)443( COPYRIGHT 2017 BY THE ARCHIVES OF BONE AND JOINT SURGERY SHORT COMMUNICATION
|
|
|
- Ross Waters
- 5 years ago
- Views:
Transcription
1 )443( COPYIGHT 2017 BY THE ACHIVES OF BONE AND JOINT SUGEY SHOT COMMUNICATION Giant Cell Tumor of the Sacrum: Series of 19 Patients and eview of the iterature Khodamorad Jamshidi, MD; Abolfazl Bagherifard, MD; Alireza Mirzaei, PhD; Mehrdad Bahrabadi, MD esearch performed at Shafa Orthopedic Hospital, Iran University of Medical Sciences, Tehran, Iran eceived: 16 January 2017 Accepted: 12 April 2017 Abstract There are still some debates regarding the best treatment of Giant Cell Tumor (GCT) of the sacrum. Since GCT of this location is rare, therapeutic strategies are mainly based on the treatment of GCT in other anatomic locations. The objective of this study was to evaluate the oncologic and clinical results of surgical management of sacral GCT with and without local adjuvant therapy. Medical records of 19 patients diagnosed with GCT of the sacrum, were retrospectively reviewed. Sixteen patients were treated by intralesional curettage and three patients with marginal resection. Musculoskeletal tumor society (MSTS) score was used for the evaluation of functional outcome. Prolonged pain was the most common complication after treatment. Mean Pre and post-operative pain based on visual analogue scale (VAS) was 6.1 ± 1.99 and 3.05 ± 1.64, respectively. Postoperative neurologic deficit appeared in six patients. In addition, infection occurred in five patients. One case of spinopelvic instability was also observed after surgery. At average follow up of ± 95.9 months (25 to 316 months), recurrence was seen in eight (42.7%) out of seventeen patients treated by intralesional curettage. The size of the tumor significantly correlated with the tumor recurrence (r=0.654, P=0.001). Mean MSTS score was 74.7 ± Those patients, in whom sacral nerve roots remained intact before and after surgery, had better functional outcome. Preservation of sacral nerve roots is associated with better functional outcome and less pain. Although an acceptable surgical outcome was observed in our cohort, the problem of local recurrence still warrants further investigations for better local control of the tumor. Keywords: Intralesional curettage, Giant cell tumor, Sacrum, ecurrence Introduction In the axial skeleton, sacrum is the most common place of involvement by where Giant cell tumors (GCT) form. The incidence of GCT in the sacrum is between 6.7% to 9.4% in different series (1, 2). Currently, there is no agreement regarding the treatment of GCTs of rare localizations, including small bones, pelvis, spine, or sacrum (1, 3, 4). Treatment of GCTs of axial skeleton even is more complicated (1). This is most likely due to its rarity, and also owing to the limited surgical accessibility and proximity of the tumor to the nerve roots (1). The literature provides only small case series of GCT of the spine or sacrum with mostly short-term follow-ups (5). In this review, we explain the results of the treatment of 19 cases of sacral GCT, with respect to the current literature. Materials and Methods During 1990 to 2014, 286 patients with confirmed GCT were surgically treated in Shafa OrthopedicHospital, from which, sacral GCT were identified in 26 patients. Seven patients were absent during follow-up, but the remaining 19 patients were assessed in the final evaluation.patient s medical and surgical records were reviewed and required necessary documents, including pathological and radiological assessments, were obtained from their medical files. Tumor size was retrospectively assessed using imaging or pathological data, available for patients treated in the last 24 years. The latest follow-up Corresponding Author: Mehrdad Bahrabadi, Shafa Orthopedic Hospital, Iran University of Medical Sciences, Tehran, Iran Mehrdad.bahrabadi@gmail.com Arch Bone Jt Surg. 2017; 5(6): the online version of this article abjs.mums.ac.ir
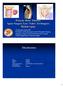
2 )444( THE ACHIVES OF BONE AND JOINT SUGEY. ABJS.MUMS.AC.I VOUME 5. NUMBE 6. NOVEMBE 2017 GIANT CE TUMO OF SACUM was performed by personal contact in the ambulatory clinic. Treatment decisions were made by a multidisciplinary team, including orthopedic oncologist, radiologist, pathologist, and clinical oncologist. Depending on the extent and level of the tumor, patients underwent intralesional curettage or marginal excision with a posterior approach alone or a combination of posterior and anterior approaches. In this regard, in those tumors, which had a large anterior soft tissue component, an anterior approach was performed in order to release anterior organs from the tumor before the posterior approach, at the same operating session. Accordingly, three patients of our series were treated by combined anteroposterior approach, while in the case of the remaining 16 patients, posterior approach was used. All of the marginal excisions were performed on tumors that were distally located (S3-S4) in sacrum and had small sizes (4 cm in largest diameter). There was no attempt for reconstruction of these defects, because the tumors were not in the weight-bearing area of the skeleton. In those patients with posterior-only approach, a posterior midline incision was used to approach the sacrum. Intra-operative radiographies were used to confirm the sacral level when necessary. After removal of the lamina of the corresponding sacral segments by using a high-speed burr, thecal sac was reached, and was dissected free from the tumor mass. By using rubber bands, sacral nerve roots were protected, and were kept away from the tumor. From this point on, dissection was different in those who had an excision and those who had curettage. In the patients with excision, ventral organs were dissected away from the tumor mass. By making an interrupted cut in the sacrum and connecting them together. Subsequently, osteotomy of the sacrum was completed and the tumor was dissected away from the remaining sacrum. In those patients with curettage, complete intralesional curettage was performed, using currets and high- speed burs. Preoperative radiographs were used for the evaluation of spinopelvic stability. Spinopelvic stability was considered intact if we could bilaterally preserve at least the cephalad, 50% of the S-1 vertebra and sacroiliac joints (6). Spinopelvic biomechanical stability, which had been previously defined as the ability of the pelvis to withstand normal physiologic loads without displacing, was assessed by the attending surgeons based on preoperative and intraoperative manual assessment (7). Spinopelvic fixation was performedin cases with spinopelvic instability. In order to manually assess sacroiliac stability, vertical and rotational forces were applied to the pelvis at the end of each surgery by the attending surgeon. If there was any vertical or rotational instability caused by destruction of the sacroiliac joint, sacroiliac instrumentation or structural allograft were implemented [Figure1] (2). Figure 1. (A&B) X-ray before and after curettage and cortico cancellous bone graft of a sacral giant cell tumor (case 1); (C&D) X-ray before and after curettage and structural bone graft of a sacral giant cell tumor (case 3).
3 )445( THE ACHIVES OF BONE AND JOINT SUGEY. ABJS.MUMS.AC.I VOUME 5. NUMBE 6. NOVEMBE 2017 GIANT CE TUMO OF SACUM After curettage, either bone grafting, or bone cement packing was used for reconstruction of the defect. The choice between bone graft and bone cement was made considering the following facts: in cases where the void was contained, corticocancellous bone grafting was used [Figure 1]. In those patients with a non-contained defect after curettage, bone cement packing was used. In the cementing group of patients, gel foam and saline irrigation were used to protect sacral nerve root against the heat of the cementing process. None of our patients received radiotherapy as the sole treatment modality, or as the adjuvant therapy for the primary operation. External beam irradiation was performed in two patients, both as postoperative adjuvant therapy, in the treatment of tumor recurrence. All patients were followed up every three months for the first two years, every six months for the third year, and yearly thereafter. In each follow-up visit, plain radiography of the pelvis and chest had been taken. In case of finding any abnormality in plain radiographs, computed tomography of the area was requested and further imaging evaluations were performed. Patients with recurrence were followed similar to primary patients with serial clinical examination and radiographs. For the functional outcome, musculoskeletal tumor society score, MSTS, was used. According to the this scoring system, numerical values (0 to 5) are given to each of the six categories of pain, function, emotional acceptance, supports, walking and gait. The total score for the system between 0 and 30 is given to each patient with 0 indicating poor and 30 indicating excellent functional result (8). Pain was assessed based on visual analogue scale (VAS) (9). esults The average follow-up time was 158 months, ranging from 25 to 316 months. The mean age of the patients was 29.47± 8.14 years, ranging from 18 to 46 years. Six Table 1. The ocation of GCT of sacrum in our series location Side ight eft Middle S2 or above S3 or below patients were male, and 13 were female. The mean size of the tumors was 6.26 ± 3.12 cm, ranging from 2 to 15 cm. Eighteen tumors were located in the sacrum and one was in the sacrum extending to Ilium. ocation of the tumors is seen in Table 1. Chief complaint of the patients was pain. Pain was present in all but one patient who was referred to us for evaluation of an incidental finding in the pelvic radiograph. Four patients had paresthesia of the lower limb or buttock, and one patient presented with had cauda equina syndrome. Clinical and demographic characteristics of the patients have been demonstrated in Table 2. After primary surgery, eight out of 19 patients had local recurrence (42.1%), which in one case coincided with pulmonary metastasis. All recurrences were observed in patients who had undergone intralesional curettage, while no recurrence was observed in the excision group (three patients). The mean time to first recurrence was months ranging from 4 to 26 months. Mean recurrence- free survival of patients was ± 34.8 months (95% CI, from to 254.7) [Figure 2]. All of recurrent tumors underwent re-operation. In all of the second surgeries, methyl methacrylate was used for the purpose of the reconstruction of the defect and as an adjuvant therapy. We had two repeat recurrences (Cases 5 and 15). Two patients of the recurrent tumor group received external beam irradiation Table 2. Demographic and clinical characteristics of the patients Case Variable Gender F F F M F F M F F M F F M M F F F F M Age (years) Preop (VAS) Pre-op neurology I I I I P I P I I P I I I P C I I I I evel & side of sacral involvement S13, S1-3 S3-4 mid S1-4&I S1-4 S1 S1-3 S1-4 S3-4 mid S1-3 S1-3 S3-4 mid S2-4 S2-5 Tumor size (cm) Approach P P P P A/P P A/P P P P P A/P P P P P P P P Follow up time (months) Campanacci Grade F: Female, M: Male, I: Intact, P: Paresthesia, C: Cauda equine; : right; : left; Mid: Middle, A: anterior, P: posterior
4 )446( THE ACHIVES OF BONE AND JOINT SUGEY. ABJS.MUMS.AC.I VOUME 5. NUMBE 6. NOVEMBE 2017 GIANT CE TUMO OF SACUM Figure 2. Kaplan-Meier curve of recurrence free survival of patients with sacrum GCT. (EBI) as an adjuvant therapy for local control of their recurrent tumors. No further recurrence was observed afterwards. At the last follow-up visit, none of the patients had any sign of tumor recurrence. Infection was seen in five patients after surgery, which was superficial in two cases, and deep in three. All patients were managed by debridement, and use of intravenous antibiotics based on the culture results. Primary or secondary wound closure was finally done in all patients. After irrigation and debridement, infection was resolved in all except one patient (Case 15). She was reluctant to have another surgery and we decided to control the infection by antibiotics. This patient is still under oral antibiotic therapy for infection control whenever there is sign of infection. Neurologic status of the patients at the time of presentation is demonstrated in table 2. We did not encounter any weakness in preoperative period in our patients. It is possible to have paresthesia without weakness when there are sacral injuries such as fractures (10). Neurologic complication after surgery occurred in 6 out of 19 patients, and these ranged from numbness to bladder or bowel dysfunctions. The patient with cauda equina syndrome showed incomplete recovery after surgery, and claw toes and neurogenic bladder were present. Patients with injury to sacral nerve roots manifested by sensory, motor disturbance, or incontinence (all cases except number 1, 2, 4, 6, 8, 11, 17, and 19), had more pain based on VAS, and lower functional outcome, according to MSTS score. The average preoperative VAS was 6, which was reduced to 2 postoperatively [Table 3]. One patient developed pulmonary metastasis;this was resolved by thoracotomy and metastasectomy leading to disease-free survival. In the last follow-up, all patients were alive. Six out of the 19 patients were free of pain. From 16 patients, who were treated by curettage, cement packing and bone grafting was used in four and twelve patients respectively. The average size of the tumors was 6.73 ± 3.01cm, ranging from 2 to 15 cm. We had only one recurrence in the group with cement packing (25% recurrence), and seven recurrences in the group with bone grafting (53.8%). A significant positive correlation was observed between local recurrence and the size of the tumors (r=0.443, P=0.029). Discussion Giant Cell Tumor (GCT) is slightly more common in female than in male, with a ratio of 1.2 to 1. In sacral GCT this gender difference is more pronounced, so that in one study 69.2% of sacral GCT patients were female (1). In our patients, 13 out of the 19 (68.4%) patients were female, but due to small numbers of patients in this study, these ratios may be incidental. ecommendations for treatment of GCT in extremities are based on the retrospective series of patients and not on randomized trials. On this basis, most authors consider intralesional excision as the treatment of choice (11). Some authors advocate the use of adjutants like phenol, alcohol, hydrogen peroxide, liquid nitrogen, or methyl methacrylate to decrease the rate of local recurrence, while others find this unnecessary (11, 12). After a tumor was is curetted, the cavity can be left unfilled or filled with bone graft or cement (11). Based
5 )447( THE ACHIVES OF BONE AND JOINT SUGEY. ABJS.MUMS.AC.I VOUME 5. NUMBE 6. NOVEMBE 2017 GIANT CE TUMO OF SACUM Table 3. Patients treatment, complication and outcome Case Surgical Treatment ecurrence Treatment rec. Complications, post-op neurol. status Post-op pain(vas) Post-op MSTS% 1 C&BG - 2cm D& Normal neurology C&BG 4M C&CE Normal neurology C&BG - Paresthesia Normal neurology C&BG 9M/37M C&CE&EBI Neurogenic bladder & Paresthesia C&BG - Normal neurology C&BG&P 11M C&CE&EBI Paresthesia& Weakness C&BG - Normal neurology C&CE - Superficial Infection (Oral antibiotics).& Paresthesia C&BG 26M C&CE Neurogenic bladder C&BG - Infection(I&D).& normal neurology C&BG 7M C&CE Foot drop C&CE - Superficial Infection (oral antibiotics).& Foot drop Paresthesia C&BG&P 13M/33M C&CE Infection. (I&D)&Neurogenic bladder (Urinary Cath.), Claw toes, paresthesia, C&BG 18M C&CE&P Paresthesia Normal neurology C&CE - Paresthesia C&CE 7M C&CE Infection(I&D), Normal neurology C: Curettage; : esection; BG: Bone graft; CE: Cement; P: umbopelvic fixation; EBI: External beam irradiation N: normal;p: paresthesia; W: Weakness; Claw: claw toes; D: eg length discrepancy; I&D: Irrigation and debridement. on some reports, the nature of the filling material or the type of adjuvant method or any combination of both did not have any significant effect on the recurrence rate after surgery, while other reports are in favor of using high-speed burr of the margins after curettage, and bone cement packing for achieving the lowest recurrence rate (11, 13). In GCT of sacrum or pelvis, the treatment goal of GCT of long bones cannot be fullyachieved. Tumors in these areas, especially in the sacrum, often compress the spinal nerve roots; therefore, complete curettage is hardly possible. In addition, local adjutants such as bone cement, phenol, or cryotherapy have limited use close to nerve roots, due to their toxic effects on nervous tissue (12). Treatment modalities of GCT of the sacrum include either surgical or nonsurgical. Possible surgical treatment options include intralesional curettage, and partial sacrectomy combined with either irradiation or arterial embolization (5, 14, 15). Wide or marginal excision of the tumoror en bloc resections may result in a lower recurrence rate but often cause unacceptable neurological damage (14). Nonsurgical treatments include a variety of modalities including external beam irradiation (EBI), selective arterial embolization (SAE), bisphosphonates and Demosumab. Nowadays, many authors would prefer to perform SAE instead of primary irradiation whenever surgery is not reasonable (1). Surgical treatments can be combined with nonsurgical methods in an attempt to decrease the rate of local recurrence. En bloc excision of the GCT of the sacrum is the best method of obtaining local control, and whenever is practically possible, it is the treatment of choice. This is mostly applicable to giant cell tumors below the S3 level (5). In eggon s series, surgical excision with wide margins had the best results in terms of local control, with 0% of local recurrence, but at the expense of iatrogenic nerve injury. This complication will be greater if the higher levels are involved (3). In 16 out of 19 patients of our series, the location and extent of the tumor would have impeded achieving wide margins without damaging multiple nerve roots leading to almost certain incontinence and impotence as well as lower limb weakness and complete lumbopelvic disassociation in the majority of the cases. Due to high morbidity and complications, resection of GCT of sacrum with wide surgical margins, is only justified when the tumor is
6 )448( THE ACHIVES OF BONE AND JOINT SUGEY. ABJS.MUMS.AC.I VOUME 5. NUMBE 6. NOVEMBE 2017 GIANT CE TUMO OF SACUM distal enough to minimize the risk of iatrogenic nerve damage (5). This treatment modality was performed in just three tumors among our patients. After resection, no attempt was performed made to reconstruct the missing part, mainly due to the small size, and distal position of the defect within the sacrum. There was no recurrence in these patients. The lack of recurrence in these patients was in concordance with the literature that shows that with en bloc excision of the GCT of sacrum, tumor recurrence is the lowest among other methods of surgery (3, 5). Intralesional curettage as the method of treatment of the GCT of sacrum, either alone or in combination with adjuvant has had results that is lower than either en bloc resection or SAE. eggon et al. found a 48% risk of local recurrence in patients treated with curettage alone and a 47% risk of local recurrence with curettage combined with radiotherapy (3). Based on some reports, intralesional curettage in most parts of the tumor as possible may have less recurrence and distant metastasis compared with the standard curettage (2, 16). ocal recurrence was observed in eight cases patients (47%) who had intralesional curettage, and in no patient who was managed by excision. We had a 25% recurrence rate in the group of patients with bone cement packing and 53.8% in those with bone grafting, which was in accordance with the previous reports favoring bone cement as a method of adjuvant and reconstruction of the tumor after surgery (12, 17). We decided to manage the local recurrences by repeat curettage and cementing, which is a well-known method of treatment in the recurrence of GCT in long bones (18). The recurrence is always more difficult to treat than the primary tumor, thus, every attempt should be made to avoid its occurrence as much as possible. Serial Arterial Embolization (SAE) offers the best results published so far in managing giant cell tumor of the sacrum (19-21). In the patient series published by Hosalkar et al., this treatment option was successful in seven out of nine cases (19). In this method, repeated embolization was stressed by Hosalkar to ensure that all the major blood vessels feeding the tumor have been controlled. Due to its high success and low morbidity, SAE is suggested as the primary treatment option for any patient with giant cell tumor of the sacrum. If the patient develops local progression or recurrence, then an alternative treatment is needed. SAE, as the sole treatment modality, may have a risk of diagnostic error, because only needle biopsy is used in this method (19). Since required equipment was not available at our center, we did not use SAE as the sole therapy, or pre-operative treatment modality in our patients. adiotherapy has been used to treat sacral giant cell tumors, but recurrence rates as high as 49% have been reported, and other complications, such as postradiation fibrosis and radiation-induced malignancy, also may arise (3). The risk of radiation-induced sarcomas, was between 3% to 11% in the series reported by different authors (3, 22). Chakravarti reported five cases of sacral giant cell tumor treated with radiotherapy with doses between 40 and 70 Gy. Two of the patients did not respond and developed progression at 5 and 8 months, respectively and both required surgery, while the other three patients remained disease free at followup between 3 and 10 years. Based on this data, they recommended a dose of 50 Gy to maximize local control (22). We only used radiotherapy in two patients after repeat surgery following local recurrence. In our two cases, a dose of 50 Gy in 25 fractions was used. We did not use radiotherapy after 2004 for in any patient mainly due to the results of the series published by eggon, which showed that the outcome of intralesional curettage with or without radiotherapy is similar (3). In addition, due to conflicting results of radiotherapy in GCT of sacrum, and the risk of malignant transformation in those receiving EBI, we were hesitant to use radiotherapy in primary surgeries, and only used this modality as an adjuvant for tumor recurrence. Improvements in radiotherapy targeting, notably the use of intensity-modulated radiotherapy, may increase efficacy and decrease the side effects in the future for these tumors. Cryotherapy is other non-surgical therapeutic modality, and different results have been reported for it. Although favorable results are reported by Marcove et al., the outcomes published by eggon et al., who reported a 62% rate of local recurrence in eight patients treated with curettage and cryosurgery, is not fascinating (3, 16). In addition, the potential complications such as permanent nerve damage make this treatment available at a few centers in the world only that have the expertise. Although there have been promising reports of biphosphonates and Denosumab in the management of giant cell tumor at the present time, these remain unproven in any clinical trial, and they might offer alternative treatment options in the future (23). We did not use any of these medications in the treatment of our patients. Pulmonary metastases have been described for GCT of long bones and axial skeleton (4, 12, 14, 24). The rate of pulmonary metastasis in GCT of the axial skeleton in different series is variable. While in some series its occurrence is higher than its rate in GCT of the appendicular skeleton, in other series there was not any case reported (14, 24). Young age during diagnosis, axial location of the primary GCT, Enneking s stage-3 disease, and local recurrence are found as risk factors for pulmonary metastasis, according to a recent report (24). Our patient series included just one pulmonary metastasis. The person was a patient with tumor recurrence and diagnosed with aneurismal bone cyst, ABC, superimposed on GCT. eceptor activator of nuclear factor κ-b ligand (ANK) has been implicated in pathophysiology of GCT (25). Denosumab, a human monoclonal antibody, binds to ANK and prevents its activation, thereby restraining both the destructive properties and the population of giant cells (26). It has been shown that subcutaneous injection of the Denosumab can decrease pain and increase functional levels of patients withunresectable or recurrent GCT (27). In another study, it is demonstrated that Denosumab can inhibit progression of GCT, leading to decreased need for surgery (28). Unresectable
7 )449( THE ACHIVES OF BONE AND JOINT SUGEY. ABJS.MUMS.AC.I VOUME 5. NUMBE 6. NOVEMBE 2017 GIANT CE TUMO OF SACUM pulmonary metastases have also been changed to resectable metastases by using Denosumab (29). Still, another report demonstrated that neoadjuvant therapy with Denosumab can make osteoclast-type giant cells disappear, both in the original tumor location, and in its pulmonary metastasis (30). All these encouraging results may introduce Denosumab as a new preoperative adjuvant therapy for patients with GCT of the sacrum as a modality to decrease the high morbidity associated with the surgery of this tumor. The small number of patients is one of limitations of this study, which makes statistical comparisons less valuable. SAE was not available in our patients, and this was another limitation of this study. We observed that preservation of sacral nerve roots was associated with better functional outcome and less pain in our patients. Although an acceptable surgical outcome was observed in our cohort, the problem of local recurrence still warrants further therapeutic modalities for better local control of the tumor. Khodamorad Jamshidi MD Abolfazl Bagherifard MD Alireza Mirzaei PhD Mehrdad Bahrabadi MD Bone and Joint econstruction esearch Center, Shafa Orthopedic Hospital, Iran University of Medical Sciences, Tehran, Iran eferences 1. Balke M, Henrichs MP, Gosheger G, Ahrens H, Streitbuerger A, Koehler M, et al. Giant cell tumors of the axial skeleton. Sarcoma. 2012;1-10:)410973( Domovitov SV, Chandhanayingyong C, Boland PJ, McKeown DG, Healey JH. Conservative surgery in the treatment of giant cell tumor of the sacrum: 35 years experience. J Neurosurg Spine. 2015; 30(2): eggon E, Zlotecki, eith J, Scarborough MT. Giant cell tumor of the pelvis and sacrum: 17 cases and analysis of the literature. Clin Orthop elat es. 2004; 423(1): Balke M, Streitbuerger A, Budny T, Henrichs M, Gosheger G, Hardes J. Treatment and outcome of giant cell tumors of the pelvis. Acta Orthop. 2009; 80(5): Thangaraj, Grimer, Carter S, Stirling AJ, Spilsbury J, Spooner D. Giant cell tumour of the sacrum: a suggested algorithm for treatment. Eur Spine J. 2010; 19(7): Gunterberg B, omanus B, Stener B. Pelvic strength after major amputation of the sacrum: an experimental study. Acta Orthop Scand. 1976; 47(6): Jimenez M. Pelvis, acetabulum, and hip trauma. In: Baratz M, Watson AD, Imbriglia JE, editors. Orthopaedic surgery: the essentials. New York: Thieme; P Enneking WF, Dunham W, Gebhardt MC, Malawar M, Pritchard DJ. A system for the functional evaluation of reconstructive procedures after surgical treatment of tumors of the musculoskeletal system. Clin Orthop elat es. 1993; 286(1): Carlsson AM. Assessment of chronic pain. I. Aspects of the reliability and validity of the visual analogue scale. Pain. 1983; 16(1): Gibbons KJ, Soloniuk DS, azack N. Neurological injury and patterns of sacral fractures. J Neurosurg. 1990; 72(6): Turcotte E, Wunder JS, Isler MH, Bell S, Schachar N, Masri BA, et al. Giant cell tumor of long bone: a Canadian Sarcoma Group study. Clin Orthop elat es. 2002; 397(1): Balke M, Schremper, Gebert C, Ahrens H, Streitbuerger A, Koehler G, et al. Giant cell tumor of bone: treatment and outcome of 214 cases. J Cancer es Clin Oncol. 2008; 134(9): Blackley H, Wunder JS, Davis AM, White M, Kandel, Bell S. Treatment of giant-cell tumors of long bones with curettage and bone-grafting. J Bone Joint Surg Am. 1999; 81(6): Martin C, McCarthy EF. Giant cell tumor of the sacrum and spine: series of 23 cases and a review of the literature. Iowa Orthop J. 2010; 30(1): Guo W, Ji T, Tang X, Yang Y. Outcome of conservative surgery for giant cell tumor of the sacrum. Spine. 2009; 34(10): Marcove C, Sheth DS, Brien EW, Huvos AG, Healey JH. Conservative surgery for giant cell tumors of the sacrum. The role of cryosurgery as a supplement to curettage and partial excision. Cancer. 1994; 74(4): Mendenhall WM, Zlotecki A, Scarborough MT, Gibbs CP, Mendenhall NP. Giant cell tumor of bone. Am J Clin Oncol. 2006; 29(1): Balke M, Ahrens H, Streitbuerger A, Koehler G, Winkelmann W, Gosheger G, et al. Treatment options for recurrent giant cell tumors of bone. J Cancer es Clin Oncol. 2009; 135(1): Hosalkar HS, Jones KJ, King JJ, ackman D. Serial arterial embolization for large sacral giant-cell tumors: mid-to long-term results. Spine. 2007; 32(10): in PP, Guzel VB, Moura MF, Wallace S, Benjamin S, Weber K, et al. ong-term follow-up of patients with giant cell tumor of the sacrum treated with selective
8 )450( THE ACHIVES OF BONE AND JOINT SUGEY. ABJS.MUMS.AC.I VOUME 5. NUMBE 6. NOVEMBE 2017 GIANT CE TUMO OF SACUM arterial embolization. Cancer. 2002; 95(6): ackman D, Khoury D, Esmail A, Donthineni-ao. The treatment of sacral giant-cell tumours by serial arterial embolisation. J Bone Joint Surg Br. 2002; 84(6): Chakravarti A, Spiro IJ, Hug EB, Mankin HJ, Efird JT, Suit HD. Megavoltage radiation therapy for axial and inoperable giant-cell tumor of bone. J Bone Joint Surg Am. 1999; 81(11): Thomas D, Chawla SP, Skubitz K, Staddon AP, Henshaw, Blay J, et al. Denosumab treatment of giant cell tumor of bone: Interim analysis of an open-label phase II study. J Clin Oncol. 2008; 26(15): Chan CM, Adler Z, eith JD, Gibbs CP. isk factors for pulmonary metastases from giant cell tumor of bone. J Bone Joint Surg Am. 2015; 97(5): oux S, Mariette X. ANK and ANK expression in giant-cell tumour of bone. ancet Oncol. 2010; 11(6): Branstetter DG, Nelson SD, Manivel JC, Blay JY, Chawla S, Thomas DM, et al. Denosumab induces tumor reduction and bone formation in patients with giant-cell tumor of bone. Clin Cancer es. 2012; 18(16): Thomas D, Henshaw, Skubitz K, Chawla S, Staddon A, Blay JY, et al. Denosumab in patients with giant-cell tumour of bone: an open-label, phase 2 study. ancet Oncol. 2010; 11(3): Chawla S, Henshaw, Seeger, Choy E, Blay JY, Ferrari S, et al. Safety and efficacy of denosumab for adults and skeletally mature adolescents with giant cell tumour of bone: interim analysis of an open-label, parallel-group, phase 2 study. ancet Oncol. 2013; 14(9): Watanabe Y, Kaya M, Sasaki M, Emori M, Murahashi Y, Mizushima E, et al. Experience using denosumab for lung metastases of giant cell tumor of bone. Eur Orthop Traumatol. 2015; 6(3): Yamagishi T, Kawashima H, Ogose A, Sasaki T, Hotta T, Inagawa S, et al. Disappearance of giant cells and presence of newly formed bone in the pulmonary metastasis of a sacral giant-cell tumor following denosumab treatment: a case report. Oncol ett. 2016; 11(1):243-6.
Giant cell tumour of the proximal femur
 ONCOLOGY Giant cell tumour of the proximal femur IS JOINT-SPARING MANAGEMENT EVER SUCCESSFUL? A. E. Wijsbek, B. L. Vazquez- Garcia, R. J. Grimer, S. R. Carter, A. A. Abudu, R. M. Tillman, L. Jeys From
ONCOLOGY Giant cell tumour of the proximal femur IS JOINT-SPARING MANAGEMENT EVER SUCCESSFUL? A. E. Wijsbek, B. L. Vazquez- Garcia, R. J. Grimer, S. R. Carter, A. A. Abudu, R. M. Tillman, L. Jeys From
Chondrosarcoma with a late local relapse
 Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Chondrosarcoma with a late local relapse J. Shinoda, T. Ozaki, T. Oka, T. Kunisada, H. Inoue Department of Orthopaedic Surgery, Okayama University Medical School, Okayama, 700-8558, Japan Correspondence:
Giant-cell tumours of the sacrum are difficult to
 The treatment of sacral giant-cell tumours by serial arterial embolisation R. D. Lackman, L. D. Khoury, A. Esmail, R. Donthineni-Rao The Hospital of the University of Pennsylvania, Philadelphia, USA Giant-cell
The treatment of sacral giant-cell tumours by serial arterial embolisation R. D. Lackman, L. D. Khoury, A. Esmail, R. Donthineni-Rao The Hospital of the University of Pennsylvania, Philadelphia, USA Giant-cell
Surgical Management for Giant Cell Tumor of Bones
 Journal of the Egyptian Nat. Cancer Inst., Vol. 6, No., September: 5-5, 00 Surgical Management for Giant Cell Tumor of Bones EL SAYED ASHRAF KHALIL, M.D. FRCS; ALAA YOUNIS, M.D.; SHERIF A. AZIZ, M.D and
Journal of the Egyptian Nat. Cancer Inst., Vol. 6, No., September: 5-5, 00 Surgical Management for Giant Cell Tumor of Bones EL SAYED ASHRAF KHALIL, M.D. FRCS; ALAA YOUNIS, M.D.; SHERIF A. AZIZ, M.D and
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine
 Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
Primary Bone Tumors: Spine Surgery Live -Video Techniques Mobile Spine Christopher Ames MD Professor of Neurosurgery and Orthopedic Surgery Director of Spine Tumor And Deformity Surgery UCSF Department
Intracanal Sacral Nerve Impingement Following Percutaneous Iliosacral Screw Pelvic Fixation
 texas orthopaedic journal CASE REPORT Intracanal Sacral Nerve Impingement Following Percutaneous Iliosacral Screw Pelvic Fixation Michael L. Brennan, MD; John M. Hamilton, MD; Christopher D. Chaput, MD;
texas orthopaedic journal CASE REPORT Intracanal Sacral Nerve Impingement Following Percutaneous Iliosacral Screw Pelvic Fixation Michael L. Brennan, MD; John M. Hamilton, MD; Christopher D. Chaput, MD;
Surgical Treatment of Spine Surgery Experience Primary Spinal Neoplasms ( ) Ziya L. Gokaslan, MD, FACS Approximately 3500 spine tumor
 Surgical Treatment of Primary Spinal Neoplasms Ziya L. Gokaslan, MD, FACS Donlin M. Long Professor Professor of Neurosurgery, Oncology & Orthopaedic Surgery Vice Chairman Director of Spine Program Department
Surgical Treatment of Primary Spinal Neoplasms Ziya L. Gokaslan, MD, FACS Donlin M. Long Professor Professor of Neurosurgery, Oncology & Orthopaedic Surgery Vice Chairman Director of Spine Program Department
Long-term administration of bisphosphonate to reduce local recurrence of sacral giant cell tumor after nerve-sparing surgery
 CLINICAL ARTICLE J Neurosurg Spine 26:716 721, 2017 Long-term administration of bisphosphonate to reduce local recurrence of sacral giant cell tumor after nerve-sparing surgery *Wei Xu, MD, 1 Yu Wang,
CLINICAL ARTICLE J Neurosurg Spine 26:716 721, 2017 Long-term administration of bisphosphonate to reduce local recurrence of sacral giant cell tumor after nerve-sparing surgery *Wei Xu, MD, 1 Yu Wang,
We considered whether a positive margin
 Classification of positive margins after resection of soft-tissue sarcoma of the limb predicts the risk of local recurrence C. H. Gerrand, J. S. Wunder, R. A. Kandel, B. O Sullivan, C. N. Catton, R. S.
Classification of positive margins after resection of soft-tissue sarcoma of the limb predicts the risk of local recurrence C. H. Gerrand, J. S. Wunder, R. A. Kandel, B. O Sullivan, C. N. Catton, R. S.
Management of infected custom mega prosthesis by Ilizarov method
 International Journal of Research in Medical Sciences Gudaru K et al. Int J Res Med Sci. 2015 Dec;3(12):3874-3878 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Case Report DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151459
International Journal of Research in Medical Sciences Gudaru K et al. Int J Res Med Sci. 2015 Dec;3(12):3874-3878 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Case Report DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151459
Laura M. Fayad, MD. Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University
 Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
Society of Pediatric Radiology, May 2013 Laura M. Fayad, MD Associate Professor of Radiology, Orthopaedic Surgery & Oncology The Johns Hopkins University Describes surgical techniques that resect and reconstruct
Therapeutic benefits of neoadjuvant and post-operative denosumab on sacral giant cell tumor: a retrospective cohort study of 30 cases
 JBUON 2018; 23(2): 453-459 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic benefits of neoadjuvant and post-operative denosumab on
JBUON 2018; 23(2): 453-459 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Therapeutic benefits of neoadjuvant and post-operative denosumab on
GIANT CELL TUMOR OF BONES: MANAGEMENT BY DIFFERENT SURGICAL TECHNIQUES
 GIANT CELL TUMOR OF BONES: MANAGEMENT BY DIFFERENT SURGICAL TECHNIQUES Sudqi A. Hamed MD*, Falah Z. Harfoushi MD* ABSTRACT Objective: To evaluate the clinical outcome of different surgical techniques used
GIANT CELL TUMOR OF BONES: MANAGEMENT BY DIFFERENT SURGICAL TECHNIQUES Sudqi A. Hamed MD*, Falah Z. Harfoushi MD* ABSTRACT Objective: To evaluate the clinical outcome of different surgical techniques used
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience. Kevin Yiee MD, MPH Resident Physician
 Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
Looking for the limit of limb sparing in pelvic bone sarcomas Isidro Gracia Hospital de la Santa Creu i Sant Pau, Barcelona
 Unidad de Cirugía Ortopédica Oncológica. Servicio COT Unidad Funcional de Tumores Mesenquimales Hospital de la Santa Creu i Sant Pau Barcelona Looking for the limit of limb sparing in pelvic bone sarcomas
Unidad de Cirugía Ortopédica Oncológica. Servicio COT Unidad Funcional de Tumores Mesenquimales Hospital de la Santa Creu i Sant Pau Barcelona Looking for the limit of limb sparing in pelvic bone sarcomas
Metastatic Disease of the Proximal Femur
 CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
CASE REPORT Metastatic Disease of the Proximal Femur WI Faisham, M.Med{Ortho)*, W Zulmi, M.S{Ortho)*, B M Biswal, MBBS** 'Department of Orthopaedic, "Department of Oncology and Radiotherapy, School of
Clinical Study The Use of Massive Endoprostheses for the Treatment of Bone Metastases
 Hindawi Publishing Corporation Sarcoma Volume 2007, Article ID 62151, 5 pages doi:10.1155/2007/62151 Clinical Study The Use of Massive Endoprostheses for the Treatment of Bone Metastases D. H. Park, P.
Hindawi Publishing Corporation Sarcoma Volume 2007, Article ID 62151, 5 pages doi:10.1155/2007/62151 Clinical Study The Use of Massive Endoprostheses for the Treatment of Bone Metastases D. H. Park, P.
Case report. Open Access. Abstract
 Open Access Case report Surgical treatment of a twice recurrent chondrosarcoma of the pubic symphysis: a case report and review of the literature George Petsatodis, Stavros I Stavridis*, Dimitrios Karataglis
Open Access Case report Surgical treatment of a twice recurrent chondrosarcoma of the pubic symphysis: a case report and review of the literature George Petsatodis, Stavros I Stavridis*, Dimitrios Karataglis
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Multidisciplinary management of retroperitoneal sarcomas
 Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
Multidisciplinary management of retroperitoneal sarcomas Eric K. Nakakura, MD UCSF Department of Surgery UCSF Comprehensive Cancer Center San Francisco, CA 7 th Annual Clinical Cancer Update North Lake
CASE STUDY: PRO-DENSE Injectable Regenerative Graft Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor
 : PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
: PRO-DENSE Used to Backfill a Bone Cavity Following Resection of a Giant Cell Tumor Contributed by: Matthew J. Seidel, MD* Lauren A. Schwartz, NP Scottsdale, AZ *Dr. Seidel is a paid consultant for Wright
Functional Outcome Study of Mega-Endoprosthetic Reconstruction in Limbs With Bone Tumour Surgery
 192 Original Article Functional Outcome Study of Mega-Endoprosthetic Reconstruction in Limbs With Bone Tumour Surgery Peh Khee Tan, 1 MBBS, MRCS (Edin), MMed (Orthop), Mann Hong Tan, 1 MBBS, FRCS (Edin
192 Original Article Functional Outcome Study of Mega-Endoprosthetic Reconstruction in Limbs With Bone Tumour Surgery Peh Khee Tan, 1 MBBS, MRCS (Edin), MMed (Orthop), Mann Hong Tan, 1 MBBS, FRCS (Edin
Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates
 ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
ORIGINAL ARTICLE SPINE SURGERY AND RELATED RESEARCH Spondylolysis repair using a pedicle screw hook or claw-hook system. a comparison of bone fusion rates Ko Ishida 1), Yoichi Aota 2), Naoto Mitsugi 1),
Advanced Pelvic Malignancy: Defining Resectability Be Aggressive. Lloyd A. Mack September 19, 2015
 Advanced Pelvic Malignancy: Defining Resectability Be Aggressive Lloyd A. Mack September 19, 2015 CONFLICT OF INTEREST DECLARATION I have no conflicts of interest Advanced Pelvic Malignancies Locally Advanced
Advanced Pelvic Malignancy: Defining Resectability Be Aggressive Lloyd A. Mack September 19, 2015 CONFLICT OF INTEREST DECLARATION I have no conflicts of interest Advanced Pelvic Malignancies Locally Advanced
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Note: Page numbers of article titles are in boldface type. A Ablative therapy, nonsurgical, for pulmonary metastases of soft tissue sarcoma, 279 280 Adipocytic tumors, atypical lipomatous tumor vs. well-differentiated
Endovascular and surgical treatment of giant pelvic tumor
 Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Endovascular and surgical treatment of giant pelvic tumor Mitrev Z., MD FETCS; Anguseva T., MD; Milev I., MD; Zafiroski G., PhD MD Center for Cardiosurgery, Filip the II, Skopje, Macedonia Background Giant
Radiotherapy symptoms control in bone mets. Francesco Cellini GemelliART. Ernesto Maranzano,MD. Session 5: Symptoms management
 Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Session 5: Symptoms management Radiotherapy symptoms control in bone mets Francesco Cellini GemelliART Ernesto Maranzano,MD Director of Oncology Department Chief of Radiation Oncology Centre S. Maria Hospital
Aneurysmal Bone Cyst of the Spine
 Copynghi 1985 8) The Journal o[ Bone and Joint.5urger IPIOrp()ratetI Aneurysmal Bone Cyst of the Spine BY R. CAPANNA, M.D.*, U. ALBISINNI, M.D.*, P. PICCI, M.D.*, P. CALDERONI, M.D.*, M. CAMPANACCI, M.D.*,
Copynghi 1985 8) The Journal o[ Bone and Joint.5urger IPIOrp()ratetI Aneurysmal Bone Cyst of the Spine BY R. CAPANNA, M.D.*, U. ALBISINNI, M.D.*, P. PICCI, M.D.*, P. CALDERONI, M.D.*, M. CAMPANACCI, M.D.*,
Case Report Treatment of Renal Cell Carcinoma with 2-Stage Total en bloc Spondylectomy after Marked Response to Molecular Target Drugs
 Case Reports in Orthopedics Volume 2013, Article ID 916501, 4 pages http://dx.doi.org/10.1155/2013/916501 Case Report Treatment of Renal Cell Carcinoma with 2-Stage Total en bloc Spondylectomy after Marked
Case Reports in Orthopedics Volume 2013, Article ID 916501, 4 pages http://dx.doi.org/10.1155/2013/916501 Case Report Treatment of Renal Cell Carcinoma with 2-Stage Total en bloc Spondylectomy after Marked
14. Background. Sarcoma. Resectable extremity soft tissue sarcomas
 96 14. Sarcoma Background Radiotherapy is widely used as an adjunct to surgery in the management of soft tissue sarcomas as the risk of failure in the surgical bed can be high. For bone sarcomas, radiotherapy
96 14. Sarcoma Background Radiotherapy is widely used as an adjunct to surgery in the management of soft tissue sarcomas as the risk of failure in the surgical bed can be high. For bone sarcomas, radiotherapy
Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D.
 J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
J Neurosurg 60:282-286, 1984 Harrington rod stabilization for pathological fractures of the spine NARAYAN SUNDARESAN, M.D., JOSEPH H. GALICICH, M.D., AND JOSEPH M. LANE, M.D. Neurosurgery and Orthopedic
PELVIC RECONSTRUCTION WITH ALLOGENEIC BONE GRAFT AFTER TUMOR RESECTION
 Original Article PELVIC RECONSTRUCTION WITH ALLOGENEIC BONE GRAFT AFTER TUMOR RESECTION Wei Wang 1, Wen Zhi Bi 1, Jing Yang 2, Gang Han 1, Jin Peng Jia 1 ABSTRACT Objectives: Pelvic reconstruction after
Original Article PELVIC RECONSTRUCTION WITH ALLOGENEIC BONE GRAFT AFTER TUMOR RESECTION Wei Wang 1, Wen Zhi Bi 1, Jing Yang 2, Gang Han 1, Jin Peng Jia 1 ABSTRACT Objectives: Pelvic reconstruction after
Over a 25-year period we have treated 36 patients
 Osteosarcoma of the pelvis R. J. Grimer, S. R. Carter, R. M. Tillman, D. Spooner, D. C. Mangham, Y. Kabukcuoglu From the Royal Orthopaedic Hospital Oncology Service, Birmingham, England Over a 25-year
Osteosarcoma of the pelvis R. J. Grimer, S. R. Carter, R. M. Tillman, D. Spooner, D. C. Mangham, Y. Kabukcuoglu From the Royal Orthopaedic Hospital Oncology Service, Birmingham, England Over a 25-year
Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft
 900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
900 Original Article Giant Cell Tumour of the Distal Radius: Wide Resection and Reconstruction by Non-vascularised Proximal Fibular Autograft Ayman Abdelaziz Bassiony, 1 MD Abstract Introduction: Giant
CASE PRESENTATION. Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN
 CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
CASE PRESENTATION Dr. Faseeh Shahab PGY3 Orthopaedic Resident, Khyber Teaching Hospital, Peshawar, PAKISTAN CASE PRESENTATION - History Ms. SB, 30yo Afghan National Presented with 3 months history of Swelling
JMSCR Vol 06 Issue 12 Page December 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 79.54 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i12.140 A Case Report of Recurrent
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested is: Please check the indication (reason) for this procedure
Functional and oncological outcomes after total claviculectomy for primary malignancy
 Acta Orthop. Belg., 2012, 78, 170-174 ORIGINAL STUDY Functional and oncological outcomes after total claviculectomy for primary malignancy Zhaoxu Li, Zhaoming YE, Miaofeng ZHAng From the Department of
Acta Orthop. Belg., 2012, 78, 170-174 ORIGINAL STUDY Functional and oncological outcomes after total claviculectomy for primary malignancy Zhaoxu Li, Zhaoming YE, Miaofeng ZHAng From the Department of
Radiation Therapy for Soft Tissue Sarcomas
 Radiation Therapy for Soft Tissue Sarcomas Alexander R. Gottschalk, MD, PhD Assistant Professor, Radiation Oncology University of California, San Francisco 1/25/08 NCI: limb salvage vs. amputation 43 patients
Radiation Therapy for Soft Tissue Sarcomas Alexander R. Gottschalk, MD, PhD Assistant Professor, Radiation Oncology University of California, San Francisco 1/25/08 NCI: limb salvage vs. amputation 43 patients
What s new in bone and soft tissue sarcoma Treatment and Guidelines 2012? Rob Grimer
 What s new in bone and soft tissue sarcoma Treatment and Guidelines 2012? Rob Grimer ESMO conference 2012 Top Oncologists in world (~ 400) Lots of sarcoma basic science key messages: 40% of STS diagnoses
What s new in bone and soft tissue sarcoma Treatment and Guidelines 2012? Rob Grimer ESMO conference 2012 Top Oncologists in world (~ 400) Lots of sarcoma basic science key messages: 40% of STS diagnoses
Radiotherapy Considerations in Extremity Sarcoma
 Radiotherapy Considerations in Extremity Sarcoma Peter Chung Department of Radiation Oncology Princess Margaret Hospital University of Toronto Role of RT in STS Local tumour eradication while allowing
Radiotherapy Considerations in Extremity Sarcoma Peter Chung Department of Radiation Oncology Princess Margaret Hospital University of Toronto Role of RT in STS Local tumour eradication while allowing
We have studied 560 patients with osteosarcoma of a
 Osteosarcoma of the limb AMPUTATION OR LIMB SALVAGE IN PATIENTS TREATED BY NEOADJUVANT CHEMOTHERAPY G. Bacci, S. Ferrari, S. Lari, M. Mercuri, D. Donati, A. Longhi, C. Forni, F. Bertoni, M. Versari, E.
Osteosarcoma of the limb AMPUTATION OR LIMB SALVAGE IN PATIENTS TREATED BY NEOADJUVANT CHEMOTHERAPY G. Bacci, S. Ferrari, S. Lari, M. Mercuri, D. Donati, A. Longhi, C. Forni, F. Bertoni, M. Versari, E.
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients
 Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Chondroblastoma of bone
 Chronology Chondroblastoma of bone LONG-TERM RESULTS AND FUNCTIONAL OUTCOME AFTER INTRALESIONAL CURETTAGE R. Suneja, R. J. Grimer, M. Belthur, L. Jeys, S. R. Carter, R. M. Tillman, A. M. Davies From The
Chronology Chondroblastoma of bone LONG-TERM RESULTS AND FUNCTIONAL OUTCOME AFTER INTRALESIONAL CURETTAGE R. Suneja, R. J. Grimer, M. Belthur, L. Jeys, S. R. Carter, R. M. Tillman, A. M. Davies From The
Unstable fractures of the pelvis treated with a trapezoid compression frame
 Acta Orthop Scand 55, 325-329, 1984 Unstable fractures of the pelvis treated with a trapezoid compression frame Sixteen patients with unstable pelvic fractures were treated by early reduction and fixation
Acta Orthop Scand 55, 325-329, 1984 Unstable fractures of the pelvis treated with a trapezoid compression frame Sixteen patients with unstable pelvic fractures were treated by early reduction and fixation
Laterally positioned hemivertebrae and the resultant. Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases.
 spine case report J Neurosurg Spine 22:84 89, 2015 Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases Shaheryar F. Ansari, MD, 1 Richard B. Rodgers, MD, 2 and Daniel H. Fulkerson,
spine case report J Neurosurg Spine 22:84 89, 2015 Dorsal midline hemivertebra at the lumbosacral junction: report of 2 cases Shaheryar F. Ansari, MD, 1 Richard B. Rodgers, MD, 2 and Daniel H. Fulkerson,
Associated Terms: Osteosarcoma, Bone Cancer, Limb Salvage, Appendicular Osteosarcoma, Pathologic Fracture, Chondrosarcoma
 1 of 9 9/29/2014 8:25 PM Associated Terms: Osteosarcoma, Bone Cancer, Limb Salvage, Appendicular Osteosarcoma, Pathologic Fracture, Chondrosarcoma The term "ACVS Diplomate" refers to a veterinarian who
1 of 9 9/29/2014 8:25 PM Associated Terms: Osteosarcoma, Bone Cancer, Limb Salvage, Appendicular Osteosarcoma, Pathologic Fracture, Chondrosarcoma The term "ACVS Diplomate" refers to a veterinarian who
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Simret Singh Randhawa, Angel Khor Nee Kwan, Chee Kidd Chiu, Chris Yin Wei Chan, Mun Keong Kwan. 1. Case 1
 Asian Spine Journal Asian Spine Case Journal Report Asian Spine J 2016;10(5):945-949 Treatment of https://doi.org/10.4184/asj.2016.10.5.945 denosumab without surgery Neurological Recovery in Two Patients
Asian Spine Journal Asian Spine Case Journal Report Asian Spine J 2016;10(5):945-949 Treatment of https://doi.org/10.4184/asj.2016.10.5.945 denosumab without surgery Neurological Recovery in Two Patients
factor for identifying unstable thoracolumbar fractures. There are clinical and radiological criteria
 NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
NMJ-Vol :2/ Issue:1/ Jan June 2013 Case Report Medical Sciences Progressive subluxation of thoracic wedge compression fracture with unidentified PLC injury Dr.Thalluri.Gopala krishnaiah* Dr.Voleti.Surya
Management of Campanacci type III giant cell tumor
 2017; 3(1): 836-841 ISSN: 2395-1958 IJOS 2017; 3(1): 836-841 2017 IJOS www.orthopaper.com Received: 15-11-2016 Accepted: 16-12-2016 Brig. Muhammad Suhail Amin Head of Orthopedics Surgery Department, Combined
2017; 3(1): 836-841 ISSN: 2395-1958 IJOS 2017; 3(1): 836-841 2017 IJOS www.orthopaper.com Received: 15-11-2016 Accepted: 16-12-2016 Brig. Muhammad Suhail Amin Head of Orthopedics Surgery Department, Combined
Modified Harrington Procedure for Acetabular Insuficiency Due to Metastatic Malignant Disease
 Malaysian Orthopaedic Journal 2009 Vol 3 No 1 WI Faisham, et al Modified Harrington Procedure for Acetabular Insuficiency Due to Metastatic Malignant Disease WI Faisham, MMed Ortho, DAJ Muslim, MRCS, VMK
Malaysian Orthopaedic Journal 2009 Vol 3 No 1 WI Faisham, et al Modified Harrington Procedure for Acetabular Insuficiency Due to Metastatic Malignant Disease WI Faisham, MMed Ortho, DAJ Muslim, MRCS, VMK
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
3D CONFORMATIONAL INTERSTITIAL BRACHYTHERAPY PLANNING FOR SOFT TISSUE SARCOMA
 3D CONFORMATIONAL INTERSTITIAL BRACHYTHERAPY PLANNING FOR SOFT TISSUE SARCOMA Alina TĂNASE 1,3, M. DUMITRACHE 2,3, O. FLOREA 1 1 Emergency Central Military Hospital Dr. Carol Davila Bucharest, Romania,
3D CONFORMATIONAL INTERSTITIAL BRACHYTHERAPY PLANNING FOR SOFT TISSUE SARCOMA Alina TĂNASE 1,3, M. DUMITRACHE 2,3, O. FLOREA 1 1 Emergency Central Military Hospital Dr. Carol Davila Bucharest, Romania,
Interesting Case Series. Ganglion Cyst of the Peroneus Longus
 Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
Soft-tissue Recurrence of Giant Cell tumor of Bone Associated with Pulmonary Metastases.
 Soft-tissue Recurrence of Giant Cell tumor of Bone Associated with Pulmonary Metastases. M. M. Abdel- Motaal 1, A. S. Othman 1, M. K. C. Katchy 2, A. K. Jassar 3 1 Al-Razi Orthopaedic Hospital, Kuwait,
Soft-tissue Recurrence of Giant Cell tumor of Bone Associated with Pulmonary Metastases. M. M. Abdel- Motaal 1, A. S. Othman 1, M. K. C. Katchy 2, A. K. Jassar 3 1 Al-Razi Orthopaedic Hospital, Kuwait,
J. Bryce Olenczak, MD, Matthew G. Stanwix, MD, and Gedge D. Rosson, MD
 CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
CASE REPORT Complex Wound Closure of Partial Sacrectomy Defect With Human Acellular Dermal Matrix and Bilateral V to Y Gluteal Advancement Flaps in a Pediatric Patient J. Bryce Olenczak, MD, Matthew G.
Osteoarticular allograft reconstruction of the distal radius after giant cell tumor resection
 Original Research Medical Journal of the Islamic Republic of Iran.Vol. 22, No.1, May 2008. pp. 1-7 Osteoarticular allograft reconstruction of the distal radius after giant cell tumor resection Khodamorad
Original Research Medical Journal of the Islamic Republic of Iran.Vol. 22, No.1, May 2008. pp. 1-7 Osteoarticular allograft reconstruction of the distal radius after giant cell tumor resection Khodamorad
A Guide to Ewing Sarcoma
 A Guide to Ewing Sarcoma Written By Physicians For Physicians WHAT IS EWING SARCOMA (ES) ES is a malignant bone tumor that can evolve from any bone in the body (and occasionally soft tissue) and mostly
A Guide to Ewing Sarcoma Written By Physicians For Physicians WHAT IS EWING SARCOMA (ES) ES is a malignant bone tumor that can evolve from any bone in the body (and occasionally soft tissue) and mostly
Transmetatarsal amputation in an at-risk diabetic population: a retrospective study
 The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
The Journal of Diabetic Foot Complications Transmetatarsal amputation in an at-risk diabetic population: a retrospective study Authors: Merribeth Bruntz, DPM, MS* 1,2, Heather Young, MD 3,4, Robert W.
Functional Results after Giant Cell Tumor Operation near Knee Joint and the Cement Radiolucent Zone as Indicator of Recurrence
 Functional Results after Giant Cell Tumor Operation near Knee Joint and the Cement Radiolucent Zone as Indicator of Recurrence K. KAFCHITSAS 1, B. HABERMANN 1, D. PROSCHEK 1, A. KURTH 1 and C. EBERHARDT
Functional Results after Giant Cell Tumor Operation near Knee Joint and the Cement Radiolucent Zone as Indicator of Recurrence K. KAFCHITSAS 1, B. HABERMANN 1, D. PROSCHEK 1, A. KURTH 1 and C. EBERHARDT
Review Article Chondrosarcoma of the Mobile Spine and Sacrum
 Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
Sarcoma Volume 2011, Article ID 274281, 4 pages doi:10.1155/2011/274281 Review Article Chondrosarcoma of the Mobile Spine and Sacrum Ryan M. Stuckey and Rex A. W. Marco Department of Orthopaedics, University
A Two-incision Approach for En Bloc Resection of Periacetabular Tumors with Illustrations from acadaver
 60 2014 Chinese Orthopaedic Association and Wiley Publishing Asia Pty Ltd SURGICAL TECHNIQUE A Two-incision Approach for En Bloc Resection of Periacetabular Tumors with Illustrations from acadaver Chang-an
60 2014 Chinese Orthopaedic Association and Wiley Publishing Asia Pty Ltd SURGICAL TECHNIQUE A Two-incision Approach for En Bloc Resection of Periacetabular Tumors with Illustrations from acadaver Chang-an
Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing Tumor Resections
 CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
CLINICAL ORTHOPAEDICS AND RELATED RESEARCH Number 426, pp. 97 102 2004 Lippincott Williams & Wilkins Intercalary Femur and Tibia Segmental Allografts Provide an Acceptable Alternative in Reconstructing
Comparison of Sacral Ratio in Normal Children and Children with Urinary and/or Faecal Complaints
 Short Comunication Iran J Pediatr Mar 2008; Vol 18 ( No 1), Pp:57-61 Comparison of Sacral Ratio in Normal Children and Children with Urinary and/or Faecal Complaints Abdol Mohammad Kajbaf Zadeh* 1, MD,
Short Comunication Iran J Pediatr Mar 2008; Vol 18 ( No 1), Pp:57-61 Comparison of Sacral Ratio in Normal Children and Children with Urinary and/or Faecal Complaints Abdol Mohammad Kajbaf Zadeh* 1, MD,
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
Giant cell tumor of the distal ulna: a case report
 Vanni et al. Journal of Medical Case Reports 2012, 6:143 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant cell tumor of the distal ulna: a case report Daniele Vanni 1, Andrea Pantalone 1,
Vanni et al. Journal of Medical Case Reports 2012, 6:143 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant cell tumor of the distal ulna: a case report Daniele Vanni 1, Andrea Pantalone 1,
Pelvic Fractures. AOCP National Course Belfast City Hospital. 11 th June D Swain BSc; FRCSI; FRCS (Orth.)
 Pelvic Fractures AOCP National Course Belfast City Hospital 11 th June 2010 Who s this bloke? Consultant orthopaedic surgeon RVH Trained in Belfast, England and Toronto Interests - pelvic and acetabular
Pelvic Fractures AOCP National Course Belfast City Hospital 11 th June 2010 Who s this bloke? Consultant orthopaedic surgeon RVH Trained in Belfast, England and Toronto Interests - pelvic and acetabular
Introduction. Epidemiology Pathophysiology Classification Treatment
 Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Diabetic Foot Introduction Epidemiology Pathophysiology Classification Treatment Epidemiology DM largest cause of neuropathy in N.A. 1 million DM patients in Canada Half don t know Foot ulcerations is
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Epidural Injection Please check the indication (reason)
Role of Bisphosphonates as Adjuvants of Surgery in Giant Cell Tumor of Spine
 International Journal of Spine Surgery, Vol. 12, No. 6, 2018, pp. 695 702 https://doi.org/10.14444/5087 ÓInternational Society for the Advancement of Spine Surgery Role of Bisphosphonates as Adjuvants
International Journal of Spine Surgery, Vol. 12, No. 6, 2018, pp. 695 702 https://doi.org/10.14444/5087 ÓInternational Society for the Advancement of Spine Surgery Role of Bisphosphonates as Adjuvants
Pelvic fractures. Dr Raymond Yean, MBBS Surgical SRMO
 Pelvic fractures Dr Raymond Yean, MBBS Surgical SRMO PELVIC FRACTURES Pelvic fracture account for 2-8% all skeletal injuries Associated with High energy trauma Soft tissue injuries and blood loss. Shock,
Pelvic fractures Dr Raymond Yean, MBBS Surgical SRMO PELVIC FRACTURES Pelvic fracture account for 2-8% all skeletal injuries Associated with High energy trauma Soft tissue injuries and blood loss. Shock,
Lytic Lesion in the Distal Phalanx of the Hand
 Shafa Ortho J. 2015 February; 2(1):e441. Published online 2015 February 15. DOI: 10.5812/soj.441 Research Article Lytic Lesion in the Distal Phalanx of the Hand Khodamorad Jamshidi 1 ; Farid Najd Mazhar
Shafa Ortho J. 2015 February; 2(1):e441. Published online 2015 February 15. DOI: 10.5812/soj.441 Research Article Lytic Lesion in the Distal Phalanx of the Hand Khodamorad Jamshidi 1 ; Farid Najd Mazhar
Management of Bone and Spinal Cord in Spinal Surgery.
 Management of Bone and Spinal Cord in Spinal Surgery. G. Saló, PhD, MD. Senior Consultant Spine Unit. Hospital del Mar. Barcelona. Ass. Prof. Universitat Autònoma de Barcelona. Introduction The management
Management of Bone and Spinal Cord in Spinal Surgery. G. Saló, PhD, MD. Senior Consultant Spine Unit. Hospital del Mar. Barcelona. Ass. Prof. Universitat Autònoma de Barcelona. Introduction The management
Symptoms and signs associated with benign and malignant proximal fibular tumors: a clinicopathological analysis of 52 cases
 Sun et al. World Journal of Surgical Oncology (2017) 15:92 DOI 10.1186/s12957-017-1162-z RESEARCH Open Access Symptoms and signs associated with benign and malignant proximal fibular tumors: a clinicopathological
Sun et al. World Journal of Surgical Oncology (2017) 15:92 DOI 10.1186/s12957-017-1162-z RESEARCH Open Access Symptoms and signs associated with benign and malignant proximal fibular tumors: a clinicopathological
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD
 STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
STAGING, BIOPSY AND NATURAL HISTORY OF TUMORS SCOTT D WEINER MD WHAT DO YOU DO WHEN THIS SHOWS UP IN YOUR OFFICE? besides panicking KEY PRINCIPLE!!! Reactive zone is the edema, neovascularity and inflammation
BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE
 BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE EDWARD HM WANG, MD UP-Musculoskeletal Tumor Unit and Tissue & Bone Bank Dept. of Orthopedics University of the Philippines-Philippine
BONE TRANSPLANTATION IN LIMB SAVING SURGERIES: THE PHILIPPINE EXPERIENCE EDWARD HM WANG, MD UP-Musculoskeletal Tumor Unit and Tissue & Bone Bank Dept. of Orthopedics University of the Philippines-Philippine
Spine Pain Management Program
 Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
Spine Pain Management Program Please complete the following information: Patient Name: Patient ID Number: Patient DOB: The procedure being requested: Facet Injection Please check the indication (reason)
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Spinal metastasis of intermediate grade chondrosarcoma without pulmonary involvement
 Spinal metastasis of intermediate grade chondrosarcoma without pulmonary involvement Dr. A.S. Parasnis, Dr. A. Duggal, Dr. S. M. Navadgi, Dr. A. Puri, Dr. M.G. Agarwal, Dr. S.B.Desai Orthopaedic Oncology
Spinal metastasis of intermediate grade chondrosarcoma without pulmonary involvement Dr. A.S. Parasnis, Dr. A. Duggal, Dr. S. M. Navadgi, Dr. A. Puri, Dr. M.G. Agarwal, Dr. S.B.Desai Orthopaedic Oncology
An acetabular-preserving procedure for pelvic giant cell tumor involving partial acetabulum
 Xiao et al. World Journal of Surgical Oncology (2017) 15:200 DOI 10.1186/s12957-017-1269-2 TECHNICAL INNOVATIONS Open Access An acetabular-preserving procedure for pelvic giant cell tumor involving partial
Xiao et al. World Journal of Surgical Oncology (2017) 15:200 DOI 10.1186/s12957-017-1269-2 TECHNICAL INNOVATIONS Open Access An acetabular-preserving procedure for pelvic giant cell tumor involving partial
Effective local and systemic therapy is necessary for the cure of Ewing tumor Most chemotherapy regimens are a combination of cyclophosphamide,
 Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Ewing Tumor Perez Ewing tumor is the second most common primary tumor of bone in childhood, and also occurs in soft tissues Ewing tumor is uncommon before 8 years of age and after 25 years of age In the
Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms.
 RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
OSSEOUS INVASION IN ALVEOLAR SARCOMA OF SOFT TISSUES: A HEALING APPROACH AND LIMB-SALVAGING SURGERY. Summary
 Kovachev V. et. al. Osseous invasion in alveolar sarcoma of soft tissues: Case report OSSEOUS INVASION IN ALVEOLAR SARCOMA OF SOFT TISSUES: A HEALING APPROACH AND LIMB-SALVAGING SURGERY Vihar Ì. Kovachev,
Kovachev V. et. al. Osseous invasion in alveolar sarcoma of soft tissues: Case report OSSEOUS INVASION IN ALVEOLAR SARCOMA OF SOFT TISSUES: A HEALING APPROACH AND LIMB-SALVAGING SURGERY Vihar Ì. Kovachev,
Result of extracorporeal irradiation and re-implantation for malignant bone tumors: A review of 30 patients
 bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2012 doi: 10.1111/ajco.12036 ORIGINAL ARTICLE Result of extracorporeal irradiation and re-implantation for malignant bone tumors: A review of 30 patients
bs_bs_banner Asia-Pacific Journal of Clinical Oncology 2012 doi: 10.1111/ajco.12036 ORIGINAL ARTICLE Result of extracorporeal irradiation and re-implantation for malignant bone tumors: A review of 30 patients
Pilon Fractures Pearls of Treatment Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSOT November 2017, Tampa
 Pilon Fractures Pearls of Treatment Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSOT November 2017, Tampa Disclosures No relevant disclosures There is more literature
Pilon Fractures Pearls of Treatment Steven Steinlauf, MD The Orthopaedic Foot and Ankle Institute of South Florida CSOT November 2017, Tampa Disclosures No relevant disclosures There is more literature
Clinical Reference Guide
 Clinical Reference Guide Table of Clinical References PREVALENCE Bernard, 1987 Cohen, 2005 Weksler, 2007 Sembrano, 2009 POST LUMBAR FUSION Maigne, 2005 Ha, 2008 Ivanov, 2009 Liliang, 2011 DePalma, 2011
Clinical Reference Guide Table of Clinical References PREVALENCE Bernard, 1987 Cohen, 2005 Weksler, 2007 Sembrano, 2009 POST LUMBAR FUSION Maigne, 2005 Ha, 2008 Ivanov, 2009 Liliang, 2011 DePalma, 2011
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
ICD-10 Service Line Overview Musculoskeletal
 ICD-10 Service Line Overview Musculoskeletal ICD-10 incorporates much greater clinical detail and specificity as well as updated terminology to be consistent with current clinical practices. ICD-10-CM
ICD-10 Service Line Overview Musculoskeletal ICD-10 incorporates much greater clinical detail and specificity as well as updated terminology to be consistent with current clinical practices. ICD-10-CM
Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage
 Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
Accepted February 13th, 2004 Iliac aneurysmal bone cyst treated by cystoscopic controlled curettage Ludwig Schwering¹, Markus Uhl² and Georg W. Herget( )¹ ¹ Department of Orthopaedics and Traumatology,
Unicameral bone cysts are benign, fluid-filled cavities
 Endoscopic Surgery for Symptomatic Unicameral Bone Cyst of the Proximal Femur Wataru Miyamoto, M.D., Masato Takao, M.D., Youichi Yasui, M.D., Shinya Miki, M.D., and Takashi Matsushita, M.D. Abstract: Recently,
Endoscopic Surgery for Symptomatic Unicameral Bone Cyst of the Proximal Femur Wataru Miyamoto, M.D., Masato Takao, M.D., Youichi Yasui, M.D., Shinya Miki, M.D., and Takashi Matsushita, M.D. Abstract: Recently,
We studied the CT and MR scans, and the
 Tumour volume as a predictor of necrosis after chemotherapy in Ewing s sarcoma A. Abudu, A. M. Davies, P. B. Pynsent, D. C. Mangham, R. M. Tillman, S. R. Carter, R. J. Grimer From the Royal Orthopaedic
Tumour volume as a predictor of necrosis after chemotherapy in Ewing s sarcoma A. Abudu, A. M. Davies, P. B. Pynsent, D. C. Mangham, R. M. Tillman, S. R. Carter, R. J. Grimer From the Royal Orthopaedic
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Laparoscopic Resection Of Colon & Rectal Cancers. R Sim Centre for Advanced Laparoscopic Surgery, TTSH
 Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Laparoscopic Resection Of Colon & Rectal Cancers R Sim Centre for Advanced Laparoscopic Surgery, TTSH Feasibility and safety Adequacy - same radical surgery as open op. Efficacy short term benefits and
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage
 Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Pedicled Fillet of Leg Flap for Extensive Pressure Sore Coverage Shareef Jandali, MD, and David W. Low, MD Division of Plastic Surgery, University of Pennsylvania Health System, Philadelphia Correspondence:
Objectives. Limb salvage surgery. Age distribution bone cancer. Age distribution soft tissue sarcomas
 LifeSource October, 2011 Disclosure Information Putting humpty dumpty back together again is easier with tissue allografts! Limb Salvage Surgery for Bone Tumors Edward Cheng, MD October 6, 2011 Disclosure
LifeSource October, 2011 Disclosure Information Putting humpty dumpty back together again is easier with tissue allografts! Limb Salvage Surgery for Bone Tumors Edward Cheng, MD October 6, 2011 Disclosure
Malignant Peripheral Nerve Sheath Tumor post Wide Excision with Multiple Lung Metastases: the Role and Treatment Consideration of RT
 Malignant Peripheral Nerve Sheath Tumor post Wide Excision with Multiple Lung Metastases: the Role and Treatment Consideration of RT Case Number: RT2009-64(M) Potential Audiences: Intent Doctor, Oncology
Malignant Peripheral Nerve Sheath Tumor post Wide Excision with Multiple Lung Metastases: the Role and Treatment Consideration of RT Case Number: RT2009-64(M) Potential Audiences: Intent Doctor, Oncology
