OF REVIEW: May 2015 REVIEW INTERVAL:
GYNAECOLOGY/ ANTENATAL CARE WIRRAL WOMEN & CHILDREN S HOSPITAL Guideline No: Hepatitis B management in pregnancy VERSION 1 AMENDMENTS MADE: N/A DATE OF ISSUE: May 2012 DATE OF REVIEW: May 2015 REVIEW INTERVAL:
Arthroscopic rotator cuff repair
 Arthroscopic rotator cuff repair This leaflet aims to answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives to the
Arthroscopic rotator cuff repair This leaflet aims to answer some of the questions you may have about having an arthroscopic rotator cuff repair. It explains the benefits, risks and alternatives to the
Epidural Analgesia in Labor
 Epidural Analgesia in Labor Epidural analgesia is one of the most advanced methods used for labor pain relief. At our maternity hospital, it is a well proven and the most frequently used method. The following
Epidural Analgesia in Labor Epidural analgesia is one of the most advanced methods used for labor pain relief. At our maternity hospital, it is a well proven and the most frequently used method. The following
Indwelling Urinary Catheter Template for Care Plan Development Problem No: be a last resort when all suprapubic catheter in CAUTI
 Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
Indwelling Urinary Catheter Template for Care Plan Development Problem No: Name: DOB Address: Indwelling Urinary Catheter (Urethral/ Suprapubic) Date Assessed Need GOAL INTERVENTION Evaluation of intervention/
REVERSAL OF ILEOSTOMY. Patient information Leaflet
 REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
REVERSAL OF ILEOSTOMY Patient information Leaflet April 2017 WHAT IS A REVERSAL OF ILEOSTOMY? A reversal of ileostomy is an operation to close your temporary ileostomy. Your surgeon will make a cut in
Women and Children s Business Unit. Document Reference: Author: E Alston M/W /SoM Impact Assessment Date: APPROVAL RECORD Committees / Group
 Policy Title: Executive Summary: Guideline for the Care of a Woman with Female Genital Mutilation Female Genital Mutilation (FGM) constitutes all the procedures that involve partial or total removal of
Policy Title: Executive Summary: Guideline for the Care of a Woman with Female Genital Mutilation Female Genital Mutilation (FGM) constitutes all the procedures that involve partial or total removal of
6 THE OPERATIONS BASIC PRINCIPLES
 6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
6 THE OPERATIONS BASIC PRINCIPLES Basic principles are described here; strategies for specific situations are discussed in later sections. The basic principles in the repair of a fistula are: adequate
OAA Survey 156: Current prescribing practices for post-operative analgesia following emergency and elective LSCS
 OAA Survey 56: Current prescribing practices for post-operative analgesia following emergency and elective LSCS Janis M Ferns, Jennifer Lambert, Dharshini Radhakrishnan 2. Specialty Trainee, Barts and
OAA Survey 56: Current prescribing practices for post-operative analgesia following emergency and elective LSCS Janis M Ferns, Jennifer Lambert, Dharshini Radhakrishnan 2. Specialty Trainee, Barts and
Pelvic Floor Ultrasound Imaging. Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague)
 Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
Pelvic Floor Ultrasound Imaging Workshop IUGA 2015 Nice Faculty: Prof HP Dietz (Sydney) A/Prof KL Shek (Sydney) Dr R Guzman Rojas (Santiago de Chile) Dr Kamil Svabik (Prague) The use of translabial ultrasound
