Predicting the risk of developing a radiationinduced second cancer when treating a primary cancer with radiation
|
|
|
- Lucinda Bryan
- 5 years ago
- Views:
Transcription
1 Remaining physics challenges in proton therapy Predicting the risk of developing a radiationinduced second cancer when treating a primary cancer with radiation H. Paganetti PhD Professor and Director of Physics Research Department of Radiation Oncology, Massachusetts General Hospital & Harvard Medical School,,
2 Disclosures Work funded by the National Cancer Institute P01 CA R01 CA R01 CA C06 CA
3 Massachusetts General Hospital, Boston ~800 patients t per year
4 Massachusetts General Hospital, Boston 79% 80% 70% 60% 50% 41% 40% 30% 21% 20% 15% 10% 10% 10% 0% 7% 8% 4% 2% 1% 2%
5 Introduction The Ideal Dose Distribution Do ose Photons BEAM Protons ideal Depth
6 Introduction Proton physics - The Bragg curve increase in de/dx as proton slows down Dose [%] depth [mm] includes contribution from secondary protons 1) Energy loss collisions with atomic electrons 2) Energy loss; fluence reduction nuclear interactions 3) Scattering multiple Coulomb scattering width due to range straggling
7 Introduction Spread-out Bragg Peak width thickness
8 Introduction Aperture and Compensator
9 Introduction Pencil Beam Scanning Pedroni, PSI potential for intensity-modulated proton therapy (IMPT)
10 Introduction Dose Photons Protons Protons IMRT Depth Main proton advantage 1: The integral dose difference : 2-3 Main proton advantage 2: The end of range
11 Remaining physics challenges in proton therapy Utilizing the integral dose advantage Predicting the range in the patient to within 1-3 mm Validating the dose in the patient
12 Integral dose IMRT plan (7 coplanar photon beams) Alex Trofimov, MGH
13 Integral dose IMPT plan (4 coplanar proton beams) Alex Trofimov, MGH
14 Integral dose Rhabdomyosarcoma of Paranasal Sinus (7 y old boy) 6 MV Photons (3 field) 160 MeV Protons oo (2 field) Photon Proton IMRT IMPT (9 field) (9 field) Alfred Smith (MDACC)
15 Integral dose In beam scanning, spot size matters! =12mm =12mm =3mm +aperture Depending on the beam characteristics, there are considerable differences between different proton beams (potentially showing inferiority compared to photon treatments) Maryam Moteabbed, MGH
16 Integral dose IMRT PBS 12mm PBS 12mm+AP PBS 3mm Rhabdomyosarcoma Total dose = 50.4 Gy Number of proton fields = 2 Number of IMRT fields = 5 Maryam Moteabbed, MGH
17 Patient with posterior fossa ependymoma
18 Integral dose Is the integral dose the decisive i parameter? Is a small volume of high dose better compared to a large volume of low dose? second cancer induction cognitive development in children (!)
19 Integral dose
20 Integral dose
21 Integral dose Note: NTCP considerations in treatment planning are based on photon dose distributions Organ doses in proton therapy are more heterogeneous. There are no proton specific normal tissue constraints
22 Integral dose Conclusion I: The total energy deposited in a patient ( integral dose ) is always lower when treating with protons. This, theoretically, should always result in an advantage for proton treatments. However, the dose distribution matters this may not always result in a significant clinical gain (site dependent; clinical trials?) the delivery system matters
23 Predicting the range Protons Medulloblastoma Photons Copyright MGH/NPTC 2003
24 Predicting the range The difference compared to photon therapy: range uncertainties symmetric margin expansion does not make sense!
25 Predicting the range Applied lidrange uncertainty tit margins for non-moving targets t MDACC, UPenn MGH UF H. Paganetti: Phys. Med. Biol. 57, R99-R117 (2012)
26 Predicting the range Applied lidrange uncertainty tit margins for non-moving targets t Source of range uncertainty in the patient Range uncertainty Independent of dose calculation: Measurement uncertainty in water for commissioning ± 0.3 mm Compensator design ± 0.2 mm Beam reproducibility ± 0.2 mm Patient setup ± 0.7 mm Dose calculation: Biology (always positive) % CT imaging and calibration ±05% 0.5 CT conversion to tissue (excluding I-values) ± 0.5 % CT grid size ± 0.3 % Mean excitation energies (I-values) in tissue ± 1.5 % Range degradation; d complex ih inhomogeneities ii - 07% 0.7 Range degradation; local lateral inhomogeneities * ± 2.5 % Total (excluding *) 2.7% mm Total 4.6% mm H. Paganetti: Phys. Med. Biol. 57, R99-R107 (2012)
27 Predicting the range Range degradation Type I (Sawakuchi et al., 2008)
28 Predicting the range Range degradation Type II analytical Monte Carlo 008) netti et al., 20 (Pagan
29 Predicting the range Applied lidrange uncertainty tit margins for non-moving targets t 2.7%+1.2mm bad beam angle in complex geometry typical scenario H. Paganetti: Phys. Med. Biol. 57, R99-R117 (2012)
30 Predicting the range Source of range uncertainty in the patient Range uncertainty Independent of dose calculation: Measurement uncertainty in water for commissioning ± 0.3 mm Compensator design ± mm Beam reproducibility ± 0.2 mm Patient setup ± 0.7 mm Dose calculation: Biology (always positive) % CT imaging and calibration ± 0.5 % CT conversion to tissue (excluding I-values) ± 0.5 % CT grid size ± 0.3 % Mean excitation energies (I-values) in tissue ± 1.5 % Range degradation; complex inhomogeneities % Range degradation; local lateral inhomogeneities * ± 2.5 % Total (excluding *) 27%+12mm 2.7% 1.2 Total 4.6% mm ± 0.2 % ± 0.1 % ± 0.1 % 2.4 % mm H. Paganetti: Range uncertainties in proton beam therapy and the impact of Monte Carlo simulations Phys. Med. Biol. 57: R99-R117 (2012)
31 Predicting the range 4 mm gain! H. Paganetti: Range uncertainties in proton beam therapy and the impact of Monte Carlo simulations Phys. Med. Biol. 57: R99-R117 (2012)
32 Predicting the range Medduloblastoma Patient Proton Dose_XiO Proton Dose_TOPAS Dose_Difference Avg. range differe nce (mm) XiO_TOPAS_Water P1 P2 P3 P4 P5 P6 P7 P8 P9 P10 P11 P12 Patient number Avg. range differe ence (mm) P1 P2 P3 P4 P5 P6 P7 P8 P9 P10 P11 P12 Patient number RMSD (mm m) P1 P2 P3 P4 P5 P6 P7 P8 P9 P10 P11 P12 Patient number
33 Predicting the range Head & Neck Patient Avg. range differen nce (mm) Proton Dose_XiO XiO_TOPAS_Water 1.0 Head&Neck_water_dose P1 P2 P3 P4 P5 P6 P7 P8 P9 P10 P11 P12 Patient number Avg. range differen nce (mm) Proton Dose_TOPAS 5 Head&Neck_patient_dose P1 P2 P3 P4 P5 P6 P7 P8 P9 P10 P11 P12 Patient number RMSD (mm m) Dose_Difference 10 Head&Neck_patient_dose P1 P2 P3 P4 P5 P6 P7 P8 P9 P10 P11 P12 Patient number
34 Predicting the range Note: In proton therapy, generic margin recipes are not sufficient! Advanced dose calculation only solves part of the problem
35 Predicting the range In addition(!): () patient geometry changes Example: Intra-fractional geometry changes Before RT After RT Parotid glands E. M. Vasques Osorio et al. IJROBP 70: Subm.glands Tumor
36 Predicting the range In addition(!): () patient geometry changes Patient weight gain / loss Filling up of sinuses (Sub-clinical) pneumonia Wet hair / gel / hairspray Lei Dong, MDACC
37 Predicting the range Mitigating range uncertainties using robust planning in IMPT Beam 1 Beam 2 Beam 3 Total dose: Unkelbach, MGH
38 Predicting the range Mitigating range uncertainties using robust planning in IMPT Beam 1 Beam 2 Beam 3 Total dose: Unkelbach, MGH
39 Predicting the range Measuring range using the ratio of two point doses Partial distributions for field pair Ratio function (b) () (a)
40 Predicting the range Range adjustment for adaptive delivery D (x) = D a (x) + D b (x) + D c (x) Dosimeter Position Dosimeter + Position + Deliver field a Measure dose D a Deliver field b Measure dose D b Calculate ratio R=D a /D b Drive WEPL of dosimeter Design subfield c (magenta) Deliver c. => Total distribution (black) has the correct range
41 Predicting the range Technical Characteristics 12 cm Number of diodes: 249 Time resolution: ~ 2 msec Pitch: ~ 10 mm Manufacturer: Sun Nuclear Applications Check the patient positioning Monitor patient morphological change (Range verification) Pre treatment Range Tuning (Cranial field Medulloblastoma)
42 Predicting the range 1. Pattern Matching Technique Minimization of the least-squares difference between measured profiles and Data Base 2. rms width (σ t ) fitting technique??? Depth =??? H M. Lu Phys. Med. Bio. 53 (2008) ; B. Gottschalk et. al. Med. Phys. 38 (4), April 2011
43 Predicting the range SOBP Range90: 20 cm Mod98: 20 cm P.I. Database
44 Predicting the range Esophagus sparing Range pullback of 4 mm for all patients
45 Predicting the range In-Vivo Range Check i (t) 1) Pedi patient under anesthesia 2) Insert esophageal dosimeter (diodes) 3) Turn on range check beam for < 1 cgy 4) Measure dose rate as function of time 5) Calculate water equivalent path length 6) Compare with treatment t t planning 7) Adjust beam range for treatment 8) Record dose delivered to esophagus 9) Only needed during 1 st treatment
46 Predicting the range Range uncertainties sometimes limit our ability to exploit the end of range and thus negate some of the potential advantages of proton therapy Example: Prostate treatments
47 Predicting the range Protons and Prostate Treatments Current technique: Lateral fields Use lateral penumbra (10 mm, 50-95%) to spare rectum (penumbra not better than 15 MV photon fields) Why not AP fields? Use much sharper distal penumbra (~ 4 mm, 50-95%) AP LAT Hsiao-Ming Lu, MGH
48 Predicting the range Effect of 5 mm Range Variation R=129mm -5mm +5mm Correct Range Undershooting Overshooting Hsiao-Ming Lu, MGH
49 Predicting the range 1) Use balloon with detector array embedded d on the surface 2) Deliver dose (< 1 cgy) for 500 ms using a few cm of extra beam range to cover dosimeters 3) Measure dose rate functions by a multi-channel electrometer 4) Match data with ruler to determine WEPL at dosimeters 5) Compare with planning calculations to adjust beam range 6) Commence treatment and measure distal tail dose by dosimeters as verification
50 Predicting the range Conclusion II: Proton treatment planning needs to be done by experienced planners who understand the impact of range uncertainties. For some sites (e.g. prostate) range uncertainties prevent us from exploiting the full potential of proton therapy. In vivo systems can potentially be used to validate the range
51 Validating the range p 12 C p n 11 C β + ν 11 B e 16 O(p,3p3n) 11 C 16 O(p,pn) 15 O 16 O(p,2p2n) 13 N 12 C(p,pn) 11 C Nucleus of tissue Target fragment A(z) D(z) Measured Activity has to be compared with calculation
52 Validating the range From treatment position into PET scanner Start scan within 2 minutes after treatment Isotope Half life (min) 15 O C N 9.96
53 Validating the range Patient s PET scan In room PET Listmode rawdata Reconstruction 3D OSEM PET+CT Measured PET In room PET scan just after irradiation Monte Carlo Simulation Comparison Dose and PET calculation with nozzle and CT Geant4 Fluence Cross Sections 11 C 15 O MATLAB Decay Washout Blurrring Normalization Simulated PET
54 Validating the range Monte Carlo Dose Tre atment Planning Dose Monte Carlo PET Measured PET K. Parodi, H. Paganetti, H.A. Shih, et al. Int. J. Radiat. Oncol. Biol. Phys. 68, (2007)
55 Validating the range Mea asured current accuracy in soft tissue ~5mm current accuracy in bone ~2mm Mon nte Carlo Shift
56 Validating the range PET Surface Comparison Lateral dis stance (mm) Meas. PET Surface Lateral distance (mm) Range (mm) Lateral dis stance (mm) MC PET Surface Lateral distance (mm) Range (mm) Lateral dista ance (mm) PET Surface Difference Distal Surface - PET Lateral distance (mm) Difference (mm) Avg. Difference n n ( X meas, i X mc, i) X meas, i X mc, i i 1 i 1 n RMSD ( ) n 2 -X meas,i = reference range of measured PET, X mc,i = reference range of MC PET - Reference range = midpoint of 50% and 25% location of maximum PET activity. - Avg. Difference = average difference in reference ranges of measured and simulated PET. - RMSD = root-mean-square deviation over PET surfaces.
57 Validating the range Avg. range difference e (mm) Case_1 Case_2 Case_3 Case_4 Case_5 Case_6 Case_7 Case_ Scan time (min) are deviatio on (mm) Root- -mean-squ Case_1 Case_2 Case_3 Case_4 Case_5 Case_6 Case_7 Case_ Scan time (min) The uncertainty t in range verification using PET does not decrease further after ~5 min of scan time In-room PET scanner is currently being replaced by in-room PET/CT
58 Validating the range Higher sensitivity - Acquisition time of 2-3 min Higher spatial resolution mm (In-room PET) vs. 2.0 mm (In-room PET/CT) CT component for accurate image co-registration - One of the largest technical obstaclesisthecoregistration the co-registration accuracy between PET and CT image
59 Validating the range Prompt gamma radiation
60 Validating the range DOSE PromptGamma PET M. Moteabbed, S. España, H. Paganetti Phys. Med. Biol. 56, (2011)
61 Validating the range Results Prompt Gamma analysis; Adenoid cystic c. - Beam scanning -
62 Validating the range Published Results
63 Validating the range After radiation exposure, vertebral bone marrow undergoes fatty replacement T-1 weighted spin-echo sequence Overall dose-signal intensity derived from the lateral penumbra in the sacrum Gensheimer M F, Yock T I, Liebsch N J, Sharp G C, Paganetti H, Madan N, Grant P E and Bortfeld T 2010 Int J Radiat Oncol Biol Phys
64 Validating the range planned 50% isodose MRI 50% isodose
65 Validating the range
66 Validating the range Conclusion III: Proton therapy offers unique imaging capabilities due to nuclear interactions in tissues The highly conformal dose distributions in proton therapy offer the potential of outcome imaging
67 SUMMARY The physical characteristics of proton beams cause dosimetric advantages compared to photon beams results in unique dosimetric uncertainties offer unique imaging i and adaptive therapy strategies t uncertainties in predicting the proton beam range in patients are ~3-5% (~2.5% with advanced dose calculation methods) uncertainties can be mitigated in (robust) IMPT optimization In vivo detectors might allow to adjust the range unique in vivo dose (range) verification methods (PET, prompt- gamma, MRI) are being worked on
68 Acknowledgements Physics Research and Physics Translational Research at Massachusetts General Hospital Radiation Oncology
Range Uncertainties in Proton Therapy
 Range Uncertainties in Proton Therapy Harald Paganetti PhD Professor of Radiation Oncology, Harvard Medical School Director of Physics Research, Massachusetts General Hospital, Department of Radiation
Range Uncertainties in Proton Therapy Harald Paganetti PhD Professor of Radiation Oncology, Harvard Medical School Director of Physics Research, Massachusetts General Hospital, Department of Radiation
Treatment Planning (Protons vs. Photons)
 Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Treatment Planning Treatment Planning (Protons vs. Photons) Acquisition of imaging data Delineation of regions of interest Selection of beam directions Dose calculation Optimization of the plan Hounsfield
Discuss the general planning concepts used in proton planning. Review the unique handling of CTV / ITV / PTV when treating with protons
 Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
Mark Pankuch, PhD Discuss the general planning concepts used in proton planning Review the unique handling of CTV / ITV / PTV when treating with protons Pencil Beam distributions and PBS optimization Cover
IN VIVO IMAGING Proton Beam Range Verification With PET/CT
 IN VIVO IMAGING Proton Beam Range Verification With PET/CT Antje-Christin Knopf 1/3 K Parodi 2, H Paganetti 1, T Bortfeld 1 Siemens Medical Solutions Supports This Project 1 Department of Radiation Oncology,
IN VIVO IMAGING Proton Beam Range Verification With PET/CT Antje-Christin Knopf 1/3 K Parodi 2, H Paganetti 1, T Bortfeld 1 Siemens Medical Solutions Supports This Project 1 Department of Radiation Oncology,
Proton Stereotactic Radiotherapy: Clinical Overview. Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS
 Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
Proton Stereotactic Radiotherapy: Clinical Overview Brian Winey, Ph.D. Physicist, MGH Assistant Professor, HMS Acknowledgements Radiation Oncologists and Physicists at various institutions (MGH, MDACC,
Hampton University Proton Therapy Institute
 Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
Hampton University Proton Therapy Institute Brief introduction to proton therapy technology, its advances and Hampton University Proton Therapy Institute Vahagn Nazaryan, Ph.D. Executive Director, HUPTI
Topics covered 7/21/2014. Radiation Dosimetry for Proton Therapy
 Radiation Dosimetry for Proton Therapy Narayan Sahoo Department of Radiation Physics University of Texas MD Anderson Cancer Center Proton Therapy Center Houston, USA Topics covered Detectors used for to
Radiation Dosimetry for Proton Therapy Narayan Sahoo Department of Radiation Physics University of Texas MD Anderson Cancer Center Proton Therapy Center Houston, USA Topics covered Detectors used for to
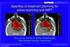
Considerations when treating lung cancer with passive scatter or active scanning proton therapy
 Mini-Review Considerations when treating lung cancer with passive scatter or active scanning proton therapy Sara St. James, Clemens Grassberger, Hsiao-Ming Lu Department of Radiation Oncology, Massachusetts
Mini-Review Considerations when treating lung cancer with passive scatter or active scanning proton therapy Sara St. James, Clemens Grassberger, Hsiao-Ming Lu Department of Radiation Oncology, Massachusetts
Protons Monte Carlo water-equivalence study of two PRESAGE formulations for proton beam dosimetry J. Phys.: Conf. Ser.
 Protons Monte Carlo water-equivalence study of two PRESAGE formulations for proton beam dosimetry T Gorjiara, Z Kuncic, J Adamovics and C Baldock 2013 J. Phys.: Conf. Ser. 444 012090 PRESAGE is a radiochromic
Protons Monte Carlo water-equivalence study of two PRESAGE formulations for proton beam dosimetry T Gorjiara, Z Kuncic, J Adamovics and C Baldock 2013 J. Phys.: Conf. Ser. 444 012090 PRESAGE is a radiochromic
8/1/2016. Motion Management for Proton Lung SBRT. Outline. Protons and motion. Protons and Motion. Proton lung SBRT Future directions
 Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
Motion Management for Proton Lung SBRT AAPM 2016 Outline Protons and Motion Dosimetric effects Remedies and mitigation techniques Proton lung SBRT Future directions Protons and motion Dosimetric perturbation
Overview. Proton Therapy in lung cancer 8/3/2016 IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS
 IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS Heng Li, PhD Assistant Professor, Department of Radiation Physics, UT MD Anderson Cancer Center, Houston, TX, 773
IMPLEMENTATION OF PBS PROTON THERAPY TREATMENT FOR FREE BREATHING LUNG CANCER PATIENTS Heng Li, PhD Assistant Professor, Department of Radiation Physics, UT MD Anderson Cancer Center, Houston, TX, 773
Clinical considerations of RBE in proton therapy
 Clinical considerations of RBE in proton therapy H. Paganetti PhD Professor, Harvard Medical School Director of Physics Research, Massachusetts General Hospital, Radiation Oncology Why do we need the RBE
Clinical considerations of RBE in proton therapy H. Paganetti PhD Professor, Harvard Medical School Director of Physics Research, Massachusetts General Hospital, Radiation Oncology Why do we need the RBE
doi: /j.ijrobp
 doi:10.1016/j.ijrobp.2010.08.006 Int. J. Radiation Oncology Biol. Phys., Vol. 80, No. 3, pp. 928 937, 2011 Copyright Ó 2011 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
doi:10.1016/j.ijrobp.2010.08.006 Int. J. Radiation Oncology Biol. Phys., Vol. 80, No. 3, pp. 928 937, 2011 Copyright Ó 2011 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
Correction of Prompt Gamma Distribution for Improving Accuracy of Beam Range Determination in Inhomogeneous Phantom
 Original Article PMP Progress in Medical Physics 28(4), December 217 https://doi.org/1.14316/pmp.217.28.4.27 pissn 258-4445, eissn 258-4453 Correction of Prompt Gamma Distribution for Improving Accuracy
Original Article PMP Progress in Medical Physics 28(4), December 217 https://doi.org/1.14316/pmp.217.28.4.27 pissn 258-4445, eissn 258-4453 Correction of Prompt Gamma Distribution for Improving Accuracy
Treatment Planning for Skull Base Tumors PTCOG 52, June 2013
 Treatment Planning for Skull Base Tumors PTCOG 52, June 2013 Judy Adams CMD Hanne Kooy Ph.D, Norbert Liebsch MD Department of Radiation Oncology Massachusetts General Hospital Chordomas and Chondrosarcomas
Treatment Planning for Skull Base Tumors PTCOG 52, June 2013 Judy Adams CMD Hanne Kooy Ph.D, Norbert Liebsch MD Department of Radiation Oncology Massachusetts General Hospital Chordomas and Chondrosarcomas
Specifics of treatment planning for active scanning and IMPT
 Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Specifics of treatment planning for active scanning and IMPT SFUD IMPT Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Treatment planning for scanning 1. Single Field,
Andrew K. Lee, MD, MPH Associate Professor Department tof fradiation Oncology M.D. Anderson Cancer Center
 Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Associate Professor Department tof fradiation Oncology M.D. Anderson Cancer Center Seungtaek Choi, MD Assistant Professor Department tof fradiation
Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Associate Professor Department tof fradiation Oncology M.D. Anderson Cancer Center Seungtaek Choi, MD Assistant Professor Department tof fradiation
Proton Beam Therapy at Mayo Clinic
 Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
Proton Beam Therapy at Mayo Clinic Jon J. Kruse, Ph.D. Mayo Clinic Dept. of Radiation Oncology Rochester, MN History of Proton Therapy at Mayo 2002: Decided to consider particle therapy analysis and education
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
State-of-the-art proton therapy: The physicist s perspective
 State-of-the-art proton therapy: Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Overview of presentation 1. State-of-the-art proton delivery 2. Current challenges 3. New
State-of-the-art proton therapy: Tony Lomax, Centre for Proton Radiotherapy, Paul Scherrer Institute, Switzerland Overview of presentation 1. State-of-the-art proton delivery 2. Current challenges 3. New
8/3/2016. Clinical Significance of RBE Variations in Proton Therapy. Why RBE (relative biological effectiveness)?
 8//06 Clinical Significance of Variations in Proton Therapy H. Paganetti PhD Professor, Harvard Medical School Director of Physics Research, Massachusetts General Hospital, Radiation Oncology Introduction
8//06 Clinical Significance of Variations in Proton Therapy H. Paganetti PhD Professor, Harvard Medical School Director of Physics Research, Massachusetts General Hospital, Radiation Oncology Introduction
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
 Interfractional Variations in the Setup of Pelvic Bony Anatomy and Soft Tissue, and Their Implications on the Delivery of Proton Therapy for Localized Prostate Cancer The Harvard community has made this
Interfractional Variations in the Setup of Pelvic Bony Anatomy and Soft Tissue, and Their Implications on the Delivery of Proton Therapy for Localized Prostate Cancer The Harvard community has made this
Image Guided Proton Therapy and Treatment Adaptation
 Image Guided Proton Therapy and Treatment Adaptation www.hollandptc.nl d.r.schaart@tudelft.nl Cancer in The Netherlands About 1 in 3 people get cancer in some stage of their life 86.800 new cancer patients
Image Guided Proton Therapy and Treatment Adaptation www.hollandptc.nl d.r.schaart@tudelft.nl Cancer in The Netherlands About 1 in 3 people get cancer in some stage of their life 86.800 new cancer patients
Medical physics is beautiful
 Translational research in particle therapy Marco Durante Medical physics is beautiful Pisa, 31.10.2014 Relative dose 1. 2 1. 0 Tumor Durante & Loeffler, Nature Rev Clin Oncol 2010 0. 8 Normal tissue 0.
Translational research in particle therapy Marco Durante Medical physics is beautiful Pisa, 31.10.2014 Relative dose 1. 2 1. 0 Tumor Durante & Loeffler, Nature Rev Clin Oncol 2010 0. 8 Normal tissue 0.
Advances in external beam radiotherapy
 International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
International Conference on Modern Radiotherapy: Advances and Challenges in Radiation Protection of Patients Advances in external beam radiotherapy New techniques, new benefits and new risks Michael Brada
8/3/2016. Implementation of Pencil Beam Scanning (PBS) Proton Therapy Treatment for Liver Patients. Acknowledgement. Overview
 Implementation of Pencil Beam Scanning (PBS) Proton Therapy Treatment for Liver Patients Liyong Lin, PhD, Assistant Professor Department of Radiation Oncology University of Pennsylvania Acknowledgement
Implementation of Pencil Beam Scanning (PBS) Proton Therapy Treatment for Liver Patients Liyong Lin, PhD, Assistant Professor Department of Radiation Oncology University of Pennsylvania Acknowledgement
Robust Optimization accounting for Uncertainties
 Robust Optimization accounting for Uncertainties Thomas Bortfeld Massachusetts General Hospital, Boston tbortfeld@mgh.harvard.edu Supported by: RaySearch Philips Medical Systems Outline 1. Optimality and
Robust Optimization accounting for Uncertainties Thomas Bortfeld Massachusetts General Hospital, Boston tbortfeld@mgh.harvard.edu Supported by: RaySearch Philips Medical Systems Outline 1. Optimality and
Proton and helium beams: the present and the future of light ion beam therapy
 Proton and helium beams: the present and the future of light ion beam therapy Dr. Andrea Mairani Group Leader Biophysics in Particle Therapy Heidelberg Ion Beam Therapy Center HIT Department of Radiation
Proton and helium beams: the present and the future of light ion beam therapy Dr. Andrea Mairani Group Leader Biophysics in Particle Therapy Heidelberg Ion Beam Therapy Center HIT Department of Radiation
Learning Objectives. Clinically operating proton therapy facilities. Overview of Quality Assurance in Proton Therapy. Omar Zeidan
 Overview of Quality Assurance in Proton Therapy Omar Zeidan AAPM 2012 Charlotte, NC July 30 st, 2012 Learning Objectives Understand proton beam dosimetry characteristics and compare them to photon beams
Overview of Quality Assurance in Proton Therapy Omar Zeidan AAPM 2012 Charlotte, NC July 30 st, 2012 Learning Objectives Understand proton beam dosimetry characteristics and compare them to photon beams
The Rise, Fall, and Rise Again of Proton Therapy or Never count out a well-financed therapy
 The Rise, Fall, and Rise Again of Proton Therapy or Never count out a well-financed therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School
The Rise, Fall, and Rise Again of Proton Therapy or Never count out a well-financed therapy Anthony Zietman MD Shipley Professor of Radiation Oncology Massachusetts General Hospital Harvard Medical School
Additional Questions for Review 2D & 3D
 Additional Questions for Review 2D & 3D 1. For a 4-field box technique, which of the following will deliver the lowest dose to the femoral heads? a. 100 SSD, equal dmax dose to all fields b. 100 SSD, equal
Additional Questions for Review 2D & 3D 1. For a 4-field box technique, which of the following will deliver the lowest dose to the femoral heads? a. 100 SSD, equal dmax dose to all fields b. 100 SSD, equal
Limits of Precision and Accuracy of Radiation Delivery Systems
 Limits of Precision and Accuracy of Radiation Delivery Systems Jean M. Moran, Ph.D. 1 and Timothy Ritter, Ph.D. 2 1 University of Michigan, Ann Arbor, Michigan 2 Ann Arbor Veterans Affairs Hospital, Ann
Limits of Precision and Accuracy of Radiation Delivery Systems Jean M. Moran, Ph.D. 1 and Timothy Ritter, Ph.D. 2 1 University of Michigan, Ann Arbor, Michigan 2 Ann Arbor Veterans Affairs Hospital, Ann
Future upcoming technologies and what audit needs to address
 Future upcoming technologies and what audit needs to address Dr R.I MacKay History of audit Absolute dose - Simple phantom standard dose measurement Point doses in beams - Phantoms of relatively simple
Future upcoming technologies and what audit needs to address Dr R.I MacKay History of audit Absolute dose - Simple phantom standard dose measurement Point doses in beams - Phantoms of relatively simple
Future Directions in Prostate Cancer: The Case for Protons. John J. Coen, MD Helen & Harry Gray Cancer Center
 Future Directions in Prostate Cancer: The Case for Protons John J. Coen, MD Helen & Harry Gray Cancer Center November 14, 2012 Protons and prostate cancer Early proton experience at the MGH The case for
Future Directions in Prostate Cancer: The Case for Protons John J. Coen, MD Helen & Harry Gray Cancer Center November 14, 2012 Protons and prostate cancer Early proton experience at the MGH The case for
Proton Therapy for Prostate Cancer. Andrew K. Lee, MD, MPH Director Proton Therapy Center
 Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director Proton Therapy Center Disclosures No relevant financial disclosures This presentation will not discuss off-label or investigational treatments
Proton Therapy for Prostate Cancer Andrew K. Lee, MD, MPH Director Proton Therapy Center Disclosures No relevant financial disclosures This presentation will not discuss off-label or investigational treatments
Martin Stuschke 1,2*, Andreas Kaiser 1,2, Jehad Abu Jawad 1, Christoph Pöttgen 1, Sabine Levegrün 1 and Jonathan Farr 2,3
 Stuschke et al. Radiation Oncology 2013, 8:145 SHORT REPORT Open Access Multi-scenario based robust intensity-modulated proton therapy (IMPT) plans can account for set-up errors more effectively in terms
Stuschke et al. Radiation Oncology 2013, 8:145 SHORT REPORT Open Access Multi-scenario based robust intensity-modulated proton therapy (IMPT) plans can account for set-up errors more effectively in terms
This content has been downloaded from IOPscience. Please scroll down to see the full text.
 This content has been downloaded from IOPscience. Please scroll down to see the full text. Download details: IP Address: 148.251.232.83 This content was downloaded on 25/11/2018 at 15:28 Please note that
This content has been downloaded from IOPscience. Please scroll down to see the full text. Download details: IP Address: 148.251.232.83 This content was downloaded on 25/11/2018 at 15:28 Please note that
Accuracy Requirements and Uncertainty Considerations in Radiation Therapy
 Departments of Oncology and Medical Biophysics Accuracy Requirements and Uncertainty Considerations in Radiation Therapy Introduction and Overview 6 August 2013 Jacob (Jake) Van Dyk Conformality 18 16
Departments of Oncology and Medical Biophysics Accuracy Requirements and Uncertainty Considerations in Radiation Therapy Introduction and Overview 6 August 2013 Jacob (Jake) Van Dyk Conformality 18 16
From position verification and correction to adaptive RT Adaptive RT and dose accumulation
 From position verification and correction to adaptive RT Adaptive RT and dose accumulation Hans de Boer Move away from Single pre-treatment scan Single treatment plan Treatment corrections by couch shifts
From position verification and correction to adaptive RT Adaptive RT and dose accumulation Hans de Boer Move away from Single pre-treatment scan Single treatment plan Treatment corrections by couch shifts
Assistant Professor Department of Therapeutic Radiology Yale University School of Medicine
 A Mechanism-Based Approach to Predict Relative Biological i Effectiveness and the Effects of Tumor Hypoxia in Charged Particle Radiotherapy David J. Carlson, Ph.D. Assistant Professor Department of Therapeutic
A Mechanism-Based Approach to Predict Relative Biological i Effectiveness and the Effects of Tumor Hypoxia in Charged Particle Radiotherapy David J. Carlson, Ph.D. Assistant Professor Department of Therapeutic
Figure 1.1 PHITS geometry for PTB irradiations with: broad beam, upper panel; mono energetic beams, lower panel. Pictures of the setups and of the
 Figure 1.1 PHITS geometry for PTB irradiations with: broad beam, upper panel; mono energetic beams, lower panel. Pictures of the setups and of the PMMA ring holder with 7 containers are also shown. Relative
Figure 1.1 PHITS geometry for PTB irradiations with: broad beam, upper panel; mono energetic beams, lower panel. Pictures of the setups and of the PMMA ring holder with 7 containers are also shown. Relative
Proton and heavy ion radiotherapy: Effect of LET
 Proton and heavy ion radiotherapy: Effect of LET As a low LET particle traverses a DNA molecule, ionizations are far apart and double strand breaks are rare With high LET particles, ionizations are closer
Proton and heavy ion radiotherapy: Effect of LET As a low LET particle traverses a DNA molecule, ionizations are far apart and double strand breaks are rare With high LET particles, ionizations are closer
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy
 Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti M. Bruzzi,M. Bucciolini, L. Marrazzo, D. Menichelli University of
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti M. Bruzzi,M. Bucciolini, L. Marrazzo, D. Menichelli University of
Independent Dose Verification for IMRT Using Monte Carlo. C-M M Charlie Ma, Ph.D. Department of Radiation Oncology FCCC, Philadelphia, PA 19111, USA
 Independent Dose Verification for IMRT Using Monte Carlo C-M M Charlie Ma, Ph.D. Department of Radiation Oncology FCCC, Philadelphia, PA 19111, USA Outline Why Monte Carlo for IMRT QA? Experimental verification
Independent Dose Verification for IMRT Using Monte Carlo C-M M Charlie Ma, Ph.D. Department of Radiation Oncology FCCC, Philadelphia, PA 19111, USA Outline Why Monte Carlo for IMRT QA? Experimental verification
Biological Optimization of Hadrontherapy. Uwe Oelfke
 4/2/2012 page 1 Biological Optimization of Hadrontherapy Uwe Oelfke DKFZ Heidelberg (E040) Im Neuenheimer Feld 280 69120 Heidelberg, Germany u.oelfke@dkfz.de 4/2/2012 page 2 Contents Introduction and General
4/2/2012 page 1 Biological Optimization of Hadrontherapy Uwe Oelfke DKFZ Heidelberg (E040) Im Neuenheimer Feld 280 69120 Heidelberg, Germany u.oelfke@dkfz.de 4/2/2012 page 2 Contents Introduction and General
Ion radiography as a tool for patient set-up & image guided particle therapy: a Monte Carlo study
 University of Wollongong Research Online Faculty of Engineering and Information Sciences - Papers: Part A Faculty of Engineering and Information Sciences 2014 Ion radiography as a tool for patient set-up
University of Wollongong Research Online Faculty of Engineering and Information Sciences - Papers: Part A Faculty of Engineering and Information Sciences 2014 Ion radiography as a tool for patient set-up
Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana
 University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
University of Groningen Potential benefits of intensity-modulated proton therapy in head and neck cancer van de Water, Tara Arpana IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's
Introduction. Measurement of Secondary Radiation for Electron and Proton Accelerators. Introduction - Photons. Introduction - Neutrons.
 Measurement of Secondary Radiation for Electron and Proton Accelerators D. Followill, Ph.D. Radiological Physics Center U. T. M. D. Anderson Cancer Center Introduction Patients undergoing radiation therapy
Measurement of Secondary Radiation for Electron and Proton Accelerators D. Followill, Ph.D. Radiological Physics Center U. T. M. D. Anderson Cancer Center Introduction Patients undergoing radiation therapy
Disclosure. Outline. Machine Overview. I have received honoraria from Accuray in the past. I have had travel expenses paid by Accuray in the past.
 Clinical Implementation of the CyberKnife Disclosure I have received honoraria from Accuray in the past. I have had travel expenses paid by Accuray in the past. Mary Ellen Masterson-McGary McGary CyberKnife
Clinical Implementation of the CyberKnife Disclosure I have received honoraria from Accuray in the past. I have had travel expenses paid by Accuray in the past. Mary Ellen Masterson-McGary McGary CyberKnife
ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER
 ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER Bro. Dr. Collie Miller IARC/WHO Based on trends in the incidence of cancer, the International Agency for Research on Cancer (IARC) and WHO
ADVANCES IN RADIATION TECHNOLOGIES IN THE TREATMENT OF CANCER Bro. Dr. Collie Miller IARC/WHO Based on trends in the incidence of cancer, the International Agency for Research on Cancer (IARC) and WHO
Non-target dose from radiotherapy: Magnitude, Evaluation, and Impact. Stephen F. Kry, Ph.D., D.ABR.
 Non-target dose from radiotherapy: Magnitude, Evaluation, and Impact Stephen F. Kry, Ph.D., D.ABR. Goals Compare out-of-field doses from various techniques Methods to reduce out-of-field doses Impact of
Non-target dose from radiotherapy: Magnitude, Evaluation, and Impact Stephen F. Kry, Ph.D., D.ABR. Goals Compare out-of-field doses from various techniques Methods to reduce out-of-field doses Impact of
Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning
 Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning Supervisors Prof. V. Patera PhD R. Van Roermund Candidate Annalisa Patriarca
Characterization and implementation of Pencil Beam Scanning proton therapy techniques: from spot scanning to continuous scanning Supervisors Prof. V. Patera PhD R. Van Roermund Candidate Annalisa Patriarca
Application of Implanted Markers in Proton Therapy. Course Outline. McLaren Proton Therapy Center Karmanos Cancer Institute McLaren - Flint
 Application of Implanted Markers in Proton Therapy Sung Yong Park, Ph.D. McLaren Proton Therapy Center Karmanos Cancer Institute McLaren - Flint AAPM 2016, SAM Therapy Educational Course, 2016.08.04. Course
Application of Implanted Markers in Proton Therapy Sung Yong Park, Ph.D. McLaren Proton Therapy Center Karmanos Cancer Institute McLaren - Flint AAPM 2016, SAM Therapy Educational Course, 2016.08.04. Course
SBRT fundamentals. Outline 8/2/2012. Stereotactic Body Radiation Therapy Quality Assurance Educational Session
 Stereotactic Body Radiation Therapy Quality Assurance Educational Session J Perks PhD, UC Davis Medical Center, Sacramento CA SBRT fundamentals Extra-cranial treatments Single or small number (2-5) of
Stereotactic Body Radiation Therapy Quality Assurance Educational Session J Perks PhD, UC Davis Medical Center, Sacramento CA SBRT fundamentals Extra-cranial treatments Single or small number (2-5) of
Use of molecular and functional imaging for treatment planning The Good, The Bad and The Ugly
 Use of molecular and functional imaging for treatment planning The Good, The Bad and The Ugly Robert Jeraj, PhD Associate Professor of Medical Physics, Human Oncology, Radiology and Biomedical Engineering
Use of molecular and functional imaging for treatment planning The Good, The Bad and The Ugly Robert Jeraj, PhD Associate Professor of Medical Physics, Human Oncology, Radiology and Biomedical Engineering
IMRT - the physician s eye-view. Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia
 IMRT - the physician s eye-view Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia The goals of cancer therapy Local control Survival Functional status Quality of life Causes
IMRT - the physician s eye-view Cinzia Iotti Department of Radiation Oncology S.Maria Nuova Hospital Reggio Emilia The goals of cancer therapy Local control Survival Functional status Quality of life Causes
RADIATION ONCOLOGY RESIDENCY PROGRAM Competency Evaluation of Resident
 Resident s Name: RADIATION ONCOLOGY RESIDENCY PROGRAM Competency Evaluation of Resident Rotation: PHYS 703: Clinical Rotation 2 Inclusive dates of rotation: Feb. 26, 2016 Aug. 25, 2016 Director or Associate
Resident s Name: RADIATION ONCOLOGY RESIDENCY PROGRAM Competency Evaluation of Resident Rotation: PHYS 703: Clinical Rotation 2 Inclusive dates of rotation: Feb. 26, 2016 Aug. 25, 2016 Director or Associate
Production and dosimetry of simultaneous therapeutic photons and electrons beam by linear accelerator: a monte carlo study
 Production and dosimetry of simultaneous therapeutic photons and electrons beam by linear accelerator: a monte carlo study Navid Khledi 1, Azim Arbabi 2, Dariush Sardari 1, Mohammad Mohammadi 3, Ahmad
Production and dosimetry of simultaneous therapeutic photons and electrons beam by linear accelerator: a monte carlo study Navid Khledi 1, Azim Arbabi 2, Dariush Sardari 1, Mohammad Mohammadi 3, Ahmad
8/2/2017. Objectives. Disclosures. Clinical Implementation of an MR-Guided Treatment Unit
 MR-Linac is a research programme. It is not available for sale and its future availability cannot be guaranteed 8/2/2017 Clinical Implementation of an MR-Guided Treatment Unit Geoffrey S. Ibbott, Ph.D.
MR-Linac is a research programme. It is not available for sale and its future availability cannot be guaranteed 8/2/2017 Clinical Implementation of an MR-Guided Treatment Unit Geoffrey S. Ibbott, Ph.D.
Leila E. A. Nichol Royal Surrey County Hospital
 2 nd UK and Ireland Dosimetry Check User Meeting Symposium Clatterbridge Cancer Centre, 24 th October 2012 Leila E. A. Nichol Royal Surrey County Hospital Leila.Nichol@nhs.net *My experience with Dosimetry
2 nd UK and Ireland Dosimetry Check User Meeting Symposium Clatterbridge Cancer Centre, 24 th October 2012 Leila E. A. Nichol Royal Surrey County Hospital Leila.Nichol@nhs.net *My experience with Dosimetry
Technical Study. Institution University of Texas Health San Antonio. Location San Antonio, Texas. Medical Staff. Daniel Saenz. Niko Papanikolaou.
 Technical Study Stereotactic Radiosurgery with Elekta Versa HD and Monaco Accuracy of a single isocenter, multiple brain metastases VMAT plan delivered to a pseudo-patient dosimetric gel phantom Institution
Technical Study Stereotactic Radiosurgery with Elekta Versa HD and Monaco Accuracy of a single isocenter, multiple brain metastases VMAT plan delivered to a pseudo-patient dosimetric gel phantom Institution
A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer
 A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer Tony Kin Ming Lam Radiation Planner Dr Patricia Lindsay, Radiation Physicist Dr John Kim, Radiation Oncologist Dr Kim Ann Ung,
A Comparison of IMRT and VMAT Technique for the Treatment of Rectal Cancer Tony Kin Ming Lam Radiation Planner Dr Patricia Lindsay, Radiation Physicist Dr John Kim, Radiation Oncologist Dr Kim Ann Ung,
Intensity Modulated Radiation Therapy: Dosimetric Aspects & Commissioning Strategies
 Intensity Modulated Radiation Therapy: Dosimetric Aspects & Commissioning Strategies ICPT School on Medical Physics for Radiation Therapy Justus Adamson PhD Assistant Professor Department of Radiation
Intensity Modulated Radiation Therapy: Dosimetric Aspects & Commissioning Strategies ICPT School on Medical Physics for Radiation Therapy Justus Adamson PhD Assistant Professor Department of Radiation
Disclosures. Overview 8/3/2016. SRS: Cranial and Spine
 SRS: Cranial and Spine Brian Winey, Ph.D. Department of Radiation Oncology Massachusetts General Hospital Harvard Medical School Disclosures Travel and research funds from Elekta Travel funds from IBA
SRS: Cranial and Spine Brian Winey, Ph.D. Department of Radiation Oncology Massachusetts General Hospital Harvard Medical School Disclosures Travel and research funds from Elekta Travel funds from IBA
Chapter 7 General conclusions and suggestions for future work
 Chapter 7 General conclusions and suggestions for future work Radiation therapy (RT) is one of the principle treatment modalities for the management of cancer. In recent decades, advances in the radiation
Chapter 7 General conclusions and suggestions for future work Radiation therapy (RT) is one of the principle treatment modalities for the management of cancer. In recent decades, advances in the radiation
Clinical Protontherapy Head and Neck cancer
 Clinical Protontherapy Head and Neck cancer Coen Rasch Department of Radiation Oncology Academic Medical Center Amsterdam No disclosures 1 Introduction Proton vsphotonin the literature Model basedindicationprotocol
Clinical Protontherapy Head and Neck cancer Coen Rasch Department of Radiation Oncology Academic Medical Center Amsterdam No disclosures 1 Introduction Proton vsphotonin the literature Model basedindicationprotocol
IMPT with Carbon Ions
 IMPT with Carbon Ions PTCOG 48, Heidelberg, 28.09.-03.10.2009 Malte Ellerbrock Medical Physics Expert Heidelberg Ion-Beam Therapy Center HIT Betriebs GmbH am Universitätsklinikum Heidelberg http://www.hit-centrum.de
IMPT with Carbon Ions PTCOG 48, Heidelberg, 28.09.-03.10.2009 Malte Ellerbrock Medical Physics Expert Heidelberg Ion-Beam Therapy Center HIT Betriebs GmbH am Universitätsklinikum Heidelberg http://www.hit-centrum.de
The objective of this lecture is to integrate our knowledge of the differences between 2D and 3D planning and apply the same to various clinical
 The objective of this lecture is to integrate our knowledge of the differences between 2D and 3D planning and apply the same to various clinical sites. The final aim will be to be able to make out these
The objective of this lecture is to integrate our knowledge of the differences between 2D and 3D planning and apply the same to various clinical sites. The final aim will be to be able to make out these
Imaging of Scattered Radiation for Real Time Tracking of Tumor Motion During Lung SBRT
 Imaging of Scattered Radiation for Real Time Tracking of Tumor Motion During Lung SBRT April 25 nd, 2015 Lung Cancer Lung cancer is the most lethal cancer: Over 224,000 new diagnoses in the U.S. predicted
Imaging of Scattered Radiation for Real Time Tracking of Tumor Motion During Lung SBRT April 25 nd, 2015 Lung Cancer Lung cancer is the most lethal cancer: Over 224,000 new diagnoses in the U.S. predicted
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy
 Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti a*, M. Bucciolini a, L. Marrazzo a, D. Menichelli a. a) Department
Dosimetric characterization with 62 MeV protons of a silicon segmented detector for 2D dose verifications in radiotherapy C. Talamonti a*, M. Bucciolini a, L. Marrazzo a, D. Menichelli a. a) Department
IMRT/IGRT Patient Treatment: A Community Hospital Experience. Charles M. Able, Assistant Professor
 IMRT/IGRT Patient Treatment: A Community Hospital Experience Charles M. Able, Assistant Professor Disclosures I have no research support or financial interest to disclose. Learning Objectives 1. Review
IMRT/IGRT Patient Treatment: A Community Hospital Experience Charles M. Able, Assistant Professor Disclosures I have no research support or financial interest to disclose. Learning Objectives 1. Review
Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments
 Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments Alana Hudson *1 1 Tom Baker Cancer Centre, Department of Medical Physics, 1331
Use of Bubble Detectors to Characterize Neutron Dose Distribution in a Radiotherapy Treatment Room used for IMRT treatments Alana Hudson *1 1 Tom Baker Cancer Centre, Department of Medical Physics, 1331
Nuclear Data for Radiation Therapy
 Symposium on Nuclear Data 2004 Nov. 12, 2004 @ JAERI, Tokai Nuclear Data for Radiation Therapy ~from macroscopic to microscopic~ Naruhiro Matsufuji, Yuki Kase and Tatsuaki Kanai National Institute of Radiological
Symposium on Nuclear Data 2004 Nov. 12, 2004 @ JAERI, Tokai Nuclear Data for Radiation Therapy ~from macroscopic to microscopic~ Naruhiro Matsufuji, Yuki Kase and Tatsuaki Kanai National Institute of Radiological
Assessing Heterogeneity Correction Algorithms Using the Radiological Physics Center Anthropomorphic Thorax Phantom
 Assessing Heterogeneity Correction Algorithms Using the Radiological Physics Center Anthropomorphic Thorax Phantom David Followill, Ph.D. Associate Director Radiological Physics Center RPC History Lesson
Assessing Heterogeneity Correction Algorithms Using the Radiological Physics Center Anthropomorphic Thorax Phantom David Followill, Ph.D. Associate Director Radiological Physics Center RPC History Lesson
Measurement of Dose to Critical Structures Surrounding the Prostate from. Intensity-Modulated Radiation Therapy (IMRT) and Three Dimensional
 Measurement of Dose to Critical Structures Surrounding the Prostate from Intensity-Modulated Radiation Therapy (IMRT) and Three Dimensional Conformal Radiation Therapy (3D-CRT); A Comparative Study Erik
Measurement of Dose to Critical Structures Surrounding the Prostate from Intensity-Modulated Radiation Therapy (IMRT) and Three Dimensional Conformal Radiation Therapy (3D-CRT); A Comparative Study Erik
HEAVY PARTICLE THERAPY
 HEAVY PARTICLE THERAPY DR. G.V. GIRI KIDWAI MEMORIAL INSTITUTE OF ONCOLOGY ICRO 2012 BHATINDA HEAVY PARTICLES USED IN A EFFORT TO IMPROVE TUMOR CONTROL, THAT DO NOT RESPOND TO PHOTONS OR ELECTRONS BETTER
HEAVY PARTICLE THERAPY DR. G.V. GIRI KIDWAI MEMORIAL INSTITUTE OF ONCOLOGY ICRO 2012 BHATINDA HEAVY PARTICLES USED IN A EFFORT TO IMPROVE TUMOR CONTROL, THAT DO NOT RESPOND TO PHOTONS OR ELECTRONS BETTER
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer
 Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
Dosimetric Analysis of 3DCRT or IMRT with Vaginal-cuff Brachytherapy (VCB) for Gynaecological Cancer Tan Chek Wee 15 06 2016 National University Cancer Institute, Singapore Clinical Care Education Research
Clinical Education A comprehensive and specific training program. carry out effective treatments from day one
 Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Proton Therapy Clinical Education A comprehensive and specific training program carry out effective treatments from day one Forewarned is forearmed Although over 100,000 patients have been treated in proton
Electron therapy Class 3: Clinical procedures
 Electron therapy Class 3: Clinical procedures Laurence Court lecourt@mdanderson.org Reference: Faiz M. Khan, The Physics of Radiation Therapy Slide acknowledgements: Karl Prado, Rebecca Howell, Kent Gifford,
Electron therapy Class 3: Clinical procedures Laurence Court lecourt@mdanderson.org Reference: Faiz M. Khan, The Physics of Radiation Therapy Slide acknowledgements: Karl Prado, Rebecca Howell, Kent Gifford,
A Dosimetric Comparison of Whole-Lung Treatment Techniques. in the Pediatric Population
 A Dosimetric Comparison of Whole-Lung Treatment Techniques in the Pediatric Population Corresponding Author: Christina L. Bosarge, B.S., R.T. (R) (T) Indiana University School of Medicine Department of
A Dosimetric Comparison of Whole-Lung Treatment Techniques in the Pediatric Population Corresponding Author: Christina L. Bosarge, B.S., R.T. (R) (T) Indiana University School of Medicine Department of
Transition to Heterogeneity Corrections. Why have accurate dose algorithms?
 Transition to Heterogeneity Corrections Eric E. Klein, M.S., Washington University, St. Louis, MO Craig Stevens, M.D., Ph.D., MD Anderson Cancer Center, Houston, TX Nikos Papinikolou, Ph.D., University
Transition to Heterogeneity Corrections Eric E. Klein, M.S., Washington University, St. Louis, MO Craig Stevens, M.D., Ph.D., MD Anderson Cancer Center, Houston, TX Nikos Papinikolou, Ph.D., University
Small field diode dosimetry
 Small field diode dosimetry Parham Alaei, Ph.D. Department of Radiation Oncology University of Minnesota NCCAAPM Symposium-October 10, 2013 1 Diodes as beam data collection detectors Diodes as in vivo
Small field diode dosimetry Parham Alaei, Ph.D. Department of Radiation Oncology University of Minnesota NCCAAPM Symposium-October 10, 2013 1 Diodes as beam data collection detectors Diodes as in vivo
4 Essentials of CK Physics 8/2/2012. SRS using the CyberKnife. Disclaimer/Conflict of Interest
 SRS using the CyberKnife Sonja Dieterich, PhD, DABR Associate Professor University of California Davis Disclaimer/Conflict of Interest Consulting agreements with Broncus Medical and CyberHeart, Inc. Scientific
SRS using the CyberKnife Sonja Dieterich, PhD, DABR Associate Professor University of California Davis Disclaimer/Conflict of Interest Consulting agreements with Broncus Medical and CyberHeart, Inc. Scientific
Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment
 Chinese Journal of Cancer Original Article Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment Suresh Rana 1 and ChihYao Cheng 2 Abstract The volumetric modulated
Chinese Journal of Cancer Original Article Feasibility of the partial-single arc technique in RapidArc planning for prostate cancer treatment Suresh Rana 1 and ChihYao Cheng 2 Abstract The volumetric modulated
NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) BONE (Version , 03/28/18)
 BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
Real-time Volumetric Scintillation Dosimetry for Radiation Therapy
 Real-time Volumetric Scintillation Dosimetry for Radiation Therapy Sam Beddar, Ph.D., FCCPM, FAAPM Professor & Chief of Research Department of Radiation Physics The University of Texas MD Anderson Cancer
Real-time Volumetric Scintillation Dosimetry for Radiation Therapy Sam Beddar, Ph.D., FCCPM, FAAPM Professor & Chief of Research Department of Radiation Physics The University of Texas MD Anderson Cancer
FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE. Geoffrey S. Ibbott, Ph.D. June 20, 2017
 FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE Geoffrey S. Ibbott, Ph.D. June 20, 2017 1 DISCLOSURES My institution holds Strategic Partnership Research Agreements with Varian, Elekta, and Philips
FROM ICARO1 TO ICARO2: THE MEDICAL PHYSICS PERSPECTIVE Geoffrey S. Ibbott, Ph.D. June 20, 2017 1 DISCLOSURES My institution holds Strategic Partnership Research Agreements with Varian, Elekta, and Philips
Radiosurgery by Leksell gamma knife. Josef Novotny, Na Homolce Hospital, Prague
 Radiosurgery by Leksell gamma knife Josef Novotny, Na Homolce Hospital, Prague Radiosurgery - Definition Professor Lars Leksell The tools used by the surgeon must be adapted to the task and where the human
Radiosurgery by Leksell gamma knife Josef Novotny, Na Homolce Hospital, Prague Radiosurgery - Definition Professor Lars Leksell The tools used by the surgeon must be adapted to the task and where the human
Optimization of the T2 parametric image map calculation in MRI polymer gel dosimetry
 Journal of Physics: Conference Series Optimization of the T parametric image map calculation in MRI polymer gel dosimetry To cite this article: Fotini Zacharopoulou et al J. Phys.: Conf. Ser. 5 9 Related
Journal of Physics: Conference Series Optimization of the T parametric image map calculation in MRI polymer gel dosimetry To cite this article: Fotini Zacharopoulou et al J. Phys.: Conf. Ser. 5 9 Related
Uncertainties in proton therapy: Analysis of the effects of density changes, calibration curve errors and setup errors in proton dose distributions.
 Uncertainties in proton therapy: Analysis of the effects of density changes, calibration curve errors and setup errors in proton dose distributions. A treatment planning study performed on water phantoms
Uncertainties in proton therapy: Analysis of the effects of density changes, calibration curve errors and setup errors in proton dose distributions. A treatment planning study performed on water phantoms
Proton Therapy Dosimetry & Clinical Implementation. Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine
 Proton Therapy Dosimetry & Clinical Implementation Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine Outline» Proton Therapy Basics» Why Proton Therapy? (Dosimetric Superiority)»
Proton Therapy Dosimetry & Clinical Implementation Baldev Patyal, Ph.D., Chief Medical Physicist Department of Radiation Medicine Outline» Proton Therapy Basics» Why Proton Therapy? (Dosimetric Superiority)»
Measurement of Dose to Implanted Cardiac Devices in Radiotherapy Patients
 Measurement of Dose to Implanted Cardiac Devices in Radiotherapy Patients Moyed Miften, PhD Professor and Chief Physicist University of Colorado Chester Reft, PhD Associate Professor University of Chicago
Measurement of Dose to Implanted Cardiac Devices in Radiotherapy Patients Moyed Miften, PhD Professor and Chief Physicist University of Colorado Chester Reft, PhD Associate Professor University of Chicago
Rectal dose and toxicity dosimetric evaluation for various beam arrangements using pencil beam scanning protons with and without rectal spacers
 Rectal dose and toxicity dosimetric evaluation for various beam arrangements using pencil beam scanning protons with and without rectal spacers 2015 MAC-AAPM Annual Meeting, Baltimore, MD Heeteak Chung,
Rectal dose and toxicity dosimetric evaluation for various beam arrangements using pencil beam scanning protons with and without rectal spacers 2015 MAC-AAPM Annual Meeting, Baltimore, MD Heeteak Chung,
Quality assurance and credentialing requirements for sites using inverse planned IMRT Techniques
 TROG 08.03 RAVES Quality assurance and credentialing requirements for sites using inverse planned IMRT Techniques Introduction Commissioning and quality assurance of planning systems and treatment delivery
TROG 08.03 RAVES Quality assurance and credentialing requirements for sites using inverse planned IMRT Techniques Introduction Commissioning and quality assurance of planning systems and treatment delivery
Implementation of an Anthropomorphic Phantom for the Evaluation of Proton Therapy Treatment Procedures
 Texas Medical Center Library DigitalCommons@TMC UT GSBS Dissertations and Theses (Open Access) Graduate School of Biomedical Sciences 5-2010 Implementation of an Anthropomorphic Phantom for the Evaluation
Texas Medical Center Library DigitalCommons@TMC UT GSBS Dissertations and Theses (Open Access) Graduate School of Biomedical Sciences 5-2010 Implementation of an Anthropomorphic Phantom for the Evaluation
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR
 Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Linac or Non-Linac Demystifying And Decoding The Physics Of SBRT/SABR PhD, FAAPM, FACR, FASTRO Department of Radiation Oncology Indiana University School of Medicine Indianapolis, IN, USA Indra J. Das,
Quality Assurance of TPS: comparison of dose calculation for stereotactic patients in Eclipse and iplan RT Dose
 Petrovic B Comparison of dose calculation algorithms for stereotaxy Quality Assurance of TPS: comparison of dose calculation for stereotactic patients in and RT Dose Borislava Petrovic 1, Aleksandra Grządziel
Petrovic B Comparison of dose calculation algorithms for stereotaxy Quality Assurance of TPS: comparison of dose calculation for stereotactic patients in and RT Dose Borislava Petrovic 1, Aleksandra Grządziel
Defining Target Volumes and Organs at Risk: a common language
 Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
Defining Target Volumes and Organs at Risk: a common language Eduardo Rosenblatt Section Head Applied Radiation Biology and Radiotherapy (ARBR) Section Division of Human Health IAEA Objective: To introduce
A simple technique for craniospinal radiotherapy in the supine position
 Radiotherapy and Oncology 78 (2006) 217 222 www.thegreenjournal.com Craniospinal radiotherapy A simple technique for craniospinal radiotherapy in the supine position William A. Parker a, *, Carolyn R.
Radiotherapy and Oncology 78 (2006) 217 222 www.thegreenjournal.com Craniospinal radiotherapy A simple technique for craniospinal radiotherapy in the supine position William A. Parker a, *, Carolyn R.
Medical Dosimetry Graduate Certificate Program IU Graduate School & The Department of Radiation Oncology IU Simon Cancer Center
 Medical Dosimetry Graduate Certificate Program IU Graduate School & The Department of Radiation Oncology IU Simon Cancer Center All students accepted into the Medical Dosimetry Graduate Certificate Program
Medical Dosimetry Graduate Certificate Program IU Graduate School & The Department of Radiation Oncology IU Simon Cancer Center All students accepted into the Medical Dosimetry Graduate Certificate Program
