TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D.
|
|
|
- Coral Della Chapman
- 6 years ago
- Views:
Transcription
1 TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D. Since you have progressed to the point of serious consideration of total hip replacement, there is a great deal of information that is important for you to understand. Prior to making your final decision and ultimately having your total hip replacement, it is important that you understand everything about the procedure and have realistic expectations about the results. You should understand why you are having problems with your hip and when you should make the decision to have hip replacement surgery. It is important to know exactly what is done at the surgery and what to expect from the surgical procedure. These expectations along with the possible complications of the procedure will allow you to decide when to proceed ahead with the operation. I also want you to understand clearly what is expected of you prior to your admission to the hospital, during your admission, and in the rehabilitation period after your discharge. I will try to summarize all this information for you. Certainly if you have any questions, please feel free to contact me. RATIONALE AND INDICATION Total hip replacement for disorders of the hip joint has been performed for over 40 years. A rapid evolution in prosthesis design and surgical techniques has occurred in the last ten years. The great majority of the operations are done for arthritic conditions of the hip. There are many different causes of arthritis all of which cause a deterioration of the hip joint. The forms of arthritis include osteoarthritis, rheumatoid arthritis, ankylosing spondylitis, traumatic arthritis (related to injury), avascular necrosis or loss of blood supply to the hip joint, and arthritis secondary to congenital or developmental problems such as congenital dislocation of the hip, Perthes disease or slipped capital epiphysis. The hip joint is a ball and socket joint which moves on a very smooth surface called the articular cartilage. The articular cartilage is worn away by the arthritis process to the point that the hip joint becomes painful. The process is usually gradual and may require months or even years for it to progress from a mild to a severe
2 state. As it becomes more severe, you will experience more pain and more limited function. There are many types of arthritis that can cause this deterioration of the hip joint. A second category of causes requiring total hip replacement are those of failed previous hip surgeries. The most common is a previous hip replacement that now has failed either through loosening of the components from bone or wear of the polyethylene liner. This is called a revision total hip replacement while the initial hip replacement is called a primary total hip replacement. The third common cause for total hip replacement is in cases of fracture of the hip. Many hip fractures are managed by pin or screw fixation; but in some circumstances where the damage is quite severe, a hip replacement is required because the bone itself will not heal. In the early stages of hip disease, the pain and loss of function may be improved by conservative means of treatment including nonsteroidal anti- inflammatory agents, intra- articular injection of steroids, the use of a cane or crutches, and restriction of activity. Weight loss, if possible, can also significantly reduce the level of pain. For many medical reasons, it is best to reach your optimal weight. This weight loss is difficult and sometimes impossible with severe disease as you cannot exercise or walk very far. At some point, the arthritic process will increase in severity and patients will have increasing pain and decreasing function which is no longer managed by conservative measures. Many patients wish to consider hip replacement at this time. The decision to perform the total hip replacement is usually based entirely on the patient s complaints. It is rare when the surgery is done on an emergent basis except in the case of fracture. There are, however, some cases where the arthritic process is so severe that it actually wears away or erodes the bone. Once this erosion occurs, the operation must be done in a reasonable period of time to prevent loss of bone which may compromise the optimal results.
3 SURGERY The hip is a ball and socket joint that remains connected or reduced by a thin capsule and muscle tension. The ball is the femoral head of the upper end of the femur, or thigh bone. The socket is the acetabulum which is part of the pelvic bone. A hip replacement replaces these abnormal or worn surfaces. The femoral head is removed and replaced by a metallic head. The acetabulum is removed and replaced by a plastic in metal socket which is made of a high- density polyethylene. The metal is a strong alloy of either titanium or a combination of chromium and cobalt. A new capsule or lining forms around the joint to maintain the ball inside the socket. A controversy that previously existed in the total hip replacement is the method of fixation of the prosthesis to the patient. Two options are available. One is the use of commercially pure acrylic bone cement called methyl- methacrylate. Early use was quite crude and the cement fixation was actually quite weak. It was typically used in patients who were older or had very weak or osteoporotic bone. This type of fixation had been thought superior for many years but evolution in surgical technique and implants has changed this practice significantly. Current literature supports the use of a newer type of fixation which involves the patient s bone growing into a roughened or porous surface of the total hip implants. It is my belief that this type of fixation is superior, with better long term longevity, in the majority of patients, regardless of age, bone type or gender. It is an extremely rare occasion that I would choose the use of methyl- methacrylate over bone ingrowth fixation. A second controversial issue is that of alternative bearing surfaces, or all metal or ceramic total hip replacements. These surfaces may have some potential advantages but also have some potential pitfalls including stability, breakage and carcinogenesis. EXPECTATIONS The operation is very successful in terms of its main goal which is pain relief. Approximately 90 percent of people have complete pain relief. The additional 10 percent of patients may have mild and intermittent
4 discomfort if they overuse the hip or become too active. The same high percentage of people no longer have a limp after the surgical procedure. A limp may occur or persist even though pain relief occurs. This occurs in situations where the muscles around the hip are very weak or in cases where the postoperative exercises are not performed. Most patients do not require any assistive devices to walk, although in some cases, patients choose to use a single prong cane for safety or balance reasons. You are usually able to increase your activity level dramatically after surgery. Patients are encouraged to walk, hike, ride a bicycle or exercycle, swim and even play golf. Sports that cause significant impact or twisting such as running, singles tennis or downhill skiing are not ideal. A frequent complaint of patients in addition to pain and limp is that of shortening of the leg. This occurs as the arthritic process wears away the articular cartilage and in some cases even the bone itself. At the time of surgery the leg can usually be lengthened to a point that the legs seem to be equal. But you must understand this is a secondary goal and the most important goal is pain relief and stability. Leg length discrepancy has become less common with the development of more versatile implant systems. The final critical issue is how long the hip replacement will last. At this point we have very good information that suggests an ingrowth/non- cemented total hip replacement will last approximately fifteen to twenty- five years. After many years of use and walking, the hip prosthesis can loosen from the bone or the plastic can wear out. If this occurs and pain is present, it may be necessary to revise or re- do the hip replacement. This technically can be accomplished successfully but obviously it is best to have the initial hip replacement last as long as possible. COMPLICATIONS The results of total hip replacements are excellent. Therefore, there must be some reason that prevents us from performing hip replacements except in patients with significant arthritis. Complications are rare but nonetheless exist. These complications include infection, blood clot formation or thrombophlebitis, dislocation of the prosthesis ball from the
5 socket, nerve injury, fracture and other general complications. The issues especially important to address include infection, blood clot formation and dislocation. The chance of infection in a total hip replacement is 1 out of 200 or 0.5%. This is a very low number but, nevertheless, can occur. If this occurs, it can be very difficult problem to treat and it is often necessary to have other surgeries to remove the infection. In some cases, removal of the implant for a temporary period of time is required. Obviously, the best way to treat the infection is to prevent it. The surgical team uses air exhaust systems which are operating room apparel often called spacesuits. This prevents the operating room staff from breathing on the area of your hip operation. In addition, all patients receive preventive or prophylactic antibiotics for 24 hours. This combination of techniques should lower the chance of infection. Our hospital infection rate for all primary joint replacements last year was 0.2%. Blood clot formation/thrombophlebitis or deep venous thrombosis is the formation of a blood clot in one of the deep veins of the lower leg. This is a common complication that occurs despite all methods of prevention. There are multiple ways to try to prevent this. Early mobilization decreases blood pooling your lower extremities. We put all patients on some type of blood thinner throughout the hospitalization, dependent upon your past medical history and the medications you take. The types of blood thinners we use include aspirin (taken twice a day), Coumadin or warfarin, lovenox (injectable) and/or xarelto. Finally, all patients also wear sequential compression TEDS which are devices placed on both legs that massage the leg from the ankle to the knee to increase blood flow to minimize the chance of clot formation. The best result, of course, is that you do not form a blood clot. If you did form a blood clot, it is important to know about it because it can be adequately treated. If you form a blood clot and it is not treated, there is a chance the blood clot could break loose and embolize/or move to your heart or to your lung. This could potential be fatal. Therefore, the safest approach is: 1) attempt to prevent DVT and 2) diagnose deep vein thrombosis prior to leaving the hospital. With this protocol the incidence of blood clots following hip replacement is 4 percent.
6 During your hospitalization you will be involved in an exercise program and instructed on the postoperative hip positions that you should avoid. If you bend your hip too far, bring your knees all the way to your chest, or turn your leg in too far, there is a chance that the ball can dislocate out of the socket. This should not occur if you use a reasonable amount of caution and follow the instructions. These restrictions should be maintained for life but are most critical during the first three months after surgery while the soft tissues about the hip are healing. If this does occur it usually requires an operation where you have to open the hip replacement. This is a potential complication that should be preventable. The dislocation rate for a primary hip replacement is less than 0.2%. Because incision sizes have become significantly smaller than they were in the past, total hip replacement rarely requires blood transfusion. Because it is rare that our patients require blood transfusion we do not suggest pre- surgery blood donation by our patients. In certain patients we might use a wound drain post- operatively that collects the blood lost from the incision site. This blood will be re- transfused as necessary although it is unusual that there would be need to use a wound drain at all. The availability of re- infusion drains can avoid the concerns of hepatitis and AIDS transmission. The chance of this occurring is exceedingly small with the estimated incidence of hepatitis transmission being 1 in 4,000 blood transfusions and AIDS being 1 in 1,000,000 transfusions. In cases of a fractured hip, I will be very cautious in using any other types of blood transfusions and will always discuss this with you first. If blood transfusion becomes necessary, the blood is very carefully screened and tested for these two problems. Other complications that might occur are rare. They are potentially associated with any major surgery and anesthesia. The potential complications include death, heart attack, heart failure, stroke, pneumonia, lung congestion, gastrointestinal problems such as nausea, vomiting, diarrhea, constipation, urinary tract infections and decubitus or bedsores, etc. The long- term complication involves failure of the implant, as
7 discussed in the previous section. This may occur by either loss of fixation or mechanical loosening of one or all of the implants or by wear of the plastic polyethylene surface. Modern hip replacements should last more than twenty years. It is advisable to stay in good physical health, avoid excessive weight gain, avoid excessive impact activities as previously noted, and exercise frequently. Although revision surgery is usually very successful, hopefully it will never be required for most patients. PREPARATATION FOR SURGERY Once you have made your decision to have a total hip replacement, you should contact our Surgery Coordinator, Renee Wood at She will help you choose a surgery date and will also schedule you for a pre- surgery appointment with my Physician s Assistant: Michelle (Shelley) Martinez. This pre- surgery appointment with Michelle is mandatory for surgery. The time you must wait for your surgery is variable depending on the surgery schedule and your other medical conditions. We will make every attempt to schedule the surgery at your convenience. Renee can answer many questions about preparation for surgery, the pre- operative sequence of events, and insurance matters. It is important to have a physical examination by your primary care physician/internist and/or cardiologist (if you have ANY cardiac history) prior to your total hip replacement surgery. Since this is a serious operation, you should be in your best medical health with all medical problems under good control. If you have had a recent physical examination, it may not be necessary to have a new examination. Once you have discussed your upcoming hip replacement with your primary care physician and/or cardiologist they will then mail or fax the results of your examination and tests results to our office. It is preferable that these documents are received by our office prior to your pre- surgery appointment with Michelle. Additionally, we request that your dental health be at its optimum. We must ensure that you do not have any active oral/dental infection prior to joint replacement surgery, and therefore
8 require that you see your dentist and undergo evaluation if you have any teeth in your mouth at all. Your dentist may also mail or fax results of your examination to our office prior to your admission to the hospital. We will send a letter to your primary care provider detailing our plans to proceed with surgery at the time your surgery is scheduled. It is your responsibility to make certain your pre- operative primary care physician, cardiology, and dental appointments are completed prior to surgery. As mentioned above, at the time that our surgery coordinator schedules your hip replacement she will also be scheduled an in depth preoperative history and physical examination with my Physician's Assistant, Michelle Martinez (Shelley). This appointment typically occurs 3-4 weeks prior to your surgery date, and we do encourage you to bring a spouse, family member or friend with you to this appointment if you would like to involve them in your care. Michelle will be greatly involved in your whole hip replacement experience as she is my operative assistant during surgery, she is greatly involved in your hospital care and will also be seeing you during various clinic follow up visits. At your pre- surgery appointment Michelle will ensure that you are medically and surgically prepared for surgery, and that all of your questions have been answered. You will understand what will happen just prior to surgery, during surgery, during your stay in the hospital, and after your discharge from the hospital. You should bring copies of your medical and/or cardiac preoperative evaluation and dental evaluation to this appointment if they have not already been faxed to our office. Upon arrival and check in at Pinehurst Surgical Clinic for your appointment with Michelle, one of our nurses will accompany you to one of our examination rooms for an anticipated minute appointment. During this appointment, please be prepared to complete specialized x- ray examination needed specifically for surgery purposes. Additionally, you will be accompanied to our Pinehurst Surgical Clinic laboratory for routine laboratory tests of your blood and urine. It is not necessary that you fast prior to your appointment with Michelle as the laboratory testing that will be completed does not require so. You will also undergo an electrocardiogram at this time (please inform us if you have undergone EKG testing by any other provider within the past six months and bring a copy of
9 this study with you to your appointment if you have). It is important that you come to your history and physical examination with the actual bottles of medications you are taking on a regular basis, including those used on an as needed basis, both prescription and over the counter. We will be carefully documenting the dosages of the medications you take including the time of day your medications are taken. Please do not bring a list of your medications, as we prefer the medications in their original bottles instead insuring accuracy. I would also like for you to compile a comprehensive list of all the medical providers you see including their name, and contact information. This will allow us to keep all of your medical providers updated with your progress before your hip replacement surgery, during your hospitalization and also during your recovery. Michelle will request this list at your pre- surgery appointment with her. At this appointment, Michelle will also provide you with individualized pre- surgery written instructions detailing any medications that need to be discontinued in preparation for surgery, medications that must be taken the morning of surgery and any other necessary instructions. She will also provide you with an application for a temporary handicapped license tag, which you will need for three to six months after your hip surgery. As part of our preoperative education program, we do encourage all patients scheduled for hip replacement to participate in a preoperative patient education class which is held at Moore Regional Hospital. Patients with MEDICARE A and B are required by our government to attend one preoperative class as of January 1, Although the class is voluntary, for all other patients, we feel strongly that this is a very important part of preparing for your surgery. The class will discuss in great detail what to bring to the hospital, what to expect during your hospitalization, what to expect during physical therapy, what to expect from discharge planning and what to expect after you are discharged from the hospital. This is a very helpful time to bring members of your family as well so that everyone can understand what is required to get the best possible result from your surgery. At this time, you will also discuss the nursing plan and philosophy for your care at First Health Moore Regional Hospital. These classes are typically held on Wednesday and Thursday afternoons from 1:00-3:30 pm.
10 Our preference is that you attend one class before your surgery date, if you are able. Michelle will provide you with a flyer detailing additional class information, she will also facilitate your class enrollment and even pre- register you for class should you have a date in mind. For those of you who are internet savvy, and have difficulty with travel distance, time and date constraints, the hospital does offer an online option/replacement for the onsite preoperative preparation class. If you are interested in viewing this online class rather than attending the onsite class, you can simply go to You will then click on Firsthealth A- Z located in the left side columns of the home page. Then click on the letter O, then on orthopedics on the next page. You will then see (at the left side margin) the icon Online hip and knee replacement classes. Simply click on the link and proceed. HOSPITALIZATION Most insurance plans do not approve hospital admittance prior to the surgery day, therefore, you will be admitted to the hospital the same day of surgery in most cases. At admission, if necessary, additional blood testing might be required. Renee Wood, our Surgery Coordinator, will call you one business day prior to your surgery date and inform you of your arrival time to Moore Regional Hospital Outpatient Registration located on Page Road. We do not assign surgery times for our patients as there are instances where certain surgeries may take longer than others. It is likely that you will wait a period of time between your arrival to the hospital and the start of your surgery. We advise that you bring a family member or friend to keep you company during this waiting period as well as some reading materials to help in passing the time. It is important that we have current, accurate contact information for you in order to facilitate the provision of information in a timely manner. Michelle will confirm your current phone number at the time of your pre- surgery appointment and also discuss the best methods of providing your arrival time to you (i.e. telephone vs. ).
11 You will find that the pre- medication process begins immediately upon hospital admission. We will be administering medications to prevent post- surgical nausea and pain. You will then be taken to the preoperative holding area in the operating room. This will allow for consultation with the anesthesiologist and starting of the intravenous line. At this point a preoperative sedative will be given to you by your anesthesiologist. In almost all cases, a spinal anesthetic is administered. You will be numb from the waist down. Although you may choose to be wide awake or we can sedate you as heavily as you would like so that you are completely relaxed and will not remember anything about the operation. This is safer than a general anesthetic and your recovery is more rapid. A general anesthetic is used in rare cases. Primary total hip replacement requires between one and two hours of surgery time, while a revision total hip replacement requires between two and four hours of surgery time. While you are in the operating room, your family will wait in the surgical waiting area or at home. As soon as surgery is completed, I will contact them in person or by telephone. You will be in the recovery room for one to three hours until the effect of the spinal anesthesia is worn off. Once that occurs and your vital signs are stable, you will be returned to your room on the orthopedic floor. Patients with severe cardiac problems may be monitored in the Intensive Care Unit overnight. After surgery, you will be able to move about the bed. You will not need to remain rigidly immobilized in one position. With the bed controls you may elevate the head of the bed or remain perfectly flat. At the time of your surgical procedure while the spinal anesthetic is still in effect, a catheter is inserted into your bladder. Therefore, the difficult task of climbing onto a bed pan during the first several days is not required. After you have been walking for one or two days, the catheter will be removed and you will be able to urinate on your own. It is also possible that you will come out of surgery with a drain from your replaced hip, although this is rare. If necessary, this drain would collect any blood that is lost from your hip after surgery for later re- infusion. If a drain were used it is typical that all drains be removed the day before hospital discharge. Most patients do
12 not come out of surgery with a drain from their hip simply because incision sizes are small enough that blood loss is minimal. With the assistance of our physical therapists, you will begin your bed exercises, standing and walking on either the day of surgery or on the first postoperative day, depending on the hour your surgery is completed. In addition to your twice daily physical therapy sessions, the therapists will instruct you on the hip precautions for prevention of hip dislocation. You will gradually increase your walking distance and frequency as tolerated. You are usually in the hospital for three days until you reach a level of independence following the surgery. When you are independent, you should be able to get in and out of bed by yourself and walk between 150 and 300 feet. If you meet these guidelines you will be able to return home. You should strive to go home. This will encourage independence. Home health care and home physical therapy will be arranged by a hospital discharge planner prior to discharge from the hospital. You should expect that once home a physical therapist will come to your home three to five times a week for the first week at home then three times per week for approximately two additional weeks to assist with your physical therapy regimen. It is also an option to forgo home physical therapy and replace home therapy with outpatient therapy instead. You would need to have someone to drive you to and from these outpatient therapy appointments. Your therapy will be tailored to the type of operation that you received. Regardless of the type of fixation used for your surgery, the majority of patients can be weight bearing as tolerated, which means you can put as much weight on the leg as you desire. Should unexpected bone fracture occur during surgery, there is the possibility you will have limited weight bearing for a short period of time, although this is not typical. While you are walking in the hospital, you will initially be using a walker but you can advance to the use of crutches if you can master the technique. It is your personal preference whether you go home on a walker or on crutches. Prior to the discharge from the hospital, the physical therapy and occupational therapy departments will be certain that you understand very clearly your discharge exercise program and have all the assistive devices
13 that will help you cope in the immediate postoperative period. You will be required to go home with the use of a walker for ambulation. In order to prevent blood clot formation you will be placed on some form of blood thinner. We will also have you continue a blood thinner at home for a period of time. However, if you do develop a blood clot in one or both of your legs you may need to stay in the hospital three to seven more days while you are placed on a stronger blood thinner for a longer period of time. The blood thinning will then be continued as an outpatient and be managed by your medical doctor, if necessary. By one to three days after surgery, which will be your time of hospital discharge, your incision should be healing well. You will not have staples in your incision after hip replacement as we choose, rather, to sew your wound closed using absorbable suture. Your incision will be evaluated approximately seven to ten days after hospital discharge at your first follow- up clinic appointment. When you go home you may still have some clear, yellow drainage (serous drainage). This is not an indication of any type of infection but just a part of the healing process in the fat below the skin level. This may continue from one to five days. After it stops you will be able to take a shower at home with the airstrip in place. When you are discharged you will have a prescription for a narcotic pain medication but you should be requiring less of the medication each day. You should moderate your activities to reduce the amount of stress that is put on the incision and muscles about the hip. This is the appropriate way to manage your pain after your discharge. It is common to have swelling in the leg, especially, if you are becoming more active in your activities at home. The one type of swelling that can be worrisome is swelling in the entire leg starting at the ankle or foot level. This is common when you sit for prolonged periods of time. If this occurs you need to spend less time sitting and more time lying down on the bed or couch with the leg elevated. If the swelling does not resolve significantly with this rest and elevation, you should contact me so that we might further evaluate this. You should stay on your crutches, cane or walker for the entire first
14 six weeks after the surgical procedure unless otherwise informed. I will only advance you to a single crutch or cane after you return to see me at your second postoperative visit six weeks following the surgery. FOLLOW- UP Once your hip is replaced, it is important to monitor closely the healing process in the first three to six months following the surgical procedure. It is also important to monitor the long- term fixation of the implant over a period of many years to be certain there is no adverse effect on the bone or any sign of loosening of the prosthesis. Therefore, the usual follow- up schedule involves your return to the office for examination and x- rays at the following times after the surgical procedure: two weeks, six weeks, six months, and one year. After the first year, you are seen on an annual basis. In some situations because of difficulty of travel, I can make arrangements for you to be seen by your local family physician who can obtain x- rays and send those to me for evaluation. Unfortunately, this is not the ideal situation. I will try to be as flexible as possible because I know travel is often quite difficult and expensive. PROPHYLACTIC ANTIBIOTICS Patients with hip replacements can develop infections of the joint in special circumstances. Any infection you might acquire in any other part of your body could potentially spread to your replaced hip. As a result, antibiotics should be taken before colonoscopy, urologic, and dental procedures. An instruction sheet has been prepared and will be given to you in your educational packet. PROBLEMS OR QUESTIONS If you have any concerns or questions about the scheduling or preoperative sequence of events, you should contact Renee Wood at She can answer questions about surgical scheduling, any insurance concerns or preparation for surgery. She can also help you after your discharge from the hospital with questions about your recovery and will forward any other specific questions to me or my Physician's assistant,
15 Michelle. If we are not in the office at the time of your call, they will make certain that we receive the message as soon as possible. Either myself or Michelle will return your phone call as soon as we are able. I want you to understand completely your disease process and the proposed surgery. It is best that you clearly understand all information about total hip replacement surgery. If you have any additional questions, please ask me when I see you prior to your admission to the hospital or at the time of your preoperative history and physical examination with Michelle. You may also contact Michelle via the internet at mmartinez@pinehurstsurgical.com. John R Moore, IV, M.D. Orthopedic and Joint Replacement Center Pinehurst Surgical Clinic 5 First Village Drive Pinehurst, N.C / FAX: SUGGESTED ADDITIONAL INTERNET RESOURCES
OUTPATIENT TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D.
 OUTPATIENT TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D. Since you have progressed to the point of serious consideration of total hip replacement, there is a great deal of information that is important
OUTPATIENT TOTAL HIP REPLACEMENT JOHN R. MOORE, IV, M.D. Since you have progressed to the point of serious consideration of total hip replacement, there is a great deal of information that is important
TOTAL KNEE REPLACEMENT JOHN R. MOORE, IV, M.D.
 TOTAL KNEE REPLACEMENT JOHN R. MOORE, IV, M.D. Since you have progressed to the point of serious consideration of total knee replacement, there is a great deal of information that is important for you
TOTAL KNEE REPLACEMENT JOHN R. MOORE, IV, M.D. Since you have progressed to the point of serious consideration of total knee replacement, there is a great deal of information that is important for you
Total Hip Replacement Surgery
 Total Hip Replacement Surgery On this page: Overview What is Total hip replacement (THA)? Anatomy Preparing for surgery The Operation Post-Operative Possible Complications Exercise Restrictions Overview
Total Hip Replacement Surgery On this page: Overview What is Total hip replacement (THA)? Anatomy Preparing for surgery The Operation Post-Operative Possible Complications Exercise Restrictions Overview
Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty
![Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty](/thumbs/90/102636395.jpg) Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Introduction Hip arthritis is a common problem, most often due to osteoarthritis. In hip arthritis affects a patient,
Vasu Pai D orth, MS, National Board [orth],mch, FRACS, FICMR Total Hip Arthroplasty Introduction Hip arthritis is a common problem, most often due to osteoarthritis. In hip arthritis affects a patient,
TOTAL HIP ARTHROPLASTY (Total Hip Replacement)
 (Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
(Total Hip Replacement) The Hip Joint The hip is a ball and socket joint. The joint is formed by the head of the femur (thighbone) and the acetabulum (pelvis). The bones are coated in cartilage, which
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
Total hip replacement
 Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Total hip replacement 2 Hip pain Arthritis is the leading cause of disability in the United States, and the most frequent cause of discomfort and chronic hip pain. In fact, it s estimated that 1 in 5 people
Total Hip Replacement
 PATIENT EDUCATION Total Hip Replacement A guide to understanding total hip replacement surgery, featuring The George Archer Story. BACK TO MOBILITY George Archer s Personal Adventure On April16, 1996,
PATIENT EDUCATION Total Hip Replacement A guide to understanding total hip replacement surgery, featuring The George Archer Story. BACK TO MOBILITY George Archer s Personal Adventure On April16, 1996,
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 12 RISKS AND COMPLICATIONS - TOTAL HIP REPLACEMENT Index Pages INTRODUCTION 3 (1) ANAESTHETIC AND MEDICAL: 4 (2) BLOOD
RISKS AND COMPLICATIONS
 PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
PATIENT INFORMATION SHEET RISKS AND COMPLICATIONS TOTAL HIP REPLACEMENT Page 1 of 8 INTRODUCTION A hip replacement is an extremely successful operation. At least 95% of patients are satisfied with their
Total Hip Replacement. Find out why Total Hip Replacement may be right for you.
 Total Hip Replacement Find out why Total Hip Replacement may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of hip anatomy, arthritis and total hip arthroplasty.
Total Hip Replacement Find out why Total Hip Replacement may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of hip anatomy, arthritis and total hip arthroplasty.
A Patient s Guide to Artificial Joint Replacement of the Ankle
 A Patient s Guide to Artificial Joint Replacement of the Ankle Introduction Surgery to replace the ankle joint with an artificial joint (called ankle arthroplasty) is becoming more common. This surgery
A Patient s Guide to Artificial Joint Replacement of the Ankle Introduction Surgery to replace the ankle joint with an artificial joint (called ankle arthroplasty) is becoming more common. This surgery
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide
 Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
Dr. Roy Davidovitch Next Day Discharge Total Hip Replacement Recovery Guide PREOPERATIVE INSTRUCTIONS Your Preadmission Testing Visit About 2 weeks prior to your surgical date, you will be required to
In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components.
 Total Hip Replacement In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components. The damaged femoral head is removed
Total Hip Replacement In a total hip replacement (also called total hip Arthroplasty), the damaged bone and cartilage is removed and replaced with prosthetic components. The damaged femoral head is removed
About Hip Replacements
 Why have I received this leaflet? About Hip Replacements You have decided or are considering undergoing total hip replacement surgery. I have discussed with you in clinic that hip replacements are successful
Why have I received this leaflet? About Hip Replacements You have decided or are considering undergoing total hip replacement surgery. I have discussed with you in clinic that hip replacements are successful
introduction jointunderstanding benefits of knee-replacement surgery
 introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
introduction When knee pain becomes so severe that drugs do not provide relief or when knee problems make daily activities painful, difficult, or even impossible, surgeons can sometimes replace the damaged
FAQ s: Hip Arthroscopy with Dr. Boyle
 AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
AUT Millennium, 17 Antares Place Telephone: 09 281 6733 Mairangi Bay, Auckland 0632 Fax: 09 479 3805 www.matthewboyle.co.nz office@matthewboyle.co.nz FAQ s: Hip Arthroscopy with Dr. Boyle What is hip arthroscopy?
THE REVERSE SHOULDER REPLACEMENT
 THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
THE REVERSE SHOULDER REPLACEMENT The Reverse Shoulder Replacement is a newly approved implant that has been used successfully for over ten years in Europe. It was approved by the FDA for use in the U.S.A.
YOUR TOTAL HIP REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE
 YOUR TOTAL HIP REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE IMPORTANT. PLEASE NOTE. This brochure offers a brief overview of hip anatomy, arthritis and hip replacement surgery. The
YOUR TOTAL HIP REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE IMPORTANT. PLEASE NOTE. This brochure offers a brief overview of hip anatomy, arthritis and hip replacement surgery. The
TOTAL HIP ARTHROPLASTY (hip replacement)
 TOTAL HIP ARTHROPLASTY (hip replacement) The condition The hip is a ball and socket joint. The ball is formed by the head of the thighbone (femur) which fits snugly into the cup shaped bone in the pelvis
TOTAL HIP ARTHROPLASTY (hip replacement) The condition The hip is a ball and socket joint. The ball is formed by the head of the thighbone (femur) which fits snugly into the cup shaped bone in the pelvis
YOUR TOTAL HIP REPLACEMENT SURGERY
 YOUR TOTAL HIP REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE Exactech_030H Rev A_Total Hip Replacement Surgery_PRINT.indd 1 IMPORTANT. PLEASE NOTE. This brochure offers a brief overview
YOUR TOTAL HIP REPLACEMENT SURGERY STEPS TO RETURNING TO A LIFESTYLE YOU DESERVE Exactech_030H Rev A_Total Hip Replacement Surgery_PRINT.indd 1 IMPORTANT. PLEASE NOTE. This brochure offers a brief overview
Anterior Approach to Hip Replacement Surgery
 Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Anterior Approach to Hip Replacement Surgery Introduction When debilitating pain and stiffness in your hip limits your daily activities, you may need a total hip replacement. The development of total hip
Total Shoulder Replacement Patient Guide
 About Your Surgery and Recovery WELCOME This booklet has been designed to answer your questions about what to expect if you will need surgery. I truly hope that this will make your surgery an easier and
About Your Surgery and Recovery WELCOME This booklet has been designed to answer your questions about what to expect if you will need surgery. I truly hope that this will make your surgery an easier and
Total Hip Replacement
 Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Please contactmethroughthegoldcoasthospitaswityouhaveanyproblemsafteryoursurgery. Dr. Benjamin Hewitt Orthopaedic Surgeon Total Hip Replacement The hip joint is a ball and socket joint that connects the
Femoral Neck (Hip) Fracture
 Patient Information Leaflet Femoral Neck (Hip) Fracture Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another
Patient Information Leaflet Femoral Neck (Hip) Fracture Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another
The Shoulder. The Shoulder Joint:
 The Shoulder The board certified physicians and surgeons at Orthopaedic Associates of Central Texas (OACT) are leaders in caring for the joints of the body. The shoulder joint is a complex and dynamic
The Shoulder The board certified physicians and surgeons at Orthopaedic Associates of Central Texas (OACT) are leaders in caring for the joints of the body. The shoulder joint is a complex and dynamic
Your Care Team. Therapy staff (PT, PTA, OT, tech) Orthopedic surgeon. Case management staff (RN, social worker) Physician s assistant.
 Your Care Team You are not alone as you consider total joint replacement surgery. You are part of a team of dedicated health professionals who will be on your side throughout the entire process. You may
Your Care Team You are not alone as you consider total joint replacement surgery. You are part of a team of dedicated health professionals who will be on your side throughout the entire process. You may
About Knee Replacements
 Why have I received this leaflet? About Knee Replacements You have decided or are considering undergoing total knee replacement surgery. I will have discussed with you in clinic that knee replacements
Why have I received this leaflet? About Knee Replacements You have decided or are considering undergoing total knee replacement surgery. I will have discussed with you in clinic that knee replacements
TOTAL KNEE REPLACEMENT. Surgical Treatment for Advanced Pain due to Arthritis. Dr. Adam S. Rosen
 TOTAL KNEE REPLACEMENT Surgical Treatment for Advanced Pain due to Arthritis Dr. Adam S. Rosen What is Arthritis? How do you treat Arthritis? Arthritis is an inflammation of the joint due to loss of cartilage.
TOTAL KNEE REPLACEMENT Surgical Treatment for Advanced Pain due to Arthritis Dr. Adam S. Rosen What is Arthritis? How do you treat Arthritis? Arthritis is an inflammation of the joint due to loss of cartilage.
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
A Patient s Guide to Arthroscopy of the Hip Introduction A hip arthroscopy is a procedure where a small video camera attached to a fiberoptic lens is inserted into the hip joint to allow a surgeon to see
Your Practice Online
 P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on hip resurfacing or arthritis management. All decisions about
P R E S E N T S Your Practice Online Disclaimer This information is an educational resource only and should not be used to make a decision on hip resurfacing or arthritis management. All decisions about
Total Knee Replacement
 Total Knee Replacement Learn About: How Your Knee Works Knee Related Problems Candidates for Knee Replacement Surgery What to Expect From Your Artificial Knee Preparing for Knee Replacement Your Surgery
Total Knee Replacement Learn About: How Your Knee Works Knee Related Problems Candidates for Knee Replacement Surgery What to Expect From Your Artificial Knee Preparing for Knee Replacement Your Surgery
TOTAL KNEE ARTHROPLASTY (Total Knee Replacement) The Knee Joint
 (Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
(Total Knee Replacement) The Knee Joint The knee is a hinge joint, formed by the end of the femur (thighbone) and the end of the tibia (shinbone). The bones are coated in cartilage, which acts as a cushion
Knee Replacement Patient Information
 Knee Replacement Patient Information This information sheet is designed to help you to understand what a knee replacement involves. I perform knee replacements frequently, several times each week, and
Knee Replacement Patient Information This information sheet is designed to help you to understand what a knee replacement involves. I perform knee replacements frequently, several times each week, and
Total Knee Replacement: Your Guide to Preparation and Recovery
 Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Patient Education Shoulder Arthroplasty
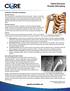 Explanation of Procedure and Diagnosis Shoulder Arthritis The shoulder joint is essentially a ball and socket joint. However, unlike the ball and socket joint of the hip, the shoulder has much greater
Explanation of Procedure and Diagnosis Shoulder Arthritis The shoulder joint is essentially a ball and socket joint. However, unlike the ball and socket joint of the hip, the shoulder has much greater
A Patient s Guide to Partial Knee Resurfacing
 A Patient s Guide to Partial Knee Resurfacing Surgical Outcomes System (SOS ) www.orthoillustrated.com OrthoIllustrated is a leading Internet-based resource for patient education. Please visit this website
A Patient s Guide to Partial Knee Resurfacing Surgical Outcomes System (SOS ) www.orthoillustrated.com OrthoIllustrated is a leading Internet-based resource for patient education. Please visit this website
Patient Information for Consent
 Patient Information for Consent ER OS01 Total Hip Replacement Enhanced Recovery Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI
Patient Information for Consent ER OS01 Total Hip Replacement Enhanced Recovery Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI
Hip Fractures. Anatomy. Causes. Symptoms
 Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
Hip Fractures A hip fracture is a break in the upper quarter of the femur (thigh) bone. The extent of the break depends on the forces that are involved. The type of surgery used to treat a hip fracture
A Patient s Guide to Artificial Joint Replacement of the Hip, Anterior Approach
 A Patient s Guide to Artificial Joint Replacement of the Hip, Anterior Approach 2321 Coronado Idaho Falls, ID 83404 Phone: 208-227-1100 jpond@summitortho.net DISCLAIMER: The information in this booklet
A Patient s Guide to Artificial Joint Replacement of the Hip, Anterior Approach 2321 Coronado Idaho Falls, ID 83404 Phone: 208-227-1100 jpond@summitortho.net DISCLAIMER: The information in this booklet
Physiotherapy Services. Physiotherapy Guide. Hip Replacement
 Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Physiotherapy Services Physiotherapy Guide to Hip Replacement AGH 01535 293656 Bingley Hospital 01274 563438 Ilkley Coronation Hospital 01943 609666 ext 241 Skipton General Hospital 01756 701726 Settle
Patient Information for Consent
 Patient Information for Consent OS01 Total Hip Replacement Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI hospital on:...... Get
Patient Information for Consent OS01 Total Hip Replacement Expires end of February 2017 Issued June 2016 Local information If you need any more information please contact your BMI hospital on:...... Get
UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION
 UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION The following information is to help you understand what is going to happen when you have a UKR. It is only a guide and some aspects will vary
UNICOMPARTMENTAL KNEE REPLACEMENT (UKR) PATIENT INFORMATION The following information is to help you understand what is going to happen when you have a UKR. It is only a guide and some aspects will vary
Patient Education GANZ PERIACETABULAR OSTEOTOMY
 GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
GANZ PERIACETABULAR OSTEOTOMY Thank you for the opportunity of allowing us to take care of you. We understand that there are many questions regarding your hip surgery for you and your parents. This information
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement
 Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement This is a general information packet for patients undergoing Total Knee Replacement. Osteoarthritis (OA) is
Brian P. McKeon MD Jason D. Rand, PA-C, PT Patient Information Sheet: Total Knee Replacement This is a general information packet for patients undergoing Total Knee Replacement. Osteoarthritis (OA) is
Advantage Orthopaedics, P.C.
 TOTAL HIP REPLACEMENT Whether you have just begun exploring treatment options or have already decided with your orthopaedic surgeon to undergo hip replacement surgery, this booklet will help you understand
TOTAL HIP REPLACEMENT Whether you have just begun exploring treatment options or have already decided with your orthopaedic surgeon to undergo hip replacement surgery, this booklet will help you understand
Total Hip Replacement
 AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
AFFIX PATIENT DETAIL STICKER HERE and on each subsequent page Forename.. Male Female Surname Hospital Number... Consultant D.O.B.././ OPERATION: Total Hip Replacement PROCEDURE: The hip joint is a ball
Dynamic hip screw (sliding hip screw)
 Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Patient Information Physiotherapy after Total Hip Replacement Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you
Total Hip Replacement: Your Guide to Preparation and Recovery
 Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Subcapital hip fracture surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Subcapital hip fracture surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
PATIENT HANDBOOK AND JOURNAL FAQ
 PATIENT HANDBOOK AND JOURNAL FAQ FREQUENTLY ASKED QUESTIONS What is the recovery time for a total hip replacement? This generally takes about three months. Everyone heals at a different pace so this time
PATIENT HANDBOOK AND JOURNAL FAQ FREQUENTLY ASKED QUESTIONS What is the recovery time for a total hip replacement? This generally takes about three months. Everyone heals at a different pace so this time
It s your knee. Help keep it that way PERSONALIZED TOTAL KNEE IMPLANTS
 It s your knee Help keep it that way PERSONALIZED TOTAL KNEE IMPLANTS Osteoarthritis the disease Osteoarthritis (OA) is the most common form of arthritis, affecting tens of millions of people worldwide.
It s your knee Help keep it that way PERSONALIZED TOTAL KNEE IMPLANTS Osteoarthritis the disease Osteoarthritis (OA) is the most common form of arthritis, affecting tens of millions of people worldwide.
Hallux Rigidus. Normal. Normal Arthritis Arthritis
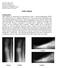 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Hallux Rigidus Explanation: Hallux Rigidus is characterized as degeneration
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Hallux Rigidus Explanation: Hallux Rigidus is characterized as degeneration
Arthroscopy for Hip Osteoarthritis
 Appendix: Script #1: Health scenarios Arthroscopy for Hip Osteoarthritis Introduction Hip arthroscopy is a surgical procedure that gives doctors a clear view of the inside of the hip joint. This helps
Appendix: Script #1: Health scenarios Arthroscopy for Hip Osteoarthritis Introduction Hip arthroscopy is a surgical procedure that gives doctors a clear view of the inside of the hip joint. This helps
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers
 CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
CEC ARTICLE: Special Medical Conditions Part 3: Hip and Knee Replacement C. Eggers Joint replacement surgery removes a damaged joint and replaces it with a prosthesis or artificial joint. The purpose of
Edward J. Whelan, III, MD
 What You Need To Know Anterior Approach Hip Replacement Over 2500 anterior approach total hip replacement surgeries performed Edward J. Whelan, III, MD Anterior Hip Replacement Hip Resurfacing Arthroplasty
What You Need To Know Anterior Approach Hip Replacement Over 2500 anterior approach total hip replacement surgeries performed Edward J. Whelan, III, MD Anterior Hip Replacement Hip Resurfacing Arthroplasty
THE RECOVERY PROCESS
 THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
THE RECOVERY PROCESS PART II If you're considering a major Orthopaedic surgical procedure to relieve pain in your back, knee, or hip, there's a lot to consider. These procedures, while common, do come
Total Hip Replacement. Find out why the Anterior Approach may be right for you.
 Total Hip Replacement Find out why the Anterior Approach may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of the Direct Anterior Approach to total hip arthroplasty.
Total Hip Replacement Find out why the Anterior Approach may be right for you. UNDERSTANDING TOTAL HIP REPLACEMENT This brochure offers a brief overview of the Direct Anterior Approach to total hip arthroplasty.
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
Hemiarthroplasty (half hip replacement)
 Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
ARE YOU HAVING HIP OR KNEE REPLACEMENT SURGERY?
 ARE YOU HAVING HIP OR KNEE REPLACEMENT SURGERY? GET TO KNOW HOW THIS LATEST-GENERATION BLOOD THINNER HELPS PROTECT YOU FROM BLOOD CLOTS. Once I got the facts, my doctor and I chose XARELTO Do not stop
ARE YOU HAVING HIP OR KNEE REPLACEMENT SURGERY? GET TO KNOW HOW THIS LATEST-GENERATION BLOOD THINNER HELPS PROTECT YOU FROM BLOOD CLOTS. Once I got the facts, my doctor and I chose XARELTO Do not stop
FOOT AND ANKLE ARTHROSCOPY
 FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
FOOT AND ANKLE ARTHROSCOPY Information for Patients WHAT IS FOOT AND ANKLE ARTHROSCOPY? The foot and the ankle are crucial for human movement. The balanced action of many bones, joints, muscles and tendons
Lesser Toe Correction
 Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Lesser Toe Correction Lesser toe deformities are classified
Richard M. Marks, MD Professor and Director Division of Foot and Ankle Department of Orthopaedic Surgery Medical College of Wisconsin Explanation: Lesser Toe Correction Lesser toe deformities are classified
Complications of Treatment: Nonsurgical and Surgical
 Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Complications of Treatment: Nonsurgical and Surgical Whenever orthopedic surgeons discuss a treatment with patients we must always consider the risks and complications of any treatment we recommend. Part
Reverse Total Shoulder Replacement
 Reverse Total Shoulder Replacement DESCRIPTION The normal shoulder is made up of a ball and socket joint. The ball is called the humeral head and the socket is called the glenoid. Shoulder anatomy Normal
Reverse Total Shoulder Replacement DESCRIPTION The normal shoulder is made up of a ball and socket joint. The ball is called the humeral head and the socket is called the glenoid. Shoulder anatomy Normal
Dr. Clark s Frequently Asked Questions
 Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
Dr. Clark s Frequently Asked Questions ACTIVITY RESTRICTIONS: Unlike a traditional hip replacement, there are no formal hip precautions after anterior hip replacement. Unless I tell you otherwise, you
Unicompartmental knee replacement. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Unicompartmental knee replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Unicompartmental knee replacement Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the
Periacetabular Osteotomy (PAO)
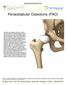 Periacetabular Osteotomy (PAO) At the top of your thigh bone, the femur, is a ball shaped structure called the femoral head, which fits in a socket in the pelvis, called the acetabulum. Both of these structures
Periacetabular Osteotomy (PAO) At the top of your thigh bone, the femur, is a ball shaped structure called the femoral head, which fits in a socket in the pelvis, called the acetabulum. Both of these structures
Pa#ent Informa#on for Consent
 Pa#ent Informa#on for Consent ER_OS02 Total Knee Replacement Enhanced Recovery Expires end of November 2018 Local Informa#on For further informa0on locally you can contact the Pa0ent Advice & Liaison Service
Pa#ent Informa#on for Consent ER_OS02 Total Knee Replacement Enhanced Recovery Expires end of November 2018 Local Informa#on For further informa0on locally you can contact the Pa0ent Advice & Liaison Service
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Bunion Surgery Most people with bunions find pain relief with simple treatments to reduce pressure on the big toe, such as wearing wider shoes or using pads in their shoes. However, if these measures do
Fracture Surgery. Post-Operative Care. And. Rehabilitation Protocol
 PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
PATIENT NAME: Fracture Surgery Post-Operative Care And Rehabilitation Protocol After Surgery Care and Information Many questions arise during the first week after surgery. There are many new sensations
A Patient s Guide to Arthroscopy of the Ankle
 A Patient s Guide to Arthroscopy of the Ankle 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete
A Patient s Guide to Arthroscopy of the Ankle 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources. It may not be complete
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
Knee Replacement , The Patient Education Institute, Inc. op Last reviewed: 06/01/2017 1
 Knee Replacement Introduction Severe arthritis in the knee can lead to serious pain and loss of motion. Health care providers may recommend surgery for people suffering from severe arthritis in the knee.
Knee Replacement Introduction Severe arthritis in the knee can lead to serious pain and loss of motion. Health care providers may recommend surgery for people suffering from severe arthritis in the knee.
TOTAL HIP REPLACEMENT Doug Thompson, MD PROCEDURE The purpose of the total hip replacement procedure is to replace diseased worn joint cartilage with
 PROCEDURE The purpose of the total hip replacement procedure is to replace diseased worn joint cartilage with metal and plastic to reduce or eliminate pain, decrease deformity, and improve function. An
PROCEDURE The purpose of the total hip replacement procedure is to replace diseased worn joint cartilage with metal and plastic to reduce or eliminate pain, decrease deformity, and improve function. An
While complications from surgery are uncommon some can be serious and may include:
 PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
PROCEDURE A Cervical Laminectomy is usually performed for spinal cord compression from cervical arthritis, nerve root compression from a cervical disc protrusion, or for an arthritic spur. These are painful
TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP
 TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP By John T. Dearborn, M.D. Please read this pamphlet before your visit so that we can answer any questions that you have during our
TOTAL HIP REPLACEMENT: MODERN SURGERY FOR SEVERE ARTHRITIS OF THE HIP By John T. Dearborn, M.D. Please read this pamphlet before your visit so that we can answer any questions that you have during our
Activities After Knee Replacement
 Activities After Knee Replacement This article is also available in Spanish: Actividades posteriores a un remplazo de rodilla (Activities After Knee Replacement) (topic.cfm?topic=a00759). After having
Activities After Knee Replacement This article is also available in Spanish: Actividades posteriores a un remplazo de rodilla (Activities After Knee Replacement) (topic.cfm?topic=a00759). After having
Micro-Posterior Total Hip Technique. It s possible to walk within hours of surgery. Body Text
 Title Text SuperPath Micro-Posterior Total Hip Technique It s possible to walk within hours of surgery. Body Text Title Text Body Text Every patient is different, and individual results will vary. There
Title Text SuperPath Micro-Posterior Total Hip Technique It s possible to walk within hours of surgery. Body Text Title Text Body Text Every patient is different, and individual results will vary. There
Patient Education Total Knee Arthroplasty
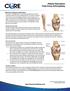 Explanation of Diagnosis and Procedure The knee is the largest joint in the body. Normal knee function is required to perform most everyday activities. The knee is made up of the lower end of the thighbone
Explanation of Diagnosis and Procedure The knee is the largest joint in the body. Normal knee function is required to perform most everyday activities. The knee is made up of the lower end of the thighbone
Knee MPFL Reconstruction FAQ
 Knee MPFL Reconstruction FAQ Ryan W. Hess, MD Office: 763-302-2223 Fax: 763-302-2402 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? MPFL stands for Medial Patellofemoral Ligament. This
Knee MPFL Reconstruction FAQ Ryan W. Hess, MD Office: 763-302-2223 Fax: 763-302-2402 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? MPFL stands for Medial Patellofemoral Ligament. This
A Patient s Guide. ACL Injury: Ø Frequently asked questions on injury, Ø Preoperative and postoperative. surgery and recovery.
 ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
ACL Injury: A Patient s Guide Ø Frequently asked questions on injury, surgery and recovery Ø Preoperative and postoperative guidelines Mia S. Hagen, M.D. Assistant Professor Department of Orthopaedics
Understanding Total Hip Replacement
 Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Western Orthopaedics Denver, Colorado Introduction This is designed to provide you with a better understanding
Understanding Total Hip Replacement Brian J. White MD Orthopaedic Specialist in Disorders of the Hip Western Orthopaedics Denver, Colorado Introduction This is designed to provide you with a better understanding
The S.T.A.R. Scandinavian Total Ankle Replacement. Patient Information
 The S.T.A.R. Scandinavian Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please
The S.T.A.R. Scandinavian Total Ankle Replacement Patient Information Patient Information This patient education brochure is presented by Small Bone Innovations, Inc. Patient results may vary. Please
Unicompartmental Knee Resurfacing
 Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Disclaimer This movie is an educational resource only and should not be used to manage knee pain. All decisions about the management of knee pain must be made in conjunction with your Physician or a licensed
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
ADULT SPINAL DEFORMITY SURGERY
 PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
PROCEDURE Spinal deformity correction surgery involves many techniques to correct the scoliosis, kyphosis, or other deformities of your spine to a more normal alignment. During the procedure, your surgeon
Integra. Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION
 Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
Integra Salto Talaris Total Ankle Prosthesis PATIENT INFORMATION Fibula Articular Surface Lateral Malleolus Tibia Medial Malleolus Talus Anterior view of the right ankle region Talo-fibular Ligament Calcaneal
ACL RECONSTRUCTION. Date of Surgery. Please bring this booklet the day of your surgery. QHC#65
 ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
ACL RECONSTRUCTION Date of Surgery Please bring this booklet the day of your surgery. QHC#65 The ACL (Anterior Cruciate Ligament) is the major stabilizing ligament of the knee. The ACL is located in the
Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Patellar Tendon / Quad Tendon Repair Surgery Discharge Instructions
A Patient s Guide to Arthroscopy of the Hip
 A Patient s Guide to Arthroscopy of the Hip 6767 Lake Woodlands Drive, Suite F, The Woodlands, TX 77382 20639 Kuykendahl Road, Suite 200, Spring, TX 77379 The Woodlands & Spring, TX. DISCLAIMER: The information
A Patient s Guide to Arthroscopy of the Hip 6767 Lake Woodlands Drive, Suite F, The Woodlands, TX 77382 20639 Kuykendahl Road, Suite 200, Spring, TX 77379 The Woodlands & Spring, TX. DISCLAIMER: The information
Can your body keep up with your lifestyle?
 Can your body keep up with your lifestyle? It s Possible to Walk within Hours of Surgery In recent years, hip replacement surgery has quietly entered a new era. The concept of tissue-sparing or minimally
Can your body keep up with your lifestyle? It s Possible to Walk within Hours of Surgery In recent years, hip replacement surgery has quietly entered a new era. The concept of tissue-sparing or minimally
The aim of this booklet is to provide you with information about your operation and the treatment you will receive.
 Patient Information Physiotherapy after Hip Resurfacing Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you will
Patient Information Physiotherapy after Hip Resurfacing Physiotherapy Department Introduction The aim of this booklet is to provide you with information about your operation and the treatment you will
Total Knee Replacement
 Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to feel pain
Total Knee Replacement If your knee is severely damaged by arthritis or injury, it may be hard for you to perform simple activities, such as walking or climbing stairs. You may even begin to feel pain
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you.
 Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
Mitral Clip Procedure You have been referred to the Hamilton General Hospital to assess if having your mitral heart valve repaired with a mitral clip is right for you. 2 Mitral Clip Procedure What is mitral
A Guide to Common Ankle Injuries
 A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
A Guide to Common Ankle Injuries Learn About: Common ankle injuries Feet and Ankle Diagnosis and Treatment Ankle exercises Beginning your recovery Frequently asked questions Do s and Don t s Arthroscopy
Knee ACL Reconstruction Allograft FAQ
 Knee ACL Reconstruction Allograft FAQ Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? ACL reconstruction
Knee ACL Reconstruction Allograft FAQ Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 Twitter: RyanHessMD Q: WHAT IS ACCOMPLISHED DURING THE PROCEDURE? ACL reconstruction
