Acinar effect of inhaled steroids evidenced by exhaled nitric oxide
|
|
|
- Mitchell Payne
- 6 years ago
- Views:
Transcription
1 Acinar effect of inhaled steroids evidenced by exhaled nitric oxide Alain Van Muylem, PhD, Yannick Kerckx, PhD, and Alain Michils, PhD Brussels, Belgium Background: The effects of inhaled corticosteroids (ICSs) on distal lung inflammation, as assessed by alveolar nitric oxide concentration (C A NO), are a matter of debate. Recently, a theoretic study suggested that acinar airway obstruction that is relieved by ICS treatment and associated with a decrease in fraction of exhaled nitric oxide (FeNO) concentration might, paradoxically, increase C A NO. This increase could be a hallmark effect of ICSs at the acinar level. Objective: In the light of this new hypothesis, we studied changes in C A NO and FeNO after administration of ICSs. Methods: C A NO and FeNO were measured before and after ICS treatment of 38 steroid-naive patients with uncontrolled asthma who showed clinical improvement after ICS therapy. Results: The average FeNO decreased from 78.3 to 28.9 ppb (P <.001); C A NO decreased from 7.7 to 4.3 ppb (P 5.009). In 14 subjects (low-slope group), slope (5 DC A NO/DFeNO) values (D 5 post-ics 2 pre-ics value) were less than the 95% normal CI (average DFeNO ppb and average DC A NO ppb). In this group, baseline C A NO was abnormally low when FeNO was taken into account. In 11 subjects (the high-slope group), the slope was above the normal interval (average DFeNO ppb and average DC A NO ppb). Conclusion: Opposite patterns (one that was predicted) can indicate peripheral actions of ICSs; this difference might account for conflicting data reported from studies using C A NO to determine the peripheral action of ICSs. We show that a low C A NO does not preclude distal inflammation. (J Allergy Clin Immunol 2010;126:730-5.) Key words: Exhaled nitric oxide, alveolar nitric oxide, asthma, inhaled corticosteroids, Asthma Control Questionnaire Studies of postmortem tissue 1 and transbronchial biopsy samples indicated that asthma affects the small airways. 2 Noninvasive analysis of the function of these airways is complex, especially at peripheral zones, such as intra-acinar airways. One noninvasive approach for measuring distal inflammation 3-8 involves quantification of alveolar nitric oxide (NO) by tracing exhaled NO. From the Chest Department, Cliniques Universitaires Erasme, Université Libre de Bruxelles. Supported by a MAP project from ESA: Airway NO in microgravity. Disclosure of potential conflict of interest: A. Michils receives consulting fees from Novartis and AstraZeneca. The rest of the authors have declared that they have no conflict of interest. Received for publication December 16, 2009; revised May 31, 2010; accepted for publication June 2, Available online August 14, Reprint request: Alain Van Muylem, PhD, Chest Department, Cliniques Universitaires Erasme, Université Libre de Bruxelles, 808 Route de Lennik, B-1070 Brussels, Belgium. avmuylem@ulb.ac.be /$36.00 Ó 2010 American Academy of Allergy, Asthma & Immunology doi: /j.jaci Abbreviations used ACQ: Asthma Control Questionnaire C A NO: Alveolar nitric oxide concentration FEF 75 : Forced expired flow at 75% of vital capacity FeNO: Fraction of exhaled nitric oxide FVC: Forced vital capacity ICS: Inhaled corticosteroid J awno: Apparent bronchial nitric oxide production LABA: Long-acting b 2 -agonist NO: Nitric oxide The exact site of action of inhaled corticosteroids (ICSs) in patients with asthma is controversial. Although ICSs have anti-inflammatory effects on bronchial airways, 9,10 their effects on distal inflammation, as assessed by alveolar nitric oxide concentration (C A NO), are unclear. Lehtimäki et al 10 did not find a difference in C A NO between asthmatic patients and control subjects at baseline or after ICS treatment. However, a crosssectional study by Gelb et al 4 revealed that overall C A NO in ICS-treated patients was greater than that of the control group, although there was wide scatter and overlap of the data from the 2 groups. The effect of ICSs on lung periphery, from terminal bronchioles to alveoli, should be determined by taking interaction between C A NO and bronchial NO production into account. Recent analyses of NO transport indicated a link between fraction of exhaled nitric oxide (FeNO) concentration, which is measured to assess bronchial (including peripheral) NO production, and C A NO. 11,12 Because of the concentration gradient between preacinar bronchioles and alveoli, some NO molecules produced in the peripheral airways diffuse toward the alveoli (back diffusion) without being expired. 13,14 This can result in a lower FeNO and a higher C A NO 13,14 compared with values predicted by perfectly mixed, 2-compartment models. When intra-acinar peripheral bronchoconstriction develops, back diffusion is impaired by the reduced caliber of the airway, 15 which hampers NO flux toward the alveolar zone. Compared with an unobstructed condition, FeNO increases (more NO molecules are available for expiration) and C A NO decreases. Therefore reduction or elimination of bronchoconstriction by therapy would increase C A NO and decrease FeNO. Similar to an ICS-induced reduction in C A NO, these changes might indicate activity of ICSs in the periphery and account for the observed absence of changes in C A NO after ICS treatment 10 or the wide range of C A NO detected in ICS-treated and untreated patients with asthma. 4 We evaluated changes in FeNO and C A NO that occurred after treatment with an ICS (Turbuhaler, a powder inhaler; AstraZeneca, S odertälje, Sweden) that significantly improved control of asthma. 730
2 J ALLERGY CLIN IMMUNOL VOLUME 126, NUMBER 4 VAN MUYLEM, KERCKX, AND MICHILS 731 METHODS Subjects This prospective study included nonsmoking adult patients who were given new diagnoses of asthma based on standard criteria 16 and treated at the Allergy and Asthma Clinic in the Chest Department of Erasme University Hospital (Brussels, Belgium). The patients had not received any treatment for asthma before the study began. Diagnosis of asthma was based either on the reversal of airflow obstruction after inhalation of a short-acting b 2 -agonist (n 5 16)oron airway hyperresponsiveness (n 5 22) depending on baseline spirometric values. All patients were atopic, as defined by at least 1 positive response on a skin prick test or RASTof common inhaled allergens. The local ethics committee approved the protocol, and each subject signed an informed consent form. Study design Patients were evaluated twice at a median interval of 3 weeks (2-6 weeks). Scores from an Asthma Control Questionnaire (ACQ), FeNO, C A NO, and standard lung function (FEV 1, forced vital capacity [FVC], and forced expired flow at 75% of vital capacity [FEF 75 ]) were recorded at each examination. At the end of visit 1, asthma therapy was initiated in line with international guidelines and recommendations 16 and regardless of ACQ scores or FeNO and C A NO, which were recorded separately. Data from a total of 38 patients with significant improvements in asthma control after the prescribed treatment were analyzed (21 male subjects; age, years; age range, years). Among these, 20 patients were treated with only ICSs (Pulmicort Turbuhaler, a dry-powder budesonide; 875 mg beclomethasone equivalent per day on average), and 18 patients received a combination of ICSs (722 mg beclomethasone equivalent per day on average) and a long-acting b 2 -agonist (LABA; Symbicort Turbuhaler, a dry-powder budesonide/formoterol; 1-2 inhalations twice daily). NO A chemiluminescence analyzer (LR 2000; Logan Research LTD, Rochester, United Kingdom) was used to measure NO levels in real time. The instrument was calibrated daily (111 ppb of NO in nitrogen). C A NO and the apparent bronchial nitric oxide production (J awno) were calculated by using the multiflow method described by Pietropaoli et al. 17 Tracings of exhaled NO were obtained for flow rates of 50, 175, and 300 ml/s. An extended discussion concerning the validity of the method is available elsewhere. 11 C A NO was also calculated by using the method described by Tsoukias and George. 18 In this study exhaled NO at 50 ml/s was referred to as FeNO, which is in line with American Thoracic Society/European Respiratory Society standards. 19 Changes in FeNO and C A NO The ratio of DC A NO to DFeNO (DC A NO/DFeNO; D is the change in concentration from before to after ICS therapy) was calculated to assess changes in C A NO after ICS treatment compared with changes in FeNO for each subject. When plotting C A NO as a function of FeNO, DC A NO/DFeNO corresponds to the slope of the line segment joining pre-ics and post-ics treatment values. The 95% CI of DC A NO/DFeNO for patients with stable and obstruction-free asthma 11 was derived by using the bootstrap method. Fig.E1 of the Online Repository showed the adjusted log-normal distribution of the slope (see the Methods section in this article s Online Repository at for details). ACQ Asthma control was assessed by using a short version of the ACQ, as created by Juniper et al, 20 that was translated into French. A score of less than 0.75 was defined as well-controlled asthma, whereas a score of greater than 1.5 was defined as poorly controlled asthma. 21 A change of 0.5 in the ACQ score was considered clinically relevant. 21 Lung function Spirometry was performed with a Zan 300 spirometer (Zan, Oberthulba, Germany). The prebronchodilator FEV 1 was used as an index of airway TABLE I. Baseline and post-ics therapy results Baseline Post-ICS P value ACQ score* 2.3 ( ) 0.5 ( ) <.001 FEV 1 (% predicted) <.001 FVC (% predicted) FEV 1 /FVC (%) <.001 FEF 75 (% predicted) <.001 FeNO (ppb)à 72.3 ( ) 28.8 ( ) <.001 J awno (pl/s) 3, ,469 1, <.001 C A NO a (ppb)à 7.4 ( ) 4.2 ( ).009 C A NO b (ppb)à 6.3 ( ) 3.6 ( ).006 C A NO a, Alveolar nitric oxide concentration obtained by using the Pietropaoli et al 17 method; C A NO b, alveolar nitric oxide concentration obtained by using the Tsoukias et al 18 method; FVC, Forced vital capacity; J awno, apparent bronchial production obtained by using the Pietropaoli et al 17 method. *Median (range) Mean 6 SD. àgeometric mean (geometric interval). caliber. FEV 1, FVC, and FEF 75 values were expressed as a percentage of predicted value. 22 Statistics FEV 1, FVC and FEF 75 were expressed as a percentage of the predicted value, and FeNO and C A NO were log-transformed. 23 These variables were compared with paired t tests, unpaired t tests, and 1-way classification AN- OVA (with post hoc comparisons in case of a significant global difference). ACQ scores were compared with Wilcoxon, Mann-Whitney U, and Kruskal-Wallis tests. The limits of significance were set at.05. RESULTS Table I shows average baseline and post-ics values for ACQ scores, FeNO, J awno, C A NO determined by using the methods of Pietropaoli et al 17 (C A NO a ) and Tsoukias et al 18 (C A NO b ), FEV 1, FVC, FEV 1 /FVC, and FEF 75. All changes were significant. FeNO and J awno were correlated at baseline (R ) and after ICS treatment (R ). The C A NO values calculated by using the methods of Pietropaoli et al 17 (C A NO a ) versus those calculated by using the methods of Tsoukias et al 18 (C A NO b ) did not differ significantly at baseline (P 5.54) or after ICS treatment (P 5.61). Therefore, except in Table I, only the C A NO calculated by using the method of Pietropaoli et al 17 is presented. Table II shows prebronchodilation and postbronchodilation pulmonary function values and post-ics values for the 16 patients who were given diagnoses of asthma based on bronchodilation. Improvements in asthma control After ICS treatment, asthma control improved for all patients (their ACQ scores decreased by >0.5). Moreover, all but 5 patients had an ACQ score of less than 0.75, which indicates wellcontrolled asthma. Changes in FeNO and C A NO Fig 1 shows FeNO (Fig 1, A) and C A NO (Fig 1, B) before and after ICS therapy for each patient. Fig 1, C, shows DC A NO/ DFeNO for each patient. A negative value means that C A NO and FeNO changed in opposite directions, such as a decrease in FeNO and an increase in C A NO. The 95% CI in a stable population of asthmatic patients (from 0.05 [5%] to 0.15 [15%], with a
3 732 VAN MUYLEM, KERCKX, AND MICHILS J ALLERGY CLIN IMMUNOL OCTOBER 2010 TABLE II. Prebronchodilation, postbronchodilation, and post-ics therapy results (n 5 16) Prebronchodilation Postbronchodilation Post-ICS P value* P valuey FEV 1 (% predicted) <.001 <.001 FVC (% predicted) <.001 <.001 FEV 1 /FVC (%) <.001 FEF 75 (% predicted) <.001 All variables are presented as means 6 SDs. FVC, Forced vital capacity. *Postbronchodilation compared with prebronchodilation. Post-ICS compared with prebronchodilation. FIG 1. A, Pre-ICS and B, post ICS therapy FeNO and C, C A NO values for each patient. C, DC A NO/DFeNO for each patient (D refers to the pre-ics/post-ics therapy difference). The gray rectangle indicates the 95% CI of DC A NO/DFeNO in patients with stable asthma. Solid and open symbols indicate treatments with ICSs alone or ICSs plus LABAs, respectively. mean of 0.08 [8%]) is also shown. In 13 patients DC A NO/DFeNO values were inside the normal interval (normal slope group, median DC A NO/DFeNO ). Two other groups can be defined with respect to the 95% CI: a high-slope group (n 5 11, median DC A NO/DFeNO ) and a low-slope group (n 5 14, median DC A NO/DFeNO ). The baseline values were similar among the normal, low-slope, and high-slope groups for FEV 1 (81.9% %, 89.3% %, and 85.4% 6 23%, respectively; P 5.558), forced vital capacity (FVC; 109.1% %, 96.9% %, and 95.9% %, respectively; P 5.342), FEV 1 /FVC (74.9% 6 8.5%, 70.9% %, and 72.9% %, respectively; P 5.683), FEF 75 (44.8% %, 54.9% %, and 55% %, respectively; P 5.580), and ACQ scores (1.7 [1-3.3], 2.5 [ ], and 2.9 [1.4-5], respectively; P 5.065). The corresponding post-ics values were also similar among the groups for FEV 1 (94.3% %, 89.3% %, and 97.5% %, respectively; P 5.797), FVC (100.8% %, 106.3% %, and 102.2% %, respectively; P 5.468), FEV 1 / FVC (78.9% 6 7.7%, 78.2% 6 7.4%, and 77.7% 6 6.9%, respectively; P 5.953), FEF 75 (64.1% 6 26%, 74.1% 6 28%, and 70% %, respectively; P 5.624), and ACQ score (0.6 [ ], 0.6 [ ], and 0.4 [0-1.2], respectively; P 5.744). All differences from before to after ICS therapy were significant (P <.001), except for FVC in the low-slope group (P 5.038) and FEV 1 /FVC in the high-slope group (P 5.042). Table III presents the average baseline and post-ics values for FeNO, J awno, and C A NO. The last row shows the post-ics therapy C A NO corrected for back diffusion contamination by bronchial NO. All changes from before to after ICS therapy were significant; most notable was the increase in C A NO in the low-slope group (P <.001). Baseline FeNO did not differ significantly between groups (P 5.073), whereas baseline C A NO did differ significantly between groups (P and P <.001 for normal vs low- and high-slope groups, respectively; P<0.001 for low-slope vs high-slope groups). Post-ICS values did not differ significantly between groups for FeNO (P 5.155) or C A NO (P 5.093). In Fig 2 C A NO was plotted as a function of FeNO; it demonstrates the average trajectories from pre-ics to post-ics therapy values in the normal slope, high-slope, and low-slope groups. The shaded area corresponds to the 95% CI for C A NO as a function of FeNO derived from 24 patients with stable asthma and normal lung function. 11 This area indicates the expected range of C A NO values for a given FeNO when alveolar production is normal. Treatment with ICSs versus ICSs plus LABAs Baseline pulmonary function of patients receiving ICSs (n 5 20) compared with ICSs plus LABAs (n 5 18) differed in FEV 1 (92% 6 10% and 79% 6 22% of predicted value, respectively; P 5.024) and FEF 75 (74% 6 24% and 49% 6 21% of predicted value, respectively; P 5.002). After treatment, however, pulmonary functions were similar; FEV 1 values for the ICS and ICS plus LABA groups were 96% 6 14% and 95% 6 12% of predicted value, respectively (P 5.801), and FEF 75 values were 86% 6 28% and 77% 6 20% of predicted value, respectively (P 5.307).
4 J ALLERGY CLIN IMMUNOL VOLUME 126, NUMBER 4 VAN MUYLEM, KERCKX, AND MICHILS 733 TABLE III. Baseline and post-ics FeNO and C A NO value in the normal, low-slope, and high-slope groups Normal group (n 5 13) Low-slope group (n 5 14) High-slope group (n 5 11) Baseline Post-ICS Baseline Post-ICS Baseline Post-ICS FeNO* (ppb) 79.6 ( ) 24.7 ( ) 78.5 ( ) 36.0 ( ) 58.2 ( ) 25.9 ( ) J awno (pl/s) 3, ,162 1, , ,491 1, , ,295 1, C A NO* (ppb) 7.1 ( ) 2.9à ( ) 3.7 ( ) 6.6 ( ) 18.4 ( ) 3.7 ( ) C A NO corr * (ppb) 0.8 ( ) 3.3 ( ) 2.0 ( ) C A NO corr, Alveolar nitric oxide concentration corrected for back diffusion; J awno, apparent bronchial production obtained by using the Pietropaoli et al 17 method. *Geometric mean (geometric interval). P <.001, pre-ics/post-ics therapy difference. àp 5.002, pre-ics/post-ics therapy difference. Mean 6 SD. FIG 2. Pre-ICS/post-ICS average values (6 SEMs) of C A NO versus FeNO trajectories for the normal (squares), low-slope (circles), and high-slope (triangles) groups. Solid and open symbols are the pre-ics and post-ics values, respectively. The shaded area corresponds to the C A NO 95% CI as a function of FeNO derived from 24 patients with stable and unobstructed asthma. 11 Baseline FeNO values were comparable between groups receiving ICSs or ICSs plus LABAs; 80.0 ppb ( ppb) and 64.6 ppb ( ppb), respectively (P 5.074). After ICS therapy, FeNO values were slightly less decreased in the group receiving ICSs only (34.0 ppb [ ppb] vs 23.9 ppb [ ppb], P 5.048). C A NO values did not differ between the groups given ICSs or ICSs plus LABAs, either at baseline (6.0 ppb [ ppb] vs 9.3 ppb [ ppb], respectively; P 5.145) or after treatment (4.9 ppb [ ppb] vs 3.6 ppb [ ppb], respectively; P 5.350). In the low- and high-slope groups 43% and 82% of the patients, respectively, received LABAs. This difference was not statistically different (P 5.099, Fisher exact test). DISCUSSION This study provides evidence of the peripheral action of ICSs; we show that ICSs reduce distal inflammation at either the alveolar or preacinar and acinar airway levels. We detected a low C A NO in asthmatic patients that did not definitively preclude distal lung inflammation. In our study FeNO and C A NO decreased after ICS treatment, indicating the bronchial and alveolar effects of ICSs. However, on closer examination, when FeNO decreased, changes in C A NO were widely scattered. Given their interdependence, which was recently demonstrated in healthy subjects 12 and patients with stable and nonobstructive asthma, 11 C A NO and FeNO must each be considered in interpreting changes in C A NO. Molecular diffusion generates a backdiffusion flux (toward the alveoli) through acinar airways, and therefore alveolar and bronchial NO concentrations are related. 13,14 This flux is proportional to the bronchoalveolar NO gradient and airway cross-sections; it removes NO molecules from expiration flux, thereby decreasing FeNO, and provides a positive source of NO for the alveolar compartment, thereby increasing C A NO. If bronchial NO production decreases (decreasing FeNO), the reduction of the bronchoalveolar NO gradient decreases the back-diffusion flux, and as a result, C A NO also decreases. Because of the interaction between FeNO and C A NO, correction formulae were proposed to extract C A NO specifically related to in situ production of NO. 11,12 This correction was not applicable to our study, at least for baseline values, because the patients with asthma presented with obvious abnormal lung function before they were treated with ICSs. Even if an increase in the bronchoalveolar gradient before treatment may compensate for an impaired back-diffusion gradient, peripheral obstruction contradicts the assumptions that were made to derive the correction formulae. DC A NO/DFeNO (the ratio of pre-ics vs post-ics differences in C A NO to pre-ics vs post-ics differences in FeNO) can be used to evaluate individual responses to ICSs in C A NO with respect to changes in FeNO. In a group of patients with stable asthma who did not have changes in alveolar production of NO, this slope averaged ;C A NO increased (decreased) by 8% of the FeNO increase (decrease). In this study 13 of 38 patients had changes in FeNO versus C A NO that were compatible with normal alveolar NO production and a decrease in C A NO that resulted from reduced bronchial inflammation after ICS treatment. However, even in this case, the modulation of the alveolar concentration by bronchial NO change indicated that the latter originated peripherally at the onset of the acinus. 14 In addition to this population, which had a normal slope, 2 groups of patients had different patterns of change in FeNO versus C A NO. The group with a high DC A NO/DFeNO (high-slope group, n 5 11) exhibited a high baseline level of C A NO, which probably resulted from high production of alveolar NO that was greatly reduced after ICS therapy, more than expected from the normal back-diffusion effect. This group displayed an obvious
5 734 VAN MUYLEM, KERCKX, AND MICHILS J ALLERGY CLIN IMMUNOL OCTOBER 2010 response to ICS therapy at the alveolar level, with normal recovery of C A NO. The group with a low DC A NO/DFeNO (low-slope group, n 5 14) had abnormally low baseline C A NO and, in 12 of 14 patients, negative DC A NO/DFeNO values because of a paradoxical increase in C A NO after ICS treatment. A recently published theoretic study 15 that addressed the issue of the effect of bronchoconstriction on FeNO might explain this finding; the study showed that FeNO increased significantly when bronchoconstriction occurred in intra-acinar airways around generation 18 of the Weibel model. 24 In this zone a reduction in airway cross-section impaired the above-described back-diffusion flux, thereby decreasing the effect of the bronchial NO production on the alveolar concentration. Therefore more molecules of NO were expired, increasing FeNO and reducing the bronchial source of the alveolar compartment; this decreased C A NO. Consequently, with decreasing levels of obstruction, FeNO decreased and C A NO increased because of back-diffusion flux recovery, which resulted in a negative DC A NO/DFeNO. The behavior of the low-slope group indicates obstruction of acinar airways, which is at least partly decreased by treatment with ICSs. These normal, high-slope, and low-slope groups might represent distinct phenotypes that are characterized by different baseline C A NO values. One of these phenotypes might present distinct characteristics in a longitudinal context (eg, more prone to exacerbations and greater decreases in lung function over time). These phenotypes must be studied further, but our findings indicate that measurements of C A NO and FeNO provide useful phenotypic information that can be used in the clinic. Several studies have shown that FeNO alone might not clearly determine asthma severity in adults. 25 It is not clear why baseline levels of alveolar production differed between the groups, despite similar baseline levels of pulmonary function, exhaled NO, and asthma control. Although some studies have reported low C A NO values in patients with uncontrolled asthma, 10,26 the dispersion of baseline C A NO values observed in this study was in agreement with the results of Gelb et al. 4 These authors showed that in asthmatic patients who are or are not being treated with ICSs, C A NO values varied widely, and there was significant overlap between values from patients with asthma and healthy subjects; these findings indicate a wide distribution of alveolar production. Lehtimäki et al 27 observed an association between increased alveolar NO levels and nocturnal symptoms in asthmatic patients. In this study only 3 of 38 patients were free from nocturnal symptoms (they had a nil value for this specific ACQ item) before treatment with ICSs. No difference in the magnitude of the nocturnal symptoms before therapy with ICSs was observed between the low- and high-slope groups (P 5.33, Mann-Whitney U test). In this study the combination of ICSs and LABAs had significant additional effects on standard pulmonary function: baseline FEV 1 and FEF 75 values were lower among patients who received LABAs, but after treatment, these values were similar. In contrast, treatment with LABAs did not affect NO indices, except for FeNO, which remained slightly higher (P 5.048) in patients treated with only ICSs. Furthermore, only 43% of patients in the low-slope group, who achieved relief from acinar obstruction, received LABAs. Relief from acinar obstruction might therefore result from the actions of ICSs. Our data indicate that the peripheral lung, from the terminal bronchioles to the alveoli, is affected in patients with poorly controlled mild-to-moderate asthma. An acinar effect was detected in 66% of the patients, involving the acinar airways or alveolar zone. This confirms the results of Verbanck et al, 28 who used the multibreath nitrogen washout technique to demonstrate abnormal acinar ventilation distribution in most patients with asthma. Further studies might compare expiratory flow-volume curves by using air and heliox to confirm peripheral involvement. In the low- and high-slope groups, changes observed in patterns of C A NO were not compatible with a purely central effect of ICSs (no average changes in C A NO associated with decreases in FeNO). This contradicts the concept that ICSs, such as the drypowder inhaler device (Turbuhaler), are centrally deposited. Although ICSs are spatially distributed to the large airways, 29 trace amounts of ICS particles might reach the lung s periphery. Alternatively, a systemic effect of ICSs cannot be excluded, as demonstrated for inhaled budesonide. 30 Based on the recently proposed relationship between FeNO and C A NO, our results show that ICSs have peripheral activities (ie, at the alveolar or acinar airways) in patients with mild-tomoderate asthma who have significantly improved control after treatment. In addition, detection of a low level of C A NO in asthmatic patients who have high levels of exhaled NO should be interpreted cautiously because it could indicate peripheral inflammation. Clinical implications: In patients with moderate or mild asthma, ICSs have positive effects on the preacinar and acinar airways and at the alveolar level. A low alveolar concentration of NO does not preclude peripheral inflammation. REFERENCES 1. Carroll N, Elliot J, Morton A, James A. The structure of large and small airways in nonfatal and fatal asthma. Am Rev Respir Dis 1993;147: Balzar S, Wenzel SE, Chu HW. Transbronchial biopsy as a tool to evaluate small airways in asthma. Eur Respir J 2002;20: Gelb AF, Flynn TC, Shinar CM, Gutierrez C, Zamel N. Role of spirometry and exhaled nitric oxide to predict exacerbations in treated asthmatics. Chest 2006;129: Gelb AF, Taylor CF, Nussbaum E, Gutierrez C, Schein A, Shinar CM, et al. Alveolar and airway sites of nitric oxide inflammation in treated asthma. Am J Respir Crit Care Med 2004;170: Paraskakis E, Brindicci C, Fleming L, Krol R, Kharitonov SA, Wilson NM, et al. Measurement of bronchial and alveolar nitric oxide production in normal children and children with asthma. Am J Respir Crit Care Med 2006;174: van Veen I, Sterk PJ, Schot R, Gauw SA, Rabe KF, Bel EH. Alveolar nitric oxide versus measures of peripheral airway dysfunction in severe asthma. Eur Respir J 2006;27: Brindicci C, Ito K, Barnes PJ, Kharitonov SA. Differential flow analysis of exhaled nitric oxide in patients with asthma of differing severity. Chest 2007;131: Berry M, Hargadon B, Morgan A, Shelley M, Richter J, Shaw D, et al. Alveolar nitric oxide in adults with asthma: evidence of distal lung inflammation in refractory asthma. Eur Respir J 2005;25: Kharitonov SA, Donnelly LE, Montuschi P, Corradi M, Collins JV, Barnes PJ. Dose-dependent onset and cessation of action of inhaled budesonide on exhaled nitric oxide and symptoms in mild asthma. Thorax 2002;57: Lehtimäki L, Kankaanranta H, Saarelainen S, Turjanmaa V, Moilanen E. Inhaled fluticasone decreases bronchial but not alveolar nitric oxide output in asthma. Eur Respir J 2001;18: Kerckx Y, Michils A, Van Muylem A. Airway contribution to alveolar nitric oxide in healthy subjects and stable asthma patients. J Appl Physiol 2008;104: Condorelli P, Shin HW, Aledia AS, Silkoff PE, George SC. A simple technique to characterize proximal and peripheral nitric oxide exchange using constant flow exhalations and an axial diffusion model. J Appl Physiol 2007;102: Shin HW, George SC. Impact of axial diffusion on nitric oxide exchange in the lungs. J Appl Physiol 2002;93: Van Muylem A, Noel C, Paiva M. Modeling of impact of gas molecular diffusion on nitric oxide expired profile. J Appl Physiol 2003;94:
6 J ALLERGY CLIN IMMUNOL VOLUME 126, NUMBER 4 VAN MUYLEM, KERCKX, AND MICHILS Verbanck S, Kerckx Y, Schuermans D, Vincken W, Paiva M, Van Muylem A. Effect of airways constriction on exhaled nitric oxide. J Appl Physiol 2008;104: Global initiative for Asthma Available at: Pietropaoli AP, Perillo IB, Torres A, Perkins PT, Frasier LM, Utell MJ, et al. Simultaneous measurement of nitric oxide production by conducting and alveolar airways of humans. J Appl Physiol 1999;87: Tsoukias NM, George SC. A two-compartment model of pulmonary nitric oxide exchange dynamics. J Appl Physiol 1998;85: American Thoracic Society/European Respiratory Society recommendations for standardized procedures for the online and offline measurement of exhaled lower respiratory nitric oxide and nasal nitric oxide, Am J Respir Crit Care Med 2005;171: Juniper EF, Svensson K, Mork AC, Stahl E. Measurement properties and interpretation of three shortened versions of the asthma control questionnaire. Respir Med 2005;99: Juniper EF, Bousquet J, Abetz L, Bateman ED. Identifying well-controlled and not well-controlled asthma using the Asthma Control Questionnaire. Respir Med 2006;100: Quanjer PH, Tammeling GJ, Cotes JE, Pedersen OF, Peslin R, Yernault JC. Lung volumes and forced ventilatory flows. Report Working Party. Standardization of lung function tests. European Community for Steel and Coal. Official Statement of the European Respiratory Society. Eur Respir J 1993;6(suppl 16): Travers J, Marsh S, Aldington S, Williams M, Shirtcliffe P, Pritchard A, et al. Reference ranges for exhaled nitric oxide derived from a random community survey of adults. Am J Respir Crit Care Med 2007;176: Weibel ER. Morphometry of the human lung. New York: Academic Press; Moore WC, Bleecker ER, Curran-Everett D, Erzurum SC, Ameredes BT, Bacharier L, et al. Characterization of the severe asthma phenotype by the National Heart, Lung, and Blood Institute s Severe Asthma Research Program. J Allergy Clin Immunol 2007;119: Lehtimäki L, Kankaanranta H, Saarelainen S, Turjanmaa V, Moilanen E. Peripheral inflammation in patients with asthmatic symptoms but normal lung function. J Asthma 2005;42: Lehtimäki L, Kankaanranta H, Saarelainen S, Turjanmaa V, Moilanen E. Increased alveolar nitric oxide concentration in asthmatic patients with nocturnal symptoms. Eur Respir J 2002;20: Verbanck S, Schuermans D, Noppen M, Van Muylem A, Paiva M, Vincken W. Evidence of acinar airway involvement in asthma. Am J Respir Crit Care Med 1999; 159: Martin GP, MacRitchie HB, Marriott C, Zeng XM. Characterisation of a carrierfree dry powder aerosol formulation using inertial impaction and laser diffraction. Pharm Res 2006;23: Wood LJ, Sehmi R, Gauvreau GM, Watson RM, Foley R, Denburg JA, et al. An inhaled corticosteroid, budesonide, reduces baseline but not allergen-induced increases in bone marrow inflammatory cell progenitors in asthmatic subjects. Am J Respir Crit Care Med 1999;159:
7 735.e1 VAN MUYLEM, KERCKX, AND MICHILS J ALLERGY CLIN IMMUNOL OCTOBER 2010 METHODS Changes in FeNO and C A NO The ratio DC A NO/DFeNO (D refers to the change from pre-ics to post-ics values) was computed to assess the individual response of C A NO to ICS treatment with respect to FeNO change. When plotting C A NO as a function of FeNO, DC A NO/DFeNO corresponds to the slope (S) of the line segment joining pre-ics and post-ics values. The problem arises of whether DC A NO/DFeNO is compatible with the normal interaction between bronchial NO production and the alveolar concentration (ie, with normal alveolar NO production and without obstruction). It is therefore difficult to longitudinally assess a normal range of DC A NO/DFeNO because DFeNO is often concomitant with asthma control and changes in lung function. The relationship between FeNO and C A NO was estimated transversally by the slope of a regression line calculated from 24 individual measurements of FeNO and C A NO in patients with stable and obstruction-free asthma. E1 The 95% CI of the slope, as computed from this sample, might be the best possible estimator of a normal interval for DC A NO/DFeNO; it was derived by using the bootstrap method. E2 Bootstrap method The bootstrap method allows empiric construction of the sampling distribution of the slope without an a priori parametric hypothesis. Briefly, this method is a resampling procedure; 24 pairs of values are randomly drawn from the original sample (some pairs are drawn several times, and others are not drawn), constituting a new sample from which the slope is calculated. By repeating this procedure 1000 times, the sampling distribution of the slope is derived. RESULTS Fig E1 shows the observed frequency distribution. This distribution fitted a log-normal distribution with a mean of (slope geometric mean, 0.08) and an SD of (P 5.66, x 2 test). Based on this adjusted distribution, the 95% CI of the slope goes from to REFERENCES E1. Kerckx Y, Michils A, Van Muylem A. Airway contribution to alveolar nitric oxide in healthy subjects and stable asthma patients. J Appl Physiol 2008;104: E2. Davison AV, Hinkley DV. Bootstrap methods and their applications. Cambridge: Cambridge University Press; 1997.
8 J ALLERGY CLIN IMMUNOL VOLUME 126, NUMBER 4 VAN MUYLEM, KERCKX, AND MICHILS 735.e2 FIG E1. Gray bars, Distribution histogram of the slope (S). Solid line, Adjusted log-normal distribution.
Inhaled fluticasone decreases bronchial but not alveolar nitric oxide output in asthma
 Eur Respir J 21; 18: 635 639 Printed in UK all rights reserved Copyright #ERS Journals Ltd 21 European Respiratory Journal ISSN 93-1936 Inhaled fluticasone decreases bronchial but not alveolar nitric oxide
Eur Respir J 21; 18: 635 639 Printed in UK all rights reserved Copyright #ERS Journals Ltd 21 European Respiratory Journal ISSN 93-1936 Inhaled fluticasone decreases bronchial but not alveolar nitric oxide
Effects of inhaled versus systemic corticosteroids on exhaled nitric oxide in severe acute asthma
 Respiratory Medicine (2009) 103, 614e620 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Effects of inhaled versus systemic corticosteroids on exhaled nitric oxide in
Respiratory Medicine (2009) 103, 614e620 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed Effects of inhaled versus systemic corticosteroids on exhaled nitric oxide in
Alveolar nitric oxide and asthma control in mild untreated asthma
 Alveolar nitric oxide and asthma control in mild untreated asthma Nicola Scichilone, MD, Salvatore Battaglia, MD, Salvatore Taormina, PhD, Viviana Modica, PhD, Elena Pozzecco, PhD, and Vincenzo Bellia,
Alveolar nitric oxide and asthma control in mild untreated asthma Nicola Scichilone, MD, Salvatore Battaglia, MD, Salvatore Taormina, PhD, Viviana Modica, PhD, Elena Pozzecco, PhD, and Vincenzo Bellia,
Exhaled nitric oxide and asthma control: a longitudinal study in unselected patients
 ERJ Express. Published on December 5, 2007 as doi: 10.1183/09031936.00020407 Exhaled nitric oxide and asthma control: a longitudinal study in unselected patients Alain Michils * PhD, Sandra Baldassarre
ERJ Express. Published on December 5, 2007 as doi: 10.1183/09031936.00020407 Exhaled nitric oxide and asthma control: a longitudinal study in unselected patients Alain Michils * PhD, Sandra Baldassarre
KEY WORDS airflow limitation, airway hyperresponsiveness, airway inflammation, airway lability, peak expiratory flow rate
 Allergology International. 2013;62:343-349 DOI: 10.2332 allergolint.13-oa-0543 ORIGINAL ARTICLE Stratifying a Risk for an Increased Variation of Airway Caliber among the Clinically Stable Asthma Atsushi
Allergology International. 2013;62:343-349 DOI: 10.2332 allergolint.13-oa-0543 ORIGINAL ARTICLE Stratifying a Risk for an Increased Variation of Airway Caliber among the Clinically Stable Asthma Atsushi
A Novel Approach to Partition Central and Peripheral Airway Nitric Oxide
 CHEST A Novel Approach to Partition Central and Peripheral Airway Nitric Oxide Paolo Paredi, MD, PhD ; Sergei A. Kharitonov, MD, PhD ; Sally Meah, RGN ; Peter J. Barnes, DM, DSc, Master FCCP ; and Omar
CHEST A Novel Approach to Partition Central and Peripheral Airway Nitric Oxide Paolo Paredi, MD, PhD ; Sergei A. Kharitonov, MD, PhD ; Sally Meah, RGN ; Peter J. Barnes, DM, DSc, Master FCCP ; and Omar
Asthma is characterized by an inflammation of. Increase in Alveolar Nitric Oxide in the Presence of Symptoms in Childhood Asthma*
 Increase in Alveolar Nitric Oxide in the Presence of Symptoms in Childhood Asthma* Bruno Mahut, MD; Christophe Delacourt, MD, PhD; Françoise Zerah-Lancner, MD; Jacques De Blic, MD; Alain Harf, MD, PhD;
Increase in Alveolar Nitric Oxide in the Presence of Symptoms in Childhood Asthma* Bruno Mahut, MD; Christophe Delacourt, MD, PhD; Françoise Zerah-Lancner, MD; Jacques De Blic, MD; Alain Harf, MD, PhD;
Central and Peripheral Airway Sites of Nitric Oxide Gas Exchange in COPD
 CHEST Central and Peripheral Airway Sites of Nitric Oxide Gas Exchange in COPD Arthur F. Gelb, MD, FCCP ; Colleen Flynn Taylor, MA ; Anita Krishnan, MD ; Christine Fraser, RCP, CPFT ; Chris M. Shinar,
CHEST Central and Peripheral Airway Sites of Nitric Oxide Gas Exchange in COPD Arthur F. Gelb, MD, FCCP ; Colleen Flynn Taylor, MA ; Anita Krishnan, MD ; Christine Fraser, RCP, CPFT ; Chris M. Shinar,
Exhaled nitric oxide levels in asthma: Personal best versus reference values
 Exhaled nitric oxide levels in asthma: Personal best versus reference values Andrew D. Smith, MRCP(UK), Jan O. Cowan, and D. Robin Taylor, MD Dunedin, New Zealand Background: Factors affecting the fraction
Exhaled nitric oxide levels in asthma: Personal best versus reference values Andrew D. Smith, MRCP(UK), Jan O. Cowan, and D. Robin Taylor, MD Dunedin, New Zealand Background: Factors affecting the fraction
Central and peripheral airway/alveolar sites of exhaled nitric oxide in acute asthma
 1 Pulmonary Division, Department of Medicine, Lakewood Regional Medical Center, and Geffen School of Medicine, University of California at Los Angeles Medical Center, Lakewood, California, USA 2 Department
1 Pulmonary Division, Department of Medicine, Lakewood Regional Medical Center, and Geffen School of Medicine, University of California at Los Angeles Medical Center, Lakewood, California, USA 2 Department
Role of Spirometry and Exhaled Nitric Oxide To Predict Exacerbations in Treated Asthmatics*
 Original Research ASTHMA Role of Spirometry and Exhaled Nitric Oxide To Predict Exacerbations in Treated Asthmatics* Arthur F. Gelb, MD, FCCP; Colleen Flynn Taylor, MA; Chris M. Shinar, PharmD; Carlos
Original Research ASTHMA Role of Spirometry and Exhaled Nitric Oxide To Predict Exacerbations in Treated Asthmatics* Arthur F. Gelb, MD, FCCP; Colleen Flynn Taylor, MA; Chris M. Shinar, PharmD; Carlos
Airway nitric oxide release is reduced after PBS inhalation in asthma
 J Appl Physiol 102: 1028 1033, 2007. First published November 16, 2006; doi:10.1152/japplphysiol.01012.2006. Airway nitric oxide release is reduced after PBS inhalation in asthma Hye-Won Shin, 1 David
J Appl Physiol 102: 1028 1033, 2007. First published November 16, 2006; doi:10.1152/japplphysiol.01012.2006. Airway nitric oxide release is reduced after PBS inhalation in asthma Hye-Won Shin, 1 David
CASE REPORT INTRODUCTION
 Allergology International. ; : - DOI: 10.2332 allergolint.10-cr-0251 CASE REPORT Centrilobular Opacities in the Asthmatic Lung Successfully Treated with Inhaled Ciclesonide and Tiotropium: With Assessment
Allergology International. ; : - DOI: 10.2332 allergolint.10-cr-0251 CASE REPORT Centrilobular Opacities in the Asthmatic Lung Successfully Treated with Inhaled Ciclesonide and Tiotropium: With Assessment
TORCH: Salmeterol and Fluticasone Propionate and Survival in COPD
 TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers?
 Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
Disclosures: Optimal Assessment of Asthma Control in Clinical Practice: Is there a role for biomarkers? Stanley Fineman, MD Past-President, American College of Allergy, Asthma & Immunology Adjunct Associate
A new role for exhaled nitric oxide as a functional marker of peripheral airway caliber changes: a theoretical study.
 A new role for exhaled nitric oxide as a functional marker of peripheral airway caliber changes: a theoretical study. Karamaoun C 1, Haut B 1, Van Muylem A 2 1 Ecole polytechnique de Bruxelles, Transfers,
A new role for exhaled nitric oxide as a functional marker of peripheral airway caliber changes: a theoretical study. Karamaoun C 1, Haut B 1, Van Muylem A 2 1 Ecole polytechnique de Bruxelles, Transfers,
A simple technique to characterize proximal and peripheral nitric oxide exchange using constant flow exhalations and an axial diffusion model
 J Appl Physiol 102: 417 425, 2007. First published August 3, 2006; doi:10.1152/japplphysiol.00533.2006. Innovative Methodology A simple technique to characterize proximal and peripheral nitric oxide exchange
J Appl Physiol 102: 417 425, 2007. First published August 3, 2006; doi:10.1152/japplphysiol.00533.2006. Innovative Methodology A simple technique to characterize proximal and peripheral nitric oxide exchange
Clinical efficacy of montelukast in anti-inflammatory treatment of asthma and allergic rhinitis
 Clinical efficacy of montelukast in anti-inflammatory treatment of asthma and allergic rhinitis Kim Hyun Hee, MD, PhD. Dept. of Pediatrics The Catholic University of Korea College of Medicine Achieving
Clinical efficacy of montelukast in anti-inflammatory treatment of asthma and allergic rhinitis Kim Hyun Hee, MD, PhD. Dept. of Pediatrics The Catholic University of Korea College of Medicine Achieving
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma
 Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
Exhaled Nitric Oxide: An Adjunctive Tool in the Diagnosis and Management of Asthma Jason Debley, MD, MPH Assistant Professor, Pediatrics Division of Pulmonary Medicine University of Washington School of
FVC to Slow Inspiratory Vital Capacity Ratio* A Potential Marker for Small Airways Obstruction
 Original Research PSYCHOLOGICAL TESTING FVC to Slow Inspiratory Vital Capacity Ratio* A Potential Marker for Small Airways Obstruction Judith Cohen, MD; Dirkje S. Postma, MD, PhD; Karin Vink-Klooster;
Original Research PSYCHOLOGICAL TESTING FVC to Slow Inspiratory Vital Capacity Ratio* A Potential Marker for Small Airways Obstruction Judith Cohen, MD; Dirkje S. Postma, MD, PhD; Karin Vink-Klooster;
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
BUDESONIDE AND FORMOTEROL (SYMBICORT ): Α A REVIEW
 Volume 23, Issue 3 December 2007 BUDESONIDE AND FORMOTEROL (SYMBICORT ): A REVIEW Donna L. Smith, Pharm. D. Candidate More than 22 million people in the United States have asthma according to the Centers
Volume 23, Issue 3 December 2007 BUDESONIDE AND FORMOTEROL (SYMBICORT ): A REVIEW Donna L. Smith, Pharm. D. Candidate More than 22 million people in the United States have asthma according to the Centers
Comparison of exhaled nitric oxide measurements between NIOX MINO â electrochemical and Ecomedics chemiluminescence analyzer
 Respiratory Medicine (2008) 102, 1667e1671 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed SHORT COMMUNICATION Comparison of exhaled nitric oxide measurements between
Respiratory Medicine (2008) 102, 1667e1671 available at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed SHORT COMMUNICATION Comparison of exhaled nitric oxide measurements between
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Exhaled Nitric Oxide during Academic Examination Stress in Students with Asthma
 Online Data Supplement Exhaled Nitric Oxide during Academic Examination Stress in Students with Asthma Thomas Ritz 1, Ana F. Trueba 1,2, Jiayan Liu 3, Richard J. Auchus 3,4, and David Rosenfield 1 1 Department
Online Data Supplement Exhaled Nitric Oxide during Academic Examination Stress in Students with Asthma Thomas Ritz 1, Ana F. Trueba 1,2, Jiayan Liu 3, Richard J. Auchus 3,4, and David Rosenfield 1 1 Department
2.6 MONITORING ASTHMA
 2.6 MONITORING ASTHMA 2.6.1 MONITORING ASTHMA IN ADULTS In the majority of patients with asthma symptom-based monitoring is adequate. Patients achieving control of symptoms with treatment have a low risk
2.6 MONITORING ASTHMA 2.6.1 MONITORING ASTHMA IN ADULTS In the majority of patients with asthma symptom-based monitoring is adequate. Patients achieving control of symptoms with treatment have a low risk
Sponsor. Generic drug name. Trial indication(s) Protocol number. Protocol title. Clinical trial phase. Study Start/End Dates.
 Sponsor Novartis Generic drug name Fluticasone propionate Trial indication(s) Moderate-severe bronchial asthma Protocol number CQAE397A2202 Protocol title A randomized open label study to assess the utility
Sponsor Novartis Generic drug name Fluticasone propionate Trial indication(s) Moderate-severe bronchial asthma Protocol number CQAE397A2202 Protocol title A randomized open label study to assess the utility
Comparison of 2 Methods to Correct for Peripheral Nitric Oxide Exchange in the Lungs
 Correction for Alveolar Nitric Oxide ORIGINAL ARTICLE Comparison of Methods to Correct for Peripheral Nitric Oxide Exchange in the Lungs L Prieto, 1 V López, D Barato, J Marin 1 1 Universidad de Valencia,
Correction for Alveolar Nitric Oxide ORIGINAL ARTICLE Comparison of Methods to Correct for Peripheral Nitric Oxide Exchange in the Lungs L Prieto, 1 V López, D Barato, J Marin 1 1 Universidad de Valencia,
A new and more accurate technique to characterize airway nitric oxide using different breath-hold times
 A new and more accurate technique to characterize airway nitric oxide using different breath-hold times Hye-Won Shin, Peter Condorelli and Steven C. George Journal of Applied Physiology 98:1869-1877, 2005.
A new and more accurate technique to characterize airway nitric oxide using different breath-hold times Hye-Won Shin, Peter Condorelli and Steven C. George Journal of Applied Physiology 98:1869-1877, 2005.
This is a cross-sectional analysis of the National Health and Nutrition Examination
 SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
SUPPLEMENTAL METHODS Study Design and Setting This is a cross-sectional analysis of the National Health and Nutrition Examination Survey (NHANES) data 2007-2008, 2009-2010, and 2011-2012. The NHANES is
The FDA Critical Path Initiative
 The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
The FDA Critical Path Initiative Clinical Considerations for Demonstration of Dose-response for Inhaled Corticosteroids - Exhaled Nitric Oxide Model Badrul A. Chowdhury, MD, PhD Director Division of Pulmonary
A comparison of global questions versus health status questionnaires as measures of the severity and impact of asthma
 Eur Respir J 1999; 1: 591±596 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 A comparison of global questions versus health status questionnaires
Eur Respir J 1999; 1: 591±596 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 1999 European Respiratory Journal ISSN 93-1936 A comparison of global questions versus health status questionnaires
Title montelukast on small airways inflam.
 Title Effects of 24-week add-on treatment montelukast on small airways inflam Nakaji, Hitoshi; Petrova, Guergana; Author(s) Toshiyuki; Ito, Isao; Oguma, Tsuyos Tomoko; Nagasaki, Tadao; Kanemitsu, Akio;
Title Effects of 24-week add-on treatment montelukast on small airways inflam Nakaji, Hitoshi; Petrova, Guergana; Author(s) Toshiyuki; Ito, Isao; Oguma, Tsuyos Tomoko; Nagasaki, Tadao; Kanemitsu, Akio;
Exhaled nitric oxide as a marker of asthma control in smoking patients
 ERJ Express. Published on January 22, 2009 as doi: 10.1183/09031936.00154008 Exhaled nitric oxide as a marker of asthma control in smoking patients Alain Michils 1, MD; Renaud Louis 2, MD; Rudi Peché 3,
ERJ Express. Published on January 22, 2009 as doi: 10.1183/09031936.00154008 Exhaled nitric oxide as a marker of asthma control in smoking patients Alain Michils 1, MD; Renaud Louis 2, MD; Rudi Peché 3,
Small Airways : How To Confident Diagnosis and Management?
 Small Airways : How To Confident Diagnosis and Management? Assistant Prof. Siwasak Juthong. M.D. Division of Respiratory and Respiratory Critical Care Medicine Faculty of Medicine Prince of Songkla University
Small Airways : How To Confident Diagnosis and Management? Assistant Prof. Siwasak Juthong. M.D. Division of Respiratory and Respiratory Critical Care Medicine Faculty of Medicine Prince of Songkla University
Do We Need Biologics in Pediatric Asthma Management?
 Do We Need Biologics in Pediatric Asthma Management? Ting Fan LEUNG, MBChB, MD, FRCPCH, FAAAAI Professor and Chairman Department of Paediatrics The Chinese University of Hong Kong Asthma and Allergy by
Do We Need Biologics in Pediatric Asthma Management? Ting Fan LEUNG, MBChB, MD, FRCPCH, FAAAAI Professor and Chairman Department of Paediatrics The Chinese University of Hong Kong Asthma and Allergy by
Choosing an inhaler for COPD made simple. Dr Simon Hart Castle Hill Hospital
 Choosing an inhaler for COPD made simple Dr Simon Hart Castle Hill Hospital 1 Declaration of interests I have received speaker fees, sponsorship to attend conferences, and funding for research from companies
Choosing an inhaler for COPD made simple Dr Simon Hart Castle Hill Hospital 1 Declaration of interests I have received speaker fees, sponsorship to attend conferences, and funding for research from companies
A diagnosis of asthma is made on the basis of compatible
 383 ASTHMA Exhaled nitric oxide in the diagnosis of asthma: comparison with bronchial provocation tests N Berkman, A Avital, R Breuer, E Bardach, C Springer, S Godfrey... See end of article for authors
383 ASTHMA Exhaled nitric oxide in the diagnosis of asthma: comparison with bronchial provocation tests N Berkman, A Avital, R Breuer, E Bardach, C Springer, S Godfrey... See end of article for authors
Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma
 Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Original Article Importance of fractional exhaled nitric oxide in diagnosis of bronchiectasis accompanied with bronchial asthma Feng-Jia Chen, Huai Liao, Xin-Yan Huang, Can-Mao Xie Department of Respiratory
Adenosine 5=-monophosphate challenge elicits a more peripheral airway response than methacholine challenge
 J Appl Physiol 110: 1241 1247, 2011. First published March 10, 2011; doi:10.1152/japplphysiol.01401.2010. Adenosine 5=-monophosphate challenge elicits a more peripheral airway response than methacholine
J Appl Physiol 110: 1241 1247, 2011. First published March 10, 2011; doi:10.1152/japplphysiol.01401.2010. Adenosine 5=-monophosphate challenge elicits a more peripheral airway response than methacholine
Phenotypes of asthma; implications for treatment. Medical Grand Rounds Feb 2018 Jim Martin MD DSc
 Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
Phenotypes of asthma; implications for treatment Medical Grand Rounds Feb 2018 Jim Martin MD DSc No conflicts to declare Objectives To understand the varied clinical forms of asthma To understand the pathobiologic
The case for extra fine particle ICS:! to cover the entire lung!
 The case for extra fine particle ICS: to cover the entire lung Richard J. Martin, M.D. Chairman Department of Medicine National Jewish Health The Edelstein Chair in Pulmonary Medicine Professor of Medicine
The case for extra fine particle ICS: to cover the entire lung Richard J. Martin, M.D. Chairman Department of Medicine National Jewish Health The Edelstein Chair in Pulmonary Medicine Professor of Medicine
Biologics in asthma Are we turning the corner? Roland Buhl Pulmonary Department Mainz University Hospital
 Biologics in asthma Are we turning the corner? Roland Buhl Pulmonary Department Mainz University Hospital Biologics in asthma - are we turning the corner? Allergic asthma anti - IgE Allergic airway inflammation
Biologics in asthma Are we turning the corner? Roland Buhl Pulmonary Department Mainz University Hospital Biologics in asthma - are we turning the corner? Allergic asthma anti - IgE Allergic airway inflammation
Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 4 Number 2 Difference Between The Slow Vital Capacity And Forced Vital Capacity: Predictor Of Hyperinflation In Patients With Airflow Obstruction
NG80. Asthma: diagnosis, monitoring and chronic asthma management (NG80)
 Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
Asthma: diagnosis, monitoring and chronic asthma management (NG80) NG80 NICE has checked the use of its content in this product and the sponsor has had no influence on the content of this booklet. NICE
#1 cause of school absenteeism in children 13 million missed days annually
 Asthma Update 2013 Jennifer W. McCallister, MD, FACP, FCCP Associate Professor Pulmonary & Critical Care Medicine The Ohio State University Wexner Medical Center Disclosures None 2 Objectives Review burden
Asthma Update 2013 Jennifer W. McCallister, MD, FACP, FCCP Associate Professor Pulmonary & Critical Care Medicine The Ohio State University Wexner Medical Center Disclosures None 2 Objectives Review burden
B Y L E S L I E K U M P F, R R T, C P F T, A E - C
 FeNO B Y L E S L I E K U M P F, R R T, C P F T, A E - C LESLIE KUMPF RRT, CPFT, AE-C Graduated from Henry Ford with a degree in Respiratory Therapy in 2006 Currently working on my BSRT Help start the RRT
FeNO B Y L E S L I E K U M P F, R R T, C P F T, A E - C LESLIE KUMPF RRT, CPFT, AE-C Graduated from Henry Ford with a degree in Respiratory Therapy in 2006 Currently working on my BSRT Help start the RRT
Predicting response to triamcinolone in severe asthma by machine learning: solving the Enigma
 Page 1 of 5 Predicting response to triamcinolone in severe asthma by machine learning: solving the Enigma Kian Fan Chung National Heart & Lung Institute, Imperial College London & Royal Brompton and Harefield
Page 1 of 5 Predicting response to triamcinolone in severe asthma by machine learning: solving the Enigma Kian Fan Chung National Heart & Lung Institute, Imperial College London & Royal Brompton and Harefield
Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma?
 Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Respiratory Medicine (2006) 100, 458 462 Do current treatment protocols adequately prevent airway remodeling in children with mild intermittent asthma? Haim S. Bibi a,, David Feigenbaum a, Mariana Hessen
Domiciliary diurnal variation of exhaled nitric oxide fraction for asthma control
 ORIGINAL ARTICLE ASTHMA Domiciliary diurnal variation of exhaled nitric oxide fraction for asthma control Junpei Saito, David Gibeon, Patricia Macedo, Andrew Menzies-Gow, Pankaj K. Bhavsar and Kian Fan
ORIGINAL ARTICLE ASTHMA Domiciliary diurnal variation of exhaled nitric oxide fraction for asthma control Junpei Saito, David Gibeon, Patricia Macedo, Andrew Menzies-Gow, Pankaj K. Bhavsar and Kian Fan
ASTHMA TREATMENT EFFICACY ASSESSMENT BY FeNO MEASUREMENT
 Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 ASTHMA TREATMENT EFFICACY ASSESSMENT BY FeNO MEASUREMENT Dana ALEXANDRESCU 1 Abstract: The author of
Bulletin of the Transilvania University of Braşov Series VI: Medical Sciences Vol. 5 (54) No. 2-2012 ASTHMA TREATMENT EFFICACY ASSESSMENT BY FeNO MEASUREMENT Dana ALEXANDRESCU 1 Abstract: The author of
Association between asthma control and bronchial hyperresponsiveness and airways inflammation: a cross-sectional study in daily practice
 Association between asthma control and bronchial hyperresponsiveness and airways inflammation: a cross-sectional study in daily practice V. Quaedvlieg, J. Sele, M. Henket and R. Louis Department of Respiratory
Association between asthma control and bronchial hyperresponsiveness and airways inflammation: a cross-sectional study in daily practice V. Quaedvlieg, J. Sele, M. Henket and R. Louis Department of Respiratory
Searching for Targets to Control Asthma
 Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Searching for Targets to Control Asthma Timothy Craig Distinguished Educator Professor Medicine and Pediatrics Penn State University Hershey, PA, USA Inflammation and Remodeling in Asthma The most important
Evidence-based recommendations or Show me the patients selected and I will tell you the results
 Respiratory Medicine (2006) 100, S17 S21 Evidence-based recommendations or Show me the patients selected and I will tell you the results Leif Bjermer Department of Respiratory Medicine & Allergology, 221
Respiratory Medicine (2006) 100, S17 S21 Evidence-based recommendations or Show me the patients selected and I will tell you the results Leif Bjermer Department of Respiratory Medicine & Allergology, 221
(Asthma) Diagnosis, monitoring and chronic asthma management
 Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
Dubai Standards of Care 2018 (Asthma) Diagnosis, monitoring and chronic asthma management Preface Asthma is one of the most common problem dealt with in daily practice. In Dubai, the management of chronic
Spirometry is the most frequently performed. Obstructive and restrictive spirometric patterns: fixed cut-offs for FEV1/FEV6 and FEV6
 Eur Respir J 2006; 27: 378 383 DOI: 10.1183/09031936.06.00036005 CopyrightßERS Journals Ltd 2006 Obstructive and restrictive spirometric patterns: fixed cut-offs for FEV1/ and J. Vandevoorde*, S. Verbanck
Eur Respir J 2006; 27: 378 383 DOI: 10.1183/09031936.06.00036005 CopyrightßERS Journals Ltd 2006 Obstructive and restrictive spirometric patterns: fixed cut-offs for FEV1/ and J. Vandevoorde*, S. Verbanck
HCT Medical Policy. Bronchial Thermoplasty. Policy # HCT113 Current Effective Date: 05/24/2016. Policy Statement. Overview
 HCT Medical Policy Bronchial Thermoplasty Policy # HCT113 Current Effective Date: 05/24/2016 Medical Policies are developed by HealthyCT to assist in administering plan benefits and constitute neither
HCT Medical Policy Bronchial Thermoplasty Policy # HCT113 Current Effective Date: 05/24/2016 Medical Policies are developed by HealthyCT to assist in administering plan benefits and constitute neither
Assessment of accuracy and applicability of a new electronic peak flow meter and asthma monitor
 Eur Respir J 18; 12: 45 42 DOI: 18/1.8.5 Printed in UK - all rights reserved Copyright ERS Journals Ltd 18 European Respiratory Journal ISSN - 1 Assessment of accuracy and applicability of a new electronic
Eur Respir J 18; 12: 45 42 DOI: 18/1.8.5 Printed in UK - all rights reserved Copyright ERS Journals Ltd 18 European Respiratory Journal ISSN - 1 Assessment of accuracy and applicability of a new electronic
Exhaled Nitric Oxide Today s Asthma Biomarker. Richard F. Lavi, MD FAAAAI FAAP
 Exhaled Nitric Oxide Today s Asthma Biomarker Richard F. Lavi, MD FAAAAI FAAP Objectives Describe exhaled nitric oxide physiology and pathophysiology Review the current literature regarding exhaled nitric
Exhaled Nitric Oxide Today s Asthma Biomarker Richard F. Lavi, MD FAAAAI FAAP Objectives Describe exhaled nitric oxide physiology and pathophysiology Review the current literature regarding exhaled nitric
CIRCULAR INSTRUCTION REGARDING ESTABLISHMENT OF IMPAIRMENT DUE TO OCCUPATIONAL LUNG DISEASE FOR THE PURPOSES OF AWARDING PERMANENT DISABLEMENT
 Circular Instruction 195 CIRCULAR INSTRUCTION REGARDING ESTABLISHMENT OF IMPAIRMENT DUE TO OCCUPATIONAL LUNG DISEASE FOR THE PURPOSES OF AWARDING PERMANENT DISABLEMENT COMPENSATION FOR OCCUPATIONAL INJURIES
Circular Instruction 195 CIRCULAR INSTRUCTION REGARDING ESTABLISHMENT OF IMPAIRMENT DUE TO OCCUPATIONAL LUNG DISEASE FOR THE PURPOSES OF AWARDING PERMANENT DISABLEMENT COMPENSATION FOR OCCUPATIONAL INJURIES
Small airways ventilation heterogeneity and hyperinfl ation in COPD: Response to tiotropium bromide
 ORIGINAL RESEARCH Small airways ventilation heterogeneity and hyperinfl ation in COPD: Response to tiotropium bromide Sylvia Verbanck Daniël Schuermans Walter Vincken Respiratory Division, University Hospital
ORIGINAL RESEARCH Small airways ventilation heterogeneity and hyperinfl ation in COPD: Response to tiotropium bromide Sylvia Verbanck Daniël Schuermans Walter Vincken Respiratory Division, University Hospital
Prevalence of undetected persistent airflow obstruction in male smokers years old
 2 Prevalence of undetected persistent airflow obstruction in male smokers 40-65 years old Geijer RMM Sachs APE Hoes AW Salomé PL Lammers J-WJ Verheij TJM Published in: Family Practice 2005;22:485-489 Abstract
2 Prevalence of undetected persistent airflow obstruction in male smokers 40-65 years old Geijer RMM Sachs APE Hoes AW Salomé PL Lammers J-WJ Verheij TJM Published in: Family Practice 2005;22:485-489 Abstract
Diagnostic value of post-bronchodilator pulmonary function testing to distinguish between stable, moderate to severe COPD and asthma
 ORIGINAL RESEARCH Diagnostic value of post-bronchodilator pulmonary function testing to distinguish between stable, moderate to severe COPD and asthma Daphne C Richter 1 James R Joubert 1 Haylene Nell
ORIGINAL RESEARCH Diagnostic value of post-bronchodilator pulmonary function testing to distinguish between stable, moderate to severe COPD and asthma Daphne C Richter 1 James R Joubert 1 Haylene Nell
Flow-independent nitric oxide exchange parameters in healthy adults
 J Appl Physiol 91: 2173 2181, 2001. Flow-independent nitric oxide exchange parameters in healthy adults HYE-WON SHIN, 1 CHRISTINE M. ROSE-GOTTRON, 5 FEDERICO PEREZ, 1 DAN M. COOPER, 3,5 ARCHIE F. WILSON,
J Appl Physiol 91: 2173 2181, 2001. Flow-independent nitric oxide exchange parameters in healthy adults HYE-WON SHIN, 1 CHRISTINE M. ROSE-GOTTRON, 5 FEDERICO PEREZ, 1 DAN M. COOPER, 3,5 ARCHIE F. WILSON,
Inhaled and systemic corticosteroid response in severe asthma assessed by alveolar nitric oxide: a randomized crossover pilot study of add-on therapy
 British Journal of Clinical Pharmacology DOI:1.1111/j.1365-2125.212.4319.x Inhaled and systemic corticosteroid response in severe asthma assessed by alveolar nitric oxide: a randomized crossover pilot
British Journal of Clinical Pharmacology DOI:1.1111/j.1365-2125.212.4319.x Inhaled and systemic corticosteroid response in severe asthma assessed by alveolar nitric oxide: a randomized crossover pilot
CHAPTER 5. Weekly self-monitoring and treatment adjustment benefit patients with partly controlled and uncontrolled asthma
 CHAPTER 5 Weekly self-monitoring and treatment adjustment benefit patients with partly controlled and uncontrolled asthma Victor van der Meer, Henk F. van Stel, Moira J. Bakker, Albert C. Roldaan, Willem
CHAPTER 5 Weekly self-monitoring and treatment adjustment benefit patients with partly controlled and uncontrolled asthma Victor van der Meer, Henk F. van Stel, Moira J. Bakker, Albert C. Roldaan, Willem
Potency ratio fluticasone propionate (Flixotide Diskus)/budesonide (Pulmicort Turbuhaler)
 Respiratory Medicine (2007) 101, 610 615 Potency ratio fluticasone propionate (Flixotide Diskus)/budesonide (Pulmicort Turbuhaler) Björn Ställberg a, Eva Pilman b, Bengt-Eric Skoogh c,, Bengt Arne Hermansson
Respiratory Medicine (2007) 101, 610 615 Potency ratio fluticasone propionate (Flixotide Diskus)/budesonide (Pulmicort Turbuhaler) Björn Ställberg a, Eva Pilman b, Bengt-Eric Skoogh c,, Bengt Arne Hermansson
Alveolar and Bronchial Nitric Oxide Output in Healthy Children
 43:1242 1248 (2008) Alveolar and Bronchial Nitric Oxide Output in Healthy Children Anna Sepponen, MD, 1,2 Lauri Lehtimäki, MD, 1,2,3 Heini Huhtala, MSc, 4 Minna Kaila, MD, 5,6 Hannu Kankaanranta, MD, 1,2,7
43:1242 1248 (2008) Alveolar and Bronchial Nitric Oxide Output in Healthy Children Anna Sepponen, MD, 1,2 Lauri Lehtimäki, MD, 1,2,3 Heini Huhtala, MSc, 4 Minna Kaila, MD, 5,6 Hannu Kankaanranta, MD, 1,2,7
Yuriy Feschenko, Liudmyla Iashyna, Ksenia Nazarenko and Svitlana Opimakh
 2018; 7(1): 74-78 ISSN (E): 2277-7695 ISSN (P): 2349-8242 NAAS Rating: 5.03 TPI 2018; 7(1): 74-78 2018 TPI www.thepharmajournal.com Received: 11-11-2017 Accepted: 12-12-2017 Yuriy Feschenko Liudmyla Iashyna
2018; 7(1): 74-78 ISSN (E): 2277-7695 ISSN (P): 2349-8242 NAAS Rating: 5.03 TPI 2018; 7(1): 74-78 2018 TPI www.thepharmajournal.com Received: 11-11-2017 Accepted: 12-12-2017 Yuriy Feschenko Liudmyla Iashyna
Supramaximal flow in asthmatic patients
 Eur Respir J ; 19: 13 17 DOI: 1.113/93193..51 Printed in UK all rights reserved Copyright #ERS Journals Ltd European Respiratory Journal ISSN 93-193 Supramaximal flow in asthmatic patients H. Sala*, A.
Eur Respir J ; 19: 13 17 DOI: 1.113/93193..51 Printed in UK all rights reserved Copyright #ERS Journals Ltd European Respiratory Journal ISSN 93-193 Supramaximal flow in asthmatic patients H. Sala*, A.
Defining COPD. Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist
 Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
International Journal of Medical Research & Health Sciences
 International Journal of Medical Research & Health Sciences www.ijmrhs.com Volume 2 Issue 3 July - Sep Coden: IJMRHS Copyright @2013 ISSN: 2319-5886 Received: 23 th May 2013 Revised: 24 th Jun 2013 Accepted:
International Journal of Medical Research & Health Sciences www.ijmrhs.com Volume 2 Issue 3 July - Sep Coden: IJMRHS Copyright @2013 ISSN: 2319-5886 Received: 23 th May 2013 Revised: 24 th Jun 2013 Accepted:
Pharmacological Management of Obstructive Airways in Humans. Introduction to Scientific Research. Submitted: 12/4/08
 Pharmacological Management of Obstructive Airways in Humans Introduction to Scientific Research Submitted: 12/4/08 Introduction: Obstructive airways can be characterized as inflammation or structural changes
Pharmacological Management of Obstructive Airways in Humans Introduction to Scientific Research Submitted: 12/4/08 Introduction: Obstructive airways can be characterized as inflammation or structural changes
Using Patient Characteristics to Individualize and Improve Asthma Care
 Using Patient Characteristics to Individualize and Improve Asthma Care Leonard B. Bacharier, M.D. Associate Professor of Pediatrics Clinical Director, Division of Allergy, Immunology, & Pulmonary Medicine
Using Patient Characteristics to Individualize and Improve Asthma Care Leonard B. Bacharier, M.D. Associate Professor of Pediatrics Clinical Director, Division of Allergy, Immunology, & Pulmonary Medicine
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Airway inflammation assessed by invasive and noninvasive means in severe asthma: Eosinophilic and noneosinophilic phenotypes
 Airway inflammation assessed by invasive and noninvasive means in severe asthma: Eosinophilic and noneosinophilic phenotypes Catherine Lemière, MD, MSc, a Pierre Ernst, MD, b Ron Olivenstein, MD, b Yasuhiro
Airway inflammation assessed by invasive and noninvasive means in severe asthma: Eosinophilic and noneosinophilic phenotypes Catherine Lemière, MD, MSc, a Pierre Ernst, MD, b Ron Olivenstein, MD, b Yasuhiro
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
Challenges in Meeting International Requirements for Clinical Bioequivalence of Inhaled Drug Products
 Challenges in Meeting International Requirements for Clinical Bioequivalence of Inhaled Drug Products Tushar Shah, M.D. Sr. VP, Global Respiratory Research and Development TEVA Pharmaceuticals 1 Presentation
Challenges in Meeting International Requirements for Clinical Bioequivalence of Inhaled Drug Products Tushar Shah, M.D. Sr. VP, Global Respiratory Research and Development TEVA Pharmaceuticals 1 Presentation
compare patients preferences and costs for asthma treatment regimens targeting three
 APPENDIX I ADDITIONAL METHODS Trial design The Accurate trial lasted from September 2009 until January 2012 and was designed to compare patients preferences and costs for asthma treatment regimens targeting
APPENDIX I ADDITIONAL METHODS Trial design The Accurate trial lasted from September 2009 until January 2012 and was designed to compare patients preferences and costs for asthma treatment regimens targeting
Asthma: diagnosis and monitoring
 Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
Asthma: diagnosis and monitoring NICE guideline: short version Draft for second consultation, July 01 This guideline covers assessing, diagnosing and monitoring suspected or confirmed asthma in adults,
Evaluation of Exhaled Nitric Oxide in Schoolchildren at Different Exhalation Flow Rates
 0031-3998/02/5203-0393 PEDIATRIC RESEARCH Vol. 52, No. 3, 2002 Copyright 2002 International Pediatric Research Foundation, Inc. Printed in U.S.A. Evaluation of Exhaled Nitric Oxide in Schoolchildren at
0031-3998/02/5203-0393 PEDIATRIC RESEARCH Vol. 52, No. 3, 2002 Copyright 2002 International Pediatric Research Foundation, Inc. Printed in U.S.A. Evaluation of Exhaled Nitric Oxide in Schoolchildren at
Strategy Aimed at Reduction of Sputum Eosinophils Decreases Exacerbation Rate in Patients with Asthma
 The Journal of International Medical Research 2006; 34: 129 139 Strategy Aimed at Reduction of Sputum Eosinophils Decreases Exacerbation Rate in Patients with Asthma J CHLUMSKÝ 1, I STRIZ 2, M TERL 3 AND
The Journal of International Medical Research 2006; 34: 129 139 Strategy Aimed at Reduction of Sputum Eosinophils Decreases Exacerbation Rate in Patients with Asthma J CHLUMSKÝ 1, I STRIZ 2, M TERL 3 AND
WEBINAR. Difficult-to-treat and severe asthma: changing the paradigm
 WEBINAR Difficult-to-treat and severe asthma: changing the paradigm A multidisciplinary discussion on new therapies, and how to identify and manage difficult-to-treat and severe asthma DIFFICULT-TO-TREAT
WEBINAR Difficult-to-treat and severe asthma: changing the paradigm A multidisciplinary discussion on new therapies, and how to identify and manage difficult-to-treat and severe asthma DIFFICULT-TO-TREAT
PULMONARY FUNCTION TESTING. Purposes of Pulmonary Tests. General Categories of Lung Diseases. Types of PF Tests
 PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
PULMONARY FUNCTION TESTING Wyka Chapter 13 Various AARC Clinical Practice Guidelines Purposes of Pulmonary Tests Is lung disease present? If so, is it reversible? If so, what type of lung disease is present?
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Papi A, Canonica GW, Maestrelli P, et al. Rescue use of beclomethasone
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Papi A, Canonica GW, Maestrelli P, et al. Rescue use of beclomethasone
Life-long asthma and its relationship to COPD. Stephen T Holgate School of Medicine University of Southampton
 Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
Life-long asthma and its relationship to COPD Stephen T Holgate School of Medicine University of Southampton Definitions COPD is a preventable and treatable disease with some significant extrapulmonary
The effect of active and passive smoking on inhaled drugs in respiratory patients
 CHAPTER 12 The effect of active and passive smoking on inhaled drugs in respiratory patients G. Invernizzi*, A. Ruprecht*, P. Paredi #, R. Mazza*, C. De Marco*, R. Boffi* *Tobacco Control Unit, National
CHAPTER 12 The effect of active and passive smoking on inhaled drugs in respiratory patients G. Invernizzi*, A. Ruprecht*, P. Paredi #, R. Mazza*, C. De Marco*, R. Boffi* *Tobacco Control Unit, National
THE COPD-ASTHMA OVERLAP SYNDROME
 THE COPD-ASTHMA OVERLAP SYNDROME NICOLA A. HANANIA, MD, MS, FRCP(C), FCCP, FACP ASSOCIATE PROFESSOR OF MEDICINE DIRECTOR OF ASTHMA & COPD CLINICAL RESEARCH CENTER BAYLOR COLLEGE OF MEDICINE HOUSTON, TX
THE COPD-ASTHMA OVERLAP SYNDROME NICOLA A. HANANIA, MD, MS, FRCP(C), FCCP, FACP ASSOCIATE PROFESSOR OF MEDICINE DIRECTOR OF ASTHMA & COPD CLINICAL RESEARCH CENTER BAYLOR COLLEGE OF MEDICINE HOUSTON, TX
Starting with a Higher Dose of Inhaled Corticosteroids in Primary Care Asthma Treatment
 Starting with a Higher Dose of Inhaled Corticosteroids in Primary Care Asthma Treatment THYS van der MOLEN, BETTY MEYBOOM-DE JONG, HELMA H. MULDER, and DIRKJE S. POSTMA Department of General Practice,
Starting with a Higher Dose of Inhaled Corticosteroids in Primary Care Asthma Treatment THYS van der MOLEN, BETTY MEYBOOM-DE JONG, HELMA H. MULDER, and DIRKJE S. POSTMA Department of General Practice,
Study designs and PD/Clinical endpoints to demonstrate therapeutic equivalence: European Views
 IPAC-RS/University of Florida Study designs and PD/Clinical endpoints to demonstrate therapeutic equivalence: European Views 20 th March 2014 Dr. Alfredo García - Arieta Head of the Service of Generic
IPAC-RS/University of Florida Study designs and PD/Clinical endpoints to demonstrate therapeutic equivalence: European Views 20 th March 2014 Dr. Alfredo García - Arieta Head of the Service of Generic
Increased nitric oxide in exhaled air: an early marker of asthma in non-smoking aluminium potroom workers?
 274 Department of Thoracic Medicine, The National Hospital, University of Oslo, Norway M B Lund R Hamre J Kongerud Health Department, Elkem Aluminium, Mosjøen, Norway P I Øksne Correspondence to: Dr M
274 Department of Thoracic Medicine, The National Hospital, University of Oslo, Norway M B Lund R Hamre J Kongerud Health Department, Elkem Aluminium, Mosjøen, Norway P I Øksne Correspondence to: Dr M
Achieving guideline-based asthma control: does the patient benefit?
 Eur Respir J ; : 88 9 DOI:.8/99..97 Printed in UK all rights reserved Copyright #ERS Journals Ltd European Respiratory Journal ISSN 9-9 Achieving guideline-based asthma control: does the patient benefit?
Eur Respir J ; : 88 9 DOI:.8/99..97 Printed in UK all rights reserved Copyright #ERS Journals Ltd European Respiratory Journal ISSN 9-9 Achieving guideline-based asthma control: does the patient benefit?
Maximal expiratory flow rates (MEFR) measured. Maximal Inspiratory Flow Rates in Patients With COPD*
 Maximal Inspiratory Flow Rates in Patients With COPD* Dan Stănescu, MD, PhD; Claude Veriter, MA; and Karel P. Van de Woestijne, MD, PhD Objectives: To assess the relevance of maximal inspiratory flow rates
Maximal Inspiratory Flow Rates in Patients With COPD* Dan Stănescu, MD, PhD; Claude Veriter, MA; and Karel P. Van de Woestijne, MD, PhD Objectives: To assess the relevance of maximal inspiratory flow rates
Difficult Asthma Assessment: A systematic approach
 Difficult Asthma Assessment: A systematic approach Dr Naghmeh Radhakrishna Respiratory, Sleep & Allergy Physician Allergy, Asthma & Clinical Immunology Service The Alfred Hospital Melbourne, Australia
Difficult Asthma Assessment: A systematic approach Dr Naghmeh Radhakrishna Respiratory, Sleep & Allergy Physician Allergy, Asthma & Clinical Immunology Service The Alfred Hospital Melbourne, Australia
Combined use of exhaled nitric oxide and airway hyperresponsiveness in characterizing asthma in a large population survey
 Eur Respir J 2000; 15: 849±855 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Combined use of exhaled nitric oxide and airway hyperresponsiveness
Eur Respir J 2000; 15: 849±855 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Combined use of exhaled nitric oxide and airway hyperresponsiveness
Lung Physiology and How Aerosol Deposits in the Lungs. 1. Physiological and Anatomical Background
 XA0100097 43 Lung Physiology and How Aerosol Deposits in the Lungs Toyoharu Isawa, M.D. 1. Physiological and Anatomical Background Weibel's morphologic data has been referred to not only for predicting
XA0100097 43 Lung Physiology and How Aerosol Deposits in the Lungs Toyoharu Isawa, M.D. 1. Physiological and Anatomical Background Weibel's morphologic data has been referred to not only for predicting
University of Dundee. Published in: Lung. DOI: /s Publication date: 2016
 University of Dundee Is Gly16Arg 2 Receptor Polymorphism Related to Impulse Oscillometry in a Real-Life Asthma Clinic Setting? Jabbal, Sunny; Manoharan, Arvind; Lipworth, Joseph; Anderson, William; Short,
University of Dundee Is Gly16Arg 2 Receptor Polymorphism Related to Impulse Oscillometry in a Real-Life Asthma Clinic Setting? Jabbal, Sunny; Manoharan, Arvind; Lipworth, Joseph; Anderson, William; Short,
Can the Asthma Control Questionnaire be used to differentiate between patients with controlled. uncontrolled asthma symptoms?
 Ó The Author (2006). Published by Oxford University Press. All rights reserved. For permissions, please email: journals.permissions@oxfordjournals.org doi:10.1093/fampra/cml041 Family Practice Advance
Ó The Author (2006). Published by Oxford University Press. All rights reserved. For permissions, please email: journals.permissions@oxfordjournals.org doi:10.1093/fampra/cml041 Family Practice Advance
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A.
 aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
aclidinium 322 micrograms inhalation powder (Eklira Genuair ) SMC No. (810/12) Almirall S.A. 05 October 2012 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and
Traiter l asthme sévère par le phénotype. Dr. Alain Michils CUB-Hôpital Erasme
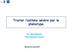 Traiter l asthme sévère par le phénotype Dr. Alain Michils CUB-Hôpital Erasme Darwin 25 mars 2017 Step 5 treatment (GINA 2016) STEP 5 STEP 4 PREFERRED CONTROLLER CHOICE STEP 1 STEP 2 Low dose ICS STEP
Traiter l asthme sévère par le phénotype Dr. Alain Michils CUB-Hôpital Erasme Darwin 25 mars 2017 Step 5 treatment (GINA 2016) STEP 5 STEP 4 PREFERRED CONTROLLER CHOICE STEP 1 STEP 2 Low dose ICS STEP
