Photodynamic Therapy for High Grade Esophageal Dysplasia. California Technology Assessment Forum
|
|
|
- Nickolas Hunt
- 5 years ago
- Views:
Transcription
1 TITLE: AUTHOR: PUBLISHER NAME: Photodynamic Therapy for High Grade Esophageal Dysplasia Jeffrey A. Tice, M.D. Assistant Adjunct Professor of Medicine Division of General Internal Medicine Department of Medicine University of California San Francisco California Technology Assessment Forum DATE OF PUBLICATION: June 15, 2005 PLACE OF PUBLICATION: San Francisco, CA 1
2 PHOTODYNAMIC THERAPY FOR HIGH GRADE ESOPHAGEAL DYSPLASIA INTRODUCTION The California Technology Assessment Forum has been asked to review the scientific literature on the safety and efficacy of photodynamic therapy (PDT) for the treatment of high-grade dysplasia in Barrett s esophagus. This review will focus on the use of porfimer sodium, as it is the only photosensitizer currently approved by the Food and Drug Administration. BACKGROUND Barrett s Esophagus and Dysplasia Barrett s esophagus describes the condition in which the normal squamous epithelium lining the esophagus is replaced by columnar epithelium that is similar to the lining of the intestines. It is thought to reflect the response of the body to recurrent exposure to acidic fluid moving from the stomach into the esophagus (gastroesophageal reflux disease (GERD)). In some people, there are further cellular changes (dysplasia) progressing eventually to adenocarcinoma. Esophageal adenocarcinoma is increasing in incidence faster than any other cancer in the U.S. (Blot et al., 1991). Prospective studies suggest that the annual risk of cancer for patients with Barrett s esophagus lies between 0.5 and 1% (Drewitz et al., 1997; Shaheen et al., 2000). The length of the abnormal mucosa and the degree of dysplasia are the primary risk factors for development of cancer (Pacifico et al., 2002). High-grade dysplasia (HGD) is the stage immediately preceding cancer. A larger proportion of patients with HGD progress on to cancer, although some lesions regress over time. Estimates of the annual incidence of cancer for patients with HGD range from as low as 2%(Schnell et al., 2001) to as high as 62% (Hameeteman et al., 1989). All of the studies are relatively small (n<100) and have short follow-up. Most estimates from the larger studies cluster near the low end of the range (4-10% per year). It is not possible to predict which cases of HGD will progress to cancer and which cases will not. However, it is clear that a large proportion of patients with HGD will have occult cancer. Pathologists find cancer in up to 57% of specimens from patients with HGD who undergo esophageal resection (Collard, 2002; Dar et al., 2003). Esophageal Resection as Primary Therapy A recent study evaluated the mortality associated with esophagectomy in the U.S. (Dimick et al., 2005). The study evaluated 8,657 esophageal resections from 1988 to 2000 captured by the Nationwide Inpatient Sample, a 20% random sample of all hospital discharges in the U.S. The overall in-hospital mortality rate was 11.3%. This tended to go down over time (13.6% to 10.5%) and was lowest at high volume hospitals (11.0% decreasing to 7.5%). 2
3 Esophageal resection is also associated with considerable morbidity (Lerut et al., 2004). In several large studies, 30 to 50% of patients experienced at least one serious post-operative complication (pneumonia, myocardial infarction, heart failure or wound infection) and the average hospital stay was at least two weeks. Late complications are also common. Stenosis at the site of anastomosis is relatively common, occurring in 10% to 56% of cases in the literature (Orringer et al., 2000), and it usually requires approximately four follow-up endoscopies with dilation for treatment. Severe reflux has been reported in 21% (De Leyn et al., 1992) to 58% (Shibuya et al., 2003) of patients often leading to recurrent Barrett s in the esophageal remnant. The surgical procedure usually requires transection of the vagus nerve and a reduction in the size of the stomach in order to connect the gastrointestinal tract with the esophageal remnant. This can lead to a variety of motility disorders including delayed gastric emptying or dumping syndrome. Finally, the recurrent nerve is damaged in up to 22% of cases (Hulscher et al., 1999) causing vocal cord paralysis which increases the risk of aspiration pneumonia. Given the high morbidity and mortality associated with esophageal resection, there is tremendous motivation to develop a less invasive treatment for HGD. Alternative therapies include laser ablation, endoscopic mucosal resection and PDT. Photodynamic Therapy PDT combines a photosensitizer that tends to accumulate in dysplastic or malignant cells with a device that delivers light of a specific wavelength to the target tissue in order to produce cell death (Prosst et al., 2003). The photosensitizing drug is activated by light of a specific wavelength matched to its absorption spectrum. In the presence of oxygen, the activated drug produces oxygen species that are cytotoxic. Thus, cellular damage and tumor necrosis occur via a nonthermal photochemical reaction. Recently, it has been suggested that the immune response and inflammation generated are partly responsible for the therapeutic effect (Oleinick et al., 1998). Mucosal healing and repair occurs over two to three months following treatment. PDT is also called phototherapy, photoradiation therapy, photosensitizing therapy and photochemotherapy. A variety of PDT techniques are reported in the literature including the use of different photosensitizing agents (porfimer sodium, hematoporphyrin derivative, 5-aminolevulinic acid, temoporfin, etc.), different light sources and either fractionated or continuous light applications. Laser irradiation is usually performed 48 to 72 hours after injection of porfimer sodium, although this varies depending on the pharmacokinetics of the drug used (Prosst et al., 2003). The depth of light penetration varies with the wavelength of the light source, but is usually 5-10 mm. Most commonly, a 630-nm visible red laser beam is directed at the target area through a flexible quartz fiber. Generally, PDT delivers therapy with light intensity between 100 and 400 J/cm 2 and a light intensity of 100 mw/cm 2 (Prosst et al., 2003). Treatment is usually performed as an outpatient. Due to the risks of stricture, the maximum extent of disease that is treated in one session is 7 cm. If a larger area needs to be treated, the patient is brought back for a second session. 3
4 Administration of photosensitizing drugs is contraindicated in patients with porphyria. Patients administered the photosensitizing drugs are instructed to avoid direct exposure to sunlight or bright indoor lights for 30 days or longer depending on the drug used. Technology Assessment (TA) TA Criterion 1: The technology must have final approval from the appropriate regulatory bodies. Photofrin PDT (porfimer sodium, Axcan Scandipharm Inc.) was approved by the FDA under section 505(b) on August 4, 2003 for the treatment of precancerous lesions of Barrett s esophagus. On August 1, 2003 the Wizard X-Cell Photodynamic Therapy Balloon with Fiber Optic Diffuser (Axcan scandipharm, Inc.) received FDA PMA approval. This device is to be used with the photosensitive drug Photofrin for the ablation of high-grade dysplasia in Barrett s esophagus patients who do not undergo esophagectomy. TA Criterion 1 is met. TA Criterion 2: The scientific evidence must permit conclusions concerning the effectiveness of the technology regarding health outcomes. The Medline database, Cochrane clinical trials database, Cochrane reviews database, and the Database of Abstracts of Reviews of Effects (DARE) were searched using the key words photodynamic therapy, porfimer, photochemotherapy or photosensitizing agents. These were cross-referenced with the keywords dysplasia and human. The search was performed for the period from 1966 through April The bibliographies of systematic reviews and key articles were manually searched for additional references. Further references were also solicited from the manufacturer, local experts and gastroenterology societies. The abstracts of citations were reviewed for relevance and all potentially relevant articles were reviewed in full. The search identified three uncontrolled case-series (Panjehpour et al., 2000; Overholt et al., 2003b; Wolfsen et al., 2004) describing the outcomes for a total of 265 patients. Each of these studies reported on a mixed population of patients being treated for low-grade dysplasia (n=24), HGD (n=192) and early adenocarcinoma (n=49). There were at least 12 publications identified describing different aspects of these three series (Overholt et al., 1993; Overholt et al., 1995b; Overholt et al., 1995a; Overholt et al., 1997; Overholt et al., 1999; Panjehpour et al., 2000; Wolfsen et al., 2002a; Wolfsen et al., 2002b; Overholt et al., 2003b; Prosst et al., 2003; Wolfsen et al., 2004). It appears that the 60 patients in the clinical trial of prednisone for the prevention of PDT-associated strictures (Panjehpour et al., 2000) were not included in the larger case-series from the same center (Overholt et al., 2003b), so both will be described. One moderate sized randomized trial has been reported in abstract form (Overholt et al. 2003a), but the complete 4
5 results have not been published in a peer-reviewed journal. The published studies were uncontrolled, single center reports without standardized entry criteria and without standardized, independent outcome assessment. The primary outcomes reported are the percentage of patients with Barrett s esophagus and HGD completely eliminated, the incidence of strictures and the incidence of cancer during follow-up. Level of evidence: 5. TA Criterion 2 is not met. TA Criterion 3: The technology must improve net health outcomes. The primary advantage of PDT would be the prevention of the development of esophageal cancer in patients at high risk due to HGD while avoiding the high morbidity and mortality associated with the standard treatment, esophageal resection. Case Series The largest study with the longest follow-up (Overholt et al., 2003b) summarized the results of the treatment of 103 patients, 80 of which were treated for HGD. The remainder of this discussion will focus on the 80 patients with HGD, when possible. Two pathologists confirmed the diagnosis of HGD. All patients received porfimer sodium followed by light therapy delivered by laser using a balloon device to flatten the esophageal mucosa and center the light source. The device attempts to deliver uniform light dosing to minimize the risk for stricture formation. In the entire caseseries, 69 patients were treated with one session of PDT, 29 patients with two sessions and 5 patients with three sessions. All patients were maintained on high dose proton pump inhibitor therapy (omeprazole 20 mg, twice daily). Endoscopy was performed at 3, 6, 9, and 12 months and then annually. If residual Barrett s mucosa was visible on endoscopy more than three months after treatment, it was treated with Nd:YAG laser photoablation. A total of 84 patients required Nd:YAG laser photoablation of residual Barrett s tissue. Average follow-up in the study was 51 months (range months). The mean age of the patients with HGD was 64 years and 80% were male. All patients with EGD required follow-up photoablation with the Nd:YAG laser. Barrett s esophagus was completely eliminated in 54% (43/80) of patients and HGD was eliminated in 78% (62/80). Strictures developed in 30% of patients overall, but were more common in patients undergoing two sessions (50% with strictures) than in those undergoing only one session (18% with strictures). A total of 7.5% (6/80) of patients with HGD were diagnosed with esophageal carcinoma during follow-up. Four of these patients were diagnosed within six months of initial treatment; the remaining two were diagnosed at 46 and 52 months after PDT. Given the widely varying estimates for progression of HGD to cancer, it is not clear whether this represents a decrease from the expected four-year rate of cancer occurrence. 5
6 The second case series (Wolfsen et al., 2004) describes 102 patients (69 with HGD, 33 with cancer) treated with one session of PDT using porfimer sodium. The median age of patients was 72 years and 20% were female. Two pathologists confirmed the diagnosis of HGD. Argon beam laser was used to ablate any residual Barrett s mucosa seen on endoscopies performed at least three months after PDT. Endoscopy was performed every three months for two years following PDT and subsequently every six months. The median follow-up was 19 months (range 6 to 78 months). Barrett s esophagus was completely eliminated in 52% (36/69) of patients with HGD. From an earlier report of the same series with fewer patients, HGD was eliminated in 98% (47/48) (Wolfsen et al., 2002b). One patient (1%) developed metastatic adenocarcinoma. Strictures developed in 22% of patients treated for HGD and required a median of five dilations per patient for treatment. Severe photosensitivity reactions requiring medical treatment (usually oral corticosteroids) developed in 18%. Additional complications included esophageal perforation (1%), atrial fibrillation (1%) and congestive heart failure (1%). Both stricture formation and incomplete ablation of Barrett s mucosa were associated with the length of the diseased segment of the esophagus. The final series (Panjehpour et al., 2000) of 60 patients (48 with HGD) was performed at the same center by the same investigators as the first series using a similar protocol. The study randomized 30 patients to PDT alone (6 patients had two sessions) and 30 patients to PDT plus oral prednisone (4 patients had two sessions, 2 patients had three sessions). Median follow-up was 9.8 months (range 3-18 months). For this review, it can be considered as a third uncontrolled series of patients with HGD treated with PDT. Endoscopies were performed every three to six months to evaluate the response. Residual or recurrent Barrett's was treated using Nd:YAG laser. Barrett s esophagus was completely eliminated in 42% (25/60) of patients and HGD was eliminated in 96% (41/43). Strictures developed in 16% of patients randomized to PDT alone and 29% of patients randomized to PDT plus prednisone. It is clear from the uncontrolled case-series above that PDT combined with follow-up laser thermoablation is effective at eliminating visible HGD in most patients (78-98%) and Barrett s esophagus in about half of patients (42-56%). However, all three studies were uncontrolled and only the first had sufficient follow-up to estimate the efficacy of PDT for preventing the development of esophageal cancer. Controlled studies with longer follow-up are needed. Randomized Clinical Trials One multi-center, randomized clinical trial has been presented in abstract form. Patients with HGD were randomized in a 2:1 ratio to either PDT with porfimer sodium plus omeprazole for acid suppression (n=138) or omeprazole therapy alone (n=70). Patients were followed for a minimum of two years. The abstract suggests that there was a significant difference in the incidence of esophageal adenocarcinoma (10% vs. 30%), but details about the study are limited. 6
7 Risks / Harms Intravenous injection of porfimer sodium is generally well tolerated. Photosensitivity reactions have been reported for up to eight weeks after injection in between 13% (Sibille et al., 1995) and 24%(Cortese et al., 1997) of patients treated for palliation of cancer. Similarly, about one-third of patients treated for HGD reported skin reactions with between 3% (Overholt et al., 2003b) and 18% (Wolfsen et al., 2004) reporting severe photosensitivity reactions requiring medical treatment. Esophageal strictures can occur in up to one-third of patients, although the incidence is closer to 15% for patients who can be treated with a single session of PDT (Sibille et al., 1995; Panjehpour et al., 2000; Wolfsen et al., 2002b; Overholt et al., 2003b). These are usually manageable with dilation (McCaughan et al., 1996). Stenoses appear to be related to the use of circumferential radiation (360 ) of the esophageal wall and can be limited by using a 180 or 240 light distributor (Savary et al., 1998). One randomized trial found no benefit to the use of oral prednisone for the prevention of stenosis (Panjehpour et al., 2000) even though steroids are typically used as an adjunct to dilation when treating stenosis occurring after PDT. Esophageal perforation, candidal esophagitis, pleural effusions and atrial fibrillation were also reported in 3-4% of treated patients. The major long-term concern is that regions of dysplasia greater than 5 to 10 mm in depth remain untreated by PDT. In addition, unsuspected carcinoma that is present in up to 50% of patients with HGD may be inadequately treated. Ideally, randomized clinical trial data would be available comparing PDT to esophageal resection with at least five years of follow-up to assess cancer free survival. Short of that, case series with several years follow-up comparing the outcomes of patients treated with PDT with controls matched on age, sex and extent of disease would allow for a more balanced assessment of the relative risks and benefits of PDT compared with esophagectomy. Cost-effectiveness Analysis At least three cost effectiveness analyses (Hur et al., 2003; Shaheen et al., 2004; Vij et al., 2004) of the use of PDT to treat HGD have been published. All used estimates of efficacy based on results from studies using porfimer sodium as well as studies using alternative agents as the photosensitizing drug. All three analyses concluded that PDT is cost-effective compared with esophagectomy or surveillance. Estimates of the increase in quality-adjusted life years gained compared with esophagectomy ranged from 0.5 to 2.2 and cost-effectiveness ranged from $12,000 to $47,000 per quality-adjusted life year. Based on their analysis, at least one of the authors called for randomized clinical trials to confirm these projected benefits. TA Criterion 3 is not met. 7
8 TA Criterion 4: The technology must be as beneficial as any established alternatives. The primary alternative treatment for HGD is esophagectomy. As noted in the background section, this therapy is associated with high mortality (7-15%) and morbidity (up to 50%). Some centers offer aggressive surveillance with high dose proton pump inhibitor therapy as an alternative with good outcomes (Schnell et al., 2001), but this has been associated with poor outcomes in other studies (Weston et al., 2000; Romagnoli et al., 2003). The complete lack of controlled clinical trials makes it difficult to relate the risks and benefits of PDT compared to either esophageal resection or acid suppressive therapy with regular endoscopy for surveillance. The three case series discussed above appear to have lower rates of cancer diagnosis than would be predicted from what is known about the natural history of HGD, but comparative studies are needed to ensure that this does not simply reflect differences in the natural history of the populations studied. It is likely that patients treated with esophagectomy are different than those treated conservatively, so direct comparisons of the results of these treatments are likely to be biased. TA Criterion 4 is not met. TA Criterion 5: The improvement must be attainable outside of the investigational setting. PDT has been performed successfully at multiple centers in the U.S. and Europe and has been found to meet TA Criteria 1 through 5 when used for palliation of esophageal cancer in an earlier review. However, given that no improvement has clearly been demonstrated in the investigational setting for PDT when treating HGD, no conclusions can be drawn regarding device effectiveness in the community setting. TA Criterion 5 is not met. CONCLUSION In Barrett s esophagus with HGD, uncontrolled trials suggest some efficacy for PDT using porfimer. Unfortunately, the published literature is limited to small, uncontrolled single center case series. In the absence of a single randomized controlled trial, there cannot be a conclusive assessment of the efficacy of PDT. One randomized trial comparing PDT to surveillance plus PPI therapy has been completed, but not yet published. Furthermore, excitement about porfimer sodium is tempered by its long half-life, which leaves patients vulnerable to cutaneous photosensitivity reactions for up to two months, and the relatively high risk of strictures in some case series. Thus, alternative photosensitizing agents are under active investigation. Given the high morbidity and mortality of esophageal resection, PDT would be a welcome alternative if it were demonstrated to be more efficacious than surveillance. No clinical trials have been reported directly comparing PDT to the current standard, esophagectomy. 8
9 DRAFT RECOMMENDATION It is recommended that the use of PDT with porfimer sodium as the photosensitizing agent does not meet Technology Assessment Criteria 2, 3, 4 or 5 for safety, effectiveness and improvement in health outcomes for patients with high-grade esophageal dysplasia. June 15, 2005 The California Technology Assessment Forum panel voted unanimously to accept the recommendation as written. 9
10 RECOMMENDATION OF OTHERS Blue Cross Blue Shield Association (BCBSA) The BCBSA Technology Evaluation Center Medical Advisory Panel has not evaluated the use of this technology for esophageal high-grade dysplasia. Centers for Medicare and Medicaid Services (CMS) The CMS does not have a national coverage determination for Photofrin for use in the treatment of Barrett s esophagus. A few Medicare contractors have developed local coverage determinations for Photofrin use in cancer of the lung and esophagus. Some of these contractors cover Photofrin for its Barrett s labeled indication. American Gastroenterological Association (AGA) American Society of Gastrointestinal Endoscopy (ASGE) A representative of the AGA and ASGE attended the meeting and provided comment supporting the use of this technology. American Cancer Society (ACS) The ACS does not have an opinion on this condition and its treatment. Association of Northern California Oncologists (ANCO) The ANCO does not have an opinion regarding this topic. Medical Oncology Association of Southern California (MOASC) A MOASC representative attended the meeting and provided testimony. American College of Surgeons, California Chapter (ACSCA) The ACS CA chapter has will have a representative at the meeting. California Thoracic Society The CTS has been invited to provide a position statement and representation at the meeting. ABBREVIATIONS USED IN THIS REVIEW GERD: Gastroesophageal Reflux Disease HGD: High-grade Dysplasia PDT: Photodynamic Therapy PPI: Proton Pump Inhibitor 10
11 REFERENCES 1. Blot, W. J., S. S. Devesa, R. W. Kneller, et al. (1991). "Rising incidence of adenocarcinoma of the esophagus and gastric cardia." Jama 265(10): Collard, J. M. (2002). "High-grade dysplasia in Barrett's esophagus. The case for esophagectomy." Chest Surg Clin N Am 12(1): Cortese, D. A., E. S. Edell and J. H. Kinsey (1997). "Photodynamic therapy for early stage squamous cell carcinoma of the lung." Mayo Clin Proc 72(7): Dar, M. S., J. R. Goldblum, T. W. Rice, et al. (2003). "Can extent of high grade dysplasia in Barrett's oesophagus predict the presence of adenocarcinoma at oesophagectomy?" Gut 52(4): De Leyn, P., W. Coosemans and T. Lerut (1992). "Early and late functional results in patients with intrathoracic gastric replacement after oesophagectomy for carcinoma." Eur J Cardiothorac Surg 6(2): 79-84; discussion Dimick, J. B., R. M. Wainess, G. R. Upchurch, Jr., et al. (2005). "National trends in outcomes for esophageal resection." Ann Thorac Surg 79(1): 212-6; discussion Drewitz, D. J., R. E. Sampliner and H. S. Garewal (1997). "The incidence of adenocarcinoma in Barrett's esophagus: a prospective study of 170 patients followed 4.8 years." Am J Gastroenterol 92(2): Hameeteman, W., G. N. Tytgat, H. J. Houthoff, et al. (1989). "Barrett's esophagus: development of dysplasia and adenocarcinoma." Gastroenterology 96(5 Pt 1): Hulscher, J. B., J. W. van Sandick, P. P. Devriese, et al. (1999). "Vocal cord paralysis after subtotal oesophagectomy." Br J Surg 86(12): Hur, C., N. S. Nishioka and G. S. Gazelle (2003). "Cost-effectiveness of photodynamic therapy for treatment of Barrett's esophagus with high grade dysplasia." Dig Dis Sci 48(7): Lerut, T. E. and J. J. van Lanschot (2004). "Chronic symptoms after subtotal or partial oesophagectomy: diagnosis and treatment." Best Pract Res Clin Gastroenterol 18(5): McCaughan, J. S., Jr., E. C. Ellison, J. T. Guy, et al. (1996). "Photodynamic therapy for esophageal malignancy: a prospective twelve-year study." Ann Thorac Surg 62(4): ; discussion Oleinick, N. L. and H. H. Evans (1998). "The photobiology of photodynamic therapy: cellular targets and mechanisms." Radiat Res 150(5 Suppl): S Orringer, M. B., B. Marshall and M. D. Iannettoni (2000). "Eliminating the cervical esophagogastric anastomotic leak with a side-to-side stapled anastomosis." J Thorac Cardiovasc Surg 119(2): Overholt, B., C. J. Lightdale and K. K. Wang (2003a). "International multicenter partially blinded randomized study of the efficacy of photodynamic therapy using porfimer sodium for ablation of high-grade dysplasia in Barrett's esophagus and results of 24 month follow up." Gastroenterology 124(Suppl 1): A Overholt, B., M. Panjehpour, E. Tefftellar, et al. (1993). "Photodynamic therapy for treatment of early adenocarcinoma in Barrett's esophagus." Gastrointest Endosc 39(1): Overholt, B. F. and M. Panjehpour (1995a). "Barrett's esophagus: photodynamic therapy for ablation of dysplasia, reduction of specialized mucosa, and treatment of superficial esophageal cancer." Gastrointest Endosc 42(1):
12 18. Overholt, B. F. and M. Panjehpour (1995b). "Photodynamic therapy in Barrett's esophagus: reduction of specialized mucosa, ablation of dysplasia, and treatment of superficial esophageal cancer." Semin Surg Oncol 11(5): Overholt, B. F., M. Panjehpour and M. Ayres (1997). "Photodynamic therapy for Barrett's esophagus: cardiac effects." Lasers Surg Med 21(4): Overholt, B. F., M. Panjehpour and D. L. Halberg (2003b). "Photodynamic therapy for Barrett's esophagus with dysplasia and/or early stage carcinoma: long-term results." Gastrointest Endosc 58(2): Overholt, B. F., M. Panjehpour and J. M. Haydek (1999). "Photodynamic therapy for Barrett's esophagus: follow-up in 100 patients." Gastrointest Endosc 49(1): Pacifico, R. J. and K. K. Wang (2002). "Nonsurgical management of Barrett's esophagus with high-grade dysplasia." Surg Oncol Clin N Am 11(2): Panjehpour, M., B. F. Overholt, J. M. Haydek, et al. (2000). "Results of photodynamic therapy for ablation of dysplasia and early cancer in Barrett's esophagus and effect of oral steroids on stricture formation." Am J Gastroenterol 95(9): Prosst, R. L., H. C. Wolfsen and J. Gahlen (2003). "Photodynamic therapy for esophageal diseases: a clinical update." Endoscopy 35(12): Romagnoli, R., J. M. Collard, C. Gutschow, et al. (2003). "Outcomes of dysplasia arising in Barrett's esophagus: a dynamic view." J Am Coll Surg 197(3): Savary, J. F., P. Grosjean, P. Monnier, et al. (1998). "Photodynamic therapy of early squamous cell carcinomas of the esophagus: a review of 31 cases." Endoscopy 30(3): Schnell, T. G., S. J. Sontag, G. Chejfec, et al. (2001). "Long-term nonsurgical management of Barrett's esophagus with high-grade dysplasia." Gastroenterology 120(7): Shaheen, N. J., M. A. Crosby, E. M. Bozymski, et al. (2000). "Is there publication bias in the reporting of cancer risk in Barrett's esophagus?" Gastroenterology 119(2): Shaheen, N. J., J. M. Inadomi, B. F. Overholt, et al. (2004). "What is the best management strategy for high grade dysplasia in Barrett's oesophagus? A cost effectiveness analysis." Gut 53(12): Shibuya, S., S. Fukudo, R. Shineha, et al. (2003). "High incidence of reflux esophagitis observed by routine endoscopic examination after gastric pull-up esophagectomy." World J Surg 27(5): Sibille, A., R. Lambert, J. C. Souquet, et al. (1995). "Long-term survival after photodynamic therapy for esophageal cancer." Gastroenterology 108(2): Vij, R., G. Triadafilopoulos, D. K. Owens, et al. (2004). "Cost-effectiveness of photodynamic therapy for high-grade dysplasia in Barrett's esophagus." Gastrointest Endosc 60(5): Weston, A. P., P. Sharma, M. Topalovski, et al. (2000). "Long-term follow-up of Barrett's high-grade dysplasia." Am J Gastroenterol 95(8): Wolfsen, H. C., L. L. Hemminger, M. B. Wallace, et al. (2004). "Clinical experience of patients undergoing photodynamic therapy for Barrett's dysplasia or cancer." Aliment Pharmacol Ther 20(10): Wolfsen, H. C. and C. S. Ng (2002a). "Cutaneous consequences of photodynamic therapy." Cutis 69(2):
13 36. Wolfsen, H. C., T. A. Woodward and M. Raimondo (2002b). "Photodynamic therapy for dysplastic Barrett esophagus and early esophageal adenocarcinoma." Mayo Clin Proc 77(11):
Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia
 ...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
...PRESENTATIONS... Evaluating Treatments of Barrett s Esophagus That Shows High-Grade Dysplasia Based on a presentation by Bergein F. Overholt, MD Presentation Summary Thermal ablation and surgery are
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus
 New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
New Developments in the Endoscopic Diagnosis and Management of Barrett s Esophagus Prateek Sharma, MD Key Clinical Management Points: Endoscopic recognition of a columnar lined distal esophagus is crucial
Endoscopic Management of Barrett s Esophagus
 Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
Endoscopic Management of Barrett s Esophagus Sammy Ho, MD Director of Pancreaticobiliary Services and Endoscopic Ultrasound Montefiore Medical Center Barrett s Esophagus Consequence of chronic GERD Mean
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery
 Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
Joel A. Ricci, MD SUNY Downstate Medical Center Department of Surgery Norman Barrett (1950) described the esophagus as: that part of the foregut, distal to the cricopharyngeal sphincter, which is lined
History. Prevalence at Endoscopy. Prevalence and Reflux Sx. Prevalence at Endoscopy. Barrett s Esophagus: Controversy and Management
 Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Barrett s Esophagus: Controversy and Management History Norman Barrett (1950) Chronic Peptic Ulcer of the Oesophagus and Oesophagitis Allison and Johnstone (1953) The Oesophagus Lined with Gastric Mucous
Gregory G. Ginsberg, M.D.
 Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Radiofrequency Ablation for Barrett s Esophagus with HGD Gregory G. Ginsberg, M.D. Professor of Medicine University of Pennsylvania School of Medicine Abramson Cancer Center Gastroenterology Division Executive
Barrett s esophagus. Barrett s neoplasia treatment trends
 Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Options for endoscopic treatment of Barrett s esophagus Patrick S. Yachimski, MD MPH Director of Pancreatobiliary Endoscopy Assistant Professor of Medicine Division of Gastroenterology, Hepatology & Nutrition
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Is Radiofrequency Ablation Effective In Treating Barrett s Esophagus Patients with High-Grade Dysplasia?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 12-2016 Is Radiofrequency Ablation Effective
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of photodynamic therapy for Barrett s oesophagus Barrett s oesophagus is a condition
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of photodynamic therapy for Barrett s oesophagus Barrett s oesophagus is a condition
Current Management: Role of Radiofrequency Ablation
 Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
Esophageal Adenocarcinoma And Barrett s Esophagus: Current Management: Role of Radiofrequency Ablation Ketan Kulkarni, MD Regional Gastroenterology Associates of Lancaster INTRODUCTION The prognosis of
Achieving Clinically Proven Treatment Results With Photodynamic Therapy (PDT) and PHOTOFRIN (porfimer sodium) for Injection
 Achieving Clinically Proven Treatment Results With Photodynamic Therapy () and PHOTOFRIN (porfimer sodium) for Injection PHOTOFRIN (porfimer sodium) IS INDICATED FOR Palliation of patients with completely
Achieving Clinically Proven Treatment Results With Photodynamic Therapy () and PHOTOFRIN (porfimer sodium) for Injection PHOTOFRIN (porfimer sodium) IS INDICATED FOR Palliation of patients with completely
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD?
 Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Barrett s Esophagus: What to Do for No Dysplasia, LGD, and HGD? Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina 1 Outline What are the risks of progression
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell
 Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
Endoscopic therapy of Barrett s esophagus Oliver Pech and Christian Ell Department of Internal Medicine 2, HSK Wiesbaden, Wiesbaden, Germany Correspondence to Oliver Pech, MD, PhD, Department of Gastroenterology,
Definition of GERD American College of Gastroenterology
 Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
Definition of GERD American College of Gastroenterology GERD is defined as chronic symptoms or mucosal damage produced by the abnormal reflux of gastric contents into the esophagus DeVault et al. Am J
AGA SECTION. Gastroenterology 2016;150:
 Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Gastroenterology 2016;150:1026 1030 April 2016 AGA Section 1027 Procedural intervention (3) Upper endoscopy indications 3 6 Non-response of symptoms to a 4 8 week empiric trial of twice-daily PPI Troublesome
Ablation for Barrett s Esophagus: Burn or Freeze
 Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Ablation for Barrett s Esophagus: Burn or Freeze John R. Saltzman MD Director of Endoscopy Brigham and Women s Hospital Professor of Medicine Harvard Medical School Disclosures No relevant disclosures
Barrett s Esophagus. lining of the lower esophagus that bears his name (i.e., Barrett's esophagus). We now
 Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Barrett s Esophagus. Radiofrequency Ablation with the HALO Technology A Reference Book
 Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Radiofrequency Ablation with the HALO Technology A Reference Book 540 Oakmead Parkway, Sunnyvale, CA 94085 What is Barrett s esophagus? Barrett s esophagus is a change that occurs within the cellular lining
Relative risk of dysplasia for patients with intestinal metaplasia in the distal oesophagus and in the gastric cardia
 Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Gut 2000;46:9 13 9 PAPERS Division of Gastroenterology, University of Kansas, VA Medical Center, Kansas City, Missouri, USA P Sharma A P Weston Department of Pathology, VA Medical Center, Kansas M Topalovski
Present Day Management of Barrett s Esophagus
 Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Slide 1 Present Day Management of Barrett s Esophagus Kinnari R. Kher, M.D. Slide 2 Goals Risk factors for development of Barrett s esophagus Risks for progression to Esophageal Adenocarcinoma Current
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus. Original Policy Date
 MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
MP 2.01.52 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett`s Esophagus Medical Policy Section Medicine Issue 12:2013 Original Policy Date 12:2013 Last Review Status/Date Reviewed with literature
RFA and Cyrotherapy for Esophageal Disease
 RFA and Cyrotherapy for Esophageal Disease Daniel L. Miller MD Chief, General Thoracic Surgery WellStar Healthcare System/ Mayo Clinic Care Network Clinical Professor of Surgery Medical College of Georgia/
RFA and Cyrotherapy for Esophageal Disease Daniel L. Miller MD Chief, General Thoracic Surgery WellStar Healthcare System/ Mayo Clinic Care Network Clinical Professor of Surgery Medical College of Georgia/
Are You Living with Barrett s Esophagus?
 Are You Living with Barrett s Esophagus? Wouldn t you rather live without it? If you re living with Barrett s esophagus you are not alone. Barrett s esophagus is caused by the long-term exposure of your
Are You Living with Barrett s Esophagus? Wouldn t you rather live without it? If you re living with Barrett s esophagus you are not alone. Barrett s esophagus is caused by the long-term exposure of your
Faculty Disclosure. Objectives. State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) 24/11/2014
 State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
Treat Barrett s, Remove the Risk. HALO System
 Treat Barrett s, Remove the Risk HALO System The HALO 360 System Advanced Ablation Technology for Barrett s Esophagus The HALO 360 System is designed to remove the Barrett s epithelium in a short, well-tolerated
Treat Barrett s, Remove the Risk HALO System The HALO 360 System Advanced Ablation Technology for Barrett s Esophagus The HALO 360 System is designed to remove the Barrett s epithelium in a short, well-tolerated
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Management of Barrett s: From Imaging to Resection
 Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
Management of Barrett s: From Imaging to Resection Michael Wallace, MD, MPH, FACG Professor of Medicine Mayo Clinic Florida Goals of Endoscopic Evaluation in Barrett s Detect Barrett s and dysplasia Reduce/eliminate
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett s Esophagus Policy Number: 2.01.80 Last Review: 6/2018 Origination: 6/2012 Next Review: 6/2019 Policy Blue Cross and Blue Shield of Kansas
ALA PDT for high grade dysplasia in Barrett s oesophagus review of a decade s experience
 ALA PDT for high grade dysplasia in Barrett s oesophagus review of a decade s experience Stephen G Bown, Gary D Mackenzie, Jason M Dunn, Sally M Thorpe, Laurence B Lovat National Medical Laser Centre,
ALA PDT for high grade dysplasia in Barrett s oesophagus review of a decade s experience Stephen G Bown, Gary D Mackenzie, Jason M Dunn, Sally M Thorpe, Laurence B Lovat National Medical Laser Centre,
Medicare Advantage Medical Policy
 Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Description/Background Barrett Esophagus and the
Medicare Advantage Medical Policy Current Policy Effective Date: 1/1/18 Title: Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Description/Background Barrett Esophagus and the
Barrett s esophagus (BE), the premalignant condition
 GASTROENTEROLOGY 2009;136:2101 2114 A Cost-Utility Analysis of Ablative Therapy for Barrett s Esophagus JOHN M. INADOMI,*, MA SOMSOUK,*, RYAN D. MADANICK, JENNIFER P. THOMAS, and NICHOLAS J. SHAHEEN *Division
GASTROENTEROLOGY 2009;136:2101 2114 A Cost-Utility Analysis of Ablative Therapy for Barrett s Esophagus JOHN M. INADOMI,*, MA SOMSOUK,*, RYAN D. MADANICK, JENNIFER P. THOMAS, and NICHOLAS J. SHAHEEN *Division
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Policy Number: Original Effective Date: MM.02.005 09/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett Esophagus Policy Number: Original Effective Date: MM.02.005 09/01/2010 Line(s) of Business: Current Effective Date: PPO; HMO; QUEST Integration
Section: Medicine Effective Date: July 15, 2015 Subsection: Original Policy Date: December 7, 2011 Subject:
 Last Review Status/Date: June 2015 Page: 1 of 16 Cryoablation for Barrett s Esophagus Description Barrett s esophagus (BE) is a condition in which the normal squamous epithelium is replaced by specialized
Last Review Status/Date: June 2015 Page: 1 of 16 Cryoablation for Barrett s Esophagus Description Barrett s esophagus (BE) is a condition in which the normal squamous epithelium is replaced by specialized
Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic management of Barrett s esophagus with dysplasia
 UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
UvA-DARE (Digital Academic Repository) Endoscopic management of Barrett s esophagus with dysplasia Phoa, Nadine Link to publication Citation for published version (APA): Phoa, K. Y. N. (2014). Endoscopic
Lasers in Gastroenterology, Otorhinolaryngology & Pulmonology
 Lasers in Gastroenterology, Otorhinolaryngology & Pulmonology Eloise Anguluan Laser-Tissue Interactions Fall Semester 2016 Gastroenterology the branch of medicine which deals with disorders of the stomach
Lasers in Gastroenterology, Otorhinolaryngology & Pulmonology Eloise Anguluan Laser-Tissue Interactions Fall Semester 2016 Gastroenterology the branch of medicine which deals with disorders of the stomach
Endoscopic Therapy of Barrett s Esophagus and Esophageal Adenocarcinoma
 Clinical imaging / therapy Endoscopic Therapy of Barrett s Esophagus and Esophageal Adenocarcinoma Marcel Tantau, Ofelia Mosteanu, Teodora Pop, Alina Tantau, Gabriela Mester University of Medicine and
Clinical imaging / therapy Endoscopic Therapy of Barrett s Esophagus and Esophageal Adenocarcinoma Marcel Tantau, Ofelia Mosteanu, Teodora Pop, Alina Tantau, Gabriela Mester University of Medicine and
5-Aminolevulinic acid photodynamic therapy versus argon plasma coagulation for ablation of Barrett s oesophagus: a randomised trial
 785 OESOPHAGUS 5-Aminolevulinic acid photodynamic therapy versus argon plasma coagulation for ablation of Barrett s oesophagus: a randomised trial M Hage, P D Siersema, H van Dekken, E W Steyerberg, J
785 OESOPHAGUS 5-Aminolevulinic acid photodynamic therapy versus argon plasma coagulation for ablation of Barrett s oesophagus: a randomised trial M Hage, P D Siersema, H van Dekken, E W Steyerberg, J
Barrett s Esophagus: Ablate Everyone?
 Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Nicholas J. Shaheen, MD, MPH, FACG Barrett s Esophagus: Ablate Everyone? Nicholas J. Shaheen, MD, MPH, FACG Center for Esophageal Diseases and Swallowing University of North Carolina Greetings from UNC,
Can erythropoietin treatment during antiviral drug treatment for hepatitis C be cost effective?
 Below Are Selected Good Abstracts from Digestive Disease Week 2006 Meeting Published in Gut. 2006 April; 55(Suppl 2): A1 A119. http://www.ncbi.nlm.nih.gov/pmc/articles/pmc1859999/?tool=pmcentrez Can erythropoietin
Below Are Selected Good Abstracts from Digestive Disease Week 2006 Meeting Published in Gut. 2006 April; 55(Suppl 2): A1 A119. http://www.ncbi.nlm.nih.gov/pmc/articles/pmc1859999/?tool=pmcentrez Can erythropoietin
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018
 MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
MANAGEMENT OF BARRETT S RELATED NEOPLASIA IN 2018 Sachin Wani Medical Director Esophageal and Gastric Center Division of Gastroenterology and Hepatology University of Colorado Anschutz Medical Campus DISCLOSURES
DISCLOSURES. This program meets the requirements for GI specific Category 1 contact hours. M
 DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
DISCLOSURES Educational Dimensions is accredited as a provider of continuing nursing education by the American Nurses Credentialing Center s Commission on Accreditation. Successful completion: Participants
1. Epidemiology of Esophageal Cancer 2. Operative Strategies 3. Minimally Invasive Esophagectomy 4. Video
 Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
Minimally Invasive Esophagectomy Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ESOPHAGEAL
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, by Am. Coll. of Gastroenterology ISSN /02/$22.00
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 1, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(01)03982-X ORIGINAL CONTRIBUTIONS
Esophageal cancer: Biology, natural history, staging and therapeutic options
 EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
EGEUS 2nd Meeting Esophageal cancer: Biology, natural history, staging and therapeutic options Michael Bau Mortensen MD, Ph.D. Associate Professor of Surgery Centre for Surgical Ultrasound, Upper GI Section,
Management of Barrett s Esophagus. Case Presentation
 Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
Management of Barrett s Esophagus Lauren B. Gerson MD, MSc Associate Clinical Professor, UCSF Director of Clinical Research Gastroenterology Fellowship Program California Pacific Medical Center San Francisco,
GERD DIAGNOSIS & TREATMENT DISCLOSURES 4/18/2018
 GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
The normal esophagus is lined with squamous epithelium.
 .. ALAN J. CAMERON, M.D. In Barrett's esophagus, the squamous lining of the lower esophagus is replaced by columnar epithelium. Barrett's esophagus is associated with gastroesophageal reflux and an increased
.. ALAN J. CAMERON, M.D. In Barrett's esophagus, the squamous lining of the lower esophagus is replaced by columnar epithelium. Barrett's esophagus is associated with gastroesophageal reflux and an increased
Sixteen-year follow-up of Barrett s esophagus, endoscopically treated with argon plasma coagulation
 Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
Original Article Sixteen-year of Barrett s esophagus, endoscopically treated with argon plasma coagulation United European Gastroenterology Journal 2014, Vol. 2(5) 367 373! Author(s) 2014 Reprints and
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus
 ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
ACG Clinical Guideline: Diagnosis and Management of Barrett s Esophagus Nicholas J. Shaheen, MD, MPH, FACG 1, Gary W. Falk, MD, MS, FACG 2, Prasad G. Iyer, MD, MSc, FACG 3 and Lauren Gerson, MD, MSc, FACG
Role of Photodynamic Therapy in the Palliation of Obstructing Esophageal Cancer
 original article korean j intern med 2012;27:278-284 pissn 1226-3303 eissn 2005-6648 Role of Photodynamic Therapy in the Palliation of Obstructing Esophageal Cancer Hyeon Young Yoon, Young Koog Cheon,
original article korean j intern med 2012;27:278-284 pissn 1226-3303 eissn 2005-6648 Role of Photodynamic Therapy in the Palliation of Obstructing Esophageal Cancer Hyeon Young Yoon, Young Koog Cheon,
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Learning Objectives:
 Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Crescent City GI Update 2018 Ochsner Clinic, NOLA Optimizing Endoscopic Evaluation of Barrett s Esophagus What Should I Do in My Practice? Gregory G. Ginsberg, M.D. Professor of Medicine University of
Slide 1. Slide 2. Slide 3 DISCLOSURES EXPECTED OUTCOMES DIAGNOSIS AND TREATMENT
 Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
Slide 1 DIAGNOSIS AND TREATMENT 1 Slide 2 DISCLOSURES Successful completion: Participants must attend the entire program, including any resulting Q & A, and submit required documentation. Conflict of interest:
Populations Interventions Comparators Outcomes Individuals: With Barrett esophagus with high-grade dysplasia
 Endoscopic Radiofrequency Ablation or Cryoablation for Barrett (20180) Medical Benefit Effective Date: 01/01/16 Next Review Date: 09/19 Preauthorization No Review Dates: 05/09, 03/10, 03/11, 03/12, 07/12,
Endoscopic Radiofrequency Ablation or Cryoablation for Barrett (20180) Medical Benefit Effective Date: 01/01/16 Next Review Date: 09/19 Preauthorization No Review Dates: 05/09, 03/10, 03/11, 03/12, 07/12,
Current challenges in Barrett s esophagus
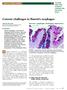 MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
MEDICAL GRAND ROUNDS TAKE-HOME POINTS FROM LECTURES BY CLEVELAND CLINIC AND VISITING FACULTY Current challenges in Barrett s esophagus GARY W. FALK, MD * Director, Center for Swallowing and Esophageal
Quiz Adenocarcinoma of the distal stomach has been increasing in the last 20 years. a. True b. False
 Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
Quiz 1 1. Which of the following are risk factors for esophagus cancer. a. Obesity b. Gastroesophageal reflux c. Smoking and Alcohol d. All of the above 2. Adenocarcinoma of the distal stomach has been
Proton Pump Inhibitors Are Associated with Reduced Incidence of Dysplasia in Barrett s Esophagus
 American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
American Journal of Gastroenterology ISSN 0002-9270 C 2004 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2004.30228.x Published by Blackwell Publishing ORIGINAL CONTRIBUTIONS Proton Pump Inhibitors
Disclosures. Gastroesophageal Reflux Disease. Gastroesophageal Reflux Disease
 Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
Kunal Jajoo, MD Brigham and Women s Hospital July 2012 Disclosures Spouse is a physician employed by Boston Scientific Corporation The content of this lecture equitably discusses products of multiple companies
In 1998, the American College of Gastroenterology issued ALIMENTARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1232 1236 ALIMENTARY TRACT Effects of Dropping the Requirement for Goblet Cells From the Diagnosis of Barrett s Esophagus MARIA WESTERHOFF,* LINDSEY HOVAN,
Surgical strategies in esophageal cancer
 Gastro-Conference Berlin 2005 October 1-2, 2005 Surgical strategies in esophageal cancer J. Rüdiger Siewert Department of Surgery, Klinikum rechts der Isar Technische Universität München Esophageal Cancer
Gastro-Conference Berlin 2005 October 1-2, 2005 Surgical strategies in esophageal cancer J. Rüdiger Siewert Department of Surgery, Klinikum rechts der Isar Technische Universität München Esophageal Cancer
Everything Esophagus: Barrett s Esophagus. Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina
 Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
Everything Esophagus: Barrett s Esophagus Nicholas Shaheen, MD, MPH Center for Esophageal Diseases and Swallowing University of North Carolina The Most Important Thing Stayed the Same Adenocarcinoma A
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia
 National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
National Oesophago-Gastric Cancer Audit New Patient Registration sheet Patients with Oesophageal High Grade Glandular Dysplasia Patient Details Surname: NHS number: Forename: Postcode: Sex: Male Female
POSTOPERATIVE COMPLICATIONS OF TRANSTHORACIC ESOPHAGECTOMY FOR ESOPHAGEAL CARCINOMA
 International International Multidisciplinary Multidisciplinary e Journal/ e-journal Dr. A. Razaque Shaikh, Dr. Khenpal Das, Dr Shahida Khatoon ISSN 2277. (133-140) - 4262 POSTOPERATIVE COMPLICATIONS OF
International International Multidisciplinary Multidisciplinary e Journal/ e-journal Dr. A. Razaque Shaikh, Dr. Khenpal Das, Dr Shahida Khatoon ISSN 2277. (133-140) - 4262 POSTOPERATIVE COMPLICATIONS OF
Determining the Optimal Surgical Approach to Esophageal Cancer
 Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
Determining the Optimal Surgical Approach to Esophageal Cancer Amit Bhargava, MD Attending Thoracic Surgeon Department of Cardiovascular and Thoracic Surgery Open Esophagectomy versus Minimally Invasive
235 60th Street, West New York, NJ T: (201) F: (201) Main Street, Hackensack, NJ T: (201)
 235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Barrett's Esophagus WHAT IS BARRETTT'S ESOPHAGUS? Barrett's esophagus
235 60th Street, West New York, NJ 07093 T: (201) 854-4646 F: (201) 854-4647 810 Main Street, Hackensack, NJ 07601 T: (201) 488-0095 Barrett's Esophagus WHAT IS BARRETTT'S ESOPHAGUS? Barrett's esophagus
Barrett's Esophagus: Sorting Out the Controversy
 Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Barrett's Esophagus: Sorting Out the Controversy Learning Objectives 1. Identify the challenges in screening for Barrett s esophagus 2. Demonstrate comprehension of the risk of progression of Barrett s
Barrett s esophagus (BE) predisposes patients to malignancy
 Squamous Overgrowth Is Not a Safety Concern for Photodynamic Therapy for Barrett s Esophagus With High-Grade Dysplasia MARY P. BRONNER,* BERGEIN F. OVERHOLT, SHARI L. TAYLOR, RODGER C. HAGGITT, KENNETH
Squamous Overgrowth Is Not a Safety Concern for Photodynamic Therapy for Barrett s Esophagus With High-Grade Dysplasia MARY P. BRONNER,* BERGEIN F. OVERHOLT, SHARI L. TAYLOR, RODGER C. HAGGITT, KENNETH
Role of Photodynamic Therapy in Unresectable Esophageal and Lung Cancer
 Lasers in Surgery and Medicine 38:396 402 (2006) Role of Photodynamic Therapy in Unresectable Esophageal and Lung Cancer Mang Chen, MD, Arjun Pennathur, MD, and James D. Luketich, MD* Heart, Lung, and
Lasers in Surgery and Medicine 38:396 402 (2006) Role of Photodynamic Therapy in Unresectable Esophageal and Lung Cancer Mang Chen, MD, Arjun Pennathur, MD, and James D. Luketich, MD* Heart, Lung, and
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Vital staining and Barrett s esophagus
 Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Marcia Irene Canto, MD, MHS Baltimore, Maryland Vital staining or chromoendoscopy refers to staining of endoscopic tissue or topical application of chemical stains or pigments to alter tissue appearances
Occult Esophageal Adenocarcinoma
 ANNALS OF SURGERY Vol. 230, No. 3, 433 440 1999 Lippincott Williams & Wilkins, Inc. Occult Esophageal Adenocarcinoma Extent of Disease and Implications for Effective Therapy John J. Nigro, MD,* Jeffrey
ANNALS OF SURGERY Vol. 230, No. 3, 433 440 1999 Lippincott Williams & Wilkins, Inc. Occult Esophageal Adenocarcinoma Extent of Disease and Implications for Effective Therapy John J. Nigro, MD,* Jeffrey
Changes to the diagnosis and management of Barrett s Oesophagus
 Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
Changes to the diagnosis and management of Barrett s Oesophagus A review of the new BSG and NICE guidelines and best practice Anjan Dhar DM, MD, FRCPE, AGAF, MBBS (Hons.), Cert. Med. Ed Senior Lecturer
National Digestive Diseases Information Clearinghouse
 Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Barrett s Esophagus National Digestive Diseases Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is Barrett s esophagus? Barrett s esophagus is
Barrett s Oesophagus Information Leaflet THE DIGESTIVE SYSTEM. gutscharity.org.
 THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
THE DIGESTIVE SYSTEM http://healthfavo.com/digestive-system-for-kids.html This factsheet is about Barrett s Oesophagus Barrett s Oesophagus is the term used for a pre-cancerous condition where the normal
The gastric tube is a commonly used reconstruction GENERAL THORACIC SURGERY
 GENERAL THORACIC SURGERY PHARYNGEAL REFLUX AFTER GASTRIC PULL-UP ESOPHAGECTOMY WITH NECK AND CHEST ANASTOMOSES Jan Johansson, MD a Folke Johnsson, MD, PhD a Susan Groshen, PhD b Bruno Walther, MD, PhD
GENERAL THORACIC SURGERY PHARYNGEAL REFLUX AFTER GASTRIC PULL-UP ESOPHAGECTOMY WITH NECK AND CHEST ANASTOMOSES Jan Johansson, MD a Folke Johnsson, MD, PhD a Susan Groshen, PhD b Bruno Walther, MD, PhD
Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment Barrett s esophagus
 E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
E318 Volumetric laser endomicroscopy can target neoplasia not detected by conventional endoscopic measures in long segment esophagus Authors Institution Arvind J. Trindade, Benley J. George, Joshua Berkowitz,
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus
 Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
Patterns of recurrent and persistent intestinal metaplasia after successful radiofrequency ablation of Barrett s esophagus Robert J. Korst, MD, a,b Sobeida Santana-Joseph, MSN, a,b John R. Rutledge, MAS,
Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System
 Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System Used abbreviations BE: Barrett s esophagus EC: Early cancer ER: Endoscopic resection HGD:
Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System Used abbreviations BE: Barrett s esophagus EC: Early cancer ER: Endoscopic resection HGD:
What Is Barrett s Esophagus?
 What Is Barrett s Esophagus? Having Barrett s esophagus means the cells lining the esophagus (the tube that links the mouth and the stomach) have changed into types of intestinal cells that are not normal
What Is Barrett s Esophagus? Having Barrett s esophagus means the cells lining the esophagus (the tube that links the mouth and the stomach) have changed into types of intestinal cells that are not normal
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER AUGMENTATION FOR THE TREATMENT OF GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MP Oncologic Applications of Photodynamic Therapy, Including Barrett Esophagus
 Medical Policy MP 8.01.06 BCBSA Ref. Policy: 8.01.06 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: Therapy Related Policies: 2.01.44 Dermatologic Applications of Photodynamic Therapy 2.01.80
Medical Policy MP 8.01.06 BCBSA Ref. Policy: 8.01.06 Last Review: 08/20/2018 Effective Date: 08/20/2018 Section: Therapy Related Policies: 2.01.44 Dermatologic Applications of Photodynamic Therapy 2.01.80
What s New in the Management of Esophageal Disease
 What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
What s New in the Management of Esophageal Disease Philip O. Katz, MD Chairman, Division of Gastroenterology Einstein Medical Center Philadelphia Clinical Professor of Medicine Jefferson Medical College
General introduction and outline of thesis
 General introduction and outline of thesis General introduction and outline of thesis 11 GENERAL INTRODUCTION AND OUTLINE OF THESIS The incidence of esophageal cancer is increasing in the western world.
General introduction and outline of thesis General introduction and outline of thesis 11 GENERAL INTRODUCTION AND OUTLINE OF THESIS The incidence of esophageal cancer is increasing in the western world.
ESOPHAGEAL CANCER AND GERD. Prof Salman Guraya FRCS, Masters MedEd
 ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
Barrett esophagus. Bible class Inselspital
 Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Barrett esophagus Bible class Inselspital 2015.08.10 Guidelines Definition? BSG: ACG: Definition? BSG: ACG: What are the arguments for and against IM as prerequisite for the Dg? What are the arguments
Professor, Department of Endoscopic Diagnostic and Therapeutics, Chiba University School of Medicine
 Gastrointestinal Diseases Esophageal Disorders JMAJ 47(): 41 47, 24 Teruo KOUZU Professor, Department of Endoscopic Diagnostic and Therapeutics, Chiba University School of Medicine Abstract: Recent trends
Gastrointestinal Diseases Esophageal Disorders JMAJ 47(): 41 47, 24 Teruo KOUZU Professor, Department of Endoscopic Diagnostic and Therapeutics, Chiba University School of Medicine Abstract: Recent trends
National Digestive Diseases Information Clearinghouse
 Barrett s Esophagus National Digestive Diseases Information Clearinghouse What is Barrett s esophagus? Barrett s esophagus is a condition in which the tissue lining the esophagus the muscular tube that
Barrett s Esophagus National Digestive Diseases Information Clearinghouse What is Barrett s esophagus? Barrett s esophagus is a condition in which the tissue lining the esophagus the muscular tube that
RADIOFREQUENCY ABLATION OR CRYOABLATION FOR ESOPHAGEAL DISORDERS
 DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
DISORDERS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Ablation. See specific types, e.g., Thermal ablation Achalasia, 53 75 described, 53 features of, 53 management of past options, 54 POEM
Index Note: Page numbers of article titles are in boldface type. A Ablation. See specific types, e.g., Thermal ablation Achalasia, 53 75 described, 53 features of, 53 management of past options, 54 POEM
Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of the distal esophagus, gastroesophageal junction and gastric cardia?
 Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Diseases of the Esophagus (2007) 20, 36 41 DOI: 10.1111/j.1442-2050.2007.00638.x Blackwell Publishing Asia Original article Is intestinal metaplasia a necessary precursor lesion for adenocarcinomas of
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France
 Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Screening of Barrett: Is it cost-effective? Is there a high-risk population? T Ponchon Ed. Herriot Hospital Lyon, France Barrett s esophagus (BE) is an acquired condition in which the normal squamous epithelium
Treating Barrett s oesophagus with photodynamic therapy
 Understanding NICE guidance Information for people who use NHS services Treating Barrett s oesophagus with photodynamic therapy NICE interventional procedures guidance advises the NHS on when and how new
Understanding NICE guidance Information for people who use NHS services Treating Barrett s oesophagus with photodynamic therapy NICE interventional procedures guidance advises the NHS on when and how new
A Novel Intrathoracic Esophagogastric Anastomotic Technique: Potential Benefit for Patients Undergoing a Robotic Assisted MIE
 Accepted Manuscript A Novel Intrathoracic Esophagogastric Anastomotic Technique: Potential Benefit for Patients Undergoing a Robotic Assisted MIE Jeffrey A. Hagen, MD, Chief PII: S0022-5223(18)31737-9
Accepted Manuscript A Novel Intrathoracic Esophagogastric Anastomotic Technique: Potential Benefit for Patients Undergoing a Robotic Assisted MIE Jeffrey A. Hagen, MD, Chief PII: S0022-5223(18)31737-9
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ
 Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
Barrett Esophagus - RadioFrequency Ablation (BE-RFA) - Project manual + FAQ Table of contents 1 General project information...3 1.1 Inclusion criteria...3 1.2 Registration time points...3 1.3 Project variable
Newly Diagnosed Cases Cancer Related Death NCI 2006 Data
 Multi-Disciplinary Management of Esophageal Cancer: Surgical and Medical Steps Forward Alarming Thoracic Twin Towers 200000 150000 UCSF UCD Thoracic Oncology Conference November 21, 2009 100000 50000 0
Multi-Disciplinary Management of Esophageal Cancer: Surgical and Medical Steps Forward Alarming Thoracic Twin Towers 200000 150000 UCSF UCD Thoracic Oncology Conference November 21, 2009 100000 50000 0
During the past 30 years, the incidence of esophageal ORIGINAL ARTICLES
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:38 43 ORIGINAL ARTICLES Optical Coherence Tomography to Identify Intramucosal Carcinoma and High-Grade Dysplasia in Barrett s Esophagus JOHN A. EVANS,* JOHN
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:38 43 ORIGINAL ARTICLES Optical Coherence Tomography to Identify Intramucosal Carcinoma and High-Grade Dysplasia in Barrett s Esophagus JOHN A. EVANS,* JOHN
Accepted Manuscript. CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D
 Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
Accepted Manuscript CGH Editorial: Sound the Alarm for Barrett s Screening! Tarek Sawas, M.D., M.P.H., David A. Katzka, M.D PII: S1542-3565(18)31093-0 DOI: 10.1016/j.cgh.2018.10.010 Reference: YJCGH 56132
