Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity
|
|
|
- Kristopher Cook
- 6 years ago
- Views:
Transcription
1 Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 ORIGINAL RESEARCH ARTICLE Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity Roberto W Dal Negro 1*, Silvia Tognella 1, Massimo Guerriero 2 and Claudio Micheletto 3 Open Access Abstract Background: Tracheobronchomalacia (TBM) is a pathologic condition in which softening of tracheal and bronchial cartilage causes the dynamic narrowing of transverse or sagittal diameters of tracheobronchial lumen; an excessive dynamic airway collapse (EDAC) may also be associated, with a substantial invagination of the posterior membrane of trachebronchial tree. The aim of this study was to assess the prevalence of both TBM and EDAC in a population of asthmatics with different degrees of disease severity compared to a reference group of subjects without any bronchial obstruction. Methods: A cohort of 202 asthmatics was investigated by means of a dynamic flexible videobronchoscopy: 74 mild persistent (MPA - age ys; 35 males; mean FEV 1 = 88.6% pred. ± 8.3 sd); 63 moderate (MA - age ys; 30 males; mean FEV 1 = 71.3% pred. ± 9.1 sd), 65 severe asthmatics (SA - age ys; 25 males; mean FEV 1 = 48.5% pred. ± 7.6 sd), and 62 non obstructed subjects (NO - age ys; 38 males; mean FEV % pred. ± 2.7 sd). TBM and EDAC were classified according to FEMOS classification. Results: TBM and EDAC were observed in only 1/62 subjects (both 1.61%) of NO group, while their prevalence was 2.70% and 6.75% in MPA group; 7.93% and 19.04% in MA group; 18.46% and 69.23% in SA group, respectively. The crude prevalence of thyroid disorders in the population was 12.9%. In particular, the prevalence of thyroid disorders was significantly higher in females than in men, but 54-fold higher in females than in men in the presence of EDAC. Conclusions: 1) The prevalence of both TBM and EDAC is directly related to age, gender (females), and asthma severity; 2) EDAC is much more frequent than TBM in all asthma patients; 3) both tracheal abnormalities proved to be more represented in asthmatics with thyroid disorders, and particularly in female asthmatics with EDAC. Keywords: Bronchial asthma, Collapse, Excessive dynamic airway, Thyroid disorders, Tracheobronchomalacia Background Tracheobronchomalacia (TBM) is a pathologic condition in which softening of tracheal and bronchial cartilage causes the dynamic narrowing of transverse or sagittal diameters of tracheobronchial lumen. This condition may or may not be associated with a substantial invagination of the posterior membrane of trachebronchial tree, an entity referred to an excessive dynamic airway collapse (EDAC), which is peculiar in some patients with * Correspondence: robertodalnegro@gmail.com 1 Respiratory Unit, Orlandi General Hospital, Via Ospedale 2, Bussolengo VR 37012, Italy Full list of author information is available at the end of the article obstructive pulmonary disease, such as chronic bronchitis, emphysema, asthma, or can represent an isolated finding in patients during cough or forced expiration. Tracheomalacia refers to a weakness of the trachea frequently due to a reduction and/or atrophy of the longitudinal elastic fibers of the pars membranacea or impaired cartilage integrity, such that the airway is softer and more susceptible to collapse [1,2]. This disease may arise congenitally (from disorders associated with impaired cartilage maturation or in combination with other abnormalities like tracheoesopageal fistula) or it may be acquired from prior intubation, trauma, infections, long standing extrinsic compression, or chronic inflammation 2013 Dal Negro et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
2 Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 Page 2 of 5 [3,4]. Localized TBM is usually seen in patients with prolonged endotracheal intubation, tracheostomy, or vascular rings. The cause of diffuse TBM is often unknown, but it is frequently seen in patients with common respiratory conditions, such as chronic bronchitis. Acquired TBM has been reported to be present in 4.5% of bronchoscopies in large general series [2]; in 12.7% of all patients undergoing bronchoscopy evaluation for respiratory disease [3], and in as many as 44% of patients undergoing bronchoscopy who have a history of chronic bronchitis [4]. It has been shown that chronic airway inflammation with diffuse panbronchiolitis might play a role in exacerbations of this disorder and the acquired form of TBM has been increasingly recognized as an important cause of chronic respiratory symptoms [5]. In TBM, central airway collapse is not closely related to airflow obstruction, and expiratory flow limitation at rest often occurs in peripheral airways without central airway collapse [6]. This pathologic airway weakening can lead to a dynamic outflow obstruction associated with symptoms (such as: dyspnea; orthopnea; intractable cough, and inability to clear secretions) which can sometimes mimic asthma worsening. Furthermore, TBM may also be associated with a substantial invagination of the posterior membrane of the tracheo-bronchial tree, an entity defined as excessive dynamic airway collapse (EDAC). [7]. To our knowledge, the incidence of TBM in patients with a reported history of asthma or Chronic Obstructive Pulmonary Disease (COPD) has not been extensively studied. However, several large studies in the general population suggest that the overall incidence of TBM is 5-10% [8,9]. However, at present, it is not generally known in which proportion patients with asthma have TBM or EDAC, and if these conditions are related to asthma severity. The aim of this study was to evaluate the prevalence of both TBM and EDAC in a population of asthmatics of different degrees of severity compared to a reference group of subjects without any airway obstruction. Methods A cohort of 202 non-smoking asthmatics was investigated: 74 mild persistent, MPA (age years; 35 males; mean FEV 1 = 88.6% pred. ± 8.3sd); 63 moderate asthmatics, MA (age years; 30 males; mean FEV 1 =71.3% pred. ± 9.1sd); 65 severe asthmatics, SA (age years; 25 males; mean FEV 1 = 48.5% pred. ±7.6sd. Criteria used for defining asthma in the present study were those accepted worldwide [10]. In particular, asthma diagnosis stemmed from subjects family and clinical data; from lung function tests (in particular, the variability of their airway obstruction; the reversibility (30 after salbutamol 400 mcg) of their flow limitation from basal values, and/or the measurement of their bronchial response to methacholine). All patients were already treated according to GINA guidelines [10]. All patients were in stable conditions at the time of their bronchoscopy. Another cohort of 62 non smoking subjects without any obstructive disease, NO (age years; 38 males; mean FEV % pred. ± 2.7sd) was also investigated from this point of view (during a bronchoscopy performed as part of an unrelated investigation) as a reference group. None of the subjects had a systemic disease or localized conditions known as possible cause of TBM. The study was approved by the local E.C. in date January 19th, 2010 (prot. n.: 1489). Diagnosis Bronchoscopic visualization of dynamic tracheal or bronchial collapse remains the gold standard for TBM diagnosis [11]. After the patients had signed the specific informed consent, all bronchoscopies were performed with topical anesthesia (lidocaine) and light sedation (midazolam mg ev). The patients were studied in the supine position and had undergone standard spirometry to determine FEV 1 the day before broncoscopy. During the examination, patients were able to breathe spontaneously and follow commands to perform deep breathing, forced exhalation, and cough maneuvers to elicit the collapsibility of the airways. The bronchoscope was introduced into the trachea, and at that point the patient was instructed to perform forced inspiratory and expiratory maneuvers with graded degrees of effort, according to a standard TBM protocol [6]. The bronchoscope was then advanced to 5 cm above the carina, and the patient was requested to perform again graded forced expiratory maneuvers. This procedure was then repeated at the entrance of the right and left main bronchi. All bronchoscopies were video recorded and reviewed after the procedure to assess the degree of airway collapse. Obviously, the airways collapsed during forced expiration, but in some cases the airway lumen was completely obliterated as the membranous trachea had collapsed to the cartilaginous rings. Dynamic CT scan images can define the normal range of intrathoracic tracheal diameters and cross-sectional areas during forced maneuvers, and it was shown that tracheal narrowing was about 80% in patients with TBM vs 35% in healthy men [12]; Stem et al. then recommended using a cutoff of 70% narrowing on forced expiration as a diagnostic threshold for TBM [12].
3 Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 Page 3 of 5 Classification TBM and EDAC were classified according to FEMOS classification, that addresses Functional status; Extent of abnormalities notes; Morfology of the abnomarlity; Origin of the abnormality, and Severity of the disease process [7]. In the present study, only moderate (expiratory airways collapse 75%) and severe (expiratory airway collapse of 100%, such as, the airway walls make contact) TBM or EDAC were considered. Statistics Quantitative variables were expressed as mean and standard deviation; categorical variables as absolute and relative frequencies. The Skewness test was used to check the normality in distribution for quantitative variables. Data were compared by t-test and Mann Whitney test, CHI-square test, and Fisher test as appropriate. The logistic regression model was used to estimate the odds ratio and to control the role of confounding variables; p < 0,05 was considered statistically significant. Statistical analysis was carried out by using STATA Release 12 (Stata Corp LP, Texas, USA). Results Bronchoscopic visualization of trachea and main bronchi was possible in all subjects, without significant adverse events. A moderate desaturation and wheezing occurred in 42 subjects immediately after the procedure, and they were quickly recovered with inhaled salbutamol (400 μg via spacer) and prednisone 40 mg e.v. All patients were monitored in the 2 hours following the bronchoscopic examination and were discharged from the Lung Unit only with normal values for systemic blood pressure, heart frequency and peripheral saturation. General characteristics of non-obstructive and of asthmatic subjects are reported in Table 1. Males were significantly prevailing in subjects of the reference group (p < 0.021); asthmatics were significantly older (p < ), and characterized by a lower mean FEV 1 value (p < ). The overall prevalence of TBM and EDAC proved quite lower (only 1 case) in non asthmatic subjects: therefore, no statistical inference is possible for groups consisting of 1 statistical unit. When considering the whole sample of asthmatics, TBM was present in 19 cases (9.4%) and EDAC in 62 cases (30.7%), being one of these abnormalities of central airways detectable in 41.1% of a general population of asthmatics (Table 1). Moreover, TBM was found in 2 (2.70%) and EDAC in 5 cases (6.75%) of mild persistent asthma (MPA), while TBM was found in 5 (7.93%) and EDAC in 12 cases (19.04%) of moderate persistent asthma (MA). Finally, TBM was found in 12 (18.46%) and EDAC in 45 cases (69.23%) of severe persistent asthma (SA). Both the TBM and the EDAC prevalence, as well as their ratio, are directly and significantly related (both p < ) to asthma severity according to an exponential function, particularly in the case of EDAC (Table 2). When compared to that of asthmatics without any tracheal abnormalities, the mean age in those with TBM or EDAC was higher (56.4 ± 10.2sd yr vs 44.6 ±13.0sd yr, p < , and 51.8 ± 12.5sd yr vs 43.5 ± 12.8 sd yr, p < 0.001, respectively). The crude prevalence of thyroid disorders in the population was 12.9% (34/264): in particular: thyroidectomy 52.9% (18/34); thyroiditis 26.5% (9/34); goiter 14.8% (5/34); malignancy 2.9% (1/34); other 2.9% (1/34) (Table 3). When the prevalence of thyroid disorders was investigated by gender, the OR calculated was = 8.77 (95% CI = (by the Fischer Exact Confidence method), such as the probability for the presence of thyroid disturbances was 5-fold higher in females than in males. Moreover, when the prevalence of both EDAC and thyroid disorders was compared by gender, the OR calculated was = (95% CI = ), such as, the probability for the presence of thyroid disturbances was 54-fold higher in females than in males with EDAC. Discussion During normal expiration, there is a physiologic reduction in all dimensions of intrathoracic airways; when changes occurring during forced inspiration and expiration are compared by a dynamic CT, a mean 35% decrease in the cross-sectional area of the trachea has been described [12]. Thus, a certain degree of dynamic airway collapse, characterized by invagination of the posterior membrane and narrowing of the cross-sectional area of the tracheobronchial tree, represents a physiologic event. However, this phenomenon is exaggerated in some patients suffering from obstructive airway disease, or it represents an isolated finding in some patients during cough and forced expiration. Table 1 General characteristics of non-obstructive and of asthmatic subjects Gender % m Age (yr) mean ± sd FEV 1 % pred. mean ± sd TBM n (%) EDAC n (%) Non-obstructive (n=62) ± ±3.7 1 (1.6%) 1 (1.6%) Asthmatics (n=202) ± ± (9.4%) 62 (30.7%) p General characteristics of asthmatic subjects are reported in Table 2 by asthma severity. Females were significantly more represented in severe asthmatics (p < 0.01).
4 Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 Page 4 of 5 Table 2 General characteristics of asthma subjects by their asthma severity, and the corresponding distribution of TBM and EDAC Gender % m Age (yr) mean±sd FEV 1 % pred. mean±sd TBM n (%) EDAC n (%) Mild Persistent Asthma (n = 74) ± ± (2.70%) 5 (6.75%) Moderate Asthma (n = 63) ± ± (7.93%) 12 (19.04%) Severe Asthma (n = 65) ± ± (18.46) 45 (69.23%) p* 0.01 (Mild-moderate vs severe) *anova. TBM is an increasingly recognized abnormality of the central airways and generally results from weakness of the tracheal or mainstem bronchial walls caused by either softening of the supporting cartilaginous rings, or redundancy of the connective tissue of the posterior membrane due to a reduction in size and number of elastic fibers, or both. TBM has been called tracheobronchial collapse, expiratory tracheobronchial collapse, expiratory tracheobronchial stenosis, and tracheobronchial dyskinesia. These various terms have not only provided an incomplete understanding of the pathophysiology of malacia and EDAC, but have also contributed to the existing confusion concerning these obstructive airway disorders and to maintain some of the uncertainty on the optimal patients management. Most published studies are case series and retrospective descriptions; in addition, few investigators regard malacia and EDAC as separate entities, often using the two words interchangeably. The clinical impact of these abnormalities is quite high. The pathologic weakening of the airway can produce dynamic outflow obstruction and severe symptoms, such as: cough, dyspnea, and wheezing resistant to corticosteroids and inhaled bronchodilators, stridor, recurrent bronchitis or pneumonia, atelectasis, difficult secretions clearing, and respiratory insufficiency. Moreover, air trapping was also observed with a higher frequency and greater severity in patients with tracheobronchomalacia when compared to patients of similar ages without TBM [13], and up to 7% of patients with severe diffuse TBM may require mechanical ventilation due to respiratory failure. [14]. Current treatments include techniques that splint the central airways, such as continuous positive pressure ventilation [15], silicone airway stents [16] and surgical tracheobronchoplasty [17]. Surgical central airway stabilization with posterior Table 3 Gender dependency of TBM or EDAC and thyroid disorders Gender n % n % males 4/ TBM 4/4 100 EDAC 0/4 0.0 females 30/ TBM 7/ EDAC 23/ tracheobronchial splinting using a polypropylene mesh improves respiratory symptoms, health-related quality of life, and functional status in highly selected patients with severe symptomatic TBM [18]. The etiology of acquired TBM in many patients is not obvious. TBM is often seen in association with COPD in patients with a smoking history, thus leading to the inference that chronic inflammation and smoking are important contributing factors [19]. Nevertheless, little is known concerning the mechanism underlying the association between inflammation and TBM or EDAC. Loring et al. [6] speculated that repeated mechanical stress from coughing or the high expiratory pleural pressures during exercise in patients with airflow obstruction might cause stretching and degeneration of the posterior membranous portion of the trachea and main bronchi over a period of years. At present very few data concerning TBM or EDAC epidemiology in asthma patients are available to our knowledge. Data from the present study, carried out in a consistent cohort of asthma patients of different severity and in whom the diagnosis of TBM o EDAC was confirmed via dynamic broncoscopy, ascertained that the prevalence of EDAC is directly related to asthma severity and is particularly high in severe asthma, while EDAC is much more frequent than TBM in asthmatic patients independently of asthma severity. This evidence supports the hypothesis that the chronic persistency of substantial airway inflammation within the airways can contribute to impair expiratory airflow just affecting intrinsically and persistently the structures of larger airways in a great proportion of cases. Thyroid disease and its association with TBM was documented, but only when tracheal cartilaginous ring can be compromised by a tumour, or most commonly after thyroidectomy, especially in patients with cancer [19]. Furthermore, in our study, thyroid disorders proved highly concomitant in TBM and in EDAC, the latter condition being much more represented in females, independently of asthma severity. Conclusions In conclusion, the presence of TBM or EDAC should be considered whenever bronchial asthma persists
5 Dal Negro et al. Multidisciplinary Respiratory Medicine 2013, 8:32 Page 5 of 5 uncontrolled and unresponsive to an appropriate pharmacological treatment. Moreover, in severe asthma the presence of TBM or EDAC should be actively investigated, not only when uncontrolled, bearing in mind the range of non pharmacological treatment options that could be offered to these patients. Furthermore, if the occurrence of EDAC is highly probable in females with thyroid disturbances, it is as much appropriate that thyroid function be investigated in females with EDAC. Competing interests The authors declare that they have no competing interests. 16. Sommer D, Forte V: Advances in the management of major airway collapse: the use of airway stents. Otolaryngol Clin. North Am 2000, 33: Wright CD: Tracheomalacia. Chest Surg Clin North Am 2003, 13: Majid A, Guerrrero J, Gangadharan S, Feller-Kopman D, Boiselle P, DeCamp M, Ashiku S, Michaud G, Herth F, Ernst A: Tracheobronchoplasty for severe tracheobronchomalacia. Chest 2008, 134: McHenry CR, Piotrowski JJ: Thyroidectomy in patients with marked thyroid enlargement: airway management, morbidity, and outcome. Am Surg 1994, 60: doi: / Cite this article as: Dal Negro et al.: Prevalence of tracheobronchomalacia and excessive dynamic airway collapse in bronchial asthma of different severity. Multidisciplinary Respiratory Medicine :32. Author details 1 Respiratory Unit, Orlandi General Hospital, Via Ospedale 2, Bussolengo VR 37012, Italy. 2 Economics Department, Statistical Section, University of Verona, Italy. 3 Respiratory Unit, Mater Salutis Hospital, Legnago, Verona, Italy. Received: 2 January 2013 Accepted: 18 March 2013 Published: 14 May 2013 References 1. Johnson TH, Mikita JJ, Wilson RJ, Feist JH: Acquired tracheomalacia. Radiology 1973, 109: Jokinen K, Palva T, Sustinen S, Nuutinen J: Acquired tracheobronchomalacia. Ann Clin Res 1977, 9: Ikeda S, Inuue Y, Fujino S, Fujioka S, Hamada H, Yokoyama A, Kohno N, Hiwada K: A case of diffuse panbronchiolitis associated with tracheomalacia. Nihon Ronen Igakkai Zasshi 1993, 30: Jokinen K, Palva T, Nuutinen J: Chronic bronchitis. Abronchologic evaluation. J. Otorhinolaryngol Relat Spec 1976, 38: Palombini BC, Villanova CA, Araùjo E, Gastal OL, Alt DC, Stolz DP, Palombini CO: A pathogenic triad in chronic cough: asthma, postnasal drip and gastroesophageal reflux disease. Chest 1999, 116: Loring SH, O Donnel CR, Feller-Kopman DJ, Ernst A: Central airway mechanics and flow limitation in acquired tracheobronchomalacia. Chest 2007, 131: Murgu DS, Colt GH: Tracheobronchomalacia and excessive dynamic airway collapse: novel diagnostic tools clarify the issues. Pulm Perspectives 2005, 22,3: Hasegawa I, Boiselle P, Raptopoulos V, Hatabu H: Tracheomalacia incidentally detected on CT pulmonary angiography of patients with suspected pulmonary embolism. AJR Am J Roentgenol 2003, 181: Ikeda SH, Hanawa T, Konishi T, Adachi M, Sawai S, Chiba W, Kosaba S, Hatakenaka R, Matsubara Y, Funatsu T: Diagnosis, incidence, clinicopathology and surgical treatment of acquired tracheobronchomalacia. Nihon Kyobu Shikkan Gakka izasshi 1992, 30: Global Strategy for asthma management and prevention: Global Initiative for Asthma (GINA): NHLB/WHO Workshop Report. National Heart, Lung, and Blood Institute, National Institutes of Health, Updated Available from Carden KA, Boiselle PM, Waltz DA, Ernst A: Tracheomalacia and tracheobronchomalacia in children and adults: an in-depth review. Chest 2005, 127: Stern EJ, Graham CM, Webb WR, Gamsu G: Normal trachea during forced expiration: dynamic CT measurements. Radiology 1993, 187: Zhang J, Hasegawa I, Hatabu H, Feller-Kopman D, Boiselle PM: Frequency and severity of air trapping at dynamic expiratory CT in patients with tracheobronchomalacia. AJR Am. J Roentgenol 2004, 182: Ernst A, Majid A, Feller-Kopman D, Guerrero J, Boiselle P, Loring SH, O'Donnell C, Decamp M, Herth FJ, Gangadharan S, Ashiku S: Airway stabilization with silicone stents for treating adult tracheobronchomalacia: a prospective observational study. Chest 2007, 132: Fergusson GT, Benoist J: Nasal continuous positive airway pressure in the treatment of tracheobronchomalacia. Am Rev Respir Dis 1993, 147: Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Pulmonary Function and Flow Volume Loop Patterns in Patients with. *Adnan Majid, MD ¹, FCCP *Andres F.
 Pulmonary Function and Flow Volume Loop Patterns in Patients with Tracheobronchomalacia. *Adnan Majid, MD ¹, FCCP (amajid@bidmc.harvard.edu); *Andres F. Sosa, MD² (andres.sosa@umassmemorial.org); Armin
Pulmonary Function and Flow Volume Loop Patterns in Patients with Tracheobronchomalacia. *Adnan Majid, MD ¹, FCCP (amajid@bidmc.harvard.edu); *Andres F. Sosa, MD² (andres.sosa@umassmemorial.org); Armin
Airway stenting in excessive central airway collapse
 Review Article on Aerodigestive Endoscopy Airway stenting in excessive central airway collapse Mihir Parikh, Jennifer Wilson, Adnan Majid, Sidhu Contributions: (I) Conception and design: All authors; (II)
Review Article on Aerodigestive Endoscopy Airway stenting in excessive central airway collapse Mihir Parikh, Jennifer Wilson, Adnan Majid, Sidhu Contributions: (I) Conception and design: All authors; (II)
Whistling in the Dark
 T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical problem-solving Whistling in the Dark Daniel A. Solomon, M.D., Christopher H. Fanta, M.D., Bruce D. Levy, M.D., and Joseph Loscalzo, M.D.,
T h e n e w e ngl a nd j o u r na l o f m e dic i n e clinical problem-solving Whistling in the Dark Daniel A. Solomon, M.D., Christopher H. Fanta, M.D., Bruce D. Levy, M.D., and Joseph Loscalzo, M.D.,
Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn Syndrome
 Case Reports in Pulmonology, Article ID 910135, 4 pages http://dx.doi.org/10.1155/2014/910135 Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn
Case Reports in Pulmonology, Article ID 910135, 4 pages http://dx.doi.org/10.1155/2014/910135 Case Report Tracheomalacia Treatment Using a Large-Diameter, Custom-Made Airway Stent in a Case with Mounier-Kuhn
Accepted Manuscript. Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD
 Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
Accepted Manuscript Robotic tracheobronchoplasty is feasible but which patients truly benefit? Steven Milman, MD, Thomas Ng, MD PII: S0022-5223(18)32271-2 DOI: 10.1016/j.jtcvs.2018.08.028 Reference: YMTC
Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods
 Syddansk Universitet Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods Nygaard, Mette; Bendstrup, Elisabeth; Dahl, Ronald; Hilberg, Ole; Rasmussen,
Syddansk Universitet Tracheal collapse diagnosed by multidetector computed tomography: evaluation of different image analysis methods Nygaard, Mette; Bendstrup, Elisabeth; Dahl, Ronald; Hilberg, Ole; Rasmussen,
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Tracheobronchomalacia: morfologic evaluation in 64-MDTC.
 Tracheobronchomalacia: morfologic evaluation in 64-MDTC. Poster No.: C-1779 Congress: ECR 2011 Type: Educational Exhibit Authors: C. A. P. Fontes, A. A. S. M. Santos, A. L. Ferreira Neto, E. Marchiori,
Tracheobronchomalacia: morfologic evaluation in 64-MDTC. Poster No.: C-1779 Congress: ECR 2011 Type: Educational Exhibit Authors: C. A. P. Fontes, A. A. S. M. Santos, A. L. Ferreira Neto, E. Marchiori,
Wheeze. Dr Jo Harrison
 Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
Wheeze Dr Jo Harrison 9.9.14 Wheeze - Physiology a continuous musical sound that lasts longer than 250 msec. can be high-pitched or low-pitched, consist of single or multiple notes, and occur during inspiration
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction
 The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
The use of metallic expandable tracheal stents in the management of inoperable malignant tracheal obstruction Alaa Gaafar-MD, Ahmed Youssef-MD, Mohamed Elhadidi-MD A l e x a n d r i a F a c u l t y o f
Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology
 Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
Title: Spirometry Teacher : Dorota Marczuk Krynicka, MD., PhD. Coll. Anatomicum, Święcicki Street no. 6, Dept. of Physiology I. Measurements of Ventilation Spirometry A. Pulmonary Volumes 1. The tidal
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients
 Yuan et al. BMC Pulmonary Medicine 2014, 14:16 RESEARCH ARTICLE Open Access Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients Wei
Yuan et al. BMC Pulmonary Medicine 2014, 14:16 RESEARCH ARTICLE Open Access Increased difference between slow and forced vital capacity is associated with reduced exercise tolerance in COPD patients Wei
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Airway management during general anesthesia in an intellectually disabled patient with undiagnosed tracheomalacia
 Case Report pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2018;18(2):119-123 https://doi.org/10.17245/jdapm.2018.18.2.119 Airway management during general anesthesia in an intellectually disabled
Case Report pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2018;18(2):119-123 https://doi.org/10.17245/jdapm.2018.18.2.119 Airway management during general anesthesia in an intellectually disabled
Expiratory central airway collapse in stable COPD and during exacerbations
 Leong et al. Respiratory Research (2017) 18:163 DOI 10.1186/s12931-017-0646-2 RESEARCH Expiratory central airway collapse in stable COPD and during exacerbations Paul Leong 1,2*, Anne Tran 1, Jhanavi Rangaswamy
Leong et al. Respiratory Research (2017) 18:163 DOI 10.1186/s12931-017-0646-2 RESEARCH Expiratory central airway collapse in stable COPD and during exacerbations Paul Leong 1,2*, Anne Tran 1, Jhanavi Rangaswamy
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Tracheal Collapse: Medical Management Versus Implantable Stents
 What is Tracheal Collapse? The trachea (windpipe) is a large tube that is reinforced by cartilage rings. The trachea runs alongside of the esophagus (food pipe) and delivers air to the lungs. Tracheal
What is Tracheal Collapse? The trachea (windpipe) is a large tube that is reinforced by cartilage rings. The trachea runs alongside of the esophagus (food pipe) and delivers air to the lungs. Tracheal
Respiratory system. Applied Anatomy &Physiology
 Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Audra Fuller MD, Mark Sigler MD, Shrinivas Kambali MD, Raed Alalawi MD
 Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
A 31-year-old female with a rare cause of recurrent lower lobar collapses
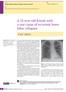 Radhika Banka, Dayle Terrington, Ajay V. Kamath radhika.banka@gmail.com Dept of Respiratory Medicine, Norfolk and Norwich University Hospital, Norwich, UK. A 31-year-old female with a rare cause of recurrent
Radhika Banka, Dayle Terrington, Ajay V. Kamath radhika.banka@gmail.com Dept of Respiratory Medicine, Norfolk and Norwich University Hospital, Norwich, UK. A 31-year-old female with a rare cause of recurrent
Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy: a case report
 Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Bisicchia and Tudisco BMC Musculoskeletal Disorders 2013, 14:285 CASE REPORT Open Access Re-growth of an incomplete discoid lateral meniscus after arthroscopic partial resection in an 11 year-old boy:
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Endobronchial valve insertion to reduce lung volume in emphysema
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endobronchial valve insertion to reduce lung volume in emphysema Emphysema is a chronic lung disease that
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Case Report Varied Presentation and Management of Tracheal Polyps in Children Vinod M Raj 1, Varun Hathiramani 2, Swathi
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
COUGH Dr. A m A it i e t sh A g A garwa w l Le L ctu t rer Departm t ent t o f f M e M dic i in i e
 COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
COUGH Dr. Amitesh Aggarwal Lecturer Department of Medicine Cough is an explosive expiration that provides a normal protective mechanism for clearing the tracheobronchial tree of secretions and foreign
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss?
 ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
ASTHMA-COPD OVERLAP SYNDROME 2018: What s All the Fuss? Randall W. Brown, MD MPH AE-C Association of Asthma Educators Annual Conference July 20, 2018 Phoenix, Arizona FACULTY/DISCLOSURES Randall Brown,
CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS
 CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS Upper Airway Obstruction* John C. Acres, M.D., and Meir H. Kryger, M.D.t chronic upper airway obstruction is frequently unrecognized or misdiagnosed as
CLINICAL SIGNIFICANCE OF PULMONARY FUNCTION TESTS Upper Airway Obstruction* John C. Acres, M.D., and Meir H. Kryger, M.D.t chronic upper airway obstruction is frequently unrecognized or misdiagnosed as
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
3/10/15. Summary. Anatomy Larynx. Anatomy Trachea
 Summary Anatomy Brachycephalic Airway Syndrome (BCAS) Crisis Anatomy Larynx Anatomy Trachea Tracheal rings are incomplete, C-shaped cartilage with the dorsal membrane being completed by tracheal muscle
Summary Anatomy Brachycephalic Airway Syndrome (BCAS) Crisis Anatomy Larynx Anatomy Trachea Tracheal rings are incomplete, C-shaped cartilage with the dorsal membrane being completed by tracheal muscle
Exercise-associated Excessive Dynamic Airway Collapse in Military Personnel
 Exercise-associated Excessive Dynamic Airway Collapse in Military Personnel Daniel J. Weinstein 1, James E. Hull 2, Brittany L. Ritchie 3, Jackie A. Hayes 2, and Michael J. Morris 2 1 Internal Medicine
Exercise-associated Excessive Dynamic Airway Collapse in Military Personnel Daniel J. Weinstein 1, James E. Hull 2, Brittany L. Ritchie 3, Jackie A. Hayes 2, and Michael J. Morris 2 1 Internal Medicine
Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600
 Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
Endobronchial valve insertion to reduce lung volume in emphysema Interventional procedures guidance Published: 20 December 2017 nice.org.uk/guidance/ipg600 Your responsibility This guidance represents
collapse in patients with tracheobronchomalacia,
 J. Zhang 1,2 I. Hasegawa 1,3 H. Hatabu 1,3 D. Feller-Kopman 1,3 P. M. Boiselle 1,3 Received June 5, 2003; accepted after revision July 23, 2003. 1 Department of Radiology, Beth Israel Deaconess Medical
J. Zhang 1,2 I. Hasegawa 1,3 H. Hatabu 1,3 D. Feller-Kopman 1,3 P. M. Boiselle 1,3 Received June 5, 2003; accepted after revision July 23, 2003. 1 Department of Radiology, Beth Israel Deaconess Medical
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
Two Cases of Tracheal Disease Misdiagnosed as Difficult-to-Treat Asthma
 Two Cases of Tracheal Disease Misdiagnosed as Difficult-to-Treat Asthma Running-Head: Are you sure about the diagnosis of asthma? Ibrahim Onur Alici 1, Ozlem Kar Kurt 2, Adile Berna Dursun 3, Aydin Yilmaz
Two Cases of Tracheal Disease Misdiagnosed as Difficult-to-Treat Asthma Running-Head: Are you sure about the diagnosis of asthma? Ibrahim Onur Alici 1, Ozlem Kar Kurt 2, Adile Berna Dursun 3, Aydin Yilmaz
Respiratory distress in patients with central airway obstruction
 Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Indian J Thorac Cardiovasc Surg (2010) 26:151 156 DOI 10.1007/s12055-010-0021-0 ORIGINAL ARTICLE Respiratory distress in patients with central airway obstruction Mohamed Abdel Hamied Regal & Yasser Ahmed
Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis?
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 12 Number 1 Swyer-James Syndrome: An Infrequent Cause Of Bronchiectasis? A Huaringa, S Malek, M Haro, L Tapia Citation A Huaringa, S Malek, M
Arkansas VMA Winter 2015
 Chronic Coughing Dogs Simple Tests & Favorite Drugs G. P. Oswald DVM, Dip ACVIM, Tampa Bay Veterinary Specialists, Largo, FL Paroxysmal non-productive coughing is a common and frustrating complaint in
Chronic Coughing Dogs Simple Tests & Favorite Drugs G. P. Oswald DVM, Dip ACVIM, Tampa Bay Veterinary Specialists, Largo, FL Paroxysmal non-productive coughing is a common and frustrating complaint in
Pulmonary Function Testing: Concepts and Clinical Applications. Potential Conflict Of Interest. Objectives. Rationale: Why Test?
 Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Pulmonary Function Testing: Concepts and Clinical Applications David M Systrom, MD Potential Conflict Of Interest Nothing to disclose pertinent to this presentation BRIGHAM AND WOMEN S HOSPITAL Harvard
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Outline FEF Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications?
 Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Reduced FEF25-75 in asthma. What does it mean and what are the clinical implications? Fernando Holguin MD MPH Director, Asthma Clinical & Research Program Center for lungs and Breathing University of Colorado
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery. By: Lillian Han
 Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
Respiratory Anesthetic Emergencies in Oral and Maxillofacial Surgery By: Lillian Han Background: Respiratory anesthetic emergencies are the most common complications during the administration of anesthesia
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Step-down approach in chronic stable asthma: A comparison of reducing dose Inhaled Formoterol/ Budesonide with maintaining Inhaled Budesonide.
 Step-down approach in chronic stable asthma: A comparison of reducing dose Inhaled Formoterol/ Budesonide with maintaining Inhaled Budesonide. By: DR MOHD SHAMSUL AMRI Supervisor: Associate Professor Dr
Step-down approach in chronic stable asthma: A comparison of reducing dose Inhaled Formoterol/ Budesonide with maintaining Inhaled Budesonide. By: DR MOHD SHAMSUL AMRI Supervisor: Associate Professor Dr
Tracheobronchomalacia
 Originales Revisión Artículo especial Arch Bronconeumol. 2010;46(4):196-202 Archivos de B r o n c o n e u m o l o g í a Volumen 46, Número 3, Marzo 2010 www.archbronconeumol.org Special Article Tracheobronchomalacia
Originales Revisión Artículo especial Arch Bronconeumol. 2010;46(4):196-202 Archivos de B r o n c o n e u m o l o g í a Volumen 46, Número 3, Marzo 2010 www.archbronconeumol.org Special Article Tracheobronchomalacia
d) Always ensure patient comfort. Be considerate and warm the diaphragm of your stethoscope with your hand before auscultation.
 Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Phases of Respiration. Chapter 18: The Respiratory System. Structures of the Respiratory System. Structures of the Respiratory System
 Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Phases of Respiration Chapter 18: The Respiratory System Respiration Process of obtaining oxygen from environment and delivering it to cells Phases of Respiration 1. Pulmonary ventilation between air and
Function of the Respiratory System. Exchange CO2 (on expiration) for O2 (on inspiration)
 Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
Function of the Respiratory System Exchange CO2 (on expiration) for O2 (on inspiration) Upper Respiratory Tract Includes: Nose Mouth Pharynx Larynx Function: Warms and humidifies the inspired air Filters
2/4/2019. GOLD Objectives. GOLD 2019 Report: Chapters
 GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
GOLD Objectives To provide a non biased review of the current evidence for the assessment, diagnosis and treatment of patients with COPD. To highlight short term and long term treatment objectives organized
A Tracheostomy Complication Resulting from Acquired Tracheomalacia: A Case report
 A Tracheostomy Complication Resulting from Acquired Tracheomalacia: A Case report Bach T. Le, MD, DDS, James M. Eyre, Jr., MD, DMD, Eric P. Holmgren, MS, Eric J. Dierks, MD, DMD, FACS Key Words: tracheomalacia,
A Tracheostomy Complication Resulting from Acquired Tracheomalacia: A Case report Bach T. Le, MD, DDS, James M. Eyre, Jr., MD, DMD, Eric P. Holmgren, MS, Eric J. Dierks, MD, DMD, FACS Key Words: tracheomalacia,
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant. Tara Brennan, MD 2,3
 Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
TORCH: Salmeterol and Fluticasone Propionate and Survival in COPD
 TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
TORCH: and Propionate and Survival in COPD April 19, 2007 Justin Lee Pharmacy Resident University Health Network Outline Overview of COPD Pathophysiology Pharmacological Treatment Overview of the TORCH
COPD. Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS
 IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
IN THE NAME OF GOD COPD Dr.O.Paknejad Pulmonologist Shariati Hospital TUMS Definition of COPD* COPD is a preventable and treatable chronic lung disease characterized by airflow limitation that is not fully
COPD COPD. C - Chronic O - Obstructive P - Pulmonary D - Disease OBJECTIVES
 COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
COPD C - Chronic O - Obstructive P - Pulmonary D - Disease 1 OBJECTIVES Following this presentation the participant should be able to demonstrate understanding of chronic lung disease by successful completion
11.3 RESPIRATORY SYSTEM DISORDERS
 11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
11.3 RESPIRATORY SYSTEM DISORDERS TONSILLITIS Infection of the tonsils Bacterial or viral Symptoms: red and swollen tonsils, sore throat, fever, swollen glands Treatment: surgically removed Tonsils: in
A Proposed Grading System for Post-Intubation Tracheal Stenosis
 Original Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 TANAFFOS A Proposed Grading System for Post-Intubation Tracheal Stenosis Ali Ghorbani 1,
Original Article 2012 NRITLD, National Research Institute of Tuberculosis and Lung Disease, Iran ISSN: 1735-0344 TANAFFOS A Proposed Grading System for Post-Intubation Tracheal Stenosis Ali Ghorbani 1,
The Respiratory System. Dr. Ali Ebneshahidi
 The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
The Respiratory System Dr. Ali Ebneshahidi Functions of The Respiratory System To allow gases from the environment to enter the bronchial tree through inspiration by expanding the thoracic volume. To allow
Differential diagnosis
 Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Differential diagnosis The onset of COPD is insidious. Pathological changes may begin years before symptoms appear. The major differential diagnosis is asthma, and in some cases, a clear distinction between
Tests Your Pulmonologist Might Order. Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital
 Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Tests Your Pulmonologist Might Order Center For Cardiac Fitness Pulmonary Rehab Program The Miriam Hospital BASIC ANATOMY OF THE LUNGS Lobes of Lung 3 lobes on the Right lung 2 lobes on the Left Blood
Stridor, Stertor, and Snoring: Pediatric Upper Airway Obstruction. Nathan Page, MD Pediatrics in the Red Rocks June?
 Stridor, Stertor, and Snoring: Pediatric Upper Airway Obstruction Nathan Page, MD Pediatrics in the Red Rocks June? I have no disclosures I do not plan to discuss unapproved or off label use of products
Stridor, Stertor, and Snoring: Pediatric Upper Airway Obstruction Nathan Page, MD Pediatrics in the Red Rocks June? I have no disclosures I do not plan to discuss unapproved or off label use of products
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days
 Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
BELLWORK page 343. Apnea Dyspnea Hypoxia pneumo pulmonary Remember the structures of the respiratory system 1
 BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
BELLWORK page 343 Apnea Dyspnea Hypoxia pneumo pulmonary respiratory system 1 STANDARDS 42) Review case studies that involve persons with respiratory disorders, diseases, or syndromes. Citing information
Respiratory System. Chapter 9
 Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Respiratory System Chapter 9 Air Intake Air in the atmosphere is mostly Nitrogen (78%) Only ~21% oxygen Carbon dioxide is less than 0.04% Air Intake Oxygen is required for Aerobic Cellular Respiration
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
MRSA pneumonia mucus plug burden and the difficult airway
 Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
Case report Crit Care Shock (2016) 19:54-58 MRSA pneumonia mucus plug burden and the difficult airway Ann Tsung, Brian T. Wessman An 80-year-old female with a past medical history of chronic obstructive
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
The RESPIRATORY System Unit 3 Transportation Systems Functions of the Respiratory System Warm, moisten, and filter incoming air Resonating chambers for speech and sound production Oxygen and Carbon Dioxide
Small Airways Disease. Respiratory Function In Small Airways And Asthma. Pathophysiologic Changes in the Small Airways of Asthma Patients
 Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
Small Airways Disease Respiratory Function In Small Airways And Relevant Questions On Small Airway Involvement In How can small airway disease be defined? What is the link between small airway abnormalities
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (1), Page
 The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (1), Page 3516-3520 Severe Tracheomalacia Secondary to Double Aortic Arch. Any Role in Posterior Aortopexy? A Case report Bayan Almehamadi
The Egyptian Journal of Hospital Medicine (July 2018) Vol. 72 (1), Page 3516-3520 Severe Tracheomalacia Secondary to Double Aortic Arch. Any Role in Posterior Aortopexy? A Case report Bayan Almehamadi
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Chapter 124: Congenital Disorders of the Trachea. Bruce Benjamin
 Chapter 124: Congenital Disorders of the Trachea Bruce Benjamin Investigation of the larynx and pharynx may be incomplete in infants and children with congenital abnormalities without investigation of
Chapter 124: Congenital Disorders of the Trachea Bruce Benjamin Investigation of the larynx and pharynx may be incomplete in infants and children with congenital abnormalities without investigation of
Problem Based Learning Session. Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days.
 Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Defining COPD. Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist
 Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
Defining COPD Georgina Grantham Community Respiratory Team Leader/ Respiratory Nurse Specialist Defining COPD Chronic Obstructive Pulmonary Disease (COPD) is a common, preventable and treatable disease
Overview. The Respiratory System. Chapter 18. Respiratory Emergencies 9/11/2012
 Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
Chapter 18 Respiratory Emergencies Slide 1 Overview Respiratory System Review Anatomy Physiology Breathing Assessment Adequate Breathing Breathing Difficulty Focused History and Physical Examination Emergency
The Respiratory System Structures of the Respiratory System Structures of the Respiratory System Structures of the Respiratory System Nose Sinuses
 CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
CH 14 D.E. Human Biology The Respiratory System The Respiratory System OUTLINE: Mechanism of Breathing Transport of Gases between the Lungs and the Cells Respiratory Centers in the Brain Function Provides
COPD. Helen Suen & Lexi Smith
 COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
COPD Helen Suen & Lexi Smith What is COPD? Chronic obstructive pulmonary disease: a non reversible, long term lung disease Characterized by progressively limited airflow and an inability to perform full
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
COPD. Breathing Made Easier
 COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
COPD Breathing Made Easier Catherine E. Cooke, PharmD, BCPS, PAHM Independent Consultant, PosiHleath Clinical Associate Professor, University of Maryland School of Pharmacy This program has been brought
DIFFICULT ASTHMA. Dr. Prathyusha Dr. S.Balasubramanian KKCTH
 DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
DIFFICULT ASTHMA Dr. Prathyusha Dr. S.Balasubramanian KKCTH CASE SUMMARY 11 yr old girl, Neyveli Treated as moderate persistent asthma x 5 years On Seroflo [ LABA + steroid ] 250 2 puffs BD and intermittent
Double Y-stenting for tracheobronchial stenosis
 ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
ERJ Express. Published on April 10, 2012 as doi: 10.1183/09031936.00015012 Double Y-stenting for tracheobronchial stenosis M. Oki and H. Saka AFFILIATIONS Dept of Respiratory Medicine, Nagoya Medical Center,
Spirometry: FEVER DISEASE DIABETES HOW RELIABLE IS THIS? 9/2/2010 BUT WHAT WE PRACTICE: Spirometers are objective tools
 SPIROMETRY PRINCIPLES, PROCEDURE AND QA Spirometry: Dr. Rahul Kodgule CHEST RESEARCH FOUNDATION, PUNE FEVER ISCHAEMIC HEART DISEASE DIABETES BUT WHAT WE PRACTICE: Spirometers are objective tools to diagnose
SPIROMETRY PRINCIPLES, PROCEDURE AND QA Spirometry: Dr. Rahul Kodgule CHEST RESEARCH FOUNDATION, PUNE FEVER ISCHAEMIC HEART DISEASE DIABETES BUT WHAT WE PRACTICE: Spirometers are objective tools to diagnose
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
A young patient with wheezing and dyspnoea on exertion: is all that wheezes asthma?
 A young patient with wheezing and dyspnoea on exertion: is all that wheezes asthma? Case history A 21-year-old nonsmoking male visited his GP complaining of dyspnoea on exertion. His symptoms had started
A young patient with wheezing and dyspnoea on exertion: is all that wheezes asthma? Case history A 21-year-old nonsmoking male visited his GP complaining of dyspnoea on exertion. His symptoms had started
Therapeutic Bronchoscopy Etiology - Benign Stenosis Post - intubation Trauma Post - operative Inflammatory Idiopathic
 Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Endobronchial Palliation of Airway Disease Douglas E. Wood, MD Professor and Chief Division of Cardiothoracic Surgery Vice-Chair, Department of Surgery Endowed Chair in Lung Cancer Research University
Chapter 10. Respiratory System and Gas Exchange. Copyright 2005 Pearson Education, Inc. publishing as Benjamin Cummings
 Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
Chapter 10 Respiratory System and Gas Exchange Function of the Respiratory System To obtain oxygen (O 2 ) for all cells in the body. To rid the cells of waste gas (CO 2 ). Oxygen (O 2 ) is vital chemical
ISPUB.COM. Rare Cases: Tracheal/bronchial Obstruction. O Wenker, L Moehn, C Portera, G Walsh HISTORY ADMISSION
 ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
ISPUB.COM The Internet Journal of Radiology Volume 1 Number 1 O Wenker, L Moehn, C Portera, G Walsh Citation O Wenker, L Moehn, C Portera, G Walsh.. The Internet Journal of Radiology. 1999 Volume 1 Number
Overview of COPD INTRODUCTION
 Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
Overview of COPD INTRODUCTION Chronic obstructive pulmonary disease (COPD) is a common lung disease that affects millions of people, and it is the fourth leading cause of death in the United States. It
SPIROMETRY TECHNIQUE. Jim Reid New Zealand
 Jim Reid New Zealand The Basics Jim Reid Spirometry measures airflow and lung volumes, and is the preferred lung function test in COPD. By measuring reversibility of obstruction, it is also diagnostic
Jim Reid New Zealand The Basics Jim Reid Spirometry measures airflow and lung volumes, and is the preferred lung function test in COPD. By measuring reversibility of obstruction, it is also diagnostic
