Percutaneous CT-Guided Radiofrequency Ablation as Supplemental Therapy After Systemic Chemotherapy for Selected Advanced Non Small Cell Lung Cancers
|
|
|
- Derick Stone
- 5 years ago
- Views:
Transcription
1 Vascular and Interventional Radiology Original Research Li et al. Vascular and Interventional Radiology Original Research Xishan Li 1 Ming Zhao 1 Jianpeng Wang 2 Weijun Fan 1 Wang Li 1 Tao Pan 1 Peihong Wu 1 Li X, Zhao M, Wang J, et al. Keywords: chemotherapy, non small cell lung cancer, radiofrequency ablation, supplemental therapy DOI: /AJR Received December 18, 2012; accepted after revision March 8, This work was supported by the Sciences and Technology Committee of Guangdong Province (grant 2011B ). 1 Minimally Invasive Interventional Division and Medical Imaging Center, State Key Laboratory of Oncology in South China, Sun Yat-sen University Cancer Center, 651 Dongfeng Rd East, Guangzhou , P. R. China. Address correspondence to M. Zhao (zhaoming@sysucc.org.cn). 2 Minimally Invasive Interventional and Target Treatment Division and Cancer Center, The First People s Hospital of Foshan City, The Affiliated Foshan Hospital of Sun Yat-sen University, Chancheng District, Foshan, P. R. China. AJR 2013; 201: X/13/ American Roentgen Ray Society Percutaneous CT-Guided Radiofrequency Ablation as Supplemental Therapy After Systemic Chemotherapy for Selected Advanced Non Small Cell Lung Cancers OBJECTIVE. The purpose of this study is to evaluate the safety and efficacy of percutaneous CT-guided radiofrequency ablation (RFA) as a supplemental therapy after systemic chemotherapy for selected patients with advanced non small cell lung cancer (NSCLC). MATERIALS AND METHODS. We retrospectively reviewed the medical records of 220 patients with advanced NSCLC who were treated with platinum-doublet chemotherapy between January 2000 and January Among them, 49 patients underwent RFA as a supplemental therapy for tumors in partial response or stable diseases after first-line chemotherapy. The progression-free survival (PFS) was evaluated by Kaplan-Meier method. RESULTS. There were nine women and 40 men (median age, 60 years; range, years), including 28 patients with stage IIIb cancer and 21 with stage IV cancer. All 49 patients (partial response, 23 patients; stable disease, 26 patients) underwent 67 RFA sessions for 61 targeted tumors after systemic chemotherapy. There were no procedure-related deaths. Pneumothorax requiring chest tubes developed in eight sessions (11.9%). Thirty-one patients (63.3%) had complete response, 12 patients (24.5%) had partial response, six patients (12.2%) had stable disease, and no patients had progressive disease. The median follow-up period was 19 months (range, 6 34), and the median PFS was 16 weeks (95% CI, ). CONCLUSION. Percutaneous CT-guided RFA can be performed as a feasible minimally invasive supplemental therapy with satisfactory PFS after systemic chemotherapy for patients L ung cancer is the leading contributor to new cancer diagnoses and to cancer-related deaths worldwide [1]. Non small cell lung cancer (NSCLC) represents more than 85% of cases of lung cancer and accounts for most of the patients with comorbid disease or advanced stages at the time of initial diagnosis [2]. Four or six cycles of platinum-doublet chemotherapy are recommended as the first-line treatment for patients with advanced disease, resulting in response or stable disease rates of 70 80% and median overall survival (OS) of 8 12 months [3, 4], whereas most patients experience progressive disease within 2 4 months of the final chemotherapy cycle [5 7]. Efforts have focused on prolonging progression-free survival (PFS) by administering well-tolerated maintenance therapy in patients who attained tumor control after first-line chemotherapy [8, 9]. Several large randomized clinical trials have suggested that pemetrexed, erlotinib, and gefitinib used as maintenance agents can improve the PFS for selected pa- tients [6, 10 12]. However, histologic subtype or epidermal growth factor receptor (EGFR) immunohistochemistry mutation status and the adverse events related to the maintenance treatment make these agents most beneficial for special kinds of advanced NSCLC, and the disease, for the most part, still will have a dismal outcome. Radiofrequency ablation (RFA), a minimally invasive procedure, has been widely used as a viable alternative or complementary treatment option for patients with unresectable pulmonary malignancies [13 17]. The rates of complete in situ tumor necrosis achieved by RFA in lung tumors ranged from 38% to 97% (median, 90%), with a median PFS of 21 months [15]. The high local control rate, together with its characteristics of minimal invasiveness and repeatability, allow RFA to maximize coagulative necrosis of the targeted lesion and to minimize the damage to the surrounding normal pulmonary parenchyma. Furthermore, the efficacy of RFA is not affected by tumor histologic profile or 1362 AJR:201, December 2013
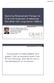
2 gene mutation status [15]. Several studies have described the synergistic effect of combination chemotherapy and RFA in treating NSCLC, and the efficacy is better than that for either treatment therapy alone [18]. All these advantages make RFA a feasible therapeutic option after systemic chemotherapy to eliminate residual tumors, to decrease the risk of chemoresistant tumor recurrence, and, ultimately, to improve PFS. RFA can be introduced as a supplemental therapy, which plays a role like that of maintenance therapy with cytotoxic or molecular-targeted agents. Some advances have been made in the RFA technique, and, because it is minimally invasive, it has been widely used clinically; however, few studies using this technique as a supplemental therapy for advanced NSCLC have been published. In this article, we retrospectively analyze our experiences with CTguided RFA for patients whose disease had not progressed after four or six cycles of chemotherapy and we evaluate the role of RFA as a supplemental therapy in treating patients Materials and Methods Patients This study was approved by the institutional review board. Written informed consent was obtained from all patients before treatment. Forty-nine patients with advanced NSCLC (nine women and 40 men; median age, 60 years; age range, years) were analyzed between January 2000 and January A total of 61 targeted tumors (mean longest diameter, 29 mm; range, mm) were treated in 67 CT-guided RFA sessions after four or six cycles of first-line chemotherapy. Patients with measurable lung tumors (with partial response or stable disease) were introduced to RFA by a multidisciplinary team comprising surgical oncologists, medical oncologists, radiation oncologists, anesthetist, and interventional oncologists. Specific inclusion criteria consisted of histologically or cytologically confirmed NSCLC, selected advanced (stage IIIb and IV) diseases, distant lung metastases controlled without progression, Eastern Cooperative Oncology Group (ECOG) performance status of 2 or less, completion of four or six cycles of platinum-doublet chemotherapy with tumors in partial response or stable diseases, the presence of at least one measurable tumor lesion, and choice of RFA as a supplemental therapy made by the patient and a multidisciplinary tumor board according to a risk-benefit analysis in patients. The exclusion criteria were maximum tumor diameter greater than 5.0 cm; more than three lesions; lesions located immediately adjacent (distance, 1.0 cm) to the pulmonary hilum, major bronchi, or major pulmonary vessels; and bleeding disorders not responding to medical treatment. The details of patient and tumor characteristics are presented in Table 1. Treatment Schedule Chemotherapy regimens Chemotherapy regimens were all platinum-doublet regimens that included cisplatin (75 80 mg/m 2 IV on day 1) plus vinorelbine (Navelbine; mg/m 2 IV on days 1 and 8) for a 3-week cycle (n = 12); cisplatin (75 mg/m 2 IV on day 1) plus gemcitabine (1250 mg/m 2 IV on days 1 and 8) for a 3-week cycle (n = 9); cisplatin (75 mg/m 2 IV on day 1) plus docetaxel (75 mg/m 2 IV on day 1) for a 3-week cycle (n = 10); and cisplatin (75 mg/m 2 IV on day 1) plus pemetrexed (500 mg/ m 2 IV on day 1) for a 3-week cycle for nonsquamous NSCLC (n = 18). Systemic chemotherapy was administered until disease progression or the patient developed intolerance to the treatment. The efficacy of systemic chemotherapy was assessed at every two cycles by revised Response Evaluation Criteria in Solid Tumors (RECIST; version 1.1) [19]. Patients with partial response or stable disease were introduced to RFA after multidisciplinary consultation. RFA procedure All the patients fasted for 12 hours. The RFA procedure was performed in a hospital CT room by two experienced interventional oncologists, an anesthetist, a technician, and a nurse. All the procedures were performed under a combination of local anesthesia and IV conscious sedation Complete Response Intense follow-up Advanced NSCLC Four or six cycles of chemotherapy Partial Response CT-guided RFA with ECG, blood pressure, and saturation of blood oxygen monitoring during the whole procedure. RFA was administered using two different radiofrequency systems and needle electrodes: a monopolar electrode system (Cool-Tip, Valleylab) under an impedance-control algorithm with an internally cooled electrode (17 gauge, 1.5-mm diameter, and a 3.0-cm exposed metallic active portion) and a multitined deployable electrode system (RITA Starburst XL, RITA Medical Systems) under a temperature-controlled algorithm with an umbrella-shaped electrode (16 gauge, 1.7-mm diameter, and an effective ablation area of 4.0 cm at full expansion). The type of device and electrode used was dependent on commercial availability and on the size of the target tumor. The electrode was carefully introduced into the optimal locations at a predetermined angle in a stepwise manner under CT guidance. The power settings and exposure times were selected according to the standard recommendations provided by the manufacturers of the equipment used and according to the experience of previous tumor RFA procedures [20, 21]. The process was targeted to achieve an overlapping ablative margin that would theoretically include the tumor and cm of surrounding tissue to eradicate microscopic foci of disease. In each treatment, tract ablation to prevent possible tumor seeding or tract bleeding was performed before the electrode was withdrawn. After ablation, an additional CT scan was performed for postprocedure surveillance, which showed no evidence of complications. A multidisciplinary tumor board Evaluated by RECIST 1.1 Stable Disease Four weeks later evaluated by modified RECIST Progressive Disease Complete Response Partial Response Stable Disease Progressive Disease Surveillance Additional RFA Second-line chemotherapy, molecularly targeted agent, or palliative treatment Fig. 1 Flowchart showing treatment algorithm used for patients with advanced non small cell lung cancer (NSCLC) in present study. RECIST = Response Evaluation Criteria in Solid Tumors, RFA = radiofrequency ablation. AJR:201, December
3 Li et al. TABLE 1: Univariate Analysis by Log-Rank Test for Prognostic Clinicopathologic and Procedure-Related Factors for Progression-Free Survival (PFS) Characteristic No. (%) of Patients Median PFS (Weeks) p Sex Male 40 (81.6) 16 Female 9 (18.4) 20 Age (y) (63.3) 17 > (36.7) 16 Smoking history < Never-smoker 22 (44.9) 21 Smoker 27 (55.1) 14 ECOG performance status < (14.3) (79.6) (6.1) 12 Histologic subtype Squamous cell carcinoma 20 (40.8) 16 Adenocarcinoma 26 (53.1) 17 Others 3 (6.1) 14 Stage IIIb 28 (57.1) 21 IV 21 (42.9) 14 Response to previous chemotherapy Partial response 23 (46.9) 16 Stable disease 26 (53.1) 17 Measurable tumor at first RFA Distribution Unilateral 31 (63.3) 20 Bilateral 18 (36.7) 14 Location Central 6 (12.2) 14 Peripheral 43 (87.8) 17 Maximum diameter (cm) (61.2) (38.8) 14 Number of tumors < (85.7) 17 > 1 7 (14.3) 14 Response to initial RFA < Complete response 31 (63.3) 21 Partial response 12 (24.5) 14 Stable disease 6 (12.2) 12 Progressive disease 0 0 Note ECOG = Eastern Cooperative Oncology Group, RFA = radiofrequency ablation. Assessment and Follow-Up The follow-up evaluations were performed at 1, 3, 6, 9, and 12 months after ablation and at 6-month intervals thereafter with radiologic and clinical examinations. The follow-up radiologic examinations were mainly contrast-enhanced three-phase CT scans. Additional examinations, such as PET/ CT scans, were performed to further evaluate the results if the CT scan and tumor marker analyses were insufficient for diagnosis, such as in the case of a local suspicious relapse or possible extrapulmonary metastasis. The target tumor s response to RFA was evaluated by use of the modified RECIST, as described elsewhere [17, 22, 23]. Additional RFA was performed for patients with a partial response or stable disease response to RFA. During the whole study, patients with a complete response after treatment were intensely followed up. For patients with progressive disease after the last RFA session, second-line chemotherapy with a molecular-targeted agent or palliative treatments were performed according to the recommendation of a multidisciplinary evaluation on the basis of a risk-benefit analysis in patients (more details are shown in Fig. 1). Statistical Analysis Follow-up was calculated from the date of last RFA session to the date of the last follow-up. PFS was defined as the time from the day of the last RFA session to the time of recurrence or detection of a newly metastatic lesion, or death for any reason (recorded according to the first event). OS was calculated from the first day of diagnosis to either the day of death from any cause or the last follow-up. The PFS and OS were estimated with the Kaplan-Meier method. Univariate analysis (log-rank) was performed to determine the prognostic factors for PFS. Multivariate analysis was performed on all factors with p less than 0.10 by using the Cox proportional hazards regression model. Because of the heterogeneity of the follow-up treatments after the progression of the disease, the prognostic factors associated with OS were not analyzed in this study. All analyses were performed using SPSS software (version 16.0, SPSS). A p value of 0.05 or less was considered statistically significant. Results Complications No death was related to the RFA procedure. The major complication was symptomatic pneumothorax requiring chest tube placement, which occurred in eight of 67 (11.9%) RFA sessions. Minor complications (19.4% [13/67]), including self-limited minor pneumothorax, slight cough, a low-grade fever ( 38.5 C), and local pain at the puncture site, were well tolerated and easily controlled AJR:201, December 2013
4 Local Efficacy Patients successfully underwent 67 RFA sessions after systemic chemotherapy. Thirty-six sessions were performed with a multitined deployable electrode system, and 31 were performed with a monopolar electrode system. At 1-month follow-up after initial RFA, 31 patients (63.3%) had a complete response, 12 patents (24.5%) had a partial response, six patients (12.2%) had stable disease, and no patients had progressive disease. For patients with partial response and stable disease, RFA was repeated. Survival During the median follow-up period after the last lung RFA session of 19 months (range, 6 34 months), 41 (83.7%) patients died and eight (16.3%) patients were still alive. The causes of death were intrapulmonary progression (n = 21), adrenal metastasis (n = 2), bone metastasis (n = 5), brain metastasis (n = 4), multiple systemic (more than two organs) metastases (n = 6), respiratory failure (n = 1), and pneumonia (n = 2). For all intention-totreat patients, the median PFS and OS were 16 weeks (95% CI, ) and 14 months (95% CI, 13 15), respectively. Factors associated with PFS identified through univariate analysis are shown in Table 1. From the multivariate analysis, ECOG performance status (hazard ratio, 2.545; 95% CI, ; p = 0.030) and response to treatment (hazard ratio, 7.244; 95% CI, ; p < ) were independent predictors for PFS (details are shown in Table 2 and Fig. 2). TABLE 2: Cox Regression Multivariate Analysis (Method = Enter) of Prognostic Factors for Progression-Free Survival (PFS) Discussion The current standard first-line therapy for advanced NSCLC is four or six cycles of platinum-based chemotherapy [4]. Although 70 80% of patients who undergo chemotherapy receive clinical benefits in terms of response or stable disease, the PFS and OS profile remains poor. For decades, the standard of care was a watch-and-wait approach after initial therapy, and then patients with NSCLC with a good performance status were offered second-line treatment at progression of disease. To date, accumulated evidence has shown that maintenance therapy with either a continuous or a switch strategy is a beneficial treatment with improved PFS ( months) [6, 11, 12, 24]. However, evidence from the SATURN study [11] shows that erlotinib has a better PFS for patients with an activating EGFR mutation status, and the PARAMOUNT study [6] emphasizes that pemetrexed is more approved for use in the nonsquamous subset on the basis of its efficacy and PFS, which might limit the benefit of maintenance therapy for selected patients RFA has been accepted as a therapeutic option, with safety, feasibility, and anticancer efficacy, for patients with NSCLC who are not candidates for curative surgical resection [13 16]. In previous studies [18], improved local disease control and increased survival rate were observed when combined chemotherapy and RFA were used for treating NSCLC. Lee et al. [18] reported that the median survival times for patients with NSCLC (stage III to IV) treated with chemotherapy and RFA, chemotherapy alone, and RFA alone were 42, 29, and 13.6 months, respectively, which indicated that RFA followed by conventional chemotherapy is feasible as a sequential therapy PFS Rate (%) Factors p < Time (wk) ECOG performance status censored censored censored A for patients However, there are no reports about RFA playing a role as a maintenance therapy after systemic chemotherapy in patients with advanced NSCLC. In our study, the survival benefit was preceded by delaying tumor progression, with PFS of 16 weeks, which is consistent with the reported maintenance therapeutic agents of months. These promising results indicate that the therapeutic efficacy of RFA is a feasible therapeutic option as a supplemental therapy after systemic chemotherapy in advanced NSCLC. In the analysis of factors associated with PFS and OS, ECOG performance status and response to RFA were correlated with PFS outcome. Patients with ECOG performance status 0 and complete response to RFA may benefit from RFA during the supplemental therapy period. There were no variables that PFS Rate (%) p < Time (wk) Response Complete Response Partial Response Stable Disease CR-censored PR-censored SD-censored Fig. 2 Univariate analysis (log-rank) was performed to determine prognostic factors for progression-free survival (PFS). A, Log-rank analysis of PFS stratified according to Eastern Cooperative Oncology Group (ECOG) performance status (p < ). B, Log-rank analysis of PFS stratified according to response to radiofrequency ablation (p < ). PFS HR 95% CI p Never-smoker vs smoker ECOG performance status, 0 vs 1 vs Stage, IIIb vs IV Distribution, unilateral vs bilateral Maximum diameter, 3 vs 3~5 cm Number, 1 vs > Response to initial RFA, CR vs PR vs SD vs PD < B AJR:201, December
5 Li et al. could predict for OS. Hence, it appears that RFA may be useful in decreasing the rate of tumor recurrence and progression and then improving the PFS outcomes, but as a monotherapy, it may not be sufficient to achieve satisfactory OS. This finding reiterates the importance of combining RFA with systemic therapies to improve survival in patients with advanced NSCLC. RFA may have several theoretic advantages as a supplemental therapy after systemic chemotherapy in patients First, RFA induced coagulation necrosis and cell death destruction of the centrally located hypoxic tumor, which is typically less responsive to chemotherapy. Second, as shown in our study, the cytoreduction induced by RFA eradicates the viable tumor cells without damage to the surrounding nontumoral lung parenchyma and without the toxicity caused by cytotoxic or molecular-targeted agents used in maintenance therapy. Third, RFA can enhance the therapeutic effectiveness of second-line chemotherapy for patients with tumor progression. Studies have shown that tumor volume was associated with local control and OS of patients treated with chemotherapy [25]. RFA can induce in situ thermal injury of the bulky tumor mass with coagulation necrosis, which can produce a chemotherapy-sensitizing effect in the second-line chemotherapy courses. Several studies have proven the synergistic effect of the combination of RFA and chemotherapy [18, 26 28]. In addition, the efficacy of RFA in NSCLC is irrespective of EGFR mutation status or histologic subtype [15], which has much broader applications. Finally, RFA can eradicate in situ the residual tumor after systemic chemotherapy with satisfactory PFS, which, in the biopsychosocial medical model, is easier for patients to accept. Percutaneous CT-guided RFA is a safe procedure. The most commonly reported complication after RFA was pneumothorax, which was mainly encountered in elderly patients with chronic obstructive pulmonary disease, with an incidence of about % [15, 29]. Most cases of pneumothorax were selflimiting, and only % (median, 11%) of cases required chest drain insertion. Symptomatic pneumothorax can be easily handled with closed pleural cavity drainage for less than 24 hours (range, 1 3 days). Less common complications, including chest pain and postoperative fever, are tolerable and easily resolved. In the current study, procedure-related complications were infrequent; the most frequent major complication was pneumothorax in ablating lung lesions larger than 3.0 cm, and the incidence was similar to those reported in previous studies [15, 29]. Other reported procedure-related complications, such as pneumonia, hemorrhage, and tumor seeding along the needle tract, were not observed in this study. On the basis of our preliminary results, we consider RFA a safe and well-tolerated procedure in the treatment of NSCLC as a supplemental therapy after systemic chemotherapy. Patients who have contraindications to cytotoxic or molecular-targeted maintenance therapy, or who are unable to tolerate the adverse events, or who are unwilling to receive these treatments could be recommended to undergo the RFA procedure. Our study has some potential limitations. First, this is a retrospective study with a small sample size, which limits the value of the findings, although the preliminary results show that RFA as a supplemental therapy is a safe therapeutic option with promising long-term PFS for advanced NSCLC. Because RFA has rarely been reported as a supplemental therapy after four or six cycles of first-line chemotherapy for advanced NSCLC clinically, we think that those promising outcomes will add to the evidence-based medicine in this field and contribute to the conduct of prospective studies with larger samples to further validate the efficacy. Second, limited by our strict matching criteria, we could not do matched-pair analysis for RFA and conventional cytotoxic or moleculartargeted agents. However, RFA would appear from our experience to be a promising alternative to conventional maintenance therapeutic agents for selected patients with advanced NSCLC. Third, we used two commercially available RFA systems, and all treatments were performed according to the manufacturer s recommended protocol. As a retrospective study, it was hard to collect completely related data and to analyze the differing efficacies between the two systems. In summary, percutaneous CT-guided RFA, as a minimally invasive therapeutic option, is safe and effective as a supplemental therapy after systemic chemotherapy for selected patients References 1. Dela Cruz CS, Tanoue LT, Matthay RA. Lung cancer: epidemiology, etiology, and prevention. Clin Chest Med 2011; 32: Yang P, Allen MS, Aubry MC, et al. Clinical features of 5,628 primary lung cancer patients: experience at Mayo Clinic from 1997 to Chest 2005; 128: Goffin J, Lacchetti C, Ellis PM, Ung YC, Evans WK. First-line systemic chemotherapy in the treatment of advanced non-small cell lung cancer: a systematic review. J Thorac Oncol 2010; 5: Azzoli CG, Temin S, Aliff T, et al focused update of 2009 American Society of Clinical Oncology clinical practice guideline update on chemotherapy for stage IV non-small-cell lung cancer. J Clin Oncol 2011; 29: Fidias PM, Dakhil SR, Lyss AP, et al. Phase III study of immediate compared with delayed docetaxel after front-line therapy with gemcitabine plus carboplatin in advanced non-smallcell lung cancer. J Clin Oncol 2009; 27: Paz-Ares L, de Marinis F, Dediu M, et al. Maintenance therapy with pemetrexed plus best supportive care versus placebo plus best supportive care after induction therapy with pemetrexed plus cisplatin for advanced non-squamous non-small-cell lung cancer (PARAMOUNT): a double-blind, phase 3, randomised controlled trial. Lancet Oncol 2012; 13: Brodowicz T, Krzakowski M, Zwitter M, et al. Cisplatin and gemcitabine first-line chemotherapy followed by maintenance gemcitabine or best supportive care in advanced non-small cell lung cancer: a phase III trial. Lung Cancer 2006; 52: Gridelli C, Maione P, Rossi A, et al. Potential treatment options after first-line chemotherapy for advanced NSCLC: maintenance treatment or early second-line? Oncologist 2009; 14: Grossi F. Management of non-small cell lung in cancer patients with stable disease. Drugs 2012; 72(suppl 1): Ciuleanu T, Brodowicz T, Zielinski C, et al. Maintenance pemetrexed plus best supportive care versus placebo plus best supportive care for non-smallcell lung cancer: a randomised, double-blind, phase 3 study. Lancet 2009; 374: Cappuzzo F, Ciuleanu T, Stelmakh L, et al.; SAT- URN Investigators. Erlotinib as maintenance treatment in advanced non-small-cell lung cancer: a multicentre, randomised, placebo-controlled phase 3 study. Lancet Oncol 2010; 11: Zhang L, Ma S, Song X, et al. Gefitinib versus placebo as maintenance therapy in patients with locally advanced or metastatic non-small-cell lung cancer (INFORM; C-TONG 0804): a multicentre, double-blind randomised phase 3 trial. Lancet Oncol 2012; 13: Simon CJ, Dupuy DE, DiPetrillo TA, et al. Pulmonary radiofrequency ablation: long-term safety and efficacy in 153 patients. Radiology 2007; 243: Lencioni R, Crocetti L, Cioni R, et al. Response to radiofrequency ablation of pulmonary tumours: a prospective, intention-to-treat, multicentre clinical trial (the RAPTURE study). Lancet Oncol 1366 AJR:201, December 2013
6 2008; 9: tients with liver metastases from nasopharyngeal cell lung cancer treated with chemoradiotherapy. 15. Zhu JC, Yan TD, Morris DL. A systematic review carcinoma. Int J Hyperthermia 2011; 27: Int J Radiat Oncol Biol Phys 2011; 79: of radiofrequency ablation for lung tumors. Ann 21. Zhao M, Wang JP, Pan CC, et al. CT-guided radio- 26. Elias D, Baton O, Sideris L, et al. Hepatectomy Surg Oncol 2008; 15: frequency ablation after with transarterial chemo- plus intraoperative radiofrequency ablation and 16. Dupuy DE. Image-guided thermal ablation of embolization in treating unresectable hepatocellular chemotherapy to treat technically unresectable lung malignancies. Radiology 2011; 260: Li X, Wang J, Li W, et al. Percutaneous CT-guided radiofrequency ablation for unresectable hepatocellular carcinoma pulmonary metastases. Int J Hyperthermia 2012; 28: Lee H, Jin GY, Han YM, et al. Comparison of survival rate in primary non-small-cell lung cancer among elderly patients treated with radiofrequency ablation, surgery, or chemotherapy. Cardiovasc Intervent Radiol 2012; 35: Eisenhauer EA, Therasse P, Bogaerts J, et al. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer 2009; 45: Pan C, Wu P, Yu J, et al. CT-guided radiofrequency ablation prolonged metastatic survival in pa- carcinoma with long overall survival improvement. Eur J Radiol 2012; 81: Fernando HC, De Hoyos A, Landreneau RJ, et al. Radiofrequency ablation for the treatment of nonsmall cell lung cancer in marginal surgical candidates. J Thorac Cardiovasc Surg 2005; 129: Pennathur A, Abbas G, Qureshi I, et al. Radiofrequency ablation for the treatment of pulmonary metastases. Ann Thorac Surg 2009; 87: ; discussion, Zhang X, Zang J, Xu J, et al. Maintenance therapy with continuous or switch strategy in advanced non-small cell lung cancer: a systematic review and meta-analysis. Chest 2011; 140: Alexander BM, Othus M, Caglar HB, Allen AM. Tumor volume is a prognostic factor in non-small- multiple colorectal liver metastases. J Surg Oncol 2005; 90: Carrafiello G, Fontana F, Cotta E, et al. Ultrasound-guided thermal radiofrequency ablation (RFA) as an adjunct to systemic chemotherapy for breast cancer liver metastases. Radiol Med (Torino) 2011; 116: Jin Y, Cai YC, Cao Y, et al. Radiofrequency ablation combined with systemic chemotherapy in nasopharyngeal carcinoma liver metastases improves response to treatment and survival outcomes. J Surg Oncol 2012; 106: Kashima M, Yamakado K, Takaki H, et al. Complications after 1000 lung radiofrequency ablation sessions in 420 patients: a single center s experiences. AJR 2011; 197:W576 W580 AJR:201, December
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer
 Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Radiofrequency ablation combined with conventional radiotherapy: a treatment option for patients with medically inoperable lung cancer Poster No.: C-0654 Congress: ECR 2011 Type: Scientific Paper Authors:
Maintenance paradigm in non-squamous NSCLC
 Maintenance paradigm in non-squamous NSCLC L. Paz-Ares Hospital Universitario Virgen del Rocío Sevilla Agenda Theoretical basis The data The comparisons Agenda Theoretical basis The data The comparisons
Maintenance paradigm in non-squamous NSCLC L. Paz-Ares Hospital Universitario Virgen del Rocío Sevilla Agenda Theoretical basis The data The comparisons Agenda Theoretical basis The data The comparisons
EGFR inhibitors in NSCLC
 Suresh S. Ramalingam, MD Associate Professor Director of Medical Oncology Emory University i Winship Cancer Institute EGFR inhibitors in NSCLC Role in 2nd/3 rd line setting Role in first-line and maintenance
Suresh S. Ramalingam, MD Associate Professor Director of Medical Oncology Emory University i Winship Cancer Institute EGFR inhibitors in NSCLC Role in 2nd/3 rd line setting Role in first-line and maintenance
Percutaneous Radiofrequency Ablation of Lung Malignant Tumours: Survival, disease progression and complication rates
 Percutaneous Radiofrequency Ablation of Lung Malignant Tumours: Survival, disease progression and complication rates Poster No.: C-2576 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit
Percutaneous Radiofrequency Ablation of Lung Malignant Tumours: Survival, disease progression and complication rates Poster No.: C-2576 Congress: ECR 2012 Type: Authors: Keywords: DOI: Scientific Exhibit
Targeted Agents as Maintenance Therapy. Karen Kelly, MD Professor of Medicine UC Davis Cancer Center
 Targeted Agents as Maintenance Therapy Karen Kelly, MD Professor of Medicine UC Davis Cancer Center Disclosures Genentech Advisory Board Maintenance Therapy Defined Treatment Non-Progressing Patients Drug
Targeted Agents as Maintenance Therapy Karen Kelly, MD Professor of Medicine UC Davis Cancer Center Disclosures Genentech Advisory Board Maintenance Therapy Defined Treatment Non-Progressing Patients Drug
Cancer Cell Research 14 (2017)
 Available at http:// www.cancercellresearch.org ISSN 2161-2609 Efficacy and safety of bevacizumab for patients with advanced non-small cell lung cancer Ping Xu, Hongmei Li*, Xiaoyan Zhang Department of
Available at http:// www.cancercellresearch.org ISSN 2161-2609 Efficacy and safety of bevacizumab for patients with advanced non-small cell lung cancer Ping Xu, Hongmei Li*, Xiaoyan Zhang Department of
MAINTENANCE TREATMENT CHEMO MAINTENANCE OR TARGETED OF BOTH? Martin Reck Department of Thoracic Oncology LungenClinic Grosshansdorf
 MAINTENANCE TREATMENT CHEMO MAINTENANCE OR TARGETED OF BOTH? Martin Reck Department of Thoracic Oncology LungenClinic Grosshansdorf OUTLINE Background and Concept Switch Maintenance Continuation Maintenance
MAINTENANCE TREATMENT CHEMO MAINTENANCE OR TARGETED OF BOTH? Martin Reck Department of Thoracic Oncology LungenClinic Grosshansdorf OUTLINE Background and Concept Switch Maintenance Continuation Maintenance
Survival of patients with advanced lung adenocarcinoma before and after approved use of gefitinib in China
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Survival of patients with advanced lung adenocarcinoma before and after approved use of gefitinib in China Yu-Tao Liu, Xue-Zhi Hao, Jun-Ling Li, Xing-Sheng
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Survival of patients with advanced lung adenocarcinoma before and after approved use of gefitinib in China Yu-Tao Liu, Xue-Zhi Hao, Jun-Ling Li, Xing-Sheng
Maintenance Therapy for Advanced NSCLC: When, What, Why & What s Left After Post-Maintenance Relapse?
 Maintenance Therapy for Advanced NSCLC: When, What, Why & What s Left After Post-Maintenance Relapse? Mark A. Socinski, MD Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive
Maintenance Therapy for Advanced NSCLC: When, What, Why & What s Left After Post-Maintenance Relapse? Mark A. Socinski, MD Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive
Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer
 Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
Original Article Ratio of maximum standardized uptake value to primary tumor size is a prognostic factor in patients with advanced non-small cell lung cancer Fangfang Chen 1 *, Yanwen Yao 2 *, Chunyan
EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence
 102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
102 Journal of Cancer Research Updates, 2012, 1, 102-107 EGFR Tyrosine Kinase Inhibitors Prolong Overall Survival in EGFR Mutated Non-Small-Cell Lung Cancer Patients with Postsurgical Recurrence Kenichi
Maintenance therapy in advanced non-small cell lung cancer. Egbert F. Smit MD PhD Dept Thoracic Oncology Netherlands Cancer Institute
 Maintenance therapy in advanced non-small cell lung cancer. Egbert F. Smit MD PhD Dept Thoracic Oncology Netherlands Cancer Institute e.smit@nki.nl Evolution of front line therapy in NSCLC unselected pts
Maintenance therapy in advanced non-small cell lung cancer. Egbert F. Smit MD PhD Dept Thoracic Oncology Netherlands Cancer Institute e.smit@nki.nl Evolution of front line therapy in NSCLC unselected pts
Technology appraisal guidance Published: 29 June 2011 nice.org.uk/guidance/ta227
 Erlotinib monotherapy for maintenance treatment of non-small-cell lung cancer Technology appraisal guidance Published: 29 June 2011 nice.org.uk/guidance/ta227 NICE 2018. All rights reserved. Subject to
Erlotinib monotherapy for maintenance treatment of non-small-cell lung cancer Technology appraisal guidance Published: 29 June 2011 nice.org.uk/guidance/ta227 NICE 2018. All rights reserved. Subject to
Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients: Patient Characteristics and Type of Chemotherapy
 SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation
 Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation Katie S. Nason, MD MPH AATS Focus on Thoracic: Mastering Surgical Innovation October 28, 2017 No disclosures Radiofrequency ablative
Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation Katie S. Nason, MD MPH AATS Focus on Thoracic: Mastering Surgical Innovation October 28, 2017 No disclosures Radiofrequency ablative
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER. Virginie Westeel Chest Disease Department University Hospital Besançon, France
 PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
PERIOPERATIVE TREATMENT OF NON SMALL CELL LUNG CANCER Virginie Westeel Chest Disease Department University Hospital Besançon, France LEARNING OBJECTIVES 1. To understand the potential of perioperative
Maintenance Therapy for Advanced NSCLC: Which Patients, Which Approach?
 Maintenance Therapy for Advanced NSCLC: Which Patients, Which Approach? Mark A. Socinski, MD Visiting Professor of Medicine and Thoracic Surgery Director, Lung Cancer Section, Division of Hematology/Oncology
Maintenance Therapy for Advanced NSCLC: Which Patients, Which Approach? Mark A. Socinski, MD Visiting Professor of Medicine and Thoracic Surgery Director, Lung Cancer Section, Division of Hematology/Oncology
RFA of Tumors of the Lung: How and Why. Radiofrequency Ablation. Radiofrequency Ablation. RFA of pulmonary metastases. Radiofrequency Ablation of Lung
 RFA of Tumors of the Lung: How and Why Radiofrequency Ablation of Lung Ernest Scalzetti MD SUNY Upstate Medical University Syracuse NY FDA WARNING: Off-label use of a medical device Radiofrequency Ablation
RFA of Tumors of the Lung: How and Why Radiofrequency Ablation of Lung Ernest Scalzetti MD SUNY Upstate Medical University Syracuse NY FDA WARNING: Off-label use of a medical device Radiofrequency Ablation
Platinum-containing first-line chemotherapy has improved
 Original Article PARAMOUNT: Descriptive Subgroup Analyses of Final Overall Survival for the Phase III Study of Maintenance Pemetrexed versus Placebo Following Induction Treatment with Pemetrexed Plus Cisplatin
Original Article PARAMOUNT: Descriptive Subgroup Analyses of Final Overall Survival for the Phase III Study of Maintenance Pemetrexed versus Placebo Following Induction Treatment with Pemetrexed Plus Cisplatin
Radiofrequency Ablation (RFA) For Lung Tumors: Seven Years Experience.
 Radiofrequency Ablation (RFA) For Lung Tumors: Seven Years Experience. Poster No.: C-1619 Congress: ECR 2011 Type: Scientific Exhibit Authors: G. DE VENUTO 1, G. XHEPA 1, M. DE CHIARA 1, M. Mangini 2,
Radiofrequency Ablation (RFA) For Lung Tumors: Seven Years Experience. Poster No.: C-1619 Congress: ECR 2011 Type: Scientific Exhibit Authors: G. DE VENUTO 1, G. XHEPA 1, M. DE CHIARA 1, M. Mangini 2,
Percutaneous Ultrasound-guided Radiofrequency Ablation of Colorectal Liver Metastases
 Chin J Radiol 2005; 30: 153-158 153 Percutaneous Ultrasound-guided Radiofrequency Ablation of Colorectal Liver Metastases YI-YOU CHIOU YI-HONG CHOU JEN-HUEY CHIANG HSIN-KAI WANG CHENG-YEN CHANG Department
Chin J Radiol 2005; 30: 153-158 153 Percutaneous Ultrasound-guided Radiofrequency Ablation of Colorectal Liver Metastases YI-YOU CHIOU YI-HONG CHOU JEN-HUEY CHIANG HSIN-KAI WANG CHENG-YEN CHANG Department
Complications of percutaneous lung radiofrequency ablation
 Complications of percutaneous lung radiofrequency ablation Poster No.: C-556 Congress: ECR 2009 Type: Educational Exhibit Topic: Interventional Radiology Authors: A. Afaq, S. Khan, U. Patel, E. Leen; London/UK
Complications of percutaneous lung radiofrequency ablation Poster No.: C-556 Congress: ECR 2009 Type: Educational Exhibit Topic: Interventional Radiology Authors: A. Afaq, S. Khan, U. Patel, E. Leen; London/UK
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW. Erlotinib for the third or fourth-line treatment of NSCLC January 2012
 Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
Disease background LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Erlotinib for the third or fourth-line treatment of NSCLC January 2012 Lung cancer is the second most common cancer in the UK (after breast),
Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010
 LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
LSU HEALTH SCIENCES CENTER NSCLC Guidelines Feist-Weiller Cancer Center Molly Boyd, MD Glenn Mills, MD Syed Jafri, MD 1/1/2010 Initial Evaluation/Intervention: 1. Pathology Review 2. History and Physical
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective
 Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Slide 1. Slide 2 Maintenance Therapy Options. Slide 3. Maintenance Therapy in the Management of Non-Small Cell Lung Cancer. Maintenance Chemotherapy
 Slide 1 Maintenance Therapy in the Management of Non-Small Cell Lung Cancer Frances A Shepherd, MD FRCPC Scott Taylor Chair in Lung Cancer Research Princess Margaret Hospital, Professor of Medicine, University
Slide 1 Maintenance Therapy in the Management of Non-Small Cell Lung Cancer Frances A Shepherd, MD FRCPC Scott Taylor Chair in Lung Cancer Research Princess Margaret Hospital, Professor of Medicine, University
Ludger Sellmann 1, Klaus Fenchel 2, Wolfram C. M. Dempke 3,4. Editorial
 Editorial Improved overall survival following tyrosine kinase inhibitor treatment in advanced or metastatic non-small-cell lung cancer the Holy Grail in cancer treatment? Ludger Sellmann 1, Klaus Fenchel
Editorial Improved overall survival following tyrosine kinase inhibitor treatment in advanced or metastatic non-small-cell lung cancer the Holy Grail in cancer treatment? Ludger Sellmann 1, Klaus Fenchel
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist
 Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Practice changing studies in lung cancer 2017
 1 Practice changing studies in lung cancer 2017 Rolf Stahel University Hospital of Zürich Cape Town, February 16, 2018 DISCLOSURE OF INTEREST Consultant or Advisory Role in the last two years I have received
1 Practice changing studies in lung cancer 2017 Rolf Stahel University Hospital of Zürich Cape Town, February 16, 2018 DISCLOSURE OF INTEREST Consultant or Advisory Role in the last two years I have received
RF Ablation: indication, technique and imaging follow-up
 RF Ablation: indication, technique and imaging follow-up Trongtum Tongdee, M.D. Radiology Department, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand Objective Basic knowledge
RF Ablation: indication, technique and imaging follow-up Trongtum Tongdee, M.D. Radiology Department, Faculty of Medicine, Siriraj Hospital, Mahidol University, Bangkok, Thailand Objective Basic knowledge
Supplementary Material
 1 Supplementary Material 3 Tumour Biol. 4 5 6 VCP Gene Variation Predicts Outcome of Advanced Non-Small-Cell Lung Cancer Platinum-Based Chemotherapy 7 8 9 10 Running head: VCP variation predicts NSCLC
1 Supplementary Material 3 Tumour Biol. 4 5 6 VCP Gene Variation Predicts Outcome of Advanced Non-Small-Cell Lung Cancer Platinum-Based Chemotherapy 7 8 9 10 Running head: VCP variation predicts NSCLC
Plotting the course: optimizing treatment strategies in patients with advanced adenocarcinoma
 Pieter E. Postmus University of Liverpool Liverpool, UK Plotting the course: optimizing treatment strategies in patients with advanced adenocarcinoma Disclosures Advisor Bristol-Myers Squibb AstraZeneca
Pieter E. Postmus University of Liverpool Liverpool, UK Plotting the course: optimizing treatment strategies in patients with advanced adenocarcinoma Disclosures Advisor Bristol-Myers Squibb AstraZeneca
Single Technology Appraisal (STA)
 Single Technology Appraisal (STA) Durvalumab for maintenance treatment of locally advanced unresectable non-small cell lung cancer that has not progressed after platinum-based chemoradiation therapy Response
Single Technology Appraisal (STA) Durvalumab for maintenance treatment of locally advanced unresectable non-small cell lung cancer that has not progressed after platinum-based chemoradiation therapy Response
Published: Address correspondence to Vidal-Jove Joan:
 Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
Oncothermia Journal 7:111-114 (2013) Complete responses after hyperthermic ablation by ultrasound guided high intensity focused ultrasound (USgHIFU) plus cystemic chemotherapy (SC) for locally advanced
LUNG CANCER. Agnieszka Słowik, MD. Department of Oncology, University Hospital in Cracow Jagiellonian University
 LUNG CANCER Agnieszka Słowik, MD Department of Oncology, University Hospital in Cracow Jagiellonian University Epidemiology Most common malignancy worldwide Place of lung cancer among other malignancies
LUNG CANCER Agnieszka Słowik, MD Department of Oncology, University Hospital in Cracow Jagiellonian University Epidemiology Most common malignancy worldwide Place of lung cancer among other malignancies
Personalized maintenance therapy in advanced non-small cell lung cancer
 China Lung Cancer Research Highlight Personalized maintenance therapy in advanced non-small cell lung cancer Kazuhiro Asami, Kyoichi Okishio, Tomoya Kawaguchi, Shinji Atagi Department of Clinical Oncology,
China Lung Cancer Research Highlight Personalized maintenance therapy in advanced non-small cell lung cancer Kazuhiro Asami, Kyoichi Okishio, Tomoya Kawaguchi, Shinji Atagi Department of Clinical Oncology,
Utility of 18 F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer
 Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Utility of F-FDG PET/CT in metabolic response assessment after CyberKnife radiosurgery for early stage non-small cell lung cancer Ngoc Ha Le 1*, Hong Son Mai 1, Van Nguyen Le 2, Quang Bieu Bui 2 1 Department
Systemic Treatment for Patients with Advanced Non-Small Cell Lung Cancer P.M. Ellis, E.T. Vella, Y.C. Ung and the Lung Cancer Disease Site Group
 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Systemic Treatment for Patients with Advanced Non-Small Cell Lung Cancer P.M. Ellis, E.T. Vella, Y.C. Ung and
A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Systemic Treatment for Patients with Advanced Non-Small Cell Lung Cancer P.M. Ellis, E.T. Vella, Y.C. Ung and
Saudi Journal of Medicine (SJM)
 Saudi Journal of Medicine (SJM) Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-3389 (Print) ISSN 2518-3397 (Online) Overview of Non-Squamous Cell
Saudi Journal of Medicine (SJM) Scholars Middle East Publishers Dubai, United Arab Emirates Website: http://scholarsmepub.com/ ISSN 2518-3389 (Print) ISSN 2518-3397 (Online) Overview of Non-Squamous Cell
The road less travelled: what options are available for patients with advanced squamous cell carcinoma?
 Robert Pirker Medical University of Vienna Vienna, Austria The road less travelled: what options are available for patients with advanced squamous cell carcinoma? Disclosures Honoraria for advisory board/consulting
Robert Pirker Medical University of Vienna Vienna, Austria The road less travelled: what options are available for patients with advanced squamous cell carcinoma? Disclosures Honoraria for advisory board/consulting
Correspondence should be addressed to Kumar Prabhash;
 Hindawi Chemotherapy Research and Practice Volume 2017, Article ID 8196434, 4 pages https://doi.org/10.1155/2017/8196434 Clinical Study Efficacy of Second-Line Pemetrexed-Carboplatin in EGFR-Activating
Hindawi Chemotherapy Research and Practice Volume 2017, Article ID 8196434, 4 pages https://doi.org/10.1155/2017/8196434 Clinical Study Efficacy of Second-Line Pemetrexed-Carboplatin in EGFR-Activating
in combination with cisplatin as first-line doublet 3 as maintenance agent following non-pemetrexed platinum doublet 4
 Overall survival (OS) results from PARAMOUNT study of maintenance plus best supportive care (BSC) versus plus BSC, immediately after induction with - Cisplatin, in patients with advanced Nonsquamous Non-small
Overall survival (OS) results from PARAMOUNT study of maintenance plus best supportive care (BSC) versus plus BSC, immediately after induction with - Cisplatin, in patients with advanced Nonsquamous Non-small
Is Bevacizumab (Avastin) Safe and Effective as Adjuvant Chemotherapy for Adult Patients With Stage IIIb or IV Non-Small Cell Lung Carcinoma (NSCLC)?
 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Bevacizumab (Avastin) Safe and Effective
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2014 Is Bevacizumab (Avastin) Safe and Effective
OUR EXPERIENCES WITH ERLOTINIB IN SECOND AND THIRD LINE TREATMENT PATIENTS WITH ADVANCED STAGE IIIB/ IV NON-SMALL CELL LUNG CANCER
 & OUR EXPERIENCES WITH ERLOTINIB IN SECOND AND THIRD LINE TREATMENT PATIENTS WITH ADVANCED STAGE IIIB/ IV NON-SMALL CELL LUNG CANCER Interim Data Report of TRUST study on patients from Bosnia and Herzegovina
& OUR EXPERIENCES WITH ERLOTINIB IN SECOND AND THIRD LINE TREATMENT PATIENTS WITH ADVANCED STAGE IIIB/ IV NON-SMALL CELL LUNG CANCER Interim Data Report of TRUST study on patients from Bosnia and Herzegovina
THORACIC MALIGNANCIES
 THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008
 Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
Special Report Temporal Trends in Demographics and Overall Survival of Non Small-Cell Lung Cancer Patients at Moffitt Cancer Center From 1986 to 2008 Matthew B. Schabath, PhD, Zachary J. Thompson, PhD,
CT guided thermal ablation of recurrent lung cancer in patients post radiotherapy. A case series review
 CT guided thermal ablation of recurrent lung cancer in patients post radiotherapy. A case series review Poster No.: R-0106 Congress: 2014 CSM Type: Scientific Exhibit Authors: S. Gray; BRISBANE/AU Keywords:
CT guided thermal ablation of recurrent lung cancer in patients post radiotherapy. A case series review Poster No.: R-0106 Congress: 2014 CSM Type: Scientific Exhibit Authors: S. Gray; BRISBANE/AU Keywords:
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón
 Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
CheckMate 012: Safety and Efficacy of First Line Nivolumab and Ipilimumab in Advanced Non-Small Cell Lung Cancer
 CheckMate 12: Safety and Efficacy of First Line Nivolumab and Ipilimumab in Advanced Non-Small Cell Lung Cancer Abstract 31 Hellmann MD, Gettinger SN, Goldman J, Brahmer J, Borghaei H, Chow LQ, Ready NE,
CheckMate 12: Safety and Efficacy of First Line Nivolumab and Ipilimumab in Advanced Non-Small Cell Lung Cancer Abstract 31 Hellmann MD, Gettinger SN, Goldman J, Brahmer J, Borghaei H, Chow LQ, Ready NE,
Radiofrequency Ablation of Liver Tumors
 Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
Radiofrequency Ablation of Liver Tumors Michael M. Awad, Michael A. Choti Indications and Contraindications Indications Unresectable malignant tumors of the liver (e.g., hepatocellular carcinoma, colorectal
North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer
 THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
THIS DOCUMENT IS North of Scotland Cancer Network Clinical Management Guideline for Non Small Cell Lung Cancer [Based on WOSCAN NSCLC CMG with further extensive consultation within NOSCAN] UNCONTROLLED
Is there a role for maintenance therapy in advanced non-small-cell lung cancer?
 Review Is there a role for maintenance therapy in advanced non-small-cell lung cancer? Cesare Gridelli*1, Paolo Maione1, Antonio Rossi1, Clorinda Schettino1, Maria Anna Bareschino1, Paola Claudia Sacco1,
Review Is there a role for maintenance therapy in advanced non-small-cell lung cancer? Cesare Gridelli*1, Paolo Maione1, Antonio Rossi1, Clorinda Schettino1, Maria Anna Bareschino1, Paola Claudia Sacco1,
Combined Modality Therapy State of the Art. Everett E. Vokes The University of Chicago
 Combined Modality Therapy State of the Art Everett E. Vokes The University of Chicago What we Know Some patients are cured (20%) Induction and concurrent chemoradiotherapy are each superior to radiotherapy
Combined Modality Therapy State of the Art Everett E. Vokes The University of Chicago What we Know Some patients are cured (20%) Induction and concurrent chemoradiotherapy are each superior to radiotherapy
Erlotinib (Tarceva) for non small cell lung cancer advanced or metastatic maintenance monotherapy
 Erlotinib (Tarceva) for non small cell lung cancer advanced or metastatic maintenance monotherapy September 2008 This technology summary is based on information available at the time of research and a
Erlotinib (Tarceva) for non small cell lung cancer advanced or metastatic maintenance monotherapy September 2008 This technology summary is based on information available at the time of research and a
Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis
 Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Jpn J Clin Oncol 1997;27(5)305 309 Revisit of Primary Malignant Neoplasms of the Trachea: Clinical Characteristics and Survival Analysis -, -, - - 1 Chest Department and 2 Section of Thoracic Surgery,
Retrospective analysis of Gefitinib and Erlotinib in EGFR-mutated non-small-cell lung cancer patients
 (2017) 1(1): 16-24 Mini Review Open Access Retrospective analysis of Gefitinib and Erlotinib in EGFR-mutated non-small-cell lung cancer patients Chao Pui I 1,3, Cheng Gregory 1, Zhang Lunqing 2, Lo Iek
(2017) 1(1): 16-24 Mini Review Open Access Retrospective analysis of Gefitinib and Erlotinib in EGFR-mutated non-small-cell lung cancer patients Chao Pui I 1,3, Cheng Gregory 1, Zhang Lunqing 2, Lo Iek
Nivolumab: esperienze italiane nel carcinoma polmonare avanzato
 NSCLC avanzato: quali novità nel 2018? Negrar, 30 Ottobre 2018 Nivolumab: esperienze italiane nel carcinoma polmonare avanzato Francesco Grossi UOC Oncologia Medica Fondazione IRCCS Ca Granda Ospedale
NSCLC avanzato: quali novità nel 2018? Negrar, 30 Ottobre 2018 Nivolumab: esperienze italiane nel carcinoma polmonare avanzato Francesco Grossi UOC Oncologia Medica Fondazione IRCCS Ca Granda Ospedale
Adjuvant Chemotherapy
 State-of-the-art: standard of care for resectable NSCLC Adjuvant Chemotherapy JY DOUILLARD MD PhD Professor of Medical Oncology Integrated Centers of Oncology R Gauducheau University of Nantes France Adjuvant
State-of-the-art: standard of care for resectable NSCLC Adjuvant Chemotherapy JY DOUILLARD MD PhD Professor of Medical Oncology Integrated Centers of Oncology R Gauducheau University of Nantes France Adjuvant
T he utility of epidermal growth factor receptor tyrosine kinase inhibitors (EGFR-TKIs) in metastatic nonsmall
 OPEN SUBJECT AREAS: NON-SMALL-CELL LUNG CANCER TARGETED THERAPIES Received 30 April 2014 Accepted 15 July 2014 Published 8 August 2014 Correspondence and requests for materials should be addressed to H.L.
OPEN SUBJECT AREAS: NON-SMALL-CELL LUNG CANCER TARGETED THERAPIES Received 30 April 2014 Accepted 15 July 2014 Published 8 August 2014 Correspondence and requests for materials should be addressed to H.L.
Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? VEGF Is the Only Angiogenic Factor Present Throughout the Tumor Life Cycle
 Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? Martin Reck Department e t of Thoracic c Oncology ogy Hospital Grosshansdorf Germany VEGF Is the Only Angiogenic Factor Present Throughout
Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? Martin Reck Department e t of Thoracic c Oncology ogy Hospital Grosshansdorf Germany VEGF Is the Only Angiogenic Factor Present Throughout
ORIGINAL ARTICLE. Oncology and Translational Medicine DOI /s Abstract
 Oncology and Translational Medicine DOI 10.1007/s10330-018-0281-1 August 2018, Vol. 4, No. 4, P158 P162 ORIGINAL ARTICLE Treatment and survival status of patients with EGFR mutation-positive stage IV lung
Oncology and Translational Medicine DOI 10.1007/s10330-018-0281-1 August 2018, Vol. 4, No. 4, P158 P162 ORIGINAL ARTICLE Treatment and survival status of patients with EGFR mutation-positive stage IV lung
Original Article. Abstract
 Japanese Journal of Clinical Oncology, 2015, 45(7) 670 676 doi: 10.1093/jjco/hyv054 Advance Access Publication Date: 15 April 2015 Original Article Original Article Efficacy of chemotherapy after first-line
Japanese Journal of Clinical Oncology, 2015, 45(7) 670 676 doi: 10.1093/jjco/hyv054 Advance Access Publication Date: 15 April 2015 Original Article Original Article Efficacy of chemotherapy after first-line
Management of advanced non small cell lung cancer
 Management of advanced non small cell lung cancer Jean-Paul Sculier Intensive Care & Thoracic Oncology Institut Jules Bordet Université Libre de Bruxelles (ULB) www.pneumocancero.com Declaration No conflict
Management of advanced non small cell lung cancer Jean-Paul Sculier Intensive Care & Thoracic Oncology Institut Jules Bordet Université Libre de Bruxelles (ULB) www.pneumocancero.com Declaration No conflict
Treatment of oligometastatic NSCLC
 Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
Treatment of oligometastatic NSCLC Jarosław Kużdżał Department of Thoracic Surgery Jagiellonian University Collegium Medicum, John Paul II Hospital, Cracow New idea? 14 NSCLC patients with solitary extrathoracic
Lung Cancer in Women: A Different Disease? James J. Stark, MD, FACP
 Lung Cancer in Women: A Different Disease? James J. Stark, MD, FACP Medical Director, Cancer Program and Director of Palliative Care Maryview Medical Center Professor of Medicine Eastern Virginia Medical
Lung Cancer in Women: A Different Disease? James J. Stark, MD, FACP Medical Director, Cancer Program and Director of Palliative Care Maryview Medical Center Professor of Medicine Eastern Virginia Medical
Thoracic and head/neck oncology new developments
 Thoracic and head/neck oncology new developments Goh Boon Cher Department of Hematology-Oncology National University Cancer Institute of Singapore Research Clinical Care Education Scope Lung cancer Screening
Thoracic and head/neck oncology new developments Goh Boon Cher Department of Hematology-Oncology National University Cancer Institute of Singapore Research Clinical Care Education Scope Lung cancer Screening
Prognosis of recurrent non small cell lung cancer following complete resection
 1300 Prognosis of recurrent non small cell lung cancer following complete resection HIDEFUMI SASAKI, AYUMI SUZUKI, TSUTOMU TATEMATSU, MASAYUKI SHITARA, YU HIKOSAKA, KATSUHIRO OKUDA, SATORU MORIYAMA, MOTOKI
1300 Prognosis of recurrent non small cell lung cancer following complete resection HIDEFUMI SASAKI, AYUMI SUZUKI, TSUTOMU TATEMATSU, MASAYUKI SHITARA, YU HIKOSAKA, KATSUHIRO OKUDA, SATORU MORIYAMA, MOTOKI
Radiofrequency ablation of lung tumors using a multitined expandable. electrode: impact of the electrode's array diameter on local tumor
 1 Radiofrequency ablation of lung tumors using a multitined expandable electrode: impact of the electrode's array diameter on local tumor progression ABSTRACT Purpose: To retrospectively investigate the
1 Radiofrequency ablation of lung tumors using a multitined expandable electrode: impact of the electrode's array diameter on local tumor progression ABSTRACT Purpose: To retrospectively investigate the
National Horizon Scanning Centre. Erlotinib (Tarceva) in combination with bevacizumab for advanced or metastatic non-small cell lung cancer
 Erlotinib (Tarceva) in combination with bevacizumab for advanced or metastatic non-small cell lung cancer This technology summary is based on information available at the time of research and a limited
Erlotinib (Tarceva) in combination with bevacizumab for advanced or metastatic non-small cell lung cancer This technology summary is based on information available at the time of research and a limited
Reference No: Author(s) Approval date: 12/05/16. Committee. June Operational Date: Review:
 Reference No: Title: Author(s) Systemic Anti-Cancer Therapy (SACT) Guidelines for Biliary Tract Cancer (BTC) Dr Colin Purcell, Consultant Medical Oncologist on behalf of the GI Oncologists Group, Cancer
Reference No: Title: Author(s) Systemic Anti-Cancer Therapy (SACT) Guidelines for Biliary Tract Cancer (BTC) Dr Colin Purcell, Consultant Medical Oncologist on behalf of the GI Oncologists Group, Cancer
Choosing Optimal Therapy for Advanced Non-Squamous (NS) Non-Small Cell Lung Cancer
 Choosing Optimal Therapy for Advanced Non-Squamous (NS) Non-Small Cell Lung Cancer Jyoti D. Patel, MD Associate Professor Feinberg School of Medicine Robert H Lurie Comprehensive Cancer Center Northwestern
Choosing Optimal Therapy for Advanced Non-Squamous (NS) Non-Small Cell Lung Cancer Jyoti D. Patel, MD Associate Professor Feinberg School of Medicine Robert H Lurie Comprehensive Cancer Center Northwestern
MANAGEMENT OF COLORECTAL METASTASES. Robert Warren, MD. The Postgraduate Course in General Surgery March 22, /22/2011
 MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
Author(s) Ohmatsu, Hironobu; Kubota, Kaoru; N. Citation Respiratory medicine (2010), 104(3)
 Title Trends in chemotherapy for elderly non-small-cell lung cancer. Author(s) Kim, Young Hak; Yoh, Kiyotaka; Niho Ohmatsu, Hironobu; Kubota, Kaoru; N Citation Respiratory medicine (2010), 104(3) Issue
Title Trends in chemotherapy for elderly non-small-cell lung cancer. Author(s) Kim, Young Hak; Yoh, Kiyotaka; Niho Ohmatsu, Hironobu; Kubota, Kaoru; N Citation Respiratory medicine (2010), 104(3) Issue
Expression of programmed death ligand-1 on tumor cells varies pre and post
 Expression of programmed death ligand-1 on tumor cells varies pre and post chemotherapy in non-small cell lung cancer Jin Sheng 1,2,3,*, Wenfeng Fang 1,2,3,*, Juan Yu 3, Yunpeng Yang 1,2,3, Yuxiang Ma
Expression of programmed death ligand-1 on tumor cells varies pre and post chemotherapy in non-small cell lung cancer Jin Sheng 1,2,3,*, Wenfeng Fang 1,2,3,*, Juan Yu 3, Yunpeng Yang 1,2,3, Yuxiang Ma
EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI
 EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI Overview Introduction Diagnostic work up Treatment Group 1 Group 2 Group 3 Stage III lung cancer Historically was defined as locoregionally advanced
EVIDENCE BASED MANAGEMENT OF STAGE III NSCLC MILIND BALDI Overview Introduction Diagnostic work up Treatment Group 1 Group 2 Group 3 Stage III lung cancer Historically was defined as locoregionally advanced
Maintenance therapies in advanced non-small-cell lung cancer
 Review Maintenance therapies in advanced non-small-cell lung cancer Advanced non-small-cell lung cancer is treated with upfront platinum doublet chemotherapy, which produces moderate survival improvements.
Review Maintenance therapies in advanced non-small-cell lung cancer Advanced non-small-cell lung cancer is treated with upfront platinum doublet chemotherapy, which produces moderate survival improvements.
General summary GENERAL SUMMARY
 General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
General summary GENERAL SUMMARY In Chapter 2.1 the long-term results and prognostic factors of radiofrequency ablation (RFA) for unresectable colorectal liver metastases (CRLM) in a single center with
PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC. Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy
 PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy Prognostic versus predictive Prognostic: In presence of the biomarker patient outcome
PROGNOSTIC AND PREDICTIVE BIOMARKERS IN NSCLC Federico Cappuzzo Istituto Toscano Tumori Ospedale Civile-Livorno Italy Prognostic versus predictive Prognostic: In presence of the biomarker patient outcome
Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery
 Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation I: Patient ER 74 y/o male with A1A
Stereotactic Body Radiation Therapy and Radiofrequency Ablation 2014 Masters of Minimally Invasive Surgery Matthew Hartwig, M.D. Duke Cancer Institute Case Presentation I: Patient ER 74 y/o male with A1A
Frequency of Epidermal Growth Factor Mutation Status and Its Effect on Outcome of Patients with Adenocarcinoma of the Lung
 Journal of Cancer Therapy, 2014, 5, 1012-1020 Published Online September 2014 in SciRes. http://www.scirp.org/journal/jct http://dx.doi.org/10.4236/jct.2014.511106 Frequency of Epidermal Growth Factor
Journal of Cancer Therapy, 2014, 5, 1012-1020 Published Online September 2014 in SciRes. http://www.scirp.org/journal/jct http://dx.doi.org/10.4236/jct.2014.511106 Frequency of Epidermal Growth Factor
TRANSPARENCY COMMITTEE OPINION. 29 April 2009
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 29 April 2009 NAVELBINE 20 mg, soft capsules B/1 (CIP: 365 948-4) NAVELBINE 30 mg, soft capsules B/1 (CIP: 365 949-0)
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 29 April 2009 NAVELBINE 20 mg, soft capsules B/1 (CIP: 365 948-4) NAVELBINE 30 mg, soft capsules B/1 (CIP: 365 949-0)
Chemotherapy and Immunotherapy in Combination Non-Small Cell Lung Cancer (NSCLC)
 Chemotherapy and Immunotherapy in Combination Non-Small Cell Lung Cancer (NSCLC) Jeffrey Crawford, MD George Barth Geller Professor for Research in Cancer Co-Program Leader, Solid Tumor Therapeutics Program
Chemotherapy and Immunotherapy in Combination Non-Small Cell Lung Cancer (NSCLC) Jeffrey Crawford, MD George Barth Geller Professor for Research in Cancer Co-Program Leader, Solid Tumor Therapeutics Program
Tumor Board Discussions: Case 1
 Tumor Board Discussions: Case 1 David S. Ettinger, MD The Alex Grass Professor of Oncology Johns Hopkins University School of Medicine Baltimore, Maryland Case #1 50-year-old Asian female, never smoker
Tumor Board Discussions: Case 1 David S. Ettinger, MD The Alex Grass Professor of Oncology Johns Hopkins University School of Medicine Baltimore, Maryland Case #1 50-year-old Asian female, never smoker
ISSN: (Print)/ (Online) Tuberc Respir Dis 2018;81:
 ORIGINAL ARTICLE https://doi.org/10.4046/trd.2017.0090 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2018;81:148-155 Pemetrexed Continuation Maintenance versus Conventional Platinum-Based
ORIGINAL ARTICLE https://doi.org/10.4046/trd.2017.0090 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2018;81:148-155 Pemetrexed Continuation Maintenance versus Conventional Platinum-Based
Heather Wakelee, M.D.
 Heather Wakelee, M.D. Assistant Professor of Medicine, Oncology Stanford University Sponsored by Educational Grant Support from Adjuvant (Post-Operative) Lung Cancer Chemotherapy Heather Wakelee, M.D.
Heather Wakelee, M.D. Assistant Professor of Medicine, Oncology Stanford University Sponsored by Educational Grant Support from Adjuvant (Post-Operative) Lung Cancer Chemotherapy Heather Wakelee, M.D.
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
Sao Paulo, Abril 2014
 Tratamento de Manutencao e outros Sao Paulo, Abril 2014 Rogerio C. Lilenbaum, M.D. Professor of Medicine Yale Cancer Center Chief Medical Officer Smilow Cancer Hospital What Is Maintenance Therapy? Use
Tratamento de Manutencao e outros Sao Paulo, Abril 2014 Rogerio C. Lilenbaum, M.D. Professor of Medicine Yale Cancer Center Chief Medical Officer Smilow Cancer Hospital What Is Maintenance Therapy? Use
Metastatic NSCLC: Expanding Role of Immunotherapy. Evan W. Alley, MD, PhD Abramson Cancer Center at Penn Presbyterian
 Metastatic NSCLC: Expanding Role of Immunotherapy Evan W. Alley, MD, PhD Abramson Cancer Center at Penn Presbyterian Disclosures: No relevant disclosures Please note that some of the studies reported in
Metastatic NSCLC: Expanding Role of Immunotherapy Evan W. Alley, MD, PhD Abramson Cancer Center at Penn Presbyterian Disclosures: No relevant disclosures Please note that some of the studies reported in
The Efficacy and Safety of Platinum/Vinorelbine as More Than Second-Line Chemotherapy for Advanced Non-small Cell Lung Cancer
 pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2015;47(4):638-644 Original Article http://dx.doi.org/10.4143/crt.2014.316 Open Access The Efficacy and Safety of Platinum/Vinorelbine as More Than Second-Line
pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2015;47(4):638-644 Original Article http://dx.doi.org/10.4143/crt.2014.316 Open Access The Efficacy and Safety of Platinum/Vinorelbine as More Than Second-Line
MOLECULAR AND CLINICAL ONCOLOGY 1: , 2013
 MOLECULAR AND CLINICAL ONCOLOGY 1: 711-715, 2013 Clinical study on gefitinib combined with γ ray stereotactic body radiation therapy as the first line treatment regimen for senile patients with adenocarcinoma
MOLECULAR AND CLINICAL ONCOLOGY 1: 711-715, 2013 Clinical study on gefitinib combined with γ ray stereotactic body radiation therapy as the first line treatment regimen for senile patients with adenocarcinoma
Original Article. Abstract
 Original Article Survival difference between EGFR Del19 and L858R mutant advanced non-small cell lung cancer patients receiving gefitinib: a propensity score matching analysis Minglei Zhuo 1*, Qiwen Zheng
Original Article Survival difference between EGFR Del19 and L858R mutant advanced non-small cell lung cancer patients receiving gefitinib: a propensity score matching analysis Minglei Zhuo 1*, Qiwen Zheng
Combining chemotherapy and radiotherapy of the chest
 How to combine chemotherapy, targeted agents and radiotherapy in locally advanced NSCLC? Dirk De Ruysscher, MD, PhD Radiation Oncologist Professor of Radiation Oncology Leuven Cancer Institute Department
How to combine chemotherapy, targeted agents and radiotherapy in locally advanced NSCLC? Dirk De Ruysscher, MD, PhD Radiation Oncologist Professor of Radiation Oncology Leuven Cancer Institute Department
When to Integrate Surgery for Metatstatic Urothelial Cancers
 When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
When to Integrate Surgery for Metatstatic Urothelial Cancers Wade J. Sexton, M.D. Senior Member and Professor Department of Genitourinary Oncology Moffitt Cancer Center Case Presentation #1 67 yo male
Virtual Journal Club: Front-Line Therapy and Beyond Recent Perspectives on ALK-Positive Non-Small Cell Lung Cancer.
 Virtual Journal Club: Front-Line Therapy and Beyond Recent Perspectives on ALK-Positive Non-Small Cell Lung Cancer Reference Slides ALK Rearrangement in NSCLC ALK (anaplastic lymphoma kinase) is a receptor
Virtual Journal Club: Front-Line Therapy and Beyond Recent Perspectives on ALK-Positive Non-Small Cell Lung Cancer Reference Slides ALK Rearrangement in NSCLC ALK (anaplastic lymphoma kinase) is a receptor
Exploring Personalized Therapy for First Line Treatment of Advanced Non-Small Cell Lung Cancer (NSCLC)
 Exploring Personalized Therapy for First Line Treatment of Advanced Non-Small Cell Lung Cancer (NSCLC) Suresh S. Ramalingam, MD Director of Thoracic Oncology Associate Professor Emory University Atlanta,
Exploring Personalized Therapy for First Line Treatment of Advanced Non-Small Cell Lung Cancer (NSCLC) Suresh S. Ramalingam, MD Director of Thoracic Oncology Associate Professor Emory University Atlanta,
Systemic Management of Malignant Pleural Mesothelioma
 ESO-ESMO EASTERN EUROPE AND BALKAN REGION MASTERCLASS IN MEDICAL ONCOLOGY 15.June-19.June 2018 Belgrade, Serbia Systemic Management of Malignant Pleural Mesothelioma Dragana Jovanovic University Hospital
ESO-ESMO EASTERN EUROPE AND BALKAN REGION MASTERCLASS IN MEDICAL ONCOLOGY 15.June-19.June 2018 Belgrade, Serbia Systemic Management of Malignant Pleural Mesothelioma Dragana Jovanovic University Hospital
Heterogeneity of N2 disease
 Locally Advanced NSCLC Surgery? No. Ramaswamy Govindan M.D Co-Director, Section of Medical Oncology Alvin J Siteman Cancer Center at Washington University School of Medicine St. Louis, Missouri Heterogeneity
Locally Advanced NSCLC Surgery? No. Ramaswamy Govindan M.D Co-Director, Section of Medical Oncology Alvin J Siteman Cancer Center at Washington University School of Medicine St. Louis, Missouri Heterogeneity
Analysis of clinical characteristics and prognosis of patients with anaplastic lymphoma kinase-positive and surgically resected lung adenocarcinoma
 Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Analysis of clinical characteristics and prognosis of patients with anaplastic lymphoma kinase-positive and surgically resected lung adenocarcinoma Hong
Thoracic Cancer ISSN 1759-7706 ORIGINAL ARTICLE Analysis of clinical characteristics and prognosis of patients with anaplastic lymphoma kinase-positive and surgically resected lung adenocarcinoma Hong
Squamous Cell Carcinoma Standard and Novel Targets.
 Squamous Cell Carcinoma Standard and Novel Targets. Mohamed K. Mohamed, MD, PhD Director of Thoracic Oncology Cone Health Cancer Center Greensboro, NC 1 Mohamed Mohamed, MD, PhD Squamous Cell Carcinoma:
Squamous Cell Carcinoma Standard and Novel Targets. Mohamed K. Mohamed, MD, PhD Director of Thoracic Oncology Cone Health Cancer Center Greensboro, NC 1 Mohamed Mohamed, MD, PhD Squamous Cell Carcinoma:
Risk factors for occurrence of local tumor progression after percutaneous radiofrequency ablation for lung neoplasms
 Diagn Interv Radiol 2007; 13:199 203 Turkish Society of Radiology 2007 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Risk factors for occurrence of local tumor progression after percutaneous radiofrequency
Diagn Interv Radiol 2007; 13:199 203 Turkish Society of Radiology 2007 INTERVENTIONAL RADIOLOGY ORIGINAL ARTICLE Risk factors for occurrence of local tumor progression after percutaneous radiofrequency
