From the Rheumatology Department, Kettering General Hospital, Kettering, UK
|
|
|
- Theresa Holland
- 5 years ago
- Views:
Transcription
1 Q J Med 2012; 105: doi: /qjmed/hcr242 Advance Access Publication 23 December 2011 Review Recent advances in management of gout E. SURESH and P. DAS From the Rheumatology Department, Kettering General Hospital, Kettering, UK Address correspondence to E. Suresh, Rheumatology Department, Kettering General Hospital, Rothwell Road, Kettering, NN16 8UZ, UK. dr_esuresh@hotmail.com Summary Incidence and prevalence of gout have markedly increased over the last few decades in keeping with the rise in prevalence of obesity and metabolic syndrome. Until recently, management of gout in patients with associated metabolic syndrome and comorbid illnesses such as renal impairment was difficult because of limited treatment options. However, significant progress has been made in the last few years, with introduction of new treatments such as interleukin-1 antagonists for management of acute gout, and febuxostat and pegloticase for chronic gout. The association of gout with alcohol, dietary purines and fructose ingestion has been Gout is the most common form of inflammatory arthritis in men over the age of 40, with estimated prevalence in the UK of 1.4%. 1,2 It is characterized by recurrent episodes of extremely painful and debilitating joint and/or soft tissue inflammation induced by monosodium urate (MSU) crystals (acute gout). Patients with chronic uncontrolled hyperuricaemia develop macroscopic aggregates of MSU in soft tissues that can lead to disabling and deforming arthropathy (chronic tophaceous gout). Some patients with persistent hyperuricaemia develop urate nephropathy and renal calculi. Additionally, >60% of patients with gout are diagnosed with metabolic syndrome that includes central obesity, hypertension, insulin resistance and hyperlipidaemia. 3 Patients with gout also have a higher risk of death, mainly because of coronary confirmed in large prospective studies, thus enabling the clinician to now provide evidencebased advice to patients. Recent efficacy and safety data favour lower over higher doses of colchicine, and oral corticosteroids over non-steroidal anti-inflammatory drugs for patients with acute gout. Local ice therapy might help to differentiate gout from other forms of inflammatory arthritis, and supplementation with vitamin C help to reduce risk of gout. Several other drugs with rational mechanisms of action are in the pipeline, and likely to be introduced over the next few years. A new era has thus begun in the field of gout. heart disease. 4 Thus, gout is associated with significant morbidity, higher mortality, functional impairment and reduced quality of life. 5 7 Several recent studies have indicated that incidence and prevalence of gout have markedly increased over the last three decades, in keeping with the rise in prevalence of obesity and metabolic syndrome. 8,9 Management of gout in patients with associated metabolic syndrome and comorbid illnesses such as chronic kidney disease was, however, difficult because of limited treatment options. For example, it was challenging to select an appropriate drug to control acute polyarticular gout in an elderly patient with history of chronic kidney disease, hypertension, diabetes and previous intolerance to colchicine because of increased likelihood of drug toxicity and potential to worsen associated! The Author Published by Oxford University Press on behalf of the Association of Physicians. All rights reserved. For Permissions, please journals.permissions@oup.com
2 408 E. Suresh and P. Das illnesses with both non-steroidal anti-inflammatory drugs (NSAIDs) as well as corticosteroids. 10 Likewise, if gout patients with chronic kidney disease developed hypersensitivity reactions with allopurinol, it was challenging to choose an appropriate prophylactic agent because alternative therapeutic options were limited. These drawbacks called for more pharmacological options, both for controlling acute attacks of gout as well as for long-term prophylaxis. Although no major advances happened in the field of gout for over 40 years since allopurinol was introduced in 1965, 11 several exciting new therapies have been studied in the last few years, marking the onset of a new era in the field of gout. Some of these drugs have already been introduced into practice. Several more drugs with rational mechanisms of action are in the pipeline, and likely to be introduced in the next few years. The remainder of this article aims to provide an update for the general physician on some of these recent advances focussing on progress in (i) management of acute gout and (ii) long-term management options. The article concludes with discussion of future directives. Information presented in this review was collected by searching Medline (from 2004 to October 2011) using several search terms in combination with gout including colchicine, NSAIDs, corticosteroid, prednisolone, biological therapies, anakinra, canakinumab, rilonacept, topical ice, allopurinol, febuxostat, rasburicase, pegloticase, vitamin C, diet, alcohol, fructose, CT scan and ultrasound. The search returned several hundreds of papers, but only key studies that led to advancement in the field of gout, and those that were published in English were included. Citations of these papers were used to get additional relevant studies. Expert reviews, some recent guidelines as well as abstracts presented at recent International conferences (American College of Rheumatology, European League against Rheumatism and British Society of Rheumatology) were also studied. Progress in management of acute gout Acute gout is a self-limiting condition that lasts for 7 10 days, but treatment ensures pain relief and speeds recovery. Drugs used to treat an acute episode of gout aim to control the inflammatory reaction induced by MSU crystals. None of the available options including NSAIDs, corticosteroids or colchicine are universally effective or completely safe. NSAIDs are the drugs of choice in patients without comorbid illnesses, but are inappropriate for patients with renal impairment, congestive cardiac failure and peptic ulcer disease, in the very elderly, and in those receiving anti-coagulant treatment. It is also worth noting that NSAIDs have to be used in a higher than usual dose for patients with acute gout, especially in the first 24 h to get adequate control of inflammation. 12 Such higher doses can potentially cause gastric toxicity, and reduce creatinine clearance by 25% in most patients (relevant in patients with pre-existing renal impairment). There have also been concerns about cardiovascular safety, especially with the use of selective COX-II (cyclooxygenase) NSAIDs, 13 and it may be prudent to avoid these drugs in patients with pre-existing ischaemic heart or cerebrovascular disease. Corticosteroids are also effective but even short courses may affect blood pressure or glucose control, and their use might be problematic among post-operative patients because of increased risk of infection and impaired wound healing. Colchicine is another useful option, particularly in patients in whom a NSAID or corticosteroids cannot be used, but it has a narrow therapeutic index. Patients can develop gastrointestinal side effects such as diarrhoea, nausea and vomiting, especially when high doses are used. 14 The good news is that some new therapies have been studied in the last few years, thus widening the choice, especially for those patients with comorbid illnesses. These newer therapies along with other recent key advances in management of acute gout are discussed further in this section. Newer treatments for gout Biological therapies, which target specific elements of the immune system that play a key role in pathogenesis, are widely used for management of various rheumatic diseases such as rheumatoid arthritis (RA), psoriatic arthritis, ankylosing spondylitis, juvenile idiopathic arthritis, systemic lupus erythematosus and systemic vasculitis. These therapies have recently been explored for patients with gout as well. There are several cytokines such as interleukin-1 (IL-1), IL-8 and TNF-a that play a role in pathogenesis of gout, but IL-1b seems to be the key mediator. 15 Based on animal experiments, it was well known that monocytes and macrophages produced IL-1b in response to MSU crystals, and that inhibition of IL-1 resulted in suppression of gout inflammation. 16 These observations led to the conduct of the first human trial with IL-1 antagonists among patients with gout a few years ago. It was an open-labelled study that tested efficacy and safety
3 Gout advances 409 of anakinra (IL-1 receptor antagonist) among 10 patients who failed conventional treatments such as NSAIDs, colchicine or corticosteroids. Anakinra, administered subcutaneously for 3 days resulted in rapid and complete pain relief in 9 out of 10 patients within 48 h and importantly, without causing any side-effects. 17 This was in contrast to the incomplete response often seen with currently available therapies. Other drugs that inhibit IL-1 have been developed since in the last few years, including rilonacept (soluble IL-1 receptor that binds with IL-1 to prevent it from binding with its original receptor) and canakinumab (monoclonal antibody against IL-1b). Some early trials have shown that much better and more rapid pain relief could be achieved with these drugs compared to placebo and corticosteroids. 18,19 They have also been shown to be effective in reducing gouty flares among patients commencing long-term prophylactic treatment with allopurinol. 20 Results of some larger trials are awaited but going by the results of these early studies, it could be predicted that IL-1 antagonists are likely to emerge as promising new addition to the therapeutic armamentarium for patients with gout. They would certainly expand treatment options for those patients in whom cardiovascular, renal and gastrointestinal comorbidity would preclude use of NSAIDs, corticosteroids and colchicine. It is also worth mentioning here that anakinra was initially tested and used for patients with RA, but it is not used for that indication at present in the UK because of disapproval by National Institute for health and Clinical Excellence (NICE). Anakinra is very expensive (a single pre-filled syringe of anakinra costs 26.23) when used for treating patients with RA, as it needs to be administered daily, but drug costs of treating gout are a lot lower because of the short treatment courses. Although not formally tested, anakinra, because of its rapid onset of action, is likely to reduce hospital stay and bed costs for in-patients who develop gout, and therefore prove cost-effective. 12 This is particularly important because studies have shown that an acute flare of gout can extend hospital stay for in-patients by at least 3 days. 21 Efficacy and safety of low-dose colchicine Another notable recent advance has been the demonstration of efficacy and safety of low-dose colchicine. Colchicine has been used for gout since ancient times but higher doses were recommended previously ( 1 mg initially followed by 500 mg every 2 3 h until relief of pain is obtained or vomiting or diarrhoea occurs or until a total dose of 6 mg has been reached according to previous editions of the British National Formulary [BNF]). Gastrointestinal toxicity is common with such high doses. Hence, this was challenged by an article in the British Medical Journal that recommended the use of lower doses of colchicine (500 mg three times daily or less frequently in patients with renal impairment) based on personal experiences of many rheumatologists and some empirical studies. 22 The EULAR (European League against Rheumatism) guidelines for management of gout also supported the use of lower doses of colchicine, 23 and the BNF then changed its recommendation to 500 mg 2 4 times daily until symptoms relieved, maximum 6 mg per course. However, only one controlled trial had ever been conducted before with colchicine among patients with gout, 24 and there was no trial evidence to support the use of lower doses of colchicine. More recently, a double-blind, randomized controlled trial among patients with acute gout flare has demonstrated that lower doses of colchicine (1.2 mg followed by 0.6 mg after an hour, total dose of 1.8 mg) were as effective as higher doses (1.2 mg followed by 0.6 mg every hour for up to 6 h, total dose of 4.8 mg) in relieving pain. 25 This was achieved at the cost of no increased risk of toxicity for the lower dose of colchicine compared to placebo. The other important key to successful control of an acute episode is timing of therapy. All patients in this trial were commenced on treatment within 12 h of onset of an attack of gout, and it has indeed been suggested before that colchicine is most effective when commenced at the onset of an attack of gout before phagocytosis establishes itself. 26 The results of this trial have important implications for promoting safer use of colchicine in practice. Efficacy of corticosteroids versus NSAIDs Several head to head trials comparing different NSAIDs have been performed among patients with acute gout before, but none comparing the three groups of drugs (colchicine, NSAID and corticosteroids) against each other. Since NSAIDs are associated with gastrointestinal, renal and cardiovascular adverse effects, one recent double-blind randomized controlled trial compared efficacy and safety of prednisolone versus naproxen for patients with acute gout. 27 Both drugs were found to be equally effective in achieving pain reduction over the first 4 days, and adverse effects were noted to be mild and similar. Another double-blind randomized controlled trial 28 showed that oral
4 410 E. Suresh and P. Das prednisolone was as effective as indomethacin in achieving pain relief, and caused fewer side effects. The results of these trials have implications for managing gout in patients with renal impairment (creatinine clearance <60 ml/min), in whom it may be preferable to choose corticosteroids. Prednisolone was used in a dose of mg/day for 5 days in these two trials. A dose of mg/ day, gradually tapering over 10 days (to prevent rebound flare) has also been suggested before. 29 Such larger doses of prednisolone are required because gout episodes are known to occur in renal transplant patients receiving 7.5 mg of prednisolone/day. 30 As discussed earlier, corticosteroids should be used with caution among diabetic and post-operative patients. Usefulness of topical ice for acute attacks of gout Local ice therapy is another useful therapeutic modality for patients with acute gout. A randomized trial with a small sample size of 19 patients had previously shown that pain reduction among patients with acute gout was greater when local ice therapy was added to their usual therapy including prednisolone and colchicines. 31 More recently, it has been suggested on the basis of a prospective study that response to topical ice is more specific for gout, and that this may help to differentiate gout from other forms of inflammatory arthritis. 32 Interestingly, patients with RA who reported improvement with topical ice subsequently had their joint effusions aspirated and were found to have MSU or calcium pyrophosphate crystals in their synovial fluid, suggesting co-existence of the two conditions or previous misdiagnosis. It is therefore worth recommending topical ice application as an adjunctive treatment for patients with acute gout. Progress in long-term management of gout There are three prerequisites for development of gout: (i) development of hyperuricaemia leading to serum urate saturation (ii) formation of MSU crystals from saturated serum and (ii) interaction between MSU crystals and inflammatory system. Drugs given for long-term prophylaxis act at step (i), aiming to reduce serum urate levels. 33 If serum urate is reduced to below saturation point, then MSU crystals will dissolve and no new crystals can form, thereby offering the potential to cure gout. 34 EULAR guidelines recommend reducing serum urate to <360 mmol/l, 23 whereas the British Society of Rheumatology recommends a stricter target of 300 mmol/l. 35 Urate lowering therapy is generally offered for patients with recurrent acute episodes, chronic tophaceous gout, structural joint damage and renal calculi. For many years, only two classes of drugs were used for lowering serum urate in patients who needed prophylactic treatment: uricostatic drugs (allopurinol), which reduced uric acid production through competitive inhibition of xanthine oxidase (the enzyme that converts xanthine and hypoxanthine to uric acid) and uricosuric drugs (sulphinpyrazone, probeneceid and benzbromarone), which increased urinary uric acid excretion by blocking renal tubular re-absorption of urate. Allopurinol is the drug of choice in almost all patients who require prophylactic treatment. It is generally a safe drug, but 2% of patients develop hypersensitivity reactions, which can sometimes be severe and fatal with mortality rate of 20%. 36 Such reactions are more likely among patients with renal impairment, in whom the dose of allopurinol has not been appropriately reduced. 37 Allopurinol desensitization can be tried for patients with milder reactions, but this is not easy to achieve in practice, and often unsuccessful. Also, lower doses of allopurinol that are used in patients with renal impairment do not adequately control gout. 38 Uricosuric drugs are an option in patients who are intolerant of allopurinol, but they are contraindicated in those with renal calculi, and ineffective in patients with renal impairment (although benzbromarone can be used in patients with creatinine clearance as low as 25 ml/min). Moreover, probeneceid is not available in the UK, 39 and benzbromarone is not licensed because of its association with fulminant hepatic failure. 40 Patients with renal impairment and those who were intolerant of allopurinol, therefore, posed therapeutic challenges because of limited alternative options. In the last few years, two new treatments have become available: febuxostat, a novel xanthine oxidase inhibitor, and pegloticase, a recombinant uricase. 41,42 These new treatments have widened therapeutic options for challenging patients, and are discussed further in this section along with some new evidence on usefulness of vitamin C in reducing risk of developing gout. Results of recent large prospective studies that confirmed association of gout with alcohol intake, dietary purines and fructose ingestion are also discussed.
5 Gout advances 411 Febuxostat: a novel xanthine oxidase inhibitor Febuxostat is a non-purine, xanthine oxidase inhibitor with a chemical structure different from allopurinol. 43 It was recently approved by NICE for use in patients intolerant of allopurinol. No hypersensitivity reactions have been reported with febuxostat so far, and it might be associated with less toxicity compared to allopurinol. This is probably because it does not inhibit any other enzyme, apart from xanthine oxidase in the purine or pyrimidine metabolic pathway. The other advantage with febuxostat is that dose adjustments are not needed in patients with mild to moderate renal impairment, as it is mainly metabolized in the liver. 44 Febuxostat has been shown to be more effective in reducing serum urate levels compared to allopurinol and placebo It should, however, be noted that allopurinol was used in a fixed dose of 300 mg/ day in trials, and it is not known if febuxostat would have been as effective as higher doses of allopurinol (in practice, allopurinol can be increased up to 900 mg/day, assuming compliance and normal renal function). There is of course an increasing risk of intolerance with higher doses of allopurinol, and hence, the recommendation to use allopurinol as first line therapy with gradual titration of the dose to achieve target urate levels, and febuxostat only in those patients who are intolerant to allopurinol. Febuxostat is initiated in a dose of 80 mg once daily, but if urate levels remain high, the dose could be increased up to 120 mg/day after 4 weeks (in the USA, approval has been granted for use of 40 and 80 mg). Like allopurinol, febuxostat should not be commenced during or soon after an acute episode of gout. Gout flares are common in the first few months after commencing treatment with febuxostat, and hence, prophylaxis with colchicine or NSAID is recommended for up to 6 months. Liver function test abnormalities are known to occur in patients taking febuxostat, and the recommendation is to check and confirm satisfactory liver function before commencing treatment. It would also be prudent to check liver function periodically after commencing treatment. Since some trials have shown numerically higher cardiovascular events among patients receiving febuxostat compared to other treatments, 45,46,50 the European Medicines Agency does not recommend its use in patients with pre-existing ischaemic heart disease or congestive cardiac failure. Febuxostat is generally well tolerated, but some patients (1 2%) may experience side effects like nausea, diarrhoea and headache. Because azathioprine is metabolized by xanthine oxidase, it is best to avoid febuxostat in patients receiving this drug (relevant in posttransplant patients on azathioprine who develop gout). In summary, treatment with febuxostat would be appropriate for (i) patients intolerant of allopurinol, (ii) patients with mild or moderate renal impairment (creatinine clearance of >30 ml/min) and (iii) patients in whom gout cannot be controlled with allopurinol or other treatments. Uricolytic drugs for treatment of refractory gout Unlike lower mammals, humans do not possess the enzyme uricase (uric acid oxidase) that catalyses conversion of uric acid to allantoin. Allantoin is highly water soluble, and hence more readily excreted by kidneys. The use of uricase is therefore an attractive option for management of gout. 51 Rasburicase, a recombinant uricase, has long been used by oncologists for management of hyperuricaemia among patients with tumour lysis syndrome, but rasburicase itself is not suitable for use in patients with gout because of its very short halflife of <18 h. 52 This would necessitate frequent administration of rasburicase, but that would be impractical because of its very high antigenicity. Hence, a pegylated form of uricase (pegloticase) has recently been developed and tested among patients with refractory gout (pegylated simply means that the drug is conjugated with polyethylene glycol to prolong its half life and reduce antigenicity). 53 Pegloticase has been shown to rapidly reduce serum urate levels and debulk tophi. In early studies, target serum urate levels were achieved in 42% of patients, and resolution of tophi noted in 40%. 54,55 Due to the rapid reduction of serum urate levels, >80% of patients experience acute gout flares, and hence, pegloticase is co-prescribed with colchicine, NSAID or corticosteroids. It was recently approved by FDA (Federation of Drugs Administration) in the USA for treatment of chronic gout in adult patients refractory to conventional therapy, and an application has been submitted for approval in the European Union as well. Pegloticase has to be given by intravenous infusion every 2 4 weeks, but it can only be used over a finite period of time (3 6 months) because many patients eventually develop anti-pegloticase antibodies that could reduce efficacy and cause infusion reactions. Infusion reactions can be predicted by serum urate rising to over the target level of 357 mmol/l (indicating presence of anti-pegloticase antibodies and loss of drug efficacy). It has been suggested that if serum urate is monitored regularly and pegloticase discontinued when urate rises to
6 412 E. Suresh and P. Das >357 mmol/l, then infusion reactions can be avoided in >90% of patients. In summary, pegloticase would be appropriate for short-term use, mainly for rapid debulking of tophi in patients with treatment-refractory, chronic tophaceous gout, prior to using other drugs such as allopurinol or febuxostat to maintain control over the longer term. Usefulness of vitamin C for patients with gout Another interesting recent development is the realization that vitamin C supplementation is useful for patients with gout. It has long been known that vitamin C lowers serum urate via a uricosuric effect but it was thought that mega doses were required to achieve this effect. 56 A recent double-blind, randomized controlled trial found that vitamin C in a dose as low as 500 mg/day was better than placebo in reducing serum urate levels. The reduction in serum urate was as much as 10% at the end of 2 months in the vitamin C group compared to no reduction in the placebo group. Another large prospective follow-up study of health professionals in the USA reported up to 45% lower risk of gout for vitamin C intake of >1500 mg/day, and 34% lower risk for vitamin C intake between 1000 and 1499 mg/day compared to no intake of vitamin C, and independent of dietary and other risk factors. 57,58 Supplemental vitamin C in doses of mg/ day could therefore be recommended for patients with gout but this should not replace standard advice on diet and alcohol. Association of gout with alcohol intake, dietary purines and fructose ingestion The association of gout with alcohol intake and increased dietary purine consumption had been known since ancient times, but there were no prospective trial data to back up this notion. The recently reported results of the large Health Professionals Follow-up study involving male participants have now confirmed these associations These subjects had been followed up since Those with gout were excluded at baseline, and 730 subjects developed gout during 12 years of follow-up. Increased risk of gout was found with higher levels of meat (particularly beef, pork or lamb) and seafood consumption but not with consumption of animal or vegetable protein and purine-rich vegetables. 63 Eating purine-rich vegetables such as beans, peas and lentils is, therefore, not associated with increased risk of gout. A lower incidence of gout was also found among those with higher intake of low-fat dairy products (explained by uricosuric effects of milk proteins such as casein and lactalbumin). Conversely, a significant increase in serum urate levels following 4 weeks of dairy-free diet was demonstrated in another randomized trial. 65 Association between gout and alcohol intake was also confirmed in the same cohort. 64 Risk of gout was proportional to the amount of alcohol consumed, with risk varying according to the type of beverage consumed. Beer conferred a larger risk than spirits (perhaps because of its purine content), while moderate drinking of wine (two 4-oz glasses per day) did not increase risk of gout. The increased risk of gout with alcohol and dietary factors was independent of other standard risk factors such as age, body mass index, hypertension, chronic renal impairment and diuretic therapy. Conventional dietary recommendations have focused on restricting purine intake but recent studies have highlighted the importance of fructose containing sugar sweetened soft drinks in increasing risk of gout. 66,67 There has been substantial increase in consumption of fructose rich beverages in parallel with the rise in prevalence of obesity, metabolic syndrome, hyperuricaemia and gout over the last few decades. Consumption of naturally occurring fructose such as fruit or fruit juices may also increase risk. Eating an apple or orange a day, for example, can increase risk of gout by 64%. Current data, however, do not support a change in current advice on fruit intake because of their benefits in reducing cardiovascular risk. Diet soft drinks, on the other hand, do not increase risk of gout, while long-term consumption of coffee may actually reduce risk. 68 These recent findings have important practical implications for prevention and management of gout. Patients should be informed that their risk of gout could be reduced even without the use of drug treatments through modification of diet, and reduction of alcohol and fructose consumption. An earlier study had, in fact, demonstrated that weight loss achieved through reducing dietary saturated fat and carbohydrate intake with proportional increase in protein and unsaturated far consumption could not only reduce serum urate levels but also frequency of gout attacks. 69 Such a diet would also, of course, have cardiovascular benefits by improving insulin sensitivity and reducing triglyceride levels. Crash dieting and fasting should, however, be discouraged because of their potential to cause ketoacidosis and precipitate acute attacks of gout.
7 Gout advances 413 Table 1 Learning points on progress in management of acute gout IL-1 antagonists can rapidly control inflammation among patients with acute gout, and without causing any side effects. IL-1 antagonists are particularly likely to be useful in patients in whom cardiovascular, renal and gastrointestinal morbidity would preclude the use of NSAIDs, corticosteroids and colchicine. Lower doses of colchicine are as effective as higher doses in controlling inflammation among patients with acute gout, and at the cost of no increased risk of toxicity compared to placebo. Corticosteroids are comparable in efficacy to NSAIDs, and cause fewer side effects; they are, therefore, a useful option for patients with renal impairment. Local ice is a useful adjunctive therapeutic modality for patients with acute gout; response to ice may help to distinguish gout from other forms of inflammatory arthritis. Table 2 Learning points on progress in long-term management of gout Therapeutic options for allopurinol-intolerant patients were limited until recently. Two new drugs have become available recently: febuxostat, a novel xanthine oxidase inhibitor, and pegloticase, a recombinant uricase. Febuxostat is recommended for patients intolerant of allopurinol. Febuxostat can safely be used in patients with mild to moderate renal impairment (creatinine clearance >30 ml/min). Pegloticase (recombinant uricase) could be used in the short-term for rapid debulking of tophi in patients with treatment-refractory chronic gout prior to using other drugs such as allopurinol or febuxostat to maintain control over the longer term. Infusion reactions are common with pegloticase, but could be predicted by rising serum urate levels (>357 mmol/l) Supplemental vitamin C ( mg/day) may be beneficial in prevention of gout. Risk of gout is increased with alcohol intake (especially beer), higher consumption of meat and seafood, and ingestion of fructose. The way forward In conclusion, several exciting developments have taken place in the field of gout in the last few years, with improved understanding of pathogenesis, introduction of new treatments, better use of existing therapies and publication of treatment guidelines. The future too appears promising, with several other drugs in the pipeline (Table 3). These experimental drugs, when they become available, would no doubt widen therapeutic options for challenging patients. Some molecular targets that are currently being studied include URAT-1(urate anion exchange transporter), which transports urate from renal tubular lumen into epithelial cells, purine nucleoside phosphorylase (PNP), an enzyme that functions in the purine salvage pathway and phosphodiesterase-4 (PDE4) that mediates inflammation Diagnostic methods for gout have also significantly improved in recent years with introduction of advanced imaging techniques such as ultrasound, computed tomography (CT) and magnetic resonance imaging (MRI). 73 They are useful to make an early and non-invasive diagnosis of gout as well as monitor response to urate lowering therapy in the long term. Ultrasound, for example, is more sensitive than plain radiographs in detecting gouty erosions, and for diagnosing tophi and guiding synovial fluid aspiration. 74,75 More recently, dual energy CT has been shown to be an extremely useful non-invasive tool for early diagnosis of gout and uric acid urolithiasis because of its ability to differentiate MSU from calcium. 76 Tophaceous deposits can be diagnosed even during pre-clinical stage using this modality. If and when dual energy CT is introduced into practice, it would allow for early commencement of treatment in patients with crystal deposition and inflammation. This would not only offer the potential to prevent articular damage, but also improve cardiovascular outcomes because of the association of gout with myocardial infarction. Despite introduction of new drugs and diagnostic modalities, practical management of gout remains sub-optimal Many patients with gout, especially those with renal impairment receive inadequate therapy in practice, and therefore do not achieve target serum urate levels. Serum urate levels are not monitored satisfactorily following commencement of urate lowering therapy, or even when they are measured, the dose of allopurinol is not titrated accordingly to achieve target urate
8 414 E. Suresh and P. Das Table 3 Some gout drugs in development Lesinurad (RDEA594) Blocks URAT-1 more selectively than currently available uricosuric drugs levels. 80 Compliance with urate lowering therapy remains poor, with only 50% of patients still receiving allopurinol after the first year of therapy Studies have also shown that about a third of patients with acute gout are treated inappropriately with a hypouricemic agent. 83 There is therefore an urgent need to educate patients as well as physicians to improve outcome. 84 There are also several other gaps that need to be addressed in future studies (Table 4). For instance, it is recommended that urate lowering therapy be continued indefinitely, but it is not known with certainty if this is essential. Results of a recent prospective observational study suggest that following a period of good control with intensive treatment (aiming for target serum urate <303 mmol/l), it might be feasible to withdraw treatment for a period, or at least that control may be less rigid during the long term. 85 Patients in whom urate lowering therapy was withdrawn after 55 years remained free from gout for as long as a mean period of 49 months. It is also not known what the lower safe limit of urate is. Since urate is an anti-oxidant and neuroprotective, there Could be safely combined with febuxostat; >90% of patients given the combination of febuxostat and lesinurad achieved target serum urate levels in phase Ib studies. BCX-4208 Inhibits PNP activity Early phase I and II studies have shown significant reduction in serum urate in patients who were given this drug. Apremilast Inhibits PDE4 Being compared with indomethacin in a single-blind trial for patients with acute gout flares. Tranilast Possesses uricosuric as well as anti-inflammatory properties Currently being studied as part of combination therapy with allopurinol. URAT-1, urate anion exchange transporter; PNP, purine nucleoside phosphorylase; PDE4, phosphodiesterase 4. Table 4 Some key research questions What is the cost-effectiveness of biological therapies for gout? Does febuxostat increase the risk of cardiac adverse events? How could we improve safety of uricase based therapies? What will be the place for newer therapies in the therapeutic armamentarium of gout? What is the role of combination drug therapy for patients with acute and chronic gout? Once commenced, should urate lowering therapy be continued indefinitely? Could target levels of serum urate be relaxed after the initial crystal depletion phase? What is the safe lower limit of serum urate? Should subjects with asymptomatic hyperuricaemia receive hypouricaemic therapy to reduce cardiovascular risk? What is the usefulness of dual energy CT scan in the pre-clinical phase? Would early treatment of patients with crystal induced inflammation improve cardiovascular outcome? is a concern that very low urate levels might increase risk of neurodegenerative diseases such as Parkinson s disease, Alzheimer s dementia and multiple sclerosis. 86,87 Further studies are required to clarify these issues. Combination drug therapy for management of gout needs to be explored further as well. Few small trials have demonstrated that allopurinol in combination with benzbromarone or sulphinpyrazone results in better control of serum urate and resolution of tophi compared to monotherapy, 88,89 but controlled trials and long-term data are needed. Trial data for usefulness of combining corticosteroids or NSAIDs with colchicine for patients with acute gout are also lacking. And lastly, the debate on whether or not asymptomatic hyperuricaemia constitutes an independent risk factor for cardiovascular disease continues Elevated uric acid levels are associated with metabolic syndrome and established cardiovascular risk factors, especially hypertension, and it is therefore difficult to deduce if hyperuricaemia increases the risk of cardiovascular disease independent of
9 Gout advances 415 other risk factors. Some studies that controlled for other risk factors have indeed suggested that hyperuricaemia may be an independent risk factor for not only cardiovascular but also renal disease, but they were generally small trials that examined well defined populations. Some recent reports have also indicated that treatment of hyperuricaemia lowers blood pressure and improves renal function among patients with chronic kidney disease stage III. 94,95 At present, there are insufficient data to recommend treatment of asymptomatic hyperuricaemia to reduce cardiovascular risk, but should more definite data become available in future, it would significantly change the way we manage gout. Conflict of interest: None declared. References 1. Mikuls TR, Farrar JT, Bilker WB, Fernandes S, Schumacher HR Jr, Saag KG. Gout epidemiology: results from the UK General Practice Research Database, Ann Rheum Dis 2005; 64: Annemans L, Spaepan E, Gaskin M, Bonnemaire M, Malier V, Gilbert T, et al. Gout in UK and Germany: prevalence, comorbidities and management in general practice Ann Rheum Dis 2008; 67: Choi HK, Ford ES, Li C, Curhan G. Prevalance of metabolic syndrome in patients with gout: the Third National Health and Nutrition Examination Survey. Arthritis Rheum 2007; 57: Krishnan E, Baker JF, Furst DE, Schumacher HR. Gout and the risk of acute myocardial infarction. Arthritis Rheum 2006; 54: Roddy E, Zhang W, Doherty M. Is gout associated with reduced quality of life? A case-control study. Rheumatology 2007; 46: Primatesta P, Plana E, Rothenbacher D. Gout treatment and comorbidities: a retrospective cohort study in a large US managed care population. BMC Musculoskelet Disord 2011; 12: Wu EQ, Forsythe A, Guerin A, Yu AP, Latremouille-Viau D, Tsaneva M. Comorbidity burden, healthcare resource utilization, and costs in chronic gout patients refractory to conventional urate-lowering therapy. Am J Ther 2011; [Epub ahead of print; 10 February 2011]. 8. Roddy E, Zhang W, Doherty M. The changing epidemiology of gout. Nat Clin Prac Rheumatol 2007; 3: Roddy E, Doherty M. Epidemiology of gout. Arthritis Res Ther 2010; 12: Stamp LK, Jordan S. The challenges of gout management in the elderly. Drugs Aging 2011; 28: Klinenberg JR, Goldfinger SE, Seegmiller JE. The effectiveness of the xanthine oxidase inhibitor allopurinol in the treatment of gout. Ann Intern Med 1965; 62: Mandell BF, Edwards NL, Sundy JS, Simkin PA, Pile JC. Preventing and treating acute gout attacks across the clinical spectrum: a roundtable discussion. Cleve Clin J Med 2010; 77(Suppl. 2):S Trelle S, Reichenbach S, Wandel S, Hildebrand P, Tschannen B, Villiger PM, et al. Cardiovascular safety of non steroidal anti-inflammatory drugs: network metaanalysis. BMJ 2011; 342:c Schlesinger N, Schumacher R, Catton M, Maxwell L. Colchicine for acute gout. Cochrane Database Syst Rev 2006; 4:CD Dinarello CA. How interleukin-1b induces gouty arthritis. Arthritis Rheum 2010; 62: Torres R, Macdonald L, Croil SD, Reinhardt J, Dore A, Stevens S, et al. Hyperalgesia, synovitis, and multiple biomarkers of inflammation are suppressed by IL-1 inhibition in a novel animal model of gouty arthritis. Ann Rheum Dis 2009; 68: So A, de Smedt T, Revaz S, Tschopp J. A pilot study of IL-1 inhibition by anakinra in acute gout. Arthritis Res Ther 2007; 9:R Terkeltaub R, Sundy JS, Schumacher HR, Murphy F, Bookbinder S, Biedermann S, et al. The interleukin 1 inhibitor rilonacept in treatment of chronic gouty arthritis: results of a placebo-controlled, monosequence crossover, nonrandomised, single-blind pilot study. Ann Rheum Dis 2009; 68: So A, de Meulemeester M, Pikhlak A, Yucell AE, Richard D, Murphy V, et al. Canakinumab for the treatment of acute flares in difficult-to-treat gouty arthritis: results of a multicenter, phase II, dose-ranging study. Arthritis Rheum 2010; 62: Schlesinger N, Mysler E, Lin HY, de Meulemeester M, Rovensky J, Arulmani U, et al. Canakinumab reduces the risk of acute gouty arthritis flares during initiation of allopurinol treatment: results of a double-blind, randomised study. Ann Rheum Dis 2011; 70: Lin YH, Hsu HL, Huang YC, Lee M, Huang WY, Huang YC, et al. Gouty arthritis in acute cerebrovascular disease. Cerebrovasc Dis 2009; 28: Morris I, Varughese G, Mattingly P. Colchicine in acute gout. BMJ 2003; 327: Zhang W, Doherty M, Bardin T, Pascual E, Barskova V, Conaghan P, et al. EULAR evidence based recommendations for gout. Part II: management. Report of a task force of the EULAR Standing Committee for International Clinical Studies Including Therapeutics (ESCISIT). Ann Rheum Dis. 2006; 65: Ahern MJ, Reid C, Gordon TP, McCredie M, Brooks PM, Jones M. Does colchicine work? The results of the first controlled study in acute gout. Aust N Z J Med 1987; 17: Terkeltaub RA, Furst DE, Bennett K, Kook KA, Crockett RS, Davis MW. High versus low dosing of oral colchicine for early acute gout flare: twenty-four-outcome of the first multicenter, randomised, double-blind, placebo-controlled, parallel group, dose comparison colchicine study. Arthritis Rheum 2010; 62: Sarkozy J. Management of gout. N Engl J Med 1996; 334: Janssens HJ, Janssen M, van de Lisdonk EH, van Riel PL, van Weel C. Use of oral prednisolone or naproxen for the
10 416 E. Suresh and P. Das treatment of gout arthritis: a double-blind, randomised equivalence trial. Lancet 2008; 371: Man CY, Cheung IT, Cameron PA, Rainer TH. Comparison of oral prednisolone/paracetamol and oral indomethacin/paracetamol combination therapy in the treatment of acute gout like arthritis: a double-blind, randomized, controlled trial. Ann Emerg Med 2007; 49: Groff GD, Franck WA, Raddatz DA. Systemic steroid therapy for acute gout: a clinical trial and review of the literature. Semin Arthritis Rheum 1990; 19: Clive DM. Renal transplant-associated hyperuricemia and gout. J Am Soc Nephrol 2000; 11: Schlesinger N, Detry MA, Holland BK, Baker DG, Beutler AM, Rull M, et al. Local ice therapy during bouts of acute gouty arthritis. J Rheumatol 2002; 29: Schlesinger N. Response to application of ice may help differentiate between gouty arthritis and other inflammatory arthritides. J Clin Rheumatol 2006; 12: Suresh E. Diagnosis and management of gout: a rational approach. Postgrad Med J 2005; 81: Perez-Ruiz F. Treating to target: a strategy to cure gout. Rheumatology 2009; 48(Suppl. 2):ii9 ii Jordan KM, Cameron JS, Snaith M, Zhang M, Doherty M, Seckl J, et al. British Society of Rheumatology and British Health Professionals in Rheumatology guideline for the management of gout. Rheumatology 2007; 46: McInnes GT, Lawson DH, Jick H. Acute adverse reactions attributed to allopurinol in hospitalised patients. Ann Rheum Dis 1981; 40: Hande KR, Noone RM, Stone WJ. Severe allopurinol toxicity: description and guidelines for prevention in patients with renal insufficiency. Am J Med 1984; 76: Stamp LK, O Donnell JL, Zhang M, James J, Frampton C, Barclay ML, et al. Using allopurinol above the dose based on creatinine clearance is effective and safe in patients with chronic gout, including those with renal impairment. Arthritis Rheum 2011; 63: Robbins N, Koch SE, Tranter M, Rubinstein J. The history and future of probenecid. Cardiovasc Toxicol 2011; [Epub ahead of print; 22 September 2011]. 40. Arai M, Yokosuka O, Fujiwara K, Kojima H, Kanda T, Hirasawa H, et al. Fulminant hepatic failure associated with benzbromarone treatment: a case report. J Gastroenterol Hepatol 2002; 17: Burns CM, Wortmann RL. Gout therapeutics: new drugs for an old disease. Lancet 2011; 377: Terkeltaub R. Update on gout: new therapeutic strategies and options. Nat Rev Rheumatol 2010; 6: Edwards NL. Febuxostat: a new treatment for hyperuricemia in gout. Rheumatology 2009; 48(Suppl 2):ii15 ii Khosravan R, Grabowski BA, Mayer MD, Wu JT, Joseph- Ridge N, Vernillet L. The effect of mild and moderate hepatic impairment on pharmacokinetics, pharmacodynamics, and safety of febuxostat, a novel nonpurine selective inhibitor of xanthine oxidase. J Clin Pharmacol 2006; 46: Becker MA, Schumacher HR, Jr, Wortmann RL, Macdonald PA, Eustace D, Palo WA, et al. Febuxostat compared with allopurinol in patients with hyperuricemia and gout. N Engl J Med 2005; 353: Schumacher HR, Jr, Becker MA, Wortmann RL, Macdonald PA, Hunt B, Streit J, et al. Effects of febuxostat versus allopurinol and placebo in reducing serum urate in subjects with hyperuricemia and gout: a 28-week, phase III, randomized, double-blind, parallel-group trial. Arthritis Rheum 2008; 59: Schumacher HR Jr, Becker MA, Lloyd E, MacDonald PA, Lademacher C. Febuxostat in the treatment of gout: 5-yr findings of the FOCUS efficacy and safety study. Rheumatology. 2009; 48: Becker MA, Schumacher HR, Espinoza LR, Wells AF, Macdonald P, Lloyd E, et al. The urate-lowering efficacy and safety of febuxostat in the treatment of the hyperuricemia of gout: the CONFIRMS trial. Arthritis Res Ther 2010; 12:R Gray CL, Walters-Smith NE. Febuxostat for treatment of chronic gout. Am J Health Syst Pharm 2011; 68: Singh JA. Advances in gout: some answers, more questions. Arthritis Res Ther 2010; 12: Sundy JS, Hershfield MS. Uricase and other novel agents for the management of patients with treatment-failure gout. Curr Rheumatol Rep 2007; 9: Terkeltaub R. Learning how and when to employ uricase as bridge therapy in refractory gout. J Rheumatol 2007; 34: Sherman MR, Saifer MG, Perez-Ruiz F. PEG-uricase in the management of treatment-resistant gout and hyperuricemia. Adv Drug Deliv Rev 2008; 60: Reinders MK, Jansen TL. New advances in the treatment of gout: review of pegloticase. Ther Clin Risk Manag 2010; 6: Sundy JS, Baraf HS, Yood RA, Edwards NL, Gutierrez- Urena SR, Treadwell EL, et al. Efficacy and tolerability of pegloticase for the treatment of chronic gout in patients refractory to conventional treatment: two randomized controlled trials. JAMA 2011; 306: Stein HB, Hasan A, Fox IH. Ascorbic acid-induced uricosuria. A consequency of megavitamin therapy. Ann Intern Med 1976; 84: Choi HK, Gao X, Curhan G. Vitamin C intake and the risk of gout in men: a prospective study. Arch Intern Med 2009; 169: Gao X, Curhan G, Forman JP, Ascherio A, Choi HK. Vitamin C intake and serum uric acid concentration in men. J Rheumatol 2008; 35: Lee SJ, Terkeltaub RA, Kavanaugh A. Recent developments in diet and gout. Curr Opin Rheumatol 2006; 18: Schlesinger N. Dietary factors and hyperuricaemia. Curr Pharm Des 2005; 11: Singh JA, Reddy SG, Kundukulam J. Risk factors for gout and prevention: a systematic review of the literature. Curr Opin Rheumatol 2011; 23: Yu KH, See LC, Huang YC, Yang CH, Sun JH. Dietary factors associated with hyperuricemia in adults. Semin Arthritis Rheum 2008; 37: Choi HK, Atkinson K, Karlson EW, Willett W, Curhan G. Purine-rich foods, dairy and protein intake, and the risk of gout in men. N Engl J Med 2004; 350:
11 Gout advances Choi HK, Atkinson K, Karlson EW, Willett W, Curhan G. Alcohol intake and risk of incident gout in men: a prospective study. Lancet 2004; 363: Ghadirian P, Shatenstein B, Verdy M, Hamet P. The influence of dairy products on plasma uric acid in women. Eur J Epidemiol 1995; 11: Choi HK, Curhan G. Soft drinks, fructose consumption, and the risk of gout in men: prospective cohort study. BMJ 2008; 336: Choi JW, Ford ES, Gao X, Choi HK. Sugar-sweetened soft drinks, diet soft drinks, and serum uric acid level: the Third National Health and Nutrition Examination Survey. Arthritis Rheum 2008; 59: Choi HK, Curhan G. Coffee, tea and caffeine consumption and serum uric acid level: the third national health and nutrition examination survey. Arthritis Rheum 2007; 57: Dessein PH, Shipton EA, Stanwix AE, Joffe BI, Ramokgadi J. Beneficial effects of weight loss associated with moderate calorie/carbohydrate restriction, and increased proportional intake of protein and unsaturated fat on serum urate and lipoprotein levels in gout: a pilot study. Ann Rheum Dis 2000; 59: Enomoto A, Kimura H, Chairoungdua A, Shigeta Y, Jutabha P, Cha SH, et al. Molecular identification of a renal urate anion exchanger that regulates blood urate levels. Nature 2002; 417: Ho MC, Shi W, Rinaldo-Matthis A, Tyler PC, Evans GB, Clinch K, et al. Four generations of transition-state analogues for human purine nucleoside phosphorylase. Proc Natl Acad Sci USA 2010; 107: Higgs G. Is PDE4 too difficult a drug target? Curr Opin Investig Drugs 2010; 11: Perez-Ruiz F, Dalbeth N, Urresola A, Miguel E, Schlesinger N. Gout. Imaging of gout: findings and utility. Arthritis Res Ther 2009; 11: Wright SA, Filippucci E, McVeigh C, Grey A, McCarron M, Grassi W, et al. High-resolution ultrasonography of the first metatarsal phalangeal joint in gout: a controlled study. Ann Rheum Dis 2007; 66: Schueller-Weidekamm C, Schueller G, Aringer M, Weber M, Kainberger F. Impact of sonography in gouty arthritis: comparison with conventional radiography, clinical examination, and laboratory findings. Eur J Radiol 2007; 62: Choi HK, Al-Arfaj AM, Eftekhari A, Munk PL, Shojania K, Reid G, et al. Dual energy computed tomography in tophaceous gout. Ann Rheum Dis 2009; 68: Singh JA. Quality of life and quality of care for patients with gout. Curr Rheumatol Rep 2009; 11: Mikuls TR. Quality of care in gout: from measurement to improvement. Clin Exp Rheumatol 2007; 25(6 Suppl. 47): Reach G. Treatment adherence in patients with gout. Joint Bone Spine 2011; [Epub ahead of print; 1 July 2011]. 80. Sundy JS. Gout management: let s get it right this time. Arthritis Rheum 2008; 59: Harold LR, Andrade SE, Briesacher BA, Raebel MA, Fouayzi H, Yood RA, et al. Adherence with urate-lowering therapies for the treatment of gout. Arthritis Res Ther 2009; 11:R Briesacher BA, Andrade SE, Fouayzi H, Chan KA. Comparison of drug adherence rates among patients with seven different medical conditions. Pharmacotherapy 2008; 28: Neogi T, Hunter DJ, Chaisson CE, Allensworth-Davies D, Zhang Y. Frequency and predictors of inappropriate management of recurrent gout attacks in a longitudinal study. J Rheumatol 2006; 33: Zhang LY, Schumacher HR, Su HH, Lie D, Dinnella J, Baker JF, et al. Development and evaluation of a survey of gout patients concerning their knowledge about gout. J Clin Rheumatol 2011; 17: Perez-Ruiz F, Atxotegi J, Hernando I, Calabozo M, Nolla JM. Using serum urate levels to determine the period free of gouty symptoms after withdrawal of long-term urate-lowering therapy: a prospective study. Arthritis Rheum 2006; 55: Bowman GL, Shannon J, Frei B, Kaye JA, Quinn JF. Uric acid as a CNS antioxidant. J Alzheimers Dis 2010; 19: Ascherio A, LeWitt PA, Xu K, Eberly S, Watts A, Matson WR, et al. Urate predicts rate of clinical decline in Parkinson disease. Arch Neurol 2009; 66: Kuzell WC, Seebach LM, Glover RP, Jackman AE. Treatment of gout with allopurinol and sulphinpyrazone in combination and with allopurinol alone. Ann Rheum Dis 1966; 25(6 Suppl.): Akkasilpa S, Osiri M, Deesomchok U, Avihingsanon Y. The efficacy of combined low dose of allopurinol and benzbromarone compared to standard dose of allopurinol in hyperuricemia. J Med Assoc Thai 2004; 87: Krishnan E, Kwoh CK, Schumacher HR, Kuller L. Hyperuricemia and incidence of hypertension among men without metabolic syndrome. Hypertension 2007; 49: Avram Z, Krishnan E. Hyperuricemia-where nephrology meets rheumatology. Rheumatology 2008; 47: Feig DI, Kang DH, Johnson RJ. Uric acid and cardiovascular risk. N Engl J Med 2008; 359: Fang J, Alderman MH. Serum uric acid and cardiovascular mortality: the NHANES I epidemiologic follow-up study, National Health and Nutrition Examination Survey. JAMA 2000; 283: Siu YP, Leung KT, Tong MK, Kwan TH. Use of allopurinol in slowing the progression of renal disease through its ability to lower serum uric acid level. Am J Kidney Dis 2006; 47: Kanbay M, Ozkara A, Selcoki Y, Isik B, Turgut F, Bavbek N, et al. Effect of treatment of hyperuricemia with allopurinol on blood pressure, creatinine clearance and proteinuria in patients with normal renal functions. Int Urol Nephrol 2007; 39:
Uloric Step Therapy Program
 Uloric Step Therapy Program Policy Number: 5.01.584 Last Review: 7/2017 Origination: 7/2014 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for brand
Uloric Step Therapy Program Policy Number: 5.01.584 Last Review: 7/2017 Origination: 7/2014 Next Review: 7/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for brand
COMPARATIVE EVALUATION OF EFFICACY AND SAFETY PROFILE OF FEBUXOSTAT WITH ALLOPURINOL IN PATIENTS WITH HYPERURICEMIA AND GOUT
 Int. J. Pharm. Med. & Bio. Sc. 2013 P K Agarwal and Bijay Kumar, 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 4, October 2013 2013 IJPMBS. All Rights Reserved COMPARATIVE EVALUATION OF
Int. J. Pharm. Med. & Bio. Sc. 2013 P K Agarwal and Bijay Kumar, 2013 Research Paper ISSN 2278 5221 www.ijpmbs.com Vol. 2, No. 4, October 2013 2013 IJPMBS. All Rights Reserved COMPARATIVE EVALUATION OF
Gout -revisited. Shrenik Shah
 Gout -revisited Shrenik Shah definition Monosodium urate (MSU) crystal deposition episodic and later persistent joint inflammation and tophi All MSU crystal deposition- broader definition EULAR- European
Gout -revisited Shrenik Shah definition Monosodium urate (MSU) crystal deposition episodic and later persistent joint inflammation and tophi All MSU crystal deposition- broader definition EULAR- European
Gout Hanan Abdel Rehim
 Review article 35 Gout Hanan Abdel Rehim Department of Internal Medicine, Kasr-Al Aini School of Medicine, Cairo University, Cairo, Egypt Correspondence to Hanan Abdel Rehim, MD, 11 Ismaiel Wahby Street,
Review article 35 Gout Hanan Abdel Rehim Department of Internal Medicine, Kasr-Al Aini School of Medicine, Cairo University, Cairo, Egypt Correspondence to Hanan Abdel Rehim, MD, 11 Ismaiel Wahby Street,
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 24 June 2009
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 24 June 2009 ADENURIC 80 mg, film-coated tablets B/28 (CIP code: 385 724-4) B/84 (CIP code: 572 820-3) ADENURIC 120
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 24 June 2009 ADENURIC 80 mg, film-coated tablets B/28 (CIP code: 385 724-4) B/84 (CIP code: 572 820-3) ADENURIC 120
1. To review the diagnosis of gout and its differential. 2. To understand the four stages of gout
 Objectives 1. To review the diagnosis of gout and its differential GOUT 2. To understand the four stages of gout 3. To develop an approach for the acute treatment of gout Anthony Lim 9/13/12 Cycle 3 4.
Objectives 1. To review the diagnosis of gout and its differential GOUT 2. To understand the four stages of gout 3. To develop an approach for the acute treatment of gout Anthony Lim 9/13/12 Cycle 3 4.
Gout 2.0. Scott Vogelgesang, M.D. Division of Immunology: Rheumatology & Allergy
 Gout 2.0 Scott Vogelgesang, M.D. Division of Immunology: Rheumatology & Allergy Case 48 year old man presents with swollen, painful left toe that started overnight. Didn t hurt when he went to bed. No
Gout 2.0 Scott Vogelgesang, M.D. Division of Immunology: Rheumatology & Allergy Case 48 year old man presents with swollen, painful left toe that started overnight. Didn t hurt when he went to bed. No
Febuxostat: a new treatment for hyperuricaemia in gout
 Rheumatology 2009;48:ii15 ii19 doi:10.1093/rheumatology/kep088 Febuxostat: a new treatment for hyperuricaemia in gout N. Lawrence Edwards 1 Febuxostat is a new non-purine xanthine oxidase inhibitor that
Rheumatology 2009;48:ii15 ii19 doi:10.1093/rheumatology/kep088 Febuxostat: a new treatment for hyperuricaemia in gout N. Lawrence Edwards 1 Febuxostat is a new non-purine xanthine oxidase inhibitor that
Current treatment options for acute and chronic gout
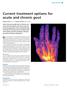 DRUG REVIEW n Current treatment options for acute and chronic gout Kelsey Jordan FRCP and Andrew Jeffries PGDip, MRCP Gout is the only curable form of arthritis, yet only a third of patients with chronic
DRUG REVIEW n Current treatment options for acute and chronic gout Kelsey Jordan FRCP and Andrew Jeffries PGDip, MRCP Gout is the only curable form of arthritis, yet only a third of patients with chronic
An update on the management of gout
 An update on the management of gout 8 The management of gout involves treatment of an acute attack, lifestyle modification and urate lowering treatment to achieve a target serum urate level. Recent evidence
An update on the management of gout 8 The management of gout involves treatment of an acute attack, lifestyle modification and urate lowering treatment to achieve a target serum urate level. Recent evidence
Gout A rapid review. Jeremy Jones
 Gout A rapid review Jeremy Jones The Hyperuricemia Cascade Dietary purines Tissue nucleic acids Urate Endogenous purine synthesis Overproduction Hyperuricemia Underexcretion Silent tissue deposition Gout
Gout A rapid review Jeremy Jones The Hyperuricemia Cascade Dietary purines Tissue nucleic acids Urate Endogenous purine synthesis Overproduction Hyperuricemia Underexcretion Silent tissue deposition Gout
Update on Gout for GPs
 Update on Gout for GPs Dr Patrick Kiely PhD FRCP Consultant Physician and Rheumatologist St George s, London 2/3 1/3 Gut bacteria have uricase Chronic erosive arthropathy Clinical spectrum Making the diagnosis
Update on Gout for GPs Dr Patrick Kiely PhD FRCP Consultant Physician and Rheumatologist St George s, London 2/3 1/3 Gut bacteria have uricase Chronic erosive arthropathy Clinical spectrum Making the diagnosis
Drugs Used to Treat Gout. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Drugs Used to Treat Gout Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Gout is a metabolic disease characterized by recurrent episodes of acute arthritis
Drugs Used to Treat Gout Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Gout is a metabolic disease characterized by recurrent episodes of acute arthritis
ARD Online First, published on November 2, 2007 as /ard
 ARD Online First, published on November 2, 2007 as 10.1136/ard.2007.076232 Gout in the UK and Germany: prevalence, comorbidities and management in general practice 2000 2005 L Annemans, E Spaepen, M Gaskin,
ARD Online First, published on November 2, 2007 as 10.1136/ard.2007.076232 Gout in the UK and Germany: prevalence, comorbidities and management in general practice 2000 2005 L Annemans, E Spaepen, M Gaskin,
GOUT. Dr Krishnan Baburaj West herts NHS Trust
 GOUT Dr Krishnan Baburaj West herts NHS Trust podagra Gout A disease of kings, the king of diseases History Louis XIV Emperor Augustus Henry VIII Introduction Gout an inflammatory arthritic condition that
GOUT Dr Krishnan Baburaj West herts NHS Trust podagra Gout A disease of kings, the king of diseases History Louis XIV Emperor Augustus Henry VIII Introduction Gout an inflammatory arthritic condition that
Gout in the UK and Germany: prevalence, comorbidities and management in general practice
 1 IMS Health, Brussels, Belgium; 2 Department of Public Health, Ghent University, Ghent, Belgium; 3 School of Pharmacy, Brussels University, Brussels, Belgium; 4 IMS Health, London, UK; 5 Ipsen, Paris,
1 IMS Health, Brussels, Belgium; 2 Department of Public Health, Ghent University, Ghent, Belgium; 3 School of Pharmacy, Brussels University, Brussels, Belgium; 4 IMS Health, London, UK; 5 Ipsen, Paris,
Rheumatoid arthritis, seronegative spondylarthritides and gout. György Nagy
 Rheumatoid arthritis, seronegative spondylarthritides and gout György Nagy Dec 4, 2017 Rheumatoid arthritis Rheumatoid arthritis Chronic, progressive, autoimmune disorder of the joints with extra-articular
Rheumatoid arthritis, seronegative spondylarthritides and gout György Nagy Dec 4, 2017 Rheumatoid arthritis Rheumatoid arthritis Chronic, progressive, autoimmune disorder of the joints with extra-articular
Gout Treatment Guidelines
 Gout Treatment Guidelines Gout is a disorder that manifests as a spectrum of clinical and pathologic features built on a foundation of an excess body burden of uric acid, manifested in part by hyperuricemia,
Gout Treatment Guidelines Gout is a disorder that manifests as a spectrum of clinical and pathologic features built on a foundation of an excess body burden of uric acid, manifested in part by hyperuricemia,
Diagnosis and Management of Gout in 2011
 October 18, 2011 Early and accurate gout diagnosis and disease management are essential. Making the clinical diagnosis takes into consideration the differential diagnosis supported by the use of clinical,
October 18, 2011 Early and accurate gout diagnosis and disease management are essential. Making the clinical diagnosis takes into consideration the differential diagnosis supported by the use of clinical,
The Clinic a l Problem
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e Gout Tuhina Neogi, M.D., Ph.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various
T h e n e w e ngl a nd j o u r na l o f m e dic i n e Gout Tuhina Neogi, M.D., Ph.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various
Febuxostat now subsidised on Special Authority
 Gout update: Febuxostat now subsidised on Special Authority 38 Febuxostat was added to the New Zealand Pharmaceutical Schedule on 1 June, 2014. It is now available as a third-line preventive treatment
Gout update: Febuxostat now subsidised on Special Authority 38 Febuxostat was added to the New Zealand Pharmaceutical Schedule on 1 June, 2014. It is now available as a third-line preventive treatment
Study of Febuxostat for the Management of Hyperuricemia in Gout
 Human Journals Review Article October 2015 Vol.:4, Issue:3 All rights are reserved by Sachin S. Shinde et al. Study of Febuxostat for the Management of Hyperuricemia in Gout Keywords: Febuxostat, Hyperuricemia,
Human Journals Review Article October 2015 Vol.:4, Issue:3 All rights are reserved by Sachin S. Shinde et al. Study of Febuxostat for the Management of Hyperuricemia in Gout Keywords: Febuxostat, Hyperuricemia,
pegloticase (Krystexxa )
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Case presentation. serum uric acid = 11.5 mg/dl 24-hour uric acid excretion = 300 mg
 GOUT 55 y/o male 12 hours pain in my big toe & ankle went to bed last night feeling fine felt as if had broken toe this morning similar problems in right ankle & left wrist Case presentation lab studies
GOUT 55 y/o male 12 hours pain in my big toe & ankle went to bed last night feeling fine felt as if had broken toe this morning similar problems in right ankle & left wrist Case presentation lab studies
MEDICAL POLICY PEGLOTICASE (KRYSTEXXA ) POLICY NUMBER MP POLICY TITLE. Original Issue Date (Created): January 1, 2011
 Original Issue Date (Created): January 1, 2011 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY PREAUTHORIZATION REQUIRED Note: Requests for pegloticase
Original Issue Date (Created): January 1, 2011 Most Recent Review Date (Revised): September 24, 2013 Effective Date: November 1, 2013 I. POLICY PREAUTHORIZATION REQUIRED Note: Requests for pegloticase
Gout- Treatment Updates. Harinder Singh, MD Rheumatology Mercy Internal Medicine Clinic Mason City, IA
 Gout- Treatment Updates Harinder Singh, MD Rheumatology Mercy Internal Medicine Clinic Mason City, IA Gout Outline of purine metabolism: (1) amidophosphoribosyltransferase (2) hypoxanthine-guanine phosphoribosyltransferase
Gout- Treatment Updates Harinder Singh, MD Rheumatology Mercy Internal Medicine Clinic Mason City, IA Gout Outline of purine metabolism: (1) amidophosphoribosyltransferase (2) hypoxanthine-guanine phosphoribosyltransferase
Gout. Clinical features Most commonly affects middle-aged males. It is an acute and usually relapsing selflimiting
 Gout Gout is a syndrome caused by an inflammatory response to the formation of monosodium urate monohydrate crystals which develop secondary to hyperuricemia. Acute and chronic forms are recognized. Hyperuricemia
Gout Gout is a syndrome caused by an inflammatory response to the formation of monosodium urate monohydrate crystals which develop secondary to hyperuricemia. Acute and chronic forms are recognized. Hyperuricemia
Gout: Update in therapeutics
 Summary Gout: Update in therapeutics 29/11/14 Caroline van Durme CHU de Liège Maastricht University Medical Centre+ Why treating gout? Guidelines: ACR 12 Drugs: Colchicine Allopurinol: what about the kidney?
Summary Gout: Update in therapeutics 29/11/14 Caroline van Durme CHU de Liège Maastricht University Medical Centre+ Why treating gout? Guidelines: ACR 12 Drugs: Colchicine Allopurinol: what about the kidney?
OBJECTIVES GOUT GOUTY INFLAMMATION 6/10/2016 GOUT INCIDENCE AND PREVALENCE MONOSODIUM URATE CRYSTAL DEPOSITION DISEASE
 GOUT Lisa Talbert, MD Family Medicine Update June 15, 2016 OBJECTIVES To be familiar with the clinical presentation and pathophysiology of gouty arthritis Be able to incorporate current guidelines when
GOUT Lisa Talbert, MD Family Medicine Update June 15, 2016 OBJECTIVES To be familiar with the clinical presentation and pathophysiology of gouty arthritis Be able to incorporate current guidelines when
Febuxostat: a safe and effective therapy for hyperuricemia and gout
 DRUG EVALUATIO Febuxostat: a safe and effective therapy for hyperuricemia and gout atasha Jordan & Geraldine M McCarthy Author for correspondence Mater Misericordiae University Hospital, Eccles St. Dublin
DRUG EVALUATIO Febuxostat: a safe and effective therapy for hyperuricemia and gout atasha Jordan & Geraldine M McCarthy Author for correspondence Mater Misericordiae University Hospital, Eccles St. Dublin
Literature Scan: Analgesics for Gout. Month/Year of Review: April 2015 Date of Last Review: January 2014
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301 1079 Phone 503 947 5220 Fax 503 947 1119 Copyright 2012 Oregon State University. All Rights
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301 1079 Phone 503 947 5220 Fax 503 947 1119 Copyright 2012 Oregon State University. All Rights
Urate Lowering Efficacy of Febuxostat Versus Allopurinol in Hyperuricemic Patients with Gout
 Philippine Journal of Internal Medicine Meta-Analysis Urate Lowering Efficacy of Febuxostat Versus Allopurinol in Hyperuricemic Patients with Gout Erika Bianca S. Villazor-Isidro, M.D.*; John Carlo G.
Philippine Journal of Internal Medicine Meta-Analysis Urate Lowering Efficacy of Febuxostat Versus Allopurinol in Hyperuricemic Patients with Gout Erika Bianca S. Villazor-Isidro, M.D.*; John Carlo G.
Journal of Advanced Scientific Research
 Bijoy Kumar Panda et al, J Adv Scient Res, 2012, 3(2): 03-11 3 Journal of Advanced Scientific Research Available online through http://www.sciensage.info/jasr ISSN 0976-9595 Review Article Febuxostat,
Bijoy Kumar Panda et al, J Adv Scient Res, 2012, 3(2): 03-11 3 Journal of Advanced Scientific Research Available online through http://www.sciensage.info/jasr ISSN 0976-9595 Review Article Febuxostat,
Rheumatology Cases for the Internist
 Rheumatology Cases for the Internist Marc C. Hochberg, MD, MPH Professor of Medicine Head, Division of Rheumatology and Clinical Immunology Vice Chair, Department of Medicine University of Maryland School
Rheumatology Cases for the Internist Marc C. Hochberg, MD, MPH Professor of Medicine Head, Division of Rheumatology and Clinical Immunology Vice Chair, Department of Medicine University of Maryland School
Cost-effectiveness of lesinurad (Zurampic ) for the treatment of adult patients with gout
 Cost-effectiveness of lesinurad (Zurampic ) for the treatment of adult patients with gout The NCPE has issued a recommendation regarding the cost-effectiveness of Lesinurad (Zurampic ) in combination with
Cost-effectiveness of lesinurad (Zurampic ) for the treatment of adult patients with gout The NCPE has issued a recommendation regarding the cost-effectiveness of Lesinurad (Zurampic ) in combination with
University of Groningen
 University of Groningen Biochemical effectiveness of allopurinol and allopurinol-probenecid in previously benzbromarone-treated gout patients Reinders, M.K.; van Roon, Eric; Houtman, Pieternella; Brouwers,
University of Groningen Biochemical effectiveness of allopurinol and allopurinol-probenecid in previously benzbromarone-treated gout patients Reinders, M.K.; van Roon, Eric; Houtman, Pieternella; Brouwers,
A Patient s Guide to Gout. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Gout Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
A Patient s Guide to Gout Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written and professionally
The 2010 Competency Standards addressed by this activity include (but may not be limited to): 4.2.2, 4.2.3, 6.1.2, 6.2.1, 7.1.2, 7.1.3,
 UPDATE ON GOUT Learning objectives: After completing this activity, pharmacists should be able to: 1. describe the mechanisms underlying hyperuricaemia 2. state the risk factors for development of gout
UPDATE ON GOUT Learning objectives: After completing this activity, pharmacists should be able to: 1. describe the mechanisms underlying hyperuricaemia 2. state the risk factors for development of gout
Podcast (Video Recorded Lecture Series): Gout for the USMLE Step One Exam. Howard J. Sachs, MD
 Podcast (Video Recorded Lecture Series): Gout for the USMLE Step One Exam Howard J. Sachs, MD www.12daysinmarch.com Email: Howard@12daysinmarch.com Podcast (Video Recorded Lecture Series): Gout for the
Podcast (Video Recorded Lecture Series): Gout for the USMLE Step One Exam Howard J. Sachs, MD www.12daysinmarch.com Email: Howard@12daysinmarch.com Podcast (Video Recorded Lecture Series): Gout for the
COPYRIGHT. Update in Internal Medicine December 4, 2016
 Update in Internal Medicine December 4, 2016 Fadi Badlissi, MD, MSc Director of the Musculoskeletal Medicine Unit The Orthopedic Department & Rheumatology Division Beth Israel Deaconess Medical Center
Update in Internal Medicine December 4, 2016 Fadi Badlissi, MD, MSc Director of the Musculoskeletal Medicine Unit The Orthopedic Department & Rheumatology Division Beth Israel Deaconess Medical Center
Practice research in the field of gout - clinical pharmacology of antihyperuricemic drugs Reinders, Mattheus Karsien
 University of Groningen Practice research in the field of gout - clinical pharmacology of antihyperuricemic drugs Reinders, Mattheus Karsien IMPORTANT NOTE: You are advised to consult the publisher's version
University of Groningen Practice research in the field of gout - clinical pharmacology of antihyperuricemic drugs Reinders, Mattheus Karsien IMPORTANT NOTE: You are advised to consult the publisher's version
Gout. Edward Roddy, 1 Christian D Mallen, 1 Michael Doherty 2 CLINICAL REVIEW
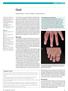 Gout Edward Roddy, 1 Christian D Mallen, 1 Michael Doherty 2 1 Arthritis Research UK Primary Care Centre, Primary Care Sciences, Keele University, Keele ST5 5BG, UK 2 Academic Rheumatology, University
Gout Edward Roddy, 1 Christian D Mallen, 1 Michael Doherty 2 1 Arthritis Research UK Primary Care Centre, Primary Care Sciences, Keele University, Keele ST5 5BG, UK 2 Academic Rheumatology, University
Initiation of Allopurinol at First Medical Contact for Acute Attacks of Gout: A Randomized Clinical Trial
 BRIEF OBSERVATION Initiation of Allopurinol at First Medical Contact for Acute Attacks of Gout: A Randomized Clinical Trial Thomas H. Taylor, MD, a,b,c John N. Mecchella, DO, b,c Robin J. Larson, MD, a,b
BRIEF OBSERVATION Initiation of Allopurinol at First Medical Contact for Acute Attacks of Gout: A Randomized Clinical Trial Thomas H. Taylor, MD, a,b,c John N. Mecchella, DO, b,c Robin J. Larson, MD, a,b
Achieving Gout Goals in Your Practice An Interview with Paul P. Doghramji, MD, FAAFP
 Achieving Gout Goals in Your Practice An Interview with Paul P. Doghramji, MD, FAAFP Dr. Paul Doghramji is attending physician at the Pottstown Memorial Medical Center and medical director of Health Services
Achieving Gout Goals in Your Practice An Interview with Paul P. Doghramji, MD, FAAFP Dr. Paul Doghramji is attending physician at the Pottstown Memorial Medical Center and medical director of Health Services
Purine-rich foods intake and recurrent gout attacks
 Clinical and epidemiological research 1 Clinical Epidemiology Research and Training Unit, Department of Medicine, Boston University School of Medicine, Boston, Massachusetts, USA 2 Data Coordinating Center,
Clinical and epidemiological research 1 Clinical Epidemiology Research and Training Unit, Department of Medicine, Boston University School of Medicine, Boston, Massachusetts, USA 2 Data Coordinating Center,
D espite reasonable understanding of its pathogenesis
 1312 EXTENDED REPORT EULAR evidence based recommendations for gout. Part II: Management. Report of a task force of the EULAR Standing Committee For International Clinical Studies Including Therapeutics
1312 EXTENDED REPORT EULAR evidence based recommendations for gout. Part II: Management. Report of a task force of the EULAR Standing Committee For International Clinical Studies Including Therapeutics
Case Report Refractory Gout Attack
 Case Reports in Medicine Volume 2012, Article ID 657694, 4 pages doi:10.1155/2012/657694 Case Report Refractory Gout Attack Simone Fargetti, Claudia Goldenstein-Schainberg, Andressa Silva Abreu, and Ricardo
Case Reports in Medicine Volume 2012, Article ID 657694, 4 pages doi:10.1155/2012/657694 Case Report Refractory Gout Attack Simone Fargetti, Claudia Goldenstein-Schainberg, Andressa Silva Abreu, and Ricardo
Retreatment with Pegloticase after a Gap in Therapy in Patients with Gout: A Report of Four Cases
 Rheumatol Ther (2018) 5:583 594 https://doi.org/10.1007/s40744-018-0111-9 CASE SERIES Retreatment with Pegloticase after a Gap in Therapy in Patients with Gout: A Report of Four Cases Allan H. Morton.
Rheumatol Ther (2018) 5:583 594 https://doi.org/10.1007/s40744-018-0111-9 CASE SERIES Retreatment with Pegloticase after a Gap in Therapy in Patients with Gout: A Report of Four Cases Allan H. Morton.
Clinical Policy Bulletin: Gout
 Gout Page 1 of 13 Clinical Policy Bulletin: Gout Number: 0810 Policy Aetna considers the following tests medically necessary for the diagnosis of gout: Measurement of blood uric acid levels Measurement
Gout Page 1 of 13 Clinical Policy Bulletin: Gout Number: 0810 Policy Aetna considers the following tests medically necessary for the diagnosis of gout: Measurement of blood uric acid levels Measurement
Coverage Criteria: Express Scripts, Inc. monograph dated 12/15/ months or as otherwise noted by indication
 BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
BENEFIT DESCRIPTION AND LIMITATIONS OF COVERAGE ITEM: PRODUCT LINES: COVERED UNDER: DESCRIPTION: CPT/HCPCS Code: Company Supplying: Setting: Kineret (anakinra subcutaneous injection) Commercial HMO/PPO/CDHP
Long-term Treatment of Gout: New Opportunities for Improved Outcomes
 Long-term Treatment of Gout: New Opportunities for Improved Outcomes Paul P. Doghramji, MD, FAAFP CONTINUING MEDICAL EDUCATION LEARNING OBJECTIVES Make a presumptive diagnosis of gout based on history
Long-term Treatment of Gout: New Opportunities for Improved Outcomes Paul P. Doghramji, MD, FAAFP CONTINUING MEDICAL EDUCATION LEARNING OBJECTIVES Make a presumptive diagnosis of gout based on history
Gout: Update on Current Therapeutics Sneha Pai, MD Ashraf Raslan, MD Naomi Schlesinger, MD *
 Curr Treat Options in Rheum (2015) 1:131 142 DOI 10.1007/s40674-015-0013-8 Gout (A Gibofsky, Section Editor) Gout: Update on Current Therapeutics Sneha Pai, MD Ashraf Raslan, MD Naomi Schlesinger, MD *
Curr Treat Options in Rheum (2015) 1:131 142 DOI 10.1007/s40674-015-0013-8 Gout (A Gibofsky, Section Editor) Gout: Update on Current Therapeutics Sneha Pai, MD Ashraf Raslan, MD Naomi Schlesinger, MD *
Acute hot swollen joint. Dr Edward Roddy Senior Lecturer in Rheumatology and Consultant Rheumatologist
 Acute hot swollen joint Dr Edward Roddy Senior Lecturer in Rheumatology and Consultant Rheumatologist Acute monoarthritis: differential diagnosis Septic arthritis Crystal arthritis (gout, pseudogout) Haemarthrosis
Acute hot swollen joint Dr Edward Roddy Senior Lecturer in Rheumatology and Consultant Rheumatologist Acute monoarthritis: differential diagnosis Septic arthritis Crystal arthritis (gout, pseudogout) Haemarthrosis
The CARI Guidelines Caring for Australasians with Renal Impairment. Uric acid GUIDELINES. No recommendations possible based on Level I or II evidence.
 Date written: July 2004 Final submission: July 2004 Author: David Johnson Uric acid GUIDELINES No recommendations possible based on Level I or II evidence. SUGGESTIONS FOR CLINICAL CARE (Suggestions are
Date written: July 2004 Final submission: July 2004 Author: David Johnson Uric acid GUIDELINES No recommendations possible based on Level I or II evidence. SUGGESTIONS FOR CLINICAL CARE (Suggestions are
Essence of the Revised Guideline for the Management of Hyperuricemia and Gout
 Research and Reviews Essence of the Revised Guideline for the Management of Hyperuricemia and Gout JMAJ 55(4): 324 329, 2012 Hisashi YAMANAKA,* 1 The Guideline Revising Committee of Japanese Society of
Research and Reviews Essence of the Revised Guideline for the Management of Hyperuricemia and Gout JMAJ 55(4): 324 329, 2012 Hisashi YAMANAKA,* 1 The Guideline Revising Committee of Japanese Society of
HARVARD PILGRIM HEALTH CARE RECOMMENDED MEDICATION REQUEST GUIDELINES
 Generic Brand HICL GCN Exception/Other PEGLOTICASE KRYSTEXXA 37154 GUIDELINES FOR USE 1. Does the patient have a diagnosis of symptomatic chronic gout (prior to initiating Krystexxa therapy) with clinical
Generic Brand HICL GCN Exception/Other PEGLOTICASE KRYSTEXXA 37154 GUIDELINES FOR USE 1. Does the patient have a diagnosis of symptomatic chronic gout (prior to initiating Krystexxa therapy) with clinical
Crystal induced arthropathies. Dr. Amitesh Aggarwal
 Crystal induced arthropathies Dr. Amitesh Aggarwal 1 Crystal induced Arthropathies Gout Pseudogout Debilitating illnesses; Recurrent episodes of pain and joint inflammation; Formation and deposition of
Crystal induced arthropathies Dr. Amitesh Aggarwal 1 Crystal induced Arthropathies Gout Pseudogout Debilitating illnesses; Recurrent episodes of pain and joint inflammation; Formation and deposition of
Treating to target: a strategy to cure gout
 Rheumatology 2009;48:ii9 ii14 doi:10.1093/rheumatology/kep087 Treating to target: a strategy to cure gout Fernando Perez-Ruiz 1 Acute gout attacks and the long-term complications of gout are associated
Rheumatology 2009;48:ii9 ii14 doi:10.1093/rheumatology/kep087 Treating to target: a strategy to cure gout Fernando Perez-Ruiz 1 Acute gout attacks and the long-term complications of gout are associated
CHAPTER:2 GOUT. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY
 CHAPTER:2 GOUT BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY DEFINITION Gout is defined as a peripheral arthritis, resulting from the deposition of MSU crystals
CHAPTER:2 GOUT BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY DEFINITION Gout is defined as a peripheral arthritis, resulting from the deposition of MSU crystals
Implementing AHRQ Effective Health Care Reviews Helping Clinicians Make Better Treatment Choices
 Implementing AHRQ Effective Health Care Reviews Helping Clinicians Make Better Treatment Choices Gout: Diagnosis and Management Practice Pointers by MATTHEW R. NOSS, DO, MSEd, U.S. Army Health Clinic,
Implementing AHRQ Effective Health Care Reviews Helping Clinicians Make Better Treatment Choices Gout: Diagnosis and Management Practice Pointers by MATTHEW R. NOSS, DO, MSEd, U.S. Army Health Clinic,
Novel uricosurics RHEUMATOLOGY. Thomas Bardin 1,2 and Pascal Richette 1,2. Abstract. Introduction REVIEW
 RHEUMATOLOGY Rheumatology 2018;57:i42 i46 doi:10.1093/rheumatology/kex433 Novel uricosurics Thomas Bardin 1,2 and Pascal Richette 1,2 REVIEW Abstract Objective. According to recent guidelines, the mainstay
RHEUMATOLOGY Rheumatology 2018;57:i42 i46 doi:10.1093/rheumatology/kex433 Novel uricosurics Thomas Bardin 1,2 and Pascal Richette 1,2 REVIEW Abstract Objective. According to recent guidelines, the mainstay
Gouty arthritis: an approach for general practice
 Gouty arthritis: an approach for general practice Abstract Tikly M, MBBCh, PhD, FCP(SA), FRCP, Professor of Rheumatology Makan K, MBChB, FCP(SA), Rheumatology Fellow Division of Rheumatology, Chris Hani
Gouty arthritis: an approach for general practice Abstract Tikly M, MBBCh, PhD, FCP(SA), FRCP, Professor of Rheumatology Makan K, MBChB, FCP(SA), Rheumatology Fellow Division of Rheumatology, Chris Hani
Uric acid and CKD. Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George
 Uric acid and CKD Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George Hospital @Badves Case Mr J, 52 Male, referred in June 2015 DM type 2 (4 years), HTN, diabetic retinopathy, diabetic
Uric acid and CKD Sunil Badve Conjoint Associate Professor, UNSW Staff Specialist, St George Hospital @Badves Case Mr J, 52 Male, referred in June 2015 DM type 2 (4 years), HTN, diabetic retinopathy, diabetic
Enhanced Primary Care Pathway: Gout
 Enhanced Primary Care Pathway: Gout 1. Focused summary of gout relevant to primary care Significance: Gout is a chronic, progressive, inflammatory disease requiring appropriate long-term management. Gout
Enhanced Primary Care Pathway: Gout 1. Focused summary of gout relevant to primary care Significance: Gout is a chronic, progressive, inflammatory disease requiring appropriate long-term management. Gout
New Drug Evaluation: lesinurad tablet, oral
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Managing Gout A Review of the Research for Adults
 Managing Gout A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* has said that you have gout. You are age 18 or
Managing Gout A Review of the Research for Adults e Is This Information Right for Me? This information is right for you if: Your health care professional* has said that you have gout. You are age 18 or
Clinical Study Allopurinol, Benzbromarone, or a Combination in Treating Patients with Gout: Analysis of a Series of Outpatients
 Hindawi Publishing Corporation International Journal of Rheumatology Volume 2014, Article ID 263720, 5 pages http://dx.doi.org/10.1155/2014/263720 Clinical Study Allopurinol, Benzbromarone, or a Combination
Hindawi Publishing Corporation International Journal of Rheumatology Volume 2014, Article ID 263720, 5 pages http://dx.doi.org/10.1155/2014/263720 Clinical Study Allopurinol, Benzbromarone, or a Combination
Guidelines for the treatment of gout: a Swiss perspective
 Published 1 September 2016, doi:10.4414/smw.2016.14341 Cite this as: Guidelines for the treatment of gout: a Swiss perspective Heloise Wüthrich* a, Fahad Alromaih* a, Alexander So a a Service de Rhumatologie,
Published 1 September 2016, doi:10.4414/smw.2016.14341 Cite this as: Guidelines for the treatment of gout: a Swiss perspective Heloise Wüthrich* a, Fahad Alromaih* a, Alexander So a a Service de Rhumatologie,
What will happen in the future? How will gout be diagnosed? How is gout treated? prevent
 Rheumatology Day Unit Dr J Hamilton 0191 4458359 0191 4455240 (9-5 Mon-Fri) Dr C Heycock 0191 4452198 Answer phone on 24hours Dr C Kelly 0191 4452193 Dr V Saravanan 0191 4456055 Dr M Rynne 0191 4458359
Rheumatology Day Unit Dr J Hamilton 0191 4458359 0191 4455240 (9-5 Mon-Fri) Dr C Heycock 0191 4452198 Answer phone on 24hours Dr C Kelly 0191 4452193 Dr V Saravanan 0191 4456055 Dr M Rynne 0191 4458359
Lesinurad in Combination With a Xanthine Oxidase Inhibitor for Treatment of Hyperuricemia Associated With Gout
 Lesinurad in Combination With a Xanthine Oxidase Inhibitor for Treatment of Hyperuricemia Associated With Gout Briefing Document for the Arthritis Advisory Committee Meeting Date: 23 October 215 Ardea
Lesinurad in Combination With a Xanthine Oxidase Inhibitor for Treatment of Hyperuricemia Associated With Gout Briefing Document for the Arthritis Advisory Committee Meeting Date: 23 October 215 Ardea
Lifestyle Interventions for the Treatment of Gout: A Summary of 2 Cochrane Systematic Reviews
 Lifestyle Interventions for the Treatment of Gout: A Summary of 2 Cochrane Systematic Reviews John H.Y. Moi, Melonie K. Sriranganathan, Louise Falzon, Christopher J. Edwards, Désirée M. van der Heijde,
Lifestyle Interventions for the Treatment of Gout: A Summary of 2 Cochrane Systematic Reviews John H.Y. Moi, Melonie K. Sriranganathan, Louise Falzon, Christopher J. Edwards, Désirée M. van der Heijde,
Class Update: Drugs for Gout
 Copyright 2012 Oregon State University. ll Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. ll Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Ad-Hoc Rheumatology Subcommittee of PTAC meeting held 8 March. (minutes for web publishing)
 Ad-Hoc Rheumatology Subcommittee of PTAC meeting held 8 March 2011 (minutes for web publishing) Ad-Hoc Rheumatology Subcommittee minutes are published in accordance with the Terms of Reference for the
Ad-Hoc Rheumatology Subcommittee of PTAC meeting held 8 March 2011 (minutes for web publishing) Ad-Hoc Rheumatology Subcommittee minutes are published in accordance with the Terms of Reference for the
Effectiveness of a pharmacist-based gout care management programme in a large integrated health plan: results from a pilot study
 Research Effectiveness of a pharmacist-based gout care management programme in a large integrated health plan: results from a pilot study Robert D Goldfien, 1 Michele S Ng, 2 Goldie Yip, 2 Alice Hwe, 2
Research Effectiveness of a pharmacist-based gout care management programme in a large integrated health plan: results from a pilot study Robert D Goldfien, 1 Michele S Ng, 2 Goldie Yip, 2 Alice Hwe, 2
Review. The modern management of gout RHEUMATOLOGY. Tom G. Rider 1 and Kelsey M. Jordan 1. Abstract. Introduction, definition and epidemiology REVIEW
 RHEUMATOLOGY Review Rheumatology 2010;49:5 14 doi:10.1093/rheumatology/kep306 Advance Access publication 5 October 2009 The modern management of gout Tom G. Rider 1 and Kelsey M. Jordan 1 Abstract Gout
RHEUMATOLOGY Review Rheumatology 2010;49:5 14 doi:10.1093/rheumatology/kep306 Advance Access publication 5 October 2009 The modern management of gout Tom G. Rider 1 and Kelsey M. Jordan 1 Abstract Gout
Prevalence of Gout and Hyperuricemia in the US General Population
 ARTHRITIS & RHEUMATISM Vol. 63, No. 10, October 2011, pp 3136 3141 DOI 10.1002/art.30520 2011, American College of Rheumatology Prevalence of Gout and Hyperuricemia in the US General Population The National
ARTHRITIS & RHEUMATISM Vol. 63, No. 10, October 2011, pp 3136 3141 DOI 10.1002/art.30520 2011, American College of Rheumatology Prevalence of Gout and Hyperuricemia in the US General Population The National
Gout: Let s Be Crystal Clear. Dr. Philip A. Baer Seacourses Asia CME December 2017
 Gout: Let s Be Crystal Clear Dr. Philip A. Baer Seacourses Asia CME December 2017 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or
Gout: Let s Be Crystal Clear Dr. Philip A. Baer Seacourses Asia CME December 2017 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or
Opinion 23 April 2014
 The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 23 April 2014 ILARIS 150 mg, powder for solution for injection B/1 vial (CIP: 34 009 397 457-6 3) ILARIS 150 mg, powder
The legally binding text is the original French version TRANSPARENCY COMMITTEE Opinion 23 April 2014 ILARIS 150 mg, powder for solution for injection B/1 vial (CIP: 34 009 397 457-6 3) ILARIS 150 mg, powder
Rheumatology Subcommittee of PTAC Meeting held 7 October (minutes for web publishing)
 Rheumatology Subcommittee of PTAC Meeting held 7 October 2014 (minutes for web publishing) Rheumatology Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Rheumatology Subcommittee of PTAC Meeting held 7 October 2014 (minutes for web publishing) Rheumatology Subcommittee minutes are published in accordance with the Terms of Reference for the Pharmacology
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
Patients' knowledge and beliefs concerning gout and its treatment: a population based study
 University of Massachusetts Medical School escholarship@umms Meyers Primary Care Institute Publications and Presentations Meyers Primary Care Institute 9-21-2012 Patients' knowledge and beliefs concerning
University of Massachusetts Medical School escholarship@umms Meyers Primary Care Institute Publications and Presentations Meyers Primary Care Institute 9-21-2012 Patients' knowledge and beliefs concerning
Krystexxa. Krystexxa (pegloticase) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.14 Subject: Krystexxa Page: 1 of 5 Last Review Date: March 16, 2018 Krystexxa Description Krystexxa
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.70.14 Subject: Krystexxa Page: 1 of 5 Last Review Date: March 16, 2018 Krystexxa Description Krystexxa
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ABCG2 gene, in gout, 283 285 Acetaminophen, for CPP crystal deposition, 347 ACTH (corticotropin), for gout, 335 336, 383 ADAMTS proteins,
Index Note: Page numbers of article titles are in boldface type. A ABCG2 gene, in gout, 283 285 Acetaminophen, for CPP crystal deposition, 347 ACTH (corticotropin), for gout, 335 336, 383 ADAMTS proteins,
Clinical Study Urate Lowering Therapy with Febuxostat in Daily Practice A Multicentre, Open-Label, Prospective Observational Study
 International Rheumatology, Article ID 123105, 6 pages http://dx.doi.org/10.1155/2014/123105 Clinical Study Urate Lowering Therapy with Febuxostat in Daily Practice A Multicentre, Open-Label, Prospective
International Rheumatology, Article ID 123105, 6 pages http://dx.doi.org/10.1155/2014/123105 Clinical Study Urate Lowering Therapy with Febuxostat in Daily Practice A Multicentre, Open-Label, Prospective
GOUT disease spectrum including
 GOUT disease spectrum including *hyperuricemia, *recurrent attacks of acute arthritis associated with monosodium urate crystals in leukocytes found in synovial fluid, *deposits of monosodium urate crystals
GOUT disease spectrum including *hyperuricemia, *recurrent attacks of acute arthritis associated with monosodium urate crystals in leukocytes found in synovial fluid, *deposits of monosodium urate crystals
GOUT IN THE ELDERLY. Learning Objectives. Disclosure. Geriatric Grand Rounds. Geriatric Grand Rounds
 Visit web sites: Tuesday, June 2, 2009 12:00 noon Dr. Bill Black Auditorium Glenrose Rehabilitation Hospital In keeping with Glenrose Rehabilitation Hospital policy, speakers participating in this event
Visit web sites: Tuesday, June 2, 2009 12:00 noon Dr. Bill Black Auditorium Glenrose Rehabilitation Hospital In keeping with Glenrose Rehabilitation Hospital policy, speakers participating in this event
Veterans Affairs databases are accurate for gout-related health care utilization: a validation study
 Singh Arthritis Research & Therapy 2013, 15:R224 RESEARCH ARTICLE Veterans Affairs databases are accurate for gout-related health care utilization: a validation study Jasvinder A Singh 1,2,3 Open Access
Singh Arthritis Research & Therapy 2013, 15:R224 RESEARCH ARTICLE Veterans Affairs databases are accurate for gout-related health care utilization: a validation study Jasvinder A Singh 1,2,3 Open Access
Drug Evaluation. Febuxostat, a novel drug for the treatment of hyperuricemia of gout. Future Rheumatology
 Febuxostat, a novel drug for the treatment of hyperuricemia of gout Fernando Perez-Ruiz, Nicola Dalbeth & Naomi Schlesinger Author for correspondence: Rheumatology Division, Hospital de Cruces, Pza Cruces
Febuxostat, a novel drug for the treatment of hyperuricemia of gout Fernando Perez-Ruiz, Nicola Dalbeth & Naomi Schlesinger Author for correspondence: Rheumatology Division, Hospital de Cruces, Pza Cruces
Subject: Krystexxa (pegloticase) Original Effective Date: 06/26/13. Policy Number: MCP-138. Revision Date(s):
 Subject: Krystexxa (pegloticase) Original Effective Date: 06/26/13 Policy Number: MCP-138 Revision Date(s): Review Date(s): 12/16/15; 6/15/2016; 3/21/2017 DISCLAIMER This Molina Clinical Policy (MCP) is
Subject: Krystexxa (pegloticase) Original Effective Date: 06/26/13 Policy Number: MCP-138 Revision Date(s): Review Date(s): 12/16/15; 6/15/2016; 3/21/2017 DISCLAIMER This Molina Clinical Policy (MCP) is
Fructose, Uric Acid and Hypertension in Children and Adolescents
 Fructose, Uric Acid and Hypertension in Children and Adolescents Daniel I. Feig, MD, PhD, MS Director, Division of Nephrology Department of Pediatrics University of Alabama, Birmingham Topics for Discussion
Fructose, Uric Acid and Hypertension in Children and Adolescents Daniel I. Feig, MD, PhD, MS Director, Division of Nephrology Department of Pediatrics University of Alabama, Birmingham Topics for Discussion
Treatment with Allopurinol is Associated with Lower Risk of Acute Kidney Injury in Patients with Gout: A Retrospective Analysis of a Nested Cohort
 Rheumatol Ther (2017) 4:419 425 DOI 10.1007/s40744-017-0082-2 ORIGINAL RESEARCH Treatment with Allopurinol is Associated with Lower Risk of Acute Kidney Injury in Patients with Gout: A Retrospective Analysis
Rheumatol Ther (2017) 4:419 425 DOI 10.1007/s40744-017-0082-2 ORIGINAL RESEARCH Treatment with Allopurinol is Associated with Lower Risk of Acute Kidney Injury in Patients with Gout: A Retrospective Analysis
Clinical Biochemistry department/ College of medicine / AL-Mustansiriyah University
 Clinical Biochemistry department/ College of medicine / AL-Mustansiriyah University Dr. Ali al-bayati NUCLEOTIDE METABOLISM Lec. 3 The salvage pathway of purine synthesis Purines that result from the normal
Clinical Biochemistry department/ College of medicine / AL-Mustansiriyah University Dr. Ali al-bayati NUCLEOTIDE METABOLISM Lec. 3 The salvage pathway of purine synthesis Purines that result from the normal
Zurampic. (lesinurad) New Product Slideshow
 Zurampic (lesinurad) New Product Slideshow Introduction Brand name: Zurampic Generic name: Lesinurad Pharmacological class: URAT1 inhibitor Strength and Formulation: 200mg; tablets Manufacturer: Ironwood
Zurampic (lesinurad) New Product Slideshow Introduction Brand name: Zurampic Generic name: Lesinurad Pharmacological class: URAT1 inhibitor Strength and Formulation: 200mg; tablets Manufacturer: Ironwood
Therapy for Gout: The Past
 Advances in Therapy for Gout: 2011 The Past, Present, and Future Therapy for Gout: The Past May 22, 1997 Pity a Tyrannosaur? Sue Had Gout By MALCOLM W. BROWNE Jonathan Graf, M.D. Associate Professor of
Advances in Therapy for Gout: 2011 The Past, Present, and Future Therapy for Gout: The Past May 22, 1997 Pity a Tyrannosaur? Sue Had Gout By MALCOLM W. BROWNE Jonathan Graf, M.D. Associate Professor of
Lecture 8 Gout Hinch. Pathogenesis of acute attacks
 Gout: disease characterized by deposition of monosodium crystals in soft tissues (cartilage, tendons, bursa) recurrent episodes of acute joint pain & inflammation Pathogenesis of acute attacks Epidemiology:
Gout: disease characterized by deposition of monosodium crystals in soft tissues (cartilage, tendons, bursa) recurrent episodes of acute joint pain & inflammation Pathogenesis of acute attacks Epidemiology:
Drugs for Gout, osteoarthritis and osteoporosis
 MMS Pharmacology Lecture 3 Drugs for Gout, osteoarthritis and osteoporosis Dr Sura Al Zoubi Revision Gout The term gout describes a disease spectrum including hyperuricemia, recurrent attacks of acute
MMS Pharmacology Lecture 3 Drugs for Gout, osteoarthritis and osteoporosis Dr Sura Al Zoubi Revision Gout The term gout describes a disease spectrum including hyperuricemia, recurrent attacks of acute
Abatacept (Orencia) for active rheumatoid arthritis. August 2009
 Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
Abatacept (Orencia) for active rheumatoid arthritis August 2009 This technology summary is based on information available at the time of research and a limited literature search. It is not intended to
N Engl J Med 2018;378: DOI: /NEJMoa Lin, Wan-Ting 2018/06/27
 N Engl J Med 2018;378:1200-10. DOI: 10.1056/NEJMoa1710895 Lin, Wan-Ting 2018/06/27 1 Introduction Gout is a chronic illness characterized by hyperuricemia, arthropathy, tophus development, and urolithiasis
N Engl J Med 2018;378:1200-10. DOI: 10.1056/NEJMoa1710895 Lin, Wan-Ting 2018/06/27 1 Introduction Gout is a chronic illness characterized by hyperuricemia, arthropathy, tophus development, and urolithiasis
