Interstitial lung diseases in a lung cancer screening trial
|
|
|
- Austin Maxwell
- 5 years ago
- Views:
Transcription
1 Eur Respir J 2011; 38: DOI: / CopyrightßERS 2011 Interstitial lung diseases in a lung cancer screening trial N. Sverzellati*, L. Guerci*, G. Randi #, E. Calabrò ", C. La Vecchia #,+, A. Marchianò 1, A. Pesci e, M. Zompatori** and U. Pastorino " ABSTRACT: We assessed the prevalence of interstitial lung disease (ILD) in a cohort of smokers included in a lung cancer screening trial. Two observers independently reviewed, for the presence of findings consistent with ILD, the computed tomography (CT) examinations of 692 heavy smokers recruited by the Multicentric Italian Lung Detection (MILD) trial. Four CT patterns were considered: usual interstitial pneumonia (UIP), other chronic interstitial pneumonia (OCIP), respiratory bronchiolitis (RB) and indeterminate. Subsequently, the evolution of ILD in those subjects who had undergone a repeat CT examination after 3 yrs was assessed. The UIP pattern and the OCIP pattern were identified in two (0.3%) out of 692 and 26 (3.8%) out of 692 patients, respectively; 109 (15.7%) out of 692 patients showed CT abnormalities consistent with RB, while an indeterminate CT pattern was reported in 21 out of 692 (3%) patients. Age, male sex and current smoking status were factors associated with the presence of OCIP and UIP (combined) pattern, although the relationship did not attain statistical significance. A progression of the disease was observed in three (25%) out of 12 subjects with OCIP who underwent repeat CT after 3 yrs. Thin-section CT features of ILD, probably representing smoking-related ILD, are not uncommon in a lung cancer screening population and should not be overlooked. KEYWORDS: Cigarette smoking, computed tomography, interstitial lung disease, lung cancer, screening Cigarette smoking is a recognised risk factor for the development of interstitial lung disease (ILD) [1 3]. The spectrum of thin-section computed tomography (CT) abnormalities associated with cigarette smoking was first defined by REMY-JARDIN and coworkers [4, 5], and since then it has widened continuously. Smokingrelated, thin-section CT abnormalities vary from signs of respiratory bronchiolitis (RB) in asymptomatic patients to severe fibrotic lung disease [1 3], although the mechanisms underlying such associations are not well established. Smoking may cause subclinical parenchymal lung disease consistent with ILD detectable by CT imaging, even among apparently healthy subjects [6]. Although the thin-section CT features of these disorders have been increasingly described in the literature, few data have beenreportedontheirsignificance in smokers participating in a lung cancer screening trial [7, 8]. A comprehensive assessment of chest CT as a screening tool should include a thorough appreciation of the prevalence and nature of those findings that may have prognostic relevance and require therapeutic interventions. The purpose of this study was to determine the frequency, appearances and evolution over time of ILD by thin-section CT in a population of smokers included in a lung cancer screening trial. METHODS Data were collected from the Multicentric Italian Lung Detection (MILD) project at the National Cancer Institute (Milan, Italy). The MILD project is an ongoing population-based, randomised controlled lung cancer screening trial, whose primary aim is the assessment of smoking cessation rate among participants, and of the impact of early lung cancer detection on mortality. The MILD project was approved by institutional review boards, and written informed consent was obtained from all participants. For the purpose of this retrospective additional study, and according to the previously obtained Ethics Committee approval and patients informed consent, we were allowed to use the original data for further research. Eligibility criteria for the MILD study included age o49 yrs, current or former smokers (having quit smoking f10 yrs before recruitment) with at AFFILIATIONS *Dept of Clinical Sciences, Division of Radiology, University of Parma, Parma, # Dept of Epidemiology, Mario Negri Institute, Divisions of " Thoracic Surgery, and, 1 Radiology, National Cancer Institute, + Institute of Medical Statistics and Biometry G.A. Maccacaro, University of Milan, Milan, e Clinical Pulmonology, S. Gerardo Hospital of Monza, University of Milano-Bicocca, Monza, and **Dept of Radiology, S.Orsola Hospital of Bologna, University of Bologna, Bologna, Italy. CORRESPONDENCE N. Sverzellati Dipartimento di Scienze Cliniche, Sezione di Radiologia University di Parma Ospedale Maggiore di Parma Padiglione Barbieri V. Gramsci Parma Italy nicolasve@tiscali.it Received: Dec Accepted after revision: Dec First published online: Jan European Respiratory Journal Print ISSN Online ISSN VOLUME 38 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
2 N. SVERZELLATI ET AL. INTERSTITIAL LUNG DISEASE least 20 pack-yrs of smoking history and no history of cancer within the previous 5 yrs. Our sampling frame comprised 700 subjects without lung cancer out of the 1,236 subjects recruited between September 2005 and September 2006 (i.e. the first year of recruitment) by MILD. Cases with the longest follow-up CT scan (i.e. after 3 yrs) obtained for the evaluation of lung nodules according to our lung cancer screening protocol were included a priori (256 (20.7%) out of 1,236 subjects), to allow an assessment of the evolution of any ILD detected to be made [9]. The repeat CT scans were extracted and compared with their corresponding baseline scans. The remaining 444 (35.9%) subjects were randomly selected by the computer and mixed up with the other 256 for review. Such cases had been included in another study addressing a separate hypothesis [10]. Demographic data and smoking history were obtained through a standardised questionnaire for MILD participants. Forced expiratory volume in 1 s and forced vital capacity expressed as % predicted were recorded. Low-dose, thin-section CT protocol CT was performed using a 16-detector row CT system (Somatom Sensation 16; Siemens Medical Solutions, Forchheim, Germany). All CT examinations of the whole lung were acquired during one deep inspiratory breath-hold without the use of contrast medium. Standard low-dose CT parameters were as follows: 120 kv, 30 mas, 0.75 mm collimation, gantry rotation time 0.5 s, pitch 1.5. Visual evaluations of ILD were performed on images reconstructed for detection of pulmonary nodules: 1- mm-thick sections with a reconstruction increment of 1 mm and a sharp kernel (Siemens B50 kernel). All images were viewed at window settings optimised for assessment of lung parenchyma (width HU; level HU). Image evaluation The CT images of the study population were transferred to a CT workstation (Leonardo; Siemens Medical Solutions) and independently reviewed by two observers (N. Sverzellati and L. Guerci, with 7 and 4 yrs experience, respectively, in interpreting thin-section CT scans for ILD) for the presence or absence of signs of ILD, without knowledge of the clinical data of the study population. Disagreements on presence variables and on the CT diagnosis were resolved by consensus review of divergent evaluations. CT examinations were evaluated for the presence of parenchymal changes consistent with ILD, with the specific recommendation to record the presence or absence of ground-glass opacities, consolidation, honeycombing, reticulation and cysts, centrilobular hazy nodules and traction bronchiectasis within areas of ILD. Observers were instructed not to take into account ground-glass opacity when limited to the dependent lung zones (in keeping with dependent atelectasis). Observers were recommended to use the glossary of the Fleischner Society [11]. After assessing the presence of CT findings, the observers evaluated their predominant distribution. The distribution was classified as being predominantly in the upper lung zone (when most of the findings were above the level of the tracheal carina), the lower lung zone (when most of the findings were below the level of the tracheal carina) or diffuse; and as being predominantly peripheral (when findings involved mainly the outer third of the lung), central (when findings were located mainly in the inner two third of the lung) or diffuse. Spatial homogeneity was evaluated through observation of a patchy versus confluent pattern. Following the initial assessment of the CT findings, each radiologist assessed the CT patterns for each patient with CT abnormalities consistent with ILD, with the provision of specific diagnostic criteria based on the current literature and the American Thoracic Society and European Respiratory Society classification for the idiopathic interstitial pneumonias [12, 13]. The CT findings were grouped into three CT patterns as following: 1) usual interstitial pneumonia (UIP)-like pattern; 2) other chronic interstitial pneumonia (OCIP)-like pattern (including either the nonspecific interstitial pneumonia and the desquamative interstitial pneumonia appearances); and 3) RB-like pattern (table 1). When the CT findings did not match any of the criteria, i.e. the abnormalities were equivocal for ILD (e.g. focal ground-glass opacity, unilateral reticulation etc.), the diagnosis was considered as indeterminate. Subsequently, for each subject with a repeat CT examination after 3 yrs, the observers jointly performed a simultaneous evaluation of the baseline and corresponding follow-up CT examinations to analyse changes over time. On the repeat CT examinations, the extent of CT abnormalities was coded as resolved, similar, greater or lower compared with baseline. The observers also assessed whether the baseline CT pattern showed any change toward another one (e.g. OCIP-like pattern changed into UIP-like pattern). TABLE 1 MDCT pattern Diagnostic criteria for the usual interstitial pneumonia (UIP)-like, other chronic interstitial pneumonia (OCIP)-like, respiratory bronchiolitis (RB)-like and indeterminate patterns MDCT findings UIP-like pattern Honeycombing, reticulation, no or minimal ground-glass opacity, peripheral and basal predominance OCIP-like pattern Predominant ground-glass opacity, no or mild to moderate reticulation, no or traction bronchiectasis, no or minimal honeycombing, bilateral distribution RB-like pattern Hazy centrilobular nodules, no or mild patches of ground-glass opacities, no or mild reticular abnormalities Indeterminate pattern Unilateral distribution, predominant consolidation or cysts, and any other finding not included in the UIP-like, OCIP-like and RB-like patterns MDCT: multidetector computed tomography. c EUROPEAN RESPIRATORY JOURNAL VOLUME 38 NUMBER 2 393
3 INTERSTITIAL LUNG DISEASE N. SVERZELLATI ET AL. TABLE 2 Distribution of the computed tomography findings according to their patterns UIP-like pattern OCIP-like pattern RB-like pattern Indeterminate pattern Subjects n Centrilobular nodules 0 (0) 8 (30.7) 97 (89) 1 (4.8) Ground-glass opacities 2 (100) 23 (88) 17 (15.6) 19 (90.5) Reticular opacities 2 (100) 4 (15.3) 8 (7.3) 1 (4.8) Consolidation 0 (0) 0 (0) 0 (0) 1 (4.8) Honeycombing 2 (100) 0 (0) 0 (0) 0 (0) Traction bronchiectasis 2 (100) 4 (15.3) 0 (0) 0 (0) Craniocaudal distribution Upper zone predominance 0 (0) 4 (15.3) 109 (100) 11 (52.4) Lower zone predominance 2 (100) 7 (27) 0 (0) 5 (23.8) Diffuse 0 (0) 15 (57.7) 0 (0) 5 (23.8) Axial distribution Peripheral predominance 2 (100) 21 (80.7) 0 (0) 14 (66.7) Central predominance 0 (0) 4 (15.3) 0 (0) 7 (33.3) Diffuse 0 (0) 1 (3.8) 109 (100) 0 (0) Homogeneity Patchy 2 (100) 18 (69.2) 109 (100) 20 (95.2) Confluent 0 (0) 8 (30.8) 0 (0) 1 (4.8) Data are presented as n (%), unless otherwise stated. UIP: usual interstitial pneumonia; OCIP: other chronic interstitial pneumonia; RB: respiratory bronchiolitis. Data analysis Unweighted kappa coefficients of agreement (k) were computed for the CT findings and their distribution. Interobserver agreement was classified as poor (k ), fair (k ), moderate (k ), good (k ) or excellent (k ) [14]. We estimated ILD prevalence rates by applying a generalised linear regression model of the Poisson family with a logarithmic link function, including adjustment terms of age, sex and smoking status. To further explore ILD prevalence rates, we considered the CT patterns only among the consecutive cases of our study cohort. Comparative analyses were obtained using both Fisher s exact test and ANOVA to evaluate differences in selected demographic, clinical and pulmonary function test results between subjects with and without ILD. An unconditional polychotomous logistic regression model was used to assess the association between the presence of the subtypes of ILD and demographic data, clinical features and pulmonary function indices; the corresponding odds ratio (OR) with 95% confidence interval (CI) were computed. The final model included age (continuous), sex, smoking status (current FIGURE 1. A 59-yr-old male with low-dose, thin-section computed tomography (CT) abnormalities resembling a usual interstitial pneumonia-like pattern. Transverse thin-section CT image shows reticular with traction bronchiectasis with minimal honeycombing, predominantly distributed in the subpleural basal regions. FIGURE 2. Transverse low-dose, thin-section computed tomography (CT) image of a characteristic other chronic interstitial pneumonia-like pattern at the basal regions, in a 64-yr-old female. The CT pattern is made of ground-glass opacities and minimal reticulation with intermingled mild traction bronchiectasis (arrows). 394 VOLUME 38 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
4 N. SVERZELLATI ET AL. INTERSTITIAL LUNG DISEASE and former smokers), number of cigarettes per day (continuous) and number of smoking years (continuous). Heterogeneity among ILD subtype risks was assessed using a Wald test with two degrees of freedom [15]. All the analyses were performed with SAS Release 9.1 (SAS Institute Inc., Cary, NC, USA). RESULTS Multidetector CT findings at baseline Interobserver agreement was fair (k50.3) for the diagnosis of the RB-like pattern, moderate (k50.6) for the OCIP-like pattern, moderate (k50.49) for the indeterminate pattern and excellent (k51.00) for the UIP-like pattern. Interobserver agreement was moderate for ground-glass opacity (k50.43) and centrilobular nodules (k50.5), good for reticulation (k50.62) and traction bronchiectasis (k 50.7), and excellent for consolidation (k51.0) and honeycombing (k51.0). Interobserver agreement was a) moderate for both upper predominant (k50.45) and lower predominant (k50.45) distribution as well as moderate for both peripheral (k50.5) and central (k50.45) distribution; and it was fair for patchy (k50.4), diffuse (k50.3) and confluent (k50.3) distribution. Eight CT examinations were not considered eligible for the visual score due to motion artefacts, and the final study cohort thus comprised 692 subjects. At baseline, the UIP-like pattern and the OCIP-like pattern were identified in two (0.3%) out of 692 and 26 (3.8%) out of 692 patients, respectively; the crude prevalence of the combined UIP/OCIP pattern was 4.0% (95% CI %), which increased to 9.3% (95% CI 5.2% 16.7%) after adjustment for age, sex and smoking status. A total of 109 (15.7%) out of 692 patients showed CT abnormalities consistent with RB, while CT abnormalities equivocal for ILD were reported in 21 (3%) out of 692 subjects. CT examinations were regarded as normal in 534 (77.2%) out of 692 subjects. Considering only consecutive cases (420 (61%) out of 692), the UIP-like pattern was identified in one (0.2%) out of 420, the OCIP-like pattern in 14 (3.3%) out of 420, the RB-like pattern in 69 (16.4%) out of 420, and the indeterminate pattern in 14 (3.3%) out of 420. The crude prevalence of the combined UIP/OCIP pattern among consecutive cases was 3.6% (95% CI 2.1% 5.9%), which increased to 10.1% (95% CI 4.8% 21.1%) after adjustment for age, sex and smoking status. Detailed descriptions of CT findings are summarised in table 2. The presence of subpleural basal honeycombing with peripheral reticular opacities and traction bronchiectasis was regarded as consistent with a UIP-like pattern in two (0.3%) out of 692 cases (fig. 1). These two subjects were current smokers with a long history of smoking (40 and 50 yrs, respectively). b) Peripheral ground-glass opacity was the most frequent finding in subjects with a OCIP-like pattern (23 (88%) out of 26), while reticular opacities were recorded in four (15.3%) out of 26 cases (figs 2 and 3). In eight (30.8%) out of 26 cases, a OCIP-like FIGURE 3. a) A 52-yr-old male with low-dose, thin-section computed tomography (CT) findings regarded as other chronic interstitial pneumonia-like pattern by both the observers. Note the evident reticular opacities at the level of the basal subpleural regions. b) Repeat CT examination 3 yrs later showing an increase in extent of reticulation with developed honeycombing regarded as usual interstitial pneumonia-like pattern by both the observers. FIGURE 4. A respiratory bronchiolitis-like pattern in a 56-yr-old female. Lowdose, thin-section computed tomography image shows peripheral ground-glass opacity in the ventral regions, centrilobular hazy nodules, scarce interlobular septal thickening (arrows) and mild paraseptal emphysema. c EUROPEAN RESPIRATORY JOURNAL VOLUME 38 NUMBER 2 395
5 INTERSTITIAL LUNG DISEASE N. SVERZELLATI ET AL. a) b) FIGURE 5. Thin-section computed tomography (CT) images in a 64-yr-old quitter. a) Thin-section CT image targeted to the right lung at baseline shows faint centrilobular micronodules. b) 3 yrs later, a decrease in profusion of the nodules was evident at repeat CT. pattern coexisted with hazy centrilobular nodules predominating in the upper zones. Small cysts intermingled with peripheral ground-glass opacity were observed in one case out of 26. Four (15.3%) out of 26 cases with a OCIP-like pattern showed traction bronchiectasis. Diffuse hazy centrilobular nodules predominating in the upper lung zone were the most frequent finding (97 (89%) out of 109) in patients with a RB-like pattern. In subjects with a RB-like pattern, patchy ground-glass opacity associated with centrilobular nodules was reported in 17 out of 109 cases (figs 4 and 5), while ground-glass opacity was identified either as an isolated finding or associated with scarce interlobular septal thickening in eight out of 109 and four out of 109 cases, respectively. Overall, mild interlobular septal thickening was reported in eight out of 109 cases with an RB-like pattern. Most (19 (90.5%) out of 21) of the indeterminate CT patterns were characterised predominantly by very mild patchy ground-glass opacities (fig. 6). In three out of 19 cases, ground-glass opacity was unilateral, while in one out of 19 it was limited to the middle lobe and the lingula. Two out of 21 cases showed indistinct (acinar) ground-glass opacities predominating in the upper lung zone, while another showed basal bilateral consolidation. Demographic, clinical and functional findings at baseline Demographic and smoking history, and pulmonary function data, are shown according to the presence of ILD in table 3. Because of the small number of cases with a UIP-like pattern, the UIP-like cases were grouped with the OCIP ones for comparison analyses. Subjects with CT abnormalities either consistent with or equivocal for ILD showed a longer history of smoking and were more frequently current smokers. Both subjects with a UIP/OCIP-like pattern and those with an indeterminate CT pattern were older than smokers without signs of ILD. According to the multivariate polychotomous logistic regression model (table 4), the risk for the presence of UIP/OCIP-like patterns was directly associated with age (OR 2.06 for 10 yrs (95% CI )), male sex (OR 2.71 (95% FIGURE 6. A 68-yr-old male with findings suggestive of interstitial lung disease, classified as indeterminate pattern on computed tomography by both the observers. Minimal ground-glass opacities are limited to the subpleural basal regions of the left lung. CI )) and current smoking status (OR 2.29 (95% CI )), whereas the RB-like pattern was inversely associated with age (OR 0.51 for 10 yrs (95% CI )) and directly associated with current smoking status (OR 3.35 (95% CI )). Heterogeneity between the RB-like pattern risk and the UIP/OCIP-like pattern risk was observed for age (p50.002), but not for smoking status (p50.545). Evolution between baseline and follow-up multidetector CT findings and smoking status There were 256 multidetector CT scans after 3 yrs, with 44 (17.1%), 13 (5%) and 12 (4.7%) of them having a RB-like pattern, an indeterminate pattern and a OCIP-like pattern on baseline CT scan, respectively. None of the subjects with a UIP-like pattern at baseline underwent a CT examination after 3 yrs. Follow-up CT scan of one subject with an OCIP-like pattern at baseline was interpreted as being consistent with UIP (fig. 3b), while two other cases with an OCIP-like pattern showed an increase in extent of the reticular abnormalities (three (25%) out of 12). The rest (nine (75%) out of 12) of the repeat CT examinations of the subjects with an OCIP-like pattern did not show any changes in either the pattern or extent of the disease. Among the 13 subjects with an indeterminate CT pattern, the CT findings were similar in eight out of 13 cases and resolved in three out of 13 cases after 3 yrs. The extent of ground-glass opacity increased in two out of 13 cases. No RB-like patterns changed their appearance. Among the 42 subjects with centrilobular nodules at baseline, nodules were similar in 36 (85.7%) out of 42, while they increased in profusion in three out of 42 cases, decreased in one out of 42 cases (fig. 5b), and completely resolved in one out of 42 cases. Among the nine subjects with ground-glass opacities at baseline, the extent of ground-glass opacities was similar in seven out of nine cases, decreased in one case and increased in one case out of nine, respectively. Ground-glass opacities superimposed ex novo on centrilobular nodules in only one case. One patient who had 396 VOLUME 38 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
6 N. SVERZELLATI ET AL. INTERSTITIAL LUNG DISEASE TABLE 3 Demographic and clinical characteristics of 692 subjects according to the presence of thin-section computed tomography patterns RB-like pattern OCIP- and UIP-like patterns Indeterminate pattern Normal p-value # Subjects n Age yrs Sex Female 36 (33.0) 4 (14.3) 4 (19.1) 185 (34.6) Male 73 (67.0) 24 (85.7) 17 (81.0) 349 (65.4) Smoking status Former 11 (10.1) 5 (18.5) 3 (14.3) 159 (29.8) Current 98 (89.9) 22 (81.5) 18 (85.7) 375 (70.2),0.001 Number of cigarettes per day,20 24 (22.0) 8 (28.6) 5 (23.8) 122 (22.9) (42.2) 7 (25.0) 10 (47.6) 230 (43.1) (35.8) 13 (46.4) 6 (28.6) 182 (34.1) Number of smoking yrs,35 29 (26.6) 5 (17.9) 5 (23.8) 183 (34.3) (29.4) 8 (28.3) 6 (28.6) 125 (23.4) o40 48 (44.0) 15 (53.6) 10 (47.6) 226 (42.3) Yrs of stopping smoking FEV1 % pred FVC % pred Data are presented as mean SD or n (%), unless otherwise stated. RB: respiratory bronchiolitis; OCIP: other chronic interstitial pneumonia; UIP: usual interstitial pneumonia; FEV1: forced expiratory volume in 1 s; % pred: % predicted; FVC: forced vital capacity. # : derived from Fisher s exact test for categorical variables and ANOVA analysis for continuous variables. mild interlobular septal thickening at baseline did not show any change in extent of those abnormalities at follow-up CT. In two out of 184 smokers without any sign of ILD at baseline, diffuse peripheral ground-glass opacity resembling an OCIPlike pattern and centrilobular hazy nodules predominating in the upper zones were respectively reported. Both of them were persistent former smokers. As detailed in table 5, the frequency of quitters among subjects with either an OCIP-like or an indeterminate CT pattern was greater than that of those with a RB-like pattern and controls. All subjects with either an OCIP-like, an RB-like or an indeterminate pattern showing an increase in the disease extent at repeat CT were persistent current smokers, whereas those in whom the disease extent decreased were quitters. DISCUSSION This study shows that important abnormalities consistent with fibrotic ILD may be encountered in participants in a lung cancer screening trial. In our study population, the crude prevalence of UIP/OCIP was 4.0% (95% CI 2.8% 5.9%), while the prevalence adjusted for age, sex and smoking status was TABLE 4 Interstitial lung disease for selected characteristics by computed tomography patterns RB-like pattern OCIP- and UIP-like patterns p Heterogeneity Age (10 yrs) 0.51 ( ) 2.06 ( ) Sex Female 1 1 Male 1.12 ( ) 2.71 ( ) Smoking status Former smokers 1 1 Current smokers 3.35 ( ) 2.29 ( ) Number of cigarettes?day -1 (10 units) 1.10 ( ) 1.18 ( ) Number of smoking yrs (10 yrs) 1.36 ( ) 1.17 ( ) Data are presented as odds ratio (95% confidence interval), estimated with polychotomous logistic regression models including all the variables listed in the table. RB: respiratory bronchiolitis; OCIP: other chronic interstitial pneumonia; UIP: usual interstitial pneumonia. c EUROPEAN RESPIRATORY JOURNAL VOLUME 38 NUMBER 2 397
7 INTERSTITIAL LUNG DISEASE N. SVERZELLATI ET AL. TABLE 5 Evolution of smoking status between baseline and repeat computed tomography examinations Persistent current smokers Persistent former smokers Quitting smokers Current ex-former smokers # RB-like pattern 34 (77.3) 6 (13.6) 4 (9.1) 0 Stable Increased Decreased OCIP-like pattern 7(58.3) 2 (16.7) 3 (25.0) 0 Stable Increased Decreased Indeterminate pattern 7(53.9) 2 (15.4) 4 (30.8) 0 Stable Increased Decreased Normal 123 (62.1) 52 (26.3) 21 (10.6) 2 (1.0) Stable Increased Data are presented as n (%) or n. RB: respiratory bronchiolitis; OCIP: other chronic interstitial pneumonia. # : ex-smokers who resumed smoking between baseline and repeat computed tomography examinations. 9.3% (95% CI 5.2% 16.7%). Importantly, such prevalence data were similar to those obtained by limiting the evaluation only to the consecutive cases of our study cohort. This prevalence is between that reported by other studies evaluating the incidental findings in lung cancer screening. In the Dutch Belgian Randomised Controlled Lung Cancer Screening Trial (NELSON study) [7], signs of pulmonary fibrosis were reported in 117 (8%) out of 1,409 cases, whereas they were observed in six (1.3%) out of 449 cases recruited by the ProActive Lung Cancer Detection (PALCAD) study [8]. Another recent study has shown by means of CT densitometric techniques in a large population-based cohort of smokers that abnormalities consistent with ILD are frequently detectable in asymptomatic smokers and cumulative and current cigarette smoking were both independently associated with them [6]. However, an advantage of our study was to assess the CT pattern among subjects with ILD to improve the discriminatory information provided by CT. To our knowledge, this is the first study that has addressed such evaluation in a lung cancer screening population, and it was useful to further elucidate the prevalence of the ILD in a large population of asymptomatic smokers and to explore the relevance of these CT features from a prognostic standpoint. The findings that two (0.3%) out of 692 cases showed a UIP-like CT pattern at baseline and another with a OCIP-like pattern came to resemble that of UIP after 3 yrs, highlights the importance of not overlooking the presence of ILD in a lung cancer screening population. A growing body of studies shows that smoking is an independent risk factor for the development of UIP, which, in the majority of cases, carries a prognosis worse than that of many lung cancers [16 18]. Notably, the relatively low prevalence of the UIP-like CT pattern (0.4% including the case detected at repeat CT) in our study cohort was slightly lower than that of the lung cancers detected by our screening project in the first year of recruitment (10 (0.8%) out of 1,236). We reported 26 (3.7%) out of 705 cases with an OCIP-like pattern, mainly characterised by peripheral ground-glass opacities. The coexistence of hazy centrilobular nodules in about one-third of these cases further emphasises the overlap between the ILD features related to smoking. The reported association between the CT abnormalities of the UIP/OCIPlike pattern and smoking status, with current smokers more at risk of developing such diseases, further corroborates the link with smoking; such a link is also supported by the longitudinal behaviour of the OCIP-like pattern, with disease progression observed among persistent current smokers and decrease in quitters. By contrast, the finding that the presence of a UIP/ OCIP-like pattern was associated with age is in keeping with recent observations of ILD findings frequently seen among asymptomatic elderly individuals independent of smoking history [19]. Of note, males were more at risk for the UIP/OCIP pattern, in keeping with previous findings showing such changes more often in male than female smokers [17, 20]. However, the relevance of such multidetector CT abnormalities remains open to debate as 25% of the OCIP cases in our study showed a progression after 3 yrs, suggesting that attention should be paid even to these more apparently indolent ILDs to prevent fibrosis progression or the occurrence of complications. However, it appears possible that abnormalities defining the OCIP-like pattern might be symptomatic as shown by the relatively higher percentages of former smokers at follow-up among subjects with an OCIP-like pattern as compared to either controls and those with RB. Although RB is seen as a very common histological finding in cigarette smokers, and of little clinical significance, we have undertaken the evaluation of CT signs of RB to extend the knowledge on their prevalence and relationship with smoking 398 VOLUME 38 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
8 N. SVERZELLATI ET AL. INTERSTITIAL LUNG DISEASE history in a large study population. In our study, the prevalence of CT changes consistent with RB was lower than those reported previously. Whilst REMY-JARDIN et al. [5] found upper zone-predominant micronodules in 26 (27%) out of 98 asymptomatic smokers, we found signs of RB in 109 (15.7%) out of 692 smokers despite the fact that individuals recruited by MILD were heavier smokers. Such a discrepancy may have several explanations: in particular, the use of a low-dose CT protocol in our lung cancer screening trial may have lowered the detection rate of hazy nodules and ground-glass opacity [21]. Furthermore, in contrast with another study of REMY-JARDIN et al. [22], which showed changes of centrilobular nodules over a mean period of 5.5 yrs in 11 (64.7%) out of 17 smokers, only five (12%) out of 42 cases with centrilobular nodules displayed changes after 3 yrs in our study. Notably, in our study, no RBlike pattern changed toward another one. However, the different time windows might certainly explain the differences with the study of REMY-JARDIN et al. [22]. In keeping with the study of FRAIG et al. [23], we showed that current smokers were more at risk of showing RB compared with former smokers, and RB findings may persist after smoking cessation, being present in both former and quitting smokers. The finding that the RBlike pattern was inversely associated with age is in keeping with previous observations showing RB changes occurring more frequently in young current smokers [24, 25]. Our study does have some limitations. The inclusion a priori of a sub-group of subjects having follow-up CT examination at the longest available time frame might have biased our observations. Nevertheless, we would like to stress that such a bias is likely to be negligible in the absence of any reason why individuals with a lung nodule should be more or less predisposed to developing ILD. The lack of histological data and a full clinical evaluation in the lung cancer screening setting induced speculation to attempt a more complete characterisation of the abnormalities consistent with or suspicious for ILD. Similarly to the scheme proposed by CHURG and MÜLLER [12], the CT findings were grouped into three fundamental CT patterns (i.e. UIP-like, OCIP-like and RB-like patterns) that generally carry different prognoses. However, a significant radiological overlap exists among those CT patterns. While the typical thin-section CT pattern is highly predictive of a histological diagnosis of UIP, the OCIP-like CT pattern may correspond to a wider spectrum of histological diagnoses such as desquamative interstitial pneumonia (DIP) (the case with some cysts intermingled with ground-glass opacities was in keeping with DIP) and even UIP (this might fit with our case showing OCIP-like pattern at baseline that changed the CT appearance into a UIP-like pattern after 3 yrs) [26 29]. The RB-like pattern was assumed to comprise both pure RB and RB-ILD, as they usually display very similar CT pattern and cannot be differentiated solely from the nature of CT abnormalities. Thus such distinction is possible only on the basis of a careful clinical evaluation that was not part of our lung cancer screening protocol. Furthermore, attempting an interpretation of the indeterminate CT patterns, as well as explaining the two normal cases who developed signs of ILD at repeat CT examination, would be very dangerous. The lack of prone images was a limitation because it is possible that some cases with true ground-glass opacity limited to dependent lung zones was not taken into account, reducing the estimation of the ILD prevalence. Of note, no CT signs of Langerhans cell histiocytosis were observed among the indeterminate CT patterns. Finally, we decided to evaluate only the repeat CT examinations after 3 yrs (i.e. the longest follow-up available in the MILD trial) as such a time window was assumed to be sufficient for a proper observation of the evolution of the ILD abnormalities; however, a longer follow-up is probably needed, particularly to evaluate the OCIP-like patterns. It has to be emphasised that the assessment of early ILD over large study populations like those of lung cancer screening trials is challenging and time-consuming. The new system of visual CT scoring proposed by WASHKO et al. [30] for the identification of changes suggestive of early ILD is intriguing as it involves a reduction of more than half in the number of chest CT evaluations compared to a consensus reading. In conclusion, our study suggests that CT signs of ILD are not uncommon in a lung cancer screening cohort and attention should be paid to not overlooking progressive fibrosis. STATEMENT OF INTEREST None declared. REFERENCES 1 Wells AU, Nicholson AG, Hansell DM. Challenges in pulmonary fibrosis. 4: smoking-induced diffuse interstitial lung diseases. Thorax 2007; 62: Attili AK, Kazerooni EA, Gross BH, et al. Smoking-related interstitial lung disease: radiologic clinical pathologic correlation. Radiographics 2008; 28: Vassallo R, Ryu JH. Tobacco smoke-related diffuse lung diseases. Semin Respir Crit Care Med 2008; 29: Remy-Jardin M, Remy J, Gosselin B, et al. Lung parenchymal changes secondary to cigarette smoking: pathologic CT correlations. Radiology 1993; 186: Remy-Jardin M, Remy J, Boulenguez C, et al. Morphologic effects of cigarette smoking on airways and pulmonary parenchyma in healthy adult volunteers: CT evaluation and correlation with pulmonary function tests. Radiology 1993; 186: Lederer DJ, Enright PL, Kawut SM, et al. Cigarette smoking is associated with subclinical parenchymal lung disease: the Multi- Ethnic Study of Atherosclerosis (MESA)-lung study. Am J Respir Crit Care Med 2009; 180: van de Wiel JC, Wang Y, Xu DM, et al. Neglectable benefit of searching for incidental findings in the Dutch Belgian lung cancer screening trial (NELSON) using low-dose multidetector CT. Eur Radiol 2007; 17: MacRedmond R, Logan PM, Lee M, et al. Screening for lung cancer using low dose CT scanning. Thorax 2004; 59: Marchianò A, Calabrò E, Civelli E, et al. Pulmonary nodules: volume repeatability at multidetector CT lung cancer screening. Radiology 2009; 251: Sverzellati N, Calabrò E, Randi G, et al. Sex differences in emphysema phenotype in smokers without airflow obstruction. Eur Respir J 2009; 33: Hansell DM, Bankier AA, MacMahon H, et al. Fleischner Society: glossary of terms for thoracic imaging. Radiology 2008; 246: Churg A, Müller NL. Cellular vs fibrosing interstitial pneumonias and prognosis: a practical classification of the idiopathic interstitial pneumonias and pathologically/radiologically similar conditions. Chest 2006; 130: American Thoracic Society, European Respiratory Society. American Thoracic Society/European Respiratory Society International c EUROPEAN RESPIRATORY JOURNAL VOLUME 38 NUMBER 2 399
9 INTERSTITIAL LUNG DISEASE N. SVERZELLATI ET AL. Multidisciplinary Consensus Classification of the Idiopathic Interstitial Pneumonias. Am J Respir Crit Care Med 2002; 165: Coblentz CL, Babcook CJ, Alton D, et al. Observer variation in detecting the radiologic features associated with bronchiolitis. Invest Radiol 1991; 26: Hosmer DW, Lemeshow S, eds. Applied Logistic Regression. 2nd Edn. New York, John Wiley & Sons Inc, Baumgartner KB, Samet JM, Stidley CA, et al. Cigarette smoking: a risk factor for idiopathic pulmonary fibrosis. Am J Respir Crit Care Med 1997; 155: Antoniou KM, Hansell DM, Rubens MB, et al. Idiopathic pulmonary fibrosis: outcome in relation to smoking status. Am J Respir Crit Care Med 2008; 177: Maher TM, Wells AU, Laurent GJ. Idiopathic pulmonary fibrosis: multiple causes and multiple mechanisms? Eur Respir J 2007; 30: Copley SJ, Wells AU, Hawtin KE, et al. Lung morphology in the elderly: comparative CT study of subjects over 75 years old versus those under 55 years old. Radiology 2009; 251: Marten K, Milne D, Antoniou KM, et al. Non-specific interstitial pneumonia in cigarette smokers: a CT study. Eur Radiol 2009; 19: Zwirewich CV, Mayo JR, Müller NL. Low-dose high-resolution CT of lung parenchyma. Radiology 1991; 180: Remy-Jardin M, Edme JL, Boulenguez C, et al. Longitudinal follow-up study of smoker s lung with thin-section CT in correlation with pulmonary function tests. Radiology 2002; 222: Fraig M, Shreesha U, Savici D, et al. Respiratory bronchiolitis: a clinicopathologic study in current smokers, ex-smokers, and never-smokers. Am J Surg Pathol 2002; 26: Niewoehner DE, Kleinerman J, Rice DB. Pathologic changes in the peripheral airways of young cigarette smokers. N Engl J Med 1974; 291: Moon J, du Bois RM, Colby TV, et al. Clinical significance of respiratory bronchiolitis on open lung biopsy and its relationship to smoking related interstitial lung disease. Thorax 1999; 54: Kligerman SJ, Groshong S, Brown KK, et al. Nonspecific interstitial pneumonia: radiologic, clinical, and pathologic considerations. Radiographics 2009; 29: Flaherty KR, Thwaite EL, Kazerooni EA, et al. Radiological versus histological diagnosis in UIP and NSIP: survival implications. Thorax 2003; 58: Vassallo R, Jensen EA, Colby TV, et al. The overlap between respiratory bronchiolitis and desquamative interstitial pneumonia in pulmonary Langerhans cell histiocytosis: high-resolution CT, histologic, and functional correlations. Chest 2003; 124: Silva CI, Müller NL, Hansell DM, et al. Nonspecific interstitial pneumonia and idiopathic pulmonary fibrosis: changes in pattern and distribution of disease over time. Radiology 2008; 247: Washko GR, Lynch DA, Matsuoka S, et al. Identification of early interstitial lung disease in smokers from the COPDGene Study. Acad Radiol 2010; 17: VOLUME 38 NUMBER 2 EUROPEAN RESPIRATORY JOURNAL
Imaging: how to recognise idiopathic pulmonary fibrosis
 REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
REVIEW IDIOPATHIC PULMONARY FIBROSIS Imaging: how to recognise idiopathic pulmonary fibrosis Anand Devaraj Affiliations: Dept of Radiology, St George s Hospital, London, UK. Correspondence: Anand Devaraj,
Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel
 Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel Poster No.: C-0698 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Chae, G. Jin, S. Chon, Y. Lee;
Combined pulmonary fibrosis and emphysema; prevalence and follow up among health-care personnel Poster No.: C-0698 Congress: ECR 2013 Type: Scientific Exhibit Authors: K. Chae, G. Jin, S. Chon, Y. Lee;
Progress in Idiopathic Pulmonary Fibrosis
 Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Progress in Idiopathic Pulmonary Fibrosis David A. Lynch, MB Disclosures Progress in Idiopathic Pulmonary Fibrosis David A Lynch, MB Consultant: t Research support: Perceptive Imaging Boehringer Ingelheim
Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after smoking cessation
 Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Eur Respir J 2007; 29: 453 461 DOI: 10.1183/09031936.00015506 CopyrightßERS Journals Ltd 2007 Changes in HRCT findings in patients with respiratory bronchiolitis-associated interstitial lung disease after
Diffuse Interstitial Lung Diseases: Is There Really Anything New?
 : Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
: Is There Really Anything New? Sujal R. Desai, MBBS, MD ESTI SPEAKER SUNDAY Society of Thoracic Radiology San Antonio, Texas March 2014 Diffuse Interstitial Lung Disease The State of Play DILDs Is There
Interstitial Lung Abnormalities in a CT Lung Cancer Screening Population: Prevalence and Progression Rate 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Gong Yong Jin, MD,
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. Gong Yong Jin, MD,
11/10/2014. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective Radiology Pathology Clinical 1 Role of HRCT Diagnosis Fibrosis vs. inflammation Next step in management Response to treatment
The concept of respiratory bronchiolitis/interstitial lung
 Respiratory Bronchiolitis/Interstitial Lung Disease Fibrosis, Pulmonary Function, and Evolving Concepts Andrew Churg, MD; Nestor L. Müller, MD, PhD; Joanne L. Wright, MD Context. The concept of respiratory
Respiratory Bronchiolitis/Interstitial Lung Disease Fibrosis, Pulmonary Function, and Evolving Concepts Andrew Churg, MD; Nestor L. Müller, MD, PhD; Joanne L. Wright, MD Context. The concept of respiratory
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia. Nitra and the Gangs.
 Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Usual Interstitial pneumonia and Nonspecific Interstitial Pneumonia Nitra and the Gangs. บทน ำและบทท ๓, ๑๐, ๑๒, ๑๓, ๑๔, ๑๕, ๑๗ Usual Interstitial Pneumonia (UIP) Most common & basic pathologic pattern
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus
 Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Cryptogenic Organizing Pneumonia Diagnosis Approach Based on a Clinical-Radiologic-Pathologic Consensus Poster No.: C-1622 Congress: ECR 2012 Type: Scientific Exhibit Authors: C. Cordero Lares, E. Zorita
Liebow and Carrington's original classification of IIP
 Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
Liebow and Carrington's original classification of IIP-- 1969 Eric J. Stern MD University of Washington UIP Usual interstitial pneumonia DIP Desquamative interstitial pneumonia BIP Bronchiolitis obliterans
IPF: Epidemiologia e stato dell arte
 IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
IPF: Epidemiologia e stato dell arte Clinical Classification Diffuse parenchimal lung diseases Exposure-related: - occupational - environmental - medication Desquamative interstitial pneumonia Idiopathic
Radiologic Approach to Smoking Related Interstitial Lung Disease
 Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Radiologic Approach to Smoking Related Interstitial Lung Disease Poster No.: C-1854 Congress: ECR 2013 Type: Educational Exhibit Authors: K.-N. Lee, J.-Y. Han, E.-J. Kang, J. Kang; Busan/KR Keywords: Toxicity,
Financial disclosure COMMON DIAGNOSES IN HRCT. High Res Chest HRCT. HRCT Pre test. I have no financial relationships to disclose. Anatomy Nomenclature
 Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
Financial disclosure I have no financial relationships to disclose. Douglas Johnson D.O. Cardiothoracic Imaging Gaston Radiology COMMON DIAGNOSES IN HRCT High Res Chest Anatomy Nomenclature HRCT Sampling
HRCT in Diffuse Interstitial Lung Disease Steps in High Resolution CT Diagnosis. Where are the lymphatics? Anatomic distribution
 Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
Steps in High Resolution CT Diagnosis Pattern of abnormality Distribution of disease Associated findings Clinical history Tomás Franquet MD What is the diagnosis? Hospital de Sant Pau. Barcelona Secondary
NONE OVERVIEW FINANCIAL DISCLOSURES UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF (UIP) FOR PATHOLOGISTS. IPF = Idiopathic UIP Radiologic UIP Path UIP
 UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
UPDATE ON IDIOPATHIC PULMONARY FIBROSIS/IPF () FOR PATHOLOGISTS Thomas V. Colby, M.D. Professor of Pathology (Emeritus) Mayo Clinic Arizona FINANCIAL DISCLOSURES NONE OVERVIEW IPF Radiologic Dx Pathologic
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
T he diagnostic evaluation of a patient with
 546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
546 REVIEW SERIES Challenges in pulmonary fibrosis? 1: Use of high resolution CT scanning of the lung for the evaluation of patients with idiopathic interstitial pneumonias Michael B Gotway, Michelle M
Differential diagnosis
 Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Differential diagnosis Idiopathic pulmonary fibrosis (IPF) is part of a large family of idiopathic interstitial pneumonias (IIP), one of four subgroups of interstitial lung disease (ILD). Differential
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings
 Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
Smoking-related Interstitial Lung Diseases: High-Resolution CT Findings Poster No.: C-2358 Congress: ECR 2013 Type: Educational Exhibit Authors: V. Cuartero Revilla, M. Nogueras Carrasco, P. Olmedilla
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review.
 Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Imaging findings in Hypersensitivity Pneumonitis - a pictorical review. Poster No.: C-1655 Congress: ECR 2014 Type: Educational Exhibit Authors: B. M. Araujo, A. F. S. Simões, M. S. C. Rodrigues, J. Pereira;
Clinical significance of respiratory bronchiolitis on open lung biopsy and its relationship to smoking related interstitial lung disease
 Thorax 1999;54:1009 1014 1009 James Moon, Ronald M du Bois, Thomas V Colby, David M Hansell, Andrew G Nicholson Interstitial Lung Disease Unit J Moon R M du Bois Department of Radiology D M Hansell Department
Thorax 1999;54:1009 1014 1009 James Moon, Ronald M du Bois, Thomas V Colby, David M Hansell, Andrew G Nicholson Interstitial Lung Disease Unit J Moon R M du Bois Department of Radiology D M Hansell Department
Diagnosis of Respiratory Bronchiolitis associated interstitial lung disease
 Monaldi Arch Chest Dis 2006; 65: 2, 96-101 ORIGINAL ARTICLE Diagnosis of Respiratory Bronchiolitis associated interstitial lung disease C. Robalo Cordeiro 1, S. Freitas 1, B. Rodrigues 1, A. Catarino 1,
Monaldi Arch Chest Dis 2006; 65: 2, 96-101 ORIGINAL ARTICLE Diagnosis of Respiratory Bronchiolitis associated interstitial lung disease C. Robalo Cordeiro 1, S. Freitas 1, B. Rodrigues 1, A. Catarino 1,
The radiological differential diagnosis of the UIP pattern
 5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
5th International Conference on Idiopathic Pulmonary Fibrosis, Modena, 2015, June 12th The radiological differential diagnosis of the UIP pattern Simon Walsh King s College Hospital Foundation Trust London,
INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX
 INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX Diagnosing fibrotic lung disease: When is high-resolution computed tomography sufficient to make a diagnosis of idiopathic
INVITED REVIEW SERIES: PULMONARY FIBROSIS SERIES EDITORS: MARTIN KOLB AND GERARD COX Diagnosing fibrotic lung disease: When is high-resolution computed tomography sufficient to make a diagnosis of idiopathic
CT Findings in the Elderly Lung
 CT Findings in the Elderly Lung Poster No.: C-2498 Congress: ECR 2015 Type: Educational Exhibit Authors: P. Ananias, R. Coelho, H. M. R. Marques, O. Fernandes, M. Simões, L. Figueiredo; Lisbon/PT Keywords:
CT Findings in the Elderly Lung Poster No.: C-2498 Congress: ECR 2015 Type: Educational Exhibit Authors: P. Ananias, R. Coelho, H. M. R. Marques, O. Fernandes, M. Simões, L. Figueiredo; Lisbon/PT Keywords:
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Hunninghake GM, Hatabu H, Okajima Y, et al. MUC5B promoter
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Hunninghake GM, Hatabu H, Okajima Y, et al. MUC5B promoter
Outline Definition of Terms: Lexicon. Traction Bronchiectasis
 HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
HRCT OF IDIOPATHIC INTERSTITIAL PNEUMONIAS Disclosures Genentech, Inc. Speakers Bureau Tadashi Allen, MD University of Minnesota Assistant Professor Diagnostic Radiology 10/29/2016 Outline Definition of
IPF - Inquadramento clinico
 IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
IPF - Inquadramento clinico Sergio Harari Unità Operativa di Pneumologia UTIR Servizio di Fisiopat. Resp. e Emodinamica Polmonare Ospedale S. Giuseppe, Milano Clinical Classification Diffuse parenchimal
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page
 The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
The Egyptian Journal of Hospital Medicine (July 2017) Vol.68 (2), Page 1135-1140 Role of High Resolution Computed Tomography in Diagnosis of Interstitial Lung Diseases in Patients with Collagen Diseases
Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP)
 Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP) Assem El Essawy (1) & Amr A. Nassef (٢) Abstract Identification of interstitial pneumonia (IP) was mainly based on histological
Criteria for confident HRCT diagnosis of usual interstitial pneumonia (UIP) Assem El Essawy (1) & Amr A. Nassef (٢) Abstract Identification of interstitial pneumonia (IP) was mainly based on histological
5/9/2015. Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective. No, I am not a pulmonologist! Radiology
 Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Multi-disciplinary Approach to Diffuse Lung Disease: The Imager s Perspective No, I am not a pulmonologist! Radiology Pathology Clinical 1 Everyone needs a CT Confidence in diagnosis Definitive HRCT +
Epidemiology and classification of smoking related interstitial lung diseases
 Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
Epidemiology and classification of smoking related interstitial lung diseases Šterclová M. Department of Respiratory Diseases, Thomayer Hospital, Prague, Czech Republic Supported by an IGA Grant No G 1207
Key words: CT scanners; interstitial lung diseases; polymyositis-dermatomyositis; x-ray
 Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
Nonspecific Interstitial Pneumonia Associated With Polymyositis and Dermatomyositis* Serial High-Resolution CT Findings and Functional Correlation Hiroaki Arakawa, MD; Hidehiro Yamada, MD; Yasuyuki Kurihara,
UIP Possibile e Probabile
 UIP Possibile e Probabile Sergio Harari U.O. di Pneumologia e UTIR Servizio di Emodinamica e Fisiopatologia Respiratoria Ospedale San Giuseppe - Milano Current definition of IPF IPF is a distinct type
UIP Possibile e Probabile Sergio Harari U.O. di Pneumologia e UTIR Servizio di Emodinamica e Fisiopatologia Respiratoria Ospedale San Giuseppe - Milano Current definition of IPF IPF is a distinct type
The role of high-resolution computed tomography in the follow-up of diffuse lung disease
 SERIES RADIOLOGY The role of high-resolution computed tomography in the follow-up of diffuse lung disease Brett M. Elicker, Kimberly G. Kallianos and Travis S. Henry Number 2 in the Series Radiology Edited
SERIES RADIOLOGY The role of high-resolution computed tomography in the follow-up of diffuse lung disease Brett M. Elicker, Kimberly G. Kallianos and Travis S. Henry Number 2 in the Series Radiology Edited
Hypersensitivity Pneumonitis: Spectrum of High-Resolution CT and Pathologic Findings
 CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
CT of Hypersensitivity Pneumonitis Chest Imaging Pictorial Essay C. Isabela S. Silva 1 ndrew Churg 2 Nestor L. Müller 1 Silva CIS, Churg, Müller NL Keywords: high-resolution CT, hypersensitivity pneumonitis,
Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping
 Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping K. R. Flaherty Division of Pulmonary and Critical Care Medicine, University of Michigan Health System, Ann Arbor,
Idiopathic Pulmonary Fibrosis: The Importance of Qualitative and Quantitative Phenotyping K. R. Flaherty Division of Pulmonary and Critical Care Medicine, University of Michigan Health System, Ann Arbor,
Cryptogenic Organizing Pneumonia: Serial High-Resolution CT Findings in 22 Patients
 Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
Cardiopulmonary Imaging Original Research Lee et al. High-Resolution CT of Cryptogenic Organizing Pneumonia Cardiopulmonary Imaging Original Research Ju Won Lee 1 Kyung Soo Lee 1 Ho Yun Lee 1 Man Pyo Chung
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS
 USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
USEFULNESS OF HRCT IN DIAGNOSIS AND FOLLOW UP OF PULMONARY INVOLVEMENT IN SYSTEMIC SCLEROSIS Brestas P., Vergadis V., Emmanouil E., Malagari K. 2 nd Dept of Radiology, University of Athens, Greece ABSTRACT
An earlier and more confident diagnosis of idiopathic pulmonary fibrosis
 Eur Respir Rev 2012; 21: 124, 141 146 DOI: 10.1183/09059180.00000812 CopyrightßERS 2012 REVIEW: IPF An earlier and more confident diagnosis of idiopathic pulmonary fibrosis Roland M. du Bois ABSTRACT:
Eur Respir Rev 2012; 21: 124, 141 146 DOI: 10.1183/09059180.00000812 CopyrightßERS 2012 REVIEW: IPF An earlier and more confident diagnosis of idiopathic pulmonary fibrosis Roland M. du Bois ABSTRACT:
Acute and Chronic Lung Disease
 KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
KATHOLIEKE UNIVERSITEIT LEUVEN Faculty of Medicine Acute and Chronic Lung Disease W De Wever, JA Verschakelen Department of Radiology, University Hospitals Leuven, Belgium Clinical utility of HRCT To detect
ARTICLE IN PRESS. Ahuva Grubstein a, Daniele Bendayan b, Ithak Schactman c, Maya Cohen a, David Shitrit b, Mordechai R. Kramer b,
 Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
Respiratory Medicine (2005) 99, 948 954 Concomitant upper-lobe bullous emphysema, lower-lobe interstitial fibrosis and pulmonary hypertension in heavy smokers: report of eight cases and review of the literature
CT in Idiopathic Pulmonary Fibrosis: Diagnosis and Beyond
 Cardiopulmonary Imaging Review Gruden CT of Idiopathic Pulmonary Fibrosis Cardiopulmonary Imaging Review James F. Gruden 1 Gruden JF FOCUS ON: Keywords: CT, diagnosis, high-resolution CT, idiopathic pulmonary
Cardiopulmonary Imaging Review Gruden CT of Idiopathic Pulmonary Fibrosis Cardiopulmonary Imaging Review James F. Gruden 1 Gruden JF FOCUS ON: Keywords: CT, diagnosis, high-resolution CT, idiopathic pulmonary
Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment
 Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
Prague, June 2014 Pulmonary manifestations of CTDs Diagnosis, differential diagnosis and treatment Katerina M. Antoniou, MD, PhD As. Professor in Thoracic Medicine ERS ILD Group Secretary Medical School,
4/17/2010 C ini n ca c l a Ev E a v l a ua u t a ion o n of o ILD U dat a e t e i n I LDs
 Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Update in ILDs Diagnosis 101: Clinical Evaluation April 17, 2010 Jay H. Ryu, MD Mayo Clinic, Rochester MN Clinical Evaluation of ILD Outline General aspects of ILDs Classification of ILDs Clinical evaluation
Daria Manos RSNA 2016 RC 401. https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html
 Daria Manos RSNA 2016 RC 401 https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html STEP1: Is this fibrotic lung disease? STEP 2: Is this a UIP pattern? If yes:
Daria Manos RSNA 2016 RC 401 https://medicine.dal.ca/departments/depar tment-sites/radiology/contact/faculty/dariamanos.html STEP1: Is this fibrotic lung disease? STEP 2: Is this a UIP pattern? If yes:
INTERSTITIAL LUNG DISEASE. Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018
 INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
INTERSTITIAL LUNG DISEASE Radhika Reddy MD Pulmonary/Critical Care Long Beach VA Medical Center January 5, 2018 Interstitial Lung Disease Interstitial Lung Disease Prevalence by Diagnosis: Idiopathic Interstitial
Idiopathic pulmonary fibrosis (IPF) is a
 Eur Respir J 2011; 38: 176 183 DOI: 10.1183/09031936.00114010 CopyrightßERS 2011 Pulmonary function measures predict mortality differently in IPF versus combined pulmonary fibrosis and emphysema S.L. Schmidt*,
Eur Respir J 2011; 38: 176 183 DOI: 10.1183/09031936.00114010 CopyrightßERS 2011 Pulmonary function measures predict mortality differently in IPF versus combined pulmonary fibrosis and emphysema S.L. Schmidt*,
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT
 Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Thoracic lung involvement in rheumatoid arthritis: Findings on HRCT Poster No.: C-2488 Congress: ECR 2015 Type: Educational Exhibit Authors: R. E. Correa Soto, M. J. Martín Sánchez, J. M. Fernandez 1 1
Idiopathic interstitial pneumonias (IIPs) are a group of
 SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
SYMPOSIA C. Isabela S. Silva, MD, PhD and Nestor L. Müller, MD, PhD Abstract: The idiopathic interstitial pneumonias (IIPs) are a group of diffuse parenchymal lung diseases of unknown etiology characterized
A Review of Interstitial Lung Diseases
 Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Outline A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Overview of diagnosis in ILD Why it is important Definition/Classification
Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
 ERJ Express. Published on February 25, 2016 as doi: 10.1183/13993003.01680-2015 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
ERJ Express. Published on February 25, 2016 as doi: 10.1183/13993003.01680-2015 ORIGINAL ARTICLE IN PRESS CORRECTED PROOF Radiologic pathologic discordance in biopsy-proven usual interstitial pneumonia
American Thoracic Society European Respiratory Society Classification of the Idiopathic Interstitial Pneumonias: Advances in Knowledge since 20021
 This copy is for personal use only. To order printed copies, contact reprints@rsna.org American Thoracic Society European Respiratory Society Classification of the Idiopathic Interstitial Pneumonias: Advances
This copy is for personal use only. To order printed copies, contact reprints@rsna.org American Thoracic Society European Respiratory Society Classification of the Idiopathic Interstitial Pneumonias: Advances
DIAGNOSTIC NOTE TEMPLATE
 DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
DIAGNOSTIC NOTE TEMPLATE SOAP NOTE TEMPLATE WHEN CONSIDERING A DIAGNOSIS OF IDIOPATHIC PULMONARY FIBROSIS (IPF) CHIEF COMPLAINT HISTORY OF PRESENT ILLNESS Consider IPF as possible diagnosis if any of the
A Review of Interstitial Lung Diseases. Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco
 A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
A Review of Interstitial Lung Diseases Paul J. Wolters, MD Associate Professor Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Why it is important Definition/Classification
Manish Powari Regional Training Day 10/12/2014
 Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
Manish Powari Regional Training Day 10/12/2014 Large number of different types of Interstitial Lung Disease (ILD). Most are very rare Most patients present with one of a smaller number of commoner diseases
An Image Repository for Chest CT
 An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
An Image Repository for Chest CT Francesco Frajoli for the Chest CT in Antibody Deficiency Group An Image Repository for Chest CT he Chest CT in Antibody Deficiency Group is an international and interdisciplinary
Outcomes in the NLST. Health system infrastructure needs to implement screening
 Outcomes in the NLST Health system infrastructure needs to implement screening Denise R. Aberle, MD Professor of Radiology and Bioengineering David Geffen School of Medicine at UCLA 1 Disclosures I have
Outcomes in the NLST Health system infrastructure needs to implement screening Denise R. Aberle, MD Professor of Radiology and Bioengineering David Geffen School of Medicine at UCLA 1 Disclosures I have
Difficulties Diagnosing Idiopathic Pulmonary Fibrosis
 1. er Encuentro Entre Neumólogos y Radiólogos, Madrid, Spain, 2016, October 14th Difficulties Diagnosing Idiopathic Pulmonary Fibrosis Simon Walsh King s College Hospital Foundation Trust London, United
1. er Encuentro Entre Neumólogos y Radiólogos, Madrid, Spain, 2016, October 14th Difficulties Diagnosing Idiopathic Pulmonary Fibrosis Simon Walsh King s College Hospital Foundation Trust London, United
Acute Exacerbation of Usual Interstitial Pneumonia After Resection of Lung Cancer
 Acute Exacerbation of Usual Interstitial Pneumonia After Resection of Lung Cancer Hiroaki Sugiura, MD, Atsuya Takeda, MD, PhD, Toshiko Hoshi, MD, PhD, Yoshinori Kawabata, MD, Koichi Sayama, MD, PhD, Masahiro
Acute Exacerbation of Usual Interstitial Pneumonia After Resection of Lung Cancer Hiroaki Sugiura, MD, Atsuya Takeda, MD, PhD, Toshiko Hoshi, MD, PhD, Yoshinori Kawabata, MD, Koichi Sayama, MD, PhD, Masahiro
Subclinical interstitial lung abnormalities; lumping and splitting revisited. Simon L.F. Walsh 1, Luca Richeldi 2
 Page 1 of 11 Subclinical interstitial lung abnormalities; lumping and splitting revisited. Simon L.F. Walsh 1, Luca Richeldi 2 1 Fibrosis Research Group, National Heart and Lung Institute, Imperial College,
Page 1 of 11 Subclinical interstitial lung abnormalities; lumping and splitting revisited. Simon L.F. Walsh 1, Luca Richeldi 2 1 Fibrosis Research Group, National Heart and Lung Institute, Imperial College,
Subsolid lung nodules, also termed ground-glass nodules
 ORIGINAL ARTICLE Long-Term Surveillance of Ground-Glass Nodules Evidence from the MILD Trial Silva Mario, MD,* Sverzellati Nicola, MD, PhD,* Manna Carmelinda, MD,* Negrini Giulio, MD,* Marchianò Alfonso,
ORIGINAL ARTICLE Long-Term Surveillance of Ground-Glass Nodules Evidence from the MILD Trial Silva Mario, MD,* Sverzellati Nicola, MD, PhD,* Manna Carmelinda, MD,* Negrini Giulio, MD,* Marchianò Alfonso,
Lung CT: Part 2, The Interstitial Pneumonias Clinical, Histologic, and CT Manifestations
 Integrative Imaging Review Ferguson and Berkowitz CT of Interstitial Pneumonia Integrative Imaging Review CME SAM Lung CT FOCUS ON: Emma C. Ferguson 1 Eugene A. Berkowitz 2 Ferguson EC, Berkowitz EA Keywords:
Integrative Imaging Review Ferguson and Berkowitz CT of Interstitial Pneumonia Integrative Imaging Review CME SAM Lung CT FOCUS ON: Emma C. Ferguson 1 Eugene A. Berkowitz 2 Ferguson EC, Berkowitz EA Keywords:
Case Presentations in ILD. Harold R. Collard, MD Department of Medicine University of California San Francisco
 Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Case Presentations in ILD Harold R. Collard, MD Department of Medicine University of California San Francisco Outline Overview of diagnosis in ILD Definition/Classification High-resolution CT scan Multidisciplinary
Non-neoplastic Lung Disease II
 Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Pathobasic Non-neoplastic Lung Disease II Spasenija Savic Prince Pathology Program Systematic approach to surgical lung biopsies with ILD Examples (chronic ILD): Idiopathic interstitial pneumonias: UIP,
Case 1 : Question. 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random
 Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
Interesting case Case 1 Case 1 : Question 1.1 What is the intralobular distribution? 1. Centrilobular 2. Perilymphatic 3. Random Case 1: Answer 1.1 What is the intralobular distribution? 1. Centrilobular
Usual Interstitial Pneumonia and Non-Specific Interstitial Pneumonia: Serial Thin-Section CT Findings Correlated with Pulmonary Function
 Usual Interstitial Pneumonia and Non-Specific Interstitial Pneumonia: Serial Thin-Section CT Findings Correlated with Pulmonary Function Yeon Joo Jeong, MD 1, 2 Kyung Soo Lee, MD 1 Nestor L. Muller, MD
Usual Interstitial Pneumonia and Non-Specific Interstitial Pneumonia: Serial Thin-Section CT Findings Correlated with Pulmonary Function Yeon Joo Jeong, MD 1, 2 Kyung Soo Lee, MD 1 Nestor L. Muller, MD
Thin-Section CT Findings of Arc-Welders Pneumoconiosis
 Thin-Section CT Findings of Arc-Welders Pneumoconiosis Daehee Han, MD 1 Jin Mo Goo, MD 1 Jung-Gi Im, MD 1 Kyung Soo Lee, MD 2 Do Myung Paek, MD 3 Seong Ho Park, MD 1 Index words: Lungs, diseases Lungs,
Thin-Section CT Findings of Arc-Welders Pneumoconiosis Daehee Han, MD 1 Jin Mo Goo, MD 1 Jung-Gi Im, MD 1 Kyung Soo Lee, MD 2 Do Myung Paek, MD 3 Seong Ho Park, MD 1 Index words: Lungs, diseases Lungs,
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2
 Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
Low-dose CT Lung Cancer Screening Guidelines for Pulmonary Nodules Management Version 2 The Committee for Management of CT-screening-detected Pulmonary Nodules 2009-2011 The Japanese Society of CT Screening
World Journal of Radiology. Pulmonary fibrosis and emphysema: Is the emphysema type associated with the pattern of fibrosis?
 W J R World Journal of Radiology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4329/wjr.v7.i9.294 World J Radiol 2015 September 28; 7(9):
W J R World Journal of Radiology Submit a Manuscript: http://www.wjgnet.com/esps/ Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx DOI: 10.4329/wjr.v7.i9.294 World J Radiol 2015 September 28; 7(9):
Combined Pulmonary Fibrosis and Emphysema - A Case Series
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 1 Ver. III (January. 2017), PP 15-19 www.iosrjournals.org Combined Pulmonary Fibrosis and Emphysema
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 1 Ver. III (January. 2017), PP 15-19 www.iosrjournals.org Combined Pulmonary Fibrosis and Emphysema
Visual Assessment of CT Findings in Smokers With Nonobstructed Spirometric Abnormalities in The COPDGene Study
 88 Chronic Obstructive Pulmonary Diseases: Journal of the COPD Foundation Original Research. Visual Assessment of CT Findings in Smokers With Nonobstructed Spirometric Abnormalities in The COPDGene Study
88 Chronic Obstructive Pulmonary Diseases: Journal of the COPD Foundation Original Research. Visual Assessment of CT Findings in Smokers With Nonobstructed Spirometric Abnormalities in The COPDGene Study
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker. Michael B. Gotway, MD
 August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
August 2018 Imaging Case of the Month: Dyspnea in a 55-Year-Old Smoker Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, AZ USA Clinical History: A 55 year old woman presented
Diagnostic challenges in IPF
 Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Medicine, Nursing and Health Sciences Diagnostic challenges in IPF Dr Ian Glaspole Central and Eastern Clinical School, Alfred Hospital and Monash University March 2015 Disclosures Consultancy fees from
Smoking-related lung pathology represents a histologically
 A Review of Smoking-Related Interstitial Fibrosis, Respiratory Bronchiolitis, and Desquamative Interstitial Pneumonia Overlapping Histology and Confusing Terminology Smoking-related lung diseases traverse
A Review of Smoking-Related Interstitial Fibrosis, Respiratory Bronchiolitis, and Desquamative Interstitial Pneumonia Overlapping Histology and Confusing Terminology Smoking-related lung diseases traverse
Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited
 Insights Imaging (2017) 8:483 489 DOI 10.1007/s13244-017-0565-2 PICTORIAL REVIEW Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited Daniel B. Green 1 & Alan C. Legasto 1 & Ian
Insights Imaging (2017) 8:483 489 DOI 10.1007/s13244-017-0565-2 PICTORIAL REVIEW Pulmonary fibrosis on the lateral chest radiograph: Kerley D lines revisited Daniel B. Green 1 & Alan C. Legasto 1 & Ian
Neurofibromatosis-associated lung disease: a case series and literature review
 Eur Respir J 2007; 29: 210 214 DOI: 10.1183/09031936.06.00044006 CopyrightßERS Journals Ltd 2007 CASE STUDY Neurofibromatosis-associated lung disease: a case series and literature review A.C. Zamora*,#,+,
Eur Respir J 2007; 29: 210 214 DOI: 10.1183/09031936.06.00044006 CopyrightßERS Journals Ltd 2007 CASE STUDY Neurofibromatosis-associated lung disease: a case series and literature review A.C. Zamora*,#,+,
Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients
 Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
Respiratory Medicine (2008) 102, 307 312 Follicular bronchiolitis in surgical lung biopsies: Clinical implications in 12 patients Michelle R. Aerni a, Robert Vassallo a,, Jeffrey L. Myers b, Rebecca M.
Lung Allograft Dysfunction
 Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Lung Allograft Dysfunction Carlos S. Restrepo M.D. Ameya Baxi M.D. Department of Radiology University of Texas Health San Antonio Disclaimer: We do not have any conflict of interest or financial gain to
Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases
 CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
CASE REPORT Combined Unclassifiable Interstitial Pneumonia and Emphysema: A Report of Two Cases Nobuhiko Nagata 1, Kentaro Watanabe 2, Michihiro Yoshimi 3, Hiroshi Okabayashi 4, Katsuo Sueishi 5, Kentaro
A case of a patient with IPF treated with nintedanib. Prof. Kreuter and Prof. Heussel
 A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
A case of a patient with IPF treated with nintedanib Prof. Kreuter and Prof. Heussel Case Overview This case describes the history of a patient with IPF who, at the time of diagnosis, had symptoms typical
COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases
 COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases «If you test one smoker with cough every day You will diagnose
COPD: early detection, screening and case-finding: what is the evidence? Prof. Jan-Willem Lammers, Md PhD Department of Respiratory Diseases «If you test one smoker with cough every day You will diagnose
Monday 10 September Interstitial lung disease 15:10 15:35. The uncommon interstitial lung diseases (ILD)
 Interstitial lung disease 15:10 15:35 The uncommon interstitial lung diseases (ILD) Dr Grant Griffiths, Cwm Taf University Health Board, Cardiff Be familiar with the Diagnostic criteria for idiopathic
Interstitial lung disease 15:10 15:35 The uncommon interstitial lung diseases (ILD) Dr Grant Griffiths, Cwm Taf University Health Board, Cardiff Be familiar with the Diagnostic criteria for idiopathic
International consensus statement on idiopathic pulmonary fibrosis
 Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
Eur Respir J 2001; 17: 163 167 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 PERSPECTIVE International consensus statement on idiopathic
October 2012 Imaging Case of the Month. Michael B. Gotway, MD Associate Editor Imaging. Department of Radiology Mayo Clinic Arizona Scottsdale, AZ
 October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
October 2012 Imaging Case of the Month Michael B. Gotway, MD Associate Editor Imaging Department of Radiology Mayo Clinic Arizona Scottsdale, AZ Clinical History: A 65-year-old non-smoking woman presented
Dr. Daria Manos: Boehringer Ingelheim CSL Behring HIT Global. Dr. Horatiu Muller: No conflicts of interest
 Dr. Daria Manos: Boehringer Ingelheim CSL Behring HIT Global Dr. Horatiu Muller: No conflicts of interest Honeycombing Centrilobular emphysema (CLE) Paraseptal emphysema (PSE) Panlobular emphysema Cystic
Dr. Daria Manos: Boehringer Ingelheim CSL Behring HIT Global Dr. Horatiu Muller: No conflicts of interest Honeycombing Centrilobular emphysema (CLE) Paraseptal emphysema (PSE) Panlobular emphysema Cystic
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Idiopathic Pulmonary Fibrosis Page 1 of 10 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Idiopathic Pulmonary Fibrosis (Esbriet /pirfenidone, Ofev /nintedanib)
Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis
 Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
Original Article Nonspecific interstitial pneumonia and usual interstitial pneumonia: comparison of the clinicopathologic features and prognosis Xia Li 1, Chang Chen 2, Jinfu Xu 1, Jinming Liu 1, Xianghua
Summary: Key Learning Points, Clinical Strategies, and Future Directions
 Summary: Key Learning Points, Clinical Strategies, and Future Directions Introduction Idiopathic pulmonary fibrosis (IPF), a peripheral lobular fibrosis of unknown cause, is a chronic, progressive lung
Summary: Key Learning Points, Clinical Strategies, and Future Directions Introduction Idiopathic pulmonary fibrosis (IPF), a peripheral lobular fibrosis of unknown cause, is a chronic, progressive lung
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
HRCT in CHILDREN. strengths and weaknesses in practice: Dr Catherine Owens BSc MBBS MRCP FRCR. Great Ormond Street Hospital for Children NHS Trust
 HRCT in CHILDREN strengths and weaknesses in practice: Dr Catherine Owens BSc MBBS MRCP FRCR Great Ormond Street Hospital for Children NHS Trust London WC1N 3JH Telephone 02074059200 Ext. 0493 or 5072
HRCT in CHILDREN strengths and weaknesses in practice: Dr Catherine Owens BSc MBBS MRCP FRCR Great Ormond Street Hospital for Children NHS Trust London WC1N 3JH Telephone 02074059200 Ext. 0493 or 5072
Automated quantification of radiological patterns predicts survival in idiopathic pulmonary fibrosis
 ORIGINAL ARTICLE INTERSTITIAL LUNG DISEASES Automated quantification of radiological patterns predicts survival in idiopathic pulmonary fibrosis Fabien Maldonado 1,5, Teng Moua 1,5, Srinivasan Rajagopalan
ORIGINAL ARTICLE INTERSTITIAL LUNG DISEASES Automated quantification of radiological patterns predicts survival in idiopathic pulmonary fibrosis Fabien Maldonado 1,5, Teng Moua 1,5, Srinivasan Rajagopalan
ORIGINAL PAPER. Department of Radiology, Nagoya University Graduate School of Medicine, Nagoya, Japan 2
 Nagoya J. Med. Sci. 81. 41 53, 2019 doi:10.18999/nagjms.81.1.41 ORIGINAL PAPER Quantitative Follow-Up Assessment of Patients with Interstitial Lung Disease by 3D-Curved High-Resolution CT Imaging Parallel
Nagoya J. Med. Sci. 81. 41 53, 2019 doi:10.18999/nagjms.81.1.41 ORIGINAL PAPER Quantitative Follow-Up Assessment of Patients with Interstitial Lung Disease by 3D-Curved High-Resolution CT Imaging Parallel
Low Grade Coal Worker's Pneumoconiosis
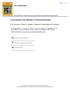 Acta Radiologica ISSN: 0284-181 (Print) 1600-04 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Low Grade Coal Worker's Pneumoconiosis P. A. Gevenois, E. Pichot, F. Dargent, S. Dedeire,
Acta Radiologica ISSN: 0284-181 (Print) 1600-04 (Online) Journal homepage: https://www.tandfonline.com/loi/iard20 Low Grade Coal Worker's Pneumoconiosis P. A. Gevenois, E. Pichot, F. Dargent, S. Dedeire,
Case 4 History. 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar
 Case 4 History 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar basilar infiltrates suggestive of pulmonary fibrosis Open
Case 4 History 58 yo man presented with prox IP joint swelling 2 months later pain and swelling in multiple joints Chest radiograph: bi-basilar basilar infiltrates suggestive of pulmonary fibrosis Open
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates
 Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Connective Tissue Disorder- Associated Interstitial Lung Disease (CTD-ILD) and Updates Maria Elena Vega, M.D Assistant Professor of Medicine Lewis Katz School of Medicine at Temple University Nothing to
Smoking-related interstitial lung disease
 Smoking-related interstitial lung disease Sergio Harari U.O. di Pneumologia UTIR Servizio di Fisiopatologia Respiratoria e Emodinamica Polmonare Ospedale S. Giuseppe MultiMedica Milano Milano, 7 Ottobre
Smoking-related interstitial lung disease Sergio Harari U.O. di Pneumologia UTIR Servizio di Fisiopatologia Respiratoria e Emodinamica Polmonare Ospedale S. Giuseppe MultiMedica Milano Milano, 7 Ottobre
Patient with IPF and no honeycombing on HRCT. Case 1 Demosthenes Bouros, Vasilios Tzilas University of Athens
 Patient with IPF and no honeycombing on HRCT Case 1 Demosthenes Bouros, Vasilios Tzilas University of Athens CASE OVERVIEW A 76-year-old male patient presented with progressive exertional dyspnoea refractory
Patient with IPF and no honeycombing on HRCT Case 1 Demosthenes Bouros, Vasilios Tzilas University of Athens CASE OVERVIEW A 76-year-old male patient presented with progressive exertional dyspnoea refractory
