Clinical Practice John E. Sutphin, MD, editor
|
|
|
- Brooke Allison
- 5 years ago
- Views:
Transcription
1 Clinical Practice John E. Sutphin, MD, editor Sulfur Mustard-Induced Ocular Surface Disorders Alireza Baradaran-Rafii, MD, 1 Medi Eslani, MD, 1 and Scheffer C. G. Tseng, MD, PhD 2 ABSTRACT Sulfur mustard is a vesicant agent with severe irritating effects on living tissues, including skin, mucous membranes, eyes, and respiratory tract. The eyes are the most susceptible tissue to mustard gas effects, and varying degrees of ocular involvement are seen in 75% to 90% of exposed individuals. Most cases resolve uneventfully; however, a minority of exposed patients will have a continuous process, which manifests clinically either as a persistent smoldering inflammation (chronic form) or late-onset lesions appearing many years after a variable silent period (delayed form). Distinctive features common to most cases with chronic involvement include chronic blepharitis, meibomian gland dysfunction, dry eye, limbal ischemia, limbal stem cell deficiency, aberrant conjunctival vessels, corneal neovascularization, and secondary degenerative changes, including lipid and amyloid deposition and corneal irregularity, thinning and scarring. Most cases can be managed with conservative measures, eg, preservative-free artificial tears, lubricants, and topical steroids. Punctal plugs or punctal cauterization is helpful in moderate and severe forms of injury. Surgical modalities, including lateral or medial tarsorrhaphies, amniotic membrane transplantation, lamellar or penetrating keratoplasty, and stem cell transplantation have been used. KEY WORDS chemical warfare agents, corneal burns, corneal transplantation, mustard gas, oxidative stress, sulfur mustard Accepted for publication May From the 1 Ophthalmic Research Center, Department of Ophthalmology, Labbafinejad Medical Center, Shahid Beheshti University of Medical Sciences, and 2 Ocular Surface Center, Ocular Surface Research and Education Foundation, Miami, Florida, USA. Dr. Tseng and his family are more than 5% shareholders of TissueTech. Inc., which owns US patents and on the method of preparation and clinical uses of human amniotic membrane and ProKera distributed by Bio-Tissue Inc. Other authors have no proprietary or commercial interests in any concept or product discussed in this article. Single-copy reprint requests to: Alireza Baradaran-Rafii, MD (address below). Corresponding author: Alireza Baradaran-Rafii, MD, Labbafinejad Medical Center, Department of Ophthalmology, Boostan 9 St., Pasdaran Ave., Tehran 16666, Iran. Tel-fax: alirbr@gmail.com Ethis Communications, Inc. The Ocular Surface ISSN: Baradaran-Rafii A, Eslani M, Tseng SCG. Sulfur mustard-induced ocular surface disorders. 2011;9(3): I. INTRODUCTION M ustard gas was first produced by Meyer in It was used initially as a vesicant agent for chemical warfare in World War I by the German army. 1,2 It is a vesicant agent with severe irritating effects on living tissues, including skin, mucous membranes, eyes, and respiratory tract. 3, 4 Because of its use as a weapon in World War I and in over 10 subsequent conflicts, including the Iraq-Iran war ( ), its properties became more widely known in the 20 th century. 3, 4 Its late-onset, progressively destructive effects were recognized years after its use. 5 A minority of exposed patients will develop late destructive ocular complications, which are usually progressive and permanent and can lead to reduction of visual acuity and even corneal blindness. 3, 4 The ubiquitous production, simple and cheap chemical synthesis, easy stockpiling, and toxic nature of this agent make it a worldwide threat. Because of its destructive properties, combined with the lack of an effective antidote, some experts have classified mustard gas as one of the most significant chemical warfare agents. 6-8 II. PHARMACOLOGY The mustard agent is a straw-colored, oily liquid and has the odor of onion, garlic, or mustard, hence its name. 9 It mainly consists of two chemical forms: sulfur mustard [S(CH2-CH2-Cl) 2 or (2,2 -dichlorethyl sulphide; HD)], and nitrogen mustard [N(CH2-CH2-Cl) or (N-methyl- 2,2 -dichlorodiethylamine; HN2)]. 2, 10 The former is longer acting and more commonly used in chemical warfare, but the latter is more toxic. 2, 4,5,11 The popular term mustard gas is a misnomer, as this agent actually appears as an aerosol of small oily droplets. 12 The toxicity of sulfur mustard (SM) as an incapacitating agent is of much greater importance than its capacity to kill via a lethal dose 50% (LD50). 12,13 The LD50 for humans is about 200 mg when the substance is swallowed, 4-5 g when it is applied to the bare skin over a long exposure time, and 1500 mg/min/m 3 when inhaled. 2,14 It is a stable compound in low temperatures, which can persist in clothing or on the ground for months. 3 On contact with human skin, 80% of the liquid evaporates and 20% penetrates; half of this remains in the skin and the other half is absorbed systemically. 2 Additionally, due to free hydrolization by the interface organs, SM causes systemic effects only at very high doses. 15 THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 / 163
2 OUTLINE I. Introduction II. Pharmacology III. Pathophysiology IV. Immunologic mechanisms V. Systemic manifestations A. Skin B. Respiratory tract C. Bone marrow D. Other organ damage VI. Ocular involvement A. Acute phase B. Chronic phase C. Pathologic findings D. Confocal microscopy VII. Initial management following sulfur mustard exposure VIII. Management of ocular injuries A. Acute phase B. Chronic phase 1. Medical treatment 2. Surgical intervention a. Tarsorrhaphy b. Amniotic membrane transplantation c. Stem cell transplantation d. Corneal transplantation 3. Treatment algorithm 4. Postoperative medical regimen and surgical outcome C. Novel and potential therapies for mustard gas injury IX. Summary The measurement of biochemical markers in aqueous humor is a tool for evaluating SM-induced damages even before the onset of clinical signs. The concentration of protein in aqueous humor increases 4-6 hours following exposure; although it decreases after 28 hours, it still remains higher than in non-exposed controls. This increase, together with the presence of cellular lymphocytic infiltration, is indicative of an inflammatory reaction. Aqueous humor glutathione at the very early stages of SM exposure may change in a similar pattern. 16,17 Alkylation products of SM with DNA and proteins (eg, hemoglobin and albumin), as well as its urinary metabolites, have proved to be useful targets for diagnosing SM exposure in humans. Urinary markers are readily accessible, although their rapid elimination limits their use for retrospective detection. Adducts with macromolecules such as proteins offer longer lasting (possibly up to several months) biological markers of exposure to SM. 23,24 The DNA adducts can also be detected in urine, processed skin, and blood samples III. PATHOPHYSIOLOGY Mustard gas damages viable tissues only, and the exact mechanism for this is not clear. Theories include liberation of intracellular hydrochloric acid, formation of new compounds acting as alkylating agents, and, finally, formation of oxidative derivatives, which collectively can lead to more cellular damage. 9,11,30-34 Mustard gas causes additional injury via skin and eye damage after absorption through the integument and the ocular surface; respiratory damage after inhalation; and systemic toxicity after ingestion or high exposures. As a result, it may further cause gastrointestinal, circulatory, and bone marrow toxicity. 34 Hence, the destructive effects of SM are not localized to the site of application, as remote cells and tissues also become affected. 3 The high sensitivity of the eye to SM is due to the readily accessible aqueous-mucous surface of the cornea and conjunctiva, as well as the high turnover rate and intense metabolic activity of corneal epithelial cells. 35 SM causes a cross-linking of the 2 complementary strands in the DNA molecule by a monofunctional alkylation of the nitrogenous bases. The major alkylating site of nucleic acids is the nitrogen residue of guanine. 36 The results are manifested in chromatid aberrations; inhibition of DNA, RNA, and protein synthesis; blocking of the cell s cycle in the G2-M phase; and, eventually, cell death. 2,37-40 SM tends to undergo intramolecular cyclization to create a hyperactive compound. 41 Conversion to this derivative is facilitated in an aqueous solution, which accounts for the sensitivity of mucosal tissues (such as in the eye) to its action. 42 The cyclic intermediate reacts with and alkylates electron-rich molecular structures, such as the sulfhydryl (-SH), amino (-NH2), carboxyl, hydroxyl, and primary phosphate groups of proteins and nucleic acids. 12,42-44 Additionally, the alkylated DNA activates poly-adp-ribose polymerase, which leads to cellular depletion of nicotinamide adenosine dinucleotide (NAD), thus inhibiting multiple reactions in the cell. 6,7 The depletion of NAD also leads to upregulation of the hexosemonophosphate shunt, which stimulates protease activity in the cell. These proteases are thought to play a role in blister formation, compounded by the death of multiple keratinocytes. 6,7,43 It also directly inhibits various glycolytic and respiratory enzymes, 36 impairs glucose uptake mechanisms, 45 and generates oxidative stress through the formation of free radicals. 2,46 Inhibition of cellular respiratory enzymes resulting in the formation of free radicals has been suggested as another pathophysiologic mechanism affecting predominantly proliferative epithelial cells in the ocular surface. 11 Evidence for oxidative stress in tissues exposed to SM or its analogs includes increased formation of reactive oxygen species and the presence of peroxidized lipid products and proteins. Although there is an increase in antioxidant enzymes, eg, superoxide dismutase, catalase, and glutathione-s-transferase, suggesting the presence of cellular defense, further inhibition of antioxidant enzymes, including thioredoxin reductase, by SM disrupts such cellular redox homeostasis. 32 A dramatic increase (30-fold) in copper levels and a decrease in ascorbic acid is observed within the anterior chamber after ocular exposure to mustard compounds, and both of these are indicators of oxidative stress. 17, THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 /
3 Free radicals have already been shown to play a role in corneal inflammation after exposure to other ocular irritants, such as alkali substances. 48,49 In such cases, tissue damage after corrosive injury to the cornea is exacerbated by penetration of reactive oxygen species to the corneal stroma, leading to fragmention of DNA chains, polymerization or depolymerization of proteins and hyaluronate, and destruction of lipid membranes. 49 Reactive oxygen species reduce ferric iron and copper and produce the highly reactive hydroxyl radicals. These reduced metal ions, in turn, can react with H2O2 to produce the hydroxyl radical, which causes further damage. 50 Other potential mechanisms of cell death are related to rapid inactivation of sulfhydryl-containing proteins and peptides, such as glutathione. These sulfhydryl compounds are critical for maintaining the appropriate oxidation-reduction state of cellular components. Glutathione is also thought to be critical for reducing reactive oxygen species in the cell and preventing peroxidation and loss of membrane integrity, which, in turn, prevents cytokine-mediated inflammatory response. 6,51-53 Clinically impaired corneas display increased matrix metalloproteinase (MMP) activity, in particular, MMP-9 in the acute phase. 54 There is a potential role for nitric oxide in tissue injury induced by SM and related analogs. Of particular importance is the reaction of nitric oxide with the reactive oxygen species superoxide anion, forming peroxynitrite. Peroxynitrite is a strong oxidant and nitrating agent and is known to trigger oxidative injury. 32 IV. IMMUNOLOGIC MECHANISMS Animal and human studies have demonstrated that SM has short- and long-term influences on both humoral and cellular immune functions. 12,55-58 The perilimbal site of the lesions, their similarity to Mooren s ulcer, and mixed inflammatory infiltrate within substantia propria suggest the immunological basis of SM-induced delayed keratitis. 3,59,60 Depression of cell-mediated immunity has been reported. 55,56 Total white blood count and percentages of monocytes and CD3+ lymphocytes are significantly higher in SM-exposed patients. 57 In addition, the percentage of NK cells (CD16+) is significantly lower in patients with severe respiratory complications up to 20 years after SM exposure. 13,55,56 A significant positive correlation has been found between hemoglobin level and the severity of ocular complications. 57 Increased levels of IgG, IgM, and C3 have been reported in the majority of SM-exposed patients during the first weeks and up to the sixth month after exposure. 13,55 It has been noted that even 20 years after exposure, the percentage of patients with increased IgM, IgG, and IgE are still significantly higher than in the control group. 12,55-57 In study of rabbits with SM injury, a significant increase in interleukin (IL)-1, IL-6, IL-8, tumor necrosis factor, MMP-2, and MMP-9 activities in the aqueous humor was observed. 61 The analysis of inflammatory mediators over time indicates that the SM injury progresses to the posterior part of the cornea, initiating the production of cytokines/ chemokines, which, in turn, may activate MMPs. MMP-2 and MMP-9 degrade collagen, thus contributing to the deterioration of the stroma. 61 It remains to be determined whether SM-damaged corneal stroma might elicit alloreactive responses that lead to further degradation, similar to Mooren s ulcers. Abnormalities in the immune system may contribute to recurrent infections, septicemia, and a higher incidence of malignancies in these patients. 12,56,62 V. SYSTEMIC MANIFESTATIONS Acute toxic effects appear after variable periods of latency, depending on the dose, mode of exposure, environmental temperature, and personal susceptibilities. 2,3,6,12,34,63 Victims may have multiple sites of injury, including skin, eye, and respiratory systems. 12 Organ damage is influenced by different concentrations of mustard gas exposure. The eye damage starts with exposure doses of 50 mg/min/ m 3. At mg/min/m 3 of exposure, respiratory and cutaneous systems are affected. At a dose of more than 200 mg/min/m 3, severe ocular and respiratory afflictions are observed. Skin burns occur at mg/min/m 3, and severe incapacitation from skin burns ensues at ,000 mg/min/m The reported fatality rates are less than 2% of the exposed soldiers during World War I and 3% to 4% in the Iraq-Iran conflict. 2,3 Death usually results from either respiratory failure due to chemical bronchitis/pneumonia or bone marrow suppression. 2,3 A. Skin The cutaneous effects of SM exposure begin after a latent period lasting for 0-24 hours. The characteristic skin lesion of SM is erythema followed by blisters. 64,65 At higher doses, vesicles form at the periphery of the erythematous areas, which later merge into pendulous bullae containing large volumes of clear yellow fluid. 6,7 Bullous lesions are particularly likely to occur on warm, moist areas, such as axilla, genitalia, and areas where tight clothing is worn. 7,8 They tend to form within 24 hours of exposure, but sometimes appear 7 12 days later. Large blisters usually break, leading to erosions and full-thickness ulceration (Figures 1 A and B). Necrosis may occur at these sites, followed by A Figure 1. Facial bullous lesions in acute phase with use of silver sulfadiazine ointment (A) and without it (B). B THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 / 165
4 formation of a scar at 72 hours post-exposure. In the case of extensive bullae formation, fluid and electrolyte imbalance combined with secondary infection may complicate recovery. 64, 65 Blistering and necrotic wounds may lead to permanent residual effects, including hyperor hypo-pigmentation, atrophy, hypertrophy, dermal scar, dryness of the skin, erythematous papular rash, multiple cherry angiomas, local hair loss, eczema, chronic urticaria, vitiligo, psoriasis, and discoid lupus erythematous. 12,14,34,63-68 Healing time varies depending on the extent of cellular damage and the ability of the body to replenish scavengers of electrophilic stress and reactive oxygen species. 6,7 SMinduced lesions tend to heal slowly, and often ulcerate and vesicate repeatedly for reasons that are still unclear. 6,7 One likely explanation is the propensity for SM to affect rapidly dividing cells, such as the basal cell layer of keratinocytes in the epidermis. 6,7 Other clinical forms of cutaneous lesions are pigmentary exfoliation, superficial vesicular to bullous form, bullous necrotization, deep necrotizing non-bullous form, allergic and toxic contact reactions. The pigmentary exfoliative form is often combined with severe lung damage. 12,14,34,63-68 B. Respiratory Tract Depending on the dose of SM and duration of the contact, pain and discomfort may develop in the nose or sinuses with increasing secretions, sneezing, nonproductive hacking cough, and sore throat 4-16 hours after exposure. This can develop into epistaxis, aphonia, tracheobronchitis, dyspnoea, and possible hemorrhage into the alveoli and microbial bronchopneumonia. 12 Necrosis of the mucosa with associated inflammation can lead to the formation of a diphtheritic-like membrane in the most severe cases, obstructing any level of the airways, 69 and later, to the clinical picture of adult respiratory distress syndrome. 35,70,71 Several years later, patients may be left with obstructive and restrictive pulmonary functions, bronchiectasis and bronchiolitis obliterans, chronic bronchitis, asthma, large airway narrowing, and pulmonary fibrosis Chronic bronchitis has been reported as the most common late complication of the respiratory system. 72,74-76,79,80 Progressive hypoxemia and hypercapnea are commonly observed in moderate-to-severe cases, leading to corpulmonale and respiratory failure. 53,63,80 The infection of the respiratory tract is a common problem, often complicated by septicemia. 42 C. Bone Marrow Bone marrow suppression can develop within 3-5 days of high-dose SM exposure, manifested as aplastic or ineffective hematopoiesis, leukopenia, and thrombocytopenia. 57 In some cases, chronic bone marrow suppression appears 7-15 days after exposure, resulting in sepsis and pneumonia 6,7 and higher mortality rates. 12 D. Other Organ Damage Gastrointestinal symptoms in the acute phase of SM injury include nausea and vomiting, which is often accompanied by respiratory distress resulting from immediate bronchospasm. 6,7 Clinical findings are acute gastroduodenitis with hemorrhagic erosions, acute desquamative enteritis, and severe hemorrhagic necrotic colitis. 6,12 Central nervous system involvement includes headache, anxiety, fear of the future, restlessness, confusion, lethargy, and convulsions. 6,12 In addition, patients can develop pulmonary, nasopharyngeal and laryngeal cancers, basal cell and Bowen s carcinomas, adenocarcinoma of the stomach, and acute myeloblastic and lymphoblastic leukemia. 66,81-86 Although an association between exposure to this chemical agent and ocular surface malignancies has not been reported, confocal microscopic findings have exhibited bizarre and abnormally enlarged pleomorphic keratocytes in all cases with SM-induced keratopathy. 14,87,88 VI. OCULAR INVOLVEMENT The moistness of the ocular surface, the extreme lipophilic nature of the gas, and the high turnover rate and metabolic activity of corneal epithelial cells make the eye the most susceptible part of the body to the effects of SM exposure. 2,6,11 Varying degrees of ocular involvement are seen in 75% to 90% of individuals exposed to mustard gas. 6 The acute symptoms usually resolve completely without further inflammation after 2-6 weeks. However, photophobia may persist for some time. In a minority of patients, a continuous process clinically appearing either as a persistent smoldering inflammation (chronic form) or late-onset lesions appearing many years after a variable silent period (delayed form) may develop. 2,3,6 It remains unclear whether mustard gas actually induces a continuous process of progressive inflammation on the ocular surface with different speeds of individual progression. In the chronic form of injury, severe acute lesions abate, but symptoms such as photophobia, dry eye, and foreign body sensation persist, and sequelae such as corneal epithelial erosions, limbal ischemia, and, occasionally, peripheral corneal thinning and neovascularization may slowly progress. 3 In the delayed form, patients become asymptomatic and enjoy improvement of their lesions several weeks after initial exposure, only to experience resurgence of symptoms several years later. 2,3,6 A. Acute Phase Within several hours of SM exposure, symptoms begin to appear. 6,15,53 The severity and timing of clinical symptoms and signs seem to be related to dose, concentration, and duration of contact. 6,15 As early as 1 hour after exposure, clinical manifestations start with a sensation of grittiness, progressive soreness, and a bloodshot appearance before proceeding to edema and giving rise to acute conjunctivitis. At 2-6 hours, patients complain of severe ocular pain, lacrimation, photophobia, blepharospasm, and decreased visual acuity. 6,12 The gradual spontaneous recovery usually occurs after 48 hours, with full regeneration of the corneal epithelium occurring within 4-5 days, although complete symptomatic recovery may take 6 weeks or longer. 2,6,7,63 Based on severity, immediate lesions can be divided into three groups: mild, moderate, and severe THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 /
5 Mild lesions are caused by exposure to mg/min/ m 3 and manifest as mild eyelid erythema/swelling and conjunctival engorgement without significant chemosis. 2,34 The cornea usually is spared, and recovery is complete within a few days. 2 Moderate lesions are caused by exposure to mg/ min/m 3 mustard gas. The eyelid, conjunctival, and corneal lesions are of the same type that occur with mild injury, but are more severe. 2,34,89 Symptoms include a dry sensation, severe ocular pain, photophobia, and severe blepharospasm. 2,5,17,34,90 The corneal epithelium begins to vesicate and slough predominantly in the interpalpebral fissure, leading to superficial punctate keratitis, corneal abrasions, superficial infiltrations, corneal ulcers, and even perforation. 9,12,61,90 The superior cornea is relatively spared, probably due to the protective effect of the upper lid. 91 After 48 hours, pain and blepharospasm gradually decrease and the corneal epithelium usually heals completely within 4-5 days. Full resolution of symptoms may take up to 6 weeks or longer. 2 Severe lesions occur after exposure to more than 200 mg/min/m 3 mustard gas. 2,3,6 Patients with such exposure often sustain associated systemic toxicity in the respiratory, gastrointestinal, and integumentary systems. 3 In addition to the moderate lesions, limbal vasculature and deeper layers of the cornea are also involved. The eyelids may become ulcerated. The nasal and temporal limbi lose their normal vasculature and become white and necrotic. In addition to having marked congestion and chemosis, severe conjunctival lesions are characterized by areas of ischemia and necrosis, particularly in the interpalpebral fissure. 2,3,6 There may be low-grade iridocyclitis, which usually leaves no synechia or cataract formation, and, rarely, the intraocular pressure is transiently elevated. 2,4,89 Because conjunctival lesions are limited to the interpalpebral fissure, adhesions between the globe and eyelid are unlikely. 3 The corneal epithelial irregularity and stromal edema combine to create an orange peel appearance, which usually does not stain with fluorescein; however, epithelial erosions and small corneal ulcers may be noted (Figure 2). 2,3 They are prone to bacterial superinfection, including Pseudomonas aeruginosa, which can lead to severe intraocular infection necessitating evisceration or urgent tectonic penetrating keratoplasty (PKP). 2,3 Corneal sensation may be affected to varying degrees. 3 There may be pupillary constriction, Figure 2. Corneal stromal edema in acute severe exposure. iris vasodilatation, hemorrhages, and necrosis, with development of anterior uveitis. Improvement often begins within 1-2 weeks, when the corneal edema resolves and the uveitis subsides. A few weeks later, neovascularization begins. These tortuous blood vessels tend to bleed into the corneal subepithelial space and stroma. They eventually undergo rapid degeneration, leaving white opacities in the otherwise clear cornea. 2,3 B. Chronic Phase A continuous process leading to a chronic form or a delayed form of injury develops in less than 1% of exposed individuals up to 40 years after their exposure. 2,3,6,12,34,92 In contrast to acute lesions, chronic and delayed mustard gas lesions usually cause permanent reduction in visual acuity and can even lead to blindness. 3 Distinctive features include chronic blepharitis, meibomian gland dysfunction, dry eye, limbal ischemia, limbal stem cell deficiency (LSCD), corneal neovascularization, lipid and amyloid deposition, and irregularity, thinning and scarring of the cornea. 2,3,6,12,34,61 It remains unknown whether disease activity correlates with hotter and drier climates. 3 In the chronic form of injury, patients suffer from photophobia, injection, tearing, and foreign body sensation. 12,91 Impaired corneal sensation, damaged limbal vasculature, and recurrent epithelial erosions produce corneal irregularity, thinning, and neovascularization, leading to descemetoceles and perforation. 2,3,6,12,34,50,61,91 Corneal neovascularization can lead to intrastromal exudation of plasma lipids and deposition of amyloids. 59,93 Despite the ongoing inflammation, the eye may appear quiet. Nonetheless, this should not be considered as quiescence, as it may be the result of vascular necrosis resulting in ischemia. 2,3, 50,59,91 In the delayed-onset form of injury, after a silent period of several years, patients begin to suffer from foreign body sensation, tearing, redness, and severe photophobia. 12,91 In early stages, the limbal region frequently presents a marbled appearance in which porcelain-like areas of ischemia are surrounded by blood vessels of irregular diameter. 2,3,6 Varicose, tortuous, ampulliform and leaking vessels that characteristically are accompanied by blood islands and hemorrhages surround perilimbal ischemic areas. 2,94 This may lead to lipoid depositions in the adjacent cornea and trigger chronic stromal inflammation and thinning. 2,3,95 It may also aggravate the clinical situation and produce severe photophobia and tearing. 59,93 Later, vascularized scars of the cornea are covered with crystal and cholesterol deposits, leading to worsening of opacification, recurrent ulcerations, and sometimes corneal perforation. 2,3,6,12,34,61,93 Opacification of the central and lower portions of the cornea is typical, while the upper sections are often protected by the eyelids. 2,9,91 These lesions even recur after corneal transplantation. 96 A minority of patients might develop corneal perforation and phthisis bulbi. 2 The presence of ischemic conjunctival areas, intrastromal corneal and conjunctival hemorrhages and bloody islands, lipoid and amyloid depositions, and aberrant neo- THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 / 167
6 Figure 3. A. Mild form of ocular involvement with tortuous, telangiectatic, conjunctival vessels surrounding some areas of severe perilimbal conjunctival ischemia. B. Invading leaking, aberrant telangiectatic ampulliform vessels with lipid deposition (moderate form). C. A patch of severe peripheral corneal thinning with amyloid deposition adjacent to perilimbal telangiectatic vessels (severe form). D. Severe nasal and temporal corneal thinning with invading segmented leaking vessels and lipid deposition (severe form). vascularization may be signs of chronic vasculitis induced by mustard gas. The chronic conjunctival and corneal inflammation can lead to chronic blepharitis with lid margin thickening and meibomian gland dysfunction. 35 No cases with keratinization have been reported to date. 3,59 Ocular surface involvement can be graded as mild, moderate, or severe. Conjunctival vessel changes, including telangiectasia, tortuosity, and segmentation, are characteristics of the mild form, and the adjacent corneal quadrant is clear in this form. Limbal ischemia and peripheral vessel invasion with or without corneal opacity are features of the moderate form. If previous findings are accompanied by severe corneal thinning and melting, the involvement is considered severe (Figures 3 A-D). 3,59 The clinical picture of SM-induced ocular surface disease is a continuous spectrum of manifestations that make it difficult to clearly grade its severity. LSCD gradually begins in moderate forms and finally ends in total LSCD in most severe cases. It appears that late clinical manifestations of SM keratopathy result from several underlying mechanisms. LSCD progresses from partial and asymmetric to total LSCD because of a direct and progressive detrimental effect of mustard gas or chronic limbal ischemia. 3,95 We cannot ignore the likelihood that chronic ischemia or the detrimental effect of mustard gas may disturb the stem cell niche, resulting in progressive stem cell attrition. Damage to corneal nerves leading to the loss of corneal sensation also contributes to this detrimental process over time. 1,17 In an animal study, degeneration of nerve fibers with a typical subsequent Wallerian degeneration was observed after exposure, and continued for weeks to months afterwards. 54 Autoimmune reactions to the corneal antigens altered by the mustard agent (collagen-mustard compound) have also been proposed. 2,97 In delayed mustard gas keratopathy, limbal ischemia plays a significant role in the corneal neurotrophic and trophic changes, including thinning, descemetocele formation, and perforation. 59 The role of known angiogenic factors in SM-induced angiogenesis has not been yet elucidated. 17, Inflammation may play a role in propagating the SM-delayed response; animal experiments have shown that anti-inflammatory treatment decreases the primary inflammatory reaction, as well as the extent of neovascularization. 17,54,104 The clinical course of corneal injuries like alkaline/ acidic burns is quite similar in all victims. 105 The question of why some eyes are more vulnerable than others to the late response of SM is still unanswered. Vulnerability may be related to concentrations, total doses, contact duration, mode of exposure, environmental temperature, the extent of use of protective equipment, personal susceptibilities, individual closeness to the ground, age, and other factors. 2,3,6,30,59,63,106 Generally, children are more severely affected by SM exposure than adults, most likely because children have thinner skin and are closer to the ground, where mustard vapors accumulate. 6,106 Reports of late response to SM exposure would also be related to type and duration of follow-up. A puzzling feature in delayed mustard gas keratitis regards the unpredictable exacerbations and remissions in the clinical course, with peripheral corneal infiltrations, at times extending to the central cornea, mimicking Mooren s ulcer. 3,60 Corneal infiltrations usually are accompanied by neovascularization (morphologically similar to conjunctival vessels), which is an unfavorable prognostic factor. 3,60 Infiltrations may be accompanied by intrastromal hemorrhages, 168 THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 /
7 corneal necrosis, thinning, descemetocele formation, and perforation. 3,54 Recurrent episodes lead to centripetal and deeper infiltrations, and degenerative changes finally take place and crystalline deposits are noted over time. 2,3,6,12,60 Stem cell deficiency is one of the main factors contributing to mustard gas-induced keratopathy. 59 However, corneal manifestations are not typical of the partial or total LSCD seen with severe chemical burns. With SM-induced keratopathy, the cornea is not covered by a total vascularized pannus; instead, corneal thinning with amyloid and lipoid depositions are prominent. In some areas, leaking telangiectatic vessels invade peripheral cornea. Corneal involvement is often asymmetric between the two eyes, and in each eye, severity of involvement is not the same in all quadrants. Most often, the interpalpebral (exposure) area of the cornea that is adjacent to conjunctival ischemic areas is more severely damaged. 59 This may be due to direct contact of the interpalpebral fissure during the exposure or to more severe perilimbal ischemia in these areas. In turn, perilimbal ischemia may be due to direct exposure of tissues with consequent vasculitis. 59 In summary, corneal manifestations seem to be a mixture of progressive chronic limbal ischemia and stem cell deficiency. 3 The differences in the clinical picture may be related to exposure pattern. In chemical burns, a high concentration of acid/alkali liquids is in direct contact with limbal stem cells, while aerosolized gas is in contact with the ocular surface during an SM attack. 2,3,59 Numerous animal studies have investigated the clinical picture and pathophysiologic mechanisms of SM-induced keratopathy, but these are beyond the scope of this review. 12,32,54 C. Pathologic Findings Light microscopic observation of corneas 48 hours after SM exposure reveals epithelial denudation and marked stromal edema accompanied by cellular infiltration, mostly of eosinophils. Endothelial destruction is occasionally observed. 60 Epithelial regeneration starts 72 hours after exposure by migration of remaining noninjured corneal or conjunctival cells. 17,60 The latter is confirmed by the presence of goblet cells scattered diffusely in the newly regenerated epithelium. 17 In moderate forms of injury, extensive loss of conjunctival mucous and goblet cells associated with occlusion of conjunctival blood vessels (as a result of destruction of vascular endothelial cells) are observed. 97 The corneal epithelium is loosened from its stroma (at the palpebral fissure), and small vesicles are formed, in which the corneal free nerve endings are exposed. 2,60 Histopathologic features of the conjunctival component in patients with chronic or delayed mustard gas keratopathy include chronic inflammation, perilimbal conjunctival ischemia, telangiectasis, vasculitis, subconjunctival hemorrhage, decreased number of goblet cells, thinning or thickening of epithelium, scar formation in substantia propria, lymphocytic infiltration, and dilated lymphatic vessels. 3,8,17,50,54,60,91,107 There are no signs of dysplasia. 59 Corneal pathologic findings include destruction of Figure 4. Markedly attenuated corneal epithelium, loss of Bowman s layer, foci of mild chronic inflammation around intrastromal vascularization, foci of stromal degeneration and severe loss of endothelial cells (H&E, x 200). the epithelium and Bowman s layer, loss of keratocytes, conjunctivalization, superficial and stromal vascularization, squamous metaplasia, focal corneal thinning and ulceration, acute and chronic infiltration of inflammatory cells, lipoid/amyloid deposition, endothelial cell loss, calcific band keratopathy, and scarring in the stroma. 3,8,17,50,54,60,91,107 Perilimbal conjunctival vasculitis and ischemia may contribute to the corneal cytopathologic features. 59, 60 Corneal squamous metaplasia, which is mild-to-moderate in most cases and has been suggested as a diagnostic factor in cases with mild or subclinical limbal deficiency, may be a reactive response to mustard gas (Figure 4). 108 D. Confocol Microscopy Although SM cannot easily achieve deep corneal penetration, in the acute phase, it targets endothelial cells, inducing apoptosis at lower concentrations and both apoptosis and necrosis at higher concentrations. In chronic and delayed-onset forms of injury, abnormal confocal microscopic findings are observed in all corneal layers. The anterior and middle portions are affected more severely than the posterior parts. 88 The mosaic pattern of basal epithelial cells is not apparent. Their density decreases and most of the cells look pleomorphic, with damaged or irregular high-contrast boundaries. Generalized decreased density of keratocytes has been reported, but their gradient pattern is controversial. 88,91,109 Keratocyte density decreases progressively from the anterior to the posterior stroma in normal cornea. Within the anterior corneal stroma, spindle-like keratocytic nuclei (perhaps representing necrotic keratocytes) close to Bowman layer could be delineated. Normal keratocytes are capable of dividing and migrating after injury. 110 It has been suggested that the genetically altered keratocytes may lose their ability to repopulate the injured stroma in mustard gas keratopathy. 88 Bizarre and abnormally enlarged pleomorphic keratocytes are observed in almost all cases. 88,91,109 Intrastromal microdots, which are compatible with foci of stromal necrosis, may be observed. 88 Foci of amyloid degeneration and lipid deposition and stromal neovascularization, have been reported, as well. 88 Degenerative processes seem to dominate in chronic and THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 / 169
8 Figure 5. Confocal microscope scans, x 500. A. Moderate loss of stromal keratocytes with a few residual keratocytes and pleomophic nuclei. B. Severe loss of stromal keratocytes and presence of hyper-reflective microdots. C. Hyper-reflective crystals of lipid keratopathy. D. Moderately reflective reticular pattern due to amyloid deposits in the stroma. delayed mustard gas keratopathy. The presence of dendritic cells without their dendrites and activated keratocyte nuclei may indicate ongoing inflammation at the microscopic level. 109 These changes in the interstitial matrix of the cornea may be a potential barrier for repopulation of stromal keratocytes. 88 Decreased sub-basal nerve plexus is observed in most of the cases, which could be secondary to destruction of the Bowman layer, occurrence of subepithelial fibrosis, and associated dry eye. 88 However, the thickness of the midstromal irregular circular node-like nerve structure may increase (Figures 5 A-D). 88,109 VII. INITIAL MANAGEMENT OF SYSTEMIC MANIFESTATIONS There is no effective antidote for mustard gas exposure, so prevention is the most effective management strategy. Special protective garments and gas masks containing a charcoal layer to absorb penetrating sulfur mustard are highly effective in preventing dermal, respiratory, and ocular injuries. 2,6,8 However, chemical goggles, gas masks, and protective clothing are cumbersome and inefficient for daily use in military or civilian populations. 111 The first priority of treatment after mustard gas exposure is to remove victims from the contaminated areas and initiate decontamination procedures. Contaminated clothes must be removed and destroyed. Rapid riddance from the skin is critical, as mustard penetrates the tissues within minutes of exposure, and its effects become irreversible. 2,12,111 When available, absorbent powders such as calcium chloride, magnesium oxide, activated charcoal, talcum powder, Fuller s earth, and flour, should be used to decontaminate the skin. The powder is sprinkled onto the exposed skin and allowed to absorb the mustard, and is then washed off with water. 2, 111 When mustard exposure is suspected, the victim should be washed with hypochlorite 0.5%, calcium hypochlorite (72 g/l), neutrogenic soap/shampoo (ph around 7.0), and copious amounts of warm water for a prolonged period of time. Complete hydrolysis of mustard renders it nontoxic. Washing of the affected area with oil, kerosene, or gasoline, followed by washing with soap and water, has also been advocated. 12,112 Even in asymptomatic patients, the eyes should be washed as soon as possible with generous amounts of water, normal saline, and Ringer solution. 12 Sodium bicarbonate1.5%, dichloramine-t 0.5%, and saturated solutions of sodium sulfate or magnesium sulfate, as well as zinc or boric acid, have also been suggested. 12 Because of the rapid and irreversible reaction of SM with ocular tissues, it may seem that irrigation would not be useful more than minutes after exposure; however, irrigation at this later point is recommended, as it does no harm and may help. 2 Of the many fluids studied for use in ocular irrigation, none has proved more effective than tap water. 2 Upon arrival at a medical facility, the victims should be quickly examined by medical doctors for severity grading of SM intoxication. The mild cases that do not reveal any sign of intoxication should be kept under observation and may be discharged after 24 hours. Those who show any sign of SM poisoning during observation should, along with moderate and severe victims, receive emergency management. If a large surface area is affected, fluid and electrolyte balance must be maintained. The management of skin lesions focuses on the prevention of secondary bacterial infections by applying sulfamylon (mefenide acetate), 170 THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 /
9 silvadene (silver sulfadiazine), povidone iodine or bacitracin zinc to the affected areas, and administration of systemic antibiotics to prevent secondary infections. 6,12, 113,114 Biosyntheic dressings, ie, hydrogels and hydrocolloiods, may accelerate healing. Steam inhalation, cough suppressants, oxygen therapy, assisted ventilation, early intubation, and bronchodilators are immediate measures for respiratory involvement. Systemic steroids and antibiotics may be helpful for severe affliction. 6 Medical treatment can be divided into antidotal/general treatments and care of specific organs. In the antidotal treatment, up to 500 mg/kg sodium thiosulphate should be administered as soon as possible. It reacts with mustard gases when these agents are in the cyclized form. Thus, it is an effective antidote against systemic intoxication, especially when taken before exposure. 6,12 Sodium thiosulphate can also be combined with a number of other drugs, such as cysteine, sodium citrate, dexamethasone, promethazine, heparin and vitamine E, to increase its protective activity against SM. 115 VIII. MANAGEMENT OF OCULAR INJURY A. Acute Phase The ocular lesions can be differentiated into conjunctival only and corneal involvement by fluorescein staining performed immediately after ocular washings. Medical therapies in this stage include topical antibiotics, preservative-free lubricants, and corticosteroids. 2,6,12 In the case of corneal involvement, close observation is necessary. Treatment should include daily ocular irrigation, artificial tears, therapeutic contact lenses, mydriatics (to reduce ocular pain produced by spasm of the ciliary muscle and to prevent posterior synechiae), antibiotic drops (to prevent secondary bacterial infections), and topical antiglaucoma medications (to control intraocular pressure). 2,6,50,63 The use of lubricants is controversial, as they may concentrate mustard gas particles trapped under the eyelids. 2 Ocular bandages should be avoided, as they might raise the corneal temperature and accelerate the toxic effects. 2,12 Topical corticosteroids should be cautiously used. 2,6,12 Although they may reduce eyelid, conjunctival, and corneal swelling and improve anterior uveitis, they may predispose the cornea to infection. 6,12 Petroleum jelly can be used on the follicular margins to prevent sticking. However, it should not be used immediately after exposure, as mustard can become concentrated in this oily medium. 2,34, 113 Dark glasses and patient reassurance are very important, as the eye lesions produce severe photophobia and fear. 9,113 Amniotic membrane transplantation can suppress inflammation and scarring and promote healing in patients suffering from a variety of ocular surface diseases Used during the acute stage of Stevens-Johnson syndrome 122 and acute chemical burn, its healing and anti-inflammatory effects have been shown to prevent late sight-threatening cicatricial complications. Therefore, it may be beneficial in the control of acute stages of SM-induced ocular surface disorders. B. Chronic Phase 1. Medical Treatment No definitive treatment for chronic and delayed mustard gas-induced ocular surface disorders is available. 2,3,6,12 Current therapy is mainly conservative and directed at symptomatic relief, as it addresses tear deficiency and ocular surface instability (ie, artificial tears, temporary or permanent punctal occlusion, blepharorrhaphy, tarsorrhaphy and therapeutic contact lenses). 2,3,6 Because the ocular surface is compromised, especially in the moderate and severe forms of injury, preservative-free artificial tears or gels should be used. Punctal plugs are usually beneficial. 1,50,61 Permanent occlusion of one or both puncti of each eye by electrocautery may be preferable. 95 Topical steroids can be used to control ocular surface inflammation and acute episodic corneal inflammatory infiltrates. 2,3 Preservative-free topical steroids are beneficial, especially for short-term usage. 3 Although systemic steroids are not usually necessary, in the case of severe corneal inflammations, they may be combined with topical steroids. 3 However, long-term steroid-induced complications, including cataract and glaucoma, should be considered. 2,6,12 Because of the loss of corneal integrity with mustard gas keratitis, the ocular surface is prone to secondary microbial infection; thus, topical steroids should be used cautiously. 95,96 High DK silicone hydrogel contact lenses can improve punctate epithelial erosions and keratitis, as well as persistent epithelial defects (PEDs) in the context of partial LSCD. With total LSCD, they are not effective, and they can increase the risk of secondary microbial infections. 2,3,6,12 Treatment of associated blepharitis is recommended in all cases. To improve visual acuity, spectacles and high DK soft/hard contact lenses may be cautiously used. 3,5 Most cases with severe and recurrent inflammatory infiltrates respond well to conservative measures, including topical/ systemic steroids. 95,96 Adjuncts such as lubricants and topical antibiotics may help. 2,3,61 2. Surgical Interventions a. Tarsorrhaphy In the case of nasal or temporal progressive corneal thinning with or without PEDs, medial or lateral tarsorrhaphy may halt progression of corneal thinning. 3,95 It can also dramatically improve the symptoms of patients with chronic ocular surface irritation and dry eye. 59 It is highly recommended after any type of stem cell or corneal transplantation. 95,96 b. Amniotic Membrane Transplantation Amniotic membrane transplantation can be used to treat PEDs that occur with partial LSCD. 54,95 However, it is not useful when LSCD is severe or total. 54 In severely irritated eyes with annoying photophobia due to corneal lipoid deposition, superficial keratectomy combined with amniotic membrane transplantation is very beneficial (Figures 6 A and B). 95 Amniotic membrane transplantation may also be used as a patch or graft as an adjunct to various kinds of THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 / 171
10 Tissue harvested from one or both eyes of an immediate family member is fresher and has closer genetic composition than KLAL. On the other hand, a KLAL graft is more accessible and has more stem cells. However, besides being less fresh than an lr-clal graft, it is more prone to chronic stem cell attrition and rejection. Due to partiality, bilaterality, and asymmetry of LSCD; and discrepancy in severity of quadrant involvement, complete 360-degree coverage of the limbal area by graft is unnecessary. 95 Sectoral KLAL/ lr-clal in areas with the most severe thinning and LSCD appears to be adequate (Figures 7 A and B). In a recent study, the rejection-free graft survival rate was reported to be 39.1% in the lr-clal group and 80.7% in the KLAL group at month 40, with a mean follow-up period of 24.9 and 68.8 months, respectively. 143 Because simultaneous systemic problems exist in patients after mustard gas exposure, minimal necessary immunosuppression should be used. 95,96 In some cases with severe ischemia, simultaneous resection of ischemic conjunctiva and advancement of near normal conjunctiva may be beneficial. It is not clear whether conjunctival advancement or tenonplasty should be used to correct ischemia before stem cell transplantation. Figure 6. A. Inferior corneal lipid deposition with leaking aberrant vessels. B. Three months after superficial keratectomy and amniotic membrane transplantation, the eye is quiet. stem cell transplantation. 54,59,95, It may also be used as an adjunct to medical therapy in cases with recurrent corneal inflammatory infiltrates to decrease ocular surface inflammation and reduce scarring. 59,134 Multilayered amniotic membrane transplantation can be used in corneas with severe thinning. 135,136 c. Stem Cell Transplantation Candidates for stem cell transplantation include patients suffering from chronic irritation, redness, and tearing of the eyes with PEDs associated with severe corneal thinning, who are unresponsive to conservative treatments (artificial tears, lubricants, punctal occlusion, blepharorrhaphy and tarsorrhaphy). 95 Limbal areas adjacent to the thinnest peripheral corneal areas with epithelial defects are selected as potential surgical sites. In some situations, simultaneous penetrating or lamellar keratoplasty can be performed. 95,96 Limbal stem cells can be harvested from immediate family members, including parents, siblings, or children (living-related conjunctival-limbal allograft [lr-clal]) or cadaveric eyes (keratolimbal allograft [KLAL]). Human leukocyte antigen (HLA) matching is not obligatory. Various surgical techniques have been previously described. 95, Figure 7. Sector keratolimbal allograft in a case with severe perilimbal corneal thinning and persistent epithelial defect before (A) and after (B) surgery. 172 THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 /
11 d. Corneal Transplantation Penetrating or lamellar keratoplasty may be sufficient when LSCD is not severe and when visual acuity is decreased due to central corneal opacification caused by amyloid/lipoid deposition. 3,96 In such circumstances, perilimbal conjunctival ischemia is usually mild. Due to the recurrent and chronic nature of the disease, it is advisable to spare the posterior stroma and corneal endothelium, avoiding the associated ocular surface derangements; thus, lamellar keratoplasty (LKP) is preferred. 88 A full-thickness graft is required for deeper lesions. Tectonic PKP may be needed in eyes with severe corneal thinning, large descemetoceles, and impending or frank corneal perforation. Tectonic LKP may also be performed in cases with small descemetoceles. 3,96 Conventional LKP, or deep anterior lamellar keratoplasty (DALK; Melles and Anwar techniques) can be performed. 144,145 The rejectionfree graft survival rate has been reported to be 39.0% in PKP patients and 90.3% in LKP patients at month 28, with a mean follow-up length of 29.6 and 85.0 months, respectively. 143 Most often, due to corneal scar formation and variability of corneal thickness and its irregularity, conventional LKP and Melles techniques are preferred. Although, corneal transplantation can be simultaneously performed with limbal stem cell transplantation, it is advisable to perform it at least 3 months after stem cell transplantation. 95 Because of the compromised ocular surface, corneal transplantation in cases with SM-induced keratopathy is considered highrisk. 59,96 Cases with severe LSCD and severe limbal ischemia with peripheral corneal thinning may have a high rate of graft failure due to rejection reactions, recurrent opacity, and corneal thinning. 95,96 3. Treatment Algorithm (Figure 8) Conservative management, which is the main modality in the mild form of SM injury, should be applied in all grades of delayed-onset SM-induced ocular surface disease. In the moderate form with partial stem cell deficiency, corneal opacity can be managed with corneal transplantation alone. In this grade, PED due to partial stem cell deficiency and limbal ischemia can be treated by AMT. In severe forms with severe LSCD associated with severe corneal thinning and melting, stem cell transplantation is the best option. Subsequent corneal transplantation can be used to improve visual acuity. 4. Postoperative Medical Regimen and Surgical Outcome Topical antibiotic and steroid drops (especially preservative-free) are used when indicated, but tapered and discontinued when corneal epithelialization is complete and ocular surface inflammation declines. Topical 20% autologous serum, preservative-free artificial tears, and lubricating gels or ointments are also useful. Oral prednisolone 1 mg/kg should be started and tapered off during 6-8 weeks with decreasing inflammation, and antiglaucoma medications should be used as necessary. 95,96 Because of the progressive nature of the disease, regular follow-up visits Figure 8. Treatment algorithm for chronic/delayed-onset sulfur mustard-induced ocular surface disorders. See text for details. AMT = amniotic membrane transplantation; LSCT = limbal stem cell transplantation; PKP = penetrating keratoplasty; LKP = lamellar keratoplasty. are highly recommended. In general, optimization of the ocular surface by the aforementioned measures is required after corneal transplantation. The dose of systemic steroids should be increased for a period after corneal transplantation to decrease ocular surface inflammation. Immunosuppressive therapy may be required in the case of recurrent rejections, previous failure, or the presence of other risk factors. 96, Different systemic and topical immunosuppressive regimens have been suggested for allogenic stem cell transplantation. 3,130,131,138,149,150 Systemic cyclosporine A 3 to 5 mg/kg has been used in patients with SM-induced ocular surface disease. 95,96,109 Combined systemic immunosuppression using more potent and safer immunosuppressives, including mycophenolate mofetil 1 to 2 gr/day and tacrolimus 2-6 mg/ day, has been shown to be more effective than cyclosporine A in promoting survival in solid organ transplantations, as it lessens acute rejection. 151 Doses should be adjusted according to ocular surface inflammation and systemic adverse effects. 131 Given the multiple organ involvement in patients with SM-induced ocular surface disease, the optimal dose, combination, and duration of therapy should be carefully adjusted and evaluated in further studies. Because of the potential side effects of systemic immunosuppression, close collaboration with an immunosuppressive therapy expert is highly recommended. Living-related limbal stem cell transplantation has been shown to be an effective way to stabilize the severely inflamed ocular surface in patients with advanced mustard gas keratopathy. This can markedly decrease subjective complaints, heal PEDs, and lead to regression of peripheral corneal neovascularization. 95 The long-term results of sectoral KLAL have not yet been reported in such cases. Acute rejection, which is more prevalent in the early months after THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 / 173
12 surgery, is manifested by the occurrence of limbal and perilimbal engorgement of vessels associated with conjunctival chemosis in the limbal transplant area. This can be treated by increasing the dose and frequency of topical and systemic steroids. The dose is gradually tapered with the elimination of vascular engorgement and local chemosis. 95,96 Graft failure due to acute rejection is rare. 88 Whether acute stem cell rejection(s) predispose the patient to chronic rejection has yet to be elucidated. The results of PKP or LKP alone or combined with stem cell transplantation has been shown to be promising with proper case selection. 88,96 Success may be related to the lack of structural defects in the ocular adnexa, symblepharon formation, partiality of stem cell deficiency, mildness of dryness, and absence of corneal exposure. 3,59,88,95,96 Corneal transplantation in these patients is high-risk due to the compromised ocular surface, especially LSCD and perilimbal conjunctival ischemia, chronic inflammation, and decreased sensation However, with appropriate management, graft clarity and visual outcomes have been reported to be favorable in long-term follow-up. 96 Even with successful corneal transplantation, SMinduced ocular surface disease may progress and recur (Figures 9 A and B). A rate of endothelial rejection up to 59% has been reported. 96 Although endothelial immune rejections were relatively common in these patients, most of them did not lead to graft failure. Optimization of the ocular surface and keeping it free of inflammation are critical for survival of the transplanted stem cells and corneal graft. It has been observed that corneal grafts performed after stem cell transplantation have better results than corneal grafts alone. 95,96,138 Graft rejection may be more frequent in eyes that receive simultaneous corneal graft and stem cell transplantation than in those that have had the procedures sequentially. 96 The major vision-limiting factors after a successful corneal transplantation are corneal epithelial breakdown, tear film instability, corneal astigmatism, steriod-induced glaucoma, and cataracts. 96,156 C. Novel and Potential Therapies for Mustard Gas Injury Although progress has been made in understanding how the cornea responds to acute insults, the design of treatment strategies for SM injury is complicated by the lack of knowledge regarding the etiology of recurrent corneal disorders. In some animal studies, topical use of corticosteroids and nonsteroidal anti-inflammatory drugs, 104 colchicine, 157 a calcium-blocker (diltiazem), 158 and MMP inhibitors (such as doxycycline) 54 have been shown to reduce ocular inflammation. Reduced dermal and systemic injury has been reported after treatment with thiosulfate, nicotinamide, flavonoids, and topically applied iodine. 46,50, Colchicine was found to inhibit the acute ocular response to nitrogen mustard in rabbits. 157 Increased survival was noted in rats treated parenterally with vitamin E or dexamethasone within 15 minutes of exposure, 162 while pre-exposure treatment of rats with nicotinamide (NAD+ Figure 9. A. Successful lamellar keratoplasty in a patient with moderate form of SM-induced ocular surface disease and decreased visual acuity due to extensive central corneal amyliod deposition. B. Recurrence of keratopathy 1.5 years after surgery. precursor) decreased the severity of skin damage induced by sulfur mustard. 2,163 Thymosin β4 is a highly conserved, 43 amino-acid polypeptide that has been shown to influence cell migration, proliferation, and differentiation, promoting corneal wound healing, decreasing inflammation, and modulating activity of MMP when applied ectopically. 61, This has been suggested as an antidote for SM injuries. 61 Metallocomplexes, such as zinc- or gallium-desferrioxamine, are known to inhibit the formation of highly reactive free radicals. It has been hypothesized that either complex exerts its protective effect by intervening in a critical step of hydroxyl radical formation during acute phase damage. 50 Nitric oxide synthase inhibitors, including topical iodine preparations and aminoguanidine, have been reported to protect or rescue cells in vitro from SM-induced toxicity. 170 Ebelson, a peroxynitrite scavenger that did not affect nitric oxide synthase activity, has also been reported to be an effective inhibitor of SM induced toxicity. 32 Several studies have shown that glutathione or the its prodrug N-acetylcysteine can reduce oxidative stress and toxicity induced by SM or its analogs. 31,32, THE OCULAR SURFACE / JULY 2011, VOL. 9, NO. 3 /
Mustard Gas Induced Ocular Surface Disorders
 Challenging Case Mustard Gas Induced Ocular Surface Disorders Section Editor: Alireza Baradaran-Rafii, MD Ophthalmic Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Sulfur
Challenging Case Mustard Gas Induced Ocular Surface Disorders Section Editor: Alireza Baradaran-Rafii, MD Ophthalmic Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran Sulfur
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA
 Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
Eye Care for Animals Micki Armour VMD DACVO THE CORNEA ANATOMY 0.5-0.6mm thick 4 primary layers Epithelium (5-7 cell layers) Stroma (90% total thickness) Descemet s membrane Endothelium (1 layer) ANATOMY-
PAINFUL PAINLESS Contact lens user BOV
 Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
Common Causes Allergies Infections Ocular Cornea, uveitis, endophthalmitis Orbital Orbital cellulitis Inflammation Uveitis Scleritis / episcleritis Glaucomas Trauma Foreign bodies Chemical injuries History
MEDICAL MANAGEMENT OF CHEMICAL CASUALTIES VESICANTS U.S. ARMY MEDICAL RESEARCH INSTITUTE OF CHEMICAL DEFENSE USAMRICD PROTECT, PROJECT, SUSTAIN
 MEDICAL MANAGEMENT OF CHEMICAL CASUALTIES VESICANTS U.S. ARMY MEDICAL RESEARCH INSTITUTE OF CHEMICAL DEFENSE PROTECT, PROJECT, SUSTAIN OBJECTIVES Know the mechanism of action (pathophysiology) Identify
MEDICAL MANAGEMENT OF CHEMICAL CASUALTIES VESICANTS U.S. ARMY MEDICAL RESEARCH INSTITUTE OF CHEMICAL DEFENSE PROTECT, PROJECT, SUSTAIN OBJECTIVES Know the mechanism of action (pathophysiology) Identify
Fleck. Pre-Descemet Dystrophies (generally good vision and comfort) Primary Pre-Descemet Dystrophy
 Fleck Etiology: bilateral, sometimes asymmetric, autosomal dominant opacities located in all levels of stroma as early as 1 st decade Slit lamp: well demarcated, small round gray-white doughnut-like, wreath-like
Fleck Etiology: bilateral, sometimes asymmetric, autosomal dominant opacities located in all levels of stroma as early as 1 st decade Slit lamp: well demarcated, small round gray-white doughnut-like, wreath-like
CORNEAL CONDITIONS CORNEAL TRANSPLANTATION
 GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
GENERAL INFORMATION CORNEAL CONDITIONS CORNEAL TRANSPLANTATION WHAT ARE CORNEAL CONDITIONS? The cornea is the clear outer layer of the eye. Shaped like a dome, it helps to protect the eye from foreign
Senile: flattening of vertical meridian, thinning of periphery, lack of luster
 Pterygia Etiology: triangular, fibrovascular, connective tissue overgrowths of bulbar conjunctiva onto cornea; distribution of ultraviolet energy- heat, wind, dust, dry atmosphere,higher prevalence nearer
Pterygia Etiology: triangular, fibrovascular, connective tissue overgrowths of bulbar conjunctiva onto cornea; distribution of ultraviolet energy- heat, wind, dust, dry atmosphere,higher prevalence nearer
Degenerations. Conditions with cloudy cornea at birth or in infancy
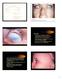 Dermoids The lesions are choristomas, which are congenital masses of tissue that have been dislocated from their normal position Limbal dermoids--overlapping the cornea and sclera, often inferotemporally
Dermoids The lesions are choristomas, which are congenital masses of tissue that have been dislocated from their normal position Limbal dermoids--overlapping the cornea and sclera, often inferotemporally
OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR.
 OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR. HET RODE OOG F. GOES, JR. Condition Signs Symptoms Causes Conjunctivitis Viral Normal vision, normal pupil size Mild to no pain, diffuse Adenovirus (most common),
OOGZIEKTEN VOOR DE HUISARTS F. GOES, JR. HET RODE OOG F. GOES, JR. Condition Signs Symptoms Causes Conjunctivitis Viral Normal vision, normal pupil size Mild to no pain, diffuse Adenovirus (most common),
 Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
Traumatic Cataract Orbital Wall Fracture Vitreous Hemorrhage Optic Disc Hemorrhage a) Amblyopia b) Strabismus c) Trauma Playing with other children Sports Fire works BB gun Injecting needles .
Dry Eye Assessment and Management Study ELIGIBILITY OCULAR EVALUATION FORM
 Page 1 of 13 BEFORE COMPLETING THE OCULAR EXAMINATION, YOU MUST BE ABLE TO ANSWER YES TO THE FOLLOWING QUESTIONS: Have you done MMP9? (SVonly) The Following are done at Baseline: Have you done Tear Osmolarity?
Page 1 of 13 BEFORE COMPLETING THE OCULAR EXAMINATION, YOU MUST BE ABLE TO ANSWER YES TO THE FOLLOWING QUESTIONS: Have you done MMP9? (SVonly) The Following are done at Baseline: Have you done Tear Osmolarity?
Photodynamic therapy for IMMK in horses
 Photodynamic therapy for IMMK in horses Overview Immune mediated keratitis in horses Traditional treatment options Sustained release implant Photodynamic therapy Use in veterinary medicine Treatment for
Photodynamic therapy for IMMK in horses Overview Immune mediated keratitis in horses Traditional treatment options Sustained release implant Photodynamic therapy Use in veterinary medicine Treatment for
Condition: Herpes Simplex Keratitis
 Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
Condition: Herpes Simplex Keratitis Description: Herpes simplex infection is very common but usually remains latent. When the virus is reactivated it travels along the trigeminal nerve to cause local infection
Dr Jo-Anne Pon. Dr Sean Every. 8:30-9:25 WS #70: Eye Essentials for GPs 9:35-10:30 WS #80: Eye Essentials for GPs (Repeated)
 Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Dr Sean Every Ophthalmologist Southern Eye Specialists Christchurch Dr Jo-Anne Pon Ophthalmologist Southern Eye Specialists, Christchurch Hospital, Christchurch 8:30-9:25 WS #70: Eye Essentials for GPs
Piratox sheet #6: "Yperite and other vesicant mustard agents"
 Edition of October 2011 Piratox sheet #6: "Yperite and other vesicant mustard agents"! Key points not to forget The 1 st emergency measures are: - extraction of victims from the hazard area: mucocutaneous
Edition of October 2011 Piratox sheet #6: "Yperite and other vesicant mustard agents"! Key points not to forget The 1 st emergency measures are: - extraction of victims from the hazard area: mucocutaneous
Ophthalmology Times Case Study Yasmin Mali, MD. Case Study
 Ophthalmology Times Case Study Yasmin Mali, MD Case Study A 57 year old female with presented with ocular irritation and discomfort in both eyes for several months. Patient was previously started on a
Ophthalmology Times Case Study Yasmin Mali, MD Case Study A 57 year old female with presented with ocular irritation and discomfort in both eyes for several months. Patient was previously started on a
Post-LASIK infections
 Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
Post-LASIK infections By Mohamed El-moddather Assiss. Prof. and head of department of ophthalmology AL-Azhar unizersity Assuit LASIK has become a common refractive procedure and is generally considered
N.B: CS, CN and CR are code names and are not derived from the chemical names or formulae.
 CROWD CONTROL AGENTS INTRODUCTION The most common crowd control agents ('CCA') are:- o-chlorobenzylidene malononitrile (CS) l-chloroacetophenone (CN, 'Mace') dibenzoxazepine (CR) oleoresin capsicum (OC,
CROWD CONTROL AGENTS INTRODUCTION The most common crowd control agents ('CCA') are:- o-chlorobenzylidene malononitrile (CS) l-chloroacetophenone (CN, 'Mace') dibenzoxazepine (CR) oleoresin capsicum (OC,
Ocular Pathology. I. Congenital and/or developmental. A. Trisomy 21. Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea)
 I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
I. Congenital and/or developmental Robbins Pathologic Basis of Disease, 6 th Ed. A. Trisomy 21 Hypertelorism (widely spaced eyes) Keratoconus (cone shaped cornea) Focal hypoplasia of iris Cataracts frequently
Corneal specimens that influence clinical decisions
 Corneal specimens that influence clinical decisions Refractive surgery Corneal dystrophies Microbial infections J. Douglas Cameron, MD Chief, Ophthalmic Pathology Division Neuropathology Department Armed
Corneal specimens that influence clinical decisions Refractive surgery Corneal dystrophies Microbial infections J. Douglas Cameron, MD Chief, Ophthalmic Pathology Division Neuropathology Department Armed
Focusing on A&E. By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel
 Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
Focusing on A&E By Sandy Cooper, (Ophthalmic Nurse Practitioner), Tel 01752 439331 Email sandra.cooper5@nhs.net sandracooper041@btinternet.com THINGS TO WORRY ABOUT WITH ANY EYE PROBLEM CHANGES IN VISION
a.superficial (adenoid layer).contain lymphoid tissue.
 Conjunctiva Dr. saifalshamarti Anatomy Microscopic: 1.Epithelium (non keratinized,includes goblet cell). 2.Epithelial basement membrane. 3.Stroma : a.superficial (adenoid layer).contain lymphoid tissue.
Conjunctiva Dr. saifalshamarti Anatomy Microscopic: 1.Epithelium (non keratinized,includes goblet cell). 2.Epithelial basement membrane. 3.Stroma : a.superficial (adenoid layer).contain lymphoid tissue.
Differential diagnosis of the red eye. Carol Slight Nurse Practitioner Ophthalmology
 Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Differential diagnosis of the red eye Carol Slight Nurse Practitioner Ophthalmology The red eye Conjunctivitis HSV Keratitis Acute angle closure glaucoma Anterior Uveitis Red eye Scleritis Subconjunctival
Ocular Allergy. Phil Lieberman, MD
 Ocular Allergy Phil Lieberman, MD Disclosure Consultant/Advisory Board: Genentech, Meda, Mylan, Teva Speaker: Genentech, Meda, Merck, Mylan, Teva Learning Objectives Upon completion of this session, participants
Ocular Allergy Phil Lieberman, MD Disclosure Consultant/Advisory Board: Genentech, Meda, Mylan, Teva Speaker: Genentech, Meda, Merck, Mylan, Teva Learning Objectives Upon completion of this session, participants
Acute Eyes for ED. Enis Kocak. The Alfred Ophthalmology
 Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
Acute Eyes for ED Enis Kocak The Alfred Ophthalmology The problem with eyes Things to cover Ocular anatomy Basic assessment Common presentations Eye first aid and procedures Ophthalmic emergencies What
Strategies for Anterior Segment Disease Management Mile Brujic, OD, FAAO 1409 Kensington Blvd Bowling Green, OH
 Strategies for Anterior Segment Disease Management Mile Brujic, OD, FAAO 1409 Kensington Blvd Bowling Green, OH 43402 brujic@prodigy.net 419-261-9161 Summary As optometry s scope of practice continues
Strategies for Anterior Segment Disease Management Mile Brujic, OD, FAAO 1409 Kensington Blvd Bowling Green, OH 43402 brujic@prodigy.net 419-261-9161 Summary As optometry s scope of practice continues
CHLOROPICRIN VAPOR EXPOSURE RESULTING FROM TREATED FIELD VAPOR
 EMERGENCY MEDICAL TREATMENT GUIDE CHLOROPICRIN VAPOR EXPOSURE RESULTING FROM TREATED FIELD VAPOR SYNONYMS: Chloropicrin, Trichloronitromethane, Nitrochloroform (label names such as Tri- Clor and Tri-Pic).
EMERGENCY MEDICAL TREATMENT GUIDE CHLOROPICRIN VAPOR EXPOSURE RESULTING FROM TREATED FIELD VAPOR SYNONYMS: Chloropicrin, Trichloronitromethane, Nitrochloroform (label names such as Tri- Clor and Tri-Pic).
Chapter 17. The Lymphatic System and Immunity. Copyright 2010, John Wiley & Sons, Inc.
 Chapter 17 The Lymphatic System and Immunity Immunity Innate Immunity Fast, non-specific and no memory Barriers, ph extremes, Phagocytes & NK cells, fever, inflammation, complement, interferon Adaptive
Chapter 17 The Lymphatic System and Immunity Immunity Innate Immunity Fast, non-specific and no memory Barriers, ph extremes, Phagocytes & NK cells, fever, inflammation, complement, interferon Adaptive
5 RIOT-CONTROL AGENTS
 Riot-Control Agents Chapter 5 RIOT-CONTROL AGENTS Summary NATO Codes: CN, CS, CR, OC, DM Signs and Symptoms: Burning and pain on exposed mucous membranes and skin, eye pain and tearing, burning in the
Riot-Control Agents Chapter 5 RIOT-CONTROL AGENTS Summary NATO Codes: CN, CS, CR, OC, DM Signs and Symptoms: Burning and pain on exposed mucous membranes and skin, eye pain and tearing, burning in the
Anatomy: There are 6 muscles that move your eye.
 Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
Thyroid Eye Disease Your doctor thinks you have thyroid orbitopathy. This is an autoimmune condition where your body's immune system is producing factors that stimulate enlargement of the muscles that
SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM
 Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML Liquifilm Sterile Eye Suspension COMPOSITION FML Liquifilm Sterile Eye Suspension contains: Fluorometholone 1,0 mg/ml Liquifilm
Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML Liquifilm Sterile Eye Suspension COMPOSITION FML Liquifilm Sterile Eye Suspension contains: Fluorometholone 1,0 mg/ml Liquifilm
INDICATIONS For steroid responsive inflammation of the palpebral and bulbar conjunctiva, cornea, and anterior segment of the eye globe.
 Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM PRED FORTE Sterile Eye Suspension COMPOSITION PRED FORTE Sterile Eye Suspension contains: Prednisolone acetate 10 mg/ml Preservative:
Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM PRED FORTE Sterile Eye Suspension COMPOSITION PRED FORTE Sterile Eye Suspension contains: Prednisolone acetate 10 mg/ml Preservative:
Table of Contents 1 Orbit 3 2 Eyelids 7
 Table of Contents Preface, x List of abbreviations xi Glossary xii Section I Atlas 1 1 Orbit 3 Clinical signs associated with orbital neoplasia 3 Clinical signs associated with orbital cellulitis 3 Enophthalmos
Table of Contents Preface, x List of abbreviations xi Glossary xii Section I Atlas 1 1 Orbit 3 Clinical signs associated with orbital neoplasia 3 Clinical signs associated with orbital cellulitis 3 Enophthalmos
The Orbit. The Orbit OCULAR ANATOMY AND DISSECTION 9/25/2014. The eye is a 23 mm organ...how difficult can this be? Openings in the orbit
 The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
The eye is a 23 mm organ...how difficult can this be? OCULAR ANATOMY AND DISSECTION JEFFREY M. GAMBLE, OD COLUMBIA EYE CONSULTANTS OPTOMETRY & UNIVERSITY OF MISSOURI DEPARTMENT OF OPHTHALMOLOGY CLINICAL
THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY
 THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY What is thyroid eye disease (TED)? TED is an autoimmune condition where the body s own immune system attacks the tissues of the thyroid gland and the eye
THYROID EYE DISEASE ORBITAL DECOMPRESSION SURGERY What is thyroid eye disease (TED)? TED is an autoimmune condition where the body s own immune system attacks the tissues of the thyroid gland and the eye
SPECIFIED PHYSICAL CONDITIONS MATRIX
 SPECIFIED PHYSICAL CONDITIONS MATRIX I. Compensation for ACUTE CONDITIONS A1 Proof Lump Sum Enhancer Declaration under penalty of perjury (1) asserting the manifestation of one or more conditions (or the
SPECIFIED PHYSICAL CONDITIONS MATRIX I. Compensation for ACUTE CONDITIONS A1 Proof Lump Sum Enhancer Declaration under penalty of perjury (1) asserting the manifestation of one or more conditions (or the
Ocular Urgencies and Emergencies
 Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Ocular Urgencies and Emergencies Pam Boyce, O.D., F.A.A.O. Boyce Family Eye Care, Ltd. 528 Devon Ave. Park Ridge, IL 60068 847-518-0303 Somebody s going to lose an eye Epidemiology 2.4 million ocular and
Learning Objectives. Disclosures 2/2/ BMT Pharmacists Conference Bandage Contact Lens Therapy for Severe Ocular GVHD
 2015 BMT Pharmacists Conference Bandage Contact Lens Therapy for Severe Ocular GVHD Tueng T. Shen, M.D., Ph.D. Professor of Ophthalmology Adjunct, Bioengineering and Global Health Feb. 13 th, 2015 Learning
2015 BMT Pharmacists Conference Bandage Contact Lens Therapy for Severe Ocular GVHD Tueng T. Shen, M.D., Ph.D. Professor of Ophthalmology Adjunct, Bioengineering and Global Health Feb. 13 th, 2015 Learning
Dystrophies. Molecular Causes. Anterior Membrane Dystrophies (epithelium, basement membrane and Bowman s layer)
 Dystrophies Characteristics of corneal dystrophies About half the members of appropriate age to have the dystrophy( usually autosomal dominant): inherited Usually seen in the first or second decade of
Dystrophies Characteristics of corneal dystrophies About half the members of appropriate age to have the dystrophy( usually autosomal dominant): inherited Usually seen in the first or second decade of
NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY
 NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY Authors: Prof univ. dr. Adriana Stănilă, Dr. Elena Mihai, Dr. Adrian Teodoru, Dr. IonuŃ Costache The Clinical Department of Op
NEW OPPORTUNITIES OF USING THERAPEUTICAL CONTACT LENSES IN OCULAR SURGERY Authors: Prof univ. dr. Adriana Stănilă, Dr. Elena Mihai, Dr. Adrian Teodoru, Dr. IonuŃ Costache The Clinical Department of Op
Lymphoid System: cells of the immune system. Answer Sheet
 Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Lymphoid System: cells of the immune system Answer Sheet Q1 Which areas of the lymph node have most CD3 staining? A1 Most CD3 staining is present in the paracortex (T cell areas). This is towards the outside
Assessment and Management of Ocular Trauma. Disclosure I have no direct financial interests in today s subject matter. 3/25/2019. Normal Eye Anatomy
 Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Assessment and Management of Ocular Trauma Samiksha Fouzdar Jain, MD,FRCS Department of Ophthalmology & Visual Sciences Truhlsen Eye Institute Disclosure I have no direct financial interests in today s
Ulcerative Keratitis (Type of Inflammation of the Cornea) Basics
 Ulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium is
Ulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium is
Trifluridine Ophthalmic Solution, 1% Sterile
 Trifluridine Ophthalmic Solution, 1% Sterile DESCRIPTION Trifluridine (also known as trifluorothymidine, F 3 TdR,F 3 T), is an antiviral drug for topical treatment of epithelial keratitis caused by herpes
Trifluridine Ophthalmic Solution, 1% Sterile DESCRIPTION Trifluridine (also known as trifluorothymidine, F 3 TdR,F 3 T), is an antiviral drug for topical treatment of epithelial keratitis caused by herpes
MINIMS AMETHOCAINE EYE DROPS
 MINIMS AMETHOCAINE EYE DROPS NAME OF THE MEDICINE Amethocaine hydrochloride Synonyms: Tetracaine hydrochloride Structural formula: Chemical name: 2-(dimethylamino)ethyl 4-(butylamino)benzoate hydrochloride
MINIMS AMETHOCAINE EYE DROPS NAME OF THE MEDICINE Amethocaine hydrochloride Synonyms: Tetracaine hydrochloride Structural formula: Chemical name: 2-(dimethylamino)ethyl 4-(butylamino)benzoate hydrochloride
Nitrogen Mustards Fact Sheet
 Nitrogen Mustards Fact Sheet Description Nitrogen mustards are vesicants and alkylating agents. They are colorless to pale yellow, oily liquids that evaporate slowly. HN-1 has a faint, fishy or musty odor.
Nitrogen Mustards Fact Sheet Description Nitrogen mustards are vesicants and alkylating agents. They are colorless to pale yellow, oily liquids that evaporate slowly. HN-1 has a faint, fishy or musty odor.
Injury. Contusion Lamellar Laceration Laceration Rupture. Penetrating IOFB. Perforating
 Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Mechanical Ocular Trauma Došková Hana, MD. Department of Ophthalmology Medicine Faculty of Masaryk University Brno General Considerations Ocular trauma constitude about 6% of all injuries, but eyes set
Innate Immunity. Bởi: OpenStaxCollege
 Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Innate Immunity Bởi: OpenStaxCollege The vertebrate, including human, immune system is a complex multilayered system for defending against external and internal threats to the integrity of the body. The
Around The Globe in 60 Minutes
 Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
Around The Globe in 60 Minutes Around the GLOBE in Sixty Minutes Basic Ocular Anatomy, Examination, and Diagnostic Techniques Introduction Focusing on canine and feline ocular anatomy and basic examination
What are some common conditions that affect the cornea?
 What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
What are some common conditions that affect the cornea? Injuries After minor injuries or scratches, the cornea usually heals on its own. Deeper injuries can cause corneal scarring, resulting in a haze
People with eye allergies typically have symptoms that include: Eye Anatomy: What Do Eye Allergies Actually Effect?
 Eye Allergies Eye Allergies People with eye allergies typically have symptoms that include: Itchy watery eyes Eyelid problems Dark circles around eyes Dry eyes Reactions to Contacts Let us help allow you
Eye Allergies Eye Allergies People with eye allergies typically have symptoms that include: Itchy watery eyes Eyelid problems Dark circles around eyes Dry eyes Reactions to Contacts Let us help allow you
NEW ZEALAND DATA SHEET 1. PRODUCT NAME
 NEW ZEALAND DATA SHEET 1. PRODUCT NAME Flucon fluorometholone 0.1% Eye Drops Suspension 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml of Flucon contains 1.0 mg of fluorometholone (0.1% w/v). Excipient
NEW ZEALAND DATA SHEET 1. PRODUCT NAME Flucon fluorometholone 0.1% Eye Drops Suspension 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each ml of Flucon contains 1.0 mg of fluorometholone (0.1% w/v). Excipient
founder of McDonald s Restaurants
 Press On Nothing in the world can take the place of persistence. Talent will not; nothing is more common than unsuccessful men with talent. Genius will not; unrewarded genius is almost a proverb. Education
Press On Nothing in the world can take the place of persistence. Talent will not; nothing is more common than unsuccessful men with talent. Genius will not; unrewarded genius is almost a proverb. Education
Oral azithromycin combined with topical anti-inflammatory agents in the treatment of blepharokeratoconjunctivitis in children
 Oral azithromycin combined with topical anti-inflammatory agents in the treatment of blepharokeratoconjunctivitis in children Daniel S. Choi, BA, and Ali Djalilian, MD Author affiliations: Department of
Oral azithromycin combined with topical anti-inflammatory agents in the treatment of blepharokeratoconjunctivitis in children Daniel S. Choi, BA, and Ali Djalilian, MD Author affiliations: Department of
VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution)
 VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution) PRODUCT OVERVIEW: VIROPTIC SOLUTION DESCRIPTION VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine,
VIROPTIC Ophthalmic Solution, 1% Sterile (trifluridine ophthalmic solution) PRODUCT OVERVIEW: VIROPTIC SOLUTION DESCRIPTION VIROPTIC is the brand name for trifluridine (also known as trifluorothymidine,
Childhood corneal neovascularization
 Miltos Balidis PhD, FEBOphth, ICOphth Sotiria Palioura MD,PhD Childhood corneal neovascularization Opacities Cornea clarity is essential for optimal vision at any age. In childhood, loss of corneal transparency
Miltos Balidis PhD, FEBOphth, ICOphth Sotiria Palioura MD,PhD Childhood corneal neovascularization Opacities Cornea clarity is essential for optimal vision at any age. In childhood, loss of corneal transparency
Sponsor. Generic Drug Name. Trial Indications. Protocol Number. Protocol Title. Clinical Trial Phase. Study Start/End Dates. Reason for Termination
 Sponsor Alcon Research, Ltd. Generic Drug Name Travoprost/timolol maleate Trial Indications Open-angle glaucoma or ocular hypertension Protocol Number C-09-007 Protocol Title An Evaluation of Patient Reported
Sponsor Alcon Research, Ltd. Generic Drug Name Travoprost/timolol maleate Trial Indications Open-angle glaucoma or ocular hypertension Protocol Number C-09-007 Protocol Title An Evaluation of Patient Reported
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM
 FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
FUCH S DYSTROPHY & CATARACT SURGERY TREATMENT ALGORITHM ΙΟΑΝΝΙS Α. MALLIAS, MD, PHD Director of the Dept. of Ophthalmology, Mediterraneo Hospital, Glyfada, Athens, Greece Clinical Fellow in Cornea and
Conjunctivitis in Cats
 Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Conjunctivitis in Cats (Inflammation of the Moist Tissues of the Eye) Basics OVERVIEW
Customer Name, Street Address, City, State, Zip code Phone number, Alt. phone number, Fax number, e-mail address, web site Conjunctivitis in Cats (Inflammation of the Moist Tissues of the Eye) Basics OVERVIEW
EYE TRAUMA: INCIDENCE
 Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Introduction EYE TRAUMA: INCIDENCE 2.5 million eye injuries per year in U.S. 40,000 60,000 of eye injuries lead to visual loss Introduction Final visual outcome of many ocular emergencies depends on prompt,
Formaldehyde (HCHO) C 1
 BASF Chemical Emergency Medical Guidelines Formaldehyde (HCHO) C 1 Information and recommendations for doctors at hospitals/emergency departments Patients exposed only to formaldehyde gas or vapor do not
BASF Chemical Emergency Medical Guidelines Formaldehyde (HCHO) C 1 Information and recommendations for doctors at hospitals/emergency departments Patients exposed only to formaldehyde gas or vapor do not
Fitting Keratoconus and Other Complicated Corneas
 Fitting Keratoconus and Other Complicated Corneas Christine W Sindt OD FAAO Professor, Clinical Ophthalmology Director, Contact Lens Service University of Iowa Disclosure Consultant: ALCON Vision Care
Fitting Keratoconus and Other Complicated Corneas Christine W Sindt OD FAAO Professor, Clinical Ophthalmology Director, Contact Lens Service University of Iowa Disclosure Consultant: ALCON Vision Care
Asthma. - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness.
 Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
Obstructive diseases Asthma - A chronic inflammatory disorder which causes recurrent episodes of wheezing, breathlessness, cough and chest tightness. - Characterized by Intermittent and reversible (the
AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION
 AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION 1 NAME OF THE MEDICINE Fluorometholone acetate. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION The active ingredient in
AUSTRALIAN PRODUCT INFORMATION FLAREX (FLUOROMETHOLONE ACETATE) EYE DROPS SUSPENSION 1 NAME OF THE MEDICINE Fluorometholone acetate. 2 QUALITATIVE AND QUANTITATIVE COMPOSITION The active ingredient in
Ammonia (NH 3 ) B 1. Information and recommendations for paramedics and doctors at the site. BASF Chemical Emergency Medical Guidelines
 BASF Chemical Emergency Medical Guidelines Ammonia (NH 3 ) B 1 Information and recommendations for paramedics and doctors at the site Before approaching the patient the paramedics and doctors at the site
BASF Chemical Emergency Medical Guidelines Ammonia (NH 3 ) B 1 Information and recommendations for paramedics and doctors at the site Before approaching the patient the paramedics and doctors at the site
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital
 Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
Sepideh Tara Rousta, MD FAAO Robert Wood Johnson University Hospital Saint Peter s University Hospital Wills Eye Hospital 14 mo old w R eye cross (parents) 9 mo old R eye crossing getting worse for past
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, :30am - 11:30am FACULTY COPY
 SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
OXFORD BIOMEDICAL RESEARCH. MSDS: Total Glutathione Assay kit Product No. GT 20
 OXFORD BIOMEDICAL RESEARCH MSDS: Total Glutathione Assay kit Product No. GT 20 This product, GT 20 Total Glutathione Assay kit, is provided and produced by Oxford Biomedical Research as an in vitro diagnostic
OXFORD BIOMEDICAL RESEARCH MSDS: Total Glutathione Assay kit Product No. GT 20 This product, GT 20 Total Glutathione Assay kit, is provided and produced by Oxford Biomedical Research as an in vitro diagnostic
Subject Index. Atopic keratoconjunctivitis (AKC) management 16 overview 15
 Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
Subject Index Acanthamoeba keratitis, see Infective keratitis Acute allergic conjunctivitis AKC, see Atopic keratoconjunctivitis Allergy acute allergic conjunctivitis 15 atopic keratoconjunctivitis 15
RESPIRATORY BLOCK. Bronchial Asthma. Dr. Maha Arafah Department of Pathology KSU
 RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
RESPIRATORY BLOCK Bronchial Asthma Dr. Maha Arafah Department of Pathology KSU marafah@ksu.edu.sa Jan 2018 Objectives Define asthma (BA) Know the two types of asthma 1. Extrinsic or atopic allergic 2.
Scleritis LEN V KOH OD
 Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Scleritis LEN V KOH OD 2014 PUCO 1 Introduction A painful, destructive, and potentially blinding disorder Highly symptomatic High association with systemic disease Immunosuppresssive agents 2014 PUCO 2
Dry eye syndrome. Lacrimal gland. Tear duct into nose. 1 of 6
 Dry eye syndrome The aim of this information sheet is to answer any questions you may have about dry eye syndrome. If you have any further questions or concerns, please ask a doctor or nurse caring for
Dry eye syndrome The aim of this information sheet is to answer any questions you may have about dry eye syndrome. If you have any further questions or concerns, please ask a doctor or nurse caring for
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST. David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.
 OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
OPHTHALMOLOGIC PEARLS FOR THE NON- OPHTHALMOLOGIST David G. Gross D.O. Deen-Gross Eye Centers Merrillville-Hobart Deengrosseye.com A FEW OF THE AREAS WE WILL DISCUSS Red Eye Glaucoma Neuro ophthalmic tid
Ocular Lecture. Sue Bednar NP Ali Atwater PA-C
 Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Ocular Lecture Sue Bednar NP Ali Atwater PA-C Triaging Ocular Complaints Painful Eye/Red eye +/-blurry vision +/-visual loss +/-floaters +/-fevers If any of the above findings exist, pt is likely to have
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics
 Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium
Nonulcerative Keratitis (Type of Inflammation of the Cornea) Basics OVERVIEW Keratitis is inflammation of the cornea; the cornea is the clear outer layer of the front of the eye The corneal epithelium
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT
 HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
HEMORRHAGIC BULLOUS HENOCH- SCHONLEIN PURPURA: A CASE REPORT Nirmala Ponnuthurai, Sabeera Begum, Lee Bang Rom Paediatric Dermatology Unit, Institute of Paediatric, Hospital Kuala Lumpur, Malaysia Abstract
Sclerokeratoplasty David S. Chu, M.D. Cases
 Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
Sclerokeratoplasty David S. Chu, M.D. Cases Case 1 40 year-old female from Peru presented to our Service with inflamed OS for 2 months duration. Her symptoms began as red painful OS, which progressively
EXPERIMENTAL THERMAL BURNS I. A study of the immediate and delayed histopathological changes of the skin.
 EXPERIMENTAL THERMAL BURNS I A study of the immediate and delayed histopathological changes of the skin. RJ Brennan, M.D. and B. Rovatti M.D. The purpose of this study was to determine the progressive
EXPERIMENTAL THERMAL BURNS I A study of the immediate and delayed histopathological changes of the skin. RJ Brennan, M.D. and B. Rovatti M.D. The purpose of this study was to determine the progressive
Title: Keeping Step with DEWS2: Clinical Applications Lecturer: Scott G. Hauswirth, OD
 Title: Keeping Step with DEWS2: Clinical Applications Lecturer: Scott G. Hauswirth, OD Course Description: The Dry Eye Workshop 2 was an assemblage of experts in dry eye disease from around the world,
Title: Keeping Step with DEWS2: Clinical Applications Lecturer: Scott G. Hauswirth, OD Course Description: The Dry Eye Workshop 2 was an assemblage of experts in dry eye disease from around the world,
SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM
 Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML-NEO Liquifilm Ophthalmic Suspension COMPOSITION FML-NEO Liquifilm Ophthalmic Suspension contains per ml: Fluorometholone 1,0
Page 1 of 5 SCHEDULING STATUS Schedule 4 PROPRIETARY NAME AND DOSAGE FORM FML-NEO Liquifilm Ophthalmic Suspension COMPOSITION FML-NEO Liquifilm Ophthalmic Suspension contains per ml: Fluorometholone 1,0
D90 (27/10/2005) Final SmPC NL/H/653/01
 1/6 1. NAME OF THE MEDICINAL PRODUCT MONOFREE DEXAMETHASON 1 mg/ml, eye drops, solution 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 ml solution contains 1 mg of dexamethasone phosphate as dexamethasone
1/6 1. NAME OF THE MEDICINAL PRODUCT MONOFREE DEXAMETHASON 1 mg/ml, eye drops, solution 2. QUALITATIVE AND QUANTITATIVE COMPOSITION 1 ml solution contains 1 mg of dexamethasone phosphate as dexamethasone
THERAPEUTIC CONTACT LENSES
 THERAPEUTIC CONTACT LENSES Prof. Univ. Dr. Adriana Stanila Victor Papilian Faculty of Medicine Emergency Academic Hospital Sibiu Ocular Surface Research Center ROMANIA INTRODUCTION therapeuein greac =
THERAPEUTIC CONTACT LENSES Prof. Univ. Dr. Adriana Stanila Victor Papilian Faculty of Medicine Emergency Academic Hospital Sibiu Ocular Surface Research Center ROMANIA INTRODUCTION therapeuein greac =
Ocular Trauma Chemical Injuries
 Ocular Trauma Chemical Injuries Ramesh Venkatesh*, Hemkala L Trivedi** Introduction Background : Chemical injuries to the eye represent one of the true ophthalmic emergencies. While almost any chemical
Ocular Trauma Chemical Injuries Ramesh Venkatesh*, Hemkala L Trivedi** Introduction Background : Chemical injuries to the eye represent one of the true ophthalmic emergencies. While almost any chemical
Cases CFEH. CFEH Facebook Case #4
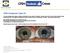 CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
CFEH Cases CFEH Facebook Case #4 A 42 year old female has noticed a floater in her left eye for many years but no flashes. She also reports hazy vision in this eye that has been present all her life. She
Chemical Names: Prednisolone acetate: 11ß,17,21-Trihydroxypregna-1,4-diene-3,20-dione 21-acetate.
 PRED-G (gentamicin and prednisolone acetate ophthalmic suspension, USP) 0.3%/1% sterile DESCRIPTION PRED-G sterile ophthalmic suspension is a topical anti-inflammatory/anti-infective combination product
PRED-G (gentamicin and prednisolone acetate ophthalmic suspension, USP) 0.3%/1% sterile DESCRIPTION PRED-G sterile ophthalmic suspension is a topical anti-inflammatory/anti-infective combination product
INVELTYS (loteprednol etabonate ophthalmic suspension) 1%, for topical ophthalmic use Initial U.S. Approval: 1998
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use INVELTYS safely and effectively. See full prescribing information for INVELTYS. INVELTYS (loteprednol
Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report
 ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
ISPUB.COM The Internet Journal of Neurology Volume 9 Number 2 Herpes Zoster Ophtalmicus in a HIV positive patient: A Case Report G Lopez Bejerano, Y Graza Fernandez Citation G Lopez Bejerano, Y Graza Fernandez..
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Dr Rachael Neiderer. Ophthalmologist Auckland. 8:35-8:50 Managing Allergic Conjunctivitis & Why Sodium Chromoglycate is Out
 Dr Rachael Neiderer Ophthalmologist Auckland 8:35-8:50 Managing Allergic Conjunctivitis & Why Sodium Chromoglycate is Out Allergic conjunctivitis Rachael Niederer Greenlane Clinical Centre, Auckland Case
Dr Rachael Neiderer Ophthalmologist Auckland 8:35-8:50 Managing Allergic Conjunctivitis & Why Sodium Chromoglycate is Out Allergic conjunctivitis Rachael Niederer Greenlane Clinical Centre, Auckland Case
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
Acid anhydrides (e.g. maleic/phthalic anhydride, C 4 H 2 O 3 /C 8 H 4 O 3 ) C 1
 BASF Chemical Emergency Medical Guidelines Acid anhydrides (e.g. maleic/phthalic anhydride, C 4 H 2 O 3 /C 8 H 4 O 3 ) C 1 Information and recommendations for doctors at hospitals/emergency departments
BASF Chemical Emergency Medical Guidelines Acid anhydrides (e.g. maleic/phthalic anhydride, C 4 H 2 O 3 /C 8 H 4 O 3 ) C 1 Information and recommendations for doctors at hospitals/emergency departments
Overview & pathophysiology of Dry Eye and the use of cyclosporine eye drops in dry eye...
 Overview & pathophysiology of Dry Eye and the use of cyclosporine eye drops in dry eye... This Allergan sponsored session was held on July 24, 2005, Hotel Satya Ashoka, Jabalpur. The session was followed
Overview & pathophysiology of Dry Eye and the use of cyclosporine eye drops in dry eye... This Allergan sponsored session was held on July 24, 2005, Hotel Satya Ashoka, Jabalpur. The session was followed
Dry eye syndrome is more likely to affect people who are over the age of 60, and the condition is more common among women than men.
 DRY EYE Introduction Dry eye syndrome, also known as keratoconjunctivitis sicca, is a condition where your eyes do not make enough tears, or your tears evaporate too quickly. This can lead to your eyes
DRY EYE Introduction Dry eye syndrome, also known as keratoconjunctivitis sicca, is a condition where your eyes do not make enough tears, or your tears evaporate too quickly. This can lead to your eyes
Deep Anterior Lamellar Keratoplasty - Techniques
 Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Deep Anterior Lamellar Keratoplasty - Techniques SHERAZ DAYA MD FACP FACS FRCS(Ed) FRCOphth Financial Disclosure Company Code 1. Abbott Medical Optics Inc. S 2. Bausch + Lomb C,L 3. Carl Zeiss Meditec
Immunocompetence The immune system responds appropriately to a foreign stimulus
 Functions of the immune system Protect the body s internal environment against invading organisms Maintain homeostasis by removing damaged cells from the circulation Serve as a surveillance network for
Functions of the immune system Protect the body s internal environment against invading organisms Maintain homeostasis by removing damaged cells from the circulation Serve as a surveillance network for
Medical Affairs Policy
 Medical Affairs Policy Service: Corneal Treatments and Specialized Contact Lenses (Corneal remodeling, Corneal transplant, Corneal collagen crosslinking, Intrastromal Rings- INTACS, Keratoconus treatments,
Medical Affairs Policy Service: Corneal Treatments and Specialized Contact Lenses (Corneal remodeling, Corneal transplant, Corneal collagen crosslinking, Intrastromal Rings- INTACS, Keratoconus treatments,
Chapter 24 The Immune System
 Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Chapter 24 The Immune System The Immune System Layered defense system The skin and chemical barriers The innate and adaptive immune systems Immunity The body s ability to recognize and destroy specific
Some of the ophthalmic surgeries
 Some of the ophthalmic surgeries Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary
Some of the ophthalmic surgeries Some of the ophthalmic surgeries performed at the DMV Center. This document presents some types of the surgeries performed by the ophthalmology service at the DMV veterinary
