Diabetic foot ulcer and poor compliance: How would you treat?
|
|
|
- Amelia Banks
- 5 years ago
- Views:
Transcription
1 Jessica Farnsworth, MD Department of Family Medicine, University of Nebraska Medical Center, Omaha Paul Paulman, MD University of Nebraska College of Medicine, Department of Family Medicine, Omaha Diabetic foot ulcer and poor compliance: How would you treat? A 45-year-old Caucasian man, M.N., visits his family physician for a follow-up examination of the ulcer on his right foot. Today the patient reports that his foot feels more swollen. He has no pain, fever, or chills. Nine months ago M.N. began to exhibit a calloused, erythematous area on his right foot that subsequently became edematous and ulcerated. He was treated with cefuroxime (Ceftin) for 10 days and encouraged to stay off his feet. In a subsequent visit it was decided to refer him to a podiatrist and also to help him procure shoe inlays. The appearance of his foot infection improved for a while, then worsened. The patient was on his feet most hours of each day at his job as a baker, and this slowed his healing. His physician then treated him with cephalexin (Keflex), and he began to wear a cam walker. He failed to improve and, in fact, worsened. He was referred to an orthopedist. Plain films of his foot showed soft tissue ulceration without definite evidence of osteomyelitis. He was referred to the wound care clinic and began using Duoderm. He received yet another course of antibiotics. Wound cultures were not obtained. FEATURE EDITORS Audrey Paulman, MD, MMM, and Paul Paulman, MD, University of Nebraska College of Medicine, Omaha CORRESPONDING AUTHOR Paul M. Paulman, MD, University of Nebraska College of Medicine, Department of Family Medicine, Nebraska Medical Center, Omaha, NE ppaulman@unmc.edu Other medical history Diabetes mellitus type II Diabetic retinopathy Hypertension Erectile dysfunction Obesity Pes planus Family history Diabetes and hypertension in father and paternal grandmother. Father had 2 myocardial infarctions and died at age 62. Mother is healthy. Sister has borderline diabetes. Social history Nonsmoker 4 to 5 beers per week Divorced Works as a baker Review of systems Negative except for increased swelling of right foot Physical exam Alert male in no distress Blood pressure 135/68 mm Hg, temperature 37.5 C, respiratory rate 14, heart rate 80, weight 236 pounds Heart, lung, and abdominal exam unremarkable Right 3rd toe has erythema at the metatarsophalangeal joint, with a draining ulcer on the plantar surface. Foot is edematous with erythema spreading proximally toward lower extremity. Erythema is <2 cm from ulcer rim. Pedal pulses are 1+, and capillary refill is <2 seconds. Monofilament testing reveals insensitivity at more than 4 sites. 768 VOL 54, NO 9 / SEPTEMBER 2005 THE JOURNAL OF FAMILY PRACTICE
2 Diabetic foot ulcer and poor compliance Q: What is the differential diagnosis of the patient s symptoms? A: Important elements of the history and exam Assess vascular integrity. Arterial insufficiency is suggested by a history of cardiac or cerebrovascular disease, leg claudication, impotence, or pain in the distal foot when the patient is supine. Exam may reveal diminished or absent pulses, pallor on elevation, redness of the foot on lowering the leg, delayed capillary refill in toes, and thickened nails or absence of toe hair. With diabetes or renal impairment, the pulse exam may be unreliable due to arterial calcification. Helpful studies may include segmental limb pressures, pulse-volume wave form, transcutaneous oxygen pressure, and ankle brachial index (which can be normal with significant calcinosis). Obtain a vascular surgery consultation immediately if you suspect arterial insufficiency, as revascularization may be necessary. 1 Evaluate for musculoskeletal problems. Examine gait, look for foot deformities, and test joint range of motion. If a mechanical basis of the ulceration is found, eliminate or reduce foot pressure with shoes, inserts, orthoses, etc. Reconstructive foot surgery may be an option for some patients. Gauge neurologic status. Most foot ulcers develop because of loss of protective sensation; therefore, screen all patients with diabetes annually for loss of protective sensation, using a 10-g nylon monofilament. Press the monofilament against the plantar skin until it buckles, hold it there for 1 second, and remove it. 2 The neurologic exam can also include testing for motor strength, deeptendon reflexes, and vibratory (128-Hz tuning fork), proprioceptive, and protective sensation. Measure the wound, watch for infection. When examining an ulcer, assess location, size, and depth. When caring for wounds, document at each visit the length and width of the wound. 3 Note any signs of infection (warmth, redness, pain, tenderness, induration, pus) or gangrene. Observe for fever, chills, and leukocytosis, but do not rely on systemic symptoms as indicators of infection. Assess the severity of infection, and explore the wound for foreign or necrotic material with a sterile metal instrument. Examine toenails for fungal infection, as this may be a significant contributor to the initiation and continuation of a foot ulcer. Callus formation, especially with hemorrhage, may be evidence of an impending ulcer. 3 M.N. s physician was increasingly concerned about the lack of healing of his ulcer. The differential diagnosis for this patient s swollen foot includes cellulitis, osteomyelitis, gout, foreign body, arthritis, trauma, deep venous thrombosis, pseudogout, and venous insufficiency. Many of these were excluded by the physical exam. A bone scan was ordered. Test for loss of protective sensation, using a 10-g nylon monofilament Q: What are the signs and symptoms of a severely infected diabetic foot ulcer? A: VOL 54, NO 9 / SEPTEMBER
3 TABLE 1 Vascular: arterial insufficiency or venous hypertension Neurologic: sensory, motor, or autonomic neuropathy Anatomical: altered biomechanics, limited joint mobility, bony deformity Infections Trauma Diabetes Risk factors predisposing to foot ulcers and inhibiting healing Referral to plastic surgeon When M.N. returns to the clinic with worsening drainage, edema, and spreading erythema, the decision is made to admit him to the hospital, start intravenous ampicillin/sulbactam (Unasyn) and ciprofloxacin (Cipro), and consult with a plastic surgeon. Following the examination and review of the bone scan results, which show osteomyelitis, the surgeon recommends surgical therapy of the affected toe. He advocates aggressive debridement, and also thinks that this wound could require a staged surgical approach or amputation. Q: Are there other laboratory or imaging studies you would like to obtain? A: Debride nonviable, infected tissue to expose healthy, bleeding soft tissue Further primary care evaluation Laboratory: Complete blood count, normal Erythrocyte sedimentation rate (ESR), 38 C-reactive protein (CRP), 2.1 Lipid panel: HDL 32 mg/dl, LDL 96 mg/dl, triglycerides 116 mg/dl Hemoglobin A1c, 6.0 Details of foot ulcers Statistics About 50% to 60% of serious foot infections are complicated by osteomyelitis, and 10% to 20% of mild to moderate infections likely involve the bone. Twenty-five percent of foot infections in persons with diabetes will spread to subcutaneous tissues or bone. Up to 50% of those with a foot infection will experience a recurrence within a few years. 2 Approximately 10% to 30% with a diabetic foot ulcer will eventually require amputation. Infected foot ulcers precede 60% of amputations. Two thirds of patients with a diabetic foot ulcer have peripheral vascular disease, and 80% have lost protective sensation. Infections most commonly involve the forefoot, usually plantar surface. 2 Pathophysiology Ulcers develop from breaks in the dermal barrier with subsequent erosion of subcutaneous tissue. Healing is inhibited when wound-repair mechanisms are corrupted by impaired perfusion, infection, or 770 VOL 54, NO 9 / SEPTEMBER 2005 THE JOURNAL OF FAMILY PRACTICE
4 Diabetic foot ulcer and poor compliance repeated trauma. Ulceration progresses due to impaired arterial supply, neuropathy, or musculoskeletal deformities. 1 Risk of ulceration correlates with number of risk factors. The risk is increased by 1.7 in persons with isolated peripheral neuropathy (TABLE 1), by 12 in those with neuropathy and foot deformity, and by 36 in those with peripheral neuropathy, deformity, and previous amputation. 1 Pathology usually mixed. The feet have sensory and motor neuropathies that cause the patient to put abnormal stresses on them, resulting in trauma that may lead to infection. Immunologic impairment due to hyperglycemia also plays a role; this can include reduced function of neutrophils, monocytes, and complement. Skin and nail disorders are more common among persons with diabetes than in the general population, and these may also increase the rate of infection. 2 TABLE 2 Clinical characteristics of a severe infection Acute or rapidly progressive Penetrating to subcutaneous tissues or involving fascia, muscle, joint, bone Extensive cellulitis (>2 cm around ulcer rim) Signs of inflammation, crepitus, bullae, necrosis, gangrene Systemic signs: fever, chills, hypotension, confusion, volume depletion, leukocytosis Metabolic abnormalities: severe hyperglycemia, acidosis, azotemia, electrolyte abnormalities Absent pulses Q: What are the patient s choices for management of his ulcer and osteomyelitis? A: Management of ulcers Optimal management should involve a multidisciplinary group of consultants. Mechanical debridement, systemic antibiotic therapy, and measures to reduce weight bearing are the main elements of effective care. Foot soaks and whirlpool therapy may be detrimental and lead to further skin breakdown, but moist dressings on granulating wounds may help. Debridement a must. Remove nonviable, infected tissue to achieve a border of healthy, bleeding soft tissue and uninfected bone. Debridement improves the outcome of foot ulcers. 3 When hospitalization is indicated. Determine whether or not the patient requires hospitalization based on the presence of a severe infection (TABLE 2) and need for surgical intervention, fluid resuscitation, IV antibiotics, or control of meta- bolic derangements. 2 Consider hospitalization also if there is concern about the patient s ability or willingness to comply with wound care, antibiotic therapy, or off-loading of the affected area. Consider need for off-loading. Most diabetic wounds develop because of unperceived trauma, and likely do not heal because of ongoing trauma. Total contact casting, whereby loading levels to a foot ulcer are drastically reduced, has been shown to be effective in healing ulcers in about 6 weeks. 4 This suggests that healing of neuropathic ulcers must include mechanical off-loading of the ulcer. Total contact casting has several limitations, and new modalities are being investigated. 5 Obtain cultures. Wound culture results can greatly assist in determining appropriate antimicrobials. Gram stain can help direct therapy, and culture results are VOL 54, NO 9 / SEPTEMBER
5 TABLE 3 WOUND GRADE Grade 0 Grade 1 Grade 2 Grade 3 Grade 4 Grade 5 Mechanical off-loading hastens healing of neuropathic ulcers Wagner ulcer grading system WOUND DEPTH Intact skin Superficial ulcer Deep ulcer to tendon, bone, or joint Deep ulcer with abscess or osteomyelitis Forefoot gangrene Whole foot gangrene The Wagner ulcer grading system does not identify infectious processes except in Grade 3. Erythema, edema, and pain may be present in foot infections, and may manifest as paronychia, cellulitis, or superficial skin infection. consistent with Gram staining in 95% of cases. Gram-stained smear is 70% sensitive for identifying organisms that grow on culture, and is much better for gram-positive organisms than for gram-negative bacilli. Deep tissue specimens collected aseptically at surgery contain the true pathogens more often than more superficial samples. Curettage, involving tissue scraping with a scalpel from the base of a debrided ulcer, is more accurate than a wound swab. Wound swabs are likely to miss key pathogens as well as include nonpathogenic bacteria that confuse the antibiotic choice. 2 When antibiotics are needed. In gross infections and cellulitis, topical antibiotics may reduce bacterial loads, but there are few published data about their efficacy in diabetic foot infections. The Wagner ulcer grading system (TABLE 3) is most widely used for tracking diabetic foot ulcers, but it does not allow for identification of superficial infection and has not been validated as an effective tool. 6 An alternate method of classifying foot ulcers, taken from Lipsky et al, is shown in TABLE 4. Currently systemic antibiotics are recommended only for established infection, although one study suggested that antibiotic therapy in clinically uninfected foot ulcers may significantly improve healing. 7 Optimal duration of antibiotic therapy has not been studied, but convention has found 1 to 2 weeks to be effective for mild to moderate infections, at least 2 weeks for serious infections, and at least 6 weeks for osteomyelitis. 2 Oral antibiotics are indicated when the ulcer is believed to be infected, and they should cover the usual pathogens, streptococci or staphylococci 7 (TABLE 5). Treat severe infections with intravenous broadspectrum antibiotics, covering for gramnegative and gram-positive aerobes and anaerobes. Studies have shown similar therapeutic outcomes between high-dose oral fluoroquinolones and intravenous cephalosporin therapy. Oral fluoroquinolones cause fewer side effects and reduce hospitalizationrelated costs compared with cephalosporins, penicillinase-resistant penicillins, and vancomycin. 8 Clindamycin or metronidazole may be added to fluoroquinolones to cover anaerobic organisms in severe or limb-threatening infections. 9 One study found that patients treated with vancomycin had a greater rate of recurrence. 5 Staphylococcus aureus is the most important pathogen in diabetic foot infections and may cause disease in isolation or as part of a mixed infection. Gram-negative rods, usually Enterobacteriaceae, are found in patients with chronic or previously treated infections. Pseudomonas species may be isolated from wounds that have been soaked or treated with wet dressings. Enterococci are more likely to be cultured from patients previously treated with a cephalosporin. Suspect anaerobes in cases of ischemic necrosis or deep tissue infections. 2 When a person with diabetes has peripheral vascular disease, therapeutic antibiotic concentrations are often not achieved in infected tissues even with adequate serum levels. 2 Novel methods of antibiotic delivery are being experimented with in an effort to solve this problem. Surgery. Surgical options may include plastic reconstruction involving debridement and either primary closure or flap coverage. Optimally, vascular-bypass is performed to allow either primary healing or surgical reconstruction. If 772 VOL 54, NO 9 / SEPTEMBER 2005 THE JOURNAL OF FAMILY PRACTICE
6 Diabetic foot ulcer and poor compliance TABLE 4 Clinical classification of diabetic foot infections CLINICAL APPEARANCE Wound lacking purulence or any manifestations of inflammation Presence of 2 or more manifestations of inflammation (purulence, erythema, pain, tenderness, warmth, or induration). Any cellulitis/erythema extends 2 or more cm around the ulcer, and infection is limited to the skin or superficial subcutaneous tissues. No other local complications or systemic illness. Infection (as above) in a patient who is systematically well and metabolically stable but which has 1 or more of the following characteristics: cellulites extending >2 cm, lymphagitic streaking, spread beneath the superficial fascia, deep-tissue abcess, gangrene, and involvement of muscle, tender, joint or bone Infection in a patient with systemic toxicity or metabolic instability (eg, fever, chills, tachycardia, hypotension, confusion, vomiting, leukocytosis, acidosis, severe hyperglycemia, or azotemia) CLASSIFICATION Uninfected Mild Moderate Severe Source: Lipsky et al, revascularization is not possible, amputation may be required. If osteomyelitis complicates the picture. No validated or well-accepted guidelines exist for diagnosing or treating diabetic foot osteomyelitis. Factors that may suggest osteomyelitis: long-standing ulcers (>4 weeks), large (>2 cm) or deep ulcers (>3 mm), elevated ESR (>70 mm/h). 2 Laboratory assays for diagnosing osteomyelitis can include measurements of erythrocyte sedimentation rate or C- reactive protein, though there are insufficient studies to assess their usefulness. One study found that 100% of patients with an ESR >70 mm/hr had osteomyelitis, despite lack of physical signs of inflammation. In diabetic patients with noninflamed foot ulcers, ESR can have a specificity of 100% and sensitivity of 28%. With inflamed ulcers, the sensitivity decreases to 23%. 8 Some believe that the ESR can be used to follow osteomyelitis, and a persistent elevation or rise after initial fall would suggest osteomyelitis. Studies are inadequate to support this, however. 5 Imaging for osteomyelitis can begin with plain films, which may show softtissue swelling, disruption of the bone cortex, and periosteal elevation. The American College of Radiology suggests this in the guidelines. 10 However, 50% of the bone may be destroyed before these changes are evident. Plain films have a sensitivity of 28% to 100% and a specificity of 69% to 92%. If initial films yield normal results, it may be useful to repeat them in 2 to 4 weeks. 9 MRI is highly sensitive (>90%) and specific (>80%), and may be even better with gadolinium. MRI is more sensitive for forefoot osteomyelitis than a leukocyte scan. 11 Positron-emission tomography (PET) scans and high-resolution ultrasound may be helpful in the future. Some studies suggest probing of sinuses and deep ulcers may be more sensitive than imaging. Palpable bone found at the base of an ulcer, with no overlying soft tissue, is highly predictive of osteomyelitis. 1 Visible bone in a nontraumatic wound suggests osteomyelitis, with a sensitivity of 32% and specificity of 100%. 12 The gold standard for diagnosis of osteomyelitis is obtaining a specimen of bone for pathology and culture. 9 Antibiotic choice should be based on High-dose oral fluoroquinolones are equivalent to IV cephalosporins and cause fewer side effects VOL 54, NO 9 / SEPTEMBER
7 TABLE 5 Selecting antibiotics for diabetic foot infections (from the Sanford Guide) DURATION DIAGNOSIS ORGANISMS SUGGESTED ANTIBIOTICS OF THERAPY Mild soft-tissue Aerobic Gram-positive Oral dicloxacillin, clindamycin, cephalexin, 1 2 weeks infection organisms trimethoprim-sulfamethoxazole Mild soft-tissue Aerobic Gram-positive Oral amoxicillin-clavulanate, levofloxacin, 1 2 weeks infection that organisms and Gram- or addition of ciprofloxacin to original antibiotics has failed to negative organisms respond to initial antibiotics Mild soft-tissue Aerobic Gram-positive If susceptible, oral clindamycin or trimethoprim- 1 2 weeks, infection that has organisms, Gram- sulfamethoxazole. Linezolid, vancomycin, or or longer if failed to respond negative organisms, daptomycin if not susceptible slow clinicalto initial antibiotics, and MRSA response and MRSA suspected Moderate soft- Gram-positive, Gram- Oral amoxicillin-clavulanate, levofloxacin, or 2 4 weeks* tissue infection negative, and anaerobic combination of ciprofloxacin plus clindamycin organisms Moderate soft- Gram-positive, Gram- Ciprofloxacin plus clindamycin, amoxicillin- 2 4 weeks* tissue infection negative, and anaerobic clavulanate, ampicillin/sulbactam, or with systemic toxicity, organisms piperacillin/tazobactam metabolic derangements, or in need of surgical procedures Moderate soft- Antibiotic-resistant Vancomycin, linezolid, or daptomycin for Gram- 2 4 weeks* tissue infection with Gram-positive, Gram- positive coverage plus ceftazidime, aztreonam, or antibiotic-resistant negative, and anaerobic ciprofloxacin for Gram-negative coverage with or organisms likely organisms without anaerobic coverage with metronidazole Severe soft- Gram-positive, Gram- Piperacillin/tazobactam; imipenem; vancomycin, 2 4 weeks tissue infection negative, and anaerobic linezolid, or daptomycin plus ceftazidime, organisms aztreonam, or ciprofloxacin with or without anaerobic coverage with metronidazole Osteomyelitis Gram-positive including Parenteral imipenem, meropenem, ticarcillin/ Duration S aureus, Gram-negative, clavulanate, piperacillin/tazobactam, ampicillin/ varies anaerobes sulbactam, cefepime plus metronidazole or aztreonam plus vancomycin plus metronidazole *If response to parenteral therapy is good, may be able to complete course with oral. 2 5 days if no residual infected tissue (post-surgery), 2 4 weeks if residual infected soft tissue, 4 6 weeks if residual infected viable bone, >3 months if residual dead bone. Source: Gilbert DN, Moellering RC, Eliopoulos GM, and Sande, AM. Sanford Guide to Antimicrobial Therapy, VOL 54, NO 9 / SEPTEMBER 2005 THE JOURNAL OF FAMILY PRACTICE
8 Diabetic foot ulcer and poor compliance Family physician commentary This case highlights several functions of the family physician and illustrates some of the challenges faced by primary caregivers. The dilemma in this scenario is that the patient ignored medical advice from specialists who had been consulted because of his worsening condition. What is a family physician s responsibility in this circumstance? If you place yourself in this physician s situation, you may experience a variety of emotions and thoughts, including frustration. How do you to provide a high standard of care for a patient who will not accept your recommendations? Patient autonomy is paramount As physicians we always need to respect patient autonomy. Though we may need to perform many roles, we always are the patient s advocate. This can be difficult when a patient deviates from what we consider appropriate medical care. We may fear complications arising from lack of cooperation with advised treatment. In this case, the physician was legitimately concerned about worsening bone and skin breakdown, which could ultimately lead to foot or limb loss. We are trained to evaluate and treat patients within our scope of knowledge and then incorporate the help of specialists as necessary. We are less well trained to deal with patients who refuse recommended medical treatments. In these situations, we must first thoroughly review with patients their options and the risks and benefits of each. We must also assess whether patients are competent to make decisions. If they are competent, then we must allow our patients to choose to do nothing, though it may not be what we would choose. The physician must make a choice of continuing to care for the patient, or begin the process of transferring care. If the patient-physician relationship continues, physician and patient should negotiate responsibility for outcomes and document the patient s understanding. In the case presented here, the patient continued seeing his physician for follow-up of his ulcer, though he had not followed the physician s treatment recommendation. This required the physician to continue his relationship with the patient despite a major difference of opinion. This is an example of respecting a patient s autonomy while continuing a therapeutic relationship. This case demonstrates several family physician functions in addition to patient advocate: Family physician as coordinator The physician obtained appropriate specialty consultations, and facilitated the patient s visits to the podiatrist, orthopedist, wound care specialist, and plastic surgeon. He remained the central point of contact for the patient and assured that the patient received adequate follow-up. as comprehensive caregiver This patient required management of several chronic diseases, including diabetes, hypertension, and obesity. He also needed health care maintenance. To give good care, the physician had to understand the patient s background, work situation, and personal values. To appropriately treat the patient s foot ulcer, the physician needed to know the patient, his work situation, and his medical history. As family physicians, we are able to build relationships with our patients that allow them to communicate their values, their history, and their wishes to us. and as educator. M.N. needed adequate and accurate information to make a final, informed decision concerning the care of his foot ulcer and osteomyelitis. As family physicians, we should be able to summarize for our patients their medical problem and present them with an overall picture of the problem and recommended treatment. This relationship allows the patient to make educated choices with a trusted healthcare provider. Jessica Farnsworth, MD VOL 54, NO 9 / SEPTEMBER
9 Osteomyelitis: select antibiotics based on bone culture, not on soft-tissue or sinus tract cultures bone culture, as soft-tissue or sinus tract cultures do not accurately predict bone pathogens. When empiric therapy is necessary, coverage should always include S aureus. Cure of osteomyelitis has traditionally been thought to require removal of infected bone, but studies are showing that antibiotics may be adequate in two thirds of cases, especially those with good bioavailability. When bone is removed, shorter antibiotic therapy may be sufficient. 2 Additional treatment options may include revascularization in an ischemic foot, which has been shown to salvage up to 98% of limbs. Hyperbaric oxygen may provide benefit, but data are insufficient to document this measure. Edema control may be beneficial for wound healing. Promising adjuvant therapies include granulocyte colony-stimulating factor (G-CSF), antibiotic-impregnated beads or orthopedic implants, and biosurgery with fly larvae. 2 Case resolution The family physician and M.N. discuss the options. The specialist recommends surgery, but the patient does not want to undergo this procedure. As his physician explains his concerns about the chronic, nonhealing ulcer and osteomyelitis, M.N. says he will negotiate a change in his work situation that would allow him to decrease the time spent on his feet and thus improve healing. The patient has small clinical improvement of his ulcer while hospitalized, and a peripherally inserted central catheter (PICC) line is placed to administer longterm antibiotics on an outpatient basis. The ulcer heals gradually in coming weeks and months. Laboratory results show improvement as well, with normalization of the ESR and CRP. Given the clinical improvement and a steady decrease in inflammatory markers, a bone scan is not repeated. The patient now has a job that allows him to sit instead of being on his feet all day. REFERENCES 1. Sumpio BE. Primary care: foot ulcers. N Engl J Med 2000; 343: Lipsky BA. Medical treatment of diabetic foot infections. Clin Infect Dis 2004; 39:S104 S Brem, Harold, Sheehan P, Boulton AJM. Protocol for treatment of diabetic foot ulcers. Am J Surg 2004; 187:1S 10S. 4. Ulbrecht JS, Cavanagh PR, Caputo GM. Foot problems in diabetes: an overview. Clin Infect Dis 2004; 39:S73 S Caputo GM, Cavanagh PR, Ulbrecht JS, et al. Assessment and management of foot disease in patients with diabetes. N Engl J Med 1994; 331: Smith RG. Validation of Wagner s classification: a literature review. Ostomy Wound Manage 2003; 49: Foster AVM, Bates M, Doxford M, Edmonds ME. Should oral antibiotics be given to clean foot ulcers with no cellulitis? Abstracts of the 3rd International Symposium of the Diabetic Foot (1998). 8. Tice AD, Hoaglund PA, Shoutlz DA. Outcomes of osteomyelitis among patients treated with outpatient parenteral antimicrobial therapy. Am J Med 2003; 114: Zimmerman J. Osteomyelitis. Am Acad Fam Pract Home Study 2005; Clinical Update Alazraki N, Dalinka MK, Berquist TH, et al. Imaging diagnosis of osteomyelitis in patients with diabetes mellitus. American College of Radiology. ACR Appropriateness Criteria. Radiology 2000; 215: Lipman BT, Collier BD, Carrera GF, et al. Detection of osteomyelitis in the neuropathic foot: nuclear medicine, MRI and conventional radiography. Clin Nucl Med 1998; 23: Newman LG, Waller J, Palestro CJ, et al. Unsuspected osteomyelitis in diabetic foot ulcers. Diagnosis and monitoring by leukocyte scanning with indium in 111 oxyquionolone. JAMA 1991; 266: VOL 54, NO 9 / SEPTEMBER 2005 THE JOURNAL OF FAMILY PRACTICE
Foot infections in persons with diabetes are
 DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
DIAGNOSIS AND MANAGEMENT OF DIABETIC FOOT INFECTION * James S. Tan, MD, MACP, FCCP ABSTRACT According to the American Diabetes Association, approximately 82 000 nontraumatic lower-limb amputations were
Foot infections are now among the most
 Article Progress in a pedestrian problem: A review of the revised Infectious Diseases Society of America diabetic foot infection guidelines Benjamin A Lipsky This article was first published in The Diabetic
Article Progress in a pedestrian problem: A review of the revised Infectious Diseases Society of America diabetic foot infection guidelines Benjamin A Lipsky This article was first published in The Diabetic
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections
 Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Bone and Joint Infections in Diabetics: Diagnosis and Management of Diabetic Foot and Other Common Lower Extremity Infections Objectives How do you to diagnose, classify and manage DFI? How do you diagnose
Definitions and criteria
 Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Several disciplines are involved in the management of diabetic foot disease and having a common vocabulary is essential for clear communication. Thus, based on a review of the literature, the IWGDF has
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
OSTEOMYELITIS. If it occurs in adults, then the axial skeleton is the usual site.
 OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
OSTEOMYELITIS Introduction Osteomyelitis is an acute or chronic inflammatory process of the bone and its structures secondary to infection with pyogenic organisms. Pathophysiology Osteomyelitis may be
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
General surgery department of SGMU Lecturer ass. Khilgiyaev R.H. Anaerobic infection. Gas gangrene
 Anaerobic infection Gas gangrene Anaerobic bacteria Anaerobic bacteria are the most numerous inhabitants of the normal gastrointestinal tract, including the mouth Bacteroides fragilis and Clostridium The
Anaerobic infection Gas gangrene Anaerobic bacteria Anaerobic bacteria are the most numerous inhabitants of the normal gastrointestinal tract, including the mouth Bacteroides fragilis and Clostridium The
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline
 Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
Wound, Ostomy and Continence Nursing Certification Board (WOCNCB) Certified Foot Care Nurse (CFCN) Detailed Content Outline Description Domain I: Assessment and Care Planning 010000 40 Task 1: Obtain focused
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29
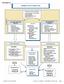 PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
PATHWAY #4 DIABETIC FOOT DISORDERS VOLUME 45, NUMBER 5, SEPTEMBER/OCTOBER 2006 S 29 be present. Hospitalization is required to treat the infection as well as systemic sequelae. Patients with poor vascular
Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections
 Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections Version 7.2 PAGL Inclusion Approved at January 2017 PGC APPROVED BY: TRUST REFERENCE: B3/2017 AWP REF: UHL Policies and
Antimicrobial Guidelines for the Empirical Management of Diabetic Foot Infections Version 7.2 PAGL Inclusion Approved at January 2017 PGC APPROVED BY: TRUST REFERENCE: B3/2017 AWP REF: UHL Policies and
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
-> Education -> Excellence
 Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Quality Conference 5/2557 Extravasations: Event -> Education -> Excellence รศ.นพ. รว ศ เร องตระก ล สาขาว ชาก มารศ ลยศาสตร ภาควชาศลยศาสตร Extravasations: Event 1. Thrombophlebitis - superficial vein 2.
Aetiology Macroangiopathy occurs mainly distally ie Popliteal artery There is arterial wall calcification Microangiopathy is less common
 DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
Wounds and Infections: Wound Management From the ID Physician Standpoint. Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department
 Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
Wounds and Infections: Wound Management From the ID Physician Standpoint Alena Klochko, MD Orlando VA Medical Center Infectious Disease Department Objectives Distinguish between colonization, critical
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Cellulitis: a practical guide
 Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
Cellulitis: a practical guide Dr John Day Consultant in Infectious Diseases & General Medicine Southend University Hospital NHS Foundation Trust 77 yr old retired civil servant A&E presentation c/o rigors
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care
 The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
The Diabetic Foot Screen and Management Foundation Series of Modules for Primary Care Anita Murray - Senior Podiatrist Diabetes, SCH Learning Outcomes Knowledge of the Model of Care For The Diabetic Foot
Abscess. A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body.
 Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
Abscess A abscess is a localized collection of pus in the skin and may occur on any skin surface and be formed in any part of body. Ethyology Bacteria causing cutaneous abscesses are typically indigenous
1 of :19
 1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
1 of 8 3-12-2012 12:19 Diabetic foot ulcer classification system for research purposes Introduction Aims of the ulcer research classification system Definitions and categorisation for the ulcer research
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA
 Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Diabetic Neuropathic Arthropathy (Charcot) Kiwon Young M.D. ( 양기원 ) Eulji Hospital Dept of Orthopaedic Foot & Ankle Clinic Seoul, KOREA Charcot 1. What is it? (definition) & Who gets it? (epidemiology
Practical guidelines on the management and prevention of the diabetic foot 2011
 DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 225 231. Published online in Wiley Online Library (wileyonlinelibrary.com).2253 IWGDF GUIDELINES Practical guidelines
DIABETES/METABOLISM RESEARCH AND REVIEWS Diabetes Metab Res Rev 2012; 28(Suppl 1): 225 231. Published online in Wiley Online Library (wileyonlinelibrary.com).2253 IWGDF GUIDELINES Practical guidelines
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Nanogen Aktiv. Naz Wahab MD, FAAFP, FAPWCA Nexderma
 Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Nanogen Aktiv Naz Wahab MD, FAAFP, FAPWCA Nexderma Patient BM 75 y.o female with a history of Type 2 Diabetes, HTN, Hypercholesterolemia, Renal insufficiency, Chronic back Pain, who had undergone a L3-L4
Diabetic Foot Infections
 PL Detail-Document #320509 This PL Detail-Document gives subscribers additional insight related to the Recommendations published in PHARMACIST S LETTER / PRESCRIBER S LETTER May 2016 Diabetic Foot Infections
PL Detail-Document #320509 This PL Detail-Document gives subscribers additional insight related to the Recommendations published in PHARMACIST S LETTER / PRESCRIBER S LETTER May 2016 Diabetic Foot Infections
Severe β-lactam allergy. Alternative (use for mild-moderate β-lactam allergy) therapy
 Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Infected cardiac-implantable electronic devices: diagnosis, and treatment
 Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Infected cardiac-implantable electronic devices: diagnosis, and treatment The incidence of infection following implantation of cardiac implantable electronic devices (CIEDs) is increasing at a faster rate
Wound Jeopardy: Name That Wound Session 142 Saturday, September 10 th 2011
 Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Initial Wound Care Consult History Physical Examination Detailed examination of the wound Photographs Cultures Procedures TCOM ABI Debridement Management Decisions A Detailed History and Physical (wound)
Diabetic Foot Complications
 Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
Diabetic Foot Complications Podiatry Specialty Clinic YKHC Bethel, Alaska August 1-3, 2017 Charles C. Edwards, DPM Alaska Native Tribal Health Consortium Peripheral Neuropathy Diabetic Peripheral Neuropathy
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Due to Perimed s commitment to continuous improvement of our products, all specifications are subject to change without notice.
 A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
A summary Disclaimer The information contained in this document is intended to provide general information only. It is not intended to be, nor does it constitute, medical advice. Under no circumstances
Diabetic Feet. Juanita Muller
 Diabetic Feet Juanita Muller Mr RR 69 year old male CHARCOT ARTHROPATHY Diabetic Feet Callus Acute injury and ulceration Infection Osteomylitis Chronic ulceration Ischaemic necrosis Charcot s arthropathy
Diabetic Feet Juanita Muller Mr RR 69 year old male CHARCOT ARTHROPATHY Diabetic Feet Callus Acute injury and ulceration Infection Osteomylitis Chronic ulceration Ischaemic necrosis Charcot s arthropathy
I have no financial interests to disclose in regards to this lecture.
 Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
Evaluation and Treatment of Diabetic Foot Ulcerations John M. Giurini, D.P.M. Associate Professor in Surgery Harvard Medical School Disclosure Statement I have no financial interests to disclose in regards
Diabetic Foot Pathophysiology. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Diabetic Foot Pathophysiology Professor Donald G. MacLellan Executive Director Health Education & Management Innovations AGEs & RAGEs in Diabetes AGE levels increased & RAGEs highly expressed in diabetic
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers. Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT
 Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
Foot Ulcer Workshop: Prevention and Management of Diabetic Foot Ulcers Aparna Pal, Consultant Endocrinologist, RBH Keith Hilston, Podiatrist, BHFT High mortality and morbidity Complex condition, longterm
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme
 Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Diabetes follow-up: What are the PHO Performance Programme goals and how are they best achieved? Supporting the PHO Performance Programme 48 BPJ Issue 39 What are the goals? The PHO Performance Programme
Osteomyelitis (Inflammation of the Bone and Bone Marrow) Basics
 Osteomyelitis (Inflammation of the Bone and Bone Marrow) Basics OVERVIEW Sudden (acute) or long-term (chronic) inflammation of bone and its associated soft-tissue elements of bone marrow, endosteum (lining
Osteomyelitis (Inflammation of the Bone and Bone Marrow) Basics OVERVIEW Sudden (acute) or long-term (chronic) inflammation of bone and its associated soft-tissue elements of bone marrow, endosteum (lining
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT
 VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
VASCULAR WOUNDS PATHOPHYSIOLOGY AND MANAGEMENT Lucy Stopher, A/CNS Vascular Surgery ...it is best to think of a wound not as a disease, but rather as a manifestation of disease. Joe McCulloch In order
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida
 Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Division of Vascular and Endovascular Surgery University of South Florida School of Medicine Tampa, Florida Appearance: oearly < 3 mo. olate > 3 mo.. Extent: Szilagyi Classification: Grade I: infection
Clinical assessment of diabetic foot in 5 minutes
 Clinical assessment of diabetic foot in 5 minutes Assoc. Prof. N. Tentolouris, MD 1 st Department of Propaedeutic Internal Medicine Medical School Laiko General Hospital Leading Innovative Vascular Education
Clinical assessment of diabetic foot in 5 minutes Assoc. Prof. N. Tentolouris, MD 1 st Department of Propaedeutic Internal Medicine Medical School Laiko General Hospital Leading Innovative Vascular Education
Diagnosis and Treatment of Diabetic Foot Infections
 IDSA GUIDELINES Diagnosis and Treatment of Diabetic Foot Infections Benjamin A. Lipsky, 1,a Anthony R. Berendt, 2,a H. Gunner Deery, 3 John M. Embil, 4 Warren S. Joseph, 5 Adolf W. Karchmer, 6 Jack L.
IDSA GUIDELINES Diagnosis and Treatment of Diabetic Foot Infections Benjamin A. Lipsky, 1,a Anthony R. Berendt, 2,a H. Gunner Deery, 3 John M. Embil, 4 Warren S. Joseph, 5 Adolf W. Karchmer, 6 Jack L.
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
Open Fractures. Ria Dindial. Photo courtesy pic2fly.com
 Open Fractures Ria Dindial Photo courtesy pic2fly.com CLINICAL PEARL TYPE WOUND DESCRIPTION OTHER CRITERIA I < 1cm (puncture wounds) - II 1-10 cm - IIIA >10 cm, coverage available Segmental fractures,
Open Fractures Ria Dindial Photo courtesy pic2fly.com CLINICAL PEARL TYPE WOUND DESCRIPTION OTHER CRITERIA I < 1cm (puncture wounds) - II 1-10 cm - IIIA >10 cm, coverage available Segmental fractures,
Case 1. July 14, th week wound gel 3 cm x 2.5 cm = 7.5 cm². May 25, st wound gel on 290 days PI treatment 4 cm x 2.4 cm = 9.
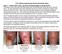 2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
2.5% Sodium Hyaluronate Wound Gel Study Cases Case 1 Patient with Lower Leg Ulcer Not Responding to Compression This patient was a 50-year old male patient with nonhealing right lower leg since January
Management Of The Diabetic foot
 Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
Management Of The Diabetic foot Aims, Pathways, Treatments Nikki Coates 12/1/18 Diabetic foot pathology Neuropathy Foot deformity Vascular disease Sensory neuropathy Limited Joint Mobility Smoking Autonomic
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Will it heal? How to assess the probability of wound healing
 Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Will it heal? How to assess the probability of wound healing Richard F. Neville, M.D. Professor of Surgery Chief, Division of Vascular Surgery George Washington University Limb center case 69 yr old male
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH)
 Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
Rochester Patient Safety C. difficile Prevention Collaborative: Long Term Care Antimicrobial Stewardship (funded by NYSDOH) Clinical Practice Guideline* for the Diagnosis and Management of Acute Bacterial
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC
 High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
High Risk Podiatry in a Vascular Setting; A new paradigm in Diabetic Foot Disease? Ereena Torpey Senior Podiatrist - FMC A new paradigm? Foot ulceration 101 Assessing Perfusion a new challenge Pressure
Sores That Will Not Heal
 Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
Sores That Will Not Heal Introduction Some sores have trouble healing on their own. Sores that will not heal are a common problem. Open sores that will not heal are also known as wounds or skin ulcers.
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR
 ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
ORIGINAL ARTICLE DIABETIC FOOT RISK CLASSIFICATION IN A TERTIARY CARE TEACHING HOSPITAL OF PESHAWAR Ghulam Shabbier, Said Amin, Ishaq Khattak, Sadeeq-ur-Rehman Department of Medicine Khyber Teaching Hospital
SKIN AND SOFT TISSUE INFECTIONS
 SKIN AND SOFT TISSUE INFECTIONS ZAIN CHAGLA SEA COURSES - PATAGONIA COPYRIGHT 2017 BY SEA COURSES INC. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in
SKIN AND SOFT TISSUE INFECTIONS ZAIN CHAGLA SEA COURSES - PATAGONIA COPYRIGHT 2017 BY SEA COURSES INC. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in
Necrotizing Fasciitis. By Lisa Banks
 Necrotizing Fasciitis By Lisa Banks Foot infections are the most common softtissue infections in pts with diabetes Necrotizing fasciitis is the most important soft tissue infection in DM pts involving
Necrotizing Fasciitis By Lisa Banks Foot infections are the most common softtissue infections in pts with diabetes Necrotizing fasciitis is the most important soft tissue infection in DM pts involving
CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care
 MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care The Benefits of the Proposition No
MANAGEMENT IN CONFIDENCE CPAG Summary Report for Clinical Panel URN 1779, Hyperbaric Oxygen Therapy for Diabetic Lower Limb Ulceration Refractory to Best Standard Care The Benefits of the Proposition No
Treatment of infection
 Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
Clinica Ortopedica e Traumatologica Università degli Studi di Pavia Fondazione IRCCS Policlinico San Matteo Chairman: Prof. F. Benazzo Goals: - Healing of infection - Healing of fracture - Try to keep
Infections Amenable to OPAT. (Nabin Shrestha + Ajay Mathur)
 3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
3 Infections Amenable to OPAT (Nabin Shrestha + Ajay Mathur) Decisions regarding outpatient treatment of infections vary with the institution, the prescribing physician, the individual patient s condition
Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery
 Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery College of Health Sciences Ladoke Akintola University
Prof Oluwadiya KS FMCS (Orthop) Consultant Orthopaedic Surgeon / Associate Professor Division of Orthopaedics and Traumatology Department of Surgery College of Health Sciences Ladoke Akintola University
Morbidity & Mortality Conference Downstate Medical Center. Daniel Kaufman, MD
 Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Surgical Management of Osteomyelitis & Infected Hardware. Michael L. Sganga, DPM Orthopedics New England Natick, MA
 Surgical Management of Osteomyelitis & Infected Hardware Michael L. Sganga, DPM Orthopedics New England Natick, MA Disclosures None relevant to the content of this material Overview Implants Timing Tenants
Surgical Management of Osteomyelitis & Infected Hardware Michael L. Sganga, DPM Orthopedics New England Natick, MA Disclosures None relevant to the content of this material Overview Implants Timing Tenants
Microbiology and Treatment of Diabetic Foot Infections
 Microbiology and Treatment of Diabetic Foot Infections 18 Adolf W. Karchmer Abstract Foot infections in diabetic patients are a major source of morbidity and an important proximate cause of amputations.
Microbiology and Treatment of Diabetic Foot Infections 18 Adolf W. Karchmer Abstract Foot infections in diabetic patients are a major source of morbidity and an important proximate cause of amputations.
Objectives. Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection
 Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
Objectives Define classes of uncomplicated skin and soft tissue infection (SSTI) that drive empiric antimicrobial selection Purulent SSTI Non-purulent SSTI Recognize conditions that suggest complications
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
Front line management of the Diabetic Foot
 Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Front line management of the Diabetic Foot n o ti e b a i D + s te k o Sm = g in p Am a t u Sam Fratesi MD Smoking + diabetes = amputation Almost 2 million Canadians have diabetes In amputated diabetics
Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems
 Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
Division of Medicine & Community Services Service Development Tool for the Assessment of Provision of Services for Patients with Diabetes Related Foot Problems Graham Holt Advanced Practitioner / Podiatrist
10/19/2017. Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI. Consultant with J&J-Depuy-Synthesis
 Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Shawn M Sanicola DPM, FACFAS Foot And Ankle Associates of WI Consultant with J&J-Depuy-Synthesis Understand the systemic effects of diabetes on the lower extremity The significance of structural and biomechanical
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Charcot Arthropathy of the Foot & Ankle. MTAPA Annual Meeting June 2018 Emily Harnden, MD
 Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
Charcot Arthropathy of the Foot & Ankle MTAPA Annual Meeting June 2018 Emily Harnden, MD Background Disclosures None Learning Objectives Define the disease Recognize presenting signs/symptoms for proper
EWMA Educational Development Programme. Curriculum Development Project. Education Module. Wound Infection
 EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
Diabetes Mellitus and the Associated Complications
 Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
Understanding and the complications relating to the disease can assist the fitter to better serve patients. and the Associated Complications Released January, 2011 Total: 25.8 million people, or 8.3% of
December 3, 2015 Severe Sepsis and Septic Shock Antibiotic Guide
 Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
Severe Sepsis and Septic Shock Antibiotic Guide Surviving Sepsis: The choice of empirical antimicrobial therapy depends on complex issues related to the patient s history, including drug intolerances,
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
a Total Hip Prosthesis by Clostridum perfringens. A Case Report
 Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Haematogenous Infection of a Total Hip Prosthesis by Clostridum perfringens. A Case Report CHAPTER 5 CHAPTER 5 5.1. Introduction In orthopaedic surgery, an infection of a prosthesis is a very serious,
Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting]
![Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting] Clinical Pearls Infectious Diseases. Pritish K. Tosh, MD MN ACP Nov 7, [Answers and discussion slides will be posted after the meeting]](/thumbs/83/87318178.jpg) Clinical Pearls Infectious Diseases Pritish K. Tosh, MD MN ACP Nov 7, 2014 [Answers and discussion slides will be posted after the meeting] Case 1 A 33-year-old male with diffuse large B-cell lymphoma
Clinical Pearls Infectious Diseases Pritish K. Tosh, MD MN ACP Nov 7, 2014 [Answers and discussion slides will be posted after the meeting] Case 1 A 33-year-old male with diffuse large B-cell lymphoma
AGONY FEET. The. of the. Prevention and management of diabetic foot ulcers
 The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
The AGONY of the FEET Prevention and management of diabetic foot ulcers By Margaret Falconio-West, BSN, rn, APN/CNS, CWOCN, DAPWCA Nearly 25 percent of people with diabetes will develop a diabetic foot
Clinical Guideline for: Diagnosis and Management of Charcot Foot
 Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
Clinical Guideline for: Diagnosis and Management of Charcot Foot SUMMARY This guideline outlines the clinical features of Charcot foot (Charcot Neuroarthropathy). It also explains the process of diagnosis
CHAPTER 16 LOWER EXTREMITY. Amanda K Silva, MD and Warren Ellsworth, MD, FACS
 CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
CHAPTER 16 LOWER EXTREMITY Amanda K Silva, MD and Warren Ellsworth, MD, FACS The plastic and reconstructive surgeon is often called upon to treat many wound problems of the lower extremity. These include
RECOGNISINGSURGICAL SITE INFECTIONS(SSIs) NOVEMBER 2017
 RECOGNISINGSURGICAL SITE INFECTIONS(SSIs) NOVEMBER 2017 Welcome to this training resource. It has been designed for all healthcare workers involved in coordinating SSI surveillance, SSI surveillance data
RECOGNISINGSURGICAL SITE INFECTIONS(SSIs) NOVEMBER 2017 Welcome to this training resource. It has been designed for all healthcare workers involved in coordinating SSI surveillance, SSI surveillance data
DIABETIC FOOT SCOPE OF THE PROBLEM. Hanan Gawish, Mansoura University Egypt Representative of the IWGDF
 DIABETIC FOOT SCOPE OF THE PROBLEM Hanan Gawish, Mansoura University Egypt Representative of the IWGDF Agenda Definition of DF Diabetic Foot among Diabetes complication Risk factors for amputation Risk
DIABETIC FOOT SCOPE OF THE PROBLEM Hanan Gawish, Mansoura University Egypt Representative of the IWGDF Agenda Definition of DF Diabetic Foot among Diabetes complication Risk factors for amputation Risk
Rapid Foot Screening
 GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
GP Symposium 2015 Workshop Rapid Foot Screening Ms Chelsea Law, Principal Podiatrist Mr Henry Lee, Podiatrist Ms Ng Jia Lin, Podiatrist Ms Polly Lim, Podiatrist Ms Wong Wan Mun, Podiatrist Mr Yeo Boon
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT
 Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
Wound Care Evaluation by Kris Dalseg MS PT CWS CLT This document is intended to describe a standard wound care evaluation for healthcare practitioners. In healthcare, all aspects of our treatment have
The Diabetic Foot Latest Statistics
 The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
The Diabetic Foot Latest Statistics There are 2.6 million people with diagnosed diabetes in the UK. There are predicted to be 500,000 who have the condition but are unaware of it. There are 11,859 in TH
Rapid Recovery Hyperbarics 9439 Archibald Ave. Suite 104 Rancho Cucamonga CA,
 Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
DISCLOSURE STATEMENT 10/8/ BASIC OF ELEMENTS OF LIMB SALVAGE MANAGEMENT
 LI MB SALVAGE MANAGEMENT October 11, 2018 DISCLOSURE STATEMENT My opinions do not represent the VA s opinions in regards to product preference No specific proprietary data from the VA has been included
LI MB SALVAGE MANAGEMENT October 11, 2018 DISCLOSURE STATEMENT My opinions do not represent the VA s opinions in regards to product preference No specific proprietary data from the VA has been included
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS
 VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
VASCULAR DISEASE: THREE THINGS YOU SHOULD KNOW JAMES A.M. SMITH, D.O. KANSAS VASCULAR MEDICINE, P.A. WICHITA, KANSAS KANSAS ASSOCIATION OF OSTEOPATHIC MEDICINE ANNUAL CME CONVENTION APRIL 13, 2018 THREE
Coffey et al ND 6 HA, 5 TSA, and 5 other MRSA (3) and Staphylococcus epidermidis (3)
 Page 1 of 6 TABLE E-1 Outcomes of the Treatment of Periprosthetic Shoulder Infections* ä Study No. Presentation Prosthesis Most Common Pathogens Braman et al. 68 7 1 acute, 2 subacute, 2 HA and 5 TSA Staphylococcus
Page 1 of 6 TABLE E-1 Outcomes of the Treatment of Periprosthetic Shoulder Infections* ä Study No. Presentation Prosthesis Most Common Pathogens Braman et al. 68 7 1 acute, 2 subacute, 2 HA and 5 TSA Staphylococcus
Osteomieliti STEOMIE
 OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
OsteomielitiSTEOMIE Osteomyelitis is the inflammation of bone caused by pyogenic organisms. Major sources of infection: - haematogenous spread - tracking from adjacent foci of infection - direct inoculation
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Fluorescence Angiography in Limb Salvage
 Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Fluorescence Angiography in Limb Salvage Ryan H. Fitzgerald, DPM, FACFAS Associate Professor of Surgery-University Of South Carolina School of Medicine, Greenville Etiology of Lower extremity wounds Neuropathy
Limb Salvage in Diabetic Ischemic Foot. Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017
 Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Limb Salvage in Diabetic Ischemic Foot Kritaya Kritayakirana, MD, FACS Assistant Professor Chulalongkorn University April 30, 2017 Case Male 67 years old Underlying DM, HTN, TVD Present with gangrene
Localized collection of pus in a cavity
 Localized collection of pus in a cavity Loss of feeling or sensation induced to permit surgery Common example: Injection given to numb up the toe prior to performing an ingrown toenail procedure Mechanical
Localized collection of pus in a cavity Loss of feeling or sensation induced to permit surgery Common example: Injection given to numb up the toe prior to performing an ingrown toenail procedure Mechanical
Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD
 Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD Department of vascular surgery, University Hospital of Nantes, France Response to the increased demand of hospital care Population is aging Diabetes
Multidisciplinary approach to BTK Y. Gouëffic, MD, PhD Department of vascular surgery, University Hospital of Nantes, France Response to the increased demand of hospital care Population is aging Diabetes
DEFINITION Cellulitis is an acute, spreading inflammation of the dermis and subcutaneous tissue, often complicating a wound or other skin condition.
 DEFINITION Cellulitis is an acute, spreading inflammation of the dermis and subcutaneous tissue, often complicating a wound or other skin condition. Cellulitis may be further classified by the unique area
DEFINITION Cellulitis is an acute, spreading inflammation of the dermis and subcutaneous tissue, often complicating a wound or other skin condition. Cellulitis may be further classified by the unique area
Diabetic Foot Problems
 http://www.medicine-on-line.com Diabetic foot disease: 1/12 Diabetic Foot Problems Author: Affiliation: Rebecca Wong BN, MSc(Health Care) Prince of Wales Hospital, Hong Kong SAR Introduction Diabetes Mellitus
http://www.medicine-on-line.com Diabetic foot disease: 1/12 Diabetic Foot Problems Author: Affiliation: Rebecca Wong BN, MSc(Health Care) Prince of Wales Hospital, Hong Kong SAR Introduction Diabetes Mellitus
Helen Gelly, MD, FUHM, FCCWS
 Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Helen Gelly, MD, FUHM, FCCWS Diabetes mellitus is a major risk factor that impairs wound healing, making foot wounds one of the major problems of diabetes. Over 60% of lower limb amputations in the US
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Common Foot Disorders Justin Wernick, DPM, C.Ped. NY College of Podiatric Medicine Orthopedic Department, New York, NY 2 Common
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Common Foot Disorders Justin Wernick, DPM, C.Ped. NY College of Podiatric Medicine Orthopedic Department, New York, NY 2 Common
Disclosures. Critical Limb Ischemia. Vascular Testing in the CLI Patient. Vascular Testing in Critical Limb Ischemia UCSF Vascular Symposium
 Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
