Low-dose Naltrexone: An Alternative Treatment for Erythrodermic Psoriasis
|
|
|
- Ethelbert Michael Mathews
- 5 years ago
- Views:
Transcription
1 Open Access Case Report DOI: /cureus.3943 Low-dose Naltrexone: An Alternative Treatment for Erythrodermic Psoriasis Eduardo P. Beltran Monasterio 1 1. Dermatology, Universidade Gama Filho (instituto De Pesquisa E Ensino Médico), Florianopolis, BRA Corresponding author: Eduardo P. Beltran Monasterio, dreduardobeltran@yahoo.com Disclosures can be found in Additional Information at the end of the article Abstract This clinical case demonstrates the benefits of patient treatment with low-dose naltrexone (LDN) used in erythrodermic psoriasis. A patient with a confirmed history of psoriasis by histopathology was treated with 4.5 mg of LDN during six months follow-up after an erythrodermic psoriasis flare-up. The patient showed significant improvement in her flare-up and psoriasis remission after only three months of 4.5 mg of LDN on a daily basis. Low-dose naltrexone (LDN) has proven to be a great ally in treating erythrodermic psoriasis flare-ups as an alternative treatment with less collateral side effects. Categories: Dermatology, Family/General Practice, Internal Medicine Keywords: ldn as a new treatment option for psoriasis, erythomatous psoriasis and ldn, ldn, ldn in dermatology, ldn for erythrodermic psoriasis Introduction Psoriasis is a chronic, inflammatory, autoimmune skin disease that results in the of formation of white-silvery, dry, itchy patches. Approximately, 2%-3% of the population develops the disease according to the National Psoriasis Foundation (NPF) [1]. The mechanisms involved in the pathogenesis of this condition is still not well-understood, but it is known to be a polygenic disorder with triggering environmental factors such as trauma, infections, medications, and emotional stress. Received 01/14/2019 Review began 01/19/2019 Review ended 01/19/2019 Published 01/23/2019 Copyright 2019 Beltran Monasterio. This is an open access article distributed under the terms of the Creative Commons Attribution License CC-BY 3.0., which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Several clinical expressions exist, and the characteristic lesion found in patients with psoriasis is the presence of erythematous-scaly (silvery-white) patches found on the skin. These lesions may usually have a chronic form of manifestation and rarely evolve to an acute form known as erythrodermic psoriasis. It generally appears on people who have unstable plaque psoriasis, i.e., in only 3% percent of the people who have psoriasis. Individuals having an erythrodermic psoriasis flare-up should see a doctor immediately. This form of psoriasis can be lifethreatening according to the National Psoriasis Foundation (NPF) [2]. Erythrodermic psoriasis is a condition involving practically the entire skin body surface, which can sometimes lead to constitutional symptoms. It is known to a be a severe and dangerous form of psoriasis, which may be life-threatening. In this particular clinical case, we shall discuss the experience of using manipulated oral low-dose naltrexone (LDN) in combined treatment with topical colloidal oat cream and oral hydroxyzine in a patient with severe erythrodermic psoriasis. Ogawa et al. [3] have described psoriasis histologically by the presence of dendritic and T-cells with increased intralesional levels of T-helper cells, interleukins, and tumor necrosis factor How to cite this article Beltran Monasterio E P (January 23, 2019) Low-dose Naltrexone: An Alternative Treatment for Erythrodermic Psoriasis. Cureus 11(1): e3943. DOI /cureus.3943
2 (TNF) at the site of the skin plaque. These immunological markers serve as therapeutical targets for psoriasis treatment. Methotrexate is one of the first and low-cost end drugs that has been used for certain forms of psoriasis, but then again has shown to have severe adverse side effects. Alanna et al. [4] have shown that newer drug therapies have been developed for the treatment of psoriasis through immune-modulating biologics such as adalimumab, ustekinumab, and secukinumab. Despite the high cost of these newer drugs and promising results, not all patients can benefit from them or can tolerate these medications. This has led some physicians to try unconventional anti-inflammatory drugs, such as low-dose naltrexone (LDN), in the treatment of autoimmune diseases, including psoriasis. Significant and credible evidence and research published on Low Dose Naltrexone Research Trust [5] has shown repeatedly the international medical community the promising benefits of this drug. Case Presentation The following clinical case is of a 38-year-old, white female patient from the municipality of São Pedro de Alcântara, State of Santa Catarina, Brazil (South America). She worked as a parttime car mechanic and as a security guard. The patient had a long history of psoriasis since the age of 22, which was later confirmed by histopathology. She consulted many dermatologists previously, having used a large variety of topical steroidal creams that showed little benefits. During her last visit to her dermatologist, she was put on oral methotrexate 7.5 mg/week as an initial dose in association with 5 mg folic acid/day with clobetasol 0.05% cream twice a day. The patient received medical treatment through the public health care system (Sistema Único de Saude - SUS) located at Santa Teresa Dermatologic Hospital in São Pedro de Alcântara, Santa Catarina, Brazil. The patient mentioned that she showed poor results after three months of treatment. The patient felt that it was necessary to interrupt the medication by her physician due to the side effects of methotrexate (anemia, thrombocytopenia, and leukopenia). After two weeks of taking a suspension of methotrexate, the patient showed acute worsening of her condition and went to the Family Medicine Health Care Clinic (Maria Rasveiler Junckes) where she consulted another dermatologist on June 22, On initial physical examination, the patient showed signs of facial swelling (Figure 1), predominantly on the right side of her face with significant "wet" edema of the upper and lower extremities (Figure 2). The patient referred to having "shivers" and severe itching and joint pain with disseminated lesions notated throughout almost all her body surface. Her Psoriasis Area Severity Index (PASI) score was of 48 (Figure 3) Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
3 FIGURE 1: Initial consultation facial photo This picture was taken on initial consultation. Dry skin with inflammatory facial edema and superficial scaling was evident, as shown by the arrow. The patient had recently suspended methotrexate treatment Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
4 FIGURE 2: Bilateral edema of upper and lower extremities (Initial consultation) Bilateral edema of the upper and lower extremities was evident, associated with itching and redness, as shown by the arrow. The patient mentioned having some difficulty in making a fist with her hand Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
5 FIGURE 3: Initial consultation photo of the dorsal back In this photo, we can appreciate the presence of disseminated erythematous plaques throughout the patient's entire body. Erythrodermic psoriasis is a condition that sometimes may "throw off" the body's chemistry, causing proteinuria with fluid loss and leading to severe illness. Infection is an important aspect to be taken into consideration, which can bring upon pneumonia and congestive heart failure. The patient was monitored closely at our clinic and regular laboratory evaluations were performed to observe any significant metabolic changes. The patient was very concerned about her condition and expressed this verbally, refusing to take any immunosuppressive cytotoxic drugs, such as methotrexate, which was prescribed previously. At this moment, a low-dose naltrexone (LDN) regimen was the only "open-door" option for her and her family, due to the less aggressive side effects of methotrexate. Treatment Oral low-dose naltrexone (LDN) was prescribed at a starting dose of 4.5 mg every night with 25 mg of hydroxyzine every 12 hours, with topical colloidal oat cream every eight hours. Her vitals signs kept within normal ranges at all times and showed progressive normalization of her laboratory values. Initial renal function showed mild proteinuria with elevated serum urea and creatinine that normalized throughout the following two weeks. Her folate levels were very low as well. Congestive heart failure and infections were excluded by electrocardiogram (ECG), chest X-ray, and laboratory results. A daily follow-up was done during the first 10 days, followed by a 20-day, three-month, and, finally, six-month follow-up. Results 2019 Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
6 After 10 Days of Treatment The patient showed significant improvement after 10 days of 4.5 mg of LDN orally every night. She no longer mentioned an itchy sensation and discontinued hydroxyzine at nine days of treatment. Signs of regression of the facial swelling and edema of upper and lower extremities were notable after 10 days. Like in the Metze et al. study [6], LDN has been proven to eliminate these symptoms. After 20 Days of Treatment The patient showed complete improvement after 20 days of treatment with 4.5 mg of LDN orally every night and applying topical colloidal oat cream on a regular, daily basis. The Phan et al. study [7] on antipruritic treatment with systemic mu-opioid receptor antagonists, such as LDN, has proven its benefits as an antipruritic agent. Noticeable reduction in facial edema (Figure 4) by more than 50%, upper extremity swelling (Figure 5), and considerable reduction of disseminated pruritic plaques on the skin surface (Figure 6) were also evident Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
7 FIGURE 4: After 20 days treatment with 4.5 mg LDN orally. In this picture, we can observe how low-dose naltrexone (LDN) has shown noticeable improvement in her facial edema. Facial redness had improved by more than 50%, as shown by the arrow. The patient was symptom-free of itching. FIGURE 5: After 20 days of treatment with LDN Significant improvement of bilateral upper extremity edema with an important reduction in the itching sensation obtained with low-dose naltrexone (LDN) Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
8 FIGURE 6: After 20 days of treatment with low-dose naltrexone (posterior dorsal back region) In this photo, we can easily identify an important reduction after 20 days of low-dose naltrexone (LDN) in disseminated erythematous plaque formation. Only a solitary main plaque was found in the central dorsal posterior region of the back as denoted by the arrow. After Three Months and Six Months Treatment A follow-up was done at three months and six months consecutively after an acute "flareup" episode. During the consultation, she showed complete psoriasis remission at three months (Figure 7), with a Psoriasis Area Severity Index (PASI) score of 0 (Figure 8) Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
9 FIGURE 7: Picture after three months of treatment with 4.5 mg LDN orally In this picture, we can see complete remission of the disease, as pointed to by the arrow after three months of low-dose naltrexone (LDN). Symptom-free (Psoriasis Area Severity Index (PASI) score = 0). The patient was compliant with treatment and did not refer to any side effects of LDN during her treatment. The patient was very pleased with her results Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
10 FIGURE 8: After three months of treatment with low dose naltrexone In this photo, we can notice complete remission of the disease after three months of low-dose naltrexone (LDN) treatment. The patient was symptom-free. The same clinical condition was evident after six months of LDN treatment (Figure 9). No side effects of LDN were referred to or observed throughout the whole treatment. Quality of life was improved dramatically by having a profound positive impact on her daily routine. The patient returned to work after 20 days of treatment. It is important to note that the patient used to work as a security corrections officer at night and worked as a car mechanic during the day. Having left her night job also played an important role in the recovery of her condition Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
11 FIGURE 9: After six months of treatment with 4.5 mg LDN orally After six months of follow-up of low-dose naltrexone (LDN) treatment, the patient showed no signs of psoriasis. Her Psoriasis Area Severity Index (PASI) was 0. Complete remission of the disease was evident. The patient expressed much content with her results and all lab work came back normal. Discussion The initial, acute flare-up (trigger) of this clinical case probably was due to the side effects and abrupt withdrawal of conventional treatment with methotrexate. Laboratory findings showed drug-induced pancytopenia (anemia, thrombocytopenia, and leukopenia). Renal function showed proteinuria with mild serum elevation of urea and creatinine values. Erythrocyte sedimentation rate (ESR) was normal. Serum uric acid was slightly elevated. ECG showed a normal sinus rhythm with normal cardiac enzymes. The histopathology of the skin showed hyperkeratosis, parakeratosis, and acanthosis, with an intense presence of neutrophils in the epidermis. The thinning of the epidermis overlying the dermal papillae with vessels close to the epidermis and elongated rete-ridges mitotic was seen on her biopsy. The diagnosis of erythrodermic psoriasis is mainly clinical. The clinical features that were observed in this case showed the presence of generalized, disseminated erythematous plaques throughout the patients' entire body. The clinical findings of facial edema along with the presence of small vesicular eruptions of the upper and lower extremities were suggestive of fluid retention. The severe disseminated redness throughout the body was contained due to the prompt use of LDN. The patient also mentioned a severe itching sensation, joint pain along with cold "shivers" on the initial consultation, suggestive of the body trying to maintain a 2019 Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
12 normal temperature. Another important aspect noted is that stressful working conditions can easily be a potential trigger in the resurfacing of any autoimmune disease such as psoriasis. It is very important that the attending physician addresses, evaluates, and identifies any precipitating factors that may induce or cause emotional stress in the patient. Adequate control of the emotional component and a balanced healthy lifestyle is crucial in avoiding future flare-ups. LDN has proven to help maintain the patient s psoriasis in remission, having a profound positive impact on her daily activities and quality of life. As mentioned by the Younger et al. [8], the following three theoretical components are of the most relevance regarding the LDN mechanism of action: 1) action on opioid receptors to increase the release of β-endorphins; 2) ability to reduce pro-inflammatory cytokines and increase anti-inflammatory cytokines; and 3) regulation of the opioid growth factor (OGF)/opioid growth factor receptors (OGFr) axis. The increase of β-endorphins for joint pain management is of significant therapeutical importance, having a big impact on the quality of life of this patient. The role that LDN plays in downregulating the multiple pro-inflammatory cytokines is a fundamental aspect in the attempt to balance out and normalize the cutaneous inflammatory state in erythrodermic psoriasis. LDN has shown us that the opioid growth factor-opioid growth factor receptor (OGF-OGFr) axis is a key element that plays a very important role in maintaining a delicate balance in the upregulation and downregulation of the immune system. Little attention has been paid to the development of newer drugs that can act upon this axis. Having obtained these results throughout the six months of treatment with LDN should be an eye opener for future LDN-prescribing physicians. LDN has proven to have strong potential therapeutical benefits and should encourage more physicians to consider the use of LDN as alternative therapy for patients who cannot tolerate conventional mainstream medicine. Conclusions This clinical case study has clearly shown the benefits of 4.5 mg low-dose naltrexone for erythrodermic psoriasis. A remarkable improvement was documented by the twentieth day of treatment. Complete remission of the disease was evident by three months, with no signs of plaques anywhere on the patient's body. Her PASI score improved rapidly, with a score of 0 along with her normal laboratory results, by the third month. No secondary side effects were reported at any time during treatment. Additional Information Disclosures Human subjects: Consent was obtained by all participants in this study. Conflicts of interest: In compliance with the ICMJE uniform disclosure form, all authors declare the following: Payment/services info: All authors have declared that no financial support was received from any organization for the submitted work. Financial relationships: All authors have declared that they have no financial relationships at present or within the previous three years with any organizations that might have an interest in the submitted work. Other relationships: All authors have declared that there are no other relationships or activities that could appear to have influenced the submitted work. References 1. National Psoriasis Foundation - psoriasis causes and triggers. (2018). Accessed: October 23, 2018: Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
13 2. National Psoriasis Foundation - erythrodermic psoriasis. (2018). Accessed: October 23, 2018: 3. Ogawa E, Sato Y, Minagawa A, Okuyama R: Pathogenesis of psoriasis and development of treatment. J Dermatol. 2018, 45: / Bridgman AC, Kirchhof MG: Treatment of psoriasis vulgaris using low-dose naltrexone. JAAD Case Rep. 2018, 4: /j.jdcr Clinical trials. (2018). Accessed: December 5, 2018: 6. Metze D, Reimann S, Beissert S, Luger T: Efficacy and safety of naltrexone, an oral opiate receptor antagonist, in the treatment of pruritus in internal and dermatological diseases. J Am Acad Dermatol. 1999, 41: Phan NQ, Bernhard JD, Luger TA, Stander S: Antipruritic treatment with systemic mu-opioid receptor antagonists: a review. J Am Acad Dermatol. 2010, 63: /j.jaad Younger J, Parkitny L, McLain D: The use of low-dose naltrexone (LDN) as a novel antiinflammatory treatment for chronic pain. Clin Rheumatol. 2014, 33: /s Beltran Monasterio et al. Cureus 11(1): e3943. DOI /cureus of 13
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA)
 Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
Retrospective 10 years review of 100 patients with psoriasis in the Kingdom of Saudi Arabia (KSA) Ahmed Abdullah Alhumidi King saud university, Riyadh, kingdom of Saudi Arabia Abstract Background: This
THE THERAPY OF THE REBEL SEVERE PSORIAZIS WITH BIOLOGICAL PREPARATS
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 THE THERAPY OF THE REBEL SEVERE PSORIAZIS WITH BIOLOGICAL PREPARATS Mădălina FRÎNCU 1 Abstract: Biological
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 THE THERAPY OF THE REBEL SEVERE PSORIAZIS WITH BIOLOGICAL PREPARATS Mădălina FRÎNCU 1 Abstract: Biological
Ustekinumab Treatment of Erythrodermic Psoriasis Occurring after Physical Stress: A Report of Two Cases
 Published online: September 26, 2013 1662 6567/13/0053 0254$38.00/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: September 26, 2013 1662 6567/13/0053 0254$38.00/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Recalcitrant Warty Erythroderma With Severe Pruritus. Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University
 Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
Recalcitrant Warty Erythroderma With Severe Pruritus Gil Yosipovitch Professor & Chair Department of Dermatology & Itch Center Temple University DISCLOSURE OF RELEVANT RELATIONSHIPS WITH INDUSTRY Gil Yosipovitch,
chemotherapeutic agents in
 Use of biologics and chemotherapeutic agents in cutaneous emergencies: Focus on lifethreatening forms of psoriasis Alice Bendix Gottlieb MD, PhD Professor of Dermatology New York Medical College Metropolitan
Use of biologics and chemotherapeutic agents in cutaneous emergencies: Focus on lifethreatening forms of psoriasis Alice Bendix Gottlieb MD, PhD Professor of Dermatology New York Medical College Metropolitan
COMMON SKIN CONDITIONS IN PRIMARY CARE. Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio
 COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
COMMON SKIN CONDITIONS IN PRIMARY CARE Ibrahim M. Zayneh, MD Dermatology Private Practice, Portsmouth, Ohio DISCLOSURE The Speaker and members of the planning committee do not have a conflict of interest
Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])
![Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV]) Phototherapy and Photochemotherapy Treatment (Ultraviolet A [PUVA] and B [UBV])](/thumbs/89/99382632.jpg) Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
Origination: 09/27/07 Revised: 08/2/17 Annual Review: 11/2/17 Purpose: To provide Phototherapy and Photochemotherapy Treatment (PUVA and UBV) guidelines for the Medical Department staff to reference when
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psoriasis: the management of psoriasis 1.1 Short title Psoriasis 2 The remit The Department of Health has asked NICE: 'to produce
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Psoriasis: the management of psoriasis 1.1 Short title Psoriasis 2 The remit The Department of Health has asked NICE: 'to produce
Minami-Hori M, Tsuji H, Takahashi H, Hanada K, Iizuka H
 The Journal of Dermatology (2013.Jan) :. Optic neuritis in a psoriatic arthritis patient treated by infliximab Minami-Hori M, Tsuji H, Takahashi H, Hanada K, Iizuka H 1 Optic neuritis in a psoriatic arthritis
The Journal of Dermatology (2013.Jan) :. Optic neuritis in a psoriatic arthritis patient treated by infliximab Minami-Hori M, Tsuji H, Takahashi H, Hanada K, Iizuka H 1 Optic neuritis in a psoriatic arthritis
What caused this refractory pruritic eruption? Patient Presentation
 What caused this refractory pruritic eruption? Patient Presentation A 67 year-old female presented with greater than 3 years of refractory and debilitating intermittent bouts of recurrent pruritus on the
What caused this refractory pruritic eruption? Patient Presentation A 67 year-old female presented with greater than 3 years of refractory and debilitating intermittent bouts of recurrent pruritus on the
Spontaneous Tumor Lysis Syndrome in Small Cell Lung Cancer
 Open Access Case Report DOI: 10.7759/cureus.1017 Spontaneous Tumor Lysis Syndrome in Small Cell Lung Cancer Venkatkiran Kanchustambham 1, Swetha Saladi 2, Setu Patolia 2, David Stoeckel 2 1. Pulmonary
Open Access Case Report DOI: 10.7759/cureus.1017 Spontaneous Tumor Lysis Syndrome in Small Cell Lung Cancer Venkatkiran Kanchustambham 1, Swetha Saladi 2, Setu Patolia 2, David Stoeckel 2 1. Pulmonary
NORLAND AVENUE PHARMACY PRESCRIPTION COMPOUNDING FOR GENERAL PRACTICE
 AUGUST 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Hemorrhoids 2 Celiac Disease 3 PRESCRIPTION
AUGUST 2011 PRESCRIPTION COMPOUNDING N ORLANDA VENUEP HARMACY. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Hemorrhoids 2 Celiac Disease 3 PRESCRIPTION
Guttate psoriasis =ﻒدﺼﻠا ﻲﻄﻘﻨﻠا
 1 / 69 Psoriasis Psoriasis may be divided into psoriasis vulgaris, generalized pustular psoriasis, and localized pustular ps Psoriasis Vulgaris Clinical Features 2 / 69 Psoriasis vulgaris is a common chronic
1 / 69 Psoriasis Psoriasis may be divided into psoriasis vulgaris, generalized pustular psoriasis, and localized pustular ps Psoriasis Vulgaris Clinical Features 2 / 69 Psoriasis vulgaris is a common chronic
Psoraisis = ﻒدﺼﻠا 1 / 84
 1 / 84 2 / 84 3 / 84 4 / 84 5 / 84 6 / 84 Psoriasis Psoriasis may be divided into psoriasis vulgaris, generalized pustular psoriasis, and localized pustular ps Psoriasis Vulgaris Clinical Features 7 /
1 / 84 2 / 84 3 / 84 4 / 84 5 / 84 6 / 84 Psoriasis Psoriasis may be divided into psoriasis vulgaris, generalized pustular psoriasis, and localized pustular ps Psoriasis Vulgaris Clinical Features 7 /
A Pilot Study. Name of investigational product:
 An Open Label, Multi Center Clinical Study to Evaluate the Efficacy and Safety of a New Topical Cosmeceutical in Relieving the Redness, Scaling and Flaking Associated with Severe Skin Conditions A Pilot
An Open Label, Multi Center Clinical Study to Evaluate the Efficacy and Safety of a New Topical Cosmeceutical in Relieving the Redness, Scaling and Flaking Associated with Severe Skin Conditions A Pilot
2017 Blue Cross and Blue Shield of Louisiana
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Psoriasis Case presentation 2 Ahmad is 50 years old male came to the on call dermatologist with a 3 day history of feeling generally unwell and
 Psoriasis Case presentation 2 Ahmad is 50 years old male came to the on call dermatologist with a 3 day history of feeling generally unwell and redness of all skin associated with de-sequamation scaling.
Psoriasis Case presentation 2 Ahmad is 50 years old male came to the on call dermatologist with a 3 day history of feeling generally unwell and redness of all skin associated with de-sequamation scaling.
What is Psoriasis? Common Areas Affected. Type Who Does it Affect Characteristics
 What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
What is? is a term derived from the Greek word psōra which means itch and is a common, long lasting, inflammatory skin condition which affects 1-3% of the UK population and about 80 million people worldwide.
Chronic Lymphedema of the Lower Limb: A Rare Cause of Dislocation of Total Hip Arthroplasty
 Open Access Case Report DOI: 10.7759/cureus.579 Chronic Lymphedema of the Lower Limb: A Rare Cause of Dislocation of Total Hip Arthroplasty Raju Vaishya 1, Amit Kumar Agarwal 1, Nishint Gupta 2, Vipul
Open Access Case Report DOI: 10.7759/cureus.579 Chronic Lymphedema of the Lower Limb: A Rare Cause of Dislocation of Total Hip Arthroplasty Raju Vaishya 1, Amit Kumar Agarwal 1, Nishint Gupta 2, Vipul
Psoriasis. Jessica Kaffenberger, M.D. Assistant Professor of Dermatology Division of Dermatology The Ohio State University Wexner Medical Center
 Psoriasis Jessica Kaffenberger, M.D. Assistant Professor of Dermatology Division of Dermatology The Ohio State University Wexner Medical Center Learning objectives Recognize the different types of psoriasis
Psoriasis Jessica Kaffenberger, M.D. Assistant Professor of Dermatology Division of Dermatology The Ohio State University Wexner Medical Center Learning objectives Recognize the different types of psoriasis
EXAMINING THE CRUCIAL COALITION BETWEEN DERMATOLOGY AND RHEUMATOLOGY IN PSORIATIC ARTHRITIS
 EXAMINING THE CRUCIAL COALITION BETWEEN DERMATOLOGY AND RHEUMATOLOGY IN PSORIATIC ARTHRITIS ACTIVITY 1: EARLY COLLABORATION IN THE TREATMENT OF PSA Key Slides COMMON COMORBIDITIES OF PSORIATIC DISEASE
EXAMINING THE CRUCIAL COALITION BETWEEN DERMATOLOGY AND RHEUMATOLOGY IN PSORIATIC ARTHRITIS ACTIVITY 1: EARLY COLLABORATION IN THE TREATMENT OF PSA Key Slides COMMON COMORBIDITIES OF PSORIATIC DISEASE
What is Enbrel? Key features
 What is Enbrel? Enbrel (also known by its generic name etanercept) is a biologic medication approved in April 2004 by the U.S. Food and Drug Administration (FDA) for the treatment of moderate to severe
What is Enbrel? Enbrel (also known by its generic name etanercept) is a biologic medication approved in April 2004 by the U.S. Food and Drug Administration (FDA) for the treatment of moderate to severe
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Proposed Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Dimethyl fumarate for treating moderate to severe Draft scope (pre-referral) Draft remit/appraisal objective To appraise
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Proposed Health Technology Appraisal Dimethyl fumarate for treating moderate to severe Draft scope (pre-referral) Draft remit/appraisal objective To appraise
Update on emollients
 Update on emollients Amal Mhanna, MD Pediatric Dermatologist Clemenceau Medical Center Disclosure: I was a member of an advisory board y for J&J and received honoraria. Emollients and moisturizers are
Update on emollients Amal Mhanna, MD Pediatric Dermatologist Clemenceau Medical Center Disclosure: I was a member of an advisory board y for J&J and received honoraria. Emollients and moisturizers are
Pediatric Use: Safety and effectiveness of Ustekinumab (STELARA ) in pediatric patients have not been evaluated.
 Original Issue Date (Created): January 1, 2010 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 I. POLICY Preauthorization Requirements for Ustekinumab (STELARA ) Note:
Original Issue Date (Created): January 1, 2010 Most Recent Review Date (Revised): January 28, 2014 Effective Date: April 1, 2014 I. POLICY Preauthorization Requirements for Ustekinumab (STELARA ) Note:
ustekinumab (Stelara )
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Psoriasis. What is Psoriasis? What causes psoriasis? Medical Topics Psoriasis
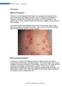 1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
1 Psoriasis What is Psoriasis? Psoriasis is a long standing inflammatory non-contagious skin disease which waxes and wanes with triggering factors. There is a genetic predisposition in psoriasis. Internationally,
Skin Side Effects U N I V E R S I T Y OF V I E N N A, D E P A R T M E N T OF O N C O L O G Y, G E N E R A L H O S P I T A L V I E N N A
 Skin Side Effects Christiane Thallinger, M D U N I V E R S I T Y OF V I E N N A, D E P A R T M E N T OF O N C O L O G Y, G E N E R A L H O S P I T A L V I E N N A Targets Substances 1 Multi Kinase Inhibitors
Skin Side Effects Christiane Thallinger, M D U N I V E R S I T Y OF V I E N N A, D E P A R T M E N T OF O N C O L O G Y, G E N E R A L H O S P I T A L V I E N N A Targets Substances 1 Multi Kinase Inhibitors
Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis with Comorbid Conditions
 Dermatology Research and Practice Volume 2, Article ID 13326, 4 pages http://dx.doi.org/.1155/2/13326 Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis
Dermatology Research and Practice Volume 2, Article ID 13326, 4 pages http://dx.doi.org/.1155/2/13326 Research Article Clinical Outcome of a Novel Anti-CD6 Biologic Itolizumab in Patients of Psoriasis
Rheumatoid arthritis
 Rheumatoid arthritis 1 Definition Rheumatoid arthritis is one of the most common inflammatory disorders affecting the population worldwide. It is a systemic inflammatory disease which affects not only
Rheumatoid arthritis 1 Definition Rheumatoid arthritis is one of the most common inflammatory disorders affecting the population worldwide. It is a systemic inflammatory disease which affects not only
Update on systemic therapies and emerging treatments How do I choose a systemic agent?
 Update on systemic therapies and emerging treatments How do I choose a systemic agent? Amy S. Paller, M.D. Walter J. Hamlin Professor and Chair of Dermatology Professor of Pediatrics Northwestern University
Update on systemic therapies and emerging treatments How do I choose a systemic agent? Amy S. Paller, M.D. Walter J. Hamlin Professor and Chair of Dermatology Professor of Pediatrics Northwestern University
Psoriasis management. A/Prof Amanda Oakley Dermatologist, Waikato
 Psoriasis management A/Prof Amanda Oakley Dermatologist, Waikato AbbVie Breakfast Session, 14 June 2014 Disclosure This breakfast session is sponsored by Abbvie Autoimmune skin disorders Psoriasis Eczema
Psoriasis management A/Prof Amanda Oakley Dermatologist, Waikato AbbVie Breakfast Session, 14 June 2014 Disclosure This breakfast session is sponsored by Abbvie Autoimmune skin disorders Psoriasis Eczema
Vulval dermatoses. Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough
 Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Vulval dermatoses Dr Fiona Lewis, Consultant Dermatologist St John s Institute of Dermatology, London & Heatherwood & Wexham Park Hospital, Slough Pigmentation Vulvodynia Ulcers Genetic Pruritus VULVAL
Systemic Lupus Erythematosus
 A Patient s Guide to Systemic Lupus Erythematosus 2 kidneys. These changes make it impossible for the kidneys to function normally. The inflammation of SLE can be seen in the lining, covering, and muscles
A Patient s Guide to Systemic Lupus Erythematosus 2 kidneys. These changes make it impossible for the kidneys to function normally. The inflammation of SLE can be seen in the lining, covering, and muscles
Difference Between Seborrheic Dermatitis and Psoriasis
 Difference Between Seborrheic Dermatitis and Psoriasis www.differencebetween.com Key Difference Seborrheic Dermatitis vs Psoriasis Dermatological conditions are perhaps the most worrisome diseases in the
Difference Between Seborrheic Dermatitis and Psoriasis www.differencebetween.com Key Difference Seborrheic Dermatitis vs Psoriasis Dermatological conditions are perhaps the most worrisome diseases in the
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
Keywords: Psoriasis vulgaris Zinc pyrithione Betamethasone dipropionate
 CLINICAL EFFICACY AND SAFETY OF A COMBINED FORMULATION OF ZINC PYRITHIONE 0.25% AND BETAMETHASONE DIPROPIONATE MICRONIZED 0.05% IN THE TREATMENT OF MILD TO MODERATE PLAQUE PSORIASIS. Abstract Background
CLINICAL EFFICACY AND SAFETY OF A COMBINED FORMULATION OF ZINC PYRITHIONE 0.25% AND BETAMETHASONE DIPROPIONATE MICRONIZED 0.05% IN THE TREATMENT OF MILD TO MODERATE PLAQUE PSORIASIS. Abstract Background
Clinical Policy: Ustekinumab (Stelara) Reference Number: ERX.SPA.01 Effective Date:
 Clinical Policy: (Stelara) Reference Number: ERX.SPA.01 Effective Date: 04.01.17 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Stelara) Reference Number: ERX.SPA.01 Effective Date: 04.01.17 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Eczema. By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University
 Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Eczema By:- Dr. Naif Al-Shahrani Salman bin Abdazziz University Dermatitis= Eczema =Spongiosis Eczema Atopic Seborrheic Contact Allergic Irritant Nummular Asteatotic Stasis Neurodermatitis/Lichen Simplex
Dermatology elective for yr. 5. Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015
 Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
Dermatology elective for yr. 5 Natta Rajatanavin, MD. Div. of dermatology Dep. Of Medicine, Ramathibodi Hospital Mahidol University 23 rd Feb 2015 How to diagnosis and manage eczema and psoriasis. Objectives
PSORIASIS PSORIASIS. Anatomic sites FACTS ABOUT PROSIASIS PSORIASIS 11/16/2017 STIGMATA OF PSORIASIS
 PSORIASIS Dr. Sami Alsuwaidan President, Saudi Society of Dermatology & Dermatologic Surgery Associate Professor and Consultant Department of Dermatology, College of Medicine King Saud University PSORIASIS
PSORIASIS Dr. Sami Alsuwaidan President, Saudi Society of Dermatology & Dermatologic Surgery Associate Professor and Consultant Department of Dermatology, College of Medicine King Saud University PSORIASIS
Biologics in Psoriasis. Peter CM van de Kerkhof Department of Dermatology Radboud University Nijmegen Medical Centre
 Biologics in Psoriasis Peter CM van de Kerkhof Department of Dermatology Radboud University Nijmegen Medical Centre Disclosures Consultancy services for Celgene, Centocor, Almirall, Amgen, Pfizer, Philips,
Biologics in Psoriasis Peter CM van de Kerkhof Department of Dermatology Radboud University Nijmegen Medical Centre Disclosures Consultancy services for Celgene, Centocor, Almirall, Amgen, Pfizer, Philips,
The Treatment Toolbox for Severe Pediatric Psoriasis
 The Treatment Toolbox for Severe Pediatric Psoriasis Dr. Kim A. Papp, MD, PhD, FRCPC, FAAD K Papp Clinical Research and Probity Medical Research Objectives: Treating severe pediatric psoriasis 1. Challenges
The Treatment Toolbox for Severe Pediatric Psoriasis Dr. Kim A. Papp, MD, PhD, FRCPC, FAAD K Papp Clinical Research and Probity Medical Research Objectives: Treating severe pediatric psoriasis 1. Challenges
SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE M. FRÎNCU 1 A. OANŢĂ 1 Abstract:
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 SYSTEMIC THERAPY OF MODERATE AND SEVERE PSORIASIS WITH METHOTREXATE M. FRÎNCU 1 A. OANŢĂ 1 Abstract:
A case of rosacea fulminans in a pregnant woman
 Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
Hong Kong J. Dermatol. Venereol. (2018) 26, 122-126 Views and Practice A case of rosacea fulminans in a pregnant woman JE Seol, SH Park, JU Kim, GJ Cho, SH Moon, H Kim Introduction Rosacea fulminans (RF)
UvA-DARE (Digital Academic Repository) Innovative therapies and new targets in psoriasis de Groot, M. Link to publication
 UvA-DARE (Digital Academic Repository) Innovative therapies and new targets in psoriasis de Groot, M. Link to publication Citation for published version (APA): de Groot, M. (2011). Innovative therapies
UvA-DARE (Digital Academic Repository) Innovative therapies and new targets in psoriasis de Groot, M. Link to publication Citation for published version (APA): de Groot, M. (2011). Innovative therapies
Psoriasis: Causes, Symptoms, And Treatment
 Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
Psoriasis: Causes, Symptoms, And Treatment We all know that a healthy immune system is good. But, do you know that an overactive immune system can cause certain conditions like Psoriasis? Read on to find
An otherwise healthy 12-year-old
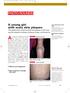 1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
1105 Photo Rounds.finalREV 10/19/05 2:05 PM Page 947 A young girl with scaly skin plaques The patient had numerous thick red plaques on her back and the extensor surfaces of elbows, knees, and forearms
CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION
 CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION IXEKIZUMAB (Taltz Eli Lilly Canada Inc.) Indication: Moderate to Severe Plaque Psoriasis Recommendation: The CADTH Canadian Drug Expert Committee
CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION IXEKIZUMAB (Taltz Eli Lilly Canada Inc.) Indication: Moderate to Severe Plaque Psoriasis Recommendation: The CADTH Canadian Drug Expert Committee
Clinical Efficacy and Safety of Naltrexone Combination Therapy in Older Patients with Severe Pruritus
 pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 2, 2016 http://dx.doi.org/10.5021/ad.2016.28.2.159 ORIGINAL ARTICLE Clinical Efficacy and Safety of Naltrexone Combination Therapy in Older Patients
pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 2, 2016 http://dx.doi.org/10.5021/ad.2016.28.2.159 ORIGINAL ARTICLE Clinical Efficacy and Safety of Naltrexone Combination Therapy in Older Patients
atorvastatin 10mg, amlodipine 5mg and dilitazem 60mg. He had unexplained iron deficiency anaemia (hemoglobin-8.4gm/dl, ferritin- 4.73ng/ml, total iron
 Pemphigus herpetiformis : A rare clinical variant of pemphigus Shrestha P 1, Tajhya RB 2, Pokharel A 3 1,2 Consultant Dermatologist, Department of Dermatology, Vayodha Hospital Pvt. Ltd, Balkhu, Kathmandu,
Pemphigus herpetiformis : A rare clinical variant of pemphigus Shrestha P 1, Tajhya RB 2, Pokharel A 3 1,2 Consultant Dermatologist, Department of Dermatology, Vayodha Hospital Pvt. Ltd, Balkhu, Kathmandu,
Cutaneous manifestations and systemic correlation in patients with lupus erythematosus and its subsets: a study of 40 cases
 International Journal of Research in Dermatology Mahajan R et al. Int J Res Dermatol. 2018 Nov;4(4):479-483 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183407
International Journal of Research in Dermatology Mahajan R et al. Int J Res Dermatol. 2018 Nov;4(4):479-483 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183407
Clinical Policy: Ixekizumab (Taltz) Reference Number: CP.PHAR.257 Effective Date: Last Review Date: 05.18
 Clinical Policy: (Taltz) Reference Number: CP.PHAR.257 Effective Date: 08.01.16 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Taltz) Reference Number: CP.PHAR.257 Effective Date: 08.01.16 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Chronic Granulomatous Disease Managing GI Issues
 Chronic Granulomatous Disease Managing GI Issues N I C H O L A S H A R T O G, M D D i r e c t o r o f P e d i a t r i c / A d u l t P r i m a r y I m m u n o d e f i c i e n c y C l i n i c A s s i s t
Chronic Granulomatous Disease Managing GI Issues N I C H O L A S H A R T O G, M D D i r e c t o r o f P e d i a t r i c / A d u l t P r i m a r y I m m u n o d e f i c i e n c y C l i n i c A s s i s t
KEY MESSAGES. Psoriasis patients are more prone to cardiovascular diseases, stroke, lymphoma and non-melanoma skin cancers, and increased mortality.
 KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
KEY MESSAGES Psoriasis is a genetically determined, systemic immune-mediated chronic inflammatory disease that affects primarily the skin and joints. Psoriasis Vulgaris is characterised by well-demarcated
Everant.in/index.php/jmpr. Journal of Medical Practice and Review
 Everant.in/index.php/jmpr Journal of Medical Practice and Review Real world Efficacy and Tolerance of Bepotastine, a new 2 nd generation antihistamine, in Pruritis and other symptoms associated with cutaneous
Everant.in/index.php/jmpr Journal of Medical Practice and Review Real world Efficacy and Tolerance of Bepotastine, a new 2 nd generation antihistamine, in Pruritis and other symptoms associated with cutaneous
Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis
 Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis T. Shehzad ( Departments of Dermatology Naval Hospital PNS Shifa, Karachi. ) N. R. Dar ( Departments
Efficacy of Concomitant Use of PUVA and Methotrexate in Disease Clearance Time in Plaque Type Psoriasis T. Shehzad ( Departments of Dermatology Naval Hospital PNS Shifa, Karachi. ) N. R. Dar ( Departments
Sarcoidosis Case. Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA. WASOG: educational material
 Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Sarcoidosis Case Robert P. Baughman Interstitial Lung Disease and Sarcoidosis Clinic University of Cincinnati, USA WASOG: educational material Sarcoidosis Case patient is a Caucasian male age 46 was diagnosed
Supplementary Figure 1 IMQ-Induced Mouse Model of Psoriasis. IMQ cream was
 Supplementary Figure 1 IMQ-Induced Mouse Model of Psoriasis. IMQ cream was painted on the shaved back skin of CBL/J and BALB/c mice for consecutive days. (a, b) Phenotypic presentation of mouse back skin
Supplementary Figure 1 IMQ-Induced Mouse Model of Psoriasis. IMQ cream was painted on the shaved back skin of CBL/J and BALB/c mice for consecutive days. (a, b) Phenotypic presentation of mouse back skin
2.0 Synopsis. Adalimumab R&D/04/118. (For National Authority Use Only) Referring to Part of Dossier: Volume:
 2.0 Synopsis Abbott Laboratories Name of Study Drug: Adalimumab Name of Active Ingredient: Adalimumab Title of Study: Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority
2.0 Synopsis Abbott Laboratories Name of Study Drug: Adalimumab Name of Active Ingredient: Adalimumab Title of Study: Individual Study Table Referring to Part of Dossier: Volume: Page: (For National Authority
Technology appraisal guidance Published: 12 July 2017 nice.org.uk/guidance/ta455
 Adalimumab, etanercept and ustekinumab for treating plaque psoriasis in children and young people Technology appraisal guidance Published: 12 July 2017 nice.org.uk/guidance/ta455 NICE 2017. All rights
Adalimumab, etanercept and ustekinumab for treating plaque psoriasis in children and young people Technology appraisal guidance Published: 12 July 2017 nice.org.uk/guidance/ta455 NICE 2017. All rights
What is Cosentyx (secukinumab)?
 What is Cosentyx (secukinumab)? Cosentyx is the first of a new class of medicines called interleukin- 17A (IL- 17A) inhibitors to be approved for the treatment of moderate- to- severe plaque psoriasis,
What is Cosentyx (secukinumab)? Cosentyx is the first of a new class of medicines called interleukin- 17A (IL- 17A) inhibitors to be approved for the treatment of moderate- to- severe plaque psoriasis,
Clinical Policy: Ixekizumab (Taltz) Reference Number: ERX.SPA.122 Effective Date:
 Clinical Policy: (Taltz) Reference Number: ERX.SPA.122 Effective Date: 10.01.16 Last Review Date: 11.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Taltz) Reference Number: ERX.SPA.122 Effective Date: 10.01.16 Last Review Date: 11.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Certolizumab pegol (Cimzia) for chronic plaque psoriasis in adults
 NIHR Innovation Observatory Evidence Briefing: April 2017 Certolizumab pegol (Cimzia) for chronic plaque psoriasis in adults NIHRIO (HSRIC) ID: 2406 NICE ID: 9112 LAY SUMMARY Plaque psoriasis is the most
NIHR Innovation Observatory Evidence Briefing: April 2017 Certolizumab pegol (Cimzia) for chronic plaque psoriasis in adults NIHRIO (HSRIC) ID: 2406 NICE ID: 9112 LAY SUMMARY Plaque psoriasis is the most
Horizon Scanning Centre March Tildrakizumab for moderate to severe plaque psoriasis SUMMARY NIHR HSC ID: 6798
 Horizon Scanning Centre March 2015 Tildrakizumab for moderate to severe plaque psoriasis SUMMARY NIHR HSC ID: 6798 This briefing is based on information available at the time of research and a limited
Horizon Scanning Centre March 2015 Tildrakizumab for moderate to severe plaque psoriasis SUMMARY NIHR HSC ID: 6798 This briefing is based on information available at the time of research and a limited
This questionnaire was used both during the face-to-face interviews with the
 Additional file 1: Primary research questionnaire This questionnaire was used both during the face-to-face interviews with the dermatologists and during the expert panel 1. During the last month, how many
Additional file 1: Primary research questionnaire This questionnaire was used both during the face-to-face interviews with the dermatologists and during the expert panel 1. During the last month, how many
S003 CPC Self-Assessment
 S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
S003 CPC Self-Assessment Alina G. Bridges, D.O. Associate Professor Program Director, Dermatopathology Fellowship Department of Dermatology, Division of Dermatopathology and Cutaneous Immunopathology Mayo
Case presentation. Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally.
 Case presentation Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally. Name : XXX Age : 33 years Sex : Female Occupation : Farmer IP no : 201608905 DOA : 15-02-2016
Case presentation Dr Rammohan Reddy 1 st year PG, Dept of DVL, Kamineni Institute of Medical Sciences, Narketpally. Name : XXX Age : 33 years Sex : Female Occupation : Farmer IP no : 201608905 DOA : 15-02-2016
Clinical Policy: Apremilast (Otezla) Reference Number: CP.PHAR.245 Effective Date: Last Review Date: Line of Business: HIM, Medicaid
 Clinical Policy: (Otezla) Reference Number: CP.PHAR.245 Effective Date: 08.16 Last Review Date: 11.18 Line of Business: HIM, Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Otezla) Reference Number: CP.PHAR.245 Effective Date: 08.16 Last Review Date: 11.18 Line of Business: HIM, Medicaid Revision Log See Important Reminder at the end of this policy for important
Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination
 CASE SERIES DERMATOLOGY // INTERNAL MEDICINE Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination Anca Chiriac 1,2,3, Piotr Brzezinski 4, Cristian
CASE SERIES DERMATOLOGY // INTERNAL MEDICINE Tinea Incognito Incorrect Initial Diagnosis. Case Series Presentation with Emphasis on the Mycological Examination Anca Chiriac 1,2,3, Piotr Brzezinski 4, Cristian
Actinic keratosis (AK): Dr Sarma s simple guide
 Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Actinic keratosis (AK): Dr Sarma s simple guide Actinic keratosis is a very common lesion that you will see in your day-to-day practice. First, let me explain the name Actinic keratosis. It means keratosis
Low Dose Naltrexone (LDN) as Cancer Therapy. LDN Research Trust Conference Las Vegas, NV Nov 2014 Akbar Khan, M.D.
 Low Dose Naltrexone (LDN) as Cancer Therapy LDN Research Trust Conference www.ldnresearchtrust.org Las Vegas, NV Nov 2014 Akbar Khan, M.D. Disclosure The presenter is the Medical Director of Medicor Cancer
Low Dose Naltrexone (LDN) as Cancer Therapy LDN Research Trust Conference www.ldnresearchtrust.org Las Vegas, NV Nov 2014 Akbar Khan, M.D. Disclosure The presenter is the Medical Director of Medicor Cancer
Clinical Policy: Apremilast (Otezla) Reference Number: CP.PHAR.245 Effective Date: 08/16 Last Review Date 08/17
 Clinical Policy: (Otezla) Reference Number: CP.PHAR.245 Effective Date: 08/16 Last Review Date 08/17 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Otezla) Reference Number: CP.PHAR.245 Effective Date: 08/16 Last Review Date 08/17 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital
 Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Dr. Venkateswari. R. Dr. Janani Sankar s unit Kanchi Kamakoti CHILDS Trust Hospital Acknowledgements: KKCTH Dr. Ramkumar Consultant Dermatologist Dr. Ramprakash Consultant Ophthalmologist Dr. Prasad Manne
Clinical Policy: Brodalumab (Siliq) Reference Number: CP.PHAR.375 Effective Date: Last Review Date: 05.18
 Clinical Policy: (Siliq) Reference Number: CP.PHAR.375 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Siliq) Reference Number: CP.PHAR.375 Effective Date: 06.01.18 Last Review Date: 05.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Grover s disease: A case report.
 320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
320 Case report Thai J Dermatol, October-December 2011 ABSTRACT: Grover s disease: A case report. Supicha Chavanich MD, Praneet Sajjachareonpong MD. CHAVANICH C, SAJJACHAREONPONG P. GROVER S DISEASE: A
Assessing and Treating the Patient with Chronic Itch
 Assessing and Treating the Patient with Chronic Itch Sonja Ständer, MD sonja.stander@uni-muenster.de Center for Chronic Pruritus Department of Dermatology University Hospital of Muenster Germany Acute
Assessing and Treating the Patient with Chronic Itch Sonja Ständer, MD sonja.stander@uni-muenster.de Center for Chronic Pruritus Department of Dermatology University Hospital of Muenster Germany Acute
Combination Nonbiologic Therapy in Psoriasis. Sushil Tahiliani, MBBS, MD
 Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
Combination Nonbiologic Therapy in Psoriasis Sushil Tahiliani, MBBS, MD Agenda Rationale Preferred and less preferred combination Morphology-specific preferred combinations Doses used in combinations Potential
Clinical Policy: Secukinumab (Cosentyx) Reference Number: ERX.SPA.165 Effective Date:
 Clinical Policy: (Cosentyx) Reference Number: ERX.SPA.165 Effective Date: 10.01.16 Last Review Date: 11.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Cosentyx) Reference Number: ERX.SPA.165 Effective Date: 10.01.16 Last Review Date: 11.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Scottish Medicines Consortium
 Scottish Medicines Consortium ustekinumab, 45mg solution for injection (Stelara ) No. (572/09) Janssen-Cilag Ltd 15 January 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of
Scottish Medicines Consortium ustekinumab, 45mg solution for injection (Stelara ) No. (572/09) Janssen-Cilag Ltd 15 January 2010 The Scottish Medicines Consortium (SMC) has completed its assessment of
Urticarial Dermatitis: Clinical Characteristics of Itch and Therapeutic Response to Cyclosporine
 Itch and Cyclosporine in Urticarial Dermatitis pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 29, No. 2, 2017 https://doi.org/10.5021/ad.2017.29.2.143 ORIGINAL ARTICLE Urticarial Dermatitis: Clinical
Itch and Cyclosporine in Urticarial Dermatitis pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 29, No. 2, 2017 https://doi.org/10.5021/ad.2017.29.2.143 ORIGINAL ARTICLE Urticarial Dermatitis: Clinical
TCIs are only available on prescription and are usually started by a dermatology specialist.
 (TCIs) What are topical calcineurin inhibitors? Topical calcineurin inhibitors are treatments that alter the immune system and have been developed for controlling eczema. There are two types available:
(TCIs) What are topical calcineurin inhibitors? Topical calcineurin inhibitors are treatments that alter the immune system and have been developed for controlling eczema. There are two types available:
Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis
 Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Original Article Comparative efficacy of topical mometasone furoate 0.1% cream vs topical tacrolimus 0.03% ointment in the treatment of atopic dermatitis Md Alauddin Khan *, Lubna Khondker **, Dilshad
Ustekinumab (Stelara )
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Case Presentation Guidelines
 http://depts.washington.edu/medclerk/student/presentation.htmloral Case Presentation Guidelines Steve McGee, M.D. The Oral Case Presentation is an art form that requires concerted effort and repeated practice.
http://depts.washington.edu/medclerk/student/presentation.htmloral Case Presentation Guidelines Steve McGee, M.D. The Oral Case Presentation is an art form that requires concerted effort and repeated practice.
Announcing HUMIRA. Psoriasis Starter Package
 Announcing HUMIRA (adalimumab) Psoriasis Starter Package HUMIRA is indicated for the treatment of adult patients with moderate to severe chronic plaque psoriasis who are candidates for systemic therapy
Announcing HUMIRA (adalimumab) Psoriasis Starter Package HUMIRA is indicated for the treatment of adult patients with moderate to severe chronic plaque psoriasis who are candidates for systemic therapy
Assessing the Current Treatment of Atopic Dermatitis: Unmet Needs
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
A case of bullous pemphigoid following pemphigus foliaceus
 #2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
#2228 A case of bullous pemphigoid following pemphigus foliaceus Priyanka Vedak MD 1, Danielle Levine MD 1,3, Lyn Duncan MD 2,3, Hensin Tsao 1,3, Daniela Kroshinsky MD MPH 1,3 1. Department of Dermatology,
Clinical Policy: Secukinumab (Cosentyx) Reference Number: CP.PHAR.261 Effective Date: 08/16 Last Review Date: 08/17
 Clinical Policy: (Cosentyx) Reference Number: CP.PHAR.261 Effective Date: 08/16 Last Review Date: 08/17 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Cosentyx) Reference Number: CP.PHAR.261 Effective Date: 08/16 Last Review Date: 08/17 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Use of abatacept in rheumatoid arthritis - patient information
 Practical management of patients receiving abatacept 1 Use of abatacept in rheumatoid arthritis - patient information Evidence-based Medicine Official Recommendations Expert opinion Key points 1. Abatacept
Practical management of patients receiving abatacept 1 Use of abatacept in rheumatoid arthritis - patient information Evidence-based Medicine Official Recommendations Expert opinion Key points 1. Abatacept
Crusted Scabies: A great mimicker of Chronic Plaque Psoriasis
 International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Case Report Volume 4, Issue 1-2018 Crusted Scabies: A great mimicker
International Journal of Current Research in Medical Sciences ISSN: 2454-5716 P-ISJN: A4372-3064, E -ISJN: A4372-3061 www.ijcrims.com Case Report Volume 4, Issue 1-2018 Crusted Scabies: A great mimicker
D E R M A T O L O G Y
 We customize individual prescriptions for the specific needs of our patients. F E B R U A R Y 2 0 1 3 I N S I D E T H I S I S S U E : Psoriasis Vulgaris 2 Atopic Dermatitis 3 P R E S C R I P T I O N C
We customize individual prescriptions for the specific needs of our patients. F E B R U A R Y 2 0 1 3 I N S I D E T H I S I S S U E : Psoriasis Vulgaris 2 Atopic Dermatitis 3 P R E S C R I P T I O N C
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 13, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 13, 2009 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
Clinical Trial Report Synopsis
 Clinical Trial Report Synopsis A phase 2a, proof of concept trial, testing twice daily application of LEO 124249 ointment 30 mg/g in the treatment of mild to moderate inverse psoriasis Design of trial:
Clinical Trial Report Synopsis A phase 2a, proof of concept trial, testing twice daily application of LEO 124249 ointment 30 mg/g in the treatment of mild to moderate inverse psoriasis Design of trial:
Clinical Policy: Ixekizumab (Taltz) Reference Number: CP.PHAR.257 Effective Date: Last Review Date: 11.18
 Clinical Policy: (Taltz) Reference Number: CP.PHAR.257 Effective Date: 08.01.16 Last Review Date: 11.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Clinical Policy: (Taltz) Reference Number: CP.PHAR.257 Effective Date: 08.01.16 Last Review Date: 11.18 Line of Business: Medicaid Revision Log See Important Reminder at the end of this policy for important
Allergic versus Contact
 Allergic versus Contact Dermatitis Julie Sterbank, DO Assistant Clinical Professor Allergy/Immunology MetroHealth Medical Center/Case Western Reserve University Disclosure I have no financial disclosures
Allergic versus Contact Dermatitis Julie Sterbank, DO Assistant Clinical Professor Allergy/Immunology MetroHealth Medical Center/Case Western Reserve University Disclosure I have no financial disclosures
1.1. Lenalidomide and (aggravation of) psoriasis
 20-4-2012 1.1. Lenalidomide and (aggravation of) psoriasis Introduction Lenalidomide (Revlimid ), was registered on the Dutch market in June 2007 and is indicated for the treatment of multiple myeloma
20-4-2012 1.1. Lenalidomide and (aggravation of) psoriasis Introduction Lenalidomide (Revlimid ), was registered on the Dutch market in June 2007 and is indicated for the treatment of multiple myeloma
Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
 International Journal of Clinical Rheumatology For reprint orders, please contact: reprints@futuremedicine.com Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
International Journal of Clinical Rheumatology For reprint orders, please contact: reprints@futuremedicine.com Adrenocorticotropic hormone gel in patients with refractory rheumatoid arthritis: a case series
Ustekinumab is used to treat moderate to severe plaque psoriasis in adults. Why have I been selected for treatment with ustekinumab?
 USTEKINUMAB What are the aims of this leaflet? This leaflet has been written to help you understand more about ustekinumab (Stelara TM ). It tells you what it is, how it works, how it is used to treat
USTEKINUMAB What are the aims of this leaflet? This leaflet has been written to help you understand more about ustekinumab (Stelara TM ). It tells you what it is, how it works, how it is used to treat
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB. Friday, February 12, :30 am 11:00 am
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSION PATHOLOGY OF THE SKIN LAB Friday, February 12, 2012 9:30 am 11:00 am FACULTY COPY GOALS: Describe the basic clinical and morphologic features of various
