Serous Cystadenomas Follow a Benign and Asymptomatic Course and Do Not Present a Significant Size Change During Follow-Up
|
|
|
- Bartholomew Blake
- 5 years ago
- Views:
Transcription
1 REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed Rev Inves Clin. 2015;67:344-9 PERMANYER BRIEF COMMUNICATIONS Serous Cystadenomas Follow a Benign and Asymptomatic Course and Do Not Present a Significant Size Change During Follow-Up Mario César Pelaez-Luna 1,2, Carlos Moctezuma-Velázquez 2, Jorge Hernández-Calleros 2 and Luis Federico Uscanga-Domínguez 2 1 School of Medicine, Research Division, Universidad Nacional Autónoma de México, Mexico City; 2 Pancreas Clinic, Gastroenterology Department, Instituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán, Mexico City, Mexico ABSTRACT Background: Serous cystadenoma is a benign pancreatic cystic neoplasm. Conservative management is favored. We studied the clinical characteristics and course of serous cystadenoma in patients undergoing surgery or conservative management only at an academic referral center. Methods: Patients presenting with serous cystadenoma in the years were selected. Hospital records were evaluated for patient and serous cystadenoma characteristics. Results: A total of 22 patients with serous cystadenoma were identified. Mean age at diagnosis was 63 years and 82% were women. Diagnosis was incidental in 59%, and 18% presented with unspecific abdominal pain, 14% unexplained weight loss, 4.5% gastrointestinal obstructive symptoms, and 4.5% cholangitis. Location was pancreas body 36%, head 32%, tail 23%, and uncinate 9%. Mean serous cystadenoma diameter at diagnosis was 37 ± 23 mm. After diagnosis five patients underwent surgery. Initial size was similar between surgical and follow-up groups (p = 0.9). Four cases were lost to follow-up; 13 continued conservative management with a mean follow-up time of 54 ± 27 months. The initial and last serous cystadenoma size in the follow-up group remained similar (p = 0.9). Six cases presented significant tumor growth during follow-up (p > 0.05). All patients remained asymptomatic throughout follow-up. No malignancy or serous cystadenoma-related death occurred. Conclusions: Size change of serous cystadenoma was minimal and patients remained asymptomatic during follow-up. Surgery should be limited to symptomatic and selected cases. (REV INVES CLIN. 2015;67:344-9) Key words: Serous cystadenoma. Pancreas cyst. Pancreas neoplasm. Cystic neoplasm. Pancreas surgery. Corresponding author: *Mario Pelaez-Luna Associate Professor of Medicine, School of Medicine Research Division Universidad Nacional Autónoma de México Pancreas Clinic, Gastroenterology Department Insitituto Nacional de Ciencias Médicas y Nutrición Salvador Zubirán Vasco de Quiroga, 15 Col. Sección XVI, Del. Tlalpan, C.P Ciudad de México, México mariopl@prodigy.net.mx Received for publication: Accepted for publication:
2 Mario Pelaez-Luna, et al.: SEROUS CYSTADENOMAS MINIMAL GROWTH INTRODUCTION Serous cystadenoma (SCA) represents 1-2% of all pancreatic exocrine tumors, usually present in subjects over 60 years old and slightly more frequent in women. It is the third to fourth most common cystic pancreatic neoplasm 1,2. It tends to follow a benign course, amenable to conservative treatment unless symptoms or rapid growth develop 3-5. Serous cystadenomas are usually incidental findings; some patients present with unspecific abdominal pain, unexplained weight loss, or symptoms of compression to adjacent organs. Some groups recommend an expectant management in all asymptomatic SCA, with the exception of those measuring 4 cm that bear an increased risk of rapid growth in which surgical treatment, even in asymptomatic patients, should be considered 6. Although mortality from pancreatic resections has significantly decreased and outcomes are acceptable in high-volume centers 7-9, operating on SCA before they become large aims to avoid the increased technical difficulty and morbidity inherent in resection procedures for big masses 10,11. Also, the type of resection carries different risks and morbidities and should be taken into consideration when management is decided. An analysis of 219 SCA cases reported a steady and slow growth rate regardless of the initial size, suggesting that resection should be considered only when there are symptoms present or if the tumor size doubles in less than 12 years 12. We aimed to analyze clinical characteristics and course of SCA at an academic referral center. MATERIAL AND METHODS We identified patients presenting with SCA between 2000 and 2013 by reviewing institutional charts as well as surgical and pathology logs. Using a questionnaire designed for a multinational study on SCA sponsored by the International Association of Pancreatology and the European Pancreatic Club (some cases presented in this manuscript were included in that study) 13, we retrospectively collected demographic (gender, age, diagnosis date, last follow-up date, fatalities), clinical (cyst-related symptoms, circumstances of discovery), imaging (computed tomography [CT], magnetic resonance imaging [MRI], endoscopic ultrasound [EUS]) findings, cyst characteristics (microcystic, macrocystic, mixed type, size, location in the pancreas, relationship with the pancreatic and bile ducts, contents, wall characteristics), fine needle aspiration and cyst fluid analysis at the moment of diagnosis and last follow-up as well as surgical (indications, findings, type of resection) and pathology data (gross and microscopic description). Serous cystadenoma diagnosis was based on typical imaging characteristics (honeycomb pattern, multicystic lesion, central scar, no communication with main pancreatic duct) by either cross-sectional studies and/or EUS with or without cyst fluid analysis), and pathology reports in those resected specimens. Cyst fluid content typical of SCA included bland cytology, no or scant mucin on periodic acid-schiff (PAS) staining, amylase < 200 mg/dl, carcinoembryonic antigen (CEA) < 5 mg/dl Serous cystadenoma size at diagnosis and during followup was calculated using the maximum tumor diameter from cross-sectional (CT, MRI) and/or EUS imaging. Statistical analysis Continuous variables are presented as mean ± standard deviation (SD) and qualitative variables as frequencies. Data comparisons were performed using X 2, Fisher exact test, Student s t test or Mann-Whitney test, accordingly. A p value < 0.05 was considered significant. All analyses were performed using SPSS V 22 (SPSS for Mac; IBM, Chicago, Illinois, USA). RESULTS We included 22 patients; mean age at diagnosis was 63 ± 14.5 SD years, and 18 (82%) were women. The SCA radiology appearance and pancreas location are shown in table 1. Serous cystadenoma was diagnosed during evaluation of unspecific abdominal pain (4, 18%), unexplained weight loss (3, 14%), gastrointestinal obstructive symptoms (1, 4.5%), cholangitis (1, 4.5%), and incidentally in 13 (59%) cases. 345
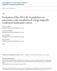
3 REV INVES CLIN. 2015;67:344-9 Table 1. Demographic, clinical and imaging characteristics Variable n (%) Gender (male:female) 4 (18) : 18 (82) Age at diagnosis (years)* 63.0 ± 14.5 SCA type Microcystic 12 (55) Macrocystic 2 (9) Mixed 8 (36) Solid 0 Location Uncinate 2 (9) Head 7 (32) Body 8 (36) Tail 5 (23) Overall size at diagnosis* 37 ± 23 mm *Mean (standard deviation). SCA: serous cystadenoma. Serous cystadenoma mean size at diagnosis was 37 ± 23 mm. Five cases underwent surgical resection (distal pancreatectomy) at the time of presentation; indications for resection were: symptoms (pain, mass effect in 3, 14%), indeterminate diagnosis (1, 4.5%), and uncertainty of malignancy (1, 4.5%). Initial tumor size was similar between surgical and non-surgical groups (39 ± 17 vs. 37 ± 27 mm, respectively; p = 0.9). Four cases were lost to follow-up and 13 continued conservative management; mean followup time was 54 ± 27 months. Overall, in the 13 nonsurgical cases, initial SCA size remained similar when compared to the last follow-up size (29 ± 17 vs. 33 ± 18 mm SD; p = 0.9). Only 6/13 (46%) cases presented significant growth during follow-up; the initial size was 25 ± 11 mm SD vs. final follow-up size 36 ± 14 mm SD (p < 0.05) (Fig. 1). All patients remained asymptomatic at the last visit. Neither malignant transformation nor SCA-related deaths were registered. DISCUSSION Since first described in , SCA has been considered a benign tumor. Most are incidentally found and remain asymptomatic during long periods of time regardless of their size. Conservative management has Figure 1. Data from the 6 patients that presented serous cystadenoma during follow-up. SCA size (cm) SCA size increments during follow-up Follow-up (years) SCA: serous cystadenoma. been widely advised, with surgery being considered only for symptomatic cases 6,16,17. Differential diagnosis includes potentially malignant cystic lesions (e.g., mucinous cystadenoma, pancreatic intraductal papillary mucinous neoplasm, etc.). An accurate diagnosis is essential since management and prognosis differ according to the type of neoplasm 15, Definitive diagnosis of SCA is achieved based on surgical pathology of resected specimens. However, presurgical diagnosis can be made when classic imaging features are present 22, except in those rare SCA variants In these cases, analysis of the cyst s contents can yield relevant diagnostic information. Once a SCA is diagnosed, whether to follow-up or perform a surgical resection, especially in asymptomatic cases, remains under discussion. Two of the largest series reported similar results regarding the clinical presentation, but disagreed on when to consider surgery in asymptomatic cases 6,12. One of them analyzed serial radiographic records in 24 patients. The overall median growth rate was 6 mm per year, but a significant difference in growth rate was noted in nine cases presenting with tumors 4 cm, having a growth rate 346
4 Mario Pelaez-Luna, et al.: SEROUS CYSTADENOMAS MINIMAL GROWTH of nearly 20 mm per year and a doubling-size time of 0.64 years, compared with 2.84 years for SCA < 4 cm 6. It is not clear whether SCA growth was associated with symptom onset; however, in this series, SCA 4 cm had a threefold risk of developing symptoms. Another series 12 followed 194 SCA for a median time of 3.2 years; only five patients underwent resection during follow-up (median size: 3.5 cm; range: ). Indications for surgery were symptoms development (n = 2), accelerated growth or mass effect (n = 2), or increased cyst fluid CEA in one case. It seems that with the exception of the last case, in the remaining four, symptoms and not tumor size were responsible for indicating surgery. The authors, instead of proposing a specific cut-off cyst size to consider surgery, advise to perform surgery if the size doubles in less than 12 years. Our study replicates most clinical and imaging characteristics from prior SCA series, including the most frequent variant (microcystic); however, the second most common variant was the mixed one (36%) compared to other series in which the macrocystic subtype was the second most frequent It is uncertain if this could be related to ethnicity or other undetermined factors. Three out of five of our surgical cases were symptomatic, and interestingly, in all of them the tumor measured < 4 cm. Although our findings are limited by the small sample size, the follow-up time is slightly longer (five years) than previous reports and confirm that SCA has a minimal or non-significant size increment, with most patients remaining asymptomatic regardless of location and size (from 13 cases in follow-up, seven remained unchanged and six presented a mean 10 mm increment regardless of the initial size). After serial CT imaging review of the six cases with increased size, four patients had four studies, one had three, and one had two. However, the small sample prevented us from performing a proper growth rate arithmetic calculation, limiting our analysis to report only changes in size during follow-up. Considering a linear growth, the annual growth rate can be calculated by obtaining the cyst s difference in size by subtracting the initial size from the size on the last imaging, and then dividing it by the number of years of follow-up for each of the six cases in which the tumor grew and then obtaining the overall arithmetic mean value of growth from all of the six cases. It is important to note that the mathematical model used and its validity will always limit growth rate assessments. Despite the limitations of our calculations that assume a linear rather than a curvilinear growth that could better resemble reality, this exercise (data not shown) yielded an overall growth rate of about 2 mm per year, with tumors < 4 cm growing slower (1.6 mm per year). These rates are similar to previous reports that estimated a 1.2 mm increase per year for small lesions 12,13. Interestingly, one case with a tumor measuring 8 cm has remained stable, and another with a 4 cm lesion grew 24 mm in seven years, with both patients being asymptomatic. Thus, a cyst size of 4 cm did not represent a risk of increased growth or symptom development (observation from two cases with a short follow-up). The lack of symptoms in patients even with big cysts could be the result of a slow tumor growth rate allowing the body to adapt. On the other hand, rapid growth rates could be responsible for a mass effect and secondary symptoms. It is unclear which factors other than size determine the growth rate as well as the presence of symptoms. Serous cystadenoma shows a low rate ( %) of malignancy regardless of the presence of symptoms and size 3-5,13. None of the patients in our series presented malignant transformation of the tumor. Considering that a detailed imaging and evaluation of the cyst s content can lead to an accurate diagnosis of SCA 29, the low or null rate of malignancy, that not every cyst 4 cm shows a rapid growth rate, and that large cysts are not always symptomatic, it seems reasonable and safe that asymptomatic SCA be observed. Periodical evaluation with serial CT imaging (every six months during the first two years and then annually as proposed by some groups) 6,28 appears to be sufficient and safe. The follow-up strategy remains under debate and amenable to consensus. 347
5 REV INVES CLIN. 2015;67:344-9 However, if we were to consider symptoms as the single factor to consider surgery, then serial imaging aiming to select potential surgical candidates ( 4 cm), and to assess stability or growth rate might be unnecessary, and control imaging should be considered only when patients become symptomatic. For such approach a 100% certainty in diagnosis is mandatory. The study with the largest number of SCA with a followup of three years 13 found that relevant clinical symptoms occurred in a very small proportion of patients, with tumor size slowly increasing in less than half. They advocate an initial conservative management in the majority of patients, and surgery should be proposed only for uncertain diagnosis after a complete workup, with the presence of significant and cyst-related symptoms, or when malignancy is a concern. A conservative and symptom-based strategy is supported by the fact that about 11% of cases become symptomatic during follow-up, regardless of cyst size 13. However, significant difficulties in management could present in those initially asymptomatic cases with a large SCA that may be fit for surgery and years later become symptomatic, at an age in which surgery might not be feasible anymore. Development in EUS therapeutics, such as EUS-guided ablation (using ethanol or other ablative agents), offers an alternative for cases with potentially malignant or malignant cysts not fit for surgery. This technique has proved to be safe, effective, and minimally invasive for the treatment of pancreatic cysts. Much of the information comes from clinical trials and case series that included mainly mucinous lesions, with information on SCA being extremely limited 30. Serous cystadenoma may represent a challenge or limitation to this approach since the greatest chance of successful ablation is in unilocular or oligolocular cysts (fewer than 2 or 3 locules). The multiple, small locules that characterize SCA would represent a greater number of needle passes, increasing the procedure risks. Data on a large SCA sample is still needed, which leaves this approach in this subset of patients to be performed only as part of research clinical trials. We consider that a precise SCA diagnosis is mandatory. Once diagnosis is certain, an initial conservative management is possible, and cyst-related symptoms could guide the treatment strategy. Surgery should be reserved for symptomatic cases and not recommended based on tumor size or doubling-size time. The surveillance strategy remains under debate and, along with surgical decisions, should be individualized. In conclusion, change in SCA size was minimal and patients remained asymptomatic during follow-up. No malignant transformation or cyst-related fatalities were observed. REFERENCES 1. Sahani DV, Dadavigere R, Saokar A, et al. Cystic pancreatic lesions: a simple imaging based classification system for guiding management. Radiographics. 2005;25: Valsangkar NP, Morales-Oyarvide V, Thayer SP, et al. 851 resected cystic tumors of the pancreas: A 33-year experience at the Massachusetts General Hospital. Surgery. 2012;152:s Abe H, Kubota K, Mori M, et al. Serous cystadenoma of the pancreas with invasive growth: benign or malignant? Am J Gastroenterol. 1998;93: Strobel O, Z graggen K, Schmitz-Winnenthal FH, et al. Risk of malignancy in serous cystic neoplasms of the pancreas. Digestion. 2003;68: Yoshimi N, Sugie S, Tanaka T, et al. A rare case of serous cystadenocarcinoma of the pancreas. Cancer. 1992;69: Tseng JF, Warshaw AL, Sahani DV, Lauwers GY, Rattner DW, Fernandez del Castillo C. Serous cystadenoma of the pancreas: tumor growth rates and recommendations for treatment. Ann Surg. 2005;31: Finks JF, Osborne NH, Birkmeyer JD. Trends in hospital volume and operative mortality for high risk surgery. N Eng J Med. 2011;364: Schmidt CM, Turrini O, Parikh P, et al. Effect of hospital volume, surgeon experience and surgeon volume on patient outcomes after pancreaticoduodenectomy: a single institution experience. Arch Surg. 2010;145: van der Gaag NA, Berkhemer OA, Sprangers MA, et al. Quality of life and functional outcome after resection of pancreatic cystic neoplasms. Pancreas. 2014;43: Bhayani NH, Enomoto LM, James BC, et al. Multivisceral and extended resections during pancreatoduodenectomy increase morbidity and mortality. Surgery. 2014;155: Sikkens EC, Cahen DL, de Witt J, Looman CW, van Eijck C, Bruno MJ. Prospective assessment of the influence of pancreatic cancer resection on exocrine pancreatic function. Br J Surg. 2014;101: El-Hayek KM, Brown N, O Rourke C, Falk G, Morris-Stiff G, Walsh M. Rate of growth of pancreatic serous cystadenoma as an indication for resection. Surgery. 2013;154: Jais B, Rebours V, Malleo G, et al. Serous cystic neoplasm of the pancreas: a multinational study of 2622 patients under the auspices of the International Association of Pancreatology and European Pancreatic Club (European Study Group on Cystic Tumors of the Pancreas). Gut. 2016;65: van der Waaij LA, Van Dullemen HM, Porte RJ. Cyst fluid analysis in the differential diagnosis of pancreatic cystic lesions: a pooled analysis. Gastrointest Endosc. 2005;62: Compagno J, Oertel JE. Microcystic adenomas of the pancreas (glycogen-rich cystadenomas): a clinicopathologic study of 34 cases. Am J Clin Pathol. 1978;69: Brugge WR, Lauwers GY, Sahani D, Fernandez-del Castillo C, Warshaw AL. Cystic neoplasms of the pancreas. N Eng J Med. 2004;351: Sheehan MK, Beck K, Pickleman J, Aranha GV. Spectrum of cystic neoplasms of the pancreas and their surgical management. Arch Surg. 2003;138:
6 Mario Pelaez-Luna, et al.: SEROUS CYSTADENOMAS MINIMAL GROWTH 18. Chen F, Liang Jy, Zhao QY, et al. Differentiation of branch duct intraductal papillary mucinous neoplasms from serous cystadenomas of the pancreas using contrast-enhanced sonography. J Ultrasound Med. 2014;33: Belsley NA, Pitman MB, Lauwers GY, Brugge WR, Deshpande V. Serous cystadenoma of the pancreas: limitations and pitfalls of endoscopic ultrasound guided fine needle aspiration biopsy. Cancer. 2008;114: Salomao M, Remotti H, Allendorf JD, et al. Fine needle aspirations of pancreatic serous cystadenomas: Improving diagnostic yield with cell blocks and a-inhibin immunohistochemistry. Cancer Cytopathol. 2014;122: Pelaez-Luna M, Chari ST. Cyst fluid analysis to diagnose pancreatic cystic lesions: an as yet unfulfilled promise. Gastroenterology. 2006;130: Chu LC, Singhi AD, Hruban RH, Fishman EK. Characterization of pancreatic serous cystadenoma on dual phase multidetector computed tomography. J Comput Assist Tomogr. 2014;38: Kishida Y, Matsubayashi H, Okamura Y, et al. A case of solid type serous cystadenoma mimicking neuroendocrine tumor of the pancreas. J Dig Dis. 2014;15: Sakorafas GH, Smyrniotis V, Reid-Lombardo KM, Sarr MG. Primary pancreatic cystic neoplasms revisited. Part I: serous cystic neoplasms. Surg Oncol. 2011;21: Leite I, Palmerio M, Farchione A, et al. Unilocular macrocystic serous cystadenoma of the pancreas atypical features: a case report. Clin Imaging. 2014;38: Khashab MA, Shin EJ, Amateau S, et al. Tumor size and location correlate with behavior of pancreatic serous cystic neoplasms. Am J Gastroenterol. 2011;106: Kimura W, Moriya T, Hirai I, et al. Multicenter study of serous cystic neoplasm of the Japan pancreas society. Pancreas. 2012; 41: Galanis C, Zamani A, Cameron JL, et al. Resected serous cystic neoplasms of the pancreas: a review of 158 patients with recommendations for treatment. J Gastrointest Surg. 2007; 11: Bose D, Tam E, Liu J, et al. Multidisciplinary management strategy for incidental cystic lesions of the pancreas. J Am Coll Surg. 2010;211: Oh HC, Brugge WR. EUS guided pancreatic cyst ablation: A critical review (with video) Gastrointest Endosc. 2013;77:
Pancreatic Cysts. Darius C. Desai, MD FACS St. Luke s University Health Network
 Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:813 817 Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts MAOR LAHAV, YAKOV MAOR, BENJAMIN AVIDAN, BEN NOVIS, and SIMON BAR MEIR Department
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:813 817 Nonsurgical Management of Asymptomatic Incidental Pancreatic Cysts MAOR LAHAV, YAKOV MAOR, BENJAMIN AVIDAN, BEN NOVIS, and SIMON BAR MEIR Department
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Cystic Pancreatic Lesions: Approach to Diagnosis
 Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
Cystic Pancreatic Lesions: Approach to Diagnosis Poster No.: R-0130 Congress: RANZCR-AOCR 2012 Type: Educational Exhibit Authors: A. AGARWAL, R. M. Mendelson; Perth/AU Keywords: Cysts, Biopsy, Endoscopy,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble?
 Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Types of IPMN. Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy. Cysts: Early Neoplasia. Mucinous Cystic Lesions. EUS-guided FNA EUS
 Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Pancreas Cysts: An Incidental Finding or Harbinger of Malignancy EUS-guided FNA William R. Brugge,, MD, FACG Professor of Medicine Harvard Medical School Director, GI Endoscopy Unit Massachusetts General
Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas
 HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
HPB Surgery Volume 2015, Article ID 791704, 7 pages http://dx.doi.org/10.1155/2015/791704 Research Article The Changing Spectrum of Surgically Treated Cystic Neoplasms of the Pancreas Jennifer K. Plichta,
Matthew McCollough, M.D. April 9, 2009 University of Louisville
 Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Patient History. A 58 year old man presents with a 16 mm cyst in the pancreatic tail. The cyst is unilocular with a thick wall and no mural nodule.
 Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
Case 1 Martha Bishop Pitman, MD Director of Cytopathology Massachusetts General Hospital Associate Professor of Pathology Harvard Medical School Boston, MA Patient History A 58 year old man presents with
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms
 The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
The role of endoscopy in the diagnosis and treatment of cystic pancreatic neoplasms CYSTIC LESIONS AND FLUID COLLECTIONS OF THE PANCREAS Their pathology ranges from pseudocysts and pancreatic necrosis
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
An Approach to Pancreatic Cysts. Introduction
 An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
An Approach to Pancreatic Cysts Nalini M. Guda, MD Aurora St. Luke s Medical Center, Milwaukee Clinical Adjunct Professor of Medicine, University of Wisconsin School of Medicine and Public Health Introduction
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Patient with incidental pancreatic cyst
 Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
Clinical problem Diego Aponte M, MD 1 1 Internal Medicine Gastroenterology Specialist. Gastroenterology Academic Coordinator for Graduate Level. Fundación Sanitas. Bogotá, Colombia.... Received: 07-09-10
Cystic pancreatic lesions A proposal for a network approach. Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth
 Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
Cystic pancreatic lesions A proposal for a network approach Chris Briggs Consultant HPB Surgeon Peninsula HPB Unit Derriford Hospital, Plymouth Aims Brief overview of cystic pancreatic lesions International
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms
 JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
JOP. J Pancreas (Online) 20 Mar 20; (2):-9. RESEARCH ARTICLE The Role of Molecular Analysis in the Diagnosis and Surveillance of Pancreatic Cystic Neoplasms Megan Winner, Amrita Sethi 2, John M Poneros
Surgical management and results for cystic neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Korean J Hepatobiliary Pancreat Surg 2013;17:118-125 Original Article Surgical management and results for cystic neoplasms of pancreas Kyung Won Han 1, Ryun Ha 1, Kun Kuk Kim 1, Jung Nam Lee 1, Yeon Suk
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget
 Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Evaluation and Management of Cystic Lesions of the Pancreas: When to Resect, When to Follow and When to Forget Randall Brand, MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition
Jefferson Digital Commons. Thomas Jefferson University. Charles Galanis The Johns Hopkins Medical Institutions
 Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery July 2007 Resected serous cystic neoplasms of the pancreas: Locally aggressive behavior
Thomas Jefferson University Jefferson Digital Commons Department of Surgery Faculty Papers Department of Surgery July 2007 Resected serous cystic neoplasms of the pancreas: Locally aggressive behavior
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period
 Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Cystic Lesions of the Pancreas: Changes in the Presentation and Management of 1,424 Patients at a Single Institution over a 15-Year Time Period Sébastien Gaujoux, MD, PhD, Murray F Brennan, MD, FACS, Mithat
Cystic neuroendocrine tumor in the pancreas detected by endoscopic ultrasound and fine-needle aspiration: a case report.
 Cystic neuroendocrine tumor in the pancreas detected by endoscopic ultrasound and fine-needle aspiration: a case report. Thorlacius, Henrik; Kalaitzakis, Evangelos; Wurm Johansson, Gabriele; Ljungberg,
Cystic neuroendocrine tumor in the pancreas detected by endoscopic ultrasound and fine-needle aspiration: a case report. Thorlacius, Henrik; Kalaitzakis, Evangelos; Wurm Johansson, Gabriele; Ljungberg,
Case 1. Case 1: EUS Report 5/1/2017. Interesting Cases of Pancreatic Masses
 Interesting Cases of Pancreatic Masses Martha Bishop Pitman, MD Professor of Pathology Harvard Medical School Director of Cytopathology Massachusetts General Hospital Boston, MA MASSACHUSETTS GENERAL PHYSICIANS
Interesting Cases of Pancreatic Masses Martha Bishop Pitman, MD Professor of Pathology Harvard Medical School Director of Cytopathology Massachusetts General Hospital Boston, MA MASSACHUSETTS GENERAL PHYSICIANS
A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients
 LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
LETTER TO THE EDITOR A Selective Approach to Resection of Cystic Lesions of the Pancreas: Results From 539 Consecutive Patients To the Editor: I would like to congratulate Dr. Allen and colleagues for
Relative Accuracy of CT and MRI for Characterization of Cystic Pancreatic Masses
 Katz et al. Characterization of Cystic Pancreatic Masses Abdominal Imaging Commentary 09_07_2772_KatzCommentary.fm 7/27/07 Douglas S. Katz 1 David M. Friedel 2 David Kho 1 Nicholas Georgiou 1 John J. Hines
Katz et al. Characterization of Cystic Pancreatic Masses Abdominal Imaging Commentary 09_07_2772_KatzCommentary.fm 7/27/07 Douglas S. Katz 1 David M. Friedel 2 David Kho 1 Nicholas Georgiou 1 John J. Hines
X-ray Corner. Imaging of The Pancreas. Pantongrag-Brown L
 X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
X-ray Corner 125 Imaging of The Pancreas Modern imaging modalities commonly used in pancreas include ultrasound (US), CT, and MRI. Pancreas is a retroperitoneal organ which makes it difficult to visualize
A pancreatic intraductal papillary mucinous neoplasm: A case report and literature review
 Case report A pancreatic intraductal papillary mucinous neoplasm: A case report and literature review Martín A. Gómez Z., MD, 1 Cristian Melgar, MD, 2 Germán Junca, MD. 3 1 Gastroenterology Professor,
Case report A pancreatic intraductal papillary mucinous neoplasm: A case report and literature review Martín A. Gómez Z., MD, 1 Cristian Melgar, MD, 2 Germán Junca, MD. 3 1 Gastroenterology Professor,
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS
 Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Pancreatic Cystic Neoplasms: Guidelines and beyond
 Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Pancreatic Cystic Neoplasms: Guidelines and beyond Kenneth J. Chang, MD, FACG, FASGE Executive Director, Comprehensive Digestive Disease Center Professor and Chief, Gastroenterology Vincent & Anna Kong
Introduction E389. Background and study aims Guidelines for management
 Impact of endoscopic ultrasound on diagnosis and management of presumed mucinous neoplasms when done for pancreatic cyst morphology change on non-invasive surveillance imaging Authors Kamraan Madhani 1,
Impact of endoscopic ultrasound on diagnosis and management of presumed mucinous neoplasms when done for pancreatic cyst morphology change on non-invasive surveillance imaging Authors Kamraan Madhani 1,
Decrease in the Prevalence of Pancreatitis Associated with Primary Hyperparathyroidism: Experience at a Tertiary Referral Center
 REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com PERMANYER Rev Inves Clin. 2015;67:177-81 ORIGINAL ARTICLE Decrease in the Prevalence of Pancreatitis
REVISTA DE INVESTIGACIÓN CLÍNICA Contents available at PubMed www.clinicalandtranslationalinvestigation.com PERMANYER Rev Inves Clin. 2015;67:177-81 ORIGINAL ARTICLE Decrease in the Prevalence of Pancreatitis
Gastric outlet obstruction secondary to solid-pseudopapillary neoplasm of the pancreas in an eight year old child.
 Bidassek et al. Diagnostic Pathology (2016) 11:7 DOI 10.1186/s13000-016-0465-7 CASE REPORT Open Access Gastric outlet obstruction secondary to solid-pseudopapillary neoplasm of the pancreas in an eight
Bidassek et al. Diagnostic Pathology (2016) 11:7 DOI 10.1186/s13000-016-0465-7 CASE REPORT Open Access Gastric outlet obstruction secondary to solid-pseudopapillary neoplasm of the pancreas in an eight
PersPeCTIves. Controversies in the management of pancreatic ipmn. Masao Tanaka
 PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas
 Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
Pancreatic Cystic Neoplasms: Predictors of Malignant Behavior and Management
 Original Article Pancreatic Cystic Neoplasms: Predictors of Malignant Behavior and Management Ehab Atef, Ayman El Nakeeb, Ehab El Hanafy, Mohamed El Hemaly, Emad Hamdy, Ahmed El Geidie Surgical Center,
Original Article Pancreatic Cystic Neoplasms: Predictors of Malignant Behavior and Management Ehab Atef, Ayman El Nakeeb, Ehab El Hanafy, Mohamed El Hemaly, Emad Hamdy, Ahmed El Geidie Surgical Center,
Management of serous cystic neoplasms of the pancreas
 Management of serous cystic neoplasms of the pancreas Expert Rev. Gastroenterol. Hepatol. Early online, 1 11 (2014) Filippo Antonini* 1, Lorenzo Fuccio 2, Carlo Fabbri 3, Giampiero Macarri 1 and Laurent
Management of serous cystic neoplasms of the pancreas Expert Rev. Gastroenterol. Hepatol. Early online, 1 11 (2014) Filippo Antonini* 1, Lorenzo Fuccio 2, Carlo Fabbri 3, Giampiero Macarri 1 and Laurent
Neoplasias Quisticas del Páncreas
 SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
Differential Expression of GNAS and KRAS Mutations in Pancreatic Cysts
 ORIGINAL ARTICLE Differential Expression of GNAS and KRAS Mutations in Pancreatic Cysts Linda S Lee 1, Leona A Doyle 2, Jeffrey Houghton 3, Sachin Sah 3, Andrew M Bellizzi 4, Anna E Szafranska-Schwarzbach
ORIGINAL ARTICLE Differential Expression of GNAS and KRAS Mutations in Pancreatic Cysts Linda S Lee 1, Leona A Doyle 2, Jeffrey Houghton 3, Sachin Sah 3, Andrew M Bellizzi 4, Anna E Szafranska-Schwarzbach
3/28/2012. Periampullary Tumors. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Eric K. Nakakura Ko Olina, HI
 Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Overview Postgraduate Course in General Surgery Case presentation Differential diagnosis Diagnosis and therapy Outcomes Principles of palliative care Eric K. Nakakura Ko Olina, HI March 27, 2012 CASE 1:
Contrast-Enhanced Ultrasonograpic Findings in Pancreatic Tumors
 Int. J. Med. Sci. 2008, 5 203 Short Research Communication International Journal of Medical Sciences ISSN 1449-1907 www.medsci.org 2008 5(4):203-208 Ivyspring International Publisher. All rights reserved
Int. J. Med. Sci. 2008, 5 203 Short Research Communication International Journal of Medical Sciences ISSN 1449-1907 www.medsci.org 2008 5(4):203-208 Ivyspring International Publisher. All rights reserved
Case report. Open Access. Abstract
 Open Access Case report Laparoscopic resection of a pancreatic serous cystadenoma preserving the integrity of main pancreatic duct: a case report Michail Pitiakoudis 1, Petros Zezos 2 *, Anastasia Oikonomou
Open Access Case report Laparoscopic resection of a pancreatic serous cystadenoma preserving the integrity of main pancreatic duct: a case report Michail Pitiakoudis 1, Petros Zezos 2 *, Anastasia Oikonomou
Intraductal Papillary Mucinous Neoplasms: The Bologna Experience
 ORIGINAL ARTICLE INTRADUCTAL PAPILLARY MUCINOUS NEOPLASM Intraductal Papillary Mucinous Neoplasms: The Bologna Experience Riccardo Casadei 1, Carlo Alberto Pacilio 1, Claudio Ricci 1, Giovanni Taffurelli
ORIGINAL ARTICLE INTRADUCTAL PAPILLARY MUCINOUS NEOPLASM Intraductal Papillary Mucinous Neoplasms: The Bologna Experience Riccardo Casadei 1, Carlo Alberto Pacilio 1, Claudio Ricci 1, Giovanni Taffurelli
Unusual case of a giant serous oligocystic adenoma with communication to main pancreatic duct
 Ruquaya Mir 57 CASE REPORT OPEN ACCESS Unusual case of a giant serous oligocystic adenoma with communication to main pancreatic duct Ruquaya Mir, Vikram Pratap Singh ABSTRACT Benign serous cystic tumors
Ruquaya Mir 57 CASE REPORT OPEN ACCESS Unusual case of a giant serous oligocystic adenoma with communication to main pancreatic duct Ruquaya Mir, Vikram Pratap Singh ABSTRACT Benign serous cystic tumors
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes
 Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
Suspicious Cytologic Diagnostic Category in Endoscopic Ultrasound-Guided FNA of the Pancreas: Follow-Up and Outcomes Evan A. Alston, MD 1 ; Sejong Bae, PhD 2 ; and Isam A. Eltoum, MD, MBA 1 BACKGROUND:
ORIGINAL ARTICLE. The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic
 ORIGINAL ARTICLE The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic Cystic Lesions Pinhas P. Schachter, MD; Yona Avni, MD; Gabriela Gvirtz, MD; Ada Rosen, MD; Abraham
ORIGINAL ARTICLE The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic Cystic Lesions Pinhas P. Schachter, MD; Yona Avni, MD; Gabriela Gvirtz, MD; Ada Rosen, MD; Abraham
PAPER. Experience With 208 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas
 PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
Analysis of clinical characteristics and treatment of pancreatic cystic tumors
 Original Article Analysis of clinical characteristics and treatment of pancreatic cystic tumors Lei You *, Jianchun Xiao *, Zhe Cao *, Wanying Zhang, Quan Liao, Menghua Dai, Taiping Zhang, Yupei Zhao Department
Original Article Analysis of clinical characteristics and treatment of pancreatic cystic tumors Lei You *, Jianchun Xiao *, Zhe Cao *, Wanying Zhang, Quan Liao, Menghua Dai, Taiping Zhang, Yupei Zhao Department
Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Report of a case of pancreatic hemangioma: A difficult preoperative diagnosis AL Hashmi Al Warith, Lagrange Xavier, Fara Régis, Camerlo Antoine
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:974 979 Endoscopic Ultrasound Guided Trucut Biopsy of the Cyst Wall for Diagnosing Cystic Pancreatic Tumors MICHAEL J. LEVY,* THOMAS C. SMYRK, RAGHURAM P.
Cystic lesions of the pancreas
 REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 155-161 Cystic lesions of the pancreas Ioannis Karoumpalis a, Dimitrios K. Christodoulou b General Hospital of Athens G. Gennimatas, Athens; University
REVIEW ARTICLE Annals of Gastroenterology (2016) 29, 155-161 Cystic lesions of the pancreas Ioannis Karoumpalis a, Dimitrios K. Christodoulou b General Hospital of Athens G. Gennimatas, Athens; University
Endoscopic Ultrasonography Clinical Impact. Giancarlo Caletti. Gastroenterologia Università di Bologna. Caletti
 Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Clinical Impact Giancarlo Gastroenterologia Università di Bologna AUSL di Imola,, Castel S. Pietro Terme (BO) 1982 Indications Diagnosis of Submucosal Tumors (SMT) Staging of Neoplasms Evaluation of Pancreato-Biliary
Select problems in cystic pancreatic lesions
 Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms
 HPB, 2008; 10: 483490 ORIGINAL ARTICLE Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms WILLIAM E. FISHER a, SALLY E. HODGES a, VIVEK YAGNIK b, FANNIE E. MORÓN b, MENG-FEN
HPB, 2008; 10: 483490 ORIGINAL ARTICLE Accuracy of CT in predicting malignant potential of cystic pancreatic neoplasms WILLIAM E. FISHER a, SALLY E. HODGES a, VIVEK YAGNIK b, FANNIE E. MORÓN b, MENG-FEN
Evaluation of the 2015 AGA guidelines on pancreatic cystic neoplasms in a large surgically confirmed multicenter cohort
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Evaluation of the 2015 AGA guidelines on pancreatic cystic neoplasms in a large surgically confirmed multicenter
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 Evaluation of the 2015 AGA guidelines on pancreatic cystic neoplasms in a large surgically confirmed multicenter
High Prevalence of Pancreatic Cysts Detected by Screening Magnetic Resonance Imaging Examinations
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:806 811 High Prevalence of Pancreatic Cysts Detected by Screening Magnetic Resonance Imaging Examinations KOEN DE JONG,* C. YUNG NIO, JOHN J. HERMANS, MARCEL
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:806 811 High Prevalence of Pancreatic Cysts Detected by Screening Magnetic Resonance Imaging Examinations KOEN DE JONG,* C. YUNG NIO, JOHN J. HERMANS, MARCEL
Morphologic features in cystic lesions of pancreas-a retrospective analysis
 International Journal of Advances in Medicine Cicy PJ et al. Int J Adv Med. 2018 Feb;5(1):192-196 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180083
International Journal of Advances in Medicine Cicy PJ et al. Int J Adv Med. 2018 Feb;5(1):192-196 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20180083
Case Report Solid Serous Adenoma of the Pancreas: A Case Report and Review of the Literature
 Case Reports in Surgery Volume 2016, Article ID 3730249, 5 pages http://dx.doi.org/10.1155/2016/3730249 Case Report Solid Serous Adenoma of the Pancreas: A Case Report and Review of the Literature Anastasios
Case Reports in Surgery Volume 2016, Article ID 3730249, 5 pages http://dx.doi.org/10.1155/2016/3730249 Case Report Solid Serous Adenoma of the Pancreas: A Case Report and Review of the Literature Anastasios
Diagnosis and Management of Cystic Pancreatic Lesions
 Gastrointestinal Imaging Best Practices/Review Sahani et al. Cystic Pancreatic Lesions Gastrointestinal Imaging Best Practices/Review Dushyant V. Sahani 1 Avinash Kambadakone 1 Michael Macari 2 Noaki Takahashi
Gastrointestinal Imaging Best Practices/Review Sahani et al. Cystic Pancreatic Lesions Gastrointestinal Imaging Best Practices/Review Dushyant V. Sahani 1 Avinash Kambadakone 1 Michael Macari 2 Noaki Takahashi
Original Article INTRODUCTION
 Original Article DOI: 10.3348/kjr.2011.12.2.187 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(2):187-195 Differentiating Pancreatic Ductal Adenocarcinoma from Pancreatic Serous Cystadenoma, Mucinous
Original Article DOI: 10.3348/kjr.2011.12.2.187 pissn 1229-6929 eissn 2005-8330 Korean J Radiol 2011;12(2):187-195 Differentiating Pancreatic Ductal Adenocarcinoma from Pancreatic Serous Cystadenoma, Mucinous
Giant pancreatic mucinous cystadenoma with malignant transformation
 Case Report Brunei Int Med J. 2014; 10 (3): 177-182 Giant pancreatic mucinous cystadenoma with malignant transformation Jerica CHAI 1, Vui Heng CHONG 2, Ian BICKLE 1 1 Department of Radiology and 2 Department
Case Report Brunei Int Med J. 2014; 10 (3): 177-182 Giant pancreatic mucinous cystadenoma with malignant transformation Jerica CHAI 1, Vui Heng CHONG 2, Ian BICKLE 1 1 Department of Radiology and 2 Department
ORIGINAL ARTICLE. Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm
 ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
Kenneth D. Chi, MD Medical Director GI Lab Advocate Lutheran General Hospital
 Kenneth D. Chi, MD Medical Director GI Lab Advocate Lutheran General Hospital Advances in Digestive Health for the Primary Care Physician Symposium May 2, 2015 None Case Presentation Types of Pancreatic
Kenneth D. Chi, MD Medical Director GI Lab Advocate Lutheran General Hospital Advances in Digestive Health for the Primary Care Physician Symposium May 2, 2015 None Case Presentation Types of Pancreatic
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics
 Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Mucin-Producing Neoplasms of the Pancreas: An Analysis of Distinguishing Clinical and Epidemiologic Characteristics The Harvard community has made this article openly available. Please share how this access
Characterization of Malignant Pancreatic Cystic Lesions in the Background of Chronic Pancreatitis
 ORIGINAL ARTICLE Characterization of Malignant Pancreatic Cystic Lesions in the Background of Chronic Pancreatitis Dhanwant Gomez 1, Sakhawat H Rahman 1, Li Fong Wong 1, Caroline S Verbeke 2, Michael J
ORIGINAL ARTICLE Characterization of Malignant Pancreatic Cystic Lesions in the Background of Chronic Pancreatitis Dhanwant Gomez 1, Sakhawat H Rahman 1, Li Fong Wong 1, Caroline S Verbeke 2, Michael J
Original article. Introduction!
 382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
382 Original article Peritoneal seeding in intraductal papillary mucinous neoplasm of the pancreas patients who underwent endoscopic ultrasound-guided fine-needle aspiration: The PIPE Study Authors Won
EUS-guided pancreatic cyst ablation: a critical review (with video) Hyoung-Chul Oh, MD, 1 William R. Brugge, MD 2
 TECHNICAL REVIEW EUS-guided pancreatic cyst ablation: a critical review (with video) Hyoung-Chul Oh, MD, 1 William R. Brugge, MD 2 The widespread use of cross-sectional imaging has dramatically increased
TECHNICAL REVIEW EUS-guided pancreatic cyst ablation: a critical review (with video) Hyoung-Chul Oh, MD, 1 William R. Brugge, MD 2 The widespread use of cross-sectional imaging has dramatically increased
Cystic Lesions of the Pancreas: Clinical and Pathologic Review of Cases in a Five Year Period
 JOP. J Pancreas (Online) Jul ; (4):38364. ORIGINAL ARTICLE Cystic Lesions of the Pancreas: Clinical and Pathologic Review of Cases in a Five Year Period Carlos E ParraHerran, Mónica T Garcia, Loren Herrera,
JOP. J Pancreas (Online) Jul ; (4):38364. ORIGINAL ARTICLE Cystic Lesions of the Pancreas: Clinical and Pathologic Review of Cases in a Five Year Period Carlos E ParraHerran, Mónica T Garcia, Loren Herrera,
Outcomes associated with robotic approach to pancreatic resections
 Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
Short Communication (Management of Foregut Malignancies and Hepatobiliary Tract and Pancreas Malignancies) Outcomes associated with robotic approach to pancreatic resections Caitlin Takahashi 1, Ravi Shridhar
MANAGEMENT RECOMMENDATIONS
 1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016
 40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
40th European Congress of Cytology Liverpool, UK, 2-5 th October 2016 EUS FNA of abdominal organs: An approach to reporting and triage for ancillary testing Date and time: Sunday 2 nd October 2016 15.00-16.30
Pancreatic cystic neoplasms - A pictorial review
 Pancreatic cystic neoplasms - A pictorial review Poster No.: C-2386 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Adu, A. McLean, A. Parsai, K. L. Shahabuddin; London/UK Keywords: Abdomen, Pancreas,
Pancreatic cystic neoplasms - A pictorial review Poster No.: C-2386 Congress: ECR 2014 Type: Educational Exhibit Authors: J. Adu, A. McLean, A. Parsai, K. L. Shahabuddin; London/UK Keywords: Abdomen, Pancreas,
Management of Rare Liver Tumours
 Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
Gian Luca Grazi Hepato-Biliary-Pancreatic Surgery National Cancer Institute Regina Elena Rome Fibrolamellar Carcinoma Mixed Hepato Cholangiocellular Carcinoma Hepatoblastoma Carcinosarcoma Primary Hepatic
CT Attenuation of Unilocular Pancreatic Cystic Lesions to Differentiate Pseudocysts from Mucin-Containing Cysts
 ORIGINAL ARTICLE CT Attenuation of Unilocular Pancreatic Cystic Lesions to Differentiate Pseudocysts from Mucin-Containing Cysts Hamid Chalian, Hüseyin Gürkan Töre, Frank H Miller, Vahid Yaghmai Department
ORIGINAL ARTICLE CT Attenuation of Unilocular Pancreatic Cystic Lesions to Differentiate Pseudocysts from Mucin-Containing Cysts Hamid Chalian, Hüseyin Gürkan Töre, Frank H Miller, Vahid Yaghmai Department
Video Microscopy Tutorial 19
 Video Microscopy Tutorial 19 EUS FNA of Pancreatic Cysts Martha Pitman, MD There are no disclosures necessary. EUS-FNA of Pancreatic Cysts Martha Bishop Pitman, M.D. Massachusetts General Hospital Harvard
Video Microscopy Tutorial 19 EUS FNA of Pancreatic Cysts Martha Pitman, MD There are no disclosures necessary. EUS-FNA of Pancreatic Cysts Martha Bishop Pitman, M.D. Massachusetts General Hospital Harvard
Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center experience with 324 patients who underwent surgical resection
 Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Management of cystic and solid pancreatic incidentalomas: A review analysis
 J BUON 2013; 18(1): 17-24 ISSN: 1107-0625 www.bu-on.org/jbuon E-mail: jbuon@ath.forthnet.gr REVIEW ARTICLE Management of cystic and solid pancreatic incidentalomas: A review analysis T. Karatzas 1, D.
J BUON 2013; 18(1): 17-24 ISSN: 1107-0625 www.bu-on.org/jbuon E-mail: jbuon@ath.forthnet.gr REVIEW ARTICLE Management of cystic and solid pancreatic incidentalomas: A review analysis T. Karatzas 1, D.
A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case report
 Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
Diagnostic performance of endoscopic ultrasound-guided fine-needle aspiration in pancreatic lesions
 European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
European Review for Medical and Pharmacological Sciences 2018; 22: 1397-1401 Diagnostic performance of endoscopic in pancreatic lesions Q.-M. WU 1, Y.-N. GUO 1, Y.-Q. XU 1 Digestive Department of Beijing
Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
American Gastroenterological Association Institute Guidelines for Management of Asymptomatic Neoplastic Pancreatic Cysts
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 American Gastroenterological Association Institute Guidelines for Management of Asymptomatic Neoplastic Pancreatic Cysts Santhi Swaroop Vege, 1 Barry Ziring, 2 Rajeev
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 American Gastroenterological Association Institute Guidelines for Management of Asymptomatic Neoplastic Pancreatic Cysts Santhi Swaroop Vege, 1 Barry Ziring, 2 Rajeev
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 PathFinderTG Molecular Testing Page 1 of 20 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: PathFinderTG Molecular Testing Professional Institutional Original Effective
PathFinderTG Molecular Testing Page 1 of 20 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: PathFinderTG Molecular Testing Professional Institutional Original Effective
pissn: , eissn: Yonsei Med J 53(1): , 2012
 Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.106 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):106-110, 2012 Comparison of Efficacy of Enucleation and Pancreaticoduodenectomy for Small
Original Article http://dx.doi.org/10.3349/ymj.2012.53.1.106 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 53(1):106-110, 2012 Comparison of Efficacy of Enucleation and Pancreaticoduodenectomy for Small
MRI features of serous oligocystic adenoma of the pancreas: differentiation from mucinous cystic neoplasm of the pancreas
 The British Journal of Radiology, 85 (2012), 571 576 MRI features of serous oligocystic adenoma of the pancreas: differentiation from mucinous cystic neoplasm of the pancreas 1,2 J H LEE, MD, 1 J K KIM,
The British Journal of Radiology, 85 (2012), 571 576 MRI features of serous oligocystic adenoma of the pancreas: differentiation from mucinous cystic neoplasm of the pancreas 1,2 J H LEE, MD, 1 J K KIM,
Role of Endoscopic Ultrasonography in the Diagnosis and Treatment of Cystic Tumors of the Pancreas
 ROUND TABLE Role of Endoscopic Ultrasonography in the Diagnosis and Treatment of Cystic Tumors of the Pancreas Manoop S Bhutani Center for Endoscopic Ultrasound - Center for Endoscopic Research, Training
ROUND TABLE Role of Endoscopic Ultrasonography in the Diagnosis and Treatment of Cystic Tumors of the Pancreas Manoop S Bhutani Center for Endoscopic Ultrasound - Center for Endoscopic Research, Training
Genetics of Pancreatic Cancer. October 6, If you experience technical difficulty during the presentation:
 Genetics of Pancreatic Cancer October 6, 2016 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-229-3239 Toll Only: 1-408-435-7088
Genetics of Pancreatic Cancer October 6, 2016 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-229-3239 Toll Only: 1-408-435-7088
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
ORIGINAL ARTICLE. Abstract. Introduction
 ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-8 Pancreatic cysts suspected to be branch duct intraductal papillary mucinous neoplasm without concerning features have low risk for development
ORIGINAL ARTICLE Annals of Gastroenterology (2015) 28, 1-8 Pancreatic cysts suspected to be branch duct intraductal papillary mucinous neoplasm without concerning features have low risk for development
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas.
 Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Pancreatic Cyst. Introduction. EUS Findings of Pancreatic Cysts. Symposium
 Symposium Symposium II - Pancreatobiliary System : Endoscopic Approach for the Early Detection of Pancreatobiliary Malignancy in Ji Kon Ryu Department of Internal Medicine, Seoul National University College
Symposium Symposium II - Pancreatobiliary System : Endoscopic Approach for the Early Detection of Pancreatobiliary Malignancy in Ji Kon Ryu Department of Internal Medicine, Seoul National University College
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Molecular Testing for the Management of Pancreatic Cysts or Barrett Esophagus
 Molecular Testing for the Management of Pancreatic Cysts or Barrett Esophagus Policy Number: 2.04.52 Last Review: 8/2018 Origination: 5/2008 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas
Molecular Testing for the Management of Pancreatic Cysts or Barrett Esophagus Policy Number: 2.04.52 Last Review: 8/2018 Origination: 5/2008 Next Review: 8/2019 Policy Blue Cross and Blue Shield of Kansas
