Barrett s esophagus: lessons from recent clinical trials
|
|
|
- Lester Bell
- 5 years ago
- Views:
Transcription
1 INVITED REVIEW Annals of Gastroenterology (2016) 29, 1-7 Barrett s esophagus: lessons from recent clinical trials Daniela Golger, Andreas Probst, Helmut Messmann Klinikum Augsburg, Germany Abstract Data from recent studies cast doubt on former recommendations on diagnosis and management of Barrett s esophagus. Based on latest research findings several Gastroenterological Associations actualized their guidelines and international experts compiled consensus statements as practical help for clinicians. In this review we discuss recent trials and their impact on clinical practice, current recommendations and persisting controversies in Barrett s esophagus. Keywords Barrett s esophagus, esophageal adenocarcinoma, endoscopic eradication, endoscopic mucosal resection, endoscopic submucosal dissection Ann Gastroenterol 2016; 29 (4): 1-7 Introduction Barrett s esophagus (BE) and its underlying condition, gastroesophageal reflux disease (GERD), predispose to esophageal adenocarcinoma (EAC), a tumor whose incidence has risen dramatically in Western countries during the past decades (in the United States more than 6-fold in 40 years from 0.4 cases per in 1975 to 2.6 cases per in 2009 [1]). The prognosis of advanced tumor is poor with a 5-year survival for distant staged disease of only 2.8% [1]. If early carcinoma is detected the patient may be offered a potentially curative endoscopic resection (ER), or, if dysplasia is detected, endoscopic ablation to prevent progression to cancer. Hence, screening and surveillance for BE seem rational. Several studies showed that endoscopic surveillance leads to carcinoma detection at earlier stages and to more favorable survival [2]. However, recent studies also showed that the incidence of cancer and the risk of malignant progression among patients with non-dysplastic BE is considerably lower than previously thought [3-5]. Low-grade dysplasia (LGD) on the other hand seems to be an overdiagnosed but underestimated entity [6]. In the past years, tremendous advances evolved as well in ER and ablation techniques as in endoscopic imaging. But is there enough evidence to change practice and what are the lessons learned from recent studies to reconsider diagnostic and therapeutic strategies? Department of Gastroenterology, Klinikum Augsburg, Germany Conflict of Interest: None Correspondence to: Prof. Dr. Helmut Messmann, Department of Gastroenterology, Klinikum Augsburg, Stenglinstr. 2, Augsburg, Germany. helmut.messmann@klinikum-augsburg.de Received 21 March 2016; accepted 17 May 2016; published online 14 July 2016 DOI: Epidemiology and cancer risk: should we perform screening? Endoscopic screening is a controversial issue. The primary goal of screening is to identify patients with BE who will benefit from surveillance or therapy to prevent EAC. But first of all who actually should be screened? Known risk factors for BE and EAC are GERD, male sex, white race, older age, obesity, metabolic syndrome, tobacco use, hiatal hernia and a family history of GERD, BE or EAC [7]. The American Gastroenterological Association (AGA) recommends screening for BE in individuals older than 50 years with symptomatic GERD and at least 1 additional risk factor for EAC [8]. There is no definitive study that supports the assumed benefit of this strategy. But the major dilemma is that a significant proportion of patients with BE and EAC lack reflux symptoms. Approximately 50% of patients with shortsegment BE deny GERD symptoms and 40% of patients with EAC reported no history of prior GERD [9,10]. Also there are different opinions about the clinical importance of short BE. Another consideration that diminishes the usefulness of screening is the very low risk of malignant progression in nondysplastic BE. Recent population based studies and large metaanalysis showed an annual cancer incidence of only % in these patients and the risk even seems to further decrease over time with follow-up endoscopies showing no progression to dysplasia [3-5,11]. All in all, it is currently difficult to clearly identify the population at risk and more accurate methods for risk stratification are needed. Molecular biomarkers and nonendoscopic technologies for cell collection may help us in the future [12-14]. Promising results have been obtained with the Cytosponge, a cell collection device composed of reticulated foam compressed within a gelatin capsule attached to a string. The capsule is swallowed by the patient and, after 5 min, allowing the dissolution of the gelatin and expansion of the foam, the sponge is retrieved by the operator. During the passage of the sponge cells are absorbed for immunohistochemical analysis Hellenic Society of Gastroenterology
2 2 D. Golger et al In a feasibility study the Cytosponge detected BE >1 cm with 73% and BE >2 cm with 90% sensitivity and a specificity of >90% [15]. The results of a large multicenter study (BEST2) will provide further information on the diagnostic accuracy. A simulation model, screening a hypothetical cohort of 50-year-old men with GERD symptoms, showed that Cytosponge screening followed by endotherapy reduces EAC mortality and is cost effective [16]. Accurate, minimal invasive and cost-effective screening tools may soon be available for clinicians. Up to now, the effectiveness of endoscopic screening is debatable and there are variable recommendations on it amongst different Medical Societies. Definition of BE: do we require goblet cells? In BE, as a consequence of GERD, the squamous epithelium that normally lines the distal esophagus is replaced by a metaplastic columnar epithelium. Endoscopically this is characterized by the typical salmon color and coarse texture. Histologically it is characterized by specialized intestinal metaplasia with goblet cells. It is a subject of controversy whether or not goblet cells are required as diagnostic criterion for BE. On the one hand, missing goblet cells in a biopsy specimen may represent a sampling error. On the other hand, there is evidence that esophageal cardiac epithelium, although lacking goblet cells, may also predispose to malignancy [17,18]. Two retrospective studies evaluated the risk of neoplasia in patients with columnar metaplasia of the esophagus either with or without goblet cells and found non-goblet cell columnar metaplasia to have the same malignant potential [19,20]. But the magnitude of this risk is unknown and so is the benefit of endoscopic surveillance. The British Society of Gastroenterology considers esophageal cardiac epithelium as a form of BE. The British guidelines point out that the distinction between columnar-lined esophagus and intestinal metaplasia at the gastric cardia can only be made definitively histologically when columnar mucosa is seen juxtaposed with native anatomical esophageal structures such as submucosal glands and/or gland ducts. But native structures are seen in only 10-15% of biopsy samples, which implies that in the great majority it is not possible to distinguish between intestinal metaplasia of the cardia and the esophagus. Biopsies of the normal cardia are not recommended routinely but if there is concern about the appearance at the site and after ablation therapy. The presence of intestinal metaplasia is considered as highly corroborative but not specific for a diagnosis of BE, as cardiac intestinal metaplasia cannot be ruled out. However, the guidelines recommend that this information should be recorded and that the diagnosis of BE should take into account the degree of confidence based on a combined analysis of endoscopic and histopathological criteria [21]. Other societies, including the AGA and the German Society of Gastroenterology, require esophageal biopsies showing intestinal metaplasia with goblet cells to establish the diagnosis [8,22]. After all, intestinal metaplasia is the only type of esophageal columnar epithelium that clearly predisposes to malignancy [8,22]. Diagnosis: can we drop the Seattle protocol with advanced endoscopic imaging? To evaluate patients with BE high resolution endoscopy is recommended in order to detect subtle abnormalities of early neoplasia [23]. Endoscopic evidence of BE should be recorded using the Prague criteria [circumferential (C) and maximum (M)] extent of endoscopically visible columnarlined esophagus in centimeters and any separate island above the main columnar-lined segment [24,25]). Current practice standards require the collection of targeted biopsies of every suspicious lesion followed by 4-quadrant biopsies specimens every 1 to 2 cm of BE (Seattle protocol). This approach is laborintensive, so there has been a great deal of research in imageenhanced technologies. Chromoendoscopy with contrast enhancing agents such as indigo carmine or acetic acid, virtual chromoendoscopy [Narrow band imaging (NBI, Olympus), Fuji Intelligent Chromo Endoscopy (FICE), and I-scan, Pentax] and confocal laser endomicroscopy, in addition to high-definition standard endoscopy, might increase the diagnostic yield for the detection of dysplastic lesions. Acetic acid showed a sensitivity of 96% for the diagnosis of high-grade intraepithelial neoplasia or cancer and a 15-fold increase in neoplasia detection compared to the standardized random biopsy protocol [26,27]. NBI, which highlights surface patterns and vessels, was found to have a sensitivity and specificity of 96% and 94% for the diagnosis of HGD in a meta-analysis [28]. In a recent trial, NBI-targeted biopsies showed the same detection rate as high-definition white light examination with the Seattle protocol while requiring fewer biopsies [29]. The Barrett s international NBI Group (BING) developed and validated a NBI classification system to identify dysplasia and EAC in BE. Based on the simple classification of mucosal and vascular patterns as regular (non-dysplastic) and irregular (dysplastic) the BING Criteria could classify BE with >90% accuracy and a high level of inter-observer agreement [30]. Overall, advanced imaging techniques increased the diagnostic yield for detection of dysplasia or cancer by 34% in a recent meta-analysis [31]. In fact they may be very helpful to detect and delineate lesions but their diagnostic power is dependent on the expertise of the individual endoscopist. However, they have not been found to be superior to the standard 4-quadrant random biopsy protocol. Hence, current evidence seems insufficient to change practice. Careful examination using high-resolution endoscopes combined with targeted and 4-quadrant biopsies remains the gold standard [23,24]. Management of BE Cancer in BE is thought to evolve through dysplasia. Dysplasia may be an imperfect marker to predict malignant progression as it can be patchy and therefore missed during routine biopsy sampling. Also, there may be significant interobserver disagreement about its grading [6]. However, dysplasia remains the basis for clinical decision making.
3 Barrett s esophagus management 3 Endoscopic therapy aims to treat dysplastic precursor tissue to reduce cancer risk. In expert hands, endoscopic therapy of BE-related dysplasia and early neoplasia has shown to be effective and safe. In inexperienced hands, it may be associated with significant complications [32]. Therefore, endoscopic treatment should only be performed in centers with expertise [23]. Before treatment, a lesion should be assessed by an experienced endoscopist, using at least a highresolution endoscope and one of the advanced endoscopic imaging modalities (NBI and/or chromoendoscopy) to determine whether the lesion is suitable for endoscopic treatment, to choose the appropriate resection technique [endoscopic mucosal resection (EMR) or endoscopic submucosal dissection (ESD)], delineate precise margins and to detect other possible lesions [33]. The management of neoplastic BE has changed considerably over the past decade. Today it consists of a multimodal approach combining tissue-acquiring and ablative techniques. Tissue acquiring techniques, which provide tissue specimens for histological examination, include EMR and ESD. Ablative techniques include radiofrequency ablation (RFA), argon plasma coagulation (APC), cryotherapy and photodynamic therapy (PDT). The common goal of ER, ablation or both is to completely eradicate all of the Barrett s metaplasia, dysplastic and non-dysplastic. This concept has shown high rates of disease reversal. A brief algorithm for the endoscopic management of BE is provided in Fig. 1; details are discussed below. High-grade dysplasia (HGD) and early cancer In BE with HGD or intramucosal cancer endoscopic therapy is well established [34]. In contrast to the low risk of malignant progression in patients with non-dysplastic BE, the risk with HGD is considered high enough to warrant intervention. In a meta-analysis, the annual rate of cancer progression with HGD was calculated approximately 6% per year, but in endoscopic intervention studies the risk was found to be considerably higher [35,36]. Also, in HGD a risk of occult adenocarcinoma has been reported as high as 40% [37]. The risk to harbor carcinoma is particularly high in high-grade intraepithelial neoplasia areas that are endoscopically visible. ER of a visible lesion is essential for proper diagnosis and staging. EMR of visible lumps diagnosed with HGD on previous biopsy led in 25-40% of cases to a histological upgrading to cancer [38,39]. Hence, visible lesions should undergo ER. After ER all residual Barrett s mucosa should be eradicated. This two-step concept can significantly reduce the risk of metachronous neoplasia. It remains the question what would be the best ablation technique. Well-studied alternatives are thermal ablation techniques as RFA and APC, PDT, and cryotherapy. Widespread EMR Figure 1 Management of Barrett s esophagus HGD, high-grade dysplasia; LGD, low-grade dysplasia; RFA, radiofrequency ablation
4 4 D. Golger et al can cause strictures, especially when more than two thirds of the circumference is removed. PDT plays no significant role any more due to its side effect of photosensitivity of the skin. Although there are no head to head comparative trials RFA seems to be superior and has become the preferred procedure for endoscopic ablation [40,41]. In a meta-analysis including more than 3800 patients RFA achieved complete eradication of dysplasia in 91% and complete eradication of intestinal metaplasia in 78% of patients. The most common adverse event was esophageal stricture, which was reported in 5% of patients [42]. Today the recommended standard of care in patients with HGD or intramucosal cancer is ER of visible lesions followed by RFA of residual Barrett s mucosa [22-43]. This combined approach has shown high rates of disease reversal [44]. However, recurrences have been reported after successful endoscopic therapy. Hence, endoscopic follow up is mandatory. The ESGE recommends regular endoscopic follow up after excision/ablation of BE-associated HGD or mucosal cancer, but more research is necessary to determine the appropriate interval. Empirically, endoscopic follow up is recommended 3-monthly for 1 year and yearly thereafter [33]. For patients with HGD in an endoscopically visible abnormality, ER is essential for proper diagnosis and staging [23] After EMR has removed visible lesions with HGD / T1m, the remaining BE segment should be eradicated regardless of whether or not it includes the presence or absence of dysplasia [23] RFA is currently the best available ablation technique for treatment of flat HGD and for eradication of residual BE mucosa after focal EMR [23] If adenocarcinoma is found in the EMR specimen the risk of lymph node metastasis has been shown to correlate with the depth of invasion. In patients with mucosal neoplasm lymph node metastases are present in less than 2% but in patients with tumor infiltration into the deep submucosa in more than 20% [45]. In contrast to surgery, endoscopic therapy does not have the potential to cure neoplasm that has metastasized to regional lymph nodes. Therefore, ER is considered curative for intramucosal carcinomas that are well or moderately differentiated (G1-G2) without lymphatic or vascular invasion (L0, V0) [33]. Endoscopic en bloc R0 resection of a sm1 (<500 μm) low risk tumor (G1-2, L0 and V0, size <3 cm) is considered potentially curative [33]. Manner et al reported for these lesions a low risk of lymph node metastasis (1.4%), but only few patients were included in that study [46]. So the risk of lymph node metastasis should be balanced against the risk of surgery for the individual patient in a multidisciplinary discussion [33]. Surgery is recommended in the presence of [33]: Lymph vascular invasion (L1,V1) Deeper infiltration of the submucosa than sm1 ( 500 μm) Poorly differentiated tumor Positive vertical margins (R1 vertical) If the horizontal margin is positive (R1 horizontal) or the tumor was resected piece meal and no other high-risk criteria are met, close endoscopic surveillance/treatment is recommended rather than surgery [33]. The standard for ER of Barrett s neoplasia in current clinical practice is EMR. But in lesions >15 mm EMR entails piece meal resection, associated with higher recurrence rates and hampers histopathological assessment of free margins [47]. ESD allows the en bloc resection of a lesion regardless of its size (Fig.2). With en bloc resection the histopathological evaluation is improved and an adequate assessment of R0-status and curative resection as defined to oncological standards is possible. The efficiency and safety of ESD with high success rates have been demonstrated by Asian studies [48-50]. But in Asian countries BE and adenocarcinoma are still rare. Therefore, available data on ESD in BE are scarce. Nevertheless, it has been shown that also in western countries ESD of Barrett s neoplasia is feasible with en bloc resection rates >95%, R0-resection rates >80%, and complication rates comparable to EMR [51-53]. In the presence of HGD or intramucosal cancer without visible lesions (flat HGD/intramucosal cancer) RFA is recommended [21-23,33]. Widespread EMR can cause strictures, especially when more than two thirds of the circumference is removed. RFA has been compared with stepwise ER for complete eradication of BE containing HGD/ mucosal cancer. Both methods showed equivalent efficacy but radical ER was associated with higher stricture rates and therapeutic sessions [54]. If HGD or intramucosal cancer are confirmed and there are no visible lesions after expert high resolution endoscopy review, then ablative therapy is the treatment of choice [21]. But to reemphasize it: RFA should only be used as a primary treatment modality in the case of flat HGD/intramucosal cancer. All visible lesions should be resected to provide adequate histological assessment, even if this demands circumferential EMR or ESD. Resulting strictures do respond well to dilatation and there exist strategies for stricture prevention, such as steroid administration. LGD The management of LGD is confounded by uncertainty of its natural history and difficulties in making the diagnosis. The diagnosis of LGD in BE is a subject of high interobserver variability among pathologists and can be challenging in the presence of inflammation. As demonstrated in a recent Dutch A Figure 2 (A) Early esophageal adenocarcinoma (narrow band imaging); (B) after endoscopic submucosal dissection B
5 Barrett s esophagus management 5 study, LGD in BE seems to be an over diagnosed and yet underestimated entity [6]. In this study 85% of patients who were initially diagnosed with LGD were down staged to either non-dysplastic or to indefinite for dysplasia (IND) after review by two expert GI pathologists. So it seems essential that the diagnosis is confirmed by at least two GI expert pathologists. The trial also showed that for patients with a consensus diagnosis of LGD, the cumulative risk of progression to HGD or carcinoma was alarming 85% in 109 months and the incidence rate for HGD or carcinoma 13.4% per patient per year. For down staged patients the corresponding incidence rate was 0.49%. Faced with this data gastroenterology societies propose that the diagnosis of dysplasia in BE should be confirmed by at least one additional pathologist, preferably one who is an expert in esophageal/gastrointestinal (GI) histopathology [21,22]. This recommendation takes in account the great medical importance of a true diagnosis of LGD but implicates challenges in its practical implementation (definition/qualification of an expert pathologist, independent evaluation, down-staging of diagnoses, financial aspects etc.). The finding of an endoscopically visible lesion in the setting of biopsy-detected LGD is of special importance as it may contain HGD or invasive cancer. Hence, visible lesions in confirmed LGD should be resected endoscopically to enable accurate histological assessment [55]. ER may result in a change of histological diagnosis, as shown in a multicenter study, where ER in patients diagnosed with LGD on biopsy led to upstaging in 33.3% and downstaging in 13.3% [56]. If HGD or mucosal cancer is detected ER should be followed by ablation [55]. We recommend that in the case of BE visible lesions in diagnosed LGD (or IND), ER should be followed by ablation if HGD or intramucosal cancer is detected, rather than continued surveillance [55] low risk does not weigh out potential therapy associated risks and does not justify therapeutic intervention. Visible lesions in non-dysplastic BE (as well as visible lesions in BE with LGD or IND) should undergo ER to enable accurate histological assessment [55]. We suggest against using ER in patients with nondysplastic BE and no visible lesion (harms outweigh benefits) [55] Endoscopic surveillance Endoscopic surveillance for BE is recommended by all Medical Societies. It is based on the assumption that the transition from BE to EAC progresses through LGD and HGD, thus justifying endoscopic surveillance for these premalignant stages. To date, the only evidence supporting this practice comes from observational studies reporting that patients whose Barrett s carcinoma was diagnosed during surveillance endoscopy have earlier stage tumor and better survival. The recommendations vary amongst different Medical Societies and further data on optimal intervals and protocols for biopsy collection is needed. Broadly speaking, in non-dysplastic BE surveillance endoscopy is recommended every 3-5 years. In the presence of LGD, confirmed by at least two expert GI pathologists, without visible lesions surveillance endoscopy every 6-12 months or eradication therapy is recommended [7]. Since recurrences of Barrett s metaplasia after apparently successful eradication are possible and recurrence rates up to 33% have been reported [59], patients should continue to undergo endoscopic surveillance even after therapy. Empirically, in patients treated for HGD, endoscopic follow up is recommended 3-monthly for 1 year and yearly thereafter. Ablation of BE with only LGD remains controversial because there is no clarity on cancer risk. As mentioned above, LGD generally seems to be overcalled but in those patients with LGD confirmed by at least two expert GI pathologists the risk of neoplastic progressions is considerably high. There are several studies that also indicate some clinical risk features such as multifocality of LGD and the length of BE-segment [57]. RFA can significantly reduce the risk of neoplastic progression to HGD/EAC. In the SURF trial it decreased the progression rate from 26.5% (control) to 1.5% (RFA) [58]. Non-dysplastic BE Noting the success of RFA in eradicating Barrett s metaplasia some physicians have proposed that RFA should be offered to all BE patients rather than to restrict it to patients with dysplasia. But patients with no dysplastic BE have a very low risk to develop HGD or EAC. Recent studies show that the risk may be as low as % per year [3]. This Practical impact BE is a combined endoscopic and pathological diagnosis The Seattle protocol (4-quadrant biopsies every 1 to 2 cm of BE and of every suspicious lesion) remains the standard; advanced imaging techniques may increase the diagnostic yield For any degree of dysplasia, at least two expert GI pathologists are required to confirm the diagnosis Visible lesions should be endoscopically resected to enable accurate histological assessment In HGD/mucosal cancer ER of visible lesions followed by field ablation of the whole Barrett s segment with RFA is now the standard of care In LGD (confirmed by at least two expert GI pathologists) with visible lesions ER should be performed. Without visible lesions surveillance endoscopy every 6-12 months or eradication therapy is recommended In non-dysplastic BE the risk of progression is low. Surveillance endoscopies are recommended every 3-5 years Recurrences after apparently successful eradication of
6 6 D. Golger et al Barrett s metaplasia are possible. Further endoscopic surveillance is indispensable. References 1. Hur C, Miller M, Kong CY, et al. Trends in esophageal adenocarcinoma incidence and mortality. Cancer 2013;119: Verbeek RE, Leenders M, Ten Kate FJ, et al. Surveillance of Barrett s esophagus and mortality from esophageal adenocarcinoma: a population-based cohort study. Am J Gastroenterol 2014;109: Hvid-Jensen F, Pedersen L, Drewes AM, Sørensen HT, Funch- Jensen P. Incidence of adenocarcinoma among patients with Barrett s esophagus. N Engl J Med 2011;365: Desai TK, Krishnan K, Samala N, et al. The incidence of oesophageal adenocarcinoma in non-dysplastic Barrett s oesophagus: a metaanalysis. Gut 2012;61: Bhat S, Coleman HG, Yousef F, et al. Risk of malignant progression in Barrett s esophagus patients: results from a large populationbased study. JNCI J Natl Cancer Inst 2011;103: Curvers WL, ten Kate FJ, Krishnadath KK, et al. Low-grade dysplasia in Barrett s esophagus: overdiagnosed and underestimated. Am J Gastroenterol 2010;105: Spechler SJ, Souza RF. Barrett s esophagus. N Engl J Med 2014;371: Spechler SJ, Sharma P, Souza RF, et al. American Gastroenterological Association medical position statement on the management of Barrett s esophagus. Gastroenterology 2011;140: Rex DK, Cummings OW, Shaw M, et al. Screening for Barrett s esophagus in colonoscopy patients with and without heartburn. Gastroenterology 2003;125: Chak A, Faulx A, Eng C, et al. Gastroesophageal reflux symptoms in patients with adenocarcinoma of the esophagus or cardia. Cancer 2006;107: Gaddam S, Singh M, Balasubramanian G, et al. Persistence of nondysplastic Barrett s esophagus identifies patients at lower risk for esophageal adenocarcinoma: Results from a large multicenter cohort. Gastroenterology 2013;145: Di Pietro M, Alzoubaidi D, Fitzgerald RC. Barrett s esophagus and cancer risk: how research advances can impact clinical practice. Gut Liver 2014;8: Gregson EM, Fitzgerald RC. Biomarkers for dysplastic Barrett s: ready for prime time? World J Surg 2015;39: Di Pietro M, Chan D, Fitzgerald R, Wang K. Screening for Barrett s esophagus. Gastroenterology 2015;148: Kadri SR, Lao-Sirieix P, Donovan M, et al. Acceptability and accuracy of a non-endoscopic screening test for Barrett s oesophagus in primary care: cohort study. BMJ 2010;341:c Benaglia T, Sharples LD, Fitzgerald RC, Lyratzopoulos G. Health benefits and cost effectiveness of endoscopic and nonendoscopic cytosponge screening for Barrett s esophagus. Gastroenterology 2013;144: Takubo K, Aida J, Naomoto Y, et al. Cardiac rather than intestinaltype background in endoscopic resection specimens of minute Barrett adenocarcinoma. Hum Pathol 2009;40: Liu W, Hahn H, Odze RD, Goyal RK. Metaplastic esophageal columnar epithelium without goblet cells shows DNA content abnormalities similar to goblet cell containing epithelium. Am J Gastroenterol 2009;104: Gatenby PAC, Ramus JR, Caygill CPJ, Shepherd NA, Watson A. Relevance of the detection of intestinal metaplasia in non-dysplastic columnar-lined oesophagus. Scand J Gastroenterol 2008;43: Kelty CJ, Gough MD, Van Wyk Q, Stephenson TJ, Ackroyd R. Barrett s oesophagus: intestinal metaplasia is not essential for cancer risk. Scand J Gastroenterol 2007;42: Fitzgerald RC, di Pietro M, Ragunath K, et al. British Society of Gastroenterology guidelines on the diagnosis and management of Barrett s oesophagus. Gut 2014;63: Koop H, Fuchs KH, Labenz J, et al. S2k Guideline: Gastroesophageal reflux disease guided by the German Society of Gastroenterology. Z Gastroenterol 2014;52: Bennett C, Vakil N, Bergman J, et al. Consensus statements for management of Barrett s dysplasia and early-stage esophageal adenocarcinoma, based on a Delphi process. Gastroenterology 2012;143: Sharma P, Katzka DA, Gupta N. Quality indicators for the management of Barrett s esophagus, dysplasia, and esophageal adenocarcinoma: international consensus recommendations from the American Gastroenterological Association Symposium. Gastroenterology 2015;149: Sharma P, Dent J, Armstrong D, et al. The development and validation of an endoscopic grading system for Barrett s esophagus: the Prague C & M criteria. Gastroenterology 2006;131: Longcroft-Wheaton G, Duku M, Mead R, Poller D, Bhandari P. Acetic acid spray is an effective tool for the endoscopic detection of neoplasia in patients with Barrett s esophagus. Clin Gastroenterol Hepatol 2010;8: Tholoor S, Bhattacharyya R, Tsagkournis O, Longcroft-Wheaton G, Bhandari P. Acetic acid chromoendoscopy in Barrett s esophagus surveillance is superior to the standardized random biopsy protocol: results from a large cohort study (with video). Gastrointest Endosc 2014;80: Mannath J, Subramanian V, Hawkey CJ, Ragunath K. Narrow band imaging for characterization of high grade dysplasia and specialized intestinal metaplasia in Barrett s esophagus: a metaanalysis. Endoscopy 2010;42: Sharma P, Hawes RH, Bansal A, et al. Standard endoscopy with random biopsies versus narrow band imaging targeted biopsies in Barrett s oesophagus: a prospective, international, randomised controlled trial. Gut 2013;62: Sharma P, Bergman J, Goda K, et al. Development and validation of a classification system to identify gigh-grade dysplasia and esophageal adenocarcinoma in Barrett s esophagus using narrowband imaging. Gastroenterology 2016;150: Qumseya BJ, Wang H, Badie N, et al. Advanced imaging technologies increase detection of dysplasia and neoplasia in patients with Barrett s esophagus: a meta-analysis and systematic review. Clin Gastroenterol Hepatol 2013;11: Van Vilsteren FGI, Pouw RE, Herrero LA, et al. Learning to perform endoscopic resection of esophageal neoplasia is associated with significant complications even within a structured training program. Endoscopy 2012;44: Pimentel-Nunes, et al. Endoscopic submucosa dissection: European Society of Gastrointestinal Endoscopy (ESGE) Guideline. Endoscopy 2015;47: Pech O, May A, Manner H, et al. Long-term efficacy and safety of endoscopic resection for patients with mucosal adenocarcinoma of the esophagus. Gastroenterology 2014;146: Rastogi A, Puli S, El-Serag HB, Bansal A, Wani S, Sharma P. Incidence of esophageal adenocarcinoma in patients with Barrett s esophagus and high-grade dysplasia: a meta-analysis. Gastrointest Endosc 2008;67: Shaheen NJ, Sharma P, Overholt BF, et al. Radiofrequency ablation in Barrett s esophagus with dysplasia. N Engl J Med 2009;360: Wright TA. High-grade dysplasia in Barrett s oesophagus. Br J Surg 1997;84:
7 Barrett s esophagus management Peters FP, Brakenhoff KP, Curvers WL, et al. Histologic evaluation of resection specimens obtained at 293 endoscopic resections in Barrett s esophagus. Gastrointest Endosc 2008;67: Pech O, Gossner L, Manner H. Prospective evaluation of the macroscopic types and location of early Barrett s neoplasia in 380 lesions. Endoscopy 2007;39: Blevins CH, Iyer PG. Endoscopic therapy for Barrett s oesophagus. Best Pract Res Clin Gastroenterol 2015;29: Haidry R, Lovat L, Sharma P. Radiofrequency ablation for Barrett s dysplasia: past, present and the future? Curr Gastroenterol Rep 2015;17: Orman ES, Li N, Shaheen NJ. Efficacy and durability of radiofrequency ablation for Barrett s esophagus: systematic review and meta-analysis. Clin Gastroenterol Hepatol 2013;11: Porschen R, Buck A, Fischbach W, et al. S3-Leitlinie diagnostik und therapie der plattenepithelkarzinome und adenokarzinome des Ösophagus. Z Gastroenterol 2015;53: (S3-Guideline on diagnosis and therapy of esophageal cancer, German Society of Gastroenterology). 44. Phoa KN, Pouw RE, Bisschops R, et al. Multimodality endoscopic eradication for neoplastic Barrett oesophagus: results of an European multicentre study (EURO-II). Gut 2016;65: Dunbar KB, Spechler SJ. The risk of lymph-node metastases in patients with high-grade dysplasia or intramucosal carcinoma in Barrett s esophagus: a systematic review. Am J Gastroenterol 2012;107: Manner H, May A, Pech O, et al. Early Barrett s carcinoma with low risk submucosal invasion: long term results of endoscopic resection with a curative intent. Am J Gastroenterol 2008;103: Pech O, Behrens A, May A. Long-term results and risk factor analysis for recurrence after curative endoscopic therapy in 349 patients with high-grade intraepithelial neoplasia and mucosal adenocarcinoma in Barrett s oesophagus. Gut 2008;57: Kakushima N, Yahagi N, Fujishiro M. Efficacy and safety of endoscopic submucosal dissection for tumors of the esophagogastric junction. Endoscopy 2006;38: Hoteya S, Matsui A, Iizuka T. Comparison of the clinicopathological characteristics and results of endoscopic submucosal dissection for esophagogastric junction and non-junctional cancers. Digestion 2013;87: Hirasawa K, Kokawa A, Oka H. Superficial adenocarcinoma of the esophagogastric junction: long-term results of endoscopic submucosal dissection. Gastrointest Endosc 2010;72: Probst A, Aust D, Märkl B, Anthuber M, Messmann H. Early esophageal cancer in Europe: endoscopic treatment by endoscopic submucosal dissection. Endoscopy 2015;47: Chevaux JB, Piessevaux H, Jouret-Mourin A, et al. Clinical outcome in patients treated with endoscopic submucosal dissection for superficial Barrett s neoplasia. Endoscopy 2015;47: Höbel S, Dautel P, Baumbach R, et al. Single center experience of endoscopic submucosal dissection (ESD) in early Barrett s adenocarcinoma. Surg Endosc 2015;29: van Vilsteren FG, Pouw RE, Seewald S, et al. Stepwise radical endoscopic resection versus radiofrequency ablation for Barrett`s oesophagus with high-grade dysplasia or early cancer: a multicentre randomized trial. Gut 2011;60: Bennett C, Moayyedi P, Corley DA, et al. BOB CAT: A largescale review and Delphi Consensus for management of Barrett s esophagus with no dysplasia, indefinite for, or low-grade dysplasia. Am J Gastroenterol 2015;110: Wani S, Abrams J, Edmundowicz SA, et al. Endoscopic mucosal resection results in change of histologic diagnosis in Barrett s esophagus patients with visible and flat neoplasia: a multicenter cohort study. Dig Dis Sci 2013;58: Thota PN, Lee HJ, Goldblum JR, et al. Risk stratification of patients with barrett s esophagus and low-grade dysplasia or indefinite for dysplasia. Clin Gastroenterol Hepatol 2015;13: Phoa KN, van Vilsteren FG, Weusten BL, et al. Radiofrequency ablation vs endoscopic surveillance for patients with Barrett esophagus and low-grade dysplasia: a randomized clinical trial. JAMA 2014;311: Gupta M, Iyer PG, Lutzke L, et al. Recurrence of esophageal intestinal metaplasia after endoscopic mucosal resection and radiofrequency ablation of Barrett s esophagus: eesults from a US multicenter consortium. Gastroenterology 2013;145:79-86.
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic management of Barrett s esophagus with dysplasia
 UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Current Management of Low-Grade Dysplasia in Barrett Esophagus
 Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
Current Management of Low-Grade Dysplasia in Barrett Esophagus Gary W. Falk, MD, MS Dr Falk is a professor of medicine in the Division of Gastroenterology at the University of Pennsylvania Perelman School
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
Ablation for Barrett s Esophagus: Burn or Freeze
 Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Barrett s Esophagus: Ablate Everyone?
 Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Editorial: Advanced endoscopic therapeutics in Barrett s neoplasia; where are we now and where are we heading?
 Editorial: Advanced endoscopic therapeutics in Barrett s neoplasia; where are we now and where are we heading? Dr. Gaius Longcroft-Wheaton MB,BS, MD, MRCP(UK), MRCP(Gastro) Consultant gastroenterologist
Editorial: Advanced endoscopic therapeutics in Barrett s neoplasia; where are we now and where are we heading? Dr. Gaius Longcroft-Wheaton MB,BS, MD, MRCP(UK), MRCP(Gastro) Consultant gastroenterologist
Management of Barrett s: From Imaging to Resection
 Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018
 MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
Current Management: Role of Radiofrequency Ablation
 Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
Present Day Management of Barrett s Esophagus
 Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Learning Objectives:
 Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Barrett's Esophagus: Sorting Out the Controversy
 Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
AGA SECTION. Gastroenterology 2016;150:
 Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Management of Barrett s Esophagus. Case Presentation
 Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
In 1998, the American College of Gastroenterology issued ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
Barrett s esophagus. Barrett s neoplasia treatment trends
 Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus
 ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
Endoscopic Management of Barrett s Esophagus
 Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
How to remove BE cancer: EMR or ESD? Expected outcome
 How to remove BE cancer: EMR or ESD? Expected outcome Presented by Horst Neuhaus Institution Dpt. of Gastroenterology Evangelisches Krankenhaus Düsseldorf, Germany Indications for endoscopic resection
How to remove BE cancer: EMR or ESD? Expected outcome Presented by Horst Neuhaus Institution Dpt. of Gastroenterology Evangelisches Krankenhaus Düsseldorf, Germany Indications for endoscopic resection
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD?
 Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Barrett esophagus. Bible class Inselspital
 Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Targeting care in Barrett s oesophagus
 HEPATO-GASTROENTEROLOGY Clinical Medicine 2014 Vol 14, No 6: s78 s83 Targeting care in Barrett s oesophagus Authors: Sebastian Zeki A and Rebecca C Fitzgerald B ABSTRACT Barretts oesophagus represents
HEPATO-GASTROENTEROLOGY Clinical Medicine 2014 Vol 14, No 6: s78 s83 Targeting care in Barrett s oesophagus Authors: Sebastian Zeki A and Rebecca C Fitzgerald B ABSTRACT Barretts oesophagus represents
Definition of GERD American College of Gastroenterology
 Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
Changes to the diagnosis and management of Barrett s Oesophagus
 Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
Endoscopic management of Barrett s esophagus:european Society of Gastrointestinal Endoscopy (ESGE) Position Statement
 Endoscopic management of Barrett s esophagus:european Society of Gastrointestinal Endoscopy (ESGE) Position Statement Authors Bas Weusten 1, 2,RafBisschops 3,EmanuelCoron 4,MárioDinis- Ribeiro 5,Jean-MarcDumonceau
Endoscopic management of Barrett s esophagus:european Society of Gastrointestinal Endoscopy (ESGE) Position Statement Authors Bas Weusten 1, 2,RafBisschops 3,EmanuelCoron 4,MárioDinis- Ribeiro 5,Jean-MarcDumonceau
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery
 Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Populations Interventions Comparators Outcomes Individuals: With Barrett esophagus with high-grade dysplasia
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett (20180) Medical Benefit Effective Date: 01/01/16 Next Review Date: 09/19 Preauthorization No Review Dates: 05/09, 03/10, 03/11, 03/12, 07/12,
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett (20180) Medical Benefit Effective Date: 01/01/16 Next Review Date: 09/19 Preauthorization No Review Dates: 05/09, 03/10, 03/11, 03/12, 07/12,
Is Radiofrequency Ablation Effective In Treating Barrett s Esophagus Patients with High-Grade Dysplasia?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Section: Medicine Effective Date: July 15, 2015 Subsection: Original Policy Date: December 7, 2011 Subject:
 Last Review Status/Date: June 2015 Page: 1 of 16 Cryoablation for Barrett s Esophagus Description Barrett s esophagus (BE) is a condition in which the normal squamous epithelium is replaced by specialized
Last Review Status/Date: June 2015 Page: 1 of 16 Cryoablation for Barrett s Esophagus Description Barrett s esophagus (BE) is a condition in which the normal squamous epithelium is replaced by specialized
Sixteen-year follow-up of Barrett s esophagus, endoscopically treated with argon plasma coagulation
 Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
Medicare Advantage Medical Policy
 Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Description/Background Barrett Esophagus and the
Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Description/Background Barrett Esophagus and the
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell
 Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
Opinion Statement. Esophagus (E Dellon, Section Editor)
 Curr Treat Options Gastro (2016) 14:1 18 DOI 10.1007/s11938-016-0080-4 Esophagus (E Dellon, Section Editor) Current Controversies in Radiofrequency Ablation Therapy for Barrett s Esophagus Kamar Belghazi,
Curr Treat Options Gastro (2016) 14:1 18 DOI 10.1007/s11938-016-0080-4 Esophagus (E Dellon, Section Editor) Current Controversies in Radiofrequency Ablation Therapy for Barrett s Esophagus Kamar Belghazi,
American Journal of Gastroenterology. Volumetric Laser Endomicroscopy Detects Subsquamous Barrett s Adenocarcinoma
 Volumetric Laser Endomicroscopy Detects Subsquamous Barrett s Adenocarcinoma Journal: Manuscript ID: AJG-13-1412.R1 Manuscript Type: Letter to the Editor Keywords: Barrett-s esophagus, Esophagus, Endoscopy
Volumetric Laser Endomicroscopy Detects Subsquamous Barrett s Adenocarcinoma Journal: Manuscript ID: AJG-13-1412.R1 Manuscript Type: Letter to the Editor Keywords: Barrett-s esophagus, Esophagus, Endoscopy
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Policy Number: Original Effective Date: MM.02.005 09/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Policy Number: Original Effective Date: MM.02.005 09/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus. Original Policy Date
 MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia
 Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Chromoendoscopy and Endomicroscopy for detecting colonic dysplasia Ralf Kiesslich I. Medical Department Johannes Gutenberg University Mainz, Germany Cumulative cancer risk in ulcerative colitis 0.5-1.0%
Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment Barrett s esophagus
 E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
This medical position statement considers a series of
 GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
GASTROENTEROLOGY 2011;140:1084 1091 American Gastroenterological Association Medical Position Statement on the Management of Barrett s Esophagus The Institute Medical Position Panel consisted of the authors
Barrett s Esophagus. Radiofrequency Ablation with the HALO Technology A Reference Book
 Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
How to characterize dysplastic lesions in IBD?
 How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
How to characterize dysplastic lesions in IBD? Name: Institution: Helmut Neumann, MD, PhD, FASGE University Medical Center Mainz What do we know? Patients with IBD carry an increased risk of developing
Oesophagus and Stomach update dysplasia and early cancer
 Oesophagus and Stomach update dysplasia and early cancer Dr Tim Bracey STR teaching 13/4/16 Please check pathkids.com for previous talks One of the biggest units in the country (100 major resections per
Oesophagus and Stomach update dysplasia and early cancer Dr Tim Bracey STR teaching 13/4/16 Please check pathkids.com for previous talks One of the biggest units in the country (100 major resections per
Gregory G. Ginsberg, M.D.
 Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Cryospray ablation using pressurized CO 2 for ablation of Barrett s esophagus with early neoplasia: early termination of a prospective series
 E17 Cryospray ablation using pressurized CO 2 for ablation of Barrett s esophagus with early neoplasia: early termination of a prospective series Authors Romy E. Verbeek 1, Frank P. Vleggaar 1, Fiebo J.
E17 Cryospray ablation using pressurized CO 2 for ablation of Barrett s esophagus with early neoplasia: early termination of a prospective series Authors Romy E. Verbeek 1, Frank P. Vleggaar 1, Fiebo J.
History. Prevalence at Endoscopy. Prevalence and Reflux Sx. Prevalence at Endoscopy. Barrett s Esophagus: Controversy and Management
 Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Everything Esophagus: Barrett s Esophagus. Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina
 Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
DISCLOSURES. This program meets the requirements for GI specific Category 1 contact hours. M
 DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
Recurrent intestinal metaplasia at the gastroesophageal junction following endoscopic eradication of dysplastic Barrett s esophagus may not be benign
 THIEME E849 Recurrent intestinal metaplasia at the gastroesophageal junction following endoscopic eradication of dysplastic Barrett s esophagus may not be benign Authors Georgina R. Cameron 1, 3, Paul
THIEME E849 Recurrent intestinal metaplasia at the gastroesophageal junction following endoscopic eradication of dysplastic Barrett s esophagus may not be benign Authors Georgina R. Cameron 1, 3, Paul
Faculty Disclosure. Objectives. State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) 24/11/2014
 State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
RFA and Cyrotherapy for Esophageal Disease
 RFA and Cyrotherapy for Esophageal Disease Daniel L. Miller MD Chief, General Thoracic Surgery WellStar Healthcare System/ Mayo Clinic Care Network Clinical Professor of Surgery Medical College of Georgia/
RFA and Cyrotherapy for Esophageal Disease Daniel L. Miller MD Chief, General Thoracic Surgery WellStar Healthcare System/ Mayo Clinic Care Network Clinical Professor of Surgery Medical College of Georgia/
Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia
 ...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
Treatment of High-Grade Dysplasia and Early Stage Esophageal Adenocarcinoma with an Endoscope: The Ultimate in Minimally Invasive, Curative Therapy
 Curr Surg Rep (2014) 2:66 DOI 10.1007/s40137-014-0066-x ESOPHAGEAL/REFLUX SURGERY (SR DEMEESTER, SECTION EDITOR) Treatment of High-Grade Dysplasia and Early Stage Esophageal Adenocarcinoma with an Endoscope:
Curr Surg Rep (2014) 2:66 DOI 10.1007/s40137-014-0066-x ESOPHAGEAL/REFLUX SURGERY (SR DEMEESTER, SECTION EDITOR) Treatment of High-Grade Dysplasia and Early Stage Esophageal Adenocarcinoma with an Endoscope:
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ
 Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France
 Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of the distal esophagus, gastroesophageal junction and gastric cardia?
 Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
malignant polyp Daily Challenges in Digestive Endoscopy for Endoscopists and Endoscopy Nurses BSGIE Annual Meeting 18/09/2014 Mechelen
 Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Chapter 2 Complications of Gastroesophageal Reflux Disease
 Chapter 2 Complications of Gastroesophageal Reflux Disease Patrick Yachimski Acute esophageal exposure to gastric and/or duodenal refluxate can result in pyrosis and symptomatic gastroesophageal reflux
Chapter 2 Complications of Gastroesophageal Reflux Disease Patrick Yachimski Acute esophageal exposure to gastric and/or duodenal refluxate can result in pyrosis and symptomatic gastroesophageal reflux
Slide 1. Slide 2. Slide 3 DISCLOSURES EXPECTED OUTCOMES DIAGNOSIS AND TREATMENT
 Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic management of Barrett s esophagus with dysplasia
 UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Endoscopic submucosal dissection: European Society of Gastrointestinal Endoscopy (ESGE) Guideline
 Guideline 829 Endoscopic submucosal dissection: European Society of Gastrointestinal Endoscopy (ESGE) Guideline Authors Institutions Bibliography DOI http://dx.doi.org/ 10.1055/s-0034-1392882 Endoscopy
Guideline 829 Endoscopic submucosal dissection: European Society of Gastrointestinal Endoscopy (ESGE) Guideline Authors Institutions Bibliography DOI http://dx.doi.org/ 10.1055/s-0034-1392882 Endoscopy
The incidence of esophageal adenocarcinoma is rising in the ENDOSCOPY CORNER
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:843 847 ENDOSCOPY CORNER Acetic Acid Spray Is an Effective Tool for the Endoscopic Detection of Neoplasia in Patients With Barrett s Esophagus GAIUS LONGCROFT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:843 847 ENDOSCOPY CORNER Acetic Acid Spray Is an Effective Tool for the Endoscopic Detection of Neoplasia in Patients With Barrett s Esophagus GAIUS LONGCROFT
Dysplas'c Barre- s Esophagus: Cut, Burn, Freeze or Watch Very Very Closely
 Dysplas'c Barre- s Esophagus: Cut, Burn, Freeze or Watch Very Very Closely Felice Schnoll- Sussman, MD, FACG Director, Jay Monahan Center Associate Professor Clinical Medicine Weill Cornell Medical Center
Dysplas'c Barre- s Esophagus: Cut, Burn, Freeze or Watch Very Very Closely Felice Schnoll- Sussman, MD, FACG Director, Jay Monahan Center Associate Professor Clinical Medicine Weill Cornell Medical Center
EMR, ESD and Beyond. Peter Draganov MD. Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida
 EMR, ESD and Beyond Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated by Endoscopy
EMR, ESD and Beyond Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated by Endoscopy
Gastrointestinal Imaging
 Endoscopic Imaging of Gastroesophageal Reflux Disease Kerry B Dunbar, MD Assistant Professor of Medicine, Division of Gastroenterology and Hepatology, Johns Hopkins University School of Medicine Abstract
Endoscopic Imaging of Gastroesophageal Reflux Disease Kerry B Dunbar, MD Assistant Professor of Medicine, Division of Gastroenterology and Hepatology, Johns Hopkins University School of Medicine Abstract
Disclosures. Gastroesophageal Reflux Disease. Gastroesophageal Reflux Disease
 Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Endoscopic Submucosal Dissection ESD
 Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Endoscopic Submucosal Dissection ESD Peter Draganov MD Professor of Medicine Division of Gastroenterology, Hepatology and Nutrition University of Florida Gastrointestinal Cancer Lesion that Can be Treated
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions
 Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
University Mainz. Early Gastric Cancer. Ralf Kiesslich. Johannes Gutenberg University Mainz, Germany. Early Gastric Cancer 15.6.
 Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
Ralf Kiesslich Johannes Gutenberg University Mainz, Germany DIAGNOSIS Unmask lesions - Chromoendoscopy -NBI Red flag technology - Autofluorescence Surface and detail analysis - Magnifying endoscopy - High
What s New in the Management of Esophageal Disease
 What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin
 The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin 24.06.15 Norman Barrett Smiles [A brief digression - Chair becoming
The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin 24.06.15 Norman Barrett Smiles [A brief digression - Chair becoming
Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection
 Editor s choice Scan to access more free content For numbered affiliations see end of article. Correspondence to Professor Thomas Rösch, Department of Interdisciplinary Endoscopy, University Hospital Hamburg-Eppendorf,
Editor s choice Scan to access more free content For numbered affiliations see end of article. Correspondence to Professor Thomas Rösch, Department of Interdisciplinary Endoscopy, University Hospital Hamburg-Eppendorf,
Accepted Manuscript. CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D
 Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
ESOPHAGEAL CANCER. Epidemiology 3/22/2017. Esophageal Carcinoma: subtypes. Esophageal Adenocarcinoma (EAC) Epidemiology.
 ESOPHAGEAL CANCER Disclosures Sushil Ahlawat, MD, FACP, FASGE, AGAF Associate Professor of Medicine Director of Endoscopy RUTGERS NJMS Nothing to disclose. Esophageal Carcinoma: subtypes Subtype Squamous
ESOPHAGEAL CANCER Disclosures Sushil Ahlawat, MD, FACP, FASGE, AGAF Associate Professor of Medicine Director of Endoscopy RUTGERS NJMS Nothing to disclose. Esophageal Carcinoma: subtypes Subtype Squamous
evidence note Radiofrequency ablation for Barrett s oesophagus with highgrade What is an evidence note Key points Literature search Introduction
 In response to an enquiry from the National Cancer Waiting Times Delivery Group What is an evidence note Evidence notes are rapid reviews of published secondary clinical and cost-effectiveness evidence
In response to an enquiry from the National Cancer Waiting Times Delivery Group What is an evidence note Evidence notes are rapid reviews of published secondary clinical and cost-effectiveness evidence
Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection
 Editor s choice Scan to access more free content ORIGINAL ARTICLE Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection Mario Anders, 1 Christina Bähr, 1 Muhammad
Editor s choice Scan to access more free content ORIGINAL ARTICLE Long-term recurrence of neoplasia and Barrett s epithelium after complete endoscopic resection Mario Anders, 1 Christina Bähr, 1 Muhammad
Barrett s esophagus (BE) is a precancerous state
 CLINICAL ALIMENTARY TRACT Gastroenterology 2017;153:681 688 Late Recurrence of Barrett s Esophagus After Complete Eradication of Intestinal Metaplasia is Rare: Final Report From Ablation in Intestinal
CLINICAL ALIMENTARY TRACT Gastroenterology 2017;153:681 688 Late Recurrence of Barrett s Esophagus After Complete Eradication of Intestinal Metaplasia is Rare: Final Report From Ablation in Intestinal
How to treat early gastric cancer? Endoscopy
 How to treat early gastric cancer? Endoscopy Presented by Pierre H. Deprez Institution Cliniques universitaires Saint-Luc, Brussels Université catholique de Louvain 2 3 4 5 6 Background Diagnostic or therapeutic
How to treat early gastric cancer? Endoscopy Presented by Pierre H. Deprez Institution Cliniques universitaires Saint-Luc, Brussels Université catholique de Louvain 2 3 4 5 6 Background Diagnostic or therapeutic
Novel endoscopic observation in Barrett s oesophagus using high resolution magnification endoscopy and narrow band imaging
 Alimentary Pharmacology & Therapeutics Novel endoscopic observation in Barrett s oesophagus using high resolution magnification endoscopy and narrow band imaging G. K. ANAGNOSTOPOULOS*, K. YAO*, P. KAYE,
Alimentary Pharmacology & Therapeutics Novel endoscopic observation in Barrett s oesophagus using high resolution magnification endoscopy and narrow band imaging G. K. ANAGNOSTOPOULOS*, K. YAO*, P. KAYE,
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus
 Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
Review Article Outcomes of Radiofrequency Ablation for Dysplastic Barrett s Esophagus: A Comprehensive Review
 Gastroenterology Research and Practice Volume 2016, Article ID 4249510, 8 pages http://dx.doi.org/10.1155/2016/4249510 Review Article Outcomes of Radiofrequency Ablation for Dysplastic Barrett s Esophagus:
Gastroenterology Research and Practice Volume 2016, Article ID 4249510, 8 pages http://dx.doi.org/10.1155/2016/4249510 Review Article Outcomes of Radiofrequency Ablation for Dysplastic Barrett s Esophagus:
Efficacy of Radiofrequency Ablation Combined With Endoscopic Resection for Barrett s Esophagus With Early Neoplasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:23 29 ENDOSCOPY CORNER Efficacy of Radiofrequency Ablation Combined With Endoscopic Resection for Barrett s Esophagus With Early Neoplasia ROOS E. POUW,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:23 29 ENDOSCOPY CORNER Efficacy of Radiofrequency Ablation Combined With Endoscopic Resection for Barrett s Esophagus With Early Neoplasia ROOS E. POUW,*
It has been estimated that 5.6% of adults in the United States have
 The new england journal of medicine review article Dan L. Longo, M.D., Editor Barrett s Esophagus Stuart J. Spechler, M.D., and Rhonda F. Souza, M.D. From the Esophageal Diseases Center, Department of
The new england journal of medicine review article Dan L. Longo, M.D., Editor Barrett s Esophagus Stuart J. Spechler, M.D., and Rhonda F. Souza, M.D. From the Esophageal Diseases Center, Department of
Screening Patients for Barrett s Esophagus with Cytosponge Coupled with Trefoil Factor 3 Expression Compared to Endoscopy
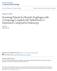 Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Summer 8-13-2016 Screening Patients for Barrett s Esophagus with Cytosponge Coupled
Pacific University CommonKnowledge School of Physician Assistant Studies Theses, Dissertations and Capstone Projects Summer 8-13-2016 Screening Patients for Barrett s Esophagus with Cytosponge Coupled
Advances in the Endoscopic Diagnosis of Barrett Esophagus
 Special Report Advances in the Endoscopic Diagnosis of Barrett Esophagus Ashley H. Davis-Yadley, MD, Kevin G. Neill, MD, Mokenge P. Malafa, MD, and Luis R. Peña, MD Background: Barrett esophagus (BE) continues
Special Report Advances in the Endoscopic Diagnosis of Barrett Esophagus Ashley H. Davis-Yadley, MD, Kevin G. Neill, MD, Mokenge P. Malafa, MD, and Luis R. Peña, MD Background: Barrett esophagus (BE) continues
RADIOFREQUENCY ABLATION OR CRYOABLATION FOR ESOPHAGEAL DISORDERS
 DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong
 Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Application of Chromoendoscopy, NBI and AFI in Esophagus why, who, and how? Philip Chiu Associate Professor Department of Surgery, Prince of Wales Hospital The Chinese University of Hong Kong Cancer of
Burning Issues in the Esophagus
 Burning Issues in the Esophagus Elizabeth Montgomery, MD Johns Hopkins Medical Institutions Dr. Montgomery reports no relevant financial relationships with commercial interests. Squamous Epithelium Muscularis
Burning Issues in the Esophagus Elizabeth Montgomery, MD Johns Hopkins Medical Institutions Dr. Montgomery reports no relevant financial relationships with commercial interests. Squamous Epithelium Muscularis
Barrett s esophagus, reflux esophagitis, and eosinophilic esophagitis F. P. Vleggaar, P. D. Siersema Utrecht, the Netherlands
 DDW HIGHLIGHTS F. P. Vleggaar, P. D. Siersema Utrecht, the Netherlands Many new and exciting endoscopy-related studies on Barrett s esophagus, reflux esophagitis, and eosinophilic esophagitis were presented
DDW HIGHLIGHTS F. P. Vleggaar, P. D. Siersema Utrecht, the Netherlands Many new and exciting endoscopy-related studies on Barrett s esophagus, reflux esophagitis, and eosinophilic esophagitis were presented
EMR is not inferior to ESD for early Barrett s and EGJ neoplasia: An extensive review on outcome, recurrence and complication rates
 E58 EMR is not inferior to ESD for early Barrett s and EGJ neoplasia: An extensive review on outcome, recurrence and complication rates Authors Institution Yoriaki Komeda, Marco Bruno, Arjun Koch Department
E58 EMR is not inferior to ESD for early Barrett s and EGJ neoplasia: An extensive review on outcome, recurrence and complication rates Authors Institution Yoriaki Komeda, Marco Bruno, Arjun Koch Department
Advances in endoscopic resection and radiofrequency ablation of early esophageal neoplasia van Vilsteren, F.G.I.
 UvA-DARE (Digital Academic Repository) Advances in endoscopic resection and radiofrequency ablation of early esophageal neoplasia van Vilsteren, F.G.I. Link to publication Citation for published version
UvA-DARE (Digital Academic Repository) Advances in endoscopic resection and radiofrequency ablation of early esophageal neoplasia van Vilsteren, F.G.I. Link to publication Citation for published version
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
Relative risk of dysplasia for patients with intestinal metaplasia in the distal oesophagus and in the gastric cardia
 Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation. See specific types, e.g., Thermal ablation Achalasia, 53 75 described, 53 features of, 53 management of past options, 54 POEM
Index Note: Page numbers of article titles are in boldface type. A Ablation. See specific types, e.g., Thermal ablation Achalasia, 53 75 described, 53 features of, 53 management of past options, 54 POEM
How to stage early BE cancer - EUS or endoscopic removal?
 How to stage early BE cancer - EUS or endoscopic removal? Presented by Bas Weusten Institution St. Antonius Hospital, Nieuwegein Academic Medical Center, Amsterdam case 56 y old female patient Lung transplant
How to stage early BE cancer - EUS or endoscopic removal? Presented by Bas Weusten Institution St. Antonius Hospital, Nieuwegein Academic Medical Center, Amsterdam case 56 y old female patient Lung transplant
Dysplasia 4/19/2017. How do I practice Chromoendoscopy for Surveillance of Colitis? SCENIC: Polypoid Dysplasia in UC. Background
 SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
SCENIC: Polypoid in UC Definition How do I practice for Surveillance of Colitis? Themos Dassopoulos, M.D. Director, BSW Center for IBD Themistocles.Dassopoulos@BSWHealth.org Tel: 469-800-7189 Cell: 314-686-2623
