Jefferson Digital Commons. Thomas Jefferson University. Charles Galanis The Johns Hopkins Medical Institutions
|
|
|
- Phoebe Davidson
- 5 years ago
- Views:
Transcription
1 Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery July 2007 Resected serous cystic neoplasms of the pancreas: Locally aggressive behavior as a predictor of malignant disease? A review of 158 patients with recommendations for treatment. Charles Galanis The Johns Hopkins Medical Institutions Amir Zamani The Johns Hopkins Medical Institutions John L. Cameron The Johns Hopkins Medical Institutions Kurtis A. Campbell The Johns Hopkins Medical Institutions Keith D. Lillemoe Indiana University School of Medicine See Let next page us for know additional how authors access to this document benefits you Follow this and additional works at: Part of the Surgery Commons Recommended Citation Galanis, Charles; Zamani, Amir; Cameron, John L.; Campbell, Kurtis A.; Lillemoe, Keith D.; Caparrelli, David; Chang, David ; Hruban, Ralph H.; and Yeo, Charles, "Resected serous cystic neoplasms of the pancreas: Locally aggressive behavior as a predictor of malignant disease? A review of 158 patients with recommendations for treatment." (2007). Department of Surgery Faculty Papers. Paper 3. This Article is brought to you for free and open access by the Jefferson Digital Commons. The Jefferson Digital Commons is a service of Thomas Jefferson University's Center for Teaching and Learning (CTL). The Commons is a showcase for Jefferson books and journals, peer-reviewed scholarly publications, unique historical collections from the University archives, and teaching tools. The Jefferson Digital Commons allows researchers and interested readers anywhere in the world to learn about and keep up to date with Jefferson scholarship. This article has been accepted for inclusion in
2 Authors Charles Galanis, Amir Zamani, John L. Cameron, Kurtis A. Campbell, Keith D. Lillemoe, David Caparrelli, David Chang, Ralph H. Hruban, and Charles Yeo This article is available at Jefferson Digital Commons:
3 Prepared for: Journal of Gastrointestinal Surgery July 2006 Resected Serous Cystic Neoplasms of the Pancreas: Locally Aggressive Behavior as a Predictor of Malignant Disease? A Review of 158 Patients with Recommendations for Treatment. Charles Galanis, M.D. Amir Zamani, B.S. John L. Cameron, M.D. Kurtis A. Campbell, M.D. Keith D. Lillemoe, M.D.# David Caparrelli, M.D. David Chang, Ph.D. Ralph H. Hruban, M.D. Charles J. Yeo, M.D.** Work originating from: Departments of Surgery and Pathology The Sol Goldman Pancreatic Cancer Research Center The Johns Hopkins Medical Institutions, Baltimore, MD Current Author Affiliations: Department of Surgery, Indiana University School of Medicine, Indianapolis, IN# Department of Surgery, Jefferson Medical College, Philadelphia, PA** Poster Presentation at Pancreas Club and SSAT May 2006, Los Angeles, CA Correspondence Charles J. Yeo, M.D. Samuel D. Gross Professor and Chair Department of Surgery Thomas Jefferson University/Jefferson Medical College 1015 Walnut Street, Suite 620 Philadelphia, PA Phone (215) Fax (215) charles.yeo@jefferson.edu
4 1 ABSTRACT Background: Serous cystic neoplasms of the pancreas are regarded as a benign entity with rare malignant potential. Surgical resection is generally considered curative. Objective: To perform the largest single institution review of patients who underwent surgical resection for serous cystic neoplasms of the pancreas in the hopes of guiding future management. Methods: Between June 1988 and January 2005, 158 patients with serous cystic neoplasms of the pancreas underwent surgical resection. A retrospective analysis was performed. Univariate and multivariate models were used to determine factors influencing perioperative morbidity and mortality. Major complications were defined as pancreatic fistula or anastomotic leak, postoperative bleed, retained operative material, or death. Minor complications were defined as wound infection, postoperative obstruction/ileus requiring TPN, delayed gastric emptying, arrhythmia, or other infection. Results: The mean age of the patients was 62.1 years, with 75% being female. The majority of patients were symptomatic at presentation (63%), with abdominal pain as the most common symptom. Of the 158 patients, 75 underwent distal pancreatectomy, 65 underwent pancreaticoduodenectomy, 9 underwent central pancreatectomy, 5 underwent local resection or enucleation, and 4 underwent total pancreatectomy. Mean tumor diameter was 5.1 cm. Mean operative time was minutes. Mean postoperative length of hospital stay was 11 days. One patient was diagnosed at presentation with serous cystadenocarcinoma. The remaining 157 patients were initially diagnosed with benign serous cystadenoma. One of three patients with locally aggressive benign disease
5 2. later presented with metastatic disease. Resection margins for all 158 patients were negative for tumor, and only 1 (0.6%) showed lymph node involvement. There was one intraoperative death. The incidence of major perioperative complications was 18%, while the incidence of minor complications was 33%. Men were significantly more likely to experience minor perioperative complications (OR = 3.74, P =.008), while patients greater than 65 years showed a trend toward fewer major complications (OR = 0.36, P =.09). Conclusions: Serous cystic neoplasms of the pancreas which are surgically resected are typically seen in asymptomatic women, as 5 cm neoplasms which are predominantly benign. Most are resected via either a left or right sided pancreatectomy with low mortality risk, but with notable major or minor morbidity. Cystadenocarcinoma is a rare finding on initial resection of serous cystic neoplasms. However, initial pathology specimens exhibiting benign but locally aggressive neoplasia may indicate an increased likelihood of recurrence or metachronous metastasis.
6 3. INTRODUCTION Serous cystic neoplasms (SCNs) of the pancreas are almost always benign. They are one of the most common primary pancreatic cystic neoplasms, and are distinguished from mucinous cystic neoplasms (MCNs) and intraductal papillary mucinous neoplasms (IPMNs) (1). SCNs constitute 10-15% of all cystic masses of the pancreas and 1-2% of all pancreatic neoplasms (2,3). However, SCNs are being increasingly diagnosed with more widespread use and improving technology of imaging techniques (4,5). These neoplasms show a predilection for middle-aged and older women and are often discovered incidentally (6). Symptoms are frequently non-specific, with abdominal pain being the most common, occurring in 50-60% of all cases (7). Computed tomography is thought to be the diagnostic test of choice to properly identify this tumor type (8). SCNs are typically unifocal and present as large, well-demarcated, often honeycombed cystic masses which can grow as large as 25 cm. Diffuse or multifocal disease is uncommon. The cysts are loculated, consist of mucin-free serous fluid, and are surrounded by cuboidal or flattened epithelium. (9) Unlike MCNs and IPMNs, SCNs are generally regarded as almost always benign, though their potential for malignant conversion remains a topic of debate (10). Due in large part to the uncertainty over malignant potential and the natural history of the disease, currently there is no accepted standard of treatment or follow-up for SCNs. For many, observation and routine surveillance are preferred (11). Some investigators recommend complete resection of all SCNs because of the perceived malignant potential of the disease, the relative frequency of symptoms and complications, and the challenge
7 4. of an accurate preoperative diagnosis (2,12,13). Those that utilize a selective approach advocate for resection in the setting of tumors that are symptomatic, poorly defined, and larger sized (7,14). Indeed, symptomatology appears to be the predominant and only universally accepted indication for operative intervention. In all cases, resection is considered curative, with no postoperative surveillance recommended. The goals of our large (158 patients) single institution review were to evaluate clinical parameters, pathologic features, and overall patient outcome following resection of SCNs of the pancreas, in the hopes of guiding future management.
8 5. METHODS Between June 1988 and January 2005, 158 patients with serous cystic neoplasms of the pancreas underwent surgical resection. A retrospective analysis of a database was performed. The study was approved by the Institutional Review Board for Human Research and complied with Health Insurance Portability and Accountability Act (HIPAA) regulations. Major complications were defined as pancreatic fistula or anastomotic leak, postoperative bleed, retained operative material, or death. Minor complications were defined as wound infection, postoperative obstruction/ileus requiring TPN, bowel obstruction responsive to conservative non-operative treatment, delayed gastric emptying, arrhythmia, or other infection. Follow-up data were collected from postoperative admissions and/or clinic visits. Univariate and multivariate models were used to determine factors influencing perioperative morbidity and mortality. The chi square test was used for comparison between categorical outcome variables versus categorical independent variables, while t test was used to compare between continuous outcome variables versus categorical independent variables. Multiple logistic regression was used in final analysis. Statistical significance was defined as p<0.05. Statistical analysis was performed using Stata 9. Data are given as mean +/- standard deviation, where appropriate.
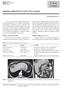
9 6. RESULTS Demographics Table 1 outlines the patient population in our series. The mean age of patients was years with most patients being non-hispanic whites (81%). The majority of patients (75%) were female. There was no significant difference in age of presentation between males and females. Presentation Most patients presented with symptoms (64%). The most common symptoms were abdominal pain (74%), weight loss (22%), nausea/vomiting (10%), jaundice (6%), and GI bleed (3%). Men tended to be symptomatic more than women (45% of men versus 34% of women, not significant). Symptoms did not correlate with location or size of tumor. Of 158 patients, 66 (42%) underwent a computed tomography (CT) scan at our institution while the remaining were referred and treated with outside studies. Figure 1 shows two representative CT scans of patients with SCNs. Operative and Postoperative Course All patients in this series were treated operatively. Of the 158 patients, 75 (47%) underwent distal pancreatectomy for neoplasm of the body or tail of the pancreas, 65 (41%) underwent pancreaticoduodenectomy for right-sided tumors, 9 (6%) underwent central pancreatectomy for neoplasms of the neck or proximal body, 5 (3%) underwent local resection or enucleation, and 4 (3%) underwent total pancreatectomy for neoplasms extensively involving the gland. The average operative time was minutes. The average transfusion requirement was units of packed red blood cells. There was
10 7. one operative death due to intraoperative hemorrhage from visceral vessels. Overall, the incidence of major complications was 18% while the incidence of minor complications was 33%. The most common major complication was pancreatic leak or fistula with an incidence of 13%. Men were significantly more likely to have minor complications than women (OR = 3.75, p =.008). Patients >65 years of age also showed a trend toward fewer major complications (OR = 0.36, p =.088). Table 2 and Table 3 describe complications by age and gender respectively. Mean postoperative length of hospital stay was 11.3 (SD = 8.9 days). Pathology For 158 resected tumors, the mean tumor size was 5.1 cm cm. Tumors were located in the head (42%), body or tail (48%), proximal neck or body (7%), and with diffuse involvement of the entire gland (3%). Tumor size did not significantly vary by tumor location. Of all 158 patients, one patient at primary resection was noted to have biopsy proven serous cystic neoplasm of the liver and was therefore diagnosed with serous cystadenocarcinoma. The remaining 157 patients were diagnosed at primary resection with serous cystadenoma of the pancreas. Of these 157 patients, 3 were noted in final pathology report to have locally aggressive disease on histologic examination. One of these 3 patients recurred 13 years later with disease in the liver and retroperitoneal tissue and was therefore diagnosed with serous cystadenocarcinoma.
11 8. DISCUSSION Classified as a benign neoplasm, serous cystic neoplasm (SCN) of the pancreas is the most common primary cystic neoplasm of the pancreas and accounts for 1-2% of all primary pancreatic neoplasms (1). SCNs had long been classified with mucinous cystic neoplasms, until Compagno and Oertel as well as Hodgkinson and others defined and separated serous from mucinous cystic neoplasms (15, 16). They recognized that the mucinous variants such as mucinous cystic neoplasms (MCNs) and intraductal papillary mucinous neoplasms (IPMNs) have a significantly greater malignant potential than SCNs. George et al. first introduced a malignant variant known as serous cystadenocarcinoma (10). There have since been multiple case reports of malignant SCN histologically indistinguishable from benign SCN of the pancreas but marked by malignant behavior, most commonly invasive or metastatic disease (12,17-23). One study suggested that up to 3% of reported SCNs were in fact malignant or had malignant potential (8). This malignant variant is defined by the presence of metastases to extrapancreatic organs or tissues (24). Vascular and perineural invasion, and local invasion into the duodenum or stomach, are not criteria for the diagnosis of malignancy. There currently exists no consensus for management of SCNs. Many advocate simple surveillance given the almost universally benign nature of the disease and the relative morbidity and mortality associated with resection (11). However, a schedule of surveillance which adequately defines when expectant management should yield to
12 9. intervention has yet to be agreed upon. Furthermore, because other cystic neoplasms of the pancreas have significant malignant potential, it is imperative that the diagnosis of SCN be certain before committing to expectant management and surveillance. Others support a selective approach to resection based on symptoms, tumor size, or indeterminate preoperative diagnosis, among other factors (13,14). There continue to be those who support resection of all SCNs. They cite the real, albeit rare, malignant potential, the risk of an incorrect preoperative diagnosis, and the potential for symptoms and complications. Resection is generally considered curative and no postoperative monitoring is advocated. Here we report the largest single institution experience with SCNs to date. The mean age of the 158 patients was 62.1 years with 75% being female (Table 1). This is consistent with previous studies which have also shown a predilection for the disease in middle aged to elderly females. Most patients were symptomatic at presentation (64%). Among symptomatic patients, the most common symptoms were abdominal pain (74%), weight loss (22%), nausea/vomiting (10%), jaundice (6%), and GI bleed (3%). The proportion of symptomatic patients is similar to or higher than that found in most other reviews. (8,14,15) The higher rate of symptomatic patients may partly be explained by the extensive referral nature of the practice at Johns Hopkins. In our series, 41% of the SCNs arose in the head of the pancreas, 48% in the body or tail, 6% in the neck or proximal body, and only 3% of lesions exhibited diffuse involvement of the entire gland. Mean tumor diameter was 5.1 cm, similar to the size found in Tseng et al. s
13 10. contemporary series (14). All resection margins were negative, with only one SCN exhibiting lymph node involvement. There was one intraoperative death, due to excessive hemorrhage. In our experience, surgery for these lesions carried minimum mortality risk (0.6%) but notable major (18%) and minor (33%) morbidity risk. This risk of complications approximates the risk of pancreatic surgery for other conditions (such as adenocarcinoma of the pancreas) but the mortality rate for resection of SCN is less (25). It is worth noting that males had a significantly greater risk of experiencing minor complications than women. The reasons for this difference are not immediately apparent and warrant further investigation. No patient died of his or her disease. This fact, in conjunction with the aforementioned risks of surgery, would support a cautious approach to the resection of these neoplasms. In our series, only 0.6% (1/158) of the patients with an SCN presented with metastatic disease. This patient presented initially with multifocal disease in the pancreas and liver, and was therefore diagnosed with a serous cystadenocarcinoma. Indeed, after resection of her pancreatic tumor, she returned to clinic one year later with extensive growth of a biopsy proven SCN in the liver which was nonoperable. Remarkably, both her primary and the liver metastases had a histologically bland appearance, lacking both architectural and cytologic atypia. An additional 3 patients in this study were noted to have locally aggressive neoplasms at the time of initial resection. These neoplasms were histologically identical to the more benign behaving tumors, but showed locally aggressive behavior by growing into neighboring structures (Figure 2). Margins were negative for these tumors. One of these patients returned in follow-up 13 years after
14 11. resection with biopsy proven recurrence in the liver and retroperitoneal soft tissue. Again, both the primary and the liver metastases had a histologically bland appearance, lacking both architectural and cytologic atypia. As this represented an extrapancreatic recurrence, the diagnosis for this patient was adjusted to reflect a serous cystadenocarcinoma. Thus, a total of two of the 158 patients (1.3%) in this series either presented with or ultimately developed metastatic disease. Currently, resection for SCN is considered curative with no follow-up beyond postoperative care recommended. Here we report one case of recurrence following resection of the primary tumor. This tumor exhibited locally aggressive behavior at time of initial resection. Only two of the remaining 157 resected specimens exhibited a similar pattern. Locally aggressive growth therefore may offer an important clue as to which neoplasms have the potential to recur as cystadenocarcinoma. It will be interesting to follow the 2 additional patients whose tumors exhibited locally aggressive growth. Their lack of metastatic disease or recurrence may be explained by the fact that their primary resections were relatively recent (1999 and 2000) as compared to the primary resection for the patient whose disease later recurred (1992). Further follow-up of this tumor characteristic is warranted, and may offer a tool in determining a subpopulation of patients who do not have metastases at presentation, but for whom additional follow-up surveillance is warranted. The proper management of patients with a SCN remains elusive. The first step is to distinguish this lesion from the more aggressive and premalignant lesions: IPMNs and MCNs. Beyond that, there are divergent paths. Based on our findings, we propose the
15 12. following algorithm (Figure 3). If SCN cannot confidently be distinguished from MCN or IPMN, the patient should undergo resection. When the diagnosis of SCN is confidently determined based on clinical and radiographic evidence, perhaps only symptomatic tumors should be resected. If the decision is made to avoid resection initially, we do recommend serial imaging at a 6 to 12 months interval, with resection for growth (more than 1 cm change in diameter) or the development of symptoms. Post resection, gross and microscopic review of the neoplasm should document not only the presence or absence of metastases, but also any locally aggressive growth. For neoplasms exhibiting this rare characteristic, patients should be counseled that although in most cases SCNs are cured with primary resection, a small sub-population of cases may recur, and may require additional imaging follow-up and treatment, as indicated.
16 13 References 1. Kosmahl M, Wagner J, Peters K et al. Cystic neoplasms of the pancreas: an immunohistochemical analysis revealing alpha-inhibin, neuron-specific enolase, and MUC6 as new markers. Am J Pathol 2004; 28: Horvath KD, Chabot JA. An aggressive resectional approach to cystic neoplasms of the pancreas. Am J Surg, 1999;178: Owen DA and Kelly JK: Pathology of the Gall Bladder, Biliary Tract, and Pancreas. Philadelphia, Sunders, 2001, vol 39, p 154) 4. Megibow AJ, Lombardo FP, Guiarise A, et al. Cystic masses: cross-sectional imaging observations and serial follow-up. Abdom Imaging 2001;26: Fernandez-del Castillo C, Targarona J, Thayer SP, et al. Incidental pancreatic cysts: clinicopathologic characteristics and comparison with symptomatic patients. Arch Surg. 2003; 138: Winter JH, Cameron JL, Lillemoe KD et al. Periampullary and pancreatic incidentaloma: A single institution s experience with an increasingly common diagnosis. Ann Surg 2006; 243; 5: Pyke CM, van Heerden JA, Colby TV, Sarr MG, Weaver AL. The spectrum of serous cystadenoma of the pancreas. Clinical, pathologic, and surgical aspects. Ann Surg 1992; 215:
17 Le Borgne J, de Chalan L, Partensky C. Cystadenomas and cystadenocarcinoma of the pancreas: a multiinstitutional and retrospective study of 398 cases. French Surgical Association. Ann Surg. 1999;230: Capella C, Solcia E, Kloppel G, Hruba RH. Serous cystic neoplasms of the pancreas. In: Hamilton SR, Aaltonen LA, editors. World Health Organization Classification of Tumors. Pathology and Genetics of Tumours of the Digestive Tract. Lyon: IARC Press, 200: George DH, Murphy F, Michalski R, Ulmer BG. Serous cystadenocarcinoma of the pancreas: a new entity? Am J Surg Path. 1989; 13: Bassi C, Salvia R, Molinari E, Biautti C, Falconi M, Pederzli P. Management of 100 consecutive cases of pancreatic serous cystadenoma: wait for images and see at imaging or vice versa? World J Surg 2003;27: Strobel O, Z graggen K, Schmitz-Winnentha FH, et al. Risk of malignancy in serous cystic neoplasms of the pancreas. Digestion 2003;68: Siech M, Tripp K, Schmidt-Rohlfing B, et al. Cystic tumors of the pancreas: diagnostic accuracy, pathologic observations, and surgical consequences. Langenbecks Arch Surg. 1998; 383: Tseng J, Warshaw A et al. Serous Cystadenoma of the Pancreas: Tumor Growth Rates and Recommendations for Treatment. Ann Surg. 2005; 242: Compagno J, Oertel JE. Microcystic adenomas of the pancreas (glycogen-rich cystadenomas): a clinicopathologic study of 34 cases. Am J Clin Pathol 1978;69:
18 Hodgkinson DJ, ReMine WH, Weiland LH. Pancreatic cystadenoma. A clinicopathologic study of 45 cases. Arch Surg 1978; 113: Matsumoto T et al. Malignant Serous Cystic Neoplasm of the Pancreas. J Clin Gastroenterol. 2005; 39: Ohta T, Nagakawa T, Itho H, et al. A case of serous cystadenoma of the pancreas with focal malignant changes. Int J Pancreatol 1993;14: Eriguchi N, Aoyagi S, Nakayama T, et al. Serous cystadenocarcinoma of the pancreas with liver metastases. J Hepatobiliary Pancreat Surg 1998;5: Abe H, Kubota K, Mori M et al. Serous cystadenoma of the pancreas with invasive growth: benign or malignant? Am J Gastroenterol 1998;93: Brenin DR, Talamonti MS, Yang EY et al. Cystic neoplasms of the pancreas. A clinicopathologic study, including DNA flow cytometry. Arch Surg 1995;130: Okata T, Nonami T, Miwa T et al. Hepatic metastasis of serous cystadenocarcinoma resected 4 years after operation a case report. Nippon Shokakibyo Gakkai Zasshi 1991; 88: Wu, CM, Hruban RH, Fishman EK, Schlott WD, Cameron JL. Serous cystic neoplasm of the pancreas involving the pancreas and liver: an unusual clinical entity. Abdom Imaging 1999; 24: Hruban RH, Klimstra DS, Pitman MB. Washington DC. Atlas of tumor pathology. Tumors of the Pancreas. 4 th Series. American Institute of Pathology. In press.
19 Sohn T, Yeo C, Cameron J et al. Resected adenocarcinoma of the pancreas 616 patients: Results, outcomes, and prognostic indicators. J Gastrointest Surg 2000; 4; 6:
20 n (%) Mean + SD Total patients 158 Sex Male 70 (25) Female 118 (75) Age (years) Symptomatic 101 (64) Abdominal pain 75 (47) Weight loss 22 (14) Nausea/vomiting 10 (6) Jaundice 6 (4) Gastrointestinal bleed 3 (2) Operation Distal pancreatectomy, splenectomy 75 (47) Whipple 65 (41) Central pancreatectomy 9 (6) Local resection or enucleation 5 (3) Total pancreatectomy 4 (3) Tumor size (cm) Operative time (minutes) Hospital stay (days) Death 1 (0.6) Major complication 29 (18) Hemorrhage 2 (1.2) Pancreatic leak 21 (13) Bile leak 5 (3) Retained operative material 1 (0.6) Minor complication 52 (33)* Wound infection 8 (5) Delayed gastric emptying 5 (3) Postoperative ileus 4 (2) Arrhythmia 8 (5) Other infection 21 (12) Final pathologic diagnosis Serous cystadenoma 156 (98) Serous cystadenocarcinoma 2 (2)** TABLE 1: Patient characteristics. Patients greater than 65 years showed a trend toward fewer major complications (OR = 0.36, P =.09). *Men had significantly more minor complications than women (OR = 3.74, p =.008). ** One patient who was diagnosed with serous cystadenoma on initial resection later recurred and was therefore re-diagnosed with cystadenocarcinoma.
21 65 years > 65 years p value Number of patients Major Complications (total) Hemorrhage 1 1 Pancreatic leak 14 7 Bile leak 3 2 Retained operative material 1 0 Minor Complications (total) N.S. Wound infection 4 4 Delayed gastric emptying 3 2 Postoperative ileus 3 1 Small bowel obstruction* 3 0 Arrhythmia 5 3 Deep Vein Thrombosis 1 0 Other infection 12 9 TABLE 2: Complications compared with age of patients. Note that patients greater than 65 years showed a trend toward fewer major complications (OR = 0.36, P =.09). Number of patients Male Female p value Major Complications (total) 6 23 N.S. Hemorrhage 0 2 Pancreatic leak 6 15 Bile leak 0 5 Retained operative material 0 1 Minor Complications (total) Wound infection 3 5 Delayed gastric emptying 1 4 Postoperative ileus 1 3 Small bowel obstruction* 1 2 Arrhythmia 3 5 Deep Vein Thrombosis 1 0 Other infection 7 14 TABLE 3: Complications compared with patient gender. Note that males had significantly more minor complications than women (OR = 3.74, p =.008).
22 b FIGURE LEGENDS FIGURE 1: Computed tomography (CT) scans of two patients, each with serous cystadenoma of the pancreas. The image on the right is from a 64 year old female who presented with abdominal pain. Her 10 cm neoplasm in the head of the pancreas was resected with a Whipple procedure without complication. The image on the left is from a 59 yo female who presented with pain and fullness. Her 27 cm mass originating from the tail of the pancreas was resected with a distal pancreatectomy and splenectomy without complication. FIGURE 2: Locally aggressive SCN. Although classically benign, SCNs may rarely exhibit locally aggressive behavior. In one patient, tumor compresses the pancreatic duct (a). On microscopic examination, this neoplasm exhibits bland histological appearance, lacking both architectural and cytologic atypia (b). However, this SCN shows uncommon locally aggressive behavior by growing up against and into a neighboring lymph node (arrows). FIGURE 3: Proposed approach to the patient with a cystic neoplasm of the pancreas.
23 FIGURE 1
24 a Pancreatic duct Compressed duct b FIGURE 2
25 PANCREATIC CYSTIC NEOPLASM MCN Indeterminate diagnosis SCN Asymptomatic Resect Symptomatic Size increase Expectant management with serial (6-12 mo) imaging No change Locally aggressive behavior on pathologic examination No aggressive behavior on pathologic examination Likely curative, serial imaging not necessary Increased likelihood of recurrence Careful clinical and radiographic follow-up with treatment as indicated FIGURE 3
Pancreatic Cysts. Darius C. Desai, MD FACS St. Luke s University Health Network
 Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble?
 Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated Pancreatectomy
 ISPUB.COM The Internet Journal of Surgery Volume 7 Number 2 A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated T Matsumoto, K Iwaki, H Uchida, K Yada, K Shibata,
ISPUB.COM The Internet Journal of Surgery Volume 7 Number 2 A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated T Matsumoto, K Iwaki, H Uchida, K Yada, K Shibata,
ORIGINAL ARTICLE. Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm
 ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
PAPER. Experience With 208 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas
 PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
Neoplasias Quisticas del Páncreas
 SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
Matthew McCollough, M.D. April 9, 2009 University of Louisville
 Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Select problems in cystic pancreatic lesions
 Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:813 817 Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts MAOR LAHAV, YAKOV MAOR, BENJAMIN AVIDAN, BEN NOVIS, and SIMON BAR MEIR Department
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:813 817 Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts MAOR LAHAV, YAKOV MAOR, BENJAMIN AVIDAN, BEN NOVIS, and SIMON BAR MEIR Department
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients
 LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
3/28/2012. Periampullary Tumors. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Eric K. Nakakura Ko Olina, HI
 Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas
 HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
Unusual Pancreatic Neoplasms RTC 2/11/2011
 Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Unusual Pancreatic Neoplasms RTC 2/11/2011 Objectives Intraductal Papillary Mucinous Neoplasm (IPMN) Mucinous Cystic Neoplasm (MCN) Islet Cell Tumors Insulinoma Glucagonoma VIPoma Somatostatinoma Gastrinoma
Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas
 Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS
 Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Cystic Pancreatic Lesions: Approach to Diagnosis
 Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Surgical management and results for cystic neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center experience with 324 patients who underwent surgical resection
 Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
p53 expression in invasive pancreatic adenocarcinoma and precursor lesions
 Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics
 Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Surgical Management of Pancreatic Cancer
 I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
I Congresso de Oncologia D Or July 5-6, 2013 Surgical Management of Pancreatic Cancer Michael A. Choti, MD, MBA, FACS Department of Surgery Johns Hopkins University School of Medicine, Baltimore, MD Estimated
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas.
 Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Cystic pancreatic lesions A proposal for a network approach. Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth
 Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
X-ray Corner. Imaging of The Pancreas. Pantongrag-Brown L
 X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Morphologic features in cystic lesions of pancreas-a retrospective analysis
 International Journal of Advances in Medicine Cicy PJ et al. Int J Adv Med. 2018 Feb;5(1):192-196 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180083
International Journal of Advances in Medicine Cicy PJ et al. Int J Adv Med. 2018 Feb;5(1):192-196 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180083
Disclosure of Relevant Financial Relationships
 Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Outcomes of pancreaticoduodenectomy in patients with metastatic cancer
 Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Korean J Hepatobiliary Pancreat Surg 2014;18:147-151 http://dx.doi.org/.14701/kjhbps.2014.18.4.147 Original Article Outcomes of pancreaticoduodenectomy in patients with metastatic cancer Joo Hwa Kwak,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Patient with incidental pancreatic cyst
 Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
Patient History. A 58 year old man presents with a 16 mm cyst in the pancreatic tail. The cyst is unilocular with a thick wall and no mural nodule.
 Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14
 Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Greater Manchester and Cheshire HPB Unit Guidelines for the Assessment & Management of Hepatobiliary and Pancreatic Disease Chapter 14 Contents 14. Neuroendocrine Tumours 161 14.1. Diagnostic algorithm
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Types of IPMN. Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy. Cysts: Early Neoplasia. Mucinous Cystic Lesions. EUS-guided FNA EUS
 Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Case report. Open Access. Abstract
 Open Access Case report Laparoscopic resection of a pancreatic serous cystadenoma preserving the integrity of main pancreatic duct: a case report Michail Pitiakoudis 1, Petros Zezos 2 *, Anastasia Oikonomou
Open Access Case report Laparoscopic resection of a pancreatic serous cystadenoma preserving the integrity of main pancreatic duct: a case report Michail Pitiakoudis 1, Petros Zezos 2 *, Anastasia Oikonomou
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016
 40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
An Approach to Pancreatic Cysts. Introduction
 An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
RESEARCH ARTICLE. Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation
 DOI:10.22034/APJCP.2017.18.1.207 RESEARCH ARTICLE Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation Vor Luvira 1 *, Kulyada Somsap 2, Ake Pugkhem
DOI:10.22034/APJCP.2017.18.1.207 RESEARCH ARTICLE Morphological Classification of Intraductal Papillary Neoplasm of the Bile Duct with Survival Correlation Vor Luvira 1 *, Kulyada Somsap 2, Ake Pugkhem
Histologic Characteristics Enhance Predictive Value of American Joint Committee on Cancer Staging in Resectable Pancreas Cancer
 Original Article Histologic Characteristics Enhance Predictive Value of American Joint Committee on Cancer Staging in Resectable Pancreas Cancer James Helm, MD, PhD 1,2,3,4,5 ; Barbara A. Centeno, MD 3,6,7
Original Article Histologic Characteristics Enhance Predictive Value of American Joint Committee on Cancer Staging in Resectable Pancreas Cancer James Helm, MD, PhD 1,2,3,4,5 ; Barbara A. Centeno, MD 3,6,7
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Recommendations for the Reporting of Pancreatic Specimens Containing Malignant Tumors
 AJCP / REPORTING RECOMMENDATIONS FOR PANCREATIC SPECIMENS CONTAINING MALIGNANT TUMORS Recommendations for the Reporting of Pancreatic Specimens Containing Malignant Tumors Jorge AlboresSaavedra, David
AJCP / REPORTING RECOMMENDATIONS FOR PANCREATIC SPECIMENS CONTAINING MALIGNANT TUMORS Recommendations for the Reporting of Pancreatic Specimens Containing Malignant Tumors Jorge AlboresSaavedra, David
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Does the Mechanism of Lymph Node Invasion Affect Survival in Patients with Pancreatic Ductal Adenocarcinoma?
 Does the Mechanism of Lymph Node Invasion Affect Survival in Patients with Pancreatic Ductal Adenocarcinoma? The Harvard community has made this article openly available. Please share how this access benefits
Does the Mechanism of Lymph Node Invasion Affect Survival in Patients with Pancreatic Ductal Adenocarcinoma? The Harvard community has made this article openly available. Please share how this access benefits
Pancreatic Cystic Neoplasms: Predictors of Malignant Behavior and Management
 Original Article Pancreatic Cystic Neoplasms: Predictors of Malignant Behavior and Management Ehab Atef, Ayman El Nakeeb, Ehab El Hanafy, Mohamed El Hemaly, Emad Hamdy, Ahmed El Geidie Surgical Center,
Original Article Pancreatic Cystic Neoplasms: Predictors of Malignant Behavior and Management Ehab Atef, Ayman El Nakeeb, Ehab El Hanafy, Mohamed El Hemaly, Emad Hamdy, Ahmed El Geidie Surgical Center,
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget
 Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Pancreatobiliary Frozen Section Nightmares
 Pancreatobiliary Frozen Section Nightmares Aatur D. Singhi, MD PhD Assistant Professor University of Pittsburgh Medical Center Department of Pathology singhiad@upmc.edu Objectives Briefly give an overview
Pancreatobiliary Frozen Section Nightmares Aatur D. Singhi, MD PhD Assistant Professor University of Pittsburgh Medical Center Department of Pathology singhiad@upmc.edu Objectives Briefly give an overview
Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
An investigation of pancreatic volume by disease using pancreatic volumetry
 Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Giant pancreatic mucinous cystadenoma with malignant transformation
 Case Report Brunei Int Med J. 2014; 10 (3): 177-182 Giant pancreatic mucinous cystadenoma with malignant transformation Jerica CHAI 1, Vui Heng CHONG 2, Ian BICKLE 1 1 Department of Radiology and 2 Department
Case Report Brunei Int Med J. 2014; 10 (3): 177-182 Giant pancreatic mucinous cystadenoma with malignant transformation Jerica CHAI 1, Vui Heng CHONG 2, Ian BICKLE 1 1 Department of Radiology and 2 Department
Serous Cystadenomas Follow a Benign and Asymptomatic Course and Do Not Present a Significant Size Change During Follow-Up
 REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com Rev Inves Clin. 2015;67:344-9 PERMANYER BRIEF COMMUNICATIONS Serous Cystadenomas Follow a Benign
REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com Rev Inves Clin. 2015;67:344-9 PERMANYER BRIEF COMMUNICATIONS Serous Cystadenomas Follow a Benign
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Distal Pancreatectomy with Celiac Axis Resection: What Are the Added Risks?
 Distal Pancreatectomy with Celiac Axis Resection: What Are the Added Risks? Joal D. Beane, MD a, Michael G. House, MD a, Susan C. Pitt, MD c, E. Molly Kilbane a, Bruce L. Hall c, Abishek Parmar d, Taylor.
Distal Pancreatectomy with Celiac Axis Resection: What Are the Added Risks? Joal D. Beane, MD a, Michael G. House, MD a, Susan C. Pitt, MD c, E. Molly Kilbane a, Bruce L. Hall c, Abishek Parmar d, Taylor.
Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study
 Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
Original article Annals of Gastroenterology (2013) 26, 346-352 Surgical resection improves survival in pancreatic cancer patients without vascular invasion- a population based study Subhankar Chakraborty
The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms
 JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms
 HPB, 2008; 10: 483490 ORIGINAL ARTICLE Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms WILLIAM E. FISHER a, SALLY E. HODGES a, VIVEK YAGNIK b, FANNIE E. MORÓN b, MENG-FEN
HPB, 2008; 10: 483490 ORIGINAL ARTICLE Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms WILLIAM E. FISHER a, SALLY E. HODGES a, VIVEK YAGNIK b, FANNIE E. MORÓN b, MENG-FEN
Misdiagnosis of pancreatic papillary mucinous cystadenocarcinoma: A case report
 1070 Misdiagnosis of pancreatic papillary mucinous cystadenocarcinoma: A case report PENG FEI QIAO, GUANG MING NIU and YANG GAO Department of Magentic Resonance Imaging, Affiliated Hospital of Inner Mongolia
1070 Misdiagnosis of pancreatic papillary mucinous cystadenocarcinoma: A case report PENG FEI QIAO, GUANG MING NIU and YANG GAO Department of Magentic Resonance Imaging, Affiliated Hospital of Inner Mongolia
Pancreatic Cystic Neoplasms: Guidelines and beyond
 Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review
 Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Review Article Common and unusual CT and MRI manifestations of pancreatic adenocarcinoma: a pictorial review Min-Jie Yang, Su Li, Yong-Guang Liu, Na Jiao, Jing-Shan Gong Department of Radiology, Shenzhen
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period
 Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Management of cystic and solid pancreatic incidentalomas: A review analysis
 J BUON 2013; 18(1): 17-24 ISSN: 1107-0625 www.bu-on.org/jbuon E-mail: jbuon@ath.forthnet.gr REVIEW ARTICLE Management of cystic and solid pancreatic incidentalomas: A review analysis T. Karatzas 1, D.
J BUON 2013; 18(1): 17-24 ISSN: 1107-0625 www.bu-on.org/jbuon E-mail: jbuon@ath.forthnet.gr REVIEW ARTICLE Management of cystic and solid pancreatic incidentalomas: A review analysis T. Karatzas 1, D.
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Case Report Solid Serous Adenoma of the Pancreas: A Case Report and Review of the Literature
 Case Reports in Surgery Volume 2016, Article ID 3730249, 5 pages http://dx.doi.org/10.1155/2016/3730249 Case Report Solid Serous Adenoma of the Pancreas: A Case Report and Review of the Literature Anastasios
Case Reports in Surgery Volume 2016, Article ID 3730249, 5 pages http://dx.doi.org/10.1155/2016/3730249 Case Report Solid Serous Adenoma of the Pancreas: A Case Report and Review of the Literature Anastasios
Small Intestine. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition
 Small Intestine Protocol applies to all invasive carcinomas of the small intestine, including those with focal endocrine differentiation. Excludes carcinoid tumors, lymphomas, and stromal tumors (sarcomas).
Small Intestine Protocol applies to all invasive carcinomas of the small intestine, including those with focal endocrine differentiation. Excludes carcinoid tumors, lymphomas, and stromal tumors (sarcomas).
Serous Cystadenocarcinoma of the Pancreas: Clinical Features and Management of a Rare Tumor
 Review Article Received: November 25, 2015 Accepted: February 14, 2016 Published online: March 22, 2016 Pancreas: Clinical Features and Management of a Rare Tumor Timothy J. Van Dyke a Frederick C. Johlin
Review Article Received: November 25, 2015 Accepted: February 14, 2016 Published online: March 22, 2016 Pancreas: Clinical Features and Management of a Rare Tumor Timothy J. Van Dyke a Frederick C. Johlin
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment
 Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Pancreatic Adenocarcinoma: Everything You Need to Know From Cross-Sectional Imaging to Treatment Andrew W. Bowman, MD PhD Assistant Professor of Radiology Mayo Clinic Florida SCBT-MR Annual Meeting Nashville,
Gastrinoma: Medical Management. Haley Gallup
 Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Gastrinoma: Medical Management Haley Gallup Also known as When to put your knife down Gastrinoma Definition and History Diagnosis Historic Management Sporadic vs MEN-1 Defining surgical candidates Nonsurgical
Surgical Management of Neuroendocrine Tumors of the Gut. Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School
 Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Intraductal papillary neoplasms in the bile ducts
 Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
Intraductal papillary neoplasms in the bile ducts Seok Hwa Youn Myunghee Yoon Dong Hoon Shin Kosin University Gospel Hospital Department of general surgery Hepato-biliary-pancreatic division Introduction
pissn: , eissn: Yonsei Med J 53(1): , 2012
 Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.106 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):106-110, 2012 Comparison of Efficacy of Enucleation and Pancreaticoduodenectomy for Small
Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.106 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):106-110, 2012 Comparison of Efficacy of Enucleation and Pancreaticoduodenectomy for Small
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Appendix 5. EFSUMB Newsletter. Gastroenterological Ultrasound
 EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
EFSUMB Newsletter 87 Examinations should encompass the full range of pathological conditions listed below A log book listing the types of examinations undertaken should be kept Training should usually
Malignant Obstructive Jaundice has dismal
 Proceeding S.Z.P.G.M.L vol: 22(2}: pp. 79-83, 2008. Anatomic Level of Biliary Obstruction and Outcome of Pre-Operative Biliary Stenting in Malignant Obstructive Jaundice -A Shaikh Zayed Hospital Experience
Proceeding S.Z.P.G.M.L vol: 22(2}: pp. 79-83, 2008. Anatomic Level of Biliary Obstruction and Outcome of Pre-Operative Biliary Stenting in Malignant Obstructive Jaundice -A Shaikh Zayed Hospital Experience
Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation
 246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
Intraductal Papillary Mucinous Neoplasm (IPMN) and Chronic Pancreatitis: Overlapping Pathological Entities? Two Case Reports
 CASE REPORT Intraductal Papillary Mucinous Neoplasm (IPMN) and Chronic Pancreatitis: Overlapping Pathological Entities? Two Case Reports Athanasios Petrou 1, Alexandros Papalambros 2, Nicholas Brennan
CASE REPORT Intraductal Papillary Mucinous Neoplasm (IPMN) and Chronic Pancreatitis: Overlapping Pathological Entities? Two Case Reports Athanasios Petrou 1, Alexandros Papalambros 2, Nicholas Brennan
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
X-Ray Corner. Imaging Approach to Cystic Liver Lesions. Pantongrag-Brown L. Solitary cystic liver lesions. Hepatic simple cyst (Figure 1)
 THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
THAI J 136 Imaging Approach to Cystic Liver Lesions GASTROENTEROL 2013 X-Ray Corner Imaging Approach to Cystic Liver Lesions Pantongrag-Brown L Cystic liver lesions are common findings in daily practice
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Analysis of clinical characteristics and treatment of pancreatic cystic tumors
 Original Article Analysis of clinical characteristics and treatment of pancreatic cystic tumors Lei You *, Jianchun Xiao *, Zhe Cao *, Wanying Zhang, Quan Liao, Menghua Dai, Taiping Zhang, Yupei Zhao Department
Original Article Analysis of clinical characteristics and treatment of pancreatic cystic tumors Lei You *, Jianchun Xiao *, Zhe Cao *, Wanying Zhang, Quan Liao, Menghua Dai, Taiping Zhang, Yupei Zhao Department
Large Colorectal Adenomas An Approach to Pathologic Evaluation
 Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
PersPeCTIves. Controversies in the management of pancreatic ipmn. Masao Tanaka
 PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
Clinical factors predictive of malignant and premalignant cystic neoplasms of the pancreas: a single institution experience
 664..670 DOI:10.1111/j.1477-2574.2009.00114.x HPB ORIGINAL ARTICLEhpb_114 Clinical factors predictive of malignant and premalignant cystic neoplasms of the pancreas: a single institution experience Natalie
664..670 DOI:10.1111/j.1477-2574.2009.00114.x HPB ORIGINAL ARTICLEhpb_114 Clinical factors predictive of malignant and premalignant cystic neoplasms of the pancreas: a single institution experience Natalie
Sun A Kim Eunsil Yu Song Cheol Kim 1 Jihun Kim
 The Korean Journal of Pathology 2010; 44: 410-9 DOI: 10.4132/KoreanJPathol.2010.44.4.410 Clinical Outcome of Surgically Resected Pancreatic Intraductal Papillary Mucinous Neoplasm ccording to the Marginal
The Korean Journal of Pathology 2010; 44: 410-9 DOI: 10.4132/KoreanJPathol.2010.44.4.410 Clinical Outcome of Surgically Resected Pancreatic Intraductal Papillary Mucinous Neoplasm ccording to the Marginal
PANCREATIC CYSTIC NEOPLASMS: A CASE SERIES
 ORIGINAL ARTICLE PANCREATIC CYSTIC NEOPLASMS: A CASE SERIES Murat Kılıç,1, Ahmet Erdoğan, Cengiz Ceylan, Barış Saylam and Mesut Tez Department of General Surgery, Numune Training and Research Hospital,
ORIGINAL ARTICLE PANCREATIC CYSTIC NEOPLASMS: A CASE SERIES Murat Kılıç,1, Ahmet Erdoğan, Cengiz Ceylan, Barış Saylam and Mesut Tez Department of General Surgery, Numune Training and Research Hospital,
Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens
 ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
Pancreatic Cystic Lesions 원자력병원
 Pancreatic Cystic Lesions 원자력병원 박선 후 Lines of cellular differentiation Ductal Acinar Undetermined Ductal adenocarcinoma Serous/ mucinous tumor Intraductal papillary mucinous neoplasm Acinar cell carcinoma
Pancreatic Cystic Lesions 원자력병원 박선 후 Lines of cellular differentiation Ductal Acinar Undetermined Ductal adenocarcinoma Serous/ mucinous tumor Intraductal papillary mucinous neoplasm Acinar cell carcinoma
