Differential effect of concurrent chemotherapy regimen on clinical outcomes of preoperative chemoradiotherapy for locally advanced rectal cancer
|
|
|
- Iris Casey
- 5 years ago
- Views:
Transcription
1 JBUON 2019; 24(2): ISSN: , online ISSN: ORIGINAL ARTICLE Differential effect of concurrent chemotherapy regimen on clinical outcomes of preoperative chemoradiotherapy for locally advanced rectal cancer Eunji Kim 1, Kyubo Kim 2, Do Hoon Oh 3, Sae-Won Han 4, Tae-You Kim 4, Seung-Yong Jung 5, Kyu Joo Park 5, Gyeong Hoon Kang 6, Eui Kyu Chie 1,7 Departments of 1 Radiation Oncology, 4 Internal Medicine, 5 Surgery, and 6 Pathology, Seoul National University College of Medicine, Seoul, Republic of Korea; 2 Department of Radiation Oncology, Ewha Womans University School of Medicine, Seoul, Republic of Korea; 3 Department of Radiation Oncology, Chung-Ang University Hospital, Seoul, Republic of Korea; 7 Institute of Radiation Medicine, Medical Research Center, Seoul National University, Seoul, Republic of Korea. Summary Purpose: The purpose of this study was to evaluate the differential effect of chemotherapy regimen in preoperative chemoradiotherapy (CRT) for locally advanced rectal cancer. Methods: The medical records of 279 patients who underwent preoperative CRT followed by surgery for ct3/4 rectal cancer from 2003 to 2010 were retrospectively reviewed. Thirty-four patients were treated with one cycle of i.v. bolus 5-fluorouracil (5-FU) during 1 st week (group A), 214 patients with two cycles of i.v. bolus 5-FU during 1 st and 5 th week (group B), and 31 patients with oral capecitabine on the days with radiotherapy (group C). Propensity score matching was performed between three groups. Results: Median follow-up was 60.1 months. Five-year locoregional recurrence-free survival (LRFS), distant metastasis-free survival (DMFS), disease-free survival (DFS) and overall survival (OS) rates were 91.2, 83.3, 75.0, and 84.5%, respectively. Thirty-one patients per group were allocated to three groups via propensity score matching. On univariate analysis, concurrent chemotherapy regimen was not a significant prognostic factor for survival outcomes in the matched group analysis (OS, p=0.175; DFS, p=0.481; DMFS, p=0.515; LRFS, p=0.456). In addition, there was no significant difference in the sphincter preserving surgery rate, circumferential resection margin status, and pathologic response between three groups (p=0.441, 1.000, 0.818, respectively). As regards to treatment-related toxicity, 9 patients showed grade 3 neutropenia in group B, while there was no grade 3 or higher toxicity in groups A and C. Conclusion: The concurrent chemotherapy regimen (5-FU #1 vs 5-FU #2 vs capecitabine) did not have a significant effect on treatment outcomes in locally advanced rectal cancer patients receiving neoadjuvant CRT. Key words: chemoradiotherapy, chemotherapy regimen, neoadjuvant, rectal cancer Introduction Several phase 3 studies showed that preoperative chemoradiotherapy (CRT) and total mesorectal excision is the standard of care for locally advanced rectal cancer [1-4]. More recent studies have intensified neoadjuvant CRT by adding oxaliplatin to standard regimen in locally advanced rectal cancer based on the results from an adjuvant treatment trial in stage III colon cancer [5]. Although the effect of oxaliplatin was mixed in advanced rectal cancer, the toxicity of treatment was increased with intensified chemotherapy [6-10]. In addition, the long-term outcome of the European Organisation Correspondence to: Eui Kyu Chie, MD, PhD. Department of Radiation Oncology, Seoul National University College of Medicine, 101 Daehak-ro, Jongno-gu, Seoul 03080, Republic of Korea. Tel: , Fax: , ekchie93@snu.ac.kr Received: 14/06/2018; Accepted: 12/07/2018 This work by JBUON is licensed under a Creative Commons Attribution 4.0 International License.
2 Impact of concurrent CTx regimen in rectal cancer 471 for Research and Treatment of Cancer trial failed to confirm the benefit of both preoperative and postoperative chemotherapy. Although this trial focused on the long-term effect of adjuvant chemotherapy, it also showed that preoperative chemotherapy does not affect 10-year DFS or OS [11]. Various concurrent chemotherapy regimens have been used to date in previous clinical trials [12-14]. It is still unclear which of these regimens is optimal. According to the NCCN guidelines, 5-fluorouracil (5-FU) and capecitabine are recommended as concurrent chemotherapy regimen [15]. In our institute, patients were treated with single or two cycles of 5-FU and capecitabine, based on previous studies [2-4,16]. Although the chemotherapy regimen has changed over time, the difference in treatment outcome was not analyzed. Therefore, we retrospectively analyzed locally advanced rectal cancer patients who were treated with neoadjuvant CRT followed by surgery to evaluate the impact of a single cycle of 5-FU compared to two cycles of 5-FU and capecitabine on clinical outcomes. Methods Patients After institutional review board approval, we reviewed the medical records of patients who underwent preoperative CRT followed by surgery between July 2003 and December The inclusion criteria were as follows: (1) histologically confirmed rectal adenocarcinoma, (2) clinical T3-4, (3) no evidence of distant metastasis, and (4) total mesorectal excision following preoperative CRT. Patients with any other malignancies at diagnosis were excluded. All patients were examined with digital rectal examination, complete blood count, liver function tests, carcinoembryonic antigen level, colonoscopy, and computed tomography. Magnetic resonance imaging was also used in the majority of patients. Selected patients, treated more recently, also underwent positron emission tomography. Pathology of primary rectal lesion was confirmed by biopsy prior to treatment in all patients. Treatment After histologic and clinical diagnosis of primary rectal cancer, all 279 patients underwent preoperative concurrent CRT and total mesorectal excision. For radiotherapy, all patients were treated with 3-dimensitonal conformal radiotherapy in prone position. The gross tumor volume (GTV) consisted of tumor and suspicious lymph nodes at diagnostic work-up. The clinical target volume (CTV) covered GTV, mesorectal tissues and regional lymphatics such as the perirectal, presacral, and internal iliac nodes. The planning target volume (PTV) included the CTV plus a 1 cm margin. Dose prescription was 45 Gy in 25 fractions to PTV, followed by 5-9 Gy in 3-5 fractions to primary lesion and enlarged pelvic lymph nodes plus 1cm margin. The median total radiation dose was 50.4 Gy (range, 45-54). Thirty-four patients received 5-FU (500 mg/m 2 ) intravenous (i.v.) bolus injection for 3 days during the first week of radiotherapy (Group A), 214 patients with two cycles of i.v. bolus 5-FU during 1 st and 5 th week of radiotherapy (Group B), and 31 patients with capecitabine (1650 mg/m 2 ) daily, on the days with radiotherapy (Group C). Our institute experienced a change in the concurrent chemotherapy regimen during neoadjuvant CRT from 2003 to When the concurrent chemotherapy was divided by time, all patients in group A were treated before More recently treated patients received two cycles of 5-FU or capecitabine. Table 1. Patient and treatment characteristics (n=279) Characteristics n (%) Age, years Gender < (84.9) (15.1) Male 202 (72.4) Female 77 (27.6) ECOG performance status 0, (98.9) 2 3 (1.1) Clinical T stage T3 258 (92.5) T4 21 (7.5) Clinical N stage N (-) 56 (20.1) N (+) 223 (79.9) Distance from anal verge, cm (64.9) >5 98 (35.1) Pretreatment CEA level, ng/ml (70.6) >5 82 (29.4) Pretreatment Hb level, g/dl <12 g/dl 157 (56.3) 12 g/dl 122 (43.7) Concurrent chemotherapy 5-FU #1 34 (12.2) 5-FU #2 214 (76.7) Capecitabine 31 (11.1) Sphincter preserving surgery Yes 260 (93.2) No 19 (6.8) Adjuvant chemotherapy Yes 248 (88.9) No 31 (11.1) CEA: carcinoembryonic antigen, Hb: hemoglobin JBUON 2019; 24(2): 471
3 472 Impact of concurrent CTx regimen in rectal cancer Surgery was performed at a median 57 days after preoperative CRT. The majority of patients (n=260, 93.2%) had sphincter preserving surgery. Abdominoperineal resection was performed in 18 patients. Adjuvant chemotherapy was administered to 248 patients (88.9%). Thirty one patients did not receive postoperative chemotherapy. The reasons of omission were as follows: pathologic complete regression in 8 patients, patient refusal in 15 patients, old age in 3 patients, medical comorbidity in 2 patients, and transfer to other hospital in 3 patients. The regimens of postoperative chemotherapy were fluorouracil-leucovorin (n=203), capecitabine (n=30), and FOLFOX (n=15). Follow-up and statistical analysis The date of endoscopic biopsy of primary tumor was used as the date of diagnosis. OS was defined as the interval from the date of diagnosis to the date of death from any cause. DFS was defined as the time from the date of diagnosis to any recurrent disease detection. DMFS was defined as the interval from the date of diagnosis to distant metastasis detection. LRFS was defined as the time from the date of diagnosis to the date of locoregional relapse detected in pelvic cavity. Therapeutic response on surgical specimen was graded according to the Korean pathology standard report [17]. This report classified the pathologic effect from Supplementary Table 1. Univariate analysis of factors affecting 5-yr clinical outcomes Variables N OS (%) p value DFS (%) p value DMFS (%) p value LRFS (%) p value Age, years < Gender Male Female Distance from AV, cm > Pathologic T stage < ypt ypt Pathologic N stage < < < < ypn ypn Angiolymphatic invasion < Yes No Venous invasion < Yes No Perineural invasion < < < < Yes No CRM status, cm > CRT response < < < Grade Grade Concurrent chemotherapy FU # FU # Capecitabine By Korean pathology standard report; grade 4 refers to near total regression, OS: overall survival, DFS: disease-free survival, DMFS: distant metastasis-free survival, LRFS: locoregional recurrence-free survival, PS: performance status, AV: anal verge, CRM: circumferential resection margin, CRT: chemoradiotherapy JBUON 2019; 24(2): 472
4 Impact of concurrent CTx regimen in rectal cancer 473 no regression to total regression as reported in previous studies [18,19]. The toxicities from radiotherapy were evaluated with the Common Terminology Criteria for Adverse Events (CTCAE) 4.0. For the statistical analyses among treatment groups, the Pearson chi-square and the Fisher exact test were used. The Kaplan-Meier method was used to estimate survival rates. The log-rank test and the Cox proportional hazards regression model were used for the univariate and multivariate analyses, respectively. Factors with a p value less than 0.05 were regarded as statistically significant. Propensity score matching was performed Table 2. Multivariate analysis of factors affecting clinical outcome Variables OS, p value DFS, p value DMFS, p value LRFS, p value Tumor location (AV > 5cm vs. 5cm) Pathologic N-stage (ypn0 vs. ypn1,2) Perineural invasion (No vs. Yes) < < < < CRT response ( Grade 4 vs. < Grade 4) By Korean pathology standard report; grade 4 refers to near total regression, OS: overall survival, DFS: disease-free survival, DMFS: distant metastasis-free survival, LRFS: locoregional recurrence-free survival, AV: anal verge, CRT: chemoradiotherapy Supplementary Table 2. Patient and treatment characteristics according to concurrent chemotherapy Variables No. of patients (%) p value Total (n=279) 5-FU #1 (n=34) 5-FU #2 (n=214) Capecitabine Age, years < (84.9) 31 (91.2) 177 (82.7) 29 (93.5) (15.1) 3 (8.8) 37 (17.3) 2 (6.5) Gender Male 202 (72.4) 25 (73.5) 150 (70.1) 27 (87.1) Female 77 (27.6) 9 (26.5) 64 (29.9) 4 (12.9) ECOG performance status , (98.9) 32 (94.1) 214 (100) 30 (96.8) 2 3 (1.1) 2 (5.9) 0 (0.0) 1 (3.2) Clinical T stage T3 258 (92.5) 31 (91.2) 197 (92.1) 30 (96.8) T4 21 (7.5) 3 (8.8) 17 (7.9) 1 (3.2) Clinical N stage N (-) 56 (20.1) 10 (29.4) 39 (18.2) 7 (22.6) N (+) 223 (79.9) 24 (70.6) 175 (87.8) 24 (77.4) Distance from anal verge, cm (64.9) 26 (76.5) 127 (59.3) 28 (90.3) > 5 98 (35.1) 8 (23.5) 87 (40.7) 3 (9.7) Pretreatment Hb level, g/dl < (56.3) 21 (61.8) 113 (52.8) 23 (74.2) (43.7) 13 (38.2) 101 (47.2) 8 (25.8) Sphincter preserving surgery Yes 260 (93.2) 27 (79.4) 206 (96.3) 27 (87.1) No 19 (6.8) 7 (20.6) 8 (3.7) 4 (12.9) Adjuvant chemotherapy Yes 248 (88.9) 30 (88.2) 192 (89.7) 26 (83.9) No 31 (11.1) 4 (11.8) 22 (10.3) 5 (6.1) Hb: hemoglobin JBUON 2019; 24(2): 473
5 474 Impact of concurrent CTx regimen in rectal cancer to minimise the bias between the groups. One-to-one matching was performed using the nearest-neighbour method. The analyses were performed using PASW Statistics for Windows, Version 23.0 (SPSS Inc., Chicago, IL, USA) and R version ( with the MatchIt package for propensity score matching. Results Patients and treatment characteristics A total of 279 patients who were diagnosed with locally advanced rectal cancer were treated with preoperative CRT and operation. Patient characteristics at baseline are shown in Table 1. The median age was 59 years (range, 31-82). All patients except three had an ECOG performance status of 0 or 1. The median CEA levels were 2.9 ng/ml (range, ) at diagnosis and 1.3 ng/ml (range, ) after surgery. Treatment response The median follow-up time was 60.1 months (range, 6-128). Complete tumor regression was found in 40 patients (14.3%) and 48 patients (17.2%) showed near total regression. The ypt stage was classified as ypt0-ypt1 and ypt2-ypt4 for statistical analysis. More than half of the patients had post-treatment pathologic stage of ypt3 A B Figure 1. Survivals of matched patients according to concurrent chemotherapy. A: Overall survival (OS). B: Disease-free survival (DFS). (ypt0 14.0%; yptis 0.7%; ypt1 5.4%; ypt2 24.7%; ypt3 54.8%; ypt4 0.4%). Regarding ypn stage, 202 patients (72.4%) showed ypn0 and 15 patients (5.4%) had ypn2 stage. Angiolymphatic, venous, and perineural invasion were found in 34 patients (12.1%), 12 patients (4.3%), and 37 patients (13.2%), respectively. Twenty-eight specimens (10%) showed close circumferential resection margin (CRM) defined as same or closer than 0.1cm. Prognostic factors for survival Five-year OS, DFS, DMFS, and LRFS were 84.5%, 75.0%, 83.3%, and 91.2%, respectively. The univariate analysis of prognostic factors on the survival outcomes is shown in Supplementary Table 1. Concurrent chemotherapy regimen was not associated with survival end-points. In the multivariate analysis, perineural invasion and post-crt nodal status (ypn- vs ypn+) were independent prognostic factors predictive of OS, DFS, DMFS, and LRFS (Table 2). Additionally, tumor location from anal verge was significant prognosticator for OS, DFS, and DMFS, and CRT response was the prognostic factor for OS. Clinical outcome according to chemotherapy regimen Patient and tumor characteristics according to concurrent chemotherapy regimen are shown in Supplementary Table 2. There were no significant differences among the three groups in age, gender, clinical stage, and prevalence of anemia. There were 3 patients with ECOG performance status 2, 2 treated with one cycle of 5-FU and one with capecitabine. The proportion of patients with tumor above 5cm from the anal verge was larger in group B (p=0.001). Patient and tumor characteristics after propensity score matching is demonstrated in Table 3. In the matched analysis, 5-year OS in groups A, B, and C was 80.7, 66.5, and 87.1%, respectively (p=0.175, Figure 1A), and DFS was 70.7, 58.8, and 70.5% (p=0.481, Figure 1B). Five-year DMFS was 87.1, 76.7, and 76.6% (p=0.515), and LRFS was 76.7, 89.7, and 90.2% (p=0.456), respectively. Table 4 displays the treatment results of matched analysis. The rates of sphincter preservation surgery, CRM >0.1 cm, and CRT response grade 4 were not statistically different between the three groups, as well. Additionally, the events of locoregional recurrence and distant metastasis were also similar in the three groups. Treatment-related toxicity No patient experienced grade 3 or higher gastrointestinal toxicity and the distribution of grade JBUON 2019; 24(2): 474
6 Impact of concurrent CTx regimen in rectal cancer 475 Table 3. Patient and tumor characteristics according to concurrent chemotherapy after propensity score matching Characteristics No. of patients (%) p value 5-FU #1 5-FU #2 Capecitabine Age, years <70 28 (90.3) 23 (74.2) 29 (93.6) (9.7) 8 (25.8) 2 (6.5) Gender Male 23 (74.2) 22 (71.0) 27 (87.1) Female 8 (25.8) 9 (29.0) 4 (12.9) ECOG performance status 0, 1 29 (93.6) 31 (100.0) 30 (96.8) (6.5) 0 (0.0) 1 (3.2) Clinical T stage T3 28 (90.3) 30 (96.8) 30 (96.8) T4 3 (9.7) 1 ( 3.2) 1 (3.2) Clinical N stage N (-) 10 (32.3) 12 (38.7) 7 (22.6) N (+) 21 (67.7) 19 (61.3) 24 (77.4) Distance from anal verge, cm 5 26 (83.9) 26 (83.9) 28 (90.3) >5 5 (16.1) 5 (16.1) 3 ( 9.7) Table 4. Treatment outcomes according to concurrent chemotherapy after propensity score matching Variables No. of patients (%) p value 5-FU #1 5-FU #2 Capecitabine Sphincter preserving surgery Yes 24 (77.4) 28 (90.3) 27 (87.1) No 7 (22.6) 3 ( 9.7) 4 (12.9) CRM status, cm > (90.3) 29 (93.6) 29 (93.6) (9.7) 2 ( 6.5) 2 ( 6.5) CRT response <Grade 4 22 (71.0) 22 (71.0) 20 (64.5) Grade 4 9 (29.0) 9 (29.0) 11 (35.5) Pathologic complete response No 25 (80.8) 27 (87.1) 27 (87.1) Yes 6 (19.4) 4 (12.9) 4 (12.9) Locoregional recurrence No 24 (77.4) 28 (90.3) 27 (87.1) Yes 7 (22.6) 3 ( 9.7) 4 (12.9) Distant metastasis No 27 (87.1) 24 (77.4) 24 (77.4) Yes 4 (12.9) 7 (22.6) 7 (22.6) By Korean pathology standard report; grade 4 refers to near total regression, CRM: circumferential resection margin, CRT: chemoradiotherapy JBUON 2019; 24(2): 475
7 476 Impact of concurrent CTx regimen in rectal cancer Table 5. Treatment-related toxicity Toxicities No. of patients p value 5-FU #1 (n=34) 5-FU #2 (n=214) Capecitabine Grade 1-2 Grade 3 Grade 1-2 Grade 3 Grade 1-2 Grade 3 Gastrointestinal Nausea Diarrhea Enteritis Hematologic Neutropenia Anemia Hand-foot syndrome < By NCI CTCAE v toxicities across the groups were not statistically significant. However, the frequency of hematologic toxicity was different among the treated groups. Grade 3 treatment-related toxicity was observed only in group B patients, all of which were grade 3 neutropenia. Likewise, skin toxicity, which was grade 1-2 hand-foot syndrome, was only observed in 4 patients in group C (Table 5). During follow-up period, 5 patients underwent adhesiolysis. Four patients were in group B, and one in group C. Other treatment related late toxicity was not observed. Discussion In this study, we analyzed the clinical outcomes of neoadjuvant CRT for locally advanced rectal cancer according to preoperative chemotherapy regimens; one cycle of 5-FU vs two cycles of 5-FU vs capecitabine. In summary, 5-year OS, DFS, LRFS and DMFS were not statistically different among the groups, and different chemotherapy regimen did not result in statistically significant difference in tumor response, CRM status and sphincter preserving surgery rate when analyzed after propensity score matching as well in the entire cohort. With regard to treatment related toxicities, grade 3 neutropenia was observed in 9 patients (4.2%) who received two cycles of 5-FU, whereas only grade 1-2 toxicities in patients who received a single cycle of 5-FU. Single cycle of 5-FU regimen employed in the current study originates from institutional phase II trial, which proved efficacy and safety as adjuvant treatment combined with radiotherapy for resectable rectal cancer [16]. Thus, patients in earlier time period were more likely treated with this regimen. In line with the intensification of concurrent chemotherapy regimen, an additional cycle was added following the recommendations of treatment guidelines. The mainstay of concurrent chemotherapy was later shifted to oral capecitabine, reflecting more focus on the patient comfort with proven efficacy compared to regimens employing intravenous delivery. The optimal chemotherapy regimen in preoperative CRT is still under debate. Although preoperative CRT was regarded as a standard treatment strategy for locally advanced rectal cancer, chemotherapy regimens were not consistent between randomized trials [12-14]. The most recent NCCN guideline recommended various chemotherapy regimens such as continuous infusion of 5-FU, bolus 5-FU/leucovorin and capecitabine [15]. It is perceived that a recommended regimen has similar efficacy, whereas adverse event profile may be different. There have been many efforts to increase the outcomes by intensifying chemotherapy by combining an additional agent such as oxaliplatin, irinotecan and bevacizumab to standard preoperative CRT [6-10,20-23]. The result of this study shows that treatment outcomes of less than standard chemotherapy, as for instance one cycle of i.v. bolus 5-FU as in this study, would not be different from that of combination with standard chemotherapy, with less treatment-related events. Futhermore, long-term analysis of EORTC has failed to demonstrate the role of both neoadjuvant and adjuvant chemotherapy [11]. This would not mean there is no role of combined chemotherapy in locally advanced rectal cancer. In ADORE trial, intensified adjuvant chemotherapy with oxaliplatin to patients with stage III disease after neoadjuvant chemoradiotherapy showed improved results over standard fluoropyrimidine chemotherapy [24]. Furthermore, JBUON 2019; 24(2): 476
8 Impact of concurrent CTx regimen in rectal cancer 477 more intensified chemotherapy in the neoadjuvant setting, often termed total neoadjuvant treatment (TNT) approach, has been introduced and is currently being explored in a prospective phase III trial [25]. Though findings seems contradictory, the results from two studies [1,24] stress the importance of patient selection. Inclusion criteria regarding treatment response or burden was non-existent for EORTC 22921, whereas only poor responders to standard preoperative chemoradiotherapy were included for ADORE trial. Likewise, poor responders to FOLFOX induction chemotherapy will be offered standard chemoradiotherapy in PROSPECT trial. However, outside clinical trials in a daily clinical setting, unselected patients would undergo standard of care treatment, which would be preoperative chemoradiotherapy. Numerous meta-analyses and reviews over the past decade have failed to nominate relevant factors for treatment response prediction [26-28]. In light of these findings, less than standard chemotherapy in combination with radiotherapy or radiotherapy alone may be a viable option for patients with poor performance, who may benefit from lower risk of treatment-related morbidity, where the likelihood of benefit from combined treatment is not quite substantial. This study has several limitations. First, this is a single-institute retrospective study, thus not free from inherent study design. Second, compared treatments were not balanced in respect to patient number. Although we performed the propensity score matching, there might be limitations in the statistical analyses due to the small size of matched population. Inverse Probability Treatment Weight (IPTW) method could be an alternative to overcome limited sample size. However, there are issues with adaptation of IPTW. In this cohort, imbalance of patient distribution in performance status and tumor location were likely the cause of poor matching. Accordingly, limited effect of concurrent chemotherapy regimen needs to be validated through further investigations. However, with the lack of studies on concurrent chemotherapy regimen, a single cycle of 5-FU may bring insights into the treatment of locally advanced rectal cancer in daily practice. In summary, the present study showed that treatment survival outcome was not significantly influenced by the regimen of concurrent preoperative chemotherapy in locally advanced rectal cancer. Although many groups have tried to show the superiority of intensified concurrent chemotherapy, our results indicate that one cycle of 5-FU, which may be considered suboptimal regimen, is associated with comparable clinical outcomes, as compared with standard chemotherapy regimen. Conflict of interests The authors declare no conflict of interests. References 1. Sebag-Montefiore D, Stephens RJ, Steele R et al. Preoperative radiotherapy versus selective postoperative chemoradiotherapy in patients with rectal cancer (MRC CR07 and NCIC-CTG C016): a multicentre, randomised trial. Lancet 2009;373: Sauer R, Becker H, Hohenberger W et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med 2004;351: Roh MS, Colangelo LH, O Connell MJ et al. Preoperative multimodality therapy improves disease-free survival in patients with carcinoma of the rectum: NSABP R-03. J Clin Oncol 2009;27: Bosset JF, Calais G, Mineur L et al. Enhanced tumoricidal effect of chemotherapy with preoperative radiotherapy for rectal cancer: preliminary results-eortc J Clin Oncol 2005;23: André T, Boni C, Mounedji-Boudiaf L et al. Oxaliplatin, fluorouracil, and leucovorin as adjuvant treatment for colon cancer. N Engl J Med 2004;350: Rödel C, Liersch T, Becker H et al. Preoperative chemoradiotherapy and postoperative chemotherapy with fluorouracil and oxaliplatin versus fluorouracil alone in locally advanced rectal cancer: initial results of the German CAO/ARO/AIO-04 randomised phase 3 trial. Lancet Oncol 2012;13: Allegra CJ, Yothers G, O Connell MJ et al. Neoadjuvant therapy for rectal cancer: Mature results from NSABP protocol R-04. J Clin Oncol 2014;32 (Suppl): Schmoll HJ, Haustermans K, Price TJ et al. Preoperative chemoradiotherapy and postoperative chemotherapy with capecitabine and oxaliplatin versus capecitabine alone in locally advanced rectal cancer: Disease-free survival results at interim analysis. J Clin Oncol 2014;32 (Suppl): Aschele C, Cionini L, Lonardi S et al. Primary tumor response to preoperative chemoradiation with or without oxaliplatin in locally advanced rectal cancer: pathologic results of the STAR-01 randomized phase III trial. J Clin Oncol 2011;29: Gérard JP, Azria D, Gourgou-Bourgade S et al. Clinical outcome of the ACCORD 12/0405 PRODIGE 2 randomized trial in rectal cancer. J Clin Oncol 2012;30: JBUON 2019; 24(2): 477
9 478 Impact of concurrent CTx regimen in rectal cancer 11. Bosset JF, Calais G, Mineur L et al. Fluorouracil-based adjuvant chemotherapy after preoperative chemoradiotherapy in rectal cancer: long-term results of the EORTC randomised study. Lancet Oncol 2014;15: Dewdney A, Cunningham D, Tabernero J et al. Multicenter randomized phase II clinical trial comparing neoadjuvant oxaliplatin, capecitabine, and preoperative radiotherapy with or without cetuximab followed by total mesorectal excision in patients with high-risk rectal cancer (EXPERT-C). J Clin Oncol 2012;30: Gollins S, Myint AS, Haylock B et al. Preoperative chemoradiotherapy using concurrent capecitabine and irinotecan in magnetic resonance imaging defined locally advanced rectal cancer: impact on long-term clinical outcomes. J Clin Oncol 2011;29: Hofheinz R-D, Wenz F, Post S et al. Chemoradiotherapy with capecitabine versus fluorouracil for locally advanced rectal cancer: a randomised, multicentre, noninferiority, phase 3 trial. Lancet Oncol 2012;13: National Comprehensive Cancer Network NCCN guidelines version 1, Rectal cancer. National Comprehensive Cancer Network. Accessed 14 June Im YH, Suh CI, Heo DS et al. The postoperative adjuvant radiation therapy and 5-fluorouracil maintenance chemotherapy for resectable rectal cancer. J Korean Cancer Assoc 1996;28: Chang HJ, Park CK, Kim WH et al. A standardized pathology report for colorectal cancer. Korean J Pathol 2006;40: Dworak O, Keilholz L, Hoffmann A. Pathological features of rectal cancer after preoperative radiochemotherapy. Int J Colorectal Dis 1997;12: Mandard AM, Dalibard F, Mandard JC et al. Pathologic assessment of tumor regression after preoperative chemoradiotherapy of esophageal carcinoma. Clinicopathologic correlations. Cancer 1994;73: Willeke F, Horisberger K, Kraus-Tiefenbacher U et al. A phase II study of capecitabine and irinotecan in combination with concurrent pelvic radiotherapy (CapIri-RT) as neoadjuvant treatment of locally advanced rectal cancer. Br J Cancer 2007;96: Navarro M, Dotor E, Rivera F et al. A Phase II study of preoperative radiotherapy and concomitant weekly irinotecan in combination with protracted venous infusion 5-fluorouracil, for resectable locally advanced rectal cancer. Int J Radiat Oncol Biol Phys 2006;66: Hurwitz H, Fehrenbacher L, Novotny W et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med 2004;350: Crane CH, Eng C, Feig BW et al. Phase II trial of neoadjuvant bevacizumab, capecitabine, and radiotherapy for locally advanced rectal cancer. Int J Radiat Oncol Biol Phys 2010;76: Hong YS, Nam BH, Kim KP et al. Oxaliplatin, fluorouracil, and leucovorin versus fluorouracil and leucovorin as adjuvant chemotherapy for locally advanced rectal cancer after preoperative chemoradiotherapy (ADORE): an open-label, multicentre, phase 2, randomised controlled trial. Lancet Oncol 2014;15: Alliance for Clinical Trials in Oncology. PROSPECT: chemotherapy alone or chemotherapy plus radiation therapy in treating patients with locally advanced rectal cancer undergoing surgery. ClinicalTrialsgov. Available at: (Accessed June 14, 2018). 26. Kuremsky JG, Tepper JE, McLeod HL. Biomarkers for response to neoadjuvant chemoradiation for rectal cancer. Int J Radiat Oncol Biol Phys 2009;74: Spolverato G, Pucciarelli S, Bertorelle R et al. Predictive factors of the response of rectal cancer to neoadjuvant radiochemotherapy. Cancers (Basel) 2011;26:2176- wq Dayde D, Tanaka I, Jain R et al. Predictive and prognostic molecular biomarkers for response to neoadjuvant chemoradiation in rectal cancer. Int J Mol Sci 2017;18. pii: E573. JBUON 2019; 24(2): 478
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
Adjuvant Chemotherapy for Rectal Cancer: Are we making progress?
 Adjuvant Chemotherapy for Rectal Cancer: Are we making progress? Hagen Kennecke, MD, MHA, FRCPC Division Of Medical Oncology British Columbia Cancer Agency October 25, 2008 Objectives Review milestones
Adjuvant Chemotherapy for Rectal Cancer: Are we making progress? Hagen Kennecke, MD, MHA, FRCPC Division Of Medical Oncology British Columbia Cancer Agency October 25, 2008 Objectives Review milestones
Evaluation of the Efficacy of Modified De Gramont and Modified FOLFOX4 Regimens for Adjuvant Therapy of Locally Advanced Rectal Cancer
 Efficacy of Modified De Gramont and FOLFOX4 Regimens for Locally Advanced Rectal Cancer RESEARCH COMMUNICATION Evaluation of the Efficacy of Modified De Gramont and Modified FOLFOX4 Regimens for Adjuvant
Efficacy of Modified De Gramont and FOLFOX4 Regimens for Locally Advanced Rectal Cancer RESEARCH COMMUNICATION Evaluation of the Efficacy of Modified De Gramont and Modified FOLFOX4 Regimens for Adjuvant
Preoperative capecitabine and pelvic radiation in locally advanced rectal cancer: preliminary results (Mansoura experience)
 Original Article Preoperative capecitabine and pelvic radiation in locally advanced rectal cancer: preliminary results (Mansoura experience) Abeer Hussien Anter 1, Ghada Ezzat Eladawei 2, Mahmoud Mosbah
Original Article Preoperative capecitabine and pelvic radiation in locally advanced rectal cancer: preliminary results (Mansoura experience) Abeer Hussien Anter 1, Ghada Ezzat Eladawei 2, Mahmoud Mosbah
Radiotherapy for rectal cancer. Karin Haustermans Department of Radiation Oncology
 Radiotherapy for rectal cancer Karin Haustermans Department of Radiation Oncology O U T L I N E RT with TME surgery? Neoadjuvant or adjuvant RT? 5 x 5 Gy or long-course CRT? RT with new drugs? Selection
Radiotherapy for rectal cancer Karin Haustermans Department of Radiation Oncology O U T L I N E RT with TME surgery? Neoadjuvant or adjuvant RT? 5 x 5 Gy or long-course CRT? RT with new drugs? Selection
Long Term Outcomes of Preoperative versus
 RESEARCH ARTICLE Long Term Outcomes of Preoperative versus Postoperative Concurrent Chemoradiation for Locally Advanced Rectal Cancer: Experience from Ramathibodi Medical School in Thailand Pichayada Darunikorn
RESEARCH ARTICLE Long Term Outcomes of Preoperative versus Postoperative Concurrent Chemoradiation for Locally Advanced Rectal Cancer: Experience from Ramathibodi Medical School in Thailand Pichayada Darunikorn
RECTAL CANCER CLINICAL CASE PRESENTATION
 RECTAL CANCER CLINICAL CASE PRESENTATION Francesco Sclafani Medical Oncologist, Clinical Research Fellow The Royal Marsden NHS Foundation Trust, London, UK esmo.org Disclosure I have nothing to declare
RECTAL CANCER CLINICAL CASE PRESENTATION Francesco Sclafani Medical Oncologist, Clinical Research Fellow The Royal Marsden NHS Foundation Trust, London, UK esmo.org Disclosure I have nothing to declare
Carcinoma del retto: Highlights
 Carcinoma del retto: Highlights Stefano Cordio Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Roma 17 Febbraio 2018 Disclosures Advisory Committee, research funding and speakers bureau
Carcinoma del retto: Highlights Stefano Cordio Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Roma 17 Febbraio 2018 Disclosures Advisory Committee, research funding and speakers bureau
Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy
 Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
Korean J Hepatobiliary Pancreat Surg 2011;15:152-156 Original Article Treatment outcomes and prognostic factors of gallbladder cancer patients after postoperative radiation therapy Suzy Kim 1,#, Kyubo
State of the art: Standard(s) of radio/chemotherapy for rectal cancer
 State of the art: Standard(s) of radio/chemotherapy for rectal cancer Dr Ian Chau Consultant Medical Oncologist The Royal Marsden Hospital London & Surrey Disclosure Advisory Board: Sanofi Oncology, Eli-
State of the art: Standard(s) of radio/chemotherapy for rectal cancer Dr Ian Chau Consultant Medical Oncologist The Royal Marsden Hospital London & Surrey Disclosure Advisory Board: Sanofi Oncology, Eli-
Case Conference. Craig Morgenthal Department of Surgery Long Island College Hospital
 Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
Preoperative or Postoperative Therapy for the Management of Patients with Stage II or III Rectal Cancer
 Evidence-Based Series 2-4 Version 2 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Preoperative or Postoperative Therapy for the Management of Patients with
Evidence-Based Series 2-4 Version 2 A Quality Initiative of the Program in Evidence-Based Care (PEBC), Cancer Care Ontario (CCO) Preoperative or Postoperative Therapy for the Management of Patients with
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp REVIEW ARTICLE Recent advances in neoadjuvant chemoradiotherapy in locally advanced rectal cancer Kazushige Kawai, Soichiro Ishihara, Hiroaki
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp REVIEW ARTICLE Recent advances in neoadjuvant chemoradiotherapy in locally advanced rectal cancer Kazushige Kawai, Soichiro Ishihara, Hiroaki
Chemoradiotherapy after gemcitabine plus erlotinib in patients with locally advanced pancreatic cancer
 JBUON 2017; 22(4): 1046-1052 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Chemoradiotherapy after gemcitabine plus erlotinib in patients with
JBUON 2017; 22(4): 1046-1052 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Chemoradiotherapy after gemcitabine plus erlotinib in patients with
Neoadjuvant Conformal Chemoradiation with Induction Chemotherapy for Rectal Adenocarcinoma. A Prospective Observational Study
 ORIGINAL PAPER Neoadjuvant Conformal Chemoradiation with Induction Chemotherapy for Rectal Adenocarcinoma. A Prospective Observational Study Zsolt Fekete 1, 2, Alina-Simona Muntean 2, Ştefan Hica 2, Alin
ORIGINAL PAPER Neoadjuvant Conformal Chemoradiation with Induction Chemotherapy for Rectal Adenocarcinoma. A Prospective Observational Study Zsolt Fekete 1, 2, Alina-Simona Muntean 2, Ştefan Hica 2, Alin
CRT AND SURGICAL resection are important elements
 Current Status and Future Directions in Preoperative Chemoradiotherapy of Rectal Cancer By Claus Rödel, MD Overview: With optimized local treatment for patients with locally advanced rectal cancer, achieved
Current Status and Future Directions in Preoperative Chemoradiotherapy of Rectal Cancer By Claus Rödel, MD Overview: With optimized local treatment for patients with locally advanced rectal cancer, achieved
M. Kripp, 1 K. Horisberger, 2 S. Mai, 3 P. Kienle, 2 T. Gaiser, 4 S. Post, 2 F. Wenz, 3 K. Merx, 1 and R.-D. Hofheinz 5. 1.
 Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2015, Article ID 273489, 8 pages http://dx.doi.org/10.1155/2015/273489 Research Article Does the Addition of Cetuximab to Radiochemotherapy
Hindawi Publishing Corporation Gastroenterology Research and Practice Volume 2015, Article ID 273489, 8 pages http://dx.doi.org/10.1155/2015/273489 Research Article Does the Addition of Cetuximab to Radiochemotherapy
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/38705 holds various files of this Leiden University dissertation. Author: Gijn, Willem van Title: Rectal cancer : developments in multidisciplinary treatment,
Cover Page The handle http://hdl.handle.net/1887/38705 holds various files of this Leiden University dissertation. Author: Gijn, Willem van Title: Rectal cancer : developments in multidisciplinary treatment,
ADJUVANT CHEMOTHERAPY FOR RECTAL CANCER
 ESMO Preceptorship Programme Colorectal Cancer Barcelona November, 25-26, 2016 ADJUVANT CHEMOTHERAPY FOR RECTAL CANCER Andrés Cervantes Professor of Medicine OLD APPROACH TO RECTAL CANCER Surgical resection
ESMO Preceptorship Programme Colorectal Cancer Barcelona November, 25-26, 2016 ADJUVANT CHEMOTHERAPY FOR RECTAL CANCER Andrés Cervantes Professor of Medicine OLD APPROACH TO RECTAL CANCER Surgical resection
Short-Course Radiation Versus Long-Course Chemoradiation for Rectal Cancer
 Original Article 1223 Short-Course Radiation Versus Long-Course Chemoradiation for Rectal Cancer Bruce D. Minsky, MD a ; Claus Rödel, MD b ; and Vincenzo Valentini, MD c Abstract The 2 broad approaches
Original Article 1223 Short-Course Radiation Versus Long-Course Chemoradiation for Rectal Cancer Bruce D. Minsky, MD a ; Claus Rödel, MD b ; and Vincenzo Valentini, MD c Abstract The 2 broad approaches
Is adjuvant radiotherapy warranted in resected pt1-2 node-positive rectal cancer?
 Peng et al. Radiation Oncology 2013, 8:290 RESEARCH Open Access Is adjuvant radiotherapy warranted in resected pt1-2 node-positive rectal cancer? Junjie Peng 1,2, Xinxiang Li 1,2, Ying Ding 3, Debing Shi
Peng et al. Radiation Oncology 2013, 8:290 RESEARCH Open Access Is adjuvant radiotherapy warranted in resected pt1-2 node-positive rectal cancer? Junjie Peng 1,2, Xinxiang Li 1,2, Ying Ding 3, Debing Shi
Jinsil Seong, MD 1 Ik Jae Lee, MD, PhD 2 Joon Seong Park, MD 3 Dong Sup Yoon, MD 3 Kyung Sik Kim, MD 4 Woo Jung Lee, MD 4 Kyung Ran Park, MD 5
 pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 216;48(2):583-595 Original Article http://dx.doi.org/1.4143/crt.215.91 Open Access Surgery Alone Versus Surgery Followed by Chemotherapy and Radiotherapy
pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 216;48(2):583-595 Original Article http://dx.doi.org/1.4143/crt.215.91 Open Access Surgery Alone Versus Surgery Followed by Chemotherapy and Radiotherapy
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain
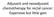 Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Patients with pathological stage N2 rectal cancer treated with early adjuvant chemotherapy have a lower treatment failure rate
 Feng et al. BMC Cancer (2017) 17:182 DOI 10.1186/s12885-017-3170-3 RESEARCH ARTICLE Open Access Patients with pathological stage N2 rectal cancer treated with early adjuvant chemotherapy have a lower treatment
Feng et al. BMC Cancer (2017) 17:182 DOI 10.1186/s12885-017-3170-3 RESEARCH ARTICLE Open Access Patients with pathological stage N2 rectal cancer treated with early adjuvant chemotherapy have a lower treatment
A clinical study of adjuvant chemotherapy in younger and elder rectal cancer patientsa
 A clinical study of adjuvant chemotherapy in younger and elder rectal cancer patientsa The role of postoperative chemotherapy (CT) is still unclear and the evidence for recommendations of adjuvant therapy
A clinical study of adjuvant chemotherapy in younger and elder rectal cancer patientsa The role of postoperative chemotherapy (CT) is still unclear and the evidence for recommendations of adjuvant therapy
Current Issues and Controversies in the Management of Rectal Cancer
 Current Issues and Controversies in the Management of Rectal Cancer Ghazi M. Nsouli MD 11 th Annual Congress of the Lebanese Society of Gastroenterology November 16, 2012 GMN 20121116 1 Staging of rectal
Current Issues and Controversies in the Management of Rectal Cancer Ghazi M. Nsouli MD 11 th Annual Congress of the Lebanese Society of Gastroenterology November 16, 2012 GMN 20121116 1 Staging of rectal
Chemotherapy of colon cancers
 Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
What Is the Ideal Tumor Regression Grading System in Rectal Cancer Patients after Preoperative Chemoradiotherapy?
 pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 216;48(3):998-19 Original Article http://dx.doi.org/1.4143/crt.215.254 Open Access What Is the Ideal Tumor Regression Grading System in Rectal Cancer Patients
pissn 1598-2998, eissn 25-9256 Cancer Res Treat. 216;48(3):998-19 Original Article http://dx.doi.org/1.4143/crt.215.254 Open Access What Is the Ideal Tumor Regression Grading System in Rectal Cancer Patients
Mini J.Elnaggar M.D. Radiation Oncology Ochsner Medical Center 9/23/2016. Background
 Mini J.Elnaggar M.D. Radiation Oncology Ochsner Medical Center 9/23/2016 Background Mostly adenocarcinoma (scc possible, but treated like anal cancer) 39, 220 cases annually Primary treatment: surgery
Mini J.Elnaggar M.D. Radiation Oncology Ochsner Medical Center 9/23/2016 Background Mostly adenocarcinoma (scc possible, but treated like anal cancer) 39, 220 cases annually Primary treatment: surgery
ACR Appropriateness Criteria Resectable Rectal Cancer EVIDENCE TABLE
 . National Cancer Institute. Comprehensive Cancer Information. http://www.cancer.gov/cancertopics/types/ colon-and-rectal. Accessed 5 January 202. 2. Rich T, Gunderson LL, Lew R, Galdibini JJ, Cohen AM,
. National Cancer Institute. Comprehensive Cancer Information. http://www.cancer.gov/cancertopics/types/ colon-and-rectal. Accessed 5 January 202. 2. Rich T, Gunderson LL, Lew R, Galdibini JJ, Cohen AM,
Opportunity for palliative care Research
 Opportunity for palliative care Research Role of Radiotherapy in Multidisciplinary Management of Rectal Cancers Dr Sushmita Pathy Associate Professor Department of Radiation Oncology Dr BRA Institute Rotary
Opportunity for palliative care Research Role of Radiotherapy in Multidisciplinary Management of Rectal Cancers Dr Sushmita Pathy Associate Professor Department of Radiation Oncology Dr BRA Institute Rotary
Retrospective analysis of the effect of CAPOX and mfolfox6 dose intensity on survival in colorectal patients in the adjuvant setting
 ORIGINAL ARTICLE CAPOX AND mfolfox6 DOSE INTENSITY AND CLINICAL OUTCOMES IN STAGE III CRC, Mamo et al. Retrospective analysis of the effect of CAPOX and mfolfox6 dose intensity on survival in colorectal
ORIGINAL ARTICLE CAPOX AND mfolfox6 DOSE INTENSITY AND CLINICAL OUTCOMES IN STAGE III CRC, Mamo et al. Retrospective analysis of the effect of CAPOX and mfolfox6 dose intensity on survival in colorectal
Irinotecan (CPT-11) in Patients with Advanced Colon Carcinoma Relapsing after 5-Fluorouracil-Leucovorin Combination
 Clinical Report Chemotherapy 2002;48:94 99 Irinotecan (CPT-11) in Patients with Advanced Colon Carcinoma Relapsing after 5-Fluorouracil-Leucovorin Combination N.B. Tsavaris a A. Polyzos b K. Gennatas c
Clinical Report Chemotherapy 2002;48:94 99 Irinotecan (CPT-11) in Patients with Advanced Colon Carcinoma Relapsing after 5-Fluorouracil-Leucovorin Combination N.B. Tsavaris a A. Polyzos b K. Gennatas c
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Clinical Study Prognostic Value of Mandard and Dworak Tumor Regression Grading in Rectal Cancer: Study of a Single Tertiary Center
 ISRN Surgery, Article ID 310542, 8 pages http://dx.doi.org/10.1155/2014/310542 Clinical Study Prognostic Value of Mandard and Dworak Tumor Regression Grading in Rectal Cancer: Study of a Single Tertiary
ISRN Surgery, Article ID 310542, 8 pages http://dx.doi.org/10.1155/2014/310542 Clinical Study Prognostic Value of Mandard and Dworak Tumor Regression Grading in Rectal Cancer: Study of a Single Tertiary
Prognostic Significance of Lymph Node Ratio in Stage III Rectal Cancer
 Original Article Journal of the Korean Society of http://dx.doi.org/10.3393/jksc.2011.27.5.252 pissn 2093-7822 eissn 2093-7830 Prognostic Significance of Lymph Node Ratio in Stage III Rectal Cancer Jin
Original Article Journal of the Korean Society of http://dx.doi.org/10.3393/jksc.2011.27.5.252 pissn 2093-7822 eissn 2093-7830 Prognostic Significance of Lymph Node Ratio in Stage III Rectal Cancer Jin
SMJ Singapore Medical Journal
 SMJ Singapore Medical Journal ONLINE FIRST PUBLICATION Online first papers have undergone full scientific review and copyediting, but have not been typeset or proofread. To cite this article, use the DOIs
SMJ Singapore Medical Journal ONLINE FIRST PUBLICATION Online first papers have undergone full scientific review and copyediting, but have not been typeset or proofread. To cite this article, use the DOIs
Neoadjuvant Therapy for Rectal Cancer is Overrated. Joon H. Lee, Research Resident University of Colorado 8/31/2009
 Neoadjuvant Therapy for Rectal Cancer is Overrated Joon H. Lee, Research Resident University of Colorado 8/31/2009 Objectives Brief overview of staging rectal cancer Current guidelines for evaluation and
Neoadjuvant Therapy for Rectal Cancer is Overrated Joon H. Lee, Research Resident University of Colorado 8/31/2009 Objectives Brief overview of staging rectal cancer Current guidelines for evaluation and
11/21/13 CEA: 1.7 WNL
 Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
Case Scenario 1 A 70 year-old white male presented to his primary care physician with a recent history of rectal bleeding. He was referred for imaging and a colonoscopy and was found to have adenocarcinoma.
RECTAL CANCER: Adjuvant Therapy. Maury Rosenstein, MD Montefiore Medical Center December 2012
 RECTAL CANCER: Adjuvant Therapy Maury Rosenstein, MD Montefiore Medical Center December 2012 Overview Indications for adjuvant therapy Preoperative Postoperative New Advances Epidemiology Approximately
RECTAL CANCER: Adjuvant Therapy Maury Rosenstein, MD Montefiore Medical Center December 2012 Overview Indications for adjuvant therapy Preoperative Postoperative New Advances Epidemiology Approximately
Adjuvant therapies for large bowel cancer Wasantha Rathnayake, MD
 LEADING ARTICLE Adjuvant therapies for large bowel cancer Wasantha Rathnayake, MD Consultant Clinical Oncologist, National Cancer Institute, Maharagama, Sri Lanka. Key words: Large bowel; Cancer; Adjuvant
LEADING ARTICLE Adjuvant therapies for large bowel cancer Wasantha Rathnayake, MD Consultant Clinical Oncologist, National Cancer Institute, Maharagama, Sri Lanka. Key words: Large bowel; Cancer; Adjuvant
Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance
 Original Article Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance Dedrick Kok Hong Chan 1,2, Ker-Kan Tan 1,2 1 Division of Colorectal Surgery, University
Original Article Lower lymph node yield following neoadjuvant therapy for rectal cancer has no clinical significance Dedrick Kok Hong Chan 1,2, Ker-Kan Tan 1,2 1 Division of Colorectal Surgery, University
ADJUVANT CHEMOTHERAPY...
 Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Management of early rectal cancer: Any role for adjuvant chemotherapy
 Management of early rectal cancer: Any role for adjuvant chemotherapy Andrés Cervantes Professor of Medicine CURRENTS CONCEPTS IN RECTAL CANCER DIAGNOSIS AND THERAPY TME surgery Optimal staging by MRI
Management of early rectal cancer: Any role for adjuvant chemotherapy Andrés Cervantes Professor of Medicine CURRENTS CONCEPTS IN RECTAL CANCER DIAGNOSIS AND THERAPY TME surgery Optimal staging by MRI
3/8/2014. Case Presentation. Primary Treatment of Anal Cancer. Anatomy. Overview. March 6, 2014
 Case Presentation Primary Treatment of Anal Cancer 65 year old female presents with perianal pain, lower GI bleeding, and anemia with Hb of 7. On exam 6 cm mass protruding through the anus with bulky R
Case Presentation Primary Treatment of Anal Cancer 65 year old female presents with perianal pain, lower GI bleeding, and anemia with Hb of 7. On exam 6 cm mass protruding through the anus with bulky R
LYMPH NODE RATIO AS A PROGNOSTIC FACTOR IN PATIENTS WITH STAGE III RECTAL CANCER TREATED WITH TOTAL MESORECTAL EXCISION FOLLOWED BY CHEMORADIOTHERAPY
 doi:10.1016/j.ijrobp.2008.08.065 Int. J. Radiation Oncology Biol. Phys., Vol. 74, No. 3, pp. 796 802, 2009 Copyright Ó 2009 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/09/$ see front
doi:10.1016/j.ijrobp.2008.08.065 Int. J. Radiation Oncology Biol. Phys., Vol. 74, No. 3, pp. 796 802, 2009 Copyright Ó 2009 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/09/$ see front
Rob Glynne-Jones Mount Vernon Cancer Centre
 ESMO Preceptorship Programme Colorectal Cancer Valencia May 2018 State of the art: Standards of care in preoperative treatment for rectal cancer Rob Glynne-Jones Mount Vernon Cancer Centre My Disclosures:
ESMO Preceptorship Programme Colorectal Cancer Valencia May 2018 State of the art: Standards of care in preoperative treatment for rectal cancer Rob Glynne-Jones Mount Vernon Cancer Centre My Disclosures:
NEOADJUVANT BEVACIZUMAB, OXALIPLATIN, 5-FLUOROURACIL, AND RADIATION FOR RECTAL CANCER
 doi:10.1016/j.ijrobp.2010.08.005 Int. J. Radiation Oncology Biol. Phys., Vol. 82, No. 1, pp. 124 129, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
doi:10.1016/j.ijrobp.2010.08.005 Int. J. Radiation Oncology Biol. Phys., Vol. 82, No. 1, pp. 124 129, 2012 Copyright Ó 2012 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/$ - see front
The impact of operation center and the prognostic factors on the outcome of patients with stage II and stage III colorectal cancer
 Turkish Journal of Cancer Volume 38, No. 4, 28 175 The impact of operation center and the prognostic factors on the outcome of patients with stage II and stage III colorectal cancer ABDULLAH BÜYÜKÇELİK
Turkish Journal of Cancer Volume 38, No. 4, 28 175 The impact of operation center and the prognostic factors on the outcome of patients with stage II and stage III colorectal cancer ABDULLAH BÜYÜKÇELİK
Advances in gastric cancer: How to approach localised disease?
 Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
UCL. Rectum Adenocarcinoma. Quality of conformal radiotherapy Impact for the surgeon P. Scalliet & K. Haustermans
 Rectum Adenocarcinoma Quality of conformal radiotherapy Impact for the surgeon P. Scalliet & K. Haustermans Fifth Belgian Surgical Week May 6th, 2004, Oostende SOR rectum adenocarcinoma Indication of radiotherapy
Rectum Adenocarcinoma Quality of conformal radiotherapy Impact for the surgeon P. Scalliet & K. Haustermans Fifth Belgian Surgical Week May 6th, 2004, Oostende SOR rectum adenocarcinoma Indication of radiotherapy
Current Status of Adjuvant Therapy for Colorectal Cancer
 Review Article [1] May 01, 2004 By Michael J. O connell, MD [2] Adjuvant therapy with chemotherapy and/or radiation therapy in addition to surgery improves outcome for patients with high-risk carcinomas
Review Article [1] May 01, 2004 By Michael J. O connell, MD [2] Adjuvant therapy with chemotherapy and/or radiation therapy in addition to surgery improves outcome for patients with high-risk carcinomas
Medicinae Doctoris. One university. Many futures.
 Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Gastroesophag Gastroesopha eal Junction Adenocarcinoma: What is the best adjuvant regimen? Michael G. G. H addock Haddock M.D.
 Gastroesophageal Junction Adenocarcinoma: What is the best adjuvant regimen? Michael G. Haddock M.D. Mayo Clinic Rochester, MN Locally Advanced GE Junction ACA CT S CT or CT S CT/RT Proposition Chemoradiation
Gastroesophageal Junction Adenocarcinoma: What is the best adjuvant regimen? Michael G. Haddock M.D. Mayo Clinic Rochester, MN Locally Advanced GE Junction ACA CT S CT or CT S CT/RT Proposition Chemoradiation
Adjuvant chemotherapy outcomes in patients over 65 years with early stage colorectal carcinoma
 JBUON 2014; 19(4): 906-912 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Adjuvant chemotherapy outcomes in patients over 65 years with early
JBUON 2014; 19(4): 906-912 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Adjuvant chemotherapy outcomes in patients over 65 years with early
Chemoradiation (CRT) Safety Analysis of ACOSOG Z6041: A Phase II Trial of Neoadjuvant CRT followed by Local Excision in ut2 Rectal Cancer
 Chemoradiation (CRT) Safety Analysis of ACOSOG Z6041: A Phase II Trial of Neoadjuvant CRT followed by Local Excision in ut2 Rectal Cancer Emily Chan, Qian Shi, Julio Garcia-Aguilar, Peter Cataldo, Jorge
Chemoradiation (CRT) Safety Analysis of ACOSOG Z6041: A Phase II Trial of Neoadjuvant CRT followed by Local Excision in ut2 Rectal Cancer Emily Chan, Qian Shi, Julio Garcia-Aguilar, Peter Cataldo, Jorge
De-Escalate Trial for the Head and neck NSSG. Dr Eleanor Aynsley Consultant Clinical Oncologist
 De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
Are we making progress? Marked reduction in operative morbidity and mortality
 Are we making progress? Surgical Progress Marked reduction in operative morbidity and mortality Introduction of Minimal-Access approaches for complex esophageal cancer resections Significantly better functional
Are we making progress? Surgical Progress Marked reduction in operative morbidity and mortality Introduction of Minimal-Access approaches for complex esophageal cancer resections Significantly better functional
Collection of Recorded Radiotherapy Seminars
 IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org Conservative Treatment of Invasive Bladder Cancer Luis Souhami, MD Professor Department of Radiation Oncology
IAEA Human Health Campus Collection of Recorded Radiotherapy Seminars http://humanhealth.iaea.org Conservative Treatment of Invasive Bladder Cancer Luis Souhami, MD Professor Department of Radiation Oncology
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
Short course radiation therapy for rectal cancer in the elderly: can radical surgery be avoided?
 Short communication Short course radiation therapy for rectal cancer in the elderly: can radical surgery be avoided? Michael A. Cummings 1, Kenneth Y. Usuki 1, Fergal J. Fleming 2, Mohamedtaki A. Tejani
Short communication Short course radiation therapy for rectal cancer in the elderly: can radical surgery be avoided? Michael A. Cummings 1, Kenneth Y. Usuki 1, Fergal J. Fleming 2, Mohamedtaki A. Tejani
Adjuvant Treatment of Pancreatic Cancer in 2009: Where Are We? Highlights from the 45 th ASCO Annual Meeting. Orlando, FL, USA. May 29 - June 2, 2009
 HIGHLIGHT ARTICLE - Slide Show Adjuvant Treatment of Pancreatic Cancer in 2009: Where Are We? Highlights from the 45 th ASCO Annual Meeting. Orlando, FL, USA. May 29 - June 2, 2009 Muhammad Wasif Saif
HIGHLIGHT ARTICLE - Slide Show Adjuvant Treatment of Pancreatic Cancer in 2009: Where Are We? Highlights from the 45 th ASCO Annual Meeting. Orlando, FL, USA. May 29 - June 2, 2009 Muhammad Wasif Saif
Original article. xx xx x xx x
 xx xx x xx x Neoadjuvant chemoradiotherapy plus adjuvant chemotherapy versus adjuvant chemoradiotherapy in the treatment of patients ANNALS with resectable OF rectal GASTROENTEROLOGY adenocarcinoma: a
xx xx x xx x Neoadjuvant chemoradiotherapy plus adjuvant chemotherapy versus adjuvant chemoradiotherapy in the treatment of patients ANNALS with resectable OF rectal GASTROENTEROLOGY adenocarcinoma: a
Treatment strategy of metastatic rectal cancer
 35.Schweizerische Koloproktologie-Tagung Treatment strategy of metastatic rectal cancer Gilles Mentha University hospital of Geneva Bern, January 18th, 2014 Colorectal cancer is the third most frequent
35.Schweizerische Koloproktologie-Tagung Treatment strategy of metastatic rectal cancer Gilles Mentha University hospital of Geneva Bern, January 18th, 2014 Colorectal cancer is the third most frequent
Present Status and Perspectives of Colorectal Cancer in Asia: Colorectal Cancer Working Group Report in 30th Asia-Pacific Cancer Conference
 Present Status and Perspectives of Colorectal Cancer in Asia: Colorectal Cancer Working Group Report in 30th Asia-Pacific Cancer Conference Jpn J Clin Oncol 2010;40(Supplement 1)i38 i43 doi:10.1093/jjco/hyq125
Present Status and Perspectives of Colorectal Cancer in Asia: Colorectal Cancer Working Group Report in 30th Asia-Pacific Cancer Conference Jpn J Clin Oncol 2010;40(Supplement 1)i38 i43 doi:10.1093/jjco/hyq125
Sponsor / Company: Sanofi Drug substance(s): Docetaxel (Taxotere )
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study
 Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Endoscopic Criteria for Evaluating Tumor Stage after Preoperative Chemoradiation Therapy in Locally Advanced Rectal Cancer
 pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2016;48(2):567-573 Original Article http://dx.doi.org/10.4143/crt.2015.195 Open Access Endoscopic Criteria for Evaluating Tumor Stage after Preoperative
pissn 1598-2998, eissn 2005-9256 Cancer Res Treat. 2016;48(2):567-573 Original Article http://dx.doi.org/10.4143/crt.2015.195 Open Access Endoscopic Criteria for Evaluating Tumor Stage after Preoperative
Introduction. Original Article
 Original Article Surgical outcomes of post chemoradiotherapy unresectable locally advanced rectal cancers improve with interim chemotherapy, is FOLFIRINOX better than CAPOX? Vikas Ostwal 1, Reena Engineer
Original Article Surgical outcomes of post chemoradiotherapy unresectable locally advanced rectal cancers improve with interim chemotherapy, is FOLFIRINOX better than CAPOX? Vikas Ostwal 1, Reena Engineer
Review Article Effect of Neoadjuvant Chemoradiotherapy with Capecitabine versus Fluorouracil for Locally Advanced Rectal Cancer: A Meta-Analysis
 Gastroenterology Research and Practice Volume 2016, Article ID 1798285, 10 pages http://dx.doi.org/10.1155/2016/1798285 Review Article Effect of Neoadjuvant Chemoradiotherapy with Capecitabine versus Fluorouracil
Gastroenterology Research and Practice Volume 2016, Article ID 1798285, 10 pages http://dx.doi.org/10.1155/2016/1798285 Review Article Effect of Neoadjuvant Chemoradiotherapy with Capecitabine versus Fluorouracil
A clinical study of metastasized rectal cancer treatment: assessing a multimodal approach
 Med Oncol (2014) 31:839 DOI 10.1007/s12032-014-0839-1 ORIGINAL PAPER A clinical study of metastasized rectal cancer treatment: assessing a multimodal approach Michaela Jung Annica Holmqvist Xiao-Feng Sun
Med Oncol (2014) 31:839 DOI 10.1007/s12032-014-0839-1 ORIGINAL PAPER A clinical study of metastasized rectal cancer treatment: assessing a multimodal approach Michaela Jung Annica Holmqvist Xiao-Feng Sun
Pre- and post-surgery treatments in rectal cancer: a long-term single-centre experience
 ORIGINAL ARTICLE Pre- and post-surgery treatments in rectal cancer: a long-term single-centre experience H. Ozyurt md phd,* A.S. Ozden md phd,* Z. Ozgen md, C. Gemici md,* and G. Yaprak md* ABSTRACT Background
ORIGINAL ARTICLE Pre- and post-surgery treatments in rectal cancer: a long-term single-centre experience H. Ozyurt md phd,* A.S. Ozden md phd,* Z. Ozgen md, C. Gemici md,* and G. Yaprak md* ABSTRACT Background
Preoperative adjuvant radiotherapy
 Preoperative adjuvant radiotherapy Dr John Hay Radiation Oncology Program BC Cancer Agency Vancouver Cancer Centre The key question for the surgeon Do you think that this tumour can be resected with clear
Preoperative adjuvant radiotherapy Dr John Hay Radiation Oncology Program BC Cancer Agency Vancouver Cancer Centre The key question for the surgeon Do you think that this tumour can be resected with clear
COLORECTAL CANCER. Bert H. O Neil, MD Jackie and Joseph Cusick Professor of Oncology Director, GI Malignancies and Phase I Program
 COLORECTAL CANCER Bert H. O Neil, MD Jackie and Joseph Cusick Professor of Oncology Director, GI Malignancies and Phase I Program Rectal Cancer Adjuvant therapy No single study specific to rectal cancer
COLORECTAL CANCER Bert H. O Neil, MD Jackie and Joseph Cusick Professor of Oncology Director, GI Malignancies and Phase I Program Rectal Cancer Adjuvant therapy No single study specific to rectal cancer
This is a repository copy of Neoadjuvant treatment strategies for locally advanced rectal cancer.
 This is a repository copy of Neoadjuvant treatment strategies for locally advanced rectal cancer. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/93146/ Version: Accepted
This is a repository copy of Neoadjuvant treatment strategies for locally advanced rectal cancer. White Rose Research Online URL for this paper: http://eprints.whiterose.ac.uk/93146/ Version: Accepted
Background: Patients and methods: Results: Conclusions:
 Chapter 7 7 Results of European pooled analysis of IORT containing multimodality treatment for locally advanced rectal cancer: adjuvant chemotherapy prevents local recurrence rather than distant metastase
Chapter 7 7 Results of European pooled analysis of IORT containing multimodality treatment for locally advanced rectal cancer: adjuvant chemotherapy prevents local recurrence rather than distant metastase
Pre-operative Chemoradiotherapy with Oral Capecitabine in Locally Advanced, Resectable Rectal Cancer
 Pre-operative Chemoradiotherapy with Oral Capecitabine in Locally Advanced, Resectable Rectal Cancer DIMITRIS P. KORKOLIS 1, CHRISTOS S. BOSKOS 2, GEORGE D. PLATANIOTIS 1, EMMANUEL GONTIKAKIS 1, IOANNIS
Pre-operative Chemoradiotherapy with Oral Capecitabine in Locally Advanced, Resectable Rectal Cancer DIMITRIS P. KORKOLIS 1, CHRISTOS S. BOSKOS 2, GEORGE D. PLATANIOTIS 1, EMMANUEL GONTIKAKIS 1, IOANNIS
Original Article. Mi Young Kim, MD 1, Jin Hee Kim, MD, PhD 1, Yonghoon Kim, MD 2, Sang Jun Byun, MD 3. Introduction
 Original Article Radiat Oncol J 16;34(4):29734 https://doi.org/1.3857/roj.16.1879 pissn 223419 eissn 22343156 Postoperative radiotherapy appeared to improve the disease free survival rate of patients with
Original Article Radiat Oncol J 16;34(4):29734 https://doi.org/1.3857/roj.16.1879 pissn 223419 eissn 22343156 Postoperative radiotherapy appeared to improve the disease free survival rate of patients with
Lymph node ratio as a prognostic factor in stage III colon cancer
 Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
Lymph node ratio as a prognostic factor in stage III colon cancer Emad Sadaka, Alaa Maria and Mohamed El-Shebiney. Clinical Oncology department, Faculty of Medicine, Tanta University, Egypt alaamaria1@hotmail.com
Advances in Multidisciplinary Treatment of Rectal Cancer
 DOI 10.1007/s11805-009-0367-5 367 Advances in Multidisciplinary Treatment of Rectal Cancer Changlin Zhao 1 Hongqin Sun 1 Yang Yang 1 Huimian Xu 2 1 Institute of Oncology Dalian University, Tumor Center,
DOI 10.1007/s11805-009-0367-5 367 Advances in Multidisciplinary Treatment of Rectal Cancer Changlin Zhao 1 Hongqin Sun 1 Yang Yang 1 Huimian Xu 2 1 Institute of Oncology Dalian University, Tumor Center,
COLORECTAL CARCINOMA
 QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
QUICK REFERENCE FOR HEALTHCARE PROVIDERS MANAGEMENT OF COLORECTAL CARCINOMA Ministry of Health Malaysia Malaysian Society of Colorectal Surgeons Malaysian Society of Gastroenterology & Hepatology Malaysian
8. The polyp in the illustration can be described as (circle all that apply) a. Exophytic b. Pedunculated c. Sessile d. Frank
 Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Differential lymph node retrieval in rectal cancer: associated factors and effect on survival
 Original Article Differential lymph node retrieval in rectal cancer: associated factors and effect on survival Cedrek McFadden 1, Brian McKinley 1, Brian Greenwell 2, Kaylee Knuckolls 1, Patrick Culumovic
Original Article Differential lymph node retrieval in rectal cancer: associated factors and effect on survival Cedrek McFadden 1, Brian McKinley 1, Brian Greenwell 2, Kaylee Knuckolls 1, Patrick Culumovic
2015 EUROPEAN CANCER CONGRESS
 2015 EUROPEAN CANCER CONGRESS 25-29 September 2015 Vienna, Austria SUMMARY The European Cancer Congress (ECC 2015) combined the 40th European Society for Medical Oncology (ESMO) congress with the 18th
2015 EUROPEAN CANCER CONGRESS 25-29 September 2015 Vienna, Austria SUMMARY The European Cancer Congress (ECC 2015) combined the 40th European Society for Medical Oncology (ESMO) congress with the 18th
Factors associated with delayed time to adjuvant chemotherapy in stage iii colon cancer
 Curr Oncol, Vol. 21, pp. 181-186 doi: http://dx.doi.org/10.3747/co.21.1963 DELAYED TIME TO ADJUVANT CHEMOTHERAPY ORIGINAL ARTICLE Factors associated with delayed time to adjuvant chemotherapy in stage
Curr Oncol, Vol. 21, pp. 181-186 doi: http://dx.doi.org/10.3747/co.21.1963 DELAYED TIME TO ADJUVANT CHEMOTHERAPY ORIGINAL ARTICLE Factors associated with delayed time to adjuvant chemotherapy in stage
Available at journal homepage:
 European Journal of Cancer (2012) 48, 1781 1790 Available at www.sciencedirect.com journal homepage: www.ejconline.com What is the clinical benefit of preoperative chemoradiotherapy with 5FU/leucovorin
European Journal of Cancer (2012) 48, 1781 1790 Available at www.sciencedirect.com journal homepage: www.ejconline.com What is the clinical benefit of preoperative chemoradiotherapy with 5FU/leucovorin
Treatment of Locally Advanced Rectal Cancer: Current Concepts
 Treatment of Locally Advanced Rectal Cancer: Current Concepts James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Treatment of Locally Advanced Rectal Cancer: Current Concepts James J. Stark, MD, FACP Medical Director, Cancer Program and Palliative Care Maryview Medical Center Professor of Medicine, EVMS Case Presentation
Oncologist. The. Gastrointestinal Cancer
 The Oncologist Gastrointestinal Cancer Addition of Bevacizumab to XELOX Induction Therapy Plus Concomitant Capecitabine-Based Chemoradiotherapy in Magnetic Resonance Imaging Defined Poor-Prognosis Locally
The Oncologist Gastrointestinal Cancer Addition of Bevacizumab to XELOX Induction Therapy Plus Concomitant Capecitabine-Based Chemoradiotherapy in Magnetic Resonance Imaging Defined Poor-Prognosis Locally
Staging of cancer patients is an important tool for the selection
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:997 1003 Improvement of Staging by Combining Tumor and Treatment Parameters: The Value for Prognostication in Rectal Cancer MARLEEN J. E. M. GOSENS,* J.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2007;5:997 1003 Improvement of Staging by Combining Tumor and Treatment Parameters: The Value for Prognostication in Rectal Cancer MARLEEN J. E. M. GOSENS,* J.
Rectal cancer: Poster Session Review
 AIOM PostASCO GI Roma, 5-6 febbraio 2016 Rectal cancer: Poster Session Review Sara Lonardi SS Trattamento Multidisciplinare Tumori Colorettali - UOC Oncologia Medica 1 Dipartimento di Oncologia Clinica
AIOM PostASCO GI Roma, 5-6 febbraio 2016 Rectal cancer: Poster Session Review Sara Lonardi SS Trattamento Multidisciplinare Tumori Colorettali - UOC Oncologia Medica 1 Dipartimento di Oncologia Clinica
Case 1 Metastatic Pancreatic Adenocarcinoma: What Therapy Should I Select First?
 Case 1 Metastatic Pancreatic Adenocarcinoma: What Therapy Should I Select First? Marc Peeters, MD, PhD Head of the Oncology Department Antwerp University Hospital Antwerp, Belgium marc.peeters@uza.be 71-year-old
Case 1 Metastatic Pancreatic Adenocarcinoma: What Therapy Should I Select First? Marc Peeters, MD, PhD Head of the Oncology Department Antwerp University Hospital Antwerp, Belgium marc.peeters@uza.be 71-year-old
Terapia neoadyuvante en cáncer de recto Estado del arte Mauricio Lema Medina MD Clínica de Oncología Astorga / Clínica SOMA - Medellín, Colombia
 Terapia neoadyuvante en cáncer de recto Estado del arte Mauricio Lema Medina MD Clínica de Oncología Astorga / Clínica SOMA - Medellín, Colombia Temario Generalidades Adyuvancia en colon y recto FU / Capecitabina
Terapia neoadyuvante en cáncer de recto Estado del arte Mauricio Lema Medina MD Clínica de Oncología Astorga / Clínica SOMA - Medellín, Colombia Temario Generalidades Adyuvancia en colon y recto FU / Capecitabina
COMETS: COlorectal MEtastatic Two Sequences
 COMETS: COlorectal MEtastatic Two Sequences A Phase III Multicenter Trial Comparing Two Different Sequences of Second/Third Line Therapy (Irinotecan/Cetuximab Followed By FOLFOX-4 vs. FOLFOX-4 Followed
COMETS: COlorectal MEtastatic Two Sequences A Phase III Multicenter Trial Comparing Two Different Sequences of Second/Third Line Therapy (Irinotecan/Cetuximab Followed By FOLFOX-4 vs. FOLFOX-4 Followed
Kaoru Takeshima, Kazuo Yamafuji, Atsunori Asami, Hideo Baba, Nobuhiko Okamoto, Hidena Takahashi, Chisato Takagi, and Kiyoshi Kubochi
 Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Original Article. Introduction
 Original Article Radiat Oncol J 216;34(4):35-312 https://doi.org/1.3857/roj.216.1914 pissn 2234-19 eissn 2234-3156 dal tumor response according to the count of peripheral blood lymphocyte subpopulations
Original Article Radiat Oncol J 216;34(4):35-312 https://doi.org/1.3857/roj.216.1914 pissn 2234-19 eissn 2234-3156 dal tumor response according to the count of peripheral blood lymphocyte subpopulations
Ning Li, Jing Jin, Jing Yu, Shuai Li, Yuan Tang, Hua Ren, Wenyang Liu, Shulian Wang, Yueping Liu, Yongwen Song, Hui Fang, Zihao Yu, Yexiong Li
 Original Article Down-staging depth score to predict outcomes in locally advanced rectal cancer achieving ypi stage after neoadjuvant chemo-radiotherapy versus de novo stage pi cohort: A propensity score-matched
Original Article Down-staging depth score to predict outcomes in locally advanced rectal cancer achieving ypi stage after neoadjuvant chemo-radiotherapy versus de novo stage pi cohort: A propensity score-matched
ESMO Preceptorship Programme, Colorectal Cancer, Vienna
 State of the art multimodal treatment of anal cancer ESMO Preceptorship Programme, Colorectal Cancer, Vienna Rob Glynne-Jones Mount Vernon Centre for Cancer Treatment Disclosures: last 5 years Speaker:
State of the art multimodal treatment of anal cancer ESMO Preceptorship Programme, Colorectal Cancer, Vienna Rob Glynne-Jones Mount Vernon Centre for Cancer Treatment Disclosures: last 5 years Speaker:
Neues zur neoadjuvanten Vorbehandlung beim Rektumkarzinom
 Neues zur neoadjuvanten Vorbehandlung beim Rektumkarzinom Prof. Dr. med. R. Fietkau Strahlenklinik Disclosure I have the following potential confilct(s) of interest to report: Type of affiliation/ financial
Neues zur neoadjuvanten Vorbehandlung beim Rektumkarzinom Prof. Dr. med. R. Fietkau Strahlenklinik Disclosure I have the following potential confilct(s) of interest to report: Type of affiliation/ financial
A multidisciplinary clinical treatment of locally advanced rectal cancer complicated with rectovesical fistula: a case report
 Zhan et al. Journal of Medical Case Reports 2012, 6:369 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A multidisciplinary clinical treatment of locally advanced rectal cancer complicated with
Zhan et al. Journal of Medical Case Reports 2012, 6:369 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access A multidisciplinary clinical treatment of locally advanced rectal cancer complicated with
