Lymphangioleiomyomatosis and tuberous sclerosis
|
|
|
- Alice Warner
- 5 years ago
- Views:
Transcription
1 Vol. 96 (2002) 7^13 ORIGINAL ARTICLES Lymphangioleiomyomatosis and tuberous sclerosis E. HANCOCK*,S.TOMKINS w,j.sampson w AND J. OSBORNE* *Bath Unit for Research into Paediatrics, The Children s Centre, Royal United Hospital, Combe Park, Bath and w Institute of Medicine Genetics,University College of Medicine of Wales, Health Park, Cardi, U.K. Abstract Tuberous sclerosis (TSC) is an inherited disorder best known for its association with severe learning di culties, epilepsy, behavioural problems, skin and renal pathology. Lymphangioleiomyomatosis (LAM), characterized by alveolar smooth muscle proliferation and cystic destruction of parenchyma, occurs as an infrequent symptomatic pulmonary complication intsc and as a very rare sporadic disease in those without signs of TSC.Considered a generalized and progressive cystic lung disease that is di cultto treat with a poor prognosis, it has been reported almost exclusively in women, most commonly presenting with dyspnoea and pneumothorax in those of childbearing age.we investigated the clinicalfeatures and prognosis of LAMin patients withtscincluding the e ects oftreatment, strati ed by the method of diagnosis of LAM (i.e. histological or radiological).we found histological proof of diagnosis in 10 of 21 patients withtsc and symptomatic lung disease, onsetin childhoodin four, three males with LAM, individuals with apparently focal disease, great variation in clinical course and no clear treatment bene t. In those withtsc, symptomatic LAM is infrequent but causes a signi cant morbidity and mortality. It was not possible to detect predisposing factors, other than being female. Males with apparent LAM should be rigorously investigated.r 2002 Harcourt Publishers Ltd doi: /rmed , available online at on Keywords tuberous sclerosis; pulmonary lymphangioleiomyomatosis; LAM. INTRODUCTION Tuberous sclerosis (TSC) is an autosomal dominant disorder with a birth incidence of around one in (1) and a spontaneous mutation rate of B65%. Initially thought to be a rare condition of unknown aetiology with a characteristic facial skin rash, severe epilepsy and severe learning di culties, it has become apparent that the disease is genetic and is more diverse than originally recognized. More than a quarter of patients have neither epilepsy nor severe learning di culties, but can have severely a ected o spring. Lutembacher rst described lymphangioleiomyomatosis (LAM) intsc in1918, although he mistook the cystic and nodular changes for metastasis from renal brosarcoma. In 1939, Berg and Vejilens gave the rst accurate and clear description of pulmonary tuberous sclerosis. Dwyer (2) described three cases of LAM intsc and reviewed a further 31 cases, and Castro (3) made a retrospective study of nine patients. Other reports of LAM Received 3 July 2001and accepted13 August 2001 Correspondence should be addressed to: Prof. John Osborne,The Children s Centre, Royal United Hospital, Combe Park, Bath BA13NG, U.K.Fax: ; mpsjpo@bath.ac.uk complicating TSC have all been of even fewer patients. Johnson (4) recently reviewed LAM. LAM predominantly a ects females of childbearing age (5).The most common presenting symptoms are dyspnoea (from pneumothorax and chylothorax), chronic cough, haemoptysis, wheeze and chest pain, but asymptomatic cases occur (2). It can lead to cyanosis, respiratory failure and cor pulmonale (2^5). Pulmonary function tests show an obstructive more often than a restrictive pattern (6). Treatment of LAM is di cult, and is usually symptomatic. Hormone manipulation has been tried but without consistent success (3,7).The long-term prognosis is often considered poor with many patients following a relentless deterioration after the onset of their symptoms (2). We aimed to document the clinical features of LAM in a cross-sectional study of patients with a diagnosis of TSC and LAM. METHODS Patients su ering from symptomatic pulmonary complications of TSCwere identi ed from several U.K. sources:
2 8 RESPIRATORY MEDICINE the Bath TSC clinic (with records on 395 TSC patients), Respiratory Physicians in the Wessex region, the Tuberous Sclerosis Association, the Medical Genetics Department in Cardi and the Renal Medicine Department in Brighton. Patients were classi ed as having de nite LAM if the diagnosis had been con rmed by histopathology at post mortem or following lung biopsy, probable LAM if they had multiple thin walled cysts on high resolution computerised tomography (HRCT) scan or honeycombing or ne reticular shadowing on chest X-ray. If their only evidence of LAM was of a pneumothorax, they were classi- ed as having possible LAM. Patients were considered to have de nite TSC according to the strict interpretation of the recently revised criteria for clinical diagnosis (8), suggesting two independent hamartomas are required to make a con dent diagnosis, but counting LAM and renal angiomyolipomas as one harmartoma for this purpose. Clinical records and, where possible, radiographic lms were reviewed. Age at diagnosis, diagnostic criteria and family history of TSC; age at onset, symptoms and diagnosis of lung disease, mode of presentation, complications, chest X-ray, HRCT and biopsy appearances, pulmonary function tests, extrapulmonary manifestations, treatment and outcome were noted. All patients still living were assessed by interview and examination and, where not precluded by the severity of learning di culties, basic lung function was measured using a portable spirometer. A history was taken from the relatives of all decreased patients. Ethical permission was obtained for the study from the Bath Local Research Ethics Committee. RESULTS Twenty-one patients withtsc (20 with de nitetsc) and pulmonary disease were identi ed (Table 1). Ten patients had de nite LAM, con rmed at post mortem in four. Their histology showed smooth muscle proliferation, honeycomb lung or multiple cysts and bullae (Table 2). Nine patients had probable LAM con rmed by HRCT in six and chest X-ray in three, two honeycombing and one with ne reticular shadowing (on chest X-ray).Two cases had pneumothoraces only on chest X-ray and HRCT had not been performed (one with probable TSC). All patients had facial angio bromas plus at least one other hamartoma (in addition to LAM) and de nite TSC, except patient 21 who was an obligate carrier for TSC, with an a ected sister and son (and her mother had ungual bromata); she had two hypopigmented macules but had not undergone fundoscopy, renal or cranial imaging. Presenting features and age at diagnosis of TSC and LAM are shown intable 1. Eighteen of the 21 cases were female and seven were known to have familial TSC. Median age of diagnosis of TSC was 17 years (range 6 weeks^3 years). Three had a diagnosis of TSC made as a result of their pulmonary disease.the median age of onset of pulmonary symptoms was 20 years (range birth^ 34 years). The median age of diagnosis of LAM was 25 years (range 6 months^ 50 years).there was a mean delay of 6 years between the onset of respiratory symptoms and the eventual diagnosis of LAM (range 0^30 years). The most common presentation was acute dyspnoea, secondary to pneumothorax in14 ( ve bilaterally) and to chylothorax in one. Five other patients presented with chronic dyspnoea and one patient presented with thick bronchopulmonary secretions as an infant. Dyspnoea occurred in 19, cough in 15, wheeze in 11, haemoptysis in six and pain in 13, usually in conjunction with pneumothoracies (Table 2). Seventeen su ered pneumothoraces, four chylothoraces, one a pericardial e usion and one a fatal pulmonary haemorrhage (Table 2). Four patients died as a result of their respiratory disease. Patient1had bilateral pneumothoracies at 25 years and gradually deteriorated, dying at the age of 47 years from cor pulmonale. Patient 2 had a left pneumothorax aged 18 years, bilateral pneumothoracies aged 21 years and subsequently complained of shortness of breath and su ered recurrent chest infections, dying of respiratory failure aged 27 years. Patient 3 developed bilateral pneumothoracies during general anaesthesia for gastroscopy at 18 years of age, dying of respirator failure1week later. Patient 4 presented with a left-sided pneumothorax at19 years of age following a 1-week history of a dry cough. She was treated conservatively and allowed home to await HRCT. She su ered an acute fatal pulmonary haemorrhage whilst asleep. Spirometry could only be performed on 11 patients. Two had normal lung function, three an obstructive picture, and six a restrictive pattern. Response to bronchodilators was not measured. Nine patients underwent pleurodesis and four pleurectomy for recurrent or severe pneumothoracies. With little or no improvement in symptoms seven patients had bronchodilator inhalers and two inhaled steroids in addition. Four patients received progesterone therapy. Patient two su ered from increasing dyspnoea and recurrent chest infections from the age of 22 years. Her condition deteriorated before, during and after 1 year of treatment with progesterone. Patient 10 had bilateral pneumothoracies aged 30 years treated by pleurodesis. Depo progesterone (as depo-provera) was started and has continued for 5 years. She has remained symptomatically stable with mild dyspnoea, wheeze on exertion and occasional cough. Patient12 had worsening dyspnoea and haemoptysis over a 16-year period. Since depo progesterone was commenced, her exercise tolerance improved and there has been no deterioration in her lung function tests. Patient 14 had a renal haemorrhage at 35 years, treated by transfusion and with depot progesterone, but 4 years later su ered a pneumothorax
3 LYMPHANGIOLEIOMYOMATOSIS ANDTUBEROUS SCLEROSIS 9 TABLE 1. Sex, age at whichtscwas diagnosed, reason for diagnosis of TSC, age of onset and presenting features of pulmonary disease, strati ed by de nite, probable and possible diagnosis of LAM Patient Sex Age at diagnosis of TSC Reason for diagnosis of TSC Age of diagnosis of pulmonary symptoms Presenting feature(s) of LAM Patients with a de nite diagnosis of LAM 1 Female 16 years Retinal phakoma 25 years Pnuemothorax 2 Female 4 years Facial angio broma CT brain 18 years Pnuemothorax 3 Female 2 years Infantile spasms CT brain 18 years Pnuemothorax 4 Female 3 years Epilepsy CT brain 19 years Pnuemothorax 5 Female 9 months Facial angio broma 7 years Dyspnoea 6 Female 37 years Investigated following diagnosis of son Teenager Dyspnoea and chest pain 7 Male 6 months PulmonaryTSC 6 months Thick pulmonary secretions 8 Female 18 months Infantile spasms CT brain 21years Pnuemothorax 9 Female 34 years PulmonaryTSC 10 years Dyspnoea and weight loss 10 Female 30 years PulmonaryTSC 30 years Pnuemothorax Patients with a probable diagnosis of LAM 11 Female 21years Investigated following diagnosis of daughter. 34 years Dyspnoea 12 Female 11months Infantile spasms CT brain 19 years Pnuemothorax 13 Female 5 years Facial angio broma CT brain 32 years Pnuemothorax 14 Female 35 years Renal haemorrhage 38 years Chylothorax 15 Female 17 years Investigated following diagnosis of son 17 years Pnuemothorax 16 Female 37 years Ungual broma Facial 23 years Pnuemothorax angio broma 17 Female 24 years Investigated following diagnosis 20 years Pnuemothorax of son 18 Male 6 weeks Epilepsy CT brain 8 years Dyspnoea and dry cough 19 Male 21years Epilepsy CT brain 32 years Pnuemothorax Patients with a possible diagnosis of LAM 20 Female 6 years Facial angio broma 20 years Pnuemothorax 21 Female 28 years Obligate carrier.two hypomelanic patches 25 years Pnuemothorax and chylous e usion. A course of oral steroids was prescribed for patients 3 and 16, with no improvement, although patient 17 made a remarkable recovery from acute respiratory failure after treatment with steroids (seetable 3). Two patients died within days of developing respiratory symptoms; the remaining patients were followed up for an average of 14 years (median of 10 years, range 6 months^38 years). Five have shown a progressive deterioration, two dying from their disease. There symptomaticpatientsimprovedandtworemainedstablewhile nine patients were asymptomatic after the presenting episode. Other manifestations of TSC All patients had skin manifestations of TSC. Fourteen had known renal involvement with angiomyolipomas. One had renal involvement found incidentally at post mortem, two patients had undergone nephrectomy, the other 11 patients had AML 7 cysts on renal ultrasound scan. Only two of the asymptomatic patients had been
4 10 RESPIRATORY MEDICINE TABLE 2. Symptoms, complications and investigations Patient Dyspnoea Cough Haemoptysis Pain Wheeze Complications Chest X-ray HRCT Biopsy/histology Patients with de nite LAM 1 Yes Yes Yes 1Bil P P Not performed lung involement 2 Yes Yes Yes 1Bil P P Unavailable appearance of LAM 3 Developed bilateral pnuemothoracies under GA and died whilst ventilated 7 days later P Not performed LAM 4 Yes Yes 1Lt P,1Chy, P Not performed LAM 1Pul Haem 5 Yes Yes Yes Yes 2 Rt P P,RS Multiple cystic spaces proliferation of immature muscle 6 Yes Yes Yes 2 Rt P,1Lt P P Not performed small cysts in the lung tissue 7 Yes Yes Yes Not performed LAM 8 Yes Yes Yes 1Bil P,1Chy P Not performed proliferation of smooth muscle 9 Yes Yes Yes 1Rt P,1Chy,1CE Emph Emphysema opinion is of honeycomb lung 10 Yes Yes Yes Yes 1Bil P P Consistent with LAM Patients with a probable diagnosis of LAM 11 Yes Yes Yes Yes Yes Thin walled cysts. proliferation of smooth muscle Not performed 12 Yes Yes Yes Yes 1Rt P P Lung cysts and bullae Not performed 13 Yes Yes Yes 1Rt P P Honeycomb Not performed pattern 14 Yes 1Chy P,E Cystic changes of TSC Not performed 15 Yes Yes Yes 1Bil P P Thin walled Not performed cysts 16 Yes Yes Yes Yes 1Rt P,1Lt P Yes Thin walled Not performed cysts 17 Yes Yes Yes Yes Yes 2 Rt P,1Lt P Yes Not performed Not performed 18 Yes Yes Yes Yes Yes Not performed Not performed 19 Yes Yes Yes 1RT P RS Not performed Not performed Patients with a possible diagnosis of LAM 20 Yes Yes Yes Yes Yes 1Rt P P Not performed Not performed 21 Yes 1Lt P P Not performed Not performed HRCT: high resolution computerised tomography scan of chest; Rt P: right pnuemothorax; Lt P: left pnuemothorax; Bil P: bilateral pnuemothorax; Chy: chylothorax; Pul Haem: pulmonary haemorrhage; CE: peri-cardial e usion; H: honeycomb appearance; P: pnuemothorax; RS: reticular shadowing; Emph: emphysema; E : pleural e usion. screened and found to have normal renal ultrasound scans, the remaining ve patients have not been screened. Epilepsy was the commonest neurological manifestation occurring in 18 (86%) patients, 10 (48%) had associated learning di culties and six (29%) autistic spectrum disorder and hyper-activity. Two patients had giant cell astrocytoma with associated hydrocephalus. One patient had a mild hemiplegia. Four patients had asymptomatic hepatic angiomyolipoma. No cardiac rhabdomyomas had been detected. Four patients had a scoliosis ( xed in two), but none had undergone surgery or bracing. All four had a mild course of LAM. DISCUSSION The Wessex TS epidemiology study identi ed 147 patients and had a prevalence of one in on1january 1997 (personal communication). Only one of these cases had symptomatic LAM, giving a prevalence of 0?66% for
5 LYMPHANGIOLEIOMYOMATOSIS ANDTUBEROUS SCLEROSIS 11 TABLE 3. Acute surgical and medical treatment, long-term medical treatment, disease course and duration of follow-up (in parentheses) Acute/surgical treatment Long-term medical treatment Disease course (follow-up) Patients with a de nite diagnosis of LAM 1 Drainage Pleurodesis Oxygen therapy Died from cor pulmonale whilst waiting for transplant (B25 years after onset of symptoms) 2 Drainage Pleurodesis Oxygen therapy progesterone Died from cor pulmonale, too ill for transplant (B10 years after onset of symptoms) 3 Drainage and ventilation None Died from respiratory and renal failure (B1week after onset of symptoms) 4 None None Died from massive pulmonary haemorrhage (B2 weeks after onset of symptoms) 5 Drainage Pleurodesis None Stable (3 years) 6 Drainage Pleurectomy None Remains well (25 years) 7 None Inhalers (no bene t) Improved (23 years) 8 Drainage Pleurectomy None Remains well (6 months) 9 Lobectomy None Remains well (38 years) 10 Drainage Pleurodesis Progesterone Remains well Patients with a probable diagnosis of LAM 11 None Atrovent (little bene t) Stable (13 years) 12 Drainage Pleurectomy Progesterone Improved (18 years) 13 Drainage Pleurodesis Atrovent (some bene t) Remains well (2 years) 14 Drainage Pleurodesis Progesterone Remains well (1year) 15 Drainage Pleurodesis None Progressive deterioration (10 years) 16 Drainage Pleurodesis Inhalers (no bene t) Progressive deterioration (30 years) 17 Drainage Pleurodesis Progressive deterioration (31years) 18 None Inhalers (no bene t) Improved slowly (6 years) 19 Aspiration None Remains well (2 years) Patients with a possible diagnosis of LAM 20 Drainage Pleurodesis None Remains well (17 years) 21 Drainage None Remains well (5 years) symptomatic LAM intsc. Patient four developed symptoms soon after. This nding is similar to previous studies. Dwyer et al. (2) and Torres et al. (7) estimated that LAM occurs in less than 1% of patients withtsc, Castro et al. (3) a slightly higher incidence of 2?3%. We know we will have missed some cases of TSC (1), but within the Wessex population we are less likely to have missed symptomatic LAM. However, incidental ndings of LAM have been described on the CXRs and CT scans of entirely asymptomatic TSC patients (2). No study has screened TSC patients for LAM and the true prevalence may be higher than that estimated from symptomatic patients. Although the numbers in our study were small there was no di erence between patients with de nite, probable or possible LAM in presentation, clinical course or outcome. All the female patients developed symptoms prior to the menopause and two with de nite LAM did so prepubertally.this shows that LAM intsc is not con- ned to females of childbearing age.there have been only ve previous reported cases (2,9^12) of LAM in males with TSC. None reported changes on HRCT, two had not been con rmed by biopsy and those con rmed by biopsy were reported as being consistent with TSC, thickened pleura with cysts or cysts empty or lled with uid. We identi ed three males withtsc who exhibited signs of lung disease. Patient 7 su ered thick pulmonary secretions with recurrent chest infections from birth until puberty only. Lung biopsy was reported as LAM and led to the diagnosis of TSC but is no longer available for repeat analysis and he is not su ciently co-operative for HRCT. His unusual course must throw some doubt on the diagnosis of LAM. Patient 18 su ered from episodes of dyspnoea and wheeze from aged 8 years: asthma medication did not relieve his symptoms and a chest X-ray showed honeycombing, suggesting LAM. He has never had HRCT or open lung biopsy. Patient 19 had been asymptomatic until 32 years when he su ered a spontaneous pneumothorax. He has had no recurrence (followup 4 years), nor su ered any other respiratory symp-
6 12 RESPIRATORY MEDICINE toms. His chest X-ray con rmed LAM. His karyotype was found to be 47XXY (Klinefelter s syndrome), possibly explaining his presentation with a lung disease that is normally limited to females. We would conclude that in any male withtsc in whom the diagnosis of LAM is suspected, other pulmonary diagnoses must be excluded, chromosomal analysis, HRCT and preferably lung biopsy should be performed to con rm the diagnosis since LAM in phenotypic males is very rare. The age of diagnosis of TSC in the patients in this series was17 years, slightly older than is usual. This may be a chance nding because of the small numbers, but it is consistent with previous observations (13) that patients diagnosed with pulmonary TSC often have otherwise mild TSC, often delaying diagnosis. We found the median age to onset of pulmonary symptoms (20 years), and the subsequent diagnosis of LAM (25 years) to be earlier than previously reported (2,3), although the delay between onset and diagnosis (6 years) was similar. The earlier age of diagnosis found in our small group of patients may be a chance nding, it is possible that due to their genetic predisposition to this disease, patients with TSC develop LAM at a younger age than patients without TSC, but Johnson (4) reported the mean age of onset of LAM to be 34 years. We observed the range of recognized presentations of LAM, but we also observed two rare manifestations. Patient14 in the current series presented with cardiac tamponade and a haemopericardium, pericardial e usion in LAM has only been reported once (14), in a patient without TSC. Patient four su ered a massive pulmonary haemorrhage resulting in sudden death. To our knowledge this has not been previously reported in the literature. LAM is described as a generalised lung disease a ecting all zones of the lung equally (15). This may not always be true in TSC: patient 9 had severe persistent disease for several years until she underwent a lobectomy, following which she has remained asymptomatic for 38 years. Since few patients with LAM and TSC have been described, it is di cult to summarize its associations with the other clinical stigmata of TSC. In Castro s study (3) eight out of nine of patients su ered from severe renal disease with haemorrhage into AML prior to diagnosis of their lung complications, suggesting a possible association between symptomatic renal disease and LAM. We looked for other clinical associations of TSC in this series of 21 patients and compared them with the 395 patients known to the Bath TSC clinic, to see if there was any phenotype at high risk of developing LAM. If this proved to be the case it might form a basis for screening highrisk patients. There was no signi cant di erence between the two groups in the prevalence of any other manifestations of TSC including renal AML. We therefore propose that, at the present time, there are no prognostic factors that assist in predicting which individuals withtsc are at greatest risk of developing lung disease, but that it is rare in men and children. Treatment is predominantly symptomatic. Johnson (4) suggested that air ow obstruction was often helped by inhaled b-agonists, anecdotally this was not the case in our patients. In our patients there was a variable response to hormone therapy. Lung transplantation is another treatment option but the presence of systemic disease and occasionally of previous pleurodesis limits the number of patients in whom this is a viable option. In three previously reported cases LAM has recurred in a transplanted lung (16^18). We do agree with Johnson that the most pressing issue in the management of LAM is to determine the place of hormonal therapy. LAM, although rare, is an important cause of mortality in TSC. Shepherd et al. (19) found lung disease to be the fourth most common cause of early mortality in TSC. Average duration of survival from the time of diagnosis LAM was reported to be 4?8 years in 1971 (2). More recent studies estimate survival to be nearer to 10 years and there are reports of apparent spontaneous resolution. In this study the clinical course of LAM intsc was extremely variable. Screening for LAM in patients withtsc remains controversial. There are no factors that can be used to identify those patients at greatest risk of developing LAM, other than being female. HRCT is likely to be the most sensitive tool for recognising LAM, but it is not known whether changes are consistently seen on chest X-ray or HRCT before the development of symptoms. It would presently be unwise to screen all females with TSC for evidence of LAM until further data on the investigation, natural history and e cacy of early intervention are available.there is an argument for considering screening female patients withtsc for lung disease before they undergo anaesthesia or y, as these circumstances may precipitate acute problems. We do not know the best method to do this. Acknowledgements We would like to thank the Bath Unit for Research into Paediatrics, thetuberous Sclerosis Association and Cow & Gate for nancial support, as well as the patients who agreed to help us, and their clinicians who did likewise and thetuberous Sclerosis association for asking a ected individuals to help us. Without their help this sort of study would never have been possible. REFERENCES 1. Webb DW, Fryer AE,Osborne JP.On the morbidity associated with tuberous sclerosis: a population study. Dev Med Child Neurol 1996; 38:146 ^ Dwyer JM, Hickie JB, Garvin J. Pulmonary tuberous sclerosis. Report of three patients and a review of the literature.q JMedNew Series 1971; 157: 115 ^125.
7 LYMPHANGIOLEIOMYOMATOSIS ANDTUBEROUS SCLEROSIS Castro M, Shepherd CW, Gomez M, et al. Pulmonary tuberous sclerosis.chest 1995; 107: 189 ^ Jonhson S. Lymphangioleiomyomatosis: clinical features, management and basic mechanisms.thorax 1999; 54: 254 ^ Miller WT, Cornog JL, Sullivan MA. Lymphangiomyomatosis; clinical-roentgenologic-pathologic syndrome. Am J Roentgenol 1971; 111: 565^ Sobonya RE, Quan SF, Fleishman JS. Pulmonary Lymphangioleiomyomatosis: Quantitative analysis of Lesions Producing Air ow Limitation. Hum Pathol 1985; 16: 112 2^ Eliasson A, PhillipsYY, Tenholder MF. Treatment of lymphangioleiomyomatosis: a meta-analysis.chest 1989; 196: 1352^ Roach ES, Gomez MR, Northrup H. Tuberous Sclerosis Complex Consensus Conference: revised clinical diagnostic criteria. JChild Neurol 1998; 13: 624 ^ Duckett JG, Lazarus A, White KM. Cutaneous masses, rib lesions and chylous pleural e ussion in a 20-year old man. Chest 1990; 97: 1227^ Bowen J, Beasley SW. Rare pulmonary manifestations of tuberous sclerosis in children. Ped Pulmonol 1997; 23: 114 ^ Dawson J. Pulmonary tuberous sclerosis.q J Med 1954; 54: 113^ Foresti V,Casati O, Zubani R, etal.chylous pleural e usion in tuberous sclerosis. Respiration 1990; 57: 398^ Slingerland JM, Grossman RF, Chamberlain D, et al. Pulmonary manifestation in rst degree relatives. Thorax 1989; 44: 212^ Fahy J, Toner M, O Sullivan J, et al. Haemopericardium and cardiac tamponade complicating pulmonary lymphangioleiomyoma.thorax 1991; 46: Kalassian KG, Doyle R, Kao P, et al.lymphangioleiomyomatosis: new insights. Am J Respir Crit Care Med 1997; 155: 1183 ^ Nine JS,Yousem SA, Paradis IL, et al.lymphangioleiomyomatosis: recurrence after lung transplantation.j Heart LungTransplant1994; 13: 714 ^ O Brien JD, Lium JH, Parosa JF, et al. Lymphangiomyomatosis recurrence in the allograft after single-lung transplantation. Am J Respir Crit Care Med 1995; 151: 2033^ Bittman I, DoseTB, Muller C, et al. Lymphangiolieomyomatosis: recurrence after single lung transplantation. Hum Pathol 1997; 28: 1420^ Shepherd CW, Gomez MR, Lie JT, et al. Causes of death in patients with tuberous sclerosis. Mayo Clin Proc 1991; 66: 792^796.
Clinical History. 29 yo woman with polyhydramnios Cardiac mass at fetal ultrasound At 35 weeks, newborn died 30 minutes after delivery
 CASE 1 a Clinical History 29 yo woman with polyhydramnios Cardiac mass at fetal ultrasound At 35 weeks, newborn died 30 minutes after delivery Interface between tumor and normal myocardium Smaller well-demarcated
CASE 1 a Clinical History 29 yo woman with polyhydramnios Cardiac mass at fetal ultrasound At 35 weeks, newborn died 30 minutes after delivery Interface between tumor and normal myocardium Smaller well-demarcated
Living with rare lung disease LYMPHANGIOLEIOMYOMATOSIS (LAM): The Patient Perspective. Gill Hollis, Edinburgh January 2010
 Living with rare lung disease LYMPHANGIOLEIOMYOMATOSIS (LAM): The Patient Perspective Gill Hollis, Edinburgh January 2010 LAM Basics Disease of the lungs and lymphatics Affects women Causes progressive
Living with rare lung disease LYMPHANGIOLEIOMYOMATOSIS (LAM): The Patient Perspective Gill Hollis, Edinburgh January 2010 LAM Basics Disease of the lungs and lymphatics Affects women Causes progressive
Lymphangioleiomyomatosis (LAM)
 Lymphangioleiomyomatosis (LAM) is a rare lung condition that mainly affects women of childbearing age. Although it has been reported in men, it is extremely rare. It is estimated that three to five in
Lymphangioleiomyomatosis (LAM) is a rare lung condition that mainly affects women of childbearing age. Although it has been reported in men, it is extremely rare. It is estimated that three to five in
Coexistence of Lymphangioleiomyomatosis and Angiomyolipomas in a Patient of Tuberous Sclerosis Complex: a case report
 Chin J Radiol 2003; 28: 329-333 329 Coexistence of Lymphangioleiomyomatosis and Angiomyolipomas in a Patient of Tuberous Sclerosis Complex: a case report FENG-CHI HSIEH 1 KAO-LANG LIU 1 YIH-LEONG CHANG
Chin J Radiol 2003; 28: 329-333 329 Coexistence of Lymphangioleiomyomatosis and Angiomyolipomas in a Patient of Tuberous Sclerosis Complex: a case report FENG-CHI HSIEH 1 KAO-LANG LIU 1 YIH-LEONG CHANG
LAM 101. Lymph-angio-leiomyo-matosis
 LAM 101 Lymph-angio-leiomyo-matosis Charlie Strange, MD Division of Pulmonary and Critical Care Medicine Medical University of South Carolina Dr. Strange has been a grant recipient in LAM from the NIH,
LAM 101 Lymph-angio-leiomyo-matosis Charlie Strange, MD Division of Pulmonary and Critical Care Medicine Medical University of South Carolina Dr. Strange has been a grant recipient in LAM from the NIH,
Diagnosing TSC by Making Clinical Connections
 Diagnosing TSC by Making Clinical Connections TSC = tuberous sclerosis complex. Diagnosing tuberous sclerosis complex: MORE CLUES Definite Diagnosis of Tuberous Sclerosis Complex (TSC) Possible Diagnosis
Diagnosing TSC by Making Clinical Connections TSC = tuberous sclerosis complex. Diagnosing tuberous sclerosis complex: MORE CLUES Definite Diagnosis of Tuberous Sclerosis Complex (TSC) Possible Diagnosis
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka
 A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
A Rare Case of Lymphangioleiomyomatosis in Sri Lanka Author s Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) Sachini Seneviratne (4) Samadara Nakandala (5) Rathnayake R.M.D.H.M - (1) (2)
Lymphangioleiomyomatosis in a 55 Year Old Female -A Rare Case Report
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 7 (2016) pp. 148-152 Journal homepage: http://www.ijcmas.com Case Study http://dx.doi.org/10.20546/ijcmas.2016.507.014
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 5 Number 7 (2016) pp. 148-152 Journal homepage: http://www.ijcmas.com Case Study http://dx.doi.org/10.20546/ijcmas.2016.507.014
Tuberous Sclerosis Complex
 Tuberous Sclerosis Complex A successful transition from the bench to the bedside Mary Kay Koenig, MD The University of Texas Medical School at Houston Children s Memorial Hermann Hospital University of
Tuberous Sclerosis Complex A successful transition from the bench to the bedside Mary Kay Koenig, MD The University of Texas Medical School at Houston Children s Memorial Hermann Hospital University of
L ymphangioleiomyomatosis (LAM) is generally described
 875 ORPHAN LUNG DISEASE Emerging clinical picture of lymphangioleiomyomatosis M M Cohen, S Pollock-BarZiv, S R Johnson... See end of article for authors affiliations... Correspondence to: Dr M M Cohen,
875 ORPHAN LUNG DISEASE Emerging clinical picture of lymphangioleiomyomatosis M M Cohen, S Pollock-BarZiv, S R Johnson... See end of article for authors affiliations... Correspondence to: Dr M M Cohen,
Teleconference on Tuberous Sclerosis Complex (TSC) Research October 28 th, 2008 and November 11 th, 2008
 Wong 1 Teleconference on Tuberous Sclerosis Complex (TSC) Research October 28 th, 2008 and November 11 th, 2008 Sponsored by the Tuberous Sclerosis Alliance Faculty Participants: Elizabeth Henske, MD,
Wong 1 Teleconference on Tuberous Sclerosis Complex (TSC) Research October 28 th, 2008 and November 11 th, 2008 Sponsored by the Tuberous Sclerosis Alliance Faculty Participants: Elizabeth Henske, MD,
Everolimus (Votubia) for angiomyolipoma associated with tuberous sclerosis complex or sporadic lymphangioleiomyomatosis first line or post surgery
 Everolimus (Votubia) for angiomyolipoma associated with tuberous sclerosis complex or sporadic lymphangioleiomyomatosis first line or post surgery April 2011 This technology summary is based on information
Everolimus (Votubia) for angiomyolipoma associated with tuberous sclerosis complex or sporadic lymphangioleiomyomatosis first line or post surgery April 2011 This technology summary is based on information
Tuberous sclerosis with giant renal angiomyolipoma and sclerotic skeletal lesions in a geriatric patient: role of imaging
 International Journal of Research in Medical Sciences Nagaraju RM et al. Int J Res Med Sci. 2015 Aug;3(8):2145-2149 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Case Report DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150346
International Journal of Research in Medical Sciences Nagaraju RM et al. Int J Res Med Sci. 2015 Aug;3(8):2145-2149 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Case Report DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20150346
Imaging of tuberous sclerosis complex
 Imaging of tuberous sclerosis complex Poster No.: C-0388 Congress: ECR 2015 Type: Educational Exhibit Authors: M. V. Vu#kovi#, N. Menkovic, A. Petkovic, S. Ognjanovic, 1 2 1 1 1 1 1 1 J. Markov, M. Ilic,
Imaging of tuberous sclerosis complex Poster No.: C-0388 Congress: ECR 2015 Type: Educational Exhibit Authors: M. V. Vu#kovi#, N. Menkovic, A. Petkovic, S. Ognjanovic, 1 2 1 1 1 1 1 1 J. Markov, M. Ilic,
Tuberous Sclerosis A Radiological Perspective
 November 2001 Tuberous Sclerosis A Radiological Perspective Heather Brandling-Bennett, Harvard Medical School, Year III Tuberous Sclerosis Also referred to as Bourneville s disease or tuberous sclerosis
November 2001 Tuberous Sclerosis A Radiological Perspective Heather Brandling-Bennett, Harvard Medical School, Year III Tuberous Sclerosis Also referred to as Bourneville s disease or tuberous sclerosis
Clinical experience of lymphangioleiomyomatosis in the UK
 1052 Division of Respiratory Medicine, University of Nottingham, City Hospital, Nottingham NG5 1PB, UK S R Johnson A E Tattersfield Correspondence to: Dr S Johnson, Division of Therapeutics, University
1052 Division of Respiratory Medicine, University of Nottingham, City Hospital, Nottingham NG5 1PB, UK S R Johnson A E Tattersfield Correspondence to: Dr S Johnson, Division of Therapeutics, University
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Herczegfalvi Ágnes. Tuberous sclerosis. Case history. SE. II. sz. Gyermekklinika. Budapest, Febr
 Herczegfalvi Ágnes Tuberous sclerosis Case history SE. II. sz. Gyermekklinika Budapest, Febr. 2016. Case history 1. GD. DOB: 05-03-1989 Pre and perinatal history: normal His development was normal till
Herczegfalvi Ágnes Tuberous sclerosis Case history SE. II. sz. Gyermekklinika Budapest, Febr. 2016. Case history 1. GD. DOB: 05-03-1989 Pre and perinatal history: normal His development was normal till
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
CURIOSITY IS A LIFELONG CONDITION TOO
 CURIOSITY IS A LIFELONG CONDITION TOO If you or a loved one has been diagnosed with tuberous sclerosis complex or TSC this booklet will help you get answers. It can also help if you think you may have
CURIOSITY IS A LIFELONG CONDITION TOO If you or a loved one has been diagnosed with tuberous sclerosis complex or TSC this booklet will help you get answers. It can also help if you think you may have
Chronic Lung Disease in vertically HIV infected children. Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre
 Chronic Lung Disease in vertically HIV infected children Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre Natural history of HIV in vertically infected children without and with
Chronic Lung Disease in vertically HIV infected children Dr B O Hare Senior Lecturer in Paediatrics and Child Health, COM, Blantyre Natural history of HIV in vertically infected children without and with
Lung Cancer Case Study
 Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
MANAGEMENT RECOMMENDATIONS
 1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
Tuberculosis - clinical forms. Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases
 Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
Tuberculosis - clinical forms Dr. A.Torossian,, M.D., Ph. D. Department of Respiratory Diseases 1 TB DISEASE Primary Post-primary (Secondary) Common primary forms Primary complex Tuberculosis of the intrathoracic
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW
 SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
SCLERODERMA LUNG DISEASE: WHAT THE PATIENT SHOULD KNOW Lung disease can be a serious complication of scleroderma. The two most common types of lung disease in patients with scleroderma are interstitial
Surgical treatment of bullous lung disease
 Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
Surgical treatment of bullous lung disease PD POTGIETER, SR BENATAR, RP HEWITSON, AD FERGUSON Thorax 1981 ;36:885-890 From the Respiratory Clinic, Groote Schuur Hospita', and Departments of Medicine, Anaesthetics,
CURIOSITY IS A LIFELONG CONDITION TOO
 CURIOSITY IS A LIFELONG CONDITION TOO If you or a loved one has been diagnosed with tuberous sclerosis complex or TSC this booklet will help you get answers. It can also help if you think you may have
CURIOSITY IS A LIFELONG CONDITION TOO If you or a loved one has been diagnosed with tuberous sclerosis complex or TSC this booklet will help you get answers. It can also help if you think you may have
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Recurrent Spontaneous Pneumothorax in a 42 Years Old Woman With Pulmonary Lymphangioleiomyomatosis: Insights and Pitfalls of the Surgical Treatment
 Elmer Case Report ress Recurrent Spontaneous Pneumothorax in a 42 Years Old Woman With Pulmonary Lymphangioleiomyomatosis: Insights and Pitfalls of the Surgical Treatment Kyriakos Spiliopoulos a, e, Angeliki
Elmer Case Report ress Recurrent Spontaneous Pneumothorax in a 42 Years Old Woman With Pulmonary Lymphangioleiomyomatosis: Insights and Pitfalls of the Surgical Treatment Kyriakos Spiliopoulos a, e, Angeliki
Exacerbations. Ronald Dahl, Aarhus University Hospital, Denmark
 1st WAO Allied Health Session - Asthma: Diagnosi Exacerbations Ronald Dahl, Aarhus University Hospital, Denmark The health professional that care for patients with asthma exacerbation must be able to Identificafy
1st WAO Allied Health Session - Asthma: Diagnosi Exacerbations Ronald Dahl, Aarhus University Hospital, Denmark The health professional that care for patients with asthma exacerbation must be able to Identificafy
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
Rare Association of Childhood Bronchiectasis with VACTERL Anomalies; a Case Report
 Rare Association of Childhood Bronchiectasis with VACTERL Anomalies; a Case Report Authors Details: Author's Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) R.M.D.H.M.RATHNAYAKE (1)(2)(3)(4)
Rare Association of Childhood Bronchiectasis with VACTERL Anomalies; a Case Report Authors Details: Author's Details: (1) Dushantha Madegedara (2) Asela Rasika Bandara (3) R.M.D.H.M.RATHNAYAKE (1)(2)(3)(4)
Bilateral Renal Angiomyolipomas with Invasion of the Renal Vein: A Case Report
 Case Study TheScientificWorldJOURNAL (2008) 8, 145 148 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2008.29 Bilateral Renal Angiomyolipomas with Invasion of the Renal Vein: A Case Report C. Blick, N. Ravindranath,
Case Study TheScientificWorldJOURNAL (2008) 8, 145 148 TSW Urology ISSN 1537-744X; DOI 10.1100/tsw.2008.29 Bilateral Renal Angiomyolipomas with Invasion of the Renal Vein: A Case Report C. Blick, N. Ravindranath,
Tuberous sclerosis complex is a genetic
 60 Journal of the association of physicians of india vol 62 december, 2014 Case Reports A Case Report of Tuberous Sclerosis in Two Generations Chandrakala *, Sharanagouda Patil **, KY Guruprasad *** Abstract
60 Journal of the association of physicians of india vol 62 december, 2014 Case Reports A Case Report of Tuberous Sclerosis in Two Generations Chandrakala *, Sharanagouda Patil **, KY Guruprasad *** Abstract
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than
 TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
TBLB is not recommended as the initial biopsy option in cases of suspected IPF and is unreliable in the diagnosis of rare lung disease (other than PAP) BAL is not required as a diagnostic tool in patients
General History. Sex : female Birth Date : 68 / 02 /10 Date of Admission : 91 /08 / 04
 General History Sex : female Birth Date : 68 / 02 /10 Date of Admission : 91 /08 / 04 Chief Complain Epigastric pain with bloody vomitus for 1 day Present Illness This 22 year-old girl is a case of tuberous
General History Sex : female Birth Date : 68 / 02 /10 Date of Admission : 91 /08 / 04 Chief Complain Epigastric pain with bloody vomitus for 1 day Present Illness This 22 year-old girl is a case of tuberous
A cross sectional study of renal involvement in tuberous sclerosis
 480 Med Genet 1996;33:480-484 A cross sectional study of renal involvement in tuberous sclerosis Departnent of Clinical Genetics, Ashley Wing, St James' University Hospital, Beckett Street, Leeds LS9 7TF,
480 Med Genet 1996;33:480-484 A cross sectional study of renal involvement in tuberous sclerosis Departnent of Clinical Genetics, Ashley Wing, St James' University Hospital, Beckett Street, Leeds LS9 7TF,
Patient Perspectives on Management of Pneumothorax in Lymphangioleiomyomatosis*
 CHEST Original Research LYMPHANGIOLEIOMYOMATOSIS Patient Perspectives on Management of Pneumothorax in Lymphangioleiomyomatosis* Lisa R. Young, MD; Khalid F. Almoosa, MD, FCCP; Stacey Pollock-BarZiv, PhD;
CHEST Original Research LYMPHANGIOLEIOMYOMATOSIS Patient Perspectives on Management of Pneumothorax in Lymphangioleiomyomatosis* Lisa R. Young, MD; Khalid F. Almoosa, MD, FCCP; Stacey Pollock-BarZiv, PhD;
COPD. Breathing Made Easier
 COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
Management of Pneumothorax in Lymphangioleiomyomatosis* Effects on Recurrence and Lung Transplantation Complications
 Original Research LYMPHANGIOLEIOMYOMATOSIS Management of Pneumothorax in Lymphangioleiomyomatosis* Effects on Recurrence and Lung Transplantation Complications Khalid F. Almoosa, MD; Jay H. Ryu, MD; Jose
Original Research LYMPHANGIOLEIOMYOMATOSIS Management of Pneumothorax in Lymphangioleiomyomatosis* Effects on Recurrence and Lung Transplantation Complications Khalid F. Almoosa, MD; Jay H. Ryu, MD; Jose
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Asthma in Children with Sickle Cell Disease
 December 18, 2018 Asthma in Children with Sickle Cell Disease Robyn Cohen, MD, MPH Director, Division of Pediatric Pulmonology and Allergy Associate Professor of Pediatrics Boston University/Boston Medical
December 18, 2018 Asthma in Children with Sickle Cell Disease Robyn Cohen, MD, MPH Director, Division of Pediatric Pulmonology and Allergy Associate Professor of Pediatrics Boston University/Boston Medical
Cystic Fibrosis. Jennifer McDaniel, BS, RRT-NPS
 Cystic Fibrosis Jennifer McDaniel, BS, RRT-NPS Overview Cystic fibrosis is the most common fatal, inherited disease in the U. S. CF results from a defective autosomal recessive gene One copy of gene =
Cystic Fibrosis Jennifer McDaniel, BS, RRT-NPS Overview Cystic fibrosis is the most common fatal, inherited disease in the U. S. CF results from a defective autosomal recessive gene One copy of gene =
Pediatric High-Resolution Chest CT
 Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Pediatric High-Resolution Chest CT Alan S. Brody, MD Professor of Radiology and Pediatrics Chief, Thoracic Imaging Cincinnati Children s s Hospital Cincinnati, Ohio, USA Pediatric High-Resolution CT Short
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
A. Chachaj, K. Drozdz, M. Chabowski, P. Dziegiel, I. Grzegorek, A. Wojnar, P. Jazwiec, A. Szuba
 53 Lymphology 45 (2012) 53-57 CHYLOPERITONEUM, CHYLOTHORAX AND LOWER EXTREMITY LYMPHEDEMA IN WOMAN WITH SPORADIC LYMPHANGIOLEIOMYOMATOSIS SUCCESSFULLY TREATED WITH SIROLIMUS: A CASE REPORT A. Chachaj,
53 Lymphology 45 (2012) 53-57 CHYLOPERITONEUM, CHYLOTHORAX AND LOWER EXTREMITY LYMPHEDEMA IN WOMAN WITH SPORADIC LYMPHANGIOLEIOMYOMATOSIS SUCCESSFULLY TREATED WITH SIROLIMUS: A CASE REPORT A. Chachaj,
TACO CASE STUDIES RTC JUNE Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner
 TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
Lymphangioleiomyomatosis (LAM) is a rare
 Eur Respir J 2010; 35: 14 26 DOI: 10.1183/09031936.00076209 CopyrightßERS Journals Ltd 2010 European Respiratory Society guidelines for the diagnosis and management of lymphangioleiomyomatosis S.R. Johnson*,
Eur Respir J 2010; 35: 14 26 DOI: 10.1183/09031936.00076209 CopyrightßERS Journals Ltd 2010 European Respiratory Society guidelines for the diagnosis and management of lymphangioleiomyomatosis S.R. Johnson*,
Case 1: Question. 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule
 HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
HRCT WORK SHOP Case 1 Case 1: Question 1.1 What is the main pattern of this HRCT? 1. Intralobular line 2. Groundglass opacity 3. Perilymphatic nodule Case 1: Question 1.2 What is the diagnosis? 1. Hypersensitivity
Chronic Obstructive Pulmonary Disease
 Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Chronic Obstructive Pulmonary Disease 07 Contributor Dr David Tan Hsien Yung Definition, Diagnosis and Risk Factors for (COPD) Differential Diagnoses Goals of Management Management of COPD THERAPY AT EACH
Asthma Tutorial. Trainer MRW. Consider the two scenarios, make an attempt at the questions, what guidance have you used?
 Registrar: LG PR RS Topic Asthma and COPD Asthma Tutorial Trainer MRW Date of Tutorial 18 th Jan 2007 Objectives of the tutorial How to diagnose What investigations and when Treatment guidelines QoF Criteria
Registrar: LG PR RS Topic Asthma and COPD Asthma Tutorial Trainer MRW Date of Tutorial 18 th Jan 2007 Objectives of the tutorial How to diagnose What investigations and when Treatment guidelines QoF Criteria
From the Archives of the AFIP
 AFIP ARCHIVES 803 CME FEATURE See accompanying test at http:// www.rsna.org /education /rg_cme.html LEARNING OBJECTIVES FOR TEST 6 After reading this article and taking the test, the reader will be able
AFIP ARCHIVES 803 CME FEATURE See accompanying test at http:// www.rsna.org /education /rg_cme.html LEARNING OBJECTIVES FOR TEST 6 After reading this article and taking the test, the reader will be able
Quality Care Innovation lead clinician for integrated respiratory service georges ng* man kwong
 Working in partnership Quality Care Innovation lead clinician for integrated respiratory service georges ng* man kwong chest physician pronounced ning qualified 1990 chief clinical information officer
Working in partnership Quality Care Innovation lead clinician for integrated respiratory service georges ng* man kwong chest physician pronounced ning qualified 1990 chief clinical information officer
Eosinophils and effusion: a clinical conundrum
 Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Ruth Sobala, Kevin Conroy, Hilary Tedd, Salem Elarbi kevin.peter.conroy@gmail.com Respiratory Dept, Queen Elizabeth Hospital, Gateshead, UK. Eosinophils and effusion: a clinical conundrum Case report A
Renal manifestations of tuberous sclerosis complex: Incidence, prognosis, and predictive factors
 http://www.kidney-international.org & 2006 International Society of Nephrology original article Renal manifestations of tuberous sclerosis complex: Incidence, prognosis, and predictive factors SK Rakowski
http://www.kidney-international.org & 2006 International Society of Nephrology original article Renal manifestations of tuberous sclerosis complex: Incidence, prognosis, and predictive factors SK Rakowski
Prolonged treatment of pulmonary sarcoidosis
 Thorax (1967), 22, 519. Prolonged treatment of pulmonary sarcoidosis with corticosteroids CLIFFORD HOYLE, HUGH SMYLLIE1, AND DAVID LEAK From King's College Hospital, London The results are described of
Thorax (1967), 22, 519. Prolonged treatment of pulmonary sarcoidosis with corticosteroids CLIFFORD HOYLE, HUGH SMYLLIE1, AND DAVID LEAK From King's College Hospital, London The results are described of
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Breathlessness in advanced disease. February 2017
 Breathlessness in advanced disease February 2017 Breathlessness Managing breathlessness in primary care Chronic breathlessness Acute exacerbation of breathlessness Breathlessness at end of life Breathlessness
Breathlessness in advanced disease February 2017 Breathlessness Managing breathlessness in primary care Chronic breathlessness Acute exacerbation of breathlessness Breathlessness at end of life Breathlessness
Uroradiology For Medical Students
 Uroradiology For Medical Students Lesson 8 Computerized Tomography 2 American Urological Association Objectives In this lesson you will: Gain more experience reading CT images Learn how computer generated
Uroradiology For Medical Students Lesson 8 Computerized Tomography 2 American Urological Association Objectives In this lesson you will: Gain more experience reading CT images Learn how computer generated
S and secondary spontaneous pneumothorax. Primary
 Secondary Spontaneous Pneumothorax Fumihiro Tanaka, MD, Masatoshi Itoh, MD, Hiroshi Esaki, MD, Jun Isobe, MD, Youichiro Ueno, MD, and Ritsuko Inoue, MD Department of Thoracic and Cardiovascular Surgery,
Secondary Spontaneous Pneumothorax Fumihiro Tanaka, MD, Masatoshi Itoh, MD, Hiroshi Esaki, MD, Jun Isobe, MD, Youichiro Ueno, MD, and Ritsuko Inoue, MD Department of Thoracic and Cardiovascular Surgery,
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Referring for specialist respiratory input. Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL
 Referring for specialist respiratory input Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL Respiratory Specialist- who? GPSI Community Team Secondary Care Respiratory physician and
Referring for specialist respiratory input Dr Melissa Heightman Consultant respiratory physician, UCLH,WH, CNWL Respiratory Specialist- who? GPSI Community Team Secondary Care Respiratory physician and
Surgical Management of Pulmonary Metastases. Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital
 Surgical Management of Pulmonary Metastases Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital Introduction Lungs 2 nd most common site of metastatic deposition
Surgical Management of Pulmonary Metastases Dr AG Jacobs Principal Specialist Dept Cardiothoracic Surgery Steve Biko Academic Hospital Introduction Lungs 2 nd most common site of metastatic deposition
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Four cases of pneumomediastinum
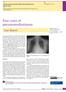 Avinash Aujayeb, Jonathan Miller, Mark Weatherhead, David Cooper aujayeb@doctors.net.uk North Tyneside General Hospital, Northumbria Health Care Foundation Trust, North Shields, UK. Four cases of pneumomediastinum
Avinash Aujayeb, Jonathan Miller, Mark Weatherhead, David Cooper aujayeb@doctors.net.uk North Tyneside General Hospital, Northumbria Health Care Foundation Trust, North Shields, UK. Four cases of pneumomediastinum
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
New Hope for Management of Tuberous Sclerosis. Anil Kapoor, MD, FRCSC Professor of Surgery (Urology), McMaster University Hamilton, Ontario
 New Hope for Management of Tuberous Sclerosis Anil Kapoor, MD, FRCSC Professor of Surgery (Urology), McMaster University Hamilton, Ontario Tuberous Sclerosis Complex (TSC) Incidence 1:6000 Genetic disorder
New Hope for Management of Tuberous Sclerosis Anil Kapoor, MD, FRCSC Professor of Surgery (Urology), McMaster University Hamilton, Ontario Tuberous Sclerosis Complex (TSC) Incidence 1:6000 Genetic disorder
Spectrum of Cystic Lung Disease and its Mimics. Kathleen Jacobs MD and Elizabeth Weihe MD UC San Diego Medical Center, Department of Radiology
 Spectrum of Cystic Lung Disease and its Mimics Kathleen Jacobs MD and Elizabeth Weihe MD UC San Diego Medical Center, Department of Radiology No Financial Disclosures Learning Objectives 1. Review the
Spectrum of Cystic Lung Disease and its Mimics Kathleen Jacobs MD and Elizabeth Weihe MD UC San Diego Medical Center, Department of Radiology No Financial Disclosures Learning Objectives 1. Review the
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Dr.Sivaramakrishnan PICU KKCTH
 Dr.Sivaramakrishnan PICU KKCTH CASE 1 11/2 year old female child Known wheezer on intermittent bronchodilators Admitted with h/o cough for 2 days Increased work of breathing for 1 day Afebrile/sick looking
Dr.Sivaramakrishnan PICU KKCTH CASE 1 11/2 year old female child Known wheezer on intermittent bronchodilators Admitted with h/o cough for 2 days Increased work of breathing for 1 day Afebrile/sick looking
Chronic obstructive pulmonary disease
 Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
Chronic obstructive pulmonary disease By: Dr. Fatima Makee AL-Hakak () University of kerbala College of nursing Out lines What is the? Overview Causes of Symptoms of What's the difference between and asthma?
REFERRAL GUIDELINES RESPIRATORY
 REFERRAL GUIDELINES RESPIRATORY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
REFERRAL GUIDELINES RESPIRATORY Referral Form: The GP Referral Template is the preferred referral tool (previously known as the Victorian Statewide Referral Form) GP Referral Template This tool is housed
Pneumothorax After Air Travel in Lymphangioleiomyomatosis, Idiopathic Pulmonary Fibrosis, and Sarcoidosis
 CHEST Original Research Pneumothorax After Air Travel in Lymphangioleiomyomatosis, Idiopathic Pulmonary Fibrosis, and Sarcoidosis PNEUMOTHORAX Angelo M. Taveira-DaSilva, MD, PhD; Dara Burstein, RN, CRNP;
CHEST Original Research Pneumothorax After Air Travel in Lymphangioleiomyomatosis, Idiopathic Pulmonary Fibrosis, and Sarcoidosis PNEUMOTHORAX Angelo M. Taveira-DaSilva, MD, PhD; Dara Burstein, RN, CRNP;
PENETRANCE ACTIONABILITY SIGNIFICANCE/BURDEN OF DISEASE NEXT STEPS. YES (Proceed to Stage II) YES ( 1 of above)
 Stage I: Rule-Out Dashboard GENE/GENE PANEL: TSC1, TSC2 DISORDER: Tuberous Sclerosis Complex (TSC) HGNC ID: 12362, 12363 OMIM ID: 191100, 613254 ACTIONABILITY 1. Is there a qualifying resource, such as
Stage I: Rule-Out Dashboard GENE/GENE PANEL: TSC1, TSC2 DISORDER: Tuberous Sclerosis Complex (TSC) HGNC ID: 12362, 12363 OMIM ID: 191100, 613254 ACTIONABILITY 1. Is there a qualifying resource, such as
Pneumothorax and Chest Tube Problems
 Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES
 ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
ERDHEIM-CHESTER DISEASE LUNG & HEART ISSUES GIULIO CAVALLI, M.D. INTERNAL MEDICINE AND CLINICAL IMMUNOLOGY IRCCS SAN RAFFAELE HOSPITAL VITA-SALUTE SAN RAFFAELE UNIVERSITY MILAN, ITALY cavalli.giulio@hsr.it
The adult with recurrent breathlessness. A/Prof Gerald Chua Medicine NTFGH
 The adult with recurrent breathlessness A/Prof Gerald Chua Medicine NTFGH Dyspnoea Subjective experience of breathing discomfort Variable among individuals with apparently similar degrees of impairment
The adult with recurrent breathlessness A/Prof Gerald Chua Medicine NTFGH Dyspnoea Subjective experience of breathing discomfort Variable among individuals with apparently similar degrees of impairment
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
SWISS SOCIETY OF NEONATOLOGY. A rare cause of neonatal seizures
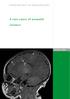 SWISS SOCIETY OF NEONATOLOGY A rare cause of neonatal seizures October 2006 2 Hagmann C, Robertson NJ, Centre for Perinatal Brain Research, Institute for Women s Health, University College London, London
SWISS SOCIETY OF NEONATOLOGY A rare cause of neonatal seizures October 2006 2 Hagmann C, Robertson NJ, Centre for Perinatal Brain Research, Institute for Women s Health, University College London, London
Combined Pulmonary Fibrosis and Emphysema - A Case Series
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 1 Ver. III (January. 2017), PP 15-19 www.iosrjournals.org Combined Pulmonary Fibrosis and Emphysema
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 1 Ver. III (January. 2017), PP 15-19 www.iosrjournals.org Combined Pulmonary Fibrosis and Emphysema
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES
 JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
JOINT CHRONIC OBSTRUCTIVE PULMONARY DISEASE (COPD) MANAGEMENT GUIDELINES Authors Dr Ian Benton Respiratory Consultant COCH Penny Rideal Respiratory Nurse COCH Kirti Burgul Respiratory Pharmacist COCH Pam
Autosomal Dominant Polycystic Kidney Disease
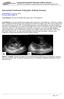 Case Studies [1] July 01, 2014 By Amar Udare, MBBS [2] Case History: 45-year-old female with vague pain in the abdomen. Case History: A 45-year-old female presented with vague pain in the abdomen. A USG
Case Studies [1] July 01, 2014 By Amar Udare, MBBS [2] Case History: 45-year-old female with vague pain in the abdomen. Case History: A 45-year-old female presented with vague pain in the abdomen. A USG
Osseous disease in patients with pulmonary sarcoidosis and musculoskeletal symptoms
 RESPIRATORY MEDICINE (2000) 94, 228±232 doi:10.1053/rmed.1999.0709, available online at http://www.idealibrary.com on Osseous disease in patients with pulmonary and musculoskeletal symptoms A. F. SHORR,
RESPIRATORY MEDICINE (2000) 94, 228±232 doi:10.1053/rmed.1999.0709, available online at http://www.idealibrary.com on Osseous disease in patients with pulmonary and musculoskeletal symptoms A. F. SHORR,
10/17/2016. Nuts and Bolts of Thoracic Radiology. Objectives. Techniques
 Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Nuts and Bolts of Thoracic Radiology October 20, 2016 Carleen Risaliti Objectives Understand the basics of chest radiograph Develop a system for interpreting chest radiographs Correctly identify thoracic
Hepatic manifestations of tuberous sclerosis complex: a genotypic and phenotypic analysis
 Clin Genet 2012: 82: 552 557 Printed in Singapore. All rights reserved Short Report 2012 John Wiley & Sons A/S. Published by Blackwell Publishing Ltd CLINICAL GENETICS doi: 10.1111/j.1399-0004.2012.01845.x
Clin Genet 2012: 82: 552 557 Printed in Singapore. All rights reserved Short Report 2012 John Wiley & Sons A/S. Published by Blackwell Publishing Ltd CLINICAL GENETICS doi: 10.1111/j.1399-0004.2012.01845.x
COPD Bronchiectasis Overlap Syndrome.
 COPD Bronchiectasis Overlap Syndrome. John R Hurst 1, J Stuart Elborn 2, and Anthony De Soyza 3 on Behalf of the BRONCH-UK Consortium (D Bilton, J Bradley, JS Brown, J Duckers, F Copeland, A Floto, J Foweraker,
COPD Bronchiectasis Overlap Syndrome. John R Hurst 1, J Stuart Elborn 2, and Anthony De Soyza 3 on Behalf of the BRONCH-UK Consortium (D Bilton, J Bradley, JS Brown, J Duckers, F Copeland, A Floto, J Foweraker,
Problem Based Learning Session. Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days.
 Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
AMERICAN THORACIC SOCIETY DOCUMENTS
 AMERICAN THORACIC SOCIETY DOCUMENTS Lymphangioleiomyomatosis Diagnosis and Management: High-Resolution Chest Computed Tomography, Transbronchial Lung Biopsy, and Pleural Disease Management An Official
AMERICAN THORACIC SOCIETY DOCUMENTS Lymphangioleiomyomatosis Diagnosis and Management: High-Resolution Chest Computed Tomography, Transbronchial Lung Biopsy, and Pleural Disease Management An Official
Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma
 Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Article ID: WMC005047 ISSN 2046-1690 Bilateral Chest X-Ray Shadowing and Bilateral leg lesions - A case of Pulmonary Kaposi Sarcoma Peer review status: No Corresponding Author: Dr. Mohammad Fawad Khattak,
Retroperitoneal Lymphangiomyoma in a Patient with Pulmonary Lymphangiomyomatosis: Case Report 1
 Retroperitoneal Lymphangiomyoma in a Patient with Pulmonary Lymphangiomyomatosis: Case Report 1 Jung Wook Seo, M.D., Yoon Jun Hwang, M.D., Soo Young Kim, M.D., Yoon Hee Han, M.D., Mi Young Kim, M.D., Yong
Retroperitoneal Lymphangiomyoma in a Patient with Pulmonary Lymphangiomyomatosis: Case Report 1 Jung Wook Seo, M.D., Yoon Jun Hwang, M.D., Soo Young Kim, M.D., Yoon Hee Han, M.D., Mi Young Kim, M.D., Yong
Opinion 20 March 2013
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 20 March 2013 VOTUBIA 2.5 mg, tablet B/30 (CIP: 219 475-8) VOTUBIA 5 mg, tablet B/30 (CIP: 219 476-4) Applicant: NOVARTIS
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 20 March 2013 VOTUBIA 2.5 mg, tablet B/30 (CIP: 219 475-8) VOTUBIA 5 mg, tablet B/30 (CIP: 219 476-4) Applicant: NOVARTIS
Starship Paediatric Respiratory and Sleep Medicine Department Outpatient Referral Criteria General Principles
 Starship Paediatric Respiratory and Sleep Medicine Department Outpatient Referral Criteria General Principles This document provides guidance for elective outpatient referrals to the Starship Tertiary
Starship Paediatric Respiratory and Sleep Medicine Department Outpatient Referral Criteria General Principles This document provides guidance for elective outpatient referrals to the Starship Tertiary
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
CHEST INJURY PULMONARY CONTUSION
 CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
CHEST INJURY PULMONARY CONTUSION Introduction Pulmonary contusion refers to blunt traumatic lung parenchymal injury which results in oedema and haemorrhaging into alveolar spaces. It may also result in
The 1-year survival rate approaches 80% for patients
 Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Lung Transplantation for Respiratory Failure Resulting From Systemic Disease Frank A. Pigula, MD, Bartley P. Griffith, MD, Marco A. Zenati, MD, James H. Dauber, MD, Samuel A. Yousem, MD, and Robert J.
Causes of mortality in individuals with tuberous sclerosis complex
 DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Causes of mortality in individuals with tuberous sclerosis complex SAM AMIN 1 ANDREW LUX 1 NUALA CALDER 2 MATTHEW LAUGHARNE 3 JOHN OSBORNE 2 FINBAR
DEVELOPMENTAL MEDICINE & CHILD NEUROLOGY ORIGINAL ARTICLE Causes of mortality in individuals with tuberous sclerosis complex SAM AMIN 1 ANDREW LUX 1 NUALA CALDER 2 MATTHEW LAUGHARNE 3 JOHN OSBORNE 2 FINBAR
Clinical review of pulmonary disease caused by Mycobacterium xenopi
 Thorax 1983;38: 373-377 Clinical review of pulmonary disease caused by Mycobacterium xenopi MJ SMITH, KM CITRON From the Cardiothoracic Institute, Brompton Hospital, London ABSTRACT Mycobacterium xenopi
Thorax 1983;38: 373-377 Clinical review of pulmonary disease caused by Mycobacterium xenopi MJ SMITH, KM CITRON From the Cardiothoracic Institute, Brompton Hospital, London ABSTRACT Mycobacterium xenopi
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1).
 PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
PATIENT CHARACTERISTICS AND PREOPERATIVE DATA (ecrf 1). 1 Inform Consent Date: / / dd / Mmm / yyyy 2 Patient identifier: Please enter the 6 digit Patient identification number from your site patient log
