Herpes B Virus Exposure Protocol
|
|
|
- Carmella Rice
- 6 years ago
- Views:
Transcription
1 Herpes B Virus Exposure Protocol ( This protocol has been revised based on new recommendations published in Clinical Infectious Diseases 2002; 35: which supercedes recommendations published in Clinical Infectious Diseases 1995; 20: ) Purpose: Scope/Risk: To provide appropriate first aid, risk assessment, and treatment for staff members who have been exposed to Herpes B virus. Herpes B Virus is enzootic among monkeys of the genus macaca (macaque). Monkeys of this genus infected with Herpes B virus show minimal morbidity from the virus. Infected macaque monkey saliva, blood, and other body fluids can be infectious to humans. Humans who become infected with Herpes B virus often develop encephalitis with a mortality rate that is approximately 80%. Infection in humans is rare and occurs as a result of exposure to macaque monkeys and secretions and tissue from macaque monkeys. The incubation period in humans ranges from 2 days to 5 weeks after exposure. Symptoms range from local rash to systemic viral symptoms and CNS symptoms (see section on post exposure counseling for listing of early, intermediate, and late signs and symptoms). Humans have become infected after exposure to infectious tissues and body fluids including ocular, oral, genital, CNS, and CSF tissues and fluids. Cell cultures from macaque kidneys are also potentially infectious. Exposure to peripheral blood from macaque monkeys has not been reported to cause infection in humans. However, exposures involving blood from macaque monkeys will be considered in the risk assessment for evaluation and treatment for this policy. Routes of infection include bites, scratches, exposure to tissue culture media, tissue obtained from autopsy, needlestick injuries, scratches from contact with cages, mucous membrane splashes. There has been one reported human to human transmission. Certain types of exposures pose a greater risk of infection. Deep puncture wounds that are difficult to clean, inadequately cleaned wounds, wounds on the face, eye, neck, and thorax. Exposures to the head and thorax can lead to quicker progression of CNS symptoms. Definition of occupational exposure: All staff who handle macaque monkey tissue, cell cultures and blood are at risk of exposure to Herpes B virus. Exposure can occur through monkey bites, percutaneous injury, non-intact skin and mucous membrane contact. 1
2 Prevention of Exposure: All monkey tissue cultures, blood, saliva, and other body fluids should be considered infectious. The most critical period for prevention of Herpes B virus infection is the first few minutes after exposure. Education of staff at initial orientation regarding the risk of B-virus infection is done by Biosafety officer. Post Exposure Evaluation: 1. Staff should immediately decontaminate even before coming to OHS: Wash intact skin with soap and water for several minutes Open wounds should be soaked and scrubbed with bleach (1:10 dilution) or Betadine for 15 minutes. Eyes or mucous membrane exposure flush eyes at eye wash station for at least 15 minutes. Thorough cleansing of the wound within minutes of exposure decreases the risk that viral contamination will progress to infection. Although detergents, bleach, and betadine can inactivate the virus, the mechanical action of scrubbing or irrigating the wound for at least 15 minutes to wash away virus is probably the most important aspect of the cleansing procedure. 2. Staff should report to OHS during regular business hours of Mon Fri from 8:30AM to 4:30PM. For off hours, holidays and weekends, the STIK beeper should be paged following the established STIK beeper process. 3. OHS Management of B Virus Exposure Initial evaluation: Exposed Staff: 1. Assess the adequacy of wound cleaning done prior to evaluation and perform wound assessment. 2. Wound cleaning procedure above should be repeated in OHS. This should be done regardless of the staff s report of cleaning the wound to ensure adequate time and procedure for wound cleansing has taken place. Mucous Membrane exposure: flush eyes or mucous membranes at eyewash station or sterile saline solution for 15 minutes. Skin exposure: wash skin thoroughly with a solution containing detergent soap (povodine iodine, chlorhexidine) for 15 minutes. Consider washing skin with bleach 1:10 dilution followed by detergent solution for 15 minutes. 2
3 3. Determine date, time, location, description of the injury, description of exposure and source material. 4. Physical exam with focus on neurological symptoms. 5. Evaluate general health and date of last Td Booster. 6. Determine need for PEP (see below) and antibiotics to prevent wound infection. Non Human Primate Source Risk Assessment: 1. Veterinarian where animal, tissue, or body fluid originated should be contacted for risk assessment of source monkey. Lab PI will have contact information regarding source tissue. 4. Wound culture and serology testing: Consider obtaining baseline serologic testing and viral cultures of bite wounds and/or exposed mucosa. Serology Testing: 1. Blood sample should be drawn in a red top tube(must be 5-7 cc tube). 2. Properly label tube with staff information (name, ID, collection date) 3. Complete National B Virus Resource Center lab form. 4. Store in refrigerator prior to transport to Lab control for shipping. Samples may be stored in our refrigerator over night and over the weekend prior to spinning and processing should an exposure occur after hours. Virology Swab Testing: 1. Culture wound and/or mucous membrane exposed areas only after wound/mucous membranes cleaned following above process. 2. Swab each wound/mucous membrane site with a separate sterile cotton swab (must be plastic or wooden handle. Available in kit with viral transport media tube). 3. Place swab in vial of sterile viral transport media (plastic tube with red cap, kits in store room). Viral transport media kits available from General Stores. Kit contains sterile swab and plastic culture tube containing transport media. 4. Sample must be stored at < 60 degrees C until shipping. Samples may be stored in our freezer over night and over the weekend prior to processing should an exposure occur after hours. 5. Complete National B Virus Resource Center lab form. 3
4 Instructions on Sample Collection & Handling from the NIH B Virus Resource Lab can be found at end of protocol. Lab control has been given copy of Sample collection and handling instructions for the National B Virus Resource Lab. 5. Post Exposure Prophylaxis: If post-exposure prophylaxis is indicated treatment should begin within hours of exposure. Antiviral treatment should be Valacyclovir 500mg 2 tabs p.o. TID X 14 days. If a pregnant woman were exposed, consult with OB/GYN physician. PEP if given should be Acyclovir 800mg 5X a day for 14 days. Prophylaxis Recommended: 1. Skin exposure* (with loss of skin integrity) or mucosal exposure (with or without injury) to a high risk source (macaque that is ill, immunocompromised, or known to be shedding virus or that has lesions compatible with B virus disease) 2. Inadequately cleaned skin exposure (with loss of skin integrity) or mucosal exposure (with or without injury). 3. Laceration of the head, neck, or torso 4. Deep puncture bite 5. Needlestick associated with tissue or fluid from the nervous system, lesions suspicious for B virus, eyelids, or mucosa. 6. Puncture or laceration after exposure to objects (a) contaminated either with fluid from monkey oral or genital lesions or with nervous system tissues, or (b) known to contain B virus. 7. A post cleansing culture is positive for B virus. Prophylaxis considered: 1. Mucosal splash that has been adequately cleaned 2. Laceration (with loss of skin integrity) that has been adequately cleaned. 3. Needlestick involving blood from an ill or immunocompromised macaque. 4. Puncture or laceration occurring after exposure to (a) objects contaminated with body fluid (other than from a lesion), or (b) potentially infected cell culture. Prophylaxis Not Recommended: 1. Skin exposure in which the skin remains intact. 2. Exposure associated with nonmacaque species of nonhuman primates. 4
5 Review Pros and Cons of antiviral treatment with exposed employee: 1. Pros: The initiation of valacyclovir therapy within 24 hours after exposure to B virus prevents death among animals. 2. Cons: The initiation of valacyclovir therapy within hours of exposure may prevent or modify symptomatic B virus disease. Infection with B virus is quite rare relative to the number of possible exposures There are no controlled studies that document the ability of immediate empirical therapy to prevent infection or symptomatic B virus infection in humans. Acyclovir therapy can suppress viral shedding and seroconversion, which may make diagnosis more difficult. 6. Post Exposure Counseling: Include the following information in post-exposure counseling with exposed employees: 1. Inform employee of incubation period which may be as short as 2 days and as long as 5 weeks. 2. Discuss risk of infection of exposure incident. 3. Review pros and cons of antiviral treatment 4. Review side effects of antiviral medications Review signs and symptoms of B virus infection: 1. Early Symptoms (inconsistently present) Vesicular eruptions or ulceration at or near the exposure site Severe pain or itching at the exposure site Regional lymphadenopathy 2. Intermediate Manifestations (Inconsistently present) Fever Numbness, paresthesia, or other neuresthesias at or near the exposure site and with or without proximal progression. Muscle weakness or paralysis in the exposed extremity Conjunctivitis Persistent hiccups 3. Late Manifestations (avoidable with early therapy) 5
6 7. Post Exposure Follow Up: Sinusitis Neck stiffness Headache lasting greater that 24 hours Brain stem findings: diplopia, dysarthria, dysphagia, dizziness, gross-hemiparesis, cerebellar signs with ataxia, crossed sensory loss, cranial nerve palsies, drop attacks. Altered mentation Other signs compatible with CNS impairment or viral encephalitis including urinary retention, respiratory failure, convulsion, twitching, hemiparesis, hemiplegia, other localized neurological signs, progressive ascending paralysis, or coma. Exposed staff will be followed closely in OHS on a weekly basis for at least 2 months post exposure. Review signs and symptoms of infection, monitor wound, monitor compliance with PEP and side effects. Follow grid below for follow up blood work schedule. Staff member will be advised to follow up with OHS immediately if any signs and symptoms suggestive of B-virus infection develop. Treatment with antiviral therapy and referral to ID specialist may be necessary and will be arranged on a case by case basis. Development of signs and symptoms of B Virus infection warrants prompt referral to ID specialist. No PEP PEP Baseline 2 Weeks 4 weeks 3 months Culture and Repeat Serology serology per testing policy Culture and serology per policy; CBC, diff, BUN, Creatinine, lytes CBC, Diff, BUN, Creatinine, lytes Repeat serology testing. If initial culture wound culture positive, perform cultures from conjunctivae, oropharynx, and any unhealed skin lesions. Repeat Serology testing 6
7 References: CDC (Centers for Disease Control and Prevention) Guidelines for the Prevention of Herpesvirus simiae (B Virus) Infection in Monkey Handlers. Morbidity and Mortality Weekly Report (MMWR) 36 (41): , ; October 23, Cohen, Jeffrey I., et al. Recommendations for Prevention of and Therapy for Exposure to B Virus (Ceropithecine Herpesvirus 1). Clinical Infectious Diseases 2002; 35: CME Resource. Zoonotic Diseases. Prevention and Nursing Care. January 2001, Vol 73, No.2. Holmes, et. al. Guidelines for the Prevention and Treatment of B-virus Infections in Exposed Persons. Clinical Infectious Diseases 1995; 20: Cercopithecine herpesvirus 1 (B Virus) infection resulting from ocular exposure. NOISE, May Publication No Reviewed 11/27/02. Revised: 6/16/03 7
SAFETY & HEALTH REQUIREMENTS FOR USE OF MATERIALS DERIVED FROM NHPS
 Introduction SAFETY & HEALTH REQUIREMENTS FOR USE OF MATERIALS DERIVED FROM NHPS 1. Experimentation with NHP-derived samples (cell cultures, tissues, body fluids or other wastes) may expose NUS staff and
Introduction SAFETY & HEALTH REQUIREMENTS FOR USE OF MATERIALS DERIVED FROM NHPS 1. Experimentation with NHP-derived samples (cell cultures, tissues, body fluids or other wastes) may expose NUS staff and
Cercopithecine Herpesvirus-1
 Cercopithecine Herpesvirus-1 B Virus Information for Researchers Cheryl S. Barbanel, MD, MBA, MPH, FACOEM 3/6/07 What is B Virus? B Virus (BV) is a common pathogen in monkeys of the genus Macaca including
Cercopithecine Herpesvirus-1 B Virus Information for Researchers Cheryl S. Barbanel, MD, MBA, MPH, FACOEM 3/6/07 What is B Virus? B Virus (BV) is a common pathogen in monkeys of the genus Macaca including
To provide the guidelines for the management of healthcare workers who have had an occupational exposure to blood and/or body fluids.
 TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
TITLE/DESCRIPTION: MANAGEMENT OF OCCUPATIONAL EXPOSURE TO HBV, HCV, and HIV INDEX NUMBER: EFFECTIVE DATE: APPLIES TO: ISSUING AUTHORITY: 01/01/2009 01/01/2013 All GCC Countries GULF COOPERATION COUNCIL
SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison
 SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
SIV/SHIV SIV/SHIV Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals
Exposure. What Healthcare Personnel Need to Know
 Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
Information from the Centers for Disease Control and Prevention National Center for Infectious Diseases Divison of Healthcare Quality Promotion and Division of Viral Hepatitis For additional brochures
EXPOSURE (HIV/HEPATITIS) BLOOD & BODY FLUIDS
 Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Page(s): 1 of 11 PURPOSE To set a standardized procedure to ensure that employees are evaluated in a consistent and timely manner.. POLICY A. The treatment of Team Member exposure to bloodborne pathogens
Effective Date: 6/10/2013 Review Date: 6/10/2016
 Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Policy Title: Sterilization and Disinfection of Patient-Care Items Policy Number: 11 6.2.2. Examples of useful items to maintain in the office sterilization log are as following: o Date and time of cycle
Clinical Education Initiative OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS. Antonio E. Urbina, MD
 Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Clinical Education Initiative Support@ceitraining.org OCCUPATIONAL POST- EXPOSURE PROPHYLAXIS Antonio E. Urbina, MD 5/22/2013 Occupational Post-Exposure Prophylaxis [Video Transcript] 00:00:15 - [Tony]
Management of Workplace Exposure to Blood-borne Pathogens
 Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Management of Workplace Exposure to Blood-borne Pathogens 11/22/2017 Management of Workplace Exposure to Blood-borne Pathogens BY SOLYMOLE KURUVILLA, PHD, RN, ACNP-BC DIRECTOR, OCCUPATIONAL HEALTH SERVICES
Exposure. Blood. Department of Health & Human Services
 Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Blood What Health-Care Workers Need to Know Department of Health & Human Services OCCUPATIONAL EXPOSURES TO BLOOD Introduction Health-care workers are at risk for occupational exposure to bloodborne
Exposure to Nonhuman Primates: Situation, Reference and Intervention Guide INSTITUT NATIONAL DE SANTÉ PUBLIQUE DU QUÉBEC
 Exposure to Nonhuman Primates: Situation, Reference and Intervention Guide INSTITUT NATIONAL DE SANTÉ PUBLIQUE DU QUÉBEC Professional Practice Guide Exposure to Nonhuman Primates: Situation, Reference
Exposure to Nonhuman Primates: Situation, Reference and Intervention Guide INSTITUT NATIONAL DE SANTÉ PUBLIQUE DU QUÉBEC Professional Practice Guide Exposure to Nonhuman Primates: Situation, Reference
Blood and Body Fluid Exposure
 Blood and Body Fluid Exposure Infection Prevention and Control Contents Policy... 1 Purpose... 1 Scope/Audience... 1 Definitions... 2 Associated documents... 2 1.1 Indications for BBFE reporting... 2 1.2
Blood and Body Fluid Exposure Infection Prevention and Control Contents Policy... 1 Purpose... 1 Scope/Audience... 1 Definitions... 2 Associated documents... 2 1.1 Indications for BBFE reporting... 2 1.2
Management of Exposure to Needlestick Injuries & Body Fluids
 Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Management of Exposure to Needlestick Injuries & Body Fluids Clinical S.O.P. No.:28 Compiled by: Approved by: Review date: November 2016 DOCUMENT HISTORY Version Detail of purpose / change Author / edited
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison
 Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison 1.0 Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about
This is risky. Rabies. Are you at risk?
 This is risky. Rabies Are you at risk? Are you at risk of rabies? You are at risk if you are in contact with potentially rabid animals: t Laboratory workers, veterinarians t Animal control workers, animal
This is risky. Rabies Are you at risk? Are you at risk of rabies? You are at risk if you are in contact with potentially rabid animals: t Laboratory workers, veterinarians t Animal control workers, animal
Bloodbourne Pathogens (BBP) Occupational Post-Exposure Chemophrophylaxis
 Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Bloodbourne Pathogens (BBP) Audience: All personnel in the. Purpose: The purpose of this document is to establish UTMB policy for the initiation of prophylaxis after occupational exposure to the human
Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids
 Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids August 2004 Table Of Contents Protocol - Management of Needlestick and Mucous Membrane Exposures to Blood/Body Fluids Assessment
Management of Needlestick and Mucous Membrane Exposures To Blood/Body Fluids August 2004 Table Of Contents Protocol - Management of Needlestick and Mucous Membrane Exposures to Blood/Body Fluids Assessment
Bloodborne Pathogens Training
 Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Bloodborne Pathogens Training OSHA S Bloodborne Pathogen Standard 29CFR 1910.1030 Employers must: Develop an Exposure Control Plan (ECP) that details their Bloodborne Pathogens (BBP) Program Provide employees
Needlestick and Splash Exposure Flow Chart Page 1 Clinical Practice Guidelines
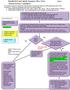 Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Needlestick and Splash Exposure Flow Chart Page 1 If ANY student experiences a needlestick or splash exposure ANY time of day/night, they need to page #11709 which will be forwarded to: (**in the event
Personal protective equipment (PPE) requirements for personnel working with non-human primates at UT-Austin Version 3 09/07/18
 This ARC guideline has been written to clearly communicate current standards for the facility users. Questions should be directed to Nachi Shukla (512/232-2043) or Dr. Glen Otto (512/471-2392). Personal
This ARC guideline has been written to clearly communicate current standards for the facility users. Questions should be directed to Nachi Shukla (512/232-2043) or Dr. Glen Otto (512/471-2392). Personal
Diphtheria rev Jan 2018
 rev Jan 2018 Infectious Agent Toxin-producing strains of Corynebacterium diphtheriae BASIC EPIDEMIOLOGY Transmission Direct person-to-person transmission by intimate respiratory and physical contact. Cutaneous
rev Jan 2018 Infectious Agent Toxin-producing strains of Corynebacterium diphtheriae BASIC EPIDEMIOLOGY Transmission Direct person-to-person transmission by intimate respiratory and physical contact. Cutaneous
Bloodborne Pathogens and Regulated Medical Waste
 Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
Bloodborne Pathogens and Regulated Medical Waste OSHA Ensure employees can safely perform their normal duties without undue health risks Bloodborne Pathogen (BBP) Standard developed to protect employees
MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3
 MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3 TITLE: POLICY: COMMUNICABLE DISEASE PREVENTION POLICIES Nursing students are required to adhere to College of Nursing policies on health
MONTANA STATE UNIVERSITY-BOZEMAN COLLEGE OF NURSING POLICY # D-3 TITLE: POLICY: COMMUNICABLE DISEASE PREVENTION POLICIES Nursing students are required to adhere to College of Nursing policies on health
5. Use of antibiotics, which disturbs balance of normal flora. 6. Poor nutritional status.
 Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
ALAT - Chapter 4. Occupational Health and Safety. Dr. Carrie Freed, DACLAM, DVM, MLAS
 ALAT - Chapter 4 Occupational Health and Safety Dr. Carrie Freed, DACLAM, DVM, MLAS Freed.36@osu.edu, 292-7319 OSHA Every institution with an animal research program must have an occupational health and
ALAT - Chapter 4 Occupational Health and Safety Dr. Carrie Freed, DACLAM, DVM, MLAS Freed.36@osu.edu, 292-7319 OSHA Every institution with an animal research program must have an occupational health and
RABIES PROTECTION PROGRAM
 Page 1 of 5 STANDARD OPERATING PROCEDURES (SOP) SCOPE Rabies is a virus causing an acute central nervous system infection, which is typically transmitted by introducing the rabies virus into open cuts
Page 1 of 5 STANDARD OPERATING PROCEDURES (SOP) SCOPE Rabies is a virus causing an acute central nervous system infection, which is typically transmitted by introducing the rabies virus into open cuts
2014 OSHA Blood-borne Pathogens (BBP) Update JHS Annual Mandatory Education
 2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
2014 OSHA Blood-borne Pathogens (BBP) Update 2014 JHS Annual Mandatory Education Objectives Discuss the epidemiology of Bloodborne Pathogens. List the statistics of HIV/AIDS cases Identify the correlation
Bloodborne Pathogens: Recognition and Treatment 2011
 Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
Bloodborne Pathogens: Recognition and Treatment 2011 Occupational Health Services at The Summit Rita M. Lopez, APRN-BC, MSN 751-4189 rlopez@krmc.org OBJECTIVES DEFINE Bloodborne Pathogen Exposure WHO must
One of your office personnel
 Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
Doug Campos-Outcalt, MD, MPA Department of Family and Community Medicine, University of Arizona College of Medicine, Phoenix HIV postexposure prophylaxis: Who should get it? CORRESPONDENCE Doug Campos-Outcalt,
The Bloodborne Pathogen Standard. An Overview
 The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
The Bloodborne Pathogen Standard An Overview The Standard l In 1990, OSHA (Occupational Safety and Health Administration), developed the Bloodborne Pathogen Standard to protect workers by limiting occupational
WVU Occupational Medicine Program for evaluation and treatment of persons exposed to Lentivirus Vectors
 Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Hazard Description: Lentivirus vector systems are derived from HIV and similar viruses because of being very effective at inserting genetic material into the genome of target cells. While most researchers
Bloodborne Pathogens. Montclair Kimberley Academy 1
 Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Bloodborne Pathogens Montclair Kimberley Academy 1 Introduction! Approximately 5.6 million workers in health care and other facilities are at risk of exposure to bloodborne pathogens such as human immunodeficiency
Policy S- 15 FLORIDA STATE UNIVERSITY COLLEGE OF NURSING BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN FOR NURSING STUDENTS
 TITLE: Policy S- 15 FLORIDA STATE UNIVERSITY COLLEGE OF NURSING BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN FOR NURSING STUDENTS Page 1 of 2 POLICY: The College of Nursing shall maintain a bloodborne pathogen
TITLE: Policy S- 15 FLORIDA STATE UNIVERSITY COLLEGE OF NURSING BLOODBORNE PATHOGEN EXPOSURE CONTROL PLAN FOR NURSING STUDENTS Page 1 of 2 POLICY: The College of Nursing shall maintain a bloodborne pathogen
Providence Medford Medical Center Pathology Department
 Providence Medford Medical Center Pathology Department Anatomic pathology services including histology, cytology and autopsies are offered through Providence Medford Medical Center Pathology Department.
Providence Medford Medical Center Pathology Department Anatomic pathology services including histology, cytology and autopsies are offered through Providence Medford Medical Center Pathology Department.
NEOMED ACADEMIC POLICY
 (A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
(A) PURPOSE The purpose of this Policy is to delineate the management of incidents of exposure to blood-borne pathogens that occur to students while they are in the educational setting. (B) SCOPE This
GENITAL HERPES. 81.1% of HSV-2 infections are asymptomatic or unrecognized. Figure 14 HSV-2 seroprevalence among persons aged years by sex.
 GENITAL HERPES Genital herpes is a chronic, lifelong, sexually transmitted disease caused by herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2). HSV-1 typically causes small, painful, fluid-filled,
GENITAL HERPES Genital herpes is a chronic, lifelong, sexually transmitted disease caused by herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2). HSV-1 typically causes small, painful, fluid-filled,
Alphaherpesvirinae. Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV)
 Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Alphaherpesvirinae Simplexvirus (HHV1&2/ HSV1&2) Varicellovirus (HHV3/VZV) HERPES SIMPLEX VIRUS First human herpesvirus discovered (1922) Two serotypes recognised HSV-1 & HSV-2 (1962) HSV polymorphism
Bloodborne Pathogens Training (OHS_BIO500) Course Material
 Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Introduction (OHS_BIO500) Course Material Welcome to the Bloodborne Pathogens (BBP) Training Course (OHS_BIO500). UAB Campus Employees whose job duties put them at increased risk for exposure to bloodborne
Bloodborne Pathogens Exposure Procedure
 Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Bloodborne Pathogens Exposure Procedure Background: Bloodborne pathogens are infectious microorganisms present in blood that can cause disease in humans. These pathogens include, but are not limited to,
Post Exposure Prophylaxis (PEP)
 Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
Post Exposure Prophylaxis (PEP) Occupational exposure Occupational exposure refers to exposure to potential blood-borne infections (HIV, HBV and HCV) that may occur in healthcare settings during performance
CMC Annual Review of BLOODBORNE DISEASES. Prevention of Transmission for School Staff
 CMC Annual Review of BLOODBORNE DISEASES Prevention of Transmission for School Staff Standard on Bloodborne Pathogens OSHA sets the standard of care We must have standards to follow in schools for everyone
CMC Annual Review of BLOODBORNE DISEASES Prevention of Transmission for School Staff Standard on Bloodborne Pathogens OSHA sets the standard of care We must have standards to follow in schools for everyone
UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HERPES SIMPLEX VIRUS EXPOSURE/INJURY RESPONSE PROTOCOL
 PLEASE POST THIS PAGE IN AREAS WHERE HERPES SIMPLEX VIRUS IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HERPES SIMPLEX VIRUS EXPOSURE/INJURY
PLEASE POST THIS PAGE IN AREAS WHERE HERPES SIMPLEX VIRUS IS USED IN RESEARCH LABORATORIES UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY HERPES SIMPLEX VIRUS EXPOSURE/INJURY
INITIAL EVALUATION AND MANAGEMENT FOLLOWING EXPOSURE TO BLOOD OR BODY FLUIDS
 Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
Page 1 of 11 Original Date of Issue: June 1991 Reviewed 2/96 5/97 11/98 11/99 5/01 5/02 12/05 Revised 9/95 5/97 5/00 7/02 3/06 6/08 6/10 The following are the procedures to be followed when a person sustains
El Paso - Ambulatory Clinic Policy and Procedure
 Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Regulation Reference: Title: NEEDLESTICK INJURIES/EXPOSURES TO BODY FLUIDS, CARE & FOLLOW UP Policy Number: EP 7.3 Effective Date: 6/2010 Policy Statement: A system is established and maintained to assure
Herpesvirus infections in pregnancy
 Herpesvirus infections in pregnancy Dr. med. Daniela Huzly Institute of Virology University Medical Center Freiburg, Germany Herpes simplex virus 1+2 Risk in pregnancy and at birth Primary infection in
Herpesvirus infections in pregnancy Dr. med. Daniela Huzly Institute of Virology University Medical Center Freiburg, Germany Herpes simplex virus 1+2 Risk in pregnancy and at birth Primary infection in
People with genital herpes require enough information and medication (when indicated) to self-manage their condition.
 Genital Herpes Summary of Guidelines Taken from: Guidelines for the Management of Genital Herpes in New Zealand 11th Edition - 2015 www.herpes.org.nz Genital Herpes Key Management Points Genital herpes
Genital Herpes Summary of Guidelines Taken from: Guidelines for the Management of Genital Herpes in New Zealand 11th Edition - 2015 www.herpes.org.nz Genital Herpes Key Management Points Genital herpes
Bloodborne Pathogens and Exposure Control
 Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
Bloodborne Pathogens and Exposure Control 2016 Information in the Exposure Control Plan The Bloodborne Pathogen Exposure Control Plan was developed to communicate information to you about: - Your risk
This SOP applies to all staff employed by NHS Greater Glasgow & Clyde and locum staff on fixed term contracts and volunteer staff.
 Page 1 of 9 Review SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients
Page 1 of 9 Review SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients
Bloodborne Pathogens Across the Continuum of Care Sue Sebazco, Arlington, Texas A Webber Training Teleclass
 Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Bloodborne Pathogens Across the Continuum of Care Objectives Sue Sebazco, RN, BS, CIC Infection Control/Employee Health Director Arlington, TX Pittsburg Mercy Health System skrystofiak@mercy.pmhs.org Define
Revised April WGH ER #5 Hospital Rd. Whitehorse Phone: (867) Outside of Whitehorse: Local Community Health Centre/Clinic/ER
 Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Where to access care Who to consult and when Please consult whenever questions arise on how to proceed with postexposure management and when exposure is beyond the scope of guidelines. Blood and Body Fluid
Environmental Health and Safety Offices BLOODBORNE PATHOGENS
 Environmental Health and Safety Offices BLOODBORNE PATHOGENS Purpose! Reduce / eliminate exposure potential Comply with Ohio s Public Employment Risk Reduction Act (reference OSHA) 2! Exposure Determination!
Environmental Health and Safety Offices BLOODBORNE PATHOGENS Purpose! Reduce / eliminate exposure potential Comply with Ohio s Public Employment Risk Reduction Act (reference OSHA) 2! Exposure Determination!
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1
 PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
PROCEDURE TITLE: BLOOD BORNE PATHOGENS EXPOSURE CONTROL PLAN PROCEDURE NO.: 5.21:1 RELATED POLICY: 5.21REV PAGE NO.: 1 OF 9 RESPONSIBLE ADMINISTRATOR(S): VPF&A/EHS EFECTIVE DATE: 07/11/14 NEXT REVIEW DATE:
Shingles Procedure. (IPC Policy Manual)
 Shingles Procedure (IPC Policy Manual) DOCUMENT CONTROL: Version: 1.1 Ratified by: Clinical Policy Approval Group Date ratified: 3 July 2018 Name of originator/author: Senior Clinical Nurse Specialist
Shingles Procedure (IPC Policy Manual) DOCUMENT CONTROL: Version: 1.1 Ratified by: Clinical Policy Approval Group Date ratified: 3 July 2018 Name of originator/author: Senior Clinical Nurse Specialist
Influenza-Associated Pediatric Mortality rev Jan 2018
 rev Jan 2018 Infectious Agent Influenza A, B or C virus BASIC EPIDEMIOLOGY Transmission Transmission occurs via droplet spread. After a person infected with influenza coughs, sneezes, or talks, influenza
rev Jan 2018 Infectious Agent Influenza A, B or C virus BASIC EPIDEMIOLOGY Transmission Transmission occurs via droplet spread. After a person infected with influenza coughs, sneezes, or talks, influenza
WOMENCARE. Herpes. Source: PDR.net Page 1 of 8. A Healthy Woman is a Powerful Woman (407)
 WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
Bloodborne Pathogens Exposure Control Plan
 Bloodborne Pathogens Exposure Control Plan Scope and Application This Bloodborne Pathogens Exposure Control Plan (ECP) is designed to minimize the potential for occupational exposure to bloodborne pathogens
Bloodborne Pathogens Exposure Control Plan Scope and Application This Bloodborne Pathogens Exposure Control Plan (ECP) is designed to minimize the potential for occupational exposure to bloodborne pathogens
Healthcare Professionals
 EMPLOYEE HEALTH Employee Health: Screening and immunization programs Counseling, follow up work restrictions Analysis and trending of occupational exposure incidents Assess risk for occupational exposure
EMPLOYEE HEALTH Employee Health: Screening and immunization programs Counseling, follow up work restrictions Analysis and trending of occupational exposure incidents Assess risk for occupational exposure
Blood Borne Pathogens. Becky Walch, R.N. Micheel Valdez, L.V.N.
 Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
Blood Borne Pathogens Becky Walch, R.N. Micheel Valdez, L.V.N. Examples of Blood Borne Pathogens Hepatitis B Hepatitis C Other Hepatitis HIV Hepatitis Hepatitis means inflammation of the liver. Hepatitis
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS
 NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
NEEDLESTICK INJURIES, BLOOD OR BODY FLUID EXPOSURE INFORMATION AND TEST FORMS Hepatitis B, Hepatitis C and HIV may be contracted through exposure to any body fluid, particularly blood. IMMEDIATE ACTION
2017 BLOODBORNE PATHOGENS
 2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
2017 BLOODBORNE PATHOGENS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE To have a basic understanding of bloodborne pathogens and the role of Greenwood School District 50 and OSHA.
VARICELLA. Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara
 VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
VARICELLA (Chicken pox) Infectious and Tropical Pediatric Division, Department of Child Health, Medical Faculty, University of Sumatera Utara Definition : Varicella is a common contagious disease caused
POLIOVIRUS EXPOSURE/INJURY RESPONSE PROTOCOL
 PLEASE POST THIS PAGE IN AREAS WHERE POLIOVIRUSES ARE USED UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY POLIOVIRUS EXPOSURE/INJURY RESPONSE PROTOCOL Organism or Agent:
PLEASE POST THIS PAGE IN AREAS WHERE POLIOVIRUSES ARE USED UNIVERSITY OF CALIFORNIA, SAN FRANCISCO ENVIRONMENT, HEALTH AND SAFETY/BIOSAFETY POLIOVIRUS EXPOSURE/INJURY RESPONSE PROTOCOL Organism or Agent:
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet. Instructions for Employees/Students:
 MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
MUSC Occupational Bloodborne Pathogen Protocol Off Campus Procedure Packet MUSC has established these protocols in accordance with the OSHA Bloodborne Pathogen Standard and Center for Disease Control recommendations
Bloodborne Pathogens. Kathleen Stefek, RN, MSN
 Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
Bloodborne Pathogens Kathleen Stefek, RN, MSN What are Bloodborne Pathogens? Infectious agents carried in the blood and other body fluids that are capable of infecting a host (people like you and me) with
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
B. Tasks and Procedures where employees, students or contractors can be exposed to bloodborne pathogens:
 Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Page 1 of 6 BLOODBORNE PATHOGEN PROGRAM INTRODUCTION The intended purpose of this document is to comply with OSHA s Occupational Exposures to Bloodborne Pathogens in Title 29 Code of Federal Regulations
Bloodborne Pathogens
 Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Bloodborne Pathogens Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Risk of exposure Protecting yourself from exposure through prevention Responding appropriately
Infection Control Standard Precautions. CDC Recommendations: Application of Standard Precautions for All Patients
 Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
Infection Control Standard Precautions Standard Precautions Hand Hygiene CDC Recommendations: Application of Standard Precautions for All Patients Component Personal Protective Equipment (PPE) Gloves Mask,
METHOTREXATE CLINICAL PRACTICE GUIDELINES FOR STAFF
 Mary Pack Arthritis Program METHOTREXATE CLINICAL PRACTICE GUIDELINES FOR STAFF Handling of premixed injectable Methotrexate (MTX) by employees who are pregnant, breast-feeding or attempting to reproduce
Mary Pack Arthritis Program METHOTREXATE CLINICAL PRACTICE GUIDELINES FOR STAFF Handling of premixed injectable Methotrexate (MTX) by employees who are pregnant, breast-feeding or attempting to reproduce
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison
 Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about the
Influenza Exposure Medical Response Guidance for the University of Wisconsin-Madison Instructions: Information in this guidance is meant to inform both laboratory staff and health professionals about the
Exposures at Non-MUSC Clinical Sites
 BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
BLOOD BORNE PATHOGEN EXPOSURE CHECKLIST Exposures at Non-MUSC Clinical Sites (Students on clinical rotations at Roper Hospital, Trident Hospital, Affiliated Local Clinical Sites, Out of Town Clinical Sites,
Varicella (Chickenpox) and Varicella Vaccines
 Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Varicella (Chickenpox) and Varicella Vaccines September 2018 Photographs and images included in this
Centers for Disease Control and Prevention National Center for Immunization and Respiratory Diseases Varicella (Chickenpox) and Varicella Vaccines September 2018 Photographs and images included in this
Greenwood School District 50 OSHA UPDATE BLOODBORNE PATHOGENS
 Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
Greenwood School District 50 OSHA UPDATE 2012 BLOODBORNE PATHOGENS TOPICS OSHA TERMS UPDATES HEPATITIS B HEPATITIS C HIV REPORTING AN EXPOSURE OBJECTIVES To have a basic understanding of bloodborne pathogens
SHASTA COUNTY Health and Human Services Agency
 FROM: 530 229 8447 TO: 15302293984 08/06/14 12:30 Pg 1 of 5 especially SHASTA COUNTY Health and Human Services Agency Public Health 2650RreslauerWay Redding, CA 96001-4297 (530) 229-8484 FAX (530) 225-3743
FROM: 530 229 8447 TO: 15302293984 08/06/14 12:30 Pg 1 of 5 especially SHASTA COUNTY Health and Human Services Agency Public Health 2650RreslauerWay Redding, CA 96001-4297 (530) 229-8484 FAX (530) 225-3743
RABIES Pr P ese e n se t n er e : J. J. K a K m a bo b n o a n a (M.B. B Ch C. h B; B M.Med e ) d
 RABIES Presenter: J.J. Kambona (M.B.Ch.B; M.Med) OBJECTIVES At the end of this session each student will be able to: 1. Define rabies. 2. Describe the epidemiology of rabies. 3. Describe the cause of rabies.
RABIES Presenter: J.J. Kambona (M.B.Ch.B; M.Med) OBJECTIVES At the end of this session each student will be able to: 1. Define rabies. 2. Describe the epidemiology of rabies. 3. Describe the cause of rabies.
RESEARCH WITH HIGHLY PATHOGENIC AVIAN INFLUENZA H5N1
 Page 1 of 8 RESEARCH WITH HIGHLY PATHOGENIC AVIAN INFLUENZA H5N1 The University of Pittsburgh has developed guidelines to establish a system of education and safeguards to ensure compliance with both the
Page 1 of 8 RESEARCH WITH HIGHLY PATHOGENIC AVIAN INFLUENZA H5N1 The University of Pittsburgh has developed guidelines to establish a system of education and safeguards to ensure compliance with both the
3/23/2016. Managing Bloodborne Pathogen Exposures. Managing Bloodborne Pathogen Exposures
 This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
This webinar begins at 11 a.m., Eastern. You will not hear anything over your telephone line until the program starts. If the system did not prompt you to enter your phone number and receive a call back,
ADMINISTRATIVE SERVICES MANUAL
 1 of 10 Purpose Scope University of Alaska Anchorage departments will develop plans and procedures to limit occupational exposure to blood and other potentially infectious materials (PIM) in compliance
1 of 10 Purpose Scope University of Alaska Anchorage departments will develop plans and procedures to limit occupational exposure to blood and other potentially infectious materials (PIM) in compliance
Management of sharps injuries in the healthcare setting
 Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
Link to this article online for CPD/CME credits Management of sharps injuries in the healthcare setting Anna Riddell, 1 Ioana Kennedy, 2 C Y William Tong 1 3 1 Department of Infection, Barts Health NHS
This SOP applies to all staff employed by NHS Greater Glasgow & Clyde and locum staff on fixed term contracts and volunteer staff.
 Page 1 of 8 SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients clinical
Page 1 of 8 SOP Objective To ensure that Healthcare Workers (HCWs) are aware of the actions and precautions necessary to minimise the risk of outbreaks and the importance of diagnosing patients clinical
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees
 BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
BLOODBORNE PATHOGENS Online Training for Buncombe County Public School Employees Buncombe County Public Schools require employees to receive annual training for Bloodborne Pathogens. This online training
2018 Infection Prevention and Control Update. Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC
 2018 Infection Prevention and Control Update Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC Influenza Influenza (1/19/18) Iowa activity IDPH has investigated 40 outbreaks in nursing homes 29 Deaths Activity will
2018 Infection Prevention and Control Update Lisa Caffery, MS,BSN,RN- BC,CIC, FAPIC Influenza Influenza (1/19/18) Iowa activity IDPH has investigated 40 outbreaks in nursing homes 29 Deaths Activity will
Polio (Paralytic and Non-paralytic
 Polio (Paralytic and Non-paralytic Infection) rev Jan 2018 Infectious Agent Poliovirus (genus Enterovirus) types, 1, 2, and 3. BASIC EPIDEMIOLOGY Transmission Poliovirus is transmitted by person-to-person
Polio (Paralytic and Non-paralytic Infection) rev Jan 2018 Infectious Agent Poliovirus (genus Enterovirus) types, 1, 2, and 3. BASIC EPIDEMIOLOGY Transmission Poliovirus is transmitted by person-to-person
Universal Precautions
 Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Universal Precautions emphasizes the need for workers and students to consider all blood and body fluids as potentially infected with HIV, HBV, and / or other blood-borne pathogens, and to adhere rigorously
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses
 Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Guidance for management of exposure events where there is a risk of transmission of blood borne viruses (HIV, Hepatitis B and Hepatitis C) in the community SUMMARY Where a child is thought to have had
Infection Control Manual. Table of Contents
 Infection Control Manual Policy Name Creutzfeldt-Jakob Disease (CJD) Policy Number Date this Version Effective April 2015 Responsible for Content Hospital Epidemiology I. Description Describes the recommendations
Infection Control Manual Policy Name Creutzfeldt-Jakob Disease (CJD) Policy Number Date this Version Effective April 2015 Responsible for Content Hospital Epidemiology I. Description Describes the recommendations
Important Information About Vaccinia (Smallpox) Vaccine Please Read This Carefully
 Important Information About Vaccinia (Smallpox) Vaccine Please Read This Carefully Introduction Vaccinia vaccine, previously known as smallpox vaccine, is highly effective in producing immunity to smallpox
Important Information About Vaccinia (Smallpox) Vaccine Please Read This Carefully Introduction Vaccinia vaccine, previously known as smallpox vaccine, is highly effective in producing immunity to smallpox
Bloodborne Pathogens. General
 Bloodborne Pathogens General Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Determine your risk of exposure Protect yourself from exposure through prevention
Bloodborne Pathogens General Session Objectives Identify bloodborne pathogens (BBPs) Understand how diseases are transmitted Determine your risk of exposure Protect yourself from exposure through prevention
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
Welcome to the UConn Health s Annual Bloodborne Pathogen Training Module
 Welcome to the UConn Health s Annual Module The Occupational Safety and Health Administration (OSHA) requires that any individual potentially exposed to human blood and/or body fluids in a clinical or
Welcome to the UConn Health s Annual Module The Occupational Safety and Health Administration (OSHA) requires that any individual potentially exposed to human blood and/or body fluids in a clinical or
43. Guidelines on Needle stick Injury
 43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
43. Guidelines on Needle stick Injury The following information is abstracted from the South African Department of Health guidelines entitled: Management of Occupational Exposure to the Human Immunodeficiency
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK)
 POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
POLICY ON BLOOD AND BODY FLUID EXPOSURE (NEEDLE STICK) Dated: January 1, 2018 Supersedes: Blood and Body Fluid Exposure (Needle stick) dated July 1, 2015 I. POLICY It is the policy of New York Medical
EMPLOYEE HEALTH TABLE OF CONTENTS
 EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
EMPLOYEE HEALTH TABLE OF CONTENTS PHYSICAL ASSESSMENT.2 REPORTING EMPLOYEE INFECTIONS...3 SUMMARY OF IMPORTANT RECOMMENDATIONS AND WORK RESTRICTIONS FOR PERSONNEL WITH INFECTIOUS DISEASES.4 HEPATITIS B
Communicable Diseases. Detection and Prevention
 Communicable Diseases Detection and Prevention Communicable Diseases Communicable Disease an infectious disease transmissible by direct contact (person to person) indirect means (body fluids, objects touched
Communicable Diseases Detection and Prevention Communicable Diseases Communicable Disease an infectious disease transmissible by direct contact (person to person) indirect means (body fluids, objects touched
Life Threatening Vocational Hazards Diseases and Toxins
 Life Threatening Vocational Hazards Diseases and Toxins INTRODUCTION What is the blood-borne pathogens standard? 29CFR 1910.1030 Who needs blood-borne pathogens (BBP) training? What content needs to be
Life Threatening Vocational Hazards Diseases and Toxins INTRODUCTION What is the blood-borne pathogens standard? 29CFR 1910.1030 Who needs blood-borne pathogens (BBP) training? What content needs to be
BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM
 Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Page 1 of 13 BLOODBORNE PATHOGENS FOR HEALTH CARE WORKERS CURRICULUM INTRODUCTION The attached materials will assist in teaching the information about bloodborne pathogens for health care workers as required
Information for Primary Care: Managing patients who require assessment for Ebola virus disease Updated 17 Oct 2014
 Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
Information for Primary Care: Managing patients who require assessment for Ebola virus This guidance is aimed at clinical staff undertaking direct patient care in primary care, including GP surgeries,
