Postpartum Complications
|
|
|
- Paulina Byrd
- 5 years ago
- Views:
Transcription
1 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline for resolution is not necessarily linear and not the same for all organs or tissues. Women in the postpartum period should be monitored for postpartum complications. Frequency of follow-up depends on specific issues encountered during childbirth and the immediate postpartum period. A thorough understanding of the labor and delivery process, including procedures (eg, perineal lacerations repair, episiotomies, operative vaginal deliveries, and cesarean deliveries) used for specific circumstances, is especially helpful when caring for the patient who develops a postpartum complication. Box 1 provides sample guidance for patients on how to perform pelvic floor exercises that will strengthen the muscles that surround the openings of the urethra, vagina, and rectum. Comprehensive prenatal care incorporates key elements of the postpartum phase into patient counseling. Anticipatory counseling in the prenatal period guides patient expectations regarding routine procedures and postpartum changes, both normal and abnormal. Equipping women with knowledge of the childbirth process and the postpartum period empowers them to understand what to expect, recognize changes, and be able to advocate for their health care needs. Urinary Incontinence Background The prevalence of urinary incontinence (UI) varies widely in the postpartum period, ranging from 3% to 40%. For many women, urinary incontinence resolves spontaneously during the first 3 months of the postpartum period and the prevalence decreases to a range of 11 23% in the 3 12 months of the postpartum period. Risk factors include vaginal delivery, increased duration of second stage of labor, older age, greater parity, increased body mass index, excess maternal weight gain during pregnancy, fetal weight (more than 4 kg), family history, and UI during pregnancy. Screening and Diagnosis Women s health care providers should routinely discuss incontinence at the postpartum visit to confirm spontaneous resolution or evaluate the need for further therapy in those with persistent UI symptoms. A urine culture should be obtained to rule out urinary tract infection. Copyright 2018 by the American College of Obstetricians and Gynecologists, th Street SW, PO Box 96920, Washington, DC
2 Postpartum Complications 2 Treatment Pelvic floor muscle (Kegel) exercises are effective at strengthening the muscles that surround the urethra, vagina, and anus and should be recommended for women with symptoms of UI who are in the postpartum period. Health care providers can instruct and coach women on Kegel exercises (see Box 1). Health care providers should consider focusing on modifiable risk factors, such as obesity and smoking, to decrease the incidence of UI. Current data are conflicting, but physical therapy with pelvic floor muscle training may be used to treat women with persistent postpartum UI at 3 months after delivery. Anticipatory Guidance and Follow-up Anticipatory counseling in the antepartum period is necessary to educate patients and set expectations. Consider referral to urogynecology if UI is persistent and disturbing to the patient. Urogynecology assessment helps to identify issues that require more immediate action (eg, revision of an obstetric laceration breakdown) affords an opportunity to educate patients about the pelvic floor, the role of Kegel exercises, and biofeedback training or pelvic floor physical therapy, or both, if deemed appropriate provides reassurance to the patient The American College of Obstetricians and Gynecologists has developed a Patient FAQ on Urinary Incontinence. Long-term follow-up is necessary to assess stability of results Box 1. Kegel Exercises Patient Education FAQ With an empty bladder, squeeze muscles used to stop flow of urine Hold for 3 seconds, then relax for 3 seconds Do 10 contractions at least three times a day Increase hold by 1 second each week up to 10-second holds Breathe normally through these exercises
3 Postpartum Complications 3 Fecal Incontinence Background Up to 10% of women report fecal incontinence during pregnancy. Obstetric anal sphincter injuries (OASIS) occurs in 18% of vaginal deliveries, and 13 25% of women experience fecal incontinence or flatus incontinence after childbirth. Significant improvement occurs in women by 3 6 months in the postpartum period; some women may experience fecal incontinence 2 or more years after delivery. Risk factors for fecal incontinence include vaginal delivery, length of second stage of labor, large birth weight, increasing maternal age, forceps delivery, OASIS by anal sphincter laceration or episiotomy, and maternal position during childbirth. The lateral position affords a slightly protective effect from OASIS in the nulliparous woman, compared with standing, squatting, or lithotomy. Screening and Diagnosis Studies reveal that women are not asked about incontinence by their health care providers at the postpartum visit. Women may not seek treatment because of embarrassment and shame. Health care providers should routinely discuss fecal incontinence at the postpartum visit to confirm spontaneous resolution or evaluate the need for further therapy in those with persistent fecal incontinence symptoms. Anal sphincter injury that is not apparent immediately after delivery is referred to as an occult sphincter laceration, and physical examination can identify the disrupted anal sphincter complex in most women. Endoanal ultrasonography is the gold standard tool used by the urogynecologist to evaluate anal sphincter pathology in the investigation of fecal incontinence. Anal sphincter disruption can be identified on sonogram because external and internal sphincters can be visualized on ultrasonography. Treatment Anal sphincter repair immediately after delivery reduces the risk of fecal incontinence. A fiber-rich diet, adequate hydration, and use of a stool softener started immediately after childbirth can control consistency of the stool and prevent constipation and straining, which allows optimal healing. Pelvic floor muscle (Kegel) exercises are not only effective for stress urinary incontinence but also have been shown to improve symptoms of fecal incontinence in postpartum women. Health care providers can instruct and coach patients on the use of Kegel exercises (see Box 1). Inadequate anal sphincter repair immediately after delivery or break down of repair requires sphincteroplasty, which is most effective in women with moderate or severe fecal incontinence. Sphincteroplasty also is used in women with occult sphincter lacerations. A sacral nerve stimulator may be implanted in women who do not desire surgical therapy or in those in whom sphincteroplasty has failed.
4 Postpartum Complications 4 Anticipatory Guidance and Follow-up Anticipatory counseling in the antepartum period is necessary for educating patients and setting expectations. For the patient with symptomatic fecal incontinence after 2 weeks in the postpartum period, refer to urogynecology or colorectal surgery. Early assessment helps to identify issues that require more immediate action (eg, revision of an obstetric laceration breakdown or repair of an occult sphincter laceration) affords an opportunity to educate patients about the pelvic floor, the role of Kegel exercises and biofeedback training or pelvic floor physical therapy, or both, if deemed appropriate helps educate patients about perianal skin care and dietary changes that affect stool consistency. The American College of Obstetricians and Gynecologists has developed a patient FAQ on Accidental Bowel Leakage provides reassurance to the patient Long-term follow-up is necessary to assess stability of results. The mode of delivery in subsequent pregnancies after OASIS has not been established. If fecal incontinence persists, it is reasonable to offer the patient a cesarean delivery, with a full discussion of the risks of abdominal surgery. Perineal Pain, Dyspareunia, and Sexual Function Background Perineal pain, dyspareunia, and low libido may occur after childbirth and, if persistent and not treated, may lead to long-term physical and psychological difficulties, including relationship discord. Prolonged postpartum perineal pain is common and has been reported in up to 10% of women 1 year after vaginal delivery. Scar tissue at the introitus from an episiotomy is a common cause. Dyspareunia is defined as genital pain that occurs just before, during, or after sexual intercourse. Physical factors, psychological factors, or both, may be involved. Postpartum dyspareunia has been reported in 50 60% of women 6 7 weeks after delivery, in 30% of women at 3 months after delivery, and in 17% of women 6 months after delivery. Risk factors that increase the risk of postpartum perineal pain and dyspareunia include infection, operative vaginal delivery, third- and fourth-degree laceration, wound separation of episiotomy or laceration repairs, pelvic organ prolapse, and breastfeeding. Vaginal atrophy secondary to the hypoestrogenic state during breastfeeding leads to inadequate lubrication and dyspareunia. Studies reveal no difference in the risk of dyspareunia in women with spontaneous perineal lacerations versus those women receiving episiotomies; however, avoidance or selective use of episiotomy decreases perineal trauma.
5 Postpartum Complications 5 A reduction in libido after childbirth is normal; however, many women are not aware of this. Contributors to reduced postpartum libido include hormonal alterations associated with breastfeeding, the adjustment and demands of a new infant, and fatigue. Studies have found that 50% of women at 3 months and 30% at 6 months after giving birth experience loss of libido. A high prevalence of postnatal sexual health issues occur during the postpartum period, and these are rarely discussed by women s health care providers at the postpartum visit. Postpartum Test and Screening Women rarely discuss sexual health issues unless health care providers ask them directly. Given the high prevalence of postpartum perineal trauma and subsequent dyspareunia, routine and direct inquiry by women s health care providers is warranted. Providing questionnaires before the office visit may be helpful; however, direct inquiries during the office visit is essential. Consider a pelvic examination in women with severe perineal pain, or dyspareunia, or both. Topical lidocaine (jelly or spray) may be used as an anesthetic for the following: Inspection of the perineum Careful and gentle digital vaginal and rectal examination if warranted. Use of vulvodynia and sensory mapping examination (use of moistened cotton swab to gently check for specific, localized areas of pain in the vulvar region). Management Considerations The management of perinea pain, dyspareunia, and sexual function depends on the cause. Education and reassurance of the patient can include the following: Inform the patient that it is normal for libido to decrease immediately after birth. Encourage the patient to communicate openly and honestly with her partner about reasons for low libido, including physiologic changes postpartum, fatigue, and lack of time. Suggest consultation with a certified therapist if or when the couple decides the issue necessitates the need to seek help or if a sexuality issue becomes problematic to the relationship. Consider ablation of granulation tissue. Use of a water-based lubricant for sexual relations. How pelvic floor physical therapy may benefit women with persistent perineal pain and dyspareunia at 3 months after giving birth, but data are scarce and conflicting. Transcutaneous electrical nerve stimulation (TENS) therapy and ultrasound therapy have been shown to decrease perineal pain and dyspareunia. However, consistent evidence is lacking, trials are of variable quality, and some studies lack adequate controls. Consider revision of perineoplasty as a treatment in women with persistent and severe perineal pain or dyspareunia unresponsive to physical therapy.
6 Postpartum Complications 6 Follow-up Goals Anticipatory counseling in the antepartum period is necessary to educate patients and set expectations. Because perineal laceration and dyspareunia are common, particularly in the primiparous woman, routine inquiry is warranted. Long-term follow-up and counseling are needed for persistent issues with dyspareunia and sexual health. References 1. American College of Obstetricians and Gynecologists. Accidental bowel leakage. ACOG FAQ 139. Washington, DC: American College of Obstetricians and Gynecologists; Available at: FAQs/Accidental-Bowel-Leakage. 2. American College of Obstetricians and Gynecologists. Pelvic support problems. ACOG FAQ 012. Washington, DC: American College of Obstetricians and Gynecologists; Available at: FAQs/Pelvic-Support-Problems. 3. American College of Obstetricians and Gynecologists. Urinary incontinence. ACOG FAQ 081. Washington, DC: American College of Obstetricians and Gynecologists; Available at: Urinary-Incontinence. Resources American College of Obstetricians and Gynecologists Clinical Guidance Prevention and management of obstetric lacerations at vaginal delivery. Practice Bulletin No American College of Obstetricians and Gynecologists. Obstet Gynecol 2018;132: e Provides evidence-based guidelines for the prevention, identification, and repair of obstetric lacerations and for episiotomy. Urinary incontinence in women. Practice Bulletin No American College of Obstetricians and Gynecologists. Obstet Gynecol 2015;126:e Reviews information on the current understanding of urinary incontinence in women and includes guidelines for diagnosis and management that are consistent with the best available scientific evidence. Health Care Provider Resources for Patient Care Burgio KL, Zyczynski H, Locher JL, Richter HE, Redden DT, Wright KC. Urinary incontinence in the 12-month postpartum period. Obstet Gynecol 2003;102: Describes prevalence and severity of urinary incontinence in the 12-month postpartum period and relates this incontinence to several potential risk factors including body mass index, smoking, oral contraceptives, breastfeeding, and pelvic floor muscle exercise. Coding See Coding for Postpartum Complications
Northwest Rehabilitation Associates, Inc.
 Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Health Patient Intake Form Name: Date: Please answer the following questions as honestly and thoroughly as you can. Your responses will help us better understand your condition and provide the best
Pelvic Support Problems
 AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
AP012, April 2010 ACOG publications are protected by copyright and all rights are reserved. ACOG publications may not be reproduced in any form or by any means without written permission from the copyright
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives
 Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
Pregnancy related pelvic floor dysfunction- suggested teaching presentation for Midwives 1 Aims of this self assessment competency To equip Midwives with the knowledge and skills to teach pelvic floor
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS
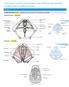 THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
THE PELVIC FLOOR, EPISIOTOMY AND PERINEAL REPAIR AND VAGINAL/RECTAL MEDICATIONS MID2010 LEARNING OBJECTIVE 1 - REVIEW THE ANATOMY OF THE PELVIC FLOOR Superficial layers cavernosus Deep layer Coccygeus
Women s and Men s Health Intake Form Comprehensive Physical Therapy Center
 Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Name: (Last, First) DOB: Date: Age: Referring Physician: Next Physician Appointment: Today s visit: What is the main reason you came to the office today? When did it start? What treatments have you had
Obstetric Anal Sphincter Injury. An update on best practices. Objectives
 Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Obstetric Anal Sphincter Injury An update on best practices Erin Crosby MD Assistant Professor Department of OB/Gyn Division of FPMRS 1 Objectives Describe the anatomy of the anal sphincter complex Discuss
Maternity Information Leaflet. Care of the Perineum (including Pelvic Floor Exercises) Version 2
 Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Maternity Information Leaflet Care of the Perineum (including Pelvic Floor Exercises) Version 2 Pelvic Floor Exercises The pelvic floor muscles are located between your legs, and run from your pubic bone
Obstetric Anal Sphincter Injury- A guideline. Mr David Sim Ms Patricia McStay. Dr Martina Hogan Dept./Division Only: YES-IMWH Directorate Only: NO
 CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
CLINICAL GUIDELINES ID TAG Title: Obstetric Anal Sphincter Injury- A guideline Author: Dr Foteini Verani Designation: Specialist Doctor Speciality / Division: Obstetrics-IMWH Directorate: Acute Services
The Perineal Clinic: - the management of women following OASI
 The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
The Perineal Clinic: - the management of women following OASI Miss Gillian Fowler Consultant Urogynaecologist MBChB, MD, MRCOG Liverpool Women s Hospital. Margie Polden University Memorial of Liverpool
Appendix B Protocol for management of obstetric anal sphincter injury THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS
 Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Appendix B Protocol for management of obstetric anal sphincter injury Document Type: THE MANAGEMENT OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS PURPOSE & SCOPE To provide a guideline that will assist in
Postoperative Care for Pelvic Fistulae. Peter Jeppson, MD October 3, 2017
 Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Postoperative Care for Pelvic Fistulae Peter Jeppson, MD October 3, 2017 No Disclosures Rational for Postoperative Care Intraoperative injury may be managed by: Identification Closure Continuous post-operative
Perineal Tears. Obstetrics & Gynaecology Women & Children s Group
 Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
Perineal Tears Obstetrics & Gynaecology Women & Children s Group This leaflet has been designed to give you important information about your condition / procedure, and to answer some common queries that
LAPAROSCOPIC REPAIR OF PELVIC FLOOR
 LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
LAPAROSCOPIC REPAIR OF PELVIC FLOOR Dr. R. K. Mishra Elements comprising the Pelvis Bones Ilium, ischium and pubis fusion Ligaments Muscles Obturator internis muscle Arcus tendineus levator ani or white
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION
 OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
OBSTETRICALLY-CAUSED ANAL SPHINCTER INJURY PREDICTION, MANAGEMENT, PREVENTION COLM O HERLIHY, MD Professor and Chair University College Dublin Department of Obstetrics and Gynaecology National Maternity
Outpatient Rehabilitation Services
 Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
2/5/2016. Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach
 Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
Evolving Surgical Treatment Approaches for Fecal Incontinence in Women: An Evidence and Cased-Based Approach Holly E Richter, PhD, MD, FACOG, FACS J Marion Sims Professor Obstetrics and Gynecology Professor
from Bowel Control Problems twitter.com/voicesforpfd
 BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
BREAK FREE from Bowel Control Problems POP Quiz THE NUMBER OF PEOPLE IN THE UNITED STATES WITH BOWEL CONTROL PROBLEMS: A. 6 million B. 12 million C. 18 million BOWEL CONTROL PROBLEMS Nearly 18 million
Impact of Delivery Types on Women s Postpartum Sexual Health
 Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Reproduction & Contraception (2003) 14 (4):237~242 Impact of Delivery Types on Women s Postpartum Sexual Health Huan-ying WANG 1, Xiao-yang XU 2, Zhen-wei YAO 1, Qin ZHOU 1 Key words: postpartum; sexual
Provenance Rehabilitation Pelvic Intake Form
 Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or???
 Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Doctor s assessment and evaluation of the pelvic floor in antenatal and postpartum women: routine or??? Dr Barry O Reilly Head of department of Urogynaecology Cork University Maternity Hospital Ireland
Anal Sphincter Injuries: Acute Management
 Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Anal Sphincter Injuries: Acute Management Dr Stephen Jeffery Urogynaecology Consultant Department of Obstetrics & Gynaecology Groote Schuur Hospital Colorectal Surgeons Gynaecologists Gynaecologists Colorectal
Vincent Letouzey, MD, PhD
 How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
How to protect the perineum and prevent obstetric perineal trauma Standards of OASIS diagnosis: Primary (clinical) and Secondary (ultrasound) Vincent Letouzey, MD, PhD Obst/Gyne Dept Nîmes University Hospital
Patient Advice for Third & Fourth Degree Tears
 Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital
 Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
Dr Anne Sneddon Director of Obstetrics and Gynaecology Lecturer, ANU Medical School The Canberra Hospital Capital city of Australia Population 350,000 but surrounding region of 500,000 Seat of government
2/25/2013. Speaker Disclosure. Learning Objectives. Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth
 Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Ob/Gyn Conference Series: Urinary and Fecal Incontinence After Vaginal Childbirth Jaime Sepulveda-Toro MD FACS FACOG Female Pelvic Medicine and Reconstructive Pelvic Surgery South Miami Hospital Speaker
Name: Date: DOB: Full Address: Phone: Home: Cell: Occupation: Emerg. contact and phone: Relationship to pt.
 Client Registration Name: Date: DOB: Email: Full Address: Phone: Home: Cell: Occupation: Emerg. contact and phone: Relationship to pt. How did you hear about ALIGN? ALIGN Integration Movement does not
Client Registration Name: Date: DOB: Email: Full Address: Phone: Home: Cell: Occupation: Emerg. contact and phone: Relationship to pt. How did you hear about ALIGN? ALIGN Integration Movement does not
Third & Fourth Degree Tears guideline (GL926)
 Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Third & Fourth Degree Tears guideline (GL926) Approval Approval Group Job Title, Chair of Committee Date Maternity & Children s Services Clinical Governance Committee Chair, Maternity Clinical Governance
Repair of vaginal tears and episiotomy guidelines
 Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Repair of vaginal tears and episiotomy guidelines Purpose These guidelines assist practitioners in the repair of vaginal and perineal tears including the reasons for, and the techniques of performing an
Childbirth Trauma & Its Complications 23/ Mr Stergios K. Doumouchtsis
 Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Mr Stergios K. Doumouchtsis Consultant Obstetrician Gynaecologist & Urogynaecologist Childbirth Trauma & Its Complications Over eighty per cent of women sustain some degree of perineal trauma during childbirth.
Pelvic floor exercises for women. Information for patients Continence Service
 Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Pelvic floor exercises for women Information for patients Continence Service page 2 of 8 Why do I need to do pelvic floor exercises? Many women experience pelvic floor problems at some time during their
Guidelines on the Management of Complications related to Female Genital Mutilation
 Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
Guidelines on the Management of Complications related to Female Genital Mutilation Scoping Survey Instructions The following is a list of 33 potential questions which could guide the evidence retrieval
The Pelvic Floor: Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology
 The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
The Pelvic Floor: What She Can Expect After Expecting (and Delivering!) Susan Barr, MD Assistant Professor Saint Louis University Division of Urogynecology Objectives Understand risk factors and treatment
Pelvic Floor Muscle Exercises
 INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
INFORMATION FOR WOMEN OF ALL AGES Pelvic Floor Muscle Exercises How to exercise and strengthen your pelvic floor muscles ASSOCIATION OF CHARTERED PHYSIOTHERAPISTS IN WOMEN S HEALTH This leaflet is supported
Royal College of Obstetricians and Gynaecologists
 Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Royal College of Obstetricians and Gynaecologists Consent Advice No. 9 June 2010 REPAIR OF THIRD- AND FOURTH-DEGREE PERINEAL TEARS FOLLOWING CHILDBIRTH This is the first edition of this guidance. This
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Rectal Incontinence After Childbirth and Surgery Webcast November 24, 2009 Anne-Marie Boller, M.D. Introduction
 Rectal Incontinence After Childbirth and Surgery Webcast November 24, 2009 Anne-Marie Boller, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern
Rectal Incontinence After Childbirth and Surgery Webcast November 24, 2009 Anne-Marie Boller, M.D. Please remember the opinions expressed on Patient Power are not necessarily the views of Northwestern
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
In the August 2016 issue of OBG Management,
 GYN coding changes to note for your maximized reimbursement Revised ICD-10 gynecologic diagnostic codes go into effect October 1. Here is a look at the added, expanded, and revised codes you will need
GYN coding changes to note for your maximized reimbursement Revised ICD-10 gynecologic diagnostic codes go into effect October 1. Here is a look at the added, expanded, and revised codes you will need
Focus on Post-Partum Incontinence
 Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
Focus on Post-Partum Incontinence A one day intensive course for Nurses, Midwives and Physiotherapists Old Main Building Law Faculty Stellenbosch 24 January 2013 9h00-17h00 Sponsored by the International
PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR
 PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR LIFE FIT CENTER 2.22.18 DR. SHERINE AUBERT, PT, DPT, PRPC OVERVIEW What What are the functions of the pelvic floor muscles? Who Who goes to pelvic
PELVIC FLOOR WORKSHOP- LEARN AND GET TO KNOW YOUR FLOOR LIFE FIT CENTER 2.22.18 DR. SHERINE AUBERT, PT, DPT, PRPC OVERVIEW What What are the functions of the pelvic floor muscles? Who Who goes to pelvic
Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence
 Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Cronicon OPEN ACCESS GYNAECOLOGY Review Article Pelvic Floor Dysfunction, Body Excreta Incontinence and Continence Abdel Karim M El Hemaly 1 * and Laila ASE Mousa 1 1 Professor of Obstetrics and gynaecology,
Care of your Perineum following 3 rd and 4 th degree tears
 Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Maternity Services Care of your Perineum following 3 rd and 4 th degree tears Introduction This leaflet aims to give you information about the repair and aftercare of the third or fourth degree tear you
Accidental Bowel Leakage (Fecal Incontinence)
 Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Accidental Bowel Leakage (Fecal Incontinence) What is Accidental Bowel Leakage (ABL)? Accidental bowel leakage is the inability to control solid or liquid stool. This is the inability to control gas and
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Treatments for Fecal Incontinence A Review of the Research for Adults
 Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Treatments for Fecal Incontinence A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* said you or your loved one
Faecal Incontinence: Assessment and Management
 Mrs PK; 56 yrs; Married; 2 children Faecal Incontinence: Assessment and Management Professor Marc A Gladman MBBS DFFP PhD MRCOG FRCS (UK) FRACS Professor of Colorectal Surgery >10 years of incontinence
Mrs PK; 56 yrs; Married; 2 children Faecal Incontinence: Assessment and Management Professor Marc A Gladman MBBS DFFP PhD MRCOG FRCS (UK) FRACS Professor of Colorectal Surgery >10 years of incontinence
The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place.
 The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place. Think of it as the hammock of muscle that holds up your uterus, vagina, bladder, small intestine,
The pelvic floor is a system of muscles, ligaments, and tissues that keep your pelvic organs firmly in place. Think of it as the hammock of muscle that holds up your uterus, vagina, bladder, small intestine,
Pelvic Floor Therapy for the Oncology Patient
 Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Therapy for the Oncology Patient CARINA SIRACUSA, PT, DPT, WCS OHIOHEALTH PELVIC FLOOR PHYSICAL THERAPIST ONCOLOGY REHABILITATION PROGRAM COORDINATOR What does a pelvic floor therapist treat? Muscles Muscles
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Stop Coping. Start Living. Talk to your doctor about pelvic organ prolapse and sacrocolpopexy
 Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Stop Coping. Start Living Talk to your doctor about pelvic organ prolapse and sacrocolpopexy Did you know? One in three women will suffer from a pelvic health condition in her lifetime. Four of the most
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Pelvic Floor Dysfunction (PFD) Interdisciplinary Treatment and Referral Consideration for Physician Assistants
 Pelvic Floor Dysfunction (PFD) Interdisciplinary Treatment and Referral Consideration for Physician Assistants Gerry Keenan, MMS, PA C Tammy Roehling, PT, DPT Learner Objectives 1. Recreate the pelvic
Pelvic Floor Dysfunction (PFD) Interdisciplinary Treatment and Referral Consideration for Physician Assistants Gerry Keenan, MMS, PA C Tammy Roehling, PT, DPT Learner Objectives 1. Recreate the pelvic
Pelvic Physio 101. OMA Sports Med 2019 Conference. Nelly Faghani PT. January 25,
 Pelvic Physio 101 OMA Sports Med 2019 Conference January 25, 2019 Nelly Faghani PT www.pelvichealthsolutions.ca CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure
Pelvic Physio 101 OMA Sports Med 2019 Conference January 25, 2019 Nelly Faghani PT www.pelvichealthsolutions.ca CFPC CoI Templates: Slide 1 used in Faculty presentation only. Faculty/Presenter Disclosure
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF)
 Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
Approach to the Repair of Chronic Perineal Lacerations and Rectovaginal Fistula (RVF) Blair B. Washington MD, MHA Urogynecology & Reconstructive Pelvic Surgery Virginia Mason Medical Center Disclosures
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
5 DIAGNOSIS. History taking
 5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
5 DIAGNOSIS All of the photographs in Chapter 4 were taken in theatre before operation. This chapter deals with how one can recognize the type of fistula by history taking and examination. (Note that the
Look Good Feel Good. after pregnancy. Physiotherapy advice and exercises for new mums
 Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Look Good Feel Good after pregnancy Physiotherapy advice and exercises for new mums How to exercise after pregnancy with physiotherapy Bowel Tail Bone Uterus Bladder Pubic Bone Pelvic Floor Muscles Urethra
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital
 Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Moneli Golara Consultant Obstetrician and Gynaecologist Royal Free NHS Trust Barnet Hospital Pelvic Organ Prolapse (POP)- herniation of pelvic organs into vaginal walls Common Huge impact on daily activities
Gynecology Dr. Sallama Lecture 3 Genital Prolapse
 Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Gynecology Dr. Sallama Lecture 3 Genital Prolapse Genital(utero-vaginal )prolapse is extremely common, with an estimated 11% of women undergoing at least one operation for this condition. Definition: A
Fecal Incontinence. What is fecal incontinence?
 Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Scan for mobile link. Fecal Incontinence Fecal incontinence is the inability to control the passage of waste material from the body. It may be associated with constipation or diarrhea and typically occurs
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Duc M. Vo, MD, FACS Northwest Surgical Specialists
 Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Duc M. Vo, MD, FACS Northwest Surgical Specialists Disclosures none Outline Definition Etiologies Exam findings Additional testing Medical management Surgical options What is fecal incontinence? Recurrent
Robotic Ventral Rectopexy
 Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Robotic Ventral Rectopexy What is a robotic ventral rectopexy? The term rectopexy refers to an operation in which the rectum (the part of the bowel nearest the anus) is put back into its normal position
Pelvic floor muscle exercises (long)
 Pelvic floor muscle exercises (long) This leaflet aims to give an overview of pelvic floor muscles, their function, how they can be exercised and why this is so important. What are pelvic floor muscles
Pelvic floor muscle exercises (long) This leaflet aims to give an overview of pelvic floor muscles, their function, how they can be exercised and why this is so important. What are pelvic floor muscles
Management of Incontinence and Pelvic Floor Disorders
 Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Management of Incontinence and Pelvic Floor Disorders Dear Colleague: Multiple studies demonstrate that pelvic floor disorders urinary or fecal leakage occurring at an inappropriate time or place has a
Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study
 ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
ORIGINAL RESEARCH Anal Incontinence After Vaginal Delivery: A Five-Year Prospective Cohort Study Johan Pollack, MD, Johan Nordenstam, MD, Sophia Brismar, MD, Annika Lopez, MD, PhD, Daniel Altman, MD, and
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Pelvic organ prolapse. Information for patients Continence Service
 Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic organ prolapse Information for patients Continence Service What is a pelvic organ prolapse? A pelvic organ prolapse occurs when the uterus (womb), vagina, bladder or bowel slips out of place, resulting
Pelvic Organ Prolapse. Natural Solutions
 Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Pelvic Organ Prolapse Natural Solutions Bringing your body back to its natural state There is a very common problem affecting millions of women. Many women are too embarrassed to talk to their physicians
Patient History. Name Age Date. 2. When did your problem first begin?
 Patient History Name Age Date 1. Describe the problem that brought you here? 2. When did your problem first begin? 3. Was your first episode of the problem related to a specific incident/injury? Yes/No
Patient History Name Age Date 1. Describe the problem that brought you here? 2. When did your problem first begin? 3. Was your first episode of the problem related to a specific incident/injury? Yes/No
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Index Note: Page numbers of article titles are in boldface type. A Abdominal mesh background of, 84 85 Age as factor in PFDs, 8 Anal plugs in FI management in women, 107 Anterior compartment native tissue
Pelvic floor weakness
 Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
FEMALE INTAKE INFORMED CONSENT FOR ASSESSMENT OF PELVIC FLOOR DYSFUNCTIONS
 Date: FEMALE INTAKE INFORMED CONSENT FOR ASSESSMENT OF PELVIC FLOOR DYSFUNCTIONS Pelvic floor dysfunctions include pelvic pain syndromes, urinary incontinence, fecal incontinence, dyspareunia or pain with
Date: FEMALE INTAKE INFORMED CONSENT FOR ASSESSMENT OF PELVIC FLOOR DYSFUNCTIONS Pelvic floor dysfunctions include pelvic pain syndromes, urinary incontinence, fecal incontinence, dyspareunia or pain with
Pelvic Prolapse. A Patient Guide to Pelvic Floor Reconstruction
 Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
Pelvic Prolapse A Patient Guide to Pelvic Floor Reconstruction Pelvic Prolapse When an organ becomes displaced, or slips down in the body, it is referred to as a prolapse. Your physician has diagnosed
INCONTINENCE. Continence and Pelvic Floor Rehabilitation TYPES OF INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE STRESS INCONTINENCE 11/08/2015
 INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
INCONTINENCE Continence and Pelvic Floor Rehabilitation Dr Irmina Nahon PhD Pelvic Floor Physiotherapist www.nahonpfed.com.au Defined as the accidental and inappropriate passage of urine or faeces (ICI
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes?
 Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Do Unsutured Second-Degree Perineal Lacerations Affect Postpartum Functional Outcomes? Lawrence M. Leeman, MD, Rebecca G. Rogers, MD, Betsy Greulich, CNM, and Leah L. Albers, DrPH Background: To compare
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem
 Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Eur. J. Obstet. Gynecol. Reprod. Biol., 27 (1988) 27-32 Elsevier 27 EJO 00556 Long-term ailments due to anal sphincter rupture caused by delivery - a hidden problem Knut Haadem, Sten Ohrlander and G6ran
Personal Background. Brenau Graduate. Practicing OT for five years Specializing in pelvic floor for three years
 Personal Background Brenau Graduate Practicing OT for five years Specializing in pelvic floor for three years Learning Objectives Identify male and female pelvic floor and pelvic girdle structures List
Personal Background Brenau Graduate Practicing OT for five years Specializing in pelvic floor for three years Learning Objectives Identify male and female pelvic floor and pelvic girdle structures List
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
period, cesarean delivery is thought to protect against anal incontinence, 3 albeit incompletely. In this study, we investigated anal incontinence
 Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Obstetrical anal sphincter laceration and anal incontinence 5-10 years after childbirth Emily C. Evers, MPH; Joan L. Blomquist, MD; Kelly C. McDermott, BS; Victoria L. Handa, MD, MHS OBJECTIVE: The purpose
Uterine prolapse & Fistulas. Raja Nursing Instructor RN, DCHN, Post RN. BSc.N
 Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
Uterine prolapse & Fistulas Raja Nursing Instructor RN, DCHN, Post RN. BSc.N 31/03/2016 Objectives 1. Review the anatomy & physiology of female reproductive system 2. Discuss the causes, pathophysiology,
Pelvic Floor Exercises
 Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Exercises Physiotherapy Department Patient information leaflet Up to a third of women experience a problem with their pelvic floor muscles at some point during their life. The muscles can
Pelvic Floor Muscle Exercises and Advice for Men
 Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Pelvic Floor Muscle Exercises and Advice for Men (formerly ACPWH) Useful resources Websites Pelvic Obstetric & Gynaecological Physiotherapy - pogp.csp.org.uk Bladder and Bowel Foundation - www.bladderandbowelfoundation.org
Latest Treatments for a Leaky Bladder None
 Latest Treatments for a Leaky Bladder None Financial Disclosures Jeremiah McNamara, MD, OBGYN Boulder Women s Care 303-500-1947 Boulder Women s Care Agenda: Prolapse & Urinary Incontinence The Pelvic Floor
Latest Treatments for a Leaky Bladder None Financial Disclosures Jeremiah McNamara, MD, OBGYN Boulder Women s Care 303-500-1947 Boulder Women s Care Agenda: Prolapse & Urinary Incontinence The Pelvic Floor
Among parous women, cesarean birth reduces the
 Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
Pelvic Floor Disorders After Vaginal Birth Effect of Episiotomy, Perineal Laceration, and Operative Birth Victoria L. Handa, MD, MHS, Joan L. Blomquist, MD, Kelly C. McDermott, BS, Sarah Friedman, MD,
SUTURING AN EPISIOTOMY/GENITAL LACERATION
 WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
WOMEN AND NEWBORN HEALTH SERVICE CLINICAL GUIDELINES SECTION B : GUIDELINES RELEVANT TO OBSTETRICS AND MIDWIFERY 5 INTRAPARTUM CARE 5.15 PERINEAL REPAIR Authorised by: OGCCU 5.15.1 SUTURING AN EPISIOTOMY/GENITAL
Pelvic Floor Muscle exercises and Bladder advice
 n The Leeds Teaching Hospitals NHS Trust Pelvic Floor Muscle exercises and Bladder advice Information for patients Leeds Centre for Women s Health This leaflet aims to explain about your pelvic floor muscles,
n The Leeds Teaching Hospitals NHS Trust Pelvic Floor Muscle exercises and Bladder advice Information for patients Leeds Centre for Women s Health This leaflet aims to explain about your pelvic floor muscles,
Not a Laughing Matter
 Not a Laughing Matter How to Incorporate Pelvic Health Rehabilitation into your STAR program Nancy Corvigno MSPT PRPC Certified Star Clinician STAR Program at Griffin Hospital Survivorship Training and
Not a Laughing Matter How to Incorporate Pelvic Health Rehabilitation into your STAR program Nancy Corvigno MSPT PRPC Certified Star Clinician STAR Program at Griffin Hospital Survivorship Training and
Guide to strengthening the pelvic floor muscles
 Exercise Cones Pelvic Exercise Made Easy Exercise Cones Pelvic Exercise Made Easy This system is clinically proven to strengthen the pelvic floor muscle to help with the control and prevention of stress
Exercise Cones Pelvic Exercise Made Easy Exercise Cones Pelvic Exercise Made Easy This system is clinically proven to strengthen the pelvic floor muscle to help with the control and prevention of stress
Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship?
 DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
DOI 10.1007/s00192-007-0431-8 ORIGINAL ARTICLE Urinary incontinence after obstetric anal sphincter injuries (OASIS) is there a relationship? Inka Scheer & Vasanth Andrews & Ranee Thakar & Abdul H. Sultan
Northeast Ohio Urogynecology Patient History Intake Form. Last Name First Name Age. Date of Birth Race Referring Physician.
 Northeast Ohio Urogynecology Patient History Intake Form Last Name _First Name Age_ Date of Birth Race Referring Physician Reason for Visit: _ Allergies: Preferred Lab (circle): QUEST LABCARE PLUS LABCORP
Northeast Ohio Urogynecology Patient History Intake Form Last Name _First Name Age_ Date of Birth Race Referring Physician Reason for Visit: _ Allergies: Preferred Lab (circle): QUEST LABCARE PLUS LABCORP
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER
 CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
CHERRY BAKER AND TRACEY GJERTSEN BSC MCSP HCPC INTRODUCTION TO DIAMOND TRAINING REHAB AND PERFORMANCE FOR PELVIC POWER What is it? Where is it? Breathing Graded relaxation Incontinence Stress Incontinence
for a review under the Accident Compensation Act
 FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
FairWay Resolution Limited Tā te Hinengaro Tōkeke Whakatau Review numbers: Application by for a review under the Accident Compensation Act Held at Date of hearing 2 November 2016, adjourned part-heard;
Introduction to GYN Specialties
 Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
Outline Introduction to GYN Specialties Gynecologic Oncology* Female Pelvic Medicine and Reconstructive Surgery* Reproductive Endocrinology and Infertility* Pediatric and Adolescent Gynecology** Family
Treating your prolapse
 Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Treating your prolapse This leaflet explains what a prolapse is, and how it can be treated and managed. If you have any questions or concerns, please speak to a doctor or nurse caring for you. What is
Information on Physical Therapy For Urogynecologic Problems
 Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
Information on Physical Therapy For Urogynecologic Problems You have scheduled an appointment for evaluation and treatment of a urogynecologic problem. Following, you will find a pelvic floor questionnaire
