Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
|
|
|
- Allison Peters
- 5 years ago
- Views:
Transcription
1 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao, BS, 1 Andres L. Maldonado-Naranjo, MD, 1 Hubert H. Fernandez, MD, 1 and Andre G. Machado, MD, PhD 1 1 Center for Neurological Restoration, Neurological Institute, Cleveland Clinic, Cleveland, Ohio; and 2 Postgraduate Program in Medicine: Surgical Sciences, Universidade Federal do Rio Grande do Sul (UFRGS), Porto Alegre, RS, Brazil OBJECTIVE The number of patients who benefit from deep brain stimulation (DBS) for Parkinson s disease (PD) has increased significantly since the therapy was first approved by the FDA. Suboptimal outcomes, infection, or device failure are risks of the procedure and may require lead removal or repositioning. The authors present here the results of their series of revision and reimplantation surgeries. METHODS The data were reviewed from all DBS intracranial lead removals, revisions, or reimplantations among patients with PD over a 6-year period at the authors institution. The indications for these procedures were categorized as infection, suboptimal outcome, and device failure. Motor outcomes as well as lead location were analyzed before removal and after reimplant or revision. RESULTS The final sample included 25 patients who underwent 34 lead removals. Thirteen patients had 18 leads reimplanted after removal. There was significant improvement in the motor scores after revision surgery among the patients who had the lead revised for a suboptimal outcome (p = 0.025). The mean vector distance of the new lead location compared to the previous location was 2.16 mm (SD 1.17), measured on an axial plane 3.5 mm below the anterior commissure posterior commissure line. When these leads were analyzed by subgroup, the mean distance was 1.67 mm (SD 0.83 mm) among patients treated for infection and 2.73 mm (SD 1.31 mm) for those with suboptimal outcomes. CONCLUSIONS Patients with PD who undergo reimplantation surgery due to suboptimal outcome may experience significant benefits. Reimplantation after surgical infection seems feasible and overall safe. KEYWORDS complication; deep brain stimulation; Parkinson s disease; lead placement; replacement; functional neurosurgery Deep brain stimulation (DBS) is an established surgical treatment for Parkinson s disease (PD), essential tremor, and dystonia. 2,4,8,10 Patient selection, target choice, and surgical accuracy are the foundation for a successful DBS outcome. However, in some cases, revision or reimplantation is needed due to limited benefits, device failure, or infection involving the hardware. There are relatively few published series describing the outcomes after lead revision or reimplantation. 5,15 Thus, little is known about the potential risks and benefits of DBS revision surgery. 16 In this study, we present our outcomes after revision or reimplantation surgery in patients with infections, device failure, or unsatisfactory results after DBS surgery for PD. As for any surgical procedure, revision surgery carries a greater complexity and thus outcomes may differ from index procedures in both safety and efficacy. Methods After institutional review board approval, we retrospectively reviewed data extracted from the electronic medical record for patients with documented intracranial DBS lead removal or revision at our institution between 2010 and This study was exempted from obtaining individual informed consent due to the nature of the study, which consisted of a retrospective review of medical records and images. Demographic data, indication for removal or revision, procedure time, outcomes, and lead location for reimplants were analyzed for all patients who underwent ABBREVIATIONS AC-PC = anterior commissure posterior commissure; DBS = deep brain stimulation; GPi = globus pallidus internus; MDS-UPDRS III = Movement Disorders Society Unified Parkinson Disease Rating Scale Part III (motor subscale); MER = microelectrode recording; PD = Parkinson s disease; STN = subthalamic nucleus. SUBMITTED July 7, ACCEPTED January 10, INCLUDE WHEN CITING Published online June 22, 2018; DOI: / JNS AANS 2018, except where prohibited by US copyright law J Neurosurg June 22,
2 FIG. 1. Summary of all surgeries in this series. Subop = suboptimal. DBS for PD. The Movement Disorders Society Unified Parkinson Disease Rating Scale Part III (motor subscale) (MDS-UPDRS III) scores were compared prior to and 6 months after reimplantation. Patients with UPDRS III scores had that score converted to MDS-UPDRS III. 7 The indications for removal or revision were categorized as follows: 1) infection; 2) suboptimal outcome; or 3) device failure. Infection was defined as clinically evident purulent discharge, erythema, or tenderness around any component of the hardware that led to the removal of the intracranial lead. In addition, hardware exposure even in the absence of inflammatory signs was also classified under infection. Suboptimal outcomes included documented adverse effects at low-amplitude thresholds and/or limited benefits despite repeat programming. Finally, device failure was defined as a malfunction of the device that prompted revision surgery. Examples under this category include high impedances in the intracranial lead and lead fractures. The iplan 3.0 planning software (BrainLab AG) was used to calculate the distance between the lead location before and after surgical revision based on the respective imaging series among the patients who had subthalamic nucleus (STN) DBS. Preoperative (i.e., prerevision or removal) and postoperative CT scans or T1-weighted MR images from each lead revision or reimplantation procedure were fused and the images were reformatted along the anterior commissure posterior commissure (AC-PC) plane. To evaluate lead shifts within the STN area, virtual targets were created for the center of the lead at 3.5 mm below the AC-PC line before and after surgery. We chose this measurement to better evaluate the lead shifts in the medial-lateral and anterior-posterior axis. The distance from the center of the electrode to the midcommissural point was then extrapolated from the virtual target in the initial implant (X1, Y1) and after the revision surgery (X2, Y2). For better spatial visualization, the lead locations pre- and postrevision or reimplantation were plotted in a schematic drawing, adapted from the Schaltenbrand and Wahren atlas, 17 representing the axial slice at 3.5 mm below the AC-PC line in that atlas. The vector distance between the initial and revised leads in the axial plan was calculated using the following equation: Vector distance =. Surgical Procedure Patient selection criteria for DBS implantation as well as surgical techniques have been published elsewhere by our group For lead reimplant surgery due to infection, it is our routine to obtain an imaging scan on all patients prior to lead removal because this may guide the planning for reimplantation once the infection has been successfully treated. Lead revision surgery due to a suboptimal outcome or lead failures were completed in stages: lead removal followed by reimplantation. In most patients, reimplanted leads were guided by awake electrophysiological techniques. For lead failures, we attempted to insert the lead using the same target where possible. Statistical Analysis Statistical analysis was performed using IBM SPSS Statistics software, version 20.0 (IBM Corp.). Descriptive statistics was used to describe our cohort. Paired t-tests were used to analyze the outcomes after revision surgeries. Patients who did not have pre- or postrevision scores were not included in this analysis. Results In total, 34 leads were removed from 25 patients (19 males and 6 females) with PD between 2010 and The mean age at removal was years (SD 9.97 years). As shown in Fig. 1, 23 leads were removed from 17 patients after an infection was diagnosed, 9 leads were removed from 7 patients who had suboptimal outcomes, and 2 leads were removed from 2 patients after a device failure (a total of 26 reasons for removal in 25 patients). As a DBS referral center, we treated 6 patients with 9 leads (26.4%) that had been initially implanted at another hospital. Among all patients who had a lead removed, 13 underwent another surgery for reimplantation (12 males and 1 female). The mean age at reimplantation was years (SD 9.59 years). The average time between removal and reimplantation surgery across all patients was days (SD days). Among infected patients the mean time to reimplantation was days (SD days), and among patients with suboptimal outcomes the mean time to reimplantation was days (SD 6.23 days). The mean procedure time for hardware removal surgery was minutes (SD minutes) and for reimplantation surgery it was minutes (SD minutes). Lead Removal Without Replacement Twelve patients who had the lead removed did not undergo reimplantation. All patients who underwent removal without reimplantation had the lead removed for an infection. The time between implant and removal, target nucleus, reason for lead removal, and why these patients elected not to undergo reimplantation are summarized in Table 1. The rationale for not reimplanting the lead included cognitive decline following the original surgery, patient choice, comorbidities, and the threat of hardware erosion in patients with impaired skin integrity at the operative site. 2 J Neurosurg June 22, 2018
3 TABLE 1. Removal surgeries without revision of DBS leads in patients with PD Case No. Target Laterality Reason for Removal Time From Implant to Removal (mos) Reason for Not Revising 1 STN Bilat Infection 1 Reduced skin integrity 2 STN Rt Infection 119 Cognitive impairment 3 STN Rt Infection 63 Waiting for reimplant 4 STN Rt Infection 9 Waiting for reimplant 5 STN Lt Infection 95 Patient choice 6 STN Bilat Infection 7 Patient choice 7 STN Lt Infection 27 Poor outcome before complication 8 STN Bilat Infection 9 Cognitive impairment 9 STN Rt Infection 168 Comorbidities (diabetes) 10 GPi Bilat Infection 2 Waiting for reimplant 11 STN Lt Infection 134 Reduced skin integrity 12 STN Lt Infection 112 Cognitive impairment Removal and Reimplantation Thirteen of 25 patients (52%) elected to have the lead reimplanted after removal. Seven leads were replaced after an infection, 9 leads were replaced because of limited benefit or side effects at low threshold, and 2 leads were replaced due to device failures. Two patients had bilateral leads revised for suboptimal outcomes. Both patients had undergone initial surgery at another hospital and bilateral revision after analyzing outcome and lead location. One patient had bilateral lead revision in a single procedure, and the other had a staged procedure. In this patient, the outcome was included after both sides were revised. Taking into consideration the entire sample size, we did not find a significant improvement in the MDS-UPDRS III score after revision surgery (34.79 [SD 17.79] versus [SD 17.54]; p = 0.054). However, when considering only the patients with limited benefits, a greater improvement in the MDS-UPDRS scores was noted (37.88 [SD 8.78] vs [SD 13.09]; p = 0.025). When considering only the patients who had the device removed and reimplanted after infection, we did not find significant differences when comparing outcomes before removal and after reimplantation (p = 0.742). Table 2 summarizes the outcome data for each lead revision. The mean total months of follow-up among the patients with reimplanted leads was months (SD months). During the follow-up period, two complications related to the revision were found: one patient who underwent a reimplantation 113 days after removal due to TABLE 2. Summarized outcomes after DBS lead revision in patients with PD Case No. Lead Side Target Reason for Revision Unilat Scores Pre-Removal Unilat Scores Post-Revision % Improvement 1 1 Lt STN SO poor tremor control % 2 2 Lt STN SO low capsular thresholds % 2 3 Rt STN SO motor fluctuations % 3 4 Rt STN SO poor tremor control % 4 5 Lt STN SO tremor &/or stiffness % 4 6 Rt STN Infection % 5 7 Lt STN SO tremor &/or rigidity NA Rt GPi SO poor motor outcome % 6 9 Lt GPi SO poor motor outcome % 7 10 Lt STN* SO lead fracture % 8 11 Lt STN* SO low capsular thresholds % 9 12 Rt STN Infection NA Lt STN Infection NA Lt STN Infection % Rt STN Infection 26 NA Lt STN SO &/or lead fracture 53 NA Rt STN Infection % Lt STN Infection % NA = not available; SO = suboptimal outcome. * In these patients the target was changed from STN to GPi. J Neurosurg June 22,
4 TABLE 3. Position of DBS leads before and after revision Case No. Lead Initial Target Final Target Side Preop Electrode at Z = 3.5 mm Postop Electrode Location at Z = 3.5 mm Distance X Y X Y (mm) 1 1 STN STN Lt STN STN Lt STN STN Rt STN STN Rt STN STN Lt STN STN Rt STN STN Lt GPi GPi Rt Initial & final target was GPi 6 9 GPi GPi Lt Initial & final target was GPi 7 10 STN GPi Lt Changed to GPi 8 11 STN GPi Lt Changed to GPi 9 12 STN STN Rt STN STN Lt STN STN Lt STN STN Rt STN VIM Lt Changed to VIM STN STN Rt STN STN Lt VIM = ventral intermediate nucleus. infection presented with poor healing and scabbing of the wound. This patient underwent 14 days of oral antibiotic therapy and the wound healed well, with no further signs of infections. The second patient had a pulmonary embolism on the first postoperative day. Heparin was started and on the third postoperative day he neurologically deteriorated. The head CT showed a left thalamic hemorrhage near the tip of the lead (< 5 ml). The patient later died at another facility, most likely due to medical or cardiopulmonary complications. Of 9 patients with lead revision procedures performed for suboptimal outcome, 3 had initially undergone implantation at our institution. Two patients had suboptimal outcomes associated with limited intraoperative physiological data, suggesting that intraoperative mapping remains an important technique for achieving consistent outcomes. One patient had undergone the procedure under anesthesia guided only by imaging, without intraoperative physiology, whereas the second patient underwent limited microelectrode recording (MER) mapping during the index surgery because of a high intraoperative blood pressure that did not rapidly respond to antihypertensive medications. A third patient was initially implanted with an STN lead but, because of stimulation-induced dyskinesias despite reprogramming, the decision was made to move the lead to the globus pallidus internus (GPi). Electrode Location The mean vector distance between the center of the STN leads before and after revision was 2.16 mm (SD 1.17 mm) at 3.5 mm below the AC-PC line. When analyzing by subgroup, the mean change distance was 1.67 mm (SD 0.83 mm) among patients treated for infection, and 2.73 mm (SD 1.31 mm) for those with suboptimal outcomes. Table 3 and Fig. 2 summarize the data. Discussion DBS systems, excluding the pulse generators, are intended for lifelong use. However, lead removal or revision is sometimes necessary. Such revisions may be more common at high-volume centers in which patients are seen for second opinions and in which surgery is performed in patients with higher risk or under experimental protocols. 9,14 Very few centers so far have reported their indications and outcomes related to revision surgery. 5,6,15 Table 4 is a summary of the series published thus far. The existing reports in the literature are generally favorable. Ellis et al. showed an improvement of 24.4% in off-medication/on-stimulation scores in a cohort of 11 patients with PD whose leads were reimplanted because of a suboptimal clinical benefit. 5 Anheim et al. demonstrated in a prospective series of 7 patients with poor results after STN stimulation that these patients can benefit from reimplantation; all but 1 patient improved in UPDRS motor scores 1 year after reimplantation. 1 In agreement with these studies, we found that in patients whose leads were reimplanted due to suboptimal outcome the improvement was significant. When we analyzed patients who had the device removed and reimplanted due to infection, we did not notice significant differences in outcome, suggesting that reimplantation after infection can be successfully accomplished. Although management of infection is costly, 3 it seems that it is possible to recapture the initial gain of DBS after reimplantation. Given the small sample size of this subgroup, we suggest that a larger study is needed to 4 J Neurosurg June 22, 2018
5 FIG. 2. Diagram based on Schaltenbrand and Wahren s atlas in a plan at 3.5 mm below the AC-PC line plan. Lead locations before and after revision for suboptimal locations (A) and infection (B) were plotted. The leads numbers match the numeric identifiers from Tables 2 and 3. IC = internal capsule; RN = red nucleus; ZI = zona incerta. Figure is available in color online only. assess potential loss of DBS efficacy after removal and reimplantation of leads due to infection. In patients with suboptimal benefit following DBS, the workflow to revise the system seems to vary from one center to the next. For example, a lead can be inserted into a new position while the existing DBS lead is kept as an internal reference point, with 6 or without MER. 15 By leaving the misplaced lead in position, the new electrode will not migrate into the previous tract. Furthermore, some centers report not removing the suboptimal lead after the new lead is implanted because of the risk of hemorrhage. 1 Repositioning can also follow removal of the index lead, as preferred by our group. 5 Advantages of 2-stage revision are avoidance of lead migration into a previous tract (by allowing the trajectory path to heal before reimplantation) and, possibly, better MER. We found a mean change of 2.16 mm (SD 1.17 mm) in lead position when considering all patients, 1.67 mm (SD 0.83 mm) for reimplantation related to infection, and 2.73 mm (SD 1.31 mm) for those patients who had reimplantation related to a suboptimal outcome. The comparison between unsuccessful and successful lead placement in the same patient can offer valuable insights regarding the best predictors for postoperative outcomes. In our series, lead reimplantation was in general effective at improving outcomes after limited benefits from an index surgery. Richardson et al. superimposed internal landmarks onto the Schaltenbrand atlas and concluded that lead revision directed to a central location within the STN can improve symptom management. We found similar results for the patients whose leads were reimplanted for suboptimal outcomes. In Richardson et al. s series, the lead was adjusted mm in the axial plane. 15 Ellis et al. found a mean euclidean distance of 5.5 mm between the active DBS contact before and after revision. 5 Conclusions Lead removal and reimplantation is feasible and mostly safe after infection, device failure, or limited benefits after the first surgery. The data indicate that it is indeed possible to improve outcomes after limited benefit is achieved from an index implantation by removing the electrode and reimplanting it in a separate surgery. The reasons for not reimplanting the lead are variable and include cognitive J Neurosurg June 22,
6 TABLE 4. Published series with intracranial lead revision surgeries Authors & Year Ellis et al., 2008 Anheim et al., 2008 Richardson et al., 2009 Falowski & Bakay, 2016 Type of Study Retrospective case series Prospective study Retrospective series ET = essential tremor. Retrospective case series No. of Patients Indications for Revision Diseases Outcomes 22 patients Suboptimal clinical benefit 7 patients, 11 leads 8 patients, 9 leads 32 patients, 44 leads Inadequate improvement &/or stimulation-induced adverse effects Loss of efficacy, adverse effect, infection, lead fracture Vector Distance After Reposition 11 PD 24% improvement 5.5 mm 7 ET 60.4% improvement 6.1 mm 4 dystonia 12.8% improvement 6.7 mm PD Improvement in UPDRS score by 26.7% before 5.52 mm reimplantation & by 59.4% at 1 yr after reimplantation (off medication/on stimulation) PD 13 PD, 7 dystonia, 4 ET Each patient had a significant functional improvement following lead revision NA 4.1 mm (4 mm below the commissures) NA decline following the original surgery, patient choice, and comorbidities. References 1. Anheim M, Batir A, Fraix V, Silem M, Chabardès S, Seigneuret E, et al: Improvement in Parkinson disease by subthalamic nucleus stimulation based on electrode placement: effects of reimplantation. Arch Neurol 65: , Blomstedt P, Hariz GM, Hariz MI, Koskinen LOD: Thalamic deep brain stimulation in the treatment of essential tremor: a long-term follow-up. Br J Neurosurg 21: , Chen T, Mirzadeh Z, Lambert M, Gonzalez O, Moran A, Shetter AG, et al: Cost of deep brain stimulation infection resulting in explantation. Stereotact Funct Neurosurg 95: , Deuschl G, Schade-Brittinger C, Krack P, Volkmann J, Schäfer H, Bötzel K, et al: A randomized trial of deep-brain stimulation for Parkinson s disease. N Engl J Med 355: , Ellis TM, Foote KD, Fernandez HH, Sudhyadhom A, Rodriguez RL, Zeilman P, et al: Reoperation for suboptimal outcomes after deep brain stimulation surgery. Neurosurgery 63: , Falowski SM, Bakay RAE: Revision surgery of deep brain stimulation leads. Neuromodulation 19: , Goetz CG, Stebbins GT, Tilley BC: Calibration of unified Parkinson s disease rating scale scores to Movement Disorder Society unified Parkinson s disease rating scale scores. Mov Disord 27: , Hamani C, Richter E, Schwalb JM, Lozano AM: Bilateral subthalamic nucleus stimulation for Parkinson s disease: a systematic review of the clinical literature. Neurosurgery 56: , Kluger BM, Foote KD, Jacobson CE, Okun MS: Lessons learned from a large single center cohort of patients referred for DBS management. Parkinsonism Relat Disord 17: , Kupsch A, Benecke R, Müller J, Trottenberg T, Schneider GH, Poewe W, et al: Pallidal deep-brain stimulation in primary generalized or segmental dystonia. N Engl J Med 355: , Liu JKC, Soliman H, Machado A, Deogaonkar M, Rezai AR: Intracranial hemorrhage after removal of deep brain stimulation electrodes. J Neurosurg 116: , Machado A, Fernandez HH, Deogaonkar M: Deep brain stimulation: what can patients expect from it? Cleve Clin J Med 79: , Machado A, Rezai AR, Kopell BH, Gross RE, Sharan AD, Benabid AL: Deep brain stimulation for Parkinson s disease: surgical technique and perioperative management. Mov Disord 21 (Suppl 14):S247 S258, Okun MS, Tagliati M, Pourfar M, Fernandez HH, Rodriguez RL, Alterman RL, et al: Management of referred deep brain stimulation failures: a retrospective analysis from 2 movement disorders centers. Arch Neurol 62: , Richardson RM, Ostrem JL, Starr PA: Surgical repositioning of misplaced subthalamic electrodes in Parkinson s disease: location of effective and ineffective leads. Stereotact Funct Neurosurg 87: , Rolston JD, Englot DJ, Starr PA, Larson PS: An unexpectedly high rate of revisions and removals in deep brain stimulation surgery: analysis of multiple databases. Parkinsonism Relat Disord 33:72 77, Schaltenbrand G, Wahren W: Atlas for Stereotaxy of the Human Brain. Stuttgart: Thieme, 1992 Disclosures Dr. Machado has received consulting fees from St. Jude and has distribution rights from Enspire, ATI, and Cardionomics. Dr. Fernandez has received honoraria from AbbVie, Biogen, GE Health Care, Inventiv, Kyowa Hakko Kirin, Lundbeck, Merz Pharmaceuticals, Voyager, Sunovion, and Pfizer Pharmaceuticals, as a consultant. Author Contributions Conception and design: Machado, Frizon, Nagel. Acquisition of data: Frizon, May, Shao, Maldonado-Naranjo. Analysis and interpretation of data: Machado, Frizon, May, Shao, Maldonado- Naranjo. Drafting the article: Machado, Frizon, Nagel. Critically revising the article: Machado, Nagel, Fernandez. Reviewed submitted version of manuscript: Machado, Frizon, Nagel, Fernandez. Approved the final version of the manuscript on behalf of all authors: Machado. Statistical analysis: Frizon. Study supervision: Machado, Frizon. Correspondence Andre G. Machado: Cleveland Clinic, Cleveland, OH. machada@ ccf.org. 6 J Neurosurg June 22, 2018
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
SUPPLEMENTAL DIGITAL CONTENT
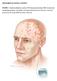 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease
 CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
Deep brain stimulation: What can patients expect from it?
 MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
MEDICAL GRAND ROUNDS ANDRE MACHADO, MD, PhD* Director, Center for Neurological Restoration, Neurological Institute, Cleveland Clinic HUBERT H. FERNANDEZ, MD Section Head, Movement Disorders, Center for
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Surgical Treatment: Patient Edition
 Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Parkinson s Disease Clinic and Research Center University of California, San Francisco 505 Parnassus Ave., Rm. 795-M, Box 0114 San Francisco, CA 94143-0114 (415) 476-9276 http://pdcenter.neurology.ucsf.edu
Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes
 Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
Case Reports in Neurological Medicine Volume 2015, Article ID 390727, 4 pages http://dx.doi.org/10.1155/2015/390727 Case Report Subacute Subdural Hematoma in a Patient with Bilateral DBS Electrodes Ha
The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery
 Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA.
 Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Shaheen Shaikh, M.D. Assistant Professor of Anesthesiology, University of Massachusetts Medical center, Worcester, MA. Shobana Rajan, M.D. Associate staff Anesthesiologist, Cleveland Clinic, Cleveland,
Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart review
 Mehanna et al. Journal of Clinical Movement Disorders 2014, 1:6 RESEARCH Open Access Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart
Mehanna et al. Journal of Clinical Movement Disorders 2014, 1:6 RESEARCH Open Access Clinical and programming pattern of patients with impending deep brain stimulation power failure: a retrospective chart
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
As clinical experience with deep-brain stimulation (DBS) of
 ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
ORIGINAL RESEARCH K.V. Slavin K.R. Thulborn C. Wess H. Nersesyan Direct Visualization of the Human Subthalamic Nucleus with 3T MR Imaging BACKGROUND AND PURPOSE: Electrical stimulation of the subthalamic
Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic surgery
 ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
ISPUB.COM The Internet Journal of Neuromonitoring Volume 7 Number 1 Deep Brain Stimulation for Treatment of Parkinson s Disease Deep brain stimulation, Parkinson s disease, subthalamic nucleus, stereotactic
Deep Brain Stimulation Surgery for Parkinson s Disease
 Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
Deep Brain Stimulation Surgery for Parkinson s Disease Demystifying Medicine 24 January 2012 Kareem A. Zaghloul, MD, PhD Staff Physician, Surgical Neurology Branch NINDS Surgery for Parkinson s Disease
Deep brain stimulation (DBS) of the ventral intermediate
 CLINICAL ARTICLE J Neurosurg 129:290 298, 2018 Intraoperative test stimulation versus stereotactic accuracy as a surgical end point: a comparison of essential tremor outcomes after ventral intermediate
CLINICAL ARTICLE J Neurosurg 129:290 298, 2018 Intraoperative test stimulation versus stereotactic accuracy as a surgical end point: a comparison of essential tremor outcomes after ventral intermediate
Accuracy of Intraoperative Computed Tomography during Deep Brain Stimulation Procedures: Comparison with Postoperative Magnetic Resonance Imaging
 Clinical Study Received: October 18, 2016 Accepted after revision: April 5, 2017 Published online: June 10, 2017 Accuracy of Intraoperative Computed Tomography during Deep Brain Stimulation Procedures:
Clinical Study Received: October 18, 2016 Accepted after revision: April 5, 2017 Published online: June 10, 2017 Accuracy of Intraoperative Computed Tomography during Deep Brain Stimulation Procedures:
Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology
 Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep Brain Stimulation for Movement Disorders Punit Agrawal, DO Clinical Assistant Professor of Neurology Division of Movement Disorders OSU Department of Neurology History of DBS 1 History of DBS 1987
Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients
 J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
J Neurosurg 98:779 784, 2003 Deep brain stimulation for movement disorders: morbidity and mortality in 109 patients ATSUSHI UMEMURA, M.D., JURG L. JAGGI, PH.D., HOWARD I. HURTIG, M.D., ANDREW D. SIDEROWF,
High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI
 Niederer 1 High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI Abstract In the past several decades the introduction of high-resolution, three-dimensional modeling techniques have
Niederer 1 High-Field in vivo Visualization of the Human Globus Pallidus Using 7T MRI Abstract In the past several decades the introduction of high-resolution, three-dimensional modeling techniques have
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
S ince the pioneering work of Benabid et and Pollak
 409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
409 PAPER Targeting the subthalamic nucleus for deep brain stimulation: technical approach and fusion of pre- and postoperative MR images to define accuracy of lead placement N A Hamid, R D Mitchell, P
Troubleshooting algorithms for common DBS related problems in tremor and dystonia
 Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Deep Brain Stimulation. Is It Right for You?
 Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Deep Brain Stimulation Is It Right for You? Northwestern Medicine Deep Brain Stimulation What is DBS? Northwestern Medicine Central DuPage Hospital is a regional destination for the treatment of movement
Parkinson disease: Parkinson Disease
 Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety
 MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety T Foltynie, L Zrinzo,,2 I Martinez-Torres, 3 E Tripoliti, E Petersen, 4 E Holl,,5 I Aviles-Olmos, M Jahanshahi,
MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety T Foltynie, L Zrinzo,,2 I Martinez-Torres, 3 E Tripoliti, E Petersen, 4 E Holl,,5 I Aviles-Olmos, M Jahanshahi,
Linköping University Post Print. Patient-specific models and simulations of deep brain stimulation for postoperative follow-up
 inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
Bilateral deep brain stimulation (DBS) has become
 technical note J Neurosurg 125:85 89, 2016 Simultaneous bilateral stereotactic procedure for deep brain stimulation implants: a significant step for reducing operation time Erich Talamoni Fonoff, MD, PhD,
technical note J Neurosurg 125:85 89, 2016 Simultaneous bilateral stereotactic procedure for deep brain stimulation implants: a significant step for reducing operation time Erich Talamoni Fonoff, MD, PhD,
SUBMITTED ACCEPTED INCLUDE WHEN CITING
 CLINICAL ARTICLE Prediction of depression and anxiety via patient-assessed tremor severity, not physician-reported motor symptom severity, in patients with Parkinson s disease or essential tremor who have
CLINICAL ARTICLE Prediction of depression and anxiety via patient-assessed tremor severity, not physician-reported motor symptom severity, in patients with Parkinson s disease or essential tremor who have
Deep brain stimulation (DBS) has been
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease
 Movement Disorders Vol. 25, No. 5, 2010, pp. 578 586 Ó 2010 Movement Disorder Society Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease Elena Moro,
Movement Disorders Vol. 25, No. 5, 2010, pp. 578 586 Ó 2010 Movement Disorder Society Long-Term Results of a Multicenter Study on Subthalamic and Pallidal Stimulation in Parkinson s Disease Elena Moro,
Delayed clinical improvement after deep brain stimulation related subdural hematoma
 Delayed clinical improvement after deep brain stimulation related subdural hematoma Report of 4 cases J Neurosurg 115:289 294, 2011 Genko Oyama, M.D., Ph.D., 1 Michael S. Okun, M.D., 1,2 Theresa A. Zesiewicz,
Delayed clinical improvement after deep brain stimulation related subdural hematoma Report of 4 cases J Neurosurg 115:289 294, 2011 Genko Oyama, M.D., Ph.D., 1 Michael S. Okun, M.D., 1,2 Theresa A. Zesiewicz,
Surgical treatment of Parkinsons disease(pd) is based. Result of Pallidotomy in Parkinson s Disease in Nepal
 Original Article Nepal Journal of Neuroscience 13:68-72, 2016 Resha Shrestha, MS Result of Pallidotomy in Parkinson s Disease in Nepal Takaomi Taira, MD, PhD Tokyo Women s Medical University, Tokyo, Japan
Original Article Nepal Journal of Neuroscience 13:68-72, 2016 Resha Shrestha, MS Result of Pallidotomy in Parkinson s Disease in Nepal Takaomi Taira, MD, PhD Tokyo Women s Medical University, Tokyo, Japan
DEEP BRAIN STIMULATION (DBS) is a standard treatment
 1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
1320 ORIGINAL ARTICLE Fast-Track Programming and Rehabilitation Model: A Novel Approach to Postoperative Deep Brain Stimulation Patient Care David B. Cohen, MD, Michael Y. Oh, MD, Susan M. Baser, MD, Cindy
EMERGING TREATMENTS FOR PARKINSON S DISEASE
 EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
EMERGING TREATMENTS FOR PARKINSON S DISEASE Katerina Markopoulou, MD, PhD Director Neurodegenerative Diseases Program Department of Neurology NorthShore University HealthSystem Clinical Assistant Professor
Deep brain stimulation (DBS) has been shown to be
 clinical article J Neurosurg 124:908 916, 2016 Clinical outcomes using ClearPoint interventional MRI for deep brain stimulation lead placement in Parkinson s disease Jill L. Ostrem, MD, 1 Nathan Ziman,
clinical article J Neurosurg 124:908 916, 2016 Clinical outcomes using ClearPoint interventional MRI for deep brain stimulation lead placement in Parkinson s disease Jill L. Ostrem, MD, 1 Nathan Ziman,
HealthTalks. Deep Brain Stimulation for Parkinson s Disease Patients
 HealthTalks Parkinson s Disease and Wellness Ali Rezai, MD Neurological Institute Director, Center for Neurological Restoration Cleveland Clinic Appointments: 216.444.4720 Deep Brain Stimulation for Parkinson
HealthTalks Parkinson s Disease and Wellness Ali Rezai, MD Neurological Institute Director, Center for Neurological Restoration Cleveland Clinic Appointments: 216.444.4720 Deep Brain Stimulation for Parkinson
10/13/2017. Disclosures. Deep Brain Stimulation in the Treatment of Movement Disorders. Deep Brain Stimulation: Objectives.
 Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep Brain Stimulation in the Treatment of Movement Disorders Disclosures None Eleanor K Orehek, M.D. Movement Disorders Specialist Noran Neurological Clinic 1 2 Objectives To provide an overview of deep
Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
 Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Original Article Medical Journal of the Islamic Republic of Iran (MJIRI) Iran University of Medical Sciences Deep brain stimulation of globus pallidus internus for DYT1 positive primary generalized dystonia
Rapid assessment of gait and speech after subthalamic deep brain stimulation
 SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
symptoms of Parkinson s disease EXCEPT.
 M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
Intracerebral microvascular measurements during deep brain stimulation implantation using laser doppler perfusion monitoring
 Intracerebral microvascular measurements during deep brain stimulation implantation using laser doppler perfusion monitoring Karin Wårdell, P. Blomstedt, Johan Richter, Johan Antonsson, Ola Eriksson, Peter
Intracerebral microvascular measurements during deep brain stimulation implantation using laser doppler perfusion monitoring Karin Wårdell, P. Blomstedt, Johan Richter, Johan Antonsson, Ola Eriksson, Peter
Indications. DBS for Tremor. What is the PSA? 6/08/2014. Tremor. 1. Tremor. 2. Gait freezing/postural instability. 3. Motor fluctuations
 Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Coordinate-Based Lead Location Does Not Predict Parkinson s Disease Deep Brain Stimulation Outcome
 Coordinate-Based Lead Location Does Not Predict Parkinson s Disease Deep Brain Stimulation Outcome Kelsey A. Nestor 1,2, Jacob D. Jones 3, Christopher R. Butson 4, Takashi Morishita 2, Charles E. Jacobson
Coordinate-Based Lead Location Does Not Predict Parkinson s Disease Deep Brain Stimulation Outcome Kelsey A. Nestor 1,2, Jacob D. Jones 3, Christopher R. Butson 4, Takashi Morishita 2, Charles E. Jacobson
DBS Programming. Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18
 DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
DBS Programming Paul S Fishman MD, PhD University of Maryland School of Medicine PFNCA 3/24/18 Disclosure The University of Maryland has received research funding form InSightec and the Focused Ultrasound
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学
 Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Intraoperative microelectrode recording (MER) for targeting during deep brain stimulation (DBS) procedures 巴黎第六大学医学院生理学 Paris 6 University (Pierre-et-Marie-Curie) Medical school physiology department 皮度
Surgical Management of Parkinson s Disease
 Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
Surgical Management of Parkinson s Disease Shyamal H. Mehta MD, PhD Assistant Professor of Neurology, Movement Disorders Division Mayo Clinic College of Medicine Mayo Clinic, Arizona 2016 MFMER slide-1
Evidence compendium. Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease
 Evidence compendium Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease CONTENTS Introduction... 4 Index of study summaries... 6 Parkinson s disease
Evidence compendium Research study summaries supporting the use of Medtronic deep brain stimulation (DBS) for Parkinson s disease CONTENTS Introduction... 4 Index of study summaries... 6 Parkinson s disease
Efficient Feature Extraction and Classification Methods in Neural Interfaces
 Efficient Feature Extraction and Classification Methods in Neural Interfaces Azita Emami Professor of Electrical Engineering and Medical Engineering Next Generation Therapeutic Devices 2 Where We Started:
Efficient Feature Extraction and Classification Methods in Neural Interfaces Azita Emami Professor of Electrical Engineering and Medical Engineering Next Generation Therapeutic Devices 2 Where We Started:
History of Deep Brain Stimulation in la Pitié-Salpêtrière hospital
 History of Deep Brain Stimulation in la Pitié-Salpêtrière hospital Since the beginning of Deep Brain Stimulation (DBS) in the 80 s, DBS changed very much following evolution of technologies, but also following
History of Deep Brain Stimulation in la Pitié-Salpêtrière hospital Since the beginning of Deep Brain Stimulation (DBS) in the 80 s, DBS changed very much following evolution of technologies, but also following
Short term surgical complications after subthalamic deep brain stimulation for Parkinson s disease: does old age matter?
 Levi et al. BMC Geriatrics (2015) 15:116 DOI 10.1186/s12877-015-0112-2 RESEARCH ARTICLE Open Access Short term surgical complications after subthalamic deep brain stimulation for Parkinson s disease: does
Levi et al. BMC Geriatrics (2015) 15:116 DOI 10.1186/s12877-015-0112-2 RESEARCH ARTICLE Open Access Short term surgical complications after subthalamic deep brain stimulation for Parkinson s disease: does
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
The Surgical Management of Essential Tremor
 The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
The Surgical Management of Essential Tremor International Essential Tremor Foundation Learning About Essential Tremor: Diagnosis and Treatment Options Albuquerque, NM September 24, 2005 Neurosurgeon Overview:
Deep Brain Stimulation
 Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
Deep Brain Stimulation Policy Number: 7.01.63 Last Review: 8/2017 Origination: 8/2001 Next Review: 8/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for deep brain
NIH, American Parkinson Disease Association (APDA), Greater St. Louis Chapter of the APDA, McDonnell Center for Higher Brain Function, Barnes-Jewish
 Mechanism of Action of Deep Brain Stimulation In Parkinson Disease Samer D. Tabbal, M.D. Associate Professor of Neurology Washington University at St Louis Department of Neurology June 2011 Conflict of
Mechanism of Action of Deep Brain Stimulation In Parkinson Disease Samer D. Tabbal, M.D. Associate Professor of Neurology Washington University at St Louis Department of Neurology June 2011 Conflict of
Since its introduction in 1987 by Benabid et al.,7 deep. Risks of common complications in deep brain stimulation surgery: management and avoidance
 J Neurosurg 120:132 139, 2014 AANS, 2014 Risks of common complications in deep brain stimulation surgery: management and avoidance Clinical article Albert J. Fenoy, M.D., 1 and Richard K. Simpson Jr.,
J Neurosurg 120:132 139, 2014 AANS, 2014 Risks of common complications in deep brain stimulation surgery: management and avoidance Clinical article Albert J. Fenoy, M.D., 1 and Richard K. Simpson Jr.,
Deep Brain Stimulation For Parkinson s Disease
 Deep Brain Stimulation For Parkinson s Disease What s new in brain circuit training Associate Professor Robert Wilcox Flinders University & University of South Australia Neurology Department, Flinders
Deep Brain Stimulation For Parkinson s Disease What s new in brain circuit training Associate Professor Robert Wilcox Flinders University & University of South Australia Neurology Department, Flinders
The posterior subthalamic area (PSA) is a promising
 clinical article J Neurosurg 126:386 390, 2017 Dystonic tics induced by deep brain stimulation of the posterior subthalamic area for essential tremor Arjun S. Chandran, MBBS, 1 Stuti Joshi, MBBS, 2 Megan
clinical article J Neurosurg 126:386 390, 2017 Dystonic tics induced by deep brain stimulation of the posterior subthalamic area for essential tremor Arjun S. Chandran, MBBS, 1 Stuti Joshi, MBBS, 2 Megan
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech?
 Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Critical Review: What effects do neurosurgical treatments for generalized dystonia have on speech? Jana Zalmanowitz M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE
 11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
Lecture XIII. Brain Diseases I - Parkinsonism! Brain Diseases I!
 Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Linköping University Post Print. Karin Wårdell, Peter Zsigmond, Johan Richter and Simone Hemm. N.B.: When citing this work, cite the original article.
 Relationship Between Laser Doppler Signals and Anatomy During Deep Brain Stimulation Electrode Implantation Toward the Ventral Intermediate Nucleus and Subthalamic Nucleus Karin Wårdell, Peter Zsigmond,
Relationship Between Laser Doppler Signals and Anatomy During Deep Brain Stimulation Electrode Implantation Toward the Ventral Intermediate Nucleus and Subthalamic Nucleus Karin Wårdell, Peter Zsigmond,
Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving contralateral parkinsonism
 Brain Advance Access published May 23, 2006 doi:10.1093/brain/awl127 Brain (2006) Page 1 of 16 Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving
Brain Advance Access published May 23, 2006 doi:10.1093/brain/awl127 Brain (2006) Page 1 of 16 Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving
UNIFORM QUALITATIVE ELECTROPHYSIOLOGICAL CHANGES IN POSTOPERATIVE REST TREMOR
 UNIFORM QUALITATIVE ELECTROPHYSIOLOGICAL CHANGES IN POSTOPERATIVE REST TREMOR Norbert Kovacs, 1 Istvan Balas, 2 Zsolt Illes 1, Lorant Kellenyi, 2 Tamas P Doczi, 2 Jozsef Czopf, 1 Laszlo Poto 3 and Ferenc
UNIFORM QUALITATIVE ELECTROPHYSIOLOGICAL CHANGES IN POSTOPERATIVE REST TREMOR Norbert Kovacs, 1 Istvan Balas, 2 Zsolt Illes 1, Lorant Kellenyi, 2 Tamas P Doczi, 2 Jozsef Czopf, 1 Laszlo Poto 3 and Ferenc
Why high-field MRI? Benefits of high-field MRI. Signal-to-noise ratio (SNR) Contrast (anatomical & functional) 8 x 8 x 8 mm 3 4 x 4 x 4 mm 3
 Why high-field MRI? 8 x 8 x 8 mm 3 4 x 4 x 4 mm 3 2 x 2 x 2 mm 3 1 x 1 x 1 mm 3 Voxel volume 2 x 2 x 2 mm 3 = 8 Voxel volume 1 x 1 x 1 mm 3 = 1 Benefits of high-field MRI Signal-to-noise ratio (SNR) Contrast
Why high-field MRI? 8 x 8 x 8 mm 3 4 x 4 x 4 mm 3 2 x 2 x 2 mm 3 1 x 1 x 1 mm 3 Voxel volume 2 x 2 x 2 mm 3 = 8 Voxel volume 1 x 1 x 1 mm 3 = 1 Benefits of high-field MRI Signal-to-noise ratio (SNR) Contrast
Reformatted Imaging to Define the Intercommissural Line for CT -Guided Stereotaxic Functional Neurosurgery
 Reformatted Imaging to Define the Intercommissural Line for CT -Guided Stereotaxic Functional Neurosurgery 429 Richard E. Latchaw1.2 L. Dade Lunsford 1. 2 William H. Kennedi Functional stereotaxic neurosurgery
Reformatted Imaging to Define the Intercommissural Line for CT -Guided Stereotaxic Functional Neurosurgery 429 Richard E. Latchaw1.2 L. Dade Lunsford 1. 2 William H. Kennedi Functional stereotaxic neurosurgery
PARKINSON S SYMPTOM TRACKER
 PARKINSON S SYMPTOM You can help your doctor make good treatment decisions by tracking your symptoms. A well-kept Symptom Tracker provides a clear picture of when you are taking your medications, when
PARKINSON S SYMPTOM You can help your doctor make good treatment decisions by tracking your symptoms. A well-kept Symptom Tracker provides a clear picture of when you are taking your medications, when
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo
 Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease
 ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease Parkinson s Disease Cardinal Signs: Resting tremor Rigidity Bradykinesia Postural instability Other Symptoms Dystonia Dysphagia Autonomic
ASSFN Clinical Case: Bilateral STN DBS Implant for Parkinson s Disease Parkinson s Disease Cardinal Signs: Resting tremor Rigidity Bradykinesia Postural instability Other Symptoms Dystonia Dysphagia Autonomic
Effect of Advancing Age on Outcomes of Deep Brain Stimulation for Parkinson Disease
 Research Original Investigation Effect of Advancing Age on Outcomes of Deep Brain Stimulation for Parkinson Disease Michael R. DeLong, BA; Kevin T. Huang, AB; John Gallis, ScM; Yuliya Lokhnygina, PhD;
Research Original Investigation Effect of Advancing Age on Outcomes of Deep Brain Stimulation for Parkinson Disease Michael R. DeLong, BA; Kevin T. Huang, AB; John Gallis, ScM; Yuliya Lokhnygina, PhD;
Technical and Safety Considerations in functional imaging of DBS leads
 Technical and Safety Considerations in functional imaging of DBS leads Stephen Jones PhD MD Cleveland Clinic Neuroradiology April 23 rd, 2017 V 3.1 Outline Motivation: Utility of DBS and MRI MRI and tissue
Technical and Safety Considerations in functional imaging of DBS leads Stephen Jones PhD MD Cleveland Clinic Neuroradiology April 23 rd, 2017 V 3.1 Outline Motivation: Utility of DBS and MRI MRI and tissue
E ssential tremor is a commonly diagnosed movement
 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II
 Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
Parkinsonism and Related Disorders 13 (2007) 399 405 www.elsevier.com/locate/parkreldis Surgery for Parkinson s disease improves disability but not impairment components of the UPDRS-II A. Haffenden, U.
P rimary generalised dystonia (PGD) is a movement disorder
 1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
1314 PAPER Effect of electrode contact location on clinical efficacy of pallidal deep brain stimulation in primary generalised dystonia S Tisch, L Zrinzo, P Limousin, K P Bhatia, N Quinn, K Ashkan, M Hariz...
Review Article Dystonia and the Role of Deep Brain Stimulation
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 193718, 5 pages doi:10.5402/2011/193718 Review Article Dystonia and the Role of Deep Brain Stimulation Thomas L. Ellis Wake
UNILATERAL STEREOTACTIC POSTEROVENTRAL GLOBUS PALLIDUS INTERNUS PALLIDOTOMY FOR PARKINSON S DISEASE: SURGICAL TECHNIQUES AND 2-YEAR FOLLOW-UP
 Pallidotomy for Parkinson s disease UILATERAL STEREOTACTIC POSTEROVETRAL GLOBUS PALLIDUS ITERUS PALLIDOTOMY FOR PARKISO S DISEASE: SURGICAL TECHIQUES AD 2-YEAR FOLLOW-UP Chun-Po Yen, Shiao-Jing Wu, Yu-Feng
Pallidotomy for Parkinson s disease UILATERAL STEREOTACTIC POSTEROVETRAL GLOBUS PALLIDUS ITERUS PALLIDOTOMY FOR PARKISO S DISEASE: SURGICAL TECHIQUES AD 2-YEAR FOLLOW-UP Chun-Po Yen, Shiao-Jing Wu, Yu-Feng
F unctional stereotactic surgery is now well established for
 PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
PAPER Effect of chronic pallidal deep brain on off period dystonia and sensory symptoms in advanced Parkinson s disease T J Loher, J-M Burgunder, S Weber, R Sommerhalder, J K Krauss... See end of article
SURGERY FOR MOVEMENT DISORDERS
 MOVEMENT DISORDERS SURGERY FOR MOVEMENT DISORDERS Ali R. Rezai, M.D. Center for Neurological Restoration, and Department of Neurosurgery, Cleveland Clinic, Cleveland, Ohio Andre G. Machado, M.D., Ph.D.
MOVEMENT DISORDERS SURGERY FOR MOVEMENT DISORDERS Ali R. Rezai, M.D. Center for Neurological Restoration, and Department of Neurosurgery, Cleveland Clinic, Cleveland, Ohio Andre G. Machado, M.D., Ph.D.
Activa RC and Activa PC
 Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
Activa RC and Activa PC neurostimulators for deep brain stimulation From the company with the most experience in DBS The Activa Family Innovative programming platform More choices for patients With the
Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September
 Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September 2015 203-212 Original Article Ablative Procedures without Microelectrode Recording in the Management of Advanced Parkinson s Disease:
Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September 2015 203-212 Original Article Ablative Procedures without Microelectrode Recording in the Management of Advanced Parkinson s Disease:
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Value Units
 Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL Policy Number: MP.108.MH Last Review Date: 05/10/2018 Effective Date: 07/01/2018
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.0108.MH Deep Brain and Dorsal Column (Spinal Cord) This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.0108.MH Deep Brain and Dorsal Column (Spinal Cord) This policy applies to the following lines of business: MedStar Employee (Select) MedStar CareFirst
Long -Te rm Sur gical and H ar dwar e - Related Complications of Deep Brain Stimulation
 Clinical Study St e r e o t a c t Fu n c t N e u r o s u r g 2011; 8 9 : 8 9 95 DOI: 10.1159/000323372 Received: August 26, 2010 Accepted after revision: December 3, 2010 Published online: February 2,
Clinical Study St e r e o t a c t Fu n c t N e u r o s u r g 2011; 8 9 : 8 9 95 DOI: 10.1159/000323372 Received: August 26, 2010 Accepted after revision: December 3, 2010 Published online: February 2,
C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak, MD, PhD D.
 ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration
 doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
doi:10.1093/brain/awn120 Brain (2008), 131,1895^1902 Outcome predictors of pallidal stimulation in patients with primary dystonia: the role of disease duration Ioannis U. Isaias, 1 Ron L. Alterman 2 and
Topic: Deep Brain Stimulation Date of Origin: April Section: Surgery Approved Date: April Policy No: 84 Effective Date: July 1, 2014
 Medical Policy Manual Topic: Deep Brain Stimulation Date of Origin: April 1998 Section: Surgery Approved Date: April 2014 Policy No: 84 Effective Date: July 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Deep Brain Stimulation Date of Origin: April 1998 Section: Surgery Approved Date: April 2014 Policy No: 84 Effective Date: July 1, 2014 IMPORTANT REMINDER Medical Policies
Basal ganglia motor circuit
 Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Deep Brain Stimulation: Complications and Attempts at Avoiding Them
 42 The Open Neurosurgery Journal, 2011, 4, (Suppl 1-M4) 42-52 Open Access Deep Brain Stimulation: Complications and Attempts at Avoiding Them Roy A.E. Bakay* and Adam P. Smith Rush University Medical Center,
42 The Open Neurosurgery Journal, 2011, 4, (Suppl 1-M4) 42-52 Open Access Deep Brain Stimulation: Complications and Attempts at Avoiding Them Roy A.E. Bakay* and Adam P. Smith Rush University Medical Center,
Over the last 20 years, Deep Brain Stimulation (DBS)
 Deep Brain Stimulation in Parkinson s Disease: Past, Present, and Future Though it has been underutilized over the past two decades, deep brain stimulation is an effective intervention for many individuals
Deep Brain Stimulation in Parkinson s Disease: Past, Present, and Future Though it has been underutilized over the past two decades, deep brain stimulation is an effective intervention for many individuals
I n 1991 Benabid et al introduced deep brain stimulation
 PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
