Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up
|
|
|
- Silas Warren
- 6 years ago
- Views:
Transcription
1 Annals of Oncology 24 (Supplement 6): vi149 vi154, 2013 doi: /annonc/mdt242 Published online 17 July 2013 Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up R. Willemze 1, E. Hodak 2, P. L. Zinzani 3, L. Specht 4 & M. Ladetto 5, on behalf of the ESMO Guidelines Working Group* 1 Department of Dermatology, Leiden University Medical Centre, Leiden, The Netherlands; 2 Department of Dermatology, Rabin Medical Centre, Beilinson Hospital, Petach Tikva, Israel; 3 Institute of Haematology and Medical Oncology, University of Bologna, Bologna, Italy; 4 Department of Oncology and Haematology, Rigshospitalet, University of Copenhagen, Copenhagen, Denmark; 5 Department of Molecular Biotechnology and Health Sciences, University of Torino, Torino, Italy, These Clinical Practice Guidelines are endorsed by the Japanese Society of Medical Oncology (JSMO) epidemiology Primary cutaneous lymphomas (PCLs) are defined as non- Hodgkin s lymphomasthatpresentintheskinwithno evidence of extracutaneous disease at the time of diagnosis. After the gastrointestinal lymphomas, PCLs are the second most common group of extranodal non-hodgkin s lymphomas with an estimated annual incidence of 1/ in Western countries. PCLs must be distinguished from nodal or systemic malignant lymphomas involving the skin secondarily, which often have another clinical behaviour, have a different prognosis and require a different therapeutic approach. In recent lymphoma classifications, PCLs are therefore included as separate entities. Within the group of PCLs, distinct types of cutaneous T-cell lymphoma (CTCL) and cutaneous B-cell lymphoma (CBCL) can be distinguished [1, 2]. In the western world, CTCL constitutes 75% 80% of all PCLs, with mycosis fungoides (MF) as the most common type of CTCL, and CBCL 20% 25% [1]. However, different distributions have been observed in other parts of the world. In southeast Asian countries, CTCLs other than MF, in particular Epstein-Barr virus-associated natural killer/t-cell lymphomas, are much more common than in Western countries, while CBCLs are much more uncommon [3, 4]. diagnosis The diagnosis and classification of PCLs should always be based on a combination of clinical, histological and immunophenotypical data. Demonstration of clonal T-cell receptor or immunoglobulin gene rearrangements in lesional *Correspondence to: ESMO Guidelines Working Group, ESMO Head Office, Via L. Taddei 4, CH-6962 Viganello-Lugano, Switzerland; clinicalguidelines@esmo.org Approved by the ESMO Guidelines Working Group: December 2006, last update June This publication supersedes the previously published version. Ann Oncol 2010; 21 (Suppl. 5): v177 v180. skin or peripheral blood may be a valuable adjunct in selected cases. However, clinical and histopathological features are, in most cases, the most important deciding factors for therapeutic planning. PCLs should be classified according to the criteria of the World Health Organisation European Organisation for Research and Treatment of Cancer (WHO EORTC) classification (Table 1)[1]. staging In all cases, adequate staging should be carried out to exclude the presence of extracutaneous disease. Staging includes complete physical examination, complete and differential blood cell count and serum biochemistry and appropriate imaging studies (computed tomography scans ± [ 18 F]2-fluoro- 2-deoxy-D-glucose positron emission tomography scans in all but stage IA), although they are not required in patients with lymphomatoid papulosis (LyP) [5, 6]. Flow cytometry of the peripheral blood should only be carried out in selected cases, but is mandatory in patients with (suspected) Sézary syndrome (SS). Bone marrow biopsy and aspiration should be carried out in cutaneous lymphomas with an intermediate or aggressive clinical behaviour, but is not required in cutaneous lymphomas with an indolent clinical behaviour (MF, cutaneous anaplastic large-cell lymphoma and cutaneous marginal zone lymphoma), unless indicated by other staging assessments [5, 6]. The significanceofbonemarrow examination in primary cutaneous follicle centre lymphoma (PCFCL) is controversial [6, 7]. Prognosis is extremely variable depending on the type of PCL and the stage of disease. For clinical staging of MF and SS, the revised International Society for Cutaneous Lymphomas/European Organization of Research and Treatment of Cancer (ISCL/EORTC) TNMB (tumour node metastasis-blood) staging system should be used (Tables 2 and 3)[5].ForPCLotherthanMF/SS,a separate ISCL/EORTC TNM classification system has been published [6]. This staging system is primarily intended to document the extent of disease and cannot be used as a prognostic guide. clinical practice guidelines The Author Published by Oxford University Press on behalf of the European Society for Medical Oncology. All rights reserved. For permissions, please journals.permissions@oup.com.
2 Annals of Oncology Table 1. World Health Organisation European Organisation for Research and Treatment of Cancer (WHO EORTC) classification Table 2. Revised TNMB classification of mycosis fungoides (MF) and Sézary syndrome (SS) Cutaneous T-cell lymphoma (CTCL) Mycosis fungoides (MF) Variants of MF Folliculotropic MF Pagetoid reticulosis Granulomatous slack skin Sézary syndrome (SS) Primary cutaneous CD30-positive lymphoproliferative disorders Primary cutaneous anaplastic large-cell lymphoma Lymphomatoid papulosis Subcutaneous panniculitis-like T-cell lymphoma Extranodal natural killer (NK)/T-cell lymphoma, nasal-type Primary cutaneous peripheral T-cell lymphoma-not otherwise specified Aggressive epidermotropic CD8+ CTCL a Cutaneous γ/δ T-cell lymphoma a CD4+ small/medium-sized pleomorphic CTCL a Cutaneous B-cell lymphoma (CBCL) Primary cutaneous marginal zone B-cell lymphoma Primary cutaneous follicle centre lymphoma Primary cutaneous diffuse large B-cell lymphoma, leg type a Provisional entities. Republished with permission of the American Society of Hematology, from Willemze R, Jaffe ES, Burg G et al., WHO/EORTC classification for cutaneous lymphomas Blood 2005; 105: ; permission conveyed through Copyright Clearance Center, Inc. therapy The choice of treatment depends on the type of PCL and the stage of disease. Due to their heterogeneity and rarity, controlled clinical trials in PCLs are almost non-existent, with a few exceptions mainly concerning recently marketed drugs. Recommendations are therefore largely based on (retrospective) cohort studies and expert opinions discussed during consensus meetings of the EORTC Cutaneous Lymphoma Group, the International Society for Cutaneous Lymphomas (ISCL), the United States Cutaneous Lymphoma Consortium (USCLC) and the International Lymphoma Radiation Oncology Group. Consensus recommendations for clinical end points and response criteria in MF/SS and in PCLs other than MF/SS have recently been published (Olsen EA, Willemze R, Wood GS et al. Clinical endpoints and response criteria in primary cutaneous lymphomas other than mycosis fungoides and Sézary syndrome: a Consensus Statement of the International Society for Cutaneous Lymphomas (ISCL), the United States Cutaneous Lymphoma Consortium (USCLC) and the Cutaneous Lymphoma Task Force of the European Organization for the Research and Treatment of Cancer (EORTC). Blood. In preparation.) [8]. mycosis fungoides and variants Since early aggressive chemotherapy is associated with considerable side-effects but does not improve survival, a stageadapted conservative therapeutic approach is recommended for T (skin) T 1 Limited patch/plaque (involving <10% of total skin surface) T 2 Generalised patch/plaque (involving 10% of total skin surface) T 3 Tumour(s) Erythroderma T 4 N (lymph node) N 0 No clinically abnormal peripheral lymph nodes N 1 Clinically abnormal peripheral lymph nodes; histologically uninvolved N 2 Clinically abnormal peripheral lymph nodes; histologically involved (nodal architecture uneffaced) N 3 Clinically abnormal peripheral lymph nodes; histologically involved (nodal architecture (partially) effaced) Nx Clinically abnormal peripheral lymph nodes; no histological confirmation M (viscera) M 0 No visceral involvement Visceral involvement M 1 B (blood) B 0 No circulating atypical (Sézary) cells (or <5% of lymphocytes) B 1 Low blood tumour burden ( 5% of lymphocytes are Sézary cells, but not B2) B 2 High blood tumour burden ( 1000/µl Sézary cells and positive clone) Republished with permission of American Society of Hematology, from Olsen E, Vonderheid E, Pimpinelli N et al., Revisions to the staging and classification of mycosis fungoides and Sézary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the Cutaneous Lymphoma Task Force of the European Organization of Research and Treatment of Cancer (EORTC), Blood 2007; 110: ; permission conveyed through Copyright Clearance Center, Inc. Table 3. Revised clinical staging system for mycosis fungoides (MF) and Sézary syndrome (SS) Clinical stage IA T 1 N 0 M 0 B 0-1 IB T 2 N 0 M 0 B 0-1 IIA T 1 2 N 1-2 M 0 B 0-1 IIB T 3 N 0-2 M 0 B 0-1 III T 4 N 0-2 M 0 B 0-1 IVA 1 T 1-4 N 0-2 M 0 B 2 IVA 2 T 1-4 N 3 M 0 B 0-2 IVB T 1-4 N 0-3 M 1 B 0-2 Republished with permission of American Society of Hematology, from Olsen E, Vonderheid E, Pimpinelli N et al., Revisions to the staging and classification of mycosis fungoides and Sézary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the Cutaneous Lymphoma Task Force of the European Organization of Research and Treatment of Cancer (EORTC), Blood 2007; 110: ; permission conveyed through Copyright Clearance Center, Inc. vi150 Willemze et al. Volume 24 Supplement 6 October 2013
3 Annals of Oncology MF and its variants [9 12]. Patients with only patches and/or plaques covering <10% (stage IA) or 10% of the skin surface (stage IB) should be treated with skin-directed therapies, including topical steroids, psoralens + ultraviolet A (PUVA), narrow-band ultraviolet B (UVB) and topical cytostatic agents, such as mechlorethamine or carmustine (BCNU). Narrow-band UVB should only be used in patients with patches or very thin plaques. Topical steroids can be recommended as monotherapy for patches/flat plaques stage IA disease. In stage IB, topical steroids can be used as adjuvant therapy for selected skin lesions. In patients developing one or few infiltrated plaques or tumours (stage IIB), additional local radiotherapy may suffice. Local radiotherapy can be curative in patients with early localised disease, particularly in patients with unilesional MF and pagetoid reticulosis. Local radiotherapy is most commonly administered with electrons (energy dependent on the thickness of the lesion), with bolus to achieve full skin dose, a margin of 2 cm and a total dose of Gy. For patients with more extensive infiltrated plaques and tumours or patients refractory to skin-directed therapies, a combination of PUVA and interferon alpha or PUVA and retinoids (including bexarotene), a combination of interferon alpha and retinoids or total skin electron beam irradiation can be considered. However, these treatments are not curative, although remission may last for several years. Total skin electron beam irradiation was often given to total doses of Gy, but recently lower doses (10 12 Gy) have been employed with the advantages of shorter duration of the treatment period, fewer side-effects and opportunity for re-treatment [13]. In patients with advanced and refractory disease, gemcitabine or liposomal doxorubicin may be considered [14, 15]. Other agents like the fusion toxin denileukin diftitox and histone deacetylase (HDAC) inhibitors, such as vorinostat and romidepsin, have been approved in the United States by the Food and Drug Administration (FDA) for patients with relapsed and refractory CTCL, but have not yet been registered for CTCL in Europe [16 18]. Multiagent chemotherapy is only indicated in patients with effaced lymph nodes or visceral involvement (stage IV), or in patients with widespread tumour stage MF which cannot be controlled with skin-targeted and immunomodulating therapies. Local palliation of cutaneous as well as extracutaneous lesions may be achieved with local radiotherapy to doses 8 Gy[19]. In relatively young patients with refractory, progressive MF or with SS, allogeneic stem cell transplantation may be considered. Durable responses have been reported, but experience is still limited, and the optimal conditioning regimen and the optimal timing for an allogeneic transplant are currently unknown [20]. Results with autologous stem cell transplantation in MF and SS have been disappointing. Sézary syndrome Being a systemic disease (i.e. leukaemia) by definition, systemic treatment is required. Skin-directed therapies like PUVA or potent topical steroids may be used as adjuvant therapy. Extracorporeal photopheresis (ECP), either alone or in combination with other treatment modalities such as interferon alpha, retinoids, total skin electron beam and PUVA, has been clinical practice guidelines suggested as the treatment of choice in SS and erythrodermic MF [10 12]. Overall response rates range from 30% to 80% with complete response rates ranging from 14% to 25%, depending on the ECP regimen and the type of combination used. However, the suggested superiority of ECP over the traditional low-dose chemotherapy regimens has not yet been substantiated by randomised, controlled trials [21]. Prolonged treatment with a combination of low-dose chlorambucil and prednisone is often effective in controlling the disease, but is unlikely to yield complete responses. Low-dose methotrexate, bexarotene, denileukin diftitox, alemtuzumab (low-dose) and multiagent chemotherapy have been recommended as second-line treatment of SS [10 12, 22]. It should be emphasised that comparison of treatment results in the different studies is almost impossible due to differences in diagnostic criteria used for SS. primary cutaneous CD30-positive lymphoproliferative disorders (LPDs) The group of primary cutaneous CD30-positive LPDs includes primary cutaneous anaplastic large lymphoma (C-ALCL) and LyP, which form a spectrum of disease. Both C-ALCL and LyP have an excellent prognosis, with a 10-year survival of 90% and almost 100%, respectively [23, 24]. Patients with C-ALCL generally present with solitary or localised (ulcerating) tumours or nodules and should be treated with radiotherapy or surgical excision. Patients with C-ALCL presenting with multifocal skin lesions can be best treated with low-dose methotrexate, as in LyP, or radiotherapy in case of only a few lesions. Radiotherapy is commonly administered with electrons, with bolus, a margin of 2 cm and a total dose of 40 Gy [25]. This dose is effective and well-tolerated. Lower doses may achieve the same result, but data have not been published. In patients with multiple lesions, lower doses of radiation may be used for palliation. In cases not responsive to these treatments, systemic retinoids including bexarotene or interferon alpha can be used [24]. Recent preliminary studies report high response rates of brentuximab vedotin (anti-cd30 monoclonal antibody coupled to the antitubulin agent monomethyl auristatin E) in patients with C- ALCL as well as patients with MF expressing CD30, but controlled clinical trials have just started [26, 27]. Multiagent chemotherapy is only indicated in patients presenting with or developing extracutaneous disease and in rare patients with rapidly progressive skin disease. subcutaneous panniculitis-like T-cell lymphoma (SPTCL) The term SPTCL is only used for cases with an α/β T-cell phenotype, which have a favourable prognosis, particularly if not associated with a haemophagocytic syndrome (HPS), which is frequently an extremely aggressive clinical syndrome requiring immediate intervention. One study reported 5-year overall survival rates of 91% and 46% in SPTCL patients without and with an HPS, respectively [28]. In SPTCL without associated HPS, systemic steroids or other immunosuppressive agents should be considered first, whereas in cases of solitary or localised skin lesions, radiotherapy with electrons is advised. Volume 24 Supplement 6 October 2013 doi: /annonc/mdt242 vi151
4 Annals of Oncology Table 4. Recommendations for the initial management of CBCL Extent First-line therapy Alternative therapies PCMZL Solitary/localised Local radiotherapy Excision (Antibiotics) a Multifocal Wait and see Local radiotherapy Chlorambucil b Rituximab i.v. (Antibiotics) a IFN alpha i.l. Rituximab i.l. Intralesional steroids IFN alpha i.l. Rituximab i.l. Topical or intralesional steroids PCFCL Solitary/localised Local radiotherapy Excision IFN alpha i.l. Rituximab i.l. Multifocal Wait and see Local radiotherapy Rituximab i.v. R-CVP/CHOP c PCLBCL, LT Solitary/localised R-CHOP ± IFRT Local radiotherapy Rituximab i.v. Multifocal R-CHOP Rituximab i.v. a In case of evidence for Borrelia burgdorferi infection, b or other single or combination regimens appropriate for low-grade B-cell lymphomas, c in exceptional cases or for patients developing extracutaneous disease i.l. intralesional; i.v.: intravenous; IFRT: involved field radiotherapy. Republished with permission of American Society of Hematology, from Senff NJ, Noordijk EM, Kim YH et al., European Organization for Research and Treatment of Cancer and International Society for Cutaneous Lymphoma consensus recommendations for the management of cutaneous B-cell lymphomas, Blood 2008; 112: ; permission conveyed through Copyright Clearance Center, Inc. Little information on radiation dose is available, but a dose of 40 Gy has been used. Bexarotene may be also effective in SPTCL [29]. Multiagent chemotherapy is required only in cases with progressive disease not responding to immunosuppressive therapy or in cases with HPS. more advanced disease, these lymphomas show an aggressive clinical behaviour and are often resistant to chemotherapy. Recently, an intensive chemotherapy regimen including L-asparaginase (the SMILE regimen) was shown to be effective [31]. extranodal natural killer (NK)/T-cell lymphoma, nasal type Extranodal NK/T-cell lymphoma, nasal type is a rare, nearly always Epstein-Barr virus-positive lymphoma, which is more common in Asia and Central and South America. The skin is the second most common site of involvement after the nasal cavity/nasopharynx. Patients generally present with multiple (ulcerating) plaques and tumours, or in the case of nasal NK/T-cell lymphoma with a midfacial destructive tumour. Skin involvement may be a primary or secondary manifestation of the disease. One study reported a median survival of 27 months for patients presenting with only skin lesions, compared with 5 months for patients presenting with cutaneous and extracutaneous diseases [30]. Since both groups have an aggressive clinical behaviour, distinction between primary and secondary cutaneous involvement seems not to be useful for this category. In patients with stage I disease, radiotherapy is the first choice of treatment. Recommended radiation doses are higher than for other lymphomas, with 50 Gy to the initial lesion and a boost of 5 10 Gy to residual disease. In the case of primary cutaneous peripheral T-cell lymphoma-not otherwise specified (PTCL-NOS) Within the group of primary cutaneous PTCL-NOS, three somewhat better defined subgroups have been included as provisional entities (see Table 1). However, most of the cases have in common a generally aggressive clinical course and poor survival, and should therefore be treated as systemic PTCL-NOS with multiagent chemotherapy. Since the results are often disappointing, early allogeneic stem cell transplantation may be considered. The only exception is the group of CD4-positive small-medium pleomorphic CTCL. These patients often present with a solitary tumour, most commonly on the head, should be treated with local radiotherapy or excision, and have an excellent prognosis. cutaneous B-cell lymphoma In the WHO EORTC classification, three main types of CBCL are distinguished: primary cutaneous marginal zone lymphoma vi152 Willemze et al. Volume 24 Supplement 6 October 2013
5 Annals of Oncology Table 5. Levels of evidence and grades of recommendation (adapted from the Infectious Diseases Society of America-United States Public Health Service Grading System a ) clinical practice guidelines (histology, blood examination, imaging, etc.) should only be carried out if required. Levels of evidence I Evidence from at least one large randomised, controlled trial of good methodological quality (low potential for bias) or meta-analyses of well-conducted, randomised trials without heterogeneity II Small randomised trials or large randomised trials with a suspicion of bias (lower methodological quality) or meta-analyses of such trials or of trials with demonstrated heterogeneity III Prospective cohort studies IV Retrospective cohort studies or case control studies V Studies without control group, case reports, experts opinions Grades of recommendation A Strong evidence for efficacy with a substantial clinical benefit, strongly recommended B Strong or moderate evidence for efficacy but with a limited clinical benefit, generally recommended C Insufficient evidence for efficacy or benefit does not outweigh the risk or the disadvantages (adverse events, costs,...), optional D Moderate evidence against efficacy or for adverse outcome, generally not recommended E Strong evidence against efficacy or for adverse outcome, never recommended a Dykewicz CA. Summary of the guidelines for preventing opportunistic infections among hematopoietic stem cell transplant recipients. Clin Infect Dis 2001; 33: By permission of the Infectious Diseases Society of America. (PCMZL), PCFCL and primary cutaneous diffuse large B-cell lymphoma, leg type (PCLBCL-LT). PCMZL and PCFCL are indolent types of CBCL with a disease-related 10-year survival rate of 90%, while PCLBCL-LT has a more unfavourable prognosis (disease-related 5-year survival, 50%). EORTC/ISCL consensus recommendations for the management of these three types of CBCL have been formulated and are summarised in Table 4 [32]. Recommended radiation doses for localised PCMZL and PCFCL are Gy, whereas for palliative treatment of multifocal disease, low-dose radiation (4 Gy) is often sufficient [19]. For the more aggressive PCLBCL-LT, a radiation dose of 40 Gy is recommended. personalised medicine In this disease setting, more research is needed to identify molecular markers which could lead to advances in personalised medicine. follow-up The frequency of follow-up visits depends on the type of PCL and the stage of disease. It may vary from every 6 or 12 months in patients with indolent types of PCL and stable disease or patients in complete remission to every 4 6 weeks in patients with active or progressive disease. Follow-up visits should focus on history and physical examination, and additional testing note According to the levels of evidence and grades of recommendation shown in Table 5, the levels of evidence in these guidelines are mostly level IV and the recommendations are grade B. This is due to the heterogeneity and rarity of the diseases. conflict of interest Dr Ladetto has reported speaker s bureau from Celgene, Janssen-Cilag, Roche, Bayer, Amgen, Mundipharma; research contracts from Celgene, Pfizer, Mundipharma, Roche; funds received from Amgen, Roche, Italfarmaco. The other authors have declared no potential conflicts of interest. references 1. Willemze R, Jaffe ES, Burg G et al. WHO EORTC classification for cutaneous lymphomas. Blood 2005; 105: Swerdlow SH, Campo E, Harris NL et al. WHO Classification of Tumours Haematopoietic and Lymphoid Tissues, 4th Edition, Geneva: WHO Press, Tan SH, Sim CS, Ong BH. Cutaneous lymphomas other than mycosis fungoides in Singapore: a clinicopathological analysis using recent classification systems. Br J Dermatol 2003; 149: Park JH, Shin HT, Lee DY et al. World Health Organization European Organization for Research and Treatment of Cancer classification of cutaneous lymphoma in Korea: a retrospective study at a single tertiary institution. J Am Acad Dermatol 2012; 67: Olsen EA, Vonderheid E, Pimpinelli N et al. Revisions to the staging and classification of mycosis fungoides and Sézary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the Cutaneous Lymphoma Task Force of the European Organization of Research and Treatment of Cancer (EORTC). Blood 2007; 110: Kim YH, Willemze R, Pimpinelli N et al. TNM classification system for primary cutaneous lymphomas other than mycosis fungoides and Sézary syndrome: a proposal of the International Society for Cutaneous Lymphomas (ISCL) and the Cutaneous Lymphoma Task Force of the European Organization of Research and Treatment of Cancer (EORTC). Blood 2007; 110: Senff NJ, Kluin-Nelemans HC, Willemze R. Results of bone marrow examination in 275 patients with histological features that suggest an indolent type of cutaneous B-cell lymphoma. Br J Haematol 2008; 142: Olsen EA, Whittaker S, Kim YH et al. Clinical endpoints and response criteria in mycosis fungoides and Sézary syndrome: a consensus statement of the International Society for Cutaneous Lymphomas (ISCL), the United States Cutaneous Lymphoma Consortium (USCLC) and the Cutaneous Lymphoma Task Force of the European Organization for Research and Treatment of Cancer (EORTC). J Clin Oncol 2011; 29: Kaye FJ, Bunn PA Jr., Steinberg SM et al. A randomized trial comparing combination electron-beam radiation and chemotherapy with topical therapy in the initial treatment of mycosis fungoides. N Eng J Med 1989; 321: Whittaker SJ, Marsden JR, Spittle M et al. Joint British Association of Dermatologists and UK Cutaneous Lymphoma Group guidelines for the management of primary cutaneous T-cell lymphomas. Br J Dermatol 2003; 149: Trautinger F, Knobler R, Willemze R et al. EORTC consensus recommendations for the treatment of mycosis fungoides/sézary syndrome. Eur J Cancer 2006; 42: Volume 24 Supplement 6 October 2013 doi: /annonc/mdt242 vi153
6 Annals of Oncology 12. Prince HM, Whittaker S, Hoppe RT. How I treat mycosis fungoides and Sézary syndrome. Blood 2009; 114: Kamstrup MR, Lindahl LM, Gniadecki R et al. Low-dose total skin electron beam therapy as a debulking agent for cutaneous T-cell lymphoma: an open-label prospective phase II study. Br J Dermatol 2012; 166: Marchi E, Alinari L, Tani M et al. Gemcitabine as frontline treatment for cutaneous T-cell lymphoma: phase II study of 32 patients. Cancer 2005; 104: Dummer R, Quaglino P, Becker JC et al. Prospective international multicenter phase II trial of intravenous pegylated liposomal doxorubicin monochemotherapy in patients with stage IIB, IVA, or IVB advanced mycosis fungoides: final results from EORTC J Clin Oncol 2012; 30: Prince HM, Duvic M, Martin A et al. Phase III placebo-controlled trial of denileukin diftitox for patients with cutaneous T-cell lymphoma. J Clin Oncol 2010; 28: Olsen EA, Kim YH, Kuzel TM et al. Phase IIb multicenter trial of vorinostat in patients with persistent, progressive, or treatment refractory cutaneous T-cell lymphoma. J Clin Oncol 2007; 25: Whittaker SJ, Demierre MF, Kim EJ et al. Final results from a multicenter, international, pivotal study of romidepsin in refractory cutaneous T-cell lymphoma. J Clin Oncol 2010; 28: Neelis KJ, Schimmel EC, Vermeer MH et al. Low-dose palliative radiotherapy for cutaneous B- and T-cell lymphomas. Int J Radiat Oncol Biol Phys 2009; 74: Duarte RF, Schmitz N, Servitje O, Sureda A. Haematopoietic stem cell transplantation for patients with primary cutaneous T-cell lymphoma. Bone Marrow Transplant 2008; 41: Russell-Jones R. Extracorporeal photopheresis in cutaneous T-cell lymphoma. Inconsistent data underline the need for randomized studies. Br J Dermatol 2000; 142: Bernengo MG, Quaglino P, Comessatti A et al. Low-dose intermittent alemtuzumab in the treatment of Sézary syndrome: clinical and immunologic findings in 14 patients. Haematologica 2007; 92: Bekkenk MW, Geelen FA, van Voorst Vader PC et al. Primary and secondary cutaneous CD30(+) lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis and treatment. Blood 2000; 95: Kempf W, Pfaltz K, Vermeer MH et al. EORTC, ISCL, USCLC consensus recommendations for the treatment of primary cutaneous CD30-positive lymphoproliferative disorders: lymphomatoid papulosis and primary cutaneous anaplastic large-cell lymphoma. Blood 2011; 118: Yu JB, McNiff JM, Lund MW, Wilson LD. Treatment of primary cutaneous CD30+ anaplastic large-cell lymphoma with radiation therapy. Int J Radiat Oncol Biol Phys 2008; 70: Pro B, Advani R, Brice P et al. Brentuximab vedotin (SGN-35) in patients with relapsed or refractory systemic anaplastic large-cell lymphoma: results of a phase II study. J Clin Oncol 2012; 30: Krathen M, Sundram U, Bashey S et al. Brentuximab vedotin demonstrates significant clinical activity in relapsed or refractory mycosis fungoides with variable CD30 expression. Blood ASH Annual Meeting Abstracts 2012; 120: Willemze R, Jansen PM, Cerroni L et al. Subcutaneous panniculitis-like T-cell lymphoma: definition, classification and prognostic factors. An EORTC Cutaneous Lymphoma Group study of 83 cases. Blood 2008; 111: Mehta N, Wayne AS, Kim YH et al. Bexarotene is active against subcutaneous panniculitis-like T-cell lymphoma in adult and pediatric populations. Clin Lymphoma Myeloma Leuk 2012; 12: Bekkenk MW, Jansen PM, Meijer CJ et al. CD56+ hematological neoplasms presenting in the skin: a retrospective analysis of 23 new cases and 130 cases from the literature. Ann Oncol 2004; 15: Yamaguchi M, Kwong YL, Kim WS et al. Phase II study of SMILE chemotherapy for newly diagnosed stage IV, relapsed, or refractory extranodal natural killer (NK)/T-cell lymphoma, nasal type: the NK-cell Tumor Study Group study. J Clin Oncol 2011; 29: Senff NJ, Noordijk EM, Kim YH et al. European Organization for Research and Treatment of Cancer and International Society for Cutaneous Lymphoma consensus recommendations for the management of cutaneous B-cell lymphomas. Blood 2008; 112: vi154 Willemze et al. Volume 24 Supplement 6 October 2013
Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up
 Annals of Oncology 29 (Supplement 4): iv30 iv40, 2018 doi:10.1093/annonc/mdy133 CLINICAL PRACTICE GUIDELINES Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and
Annals of Oncology 29 (Supplement 4): iv30 iv40, 2018 doi:10.1093/annonc/mdy133 CLINICAL PRACTICE GUIDELINES Primary cutaneous lymphomas: ESMO Clinical Practice Guidelines for diagnosis, treatment and
clinical recommendations
 19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
19 (Supplement 2): ii72 ii76, 2008 doi:10.1093/annonc/mdn095 Primary cutaneous lymphoma: ESMO Clinical Recommendations for diagnosis, treatment and follow-up R. Dummer 1 & M. Dreyling 2 On behalf of the
Therapeutic Management of Early Cutaneous Mycosis Fungoides
 Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Therapeutic Management of Early Cutaneous Mycosis Fungoides L Frank Glass, MD Cutaneous Lymphoma Programs H Lee Moffitt Cancer Center and Research Institute George Washington University Dermatology and
Overview of Cutaneous Lymphomas: Diagnosis and Staging. Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology
 Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Overview of Cutaneous Lymphomas: Diagnosis and Staging Lauren C. Pinter-Brown MD, FACP Health Sciences Professor of Medicine and Dermatology Definition of Lymphoma A cancer or malignancy that comes from
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology
 Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Michi Shinohara MD Associate Professor University of Washington/Seattle Cancer Care Alliance Dermatology, Dermatopathology Agenda Overview of cutaneous T and B- cell lymphomas Diagnosis, Staging, Prognosis
Index. derm.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Acitretin and cutaneous T-cell lymphomas, 716 719, 722, 725 ADCC. See Antibody-dependent cell-mediated cytotoxicity. Adjunctive therapies and
Note: Page numbers of article titles are in boldface type. A Acitretin and cutaneous T-cell lymphomas, 716 719, 722, 725 ADCC. See Antibody-dependent cell-mediated cytotoxicity. Adjunctive therapies and
Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11
 Clinical Policy: (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11 Last Review Date: 12/16 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information.
Clinical Policy: (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10/11 Last Review Date: 12/16 Revision Log See Important Reminder at the end of this policy for important regulatory and legal information.
Disclosures. Advisory Board. Consultant. Investigator. MiRagen, Actelion, Celgene, Therakos. Mindera
 Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
Cutaneous Lymphomas Christiane Querfeld, MD, PhD Director, Cutaneous Lymphoma Program City of Hope ~ How the Experts Treat Hematologic Malignancies Symposium March 10 13, 2017 Disclosures Advisory Board
CUTANEOUS T-CELL LYMPHOMA: SYSTEMIC THERAPY. Anne W. Beaven, MD Associate Professor Director, Lymphoma Program University of North Carolina
 CUTANEOUS T-CELL LYMPHOMA: SYSTEMIC THERAPY Anne W. Beaven, MD Associate Professor Director, Lymphoma Program University of North Carolina CTCL Extranodal Nodal Leukemia Mycosis fungoides Sezary Syndrome
CUTANEOUS T-CELL LYMPHOMA: SYSTEMIC THERAPY Anne W. Beaven, MD Associate Professor Director, Lymphoma Program University of North Carolina CTCL Extranodal Nodal Leukemia Mycosis fungoides Sezary Syndrome
Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas
 Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
Review Article DOI: 10.1159/000470845 Received: February 06, 2017 Accepted: March 13, 2017 Published online: April 6, 2017 Renaissance of Low-Dose Radiotherapy Concepts for Cutaneous Lymphomas Bouthaina
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10.01.18 Last Review Date: 07.13.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end
Clinical Policy: Vorinostat (Zolinza) Reference Number: CP.PHAR.83 Effective Date: 10.01.18 Last Review Date: 07.13.18 Line of Business: Oregon Health Plan Revision Log See Important Reminder at the end
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
Cover Page The handle http://hdl.handle.net/1887/2010 holds various files of this Leiden University dissertation. Author: Benner, Marchina Frederika Title: Cutaneous CD30-positive lymphoproliferations
See Important Reminder at the end of this policy for important regulatory and legal information.
 Clinical Policy: (Istodax) Reference Number: CP.PHAR.314 Effective Date: 01.01.17 Last Review Date: 11.18 Line of Business: Medicaid, HIM-Medical Benefit Coding Implications Revision Log See Important
Clinical Policy: (Istodax) Reference Number: CP.PHAR.314 Effective Date: 01.01.17 Last Review Date: 11.18 Line of Business: Medicaid, HIM-Medical Benefit Coding Implications Revision Log See Important
CUTANEOUS T-CELL LYMPHOMA PROFORMA
 STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
STATE OF KUWAIT MINISTRY OF HEALTH AS AD ALHAMAD DERMATOLOGY CENTER ALSABAH HOSPITAL دولة الكویت وزارة الصحة مرآز أسعد الحمد للا مراض الجلدیة مستشفى الصباح بسم االله الرحمن الرحيم CUTANEOUS TCELL LYMPHOMA
Guidelines for the management of cutaneous lymphomas (2011): A consensus statement by the Japanese Skin Cancer Society Lymphoma Study Group
 doi: 10.1111/j.1346-8138.2012.01639.x Journal of Dermatology 2013; 40: 2 14 GUIDELINE Guidelines for the management of cutaneous lymphomas (2011): A consensus statement by the Japanese Skin Cancer Society
doi: 10.1111/j.1346-8138.2012.01639.x Journal of Dermatology 2013; 40: 2 14 GUIDELINE Guidelines for the management of cutaneous lymphomas (2011): A consensus statement by the Japanese Skin Cancer Society
Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified
 NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
NIHR Innovation Observatory Evidence Briefing: May 2017 Synthetic hypericin (SGX301; VIMRxyn) for cutaneous T cell lymphoma, unspecified NIHRIO (HSRIC) ID: 10761 NICE ID: 8375 LAY SUMMARY Cutaneous T cell
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD
 Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
Classification of Cutaneous T cell Lymphomas (CTCLs) Hernani Cualing, MD Pathology and Cell Biology, USF IFLOW, Inc. CTCL, MF, and Sézary syndrome In 1806, mycosis fungoides (MF) was first described 1
UKCLG Guidelines for Primary Cutaneous Lymphomas
 UKCLG Guidelines for Primary Cutaneous Lymphomas Sean Whi:aker Di Gilson Fiona Child Julia Scarisbrick Tim Illidge Eileen Parry Katy Rezvani Claire Dearden and Stephen Morris Diagnosis, staging, prognosis
UKCLG Guidelines for Primary Cutaneous Lymphomas Sean Whi:aker Di Gilson Fiona Child Julia Scarisbrick Tim Illidge Eileen Parry Katy Rezvani Claire Dearden and Stephen Morris Diagnosis, staging, prognosis
Sézary syndrome. Diagnosis and staging
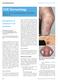 CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
CME DERMATOLOGY Clinical Medicine 2012, Vol 12, No 2: 160 4 Edited by Clive B Archer, consultant dermatologist and lead for Medical Education, St John s Institute of Dermatology, Guy s and St Thomas NHS
ISPUB.COM. Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose Methotrexate. S Parker INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Primary Cutaneous Anaplastic Large Cell Lymphoma Long-term Management with Low Dose S Parker Citation S Parker.. The Internet Journal of
Forum 115 Management Issues in Cutaneous Lymphomas. Management of Transformed Mycosis Fungoides
 Forum 115 Management Issues in Cutaneous Lymphomas Management of Transformed Mycosis Fungoides Madeleine Duvic, MD Deputy Chairman -Department of Dermatology Blanche Bender Professor of Cancer Research
Forum 115 Management Issues in Cutaneous Lymphomas Management of Transformed Mycosis Fungoides Madeleine Duvic, MD Deputy Chairman -Department of Dermatology Blanche Bender Professor of Cancer Research
ISPUB.COM. M Duvic, E Olsen PURPOSE OF REVISION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 International Society of Cutaneous Lymphoma (ISCL) and the European Organization of Research and Treatment of Cancer (EORTC) revisions to
Changing the landscape of treatment in Peripheral T-cell Lymphoma
 Changing the landscape of treatment in Peripheral T-cell Lymphoma Luis Fayad Associate Professor MD Anderson Cancer Center Department of Lymphoma and Myeloma 1 6 What is peripheral 2008 WHO CLASSIFICATION
Changing the landscape of treatment in Peripheral T-cell Lymphoma Luis Fayad Associate Professor MD Anderson Cancer Center Department of Lymphoma and Myeloma 1 6 What is peripheral 2008 WHO CLASSIFICATION
Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center
 Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center Madeleine Duvic, MD Professor and Deputy Chairman Blanche Bender Professor in Cancer Research Departments
Allogeneic Stem Cell Transplantation for Cutaneous T-cell Lymphoma: Updated results from a single center Madeleine Duvic, MD Professor and Deputy Chairman Blanche Bender Professor in Cancer Research Departments
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary cutaneous large cell lymphoma CD30+: a case-based review
 Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Case-based review Primary cutaneous large cell lymphoma CD30+: a case-based review Anna Campanati 1 Katia Giuliodori 1 Emanuela Martina 1 Luca Conocchiari 1 Giulia Ganzetti 1 Gaia Goteri 2 Annamaria Offidani
Sézary syndrome presenting with leonine facies ajd_560
 285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
285..288 Australasian Journal of Dermatology (2009) 50, 285 288 doi: 10.1111/j.1440-0960.2009.00560.x CASE REPORT Sézary syndrome presenting with leonine facies ajd_560 Shano Nassem, 1 Rajesh Kashyap,
SH/EAHP Workshop 2011 Los Angeles, California, USA
 SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
SH/EAHP Workshop 2011 Los Angeles, California, USA October 27-29, 2011 Session 3 Non-Mycosis Fungoides CTCL Patty Jansen & Rein Willemze Introduction Submitted: 101 cases + 7 cases group 1: 108 Deactivated
Cutaneous B-cell lymphomas: 2016 update on diagnosis, riskstratification,
 Page 1 of 11 Cutaneous B-cell lymphomas: 2016 update on diagnosis, riskstratification, and management Ryan A. Wilcox* Conflict of interest: Nothing to report *Correspondence to: Ryan Wilcox, MD, PhD Division
Page 1 of 11 Cutaneous B-cell lymphomas: 2016 update on diagnosis, riskstratification, and management Ryan A. Wilcox* Conflict of interest: Nothing to report *Correspondence to: Ryan Wilcox, MD, PhD Division
Cutaneous T-Cell Lymphoma
 PROVIDING THE LATEST INFORMATION FOR PATIENTS & CAREGIVERS Cutaneous T-Cell Lymphoma Revised 2019 Support for this publication provided by A six-word narrative about living with blood cancer from patients
PROVIDING THE LATEST INFORMATION FOR PATIENTS & CAREGIVERS Cutaneous T-Cell Lymphoma Revised 2019 Support for this publication provided by A six-word narrative about living with blood cancer from patients
Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated with Interferon-Alfa 2a
 Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Hindawi Case Reports in Dermatological Medicine Volume 2017, Article ID 3194738, 5 pages https://doi.org/10.1155/2017/3194738 Case Report A Severe Case of Lymphomatoid Papulosis Type E Successfully Treated
Cutaneous T cell lymphoma
 Cutaneous T cell lymphoma Belgian Hematology Society (BHS) course on indolent lymphomas 05-02-2015 Pascal Wolter, Department of General Medical Oncology, pascal.wolter@uzleuven.be Overview: I. Cutaneous
Cutaneous T cell lymphoma Belgian Hematology Society (BHS) course on indolent lymphomas 05-02-2015 Pascal Wolter, Department of General Medical Oncology, pascal.wolter@uzleuven.be Overview: I. Cutaneous
Clinical outcomes and prognostic factors in patients with mycosis fungoides who underwent radiation therapy in a single institution
 Original Article Radiat Oncol J 2018;36(2):153-162 https://doi.org/10.3857/roj.2017.00542 pissn 2234-1900 eissn 2234-3156 Clinical outcomes and prognostic factors in patients with mycosis fungoides who
Original Article Radiat Oncol J 2018;36(2):153-162 https://doi.org/10.3857/roj.2017.00542 pissn 2234-1900 eissn 2234-3156 Clinical outcomes and prognostic factors in patients with mycosis fungoides who
ISPUB.COM. Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis. E Kim PHYSICAL FINDINGS INTRODUCTION INITIAL PRESENTATION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Management of Co-existing Mycosis Fungoides and Lymphomatoid Papulosis E Kim Citation E Kim. Management of Co-existing Mycosis Fungoides
Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective Study
 International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
International Scholarly Research Notices, Article ID 820921, 5 pages http://dx.doi.org/10.1155/2014/820921 Research Article Characteristics of Primary Cutaneous T-Cell Lymphoma in Iran: A 10-Year Retrospective
Fig. 3.1 Fig Past history: She was previously healthy and not taking any medication.
 Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
Case 3 A 41-year-old Thai female from Bangkok Chief compliant: Erythematous patch at left thigh for 2 months Present illness: The patient presented with a 10- year history of erythematous patch on her
CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides
 Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
Case Report DOI: 10.6003/jtad.16102c5 CD30+ Lymphoproliferative Disorders Associated with Longstanding Mycosis Fungoides Esra Adışen, 1 MD, Özlem Erdem, 2 MD, Mehmet Ali Gürer, 1 MD Address: 1 Gazi University
1) Title: Cutaneous lymphoma in Japan: a nationwide study of 1,733 patients.
 1) Title: Cutaneous lymphoma in Japan: a nationwide study of 1,733 patients. 2) The short running title: Cutaneous lymphoma in Japan. 3) Toshihisa Hamada and Keiji Iwatsuki 4) Departments of Dermatology,
1) Title: Cutaneous lymphoma in Japan: a nationwide study of 1,733 patients. 2) The short running title: Cutaneous lymphoma in Japan. 3) Toshihisa Hamada and Keiji Iwatsuki 4) Departments of Dermatology,
BJD British Journal of Dermatology. 1.0 Purpose and scope. 2.0 Methodology GUIDELINES. Linked Editorial: Wang and Bagot. Br J Dermatol 2019; 180:
 GUIDELINES BJD British Journal of Dermatology British Association of Dermatologists and U.K. Cutaneous Lymphoma Group guidelines for the management of primary cutaneous lymphomas 2018 D. Gilson, 1 S.J.
GUIDELINES BJD British Journal of Dermatology British Association of Dermatologists and U.K. Cutaneous Lymphoma Group guidelines for the management of primary cutaneous lymphomas 2018 D. Gilson, 1 S.J.
NCCN Guidelines Version Primary Cutaneous CD30+ T-Cell Lymphoproliferative Disorders
 Primary Cutaneous CD30+ T-Cell Lymphoproliferative Disders OVERVIEW & DEFINITION Primary cutaneous CD30+ T-cell lymphoproliferative disders (LPDs) represent a spectrum that includes primary cutaneous anaplastic
Primary Cutaneous CD30+ T-Cell Lymphoproliferative Disders OVERVIEW & DEFINITION Primary cutaneous CD30+ T-cell lymphoproliferative disders (LPDs) represent a spectrum that includes primary cutaneous anaplastic
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week
 CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
CASE 15 Patient: A 41-year-old Thai female Chief Compliant: Generalized papulovesicular rash for 1 month Present Illness: She presented with a 1-week history of the generalized asymptomatic erythematous
Supportive Care in the Management of T-cell Lymphomas
 Supportive Care in the Management of T-cell Lymphomas Erin Kopp, ACNP-BC City of Hope Comprehensive Cancer Center NCCN.org For Clinicians NCCN.org/patients For Patients Objectives Discuss the role of supportive
Supportive Care in the Management of T-cell Lymphomas Erin Kopp, ACNP-BC City of Hope Comprehensive Cancer Center NCCN.org For Clinicians NCCN.org/patients For Patients Objectives Discuss the role of supportive
Clinical manifestations and pathogenesis of cutaneous lymphomas: current status and future directions
 review Clinical manifestations and pathogenesis of cutaneous lymphomas: current status and future directions Belen Rubio-Gonzalez, 1 Jasmine Zain, 2 Steven T. Rosen 2 and Christiane Querfeld 1,2,3 1 Department
review Clinical manifestations and pathogenesis of cutaneous lymphomas: current status and future directions Belen Rubio-Gonzalez, 1 Jasmine Zain, 2 Steven T. Rosen 2 and Christiane Querfeld 1,2,3 1 Department
Oncologic Dermatology and Surgery. Dra. Elena de las Heras
 Oncologic Dermatology and Surgery Dra. Elena de las Heras Review and Updates: Clinical oncology: Lymphomas PROspective Cutaneous Lymphoma International Prognostic Index (PROCLIPI) study Launched in 2015
Oncologic Dermatology and Surgery Dra. Elena de las Heras Review and Updates: Clinical oncology: Lymphomas PROspective Cutaneous Lymphoma International Prognostic Index (PROCLIPI) study Launched in 2015
Plenary paper. Introduction
 Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
Plenary paper Primary and secondary cutaneous CD30 lymphoproliferative disorders: a report from the Dutch Cutaneous Lymphoma Group on the long-term follow-up data of 219 patients and guidelines for diagnosis
NCCN Non Hodgkin s Lymphomas Guidelines V Update Meeting 06/14/12 and 06/15/12
 NCCN Non Hodgkin s Lymphomas Guidelines V.1.213 Update Meeting 6/14/12 and 6/15/12 Guidelines Page and Request Chronic Lymphocytic Leukemia/ Small Lymphocytic Lymphoma (CLL/SLL) Panel Discussion References
NCCN Non Hodgkin s Lymphomas Guidelines V.1.213 Update Meeting 6/14/12 and 6/15/12 Guidelines Page and Request Chronic Lymphocytic Leukemia/ Small Lymphocytic Lymphoma (CLL/SLL) Panel Discussion References
Recent diagnostic and therapeutic innovations of T-cell-lymphoma. Prof. Nossrat Firusian, Recklinghausen, Germany
 Recent diagnostic and therapeutic innovations of T-cell-lymphoma Prof. Nossrat Firusian, Recklinghausen, Germany NODAL Angioimmunoblastic T-cell Lymphoma Peripheral T-cell-Lymphoma Anaplastic Large-cell-Lymphoma
Recent diagnostic and therapeutic innovations of T-cell-lymphoma Prof. Nossrat Firusian, Recklinghausen, Germany NODAL Angioimmunoblastic T-cell Lymphoma Peripheral T-cell-Lymphoma Anaplastic Large-cell-Lymphoma
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin
 Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Cutaneous Lymphoid Proliferations: A Comprehensive Textbook of Lymphocytic Infiltrates of the Skin Magro, Cynthia M., MD ISBN-13: 9780471695981 Table of Contents Chapter One: Introduction to the Classification
Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases
 Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
Acta Derm Venereol 2016; 96: 669 673 CLINICAL REPORT Mycosis Fungoides: A Retrospective Study of 44 Swedish Cases Yvonne EKLUND 1, Annika ARONSSON 1, Artur SCHMIDTCHEN 1 and Thomas RELANDER 2 1 Section
2. Sézary syndrome (SS)
 Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
Go Back to the Top To Order, Visit the Purchasing Page for Details Clinical images are available in hardcopy only. Clinical images are available in Clinical images are available in d e f g h i j Fig..36-2
Lymphoma and Pseudolymphoma
 Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
Lymphoma and Pseudolymphoma Laura B. Pincus, MD Co-Director, Cutaneous Lymphoma Clinic Associate Professor Dermatology and Pathology University of California, San Francisco I HAVE NO RELEVANT RELATIONSHIPS
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
Sezary Syndrome(SS) and other malignancies. Hernani Cualing MD Hematopathologist IHCFLOW Lab
 Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
Sezary Syndrome(SS) and other malignancies Hernani Cualing MD Hematopathologist IHCFLOW Lab Disclosures IHCFLOW Laboratory:consultant and director NEOGENOMICS: contract consultant USF: contract reviewer
During past decades, because of the lack of knowledge
 Staging and Classification of Lymphoma Ping Lu, MD In 2004, new cases of non-hodgkin s in the United States were estimated at 54,370, representing 4% of all cancers and resulting 4% of all cancer deaths,
Staging and Classification of Lymphoma Ping Lu, MD In 2004, new cases of non-hodgkin s in the United States were estimated at 54,370, representing 4% of all cancers and resulting 4% of all cancer deaths,
Chapter 2. Journal of Clinical Oncology 2007; 25(12):1581-7
 Chapter 2. Reclassification of 300 primary cutaneous B-cell lymphomas according to the new WHO-EORTC classification for cutaneous lymphomas: comparison with previous classifications and identification
Chapter 2. Reclassification of 300 primary cutaneous B-cell lymphomas according to the new WHO-EORTC classification for cutaneous lymphomas: comparison with previous classifications and identification
Review Article. Cutaneous lymphoproliferative disorders. NJ Trendell-Smith
 Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
Hong Kong J. Dermatol. Venereol. (2010) 18, 190-201 Review Article Cutaneous lymphoproliferative disorders NJ Trendell-Smith Cutaneous lymphoproliferative disorders (CLD) include reactive lymphoid hyperplasias,
TRANSPARENCY COMMITTEE OPINION. 27 January 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 January 2010 TORISEL 25 mg/ml, concentrate for solution and diluent for solution for infusion Box containing 1
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 January 2010 TORISEL 25 mg/ml, concentrate for solution and diluent for solution for infusion Box containing 1
WHO Classification. B-cell chronic lymphocytic leukemia/small T-cell granular lymphocytic leukemia
 Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
Blood Malignancies-II Prof. Dr. Herman Hariman, a Ph.D, SpPK (KH). Prof. Dr. Adikoesoema Aman, SpPK (KH) Dept. of Clinical Pathology, School of Medicine, University of North Sumatra WHO classification
WORKUP. USEFUL IN SELECTED CASES: PET-CT scan Bone marrow biopsy
 DIAGNOSIS a WORKUP ESSENTIAL: Review of all slides with at least one paraffin lock representative of the tum should e done y a pathologist with expertise in the diagnosis of primary cutaneous B-cell lymphoma.
DIAGNOSIS a WORKUP ESSENTIAL: Review of all slides with at least one paraffin lock representative of the tum should e done y a pathologist with expertise in the diagnosis of primary cutaneous B-cell lymphoma.
ISPUB.COM. Advanced Stage CTCL, PTCL with Cutaneous Involvement. J Messenger, P Porcu INTRODUCTION INITIAL PRESENTATION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Advanced Stage CTCL, PTCL with Cutaneous Involvement J Messenger, P Porcu Citation J Messenger, P Porcu. Advanced Stage CTCL, PTCL with Cutaneous
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Advanced Stage CTCL, PTCL with Cutaneous Involvement J Messenger, P Porcu Citation J Messenger, P Porcu. Advanced Stage CTCL, PTCL with Cutaneous
Skin SSG (Anglia East & Anglia West)
 Guidelines for the Management of Primary Cutaneous T-Cell Lymphomas Skin SSG (Anglia East & Anglia West) Author: S J Whittaker, J R Marsden, M Spittle and R Russell Jones Approved by: Anglia Cancer Network
Guidelines for the Management of Primary Cutaneous T-Cell Lymphomas Skin SSG (Anglia East & Anglia West) Author: S J Whittaker, J R Marsden, M Spittle and R Russell Jones Approved by: Anglia Cancer Network
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/39089 holds various files of this Leiden University dissertation. Author: Cetinozman, F. Title: PD-1 Expression in primary cutaneous lymphoma Issue Date:
Cover Page The handle http://hdl.handle.net/1887/39089 holds various files of this Leiden University dissertation. Author: Cetinozman, F. Title: PD-1 Expression in primary cutaneous lymphoma Issue Date:
NIH Public Access Author Manuscript Bone Marrow Transplant. Author manuscript; available in PMC 2013 January 01.
 NIH Public Access Author Manuscript Published in final edited form as: Bone Marrow Transplant. 2012 July ; 47(7): 940 945. doi:10.1038/bmt.2011.201. Allogeneic hematopoietic stem cell transplantation for
NIH Public Access Author Manuscript Published in final edited form as: Bone Marrow Transplant. 2012 July ; 47(7): 940 945. doi:10.1038/bmt.2011.201. Allogeneic hematopoietic stem cell transplantation for
Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides
 Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Anatomic Pathology / Clusterin Expression in Mycosis Fungoides Clusterin Expression Correlates With Stage and Presence of Large Cells in Mycosis Fungoides Pranil Chandra, DO, 1 Jose A. Plaza, MD, 2,4 Zhuang
Extranodal natural killer/t-cell lymphoma with long-term survival and repeated relapses: does it indicate the presence of indolent subtype?
 VOLUME 47 ㆍ NUMBER 3 ㆍ September 2012 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE Extranodal natural killer/t-cell lymphoma with long-term survival and repeated relapses: does it indicate the presence
VOLUME 47 ㆍ NUMBER 3 ㆍ September 2012 THE KOREAN JOURNAL OF HEMATOLOGY ORIGINAL ARTICLE Extranodal natural killer/t-cell lymphoma with long-term survival and repeated relapses: does it indicate the presence
Mycosis Fungoides, then and now Have we travelled?
 USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
USCAP 103 rd Annual Meeting 2014 American Society of Dermatopathology Companion Meeting Mycosis Fungoides, then and now Have we travelled? Vijaya B. Reddy, MD, MBA Professor of Pathology Rush University
Outcomes of patients with peripheral T-cell lymphoma in first complete remission: data from three tertiary Asian cancer centers
 Tang et al. (2017) 7:653 DOI 10.1038/s41408-017-0030-y CORRESPONDENCE Outcomes of patients with peripheral T-cell lymphoma in first complete remission: data from three tertiary Asian cancer centers Open
Tang et al. (2017) 7:653 DOI 10.1038/s41408-017-0030-y CORRESPONDENCE Outcomes of patients with peripheral T-cell lymphoma in first complete remission: data from three tertiary Asian cancer centers Open
East Midlands Cancer Network Guidelines for diagnosis and management of mature T cell and NK cell lymphomas (excluding cutaneous T cell lymphoma)
 East Midlands Cancer Network Guidelines for diagnosis and management of mature T cell and NK cell lymphomas (excluding cutaneous T cell lymphoma) Written by: Dr Chris Fox with input from Dr Fiona Miall
East Midlands Cancer Network Guidelines for diagnosis and management of mature T cell and NK cell lymphomas (excluding cutaneous T cell lymphoma) Written by: Dr Chris Fox with input from Dr Fiona Miall
ISPUB.COM. Bexarotene in Tumor stage Mycosis Fungoides. R Talpur, M Duvic INITIAL PRESENTATION TREATMENT COURSE INTRODUCTION
 ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Bexarotene in Tumor stage Mycosis Fungoides R Talpur, M Duvic Citation R Talpur, M Duvic. Bexarotene in Tumor stage Mycosis Fungoides. The
ISPUB.COM The Internet Journal of Dermatology Volume 7 Number 3 Bexarotene in Tumor stage Mycosis Fungoides R Talpur, M Duvic Citation R Talpur, M Duvic. Bexarotene in Tumor stage Mycosis Fungoides. The
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Change Summary - Form 2018 (R3) 1 of 12
 Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Summary - Form 2018 (R3) 1 of 12 Form Question Number (r3) Type Description New Text Previous Text Today's date was removed 2018 N/A Today's Date Removed from Key Fields 2018 N/A HCT Type 2018 N/A Product
Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary Study
 Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Skin Cancer, Article ID 624143, 4 pages http://dx.doi.org/10.1155/2014/624143 Clinical Study The Influence of the Coexpression of CD4 and CD8 in Cutaneous Lesions on Prognosis of Mycosis Fungoides: A Preliminary
Peripheral T-cell lymphoma. Matt Ahearne Clinical Lecturer, Leicester
 Peripheral T-cell lymphoma Matt Ahearne Clinical Lecturer, Leicester PTCL Objectives To understand the natural history of PTCL To appreciate the importance of accurate diagnosis of PTCL including recent
Peripheral T-cell lymphoma Matt Ahearne Clinical Lecturer, Leicester PTCL Objectives To understand the natural history of PTCL To appreciate the importance of accurate diagnosis of PTCL including recent
TRANSPARENCY COMMITTEE OPINION. 8 November 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 8 November 2006 MABTHERA 100 mg, concentrate for solution for infusion (CIP 560 600-3) Pack of 2 MABTHERA 500 mg,
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 8 November 2006 MABTHERA 100 mg, concentrate for solution for infusion (CIP 560 600-3) Pack of 2 MABTHERA 500 mg,
Primary Cutaneous Large B-Cell Lymphoma, Leg Type, Localized on the Dorsum
 87 Primary Cutaneous Large B-Cell Lymphoma, Leg Type, Localized on the Dorsum A. Patrizi a B. Raone a E. Sabattini b C. Gurioli a A. Pileri Jr. a C. D Acunto a a Dermatology, Department of Internal Medicine,
87 Primary Cutaneous Large B-Cell Lymphoma, Leg Type, Localized on the Dorsum A. Patrizi a B. Raone a E. Sabattini b C. Gurioli a A. Pileri Jr. a C. D Acunto a a Dermatology, Department of Internal Medicine,
A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs
 Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Hong Kong J. Dermatol. Venereol. (2011) 19, 30-34 Case Report A middle-aged man with self-healing papulonecrotic lesions over the trunk and proximal limbs JC Chan, N Trendell-Smith, CK Yeung Lymphomatoid
Emerging Therapies for Cutaneous Malignancies. Genevieve Kelly AAD Highlights Meeting Thurs 15 th March 2018
 Emerging Therapies for Cutaneous Malignancies Genevieve Kelly AAD Highlights Meeting Thurs 15 th March 2018 Topics Basal Cell Carcinoma Squamous Cell Carcinoma Merkel Cell Carcinoma Cutaneous Lymphoma
Emerging Therapies for Cutaneous Malignancies Genevieve Kelly AAD Highlights Meeting Thurs 15 th March 2018 Topics Basal Cell Carcinoma Squamous Cell Carcinoma Merkel Cell Carcinoma Cutaneous Lymphoma
Poteligeo (mogamulizmuab-kpkc)
 Poteligeo (mogamulizmuab-kpkc) Policy Number: 5.02.556 Last Review: 1/2019 Origination: 1/2019 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Poteligeo
Poteligeo (mogamulizmuab-kpkc) Policy Number: 5.02.556 Last Review: 1/2019 Origination: 1/2019 Next Review: 1/2020 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Poteligeo
U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD
 U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD hurleyy@slu.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Actelion: Speaker Honoraria, Investigator Grants, Consultant
U006 Primary Cutaneous Lymphomas: Diagnosis, Staging and When to Refer M. Yadira Hurley, MD hurleyy@slu.edu DISCLOSURE OF RELATIONSHIPS WITH INDUSTRY Actelion: Speaker Honoraria, Investigator Grants, Consultant
Cluster of differentiation (CD) markers in erythrodermic patients: A case series study
 Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Original Article Cluster of differentiation (CD) markers in erythrodermic patients: A case series study Fariba Ghalamkarpour, MD Faranak Niknafs, MD Shima Younespour, PhD Skin Research Center, Shahid Beheshti
Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies
![Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies](/thumbs/90/104309591.jpg) Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies UNCONTROLLED WHEN PRINTED Note: NOSCAN Haematology MCN has approved the information contained within this document to guide
Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies UNCONTROLLED WHEN PRINTED Note: NOSCAN Haematology MCN has approved the information contained within this document to guide
Corporate Medical Policy
 Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
Corporate Medical Policy Extracorporeal Photopheresis File Name: Origination: Last CAP Review: Next CAP Review: Last Review: extracorporeal_photopheresis 9/2010 8/2017 8/2018 8/2017 Description of Procedure
A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature
 Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Original article A rare clinical presentation of non Hodgkin Lymphoma as multiple neurofibromas with review of literature Dr.C.R.Sirajunnisa Begum, Professor 1, Dr. Ira Bharadhwaj, Professor 1, Dr. Lavanya,
Introduction. Structure
 SOPs/Instructions for Authors and templates for standard ESMO Clinical Practice Guidelines (CPGs) and ESMO-MCBS Scores ESMO Guidelines Committee, October 2015, latest revision April 2018 Introduction The
SOPs/Instructions for Authors and templates for standard ESMO Clinical Practice Guidelines (CPGs) and ESMO-MCBS Scores ESMO Guidelines Committee, October 2015, latest revision April 2018 Introduction The
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Mycosis Fungoides Presentation in Emergency
 The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
The Open Emergency Medicine Journal, 2011, 4, 17-21 17 Mycosis Fungoides Presentation in Emergency Asaad Shujaa*,1 and M. Owais Suriya 2 Open Access Department of Emergency Medicine College of Medicine,
Development of Mogamulizumab, a defucosylated anti-ccr4 humanized monoclonal antibody
 New Drugs in Hematology Development of Mogamulizumab, a defucosylated anti-ccr4 humanized monoclonal antibody Michinori Ogura, MD, PhD Department of Hematology Tokai Central Hospital Bologna, Royal Hotel
New Drugs in Hematology Development of Mogamulizumab, a defucosylated anti-ccr4 humanized monoclonal antibody Michinori Ogura, MD, PhD Department of Hematology Tokai Central Hospital Bologna, Royal Hotel
Clinical Trial Outcomes
 l Recent clinical evidence for topical mechlorethamine in mycosis fungoides Mycosis fungoides (MF) is a rare, potentially life-threatening cutaneous T-cell lymphoma characterized by cutaneous homing of
l Recent clinical evidence for topical mechlorethamine in mycosis fungoides Mycosis fungoides (MF) is a rare, potentially life-threatening cutaneous T-cell lymphoma characterized by cutaneous homing of
A Unique Case of Nasal NK/T Cell Lymphoma with Frequent Remission and Relapse Showing Different Histological Features During 12 Years of Follow Up
 J Clin Exp Hematopathol Vol. 50, No. 1, May 2010 Case Study A Unique Case of Nasal NK/T Cell Lymphoma with Frequent Remission and Relapse Showing Different Histological Features During 12 Years of Follow
J Clin Exp Hematopathol Vol. 50, No. 1, May 2010 Case Study A Unique Case of Nasal NK/T Cell Lymphoma with Frequent Remission and Relapse Showing Different Histological Features During 12 Years of Follow
original articles introduction
 Annals of Oncology original articles Annals of Oncology 25: 1807 1812, 2014 doi:10.1093/annonc/mdu231 Published online 19 June 2014 Final results of a multicenter phase II study of the purine nucleoside
Annals of Oncology original articles Annals of Oncology 25: 1807 1812, 2014 doi:10.1093/annonc/mdu231 Published online 19 June 2014 Final results of a multicenter phase II study of the purine nucleoside
NK/T cell lymphoma Recent advances. Y.L Kwong University Department of Medicine Queen Mary Hospital
 NK/T cell lymphoma Recent advances Y.L Kwong University Department of Medicine Queen Mary Hospital Natural killer cell lymphomas NK cell lymphomas are mainly extranodal lymphomas Clinical classification
NK/T cell lymphoma Recent advances Y.L Kwong University Department of Medicine Queen Mary Hospital Natural killer cell lymphomas NK cell lymphomas are mainly extranodal lymphomas Clinical classification
CD30+ Cutaneous T Cell Lymphoma: Response to Rotational Total Skin Electron Irradiation
 CD30+ Cutaneous T Cell Lymphoma: Response to Rotational Total Skin Electron Irradiation Hasan H. Danish, Emory University Thatcher R. Heumann, Emory University Kyle Bradley, Emory University Jeffrey M.
CD30+ Cutaneous T Cell Lymphoma: Response to Rotational Total Skin Electron Irradiation Hasan H. Danish, Emory University Thatcher R. Heumann, Emory University Kyle Bradley, Emory University Jeffrey M.
NCCN Guidelines Version Mycosis Fungoides/Sezary Syndrome
 DIAGNOSIS ESSENTIAL: Biopsy of suspicious skin sites Dermatopathology review of slides USEFUL UNDER CERTAIN CIRCUMSTANCES: Immunohistochemical studies of skin biopsy a,b (CD2, CD3, CD4, CD5, CD7, CD8,
DIAGNOSIS ESSENTIAL: Biopsy of suspicious skin sites Dermatopathology review of slides USEFUL UNDER CERTAIN CIRCUMSTANCES: Immunohistochemical studies of skin biopsy a,b (CD2, CD3, CD4, CD5, CD7, CD8,
How I treat patients whose biopsies are reported descriptively Youn H Kim, MD
 How I treat patients whose biopsies are reported descriptively Youn H Kim, MD Director, Multidisciplinary Cutaneous Lymphoma Group Stanford Cancer institute & School of Medicine NCCN NHL Panel Member Disclosure
How I treat patients whose biopsies are reported descriptively Youn H Kim, MD Director, Multidisciplinary Cutaneous Lymphoma Group Stanford Cancer institute & School of Medicine NCCN NHL Panel Member Disclosure
Learn more about diffuse large B-cell lymphoma (DLBCL), the most common aggressive form of B-cell non-hodgkin s lymphoma 1
 Learn more about diffuse large B-cell lymphoma (DLBCL), the most common aggressive form of B-cell non-hodgkin s lymphoma 1 Expression of B-cell surface antigens drives several non-hodgkin s lymphomas (NHLs)
Learn more about diffuse large B-cell lymphoma (DLBCL), the most common aggressive form of B-cell non-hodgkin s lymphoma 1 Expression of B-cell surface antigens drives several non-hodgkin s lymphomas (NHLs)
Indolent Lymphomas. Dr. Melissa Toupin The Ottawa Hospital
 Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 28 March 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 28 March 2012 TARGRETIN 75 mg, soft capsule B/1 high-density polyethylene (HDPE) bottle of 100 capsules (CIP code:
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 28 March 2012 TARGRETIN 75 mg, soft capsule B/1 high-density polyethylene (HDPE) bottle of 100 capsules (CIP code:
Belinostat (Beleodaq) with CHOP for treatment of patients with peripheral T cell lymphoma, 1st line
 NIHR Innovation Observatory Evidence Briefing: September 2017 Belinostat (Beleodaq) with CHOP for treatment of patients with peripheral T cell lymphoma, 1st line NIHRIO (HSRIC) ID: 12674 NICE ID: 9532
NIHR Innovation Observatory Evidence Briefing: September 2017 Belinostat (Beleodaq) with CHOP for treatment of patients with peripheral T cell lymphoma, 1st line NIHRIO (HSRIC) ID: 12674 NICE ID: 9532
