Case Report Primary intracranial squamous cell carcinoma with brainstem invasion: a rare case in China with a 41-month follow-up
|
|
|
- Theodore Perry
- 5 years ago
- Views:
Transcription
1 Int J Clin Exp Med 2016;9(2): /ISSN: /IJCEM Case Report Primary intracranial squamous cell carcinoma with brainstem invasion: a rare case in China with a 41-month follow-up Tao Sun, Weiqing Wan, Yongji Tian, Liwei Zhang Department of Neurosurgery, Beijing Tiantan Hospital, Capital Medical University, China National Clinical Research Center for Neurological Diseases, Beijing, China Received October 27, 2015; Accepted January 18, 2016; Epub February 15, 2016; Published February 29, 2016 Abstract: Primary intracranial squamous cell carcinoma (SCC) is extremely rare and mostly associated with an intracranial epidermoid or dermoid cyst. Here, we present a rare case of primary intracranial SCC with brainstem invasion in a 22-year-old Chinese woman followed up for 41 months. The patient presented in February 2011 with a lesion in the right cerebellopontine area, and was treated by subtotal surgical resection. Histopathology confirmed SCC. Adjuvant radiotherapy (total dose, 50.4 Gy) was given 6 months after surgery, resulting in lesion shrinkage and symptom relief. However, symptom recurrence occurred 13 months after radiotherapy, and imaging revealed invasion into the pons. This was treated by gross total resection, and 12 months later by stereotactic radiosurgery after another recurrence at the same site. The patient died from severe dyspnea and pulmonary infection in June 2014, 41 months after the initial presentation. Surgery with adjuvant radiotherapy is appropriate for primary intracranial SCC, but long-term recurrence is likely. Keywords: Carcinoma squamous cell carcinoma, malignant primary brain neoplasms, intracranial neoplasms, carcinoma epidermoid Introduction Primary intracranial squamous cell carcinomas (SCCs) are rare and mostly associated with malignant transformation of intracranial epidermoid or dermoid cysts [1-8]. These tumors are commonly found in regions of the skull base, such as the cerebellopontine angle (CPA) and jugular foramen [1-8]. Here, we present a case of a 22-year-old woman with primary intracranial SCC in the CPA, who was followed up for 41 months. The patient was treated surgically with subtotal tumor resection, followed 6 months later by adjuvant radiotherapy (total dose, 50.4 Gy). Thirteen months after radiotherapy, the lesion was found to have invaded the pons; this was treated surgically by gross total resection. Tumor recurrence occurred 12 months after this second surgery, and the patient died 10 months later. To the best of our knowledge, this is the first report of this type of primary intracranial SCC in China. Case presentation Initial presentation and management This study was approved ethically by Beijing Tiantan Hospital Affiliated to Capital Medical University. The patient provided informed written consent. The patient and her next-of-kin provided informed written consent for the publication of this case report. The 22-year-old woman presented to the Department of Neurosurgery, Tiantan Hospital (Beijing, China) in February 2011, with a one-month history of weakness of the left limbs, headache, reduced appetite, recurrent vomiting, cough, dysphagia and weight loss. The patient had apparently been well before this episode. At the time of admission, the patient had a right facial cranial nerve paralysis, dysphagia, decreased sensation to touch in the left half of the body, reduced muscle tone in the left limbs, and a preoperative
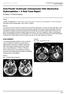
2 Figure 1. Magnetic resonance imaging (MRI) of the cranium before the first surgical procedure. A, B. A heterogeneous midline mass lesion is present. C. There is enhancement of the wall and an irregular nodule. D. A long T2 intensity lesion is evident in the right and left cerebellopontine angle and prepontine cistern. The brain stem is compressed and there is significant edema. Figure 2. Light microscopy images of resected tumor specimens, demonstrating malignant transformation of the epidermoid cyst to squamous cell carcinoma. A. Portions of a dense, fibrotic cyst wall lined by benign squamous epithelium are shown, in continuity with dysplastic squamous epithelium showing marked hyperplasia (HE, 100 ). B. The dysplastic squamous epithelium merged with areas of nested schistose infiltrating into interfibrillar substance and the mammillary protuberance (HE, 400 ). C. There were numerous typical and atypical mitoses, and extensive areas of necrosis. The adjacent stroma showed hemorrhage, hemosiderin deposition and cholesterol clefts (HE, 100 ). D. Malignant cells, with small-to-large anaplastic nuclei and a variable amount of finely vacuolated cytoplasm, can be seen. Scattered multinucleated tumor giant cells are also present (HE, 100 ). Immunohistochemical staining showed that the cells of the SCC were: E. Positive for cytokeratin 5/6 (100 ); F. Focally positive for carcinoembryonic antigen (CEA; 200 ); G. 60% positive for Ki-67 (200 ). Karnofsky performance score of 60. There was no visual impairment or papilledema. Routine hematologic and serum biochemistry investigations revealed no abnormalities. Magnetic resonance imaging (MRI) of the cranium (Magnetom 3.0 T; Siemens Corp. Germen) revealed a heterogeneous midline mass lesion of size cm, located in the right and left CPA and prepontine cistern (Figure 1). Compression of the brainstem and significant edema were evident, but there was no oppression of the ventricle or hydrocephalus (Figure 1). Computed tomography (CT) revealed an absence of calcification. The lesion was diagnosed initially as an epidermoid or dermoid cyst. Resection of the tumor was carried out by a surgeon with substantial experience of skull base neurosurgery. A right retromastoid approach was used. On gross inspection, the lower part of the lesion was firm in consistency and adhered to the brainstem, while the upper part 4784 Int J Clin Exp Med 2016;9(2):
3 Figure 3. Magnetic resonance imaging (MRI) of the cranium after the first surgical procedure and radiotherapy. A-C. A cm remnant of tumor remained in the right cerebellopontine angle. D-E. The residual tumor shrank after radiotherapy, but a tumor nodule remained in the brainstem. consisted of a yellowish caseous material with pearly cyst contents, features suggestive of an epidermoid cyst. Since a solid part of the tumor was adhered to the brainstem, a subtotal resection was carried out to minimize potentially serious damage to the brainstem. Multiple surgical specimens were submitted for histologic evaluation. The residual tumor comprised a cm nodule in the right medial brainstem. Histopathology findings Pathologic assessment of the excised tumor revealed SCC and an epidermoid cyst with malignant transformation (Figure 2). Exam ination under the light microscope revealed a dense, fibrotic cyst wall lined by benign squamous epithelium in continuity with dysplastic squamous epithelium showing marked hyperplasia (Figure 2A). The dysplastic squamous epithelium merged with areas of nested schistose infiltrating into the interfibrillar substance and mammillary protuberance (Figure 2B). There were numerous typical and atypical mitoses, and extensive areas of necrosis. The adjacent stroma showed evidence of hemorrhage, hemosiderin deposition and cholesterol clefts (Figure 2C). Malignant cells were also present, with small-to-large anaplastic nuclei and a variable amount of finely vacuolated cytoplasm, as well as multinucleated tumor giant cells (Figure 2D). Immunohistochemical staining techniques revealed that the SCC cells were: positive for cytokeratin 5/6 (Figure 2E); negative for P53; focally positive for carcinoembryonic antigen (CEA; Figure 2F); negative for neuron-specific enolase (NSE); negative for the epidermal growth factor receptor (EGFR); weakly positive for vascular endothelial growth factor (VEGF); and 60% positive for Ki-67 (Figure 2G). Postoperative course The patient was reviewed every 6 months by means of MRI and physical examinations, including neurologic examination of the limbs, and assessments of the cough reflex, swallow Int J Clin Exp Med 2016;9(2):
4 Figure 4. Magnetic resonance imaging (MRI) of the cranium before the second surgical procedure, and histology of the tumor that was subsequently resected. A, B. The tumor nodule had enlarged and invaded the pons. A cyst had formed and was causing a mass effect. C. Histology of the resected tumor revealed a squamous cell carcinoma similar to that seen in the original presentation. ing reflex and facial sensation. Postoperatively, there were improvements in symptoms associated with high intracranial pressure, such as headache and vomiting, but not in limb weakness, cough or dysphagia. Positron emission tomography (PET) revealed normal uptake and no signs of tumor in any other regions of the body, including the nasopharynx, oropharynx, visualized sinuses, orbits, chest, abdomen, pelvis, and cutaneous and subcutaneous tissues. Systemic X-ray and ultrasound scanning excluded the possibility that the tumor was a cerebral metastasis from a primary focus located elsewhere in the body. Post-operative MRI demonstrated residual tumor, of size cm, in the right CPA (Figure 3A-C). Six months after surgery (August 2011), the patient received intensity-modulated radiation therapy applied to the tumor remnant (total dose, 50.4 Gy: 28 applications of 1.8 Gy each; total course were 38 days). No chemotherapy was administered. Subsequent to the radiotherapy, there was resolution of the symptoms of left limb weakness, right facial cranial nerve paralysis and dysphagia. A follow-up MRI on January 2012 showed shrinkage of the residual tumor in the brainstem to a volume < 0.5 cm 3 (Figure 3D-F). As the patient was symptom free, no further treatment was given, but followup was continued every 6 months. Second presentation and management Thirteen months after radiotherapy (September 2012), the patient presented at our department with a one-week history of headaches and weakness of the left limbs. MRI showed a solid and cystic mass in the right pons with an enhanced tubercle. However, there was no evidence of recurrence at the original site of the tumor, namely the CPA and prepontine cistern (Figure 4A, 4B). A gross total resection of the tumor was undertaken, using a far-lateral approach. During the operation, cicatrix-like tissue was found in the right CPA, and was presumed to be the remnant of the first operation. A relatively soft tumor nodule was identified in the brainstem, with no distinct boundary between it and the adjacent brain tissue. A stoma was made into the pons, and the tumor nodule removed. Intraoperative bleeding was not considered excessive. Pathologic examination of the tumor revealed a similar SCC to that identified following the first surgical resection. Under the light microscope, irregular atypical cells and keratinization were seen, together with atypical mitoses and extensive areas of necrosis. On immunohistochemical staining, the cells of the SCC were positive for cytokeratin 5/6, weakly positive for VEGF, and 70% positive for Ki-67. After the operation, the patient showed progressive improvements in the symptoms and signs of left limb weakness, paresis of the sixth cranial nerve and dysphagia. The patient was discharged after two weeks and subsequently followed-up every 3 months. Long-term outcome Tumor relapse at the same site in the brainstem was discovered 12 months after the second operation (September 2013) and was accompanied by symptoms of bulbar palsy, 4786 Int J Clin Exp Med 2016;9(2):
5 such as dyspnea, dysphagia and choking. Stereotactic radiosurgery was used as a treatment modality, but the tumor was not controlled, resulting in a gradual worsening of the patient s condition. The patient died in J uly 2014, due to severe dyspnea and pulmonary infection. The total survival time was 41 months from the initial presentation at our department. Conclusions To the best of our knowledge, this is the first report of primary intracranial SCC, without a previous history of epidermoid or dermoid cyst, in a patient in China. Primary intracranial SCC is extremely rare. The mechanisms underlying the malignant transformation of an epidermoid cyst are unknown, but chronic inflammation, due to repeated cyst wall rupture and/or subtotal resection, resulting in mesenchymal metaplasia has been suggested as a possibility [9, 10]. When malignant transformation does occur, the course is more aggressive than that of a benign epidermoid cyst [11, 12]. Garcia et al. and Hamlat et al. have proposed a set of criteria that need to be met for a lesion to be classified as primary intracranial SCC: the tumor is restricted to the intracranial intradural compartment; there is no invasion of or extension beyond the dura or cranial bones, or through cranial orifices; there is no communication with the middle ear, air sinuses or sella turcica; there is no evidence of a nasopharyngeal tumor; benign squamous epithelium is present within the tumor mass; and there is no evidence of a tumor elsewhere [1, 5]. In the present case, the patient presented with only a short (1-month) history of symptoms, and there was neither any history of previous surgery nor any evidence indicative of a preceding benign intracranial cyst. A thorough workup, including multiple PET-CT scans, revealed no evidence of a primary tumor at an alternative location. Furthermore, histopathologic examination of the resected tumor specimen showed features of a SCC. Therefore, the present case met the criteria for a primary SCC, as proposed by Garcia et al. and Hamlat et al. [1, 5]. The treatment of choice for primary intracranial SCCs is gross total resection followed by radiotherapy, which is especially useful in cases where complete resection is not possible [13-15]. The effectiveness of chemotherapy has yet to be definitely established. If there is intimate involvement of the brainstem, an attempt to completely remove an adherent lesion can result in unacceptable morbidity. Of 27 patients described in the literature, four were reported to have died in the immediate postoperative period following aggressive surgical resection [3, 16-18]. Thus, the desire to achieve gross total surgical resection must be tempered by the natural history of this tumor. As surgery alone is not curative and frequently limited by the necessity for subtotal resection, adjuvant therapy has often been used in an effort to control the disease process. The survival time with combined adjuvant therapy is longer than that with surgery alone [2, 19, 20], and this is dependent on the sensitivity of the SCC to radiotherapy and/or chemotherapy. Radiosurgery has been used widely to control malignant epidermoid tumors, and the benefits have been well documented [6, 21, 22]. Patients who receive surgical treatment alone for intracranial SCCs tend not to survive for more than 3 months. In contrast, the survival time for patients who receive postoperative radiotherapy is 21.5 ± 17.4 months [3, 18, 19, 23-25]. Indeed, Nishio et al. reported a disease-free survival of > 2.5 years in one patient with primary intracranial SCC after local irradiation [19], while Link et al. reported the successful control of an intracranial SCC for 27 months following stereotactic radiosurgery and external-beam radiotherapy [11]. In the case we present here, only subtotal resection of the tumor was possible during the first surgery due to tight adherence of the lesion to the brainstem. The patient received postoperative intensity-modulated radiotherapy to the resection bed, and this led to shrinkage of the tumor remnant and a progression-free period of 13 months. However, subsequent invasion of the tumor into the pons resulted in a recurrence of symptoms. We believe that the mass effect of the cyst was the cause of symptom recurrence. During the second surgery, gross total resection of the tumor was achieved with minimal disturbance to the brainstem. As a result, the condition was controlled for 12 months, at which point the next relapse occurred. The stereotactic radiosurgery that 4787 Int J Clin Exp Med 2016;9(2):
6 was used to treat this further relapse was not as effective as the first adjuvant radiotherapy. In summary, we report a case of primary intracranial SCC with a follow-up of nearly 3.5 years. The case was characterized by initial shrinkage of the tumor remnant and subsequent invasion into the brainstem after subtotal resection and adjuvant radiotherapy. Since intracranial SCC involves important brain structures, including the brainstem and/or cranial nerves, complete removal of the tumor is essentially impossible; therefore, gross total or subtotal resection coupled with adjuvant therapy is likely to be the optimal management strategy. Radiotherapy may be useful for short-term control of intracranial SCCs, but the effects are not well maintained long-term. In the present case, stereotactic radiosurgery was of little benefit. Disclosure of conflict of interest None. Address correspondence to: Liwei Zhang, Department of Neurosurgery, Beijing Tiantan Hospital, Capital Medical University, China National Clinical Research Center for Neurological Diseases, 6 Tiantan Xili, Chongwen District, Beijing , P. R. China. Tel: ; Fax: ; s.tao76@263.net References [1] Garcia CA, McGarry PA and Rodriguez F. Primary intracranial squamous cell carcinoma of the right cerebellopontine angle. J Neurosurg 1981; 54: [2] Guan LM, Qi XX, Zhang JR, Xu K, Cui LJ and Zhang Q. Intracranial squamous cell carcinoma developing in remnant of an epidermoid cyst: case report and literature review. Chin Med J (Engl) 2004; 117: [3] Michael LM 2nd, Moss T, Madhu T and Coakham HB. Malignant transformation of posterior fossa epidermoid cyst. Br J Neurosurg 2005; 19: [4] Nuno-Arana I, Garcia-Garcia VA, Espejo- Plascencia I, Ramos-Zavala AL and Rivera H. An intracranial carcinoma in a Mexican woman with Bloom syndrome. Ann Genet 2000; 43: [5] Hamlat A, Hua ZF, Saikali S, Laurent JF, Gedouin D, Ben-Hassel M and Guegan Y. Malignant transformation of intra-cranial epithelial cysts: systematic article review. J Neurooncol 2005; 74: [6] Tamura K, Aoyagi M, Wakimoto H, Tamaki M, Yamamoto K, Yamamoto M and Ohno K. Malignant transformation eight years after removal of a benign epidermoid cyst: a case report. J Neurooncol 2006; 79: [7] Agarwal S, Rishi A, Suri V, Sharma MC, Satyarthi GD, Garg A and Sarkar C. Primary intracranial squamous cell carcinoma arising in an epidermoid cyst--a case report and review of literature. Clin Neurol Neurosurg 2007; 109: [8] Mallick S, Biswas A, Kumar N, Chand Sharma M, Kumar R, Mohan Reddy R, Kumar Julka P and Kishore Rath G. Primary intracranial basaloid squamous cell carcinoma: an enigma. Neurol Neurochir Pol 2012; 46: [9] Abramson RC, Morawetz RB and Schlitt M. Multiple complications from an intracranial epidermoid cyst: case report and literature review. Neurosurgery 1989; 24: [10] Giangaspero F, Manetto V, Ferracini R and Piazza G. Squamous cell carcinoma of the brain with sarcoma-like stroma. Virchows Arch A Pathol Anat Histopathol 1984; 402: [11] Link MJ, Cohen PL, Breneman JC and Tew JM Jr. Malignant squamous degeneration of a cerebellopontine angle epidermoid tumor. Case report. J Neurosurg 2002; 97: [12] Sawan B, Vital A, Loiseau H, Dousset V, Strub D and Vital C. Squamous cell carcinoma developing in an intracranial prepontine epidermoid cyst. Ann Pathol 2000; 20: [13] Darrouzet V, Franco-Vidal V, Hilton M, Nguyen DQ, Lacher-Fougere S, Guerin J and Bebear JP. Surgery of cerebellopontine angle epidermoid cysts: role of the widened retrolabyrinthine approach combined with endoscopy. Otolaryngol Head Neck Surg 2004; 131: [14] Mohanty A, Venkatrama SK, Rao BR, Chandramouli BA, Jayakumar PN and Das BS. Experience with cerebellopontine angle epidermoids. Neurosurgery 1997; 40: 24-29; discussion [15] Samii M, Tatagiba M, Piquer J and Carvalho GA. Surgical treatment of epidermoid cysts of the cerebellopontine angle. J Neurosurg 1996; 84: [16] Lewis AJ, Cooper PW, Kassel EE and Schwartz ML. Squamous cell carcinoma arising in a suprasellar epidermoid cyst. Case report. J Neurosurg 1983; 59: [17] Acciarri N, Padovani R, Foschini MP, Giulioni M and Finizio FS. Intracranial squamous cell carcinoma arising in an epidermoid cyst. Br J Neurosurg 1993; 7: [18] Tognetti F, Lanzino G, Manetto V and Calbucci F. Intracranial squamous cell carcinoma arising in remnant of extirpated epidermoid cyst. Br J Neurosurg 1991; 5: [19] Nishio S, Takeshita I, Morioka T and Fukui M. Primary intracranial squamous cell carcinomas: report of two cases. Neurosurgery 1995; 37: Int J Clin Exp Med 2016;9(2):
7 [20] Kim MS and Kim OL. Primary intracranial squamous cell carcinoma in the brain stem with a cerebellopontine angle epidermoid cyst. J Korean Neurosurg Soc 2008; 44: [21] Landers JW and Danielski JJ. Malignant intracranial epidermoid cyst. Report of a case with leptomeningeal spread. Arch Pathol 1960; 70: [22] Murase S, Yamakawa H, Ohkuma A, Sumi Y, Kajiwara M, Takami T and Sakai N. Primary intracranial squamous cell carcinoma--case report. Neurol Med Chir (Tokyo) 1999; 39: [23] Dubois PJ, Sage M, Luther JS, Burger PC, Heinz ER and Drayer BP. Case report. Malignant change in an intracranial epidermoid cyst. J Comput Assist Tomogr 1981; 5: [24] Goldman SA and Gandy SE. Squamous cell carcinoma as a late complication of intracerebroventricular epidermoid cyst. Case report. J Neurosurg 1987; 66: [25] Hao S, Tang J, Wu Z, Zhang L, Zhang J and Wang Z. Natural malignant transformation of an intracranial epidermoid cyst. J Formos Med Assoc 2010; 109: Int J Clin Exp Med 2016;9(2):
Case Report Malignant Transformation Six Months after Removal of Intracranial Epidermoid Cyst: A Case Report
 Case Reports in Neurological Medicine Volume 2011, Article ID 525289, 4 pages doi:10.1155/2011/525289 Case Report Malignant Transformation Six Months after Removal of Intracranial Epidermoid Cyst: A Case
Case Reports in Neurological Medicine Volume 2011, Article ID 525289, 4 pages doi:10.1155/2011/525289 Case Report Malignant Transformation Six Months after Removal of Intracranial Epidermoid Cyst: A Case
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Intracranial squamous cell carcinoma arising in a cerebellopontine angle epidermoid cyst A case report and literature review
 Clinical Case Report Medicine Intracranial squamous cell carcinoma arising in a cerebellopontine angle epidermoid cyst A case report and literature review Tae Hoon Roh, MD a,b, Yong Sook Park, MD, PhD
Clinical Case Report Medicine Intracranial squamous cell carcinoma arising in a cerebellopontine angle epidermoid cyst A case report and literature review Tae Hoon Roh, MD a,b, Yong Sook Park, MD, PhD
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Brain Tumors. What is a brain tumor?
 Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
Management of Neck Metastasis from Unknown Primary
 Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
Management of Neck Metastasis from Unknown Primary.. Definition Histologic evidence of malignancy in the cervical lymph node (s) with no apparent primary site of original tumour Diagnosis after a thorough
ISSN: Volume 4 Issue CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS
 ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
Malignant squamous degeneration of a cerebellopontine angle epidermoid tumor
 J Neurosurg 97:1237 1243, 2002 Malignant squamous degeneration of a cerebellopontine angle epidermoid tumor Case report MICHAEL J. LINK, M.D., PAUL L. COHEN, M.D., JOHN C. BRENEMAN, M.D., AND JOHN M. TEW,
J Neurosurg 97:1237 1243, 2002 Malignant squamous degeneration of a cerebellopontine angle epidermoid tumor Case report MICHAEL J. LINK, M.D., PAUL L. COHEN, M.D., JOHN C. BRENEMAN, M.D., AND JOHN M. TEW,
Primary Intracranial Squamous Cell Carcinoma
 Neurol Med Chir (Tokyo) 39, 49 `54, 1999 Primary Intracranial Squamous Cell Carcinoma -Case Report- Satoru MURASE, Hiroyasu YAMAKAWA, Akio OHKUMA* *, Yasuhiko SUMI * * *, Masaharu KAJIWARA*, Tsuyoshi TAKAMI*,
Neurol Med Chir (Tokyo) 39, 49 `54, 1999 Primary Intracranial Squamous Cell Carcinoma -Case Report- Satoru MURASE, Hiroyasu YAMAKAWA, Akio OHKUMA* *, Yasuhiko SUMI * * *, Masaharu KAJIWARA*, Tsuyoshi TAKAMI*,
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, :30am - 11:30am FACULTY COPY
 SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
SESSION 1: GENERAL (BASIC) PATHOLOGY CONCEPTS Thursday, October 16, 2008 9:30am - 11:30am FACULTY COPY GOAL: Describe the basic morphologic (structural) changes which occur in various pathologic conditions.
An enterogenous cyst with atypical pathological findings and chemical meningitis
 DOI 10.1186/s40064-016-3677-0 CASE STUDY Open Access An enterogenous cyst with atypical pathological findings and chemical meningitis Lu Wang 1, Xiaona Chang 2, Chao Fu 1, Weidong Yu 1 and Xiaoxuan Fang
DOI 10.1186/s40064-016-3677-0 CASE STUDY Open Access An enterogenous cyst with atypical pathological findings and chemical meningitis Lu Wang 1, Xiaona Chang 2, Chao Fu 1, Weidong Yu 1 and Xiaoxuan Fang
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
3/27/2017. Pulmonary Pathology Specialty Conference. Disclosure of Relevant Financial Relationships. Clinical History:
 Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Pulmonary Pathology Specialty Conference Saul Suster, M.D. Medical College of Wisconsin Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Scenario 1. The patient agreed to a CT guided biopsy of the left upper lobe mass. This was performed and confirmed non-small cell carcinoma.
 Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY
 Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY SEARCHING FOR THE PRIMARY? P r o f J P P r e t o r i u s H e a d : C l i n i c a l U n i t C r i t i c a l C a r e U n i v e r s i t y O f
Carcinoma of Unknown Primary site (CUP) in HEAD & NECK SURGERY SEARCHING FOR THE PRIMARY? P r o f J P P r e t o r i u s H e a d : C l i n i c a l U n i t C r i t i c a l C a r e U n i v e r s i t y O f
Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature
 Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Evaluation of Neck Mass. Disclosure. Learning Objectives 3/24/2014. Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ. Nothing to disclose
 Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
Case Report A case report on intermediate-grade malignant meningeal melanocytoma with elevated cell proliferation index
 Int J Clin Exp Pathol 2015;8(9):11698-11703 www.ijcep.com /ISSN:1936-2625/IJCEP0012900 Case Report A case report on intermediate-grade malignant meningeal melanocytoma with elevated cell proliferation
Int J Clin Exp Pathol 2015;8(9):11698-11703 www.ijcep.com /ISSN:1936-2625/IJCEP0012900 Case Report A case report on intermediate-grade malignant meningeal melanocytoma with elevated cell proliferation
EXTRACRANIAL MENINGIOMA PRESENTING AS INFRATEMPORAL FOSSA MASS: A CASE SERIES
 Case Series EXTRACRANIAL MENINGIOMA PRESENTING AS INFRATEMPORAL FOSSA MASS: A CASE SERIES Sunil Mathew * 1, Reddy Ravikanth 2, Vijaykishan B 3. ABSTRACT Extradural meningioma occurs as extracranial extension
Case Series EXTRACRANIAL MENINGIOMA PRESENTING AS INFRATEMPORAL FOSSA MASS: A CASE SERIES Sunil Mathew * 1, Reddy Ravikanth 2, Vijaykishan B 3. ABSTRACT Extradural meningioma occurs as extracranial extension
ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY
 ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY James G. Douglas, MD, MS, 1,2 Robert Goodkin, MD, 1,2 George
ORIGINAL ARTICLE GAMMA KNIFE STEREOTACTIC RADIOSURGERY FOR SALIVARY GLAND NEOPLASMS WITH BASE OF SKULL INVASION FOLLOWING NEUTRON RADIOTHERAPY James G. Douglas, MD, MS, 1,2 Robert Goodkin, MD, 1,2 George
Cystic carcinoma of the neck
 Case Report Brunei Int Med J. 2010; 6 (1): 56-60 Cystic carcinoma of the neck Prathibha Parampalli SUBRHAMANYA, Ghazala KAFEEL, Hla OO, Pemasiri Upali TELISINGHE, Department of Pathology, RIPAS Hospital,
Case Report Brunei Int Med J. 2010; 6 (1): 56-60 Cystic carcinoma of the neck Prathibha Parampalli SUBRHAMANYA, Ghazala KAFEEL, Hla OO, Pemasiri Upali TELISINGHE, Department of Pathology, RIPAS Hospital,
Esophageal Cancer Initially Thought to be Accompanied by a Solitary Metastasis to an Intrathoracic Paraaortic Lymph Node
 2012 66 5 417 421 Esophageal Cancer Initially Thought to be Accompanied by a Solitary Metastasis to an Intrathoracic Paraaortic Lymph Node a b* a a a a a a a b ʼ 418 Horio et al. Acta Med. Okayama Vol.
2012 66 5 417 421 Esophageal Cancer Initially Thought to be Accompanied by a Solitary Metastasis to an Intrathoracic Paraaortic Lymph Node a b* a a a a a a a b ʼ 418 Horio et al. Acta Med. Okayama Vol.
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience. Kevin Yiee MD, MPH Resident Physician
 Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
ISPUB.COM The Internet Journal of Neurosurgery Volume 7 Number 1 Intra-Fourth Ventricular Schwannoma With Obstructive Hydrocephalus A Rare Case Report A Babbu, R Katheerayson Citation A Babbu, R Katheerayson..
Nature and Science 2017;15(7) Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus
 Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Index. Surg Oncol Clin N Am 16 (2007) Note: Page numbers of article titles are in boldface type.
 Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Surg Oncol Clin N Am 16 (2007) 465 469 Index Note: Page numbers of article titles are in boldface type. A Adjuvant therapy, preoperative for gastric cancer, staging and, 339 B Breast cancer, metabolic
Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation
 246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
Case Report Squamous Cell Carcinoma of the External Auditory Canal: ACaseReport
 Case Reports in Otolaryngology Volume 2011, Article ID 615210, 4 pages doi:10.1155/2011/615210 Case Report Squamous Cell Carcinoma of the External Auditory Canal: ACaseReport Harry Boamah, 1 Glenn Knight,
Case Reports in Otolaryngology Volume 2011, Article ID 615210, 4 pages doi:10.1155/2011/615210 Case Report Squamous Cell Carcinoma of the External Auditory Canal: ACaseReport Harry Boamah, 1 Glenn Knight,
CASE REPORT PLEOMORPHIC LIPOSARCOMA OF PECTORALIS MAJOR MUSCLE IN ELDERLY MAN- CASE REPORT & REVIEW OF LITERATURE.
 PLEOMORPHIC LIPOSARCOMA OF PECTORALIS MAJOR MUSCLE IN ELDERLY MAN- CASE REPORT & REVIEW OF LITERATURE. M. Madan 1, K. Nischal 2, Sharan Basavaraj. C. J 3. HOW TO CITE THIS ARTICLE: M. Madan, K. Nischal,
PLEOMORPHIC LIPOSARCOMA OF PECTORALIS MAJOR MUSCLE IN ELDERLY MAN- CASE REPORT & REVIEW OF LITERATURE. M. Madan 1, K. Nischal 2, Sharan Basavaraj. C. J 3. HOW TO CITE THIS ARTICLE: M. Madan, K. Nischal,
Rare Presentation Of Adenoidcystic Carcinoma Of External Auditory Canal With Subcutaneous Metastasis In Temporal Region
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 13 Number 2 Rare Presentation Of Adenoidcystic Carcinoma Of External Auditory Canal With Subcutaneous Metastasis In Temporal Region S Kaushik,
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 13 Number 2 Rare Presentation Of Adenoidcystic Carcinoma Of External Auditory Canal With Subcutaneous Metastasis In Temporal Region S Kaushik,
BONE METASTASIS OF MEDIASTINAL PARAGANGLIOMA: CASE REPORT
 BONE METASTASIS OF MEDIASTINAL PARAGANGLIOMA: CASE REPORT Dr. Abhinandan Gupta 1*, Kong Long 1, Prof. Huang Jing Bai 1, Dr. Deepikal Dhakal 1, Dr. Sunil Shrestha 1, Dr. Roshan Kumar Yadav 2 and Dr. Shashi
BONE METASTASIS OF MEDIASTINAL PARAGANGLIOMA: CASE REPORT Dr. Abhinandan Gupta 1*, Kong Long 1, Prof. Huang Jing Bai 1, Dr. Deepikal Dhakal 1, Dr. Sunil Shrestha 1, Dr. Roshan Kumar Yadav 2 and Dr. Shashi
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION. Mustafa Rashid Issa
 THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
THE EFFECTIVE OF BRAIN CANCER AND XAY BETWEEN THEORY AND IMPLEMENTATION Mustafa Rashid Issa ABSTRACT: Illustrate malignant tumors that form either in the brain or in the nerves originating in the brain.
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
Synchronous squamous cell carcinoma of the breast. and invasive lobular carcinoma
 Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Sentani K et al. 1 Letter to the editor Synchronous squamous cell carcinoma of the breast and invasive lobular carcinoma Kazuhiro Sentani, 1 Takashi Tashiro, 2 Naohide Oue, 1 Wataru Yasui 1 1 Department
Brain Tumor Treatment
 Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Scan for mobile link. Brain Tumor Treatment Brain Tumors Overview A brain tumor is a group of abnormal cells that grows in or around the brain. Tumors can directly destroy healthy brain cells. They can
Carcinoma ex Pleomorphic Adenoma on Right Parotid Gland: A Case Report. School of Dentistry, Kyungpook National University
 Korean Journal of Oral and Maxillofacial Pathology 2017;41(4):189-194 ISSN:1225-1577(Print); 2384-0900(Online) Available online at http://journal.kaomp.org https://doi.org/10.17779/kaomp.2017.41.4.006
Korean Journal of Oral and Maxillofacial Pathology 2017;41(4):189-194 ISSN:1225-1577(Print); 2384-0900(Online) Available online at http://journal.kaomp.org https://doi.org/10.17779/kaomp.2017.41.4.006
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
A CASE OF A Huge Submandibular Pleomorphic Adenoma
 ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 4 Number 2 S VERMA Citation S VERMA.. The Internet Journal of Head and Neck Surgery. 2009 Volume 4 Number 2. Abstract Pleomorphic adenoma
ISPUB.COM The Internet Journal of Head and Neck Surgery Volume 4 Number 2 S VERMA Citation S VERMA.. The Internet Journal of Head and Neck Surgery. 2009 Volume 4 Number 2. Abstract Pleomorphic adenoma
ABSTRACT. Epidermoid Cysts in the Frontal Lobe A Case Series. Key words: Epidermoid Cyst; Frontal Lobe; Case Series
 Epidermoid Cysts in the Frontal Lobe A Case Series Hina Abdul Qayoom Khan 1, Zain A. Sobani 2, Arshad A. Siddiqui 3 1 Department of Surgery, Jinnah Post-graduate Medical Center, Karachi, Pakistan 2 Section
Epidermoid Cysts in the Frontal Lobe A Case Series Hina Abdul Qayoom Khan 1, Zain A. Sobani 2, Arshad A. Siddiqui 3 1 Department of Surgery, Jinnah Post-graduate Medical Center, Karachi, Pakistan 2 Section
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX
 QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
5/26/16: CT scan of the abdomen showed a multinodular liver disease highly suspicious for metastasis and hydronephrosis of the right kidney.
 Bladder Case Scenario 1 History 5/23/16: A 52-year-old male, smoker was admitted to our hospital with a 3-month history of right pelvic pain, multiple episodes of gross hematuria, dysuria, and extreme
Bladder Case Scenario 1 History 5/23/16: A 52-year-old male, smoker was admitted to our hospital with a 3-month history of right pelvic pain, multiple episodes of gross hematuria, dysuria, and extreme
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
University Journal of Surgery and Surgical Specialities
 University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 EXTRA SKELETAL MESENCHYMAL CHONDROSARCOMA :A CASE REPORT Rajaraman R Subbiah S Navin Naushad Kilpaulk Medical College Abstract:
University Journal of Surgery and Surgical Specialities Volume 1 Issue 1 2015 EXTRA SKELETAL MESENCHYMAL CHONDROSARCOMA :A CASE REPORT Rajaraman R Subbiah S Navin Naushad Kilpaulk Medical College Abstract:
Intra-cranial malignant peripheral nerve sheath tumor of olfactory nerve: a case report and review of literature
 DOI: 10.2478/romneu-2018-0059 Article Intra-cranial malignant peripheral nerve sheath tumor of olfactory nerve: a case report and review of literature Varun Aggarwal, Amit Narang, Chandni Maheshwari, Divya
DOI: 10.2478/romneu-2018-0059 Article Intra-cranial malignant peripheral nerve sheath tumor of olfactory nerve: a case report and review of literature Varun Aggarwal, Amit Narang, Chandni Maheshwari, Divya
Results of Surgery of Cerebellopontine angle Tumors
 Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
doi: /j.anl
 doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
doi: 10.1016/j.anl.2006.07.001 Synchronous unilateral parotid gland neoplasms of three different histological types Shuho Tanaka 1, Keiji Tabuchi 1, Keiko Oikawa 1, Rika Kohanawa 1, Hideki Okubo 1, Dai
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 Final Pathology:
 Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX
 QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
QUIZZES WITH ANSWERS FOR COLLECTING CANCER DATA: PHARYNX MP/H Quiz 1. A patient presented with a prior history of squamous cell carcinoma of the base of the tongue. The malignancy was originally diagnosed
Patient Information. Age: 8 y/o Sex: Female. Date of Admission: Date of Discharge:
 Patient Information Age: 8 y/o Sex: Female Date of Admission: 92-10-08 Date of Discharge: 92-10-18 Chief Complaint Severe admominal pain and vomiting with dysuria since last afternoon Present Illness Lower
Patient Information Age: 8 y/o Sex: Female Date of Admission: 92-10-08 Date of Discharge: 92-10-18 Chief Complaint Severe admominal pain and vomiting with dysuria since last afternoon Present Illness Lower
Central Poorly Differentiated Adenocarcinoma of the Maxilla: Report of a Case
 Kobe J. Med. Sci., Vol. 49, No. 2, pp. 45-49, 2003 Central Poorly Differentiated Adenocarcinoma of the Maxilla: Report of a Case MASAHIRO UMEDA 1), SATOSHI YOKOO 1), YASUYUKI SHIBUYA 1), TAKAHIDE KOMORI
Kobe J. Med. Sci., Vol. 49, No. 2, pp. 45-49, 2003 Central Poorly Differentiated Adenocarcinoma of the Maxilla: Report of a Case MASAHIRO UMEDA 1), SATOSHI YOKOO 1), YASUYUKI SHIBUYA 1), TAKAHIDE KOMORI
HPV and Head and Neck Cancer: What it means for you and your patients
 HPV and Head and Neck Cancer: What it means for you and your patients Financial Disclosure: None November 8, 2013 Steven J. Wang, MD Associate Professor Department of Otolaryngology-Head and Neck Surgery
HPV and Head and Neck Cancer: What it means for you and your patients Financial Disclosure: None November 8, 2013 Steven J. Wang, MD Associate Professor Department of Otolaryngology-Head and Neck Surgery
أملس عضلي غرن = Leiomyosarcoma. Leiomyosarcoma 1 / 5
 Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Leiomyosarcoma 1 / 5 EPIDEMIOLOGY Exact incidence is unknown, but older studies suggest that leiomyosarcomas comprise approximately 3 percent of soft-tissue sarcomas. Superficial leiomyosarcoma occurs
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
What is head and neck cancer? How is head and neck cancer diagnosed and evaluated? How is head and neck cancer treated?
 Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that start in the oral cavity, larynx, pharynx, salivary glands, nasal cavity or paranasal sinuses. They usually begin
Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that start in the oral cavity, larynx, pharynx, salivary glands, nasal cavity or paranasal sinuses. They usually begin
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis
 Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Da Costa was the first to coin the term. Marjolin s Ulcer: A Case Report and Literature Review. Case Report. Introduction
 E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
E-Da Medical Journal 2016;3(2):24-28 Case Report Marjolin s Ulcer: A Case Report and Literature Review Yue-Chiu Su 1, Li-Ren Chang 2 Marjolin s ulcer is an aggressive cutaneous malignancy, which is common
New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma
 July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
July 2016 New lung lesion in a 55 year-old male treated with chemoradiation for non-small cell lung carcinoma Contributed by: Laurel Rose, MD, Resident Physician, Indiana University School of Medicine,
1/25/13 Right partial nephrectomy followed by completion right radical nephrectomy.
 History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
History and Physical Case Scenario 1 45 year old white male presents with complaints of nausea, weight loss, and back pain. A CT of the chest, abdomen and pelvis was done on 12/8/12 that revealed a 12
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
PET IMAGING (POSITRON EMISSION TOMOGRAPY) FACT SHEET
 Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Positron Emission Tomography (PET) When calling Anthem (1-800-533-1120) or using the Point of Care authorization system for a Health Service Review, the following clinical information may be needed to
Craniopharyngioma. Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital
 Craniopharyngioma Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital Objectives Incidence Clinical Presentation Treatment Options Perioperative concerns Long-term endocrine
Craniopharyngioma Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital Objectives Incidence Clinical Presentation Treatment Options Perioperative concerns Long-term endocrine
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Report Carbon Ion Beam Radiotherapy for Sinonasal Malignant Tumors Invading Skull Base
 Case Reports in Otolaryngology, Article ID 241856, 4 pages http://dx.doi.org/10.1155/2014/241856 Case Report Carbon Ion Beam Radiotherapy for Sinonasal Malignant Tumors Invading Skull Base Nobuo Ohta,
Case Reports in Otolaryngology, Article ID 241856, 4 pages http://dx.doi.org/10.1155/2014/241856 Case Report Carbon Ion Beam Radiotherapy for Sinonasal Malignant Tumors Invading Skull Base Nobuo Ohta,
Congenital Neck Masses C. Stefan Kénel-Pierre, MD
 Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
American Journal of. Cancer Case Reports
 American Journals of Cancer Case Reports http://ivyunion.org/index.php/ajccr/index Cancer Case Reports AK H et al. American Journal of Cancer Case Reports 2013, 1:93-97 Vol. 1, Article ID Page 201300216,
American Journals of Cancer Case Reports http://ivyunion.org/index.php/ajccr/index Cancer Case Reports AK H et al. American Journal of Cancer Case Reports 2013, 1:93-97 Vol. 1, Article ID Page 201300216,
A Case of Giant Mesenteric Cyst Originating from the Small Intestine
 Showa Univ J Med Sci 27 2, 125 129, June 2015 Case Report A Case of Giant Mesenteric Cyst Originating from the Small Intestine Takahiro UMEMOTO 1, Tetsuji WAKABAYASHI 1, Nobuyuki OHIKE 2, Ryuichi SEKINE
Showa Univ J Med Sci 27 2, 125 129, June 2015 Case Report A Case of Giant Mesenteric Cyst Originating from the Small Intestine Takahiro UMEMOTO 1, Tetsuji WAKABAYASHI 1, Nobuyuki OHIKE 2, Ryuichi SEKINE
Disclosures. The Thin Red Line Between Neuropathology and Head & Neck Pathology. Introduction CASE 1. Current Issues Tihan
 Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Case Scenario 1. 2/15/2011 The patient received IMRT 45 Gy at 1.8 Gy per fraction for 25 fractions.
 Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Scenario 1 1/3/11 A 57 year old white female presents for her annual mammogram and is found to have a suspicious area of calcification, spread out over at least 4 centimeters. She is scheduled to
Case Studies in Sella/Parasellar Region. Child thirsty, increased urination. Imaging. Suprasellar Germ Cell Tumor (Germinoma) No Disclosures
 Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
SPECIAL PAPER IN CELEBRATION OF PROF. YANG'S 50 YEARS CAREER IN MEDICINE
 JOURNAL OF OTOLOGY SPECIAL PAPER IN CELEBRATION OF PROF. YANG'S 50 YEARS CAREER IN MEDICINE ADVANCES IN SURGICAL TREATMENT OF ACOUSTIC NEUROMA HAN Dongyi,CAI Chaochan Acoustic Neuroma (AN) arises from
JOURNAL OF OTOLOGY SPECIAL PAPER IN CELEBRATION OF PROF. YANG'S 50 YEARS CAREER IN MEDICINE ADVANCES IN SURGICAL TREATMENT OF ACOUSTIC NEUROMA HAN Dongyi,CAI Chaochan Acoustic Neuroma (AN) arises from
Pure Intracavernous Sinus Epidermoid Cyst: Diffusion-Weighted (DW) and Constructive Interference in Steady State (CISS) Images 1
 Pure Intracavernous Sinus Epidermoid Cyst: Diffusion-Weighted (DW) and Constructive Interference in Steady State (CISS) Images 1 Suk Jin Park, M.D., In Kyu Yu, M.D., Min Sun Kim, M.D., Hyeon Mi Yoo, M.D.,
Pure Intracavernous Sinus Epidermoid Cyst: Diffusion-Weighted (DW) and Constructive Interference in Steady State (CISS) Images 1 Suk Jin Park, M.D., In Kyu Yu, M.D., Min Sun Kim, M.D., Hyeon Mi Yoo, M.D.,
Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor
 Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
Case Reports in Medicine Volume 2015, Article ID 742920, 4 pages http://dx.doi.org/10.1155/2015/742920 Case Report A Rare Cutaneous Adnexal Tumor: Malignant Proliferating Trichilemmal Tumor Omer Alici,
NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE
 THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
THE UNIVERSITY OF NORTH CAROLINA at CHAPEL HILL SEPTEMBER 2013 NEURORADIOLOGY-NEUROPATHOLOGY CONFERENCE Claudia da Costa Leite, MD, PhD Thomas Bouldin, MD CASE 1 6 y-o female with headaches and vomiting
Nasopharynx. 1. Introduction. 1.1 General Information and Aetiology
 Nasopharynx 1. Introduction 1.1 General Information and Aetiology The nasopharynx is the uppermost, nasal part of the pharynx. It extends from the base of the skull to the upper surface of the soft palate.
Nasopharynx 1. Introduction 1.1 General Information and Aetiology The nasopharynx is the uppermost, nasal part of the pharynx. It extends from the base of the skull to the upper surface of the soft palate.
Nasopharyngeal Carcinoma. Rusty Stevens, MD Christopher Rassekh, MD
 Nasopharyngeal Carcinoma Rusty Stevens, MD Christopher Rassekh, MD Introduction Rare in the US, more common in Asia High index of suspicion required for early diagnosis Nasopharyngeal malignancies SCCA
Nasopharyngeal Carcinoma Rusty Stevens, MD Christopher Rassekh, MD Introduction Rare in the US, more common in Asia High index of suspicion required for early diagnosis Nasopharyngeal malignancies SCCA
Breast Cancer Diagnosis, Treatment and Follow-up
 Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Breast Cancer Diagnosis, Treatment and Follow-up What is breast cancer? Each of the body s organs, including the breast, is made up of many types of cells. Normally, healthy cells grow and divide to produce
Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences
 Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences Describe the typical imaging findings of GIST at initial
Imaging of Gastrointestinal Stromal Tumors (GIST) Amir Reza Radmard, MD Assistant Professor Shariati hospital Tehran University of Medical Sciences Describe the typical imaging findings of GIST at initial
Head & Neck Clinical Sub Group. Network Agreed Imaging Guidelines for UAT and Thyroid Cancer. Measure Nos: 11-1C-105i & 11-1C-106i
 Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
CASE REPORT What Is It? A Rare Presentation of a Meningioma
 CASE REPORT What Is It? A Rare Presentation of a Meningioma Matthew A. Applebaum, MS, a Connor Barnes, MD, b and Michael Harrington, MD MPH b a University of South Florida Morsani College of Medicine,
CASE REPORT What Is It? A Rare Presentation of a Meningioma Matthew A. Applebaum, MS, a Connor Barnes, MD, b and Michael Harrington, MD MPH b a University of South Florida Morsani College of Medicine,
Cranium eroding sweat gland carcinoma: a case report
 Cranium eroding sweat gland carcinoma: a case report Mehmet Arslan, Ahmet N. Karadeniz, Görkem Aksu, Murat Güveli Istanbul University, Institute of Oncology, Istanbul, Turkey Background. Sweat gland carcinomas
Cranium eroding sweat gland carcinoma: a case report Mehmet Arslan, Ahmet N. Karadeniz, Görkem Aksu, Murat Güveli Istanbul University, Institute of Oncology, Istanbul, Turkey Background. Sweat gland carcinomas
ISPUB.COM. Breast Angiosarcoma. C Lilaia, F Pereira, S André, B Cabrita INTRODUCTION CASE REPORT
 ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 6 Number 2 C Lilaia, F Pereira, S André, B Cabrita Citation C Lilaia, F Pereira, S André, B Cabrita.. The Internet Journal of Gynecology
ISPUB.COM The Internet Journal of Gynecology and Obstetrics Volume 6 Number 2 C Lilaia, F Pereira, S André, B Cabrita Citation C Lilaia, F Pereira, S André, B Cabrita.. The Internet Journal of Gynecology
Head and Neck Cancer. What is head and neck cancer?
 Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that usually originate in the squamous cells that line the mouth, nose and throat. Typical symptoms include a persistent
Scan for mobile link. Head and Neck Cancer Head and neck cancer is a group of cancers that usually originate in the squamous cells that line the mouth, nose and throat. Typical symptoms include a persistent
ONCOLOGY LETTERS 10: , 2015
 ONCOLOGY LETTERS 10: 749-753, 2015 Inability of PET/CT to identify a primary sinonasal inverted papilloma with squamous cell carcinoma in a patient with a submandibular lymph node metastasis: A case report
ONCOLOGY LETTERS 10: 749-753, 2015 Inability of PET/CT to identify a primary sinonasal inverted papilloma with squamous cell carcinoma in a patient with a submandibular lymph node metastasis: A case report
Imaging The Turkish Saddle. Russell Goodman, HMS III Dr. Gillian Lieberman
 Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Case Scenario 1. Pathology report Specimen from mediastinoscopy Final Diagnosis : Metastatic small cell carcinoma with residual lymphatic tissue
 Case Scenario 1 Oncology Consult: Patient is a 51-year-old male with history of T4N3 squamous cell carcinoma of tonsil status post concurrent chemoradiation finished in October two years ago. He was hospitalized
Case Scenario 1 Oncology Consult: Patient is a 51-year-old male with history of T4N3 squamous cell carcinoma of tonsil status post concurrent chemoradiation finished in October two years ago. He was hospitalized
Primary intracranial malignant melanoma: A case with review of literature
 ISSN (print form): 25931431 Primary intracranial malignant melanoma: A case with review of literature K.SAHRAOUI 1, M.A KAIM 2, K.BOUYOUCEF 3 ABSTRACT Introduction: Primary intracranial melanoma is an
ISSN (print form): 25931431 Primary intracranial malignant melanoma: A case with review of literature K.SAHRAOUI 1, M.A KAIM 2, K.BOUYOUCEF 3 ABSTRACT Introduction: Primary intracranial melanoma is an
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Adjuvant therapy for thyroid cancer
 Carcinoma of the thyroid Adjuvant therapy for thyroid cancer John Hay Department of Radiation Oncology Vancouver Cancer Centre Department of Surgery UBC 1% of all new malignancies 0.5% in men 1.5% in women
Carcinoma of the thyroid Adjuvant therapy for thyroid cancer John Hay Department of Radiation Oncology Vancouver Cancer Centre Department of Surgery UBC 1% of all new malignancies 0.5% in men 1.5% in women
Melanoma Case Scenario 1
 Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Melanoma Case Scenario 1 History and physical 11/5/16 Patient is a single, 48-year-old male in good health who presented to his primary physician for a yearly physical exam during which a 3.4 x 2.8 x 1.5
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT
 Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Maligna Melanoma and Atypical Fibroxanthoma: An Unusual Collision Tumour G Türkcü 1, A Keleş 1, U Alabalık 1, D Uçmak 2, H Büyükbayram 1 ABSTRACT Two different neoplasia in the same biopsy material called
Giant Epidermoid Cyst: A Rare Cause of Temporal Lobe Epilepsy
 THIEME Case Report e101 Giant Epidermoid Cyst: A Rare Cause of Temporal Lobe Epilepsy Vinicius Gomes Trindade 1 Marcos de Queiroz Teles Gomes 1 Marcelo Prudente do Espirito Santo 1 Manoel Jacobsen Teixeira
THIEME Case Report e101 Giant Epidermoid Cyst: A Rare Cause of Temporal Lobe Epilepsy Vinicius Gomes Trindade 1 Marcos de Queiroz Teles Gomes 1 Marcelo Prudente do Espirito Santo 1 Manoel Jacobsen Teixeira
