case series and historical review
|
|
|
- Bertram Baker
- 6 years ago
- Views:
Transcription
1 Kim et al. Diagnostic Pathology (2017) 12:78 DOI /s RESEARCH Open Access Composite intestinal adenomamicrocarcinoid in the colon and rectum: a case series and historical review Mi-Jung Kim 1, Eun-Jung Lee 2, Do Sun Kim 2, Doo Han Lee 2, Eui Gon Youk 2 and Hyun-Jung Kim 3* Abstract Background: Composite intestinal adenoma-microcarcinoid (CIAM) is a rare colorectal lesion that mostly comprises a conventional adenomatous component with a minute proportion of neuroendocrine (NE) component. Although microcarcinoids are well-recognized in the setting of chronic inflammatory disorders of the gastrointestinal tract, large intestinal microcarcinoids associated with intestinal adenoma are exceedingly rare and their clinicopathologic characteristics are yet to be elucidated. This study was performed to clarify their clinicopathologic characteristics and to review the relevant literature. Methods: In total, 24 cases of CIAM in which tumors were excised endoscopically (n = 22) or surgically (n =2) were retrieved from the Department of Pathology, Daehang Hospital. We analyzed their clinicopathologic characteristics and performed immunohistochemical staining for NE markers to determine their endocrine nature. Results: CIAM usually developed in middle-aged and elderly patients, with a mean age of 62.0 years (range, years). Thirteen patients were men and 11 were women, indicating a nearly equal sex ratio. Unlike classic carcinoid tumors, CIAMs occurred mostly in the colon (83.3% of cases), particularly in the proximal colon. Histologically, the microcarcinoid component consisted of low-grade NE cells arranged in small nests, glands or cords interspersed with glandular elements or less frequently resembled squamous morules. There was no expansile nodular or organoid growth pattern, which is typical of carcinoid tumors. The microcarcinoids were 1 20 mm in size (mean size, 4.7 mm) and were mostly situated in the basal lamina propria with no submucosal layer involvement; none showed desmoplastic reaction or increased proliferative activity. Follow-up data (mean, 23.1 months) were available for 18 patients; all patients are alive and well. Conclusions: To the best of our knowledge, ours is the largest series of patients with CIAM in the English-language literature. Microcarcinoids found in CIAMs appear to show favorable clinical outcomes regardless of their size, likely due to the absence of submucosal extension and/or increased proliferative activity. We recommend avoiding additional radical surgeries in patients who have endoscopically undergone complete CIAM excision unless they exhibit ominous histologic features such as submucosal extension or increased proliferative activity. Keywords: Composite intestinal adenoma, Microcarcinoid, Neuroendocrine tumor, Colorectal lesions * Correspondence: hjkim@paik.ac.kr 3 Department of Pathology, University of Inje College of Medicine, Sanggye Paik hospital, Dongil-ro 1342, Nowon-gu, Seoul, Republic of Korea Full list of author information is available at the end of the article The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Kim et al. Diagnostic Pathology (2017) 12:78 Page 2 of 9 Background Composite intestinal adenoma-microcarcinoid (CIAM) is a rare colorectal lesion that comprises conventional adenomatous components intermingled with smaller microcarcinoids [1]. Microcarcinoids refer to microscopic aggregates of monotonous cells with neuroendocrine (NE) features that do not form grossly evident masses; they have been well-described in the setting of chronic inflammatory disorders of the gastrointestinal tract, particularly the stomach [2, 3]. Large intestinal microcarcinoids are extremely rare compared to gastric lesions, and have been observed almost exclusively in patients with ulcerative colitis [4 6]. CIAM appears to be a much rarer condition than microcarcinoids that occur in the setting of ulcerative colitis; their NE cells are well-differentiated (WD) and are situated within the basal lamina propria [1, 7, 8]. They have been reported sporadically since they were first described by Pulitzer et al. [1, 7 9]. However, the nature and clinical behavior of CIAMs remain poorly understood. To attain a clearer understanding of this tumor type, we analyzed the clinicopathologic features of 24 new cases of CIAM and also reviewed previous reports of patients with this disease [1, 7 10]. Methods Study sample and histologic evaluation Twenty-four cases of CIAM were retrieved from the Department of Pathology, Daehang Hospital, between March 2011 and March Ten were retrospectively collected from pathological data files of patients treated between March 2011 and December 2013, while 14 were identified prospectively between January 2014 and March All lesions were completely excised either endoscopically (n = 22) or surgically (n = 2); 1 of the latter lesions was removed by right hemicolectomy because of the presence of a synchronous huge adenoma, and the other was removed via low anterior resection because the physician suspected a malignancy. None of the patients had any history of inflammatory bowel disease (IBD) or familial adenomatous polyposis (FAP). All specimens were routinely processed, stained with hematoxylin and eosin, and evaluated by a gastrointestinal pathology specialist (M.J.K.). The degree of dysplasia in the epithelial component was assessed according to the architectural complexity, extent of nuclear stratification, and severity of abnormal nuclear morphology, and was classified into low-grade dysplasia (LGD) or high-grade dysplasia (HGD) [11]. Tumors exhibiting lamina propria invasion with no submucosal extension were diagnosed as intramucosal carcinomas. The sizes of the polyps were measured by the pathologist, while the anatomical locations were identified and classified as the proximal colon (up to the splenic flexure) versus the distal colon/rectum. The study was performed according to the Declaration of Helsinki, and was approved by the institutional review board at Daehang Hospital (approval number DH17 001). Obtaining additional informed consent for the use of patient samples was not required, as the specimens were coded to protect patient confidentiality. Patients were assessed for clinicopathologic characteristics including age, sex, and pathology reports. Followup data (mean, 23.1 months) were available for 18 patients who underwent endoscopic procedures (n = 17) or surgery (n = 1) between March 2011 and May Two patients were lost to follow-up. The remaining samples (n = 6) were collected subsequently from patients who had not yet undergone routinely scheduled follow-up visits. Immunohistochemical staining Immunohistochemistry was manually performed by using formalin-fixed, paraffin-embedded blocks. Sections (3 μm) were cut, deparaffinized in xylene, and dehydrated in increasing concentrations of ethanol. Immunohistochemical staining was performed with antisynaptophysin (clone Z66, 1:100 dilution; Invitrogen, Melbourne, Australia), anti-chromogranin (clone NS55, 1:100 dilution; Invitrogen), and mouse monoclonal anti- Ki-67 (clone 7B11, 1:100 dilution; Invitrogen) after routine microwave antigen retrieval. Negative control samples underwent the same procedure with the omission of the primary antibody. Slides were counterstained with Mayer s hematoxylin. Immunoreactivity for synaptophysin and chromogranin was evaluated as positive or negative. Negative protein expression was defined as the complete absence of cytoplasmic staining in the microcarcinoid component in the presence of positive labeling in non-neoplastic internal control cells, while the opposite staining pattern was considered positive expression. Ki-67 immunostaining was performed to determine the proliferative activity and grade of the microcarcinoid NE cells. Nuclear immunostaining at known proliferative locations, such as germinal centers and the basal half of the crypt epithelium, was used as an internal positive control for each sample. Statistical analysis Data analyses were performed using SPSS version 21.0 (SPSS Inc., Chicago, IL, USA). Student s t-test was used to compare parametric distributions, while the χ 2 or Fisher s exact test was used for frequency distributions. A P-value <0.05 was considered statistically significant.
3 Kim et al. Diagnostic Pathology (2017) 12:78 Page 3 of 9 Results Patient demographics and tumor characteristics The patients ages ranged between 44 and 81 years (mean, 62.0 years). Samples were obtained from 13 men and 11 women(themaletofemaleratiowas1.2:1).amongthe24 cases, the majority (n = 20; 83.3%) occurred in the colon, the remaining 4 were in the rectum. Sixteen of the 20 CIAMs occurring in the colon (80.0%) affected the proximal colon. The polyp sizes ranged from 5 to 127 mm (mean, 27.2 mm). Follow-up data were available for 18 patients, all of whom are alive and well. The results are summarized in Table 1. Histologic findings and immunohistochemical staining results The microcarcinoid component was most often located in the center of the polyp with no clear demarcation from the glandular component. The microcarcinoids were 1 20 mm in size (mean size, 4.7 mm) and were mostly situated in the basal lamina propria beneath the glandular component (Fig. 1a, b). Only 5 microcarcinoids were focally extended to the muscularis mucosae with no involvement of the submucosal layer, while 1 case involved both the upper and basal portions of the lamina propria. Histologically, the NE cells within the microcarcinoid component were arranged in small nests or glands, irregular clusters, and cords with or without connections to the glandular component. Specifically 11 of 24 cases (45.8%) were connected to the glandular component (Fig. 1b). The glandular component was a conventional adenoma with LGD in most cases (86.4%) except for 2 intramucosal and 1 submucosal invasive carcinoma cases. The NE cells were sometimes scattered individually or else resembled Table 1 Clinicopathologic features of the present study Case Age (yrs) / Sex Location of polyp Procedure Polyp size (mm) Histology of glandular component Initial diagnosis Size of microcarcinoid (mm) 1 76/F Ascending colon ESD 18 IMAC, WD IMAC, WD /M Transverse colon ESD 25 IMAC, WD IMAC, WD /M Splenic flexure EMR 27 TA TA with endocrine cell proliferation 4 65/F Hepatic flexure ESD 33 TA TA /F Sigmoid colon EMR 18 TA Composite TA and 5 + carcinoid tumor 6 74/F Ascending colon ESD 23 TVA, HGD TVA, HGD, with microcarcinoid component 7 55/M Ascending colon EMR 10 TA TA and microcarcinoid /F Cecum EMR 18 TVA TVA and microcarcinoid /M Hepatic flexure RHC 17 TA TA and microcarcinoid /M Ascending colon EMR 11 SIAC, WD Adenocarcinoma, WD, with microcarcinoid component 11 59/M Splenic flexure Polypectomy 5 TA TA and microcarcinoid /M Rectum ESD 20 TVA, HGD TVA and microcarcinoid /M Rectum ESD 36 TVA, HGD TVA and microcarcinoid /M Sigmoid colon ESD 17 TA, HGD TA and microcarcinoid /F Ascending colon ESD 30 TA TA and microcarcinoid /F Rectosigmoid colon EMR 11 TA TA and microcarcinoid /F Ascending colon ESD 25 TA, HGD TA and microcarcinoid /M Ascending colon Polypectomy 20 TVA TVA and microcarcinoid /M Hepatic flexure Polypectomy 8 TA TA and microcarcinoid /M Rectum ESD 127 TVA TVA and microcarcinoid /M Transverse colon Polypectomy 12 TA TA and microcarcinoid /F Rectum LAR 100 TVA, HGD TVA and microcarcinoid /F Ascending colon ESD 28 TA TA and microcarcinoid /F Sigmoid colon EMR 13 TA TA and microcarcinoid CHR chromogranin, EMR endoscopic mucosal resection, ESD endoscopic submucosal dissection, F female, HGD high-grade dysplasia, IMAC intramucosal adenocarcinoma, LAR low anterior resection, M male, RHC right hemicolectomy, SIAC submucosal invasive adenocarcinoma, SYN synaptophysin, TA tubular adenoma, TVA tubulovillous adenoma, WD well-differentiated SYN CHR
4 Kim et al. Diagnostic Pathology (2017) 12:78 Page 4 of 9 infiltrative glands or tumor budding; however, there was no desmoplastic reaction characterized by myofibroblastic proliferation (Fig. 2a, b). Expansile nodular growth patterns or interconnected trabecular and/or lobular structures were not observed in any of the cases. The NE cells had scant to abundant eosinophilic, granular cytoplasm and round central nuclei with stippled or dusty chromatin. Two cases showed endocrine cell aggregates resembling squamous morules or metaplasia (Fig. 3a, b). All microcarcinoids consisted of monotonous cells lacking significant nuclear atypia, mitotic activity, or necrosis; however, some cases showed mild nuclear atypia. All cases were positive for synaptophysin; moreover, 18 (75.0%) expressed chromogranin-a, which was indicative of their endocrine differentiation (Figs. 1c, d, 2c, d, and 3c, d). The glandular component of the polyps did not show any generalized increase in the expression of NE markers. None of the samples exhibited an increase in the Ki-67 labeling index (all were less than 1%). The results are summarized in Table 1. Discussion Since first described by Pulitzer et al. in 2006, CIAMs have been recognized as a rare intestinal neoplasm consisting of intermingled adenomatous and WD NE components [1]. Unlike other mixed adenoneuroendocrine tumors of the large intestine in which the NE component occupies a substantial proportion of the tumor, the NE component of a CIAM occupies only a minute region of the polyp without disturbing the overall architecture [1, 11]. The NE component found in CIAM differs from classic colorectal neuroendocrinetumors(nets)inthatitdoesnotformavisible nodule and is always accompanied by a glandular neoplasm occupying the majority of the polyp by definition [1]. Additionally, most microcarcinoids in CIAMs are reportedly located in the basal lamina propria, contrary to classic NETs in which the epicenters are located in the submucosa [1, 11]. Therefore, the NE component in CIAMs is always incidentally found during the pathologic examination of adenomatous polyps, while rectal NETs are discovered during routine rectal examinations or endoscopies as submucosal masses or due to the presence of clinical symptoms such as rectal bleeding, pain, or constipation [11]. The majority of colonic NETs are large, with average sizes of 4.9 cm; therefore, they are frequently symptomatic [11]. To date, reports of CIAMs have been sporadic. The largest study was conducted by Salaria et al., who investigated 11 prospectively collected cases over a 7-year period [1, 7 10]. However, their study was limited by the fact that most cases (n = 9, 81.8%) were obtained by external consultation; therefore, clinicopathologic data regarding polyp location, procedure type, and immunohistochemical staining results for NE markers were lacking. Another study of 7 CIAM cases by Lin et al. included 5 in the large intestine and 2 in the duodenum [7]. We excluded 2 duodenal cases from our literature review because our study includes CIAMs that occurred only in the colon and rectum. We also excluded 1 of Lin Fig. 1 Histological and immunohistochemical findings of composite intestinal adenoma-microcarcinoid. a Low power magnification shows adenomatous polyp with hardly recognizable microcarcinoid component ( 40). Black arrows indicate microcarcinoid component. b High power magnification displays adenomatous glands and neuroendocrine cell nests in the lamina propria, which are connected to each other ( 200). c Immunohistochemical staining for synaptophysin shows diffuse cytoplasmic reactivity in the microcarcinoid component ( 200). d The microcarcinoid component is diffusely stained for chromogranin-a on immunostaining ( 200)
5 Kim et al. Diagnostic Pathology (2017) 12:78 Page 5 of 9 Fig. 2 Histological and immunohistochemical features of composite intestinal adenoma-microcarcinoid, mimicking invasive carcinoma. a Low power magnification shows adenomatous glands with minute microcarcinoid component (black arrows, 40). Arrow heads indicate adjacent carcinomatous area. b High power magnification reveals endocrine cell nests with angulated shape and infiltrative growth pattern, harboring the potential for misdiagnosis as carcinoma invasion ( 200). c Immunohistochemical staining for synaptophysin shows diffuse cytoplasmic reactivity in microcarcinoid component ( 200). d The microcarcinoid component displays focal positivity for chromogranin-a on immunostaining ( 200) et al. s remaining 5 cases because the lesion resembled a goblet cell carcinoid based on histologic photographs showing bland-looking glands with prominent goblet cells infiltrating the submucosa [7]. A goblet cell carcinoid is a distinct form of mixed adenoneuroendocrine tumors, which usually shows aggressive biologic behavior despite its bland-looking histology [11, 12]. We also excluded a study published by Estrella et al. because we could not clearly distinguish CIAM cases from adenoma/low-grade NETs [13]; in their study, the majority of Fig. 3 Histological and immunohistochemical features of composite intestinal adenoma-microcarcinoid, mimicking adenoma with squamous metaplasia (squamous morules). a Low power magnification shows adenomatous glands with a few eosinophilic cell nests (black arrows) in basal lamina propria ( 40). b High power magnification shows adenomatous glands and eosinophilic cell nests resembling squamous metaplasia ( 200). c Immunohistochemical staining for synaptophysin shows diffuse cytoplasmic reactivity in the eosinophilic cells nests, supporting the neuroendocrine differentiation ( 200). d The neuroendocrine component is negative for chromogranin-a on immunostaining ( 200)
6 Kim et al. Diagnostic Pathology (2017) 12:78 Page 6 of 9 cases included in the adenoma/low-grade NET category are presumed to be mixed adenoma/classic NET because a substantial proportion of their cases (40%) invaded the submucosa. Additionally, the authors classified 4 cases arising from the duodenum under the same category as 19 colorectal cases, despite pre-existing evidence indicating that the anatomic site is one of the most important factors that affect the clinical behavior of NETs [11]. Four patients known to have FAP were also included in the adenoma/low-grade NET category, raising our concerns over the pathogenetic heterogeneity of their cases, which can potentially affect the analysis of clinical outcomes. After excluding the above-mentioned cases, we summarized the clinicopathologic data of 21 previously reported CIAMs in Table 2. In our present study, we enrolled and analyzed CIAM cases that only occurred in the colon and rectum, and did not include any patients with a history of IBD or FAP to minimize the genetic and pathogenetic heterogeneity of the investigated cases (Table 1). Herein, we summarized the clinicopathologic findings of a total of 45 CIAM cases, including results from previous studies as well as our own. There were 24 men and 21 women, indicating a nearly equal sex ratio (male:female = 1.1:1). The patients ages ranged from 28 to 82 years, with a mean age of 62.6 years. Notably, the mean age among our 24 patients (62.0 years) did not significantly differ from the 21 patients in the previous studies (63.1 years, p = 0.767). Approximately two-thirds (n = 29, 64.5%) of the microcarcinoid components were accompanied by adenoma with LGD (17 tubular, 11 tubulovillous, and 1 unspecified), 12 by adenoma with HGD (4 tubular, 8 tubulovillous), 2 by intramucosal carcinoma arising in tubulovillous adenoma, and 2 by submucosal invasive adenocarcinoma. Therefore, we suggest that the terminology of CIAM might be misleading because microcarcinoids can be associated with glandular lesions that exhibit various histologic degrees of dysplasia. Contrary to classic NET, CIAMs tended to occur in the colon according to data from previous studies as well as ours, which indicated that most lesions (38 of 44, 86.4%) were located in the colon except for 6 (13.6%) that occurred in the rectum and 1 that had an unknown location. In particular, more than half of the polyps were located in the proximal colon (27 of 44 cases, 61.4%), with the most frequent site being the ascending colon (9 of 44 cases, 20.5%). The size of the polyps ranged from 5 to 127 mm, with a mean size of 23.8 mm. There was no significant difference in polyp size between our study and previous findings (27.2 mm vs mm, respectively; p = 0.277). The microcarcinoid component was confined to the mucosa with (22 of 40 cases) or without (18 of 40 cases) a connection to the glandular component. The mean size of the microcarcinoid component was 4.7 mm, and did not differ significantly in our patients compared to those in previous studies (4.7 mm vs. 3.1 mm, respectively; p = 0.201). In our study, all lesions were completely removed either by endoscopic procedures (n = 22) or surgical resection (n = 2), and no subsequent surgeries were required. This is inconsistent with the results of previous studies in which most patients underwent subsequent surgery (n = 7, 77.8%) because of incomplete or partial prior polypectomy (n = 9). Moreover, removal of the majority of samples (83.3%) by endoscopic mucosal resection (EMR, n = 7), endoscopic submucosal dissection (ESD, n = 11), and surgery (n = 2) in our study facilitated the procurement of well-oriented tissue sections perpendicular to the basal lamina and muscularis mucosae; this assisted us in collecting the largest series of CIAM samples. A microcarcinoid component cannot be detected in poorly-oriented tissue samples such as small polypectomy specimen because it is mainly located in the basal lamina propria. Nevertheless, the prevalence rate of CIAM appears to be extremely low based on our estimates. We prospectively collected 13 CIAM cases from among 40,939 patients who underwent endoscopic procedures including polypectomy, EMR, and ESD between January 2014 and March So far, the natural history as well as the pathogenetic mechanism of colorectal microcarcinoids have not been fully elucidated because of their rarity, which in turn may partly be due to their under-recognition. As a result, microcarcinoids occurring in the colon and rectum have remained an ambiguous entity denoting small-sized NE lesions in many instances. According to the definition of microcarcinoid described by Pulitzer et al., most previously reported microcarcinoids occurring in ulcerative colitis patients appear to correspond to small-sized classic NETs [1]. As for the stomach, most enterochromaffin-like cell NETs arise in patients with chronic atrophic gastritis or multiple endocrine neoplasia type 1-Zollinger-Ellison syndrome through a sequence of hyperplasia-dysplasianeoplasia, where growth patterns as well as endocrine cell sizes are known to be important for the classification of such lesions [2, 3, 11]. A gastric NE lesion is classified as a microcarcinoid when the nodule is greater than 0.5 mm but less than 5 mm in size, or if it invades the submucosa; lesions less than 0.5 mm and confined to the mucosa are designated as carcinoma in situ/dysplasia [11]. However, to our knowledge, such size-based criteria have not yet been defined in colorectal microcarcinoids. Based on our findings, the clinical outcomes of colorectal microcarcinoids appear to be quite favorable regardless of their sizes, likely because none of the patients showed submucosal invasion and/or increased proliferative activity. Considering that none of the 45 CIAM patients showed recurrence or metastasis after endoscopic or surgical treatment, even in lesions larger than or equal to 5 mm
7 Kim et al. Diagnostic Pathology (2017) 12:78 Page 7 of 9 Table 2 Clinicopathologic features of the previous studies Case Reference Age (yrs) / Sex Location of polyp Procedure Polyp size (mm) Histology of glandular component Initial diagnosis Size of microcarcinoid (mm) 1 Lyda et al., 1988 [10] 80/M Ascending colon Polypectomy followed by RHC 30 TVA, HGD TVA and carcinoid tumor NS + NS 2 Pulitzer et al., 2006 [1] 77/F Cecum Polypectomy followed by RHC <10 TA, HGD TA with HGD and endocrine NS + + neoplasia of UMP 3 Pulitzer et al., 2006 [1] 77/M Cecum Polypectomy 13 TA TA with squamous metaplasia NS + 4 Pulitzer et al., 2006 [1] 77/F Cecum Polypectomy followed by RHC 20 SIAC TVA, HGD NS Pulitzer et al., 2006 [1] 62/F Descending colon Polypectomy 5 TA TA with microcarcinoid NS Lin et al., 2012 [7] 51/M Rectum Polypectomy followed by 20 TVA TVA with microcarcinoid proctosigmoidectomy 7 Lin et al., 2012 [7] 59/M Rectum Polypectomy followed by 13 Adenoma Adenocarcinoma proctosigmoidectomy 8 Lin et al., 2012 [7] 66/F Cecum Polypectomy followed by RHC 15 TA TA and microcarcinoid 1 NS NS 9 Lin et al., 2012 [7] 56/M Sigmoid colon Polypectomy followed by 25 TVA TVA and microcarcinoid 1 NS NS transanal excision 10 Salaria et al., 2013 [8] 55/M Right colon NS 53 TA Suspicion of invasive carcinoma 2 + NS 11 Salaria et al., 2013 [8] 54/F Transverse colon NS 14 TA, HGD TA, HGD 1 NS NS 12 Salaria et al., 2013 [8] 81/F Left colon NS 12 TVA, HGD TVA, HGD Salaria et al., 2013 [8] 28/F Right colon NS 34 TVA, HGD TVA, HGD, with squamous morules Salaria et al., 2013 [8] 82/M Right colon NS 15 TVA Suspicion of invasive carcinoma Salaria et al., 2013 [8] 72/F NS NS 15 TVA NS 5 NS NS 16 Salaria et al., 2013 [8] 60/F Right colon NS 7 TVA, HGD TVA, HGD 3 17 Salaria et al., 2013 [8] 55/M Left colon NS 12 TA TA with squamous morules 7 NS NS 18 Salaria et al., 2013 [8] 48/M Left colon NS 15 TVA TVA with squamous morules Salaria et al., 2013 [8] 62/M Left colon NS 25 TVA TVA with squamous morules 4 NS NS 20 Salaria et al., 2013 [8] 51/F Left colon NS 30 TVA TVA with squamous morules 2 NS 21 Thosani et al., 2014 [9] 73/M Hepatic flexure NS NS TVA NS NS + CHR chromogranin, F female, HGD high-grade dysplasia, M male, NS not specified, RHC right hemicolectomy SIAC submucosal invasive adenocarcinoma, SYN synaptophysin, TA tubular adenoma, TVA tubulovillous adenoma, UMP uncertain malignant potential, WD well-differentiated SYN CHR
8 Kim et al. Diagnostic Pathology (2017) 12:78 Page 8 of 9 (8 of 39 cases, 20.5%), the 5 mm-size cutoff appears to be meaningless. Therefore, we posit that the absence of submucosal invasiveness and/or proliferative activity of the NE cells, and not their size, explain the favorable biologic behavior of microcarcinoids. It is also worth considering whether or not colorectal microcarcinoids are neoplastic lesions and how best to define them. We suggest that it is premature to define colorectal microcarcinoids as neoplastic lesions, particularly when these lesions are confined to the mucosa with no obvious signs of proliferative activity. Indeed, 7 of 9 patients (77.8%) in previous studies underwent additional surgery after polypectomy for fear of residual lesions and possible ominous outcome. We suggest that intramucosal WD NE lesions in the colorectum should be distinguished from classic small-sized or microscopic NETs. From a pathologist s perspective of view, awareness of microcarcinoids is critical; however, it is also important to avoid over-interpretation while not overlooking or underrecognizing such lesions. Pathologists can misinterpret microcarcinoids as high-grade lesions such as invasive components of associated glandular lesions, particularly when microcarcinoids show infiltrative or single-cell patterns, or else can consider them small-sized classic NET. In the former case, identifying desmoplastic reactions that appear as myofibroblastic proliferation as well as checking for NE differentiation are important. According to our analysis, the most common mistake was to overlook the microcarcinoid component (7 of 43 cases, 16.3%), followed by misdiagnosis of the microcarcinoid as a squamous metaplasia (squamous morules) (6 cases, 14.0%) or invasive glandular component (3 cases, 7.0%) [1, 7, 8]. To that point, a CIAM reported by Lyda et al. was diagnosed as a composite adenoma-carcinoid tumor [10]. Conclusions To our knowledge, we have reported the largest series of colorectal CIAM. Clinically, CIAM tends to develop in middle-aged to elderly patients and manifests as a colorectal polyp that is usually located in the proximal colon. Microcarcinoids found in CIAM exhibits 2 histologic patterns: they are more commonly observed as WD NE cells arranged in small clusters, glands, or cords interspersed with glandular elements; and are less commonly observed as cell aggregates resembling squamous morules. Microcarcinoids found in CIAMs appear to have favorable clinical outcomes, likely because they are not accompanied by submucosal extension and/or increased proliferative activity. We recommend avoiding further radical surgeries in patients with CIAM that was completely removed endoscopically unless they show submucosal extension or increased proliferative activity. Abbreviations CIAM: Composite intestinal adenoma-microcarcinoid; EMR: Endoscopic mucosal resection; ESD: Endoscopic submucosal dissection; FAP: Familial adenomatous polyposis; HGD: High-grade dysplasia; IBD: Inflammatory bowel disease; LAR: Low anterior resection; LGD: Low-grade dysplasia; NE: Neuroendocrine; NET: Neuroendocrine tumor; TA: Tubular adenoma; TVA: Tubulovillous adenoma; WD: Well-differentiated Acknowledgements Not applicable. Funding This study was supported by a grant-in-aid for Scientific Research from Inje University Research Foundation ( ) to Hyun-Jung Kim. Availability of data and materials Please contact author for data requests. Authors contributions MJK performed histopathological evaluations and drafted the manuscript. EJL, DSK, DHL, and EGY were responsible for the clinical data. HJK conceived the study and revised the manuscript. All authors read and approved the final manuscript. Ethics approval and consent to participate The study was performed according to the Declaration of Helsinki, and was approved by the institutional review board at Daehang Hospital (approval number DH17 001). Obtaining additional informed consent for the use of patient samples was not required, as approved by the institutional review board. Specimens were coded to protect patient confidentiality. Consent for publication Not applicable. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Pathology, Daehang hospital, BangBae3-dong, Seocho-gu, Seoul, Republic of Korea. 2 Department of Surgery, Daehang hospital, BangBae3-dong, Seocho-gu, Seoul, Republic of Korea. 3 Department of Pathology, University of Inje College of Medicine, Sanggye Paik hospital, Dongil-ro 1342, Nowon-gu, Seoul, Republic of Korea. Received: 6 August 2017 Accepted: 19 October 2017 References 1. Pulitzer M, Xu R, Suriawinata AA, Waye JD, Harpaz N. Microcarcinoids in large intestinal adenomas. Am J Surg Pathol. 2006;30: Solcia E, Bordi C, Creutzfeldt W, Dayal Y, Dayan AD, Falkmer S, et al. Histopathological classification of nonantral gastric endocrine growths in man. Digestion. 1988;41: Reinecke P, Borchard F. Pattern of gastric endocrine cells in microcarcinoidosis an immunohistochemical study of 14 gastric biopsies. Virchows Arch. 1996;428: Nascimbeni R, Villanacci V, Di Fabio F, Gavazzi E, Fellegara G, Rindi G. Solitary microcarcinoid of the rectal stump in ulcerative colitis. Neuroendocrinology. 2005;81: Stewart CJ, Matsumoto T, Jo Y, Mibu R, Hirahashi M, Yao T, et al. Multifocal microcarcinoid tumours in ulcerative colitis. J Clin Pathol. 2005;58: author reply Haidar A, Dixon MF. Solitary microcarcinoid in ulcerative colitis. Histopathology. 1992;21: Lin J, Goldblum JR, Bennett AE, Bronner MP, Liu X. Composite intestinal adenoma-microcarcinoid. Am J Surg Pathol. 2012;36:292 5.
9 Kim et al. Diagnostic Pathology (2017) 12:78 Page 9 of 9 8. Salaria SN, Abu Alfa AK, Alsaigh NY, Montgomery E, Arnold CA. Composite intestinal adenoma-microcarcinoid clues to diagnosing an under-recognised mimic of invasive adenocarcinoma. J Clin Pathol. 2013;66: Thosani N, Rao B, Ertan A, Guha S. Wide spectrum of neuroendocrine differentiation in identical appearing colon polyps: a report of 2 mixed endocrine-glandular polyps. Turk J Gastroenterol. 2014;25(Suppl 1): Lyda MH, Fenoglio-Preiser CM. Adenoma-carcinoid tumors of the colon. Arch Pathol Lab Med. 1998;122: Bosman FT, Carneiro F, Hruban RH, Theise ND. World Health Organization classification of Tumours of the digestive system. 4th ed. Lyon: IARC Press; p Tang LH, Shia J, Soslow RA, Dhall D, Wong WD, O Reilly E, et al. Pathologic classification and clinical behavior of the spectrum of goblet cell carcinoid tumors of the appendix. Am J Surg Pathol. 2008;32: Estrella JS, Taggart MW, Rashid A, Abraham SC. Low-grade neuroendocrine tumors arising in intestinal adenomas: evidence for alterations in the adenomatous polyposis coli/β-catenin pathway. Hum Pathol. 2014;45: Submit your next manuscript to BioMed Central and we will help you at every step: We accept pre-submission inquiries Our selector tool helps you to find the most relevant journal We provide round the clock customer support Convenient online submission Thorough peer review Inclusion in PubMed and all major indexing services Maximum visibility for your research Submit your manuscript at
Large Colorectal Adenomas An Approach to Pathologic Evaluation
 Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
Anatomic Pathology / LARGE COLORECTAL ADENOMAS AND PATHOLOGIC EVALUATION Large Colorectal Adenomas An Approach to Pathologic Evaluation Elizabeth D. Euscher, MD, 1 Theodore H. Niemann, MD, 1 Joel G. Lucas,
GOBLET CELL CARCINOID. Hanlin L. Wang, MD, PhD University of California Los Angeles
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to
Disclosure of Relevant Financial Relationships
 Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any relevant financial relationship WITH COMMERCIAL INTERESTS
The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin
 The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin 24.06.15 Norman Barrett Smiles [A brief digression - Chair becoming
The Pathologist s Role in the Diagnosis and Management of Neoplasia in Barrett s Oesophagus Cian Muldoon, St. James s Hospital, Dublin 24.06.15 Norman Barrett Smiles [A brief digression - Chair becoming
5/2/2018. Low Grade Dysplasia of GI Tract. High Grade Dysplasia of GI Tract. Dysplasia in Gastrointestinal Tract: Practical Pearls and Issues
 Dysplasia in Gastrointestinal Tract: Practical Pearls and Issues Arief Suriawinata, M.D. Professor of Pathology and Laboratory Medicine Geisel School of Medicine at Dartmouth Department of Pathology and
Dysplasia in Gastrointestinal Tract: Practical Pearls and Issues Arief Suriawinata, M.D. Professor of Pathology and Laboratory Medicine Geisel School of Medicine at Dartmouth Department of Pathology and
Oesophagus and Stomach update dysplasia and early cancer
 Oesophagus and Stomach update dysplasia and early cancer Dr Tim Bracey STR teaching 13/4/16 Please check pathkids.com for previous talks One of the biggest units in the country (100 major resections per
Oesophagus and Stomach update dysplasia and early cancer Dr Tim Bracey STR teaching 13/4/16 Please check pathkids.com for previous talks One of the biggest units in the country (100 major resections per
Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens
 ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
ISPUB.COM The Internet Journal of Pathology Volume 12 Number 1 Morphologic Criteria of Invasive Colonic Adenocarcinoma on Biopsy Specimens C Rose, H Wu Citation C Rose, H Wu.. The Internet Journal of Pathology.
Gastric Polyps. Bible class
 Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Gastric Polyps Bible class 29.08.2018 Starting my training in gastroenterology, some decades ago, my first chief always told me that colonoscopy may seem technically more challenging but gastroscopy has
Colon and Rectum. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6th edition
 Colon and Rectum Protocol applies to all invasive carcinomas of the colon and rectum. Carcinoid tumors, lymphomas, sarcomas, and tumors of the vermiform appendix are excluded. Protocol revision date: January
Colon and Rectum Protocol applies to all invasive carcinomas of the colon and rectum. Carcinoid tumors, lymphomas, sarcomas, and tumors of the vermiform appendix are excluded. Protocol revision date: January
CASE REPORT. Introduction. Case Report. Kimitoshi Kubo 1, Noriko Kimura 2, Katsuhiro Mabe 1, Yusuke Nishimura 1 and Mototsugu Kato 1
 doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
doi: 10.2169/internalmedicine.0842-18 Intern Med 57: 2951-2955, 2018 http://internmed.jp CASE REPORT Synchronous Triple Gastric Cancer Incorporating Mixed Adenocarcinoma and Neuroendocrine Tumor Completely
Colonic Polyp. Najmeh Aletaha. MD
 Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Colonic Polyp Najmeh Aletaha. MD 1 Polyps & classification 2 Colorectal cancer risk factors 3 Pathogenesis 4 Surveillance polyp of the colon refers to a protuberance into the lumen above the surrounding
Case history: Figure 1. H&E, 5x. Figure 2. H&E, 20x.
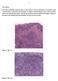 1 Case history: A 49 year-old female presented with a 5 year history of chronic anal fissure. The patient s past medical history is otherwise unremarkable. On digital rectal examination there was a very
1 Case history: A 49 year-old female presented with a 5 year history of chronic anal fissure. The patient s past medical history is otherwise unremarkable. On digital rectal examination there was a very
Hyperplastische Polyps Innocent bystanders?
 Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
Hyperplastische Polyps Innocent bystanders?? K. Geboes P th l i h O tl dk d Pathologische Ontleedkunde, KULeuven Content Historical Classification Relation Hyperplastic polyps carcinoma The concept cept
8. The polyp in the illustration can be described as (circle all that apply) a. Exophytic b. Pedunculated c. Sessile d. Frank
 Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
Quiz 1 Overview 1. Beginning with the cecum, which is the correct sequence of colon subsites? a. Cecum, ascending, splenic flexure, transverse, hepatic flexure, descending, sigmoid. b. Cecum, ascending,
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID
 ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
ENDOLUMINAL APPROACH FOR THE MANAGEMENT OF GASTROINTESTINAL CARCINOID Manoop S. Bhutani, MD, FASGE, FACG, FACP, AGAF, Doctor Honoris Causa Professor of Medicine Eminent Scientist of the Year 2008, World
Expert panel observations
 Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
Expert panel observations Professor Neil A Shepherd Gloucester and Cheltenham, UK Gloucestershire Cellular Pathology Laboratory Three big issues in BCSP pathology serrated pathology & what do we do about
removal of adenomatous polyps detects important effectively as follow-up colonoscopy after both constitute a low-risk Patients with 1 or 2
 Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Supplementary Table 1. Study Characteristics Author, yr Design Winawer et al., 6 1993 National Polyp Study Jorgensen et al., 9 1995 Funen Adenoma Follow-up Study USA Multi-center, RCT for timing of surveillance
Gastric and Oesophageal Neuroendocrine tumours. Dr Tim Bracey, Consultant Pathologist MBChB PhD MRCS FRCPath
 Gastric and Oesophageal Neuroendocrine tumours Dr Tim Bracey, Consultant Pathologist MBChB PhD MRCS FRCPath Intestinal (and BO) endocrine cells in crypt bases NE cell (granules towards vessels) Paneth
Gastric and Oesophageal Neuroendocrine tumours Dr Tim Bracey, Consultant Pathologist MBChB PhD MRCS FRCPath Intestinal (and BO) endocrine cells in crypt bases NE cell (granules towards vessels) Paneth
Imaging Evaluation of Polyps. CT Colonography: Sessile Adenoma. Polyps, DALMs & Megacolon Objectives
 Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
Polyps, DALMs & Megacolon: Pathology and Imaging of the Colon and Rectum Angela D. Levy and Leslie H. Sobin Washington, DC Drs. Levy and Sobin have indicated that they have no relationships which, in the
Mody. AIS vs. Invasive Adenocarcinoma of the Cervix
 Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
Surveying the Colon; Polyps and Advances in Polypectomy
 Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
Surveying the Colon; Polyps and Advances in Polypectomy Educational Objectives Identify classifications of polyps Describe several types of polyps Verbalize rationale for polypectomy Identify risk factors
malignant polyp Daily Challenges in Digestive Endoscopy for Endoscopists and Endoscopy Nurses BSGIE Annual Meeting 18/09/2014 Mechelen
 Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Plan Incidental finding of a malignant polyp 1. What is a polyp malignant? 2. Role of the pathologist and the endoscopist 3. Quantitative and qualitative risk assessment 4. How to decide what to do? Hubert
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Kaminski MF, Regula J, Kraszewska E, et al. Quality indicators
Synchronous and Subsequent Lesions of Serrated Adenomas and Tubular Adenomas of the Colorectum
 Tsumura T, et al 1 Synchronous and Subsequent Lesions of Serrated Adenomas and Tubular Adenomas of the Colorectum T. Tsumura a T. Hiyama d S. Tanaka b M. Yoshihara d K. Arihiro c K. Chayama a Departments
Tsumura T, et al 1 Synchronous and Subsequent Lesions of Serrated Adenomas and Tubular Adenomas of the Colorectum T. Tsumura a T. Hiyama d S. Tanaka b M. Yoshihara d K. Arihiro c K. Chayama a Departments
Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects
 Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects Patient Group Macroscopic examination Ileum Histology Colon/rectum Histology 1 INR Normal Acute and chronic
Supplemental Digital Content 1. Endoscopic and histolological findings in INR and FR study subjects Patient Group Macroscopic examination Ileum Histology Colon/rectum Histology 1 INR Normal Acute and chronic
A916: rectum: adenocarcinoma
 General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
General facts of colorectal cancer The colon has cecum, ascending, transverse, descending and sigmoid colon sections. Cancer can start in any of the r sections or in the rectum. The wall of each of these
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus
 Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Histopathology of Endoscopic Resection Specimens from Barrett's Esophagus Br J Surg 38 oct. 1950 Definition of Barrett's esophagus A change in the esophageal epithelium of any length that can be recognized
Page 1. Is the Risk This High? Dysplasia in the IBD Patient. Dysplasia in the Non IBD Patient. Increased Risk of CRC in Ulcerative Colitis
 Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Screening for Colorectal Neoplasia in Inflammatory Bowel Disease Francis A. Farraye MD, MSc Clinical Director, Section of Gastroenterology Co-Director, Center for Digestive Disorders Boston Medical Center
Figure 1. Polypectomy specimen. Inset: Colonoscopy.
 Case: A 69 year- old man with a history of gastrointestinal polyps presents with occult blood in the stool and iron deficiency anemia. He reports no weight loss, melena or hematochezia. Colonoscopy shows
Case: A 69 year- old man with a history of gastrointestinal polyps presents with occult blood in the stool and iron deficiency anemia. He reports no weight loss, melena or hematochezia. Colonoscopy shows
References. GI Biopsies. What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD
 What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD jcrawford1@nshs.edu Executive Director and Senior Vice President for Laboratory Services North
What Should Pathologists Assistants Know About Gastrointestinal Histopathology? James M Crawford, MD, PhD jcrawford1@nshs.edu Executive Director and Senior Vice President for Laboratory Services North
Serotonin- and Somatostatin-Positive Goblet Cell Carcinoid of the Duodenum
 2012 66 4 351 356 Serotonin- and Somatostatin-Positive Goblet Cell Carcinoid of the Duodenum a b* c c c a a b d a c b d 352 Ohara et al. received remedies at another hospital. Hematemesis then recurred
2012 66 4 351 356 Serotonin- and Somatostatin-Positive Goblet Cell Carcinoid of the Duodenum a b* c c c a a b d a c b d 352 Ohara et al. received remedies at another hospital. Hematemesis then recurred
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci. Colon polyps. Colorectal cancer
 Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Patologia sistematica V Gastroenterologia Prof. Stefano Fiorucci Colon polyps Colorectal cancer Harrison s Principles of Internal Medicine 18 Ed. 2012 Colorectal cancer 70% Colorectal cancer CRC and colon
Primary mucinous adenocarcinoma developing in an ileostomy stoma
 Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
Gut, 1988, 29, 1607-1612 Primary mucinous adenocarcinoma developing in an ileostomy stoma P J SMART, S SASTRY, AND S WELLS From the Departments of Histopathology and Surgery, Bolton General Hospital, Fan
DIGESTIVE TRACT ESOPHAGUS
 DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
DIGESTIVE TRACT From the lower esophagus to the lower rectum four fundamental layers comprise the wall of the digestive tube: mucosa, submucosa, muscularis propria (externa), and adventitia or serosa (see
12/7/2011. Pathological mimics of malignancy in the GI tract. Professor Neil A Shepherd President, British Division of the IAP
 Pathological mimics of malignancy in the GI tract Professor Neil A Shepherd President, British Division of the IAP IAP-AD, Beirut, Lebanon 1 December 2011 How do we become aware of the problems and the
Pathological mimics of malignancy in the GI tract Professor Neil A Shepherd President, British Division of the IAP IAP-AD, Beirut, Lebanon 1 December 2011 How do we become aware of the problems and the
Clinicopathological Characteristics of Superficial Type
 Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 99-105 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 99-105 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
Neoplastic Colon Polyps. Joyce Au SUNY Downstate Grand Rounds, October 18, 2012
 Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Neoplastic Colon Polyps Joyce Au SUNY Downstate Grand Rounds, October 18, 2012 CASE 55M with Hepatitis C, COPD (FEV1=45%), s/p vasectomy, knee surgery Meds: albuterol, flunisolide, mometasone, tiotropium
Wendy L Frankel. Chair and Distinguished Professor
 1 Wendy L Frankel Chair and Distinguished Professor Case 1 59 y/o woman Abdominal pain No personal or family history of cancer History of colon polyps Colonoscopy Polypoid rectosigmoid mass Biopsy 3 4
1 Wendy L Frankel Chair and Distinguished Professor Case 1 59 y/o woman Abdominal pain No personal or family history of cancer History of colon polyps Colonoscopy Polypoid rectosigmoid mass Biopsy 3 4
Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens
 The Korean Journal of Pathology 2006; 40: 32-8 Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens In Gu Do Youn Wha Kim Yong-Koo Park Department
The Korean Journal of Pathology 2006; 40: 32-8 Expression of the GLUT1 and p53 Protein in Atypical Mucosal Lesions Obtained from Gastric Biopsy Specimens In Gu Do Youn Wha Kim Yong-Koo Park Department
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines
 Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
Alberta Colorectal Cancer Screening Program (ACRCSP) Post Polypectomy Surveillance Guidelines June 2013 ACRCSP Post Polypectomy Surveillance Guidelines - 2 TABLE OF CONTENTS Background... 3 Terms, Definitions
3/30/2017. Disclosure of Relevant Financial Relationships. Case 5: Polypoid mass in ulcerative colitis. Case 5. TC Smyrk
 Case 5: Polypoid mass in ulcerative colitis TC Smyrk Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any
Case 5: Polypoid mass in ulcerative colitis TC Smyrk Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control the content of CME disclose any
Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of
 Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Disorders of Cell Growth & Neoplasia. Histopathology Lab
 Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
Colon and Rectum: 2018 Solid Tumor Rules
 2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Colon and Rectum: 2018 Solid Tumor Rules 1 Colon and Rectum Solid Tumor Rules Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent
Synonyms. Nephrogenic metaplasia Mesonephric adenoma
 Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you)
 What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
What Every Pathologist Wants the GI Nurse to Know (and how you can help us help you) Jonathan N. Glickman MD PhD Director, GI Pathology, Caris Diagnostics, Newton, MA Associate Professor of Pathology,
Cross-sectional Imaging of Neuroendocrine Tumors of the Gastrointestinal Tract
 Cross-sectional Imaging of Neuroendocrine Tumors of the Gastrointestinal Tract Eric J. May 1, Shannon P. Sheedy 1, Joel G. Fletcher 1, Mark J. Truty 2, Thomas C. Smyrk 3, Jeff L. Fidler 1 1. Radiology,
Cross-sectional Imaging of Neuroendocrine Tumors of the Gastrointestinal Tract Eric J. May 1, Shannon P. Sheedy 1, Joel G. Fletcher 1, Mark J. Truty 2, Thomas C. Smyrk 3, Jeff L. Fidler 1 1. Radiology,
Incidence and Multiplicities of Adenomatous Polyps in TNM Stage I Colorectal Cancer in Korea
 Original Article Journal of the Korean Society of J Korean Soc Coloproctol 2012;28(4):213-218 http://dx.doi.org/10.3393/jksc.2012.28.4.213 pissn 2093-7822 eissn 2093-7830 Incidence and Multiplicities of
Original Article Journal of the Korean Society of J Korean Soc Coloproctol 2012;28(4):213-218 http://dx.doi.org/10.3393/jksc.2012.28.4.213 pissn 2093-7822 eissn 2093-7830 Incidence and Multiplicities of
Colorectal Cancer Structured Pathology Reporting Proforma DD MM YYYY
 Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
Colorectal Cancer Structured Pathology Reporting Proforma Mandatory questions (i.e. protocol standards) are in bold (e.g. S1.03). Family name Given name(s) Date of birth DD MM YYYY S1.02 Clinical details
GOBLET CELL CARCINOID. Hanlin L. Wang, MD, PhD University of California Los Angeles
 GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles hanlinwang@mednet.ucla.edu Goblet cell carcinoid (GCC) is a unique type of mixed endocrine-exocrine neoplasm, almost exclusively
GOBLET CELL CARCINOID Hanlin L. Wang, MD, PhD University of California Los Angeles hanlinwang@mednet.ucla.edu Goblet cell carcinoid (GCC) is a unique type of mixed endocrine-exocrine neoplasm, almost exclusively
Neuroendocrine tumors of GI and Pancreatobiliary tracts. N. Volkan Adsay, MD
 Neuroendocrine tumors of GI and Pancreatobiliary tracts N. Volkan Adsay, MD New (2017) WHO WHO 2017 (endocrine book; for pancreas) WHO 2017 (endocrine book; for pancreas) PD-NE ca WD-NE Tumor Intended
Neuroendocrine tumors of GI and Pancreatobiliary tracts N. Volkan Adsay, MD New (2017) WHO WHO 2017 (endocrine book; for pancreas) WHO 2017 (endocrine book; for pancreas) PD-NE ca WD-NE Tumor Intended
Gastroenterology Tutorial
 Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Gastroenterology Tutorial Gastritis Poorly defined term that refers to inflammation of the stomach. Infection with H. pylori is the most common cause of gastritis. Most patients remain asymptomatic Some
Unexpected Findings at Endoscopy
 The Endoscopic Incidentaloma: What to Tell Your Patient t with Unexpected Endoscopic Findings: Gastric Intestinal Metaplasia, Silent Ileitis, Carcinoid David Greenwald, MD Montefiore Medical Center Albert
The Endoscopic Incidentaloma: What to Tell Your Patient t with Unexpected Endoscopic Findings: Gastric Intestinal Metaplasia, Silent Ileitis, Carcinoid David Greenwald, MD Montefiore Medical Center Albert
IMMUNOHISTOCHEMICAL ASSESSMENT OF ULCERATIVE COLITIS-RELATED DYSPLASIA Tiberia Ilias 1, O. Fratila 2, T. Maghiar 2, Dana Puscasiu 2
 IMMUNOHISTOCHEMICAL ASSESSMENT OF ULCERATIVE COLITIS-RELATED DYSPLASIA Tiberia Ilias 1, O. Fratila 2, T. Maghiar 2, Dana Puscasiu 2 ¹ORADEA CLINICAL COUNTY HOSPITAL- 3 RD MEDICAL CLINIC ²UNIVERSITY OF
IMMUNOHISTOCHEMICAL ASSESSMENT OF ULCERATIVE COLITIS-RELATED DYSPLASIA Tiberia Ilias 1, O. Fratila 2, T. Maghiar 2, Dana Puscasiu 2 ¹ORADEA CLINICAL COUNTY HOSPITAL- 3 RD MEDICAL CLINIC ²UNIVERSITY OF
A Significant Number of Sessile Serrated Adenomas Might Not Be Accurately Diagnosed in Daily Practice
 Gut and Liver, Vol. 4, No. 4, December 2010, pp. 498-502 original article A Significant Number of Sessile Serrated Adenomas Might Not Be Accurately Diagnosed in Daily Practice Soo Woong Kim*, Jae Myung
Gut and Liver, Vol. 4, No. 4, December 2010, pp. 498-502 original article A Significant Number of Sessile Serrated Adenomas Might Not Be Accurately Diagnosed in Daily Practice Soo Woong Kim*, Jae Myung
Surgical Management of Neuroendocrine Tumors of the Gut. Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School
 Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Surgical Management of Neuroendocrine Tumors of the Gut Richard Hodin MD Professor of Surgery Massachusetts General Hospital Harvard Medical School Sites of GI Carcinoid Tumors Small intestine 44% Rectum
Colorectal adenocarcinoma leading cancer in developed countries In US, annual deaths due to colorectal adenocarcinoma 57,000.
 Colonic Neoplasia Remotti Colorectal adenocarcinoma leading cancer in developed countries In US, annual incidence of colorectal adenocarcinoma 150,000. In US, annual deaths due to colorectal adenocarcinoma
Colonic Neoplasia Remotti Colorectal adenocarcinoma leading cancer in developed countries In US, annual incidence of colorectal adenocarcinoma 150,000. In US, annual deaths due to colorectal adenocarcinoma
ESMO Preceptorship Gastrointestinal Tumours Valencia October 2017
 www.esmo.org ESMO Preceptorship Valencia 06-07 October 2017 Gastrointestinal Tumours I have no conflicts of interest to declare Fátima Carneiro Gastrointestinal tumours Multidisciplinary management, standards
www.esmo.org ESMO Preceptorship Valencia 06-07 October 2017 Gastrointestinal Tumours I have no conflicts of interest to declare Fátima Carneiro Gastrointestinal tumours Multidisciplinary management, standards
Principles of diagnosis, work-up and therapy The Gastroenterologist s role
 Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Principles of diagnosis, work-up and therapy The Gastroenterologist s role Dr. Christos G. Toumpanakis MD PhD FRCP Consultant in Gastroenterology/Neuroendocrine Tumours Hon. Senior Lecturer University
Four Cases of Large Cell Neuroendocrine Carcinoma of the Stomach: Findings on CT and Barium Studies 1
 Four Cases of Large Cell Neuroendocrine Carcinoma of the Stomach: Findings on CT and arium Studies 1 Hee Jung Kim, M.D., Dongil Choi, M.D., Soon Jin Lee, M.D., Won Jae Lee, M.D., Sung Kim, M.D. 2, Jae
Four Cases of Large Cell Neuroendocrine Carcinoma of the Stomach: Findings on CT and arium Studies 1 Hee Jung Kim, M.D., Dongil Choi, M.D., Soon Jin Lee, M.D., Won Jae Lee, M.D., Sung Kim, M.D. 2, Jae
Polypoid lesions of the gastrointestinal tract
 Polypoid lesions of the gastrointestinal tract Professor Neil A Shepherd Gloucester & Cheltenham, UK 27 th IAP-AD Congress 2 nd Emirates Surgical Pathology Conference Dubai, 26 November 2015 Polypoid lesions
Polypoid lesions of the gastrointestinal tract Professor Neil A Shepherd Gloucester & Cheltenham, UK 27 th IAP-AD Congress 2 nd Emirates Surgical Pathology Conference Dubai, 26 November 2015 Polypoid lesions
FINAL HISTOLOGICAL DIAGNOSIS: Villo-adenomatous polyp with in-situ-carcinomatous foci (involving both adenomatous and villous component).
 SOLITARY VILLO ADENOMATOUS POLYP WITH CARCINOMATOUS CHANGES RECTUM: A Divvya B 1, M. Valluvan 2, Rehana Tippoo 3, P. Viswanathan 4, R. Baskaran 5 HOW TO CITE THIS ARTICLE: Divvya B, M. Valluvan, Rehana
SOLITARY VILLO ADENOMATOUS POLYP WITH CARCINOMATOUS CHANGES RECTUM: A Divvya B 1, M. Valluvan 2, Rehana Tippoo 3, P. Viswanathan 4, R. Baskaran 5 HOW TO CITE THIS ARTICLE: Divvya B, M. Valluvan, Rehana
Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors
 Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors Jaume Capdevila, MD, PhD Vall d'hebron University Hospital Vall d'hebron Institute of Oncology (VHIO)
Gastrointestinal Neuroendocrine Tumors: A Closer Look at the Characteristics of These Diverse Tumors Jaume Capdevila, MD, PhD Vall d'hebron University Hospital Vall d'hebron Institute of Oncology (VHIO)
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy
 Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Greater Manchester & Cheshire Guidelines for Pathology Reporting for Oesophageal and Gastric Malignancy Authors: Dr Gordon Armstrong, Dr Sue Pritchard 1. General Comments 1.1 Cancer reporting: Biopsies
Rectal biopsy as an aid to cancer control in ulcerative colitis
 Rectal biopsy as an aid to cancer control in ulcerative colitis B. C. MORSON AND LILLIAN S. C. PANG From the Research Department, St. Mark's Hospital, London Gut, 1967, 8, 423 EDITORIAL COMMENT This is
Rectal biopsy as an aid to cancer control in ulcerative colitis B. C. MORSON AND LILLIAN S. C. PANG From the Research Department, St. Mark's Hospital, London Gut, 1967, 8, 423 EDITORIAL COMMENT This is
Is Endoscopic Resection for Type 1 Gastric Neuroendocrine Tumors Essential for Treatment?: Multicenter, Retrospective Long-term Follow-up Results
 ORIGINAL ARTICLE ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2016.16.1.13 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2016;16(1):13-18 Is Endoscopic Resection for Type
ORIGINAL ARTICLE ISSN 1738-3331, http://dx.doi.org/10.7704/kjhugr.2016.16.1.13 The Korean Journal of Helicobacter and Upper Gastrointestinal Research, 2016;16(1):13-18 Is Endoscopic Resection for Type
COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING
 COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING COLON AND RECTUM SOLID TUMOR RULES Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent Terms Terms that are NOT Equivalent
COLON AND RECTUM SOLID TUMOR RULES ABSTRACTORS TRAINING COLON AND RECTUM SOLID TUMOR RULES Separate sections for: Introduction Changes from 2007 MP/H rules Equivalent Terms Terms that are NOT Equivalent
Histopathology: gastritis and peptic ulceration
 Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Histopathology: gastritis and peptic ulceration These presentations are to help you identify, and to test yourself on identifying, basic histopathological features. They do not contain the additional factual
Cytokeratin 5/6 expression in bladder cancer: association with clinicopathologic parameters and prognosis
 https://doi.org/10.1186/s13104-018-3319-4 BMC Research Notes RESEARCH NOTE Open Access Cytokeratin 5/6 expression in bladder cancer: association with clinicopathologic parameters and prognosis Atif Ali
https://doi.org/10.1186/s13104-018-3319-4 BMC Research Notes RESEARCH NOTE Open Access Cytokeratin 5/6 expression in bladder cancer: association with clinicopathologic parameters and prognosis Atif Ali
Sessile Serrated Polyps
 Årsmøtet i Den norske Patologforening 2014 Sessile Serrated Polyps Tor J. Eide Oslo Universitetssykehus The term serrated include a group of lesions with a sawtoothlike appearance of the crypts and the
Årsmøtet i Den norske Patologforening 2014 Sessile Serrated Polyps Tor J. Eide Oslo Universitetssykehus The term serrated include a group of lesions with a sawtoothlike appearance of the crypts and the
Small Bowel Cases. Introduction. Introduction, Continued 12/7/2011. Lesions Found on endoscopic biopsies Just Like Signing Out
 Small Bowel Cases Lesions Found on endoscopic biopsies Just Like Signing Out Introduction Small intestinal biopsies have a few special pitfalls, for example: Neuroendocrine tumors are readily mistaken
Small Bowel Cases Lesions Found on endoscopic biopsies Just Like Signing Out Introduction Small intestinal biopsies have a few special pitfalls, for example: Neuroendocrine tumors are readily mistaken
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions
 Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
Barrett s Esophagus: Review of Diagnostic Issues and Pre- Neoplastic Lesions Robert Odze, MD, FRCPC Chief, Gastrointestinal Pathology Associate Professor of Pathology Brigham and Women s Hospital Harvard
SAM PROVIDER TOOLKIT
 THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
THE AMERICAN BOARD OF PATHOLOGY Maintenance of Certification (MOC) Program SAM PROVIDER TOOLKIT Developing Self-Assessment Modules (SAMs) www.abpath.org The American Board of Pathology (ABP) approves educational
Endometriosis in the rectum accompanied by hemorrhoids leading to diagnostic pitfalls: a rare case report
 Shi and Fan BMC Women's Health (2018) 18:120 https://doi.org/10.1186/s12905-018-0615-z CASE REPORT Open Access Endometriosis in the rectum accompanied by hemorrhoids leading to diagnostic pitfalls: a rare
Shi and Fan BMC Women's Health (2018) 18:120 https://doi.org/10.1186/s12905-018-0615-z CASE REPORT Open Access Endometriosis in the rectum accompanied by hemorrhoids leading to diagnostic pitfalls: a rare
Small Intestine. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition
 Small Intestine Protocol applies to all invasive carcinomas of the small intestine, including those with focal endocrine differentiation. Excludes carcinoid tumors, lymphomas, and stromal tumors (sarcomas).
Small Intestine Protocol applies to all invasive carcinomas of the small intestine, including those with focal endocrine differentiation. Excludes carcinoid tumors, lymphomas, and stromal tumors (sarcomas).
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis.
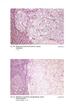 Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
Fig. 59 Malignant phaeochromocytoma, hepatic metastasis. X 120 Hyperte nsion Fig. 60 Malignant sympathetic paraganglioma, lymph node metastasis Primary in bladder. x 1 20 Hypertension Fig. 61 Malignant
Chapter 6 Frozen Section Evaluation of the Appendix
 Chapter 6 Frozen Section Evaluation of the Appendix Abstract Appendiceal tumors are rarely diagnosed preoperatively, and their classification is both challenging and controversial owing to their tendency
Chapter 6 Frozen Section Evaluation of the Appendix Abstract Appendiceal tumors are rarely diagnosed preoperatively, and their classification is both challenging and controversial owing to their tendency
Barrett s Esophagus: Old Dog, New Tricks
 Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
Barrett s Esophagus: Old Dog, New Tricks Stuart Jon Spechler, M.D. Chief, Division of Gastroenterology, VA North Texas Healthcare System; Co-Director, Esophageal Diseases Center, Professor of Medicine,
colorectal cancer Colorectal cancer hereditary sporadic Familial 1/12/2018
 colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
colorectal cancer Adenocarcinoma of the colon and rectum is the third most common site of new cancer cases and deaths in men (following prostate and lung or bronchus cancer) and women (following breast
Case presentation. Eran Zittan. MD Mount Sinai Hospital, Toronto, Canada. Emek Medical Center, Afula, Israel. March, 2016
 Case presentation Eran Zittan. MD Mount Sinai Hospital, Toronto, Canada. Emek Medical Center, Afula, Israel. March, 2016 60 y/o man with long standing UC+PSC. Last 10 years on clinical and endoscopic remission.
Case presentation Eran Zittan. MD Mount Sinai Hospital, Toronto, Canada. Emek Medical Center, Afula, Israel. March, 2016 60 y/o man with long standing UC+PSC. Last 10 years on clinical and endoscopic remission.
polyps of the colon and rectum
 J. clin. Path., 1973, 26, 25-31 Pseudo-carcinomatous invasion in adenomatous polyps of the colon and rectum T. MUTO, H. J. R. BUSSEY, AND B. C. MORSON From St Mark's Hospital, London SYNOPSIS The histology
J. clin. Path., 1973, 26, 25-31 Pseudo-carcinomatous invasion in adenomatous polyps of the colon and rectum T. MUTO, H. J. R. BUSSEY, AND B. C. MORSON From St Mark's Hospital, London SYNOPSIS The histology
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST QUESTIONS. Ver. #
 SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
SAMs Guidelines DEVELOPING SELF-ASSESSMENT MODULES TEST Ver. #5-02.12.17 GUIDELINES FOR DEVELOPING SELF-ASSESSMENT MODULES TEST The USCAP is accredited by the American Board of Pathology (ABP) to offer
Although current American Cancer Society guidelines
 ORIGINAL ARTICLE Diffuse Adenosis of the Peripheral Zone in Prostate Needle Biopsy and Prostatectomy Specimens Tamara L. Lotan, MD* and Jonathan I. Epstein, MD*w z Abstract: We have observed a group of
ORIGINAL ARTICLE Diffuse Adenosis of the Peripheral Zone in Prostate Needle Biopsy and Prostatectomy Specimens Tamara L. Lotan, MD* and Jonathan I. Epstein, MD*w z Abstract: We have observed a group of
Billing Guideline. Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16
 Billing Guideline Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16 Florida Hospital Care Advantage plans include full coverage of in-network
Billing Guideline Subject: Colorectal Cancer Screening Exams (Invasive Procedures) Effective Date: 1/1/14 Last revision effective 4/16 Florida Hospital Care Advantage plans include full coverage of in-network
Case Report Intramucosal Signet Ring Cell Gastric Cancer Diagnosed 15 Months after the Initial Endoscopic Examination
 Hindawi Publishing Corporation Case Reports in Medicine Volume 2015, Article ID 479625, 5 pages http://dx.doi.org/10.1155/2015/479625 Case Report Intramucosal Signet Ring Cell Gastric Cancer Diagnosed
Hindawi Publishing Corporation Case Reports in Medicine Volume 2015, Article ID 479625, 5 pages http://dx.doi.org/10.1155/2015/479625 Case Report Intramucosal Signet Ring Cell Gastric Cancer Diagnosed
A WHO update on Serrated Polyps
 A WHO update on Serrated Polyps Arzu Ensari, MD, PhD Department of Pathology Ankara University Medical School Am J Gastroenterol. 2010 Nov 2. [Epub ahead of The Clinical Significance of Serrated Polyps.
A WHO update on Serrated Polyps Arzu Ensari, MD, PhD Department of Pathology Ankara University Medical School Am J Gastroenterol. 2010 Nov 2. [Epub ahead of The Clinical Significance of Serrated Polyps.
LOINC. Clinical information. RCPA code. Record if different to report header Operating surgeon name and contact details. Absent.
 Complete as narrative or use the structured format below 55752-0 17.02.28593 Clinical information 22027-7 17.02.30001 Record if different to report header Operating surgeon name and contact details 52101004
Complete as narrative or use the structured format below 55752-0 17.02.28593 Clinical information 22027-7 17.02.30001 Record if different to report header Operating surgeon name and contact details 52101004
p53 expression in invasive pancreatic adenocarcinoma and precursor lesions
 Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Malaysian J Pathol 2011; 33(2) : 89 94 ORIGINAL ARTICLE p53 expression in invasive pancreatic adenocarcinoma and precursor lesions NORFADZILAH MY MBBCH,* Jayalakshmi PAILOOR MPath, FRCPath,* RETNESWARI
Serrated Lesions in the Bowel Cancer Screening Programme
 Serrated Lesions in the Bowel Cancer Screening Programme Mark Arends Cambridge & Edinburgh Serrated Lesions of Large Bowel 1. Hyperplastic polyp 2. Serrated adenoma 3. Mixed polyp 4. Sessile serrated lesion
Serrated Lesions in the Bowel Cancer Screening Programme Mark Arends Cambridge & Edinburgh Serrated Lesions of Large Bowel 1. Hyperplastic polyp 2. Serrated adenoma 3. Mixed polyp 4. Sessile serrated lesion
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Multifocal Adenocarcinomas Arising within a Gastric Inverted Hyperplastic Polyp
 The Korean Journal of Pathology 2012; 46: 387-391 CSE REPORT Multifocal denocarcinomas rising within a Gastric Inverted Hyperplastic Polyp Hyun-Soo Kim Eun-Jung Hwang 1 Jae-Young Jang 1 Juhie Lee 2 Youn
The Korean Journal of Pathology 2012; 46: 387-391 CSE REPORT Multifocal denocarcinomas rising within a Gastric Inverted Hyperplastic Polyp Hyun-Soo Kim Eun-Jung Hwang 1 Jae-Young Jang 1 Juhie Lee 2 Youn
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Burning Issues in the Esophagus
 Burning Issues in the Esophagus Elizabeth Montgomery, MD Johns Hopkins Medical Institutions Dr. Montgomery reports no relevant financial relationships with commercial interests. Squamous Epithelium Muscularis
Burning Issues in the Esophagus Elizabeth Montgomery, MD Johns Hopkins Medical Institutions Dr. Montgomery reports no relevant financial relationships with commercial interests. Squamous Epithelium Muscularis
Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital
 Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital jmisdraji@partners.org Adenoma Low-grade appendiceal mucinous neoplasm High-grade appendiceal mucinous neoplasm Adenocarcinoma Serrated
Joseph Misdraji, M.D. GI pathology Unit Massachusetts General Hospital jmisdraji@partners.org Adenoma Low-grade appendiceal mucinous neoplasm High-grade appendiceal mucinous neoplasm Adenocarcinoma Serrated
Update on Colonic Serrated (and Conventional) Adenomatous Polyps
 Update on Colonic Serrated (and Conventional) Adenomatous Polyps Maui, HI 2018 Robert D. Odze, MD, FRCPC Chief, Division of GI Pathology Professor of Pathology Brigham and Women s Hospital Harvard Medical
Update on Colonic Serrated (and Conventional) Adenomatous Polyps Maui, HI 2018 Robert D. Odze, MD, FRCPC Chief, Division of GI Pathology Professor of Pathology Brigham and Women s Hospital Harvard Medical
CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall
 Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Malaysian J Pathol 2015; 37(3) : 281 285 CASE REPORT Malignant transformation of breast ductal adenoma: a diagnostic pitfall Hiroko HAYASHI, Hiroshi OHTANI,* Junzo YAMAGUCHI,** and Isao SHIMOKAWA Department
Staging Challenges in Lower GI Cancers. Disclosure of Relevant Financial Relationships. AJCC 8 th edition and CAP protocol updates
 Staging Challenges in Lower GI Cancers Sanjay Kakar, MD University of California, San Francisco March 05, 2017 Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education
Staging Challenges in Lower GI Cancers Sanjay Kakar, MD University of California, San Francisco March 05, 2017 Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care
 Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
Quality ID #249 (NQF 1854): Barrett s Esophagus National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS ONLY MEASURE TYPE: Process DESCRIPTION: Percentage
