EVIDENCE TABLES Table 1: Recommendations from United Kingdom (UK) and international referral guidelines for patients with suspected lung cancer
|
|
|
- Carol Lawrence
- 5 years ago
- Views:
Transcription
1 EVIDENCE TABLES Table 1: Recommendations from United Kingdom (UK) and international referral guidelines for patients with suspected lung cancer Title authors, date and country Lung cancer: the diagnosis and treatment of lung cancer - NICE clinical guideline UK Referral and indications for chest radiography: 1. Urgent referral for a chest X-ray should be offered when a patient presents with: [2005] haemoptysis, or any of the following unexplained or persistent (that is, lasting more than 3 weeks) symptoms or signs: - cough - chest/shoulder pain - dyspnoea - weight loss - chest signs - hoarseness - finger clubbing - features suggestive of metastasis from a lung cancer (for example, in brain, bone, liver or skin) - cervical/supraclavicular lymphadenopathy. Quality: 7 Recommend: Yes [2005]: means that the evidence has not been updated and reviewed since
2 authors, date and country 2. If a chest X-ray or chest computed tomography (CT) scan suggests lung cancer (including pleural effusion and slowly resolving consolidation), patients should be offered an urgent referral to a member of the lung cancer multidisciplinary team (MDT), usually a chest physician. [2005] 3. If the chest X-ray is normal but there is a high suspicion of lung cancer, patients should be offered urgent referral to a member of the lung cancer MDT, usually the chest physician. [2005] 4. Patients should be offered an urgent referral to a member of the lung cancer MDT, usually the chest physician, while awaiting the result of a chest X-ray, if any of the following are present: persistent haemoptysis in smokers/ex-smokers older than 40 years signs of superior vena cava obstruction (swelling of the face/neck with fixed elevation of jugular venous pressure) stridor. [2005] 5. Where a chest X-ray has been requested in primary or secondary care and is incidentally suggestive of lung cancer, a second copy of the radiologist s report should be sent to a designated member of the lung cancer MDT, usually the chest physician. The MDT should have a mechanism in place to follow up these reports to enable the patient s GP to have a management plan in place. [2005] 2
3 authors, date and country Suspected cancer in primary care: guidelines for investigations, referral and reducing ethnic disparities - New Zealand Guidelines Group New Zealand Urgent referral (within 2 weeks): 1. A person should be referred urgently to a specialist if they have: Grade C persistent haemoptysis and are smokers or ex-smokers aged 40 years or older a chest x-ray suggestive of lung cancer (including pleural effusion and slowly resolving consolidation) 2. A person should be referred urgently for a chest x-ray if they have: Grade C or unexplained haemoptysis any of the following unexplained, persistent (lasting more than 3 weeks or less than 3 weeks in people with known risk factors ) symptoms and signs: - chest and/or shoulder pain - shortness of breath - weight loss/loss of appetite - abnormal chest signs - hoarseness - finger clubbing - cervical and/or supraclavicular lymphadenopathy - cough - features suggestive of metastasis from a lung cancer (for example in brain, bone, liver or skin). Quality: 7 Recommend: Yes, with modifications Grades of recommendation: All grades indicate the strength of the supporting evidence, rather than the importance of the recommendations. Grade C refers to recommendations supported by international expert opinion. Good practice points are developed, where no evidence is available, based on the opinion of the Guideline Development Team, or feedback from consultation within New Zealand. Current or ex-smokers, smoking-related chronic obstructive 3
4 authors, date and country pulmonary disease, previous exposure to asbestos, history of cancer (especially head and neck cancer) 3. A person should be referred urgently to a specialist if they have a normal chest x-ray, but there is a high suspicion of lung cancer. Grade C This guideline further addressed a number of areas that were not covered in the NICE recommendations. This resulted in the development of four good practice points (based on clinical expert opinion). Good practice points :cancer: referral/investigation The smoking status of all patients should be recorded and regularly updated in the practice notes. After urgent referral for chest x-ray, the chest x-ray should be completed and reported within one week. A person with risk factors* for lung cancer who has consolidation on an initial chest x-ray should have a repeat chest x-ray within 6 weeks to confirm resolution. Sputum cytology is not recommended for the investigation of lung cancer. *Current or ex-smokers, smoking-related chronic obstructive pulmonary disease, previous exposure to asbestos, history of cancer (especially head and neck cancer) 4
5 authors, date and country Management of patients with lung cancer - SIGN clinical guideline UK Symptoms and signs: 1. Patients should be referred urgently for a chest X-ray if they have experienced unexplained or persistent haemoptysis. Grade D 2. Patients should be referred for a chest X-ray if any of the following symptoms persist for more than 3 weeks without an obvious cause: Grade D cough chest/shoulder pain dyspnoea weight loss chest signs hoarseness finger clubbing features suggestive of metastases from lung cancer (for example brain, bone, liver or skin) persistent cervical/supraclavicular lymphadenopathy. Referral to a respiratory physician: 3. Patients should be referred urgently to a chest physician if they have any of the following: Grade D persistent haemoptysis in smokers or ex-smokers over 40 years of age a chest X-ray suggestive or suspicious of lung cancer (including pleural effusion and slowly resolving or recurrent consolidation) Quality: 7 Recommend: Yes Grades of recommendation: Grades indicate the strength of the supporting evidence, rather than the clinical importance of the recommendations. Grade D refers to refers to recommendations supported by evidence from level 3 or 4; or extrapolated evidence from studies rated as 2 +. Good practice points are recommended best practice based on the clinical experience of the guideline development group. Levels of evidence: 2 + : Well-conducted case-control or cohort studies with a low risk of confounding or bias and a moderate probability that the relationship is causal 3: Non-analytic studies, such as case reports, case series 4: Expert opinion. 5
6 authors, date and country signs of superior vena caval obstruction (swelling of the face and or neck with fixed elevation of jugular venous pressure) stridor (emergency referral). 4. Even with a normal chest X-ray, patients who have experienced unexplained, non-specific symptoms, such as fatigue potentially attributable to lung cancer, for more than 6 weeks should be referred urgently to a respiratory physician. Grade D Good practice statement Patients referred to a respiratory physician should be seen promptly, ideally within 2 weeks. 6
7 authors, date and country Referral guidelines for suspected cancer - NICE clinical guideline UK General recommendations: 1. A patient who presents with symptoms suggestive of lung cancer should be referred to a team specialising in the management of lung cancer, depending on local arrangements. Grade D Specific recommendations: 2. An urgent referral for a chest X-ray should be made when a patient presents with: Grade D haemoptysis, or any of the following unexplained persistent (that is, lasting more than 3 weeks) symptoms and signs: - chest and/or shoulder pain - dyspnoea - weight loss - chest signs - hoarseness - finger clubbing - cervical and/or supraclavicular lymphadenopathy - cough with or without any of the above - features suggestive of metastasis from a lung cancer (for example, in brain, bone, liver or skin). A report should be made back to the referring primary healthcare professional within 5 days of referral. Quality: 7 Recommend: Yes The referral timelines used in the guideline are as follows: immediate: an acute admission or referral occurring within a few hours, or even more quickly if necessary urgent: the patient is seen within the national target for urgent referrals (currently 2 weeks) non-urgent: all other referrals. Other definitions: Unexplained refers to a symptom(s) and/or sign(s) that has not led to a diagnosis being made by the primary care professional after initial assessment of the history, examination and primary care investigations (if any). Persistent refers to the continuation of specified symptoms and/or signs beyond a period that would normally be associated with self-limiting problems. The precise period will vary depending on the severity of symptoms and 7
8 authors, date and country 3. An urgent referral should be made for either of the following: Grade D persistent haemoptysis in smokers or ex-smokers who are aged 40 years and older a chest X-ray suggestive of lung cancer (including pleural effusion and slowly resolving consolidation). 4. Immediate referral should be considered for the following: Grade D signs of superior vena caval obstruction (swelling of the face and/or neck with fixed elevation of jugular venous pressure) stridor. Investigations: 5. Unexplained changes in existing symptoms in patients with underlying chronic respiratory problems should prompt an urgent referral for chest X-ray. Grade D 6. If the chest X-ray is normal, but there is a high suspicion of lung cancer, patients should be offered an urgent referral. Grade D 7. In individuals with a history of asbestos exposure and recent onset of chest pain, shortness of breath or unexplained systemic symptoms, lung cancer should be considered and a chest X-ray arranged. If this indicates a pleural effusion, pleural mass or any suspicious lung pathology, an urgent referral should be made. Grade C associated features, as assessed by the healthcare professional. In many cases, the upper limit the professional will permit symptoms and/or signs to persist before initiating referral will be 4 6 weeks. Grades of recommendation: Grade C is directly based on: category III evidence, or extrapolated recommendation from category I or II evidence Grade D is directly based on: category IV evidence, or extrapolated recommendation from category I, II, or III evidence. Levels of evidence: Ia: Evidence from systematic review or meta-analysis of randomised controlled trials Ib: Evidence from at least one randomised controlled trial IIa: Evidence from at least one welldesigned controlled study without randomisation IIb: Evidence from at least one welldesigned quasi-experimental study, 8
9 authors, date and country such as a cohort study III: Evidence from well-designed nonexperimental descriptive studies, casecontrol studies, or case series IV: Evidence from expert committee reports, opinions and/or clinical experience of respected authorities. Clinical Practice Guidelines for the Prevention, Diagnosis and Management of Lung Cancer - National Health and Medical Research Council Australia Lung cancer. Practice organization - Alberts WM, Bepler G, Hazelton T, Ruckdeschel JC, Williams JH Jr US All individuals with suspected lung cancer should be referred to a specialist with expertise in the management of lung disease for an opinion. Level IV evidence Referral pattern 1. All patients with known or suspected lung cancer should be referred to a multidisciplinary team of physicians or a physician with experience in the management of lung cancer. (Quality of evidence: poor; net benefit: substantial; strength of recommendation: C) 2. For patients in whom tissue diagnosis or staging remains incomplete, referral should be to a specialist with expertise in Quality: 7 Recommend: Yes, with modifications Levels of evidence: Level IV refers to evidence obtained from case series, either post-test or pretest and post-test. Quality: 7 Recommend: Yes, with modifications Grades of recommendation: Grade C recommendation indicates that there was consensus among the panel to recommend [the service] but that the evidence that [the service] is effective is 9
10 authors, date and country these areas. When completed, the choice of referral may vary with the interventions(s) proposed. (Quality of evidence: poor; net benefit: moderate; strength of recommendation: C) lacking, of poor quality, or conflicting, or the balance of benefits and harm cannot be reliably determined from available evidence. Definition of net benefit types: The levels of net benefit are based on clinical assessment. Estimated net benefit may be downgraded based on uncertainty in estimates of benefits and harms. Substantial benefit: Benefit greatly outweighs harm. Moderate benefit: Benefit outweighs harm. Small/weak benefit: Benefit outweighs harm to a minimally clinically important degree. None/negative benefit: Harms equal or outweigh benefit, less than clinically important. 10
11 authors, date and country Referral Guidelines for Suspected Cancer - UK Department of Health UK Guidelines for urgent referral Note: In most cases where lung cancer is suspected it is appropriate to arrange an urgent chest x-ray before urgent referral to a chest physician. 1. Urgent referral for a chest x-ray haemoptysis unexplained or persistent (more than 3 weeks) - cough - chest/shoulder pain - dyspnoea - weight loss - chest signs - hoarseness - finger clubbing - features suggestive of metastasis from a lung cancer (for example brain, bone, liver or skin) - persistent cervical/supraclavicular lymphadenopathy. 2. Urgent referral to a chest physician Any of the following: chest x-ray suggestive/suspicious of lung cancer (including pleural effusion and slowly resolving consolidation). persistent haemoptysis in smokers/ex-smokers over 40 years of age. signs of superior vena caval obstruction (swelling of face/neck Quality: 7 Recommend: Yes 11
12 authors, date and country with fixed elevation of jugular venous pressure). stridor (consider emergency referral). 12
13 Table 2: Recommendations from UK and international referral guidelines for patients with suspected breast cancer Title Healthcare guideline: diagnosis of breast disease - Institute for Clinical Systems Improvement USA Suspected cancer in primary care: guidelines for investigations, referral and reducing ethnic disparities - New Zealand Guidelines Group New Zealand Clinical highlights: 1. Patients with a bloody or clear discharge should be referred to a radiologist and/or surgeon for further evaluation. 2. A persistent mass with negative imaging does not rule out malignancy and requires a referral to a surgeon. Recommendations for urgent referral (within 2 weeks): 1. A woman with a palpable hard, fixed or tethered breast lump should be referred urgently to a specialist.* Grade C 2. A person presenting with unilateral eczematous skin or nipple change that does not respond to topical treatment, or with nipple distortion of recent onset, should be referred urgently to a specialist.* Grade C 3. A person presenting with spontaneous unilateral bloody nipple discharge should be referred urgently to a specialist.* Grade C Recommendations for referral/investigation: 1. A palpable breast lump in a woman should be investigated. Grade C 2. A woman with an abscess or mastitis which does not Quality: 6 Recommend: Yes, with modifications Annotations: The work group utilised information from current and optimal practices to develop or revise clinical patient pathways and algorithms, and to draft annotations. Quality: 7 Recommend: Yes, with modifications Grades of recommendation: Grades indicate the strength of the supporting evidence, rather than the importance of the recommendations. Grade C refers to recommendations supported by international expert opinions Good practice points are developed, where no evidence is available, based on the opinion of the Guideline Development Team, or feedback from consultation within New Zealand. *Recommendation consistent with: Referral guidelines for suspected cancer. NICE clinical guideline
14 settle after one course of antibiotics should be referred to a specialist. Grade C 3. A woman over 40 years of age with a breast abscess that has settled should be referred for mammography. Grade C 4. Persistent, unilateral, unexplained breast pain in a postmenopausal woman should be investigated. Grade C 5. For a person presenting solely with breast pain, with no palpable abnormality, referral to a specialist may be considered in the event of failure of initial treatment and/or unexplained persistent symptoms. Initial mammography is not recommended.* Grade C Good practice points for referral/investigation 1. An adult man with a unilateral, firm subareolar mass should be referred to a specialist.* 2. For a person presenting with symptoms and/or signs suggestive of breast cancer, investigation may be instigated by the practitioner, but should not delay referral to a specialist. Recommendation consistent with: Scottish Intercollegiate Guidelines Network. Management of breast cancer in women. National clinical guideline No. 84. Edinburgh: SIGN; A woman under 30 years of age presenting with generalised lumpiness in the breast tissue, where a focal area of concern, unchanged following a menstrual period, is identified, should be referred to a specialist. If a woman has a family history of premature breast cancer 14
15 Familial breast cancer: The classification and care of women at risk of familial breast cancer in primary, secondary and tertiary care - NICE clinical guideline UK an earlier referral for investigation should be considered. When a woman presents with breast symptoms or has concerns about relatives with breast cancer, a first- and second-degree family history should be taken in primary care to assess risk, because this allows appropriate classification and care. Referral from primary care: 1. Women who meet the following criteria should be offered referral to secondary care: one first-degree female relative diagnosed with breast cancer at younger than age 40 years, or one first-degree male relative diagnosed with breast cancer at any age, or one first-degree relative with bilateral breast cancer where the first primary was diagnosed at younger than age 50 years or two first-degree relatives, or one first-degree and one second-degree relative, diagnosed with breast cancer at any age, or one first-degree or second-degree relative diagnosed with breast cancer at any age and one first-degree or second-degree relative diagnosed with ovarian cancer at any age (one of these should be a first-degree relative) or three first-degree or second-degree relatives diagnosed Quality: 7 Recommend: Yes 15
16 with breast cancer at any age. Referral guidelines for suspected cancer - NICE clinical guideline UK 2. Direct referral to a specialist genetics service should take place where a high-risk predisposing gene mutation has been identified (for example, BRCA1, BRCA2 or TP53). General recommendations: 1. A patient who presents with symptoms suggestive of breast cancer should be referred to a team specialising in the management of breast cancer. Grade D 2. In most cases, the definitive diagnosis will not be known at the time of referral, and many patients who are referred will be found not to have cancer. However, primary healthcare professionals should convey optimism about the effectiveness of treatment and survival because a patient being referred with a breast lump will be naturally concerned. Grade C 3. People of all ages who suspect they have breast cancer may have particular information and support needs. The primary healthcare professional should discuss these needs with the patient and respond sensitively to them. Grade D 4. Primary healthcare professionals should encourage all patients, including women over 50 years old, to be breast aware in order to minimise delay in the presentation of symptoms. Grade D Quality: 7 Recommend: Yes Grades of recommendation: Grade C is directly based on: category III evidence, or extrapolated recommendation from category I or II evidence Delete space for consistency with others Grade D is directly based on: category IV evidence, or extrapolated recommendation from category I, II, or III evidence Delete space Grade B (DS) is directly based on category II evidence (evidence from level 2 studies, or systematic reviews of level 2 studies) DS refers to diagnostic studies. Levels of evidence: Ia: Evidence from systematic review or meta-analysis of randomised controlled 16
17 Specific recommendations: 1. A woman s first suspicion that she may have breast cancer is often when she finds a lump in her breast. The primary healthcare professional should examine the lump with the patient s consent. The features of a lump that should make the primary healthcare professional strongly suspect cancer are a discrete, hard lump with fixation, with or without skin tethering. In patients presenting in this way an urgent referral should be made, irrespective of age. Grade C 2. In a woman aged 30 years and older with a discrete lump that persists after her next period, or presents after menopause, an urgent referral should be made. Grade C 3. Breast cancer in women aged younger than 30 years is rare, but does occur. Benign lumps (for example, fibroadenoma) are common, however, and a policy of referring these women urgently would not be appropriate; instead, non-urgent referral should be considered. However, an urgent referral should be made in women aged younger than 30 years: with a lump that enlarges, Grade C or with a lump that has other features associated with cancer (fixed and hard), Grade C or in whom there are other reasons for concern such as family history. Grade D trials Ib: Evidence from at least one randomised controlled trial IIa: Evidence from at least one welldesigned controlled study without randomisation IIb: Evidence from at least one welldesigned quasi-experimental study, such as a cohort study III: Evidence from well-designed nonexperimental descriptive studies, casecontrol studies, or case series IV: Evidence from expert committee reports, opinions and/or clinical experience of respected authorities. Level-2 studies are studies that have only one of the following: narrow population (the sample does not reflect the population to whom the test would apply) use a poor reference standard (defined as that where a test is included in the reference, or where the testing affects the reference ) the comparison between the test and reference standard is not blind are case-control studies. 17
18 4. The patient s history should always be taken into account. For example, it may be appropriate, in discussion with a specialist, to agree referral within a few days in patients reporting a lump or other symptom that has been present for several months. Grade D 5. In a patient who has previously had histologically confirmed breast cancer, who presents with a further lump or suspicious symptoms, an urgent referral should be made, irrespective of age. Grade C 6. In patients presenting with unilateral eczematous skin or nipple change that does not respond to topical treatment, or with nipple distortion of recent onset, an urgent referral should be made. Grade C 7. In patients presenting with spontaneous unilateral bloody nipple discharge, an urgent referral should be made. Grade C 8. Breast cancer in men is rare and is particularly rare in men under 50 years of age. However, in a man aged 50 years and older with a unilateral, firm subareolar mass with or without nipple distortion or associated skin changes, an urgent referral should be made. Grade C Investigations: 9. In patients presenting with symptoms and/or signs suggestive of breast cancer, investigation prior to referral is not recommended. Grade D 18
19 10. In patients presenting solely with breast pain, with no palpable abnormality, there is no evidence to support the use of mammography as a discriminatory investigation for breast cancer. Therefore, its use in this group of patients is not recommended. Non-urgent referral may be considered in the event of failure of initial treatment and/or unexplained persistent symptoms. Grade B (DS) 19
20 Management of breast cancer in women - SIGN clinical guideline UK Clinical practice guidelines for the management and support of younger women with breast cancer - National Health and Medical research Council Australia Triggers for prompt referral to a breast clinic: Referral from primary to specialist care should be made in accordance with the Scottish Cancer Group referral guideline (see Appendix 1). Younger age has been associated with physician delay in referral for investigation of breast symptoms. For this reason, young women presenting with breast symptoms should be evaluated by means of the triple test approach to exclude or establish a diagnosis of cancer. Level III-2 Quality: 7 Recommend: Yes Good practice points are recommended best practice based on the clinical experience of the guideline development group. Quality: 6 Recommend: Yes, with modifications Level III-2 refers to evidence which is obtained from comparative studies with concurrent controls and allocation not randomised (cohort studies). Clinical practice guidelines for the management of early breast cancer: Second edition - National Health and Medical research Council Australia Key point (not recommendation): When organising referral for women with breast cancer, GPs should consider both the preferences of the patient and the fact that patient outcomes are better if treated by clinicians who are part of a multidisciplinary team. Quality: 7 Recommend: Yes, with modifications 20
21 Guidance on cancer service: improving outcomes in breast cancer - NICE UK Conditions that require urgent referral (within 2 weeks): 1. Patients aged 30 or over (the precise age criterion to be agreed by each network) with a discrete lump in the breast. 2. Patients with breast signs or symptoms which are highly suggestive of cancer. These include: ulceration skin nodule skin distortion nipple eczema recent nipple retraction or distortion (< 3 months) unilateral nipple discharge which stains clothes. Conditions that require referral, not necessarily urgent: 1. Breast lumps in the following patients, or of the following types: discrete lump in a younger woman (age < 30 years) asymmetrical nodularity that persists at review after menstruation abscess persistently refilling or recurrent cyst. 2. Intractable pain which does not respond to simple measures such as wearing a well-fitting bra and using over-the-counter analgesics such as paracetamol. Quality: 7 Recommend: Yes 21
22 3. Nipple discharge: bilateral discharge sufficient to stain clothes in patients aged < 50 years bloodstained discharge in patients aged < 50 years (urgent referral required if discharge is unilateral) any nipple discharge in patients over 50 years of age. 22
23 Referral guidelines for suspected cancer - UK Department of Health UK Guidelines for urgent referral: 1. Patients with a discrete lump in the appropriate age group (for example age > 30). 2. Signs which are highly suggestive of cancer such as: ulceration skin nodule skin distortion nipple eczema recent nipple retraction or distortion (< 3 months). Conditions that require referral but not necessarily urgently: 1. Lump discrete lump in a younger woman (for example age < 30 years) asymmetrical nodularity that persists at review after menstruation abscess persistently refilling or recurrent cyst. 2. Pain intractable pain not responding to reassurance, simple measures such as wearing a well supporting bra and common drugs. Quality: 7 Recommend: Yes Note: The guidelines for urgent referral of patients with suspected breast cancer in this document are based on recommendations set out in Guidelines for Referral of Patients with Breast Problems second edition 1999 prepared by Joan Austoker and Robert Mansel under the auspices of the NHS Breast Screening Programme and the Cancer Research Campaign. 23
24 3. Nipple age < 50 with bilateral discharge sufficient to stain clothes. 4. Discharge age < 50 with bloodstained discharge age > 50 with any nipple discharge. 24
25 Table 3: Recommendations from UK and international referral guidelines for patients with suspected lower gastrointestinal cancer Title Diagnosis and management of colorectal cancer - SIGN clinical guideline UK Recommendations for primary care and referral: 1. Patients over the age of 40 who present with new onset, persistent or recurrent rectal bleeding should be referred for investigation. Grade B 2. Review of the patient by a regional clinical genetics service is recommended for accurate risk assessment if family history of colorectal cancer is the principal indication for referral for investigation. Grade C 3. General practitioners should perform an abdominal and rectal examination on all patients with symptoms indicative of colorectal cancer. A positive finding should expedite referral, but a negative rectal examination should not rule out the need to refer. Grade B 4. All symptomatic patients should have a full blood count. In cases of anaemia the presence of iron deficiency should be determined. Grade B Quality: 7 Recommend: Yes Grades of recommendation: Grade B refers to a body of evidence including studies rated as 2 ++, directly applicable to the target population, and demonstrating overall consistency of results; or extrapolated evidence from studies rated as 1 ++ or 1 +. Grade C refers to a body of evidence including studies rated as 2 +, directly applicable to the target population and demonstrating overall consistency of results; or extrapolated evidence from studies rated as Levels of evidence: 1 ++ : High quality meta-analyses, systematic reviews of RCTs, or RCTs with a very low risk of bias + 1 : Well-conducted meta-analyses, systematic reviews, or RCTs with a low risk of bias 2 ++ : High quality systematic reviews of casecontrol or cohort studies OR high quality casecontrol or cohort studies with a very low risk of confounding or bias and a high probability that 25
26 Guidelines for colorectal cancer screening and surveillance in moderate and high risk groups (update from 2002) - The British Society of Gastroenterology (BSG) and the Association of Coloproctology for Great Britain and Ireland (ACPGBI) UK Guidance on large bowel surveillance for individuals with a family history indicating a moderate risk: 1. Referrals on the basis of family history are best coordinated through centres with a specialist interest, such as regional genetics services or medical/surgical gastroenterology centres. Such centralisation enables audit of family history ascertainment, assigned level of risk, collection of outcome data and research. Grade C the relationship is causal. 2 + : Well-conducted case-control or cohort studies with a low risk of confounding or bias and a moderate probability that the relationship is causal. Quality: 5 Recommend: Yes, with modifications The strength of each recommendation is dependent upon the category of the evidence supporting it. Grade C is based on evidence obtained from expert committee reports or opinions or clinical experiences of respected authorities. 26
27 Suspected cancer in primary care: guidelines for investigations, referral and reducing ethnic disparities - New Zealand Guidelines Group New Zealand Recommendations for urgent referral (within 2 weeks): 1. A person aged 40 years and older reporting rectal bleeding with a change of bowel habit towards looser stools and/or increased stool frequency persisting for 6 weeks or more should be referred urgently to a specialist.* Grade C 2. A person aged 60 years and older with rectal bleeding persisting for 6 weeks or more without a change in bowel habit and without anal symptoms should be referred urgently to a specialist.* Grade C 3. A person aged 60 years and older with a change in bowel habit to looser stools and/or more frequent stools persisting for 6 weeks or more without rectal bleeding should be referred urgently to a specialist.* Grade C 4. A person presenting with a palpable rectal mass (intraluminal and not pelvic), should be referred urgently to a specialist, irrespective of age. Note that a pelvic mass outside the bowel should be referred urgently to a urologist or gynaecologist.* Grade C 5. A man of any age with unexplained iron deficiency anaemia and a haemoglobin of 110 g/l or below, should be referred urgently to a specialist.* Grade C 6. A non-menstruating woman with unexplained iron Quality: 7 Recommend: Yes, with modifications Grades of recommendation: Grades indicate the strength of the supporting evidence, rather than the importance of the recommendations. Grade C refers to recommendations supported by international expert opinions. Good practice points are developed, where no evidence is available, based on the opinion of the Guideline Development Team, or feedback from consultation within New Zealand. *Recommendation consistent with: Referral guidelines for suspected cancer. NICE clinical guideline **Unexplained iron deficiency anaemia means unrelated to other sources of blood loss, for example, non-steroidal anti-inflammatory drug treatment or blood dyscrasia. 27
28 deficiency anaemia and a haemoglobin of 100 g/l or below, should be referred urgently to a specialist.* Grade C Good practice points for urgent referral (within 2 weeks): 1. A person presenting with a right-sided abdominal mass, should be referred urgently for a surgical opinion. 2. A menstruating woman with unexplained iron deficiency anaemia** and a haemoglobin of 100 g/l or below, should be referred urgently to a specialist. Recommendations for referral/investigation: 1. For a person with equivocal symptoms, a complete blood count may help in identifying the possibility of colorectal cancer by demonstrating iron deficiency anaemia. This should determine if a referral is needed and whether the person should be urgently referred to a specialist.* Grade C 2. For a person where the decision to refer to a specialist has been made, a complete blood count may be considered to assist specialist assessment in the outpatient clinic.* Grade C 3. For a person where the decision to refer to a specialist has been made, no examinations or investigations other than an abdominal and rectal 28
29 examination, and a complete blood count should be undertaken as this may delay referral.* Grade C Good practice points for referral/investigation: 1. A person at low risk of colorectal cancer with a significant symptom (rectal bleeding or a change in bowel habit) and a normal rectal examination, no anaemia and no abdominal mass, should be managed by a strategy of treat, watch and review in 3 months. 2. In a person presenting with a left-sided abdominal mass, faecal loading should first be excluded as the cause. A referral should then be made for a surgical opinion. 3. Faecal occult blood and carcinogenic embryonic antigen testing are of little value in a person with symptoms suggestive of colorectal cancer and should not be used. 4. A person with any unexplained gastrointestinal symptoms and known high-risk factors, for example, familial adenomatous polyposis, hereditary nonpolyposis colorectal cancer, other familial colorectal syndromes or a past history of lower gastrointestinal cancer should be referred to a specialist. 29
30 Referral guidelines for suspected cancer - NICE clinical guideline UK General recommendations: 1. A patient who presents with symptoms suggestive of colorectal or anal cancer should be referred to a team specialising in the management of lower gastrointestinal cancer, depending on local arrangements. Grade D Specific recommendations: 1. In patients aged 40 years and older, reporting rectal bleeding with a change of bowel habit towards looser stools and/or increased stool frequency persisting for 6 weeks or more, an urgent referral should be made. Grade C 2. In patients aged 60 years and older, with rectal bleeding persisting for 6 weeks or more without a change in bowel habit and without anal symptoms, an urgent referral should be made. Grade C 3. In patients aged 60 years and older, with a change in bowel habit to looser stools and/or more frequent stools persisting for 6 weeks or more without rectal bleeding, an urgent referral should be made. Grade C 4. In patients presenting with a right lower abdominal mass consistent with involvement of the large bowel, an urgent referral should be made, irrespective of age. Grade C Quality: 7 Recommend: Yes Grades of recommendation: Grade C is directly based on: category III evidence, or extrapolated recommendation from category I or II evidence. Grade D is directly based on: category IV evidence, or extrapolated recommendation from category I, II, or III evidence. Levels of evidence: Ia: Evidence from systematic review or metaanalysis of randomised controlled trials Ib: Evidence from at least one randomised controlled trial IIa: Evidence from at least one well-designed controlled study without randomisation IIb: Evidence from at least one well-designed quasi-experimental study, such as a cohort study III: Evidence from well-designed nonexperimental descriptive studies, case-control studies, or case series IV: Evidence from expert committee reports, opinions and/or clinical experience of 30
31 5. In patients presenting with a palpable rectal mass (intraluminal and not pelvic), an urgent referral should be made, irrespective of age. (A pelvic mass outside the bowel would warrant an urgent referral to a urologist or gynaecologist.) Grade C 6. In men of any age with unexplained iron deficiency anaemia and a haemoglobin of 11 g/100 ml or below, an urgent referral should be made. Grade C 7. In non-menstruating women with unexplained iron deficiency anaemia and a haemoglobin of 10 g/100 ml or below, an urgent referral should be made. Grade C Recommendations for patients with risk factors: 1. In patients with ulcerative colitis or a history of ulcerative colitis, a plan for follow up should be agreed with a specialist and offered to the patient as a normal procedure in an effort to detect colorectal cancer in this high-risk group. Grade C 2. There is insufficient evidence to suggest that a positive family history of colorectal cancer can be used as a criterion to assist in the decision about referral of a symptomatic patient. Grade C respected authorities. 31
32 Clinical Practice Guidelines for the prevention, early detection and management of colorectal cancer - National Health and Medical Research Council Australia Investigation: 1. In symptomatic patients aged over 40 years, referral to a specialist should be considered and consideration of full examination of the colon with colonoscopy is recommended. Level III-3; Equivocal Quality: 7 Recommend: Yes, with modifications Levels of evidence: Level III-3 refers to evidence obtained from comparative studies with historical control, two or more single arm studies, or interrupted time series without a parallel control group. Grades of recommendation: Strength of evidence was determined by the expert advisory panel. Equivocal refers to situations where there is lack of higher levels of evidence (such as III-3 or IV) OR equivocal level I or II evidence for and against clinical question no recommendation for or against, as evidence is inconclusive recommend further research. 32
33 Guidance on cancer services: improving outcomes in colorectal cancers - NICE UK Action should be taken to improve recognition of potential symptoms of colorectal cancer in primary care and in the community. Efficient systems should be set up to ensure that patients who may have colorectal cancer are rapidly referred for endoscopy. Criteria for urgent referral: Age threshold Quality: 7 Recommend: Yes rectal bleeding WITH a change in bowel habit to looser stools and/or increased frequency of defecation persistent for 6 weeks a definite palpable right-sided abdominal mass a definite palpable rectal (not pelvic) mass rectal bleeding persistently WITHOUT anal symptoms* change of bowel habit to looser stools and/or increased frequency of defecation, WITHOUT rectal bleeding and persistent for 6 weeks iron deficiency anaemia All ages All ages All ages Over 60 years Over 60 years No age 33
34 WITHOUT an obvious cause (Hb < 11 g/dl in men or < 10 g/dl in postmenopausal women). criterion * Anal symptoms include soreness, discomfort, itching, lumps and prolapse as well as pain. Age 60 years is considered to be the maximum age threshold. Local Cancer Networks may elect to set a lower age threshold (such as 55 years or 50 years). Additional notes 1. Symptoms other than those in the list above, which should also prompt referral for endoscopy, include faecal incontinence and passing mucus via the rectum. 2. Patients with iron-deficiency anaemia (apart from menstruating women) should be referred for colonoscopy 3. The threshold for referral for investigation should be reduced if other members of the patient s family have had a diagnosis of colorectal cancer. 4. GPs should not refer patients with suspected colorectal cancer to a specific clinician (as opposed to a diagnostic clinic) who is not a core member of a colorectal cancer multidisciplinary team 34
35 Referral Guidelines for Suspected Cancer - UK Department of Health Patients with non-specific symptoms: 1. The most common non-specific symptoms of colorectal cancer for example, tiredness are due to iron-deficiency anaemia caused by undetected blood loss, particularly in older men or postmenopausal women; patients with bowel polyps or cancer may have no other symptoms. Trusts should agree specific local guidelines which ensure that such patients are referred promptly to the endoscopy service. 2. People with two first-degree relatives with colorectal cancer, or one first-degree relative whose colorectal cancer is diagnosed before the age of 45, have a lifetime risk of death from colorectal cancer of 1 in 6, or 1 in 10, respectively. The British Society of Gastroenterology (BSG) and the Association of Coloproctology for Great Britain and Ireland (ACPGBI) guidelines suggest that people who meet these criteria should be referred for colonoscopy at years of age, or as soon thereafter as the risk is recognised. Guidelines for urgent referral: It is recommended that the following symptom and sign combinations when occurring for the first time should be used to identify patients for urgent referral under the 2 week standard: Quality: 6 Recommend: Yes 35
36 - UK Age threshold rectal bleeding WITH a change in bowel habit to looser stools and/or increased frequency of defecation persistent for 6 weeks a definite palpable right-sided abdominal mass a definite palpable rectal (not pelvic) mass rectal bleeding persistently WITHOUT anal symptoms* change of bowel habit to looser stools and/or increased frequency of defecation, WITHOUT rectal bleeding and persistent for 6 weeks. All ages All ages All ages Over 60 years Over 60 years Iron deficiency anaemia WITHOUT an obvious cause (Hb < 11 g/dl in men or < 10 g/dl in postmenopausal women). Note: Patients with the following symptoms and no 36
37 abdominal or rectal mass, are at very low risk of cancer: rectal bleeding with anal symptoms* change in bowel habit to decreased frequency of defecation and harder stools abdominal pain without clear evidence of intestinal obstruction. * Anal symptoms include soreness, discomfort, itching, lumps and prolapse as well as pain. Age 60 years is considered to be the maximum age threshold. Local Cancer Networks may elect to set a lower age threshold (such as 55 years or 50 years). 37
38 Appendix 1: Scottish Cancer Group Referral Guideline Source of problem Who to refer Who to manage in primary care Lump 1. women with any new discrete lump 2. women with any new lump in pre-existing nodularity 3. women with any new asymmetrical nodularity that persists at review after menstruation 4. women with a non lactational abscess or mastitis which does not settle after one course of antibiotics 5. abscess in patient > 40 years even after settled (for mammogram) 6. women with any cyst persistently refilling or recurrent cyst 7. women with unilateral axillary lymph node lump 1. young women < 35 years with longstanding tender, lumpy breasts 2. older women with symmetrical nodularity if no localised abnormality 3. young girls with tender developing breasts 4. women with bilateral fatty gynaecomastia without focal abnormality Pain 1. post-menopausal women with unilateral persistent pain 2. women with pain associated with a lump 3. women with intractable pain that interferes with a patient s lifestyle or sleep and which has failed to respond to reassurance or simple measures such as wearing a well-supporting bra and common drugs 1. women with moderate degrees of breast pain no discrete palpable 38
39 Source of problem Who to refer Who to manage in primary care 1. women < 50 years with nipple discharge from > 1 Nipple symptom 1. women < 50 years with persistent discharge, which is: bloodstained; (dipstick for blood) or single duct duct, intermittent - not bloodstained (urine dipstick for blood) 2. women with bilateral troublesome discharge sufficient to stain outer clothes (would consider surgery) 2. women with longstanding nipple retraction 3. all women > 50 years with discharge 4. women with new nipple retraction 5. women with nipple eczema if not elsewhere or unresponsive to topical steroids Skin changes 1. women with skin tethering 2. fixation 3. women with ulceration 4. women with abscess or breast inflammation if not settled after one course of antibiotics 5. women > 40 with abscess or inflammation even after settled to exclude underlying cause (mammogram) 1. women with obvious simple skin lesions, such as sebaceous cysts should be managed as when present elsewhere and not referred to a breast clinic 39
Investigating Symptoms of Lung Cancer An evidence based Guide for general practitioners
 Medicine, Nursing and Health Sciences Investigating Symptoms of Lung Cancer An evidence based Guide for general practitioners Dr Kay Jones Professor Danielle Mazza Dr Samantha Chakraborty Prof essor Ian
Medicine, Nursing and Health Sciences Investigating Symptoms of Lung Cancer An evidence based Guide for general practitioners Dr Kay Jones Professor Danielle Mazza Dr Samantha Chakraborty Prof essor Ian
PRIORITIES AND CLINICAL EFFECTIVENESS FORUM
 PRIORITIES AND CLINICAL EFFECTIVENESS FORUM CANCER - GUIDELINES FOR URGENT REFERRAL OF PATIENTS WITH These guidelines are intended as a quick reference for GPs to ensure appropriate referral of those patients
PRIORITIES AND CLINICAL EFFECTIVENESS FORUM CANCER - GUIDELINES FOR URGENT REFERRAL OF PATIENTS WITH These guidelines are intended as a quick reference for GPs to ensure appropriate referral of those patients
NHS Cancer Screening Programmes. with breast problems. Second edition. (with amendments) revised by. Joan Austoker. Robert Mansel
 NHS Cancer Screening Programmes with breast problems Second edition (with amendments) revised by Joan Austoker Robert Mansel Authors Dr Joan Austoker Director CRC Primary Care Education Research Group
NHS Cancer Screening Programmes with breast problems Second edition (with amendments) revised by Joan Austoker Robert Mansel Authors Dr Joan Austoker Director CRC Primary Care Education Research Group
Lung Cancer - Suspected
 Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Value of symptoms and additional diagnostic tests for colorectal cancer in primary care: systematic review and meta-analysis
 Value of symptoms and additional diagnostic tests for colorectal cancer in primary care: systematic review and meta-analysis BMJ 2010;340:c1269 doi:10.1136/bmj.c1269 Mr DC 62 year old man Borderline anaemia
Value of symptoms and additional diagnostic tests for colorectal cancer in primary care: systematic review and meta-analysis BMJ 2010;340:c1269 doi:10.1136/bmj.c1269 Mr DC 62 year old man Borderline anaemia
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography
 Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Referral Criteria for Direct Access Outpatient Colonoscopy or Computed Tomography Colonography 2019 Released 2019 health.govt.nz Citation: Ministry of Health. 2019. Referral Criteria for Direct Access
Current issues and controversies in breast imaging. Kate Brown, South GP CME 2015
 Current issues and controversies in breast imaging Kate Brown, South GP CME 2015 JUDICIOUS USE OF RESOURCES IN REFERRALS FOR BREAST IMAGING THE DILEMMA How do target referrals for breast imaging? Want
Current issues and controversies in breast imaging Kate Brown, South GP CME 2015 JUDICIOUS USE OF RESOURCES IN REFERRALS FOR BREAST IMAGING THE DILEMMA How do target referrals for breast imaging? Want
NICE Quality Standards and COF
 NICE Quality Standards and COF David Baldwin Consultant Respiratory Physician NUH Hon Senior Lecturer Nottingham University Clinical lead NICE lung cancer GL Chair NICE QS Topic Expert Group Quality Standards
NICE Quality Standards and COF David Baldwin Consultant Respiratory Physician NUH Hon Senior Lecturer Nottingham University Clinical lead NICE lung cancer GL Chair NICE QS Topic Expert Group Quality Standards
Referral guidelines for suspected cancer
 Referral guidelines for suspected cancer NICE guideline Second draft for consultation, September 2004 If you wish to comment on the recommendations, please make your comments on the full version of the
Referral guidelines for suspected cancer NICE guideline Second draft for consultation, September 2004 If you wish to comment on the recommendations, please make your comments on the full version of the
Transforming Cancer Services for London
 Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
SCOTTISH CANCER REFERRAL GUIDELINES REVIEW 2018
 SCOTTISH CANCER REFERRAL GUIDELINES REVIEW 2018 Dr Peter Hutchison, Chair of Review Group WHAT & WHY? Scottish Cancer Referral Guidelines 2014 Scottish Primary Care Cancer Group identified need for some
SCOTTISH CANCER REFERRAL GUIDELINES REVIEW 2018 Dr Peter Hutchison, Chair of Review Group WHAT & WHY? Scottish Cancer Referral Guidelines 2014 Scottish Primary Care Cancer Group identified need for some
Disclaimer no conflict of interest
 Disclaimer no conflict of interest Benign Breast Disease Alison Hayes FRACS Content Clinical assessment of the breast Triple assessment Focal nodularity Breast pain Cysts Infection Nipple discharge Gynaecomastia
Disclaimer no conflict of interest Benign Breast Disease Alison Hayes FRACS Content Clinical assessment of the breast Triple assessment Focal nodularity Breast pain Cysts Infection Nipple discharge Gynaecomastia
Dr Greg Frazer. Respiratory Physician Christchurch Hospital Christchurch. 15:10-15:35 Primary and Secondary Healthcare Interface Supported by:
 Dr Greg Frazer Respiratory Physician Christchurch Hospital Christchurch 15:10-15:35 Primary and Secondary Healthcare Interface Supported by: Primary and Secondary Healthcare Interface How Working Together
Dr Greg Frazer Respiratory Physician Christchurch Hospital Christchurch 15:10-15:35 Primary and Secondary Healthcare Interface Supported by: Primary and Secondary Healthcare Interface How Working Together
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Urgent referral for suspected cancer in Scotland
 270 Oncology Urgent referral for suspected cancer in Scotland Cancer is a common problem, but an individual GP may only see about seven to eight new cases of cancer per annum (although they will see many
270 Oncology Urgent referral for suspected cancer in Scotland Cancer is a common problem, but an individual GP may only see about seven to eight new cases of cancer per annum (although they will see many
Early Detection of Lung Cancer
 UK Data Archive Study Number 6647 - National Awareness and Early Diagnosis Initiative: Cancer Awareness Measure, Doncaster, 2008: Special Licence Access Early Detection of Lung Cancer Information for General
UK Data Archive Study Number 6647 - National Awareness and Early Diagnosis Initiative: Cancer Awareness Measure, Doncaster, 2008: Special Licence Access Early Detection of Lung Cancer Information for General
Faster Cancer Treatment Indicators: Use cases
 Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Faster Cancer Treatment Indicators: Use cases 2014 Date: October 2014 Version: Owner: Status: v01 Ministry of Health Cancer Services Final Citation: Ministry of Health. 2014. Faster Cancer Treatment Indicators:
Breast lumps to refer or not to refer? Simon Cawthorn Breast Specialist
 Breast lumps to refer or not to refer? Simon Cawthorn Breast Specialist Learning objectives Know the indications to refer urgently Who to reassure and review How to reassure patients with non-urgent symptoms
Breast lumps to refer or not to refer? Simon Cawthorn Breast Specialist Learning objectives Know the indications to refer urgently Who to reassure and review How to reassure patients with non-urgent symptoms
NICE guideline on Suspected cancer: recognition and referral (2015) Education package for GPs and Nurse Practitioners Case scenarios
 NICE guideline on Suspected cancer: recognition and referral (2015) Education package for GPs and Nurse Practitioners Case scenarios How to use the case scenarios The case scenarios can be used in a training
NICE guideline on Suspected cancer: recognition and referral (2015) Education package for GPs and Nurse Practitioners Case scenarios How to use the case scenarios The case scenarios can be used in a training
COLORECTAL CARCINOMA
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY
 Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Position Statement produced by BSG, AUGIS and ACPGBI GUIDANCE ON THE INDICATIONS FOR DIAGNOSTIC UPPER GI ENDOSCOPY, FLEXIBLE SIGMOIDOSCOPY AND COLONOSCOPY Introduction In 2011 the Independent Practice
Referral of Suspected Lung Cancer by Family Physicians and Other Primary Care Providers
 Evidence-Based Series 24-2 IN REVIEW Referral of Suspected Lung Cancer by Family Physicians and Other Primary Care Providers L. Del Giudice, S. Young, E. Vella, M. Ash, P. Bansal, A. Robinson, R. Skrastins,
Evidence-Based Series 24-2 IN REVIEW Referral of Suspected Lung Cancer by Family Physicians and Other Primary Care Providers L. Del Giudice, S. Young, E. Vella, M. Ash, P. Bansal, A. Robinson, R. Skrastins,
Referral guidelines for suspected cancer
 Referral guidelines for suspected cancer Understanding NICE guidance information for people who may need a referral, their families and carers, and the public Prepared for second consultation The paragraphs
Referral guidelines for suspected cancer Understanding NICE guidance information for people who may need a referral, their families and carers, and the public Prepared for second consultation The paragraphs
BOWEL CANCER. Causes of bowel cancer
 A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
A cancer is an abnormality in an organ that grows without control. The growth is often quite slow, but will continue unabated until it is detected. It can cause symptoms by its presence in the organ or
Bowel cancer risk in the under 50s. Greg Rubin Professor of General Practice and Primary Care
 Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Bowel cancer risk in the under 50s Greg Rubin Professor of General Practice and Primary Care Prevalence of GI problems in the consulting population Thompson et al, Gut 2000 Number of patients % of patients
Referral guidelines for suspected cancer
 Quick reference guide Issue date: June 2005 Referral guidelines for suspected cancer Clinical Guideline 27 Developed by the National Collaborating Centre for Primary Care Ordering information Copies of
Quick reference guide Issue date: June 2005 Referral guidelines for suspected cancer Clinical Guideline 27 Developed by the National Collaborating Centre for Primary Care Ordering information Copies of
Rapid referral toolkit
 Menu Introduction and help Cancer types and contacts Cancer services team Rapid referral toolkit Macmillan resources Acknowledgements www.macmillan.org.uk Macmillan Cancer Support, registered charity in
Menu Introduction and help Cancer types and contacts Cancer services team Rapid referral toolkit Macmillan resources Acknowledgements www.macmillan.org.uk Macmillan Cancer Support, registered charity in
Lung Cancer Case Study
 Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
Lung Cancer Case Study Presented by s GP Education Programme 2 Part One Initial presentation 60 year old lady, presents with a 6 week history of right sided chest pain. The pain is like a dull ache, but
Introduction. Please note the toolkit aims to share learning and good practice, but it is, of necessity, brief in nature.
 July 2015 edition Introduction The Rapid Referral guidance toolkit has been produced by Macmillan Cancer Support. It contains the NICE referral guidelines for suspected cancer (2015 update) with additional
July 2015 edition Introduction The Rapid Referral guidance toolkit has been produced by Macmillan Cancer Support. It contains the NICE referral guidelines for suspected cancer (2015 update) with additional
SIGNS, SYMPTOMS AND SCREENING GUIDELINES
 SIGNS, SYMPTOMS AND SCREENING GUIDELINES SIGNS AND SYMPTOMS You may think it s normal, but it could be a sign or symptom of an illness or cancer-related disease. If you are experiencing any of these signs
SIGNS, SYMPTOMS AND SCREENING GUIDELINES SIGNS AND SYMPTOMS You may think it s normal, but it could be a sign or symptom of an illness or cancer-related disease. If you are experiencing any of these signs
Guidelines for Breast, Cervical and Colorectal Cancer Screening
 Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
Guidelines for Breast, Cervical and Colorectal Cancer Screening Your recommendation counts. Talk to your patients about screening for cancer. CancerCare Manitoba provides organized, population-based screening
South Yorkshire, Bassetlaw and North Derbyshire Cancer Alliance
 South Yorkshire, Bassetlaw and North Derbyshire Cancer Alliance Patient Details: Patient Name Address DOB Home Tel. No. Mobile Tel. No. Preferred Tel. No. Main Spoken Language Transport needed? Registered
South Yorkshire, Bassetlaw and North Derbyshire Cancer Alliance Patient Details: Patient Name Address DOB Home Tel. No. Mobile Tel. No. Preferred Tel. No. Main Spoken Language Transport needed? Registered
Information leaflet for women with an increased lifetime risk of breast and ovarian cancer. Hereditary Breast and Ovarian Cancer (HBOC)
 Information leaflet for women with an increased lifetime risk of breast and ovarian cancer Hereditary Breast and Ovarian Cancer (HBOC) What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast
Information leaflet for women with an increased lifetime risk of breast and ovarian cancer Hereditary Breast and Ovarian Cancer (HBOC) What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast
Better Outcomes for Lung Cancer in Family Practice. AProf Jeff Garrett Respiratory Physician
 Better Outcomes for Lung Cancer in Family Practice AProf Jeff Garrett Respiratory Physician Lung Cancer Leading cause of cancer death in NZ overall Maori have especially poor lung cancer outcomes 19% cancer
Better Outcomes for Lung Cancer in Family Practice AProf Jeff Garrett Respiratory Physician Lung Cancer Leading cause of cancer death in NZ overall Maori have especially poor lung cancer outcomes 19% cancer
Single Suspected Cancer Pathway Definitions pathway start date
 Single Suspected Cancer Pathway Definitions pathway start date Date: March 2018 Version: 1.2.1 Wales Cancer Owner: Network and Welsh Government Status Published 1 P a g e Purpose of Document This document
Single Suspected Cancer Pathway Definitions pathway start date Date: March 2018 Version: 1.2.1 Wales Cancer Owner: Network and Welsh Government Status Published 1 P a g e Purpose of Document This document
Information Pack for GP s The implementation of the Faecal Immunochemical Test (FIT) across the South West
 Information Pack for GP s The implementation of the Faecal Immunochemical Test (FIT) across the South West The South West Cancer Alliances have been awarded transformation funding to provide access to
Information Pack for GP s The implementation of the Faecal Immunochemical Test (FIT) across the South West The South West Cancer Alliances have been awarded transformation funding to provide access to
FIT for symptomatic patients. Facilitator name
 FIT for symptomatic patients Facilitator name Context colorectal cancer Colorectal cancer in the UK 41,804 new cases in 2015 15,903 deaths in 2014 Fourth most common cancer Second most common cause of
FIT for symptomatic patients Facilitator name Context colorectal cancer Colorectal cancer in the UK 41,804 new cases in 2015 15,903 deaths in 2014 Fourth most common cancer Second most common cause of
Alabama Breast and Cervical Cancer Early Detection Program (ABCCEDP) County Health Department Protocol
 Alabama Breast and Cervical Cancer Early Detection Program (ABCCEDP) County Health Department Protocol BREAST AND CERVICAL CANCER TABLE OF CONTENTS ABCCEDP Overview and Purpose... 1 Clinical Guidelines...
Alabama Breast and Cervical Cancer Early Detection Program (ABCCEDP) County Health Department Protocol BREAST AND CERVICAL CANCER TABLE OF CONTENTS ABCCEDP Overview and Purpose... 1 Clinical Guidelines...
Menopause and Cancer risk; What to do overcome the risks? Fatih DURMUŞOĞLU,M.D
 Menopause and Cancer risk; What to do overcome the risks? Fatih DURMUŞOĞLU,M.D Menopause and Cancer How does menopause affect a woman s cancer risk? Ø Menopause does not cause cancer.but risk of developing
Menopause and Cancer risk; What to do overcome the risks? Fatih DURMUŞOĞLU,M.D Menopause and Cancer How does menopause affect a woman s cancer risk? Ø Menopause does not cause cancer.but risk of developing
Governing Body (Public) Meeting
 ENCLOSURE: T Agenda Item: 86/13 Governing Body (Public) Meeting DATE: 25 July 2013 Title Recommended action for the Governing Body Expanding the Treatment Access Policy for Bexley That the Governing Body:
ENCLOSURE: T Agenda Item: 86/13 Governing Body (Public) Meeting DATE: 25 July 2013 Title Recommended action for the Governing Body Expanding the Treatment Access Policy for Bexley That the Governing Body:
Cancer is the single name assigned to more than 100 diseases that can occur in any part of body
 Cancer is the single name assigned to more than 100 diseases that can occur in any part of body It s actually the result of abnormal cells that multiply and spread out of control, damaging healthy cells
Cancer is the single name assigned to more than 100 diseases that can occur in any part of body It s actually the result of abnormal cells that multiply and spread out of control, damaging healthy cells
This is the portion of the intestine which lies between the small intestine and the outlet (Anus).
 THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
THE COLON This is the portion of the intestine which lies between the small intestine and the outlet (Anus). 3 4 5 This part is responsible for formation of stool. The large intestine (colon- coloured
Program Guidelines Clinical Guidelines Patient Enrollment Resource Documents Eligibility Guidelines... 2
 BREAST AND CERVICAL CANCER TABLE OF CONTENTS Program Guidelines... 1 Clinical Guidelines... 1 Patient Enrollment... 1 Resource Documents... 1 Eligibility Guidelines... 2 Breast Screening Guidelines and
BREAST AND CERVICAL CANCER TABLE OF CONTENTS Program Guidelines... 1 Clinical Guidelines... 1 Patient Enrollment... 1 Resource Documents... 1 Eligibility Guidelines... 2 Breast Screening Guidelines and
East Kent Summary Guidance suspected cancer referrals and notes GP reference document May 2018
 East Kent Summary Guidance suspected cancer referrals and notes GP reference document May 2018 GP INTIATIED DIAGNOSITCS USS Gall Bladder or Liver Fast-track ultrasound to assess for gall bladder or liver
East Kent Summary Guidance suspected cancer referrals and notes GP reference document May 2018 GP INTIATIED DIAGNOSITCS USS Gall Bladder or Liver Fast-track ultrasound to assess for gall bladder or liver
Colon, or Colorectal, Cancer Information
 Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
Colon, or Colorectal, Cancer Information Definition Colon, or colorectal, cancer is cancer that starts in the large intestine (colon) or the rectum (end of the colon). Other types of cancer can affect
Cancer in Women. Lung cancer. Breast cancer
 Cancer in Women You can get cancer at any age, but it is more likely as you get older. The types of cancer people get and the risk of dying from cancer are not the same for all ethnic groups. Here are
Cancer in Women You can get cancer at any age, but it is more likely as you get older. The types of cancer people get and the risk of dying from cancer are not the same for all ethnic groups. Here are
Guideline scope Diverticular disease: diagnosis and management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Diverticular disease: diagnosis and management The Department of Health in England has asked NICE to develop a clinical guideline on diverticular
SIGN. Management of breast cancer in women. December Scottish Intercollegiate Guidelines Network. A national clinical guideline
 SIGN Scottish Intercollegiate Guidelines Network 84 Management of breast cancer in women A national clinical guideline 1 Introduction 1 2 Diagnosis, referral and investigation 2 3 Surgery 7 4 Radiotherapy
SIGN Scottish Intercollegiate Guidelines Network 84 Management of breast cancer in women A national clinical guideline 1 Introduction 1 2 Diagnosis, referral and investigation 2 3 Surgery 7 4 Radiotherapy
PATHWAY FOR INVESTIGATION OF ADULTS PRESENTING WITH ASCITES. U/S Abdo/pelvis shows ascites without obvious evidence of 1 liver disease
 PATHWAY FOR INVESTIGATION OF ADULTS PRESENTING WITH ASCITES U/S Abdo/pelvis shows ascites without obvious evidence of 1 liver disease Refer back to original requester with this paperwork and review previous
PATHWAY FOR INVESTIGATION OF ADULTS PRESENTING WITH ASCITES U/S Abdo/pelvis shows ascites without obvious evidence of 1 liver disease Refer back to original requester with this paperwork and review previous
Cancer Care Kenya Notes for General Practioners:
 Cancer Care Kenya Notes for General Practioners: Site specific symptoms for detecting cancers at an early stage is given below. Please refer patients for detailed work up. 1. Brain /CNS tumors: Sub acute
Cancer Care Kenya Notes for General Practioners: Site specific symptoms for detecting cancers at an early stage is given below. Please refer patients for detailed work up. 1. Brain /CNS tumors: Sub acute
Pathway Gynaecology Cancer & Diagnostic Protocol for Inter Trust transfer
 NICaN Pathway Gynaecology Cancer & Diagnostic Protocol for Inter Trust transfer Timed schedules to enable the proactive management of the patient from point of receipt of referral to first definitive treatment
NICaN Pathway Gynaecology Cancer & Diagnostic Protocol for Inter Trust transfer Timed schedules to enable the proactive management of the patient from point of receipt of referral to first definitive treatment
Cancer of Unknown Primary (CUP) Protocol
 1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
1 Department of Oncology. Cancer of Unknown Primary (CUP) Protocol Version: Document type: Document sponsor Designation Document author [ s] Designation[s] Approving committee / Group Ratified by: Date
Single Suspected Cancer Pathway Definitions pathway start date
 Single Suspected Cancer Pathway Definitions pathway start date Date: December 2018 Version: 8.0 Wales Cancer Owner: Network and Welsh Government Status Draft 1 P a g e Purpose of Document This document
Single Suspected Cancer Pathway Definitions pathway start date Date: December 2018 Version: 8.0 Wales Cancer Owner: Network and Welsh Government Status Draft 1 P a g e Purpose of Document This document
Information leaflet for women with a slightly increased risk of breast cancer. Breast cancer in the family
 Information leaflet for women with a slightly increased risk of breast cancer Breast cancer in the family Breast cancer in the family what does this mean? Breast cancer is the most common cancer affecting
Information leaflet for women with a slightly increased risk of breast cancer Breast cancer in the family Breast cancer in the family what does this mean? Breast cancer is the most common cancer affecting
Clinical Guidelines for the Management of Breast Cancer West Midlands Expert Advisory Group for Breast Cancer
 Clinical Guidelines for the Management of Breast Cancer West Midlands Expert Advisory Group for Breast Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory
Clinical Guidelines for the Management of Breast Cancer West Midlands Expert Advisory Group for Breast Cancer West Midlands Clinical Networks and Clinical Senate Coversheet for Network Expert Advisory
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer
 Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
Wellness Along the Cancer Journey: Healthy Habits and Cancer Screening Revised October 2015 Chapter 7: Cancer Screening and Early Detection of Cancer Healthy Habits and Cancer Screening Rev 10.20.15 Page
A patient s guide to understanding. Cancer. Screening
 A patient s guide to understanding Cancer Screening Contents 04 06 10 12 Cancer Screening Who Should Go For Cancer Screening 05 Nasopharyngeal Carcinoma Colorectal Cancer 08 Lung Cancer Liver Cancer Breast
A patient s guide to understanding Cancer Screening Contents 04 06 10 12 Cancer Screening Who Should Go For Cancer Screening 05 Nasopharyngeal Carcinoma Colorectal Cancer 08 Lung Cancer Liver Cancer Breast
Recognition and Referral of Suspected Cancer - NICE guidance and local initiatives
 Recognition and Referral of Suspected Cancer - NICE guidance and local initiatives Dr. Louise Merriman GP Clinical Lead for South Yorkshire, Bassetlaw and Derbyshire Cancer Alliance Topics to be covered
Recognition and Referral of Suspected Cancer - NICE guidance and local initiatives Dr. Louise Merriman GP Clinical Lead for South Yorkshire, Bassetlaw and Derbyshire Cancer Alliance Topics to be covered
Philippine Cancer Society Forum: Cancer can be cured!
 Philippine Cancer Society Forum: Cancer can be cured! Throughout history, doctors and scientists have extensively studied Their researchers have not only yielded a wealth of information on the disease,
Philippine Cancer Society Forum: Cancer can be cured! Throughout history, doctors and scientists have extensively studied Their researchers have not only yielded a wealth of information on the disease,
Page 1. Selected Controversies. Cancer Screening! Selected Controversies. Breast Cancer Screening. ! Using Best Evidence to Guide Practice!
 Cancer Screening!! Using Best Evidence to Guide Practice! Judith M.E. Walsh, MD, MPH! Division of General Internal Medicine! Womenʼs Health Center of Excellence University of California, San Francisco!
Cancer Screening!! Using Best Evidence to Guide Practice! Judith M.E. Walsh, MD, MPH! Division of General Internal Medicine! Womenʼs Health Center of Excellence University of California, San Francisco!
Telephone: Learning objectives
 BreastScreen WA Breast Cancer Screening Investigation of a New Breast Symptom Dr Eric Khong, Liaison GP Telephone: 13 20 50 Learning objectives Increased understanding of the availability, benefits and
BreastScreen WA Breast Cancer Screening Investigation of a New Breast Symptom Dr Eric Khong, Liaison GP Telephone: 13 20 50 Learning objectives Increased understanding of the availability, benefits and
CA125 in the diagnosis of ovarian cancer: the art in medicine
 CA125 in the diagnosis of ovarian cancer: the art in medicine Dr Marcia Hall Consultant Medical Oncology Mount Vernon Cancer Centre Hillingdon Hospital Wexham Park Hospital Epidemiology Ovarian cancer
CA125 in the diagnosis of ovarian cancer: the art in medicine Dr Marcia Hall Consultant Medical Oncology Mount Vernon Cancer Centre Hillingdon Hospital Wexham Park Hospital Epidemiology Ovarian cancer
Cancer of Unknown Primary Service
 Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
Cancer of Unknown Primary Service Dr Maurice Fernando Consultant In Specialist Palliative Care and CUP lead Doncaster and Bassetlaw Hospitals NHS FT Wakefield meeting -14-07-2016 CUP service CUP MDT
Caring for a Patient with Colorectal Cancer. Objectives. Poll question. UNC Cancer Network Presented on 10/15/18. For Educational Use Only 1
 Caring for a Patient with Colorectal Cancer Tammy Triglianos RN, APRN-BC, AOCNP Nurse Practitioner, GI Oncology 10/15/2018 Objectives Describe common signs and symptoms of colorectal cancer Understand
Caring for a Patient with Colorectal Cancer Tammy Triglianos RN, APRN-BC, AOCNP Nurse Practitioner, GI Oncology 10/15/2018 Objectives Describe common signs and symptoms of colorectal cancer Understand
Cancer: NICE (symptom based)- what s new November 2016
 Cancer: NICE (symptom based)- what s new November 2016 Dr Katy Gardner, Dr Cathy Hubbert, Macmillan GP Cancer Leads, Liverpool CCG See stalls for more information and local pathways (Cheshire & Merseyside)
Cancer: NICE (symptom based)- what s new November 2016 Dr Katy Gardner, Dr Cathy Hubbert, Macmillan GP Cancer Leads, Liverpool CCG See stalls for more information and local pathways (Cheshire & Merseyside)
Cancer Facts for People Over 50
 National Institute on Aging AgePage Cancer Facts for People Over 50 Cancer strikes people of all ages, but you are more likely to get cancer as you get older, even if no one in your family has ever had
National Institute on Aging AgePage Cancer Facts for People Over 50 Cancer strikes people of all ages, but you are more likely to get cancer as you get older, even if no one in your family has ever had
CANCER. Mrs. Davis Health Education
 CANCER Mrs. Davis Health Education Cancer Terms: Tumors: Masses of useless tissue Benign: Non-cancerous Malignant: Cancerous Metastasis: Spread of cancer from the point where it originated to other parts
CANCER Mrs. Davis Health Education Cancer Terms: Tumors: Masses of useless tissue Benign: Non-cancerous Malignant: Cancerous Metastasis: Spread of cancer from the point where it originated to other parts
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
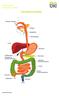 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
National Breast Cancer Audit next steps. Martin Lee
 National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
Bronchiectasis in Adults - Suspected
 Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Bronchiectasis in Adults - Suspected Clinical symptoms which may indicate bronchiectasis for patients Take full respiratory history including presenting symptoms, past medical & family history Factors
Advice about familial aspects of breast cancer and epithelial ovarian cancer
 Advice about familial aspects of breast cancer and epithelial ovarian cancer a guide for health professionals FEBRUARY 2006 These guidelines contain three parts: 1. Information for health professionals
Advice about familial aspects of breast cancer and epithelial ovarian cancer a guide for health professionals FEBRUARY 2006 These guidelines contain three parts: 1. Information for health professionals
Name: Date: Referring Provider: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary).
 Name: Date: Referring Provider: Age: D.O.B. Race/ ethnicity: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary). We are interested in learning
Name: Date: Referring Provider: Age: D.O.B. Race/ ethnicity: What is the nature of your current gynecologic or urologic medical problem (use the other side if necessary). We are interested in learning
Gynaecology Cancer Red Flags. Dr Dina Bisson Consultant Obstetrician and Gynaecologist Southmead Hospital North Bristol NHS Trust 27 April 2017
 Gynaecology Cancer Red Flags Dr Dina Bisson Consultant Obstetrician and Gynaecologist Southmead Hospital North Bristol NHS Trust 27 April 2017 Gynaecological Cancers Endometrial Cancer Ovarian Cancer Cervical
Gynaecology Cancer Red Flags Dr Dina Bisson Consultant Obstetrician and Gynaecologist Southmead Hospital North Bristol NHS Trust 27 April 2017 Gynaecological Cancers Endometrial Cancer Ovarian Cancer Cervical
Guideline Ulcerative colitis: management
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Ulcerative colitis: management Draft for consultation, December 0 This guideline covers the care and treatment of adults, children and young
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline Ulcerative colitis: management Draft for consultation, December 0 This guideline covers the care and treatment of adults, children and young
Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families
 Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast and Ovarian Cancer is a genetic condition which
Hereditary Breast and Ovarian Cancer (HBOC) Information for individuals and families What is Hereditary Breast and Ovarian Cancer (HBOC)? Hereditary Breast and Ovarian Cancer is a genetic condition which
There are a number of national guidelines and performance standards which support the implementation of a straight to CT pathway.
 December 2015 CONTENTS Contents... 2 1 Introduction... 3 2 Case for Change... 3 3 Evidence... 3 3.1 National and regional policy... 3 3.2 Local audit... 4 4 Supporting Work Initiatives... 5 4.1 Identification
December 2015 CONTENTS Contents... 2 1 Introduction... 3 2 Case for Change... 3 3 Evidence... 3 3.1 National and regional policy... 3 3.2 Local audit... 4 4 Supporting Work Initiatives... 5 4.1 Identification
Breast Cancer Screening and Treatment Mrs Belinda Scott Breast Surgeon Breast Associates Auckland
 Breast Cancer Screening and Treatment 2009 Mrs Belinda Scott Breast Surgeon Breast Associates Auckland BREAST CANCER THE PROBLEM 1.1 million women per year 410,000 deaths each year Increasing incidence
Breast Cancer Screening and Treatment 2009 Mrs Belinda Scott Breast Surgeon Breast Associates Auckland BREAST CANCER THE PROBLEM 1.1 million women per year 410,000 deaths each year Increasing incidence
Advice Statement. Advice Statement November Advice for NHSScotland. Why is SHTG looking at this topic?
 Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
FAQ-Protocol 3. BRCA mutation carrier guidelines Frequently asked questions
 ULast updated: 09/02/2015 Protocol 3 BRCA mutation carrier guidelines Frequently asked questions UQ: How accurate are the remaining lifetime and 5 year breast cancer risks in the table? These figures are
ULast updated: 09/02/2015 Protocol 3 BRCA mutation carrier guidelines Frequently asked questions UQ: How accurate are the remaining lifetime and 5 year breast cancer risks in the table? These figures are
3 Summary of clinical applications and limitations of measurements
 CA125 (serum) 1 Name and description of analyte 1.1 Name of analyte Cancer Antigen 125 (CA125) 1.2 Alternative names Mucin-16 1.3 NLMC code To follow 1.4 Description of analyte CA125 is an antigenic determinant
CA125 (serum) 1 Name and description of analyte 1.1 Name of analyte Cancer Antigen 125 (CA125) 1.2 Alternative names Mucin-16 1.3 NLMC code To follow 1.4 Description of analyte CA125 is an antigenic determinant
Cancer Facts for Women
 Cancer Facts for Women Some of the cancers that most often affect women are breast, colorectal, endometrial, lung, cervical, skin, and ovarian cancers. Knowing about these cancers and what you can do to
Cancer Facts for Women Some of the cancers that most often affect women are breast, colorectal, endometrial, lung, cervical, skin, and ovarian cancers. Knowing about these cancers and what you can do to
Cancer Screenings and Early Diagnostics
 Cancer Screenings and Early Diagnostics Ankur R. Parikh, D.O. Medical Director, Center for Advanced Individual Medicine Hematologist/Medical Oncologist Atlantic Regional Osteopathic Convention April 6
Cancer Screenings and Early Diagnostics Ankur R. Parikh, D.O. Medical Director, Center for Advanced Individual Medicine Hematologist/Medical Oncologist Atlantic Regional Osteopathic Convention April 6
Lung Cancer and the Cancer Alliance DR JAMES RAMSAY
 Lung Cancer and the Cancer Alliance DR JAMES RAMSAY Background Lung cancer is the second commonest cancer in the UK (37,000 new cases in England each year). Commonest cause of cancer death (28,500 people
Lung Cancer and the Cancer Alliance DR JAMES RAMSAY Background Lung cancer is the second commonest cancer in the UK (37,000 new cases in England each year). Commonest cause of cancer death (28,500 people
This information explains the advice about suspected cancer that is set out in NICE guideline NG12.
 Recognising, investigating and referring people with symptoms of suspected cancer Information for the public Published: 25 June 2015 nice.org.uk About this information NICE guidelines provide advice on
Recognising, investigating and referring people with symptoms of suspected cancer Information for the public Published: 25 June 2015 nice.org.uk About this information NICE guidelines provide advice on
Days. Visits, Tests and Procedures
 01 02 03 04 05 06 07 08 09 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 57 58 59 60 SURGICAL, MED ONC OR
01 02 03 04 05 06 07 08 09 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 47 48 49 50 51 52 53 54 55 56 57 58 59 60 SURGICAL, MED ONC OR
BREAST HEALTH: WHAT IS NORMAL?
 BREAST HEALTH: WHAT IS NORMAL? BREAST HEALTH Breast health is an important part of overall health and well-being. To keep your breasts as healthy as possible: 1 1. Be breast aware 2. Be informed 3. Make
BREAST HEALTH: WHAT IS NORMAL? BREAST HEALTH Breast health is an important part of overall health and well-being. To keep your breasts as healthy as possible: 1 1. Be breast aware 2. Be informed 3. Make
Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122
 Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Ovarian cancer: recognition and initial management Clinical guideline Published: 27 April 2011 nice.org.uk/guidance/cg122 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Breast Evaluation & Management Guidelines
 Breast Evaluation & Management Guidelines Pamela L. Kurtzhals, M.D. F.A.C.S. Head, Dept. of General Surgery Scripps Clinic, La Jolla Objective Review screening & diagnostic guidelines Focused patient complaints
Breast Evaluation & Management Guidelines Pamela L. Kurtzhals, M.D. F.A.C.S. Head, Dept. of General Surgery Scripps Clinic, La Jolla Objective Review screening & diagnostic guidelines Focused patient complaints
Identifying distinguishing features of the MDC model within the five ACE projects
 Identifying distinguishing features of the MDC model within the five ACE projects Context: The ACE Programme (Wave 2) has been working with five projects across England to trial and evaluate the concept
Identifying distinguishing features of the MDC model within the five ACE projects Context: The ACE Programme (Wave 2) has been working with five projects across England to trial and evaluate the concept
Greater Manchester Commissioning Hub: Cancer Programme. The ACE Programme. Wave 2 Multidisciplinary Diagnostic Centres
 Greater Manchester Commissioning Hub: Cancer Programme The ACE Programme Wave 2 Multidisciplinary Diagnostic Centres Background / Context GM Pilot focuses on 2 areas of Greater Manchester: Oldham South
Greater Manchester Commissioning Hub: Cancer Programme The ACE Programme Wave 2 Multidisciplinary Diagnostic Centres Background / Context GM Pilot focuses on 2 areas of Greater Manchester: Oldham South
The London Gastroenterology Partnership CROHN S DISEASE
 CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
CROHN S DISEASE What is Crohn s disease? Crohn s disease is a condition, in which inflammation develops in parts of the gut leading to symptoms such as diarrhoea, abdominal pain and tiredness. The inflammation
Cervical Cancer - Suspected
 Cervical Cancer - Suspected Presentation for patients Asymptomatic presentation Symptomatic presentation History and examination Consider differential diagnoses RED FLAG! Cervix appears normal after examination
Cervical Cancer - Suspected Presentation for patients Asymptomatic presentation Symptomatic presentation History and examination Consider differential diagnoses RED FLAG! Cervix appears normal after examination
The Virtual Lung Nodule Clinic
 The Virtual Lung Nodule Clinic Poster No.: C-1023 Congress: ECR 2016 Type: Educational Exhibit Authors: S. Higgins, F. C. Lyall, J. Taylor, J. goldman, S. Rolin, B. 1 2 1 2 2 3 2 2 3 Soar ; Torbay/UK,
The Virtual Lung Nodule Clinic Poster No.: C-1023 Congress: ECR 2016 Type: Educational Exhibit Authors: S. Higgins, F. C. Lyall, J. Taylor, J. goldman, S. Rolin, B. 1 2 1 2 2 3 2 2 3 Soar ; Torbay/UK,
The London BreasT CenTre
 The London Breast Centre Contents Introduction 4 One-Stop Breast Care Clinic 5 Common breast problems 6 Hereditary breast cancer 8 Breast cancer and cancer screening 9 Breast diagnostic tests 10 Breast
The London Breast Centre Contents Introduction 4 One-Stop Breast Care Clinic 5 Common breast problems 6 Hereditary breast cancer 8 Breast cancer and cancer screening 9 Breast diagnostic tests 10 Breast
Clinical Biochemistry Department City Hospital
 Cancer Biochemistry and Tumour Markers Clinical Biochemistry Department City Hospital In this lecture Cancer basics Definition of Tumour Marker (TM) What is the perfect TM? History of TMs Examples of TMs
Cancer Biochemistry and Tumour Markers Clinical Biochemistry Department City Hospital In this lecture Cancer basics Definition of Tumour Marker (TM) What is the perfect TM? History of TMs Examples of TMs
Prostate Cancer THE BIG 5 CANCERS AFFECTING MEN IN SA IT IS ESTIMATED THAT 1 IN 19 SOUTH AFRICAN MEN WILL DEVELOP PROSTATE CANCER SYMPTOMS SCREENING
 #1 Prostate Cancer IT IS ESTIMATED THAT 1 IN 19 SOUTH AFRICAN MEN WILL DEVELOP PROSTATE CANCER Prostate cancer often occurs without any symptoms Symptoms more likely if advanced: Frequent urination, esp
#1 Prostate Cancer IT IS ESTIMATED THAT 1 IN 19 SOUTH AFRICAN MEN WILL DEVELOP PROSTATE CANCER Prostate cancer often occurs without any symptoms Symptoms more likely if advanced: Frequent urination, esp
Cancer Genetics Services in Scotland
 abcdefghijklm Cancer Genetics Services in Scotland Guidance to support the Implementation of Genetics Services for Breast, Ovarian and Colorectal Cancer Predisposition Scottish Cancer Group Cancer Genetics
abcdefghijklm Cancer Genetics Services in Scotland Guidance to support the Implementation of Genetics Services for Breast, Ovarian and Colorectal Cancer Predisposition Scottish Cancer Group Cancer Genetics
Detecting and Treating Breast Problems
 WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Detecting and Treating Breast Problems A woman's breasts are always changing. They change during the menstrual cycle, pregnancy, breastfeeding,
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Detecting and Treating Breast Problems A woman's breasts are always changing. They change during the menstrual cycle, pregnancy, breastfeeding,
Gynaecological cancers. Mr Vivek Nama MD MRCOG Consultant Gynaecological Oncologist
 Gynaecological cancers Mr Vivek Nama MD MRCOG Consultant Gynaecological Oncologist Gynaecological cancers Why do we need 2 week wait? Early/timely diagnosis of cancer Possibly less invasive treatment and
Gynaecological cancers Mr Vivek Nama MD MRCOG Consultant Gynaecological Oncologist Gynaecological cancers Why do we need 2 week wait? Early/timely diagnosis of cancer Possibly less invasive treatment and
Trust Guideline for the inclusion of women at High Risk of Breast Cancer in the NHS Breast Screening Programme
 Trust Guideline for the inclusion of women at High Risk of Breast Cancer in the NHS Breast Screening Programme For Use in: By: For: Division responsible for document: Key words: Name and job title of document
Trust Guideline for the inclusion of women at High Risk of Breast Cancer in the NHS Breast Screening Programme For Use in: By: For: Division responsible for document: Key words: Name and job title of document
