CASE #1 CASE #1 DISCLOSURES. Arthritis, Osteomyelitis, and Prosthetic Joint Infections
|
|
|
- Mervin Chapman
- 6 years ago
- Views:
Transcription
1 Arthritis, Osteomyelitis, and Prosthetic Joint Infections Speaker Associate Dean for Medical Education The Warren Alpert Medical School of Brown University C Off-Label Usage DISCLOSURES Financial Relationships with Relevant Commercial Interests None Resolution CASE #1 This presentation was originally presented at the 2012 course. Minor edits have been made to this version of the presentation. The version in the audio recordings section was not edited. 21-year-old female injection drug user and no significant PMH presents with fever and rightsided chest pain. On exam, she is febrile to 102 o F. She has a 2/6 systolic murmur that increases on inspiration, and swelling and tenderness over right sternoclavicular joint. Rest of examination is the normal. Aspiration of the sternoclavicular joint reveals a small amount of purulent material. TEE shows a vegetation on the tricuspid valve. CASE #1 Pending culture results from blood and joint fluid, which of the following empiric antimicrobial regimens should be initiated? A. Daptomycin + caspofungin B. Nafcillin + gentamicin C. Clindamycin + trimethoprimsulfamethoxazole D. Vancomycin + cefepime E. Cefepime + gentamicin EPIDEMIOLOGY OF BACTERIAL ARTHRITIS 2-10 cases/100,000/year cases/100,000/year in those with rheumatoid arthritis Published mortality 7-15% Morbidity up to 50% Usually hematogenously acquired; other routes are direct inoculation or contiguous spread (c) 2013 Infectious Disease Board Review Course 1
2 MICROBIOLOGY OF NONGONOC0CCAL SEPTIC ARTHRITIS EPIDEMIOLOGY/ETIOLOGY OF NONGONOCOCCAL ARTHRITIS Microorganism Frequency (%) S. aureus Coag-negative staph 4 Streptococci 22 Gram-negatives 5-20 Culture-negative Polymicrobial 8 Feature Etiologic Agent(s) Rheumatoid arthritis S. aureus (~75%) Injection drug use S. aureus, P. aeruginosa Diabetes, malignancy S. aureus, group B streptococci Immunocompromised S. aureus, strep, gram-negatives, Listeria monocytogenes Fibrocartilagenous joints S. aureus, P. aeruginosa CASE #2 CASE #2 45-year-old man vacationing in Spain presents with fever, malaise, anorexia and left lower back pain; about 3 weeks earlier, he ingested unpasteurized milk while visiting a local farm On exam, temperature is 101 o F. He has tenderness over the left sacroiliac joint; the pain is accentuated with flexion and external rotation of the hip Radiographs reveal blurring of the articular margins of the left sacroiliac joint and widening of the sacroiliac space Which of the following is the most likely etiology of this patient s sacroiliitis? A. Brucella melitensis B. Mycobacterium bovis C. Bacillus arthracis D. Coxiella burnetii E. Ankylosing spondylitis EPIDEMIOLOGY/ETIOLOGY OF NONGONOCOCCAL ARTHRITIS EPIDEMIOLOGY/ETIOLOGY OF NONGONOCOCCAL ARTHRITIS Feature Cat/dog bite Human bite Rat bite Etiologic Agent(s) Pasteurella multocida, anaerobes Capnocytophaga sp. Eikenella, anaerobes, oral flora Streptobacillus moniliformis Feature Postpartum women Hypogammaglobulemia Arthroscopy Etiologic Agent(s) Mycoplasma hominis Mycoplasma sp. S. aureus, coag-neg staph, Clostridium sp., gram-negative bacilli Ingestions (goat cheese, unpasteurized milk); occupation Living/travel SE Asia Brucella sp. Burkholderia pseudomallei, Streptococcus suis Reconstructive surgery (tissue allograft) Multiple purpuric lesions Clostridium sp. Neisseria meningitidis (c) 2013 Infectious Disease Board Review Course 2
3 CLINICAL FEATURES OF NONGONOCOCCAL ARTHRITIS Monoarticular in 80-90%; knee in 50% Pain and loss of function (>90%); swelling, redness, increased warmth Fever in 60-80% Focal joint tenderness, inflammation, effusion, limited and painful motion Symptoms and signs more subtle in the immunocompromised or those with RA DIAGNOSIS OF NONGONOCOCCAL ARTHRITIS Arthrocentesis reveals purulent (>50,000 WBC/mm 3 ), low viscosity fluid with increased neutrophils (>75%) Gram stain positive in up to 50%; depends on microorganism Synovial fluid cultures positive in 80-90% Blood cultures positive in 50-70% EPIDEMIOLOGY OF DISSEMINATED GONOCOCCAL INFECTION (DGI) Sexually active adolescents and adults (<30 years of age) DGI produces two syndromes (may overlap) Gonococcal arthritis Tenosynovitis, dermatitis, polyarthralgia without purulent joint infection Less than half of the patients have a true septic arthritis 4 times more common in women Complicates 0.5-3% of cases of mucosal GC infection PATHOGENESIS OF DGI Occult bacteremia secondary to mucosal infection of urethra, cervix, rectum, oropharynx DGI most likely results from asymptomatic mucosal infection; risk increases during menstruation, pregnancy, postpartum period Host factors terminal complement deficiencies (C5-C8), systemic lupus erythematosus CLINICAL FEATURES OF DGI DIAGNOSIS OF DGI AND GONOCOCCAL ARTHRITIS Dermatitis (2/3 of patients) painless, nonpruritic, few in number macules, papules, and pustules on an erythematous base) Tenosynovitis (2/3 of patients) usually in fingers, hands, wrists occurs simultaneously with rash Migratory polyarthralgia or polyarthritis asymmetric, severe joint symptoms Gonococcal arthritis Synovial fluid WBC ,000/mm 3 (neutrophils) Synovial fluid Gram stain positive in 25% Synovial fluid culture positive in 50% DGI without suppurative arthritis Synovial fluid WBC count lower Synovial fluid cultures positive in 20-30% Synovial fluid PCR sensitivity of 80% (c) 2013 Infectious Disease Board Review Course 3
4 DIAGNOSIS OF DGI AND GONOCOCCAL ARTHRITIS EMPIRIC ANTIMICROBIAL THERAPY OF BACTERIAL ARTHRITIS Positive blood cultures in <30% Culture yield of mucosal sites Cervical swabs positive in 80-90% of women Urethral swabs positive in 50-70% of men Lower yields from rectal and oropharyngeal swabs, but may be positive Risk Factor / Gram Stain Joint disease / GPC Young & sexually active / GNC GNR Negative Gram stain Therapy Vancomycin (pending in vitro susceptibility) Ceftriaxone Ceftazidime, cefepime, pip/tazo, carbapenem Vancomycin + either ceftazidime, cefepime, or a fluoroquinolone JOINT DRAINAGE FOR BACTERIAL ARTHRITIS Gonococcal arthritis not required Repeated needle aspiration First 5-7 days until purulence is minimal Arthroscopy Irrigation, lysis of adhesions, removal of purulent material Effective for knee, shoulder, ankle Open surgical drainage Hip joints Poor response to therapy Aspiration or arthroscopy impractical DURATION OF ANTIMICROBIAL THERAPY FOR BACTERIAL ARTHRITIS IV therapy for 2-4 weeks 7-10 days for gonococcal arthritis 4 weeks generally for S. aureus (including MRSA) and gram-negative bacilli If gram-negative organism is sensitive to fluoroquinolones, oral therapy used in latter half of treatment course CASE #3 CASE #3 30-year-old woman presents with acute onset of bilateral hand pain Married and monogamous; 4-year-old son with recent fever and rash; 2 cats, dog, parrot, snake, and rabbit; traveled to India 2 years ago Febrile to 39 o C, bilateral pain and swelling in PIP and MCP joints WBC count is 3,500/mm 3 Which of the following is the most likely etiology of the patient s illness? A. Bartonella henselae B. Parvovirus B19 C. Chikungunya virus D. Salmonella enteritidis E. Pasteurella multocida (c) 2013 Infectious Disease Board Review Course 4
5 VIRAL ARTHRITIS VIRAL ARTHRITIS Agent Percent of Cases Features Rubella 51-61% No prior vaccination Symmetric polyarthritis Parvovirus B19 60% of adult cases Unusual in children Sudden, severe polyarthritis Small joints May mimic RA Hepatitis A 10-14% Associated rash Hepatitis B 10-25% Severe, sudden onset symmetric polyarthritis in hands and knees Resolves during preicteric phase Hepatitis C 9-19% Controversial whether associated with inflammatory arthritis Agent Features HIV 8% of cases Usually monoarticular HTLV-1 Chronic joint infection resembling RA Arthropod-borne alpha viruses May occur in epidemics Rash may be present Spontaneous resolution Chikungunya virus Islands of Indian Ocean and South Asia Acute illness with joint symptoms involving wrists, ankles, small joints of hands and feet After 5-7 days of fever and brief improvement, polyarthritis (± tenosynovitis) that may recur and last weeks to months (rarely years) REACTIVE ARTHRITIS REACTIVE ARTHRITIS Onset of inflammatory arthritis after an infection elsewhere in the body Enthesitis (Achilles tendonitis/plantar fasciitis) Microorganisms not cultured from synovial fluid Begins several weeks after antecedent infection Asymmetric oligoarticular arthritis Treatment is anti-inflammatory agents; role of antimicrobial therapy is controversial Chlamydia trachomatis Shigella flexneri Salmonella enteritidis Salmonella typhimurium Yersinia enterocolitica Yersinia pseudotuberculosis Campylobacter jejuni REACTIVE ARTHRITIS WITH EXTRA- ARTICULAR FEATURES Urethritis Conjunctivitis (bilateral and painful) Uveitis (unilateral and painless) Keratoderma blennorrhagium Circinate balantitis/vulvitis Lingual or oral ulcerations (painless) Nail dystrophy CASE #4 80-year-old male with diabetes underwent right TKA 3 months ago for severe osteoarthritis presents with constant pain and swelling of his right knee. On exam, he is afebrile with normal vital signs. His right knee is painful, swollen, and there is decreased range of motion. (c) 2013 Infectious Disease Board Review Course 5
6 CASE #4 Which of the following is the best test for establishing that this patient has a prosthetic joint infection? A. Radiograph of right knee B. Technitium bone scan C. Indium-labeled leukocyte scan D. Fluorodeoxyglucose PET Scan E. Aspiration and culture of joint fluid EPIDEMIOLOGY OF PROSTHETIC JOINT 1-3% of indwelling prostheses become infected Predisposing factors include prior surgery at prosthesis site, RA, immunocompromised state, diabetes, poor nutritional state, obesity, psoriasis, extremely advanced age Infection may be locally introduced or hematogenous (20-40% of cases) Any factor that delays wound healing increases risk of infection ETIOLOGY OF PROSTHETIC JOINT Microorganism Frequency (%) Coag-negative staph S. aureus Streptococci 9-10 Enterococci 3-7 Gram-negative bacilli 5-25 Anaerobes 2-10 Mixed flora Culture-negative 7-11 CLINICAL FEATURES OF PROSTHETIC JOINT Early Less than 3 months after surgery Virulent organisms (S. aureus, gram-negative bacilli) Coagulase-negative staphylococci, streptococci Delayed 3-12 months after surgery Caused by less virulent organisms (coagulasenegative staph, P. acnes), but may also be S. aureus Late More than 12 months, including hematogenous seeding Staphylococci (S. aureus and coag-negative), other skin commensals, gram-negative bacilli, anaerobes CLINICAL FEATURES OF PROSTHETIC JOINT Most patients present with long, indolent course with progressive increase in joint pain Joint pain (95%) Fever (43%) Periarticular swelling (38%) Wound or cutaneous sinus drainage (32%) Presentation depends on virulence of causative microorganism DIAGNOSIS OF PROSTHETIC JOINT Need to differentiate infection from aseptic or mechanical problems Infection constant pain Mechanical pain with motion or weight-bearing Plain radiographs (findings in 50% of cases) Abnormal lucencies at bone-cement interface Changes in position of prosthesis components Cement fractures Periosteal reaction Motion of components on stress views (c) 2013 Infectious Disease Board Review Course 6
7 DIAGNOSIS OF PROSTHETIC JOINT DIAGNOSIS OF PROSTHETIC JOINT Radioisotope scans Increased technitium uptake seen around normal prostheses for 6 months after arthroplasty; positive scans after 6 months are abnormal, but do not necessarily indicate infection Sequential gallium scanning is nondiagnostic because of unacceptable sensitivity and specificity Indium-labeled leukocyte scanning in inconsistently sensitive and provides only nonspecific results FDG-PET has reported low specificity (55%); more recently, 90% for hip and 75% for knee Isolation of pathogen by aspiration of joint fluid Gram stain positive in 32% Culture sensitivity 86-92% Culture specificity 82-97% Culture of tissue at arthrotomy Optimally obtain 5-6 specimens of tissue and fluid 3 positive cultures 94.8% probability of infection No positive cultures 3.4% probability of infection MANAGEMENT OF PROSTHETIC JOINT (2-STAGE) Removal of prosthesis and cement Use of methylmethacrylate cement spacer impregnated with antimicrobial agent (no controlled trials but commonly practiced) 4-6 weeks of bactericidal antimicrobial therapy Re-implantation at conclusion of antimicrobial therapy (?antimicrobial free period) Success 90-96% in hip replacement infections Success 97% in knee replacement infections MANAGEMENT OF PROSTHETIC JOINT Extraction with re-implantation after only 2 weeks of antimicrobial therapy, followed by additional 4 weeks of antimicrobial therapy (pathogen eradication in 79%; good function in 35%) Extraction of metallic joint and cement with immediate re-implantation of new prosthesis with antibiotic-loaded cement in 1-step procedure and antimicrobial therapy (success 70-83%) One-step procedure with infections caused by less virulent organisms and satisfactory condition of soft tissue (success %) MANAGEMENT OF PROSTHETIC JOINT Simple surgical drainage with prosthesis retention and antimicrobials (success 14-68%) Debridement with retention is reasonable, as follows: Those with early postoperative or acute hematogenous infection Clinical symptoms and signs <3 weeks (<1 week?) Stable implant Soft tissue in good condition; no sinus tract Treat with effective agent for 3 months for infected hip prosthesis and 6 months for infected knee prosthesis Success % for staph and 89% for strep CASE #5 16-year old male steps on a nail which punctures his sneaker and enters his heel. Sees his physician who administers a tetanus booster and prescribes a 5-day course of amoxicillin/clavulanate Three weeks later has pain and purulent drainage from his right heel. On exam, T 100 o F and purulent drainage from sinus track of right heel Cultures of drainage reveal S. aureus, E. coli, and E. faecalis (c) 2013 Infectious Disease Board Review Course 7
8 CASE #5 After appropriate bone cultures are obtained, which of the following antimicrobial regimens should be initiated? A. Vancomycin + ceftriaxone B. Vancomycin + metronidazole + ceftriaxone C. Ampicillin/sulbactam + gentamicin D. Vancomycin + piperacillin/tazobactam E. Clindamycin + trimethoprimsulfamethoxazole EPIDEMIOLOGY AND ETIOLOGY OF CONTIGUOUS OSTEOMYELITIS EPIDEMIOLOGY AND ETIOLOGY OF HEMATOGENOUS OSTEOMYELITIS Risk Factor Presence of foreign body Puncture injury to foot Malignant external otitis Periodontal infection Soil contamination Microorganism(s) Coag-neg staph, S. aureus P. aeruginosa P. aeruginosa Oral flora, Actinomyces S. aureus, Clostridium, Enterobacteriaceae, Bacillus, Nocardia, atypical mycobacteria Risk Factor Microorganism (s) Sickle cell disease Salmonella, S. aureus, S. pneumoniae IDU, hemodialysis S. aureus, P. aeruginosa Immunocompromised (including Aspergillus, Candida, atypical mycobacteria, HIV) Bartonella henselae GENERAL CONSIDERATIONS AND APPROACH TO OSTEOMYELITIS Pathogenesis may be hematogenous (monomicrobial), contiguous to a soft tissue infection (polymicrobial), or direct inoculation from surgery or trauma Conventional radiographs are inexpensive, with abnormalities seen in days Nuclear bone scans are sensitive, but expensive and sometimes nonspecific MRI and CT are now considered standard of care, and are sensitive and specific in diagnosis DIAGNOSTIC TESTS FOR OSTEOMYELITIS Test Sen Spec PPV NPV 3-phase bone scan 95% 33% 53% 90% Gallium scan 81% 69% 71% 80% Indium WBC scan 88% 85% 86% 87% MRI 95% 88% 93% 92% (c) 2013 Infectious Disease Board Review Course 8
9 GENERAL CONSIDERATIONS AND APPROACH TO OSTEOMYELITIS Identification of causative microorganism is crucial to optimize medical therapy; if possible, withhold therapy until adequate cultures obtained Swab cultures from draining wounds and sinus tracts may be of value Infection control for resistant microorganisms Isolation of S. aureus correlates with deep infection Most infections require combined medical and surgical therapy for success Optimal duration of therapy is unknown (4-6 wks) CASE #6 65-year-old man presented with hematuria; cystoscopy revealed a superficial transitional cell carcinoma of the bladder Treated with intravesicular therapy with successful resolution 2 months after completing therapy, presented with low-grade fever and moderate low back pain CASE #6 Which of the following is the most likely etiology of his vertebral lesions? A. Enterococcus faecium B. Pseudomonas aeruginosa C. Mycobacterium bovis D. Candida glabrata E. Metastatic bladder cancer VERTEBRAL OSTEOMYELITIS AND SPONDYLODISKITIS VERTEBRAL OSTEOMYELITIS AND SPONDYLODISKITIS Hematogenous in most cases Clinical features Localized insidious pain and tenderness (90%) Fever (<50%) Etiology S. aureus and coag-neg staph most common Gram-negative bacilli and Candida in injection drug users, immunosuppressed, postoperative Consider Mycobacteria and Brucella in appropriate clinical setting Diagnosis MRI is gold standard; best for detecting disk space infection (98% sensitivity, 93% specificity) Blood cultures CT-guided percutaneous biopsy and aspiration off antibiotics (sensitivity 50%); repeat or do open biopsy if inconclusive (c) 2013 Infectious Disease Board Review Course 9
10 VERTEBRAL OSTEOMYELITIS AND SPONDYLODISKITIS Management Stabilize spine; surgery usually not needed Antimicrobial therapy (6-8 weeks or longer) If hardware present with early postop infection, debridement + long-term antimicrobial therapy (until evidence of bone vertebral fusion) If hardware present with late postop infection, remove hardware + antimicrobial therapy Follow-up ESR/CRP OSTEOMYELITIS IN PATIENTS WITH DIABETES MELLITUS OR VASCULAR INSUFFICIENCY Foot is most commonly involved Probe to the bone test Positive predictive value 89% Negative predictive value 56% Revascularization in those with poor arterial vascular supply to provide flow to debrided area and minimize possible amputation TESTS FOR OSTEOMYELITIS IN DIABETIC FOOT ULCERS OSTEOMYELITIS IN PATIENTS WITH DIABETES MELLITUS OR VASCULAR INSUFFICIENCY Test Sen Spec Probe to bone/exposed bone 60% 91% Radiography 54% 68% Bone scan 81% 28% Leukocyte scan 74% 68% MRI 90% 79% Management of dead space and adequate surgical drainage of soft tissue and bone Treatment failure often due to lack of adequate debridement Empiric antimicrobial therapy directed multiple aerobic and anaerobic microorganisms Dinh et al. CID 2008; 47: (c) 2013 Infectious Disease Board Review Course 10
SEPTIC ARTHRITIS. Dr Ahmed Husam Al Ahmed Rheumatologist SYRIA. University of Science and technology Hospital Sanaa Yemen 18/Dec/2014
 SEPTIC ARTHRITIS Dr Ahmed Husam Al Ahmed Rheumatologist SYRIA University of Science and technology Hospital Sanaa Yemen 18/Dec/2014 Objectives be able to define Septic Arthritis know what factors predispose
SEPTIC ARTHRITIS Dr Ahmed Husam Al Ahmed Rheumatologist SYRIA University of Science and technology Hospital Sanaa Yemen 18/Dec/2014 Objectives be able to define Septic Arthritis know what factors predispose
Types of bone/joint infections. Bone and Joint Infections. Septic Arthritis. Pathogenesis. Pathogenesis. Bacterial arthritis: predisposing factors
 Bone and Joint Infections Types of bone/joint infections Arthritis (infective/septic) Osteomyelitis Prosthetic bone and joint infections Septic Arthritis Common destructive athroplasty Mono-articular Poly-articular
Bone and Joint Infections Types of bone/joint infections Arthritis (infective/septic) Osteomyelitis Prosthetic bone and joint infections Septic Arthritis Common destructive athroplasty Mono-articular Poly-articular
ESPID New Bone and Joint Infection Guidelines
 ESPID New Bone and Joint Infection Guidelines Theoklis Zaoutis, MD, MSCE Professor of Pediatrics and Epidemiology Perelman School of Medicine at the University of Pennsylvania Chief, Division of Infectious
ESPID New Bone and Joint Infection Guidelines Theoklis Zaoutis, MD, MSCE Professor of Pediatrics and Epidemiology Perelman School of Medicine at the University of Pennsylvania Chief, Division of Infectious
Treatment of infection
 Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
Nuclear medicine and Prosthetic Joint Infections
 Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
Nuclear medicine and Prosthetic Joint Infections Christophe Van de Wiele, M.D., Ph.D. Department of Nuclear Medicine, University Hospital Ghent, Belgium Orthopedic prostheses: world market 1996 Prosthetic
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
Osteomyelitis and septic arthritis. Osteomyelitida. Cierny- Mader (1) Bone anatomy. Cierny- Mader (2) Pathogenesis (1)
 Osteomyelitis and septic arthritis M A R E K Š TEFAN ID UNIT, MILITAR Y UNIVERSITY HOSPITAL P R A G U E Bone infection Osteomyelitida Inflammatorydestructionof the bone with resultant necrosis Bone anatomy
Osteomyelitis and septic arthritis M A R E K Š TEFAN ID UNIT, MILITAR Y UNIVERSITY HOSPITAL P R A G U E Bone infection Osteomyelitida Inflammatorydestructionof the bone with resultant necrosis Bone anatomy
Osteomyelitis (Inflammation of the Bone and Bone Marrow) Basics
 Osteomyelitis (Inflammation of the Bone and Bone Marrow) Basics OVERVIEW Sudden (acute) or long-term (chronic) inflammation of bone and its associated soft-tissue elements of bone marrow, endosteum (lining
Osteomyelitis (Inflammation of the Bone and Bone Marrow) Basics OVERVIEW Sudden (acute) or long-term (chronic) inflammation of bone and its associated soft-tissue elements of bone marrow, endosteum (lining
Update on Prosthetic Joint Infections 2017
 Update on Prosthetic Joint Infections 2017 George F. Chimento, MD, FACS Chair, Department of Orthopaedic Surgery Associate Professor, University of Queensland School of Medicine Ochsner Medical Center
Update on Prosthetic Joint Infections 2017 George F. Chimento, MD, FACS Chair, Department of Orthopaedic Surgery Associate Professor, University of Queensland School of Medicine Ochsner Medical Center
BONE & JOINT INFECTIONS
 BONE & JOINT INFECTIONS Henry F. Chambers, MD Disclosures AstraZeneca advisory board Cubist research grant, advisory panel Genentech advisory board Merck stock Pfizer advisory board Theravance advisory
BONE & JOINT INFECTIONS Henry F. Chambers, MD Disclosures AstraZeneca advisory board Cubist research grant, advisory panel Genentech advisory board Merck stock Pfizer advisory board Theravance advisory
Acute Osteomyelitis: similar to septic arthritis but up to 40% may be afebrile swelling overlying the bone & tenderness
 Osteomyelitis / Bone and Joint Infections Bone infections in children are usually from haematogenous bacterial seeding to a single joint, usually the lower limbs, but may be multifocal. Approximately 10%
Osteomyelitis / Bone and Joint Infections Bone infections in children are usually from haematogenous bacterial seeding to a single joint, usually the lower limbs, but may be multifocal. Approximately 10%
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections
 Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Types of osteoarthritis
 ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
Coffey et al ND 6 HA, 5 TSA, and 5 other MRSA (3) and Staphylococcus epidermidis (3)
 Page 1 of 6 TABLE E-1 Outcomes of the Treatment of Periprosthetic Shoulder Infections* ä Study No. Presentation Prosthesis Most Common Pathogens Braman et al. 68 7 1 acute, 2 subacute, 2 HA and 5 TSA Staphylococcus
Page 1 of 6 TABLE E-1 Outcomes of the Treatment of Periprosthetic Shoulder Infections* ä Study No. Presentation Prosthesis Most Common Pathogens Braman et al. 68 7 1 acute, 2 subacute, 2 HA and 5 TSA Staphylococcus
Infection. Arthrocentesis: Cell count Differential Culture. Infection and associated microorganism(s) confirmed
 Painful joint History and examination Radiograph of affected joint Erythrocyte sedimentation rate C-reactive protein Infection No infection suspected Arthrocentesis: Cell count Differential Culture Stop
Painful joint History and examination Radiograph of affected joint Erythrocyte sedimentation rate C-reactive protein Infection No infection suspected Arthrocentesis: Cell count Differential Culture Stop
INFECTION & INFLAMMATION IMAGING
 INFECTION & INFLAMMATION IMAGING Radiopharmaceutical Drug Interactions & Other Interesting Case Studies MICHELLE RUNDIO, CNMT NCT MBA PCI NUCLEAR IN-111 WHITE BLOOD CELL IMAGING Interactions, Imaging Parameters
INFECTION & INFLAMMATION IMAGING Radiopharmaceutical Drug Interactions & Other Interesting Case Studies MICHELLE RUNDIO, CNMT NCT MBA PCI NUCLEAR IN-111 WHITE BLOOD CELL IMAGING Interactions, Imaging Parameters
Microbiology of joints and bone infections
 Microbiology of joints and bone infections Important Doctor Notes Extra Editing File Musculoskeletal Block - Microbiology Team 438 Objectives: Recognize the differences between osteomyelitis and arthritis.
Microbiology of joints and bone infections Important Doctor Notes Extra Editing File Musculoskeletal Block - Microbiology Team 438 Objectives: Recognize the differences between osteomyelitis and arthritis.
SEPTIC ARTHRITIS Native Joint BONE & JOINT INFECTIONS. Case. What is the most appropriate initial therapy for this patient? Henry F.
 BONE & JOINT INFECTIONS SEPTIC ARTHRITIS Native Joint Henry F. Chambers, MD Curr Rheumatol Rep 15:332, 2013; Best Prac Res Clin Rheumatol 25:407, 2011 Case 38 y/o type 2 diabetic women, single, sexually
BONE & JOINT INFECTIONS SEPTIC ARTHRITIS Native Joint Henry F. Chambers, MD Curr Rheumatol Rep 15:332, 2013; Best Prac Res Clin Rheumatol 25:407, 2011 Case 38 y/o type 2 diabetic women, single, sexually
Central Nervous System Infection
 Central Nervous System Infection Lingyun Shao Department of Infectious Diseases Huashan Hospital, Fudan University Definition Meningitis: an inflammation of the arachnoid membrane, the pia mater, and the
Central Nervous System Infection Lingyun Shao Department of Infectious Diseases Huashan Hospital, Fudan University Definition Meningitis: an inflammation of the arachnoid membrane, the pia mater, and the
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
ID Emergencies. BGSMC Internal Medicine Edwin Yu
 ID Emergencies BGSMC Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
ID Emergencies BGSMC Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
Overview. Clinical Scenario. Endocarditis: Treatment & Prevention. Prophylaxis The Concept. Jeremy D. Young, MD, MPH. Division of Infectious Diseases
 Endocarditis: Treatment & Prevention Jeremy D. Young, MD, MPH Division of Infectious Diseases Clinical Scenario Patient with MVP scheduled to have wisdom teeth extracted. Has systolic murmur with mid-systolic
Endocarditis: Treatment & Prevention Jeremy D. Young, MD, MPH Division of Infectious Diseases Clinical Scenario Patient with MVP scheduled to have wisdom teeth extracted. Has systolic murmur with mid-systolic
Primary foci of hematogenous periprosthetic joint infections
 Primary foci of hematogenous periprosthetic joint infections Dr. Anastasia Rakow Dr. Nora Renz Charité-Universitätsmedizin Berlin C.S., w. 73 y.o. 07/2015: presentation with painful knee prosthesis, back
Primary foci of hematogenous periprosthetic joint infections Dr. Anastasia Rakow Dr. Nora Renz Charité-Universitätsmedizin Berlin C.S., w. 73 y.o. 07/2015: presentation with painful knee prosthesis, back
Surgical Management of Osteomyelitis & Infected Hardware. Michael L. Sganga, DPM Orthopedics New England Natick, MA
 Surgical Management of Osteomyelitis & Infected Hardware Michael L. Sganga, DPM Orthopedics New England Natick, MA Disclosures None relevant to the content of this material Overview Implants Timing Tenants
Surgical Management of Osteomyelitis & Infected Hardware Michael L. Sganga, DPM Orthopedics New England Natick, MA Disclosures None relevant to the content of this material Overview Implants Timing Tenants
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
Bad Bugs in the Blood!
 Bad Bugs in the Blood! How to Work Up and Treat Bloodstream Infections Sharanjeet Thind M.D. Director of Inpatient Infectious Diseases, VA Medical Center Assistant Professor of Medicine, OUHSC, College
Bad Bugs in the Blood! How to Work Up and Treat Bloodstream Infections Sharanjeet Thind M.D. Director of Inpatient Infectious Diseases, VA Medical Center Assistant Professor of Medicine, OUHSC, College
Osteomieliti STEOMIE
 OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
Urinary Tract Infections in Hospitalized Patients
 Urinary Tract Infections in Hospitalized Patients Puerto Rico Chapter Annual Meeting Daniel C. DeSimone, MD March 9, 2019 2017 MFMER slide-1 Disclosures for speaker: Date of presentation: 3/9/2019 No relevant
Urinary Tract Infections in Hospitalized Patients Puerto Rico Chapter Annual Meeting Daniel C. DeSimone, MD March 9, 2019 2017 MFMER slide-1 Disclosures for speaker: Date of presentation: 3/9/2019 No relevant
Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery
 Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery College of Health Sciences Ladoke Akintola University
Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery College of Health Sciences Ladoke Akintola University
ACCME/Disclosures 4/13/2016 IDPB
 ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
ACCME/Disclosures The USCAP requires that anyone in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS which they or their spouse/partner
ID Emergencies. BUMC-P Internal Medicine Edwin Yu
 ID Emergencies BUMC-P Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
ID Emergencies BUMC-P Internal Medicine Edwin Yu Learning Objectives Bacterial meningitis IDSA guidelines: Clin Infect Dis 2004; 39:1267-84 HSV encephalitis IDSA guidelines: Clin Infect Dis 2008; 47:303-27
CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION 6. Friday, MARCH 18, 2016 STUDENT COPY
 MHD II, Session 6, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION 6 Friday, MARCH 18, 2016 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
MHD II, Session 6, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION 6 Friday, MARCH 18, 2016 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
Pressure Injury Complications: Diagnostic Dilemmas
 Pressure Injury Complications: Diagnostic Dilemmas Aimée D. Garcia, MD, CWS, FACCWS Associate Professor, Department of Medicine, Geriatrics Section Baylor College of Medicine Medical Director, Wound Clinic
Pressure Injury Complications: Diagnostic Dilemmas Aimée D. Garcia, MD, CWS, FACCWS Associate Professor, Department of Medicine, Geriatrics Section Baylor College of Medicine Medical Director, Wound Clinic
Introduction. Paronychia. Hand Infections. Eponychium. Paronychia 1/26/2015. INFECTIONS OF THE UPPER EXTREMITY Mark Rekant M.D.
 Introduction INFECTIONS OF THE UPPER EXTREMITY Mark Rekant M.D. Thomas Jefferson University Philadelphia Hand Center South Jersey Hand Center Hand infections are frequent Taking into account the countless
Introduction INFECTIONS OF THE UPPER EXTREMITY Mark Rekant M.D. Thomas Jefferson University Philadelphia Hand Center South Jersey Hand Center Hand infections are frequent Taking into account the countless
BONE AND JOINT INFECTION. Dr.Jónás Zoltán Dept.of Orthopaedics
 BONE AND JOINT INFECTION Dr.Jónás Zoltán Dept.of Orthopaedics www.ortopedia.dote.hu Order of verbal exams: The students are able to register for the exam on the Neptun system. The students pick two titles,
BONE AND JOINT INFECTION Dr.Jónás Zoltán Dept.of Orthopaedics www.ortopedia.dote.hu Order of verbal exams: The students are able to register for the exam on the Neptun system. The students pick two titles,
Microbiological diagnosis of infective endocarditis; what is new?
 Microbiological diagnosis of infective endocarditis; what is new? Dr Amani El Kholy, MD Professor of Clinical Pathology (Microbiology), Faculty of Medicine, Cairo University ESC 2017 1 Objectives Lab Diagnostic
Microbiological diagnosis of infective endocarditis; what is new? Dr Amani El Kholy, MD Professor of Clinical Pathology (Microbiology), Faculty of Medicine, Cairo University ESC 2017 1 Objectives Lab Diagnostic
The microbial diagnosis of infective endocarditis (IE)
 The microbial diagnosis of infective endocarditis (IE) Pierrette Melin Medical Microbiology pm-chulg sbimc 10.05.2007 1 Introduction for diagnosis Review of microbiological investigation of IE and perspectives
The microbial diagnosis of infective endocarditis (IE) Pierrette Melin Medical Microbiology pm-chulg sbimc 10.05.2007 1 Introduction for diagnosis Review of microbiological investigation of IE and perspectives
6/18/2014. John K. Midturi, DO, MPH June 5 th, 2014
 John K. Midturi, DO, MPH June 5 th, 2014 Heterogeneous disease Disease of antiquity Evolved from disease of high mortality disease with high morbidity One of the most difficult infections to treat Thomas
John K. Midturi, DO, MPH June 5 th, 2014 Heterogeneous disease Disease of antiquity Evolved from disease of high mortality disease with high morbidity One of the most difficult infections to treat Thomas
Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting]
![Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting] Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting]](/thumbs/83/87318178.jpg) Clinical Pearls Infectious Diseases Pritish K. Tosh, MD MN ACP Nov 7, 2014 [Answers and discussion slides will be posted after the meeting] Case 1 A 33-year-old male with diffuse large B-cell lymphoma
Clinical Pearls Infectious Diseases Pritish K. Tosh, MD MN ACP Nov 7, 2014 [Answers and discussion slides will be posted after the meeting] Case 1 A 33-year-old male with diffuse large B-cell lymphoma
Morbidity & Mortality Conference Downstate Medical Center. Daniel Kaufman, MD
 Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
BONE AND JOINT INFECTIONS: CRASH COURSE. Objectives: Technicians. Objectives: Pharmacists. Overview 2/27/2015. Osteomyelitis (OM)
 BONE AND JOINT INFECTIONS: CRASH COURSE Yanina Pasikhova, Pharm.D., BCPS AQ-ID, AAHIVP Infectious Diseases Clinical Pharmacist Moffitt Cancer Center Last Updated: 03/2015 Objectives: Pharmacists Objectives:
BONE AND JOINT INFECTIONS: CRASH COURSE Yanina Pasikhova, Pharm.D., BCPS AQ-ID, AAHIVP Infectious Diseases Clinical Pharmacist Moffitt Cancer Center Last Updated: 03/2015 Objectives: Pharmacists Objectives:
Life-threatening infections. Frank Bowden October 5, 2018
 Life-threatening infections Frank Bowden October 5, 2018 David Sackett Evidence Based Medicine is the integration of best research evidence with clinical expertise and patient values. The Golden Rules
Life-threatening infections Frank Bowden October 5, 2018 David Sackett Evidence Based Medicine is the integration of best research evidence with clinical expertise and patient values. The Golden Rules
P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis?
 Pediatrics Prevention P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis? RESEARCHED BY: Muhammad Amin Chinoy MD, Pakistan Literature:
Pediatrics Prevention P-1 (Former P-1) Are pediatric patients on oral or intravenous steroids at an increased risk of developing septic arthritis? RESEARCHED BY: Muhammad Amin Chinoy MD, Pakistan Literature:
Introduction. Disclosure. Biomet-Royalties. Infection after Shoulder Arthroplasty. Infection. John W. Sperling MD, MBA
 Infection after Shoulder Arthroplasty John W. Sperling MD, MBA Biomet-Royalties Disclosure Introduction Infection Rare, but devastating complication Reported incidence ranges from 0% to 4% Coste et al.
Infection after Shoulder Arthroplasty John W. Sperling MD, MBA Biomet-Royalties Disclosure Introduction Infection Rare, but devastating complication Reported incidence ranges from 0% to 4% Coste et al.
Balgrist Shoulder Course 2017
 Diagnosis and Management of Infection in Revision Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflict
Diagnosis and Management of Infection in Revision Shoulder Arthroplasty Joseph P. Iannotti MD, PhD Maynard Madden Professor and Chairman Orthopaedic and Rheumatologic Institute Cleveland Clinic Conflict
Reading Test 1 Part A
 Reading Test 1 Part A Page 1 w Copy w Rights w. Reserved o e t ::: m www.oetmaterial.com a t e r i a l. c o m. a u Reading: Part A TIME LIMIT: 15 MINUTES Instructions: Complete the following summary using
Reading Test 1 Part A Page 1 w Copy w Rights w. Reserved o e t ::: m www.oetmaterial.com a t e r i a l. c o m. a u Reading: Part A TIME LIMIT: 15 MINUTES Instructions: Complete the following summary using
Osteomyelitis and Septic Joints; Practical Considerations. Coleen K. Cunningham
 Osteomyelitis and Septic Joints; Practical Considerations Coleen K. Cunningham Goals/objectives To improve understanding of the diagnosis, treatment, and follow-up of pediatric bone and joint infections
Osteomyelitis and Septic Joints; Practical Considerations Coleen K. Cunningham Goals/objectives To improve understanding of the diagnosis, treatment, and follow-up of pediatric bone and joint infections
Daniel C. DeSimone, MD Assistant Professor of Medicine
 Daniel C. DeSimone, MD Assistant Professor of Medicine Faculty photo will be placed here Desimone.Daniel@mayo.edu 2015 MFMER 3543652-1 Infective Endocarditis Mayo School of Continuous Professional Development
Daniel C. DeSimone, MD Assistant Professor of Medicine Faculty photo will be placed here Desimone.Daniel@mayo.edu 2015 MFMER 3543652-1 Infective Endocarditis Mayo School of Continuous Professional Development
Complicated Skin and Soft Tissue Infection diagnosis and severity stratification
 Complicated Skin and Soft Tissue Infection diagnosis and severity stratification Muhammad Hussein Gasem Div Infectious Disease, TropMed, and Immunology Dr. Kariadi Hospital, Diponegoro University Semarang,
Complicated Skin and Soft Tissue Infection diagnosis and severity stratification Muhammad Hussein Gasem Div Infectious Disease, TropMed, and Immunology Dr. Kariadi Hospital, Diponegoro University Semarang,
CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI. Friday, MARCH 20, 2015 STUDENT COPY
 MHD II, Session VI, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI Friday, MARCH 20, 2015 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
MHD II, Session VI, STUDENT Copy Page 1 CASE-BASED SMALL GROUP DISCUSSION MHD II SESSION VI Friday, MARCH 20, 2015 STUDENT COPY Resource for cases: ACP Medicine (Scientific American Medicine) - Vaginitis
Foot infections in persons with diabetes are
 DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
December 3, 2015 Severe Sepsis and Septic Shock Antibiotic Guide
 Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
The EM Educator Series
 The EM Educator Series The EM Educator Series: Why is my patient with gallbladder pathology so sick? Author: Alex Koyfman, MD (@EMHighAK) // Edited by: Brit Long, MD (@long_brit) and Manpreet Singh, MD
The EM Educator Series The EM Educator Series: Why is my patient with gallbladder pathology so sick? Author: Alex Koyfman, MD (@EMHighAK) // Edited by: Brit Long, MD (@long_brit) and Manpreet Singh, MD
Objectives. Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection
 Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Sepsis and Infective Endocarditis
 Sepsis and Infective Endocarditis Michal Holub Department of Infectious Diseases First Faculty of Medicine Charles University in Prague and University Military Hospital Bacteremia and Sepsis bacteremia
Sepsis and Infective Endocarditis Michal Holub Department of Infectious Diseases First Faculty of Medicine Charles University in Prague and University Military Hospital Bacteremia and Sepsis bacteremia
MICROBIOLOGICAL TESTING IN PICU
 MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
MICROBIOLOGICAL TESTING IN PICU This is a guideline for the taking of microbiological samples in PICU to diagnose or exclude infection. The diagnosis of infection requires: Ruling out non-infectious causes
Assessment of limping child (beware the child who does not weight bear at all):
 Department of Paediatrics Clinical Guideline Acutely Limping Child and Septic Arthritis Assessment of limping child (beware the child who does not weight bear at all): History Careful history of any significant
Department of Paediatrics Clinical Guideline Acutely Limping Child and Septic Arthritis Assessment of limping child (beware the child who does not weight bear at all): History Careful history of any significant
-> Education -> Excellence
 Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Septic Arthritis and Concern for Osteomyelitis in a Child with Rat Bite Fever. Dustin D Flannery DO
 JCM Accepts, published online ahead of print on 3 April 2013 J. Clin. Microbiol. doi:10.1128/jcm.03139-12 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 1 Septic Arthritis and
JCM Accepts, published online ahead of print on 3 April 2013 J. Clin. Microbiol. doi:10.1128/jcm.03139-12 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 1 Septic Arthritis and
The Painful Prosthetic Joint: Role of Nuclear Medicine
 The Painful Prosthetic Joint: Role of Nuclear Medicine Christopher J. Palestro, M.D. Professor of Radiology Hofstra North Shore-LIJ of Medicine Chief Division of Nuclear Medicine & Molecular Imaging North
The Painful Prosthetic Joint: Role of Nuclear Medicine Christopher J. Palestro, M.D. Professor of Radiology Hofstra North Shore-LIJ of Medicine Chief Division of Nuclear Medicine & Molecular Imaging North
Zoonosis = an infection or infestation which is shared in nature by man and lower vertebrate animals.
 Zoonosis = an infection or infestation which is shared in nature by man and lower vertebrate animals. For the purposes of this presentation, "zoonotic disease" will be defined as a disease that is caused
Zoonosis = an infection or infestation which is shared in nature by man and lower vertebrate animals. For the purposes of this presentation, "zoonotic disease" will be defined as a disease that is caused
Disclosures! Infection & Nonunions. Infection workup. Skip early infection. Culture (+) fractures. Gross Infection
 The Infected Nonunion Paul Tornetta III, MD Professor Boston Medical Center Disclosures! Publications: Rockwood and Green, Tornetta and Ricci TIFS, Tornetta and Einhorn; Subspecialty series, Court-Brown,
The Infected Nonunion Paul Tornetta III, MD Professor Boston Medical Center Disclosures! Publications: Rockwood and Green, Tornetta and Ricci TIFS, Tornetta and Einhorn; Subspecialty series, Court-Brown,
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任
 Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Infective Endocarditis
 Infective Endocarditis Infective Endocarditis Historical Perspective.. A concretion larger than a pigeon s egg; contained in the left auricle. Burns, 1809 Osler s Gulstonian lectures provided the 1 st
Infective Endocarditis Infective Endocarditis Historical Perspective.. A concretion larger than a pigeon s egg; contained in the left auricle. Burns, 1809 Osler s Gulstonian lectures provided the 1 st
a Total Hip Prosthesis by Clostridum perfringens. A Case Report
 Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Mechanisms of Pathogenicity
 Mechanisms of Pathogenicity The Microbes Fight Back Medically important bacteria Salmonella Bacillus anthracis Shigella dysenteriae Campylobacter Shigella sonnei Clostridium botulinum Staphylococcus aureus
Mechanisms of Pathogenicity The Microbes Fight Back Medically important bacteria Salmonella Bacillus anthracis Shigella dysenteriae Campylobacter Shigella sonnei Clostridium botulinum Staphylococcus aureus
APPROACH TO PATIENTS WITH POLYARTHRALGIA
 APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
Disclosures. Orthopedic infections. Case 1. Pen Barnes MBBS PhD. Clinical Associate Professor Departments of Medicine Pathology and Orthopedics OHSU
 Orthopedic infections Disclosures Pen Barnes MBBS PhD I have nothing to disclose Clinical Associate Professor Departments of Medicine Pathology and Orthopedics OHSU Case 1 48 year old woman presents to
Orthopedic infections Disclosures Pen Barnes MBBS PhD I have nothing to disclose Clinical Associate Professor Departments of Medicine Pathology and Orthopedics OHSU Case 1 48 year old woman presents to
Neutropenic Fever. CID 2011; 52 (4):e56-e93
 Neutropenic Fever www.idsociety.org CID 2011; 52 (4):e56-e93 Definitions Fever: Single oral temperature of 101 F (38.3 C) Temperature 100.4 F (38.0 C) over 1 hour Neutropenia: ANC < 500 cells/mm 3 Expected
Neutropenic Fever www.idsociety.org CID 2011; 52 (4):e56-e93 Definitions Fever: Single oral temperature of 101 F (38.3 C) Temperature 100.4 F (38.0 C) over 1 hour Neutropenia: ANC < 500 cells/mm 3 Expected
Wounds and Infections: Wound Management From the ID Physician Standpoint. Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department
 Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
BACTERIOLOGY PROGRAMME AND PLAN OF TEACHING 3 rd Semester (academic year )
 BACTERIOLOGY PROGRAMME AND PLAN OF TEACHING 3 rd Semester (academic year 2012-2013) 19. 10. 2012. Introduction in microbiology, bacterial taxonomy, general bacterial prop Bacterial structures, biosynthesis
BACTERIOLOGY PROGRAMME AND PLAN OF TEACHING 3 rd Semester (academic year 2012-2013) 19. 10. 2012. Introduction in microbiology, bacterial taxonomy, general bacterial prop Bacterial structures, biosynthesis
Seronegative spondyloarthropathies : A Pictorial Review
 Seronegative spondyloarthropathies : A Pictorial Review Poster No.: P-0008 Congress: ESSR 2012 Type: Scientific Exhibit Authors: J. Acosta Batlle, B. Palomino Aguado, M. D. Lopez Parra, S. 1 2 3 2 4 1
Seronegative spondyloarthropathies : A Pictorial Review Poster No.: P-0008 Congress: ESSR 2012 Type: Scientific Exhibit Authors: J. Acosta Batlle, B. Palomino Aguado, M. D. Lopez Parra, S. 1 2 3 2 4 1
Urinary tract infections Dr. Hala Al Daghistani
 Urinary tract infections Dr. Hala Al Daghistani UTIs are considered to be one of the most common bacterial infections. Diagnosis depends on the symptoms, urinalysis, and urine culture. UTIs occur more
Urinary tract infections Dr. Hala Al Daghistani UTIs are considered to be one of the most common bacterial infections. Diagnosis depends on the symptoms, urinalysis, and urine culture. UTIs occur more
BASIC KNOWLEDGE ABOUT INFECTIVE ENDOCARDITIS FOR CLINICIAN
 BASIC KNOWLEDGE ABOUT INFECTIVE ENDOCARDITIS FOR CLINICIAN When should I suspect infective endocarditis? Antibiotic regimen Patient care after completion of treatment Prophylactic Regimens Prosthetic Valve
BASIC KNOWLEDGE ABOUT INFECTIVE ENDOCARDITIS FOR CLINICIAN When should I suspect infective endocarditis? Antibiotic regimen Patient care after completion of treatment Prophylactic Regimens Prosthetic Valve
Musculoskeletal Infection and Inflammation
 F.A. Davis: Advantage Musculoskeletal Infection and Inflammation(10.6.15) Page 1 Musculoskeletal Infection and Inflammation The musculoskeletal system is affected by infections and inflammatory conditions.
F.A. Davis: Advantage Musculoskeletal Infection and Inflammation(10.6.15) Page 1 Musculoskeletal Infection and Inflammation The musculoskeletal system is affected by infections and inflammatory conditions.
Michael Stander, Pharm.D.
 Michael Stander, Pharm.D. Endocarditis: Goals Epidemiology Presentation of acute and subacute. Diagnosis: What is Dukes Criteria and how do we approach the diagnosis of endocarditis? Treatment: Understand
Michael Stander, Pharm.D. Endocarditis: Goals Epidemiology Presentation of acute and subacute. Diagnosis: What is Dukes Criteria and how do we approach the diagnosis of endocarditis? Treatment: Understand
Infection Imaging In Nuclear Medicine: Arguing The Case for PET/CT.
 Infection Imaging In Nuclear Medicine: Arguing The Case for PET/CT. LUIS A. TAMARA M.D. NUCLEAR MEDICINE /PET-CT SERVICE CHIEF MEDVAMC DISCLOSURES. 2 3 Not difficult to appreciate the difference! GA-67
Infection Imaging In Nuclear Medicine: Arguing The Case for PET/CT. LUIS A. TAMARA M.D. NUCLEAR MEDICINE /PET-CT SERVICE CHIEF MEDVAMC DISCLOSURES. 2 3 Not difficult to appreciate the difference! GA-67
MICROBIOLOGY - An Overview
 MICROBIOLOGY - An Overview Hieucam Phan, MD Pediatrics St. Luke s Hospital San Francisco, CA Microbiology 6/01 1 Introduction Major Achievements of Medical Sciences in the 20th Century Microbiology DNA
MICROBIOLOGY - An Overview Hieucam Phan, MD Pediatrics St. Luke s Hospital San Francisco, CA Microbiology 6/01 1 Introduction Major Achievements of Medical Sciences in the 20th Century Microbiology DNA
Staphylococci. What s to be Covered. Clinical Scenario #1
 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
What s to be Covered. Microbiology of staphylococci Epidemiology of S. aureus infections Pathogenesis of S. aureus infections
 Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Staphylococci Micrococcus, which, when limited in its extent and activity, causes acute suppurative inflammation (phlegmon), produces, when more extensive and intense in its action on the human system,
Where has SARA gone? Prof. David Kane Consultant Rheumatologist Beacon & Tallaght Hospitals. Clinical Professor in Rheumatology Trinity College Dublin
 Where has SARA gone? Prof. David Kane Consultant Rheumatologist Beacon & Tallaght Hospitals Clinical Professor in Rheumatology Trinity College Dublin 1 Reactive Arthritis Seronegative Asymmetrical Arthritis
Where has SARA gone? Prof. David Kane Consultant Rheumatologist Beacon & Tallaght Hospitals Clinical Professor in Rheumatology Trinity College Dublin 1 Reactive Arthritis Seronegative Asymmetrical Arthritis
The Streptococci. Diverse collection of cocci. Gram-positive Chains or pairs significant pathogens
 The Streptococci Diverse collection of cocci. Gram-positive Chains or pairs significant pathogens Strong fermenters Facultative anaerobes Non-motile Catalase Negative 1 Classification 1 2 Classification
The Streptococci Diverse collection of cocci. Gram-positive Chains or pairs significant pathogens Strong fermenters Facultative anaerobes Non-motile Catalase Negative 1 Classification 1 2 Classification
Abscess. A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body.
 Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Chapter 4 Inflammation and Infection
 Chapter 4 Inflammation and Infection Defense Mechanisms Three lines of defense protect the body against foreign invasion: Physical or surface barriers Inflammation Immune response Inflammation Non-specific
Chapter 4 Inflammation and Infection Defense Mechanisms Three lines of defense protect the body against foreign invasion: Physical or surface barriers Inflammation Immune response Inflammation Non-specific
Infective Endocarditis
 Frank Lowy Infective Endocarditis 1. Introduction Infective endocarditis (IE) is an infection of the heart valves. A large number of different bacteria are capable of causing this disease. Depending on
Frank Lowy Infective Endocarditis 1. Introduction Infective endocarditis (IE) is an infection of the heart valves. A large number of different bacteria are capable of causing this disease. Depending on
Selected Issues in Nonneoplastic. Orthopaedic Pathology. Diseases of Diarthrodial Joints and their Complications
 1 2 3 Selected Issues in Nonneoplastic Orthopaedic Pathology Diseases of Diarthrodial Joints and their Complications Biology of articular hyaline cartilage Arthritis Osteonecrosis Prosthetic Joints Metabolic
1 2 3 Selected Issues in Nonneoplastic Orthopaedic Pathology Diseases of Diarthrodial Joints and their Complications Biology of articular hyaline cartilage Arthritis Osteonecrosis Prosthetic Joints Metabolic
Rapid and progressive necrosis of the tissue underlying epidermis (cellulitis)
 Table 1. Infections of the Skin, Eyes and Ears Folliculitis Furuncles (boils) & Carbuncles Staphylococcus aureus (G+) Scald Skin Syndrome Peeling skin on infants Staphylococcus aureus (G+) Impetigo Lesions
Table 1. Infections of the Skin, Eyes and Ears Folliculitis Furuncles (boils) & Carbuncles Staphylococcus aureus (G+) Scald Skin Syndrome Peeling skin on infants Staphylococcus aureus (G+) Impetigo Lesions
Dr Babak Tamizi far MD. Assistant Professor Of Internal Medicine Al-Zahra Hospital Isfahan University Of Medical Sciences
 Dr Babak Tamizi far MD. Assistant Professor Of Internal Medicine Al-Zahra Hospital Isfahan University Of Medical Sciences ١ ٢ ٣ A 57-year-old man presents with new-onset fever, shortness of breath, lower
Dr Babak Tamizi far MD. Assistant Professor Of Internal Medicine Al-Zahra Hospital Isfahan University Of Medical Sciences ١ ٢ ٣ A 57-year-old man presents with new-onset fever, shortness of breath, lower
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29
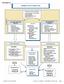 PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
In the absence of underlying edema or other skin abnormalities, erysipelas
 ERYSIPELAS Erysipelas is a distinct type of superficial cutaneous cellulitis with marked dermal lymphatic vessel involvement caused by group A β-hemolytic streptococcus (very uncommonly group C or G streptococcus)
ERYSIPELAS Erysipelas is a distinct type of superficial cutaneous cellulitis with marked dermal lymphatic vessel involvement caused by group A β-hemolytic streptococcus (very uncommonly group C or G streptococcus)
 www.fisiokinesiterapia.biz Peak onset between 20 and 30 years Form of spondyloarthritis (cause inflammation around site of ligament insertion into bone) and association with HLA-B27 Prevalence as high
www.fisiokinesiterapia.biz Peak onset between 20 and 30 years Form of spondyloarthritis (cause inflammation around site of ligament insertion into bone) and association with HLA-B27 Prevalence as high
Primary haematogenous septic arthritis of the wrist in immunocompetent healthy patients : A report of four cases
 Acta Orthop. Belg., 2011, 77, 590-594 ORIGINAL STUDY Primary haematogenous septic arthritis of the wrist in immunocompetent healthy patients : A report of four cases Lore VAnDEnBERghE, Jos StUyCk, Ilse
Acta Orthop. Belg., 2011, 77, 590-594 ORIGINAL STUDY Primary haematogenous septic arthritis of the wrist in immunocompetent healthy patients : A report of four cases Lore VAnDEnBERghE, Jos StUyCk, Ilse
Bone and prosthetic joint infections: what the ID specialist needs?
 Bone and prosthetic joint infections: what the ID specialist needs? Andrej Trampuz Charité University Medicine Berlin Center for Septic Surgery Hip and knee replacements in Europe Germany Austria Belgium
Bone and prosthetic joint infections: what the ID specialist needs? Andrej Trampuz Charité University Medicine Berlin Center for Septic Surgery Hip and knee replacements in Europe Germany Austria Belgium
Prosthetic Joint Infections Review of diagnosis including the role of molecular techniques. Dr Prema Singh
 Prosthetic Joint Infections Review of diagnosis including the role of molecular techniques Dr Prema Singh Consultant Microbiologist Watford General Hospital Structure of talk Introduction Case scenario
Prosthetic Joint Infections Review of diagnosis including the role of molecular techniques Dr Prema Singh Consultant Microbiologist Watford General Hospital Structure of talk Introduction Case scenario
Aerobic bacteria isolated from diabetic septic wounds
 Aerobic bacteria isolated from diabetic septic wounds Eithar Mohammed Mahgoub*, Mohammed Elfatih A. Omer Faculty of Pharmacy, Omdurman Islamic University Department of Pharmaceutical Microbiology, Omdurman
Aerobic bacteria isolated from diabetic septic wounds Eithar Mohammed Mahgoub*, Mohammed Elfatih A. Omer Faculty of Pharmacy, Omdurman Islamic University Department of Pharmaceutical Microbiology, Omdurman
BONES & JOINTS INFECTION BONE TUMOURS
 BONES & JOINTS INFECTION BONE TUMOURS IMPORTANT SERIOUS CONSEQUENCE PLEASE DON T MISS!! EARLY DIAGNOSIS & PROPER TREATMENT HOW?? AWARE of THEIR EXISTENCE (Knowledge) PREPARE for THEIR OCCURRENCE A HIGH
BONES & JOINTS INFECTION BONE TUMOURS IMPORTANT SERIOUS CONSEQUENCE PLEASE DON T MISS!! EARLY DIAGNOSIS & PROPER TREATMENT HOW?? AWARE of THEIR EXISTENCE (Knowledge) PREPARE for THEIR OCCURRENCE A HIGH
SYMPOSIUM 10TH MAY 2007 BELGIUM. Blood culture-negative endocarditis
 SYMPOSIUM 10TH MAY 2007 BELGIUM Blood culture-negative endocarditis Didier RAOULT Didier.raoult@gmail.com Modified Duke criteria for diagnosis of infective endocarditis (IE) Li JS, et al. Proposed modifications
SYMPOSIUM 10TH MAY 2007 BELGIUM Blood culture-negative endocarditis Didier RAOULT Didier.raoult@gmail.com Modified Duke criteria for diagnosis of infective endocarditis (IE) Li JS, et al. Proposed modifications
Infective endocarditis (IE) By Assis. Prof. Nader Alaridah MD, PhD
 Infective endocarditis (IE) By Assis. Prof. Nader Alaridah MD, PhD Infective endocarditis (IE) is an inflammation of the endocardium.. inner of the heart muscle & the epithelial lining of heart valves.
Infective endocarditis (IE) By Assis. Prof. Nader Alaridah MD, PhD Infective endocarditis (IE) is an inflammation of the endocardium.. inner of the heart muscle & the epithelial lining of heart valves.
