JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T. preclinical development for cancer indications 6 and one, the vascular endothelial
|
|
|
- Marshall Julian Gilbert
- 6 years ago
- Views:
Transcription
1 NUMBER FEBRUARY VOLUME 23 d 5 d JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T A Multitargeted, Metronomic, and Maximum-Tolerated Dose Chemo-Switch Regimen is Antiangiogenic, Producing Objective Responses and Survival Benefit in a Mouse Model of Cancer Kristian Pietras and Douglas Hanahan From the Department of Biochemistry and Biophysics, Diabetes and Comprehensive Cancer Centers, University of California San Francisco, San Francisco, CA. Submitted July 16, 04; accepted September 22, 04. Supported by grants from the National Cancer Institute and the William K. Bowes, Jr Foundation. K.P. is the recipient of a Swedish Cancer Foundation postdoctoral fellowship. Terms in blue are defined in the glossary, found at the end of this issue and online at Authors disclosures of potential conflicts of interest are found at the end of this article. Address reprint requests to Douglas Hanahan, MD, University of California San Francisco, 513 Parnassas Avenue, San Francisco, CA 94143; dh@biochem.ucsf.edu. 05 by American Society of Clinical Oncology X/05/ /$.00 DOI: 10.10/JCO A B S T R A C T Purpose A transgenic mouse model has revealed parameters of the angiogenic switch during multistep tumorigenesis of pancreatic islets, and demonstrated efficacy of antiangiogenic therapies. Pericytes have been revealed as functionally important for tumor neovasculature, using kinase inhibitors targeting their platelet-derived growth factor receptors (PDGFRs). Additionally, vascular endothelial growth factor receptor (VEGFR) inhibitors and metronomic chemotherapy show modest benefit against early- but not late-stage disease. Materials and Methods Seeking to improve efficacy against otherwise intractable end-stage pancreatic islet tumors, two receptor tyrosine kinase inhibitors, imatinib and SU11248, were used to disrupt PDGFRmediated pericyte support of tumor endothelial cells in concert with maximum-tolerated dose (MTD) or metronomic chemotherapy and/or VEGFR inhibition. Results Imatinib, despite equivocal efficacy as monotherapy, reduced pericyte coverage of tumor vessels and enhanced efficacy in combination with metronomic chemotherapy or VEGFR inhibition. A regimen involving all three was even better. MTD using cyclophosphamide caused transitory regression, but then rapid regrowth, in contrast to metronomic cyclophosphamide plus imatinib, which produced stable disease. The MTD regimen elicited apoptosis of tumor cells but not endothelial cells, whereas the other regimens increased endothelial cell apoptosis concordant with efficacy. A chemo-switch protocol, involving sequential MTD and then metronomic chemotherapy, overlaid with multitargeted inhibition of PDGFR and VEGFR, gave complete responses and unprecedented survival advantage in this model. Conclusion This study demonstrates a potentially tractable clinical strategy in a stringent preclinical model, wherein standard-of-care chemotherapy is followed by a novel maintenance regimen: PDFGR is targeted to disrupt pericyte support, while metronomic chemotherapy and/or VEGFR inhibitors target consequently sensitized endothelial cells, collectively destabilizing pre-existing tumor vasculature and inhibiting ongoing angiogenesis. J Clin Oncol 23: by American Society of Clinical Oncology INTRODUCTION The endothelial cell compartment is an attractive target for anticancer therapy as a result of the now evident importance of the tumor vasculature for sustaining tumor growth and metastasis. 1-5 Dozens of angiogenesis inhibitors are in clinical trials or preclinical development for cancer indications 6 and one, the vascular endothelial growth factor (VEGF) inhibitor bevacizumab (Avastin; Genentech, South San Francisco, CA), has been approved. 7 In addition to this pipeline of designer drugs, it has recently become apparent that tumor 939
2 Pietras and Hanahan endothelial cells are sensitive to the action of conventional cytotoxic drugs, if the dosing regimen is altered. The concept, known as antiangiogenic scheduling or metronomic chemotherapy, was demonstrated in preclinical studies using transplanted tumor models While most standard chemotherapies likely target the proliferating endothelial cells in tumors, the obligatory rest periods in traditional maximum-tolerated dose (MTD) regimens of chemotherapy are thought to allow the endothelial cells to recover by using their intact p53-based damage sensor to effect G1 arrest, allowing genome repair and thereby diminishing the antiangiogenic effects of the treatment. 8,11,12 Metronomic chemotherapy involves regular administration of cytotoxic drugs at doses that are low enough to avoid myleosuppression and other dose-limiting side effects that otherwise obligate rest periods, thus continuously exposing the more slowly proliferating tumor endothelial cells to damaging actions of the cytotoxic drug, thereby limiting their opportunity to repair and recover. The incorporation into metronomic chemotherapy regimens of antiangiogenic drugs, such as TNP-470 or inhibitors of VEGF receptors (VEGFRs) or matrix metalloproteases, has been shown to further enhance efficacy in preclinical models. 8,9,13 While the tumor endothelial cell is increasingly accepted as a valid target for cancer therapies, another vascular cell type, the pericyte, has recently been recognized as a potentially important, and complimentary, target. Pericytes are fibroblastic/smooth muscle-like cells found in close contact with endothelial cells in small blood vessels and capillaries, where they serve as regulators of blood vessel formation and function. 14 Pericyte homeostasis is regulated in significant part by signaling through the plateletderived growth factor ligand/receptor (PDGF/PDGFR) system Pericytes have begun to attract attention as drug targets due to their apparent involvement in a variety of diseases and disorders, including cancer, diabetic retinopathy, and atherosclerosis. 14 Moreover, pericytes are thought to provide endothelial cells with crucial survival signals, the complete nature of which remains to be elucidated, but evidently includes signaling by angiopoietin and N-cadherin. 22 In the current study, we investigate the effect of targeting pericytes (via inhibition of PDGFRs) on the efficacy of metronomic chemotherapy and endothelial cell survival in the RIP1-Tag2 transgenic mouse model of pancreatic neuroendocrine cancer. 23 The tumors that arise in this mouse model from targeted oncogene expression in the insulin-producing beta cells are ostensibly similar to the non multiple endocrine neoplasia class of human islet tumors, although careful cross-comparative studies on molecular signatures have not been performed. Rather, the model is viewed as a general prototype for the stepwise process of tumor development and progression via distinctive lesional stages thought to reflect rate-limiting secondary events. Notably, the angiogenic switch was first identified as one of those events, being activated in the multifocal premalignant phase of this pathway and subsequently sustained, critical for tumor formation, growth, and progression. 3,24 The experimental design (Fig 1) was motivated by preclinical trials of receptor tyrosine kinase inhibitors in this model that revealed synergistic efficacy when endothelial cells and pericytes were jointly targeted by drugs that inhibited VEGFR and PDGFR, respectively. 25 Inhibition of PDGFR was associated with pericyte detachment from tumor vessels, apparently rendering the endothelial cells more susceptible to the effects of VEGFR blockade. Studies in traditional xenotransplant tumormodelshavealsoshownbenefitsinjointlytargeting VEGFR and PDGFR, and documented pericyte disruption in tumors, 26,27 suggestive of a general mechanism. We reasoned that pericyte detachment induced by PDGFR inhibition would also sensitize the endothelial cells to chemotherapy, in particular metronomic chemotherapy, and evaluate that possibility herein. Furthermore, we assess the benefits of combining multitargeted tyrosine kinase inhibitors, concurrently directed against PDGFR and VEGFR, with metronomic chemotherapy. Finally, we design and validate a new chemo-switch protocol, combining an analog of a standard-of-care MTD regimen with metronomic chemotherapy and novel multitargeted kinase inhibitors, the results of which encourage consideration of clinical trials aimed to assess the potential of chemo-switch regimens for treating human cancers. MATERIALS AND METHODS Animal Care All animal studies described were approved by the local committee for animal care. From 12 weeks of age, all RIP1- Tag2 mice received 50% sugar food (Harlan Teklad, Madison, WI) and 5% sugar water to relieve hypoglycemia induced by the insulin-secreting tumors. Drugs and Treatments The drug doses were set at a concentration that alone, or in combination with other drugs, did not cause drug-related deaths or weight loss of more than 15%. Imatinib (UCSF Medical Center pharmacy, San Francisco, CA) was administered orally by gavage in a volume of 100 l of phosphate-buffered saline (PBS) at a total dose of 150 mg/kg 1 day 1, divided into one administration of 50 mg/kg 1 in the morning, and one of 100 mg/kg 1 in the afternoon. SU10944 (SUGEN, South San Francisco, CA) was administered orally by gavage in a volume of 100 l of a carboxymethylcellulose suspension at a dose of 100 mg/kg 1 day 1. SU11248 (SUGEN, South San Francisco, CA) was administered orally by gavage in a volume of 100 l at a dose of mg/kg 1 day 1. After 6 weeks of treatment in the survival trial, mice treated with SU11248 displayed signs of fatigue, and treatment was changed to mg/kg 1 day 1 delivered on 5 consecutive days, followed by 2 days of rest for the remainder of the trial. For the purpose of metronomic scheduling of cyclophosphamide (CTX; Sigma, St Louis, MO), each mouse was estimated to drink 9 JOURNAL OF CLINICAL ONCOLOGY
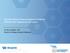
3 Multitargeted Chemo-Switch Regimen Pericytes provide survival functions to endothelial cells Targeting pericytes, eg, via PDGF receptors (Imatinib, SU11248) Impaired support or protection by pericytes Endothelial cells are partially resistant to VEGFR inhibition Endothelial cells are less sensitive to chemotherapy Fig 1. Pericytes (green) line tumor blood vessels and normal capillaries, providing endothelial cells (red) with survival cues (arrows). Impairment of pericyte function via inhibition of platelet-derived growth factor (PDGF) receptor disrupts cell-to-cell contacts between pericytes and endothelial cells in tumor vasculature, rendering endothelial cells more susceptible to pharmacologically induced apoptotic cell death (dashed cell membrane, condensed chromatin). VEGFR, vascular endothelial growth factor receptor. Endothelial cells are very sensitive to VEGFR inhibition Endothelial cells are very sensitive to chemotherapy 1.5 ml 10 g 1 day 1. A stock solution of CTX was prepared fresh every week at a concentration of mg/ml and stored in 4 C. Twice weekly, 0.66 ml of the stock solution was diluted in 0 ml of 5% sugar water, approximating an estimated dose of CTX of 10 mg/kg 1 day 1 for each mouse. The MTD regimen of CTX for RIP1-Tag2 mice was delivered as a previously reported 21-day cycle 9 of 105 mg/kg 1 administered intraperitoneally every other day for a total of three doses, followed by 2 weeks of rest. The total dose was chosen because of severe toxicity in terms ofweight loss and morbidity in RIP1-Tag2 mice associated with higher doses. Experimental Trials Drug treatments were started when the mice reached an age of 12 weeks, except for mice treated with imatinib, which were pretreated for 3 days. Mice were continuously monitored for signs of hypoglycemic shock or drug side effects and were sacrificed if found cachexic or if body weight loss exceeded 15%. For regression trials, following 4 weeks of treatment, mice were anesthetized and heart perfused using 10 ml PBS, followed by 10 ml 10% zinc-buffered formalin (Medical Chemical Corp, Torrance, CA). Subsequently, the pancreas and spleen of the mice were dissected and macroscopic tumors ( 1 1 mm) were excised and measured and the number of tumors in each mouse was noted. Tumor volume was calculated using the formula V Z a*b 2 * /6, where a and b equal the longer and the shorter diameter of the tumor, respectively. The tumor volume of all tumors from each mouse was combined to arrive at the total tumor burden. Tumors were then fixed in 10% zinc-formalin for 1 hour at 4 C and subsequently placed in PBS containing 30% sucrose until the tissue sank to the bottom. Then the tissue was embedded in optimal cutting temperature medium and frozen for cryosectioning and histologic analysis. Immunostaining Cryosections (10 m) from tumors were allowed to dry in air for 10 minutes before they were equilibrated in PBS three times for 5 minutes. Following blocking of nonspecific binding using a serum-free protein block (DAKO, Carpinteria, CA) for 45 minutes at room temperature (rt), sections were incubated in PBS 1% bovine serum albumin (wash buffer) containing polyclonal antibodies directed against CD31 (1:100; Pharmingen, San Diego, CA) and NG2 (1:0; Chemicon, Temecula, CA) over night at 4 C. Subsequently, sections were washed in wash buffer three times for 10 minutes and further incubated for minutes with secondary antibodies coupled to fluorescent labels (1:100; Jackson Immunolaboratories, West Grove PA) at rt. After washing in wash buffer three times for 10 minutes, sections were mounted in solution containing DAPI (Vector, Burlingame, CA). TUNEL Staining Cryosections (10 m) from tumors were allowed to dry in air for 10 minutes before they were equilibrated in PBS three times for 5 minutes. Subsequently, sections were preincubated with TdT buffer (Invitrogen, Carlsbad, CA) for 10 minutes at rt and then incubated in TdT buffer containing 0 U/mL TdT enzyme and 4 mol/l digoxigenin-conjugated dutp (Enzo Life Sciences, Farmingdale, NY) for 30 minutes at 37 C. Following washing three times for 5 minutes in PBS, sections were incubated with fluorescein-conjugated anti-digoxigenin antibodies over night at 4 C. After washing three times for 5 minutes in PBS, sections were mounted in solution containing DAPI. Quantitation of Pericyte Coverage Pericyte coverage was quantified as the percent of the CD31 circumference of vessel cross-sections or CD31 length 941
4 Pietras and Hanahan of longitudinal vessel sections that is covered by NG2 structures. Quantitations were performed using the Openlab software (Improvision, Lexington, MA) on to 22 vessel profiles from each mouse; for each group, four different mice treated between 12 and 16 weeks were used. Quantitation of Vessel Density Vessel density was quantitated as the total number of CD31 structures observed in four high power (0 ) fields of vision per tumor; for each group, tumors from four different mice treated between 12 and 16 weeks were used. Quantitation of Endothelial Cell Apoptosis Endothelial cell apoptosis was quantitated as the percentage of CD31 structures containing TUNEL endothelial cells in four high power (0 ) fields of vision per tumor; for each group, tumors from four different mice treated between 12 and 16 weeks were used. Statistical Analysis All measurements are depicted as average SE of the mean. Statistical analysis of data from regression trials and quantitations of immunostaining was performed using a two-tailed, unpaired Mann-Whitney U-test. Statistical analysis of data from survival trials was performed using a log-rank test. A P value below.05 was considered statistically significant. RESULTS Imatinib Enhances the Efficacy of Metronomic Cyclophosphamide in RIP1-Tag2 Mice The RIP1-Tag2 transgenic mouse model of pancreatic islet carcinogenesis 23 has been used to elucidate mechanisms employed by tumors to activate the angiogenic switch 24,28 and to assess the impact of antiangiogenic drugs on the distinctive stages of multistep tumor development. 13,25,29,30 The relative synchronicity with which neuroendocrine tumors (insulinomas) develop from 0 oncogene-expressing islet progenitor lesions in the pancreas through successive temporal stages hyperplastic/ dysplastic islets, angiogenic islets, and progressive grades of islet carcinoma enabled the design of three distinctive preclinical trials, targeting the angiogenic switch in progenitor lesions, or asymptomatic small tumors, or advanced near-end-stage cancers. 29 In this study we focused on the latter, called a regression trial, as it most closely mimics the typical situation in the clinic, where a patient presents with advanced disease and significant tumor burden. The activity profiles of the kinase inhibitors used in this study are summarized in Table 1. A previous study documented that PDGFRs are predominantly expressed by, and functionally important for, maintenance of pericytes in the vasculature of RIP1-Tag2 tumors, 25 presenting imatinib (Gleevec; Novartis, Basel, Switzerland; Table 1) as a relatively selective, pericyte-targeting drug. The oncogene-expressing tumor cells in this model do not express any of the four PDGF ligands or either of the two PDGFRs in vivo 25 or in culture (unpublished results); thus, imatinib is not expected to interfere with autocrine tumor growth. To assess whether imatinib could enhance the efficacy of metronomic chemotherapy by dissociating pericytes from endothelial cells, we performed a regression trial. Treatment of RIP1-Tag2 mice was started at 12 weeks of age, at which point the mice had several well-established solid tumors. Metronomic chemotherapy involving CTX was administered continuously through the drinking water, alone or in combination with twice-daily administration of imatinib, until 16 weeks of age. mice were sacrificed at 12 weeks of age to determine the initial tumor burden of the mice in these highly synchronous, age-matched cohorts, and at 14.5 weeks, when approximately half of the untreated mice had died from the effects of their tumors. Consistent with previous results, 25 treatment with imatinib alone did not demonstrably affect the growth of tumors, and the mice had to be sacrificed at the same time (14.5 weeks) as the untreated control group (Fig 2A). In accordance with previous studies in the RIP1-Tag2 model, 13,36 in this study the mice treated with metronomic CTX had a reduced average tumor burden of 59.5 L at 16 weeks compared with the 14.5-week control group burden of 91.8 L (Fig 2A). The combination of imatinib and metronomic CTX resulted in apparent stable disease, with an average tumor burden of 30.4 L at the prescribed end point of the trial (Fig 2A), comparable to that of mice analyzed at the 12-week starting point of the trial (29.6 L), and significantly lower than metronomic CTX alone. Notably, none of these treatments produced obvious toxicity, Table 1. Activity Profiles for Receptor Tyrosine Kinase Inhibitors Used in This Study Receptor Kinase Drug PDGFR VEGFR-1 VEGFR-2 c-kit FGFR-1 EGFR Reference Imatinib ,000 11, ,000 30,000 31, 32 SU ,000 6* 102 1,0 50,000 50, SU ,900 34, 35 NOTE. Data shown are IC 50 (nm) for inhibition of the noted receptor tyrosine kinases in cell-based assays of the drugs used in the present study. Abbreviations: PDGFR, platelet-derived growth factor receptor; VEGFR, vascular endothelial growth factor receptor; FGFR; fibroblast growth factor receptor; EGFR, epidermal growth factor receptor. *Determined in a cell-free biochemical assay. 942 JOURNAL OF CLINICAL ONCOLOGY
5 Multitargeted Chemo-Switch Regimen A B Survival (%) Tumor Volume (µl) Age (weeks) Imatinib Treatment Age (weeks) Imatinib Imatinib + suggesting the existence of a therapeutic window in that deleterious effects (eg, pericyte dissociation) were evident in tumor but not normal tissue vasculature, including that of the exocrine pancreas in which the neuroendocrine tumors and their progenitor lesions are embedded, consistent with a previous report. 25 Since metronomic chemotherapy is still largely an investigational drug protocol, we also assessed an analog of a standard-of-care MTD chemotherapeutic regimen for comparison, also using CTX. Although CTX is not traditionally used against human neuroendocrine tumors, we chose to use it based on preliminary studies indicating that MTD CTX had activity against these mouse tumors, reasoning that use of the same drug in metronomic and MTD regimens would facilitate comparison. The MTD regimen consisted of a 1-week treatment series (one 16 MTD CTX Fig 2. (A) Tumor volume of untreated RIP1-Tag2 mice at 12 weeks (n Z 11) and 14.5 weeks of age (n Z 17) and mice treated with: imatinib (n Z 8); metronomic cyclophosphamide (met CTX; n Z 7); imatinib met CTX (n Z 9); or maximum-tolerated dose CTX (MTD CTX; n Z 10). (B) Survival of RIP1-Tag2 mice treated as indicated (all groups, n Z 6). dose given every other day for a total of three doses), followed by 2 weeks of rest, another week of treatment, and then immediate termination of the trial at the defined 4- week end point for a regression trial. The mice treated with MTD CTX had a similar tumor burden at 16 weeks to that at the start of the trial (Fig 2A). This regimen ostensibly produced a condition of stable disease, comparable to metronomic CTX plus imatinib and better than metronomic CTX alone, a condition that was, however, transitory, as shown in the following sections. Moreover, in contrast to mice treated with metronomic CTX, either alone or in combination with imatinib and/or a VEGFR inhibitor (see following sections), none of which showed obvious signs of toxicity such as weight loss, mice treated with MTD CTX lost approximately 15% of their body weight during the course of the trial (data not shown). We next performed a regression/survival trial, in which treatment starts at 12 weeks of age and persists until death is imminent or a milestone at 24 weeks of age is reached. This trial places stringent demands on treatment regimens due to the multifocal nature of the model and the physiological stress of hyperinsulinemia and pancreatic disruption. Consequently, mice left untreated will die shortly after the trial commences, with a median survival of only 2.5 weeks (Fig 2B). Treatment with metronomic CTX extended median survival to 4.5 weeks (Fig 2B). The median survival of mice treated with the combination of imatinib and metronomic CTX was 6.1 weeks, significantly prolonged compared to metronomic CTX alone (Fig 2B). We also tested the combination of imatinib and MTD CTX to assess possible combinatorial benefit, both for completeness and in light of previous studies showing that imatinib reduces tumor interstitial fluid pressure and thereby enhances drug delivery into solid tumors. 37,38 Tumor burden was reduced compared with the single agents at 16 weeks, but there was no survival benefit (data not shown), likely due to the rapid resistance that develops to MTD CTX (see following sections). Treatment With Imatinib and Metronomic CTX Reduces Pericyte Coverage of Tumor Blood Vessels Our therapeutic trial design was based on the proposition that PDGFR blockage would cause pericyte dissociation from tumor vessels. Therefore, we assessed the extent of pericyte coverage of tumor blood vessels following treatment with metronomic CTX alone, or in combination with imatinib. As witnessed by immunostaining for the pericyte marker NG2, z% of the blood vessel area in RIP1-Tag2 tumors was covered by pericytes (Figs 3A and B). Treatment with metronomic CTX did not alter the extent of pericyte coverage of tumor blood vessels (Figs 3A and B). In contrast, treatment with the combination of imatinib and metronomic CTX significantly 943
6 Pietras and Hanahan A Imatinib + RIP-Tag2 Tumor Exocrine Pancreas B Pericyte Coverage (% circumference of CD31+ structures covered by NG2+ cells) Fig 3. (A) Visualization of pericytes using immunostaining of the marker NG2 (green), blood vessels using the endothelial marker CD31 (red), and cell nuclei using DAPI (blue) in treated versus controltissues. Tumors, 1,000 magnification; exocrine pancreas, 0 magnification. (B) Quantitation of pericyte coverage of tumor vasculature from mice treated between 12 to 16 weeks of age., metronomic cyclophosphamide. 10 Treatment reduced pericyte coverage on tumor blood vessels, to 31.3% (Figs 3A and B). A similar result was obtained using immunostaining for desmin, a different pericyte marker (data not shown). Neither regimen affected pericyte coverage on vessels in the exocrine pancreas (Fig 3A), supporting and extending previous results 25 that normal vasculature is comparably insensitive to pericyte disruption by inhibition of PDGFR, indicative of a substantive difference in normal versus tumor endothelial-pericyte homeostasis, revealing the existence of a therapeutic window. Multitargeted Inhibition of Angiogenesis in Combination With Metronomic CTX Produces Regression of Established Tumors We have previously reported on the benefits of jointly targeting VEGFR and PDGFR in this tumor type. 25 Further, we, and others, have previously shown that a VEGFR-inhibitor produced combinatorial efficacy with metronomic chemotherapy. 9,13 Now we have demonstrated that a PDGFR inhibitor enhances the therapeutic benefit of metronomic chemotherapy, and that it disrupts 944 JOURNAL OF CLINICAL ONCOLOGY
7 Multitargeted Chemo-Switch Regimen pericyte association with the endothelial cells of the tumor vasculature. Therefore, we sought to compare the three pair-wise multitargeting strategies side by side, and in addition, evaluate the combination of the three. To do so, we made use of the orally bioavailable, relatively selective VEGFR tyrosine kinase inhibitor SU10944 (Table 1). 33 Treatment of RIP1-Tag2 mice from 12 to 16 weeks of age with SU10944 alone for 4 weeks resulted in a modest retardation of tumor growth (Fig 4A). Notably, RIP1-Tag2 tumor cells do not express VEGFR-1 or -2, as shown in previous studies, 3,28 making antiangiogenic effects the most likely basis for the observed response. The combination of SU10944 with either imatinib or metronomic CTX proved to be more efficacious than any of the monotherapies (Figs 2A and 4A), in that the mice had tumor burdens at the 16-week defined end point comparable with the starting point of the trial (apparent stable disease; Fig A Tumor Volume (µl) Age (weeks) 12 B Survival (%) SU SU10944 Treatment Age (weeks) 16 P <.0001 P <.001 SU10944 SU SU Imatinib + SU10944 Imatinib + SU Fig 4. (A) Tumor volume of untreated RIP1-Tag2 mice at 12 weeks (n Z 11) and 14.5 weeks of age (n Z 17), and mice treated with: SU10944 (n Z 9); imatinib SU10944 (n Z 7); or imatinib SU10944 metronomic cyclophosphamide (met CTX; n Z 10). (B) Survival of RIP1-Tag2 mice treated as indicated (all groups, n Z 6, except triple combination, n Z 5). 4A); thus both combinations were beneficial, consistent with previous reports. 9,13,25 Since all three pair-wise combinations had additive benefit, we combined the three agents. The result was substantial reduction in tumor burden (Fig 4A). The mice treated with SU10944, imatinib, and metronomic CTX exhibited an average tumor burden of 5.6 L, compared with 29.6 L at the start of the trial (Fig 4A). Consistent with the tumor burden data, the median survival of mice treated with the triple combination was 10.6 weeks, compared with 4.5 weeks and 5 weeks for SU10944 plus metronomic CTX and SU10944 plus imatinib, respectively (Fig 4B). We thus conclude that multitargeted inhibition of angiogenesis in combination with metronomic chemotherapy produces objective responses in established tumors and significantly prolongs survival of RIP1-Tag2 mice. Multitargeted Inhibition of Angiogenesis Combined With Metronomic Chemotherapy Reduces Blood Vessel Density in Tumors Immunostaining with antibodies against CD31, an endothelial cell antigen, revealed that treatment of RIP1- Tag2 mice with metronomic CTX reduced tumor blood vessel density (Figs 5A and B). In parallel, the endothelial cell apoptotic index was increased (Fig 5C). The combination of imatinib and metronomic CTX further reduced the blood vessel density by 52.7% and increased the apoptotic index of endothelial cells by 2.2-fold (Figs 5A-C). In marked contrast, treatment with MTD CTX did not affect vessel density or endothelial cell apoptosis of RIP1-Tag2 tumors (Figs 5A-C), illustrating that, even though the efficacy of MTD CTX versus imatinib plus metronomic CTX was similar in a 4-week regression trial, the two treatment regimens were not targeting the same tumor compartment. The fact that an increased rate of tumor cell apoptosis was observed following the first week of treatment with MTD CTX compared with control-treated tumors (data not shown) further demonstrates that MTD chemotherapy is largely targeting the oncogene-expressing p53 deficient cancer cells, and not endothelial cells or pericytes. The triple combination of imatinib, SU10944, and metronomic CTX dramatically reduced blood vessel density ( 89.6%) and elicited a 12.5-fold increase in endothelial cell apoptosis compared with control tumors (Figs 5A-C). Disease Stabilization by MTD CTX Is Transitory Conventional MTD regimens with cytotoxic drugs are known to give rise to various forms of resistance to treatment. 39 To investigate whether the MTD CTX regimen induced resistance in RIP1-Tag2 tumors, we monitored tumor burden over time in a regression trial, comparing the standard regimen with the similarly efficacious combination of imatinib plus metronomic CTX. As expected, after the first week of treatment with MTD CTX, tumors 945
8 Pietras and Hanahan A Imatinib Imatinib + SU10944 SU MTD CTX Imatinib + SU Fig 5. (A) Immunostaining of the endothelial cell marker CD31 (red) reveals tumor vasculature in treated and control mice; 0 magnification. (B) Quantitation of blood vessel density in tumors from mice treated as indicated. B Vessel Density (No. of CD31 + structures in 4 hpfs) Imatinib SU10944 Treatment SU SU MTD CTX 946 JOURNAL OF CLINICAL ONCOLOGY
9 Multitargeted Chemo-Switch Regimen C Endothelial Cell Apoptosis (No. of CD31 + TUNEL + structures in 4 hpfs) Fig 5. (continued) (C) Quantitation of endothelial cell apoptosis in tumors from mice treated as indicated. Met CTX, metronomic cyclophosphamide; MTD CTX, maximum-tolerated dose cyclophosphamide; hpfs, high power fields. Imatinib SU10944 Treatment SU SU MTD CTX showed significant regression from the start of the trial (Fig 6). During the 2 weeks of rest between 13 and 15 weeks, tumors rapidly regrew (Fig 6). Assessment after the second round of MTD chemotherapy revealed that tumor volume continued to increase during this course of treatment, indicative of development of resistance to the action of CTX (Fig 6). In contrast to the initial regression and subsequent regrowth of tumors from mice treated with MTD CTX, the tumor burden of mice treated with imatinib plus metronomic CTX was stable during the Tumor Volume (µl) Age (weeks) MTD Regimen 12 treat MTD CTX rest treat Imatinib + Fig 6. Tumor burden of untreated RIP1-Tag2 mice at 12 weeks of age (n Z 9) and mice treated from 12 weeks of age with maximum-tolerated dose cyclophosphamide (MTD CTX) or imatinib metronomic cyclophosphamide () and sacrificed at the indicated time points (all treated groups, n Z 5). course of the trial (Fig 6); there was no rapid regression, nor was there rebound and expansion. Chemo-Switch Regimen Regresses Established Tumors and Prolongs Survival Seeing that the MTD CTX regimen produced an initial dramatic regression of tumors followed by a rapid rebound, whereas the imatinib plus metronomic CTX regimen effected stable disease without regression, and since certain tumors that are resistant to MTD chemotherapy can still respond to a metronomic treatment regimen, 9 we reasoned that by switching mice to a regimen of metronomic CTX following an initial period of MTD chemotherapy (a chemo-switch regimen), we would be able to achieve long-term treatment benefits. Indeed, treatment with the chemo-switch regimen proved significantly more efficacious in terms of reducing tumor burden than MTD CTX alone (Fig 7A). Moreover, the chemoswitch regimen in combination with imatinib further enhanced efficacy (Fig 7A). The chemo-switch regimen also significantly improved the median survival of the mice, from 5.5 weeks for MTD CTX to 6.8 weeks and 8 weeks for the chemo-switch regimen, alone or in combination with imatinib, respectively (Fig 7B). Combining Multitargeted Angiogenesis Inhibition With the Chemo-Switch Regimen Produces Enduring Responses and Improves Survival To investigate whether the efficacy of the chemo-switch regimen could be further improved by concomitant inhibition of PDGFRs and VEGFRs, we treated mice with the multitargeted tyrosine kinase inhibitor SU , SU11248 is in late-stage clinical trials for various indications, 947
10 Pietras and Hanahan A Tumor Volume (µl) P =.76 Age (weeks) B MTD CTX MTD CTX Chemo-switch Treatment Chemo-switch SU Chemo-switch SU Chemo-switch Fig 7. (A) Tumor burden of untreated RIP1-Tag2 mice at 12 weeks (n Z 5) and mice treated from 12 weeks with maximum-tolerated dose cyclophosphamide (MTD CTX; 13 weeks, n Z 8; 16 weeks, n Z 5), chemo-switch (n Z 5), imatinib chemo-switch (n Z 7), or SU11248 chemo-switch (16 weeks, n Z 6; 24 weeks, n Z 4) and sacrificed at the indicated time points. (B) Survival of RIP1-Tag2 mice treated as indicated (all groups, n Z 6). Survival (%) Age (weeks) MTD CTX Chemo-switch Imatinib + Chemo-switch SU Chemo-switch including highly angiogenic renal cancers; this agent is a potent inhibitor of several receptor tyrosine kinases including VEGFR and PDGFR (Table 1). Due to its continuing development as a clinical candidate, the translation into clinical trials of positive preclinical results obtained with SU11248 would be tractable. Another logical multitargeting strategy with clinical translatability would have been imatinib plus bevacizumab, except for the conundrum that the latter does not target mouse VEGF, making the combination nonapplicableto this de novo mousemodelof cancer.in work to be presented elsewhere, SU11248 was evaluated as a monotherapy in both regression and regression/survival trials. SU11248 produced stable disease in a 4-week regression trial, and both reduced tumor burden and conveyed a survival advantage in a regression/survival trial (data not shown; G. Bergers, personal communication, August 04). The combination of SU11248 with the chemo-switch regimen improved this efficacy in both trials: The combinatorial regimen caused substantive reductions in tumor mass in the 4-week regression trial; the average tumor burden was 1 L, and two of six mice were completely free of macroscopic tumors (Fig 7A). In the regression/survival trial, four of six mice treated with SU11248 plus the chemoswitch regimen were still alive at the predefined endpoint at 24 weeks of age (Fig 7B). Furthermore, two of the surviving mice had complete responses to treatment and were tumor-free at the 24-week end point, whereas the other two had small lesions(fig 7A). Further trials on larger cohorts will be required to see if there is modest regrowth from 16 to 24 weeks as suggested by the data, which is currently not statistically significant in the comparison of tumor burden at the two end points. The treatment appeared well tolerated; no weight loss was observed and the well-being of the mice was normal. However, fatigue, a common side effect from treatment with SU11248 in patients, 41 was observed in all mice after 6 weeks of treatment, but was effectively 948 JOURNAL OF CLINICAL ONCOLOGY
11 Multitargeted Chemo-Switch Regimen managed by altering the SU11248 dosing to a 5-day-on/ 2-day-off regimen, while continuing metronomic chemotherapy. We thus conclude that treatment with a multitargeted inhibitor of angiogenesis together with a chemo-switch regimen impressively prolongs survival in a remarkably challenging mouse model of cancer, recognizing its prevalent oncogene expression throughout the endocrine pancreas and consequent multifocal progression of disease. DISCUSSION We report that inhibition of PDGFR signaling, by administration of imatinib or a multitargeted kinase inhibitor, enhances the efficacy of metronomic chemotherapy in a transgenic mouse model of neuroendocrine cancer. Treatment with imatinib reduced the pericyte coverage of tumor blood vessels, apparently rendering endothelial cells more sensitive to the damaging action of cytotoxic drugs. Furthermore, treatment with the combination of imatinib, metronomic chemotherapy, and SU10944 (a selective VEGFR kinase inhibitor) elicited regression of established tumors and prolonged median survival of the mice. Lastly, by combining an initial MTD chemotherapeutic regimen with maintenance therapy consisting of metronomic chemotherapy plus the multitargeted kinase inhibitor SU11248, remarkable efficacy was achieved in terms of objective response to treatment and survival. A summary of the efficacy and survival benefit obtained with the various treatment regimens evaluated in this study is presented in Table 2. Pericytes promote stabilization of blood vessels via cell-cell contact and/or secreted factors, 14,,42,43 and PDGF signaling is evidently involved in their regulation. Thus, mice defective in PDGF-B/PDGFR- display abnormal development and maturation of the vasculature due to impaired recruitment of pericytes and smooth muscle cells. 44,45 Administration to newborn mice of neutralizing antibodies for the PDGF- receptor results in severe vascular malformation in the retina due to a lack of pericyte recruitment. 46 Now, in this and several recent reports, it has been shown that pericyte function in tumor blood vessels is impaired following treatment with PDGFR inhibitors Notably, normal tissue vasculature was not evidently disrupted by PDGFR inhibition, and there was no obvious toxicity, suggesting that other signals normally help maintain endothelial-pericyte interactions in quiescent blood vessels, thus affording a therapeutic window. Looking forward, it will be important to further investigate the prospect that inhibition of PDGFR to effect pericyte disruption in tumors could serve as a general strategy for enhancing the efficacy of agents targeting tumor endothelial cells, 15 and to assess potential toxicities not evident in this study, such as the edema associated with inhibition of PDGFR seen in certain tumor types Furthermore, it will be pertinent to utilize agents (monoclonal antibodies, ligand aptamers, etc) targeting mouse VEGFR and PDGFR with higher selectivity to further substantiate the mechanistic hypothesis; meanwhile, the weight of the evidence from this and previous studies 3,5,13,25-28 supports the conceptual basis of the design principle that targeting both pericytes and endothelial cells in the tumor vasculature produces significant therapeutic benefits. This study adds further support for the potential therapeutic value of metronomic chemotherapy, 11 and moreover suggests a strategy for enhancing its antiangiogenic efficacy, involving concurrent inoculation of a drug that sensitizes tumor endothelial cells by disrupting pericyte support functions (Fig 1). In considering how one might translate this new concept into clinical practice, we devised (and demonstrated the utility of) a multitargeted chemo-switch protocol (Fig 8) that should be adaptable for testing in clinical trials, Treatment Table 2. Summary of Data From Efficacy and Survival Trials Using Different Treatment Regimens* Efficacy (% regression at 16 weeks v start of trial) Median Survival Age (weeks) Figure No. PD Imatinib PD Metronomic CTX PD Metronomic CTX imatinib SD MTD CTX SD , 7B MTD CTX imatinib PR (67%) 17.9 dns SU10944 PD ND 4 SU10944 imatinib SD Metronomic CTX SU10944 PR (30%) Metronomic CTX SU10944 imatinib PR (81%) Chemo-switch PR (42%) Chemo-switch imatinib PR (78%).0 7 Chemo-switch SU11248 PR/CR (97%) Abbreviations: PD, progressive disease; CTX, cyclophosphamide; SD, stable disease; MTD, maximum-tolerated dose; PR, partial response; dns, data not shown; ND, not determined; CR, complete response. *Efficacy is defined according to the Response Evaluation Criteria in Solid Tumors of the National Cancer Institute
12 Pietras and Hanahan Standard of care MTD chemotherapy rest Maintenance therapy (oral, low-dose, low toxicity) Metronomic chemotherapy Imatinib; SU11248; Imatinib + bevacizumab Multi-targeted inhibition of tumor angiogenesis via PDGFR +/- VEGFR Fig 8. Schematic of a clinically relevant chemo-switch therapeutic trial design, involving sequential standardof-care (maximum-tolerated dose [MTD]) chemotherapy followed by multitargeted, antiangiogenic maintenance therapy, involving metronomic chemotherapy combined with multitargeted inhibition of pericytes and endothelial cells in the angiogenic tumor vasculature, using drugs directed at their platelet-derived growth factor receptor (PDGFR) and vascular endothelial growth factor receptor (VEGFR), respectively. having the following parameters: (1) standard-of-care (MTD) chemotherapy (or in principle radiotherapy), followed by (2) multitargeted antiangiogenic maintenance therapy, involving: disruption of pericyte support of tumor endothelial cells(eg, with PDGFR inhibitors such as imatinib or multitargeted kinase inhibitors); metronomic chemotherapy targeting the sensitized endothelial cells, ideally orally bioavailable and low-dose/low toxicity; and direct inhibition of endothelial cell functions and survival (eg, with VEGFR inhibitors, or multitargeted receptor tyrosine kinase inhibitors, or VEGF ligand blockade, such as with bevacizumab). The notion is that standard of care must be used, and moreover can serve to de-bulk a tumor by directly targeting the cancer cells. Then, before the inevitable rebound and regrowth (resistance), a multitargeted, antiangiogenic maintenance regimen is initiated, exploiting the results of this and previous studies to render both metronomic chemotherapy and other drugs targeting endothelial cells more efficacious by disrupting crucial pericyte support with PDGFR inhibitors. We show that a multitargeted kinase inhibitor, SU11248, has particular promise for incorporation into this therapeutic strategy, and suggest that clinical trials in a chemo-switch regimen be considered. Similarly, the chemo-switch regimen could be tested in the clinic by using bevacizumab to target the endothelial compartment, imatinib to target pericytes, low-dose oral CTX as the metronomic chemotherapy, and standard of care for the particular cancer indication (Fig 8). It should be emphasized that the particular disease indications where this strategy might prove most successful remain to be determined in the course of clinical trials that incorporate these design principles in the context of the particular characteristics and accepted treatment modalities for a given tumor type. We do not necessarily predict that analogous pancreatic non-men neuroendocrine tumors will be the most amenable, although it would be interesting to test the possibility. Rather, viewing the RIP-Tag2 model as a general prototype for de novo tumor progression, we imagine other tumor types, particularly ones that are highly vascularized, VEGF-expressing, and pericyte rich, might respond to a chemo-switch trial design. There is precedent to the chemo-switch regimen explored in the present study 11 ; for example, children with acute lymphoblastic leukemia are successfully treated with a long-term maintenance chemotherapy regimen following a high-dose standard regimen. 50 As for the choice of the metronomic chemotherapy, in our view the best option would be oral and low-dose/low toxicity (eg, 50 mg/d CTX pills). 11,51 Since the metronomic chemotherapy is targeting the endothelial cells, in contrast to the MTD standard of care, which primarily affects the overt tumor cells, it is possible that the same agent can be used in both phases of the chemo-switch regimen, as we have demonstrated herein in a preclinical model, even if resistance has developed to the MTD. Indeed, there are examples of patients responding to a more frequent, but low-dose, administration of chemotherapeutic drugs after having progressed on a conventional schedule of the same drug Nevertheless, there may be good reason to use different drugs in the MTD and metronomic phases of the chemo-switch protocol, and we are exploring such possibilities in the mouse model. The introduction of targeted cancer therapeutics into the clinic has been greatly anticipated. However, the initial reports from clinical trials using various targeted drugs as monotherapies, or in combination with MTD chemotherapy, have been sobering. It is increasingly appreciated that sustainable tumor regression and long-term survival will likely come from rationally designed combinations of targeted therapeutics and/or conventional chemotherapeutic agents that collectively target different cell types that contribute to tumor progression, including the tumor cells themselves, endothelial cells, pericytes, cancer-associated fibroblasts, and infiltrating tumor-enhancing, proangio- 950 JOURNAL OF CLINICAL ONCOLOGY
13 Multitargeted Chemo-Switch Regimen genic leukocytes. 55 To that end, it will be increasingly important to test combinations of clinically approved drugs, or drugs in late-stage clinical trials, in the preclinical setting, using organ-specific mouse models of human cancer development and progression to guide the design of future studies in patients. The striking results of this study suggest new avenues involving the use of imatinib and other PDGFR inhibitors to target pericytes and thereby sensitize tumor endothelial cells to cytotoxic killing. A chemoswitch protocol that incorporates this knowledge into a clinical trial design integrating standard-of-care MTD chemotherapy with a novel regimen of multitargeted, metronomic inhibition of tumor angiogenesis has prospect for producing enduring responses Acknowledgment We gratefully acknowledge Katie Gililland and Ehud Drori for excellent technical assistance, Alex McMillan for help with statistical analyses, and Bill Bowes for support and encouragement. We thank Gabriele Bergers for ongoing advice, discussions, and communication of preliminary results, along with Olivier Nolan-Stevaux for insightful comments and suggestions on the manuscript. Finally, we thank Douglas Laird, Jerry McMahon, and Sugen Corp (now Pfizer) for providing SU10944 and SU Authors Disclosures of Potential Conflicts of Interest The following authors or their immediate family members have indicated a financial interest. No conflict exists for drugs or devices used in a study if they are not being evaluated as part of the investigation. Honoraria: Douglas Hanahan, Novartis. For a detailed description of this category, or for more information about ASCO s conflict of interest policy, please refer to the Author Disclosure Declaration form and the Disclosures of Potential Conflicts of Interest section of Information for Contributors found in the front of every issue. REFERENCES 1. Folkman J: Anti-angiogenesis: New concept for therapy of solid tumors. Ann Surg 175:9-416, Hanahan D, Folkman J: Patterns and emerging mechanisms of the angiogenic switch during tumorigenesis. Cell 86: , Inoue M, Hager JH, Ferrara N, et al: VEGF- A has a critical, nonredundant role in angiogenic switching and pancreatic beta cell carcinogenesis. Cancer Cell 1:193-2, Bergers G, Benjamin LE: Tumorigenesis and the angiogenic switch. Nat Rev Cancer 3:1-410, Cao Y: Antiangiogenic cancer therapy. Semin Cancer Biol 14: , US National Cancer Institute: Angiogenesis Inhibitors in Clinical Trials, 3/03 update. anti-angio-table 7. Ferrara N, Hillan KJ, Gerber HP, et al: Discovery and development of bevacizumab, an anti-vegf antibody for treating cancer. Nat Rev Drug Discov 3:391-0, Browder T, Butterfield CE, Kraling BM, et al: Antiangiogenic scheduling of chemotherapy improves efficacy against experimental drug-resistant cancer. Cancer Res : , Klement G, Baruchel S, Rak J, et al: Continuous low-dose therapy with vinblastine and VEGF receptor-2 antibody induces sustained tumor regression without overt toxicity. J Clin Invest 105:R15-R24, Hanahan D, Bergers G, Bergsland E: Less is more, regularly: Metronomic dosing of cytotoxic drugs can target tumor angiogenesis in mice. J Clin Invest 105: , Kerbel RS, Kamen BA: The anti-angiogenic basis of metronomic chemotherapy. Nat Rev Cancer 4: , Gasparini G: Metronomic scheduling: The future of chemotherapy? Lancet Oncol 2:733-7, Bergers G, Hanahan D: Combining antiangiogenic agents with metronomic chemotherapy enhances efficacy against late-stage pancreatic islet carcinomas in mice. Cold Spring Harb Symp Quant Biol 67: , Gerhardt H, Betsholtz C: Endothelial-pericyte interactions in angiogenesis. Cell Tissue Res 314:15-23, Pietras K, Sjoblom T, Rubin K, et al: PDGF receptors as cancer drug targets. Cancer Cell 3: , Lindahl P, Bostrom H, Karlsson L, et al: Role of platelet-derived growth factors in angiogenesis and alveogenesis. Curr Top Pathol 93:27-33, Abramsson A, Lindblom P, Betsholtz C: Endothelial and nonendothelial sources of PDGF- B regulate pericyte recruitment and influence vascular pattern formation in tumors. J Clin Invest 112: , Lindblom P, Gerhardt H, Liebner S, et al: Endothelial PDGF-B retention is required for proper investment of pericytes in the microvessel wall. Genes Dev 17: , Furuhashi M, Sjoblom T, Abramsson A, et al: Platelet-derived growth factor production by B16 melanoma cells leads to increased pericyte abundance in tumors and an associated increase in tumor growth rate. Cancer Res 64: , 04. Benjamin LE, Golijanin D, Itin A, et al: Selective ablation of immature blood vessels in established human tumors follows vascular endothelial growth factor withdrawal. J Clin Invest 103: , Sundberg C, Kowanetz M, Brown LF, et al: Stable expression of angiopoietin-1 and other markers by cultured pericytes: Phenotypic similarities to a subpopulation of cells in maturing vessels during later stages of angiogenesis in vivo. Lab Invest 82:387-1, Gerhardt H, Wolburg H, Redies C: N-cadherin mediates pericytic-endothelial interaction during brain angiogenesis in the chicken. Dev Dyn 218: , Hanahan D: Heritable formation of pancreatic beta-cell tumours in transgenic mice expressing recombinant insulin/simian virus oncogenes. Nature 315: , Folkman J, Watson K, Ingber D, et al: Induction of angiogenesis during the transition from hyperplasia to neoplasia. Nature 339:58-61, Bergers G, Song S, Meyer-Morse N, et al: Benefits of targeting both pericytes and endothelial cells in the tumor vasculature with kinase inhibitors. J Clin Invest 111: , Erber R, Thurnher A, Katsen AD, et al: Combined inhibition of VEGF and PDGF signaling enforces tumor vessel regression by interfering with pericyte-mediated endothelial cell survival mechanisms. FASEB J 18:338-3, Shaheen RM, Tseng WW, Davis DW, et al: Tyrosine kinase inhibition of multiple angiogenic growth factor receptors improves survival in mice bearing colon cancer liver metastases by inhibition of endothelial cell survival mechanisms. Cancer Res 61: , Bergers G, Brekken R, McMahon G, et al: Matrix metalloproteinase-9 triggers the angiogenic switch during carcinogenesis. Nat Cell Biol 2: , Bergers G, Javaherian K, Lo KM, et al: Effects of angiogenesis inhibitors on multistage carcinogenesis in mice. Science 284: , Parangi S, O Reilly M, Christofori G, et al: Antiangiogenic therapy of transgenic mice impairs de novo tumor growth. Proc Natl Acad Sci USA 93:02-07,
RIP-Tag2 mouse model as a Paradigm for Target. Search in NETs
 RIP-Tag2 mouse model as a Paradigm for Target Search in NETs Oriol Casanovas, Ph.D. Tumor Angiogenesis Group INSTITUT CATALÀ d ONCOLOGIA IDIBELL Barcelona (SPAIN) Therapeutic Targeting of the Tumor Stroma
RIP-Tag2 mouse model as a Paradigm for Target Search in NETs Oriol Casanovas, Ph.D. Tumor Angiogenesis Group INSTITUT CATALÀ d ONCOLOGIA IDIBELL Barcelona (SPAIN) Therapeutic Targeting of the Tumor Stroma
The Process of Angiogenesis & Inhibition of Angiogenesis and/or Lymphangiogenesis
 The Process of Angiogenesis & Inhibition of Angiogenesis and/or Lymphangiogenesis Nam Deuk Kim, Ph.D. Pusan National University Contents Part 1. The process of angiogenesis Part 2. The role of angiopoietins
The Process of Angiogenesis & Inhibition of Angiogenesis and/or Lymphangiogenesis Nam Deuk Kim, Ph.D. Pusan National University Contents Part 1. The process of angiogenesis Part 2. The role of angiopoietins
UNIVERSITY OF MEDICINE AND PHARMACY CRAIOVA PhD SCHOOL. PhD THESIS
 UNIVERSITY OF MEDICINE AND PHARMACY CRAIOVA PhD SCHOOL PhD THESIS THE IMPORTANCE OF TUMOR ANGIOGENESIS IN CEREBRAL TUMOR DIAGNOSIS AND THERAPY ABSTRACT PhD COORDINATOR: Prof. univ. dr. DRICU Anica PhD
UNIVERSITY OF MEDICINE AND PHARMACY CRAIOVA PhD SCHOOL PhD THESIS THE IMPORTANCE OF TUMOR ANGIOGENESIS IN CEREBRAL TUMOR DIAGNOSIS AND THERAPY ABSTRACT PhD COORDINATOR: Prof. univ. dr. DRICU Anica PhD
Signaling Vascular Morphogenesis and Maintenance
 Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
Signaling Vascular Morphogenesis and Maintenance Douglas Hanahan Science 277: 48-50, in Perspectives (1997) Blood vessels are constructed by two processes: vasculogenesis, whereby a primitive vascular
Cancer Metronomic Therapy Milan, February 26, 2016
 Cancer Metronomic Therapy Milan, February 26, 2016 Metronomic Chemotherapy: Evolution and Development of the Concept Robert S. Kerbel, PhD Senior Scientist Sunnybrook Research Institute Professor, Dept.
Cancer Metronomic Therapy Milan, February 26, 2016 Metronomic Chemotherapy: Evolution and Development of the Concept Robert S. Kerbel, PhD Senior Scientist Sunnybrook Research Institute Professor, Dept.
Angiogenesis as a therapeutic target
 Angiogenesis as a therapeutic target Lecture Experimentelle Krebsforschung SS 07 Prof. Gerhard Christofori Institute of Biochemistry and Genetics Department of Clinical-Biological Sciences University of
Angiogenesis as a therapeutic target Lecture Experimentelle Krebsforschung SS 07 Prof. Gerhard Christofori Institute of Biochemistry and Genetics Department of Clinical-Biological Sciences University of
Benefits of targeting both pericytes and endothelial cells in the tumor vasculature with kinase inhibitors
 Benefits of targeting both pericytes and endothelial cells in the tumor vasculature with kinase inhibitors See the related Commentary beginning on page 1277. Gabriele Bergers, 1,2 Steven Song, 1,2 Nicole
Benefits of targeting both pericytes and endothelial cells in the tumor vasculature with kinase inhibitors See the related Commentary beginning on page 1277. Gabriele Bergers, 1,2 Steven Song, 1,2 Nicole
The Angiopoietin Axis in Cancer
 Ang2 Ang1 The Angiopoietin Axis in Cancer Tie2 An Overview: The Angiopoietin Axis Plays an Essential Role in the Regulation of Tumor Angiogenesis Growth of a tumor beyond a limiting size is dependent upon
Ang2 Ang1 The Angiopoietin Axis in Cancer Tie2 An Overview: The Angiopoietin Axis Plays an Essential Role in the Regulation of Tumor Angiogenesis Growth of a tumor beyond a limiting size is dependent upon
STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy. Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI)
 STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI) Topics for Consideration What are the rules for integrating
STATE OF THE ART 4: Combination Immune Therapy-Chemotherapy Elizabeth M. Jaffee (JHU) James Yang (NCI) Jared Gollob (Duke) John Kirkwood (UPMI) Topics for Consideration What are the rules for integrating
The 2010 Gastrointestinal Cancers Symposium Oral Abstract Session: Cancers of the Pancreas, Small Bowel and Hepatobilliary Tract
 The 2010 Gastrointestinal Cancers Symposium : Cancers of the Pancreas, Small Bowel and Hepatobilliary Tract Abstract #131: Phase I study of MK 0646 (dalotuzumab), a humanized monoclonal antibody against
The 2010 Gastrointestinal Cancers Symposium : Cancers of the Pancreas, Small Bowel and Hepatobilliary Tract Abstract #131: Phase I study of MK 0646 (dalotuzumab), a humanized monoclonal antibody against
Backgrounder. 1. What are targeted therapies? 2. How do targeted therapies work?
 Backgrounder TARGETED THERAPIES FOR CANCER 1. What are targeted therapies? 2. How do targeted therapies work? 3. What are some of the different types of targeted therapy? 4. What are the potential benefits
Backgrounder TARGETED THERAPIES FOR CANCER 1. What are targeted therapies? 2. How do targeted therapies work? 3. What are some of the different types of targeted therapy? 4. What are the potential benefits
METRONOMIC CHEMOTHERAPY
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk METRONOMIC CHEMOTHERAPY Author : Shasta Lynch Categories : Vets Date : October 3, 2011 Shasta Lynch looks at the promising
Vet Times The website for the veterinary profession https://www.vettimes.co.uk METRONOMIC CHEMOTHERAPY Author : Shasta Lynch Categories : Vets Date : October 3, 2011 Shasta Lynch looks at the promising
Rationale for VEGFR-targeted Therapy in RCC
 Rationale for VEGFR-targeted Therapy in RCC EIKCS, Budapest, May 2013 Tim Eisen Tim Eisen - Disclosures Company Research Support Advisory Board Trial Management Group Honoraria Astra Zeneca + + + Astellas
Rationale for VEGFR-targeted Therapy in RCC EIKCS, Budapest, May 2013 Tim Eisen Tim Eisen - Disclosures Company Research Support Advisory Board Trial Management Group Honoraria Astra Zeneca + + + Astellas
Mechanisms of Resistance to Antiangiogenic. Martin J. Edelman, MD University of Maryland Greenebaum Cancer Center Dresden, 2012
 Mechanisms of Resistance to Antiangiogenic Agents Martin J. Edelman, MD University of Maryland Greenebaum Cancer Center Dresden, 2012 Angiogenesis: A fundamental attribute of cancer Premise of Anti-angiogenic
Mechanisms of Resistance to Antiangiogenic Agents Martin J. Edelman, MD University of Maryland Greenebaum Cancer Center Dresden, 2012 Angiogenesis: A fundamental attribute of cancer Premise of Anti-angiogenic
Nintedanib in Oncology Backgrounder
 For media outside the US, UK and Canada only Nintedanib in Oncology Backgrounder 1. What is nintedanib? 2. How does nintedanib work? 3. Data overview 4. Additional clinical data 5. Nintedanib approval
For media outside the US, UK and Canada only Nintedanib in Oncology Backgrounder 1. What is nintedanib? 2. How does nintedanib work? 3. Data overview 4. Additional clinical data 5. Nintedanib approval
Predicting benefit from antiangiogenic
 Predicting benefit from antiangiogenic agents in malignancy Adrian M. Jubb*, Adam J. Oates, Scott Holden and Hartmut Koeppen Abstract A high probability of benefit is desirable to justify the choice of
Predicting benefit from antiangiogenic agents in malignancy Adrian M. Jubb*, Adam J. Oates, Scott Holden and Hartmut Koeppen Abstract A high probability of benefit is desirable to justify the choice of
Inflammatory Cells and Metastasis
 Inflammatory Cells and Metastasis Experimentelle Krebsforschung SS 07 Gerhard Christofori Institute of Biochemistry and Genetics Department of Clinical-Biological Sciences Center of Biomedicine University
Inflammatory Cells and Metastasis Experimentelle Krebsforschung SS 07 Gerhard Christofori Institute of Biochemistry and Genetics Department of Clinical-Biological Sciences Center of Biomedicine University
Integrin v 3 targeted therapy for Kaposi s sarcoma with an in vitro evolved antibody 1
 Integrin v 3 targeted therapy for Kaposi s sarcoma with an in vitro evolved antibody 1 CHRISTOPH RADER, 2 MIKHAIL POPKOV, JOHN A. NEVES, AND CARLOS F. BARBAS III 2 Department of Molecular Biology and The
Integrin v 3 targeted therapy for Kaposi s sarcoma with an in vitro evolved antibody 1 CHRISTOPH RADER, 2 MIKHAIL POPKOV, JOHN A. NEVES, AND CARLOS F. BARBAS III 2 Department of Molecular Biology and The
Chapter 7 Conclusions
 VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
Revolutionizing the Treatment of Cancer
 Revolutionizing the Treatment of Cancer June 2014 Safe Harbor Statement The statements that follow (including projections and business trends) are forward looking statements. Rexahn's actual results may
Revolutionizing the Treatment of Cancer June 2014 Safe Harbor Statement The statements that follow (including projections and business trends) are forward looking statements. Rexahn's actual results may
OMP-305B83: A Novel, Potent DLL4 & VEGF Targeting Bispecific Antibody for the Treatment Of Solid Tumors
 OMP-305B83: A Novel, Potent DLL4 & VEGF Targeting Bispecific Antibody for the Treatment Of Solid Tumors Jakob Dupont MD MA CMO, SVP: OncoMed Pharmaceuticals Adjunct Clinical Faculty: Stanford University
OMP-305B83: A Novel, Potent DLL4 & VEGF Targeting Bispecific Antibody for the Treatment Of Solid Tumors Jakob Dupont MD MA CMO, SVP: OncoMed Pharmaceuticals Adjunct Clinical Faculty: Stanford University
My name is Dr. David Ilson, Professor of Medicine at Memorial Sloan Kettering Cancer Center and Weill Cornell Medical Center in New York, New York.
 Welcome to this CME/CE-certified activity entitled, Integrating the Latest Advances Into Clinical Experience: Data and Expert Insights From the 2016 Meeting on Gastrointestinal Cancers in San Francisco.
Welcome to this CME/CE-certified activity entitled, Integrating the Latest Advances Into Clinical Experience: Data and Expert Insights From the 2016 Meeting on Gastrointestinal Cancers in San Francisco.
VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization
 Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? VEGF Is the Only Angiogenic Factor Present Throughout the Tumor Life Cycle
 Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? Martin Reck Department e t of Thoracic c Oncology ogy Hospital Grosshansdorf Germany VEGF Is the Only Angiogenic Factor Present Throughout
Antiangiogenic Agents in NSCLC Where are we? Which biomarkers? Martin Reck Department e t of Thoracic c Oncology ogy Hospital Grosshansdorf Germany VEGF Is the Only Angiogenic Factor Present Throughout
Introduction to Targeted Therapy
 Introduction to Targeted Therapy Cancer remains the second leading cause of death in the United States, despite the significant advances in cancer therapy made over the past several decades. Many factors
Introduction to Targeted Therapy Cancer remains the second leading cause of death in the United States, despite the significant advances in cancer therapy made over the past several decades. Many factors
Novel RCC Targets from Immuno-Oncology and Antibody-Drug Conjugates
 Novel RCC Targets from Immuno-Oncology and Antibody-Drug Conjugates Christopher Turner, MD Vice President, Clinical Science 04 November 2016 Uveal Melanoma Celldex Pipeline CANDIDATE INDICATION Preclinical
Novel RCC Targets from Immuno-Oncology and Antibody-Drug Conjugates Christopher Turner, MD Vice President, Clinical Science 04 November 2016 Uveal Melanoma Celldex Pipeline CANDIDATE INDICATION Preclinical
Author's response to reviews
 Author's response to reviews Title: Rapid Induction of Orthotopic Hepatocellular Carcinoma in Immune-competent Rats by Ultrasound-guided Method and the Subsequent Low-dose Chemotherapy Authors: Hoi-Hung
Author's response to reviews Title: Rapid Induction of Orthotopic Hepatocellular Carcinoma in Immune-competent Rats by Ultrasound-guided Method and the Subsequent Low-dose Chemotherapy Authors: Hoi-Hung
(PDGF), 9 ( -2 (FGF-2), SMO
 Abstract An ethanol extract from shark muscle has been shown to have potent angiogenic activity when mixed together with olive oil in a ratio of 1part extract to 9 parts olive oil. This mixture has been
Abstract An ethanol extract from shark muscle has been shown to have potent angiogenic activity when mixed together with olive oil in a ratio of 1part extract to 9 parts olive oil. This mixture has been
Immunotherapy for Breast Cancer. Aurelio B. Castrellon Medical Oncology Memorial Healthcare System
 Immunotherapy for Breast Cancer Aurelio B. Castrellon Medical Oncology Memorial Healthcare System Conflicts Research support : Cascadian therapeutics, Puma biotechnology, Odonate therapeutics, Pfizer,
Immunotherapy for Breast Cancer Aurelio B. Castrellon Medical Oncology Memorial Healthcare System Conflicts Research support : Cascadian therapeutics, Puma biotechnology, Odonate therapeutics, Pfizer,
Jefferies 2015 Global Healthcare Conference June 1, 2015
 Jefferies 2015 Global Healthcare Conference June 1, 2015 Page 0 Acceleron Forward-Looking Statements This presentation contains forward-looking statements. Forward-looking statements are neither historical
Jefferies 2015 Global Healthcare Conference June 1, 2015 Page 0 Acceleron Forward-Looking Statements This presentation contains forward-looking statements. Forward-looking statements are neither historical
National Horizon Scanning Centre. Sunitinib (Sutent) for advanced and/or metastatic breast cancer. December 2007
 Sunitinib (Sutent) for advanced and/or metastatic breast cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search. It is not
Sunitinib (Sutent) for advanced and/or metastatic breast cancer December 2007 This technology summary is based on information available at the time of research and a limited literature search. It is not
Cancer Tumor Therapy Drug Vicrostatin Shows. Promising Inhibition of Glioma Growth and. Angiogenesis in Vivo. Rupan Bose
 Bose p. 1 of 23. Cancer Tumor Therapy Drug Vicrostatin Shows Promising Inhibition of Glioma Growth and Angiogenesis in Vivo Rupan Bose B.A. Neuroscience 2011 Candidate Senior Thesis Dana and David Dornsife
Bose p. 1 of 23. Cancer Tumor Therapy Drug Vicrostatin Shows Promising Inhibition of Glioma Growth and Angiogenesis in Vivo Rupan Bose B.A. Neuroscience 2011 Candidate Senior Thesis Dana and David Dornsife
Targeting angiogenesis in cancer
 New Indigo workshop on Antiparasitic and Antitumour drugs IBMC, 9 th September, 2011 Targeting angiogenesis in cancer Raquel Soares Department of Biochemistry Tumor angiogenesis: therapeutic implications
New Indigo workshop on Antiparasitic and Antitumour drugs IBMC, 9 th September, 2011 Targeting angiogenesis in cancer Raquel Soares Department of Biochemistry Tumor angiogenesis: therapeutic implications
Research Article. Katherine M. Bell-McGuinn, 1 Alfred L. Garfall, 1 Matthew Bogyo, 2 Douglas Hanahan, 3 and Johanna A. Joyce 1. Abstract.
 Research Article Inhibition of Cysteine Cathepsin Protease Activity Enhances Chemotherapy Regimens by Decreasing Tumor Growth and Invasiveness in a Mouse Model of Multistage Cancer Katherine M. Bell-McGuinn,
Research Article Inhibition of Cysteine Cathepsin Protease Activity Enhances Chemotherapy Regimens by Decreasing Tumor Growth and Invasiveness in a Mouse Model of Multistage Cancer Katherine M. Bell-McGuinn,
A549 and A549-fLuc cells were maintained in high glucose Dulbecco modified
 Cell culture and animal model A549 and A549-fLuc cells were maintained in high glucose Dulbecco modified Eagle medium supplemented with 10% fetal bovine serum at 37 C in humidified atmosphere containing
Cell culture and animal model A549 and A549-fLuc cells were maintained in high glucose Dulbecco modified Eagle medium supplemented with 10% fetal bovine serum at 37 C in humidified atmosphere containing
Evidence for Systemic Effects Moves PV-10 Toward Further Clinical Trials
 PV-10 Moves Forward-1 Evidence for Systemic Effects Moves PV-10 Toward Further Clinical Trials At the same time that current research projects are solidifying and reinforcing the evidence for PV-10 s systemic
PV-10 Moves Forward-1 Evidence for Systemic Effects Moves PV-10 Toward Further Clinical Trials At the same time that current research projects are solidifying and reinforcing the evidence for PV-10 s systemic
Horizon Scanning Technology Briefing. Sutent (Sunitinib) for first-line and adjuvant treatment of renal cell carcinoma
 Horizon Scanning Technology Briefing National Horizon Scanning Centre Sutent (Sunitinib) for first-line and adjuvant treatment of renal cell carcinoma August 2006: Updated October 2006 This technology
Horizon Scanning Technology Briefing National Horizon Scanning Centre Sutent (Sunitinib) for first-line and adjuvant treatment of renal cell carcinoma August 2006: Updated October 2006 This technology
Revolutionizing the Treatment of Cancer
 Revolutionizing the Treatment of Cancer January 2014 Safe Harbor Statement The statements that follow (including projections and business trends) are forward looking statements. Rexahn's actual results
Revolutionizing the Treatment of Cancer January 2014 Safe Harbor Statement The statements that follow (including projections and business trends) are forward looking statements. Rexahn's actual results
Biologics Effects of Targeted Therapeutics
 Report on the isbtc Mini-symposium on Biologics Effects of Targeted Therapeutics Michael B. Atkins, MD Beth Israel Deaconess Medical Center Louis Weiner, M.D. Fox Chase Cancer Center Report on the isbtc
Report on the isbtc Mini-symposium on Biologics Effects of Targeted Therapeutics Michael B. Atkins, MD Beth Israel Deaconess Medical Center Louis Weiner, M.D. Fox Chase Cancer Center Report on the isbtc
Novel Molecular Molecular Therapies In Hepatocarcinoma Prof Eric
 Novel Molecular Therapies In Hepatocarcinoma Prof. Eric Raymond Department of Médical Oncology Hôpital Beaujon, Clichy Université Paris 7 Denis Diderot INSERM-U728 eric.raymond@bjn.aphp.fr HCC is a highly
Novel Molecular Therapies In Hepatocarcinoma Prof. Eric Raymond Department of Médical Oncology Hôpital Beaujon, Clichy Université Paris 7 Denis Diderot INSERM-U728 eric.raymond@bjn.aphp.fr HCC is a highly
Breast Cancer: the interplay of biology, drugs, radiation. Prof. L. Livi Università degli Studi di Firenze. Brescia, October 3rd 4th, 2013
 Breast Cancer: the interplay of biology, drugs, radiation Prof. L. Livi Università degli Studi di Firenze Brescia, October 3rd 4th, 2013 BACKGROUND (1) The complex interactions between tumor-specific signaling
Breast Cancer: the interplay of biology, drugs, radiation Prof. L. Livi Università degli Studi di Firenze Brescia, October 3rd 4th, 2013 BACKGROUND (1) The complex interactions between tumor-specific signaling
Supplemental Data. Wnt/β-Catenin Signaling in Mesenchymal Progenitors. Controls Osteoblast and Chondrocyte
 Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
Supplemental Data Wnt/β-Catenin Signaling in Mesenchymal Progenitors Controls Osteoblast and Chondrocyte Differentiation during Vertebrate Skeletogenesis Timothy F. Day, Xizhi Guo, Lisa Garrett-Beal, and
Targeted Therapies in Metastatic Colorectal Cancer: An Update
 Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
Personalized medicine by the use of mathematical models for angiogenesis: validation in a Mesenchymal Chondrosarcoma patient
 Personalized medicine by the use of mathematical models for angiogenesis: validation in a Mesenchymal Chondrosarcoma patient Agur Zvia Institute for Medical BioMathematics, IMBM Agenda Medical problem:
Personalized medicine by the use of mathematical models for angiogenesis: validation in a Mesenchymal Chondrosarcoma patient Agur Zvia Institute for Medical BioMathematics, IMBM Agenda Medical problem:
Adverse side effects associated to metronomic chemotherapy
 Adverse side effects associated to metronomic chemotherapy Elisabetta Munzone, MD Division of Medical Senology Istituto Europeo di Oncologia Milano, Italy LDM: the optimal biological dose Although there
Adverse side effects associated to metronomic chemotherapy Elisabetta Munzone, MD Division of Medical Senology Istituto Europeo di Oncologia Milano, Italy LDM: the optimal biological dose Although there
Revolutionizing the Treatment of Cancer
 Revolutionizing the Treatment of Cancer March 2014 Safe Harbor Statement The statements that follow (including projections and business trends) are forward-looking statements. Rexahn's actual results may
Revolutionizing the Treatment of Cancer March 2014 Safe Harbor Statement The statements that follow (including projections and business trends) are forward-looking statements. Rexahn's actual results may
PATHOBIOLOGY OF NEOPLASIA
 PATHOBIOLOGY OF NEOPLASIA Department of Pathology Gadjah Mada University School of Medicine dr. Harijadi Blok Biomedis, 6 Maret 2009 [12] 3/17/2009 1 The pathobiology of neoplasia Normal cells Malignant
PATHOBIOLOGY OF NEOPLASIA Department of Pathology Gadjah Mada University School of Medicine dr. Harijadi Blok Biomedis, 6 Maret 2009 [12] 3/17/2009 1 The pathobiology of neoplasia Normal cells Malignant
Critical Clinical Updates
 Critical Clinical Updates ASTRO Spring Refresher Course JW Marriott Hotel Ramesh Rengan MD PhD Department of Radiation Oncology Friday March 22, 2013 Learning Objectives At the conclusion of this activity,
Critical Clinical Updates ASTRO Spring Refresher Course JW Marriott Hotel Ramesh Rengan MD PhD Department of Radiation Oncology Friday March 22, 2013 Learning Objectives At the conclusion of this activity,
BLU-554, A Novel, Potent and Selective Inhibitor of FGFR4 for the Treatment of Liver Cancer
 BLU-554, A Novel, Potent and Selective Inhibitor of FGFR4 for the Treatment of Liver Cancer Dr Klaus Hoeflich, PhD Director of Biology, Blueprint Medicines Disclosures Employee and shareholder of Blueprint
BLU-554, A Novel, Potent and Selective Inhibitor of FGFR4 for the Treatment of Liver Cancer Dr Klaus Hoeflich, PhD Director of Biology, Blueprint Medicines Disclosures Employee and shareholder of Blueprint
Antibody-Drug Conjugates in Glioblastoma Multiforme: Finding Ways Forward
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Pediatric Preclinical Testing Program (PPTP) evaluation of the Bcl-2 inhibitor ABT-263
 Pediatric Preclinical Testing Program (PPTP) evaluation of the Bcl-2 inhibitor ABT-263 Malcolm A. Smith, John M. Maris, Stephen T. Keir, Henry S. Friedman, Richard B. Lock, Hernan Carol, Mayamin Tajbakhsh,
Pediatric Preclinical Testing Program (PPTP) evaluation of the Bcl-2 inhibitor ABT-263 Malcolm A. Smith, John M. Maris, Stephen T. Keir, Henry S. Friedman, Richard B. Lock, Hernan Carol, Mayamin Tajbakhsh,
NEWS RELEASE Media Contact: Megan Pace Investor Contact: Kathee Littrell Patient Inquiries: Ajanta Horan
 NEWS RELEASE Media Contact: Megan Pace 650-467-7334 Investor Contact: Kathee Littrell 650-225-1034 Patient Inquiries: Ajanta Horan 650-467-1741 GENENTECH RECEIVES COMPLETE RESPONSE LETTER FROM FDA FOR
NEWS RELEASE Media Contact: Megan Pace 650-467-7334 Investor Contact: Kathee Littrell 650-225-1034 Patient Inquiries: Ajanta Horan 650-467-1741 GENENTECH RECEIVES COMPLETE RESPONSE LETTER FROM FDA FOR
Type 1 Diabetes: Islet expressing GAD65 (green) with DAPI (Blue) Islet expressing Insulin (red) in 3D confocal imaging
 Type 1 Diabetes: Our group has been studying autoimmune diabetes for many years. Recently, we have developed a humanized mouse model of Type 1 Diabetes (T1D). We believe this model will help understand
Type 1 Diabetes: Our group has been studying autoimmune diabetes for many years. Recently, we have developed a humanized mouse model of Type 1 Diabetes (T1D). We believe this model will help understand
Anti-angiogenesis in cancer; met and unmet goals - an interview with Robert Kerbel
 Int. J. Dev. Biol. 55: 395-398 doi: 10.1387/ijdb.103217fb www.intjdevbiol.com Anti-angiogenesis in cancer; met and unmet goals - an interview with Robert Kerbel FRANCESCO BERTOLINI* Laboratory of Hematology-Oncology,
Int. J. Dev. Biol. 55: 395-398 doi: 10.1387/ijdb.103217fb www.intjdevbiol.com Anti-angiogenesis in cancer; met and unmet goals - an interview with Robert Kerbel FRANCESCO BERTOLINI* Laboratory of Hematology-Oncology,
Targeting the Expression of the Angiogenic Phenotype in Head and Neck Cancer
 Targeting the Expression of the Angiogenic Phenotype in Head and Neck Cancer Mark W. Lingen, DDS, PhD, FRCPath Introduction With over 600,000 new cases annually, squamous cell carcinoma of the head and
Targeting the Expression of the Angiogenic Phenotype in Head and Neck Cancer Mark W. Lingen, DDS, PhD, FRCPath Introduction With over 600,000 new cases annually, squamous cell carcinoma of the head and
Fifteenth International Kidney Cancer Symposium November 4-5, 2016 Marriott Miami Biscayne Bay, Miami, Florida, USA
 The following presentation should not be regarded as an endorsement of a particular product/drug/technique by the speaker. The presentation topics were assigned to the speakers by the scientific committee
The following presentation should not be regarded as an endorsement of a particular product/drug/technique by the speaker. The presentation topics were assigned to the speakers by the scientific committee
Imaging Cancer Treatment Complications in the Chest
 Imaging Cancer Treatment Complications in the Chest Michelle S. Ginsberg, MD Objectives Imaging Cancer Treatment Complications in the Chest To understand the mechanisms of action of different classes of
Imaging Cancer Treatment Complications in the Chest Michelle S. Ginsberg, MD Objectives Imaging Cancer Treatment Complications in the Chest To understand the mechanisms of action of different classes of
Supplementary Materials. for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis
 Supplementary Materials for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis 1 Supplementary Figure Legends Supplementary Figure 1: Integrin expression
Supplementary Materials for Garmy-Susini, et al, Integrin 4 1 signaling is required for lymphangiogenesis and tumor metastasis 1 Supplementary Figure Legends Supplementary Figure 1: Integrin expression
Correlation between expression and significance of δ-catenin, CD31, and VEGF of non-small cell lung cancer
 Correlation between expression and significance of δ-catenin, CD31, and VEGF of non-small cell lung cancer X.L. Liu 1, L.D. Liu 2, S.G. Zhang 1, S.D. Dai 3, W.Y. Li 1 and L. Zhang 1 1 Thoracic Surgery,
Correlation between expression and significance of δ-catenin, CD31, and VEGF of non-small cell lung cancer X.L. Liu 1, L.D. Liu 2, S.G. Zhang 1, S.D. Dai 3, W.Y. Li 1 and L. Zhang 1 1 Thoracic Surgery,
Current Status of Studies on Targeted Therapy for Renal Cell Carcinoma
 294 Chin J Clin Oncol (2008) 5: 294~298 DOI 10.1007/s11805-008-0294-x Current Status of Studies on Targeted Therapy for Renal Cell Carcinoma Shaoqi Wang 1 Shaoxiang Wang 2 Juan Wang 1 1 Department of Oncology,
294 Chin J Clin Oncol (2008) 5: 294~298 DOI 10.1007/s11805-008-0294-x Current Status of Studies on Targeted Therapy for Renal Cell Carcinoma Shaoqi Wang 1 Shaoxiang Wang 2 Juan Wang 1 1 Department of Oncology,
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
Metronomic chemotherapy for breast cancer
 Metronomic chemotherapy for breast cancer M. Colleoni International Breast Cancer Study Group (IBCSG), Division of Medical Senology, European Institute of Oncology Metronomic Scheduling and Inhibition
Metronomic chemotherapy for breast cancer M. Colleoni International Breast Cancer Study Group (IBCSG), Division of Medical Senology, European Institute of Oncology Metronomic Scheduling and Inhibition
SHREE ET AL, SUPPLEMENTAL MATERIALS. (A) Workflow for tumor cell line derivation and orthotopic implantation.
 SHREE ET AL, SUPPLEMENTAL MATERIALS SUPPLEMENTAL FIGURE AND TABLE LEGENDS Supplemental Figure 1. Derivation and characterization of TS1-TGL and TS2-TGL PyMT cell lines and development of an orthotopic
SHREE ET AL, SUPPLEMENTAL MATERIALS SUPPLEMENTAL FIGURE AND TABLE LEGENDS Supplemental Figure 1. Derivation and characterization of TS1-TGL and TS2-TGL PyMT cell lines and development of an orthotopic
Simultaneous blockade of PD-1 and VEGFR2 induces synergistic. Short title: Synergistic antitumour effect by dual blockade of PD-1 and VEGFR2
 carticle Simultaneous blockade of PD-1 and VEGFR2 induces synergistic antitumour effect in vivo 1 Short title: Synergistic antitumour effect by dual blockade of PD-1 and VEGFR2 S. Yasuda 1, M. Sho 1, I.
carticle Simultaneous blockade of PD-1 and VEGFR2 induces synergistic antitumour effect in vivo 1 Short title: Synergistic antitumour effect by dual blockade of PD-1 and VEGFR2 S. Yasuda 1, M. Sho 1, I.
Inhibitors of Methionine Aminopeptidase-2 2 in the Treatment of Non-Hodgkin
 Inhibitors of Methionine Aminopeptidase-2 2 in the Treatment of Non-Hodgkin Hodgkin s s Lymphoma Targeted Cancer Therapies William Westlin, Ph.D. Vice President, Preclinical Research Discovery of Fumagillin
Inhibitors of Methionine Aminopeptidase-2 2 in the Treatment of Non-Hodgkin Hodgkin s s Lymphoma Targeted Cancer Therapies William Westlin, Ph.D. Vice President, Preclinical Research Discovery of Fumagillin
Angiogenesis and tumor growth
 Anti-angiogenic agents: where we are? Martin Reck Department of Thoracic Oncology Hospital Grosshansdorf Germany Angiogenesis and tumor growth Journal of experimental Medicine 1972; 133: 275-88 1 Angiogenesis
Anti-angiogenic agents: where we are? Martin Reck Department of Thoracic Oncology Hospital Grosshansdorf Germany Angiogenesis and tumor growth Journal of experimental Medicine 1972; 133: 275-88 1 Angiogenesis
Heterotypy and Angiogenesis
 Heterotypy and Angiogenesis Tumors are perpetual wounds 1. Normally stroma and epithelia converse at a distance. 2. Juxtaposition of stroma and epithelia is indicative of tissue damage. 4. Activate strategies
Heterotypy and Angiogenesis Tumors are perpetual wounds 1. Normally stroma and epithelia converse at a distance. 2. Juxtaposition of stroma and epithelia is indicative of tissue damage. 4. Activate strategies
Quantification of early stage lesions for loss of p53 should be shown in the main figures.
 Reviewer #1 (Remarks to the Author): Expert in prostate cancer The manuscript "Clonal dynamics following p53 loss of heterozygosity in Kras-driven cancers" uses a number of novel genetically engineered
Reviewer #1 (Remarks to the Author): Expert in prostate cancer The manuscript "Clonal dynamics following p53 loss of heterozygosity in Kras-driven cancers" uses a number of novel genetically engineered
Neuroendocrine Tumors: Just the Basics. George Fisher, MD PhD
 Neuroendocrine Tumors: Just the Basics George Fisher, MD PhD Topics that we will not discuss Some types of lung cancer: Small cell neuroendocrine lung cancer Large cell neuroendocrine lung cancer Some
Neuroendocrine Tumors: Just the Basics George Fisher, MD PhD Topics that we will not discuss Some types of lung cancer: Small cell neuroendocrine lung cancer Large cell neuroendocrine lung cancer Some
DAWNING OF THE AGE OF ANGIOGENESIS
 DAWNING OF THE AGE OF ANGIOGENESIS Bob Leibowitz, M.D. DIPLOMATE AMERICAN BOARDS OF INTERNAL MEDICINE AND SUBSPECIALTIES OF MEDICAL ONCOLOGY AND HEMATOLOGY December 1997 April 2004 (Revised) Angiogenesis
DAWNING OF THE AGE OF ANGIOGENESIS Bob Leibowitz, M.D. DIPLOMATE AMERICAN BOARDS OF INTERNAL MEDICINE AND SUBSPECIALTIES OF MEDICAL ONCOLOGY AND HEMATOLOGY December 1997 April 2004 (Revised) Angiogenesis
BNC105 Results Presentation
 Creating and developing innovative therapies BNC105 Results Presentation Dr Deborah Rathjen CEO & Managing Director, Bionomics Limited Dr José Iglesias Chief Medical Officer, Bionomics Limited Dr Tom Hutson
Creating and developing innovative therapies BNC105 Results Presentation Dr Deborah Rathjen CEO & Managing Director, Bionomics Limited Dr José Iglesias Chief Medical Officer, Bionomics Limited Dr Tom Hutson
Reviewers' comments: Reviewer #1 (Remarks to the Author):
 Reviewers' comments: Reviewer #1 (Remarks to the Author): In the manuscript Rational Combination of CXCL11-Expressing Oncolytic Virus and PD-L1 Blockade Works Synergistically to Enhance Therapeutic Efficacy
Reviewers' comments: Reviewer #1 (Remarks to the Author): In the manuscript Rational Combination of CXCL11-Expressing Oncolytic Virus and PD-L1 Blockade Works Synergistically to Enhance Therapeutic Efficacy
Society for Immunotherapy of Cancer (SITC) Immunotherapy for the Treatment of Brain Metastases
 Society for Immunotherapy of Cancer (SITC) Immunotherapy for the Treatment of Brain Metastases Geoffrey T. Gibney, MD Georgetown-Lombardi Comprehensive Cancer Center Medstar-Georgetown University Hospital
Society for Immunotherapy of Cancer (SITC) Immunotherapy for the Treatment of Brain Metastases Geoffrey T. Gibney, MD Georgetown-Lombardi Comprehensive Cancer Center Medstar-Georgetown University Hospital
Supplementary Figure 1
 Supplementary Figure 1 # nonsynonymous mutations (tngs, 1561 genes) 600 p=0.056 500 250 200 150 100 50 0 HLA-DR (-) HLA-DR (+) Supplementary Figure 1: HLA-DR(+) melanoma cell lines are associated with
Supplementary Figure 1 # nonsynonymous mutations (tngs, 1561 genes) 600 p=0.056 500 250 200 150 100 50 0 HLA-DR (-) HLA-DR (+) Supplementary Figure 1: HLA-DR(+) melanoma cell lines are associated with
Study No Title : Rationale: Phase: Study Period: Study Design: Centres: Indication: Treatment:
 The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
The study listed may include approved and non-approved uses, formulations or treatment regimens. The results reported in any single study may not reflect the overall results obtained on studies of a product.
(212) Investors Contact: Ryan Crowe (212)
 For immediate release: February 5, 2014 Media Contact: Sally Beatty (212) 733-6566 Investors Contact: Ryan Crowe (212) 733-8160 Pfizer And Merck To Collaborate On Innovative Anti-Cancer Combination Studies
For immediate release: February 5, 2014 Media Contact: Sally Beatty (212) 733-6566 Investors Contact: Ryan Crowe (212) 733-8160 Pfizer And Merck To Collaborate On Innovative Anti-Cancer Combination Studies
Targeted Medicine and Molecular Therapeutics. Angus McIntyre, M.D. Medical Oncologist, Addison Gilbert Hospital and Beverly Hospital October 6, 2009
 Targeted Medicine and Molecular Therapeutics Angus McIntyre, M.D. Medical Oncologist, Addison Gilbert Hospital and Beverly Hospital October 6, 2009 Approaches to Cancer Prevention Screening and early diagnosis
Targeted Medicine and Molecular Therapeutics Angus McIntyre, M.D. Medical Oncologist, Addison Gilbert Hospital and Beverly Hospital October 6, 2009 Approaches to Cancer Prevention Screening and early diagnosis
2/1/2017. Agenda. David F. Williams, MD, MBA. History of Current Treatment. Current Treatment/Wet AMD Anti-VEGF Drugs. History of Current Treatment
 UPDATE ON CLINICAL TRIALS FOR AMD David F. Williams, MD, MBA Agenda Brief History of Current Rx Recently Completed/New CTs: Wet AMD Recently Completed/New CTs: Dry AMD Current Treatment/Wet AMD Anti-VEGF
UPDATE ON CLINICAL TRIALS FOR AMD David F. Williams, MD, MBA Agenda Brief History of Current Rx Recently Completed/New CTs: Wet AMD Recently Completed/New CTs: Dry AMD Current Treatment/Wet AMD Anti-VEGF
Revolutionizing the Treatment of Cancer
 Revolutionizing the Treatment of Cancer September 2013 Safe Harbor Statement The statements that follow (including projections and business trends) are forward looking statements. Rexahn's actual results
Revolutionizing the Treatment of Cancer September 2013 Safe Harbor Statement The statements that follow (including projections and business trends) are forward looking statements. Rexahn's actual results
Imaging of glycolytic metabolism in primary glioblastoma cells with
 63 Chapter 5 Imaging of glycolytic metabolism in primary glioblastoma cells with RIMChip 5.1. Introduction Glioblastoma(GBM) is one of the most common brain tumors 1. It is composed of heterogeneous subpopulations
63 Chapter 5 Imaging of glycolytic metabolism in primary glioblastoma cells with RIMChip 5.1. Introduction Glioblastoma(GBM) is one of the most common brain tumors 1. It is composed of heterogeneous subpopulations
The Annexin V Apoptosis Assay
 The Annexin V Apoptosis Assay Development of the Annexin V Apoptosis Assay: 1990 Andree at al. found that a protein, Vascular Anticoagulant α, bound to phospholipid bilayers in a calcium dependent manner.
The Annexin V Apoptosis Assay Development of the Annexin V Apoptosis Assay: 1990 Andree at al. found that a protein, Vascular Anticoagulant α, bound to phospholipid bilayers in a calcium dependent manner.
David N. Robinson, MD
 David N. Robinson, MD Background and Treatment of mrcc Background ~ 64,770 new cases of kidney/renal pelvis cancers will be diagnosed in the US in 2012 with an estimated 13,570 deaths [1] ~ 75% are clear-cell
David N. Robinson, MD Background and Treatment of mrcc Background ~ 64,770 new cases of kidney/renal pelvis cancers will be diagnosed in the US in 2012 with an estimated 13,570 deaths [1] ~ 75% are clear-cell
José Baselga, MD, PhD
 i n t e r v i e w José Baselga, MD, PhD Dr Baselga is Physician-in-Chief at Memorial Sloan-Kettering Cancer Center in New York, New York. Tracks 1-15 Track 1 Track 2 Track 3 Track 4 Track 5 Track 6 Track
i n t e r v i e w José Baselga, MD, PhD Dr Baselga is Physician-in-Chief at Memorial Sloan-Kettering Cancer Center in New York, New York. Tracks 1-15 Track 1 Track 2 Track 3 Track 4 Track 5 Track 6 Track
Vascular Endothelial Growth Factor in Human Colon Cancer: Biology and Therapeutic Implications
 Vascular Endothelial Growth Factor in Human Colon Cancer: iology and Therapeutic Implications LEE M. ELLIS, YUTK TKHSHI, WENIO LIU, RYMOND M. SHHEEN University of Texas M.D. nderson Cancer Center, Departments
Vascular Endothelial Growth Factor in Human Colon Cancer: iology and Therapeutic Implications LEE M. ELLIS, YUTK TKHSHI, WENIO LIU, RYMOND M. SHHEEN University of Texas M.D. nderson Cancer Center, Departments
Durable Response Rate in High Grade Glioma: an Emerging Endpoint for Immunotherapeutics. Timothy Cloughesy, MD University of California, Los Angeles
 Durable Response Rate in High Grade Glioma: an Emerging Endpoint for Immunotherapeutics Timothy Cloughesy, MD University of California, Los Angeles Disclosure 2 FDA Endpoints for the Approval of Cancer
Durable Response Rate in High Grade Glioma: an Emerging Endpoint for Immunotherapeutics Timothy Cloughesy, MD University of California, Los Angeles Disclosure 2 FDA Endpoints for the Approval of Cancer
Introduction. Cancer Biology. Tumor-suppressor genes. Proto-oncogenes. DNA stability genes. Mechanisms of carcinogenesis.
 Cancer Biology Chapter 18 Eric J. Hall., Amato Giaccia, Radiobiology for the Radiologist Introduction Tissue homeostasis depends on the regulated cell division and self-elimination (programmed cell death)
Cancer Biology Chapter 18 Eric J. Hall., Amato Giaccia, Radiobiology for the Radiologist Introduction Tissue homeostasis depends on the regulated cell division and self-elimination (programmed cell death)
Tumor Associated Macrophages as a Novel Target for Cancer Therapy
 Tumor mass Tumor Associated Macrophage Tumor Associated Macrophages as a Novel Target for Cancer Therapy This booklet contains forward-looking statements that are based on Amgen s current expectations
Tumor mass Tumor Associated Macrophage Tumor Associated Macrophages as a Novel Target for Cancer Therapy This booklet contains forward-looking statements that are based on Amgen s current expectations
Therapeutic targeting neuraminidase-1 in multi-stage of tumorigenesis
 Therapeutic targeting neuraminidase-1 in multi-stage of tumorigenesis Myron R. Szewczuk Dept. Biomedical and Molecular Sciences, Queen's University, Kingston, K7L 3N6 Ontario, Canada HIGHLIGHTS. An innovative
Therapeutic targeting neuraminidase-1 in multi-stage of tumorigenesis Myron R. Szewczuk Dept. Biomedical and Molecular Sciences, Queen's University, Kingston, K7L 3N6 Ontario, Canada HIGHLIGHTS. An innovative
CANCER THERAPEUTICS: A NOVEL APPROACH
 CANCER THERAPEUTICS: A NOVEL APPROACH Mary Dwyer, Ph.D. HBRI and ChemRegen, Inc. SCDMDG Meeting October 23, 212 Outline Introduction Hit, HBRI1: identification & characterization Leads, HBRI2 & HBRI3:
CANCER THERAPEUTICS: A NOVEL APPROACH Mary Dwyer, Ph.D. HBRI and ChemRegen, Inc. SCDMDG Meeting October 23, 212 Outline Introduction Hit, HBRI1: identification & characterization Leads, HBRI2 & HBRI3:
NGR-TNF selectively binds to tumor blood vessels via CD13, inducing the activation of caspases and promoting apoptotic endothelial cell death in vivo
 AACR 100 th Annual Meeting 2009 Denver NGR-TNF selectively binds to tumor blood vessels via CD13, inducing the activation of caspases and promoting apoptotic endothelial cell death in vivo The NGR-hTNF
AACR 100 th Annual Meeting 2009 Denver NGR-TNF selectively binds to tumor blood vessels via CD13, inducing the activation of caspases and promoting apoptotic endothelial cell death in vivo The NGR-hTNF
Ipilimumab ASCO Data Review and Discussion Webcast. Monday, June 2, 2008
 Ipilimumab ASCO Data Review and Discussion Webcast Monday, June 2, 2008 Slide 2 Forward Looking Statements Except for historical information, the matters contained in this slide presentation may constitute
Ipilimumab ASCO Data Review and Discussion Webcast Monday, June 2, 2008 Slide 2 Forward Looking Statements Except for historical information, the matters contained in this slide presentation may constitute
Pharmacokinetics, pharmacodynamics and pharmacogenetics of metronomic chemotherapy
 Divisione di Farmacologia Dipartimento di Medicina Clinica and Sperimentale Università di Pisa U.O. Farmacologia Clinica Azienda Ospedaliero Universitaria Pisana Pharmacokinetics, pharmacodynamics and
Divisione di Farmacologia Dipartimento di Medicina Clinica and Sperimentale Università di Pisa U.O. Farmacologia Clinica Azienda Ospedaliero Universitaria Pisana Pharmacokinetics, pharmacodynamics and
NEWS RELEASE Media Contact: Krysta Pellegrino (650) Investor Contact: Sue Morris (650) Advocacy Contact: Kristin Reed (650)
 NEWS RELEASE Media Contact: Krysta Pellegrino (650) 225-8226 Investor Contact: Sue Morris (650) 225-6523 Advocacy Contact: Kristin Reed (650) 467-9831 FDA APPROVES AVASTIN IN COMBINATION WITH CHEMOTHERAPY
NEWS RELEASE Media Contact: Krysta Pellegrino (650) 225-8226 Investor Contact: Sue Morris (650) 225-6523 Advocacy Contact: Kristin Reed (650) 467-9831 FDA APPROVES AVASTIN IN COMBINATION WITH CHEMOTHERAPY
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only.
 The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
The following slides are provided as presented by the author during the live educa7onal ac7vity and are intended for reference purposes only. If you have any ques7ons, please contact Imedex via email at:
Supplemental Material
 Supplemental Material Supplementary Fig. 1. EETs stimulate primary tumor growth. a) Schematic presentation of genetic and pharmacological tools used to manipulate endogenous EET levels. b) Endothelial
Supplemental Material Supplementary Fig. 1. EETs stimulate primary tumor growth. a) Schematic presentation of genetic and pharmacological tools used to manipulate endogenous EET levels. b) Endothelial
SU2C TOP SCIENCE ACCOMPLISHMENTS
 SU2C TOP SCIENCE ACCOMPLISHMENTS INTRODUCTION Since our founding in 2008, Stand Up To Cancer has funded 87 team science projects, with budgets ranging from $250,000 for a short research project to over
SU2C TOP SCIENCE ACCOMPLISHMENTS INTRODUCTION Since our founding in 2008, Stand Up To Cancer has funded 87 team science projects, with budgets ranging from $250,000 for a short research project to over
For personal use only
 ASX and Media release 6 April 211 Circadian s Inhibits Tumour Growth in Models of Lung, Ovarian and Prostate Cancer Data demonstrates efficacy of with other therapeutic agents in mouse models of lung,
ASX and Media release 6 April 211 Circadian s Inhibits Tumour Growth in Models of Lung, Ovarian and Prostate Cancer Data demonstrates efficacy of with other therapeutic agents in mouse models of lung,
Antiangiogenic Potency of Various Chemotherapeutic Drugs for Metronomic Chemotherapy
 Antiangiogenic Potency of Various Chemotherapeutic Drugs for Metronomic Chemotherapy JOACHIM DREVS 1, JULIA FAKLER 1, SILKE EISELE 1, MICHAEL MEDINGER 1, GERLINDE BING 1, NORBERT ESSER 2, DIETER MARMÉ
Antiangiogenic Potency of Various Chemotherapeutic Drugs for Metronomic Chemotherapy JOACHIM DREVS 1, JULIA FAKLER 1, SILKE EISELE 1, MICHAEL MEDINGER 1, GERLINDE BING 1, NORBERT ESSER 2, DIETER MARMÉ
NASDAQ: CYTR FIGHTING CANCER WITH CUTTING EDGE SCIENCE. Corporate Overview. July 2018
 NASDAQ: CYTR Corporate Overview July 2018 CytRx Safe Harbor Statement THIS PRESENTATION CONTAINS FORWARD-LOOKING STATEMENTS THAT INVOLVE CERTAIN RISKS AND UNCERTAINTIES. ACTUAL RESULTS COULD DIFFER MATERIALLY
NASDAQ: CYTR Corporate Overview July 2018 CytRx Safe Harbor Statement THIS PRESENTATION CONTAINS FORWARD-LOOKING STATEMENTS THAT INVOLVE CERTAIN RISKS AND UNCERTAINTIES. ACTUAL RESULTS COULD DIFFER MATERIALLY
June IMMUNE DESIGN The in vivo generation of cytotoxic CD8 T cells (CTLs)
 June 2015 IMMUNE DESIGN The in vivo generation of cytotoxic CD8 T cells (CTLs) 1 Forward-looking Statements This presentation contains forward-looking statements with respect to, among other things, our
June 2015 IMMUNE DESIGN The in vivo generation of cytotoxic CD8 T cells (CTLs) 1 Forward-looking Statements This presentation contains forward-looking statements with respect to, among other things, our
