Optic Nerve Evaluation in Glaucoma (TPG)
|
|
|
- Gertrude Jenkins
- 5 years ago
- Views:
Transcription
1 Optic Nerve Evaluation in Glaucoma (TPG) Introduction Glaucoma is a progressive optic nerve disease characterized by retinal ganglion cell death and resultant axon loss, ultimately manifesting as excavation of the optic nerve head with consequent defects in retinal sensitivity that can be measured with visual field tests1,5,15,17. Glaucomatous damage may be due to elevated intraocular pressure, poor perfusion pressure to the optic nerve head, obstruction of axoplasmic flow within the ganglion cell axons, anatomic weakening of the lamina cribrosa, and programmed cell death of the ganglion cell axons2,9,14,16,20. Knowing that 25 35% of ganglion cells are lost before visual field defects are detected on standard automated perimetry and that careful evaluation of the optic nerve head has high specificity and good precision for glaucoma diagnosis1,13,14,15,19,21, accurate assessment of the optic nerve becomes essential for early diagnosis and management of glaucoma in order to prevent visual field defects before they occur. A sound knowledge of the subtle changes of the optic nerve and its surrounding tissues is thus critical in order for the astute clinician to become proficient in evaluating the optic nerve to be able to detect glaucoma as early as possible. Once characteristic cupping and visual field decline has occurred the diagnosis is easy the challenge therefore lies in critically evaluating the optic nerve before significant cupping takes place. In the discussion that follows, we will first discuss the normal anatomy and non pathologic variations of the healthy optic nerve and peripapillary tissues, and will conclude by reviewing cardinal features to look for so that glaucomatous optic nerve damage can be detected as early as possible. Naida Jakirlic, OD, FAAO Dr. Jakirlic, graduated from SUNY College of Optometry and completed a residency in ocular disease at SUNY. She was a staff optometrist at two New York City hospitals for several years prior to joining the faculty at Western University of Health Sciences in 2014 where she is involved in both didactic and clinical education of first, second, and third year optometry students. E mail address: njakirlic@westernu.edu
2 Normal anatomy of the optic nerve Ganglion cell axons make up the vast majority of the neuroretinal rim tissue of the optic disc. One to 1.5 million axons leave via the optic nerve head through the scleral canal, while the remainder of the neuroretinal rim is composed of capillaries and astrocytes2,8. There are four distinct layers of the optic nerve head, including the surface, prelaminar, laminar, and retrolaminar layers8. The surface layer is the anterior limit of the optic nerve and is the point of contact with the vitreous8. Its peripheral edge is defined by the anterior limits of the scleral ring, and its posterior limit is where the axon bundles have completed a 90 degree turn from the plane of the retina and reached the level of the choroid8. The prelaminar optic nerve is an indistinct segment of axons surrounded by outer retina, choriocapillaris, and choroid8. Within the laminar optic nerve, the ganglion cell axon bundles are wrapped in glial cells and confined in the rigid pores of the lamina cribrosa8. The retrolaminar optic nerve thickness is doubled by the presence of myelinating oligodendrocytes8. The lamina cribrosa is a part of the scleral tissue through which ganglion cell axons exit as they leave the globe. It is composed of several sheets of connective tissue that is fenestrated to allow the passage of the nerve fiber bundles8,9,10. The superior and inferior poles have the largest pores, thus providing less structural support for the axon bundles leaving the nerve in these two areas8,9,10,13. This may explain why there is typically greater damage to the retinal ganglion cell axons in the superior and inferior poles of the optic nerve that we see clinically9. Furthermore, as ganglion cell axons are lost, the laminar dots become more exposed, which can also be visualized clinically. While laminar dots may certainly be present in healthy non glaucomatous eyes, their presence should alert the clinician to look for other signs of glaucoma. The lamina is also susceptible to thinning and bowing backward due to effects of the intraocular pressure, which results in a clinically visible deeper cup in glaucomatous eyes1,2,14. The surface optic nerve receives its blood supply from small branches of the central retinal artery8,9. The pre laminar optic nerve is supplied by the short posterior ciliary arteries (SPCA), and their integrity is responsible for the reddish hue that is observed clinically in healthy optic nerves2,8,9. The laminar optic nerve is supplied by the Circle of Zinn Haller, which is composed of anastomoses from adjacent SPCA s8,9. The retro laminar optic nerve head is supplied by axial vasculature from the central retinal artery, the pial vascular plexus, and the SPCA s8,9. Knowing the vasculature of the optic nerve is critical when evaluating the health and integrity of the neuroretinal rim as it is necessary to remember that glaucoma is cupping without pallor1,11,14. If pallor of the optic nerve is observed, it indicates insult to the prelaminar vasculature and should always alert the clinician that a different or an additional optic neuropathy is present. Venous drainage of the optic nerve occurs via the central retinal vein8,9. In chronic glaucoma, optociliary shunt vessels may appear due to disturbed retinal circulation. These vessels are pre existing venules that become more visible as they dilate to re route blood around an area of obstruction8. They can be differentiated from neovascular vessels as optociliary shunt vessels will not leak on fluorescein angiography, while neovascular vessels will always leak fluorescein dye.
3 Figure 5: Color photograph of optociliary shunt vessels in a patient with advanced glaucomatous optic neuropathy. Figuree 6: Color photograph of optociliary vesselss in a patient with glaucomatous neuropathy. shunt optic The optic cup, which is given the most attention in glaucoma,, is a central excavation in the optic nerve head. It is devoid of axons and capillaries and is pale due to visibility of the collagenous lamina cribrosa that forms its floor1,19. Its size is dependent on the number of nerve fibers leaving the eye and the size of the scleral canal10,11. The border of the cup and rim is determined by contour, not by color, therefore viewing the nerve stereoscopically under high magnification is essential in accurately assessing where the contour is located14. The best way to determine the contour iss by visualizing the point of deviation of vessels on the surface of the optic nerve head14. Clinicians must become proficient in this assessment as color can sometimess be very misleading whenn determining the cup to disc (C/D) ratio. Lastly, it is critical to remember that the size of the scleral opening will determine the size of the optic cup, therefore large scleral openings will result in large C/D ratios, whereas small scleral openings will present clinically as small C/D ratios1,10,11,19. The take home point heree is that a large C/D in a large nerve is probably normal, while an average C/D in a small nerve might be glaucomatous thereforee it is necessary for every C/ D ratio to be considered directly in relation to the disc size and not as an independent finding because it can be highly misleading and can lead to both an over diagnosis of glaucomaa in large nerves, as well as an under diagnosis of glaucoma in small nerves. A discussion on normal optic nerve anatomy is incomplete without addressing the peripapillary area because non patholog ic variations of this area must be distinguished from pathologic changes seen in glaucoma. Elschnig s scleral ring is a normal anatomic variation whereby a thin white ring, also known as the scleral lip, is seen immediately adjacent to the optic disc margin11,12,,14. It is caused by an anterior extensionn of the sclera between the choroid and optic nerve; ; more simply, the RPE and choroid tissue terminates just short of the optic disc, thus allowing visualization of scleral tissue through the transparent nerve fiber bundles4,7. Choroidal crescents are also a normal peripapillary variation, and
4 are caused by non pathologic termination of the RPE prior to reaching the optic disc, thus causing the underlying choroid to be visible as a uniform slate gray crescent directly adjacent to the optic disc7. Choroidal crescents are typically present temporally, although they can span the optic disc 360 degrees7. These two normal variants should not be confused with zone alpha and zone beta peripapillary atrophy that will be discussed shortly. Optic nerve evaluation in glaucoma Slit lamp biomicroscopy with a fundus condensing lens is the ideal method to evaluate the optic nerve because it allows for a magnified stereoscopic view, thus enabling the observer to directly measure the vertical height of the optic disc6,18. While direct ophthalmoscopy provides good magnification, it unfortunately has the disadvantage of lacking stereopsis and is therefore not the ideal tool for optic nerve assessment. Indirect ophthalmoscopy is also sub optimal as it provides poor magnification and detail. Optic disc photography is an excellent tool for both documentation and monitoring for any progression; typically, it is performed at baseline and every year afterwards unless progression of disease is suspected6,10,18. There are several key findings to look for when evaluating the optic nerve. First, the clinician should assess the optic disc size and shape. This allows for the determination of whether the cup size is normal or suspicious in relation to the size of the scleral opening6,11,21. Next, the size, color, and integrity of the neuroretinal rim tissue should be assessed6. Here it is critical to remember that glaucoma causes cupping without pallor, therefore any presence of pallor necessitates a different or additional workup for a non glaucomatous optic neuropathy. Next, the cup size and shape should be assessed in relation to the optic disc size. The clinician should then examine the retinal nerve fiber layer, the peripapillary region, and carefully look for the presence of optic disc hemorrhages, as well as other less obvious vascular changes that will be discussed below6. Optic disc size The scleral foramen through which the ganglion cell axons exit the eye ranges in diameter such that a large foramen will result in a large disc and a large cup, whereas a small foramen will result in the opposite6,10,11. Measurement of the vertical disc diameter is therefore essential in order for clinicians to assess whether an optic disc is small, average, or large6,10. Measurement of the optic disc size is best performed at the slit lamp using a narrow vertical beam of light and a fundus condensing lens6,10. Depending on the fundus lens that is used, the size measured at the slit lamp may need to be multiplied by a correction factor. A 60D condensing lens gives a 1:1 ratio, therefore it is the optimal lens for this purpose as the correction factor is simply The correction factor for a 78D lens is 1.1, and for a 90D lens it is 1.36,21. Another way to document the vertical height is by simply recording the vertical height measured at the slit lamp and the condensing lens that was used without needing to multiply by the correction factor. The average vertical height of the healthy optic nerve ranges from 1.8 to 2.0 millimeters18,19. A small vertical diameter is equal to or less than 1.5 millimeters; a large vertical diameter is greater than 2.2 millimeters6,18. This assessment becomes essential in order to avoid over testing and over diagnosis in large nerves due to the knee jerk reaction that any C/D greater than 0.4 is immediately suspicious for glaucoma. Perhaps even more importantly, it is necessary to carefully measure the vertical height of the optic nerve in order to prevent under diagnosing glaucoma in small optic nerves due to observing a C/D ratio that would not typically raise suspicion solely due to its low value. Thus it is imperative to keep in
5 mind that a C/D of 0.8 is probably not glaucomatous in a nerve with a 2.7 millimeter vertical height, whereas a C/D of 0.3 is probably glaucomatous in a nerve with a vertical height of 1.5 millimeters. Neuroretinal Rim The neuroretinal rim will reflect selective loss of ganglion cell axons and is the primary location of pathologic changes seen in glaucoma17. Because C/D ratio is often a poor indicator of early glaucoma, clinicians should pay close attention to the width and health of the neuroretinal rim instead we should be looking more carefully at the donut, not at the hole21. When assessing the neuroretinal rim tissue, its size, shape, and color must be taken into consideration6. The ISNT rule has been ingrained in us, and this is for a reason. When looking at the average nerve, the inferior rim tissue should always be the widest, followed by superior, nasal, and temporal, and this has to do with the anatomic distribution of the nerve fiber bundles as they leave through the scleral canal6,14. However, in normal anatomic variations whereby the nerve might be horizontally oval, the ISNT rule may not always apply, which is also important to keep in mind in order to avoid over diagnosing glaucoma in healthy eyes15. As clinicians, we should look at the neuroretinal rim carefully and evaluate for any thinning and notching of the rim tissue, which would indicate glaucomatous damage. The typical sequence of neuroretinal rim loss in glaucoma is loss of rim tissue at the infero temporal and supero temporal poles, followed by the temporal rim, and lastly by the nasal rim17. Peripapillary chorioretinal atrophy Irregular pigmentation around the optic nerve is a non specific finding that can be seen in many healthy eyes3. However, its presence should raise suspicion for glaucoma, particularly if additional risk factors are identified in the patient. It differs from normal peripapillary variants discussed earlier in the respect that atrophy is typically irregular and patchy, whereas crescents are typically very uniform in color and shape. The clinical appearance of peripapillary atrophy is a moth eaten pattern of the RPE temporal to the optic nerve head; if truly associated with glaucoma, there is typically neuro retinal rim thinning adjacent to the area of atrophy1,3,4,5,6,11,22. Zone alpha is a hypo and hyper pigmented area of RPE irregularity. Nasally it is always separated from the neuro retinal rim by either zone beta if present, or by the scleral ring if zone beta is absent, and temporally it is bounded by normal retina5,11,14. Zone alpha is a non specific finding that is present in both normal and glaucomatous eyes4,5. Zone beta is an irregular area of complete RPE and choriocapillaris atrophy immediately adjacent to the optic disc, thus resulting in visualization of large choroidal vessels and underlying sclera5. It is thought to be caused by poor perfusion of the peripapillary area, and though it may also be present in normal eyes, it is much more common in glaucomatous eyes4,5,11,14. The usefulness of zone alpha and zone beta is to help the clinician differentiate between glaucomatous and non glaucomatous optic nerves, particularly when additional anatomic changes suggest the presence of early glaucoma damage. Additionally, because progression of zone beta is associated with progression of glaucoma, it may be a subtle yet important indication to alert the clinician that more aggressive glaucoma therapy may be necessary in a patient already diagnosed with the disease4,5,14.
6 Figure 7: Color photograph demonstrating clear areas of zone alpha and beta peripapillary atrophy. Vascular Changes Several vascular changes can be observed in glaucomatous eyes, including optic disc hemorrhages, baring of circumlinear vessels, bayonetting of vessels, nasalization of vessels, optic nerve shunts, and retinal artery attenuation. Optic disc hemorrhage, also known as drance hemorrhage, is a splinter or flame shaped hemorrhage located on the disc margin1,5,6,11,14,19. It is a hallmark of glaucomatous optic nerve damage and can be found in early and moderate stages of glaucoma, but is rare in advanced glaucomatous cupping likely due to absence of sufficient neuroretinal rim tissue1,5,6,11,14,19. It is usually located on the superotemporal and infero temporal disc margins and is more common in patients with normal tension glaucoma. It typically resolves within 6 10 weeks of onset and is associated with localized RNFL defects and rim notching5. Though highly pathognomonic for glaucoma, it can also occur in patients with posterior vitreous detachment, BRVO, hypertensive retinopathy, and non arteritic anterior ischemic optic neuropathy, therefore its presence must always be considered in relation to the clinical picture at hand. In glaucoma patients, it is strongly indicative of disease progression and is a strong indicator that more aggressive therapy should be instituted.
7 Figure 8: Color and red free photographs of a patient with an obvious inferior temporal disc hemorrhage. Figure 9: Color and red free photographs of a patient with a subtle inferior temporal disc hemorrhage. Baring of circumlinear vessels occurs in areas where neuroretinal rim tissue has been lost, thus the structural support for the vessels leaving the optic nerve is no longer present and is clinically seen as vessels hanging across the optic nerve cup without adjacent support of neuroretinal rim19. It is a subtle change to look for carefully in order to aid in the diagnosis of glaucoma. Bayonetting of vessels is seen in areas of significant neuroretinal rim tissue loss, whereby visualization of the course of a particular blood vessel is temporarily lost as it makes its way along the excavated nerve borders and re emerges at the edge of the rim from the deeply excavated cup19. It is typically seen in advanced cupping or in nerves with localized notching of the neuroretinal rim. Nasalization of blood vessels occurs in very advanced glaucoma whereby the only structural support remains along the nasal rim due to severe loss of superior, inferior, and temporal rim tissue19. It is easily observable in advanced cupping and will not be present in early disease. Retinal artery attenuation can also occur in glaucomatous eyes, but is typically a subtler finding than the aforementioned vascular changes. It likely results due to decreased metabolic demand from an increasingly thinner rim tissue11,14. It is a very subtle but important change to look for in helping the clinician determine the level of suspicion for early glaucoma.
8 Retinal Nerve Fiber Layer (RNFL) Discussion of the optic nerve in relation to glaucoma would be incomplete without mentioning the RNFL, which is composed of retinal ganglion cell axons which are covered by astrocytes and bundled by Muller cell processes14. The RNFL is seen as bright fine striations fanning off the optic disc and is most prominent infero temporally and supero temporally6,13,14. Healthy RNFL will obscure the details of underlying peripapillary retinal vascular walls, therefore RNFL loss will present as increased sharpness of vascular walls13. Clinical assessment of the RNFL requires a fundus condensing lens, bright light, and a red free filter at the slit lamp6,13. The green light produced by the filter is absorbed by the RPE and choroid, creating a dark background against which the light that is reflected by the RNFL is well contrasted against the dark background, which allows clinicians easy visualization of the RNFL. RNFL defects in glaucoma are caused by selective damage to the superior and inferior arcuate bundles, with relative sparing of papillomacular and nasal bundles. Defects within the RNFL appear as darker zones in areas of expected brightness4. This will cause retinal vessels to appear redder and darker, and will allow small vessels to become more visible4. Diffuse RNFL defects are the most common yet most difficult to detect. The clinician should compare the striations between the superior and inferior bundles of the same eye, as well as the striations between the right and left eyes and look for any loss of brightness, increased sharpness and prominence of peripapillary vessels, and clearer visualization of the underlying choroid. Focal loss of the RNFL is easiest to identify, but is typically the least common and is usually associated with a notch at the disc or a current or prior disc hemorrhage6. It is seen as a dark slit or wedge in the bright superior or inferior striations traveling all the way back to the optic nerve head6,13. Figure 1: Color photograph of superior temporal RNFL wedge defect. Figure 2: Red free image of superior temporal and inferior temporal RNFL wedge defect.
9 Changes in the optic cup Several characteristic changes of the optic cup can be observed clinically. They include increased cup size, increased depth, visualization and/or increase of laminar dots, vertical enlargement, and asymmetry between two eyes greater than 0.2 in the absence of disc size asymmetry1,2,16,17. Therefore although the optic cup is not the only feature to consider when evaluating the optic nerve in glaucoma, it is still a very important one to take into consideration. Figure 4: Color photograph of prominent laminar dot sign. Conclusion Evaluation of the optic nerve head is essential for the early diagnosis and management of glaucoma. Clinicians must keep in mind that the C/D ratio is not the only factor to consider when evaluating the optic nerve, and must therefore give due diligence to the neuroretinal rim and its surrounding peripapillary tissue and vasculature. Clinicians must also remember that glaucoma causes cupping without pallor, therefore the presence of pallor of the neuroretinal rim must prompt the investigation for a different or additional optic neuropathy. Once characteristic cupping has taken place, the diagnosis of glaucoma is easy; the challenge lies in diligently assessing the optic nerve and peripapillary tissues prior to development of significant structural and functional damage in order to make an accurate diagnosis as early as possible. By utilizing the steps outlined below, one should be able to become proficient in this evaluation over time in order to prevent under diagnosis, delayed diagnosis, as well as over diagnosis of a disease that is still in many ways very elusive even to the most seasoned clinician.
10 Figure 3: Color photograph of the right eye demonstrating prominent laminar dot sign, inferior notch between 7 8 o clock, temporal zone beta and alpha peripapillary atrophy, and nasal zone beta peripapillary atrophy. Optic Nerve Evaluation Checklist o o o o o o Measure the vertical size of the optic nerve at the slit lamp through dilated pupils Determine the vertical and horizontal C/D ratio and consider it carefully in relation to the size of the disc Evaluate the integrity of the neuroretinal rim, specifically looking for the presence of diffuse thinning, notching, and pallor keep in mind that the ISNT rule should be observed for the average vertically oval optic nerve Evaluate for the presence of any vascular changes: disc hemorrhages, nasalization of vessels, baring of vessels, optociliary shunt vessels, and arteriole narrowing Evaluate for the presence and extent of peripapillary atrophy Evaluate the integrity of the RNFL with a red free filter
11 References: 1. Broadway DC, Nicolela MT, Drance SM. Optic Disc Appearances in Primary Open Angle Glaucoma. Survey of Ophthalmology. 1999;43(1):S223 S Burgoyne CF, Downs JC. Premise and prediction how optic nerve head biomechanics underlies the susceptibility and clinical behavior of the aged optic nerve head. J Glaucoma. 2008; 17: Chui TYP, Zhong Z, Burns SA. The relationship between peripapillary crescent and axial length: Implications for differential eye growth. Vision Research. 2011;51: Curico et al. Peripapillary Chorioretinal Atrophy: Bruch's Membrane Changes and Photoreceptor Loss. Ophthalmology. 2000;107(2): De Moraes CG et al. Predictive factors within the optic nerve complex for glaucoma progression: disc hemorrhage and parapapillary atrophy. Asia Pacific J Ophthalmol. 2012; 1(2): Fingeret M et al. Five rules to evaluate the optic disc and retinal nerve fiber layer for glaucoma. Optometry. 2005;76(11): Grosvenor T. (2007). Primary Care Optometry. (pp. 153). St. Louis: Butterworth Heinmann Elsevier. 8. Hayreh SS. Blood supply of the optic nerve head and its role in optic atrophy, glaucoma, and oedema of the optic disc. Brit J Ophthal. 1969;53: Hayreh, S.S. (2011). Ischemic Optic Neuropathies. (pp. 7 35). New York: Springer. 10. Hoffmann EM et al. Optic Disk Size and Glaucoma. Survey of Ophthalmology. 2007;52(1): Jonas JB, Budde WM. Diagnosis and Pathogenesis of Glaucomatous Optic Neuropathy: Morphological Aspects. Progress in Retinal and Eye Research. 2000;19(1): Jonas JB. Clinical implications of peripapillary atrophy in glaucoma. Current Opinion in Ophthalmology. 2005;16: Jonas JB, Dichtl A. Evaluation of the Retinal Nerve Fiber Layer. Survey of Ophthalmology. 1996;40(5): Jonas JB, Budde WM, Panda Jonas S. Ophthalmoscopic Evaluation of the Optic Nerve Head. Survey of Ophthalmology. 1999;43(4): Kampougeris G et al. Peripapillary retinal nerve fibre layer thickness measurement with SD OCT in normal and glaucomatous eyes: distribution and correlation with age. International Journal of Ophthalmology. 2013;6(5): Lee EJ et al. Visualization of the Lamina Cribrosa Using Enhanced Depth Imaging Spectral Domain Optical Coherence Tomography. American Journal of Ophthalmology. 2011;152(1): Lee JLS, Nicolela MT, Chauhan BC. Rates of Neuroretinal Rim and Peripapillary Atrophy Area Change. Ophthalmology. 2009;116: Lim CS, O Brien C, Bolton NM. A simple clinical method to measure the optic disk size in glaucoma. J Glaucoma. 1996;5: Reis ASC, Toren A, Nicolela MT. Clinical Optic Disc Evaluation in Glaucoma. European Ophthalmic Review. 2012;6(2): Sigal IA et al. Factors influencing optic nerve head biomechanics. Invest Ophthalmol Vis Sci. 2005; 46(11): Spaeth GL et al. Systems for Staging the Amount of Optic Nerve Damage in Glaucoma: A Critical Review and New Material. Survey of Ophthalmology. 2006;51(4): Uhm KB et al. Peripapillary Atrophy in Normal and Primary Open Angle Glaucoma. Korean Journal of Ophthalmology. 1998;12:37 50.
12 May/June Optic Nerve Evaluation in Glaucoma (TPG) Name License 1. Approximately how many ganglion cell axons leave through the scleral canal in a healthy eye? a. 0.5 million b. 1.5 million c. 2.5 million d. 3.0 million 2. Which of the following vascular channels supplies arterial blood to the pre laminar optic nerve? a. Central retinal artery b. Long posterior ciliary artery c. Short posterior ciliary artery d. Pial vascular plexus 3. Which of the following measurements of the vertical height of the optic nerve would indicate a smaller than average disc size? a. 1.5mm b. 1.8mm c. 2.0mm d. 2.2mm 4. When using a Volk 78D condensing fundus lens to measure the vertical height of the optic nerve, which of the following is the correction factor that should be utilized in order to record the height of the optic nerve in millimeters? 5. a. 1.0x b. 1.1x c. 1.2x d. 1.3x 6. Which of the following is a TRUE statement regarding zone alpha peripapillary atrophy? a. It is caused by a complete loss of RPE and choriocapillaris b. It is more commonly found in patients with glaucoma c. Its temporal edge is bounded by normal retina d. It is usually found in an area of neuroretinal rim thinning 6. Which of the following statements is TRUE about drance hemorrhages? a. They are typically seen in very advanced glaucoma b. They typically resolve in 1 2 weeks c. They are indicative of disease stability d. They may be caused by posterior vitreous detachment 7. Which of the following statements is TRUE about the retinal nerve fiber layer? a. The nasal bundles are typically the brightest b. The papillomacular bundles are typically the brightest c. It is best visualized with a red free filter d. It is best visualized with a diffuse white light 8. Which of the following findings would arouse the MOST suspicion for possible glaucomatous optic nerve damage? a. C/D ratio of 0.3 in a 1.5mm sized nerve b. C/D ratio of 0.3 in a 2.0mm sized nerve c. C/D ratio of 0.5 in a 2.2mm sized nerve d. C/D ratio of 0.8 in a 2.6mm sized nerve 9. Which of the following vascular changes is typically seen in very advanced glaucomatous optic nerve damage? a. Retinal artery attenuation b. Baring of circumlinear vessels c. Nasalization of blood vessels d. Increased sharpness of blood vessels 10. Approximately how many ganglion cells may be lost before visual field defects are detected on standard automated perimetry? a. 5 15% b % c % d %
The Optic Nerve Head In Glaucoma. Clinical Pearl #1. Characteristics of Normal Disk 9/26/2017. Initial detectable damage Structure vs function
 The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
The Optic Nerve Head In Glaucoma Clinical Pearl #1 Eric E. Schmidt, O.D., F.A.A.O. Omni Eye Specialists Wilmington,NC schmidtyvision@msn.com Glaucoma is an optic neuropathy Initial detectable damage Structure
Dr/ Marwa Abdellah EOS /16/2018. Dr/ Marwa Abdellah EOS When do you ask Fluorescein angiography for optic disc diseases???
 When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
When do you ask Fluorescein angiography for optic disc diseases??? 1 NORMAL OPTIC DISC The normal optic disc on fluorescein angiography is fluorescent due to filling of vessels arising from the posterior
Beyond the C/D Ratio: Evaluating a Glaucomatous Optic Nerve. Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic COPE ID#: GL
 Beyond the C/D Ratio: Evaluating a Glaucomatous Optic Nerve Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic COPE ID#: 27809-GL Points to Remember Glaucoma affects the ONH in characteristic patterns
Beyond the C/D Ratio: Evaluating a Glaucomatous Optic Nerve Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic COPE ID#: 27809-GL Points to Remember Glaucoma affects the ONH in characteristic patterns
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
The evaluation of the optic nerve and retinal nerve
 Five rules to evaluate the optic disc and retinal nerve fiber layer for glaucoma Murray Fingeret, O.D., a,b Felipe A. Medeiros, M.D., c Remo Susanna, Jr, M.D., d and Robert N. Weinreb, M.D. c a Department
Five rules to evaluate the optic disc and retinal nerve fiber layer for glaucoma Murray Fingeret, O.D., a,b Felipe A. Medeiros, M.D., c Remo Susanna, Jr, M.D., d and Robert N. Weinreb, M.D. c a Department
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed?
 Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
Optic Disc Evaluation: Is the Optic Disc Glaucomatous and Has it Progressed? Jody Piltz-Seymour, M.D. Clinical Professor Perelman School of Medicine University of Pennsylvania Wills Glaucoma Service Valley
Optic Nerve: Clinical Examination
 Optic Nerve: Clinical Examination Marcelo T. Nicolela 2 Core Messages Optic disc evaluation is of fundamental importance in the management of glaucoma. Clinical examination of the optic disc is best performed
Optic Nerve: Clinical Examination Marcelo T. Nicolela 2 Core Messages Optic disc evaluation is of fundamental importance in the management of glaucoma. Clinical examination of the optic disc is best performed
Ophthalmoscopic Evaluation of the Optic Nerve Head JOST B. JONAS, MD, WIDO M. BUDDE, MD, AND SONGHOMITRA PANDA-JONAS, MD
 SURVEY OF OPHTHALMOLOGY VOLUME 43 NUMBER 4 JANUARY FEBRUARY 1999 MAJOR REVIEW Ophthalmoscopic Evaluation of the Optic Nerve Head JOST B. JONAS, MD, WIDO M. BUDDE, MD, AND SONGHOMITRA PANDA-JONAS, MD Department
SURVEY OF OPHTHALMOLOGY VOLUME 43 NUMBER 4 JANUARY FEBRUARY 1999 MAJOR REVIEW Ophthalmoscopic Evaluation of the Optic Nerve Head JOST B. JONAS, MD, WIDO M. BUDDE, MD, AND SONGHOMITRA PANDA-JONAS, MD Department
Early Detection Of Glaucoma Clinical Clues. Points To Live By. Glaucoma Risk Factors 10/3/2014
 Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com Points To Live By 25% of G pxs NEVER have IOP >21mm 50% of G pxs have trough
Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com Points To Live By 25% of G pxs NEVER have IOP >21mm 50% of G pxs have trough
A Review Of Risk Factors. Early Detection Of Glaucoma Clinical Clues. A risk factor analysis is critical. Points To Live By
 A Review Of Risk Factors Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com FINDACAR Family history IOP Nearsightedness Diabetes/Vascular
A Review Of Risk Factors Early Detection Of Glaucoma Clinical Clues Eric E. Schmidt, O.D. Omni Eye Specialists Wilmington, NC schmidtyvision@msn.com FINDACAR Family history IOP Nearsightedness Diabetes/Vascular
Advances in OCT Murray Fingeret, OD
 Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
Disclosures Advances in OCT Murray Fingeret, OD Consultant Alcon, Allergan, Bausch & Lomb, Carl Zeiss Meditec, Diopsys, Heidelberg Engineering, Reichert, Topcon Currently Approved OCT Devices OCT Devices
The Missing Piece in Glaucoma?
 Open Journal of Ophthalmology, 2016, 6, 56-62 Published Online February 2016 in SciRes. http://www.scirp.org/journal/ojoph http://dx.doi.org/10.4236/ojoph.2016.61008 The Missing Piece in Glaucoma? Syed
Open Journal of Ophthalmology, 2016, 6, 56-62 Published Online February 2016 in SciRes. http://www.scirp.org/journal/ojoph http://dx.doi.org/10.4236/ojoph.2016.61008 The Missing Piece in Glaucoma? Syed
10/27/2013. Optic Red Herrings
 Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
Optic Red Herrings 1 Optic neuropathy Compressive Inflammatory Toxic Glaucomatous Ischemic Post traumatic GLAUCOMATOUS OPTIC NEUROPATHY Glaucoma: Traditionally defined as a progressive optic neuropathy
THE EYE: RETINA AND GLOBE
 Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Neuroanatomy Suzanne Stensaas February 24, 2011, 10:00-12:00 p.m. Reading: Waxman Ch. 15. Your histology and gross anatomy books should be useful. Reading: Histology of the Eye from any histology book
Evaluating Optic Nerve Damage: Pearls and Pitfalls
 54 The Open Ophthalmology Journal, 9, 3, 54-58 Evaluating Optic Nerve Damage: Pearls and Pitfalls Open Access Paul J. Mackenzie * and Frederick S. Mikelberg Division of Glaucoma, Department of Ophthalmology
54 The Open Ophthalmology Journal, 9, 3, 54-58 Evaluating Optic Nerve Damage: Pearls and Pitfalls Open Access Paul J. Mackenzie * and Frederick S. Mikelberg Division of Glaucoma, Department of Ophthalmology
Peripapillary circle of Zinn Haller revealed by fundus fluorescein angiography
 British Journal of Ophthalmology 1997;81:663 667 663 Department of Ophthalmology, School of Medicine, Hanyang University, Seoul, Korea M-K Ko D-S Kim Y-K Ahn Correspondence to: Myung-Kyoo Ko, MD, Department
British Journal of Ophthalmology 1997;81:663 667 663 Department of Ophthalmology, School of Medicine, Hanyang University, Seoul, Korea M-K Ko D-S Kim Y-K Ahn Correspondence to: Myung-Kyoo Ko, MD, Department
3/16/2018. Optic Nerve Examination. Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital
 Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
Optic Nerve Examination Hassan Eisa Swify FRCS Ed (Ophthalmology) Air Force Hospital 1 Examination Structure ( optic disc) Function Examination of the optic disc The only cranial nerve (brain tract) which
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
ADVANCED DIAGNOSTIC TECHNIQUES
 DIVISION OF VISION SCIENCES SESSION: 2008/2009 DIET: 1ST ADVANCED DIAGNOSTIC TECHNIQUES VISP216 LEVEL:2 MODULE LEADER: DR GUNTER LOFFLER B.Sc/B.Sc. (HONS) OPTOMETRY MAY 2009 DURATION: 2 HOURS CANDIDATES
DIVISION OF VISION SCIENCES SESSION: 2008/2009 DIET: 1ST ADVANCED DIAGNOSTIC TECHNIQUES VISP216 LEVEL:2 MODULE LEADER: DR GUNTER LOFFLER B.Sc/B.Sc. (HONS) OPTOMETRY MAY 2009 DURATION: 2 HOURS CANDIDATES
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
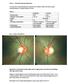 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
OCT in the Diagnosis and Follow-up of Glaucoma
 OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
OCT in the Diagnosis and Follow-up of Glaucoma Karim A Raafat MD. Professor Of Ophthalmology Cairo University Hmmmm! Do I have Glaucoma or not?! 1 Visual Function 100% - N Gl Structure : - 5000 axon /
Question 1: Comment on the optic nerve appearance of each eye.
 Case 2 - Right Optic Nerve Head Drusen (ONHD) A 41 year old female was referred by her optometrist for a workup for unilateral optic disc drusen, OCT, and visual field changes. The patient was otherwise
Case 2 - Right Optic Nerve Head Drusen (ONHD) A 41 year old female was referred by her optometrist for a workup for unilateral optic disc drusen, OCT, and visual field changes. The patient was otherwise
Funduscopic Interpretation Understanding the Fundus: is that normal?
 Funduscopic Interpretation Understanding the Fundus: is that normal? Gillian McLellan BVMS PhD DVOphthal DECVO DACVO MRCVS With thanks to Christine Heinrich and all who contributed images Fundus Retina
Funduscopic Interpretation Understanding the Fundus: is that normal? Gillian McLellan BVMS PhD DVOphthal DECVO DACVO MRCVS With thanks to Christine Heinrich and all who contributed images Fundus Retina
FACING YOUR FUNDIC FEARS: EXAMINATION OF THE OCULAR FUNDUS J. Seth Eaton, VMD, DACVO Cornell University Veterinary Specialists
 FACING YOUR FUNDIC FEARS: EXAMINATION OF THE OCULAR FUNDUS J. Seth Eaton, VMD, DACVO Cornell University Veterinary Specialists The goal of a thorough fundus examination is to clinically evaluate the structures
FACING YOUR FUNDIC FEARS: EXAMINATION OF THE OCULAR FUNDUS J. Seth Eaton, VMD, DACVO Cornell University Veterinary Specialists The goal of a thorough fundus examination is to clinically evaluate the structures
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD
 New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
New Concepts in Glaucoma Ben Gaddie, OD Moderator Murray Fingeret, OD Louis Pasquale, MD New Concepts in Glaucoma Optical Coherence Tomography: Is it necessary and needed to diagnose and monitor glaucoma?
The optic disc in glaucoma, III: diffuse optic disc pallor with raised intraocular pressure
 British Journal of Ophthalmology, 1978, 62, 670-675 The optic disc in glaucoma, III: diffuse optic disc pallor with raised intraocular pressure R. A. HITCHINGS From the Institute of Ophthalmology, Moorfields
British Journal of Ophthalmology, 1978, 62, 670-675 The optic disc in glaucoma, III: diffuse optic disc pallor with raised intraocular pressure R. A. HITCHINGS From the Institute of Ophthalmology, Moorfields
Evaluation of ONH Pallor in Glaucoma Patients and Suspects. Leticia Rousso, O.D. Joseph Sowka, O.D
 Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
Evaluation of ONH Pallor in Glaucoma Patients and Suspects Leticia Rousso, O.D Joseph Sowka, O.D I. Abstract This case report will evaluate a young glaucoma suspect with unilateral sectoral optic nerve
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
What Is O.C.T. and Why Should I Give A Rip? OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist 5/19/2014
 OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema. Jonathan A. Micieli, MD Valérie Biousse, MD
 Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Study of correlation of cup disc ratio with visual field loss in primary open angle glaucoma
 Original Research Article DOI: 10.18231/2395-1451.2017.0003 Study of correlation of cup disc ratio with visual field loss in primary open angle glaucoma Pankaj Soni 1,*, Ashwani Srivastava 2, Akash Srivastava
Original Research Article DOI: 10.18231/2395-1451.2017.0003 Study of correlation of cup disc ratio with visual field loss in primary open angle glaucoma Pankaj Soni 1,*, Ashwani Srivastava 2, Akash Srivastava
Patterns of Subsequent Progression of Localized Retinal Nerve Fiber Layer Defects on Red-free Fundus Photographs in Normal-tension Glaucoma
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(4):330-336 http://dx.doi.org/10.3341/kjo.2014.28.4.330 Original Article Patterns of Subsequent Progression of Localized Retinal Nerve Fiber
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Il contributo dell'angio-oct: valutazione integrata della componente nervosa e vascolare della malattia glaucomatosa
 SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
SIMPOSIO G.O.A.L. - LE NUOVE FRONTIERE DIAGNOSTICHE E LE LINEE DI INDIRIZZO AMBULATORIALI DEL GLAUCOMA Coordinatore e moderatore: D. Mazzacane Presidente: L. Rossetti Il contributo dell'angio-oct: valutazione
1/25/2019 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! THE ORIGINAL RAGING GLAUCOMA OCT RETINAL IMAGING OPTIC NERVE HEAD EXAMINATION
 OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
OCT & OCTA RETINAL IMAGING: HOW TO PREVENT RAGING GLAUCOMA! Craig Thomas, O.D. 3900 West Wheatland Road Dallas, Texas 75237 972-780-7199 thpckc@yahoo.com THE ORIGINAL RAGING GLAUCOMA 47-year-old Black
Cirrus TM HD-OCT. Details defi ne your decisions
 Cirrus TM HD-OCT Details defi ne your decisions 2 With high-defi nition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl
Cirrus TM HD-OCT Details defi ne your decisions 2 With high-defi nition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl
(the 'laminar dots' sign (Reed and Spaeth, 1974));
 Brit. Y. Ophthal. (1976) 6o, 778 The optic disc i: Classification in glaucoma R. A. HITCHINGS Moorfields Eye Hospital, City Road, London AND G. L. SPAETH Wills Eye Hospital, Spring Garden Street, Philadelphia
Brit. Y. Ophthal. (1976) 6o, 778 The optic disc i: Classification in glaucoma R. A. HITCHINGS Moorfields Eye Hospital, City Road, London AND G. L. SPAETH Wills Eye Hospital, Spring Garden Street, Philadelphia
Moving forward with a different perspective
 Moving forward with a different perspective The Leader In Vision Diagnostics Offers A New Perspective Marco has served the eyecare community by offering exceptional lane products and automated high tech
Moving forward with a different perspective The Leader In Vision Diagnostics Offers A New Perspective Marco has served the eyecare community by offering exceptional lane products and automated high tech
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
THE NERVE FIBER LAYER ITS VALUE IN THE DIAGNOSIS AND MANAGEMENT OF GLAUCOMA. Tamara Bonnes. Spring 1993
 THE NERVE FIBER LAYER & ITS VALUE IN THE DIAGNOSIS AND MANAGEMENT OF GLAUCOMA Tamara Bonnes Spring 1993 I. Introduction In the past six months, many of the faculty and also my fellow students have inquired
THE NERVE FIBER LAYER & ITS VALUE IN THE DIAGNOSIS AND MANAGEMENT OF GLAUCOMA Tamara Bonnes Spring 1993 I. Introduction In the past six months, many of the faculty and also my fellow students have inquired
Zinn Haller arterial ring observed by ICG angiography in high myopia
 Br J Ophthalmol 1998;82:1357 1362 1357 ORIGINAL ARTICLES Clinical science Department of Ophthalmology, School of Medicine, Tokyo Medical and Dental University, Japan K Ohno-Matsui S Futagami S Yamashita
Br J Ophthalmol 1998;82:1357 1362 1357 ORIGINAL ARTICLES Clinical science Department of Ophthalmology, School of Medicine, Tokyo Medical and Dental University, Japan K Ohno-Matsui S Futagami S Yamashita
The Glaucoma Suspect. Evaluating the Suspect Disk. Dr Michael Forrest. ! the usual suspects: ! is it glaucoma? ! is it swollen?
 Evaluating the Suspect Disk Dr Michael Forrest Senior Lecturer, The University of Queensland Northside Eye Specialists, Nundah Visiting Ophthalmologist, Mater Hospital, Brisbane Australian Vision Convention
Evaluating the Suspect Disk Dr Michael Forrest Senior Lecturer, The University of Queensland Northside Eye Specialists, Nundah Visiting Ophthalmologist, Mater Hospital, Brisbane Australian Vision Convention
The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation
 C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
C L I N I C A L S C I E N C E The Effect of Pupil Dilation on Scanning Laser Polarimetry With Variable Corneal Compensation Amjad Horani, MD; Shahar Frenkel, MD, PhD; Eytan Z. Blumenthal, MD BACKGROUND
Optic Disc: Anatomy, Variants, Unusual discs. Kathleen B. Digre, MD Professor Neurology, Ophthalmology
 Optic Disc: Anatomy, Variants, Unusual discs Kathleen B. Digre, MD Professor Neurology, Ophthalmology THE OPHTHALMOSCOPE DIRECT OPHTHALMOSCOPY Jan Purkinje 1823 Hermann von Helmholtz 1851 Hand held ophthalmoscope
Optic Disc: Anatomy, Variants, Unusual discs Kathleen B. Digre, MD Professor Neurology, Ophthalmology THE OPHTHALMOSCOPE DIRECT OPHTHALMOSCOPY Jan Purkinje 1823 Hermann von Helmholtz 1851 Hand held ophthalmoscope
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion
 Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
OCT Angiography in Primary Eye Care
 OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
S uperior segmental optic hypoplasia (SSOH), also termed
 910 CLINICAL SCIENCE Optical coherence tomography of superior segmental optic hypoplasia K Unoki, N Ohba, W F Hoyt... See end of article for authors affiliations... Correspondence to: Kazuhiko Unoki, MD,
910 CLINICAL SCIENCE Optical coherence tomography of superior segmental optic hypoplasia K Unoki, N Ohba, W F Hoyt... See end of article for authors affiliations... Correspondence to: Kazuhiko Unoki, MD,
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature of
 1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
1.2.4 OPHTHALMOLOGICAL ABNORMALITIES Ocular abnormalities are well documented in patients with NPS 6 62 81 95. 1.2.4.1 Glaucoma Glaucoma is a complication which has only recently been confirmed as a feature
Step 4: Ask permission to turn off lights or draw the curtains
 STEPS OF EYE EXAMINATION - FUNDUS Step 1: Approach the patient Read the instructions carefully for clues Shake hands, introduce yourself Ask permission to examine him I would like to examine your eyes,
STEPS OF EYE EXAMINATION - FUNDUS Step 1: Approach the patient Read the instructions carefully for clues Shake hands, introduce yourself Ask permission to examine him I would like to examine your eyes,
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Optical coherence tomography of the retinal nerve fibre layer in mild papilloedema and pseudopapilloedema
 294 SCIENTIFIC REPORT Optical coherence tomography of the retinal nerve fibre layer in mild papilloedema and pseudopapilloedema E Z Karam, T R Hedges... Aims: To determine the degree to which optical coherence
294 SCIENTIFIC REPORT Optical coherence tomography of the retinal nerve fibre layer in mild papilloedema and pseudopapilloedema E Z Karam, T R Hedges... Aims: To determine the degree to which optical coherence
SOUTH-EAST EUROPEAN JOURNAL of OPHTHALMOLOGY 2015; 1 (1) 34 40
 Review article SOUTH-EAST EUROPEAN JOURNAL of OPHTHALMOLOGY 2015; 1 (1) 34 40 Retinal nerve fiber layer versus peripapillary capillary density assessment A powerful tool for detecting optic nerve head
Review article SOUTH-EAST EUROPEAN JOURNAL of OPHTHALMOLOGY 2015; 1 (1) 34 40 Retinal nerve fiber layer versus peripapillary capillary density assessment A powerful tool for detecting optic nerve head
OtticaFisiopatologica
 Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Anno quindicesimo dicembre 2010 How to assess the retinal nerve fiber layer thickness Antonio Ferreras Miguel Servet University Hospital, Zaragoza. Aragón Health Sciences Institute University of Zaragoza
Two Pits in a Pod: Using EDI-OCT to evaluate the lamina cribrosa in a patient with openangle glaucoma and multiple optic pits
 Two Pits in a Pod: Using EDI-OCT to evaluate the lamina cribrosa in a patient with openangle glaucoma and multiple optic pits Abstract: EDI-OCT imaging is used to evaluate glaucoma by examining the thinning
Two Pits in a Pod: Using EDI-OCT to evaluate the lamina cribrosa in a patient with openangle glaucoma and multiple optic pits Abstract: EDI-OCT imaging is used to evaluate glaucoma by examining the thinning
T he optic disc as the bottleneck of the whole visual
 189 CLINICAL SCIENCE Optic disc morphology in south India: the Vellore Eye Study J B Jonas, R Thomas, R George, E Berenshtein, J Muliyil... See end of article for authors affiliations... Correspondence
189 CLINICAL SCIENCE Optic disc morphology in south India: the Vellore Eye Study J B Jonas, R Thomas, R George, E Berenshtein, J Muliyil... See end of article for authors affiliations... Correspondence
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Diagnosis. Definition of Glaucoma. Diagnosing Glaucoma. Vision Institute Annual Fall Conference
 Glaucoma Diagnosis Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Definition of Glaucoma Glaucoma can be regarded
Glaucoma Diagnosis Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Definition of Glaucoma Glaucoma can be regarded
Parapapillary Atrophy and Retinal Vessel Diameter in Nonglaucomatous Optic Nerve Damage
 Investigative Ophthalmology & Visual Science, Vol. 32, No. 11, October 1991 Copyright Association for Research in Vision and Ophthalmology Parapapillary Atrophy and Retinal Vessel Diameter in Nonglaucomatous
Investigative Ophthalmology & Visual Science, Vol. 32, No. 11, October 1991 Copyright Association for Research in Vision and Ophthalmology Parapapillary Atrophy and Retinal Vessel Diameter in Nonglaucomatous
The Pathology and Pathogenesis of Acute Glaucoma in Dogs. Richard R Dubielzig
 The Pathology and Pathogenesis of Acute Glaucoma in Dogs Richard R Dubielzig Overview of Glaucoma Intraocular Pressure too High to Support a Healthy Optic Nerve Terminology used in the classification of
The Pathology and Pathogenesis of Acute Glaucoma in Dogs Richard R Dubielzig Overview of Glaucoma Intraocular Pressure too High to Support a Healthy Optic Nerve Terminology used in the classification of
Recent studies have suggested that the pattern of loss of
 Influence of Cilioretinal Arteries on Neuroretinal Rim and Parapapillary Atrophy in Glaucoma Wido M. Budde 1,2 and Jost B. Jonas 1,2 PURPOSE. The pattern of neuroretinal rim loss and increase in the area
Influence of Cilioretinal Arteries on Neuroretinal Rim and Parapapillary Atrophy in Glaucoma Wido M. Budde 1,2 and Jost B. Jonas 1,2 PURPOSE. The pattern of neuroretinal rim loss and increase in the area
Localised retinal nerve fibre layer defects in. chronic experimental high pressure glaucoma. rhesus monkeys. Jost B Jonas, Sohan Singh Hayreh
 Br J Ophthalmol 1999;83:1291 1295 1291 Department of Ophthalmology and Eye Hospital, Friedrich-Alexander- University Erlangen-Nürnberg in Erlangen, Schwabachanlage 6, 91054 Erlangen, Germany J B Jonas
Br J Ophthalmol 1999;83:1291 1295 1291 Department of Ophthalmology and Eye Hospital, Friedrich-Alexander- University Erlangen-Nürnberg in Erlangen, Schwabachanlage 6, 91054 Erlangen, Germany J B Jonas
Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications
 United States and Canadian Academy of Pathology 2007 Annual Meeting Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications J. Douglas Cameron, MD Professor of Ophthalmology Mayo Clinic School
United States and Canadian Academy of Pathology 2007 Annual Meeting Shaken Baby Syndrome (SBS) Ocular Findings with Legal Implications J. Douglas Cameron, MD Professor of Ophthalmology Mayo Clinic School
Differences between Non-arteritic Anterior Ischemic Optic Neuropathy and Open Angle Glaucoma with Altitudinal Visual Field Defect
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2015;29(6):418-423 http://dx.doi.org/10.3341/kjo.2015.29.6.418 Original Article Differences between Non-arteritic Anterior Ischemic Optic Neuropathy
Year 2 MBChB Clinical Skills Session Ophthalmoscopy. Reviewed & ratified by: Mr M Batterbury Consultant Ophthalmologist
 Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
Year 2 MBChB Clinical Skills Session Ophthalmoscopy Reviewed & ratified by: o Mr M Batterbury Consultant Ophthalmologist Learning objectives o To understand the anatomy and physiology of the external and
Medicine. Observational Study. 1. Introduction OPEN
 Observational Study Medicine The association between prelaminar tissue thickness and peripapillary choroidal thickness in untreated normal-tension glaucoma patients Ji-Hye Park, MD, PhD a, Chungkwon Yoo,
Observational Study Medicine The association between prelaminar tissue thickness and peripapillary choroidal thickness in untreated normal-tension glaucoma patients Ji-Hye Park, MD, PhD a, Chungkwon Yoo,
Perspectives on Screening for Diabetic Retinopathy. Dr. Dan Samaha, Optometrist, MSc Clinical Lecturer School of Optometry, Université de Montréal
 Perspectives on Screening for Diabetic Retinopathy 1 Dr. Dan Samaha, Optometrist, MSc Clinical Lecturer School of Optometry, Université de Montréal Current standards 2 According to the Canadian Diabetes
Perspectives on Screening for Diabetic Retinopathy 1 Dr. Dan Samaha, Optometrist, MSc Clinical Lecturer School of Optometry, Université de Montréal Current standards 2 According to the Canadian Diabetes
Singapore Eye Research Institute, Singapore
 AGLAIA System Architecture for Glaucoma Diagnosis J. Liu *, D.W.K. Wong *, N.M. Tan *, Z. Zhang *, F. Yin *, J. Cheng *, B.H. Lee *, Z.Y. Liang *, J.H. Lim *, H. Li *, T.Y. Wong * Institute For Infocomm
AGLAIA System Architecture for Glaucoma Diagnosis J. Liu *, D.W.K. Wong *, N.M. Tan *, Z. Zhang *, F. Yin *, J. Cheng *, B.H. Lee *, Z.Y. Liang *, J.H. Lim *, H. Li *, T.Y. Wong * Institute For Infocomm
Parapapillary Gamma Zone and Axial Elongation Associated Optic Disc Rotation: The Beijing Eye Study
 Anatomy and Pathology/Oncology Parapapillary Gamma Zone and Axial Elongation Associated Optic Disc Rotation: The Beijing Eye Study Jost B. Jonas, 1,2 Ya Xing Wang, 1 Qi Zhang, 1 Yuan Yuan Fan, 3 Liang
Anatomy and Pathology/Oncology Parapapillary Gamma Zone and Axial Elongation Associated Optic Disc Rotation: The Beijing Eye Study Jost B. Jonas, 1,2 Ya Xing Wang, 1 Qi Zhang, 1 Yuan Yuan Fan, 3 Liang
Structural examina.on: Imaging
 ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
ManaMa: Glaucoma Structural examina.on: Imaging Luís Abegão Pinto, MD, PhD Department of Ophthalmology CHLC Lisbon Faculty of Medicine, Lisbon University 1 11-10- 2013 Structural changes Qualitative changes
EXPERIMENTAL AND THERAPEUTIC MEDICINE 6: , 2013
 268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
268 Comparison of optic nerve morphology in eyes with glaucoma and eyes with non-arteritic anterior ischemic optic neuropathy by Fourier domain optical coherence tomography YUXIN YANG 1, HAITAO ZHANG 1,
Glaucoma Evaluation. OCT Pearls for Glaucoma. OCT: Retinal Nerve Fiber Layer. Financial Disclosures. OCT: Macula. Case Example
 OCT Pearls for Glaucoma using OCT of the macula for glaucoma Glaucoma Evaluation Right eye Visual Acuity 20/25 20/25 IOP 13 13 Central corneal 530 530 thickness Anterior exam Normal with PCIOL Normal with
OCT Pearls for Glaucoma using OCT of the macula for glaucoma Glaucoma Evaluation Right eye Visual Acuity 20/25 20/25 IOP 13 13 Central corneal 530 530 thickness Anterior exam Normal with PCIOL Normal with
Analysis of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography
 Analysis of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters.
Analysis of Peripapillary Atrophy Using Spectral Domain Optical Coherence Tomography The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters.
Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy young patients
 Moon et al. BMC Ophthalmology (2018) 18:172 https://doi.org/10.1186/s12886-018-0833-z CASE REPORT Open Access Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy
Moon et al. BMC Ophthalmology (2018) 18:172 https://doi.org/10.1186/s12886-018-0833-z CASE REPORT Open Access Intrapapillary hemorrhage with concurrent peripapillary and vitreous hemorrhage in two healthy
This study was limited to those discs in which all 3 THE CRESCENT
 British Journal of Ophthalmology, 1978, 62, 16-20 The tilted disc DAVID DORRELL From the Department of Neuro-Ophthalmology, National Hospitals for Nervous Diseases, Queen Square, London SUMMARY Sixty tilted
British Journal of Ophthalmology, 1978, 62, 16-20 The tilted disc DAVID DORRELL From the Department of Neuro-Ophthalmology, National Hospitals for Nervous Diseases, Queen Square, London SUMMARY Sixty tilted
Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD
 Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD Figure 1. Normal OCT of the macula (cross section through the line indicated on the fundus photo)
Ganglion cell analysis by optical coherence tomography (OCT) Jonathan A. Micieli, MD Valérie Biousse, MD Figure 1. Normal OCT of the macula (cross section through the line indicated on the fundus photo)
SOCT Copernicus REVO. * - Currently import and overlay are avaibale in manual mode only
 SOCT Copernicus REVO Easy Operation (Full auto & Auto mode) Auto alignment (Z-position, C-gate, Focus, Tomogram) Voice guide (support patient through examination) Powerful analysis tools Enhanced tomograms
SOCT Copernicus REVO Easy Operation (Full auto & Auto mode) Auto alignment (Z-position, C-gate, Focus, Tomogram) Voice guide (support patient through examination) Powerful analysis tools Enhanced tomograms
Influence of Myopic Disc Shape on the Diagnostic Precision of the Heidelberg Retina Tomograph
 Influence of Myopic Disc Shape on the Diagnostic Precision of the Heidelberg Retina Tomograph Yoshio Yamazaki,* Keiji Yoshikawa, Shiho Kunimatsu, Nobuyuki Koseki, Yasuyuki Suzuki, Shun Matsumoto and Makoto
Influence of Myopic Disc Shape on the Diagnostic Precision of the Heidelberg Retina Tomograph Yoshio Yamazaki,* Keiji Yoshikawa, Shiho Kunimatsu, Nobuyuki Koseki, Yasuyuki Suzuki, Shun Matsumoto and Makoto
Histology of the Eye
 Histology of the Eye Objectives By the end of this lecture, the student should be able to describe: The general structure of the eye. The microscopic structure of:»cornea.»retina. EYE BULB Three coats
Histology of the Eye Objectives By the end of this lecture, the student should be able to describe: The general structure of the eye. The microscopic structure of:»cornea.»retina. EYE BULB Three coats
Follow up of focal narrowing of retinal arterioles in glaucoma
 Br J Ophthalmol 1999;83:285 289 285 Department of Ophthalmology and Eye Hospital, Friedrich-Alexander- University Erlangen-Nürnberg, Erlangen, Germany K I Papastathopoulos J B Jonas Correspondence to:
Br J Ophthalmol 1999;83:285 289 285 Department of Ophthalmology and Eye Hospital, Friedrich-Alexander- University Erlangen-Nürnberg, Erlangen, Germany K I Papastathopoulos J B Jonas Correspondence to:
Cerebrospinal Fluid Pressure and Glaucoma
 Review Article Cerebrospinal Fluid Pressure and Glaucoma Jost B. Jonas 1, MD; Ningli Wang 2, MD 1Department of Ophthalmology, Medical Faculty Mannheim, University of Heidelberg, Germany 2Beijing Tongren
Review Article Cerebrospinal Fluid Pressure and Glaucoma Jost B. Jonas 1, MD; Ningli Wang 2, MD 1Department of Ophthalmology, Medical Faculty Mannheim, University of Heidelberg, Germany 2Beijing Tongren
Goals. Glaucoma PARA PEARL TO DO. Vision Loss with Glaucoma
 Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
Glaucoma Janet R. Fett, OD Drs. Kincaid, Fett and Tharp So Sioux City, NE eyewear21@hotmail.com Goals Understand Glaucoma Disease process Understand how your data (objective and subjective) assists in
CHAPTER 2 LITERATURE REVIEW
 CHAPTER 2 LITERATURE REVIEW 2.1 Introduction The retina is a light-sensitive tissue lining the inner surface of the eye. The optics of the eye create an image of the visual world on the retina, which serves
CHAPTER 2 LITERATURE REVIEW 2.1 Introduction The retina is a light-sensitive tissue lining the inner surface of the eye. The optics of the eye create an image of the visual world on the retina, which serves
Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic Anterior Ischemic Optic Neuropathy and Optic Neuritis
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):289-294 http://dx.doi.org/10.3341/kjo.2016.30.4.289 Original Article Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2016;30(4):289-294 http://dx.doi.org/10.3341/kjo.2016.30.4.289 Original Article Analysis of Fundus Photography and Fluorescein Angiography in Nonarteritic
Cirrus TM HD-OCT. Details define your decisions
 Cirrus TM HD-OCT Details define your decisions 2 With high-definition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl Zeiss
Cirrus TM HD-OCT Details define your decisions 2 With high-definition OCT Carl Zeiss Meditec takes you beyond standard spectral domain Built on 10 years experience at the vanguard of innovation, Carl Zeiss
Seiji T. Takagi, Yoshiyuki Kita, Asuka Takeyama, and Goji Tomita. 1. Introduction. 2. Subjects and Methods
 Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
Ophthalmology Volume 2011, Article ID 914250, 5 pages doi:10.1155/2011/914250 Clinical Study Macular Retinal Ganglion Cell Complex Thickness and Its Relationship to the Optic Nerve Head Topography in Glaucomatous
Ganglion cell complex scan in the early prediction of glaucoma
 Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
Detection of Glaucoma Based on CDR, CAR and Blood Vessel Extraction
 402 P a g e INTERNATIONAL RESEARCH JOURNAL IN ADVANCED ENGINEERING AND TECHNOLOGY (IRJAET) www.irjaet.com ISSN (PRINT) : 2454-4744 ISSN (ONLINE): 2454-4752 Vol. 1, Issue 4, pp.402-411, December, 2015 Detection
402 P a g e INTERNATIONAL RESEARCH JOURNAL IN ADVANCED ENGINEERING AND TECHNOLOGY (IRJAET) www.irjaet.com ISSN (PRINT) : 2454-4744 ISSN (ONLINE): 2454-4752 Vol. 1, Issue 4, pp.402-411, December, 2015 Detection
Incorporating OCT Angiography Into Patient Care
 Incorporating OCT Angiography Into Patient Care Beth A. Steele, OD, FAAO OCT A: Introduction Isolates microvascular circulation from OCT image data Axial resolution = 5 microns (i.e. fine capillaries visible)
Incorporating OCT Angiography Into Patient Care Beth A. Steele, OD, FAAO OCT A: Introduction Isolates microvascular circulation from OCT image data Axial resolution = 5 microns (i.e. fine capillaries visible)
The use of a high-intensity laser to create an anastomotic
 Case Report 866 Laser Chorioretinal Venous Anastomosis for Progressive Nonischemic Central Retinal Vein Occlusion Chih-Hsin Chen, MD; Chien-Hsiung Lai 1, MD; Hsi-Kung Kuo, MD The use of high or medium-intensity
Case Report 866 Laser Chorioretinal Venous Anastomosis for Progressive Nonischemic Central Retinal Vein Occlusion Chih-Hsin Chen, MD; Chien-Hsiung Lai 1, MD; Hsi-Kung Kuo, MD The use of high or medium-intensity
p f .'''a.".: ;i.l i PAPILLOEDEMA brain. The ophthalmoscope may be looked upon as the Plate i is that of papilloedema of the optic nerve.
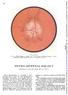 382 * s. ii d:.'. ; z. j:.'''a.".: : ;i.l i 4 PAPILLOEDEMA FIG. I.-Papilloedema or 'choked disc' due to raised intracranial tension. In this instance the papilloedema was due to a frontal lobe tumour.
382 * s. ii d:.'. ; z. j:.'''a.".: : ;i.l i 4 PAPILLOEDEMA FIG. I.-Papilloedema or 'choked disc' due to raised intracranial tension. In this instance the papilloedema was due to a frontal lobe tumour.
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
