South West Strategic Clinical Network Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services
|
|
|
- Earl Parsons
- 6 years ago
- Views:
Transcription
1 Meeting of the SWAG Network Colorectal Site Specific Group (SSG) 10:00 16:00, Wednesday, 22nd April 2015, South West House, Blackbrook Park Avenue, Taunton, TA1 2PX Chair: Mr Michael Williamson (MW) This meeting was sponsored by Merch Serono Notes (To be agreed at the next SSG meeting) Actions 1. Welcome and Apologies Please see the separate list of attendees and apologies uploaded on to the SWSCN website Representatives from Gloucestershire Hospitals were welcomed as new members of the group. Due to patient referrals going both to the Midlands and to the SWAG region from Gloucestershire Hospitals (Glos), it would be necessary for representatives from Glos to attend both the SWAG and Midlands SSG group meetings. 2. Review of last meeting notes As there were no amendments or comments following distribution of the notes from the meeting on the 24 th September 2014, the notes were accepted. 3. Clinical opinion on network issues 3.1 Network Update The cancer network is no longer called ASWCS. To reflect the addition of Gloucestershire Hospitals to the network it is now called Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. The SSG Support Manager, Helen Dunderdale (HD), and SSG Support Administrator, Samantha Larsen (SL), have now been in post for 8 months. Their posts will be funded for one year by the South West Strategic Clinical Network. Funding for the posts after this year will be provided by the acute Trusts, with the cost of the SSG service divided, based on Trust size (calculated from numbers of cancer treatments), plus the number of SSGs within the region in which each Trust would participate. This has been agreed by all Trusts for the next 5 years. Any operational issues that are identified within the SSG meetings will be escalated to the Cancer Operational Group, and any funding issues will be escalated to the commissioning groups via the South West Strategic Network Cancer Manager, Jonathan Miller. Commercial sponsorship will be sought to assist with funding venues and refreshments for SSG meetings.
2 Continuous Professional Development accreditation from the Royal College of Physicians will be applied for when the SSG meetings have educational content. HD has been nominated by the SSG Chairs as the NHS member of staff responsible for user representatives issues and information and will provide user representatives with information prior to the meetings, supply user involvement handbooks and opportunities to attend relevant workshops. Rowland Hackett is happy to continue as the user representative of the group. The SSG Support Manager will create drafts of the following SSG key documents by April 2015 for approval by the group by the end of June 2015: Constitutions Clinical Guidelines Work Plans The SSG support team have been granted access to add content to the South West Strategic Clinical Network website: Once notes and actions have been uploaded, the link will be ed to the group. Sections have also been added where it is possible to upload GP referral information, information for SSG members, and patient and public information. SSG members are to inform the SSG support team if they have any content to add to the website. 3.2 Review of MDT membership / changes A list of the SSG delegates was circulated so that members could check that relevant colleagues had been identified. Additions were made to the list. A shortage of imaging specialist members was noted. The list will be updated and relevant radiologists will be invited to attend. HD / SL 4. The National Survivorship Programme Presentation by Catherine Neck (CN) Please see the presentation uploaded on to the SWSCN website. Due to the ever increasing population of patients living with and beyond cancer, the current follow up systems are not sustainable, therefore new methods need to be established to provide the support that patients require to lead as healthy and active a life as possible, for as long as possible. In order to achieve this, a risk stratified redesign of the follow up pathways is required, which will be based on the clinical condition and the individual needs of patients. Conventional follow up leaves patients with various needs not met, and has been found to be ineffective in the detection of recurrence, with most recurrences of disease occurring outside routine follow up. Implementation of the
3 Recovery Package is recommended as an alternative. The Recovery Package consists of holistic needs assessments, extended treatment summaries to improve the communication between secondary and primary care, patient education and support events. Access to remote monitoring and open access back into specialist services would have to be made available. A General Practitioner Cancer Care review (CCR) also requires completion by GP practices within 6 months of the practice being notified that a person has been diagnosed with cancer, to ensure consistency and quality of care. Implementation of these changes is one of the four priorities of the commissioning groups, with the emphasis not being on making cuts, but using the money for follow up more effectively. The group was invited to contact CN if they require any help to map follow-up pathways relating to this. Gloucestershire Hospitals are under the remit of a different Macmillan Survivorship Lead. The presentation also introduced the Prehabilitation project. This has been piloted in Upper GI services in UH Bristol for patients having an oesophagectomy and surgery for gynaecological cancers, and in NBT for patients with kidney cancer. At the point of diagnosis, the patients have an interview with the Band 4 Macmillan cancer support workers prior to the neoadjuvant chemotherapy period of their treatment. Health and wellbeing advice is provided. The feedback from patients is that they feel very much supported. Patients have managed to maintain and improve their physical function during their treatment. CN is currently seeking funding to extend this service to other disease sites. The issues with managing remote surveillance were discussed. The complete transfer of surveillance to primary care was not considered a possibility. Some Trusts within the network have remote monitoring IT systems which send alerts when patients tests are due. The system within NBT was thought to have cost approximately 10,000. RUH also have a PSA tracking system that was accessible anywhere and thought to be less expensive. Due to IT issues, it was 2-3 years before the system at TST ran correctly. Weston has a remote surveillance system in place for the last ten years that works well. The various software systems in the other Trusts will be investigated by Yeovil. It was felt that the wording associated with the Survivorship Initiative was not thought to be intuitive to the general public. For example, the terms holistic needs assessment and key worker might be unfamiliar and potentially confusing. There was concern about the potential risks associated with making patients responsible for managing their own follow up. Rowland Hackett had recently attended a survivorship meeting with two other user representatives to give their opinions on three potential risk stratified pathways. They all thought it was a good idea to have your follow up tailored to suit the individual needs of patients. For example, no one wants to wait in a clinic for hours just to be told good news. If the results of a blood test or CT are reported as normal, it can be arranged with the patient how they would like to be informed, be it by letter, or text. This frees up the capacity of the clinics and stops the patient having to wait for an unnecessary appointment. Representatives from the individual Trusts were asked how the implementation of the
4 recovery package was progressing. Wellbeing events are being held in the Trusts in different formats aside from GLOS and RUH who are looking to establish this in the near future. All Trusts aside from RUH are doing the extended treatment summaries, which is work related to a CQUIN, and completing holistic needs assessments. 5. Cancer Waits: The Good, The Bad and Patient Choice Presented by Teresa Coombes (TC) Please see the presentation uploaded on to the SWSCN website. The presentation brought together the collective views of the Cancer Managers. There has been a National slide in Cancer Waits Performance that has created anxiety across all areas. Cancer Managers are discussing the need to identify where the issues are occurring in the pathways with all SSGs so that unnecessary delays can be avoided. For many of the cancer sites, problems occur when patients move between Trusts, which is not so much of an issue for colorectal patients, apart from the need for access to radiotherapy. None of the SSGs are consistently achieving the 62 day target. Examples of good and challenging pathways, pathways affected by patient choice, and potential ways to problem solve the challenging pathways, were discussed as documented in the presentation. Access to endoscopy was identified as one of the biggest challenges. The group were encouraged to share best practice and rethink the current pathways to make them as streamlined as possible. TC is currently doing some work on this. 6. Clinical Guidelines 6.1 Review of any amendments to imaging, pathology, chemotherapy, surgery and radiotherapy practices: The clinical guidelines are currently being updated and will be circulated to the MDT Chairs for their consideration prior to the end of June. 6.2 An update on the genetics of colorectal cancer, with specific regard to lynch testing: Presented by Alan Donaldson Please see the presentation uploaded on to the SWSCN website. A freedom of information (FOI) request was recently sent to all of the Trusts in the network, to establish whether they were performing mismatch repair immunohistochemistry testing for Lynch syndrome in patients diagnosed with bowel cancer, who were under 50 years at time of diagnosis. This was recommended in the Royal College of Pathologists minimum dataset guidelines for colorectal cancer (July 2014). RUH had not been routinely performing this. Alan Donaldson was invited to the group to explain its importance and give a general update on the genetics of colorectal cancer. Tumour analysis is performed to identify those individuals for DNA analysis whose
5 colorectal cancer may be due to Lynch syndrome. The information may be important to the decisions made by oncologists due to the poorer response patients have to 5 Flurorouracil. Lynch syndrome (also known as hereditary non polyposis colorectal cancer) is an autosomal dominant disorder that accounts for 1-5% of all colorectal cancers. It is due to mutations in one of the mismatch repair genes and causes a 50% accelerated process from normal polyp to cancer in females, and 80% in males. The mismatch repair genes produce proteins that identify and repair DNA replication mistakes, so mutations of the genes impair this process. The Amsterdam Criteria for testing for the syndrome can be found in the presentation. The tumour is stained to look for the mismatch repair proteins. In Lynch syndrome, one of the proteins will be missing. The DNA analysis will look for microsatellite instability (MSI) present in an electropherogram trace. In normal tissue, one peak will be recorded, whereas in abnormal tissue, there will be a double peak (as shown in the presentation). There can be sporadic loss of MLH1 in 10 15% of all colorectal cancers; this is associated with DNA methylation and Brafv600E in colonic tumours, but not endometrial. The advantages of testing for MSI are that it has better sensitivity and specificity than immunohistochemistry (IHC) and is able to detect BRAFV600E mutations. The disadvantages are that it is more expensive than IHC and doesn t tell you which genes are involved. Newton Wong at the Bristol Royal Infirmary does both IHC and MSI tests. Many more clinicians across the cancer sites are requesting genetic tests and the costs are being reduced. The process for consenting patients to have DNA testing and where this should fall in the patients pathway needs to be defined. If the results are going to inform what chemotherapy a patient may have, the potential to have the DNA testing prior to the tumour test might be necessary. With the current service, it was not thought to be possible for the geneticists themselves to consent and process the test within a short time frame. Patients under 50 could be consented at the same time that they were consented for their operation. Patients can be reassured that there is a voluntary agreement that insurance companies will not ask about genetic testing. It was decided that the results of the testing should be sent back to the MDT. The plan for the network will be to test all patients under 50 for Lynch syndrome. The consent forms will be sent by AD to HD to publish on the website. A flow chart will be developed to show where the test will sit on the patient s pathway. 6.3 Self-expanding metal stents usage in the region AD / HD All Trusts usage of self-expanding metal stents will be in accordance with the updated clinical guidelines. 6.4 Barium enema (BE) usage in the region TST were still using BE when there were restrictions in the capacity to provide CT colonoscopies, but this has been resolved due to the national shortage of BE leaving no other option than to make the resources available to the radiographers. Weston also used to use BE when there were problems with capacity; this has been resolved in the same way.
6 6.5 The management of early rectal cancer Presented by Jonathan Ockrim The management of early rectal cancer was discussed in relation to MDT decision making and methods of surgical procedures. The current clinical guidelines state that all patients with early rectal cancer should be referred to the trans anal endoscopic microsurgery (TEMS) service in Bristol Royal Infirmary. Referral to Cheltenham s service needed to be added to this list. The group were asked to consider whether it would be appropriate to offer patients a local palliative resection if that patient refuses to travel to the centres and was comorbid, but would benefit from surgery to relieve uncomfortable symptoms. In this scenario, the patient would be fully informed that the gold standard for the management of early rectal cancer would be to travel to the services at either Bristol or Cheltenham. The group agreed that they would support the decision for local surgery in this particular set of circumstances. All persons with potentially curative early rectal cancer should be referred to the specialist centres. The equipment to perform TEMS was considered expensive and other options were now available. For example, the equipment to perform trans anal minimal invasive surgery (TAMIS) is a totally disposable piece of kit that can be used with other equipment such as diathermy or a scalpel. There were also other platforms available. The clinical guidelines will be amended to state surgical resection rather than limit performing the procedure to one platform. Agreed MW 7. Coordination of patient care pathways 7.1 Update of NICE suspected cancer guidelines and two week wait (2WW) referral forms The NICE guidelines for the referral of suspected cancer are currently being updated and will be published on the 23 rd June The two week wait forms will have to be revised to reflect the NICE recommendations and this will provide an opportunity to standardise the form across the network. The guidelines have been based on a mathematical model that aims to increase referrals to cancer services. Statistics indicate that there will be a 15% increase in referrals per year. 7.2 Update on the colorectal pathway project Presented by Mark Rawles The colorectal diagnostic pathway project is running to timeline. It is fully included in the ACE programme and details will be published on the SWSCN website in the next few weeks. The initial fact finding stage is complete and the project is now moving to the next stage. Challenges have arisen around obtaining timely, accurate data from the National datasets. The intention of the project is to develop a business model that will inform commissioning intentions. Having assessed the current services across the region, there are many variations in the diagnostic pathways and good practice that will be useful to
7 share. The results will be presented at the next SSG meeting. MR 7.3 Primary care referral process in North Bristol Trust Presented by Sarah John Please see the presentation uploaded on to the SWSCN website. North Bristol Trust changed its colorectal referral pathway in January. Referrals can now be made through the new referral route on ICE. NBT was aware that the previous colorectal 2 week wait pathway did not meet the NICE guidelines for best practice. The Trust therefore undertook a large scale review of the pathway aiming to streamline the process, and ensure that diagnostic tests and decisions were made at the earliest possible stage, as detailed in the presentation. So far the average referral time has been reduced from 14 to 8 days and is already improving the 62 day target, and reducing the pressure on the radiology department. So far no inappropriate referrals have been received through the system. UH Bristol and Weston also have ICE, but this is not available in the other Trusts. The CNSs at TST triage patients via their nurse led telephone clinic. 8. Patient experience 8.1 User representative input from Rowland Hackett (RH) The web pages developed by the SWAG user involvement group have not yet been published on the SWSCN website. HD currently has to prioritise completing Peer Review documents. User involvement information will be revisited later in the summer. The user representative groups in the Peninsula operate differently from the former SWAG user group as they are based within the Trusts, and have strong links with the clinical teams and current issues. The possibility for setting up similar user involvement groups within the SWAG region was raised. This will be escalated to the Cancer Operational Group. HD HD RH was asked by YDH to produce a detailed list of all of the different people that he encountered as a patient, the different areas that he had to go to and the nights spent as an inpatient. This will be used to raise awareness among the CNSs of the whole patient pathway. An update on the effect of the flexible sigmoidoscopy screening trial for people aged from 55 years was requested. This will be completed in the South West by the end of the year. The success of the trial will be measured in approximately 10 years time. 8.2 Review of the National Patient Experience Survey Please see the presentations uploaded on to the SWSCN website
8 The Clinical Nurse Specialists (CNSs) discussed the results from the National Patient Experience Survey, looking at Trust level best practice to be shared, Trust / network level priorities identified for pathway improvements, and the actions required to address identified priorities, as detailed in the presentations. Overall, an increased need for patient information was the most common issue, particularly on how to get financial help and information on clinical trials. The CNSs had already addressed this by adding relevant leaflets to the patient information packs. The methodology of the survey was questioned as local surveys conducted in some of the Trusts get very different results. The survey is currently out to tender. 9. Quality indicators, audits and data collection 9.1 Auditing MDT discussion recommendations versus eventual treatment Presented by Ann Lyons (AL) A network wide observational audit of whether MDT decisions are followed through in reality will be undertaken by looking at prospectively recorded data. Data will be collected on the patients discussed in the past 50 MDTs by going backwards from the 1 st of March to identify if the decisions were implemented. The information can be gathered from the SCR or clinic letters / notes and there will also be an MDT team questionnaire. Once completed, the potential to publish the results will be explored. The audit department and various junior doctors in NBT are ready to start the data collection. A few questions are specifically for the MDT coordinator to answer. Treatment will be defined as the decision to treat for the first definitive treatment (within 31 days). This will be written into the inclusion criteria. The audit department in NBT will contact the audit departments within the other Trusts to ask for their assistance. There are still some decisions to be made on defining the inclusion criteria and AL will doodle-poll the group to facilitate agreement on these. AL day mortality statistics A funnel graph from the National Bowel Cancer Audit Report (2014) that showed the observed and adjusted 90 day post-operative mortality (elective and emergency) by Trusts was reviewed. It had only been possible to distinguish where Gloucestershire Hospitals was placed in the graph prior to the meeting. A funnel graph of the individual Trusts results will be plotted for review at an SSG meeting in the future. HD / MW 9.3 Feedback from NBOCAP / data collection issues The death rate reported by NBOCAP from TST appeared to have been corrupted. A figure of 8.7% was reported. On repeating the analysis of the data over the same period of time, a figure of 2.2% was calculated. A possible explanation was thought to be that the Trust data is compared with HES data, and if the data doesn t match up, the HES data is used for the final results. Data collection and surgeon level reporting will be explored in more
9 depth at an SSG meeting in the near future. 10. Service Development 10.1 Cheltenham s brachytherapy unit Neil Borley (NB) explained that, although funding had been agreed for Cheltenham s brachytherapy unit several years ago, the service was not currently running due to low patient numbers. However, if there is a will to refer patients, and sufficient patient numbers, the service is all ready to run. Brachytherapy is suitable when local excision from other platforms cannot be offered due to a patient not being able to tolerate a general anaesthetic, or to avoid potential unpleasant side effects from a surgical procedure. For a lesion of the right size (the maximum capacity is 4 ½ cm), it can offer the patient a complete ablation of the tumour in 1-2 treatments. It was thought to be highly beneficial to have this different treatment option available, and several clinicians felt that they had patients who would benefit from brachytherapy The Enhanced Recovery Programme (ERP) The Enhance Recovery Programme was not discussed due to time constraints in the meeting Training opportunities A list of Pelican Courses that are available in 2015 was reviewed. This will be uploaded to the SWSCN website. HD 11. Research Update Please see the presentation uploaded on to the SWSCN website. Maxine Taylor (MT) provided a research report that detailed the clinical trials which were open across the region, and the most recent recruitment figures. Stephen Falk has agreed to remain the research lead for the SSG. All members were encouraged to continue recruiting patients to the relevant trials. 12. Peer Review Review of draft constitution The MDT leads provided information that will be updated in the Colorectal Constitution. This will be circulated for proof reading prior to the end of June. HD 13. Any other business
10 It was agreed that Rob Longman (RL) will give a presentation of the management of anal cancer and AIN practice at the next SSG meeting. RL Date of next meeting: 14 th October 2015
South West Clinical Network Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services
 Meeting of the SWAG Network Colorectal SSG 09:30-15:30, Wednesday, 30 th November 2016 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, BS20 OHH THIS MEETING WAS SPONSORED BY NORGINE, MERCK SERONO AND
Meeting of the SWAG Network Colorectal SSG 09:30-15:30, Wednesday, 30 th November 2016 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, BS20 OHH THIS MEETING WAS SPONSORED BY NORGINE, MERCK SERONO AND
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Haematology Cancer Network Site Specific Group.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Haematology Cancer Network Site Specific Group Annual Report 2014 Version 1.0 1 This annual report was prepared by: Sophie Otton Chair
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Haematology Cancer Network Site Specific Group Annual Report 2014 Version 1.0 1 This annual report was prepared by: Sophie Otton Chair
2. Review of previous notes
 Meeting of the SWAG Network Colorectal Site Specific Group (SSG) Wednesday, 27 th June 2018, 09:30-15:30 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, Bristol, BS20 0HH THIS MEETING WAS SPONSORED BY
Meeting of the SWAG Network Colorectal Site Specific Group (SSG) Wednesday, 27 th June 2018, 09:30-15:30 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, Bristol, BS20 0HH THIS MEETING WAS SPONSORED BY
Please see the separate list of attendees and apologies uploaded on to the South West Clinical Network website here.
 Meeting of the SWAG Network Colorectal Site Specific Group (SSG) 09:30-15:00, Wednesday, 7 th June 2017 Taunton Hyde Park Conference Centre, Hyde Lane, Taunton, Somerset, TA2 8BU Chair: Mr Michael Williamson
Meeting of the SWAG Network Colorectal Site Specific Group (SSG) 09:30-15:00, Wednesday, 7 th June 2017 Taunton Hyde Park Conference Centre, Hyde Lane, Taunton, Somerset, TA2 8BU Chair: Mr Michael Williamson
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Brain and CNS Cancer Network Site Specific Group.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Brain and CNS Cancer Network Site Specific Group Annual Report 2015 Version 1.0 1 This Annual Report was prepared by: Venkat Iyer, Chair
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Brain and CNS Cancer Network Site Specific Group Annual Report 2015 Version 1.0 1 This Annual Report was prepared by: Venkat Iyer, Chair
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Head and Neck Cancer Network Site Specific Group. Constitution.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Head and Neck Cancer Network Site Specific Group Constitution August 2015 Revision due: April 2017 Page 1 of 24 VERSION CONTROL THIS
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Head and Neck Cancer Network Site Specific Group Constitution August 2015 Revision due: April 2017 Page 1 of 24 VERSION CONTROL THIS
Meeting of the SWAG Network Haematology SSG
 Meeting of the SWAG Network Haematology SSG Tuesday 21 st November 2017, 14:00-16:30 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, Bristol, BS20 0HH This meeting was sponsored by Celgene and Novartis
Meeting of the SWAG Network Haematology SSG Tuesday 21 st November 2017, 14:00-16:30 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, Bristol, BS20 0HH This meeting was sponsored by Celgene and Novartis
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Cancer of Unknown Primary Network Site Specific Group. Clinical Guidelines
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary Network Site Specific Group Revision due: April 2019 Page 1 of 11 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician ASWCN TAUNTON AND SOMERSET Taunton Lung MDT (11-2C-1) - 2011/12 Dr Sarah Foster Compliance Self Assessment LUNG MDT
Colorectal Pathway Meeting minutes Wednesday 11 th March 2015, 2 pm 4 pm Nightingale Lecture Theatre, UHSM
 Colorectal Pathway Meeting minutes Wednesday 11 th March 2015, 2 pm 4 pm Nightingale Lecture Theatre, UHSM Attendance: Sarah Duff Clinical Director and Consultant Colorectal Surgeon, UHSM Mohammed Sadat
Colorectal Pathway Meeting minutes Wednesday 11 th March 2015, 2 pm 4 pm Nightingale Lecture Theatre, UHSM Attendance: Sarah Duff Clinical Director and Consultant Colorectal Surgeon, UHSM Mohammed Sadat
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Alliance
 Meeting of the SWAG Network Urology SSG Thursday 15 th March 2018, 13:30-17:00 Spire Specialist Care Centre, 300 Park Avenue, Aztec West Almondsbury, Bristol, BS32 4SY Chairs: Mr Jaspal Phull (JP) & Ms
Meeting of the SWAG Network Urology SSG Thursday 15 th March 2018, 13:30-17:00 Spire Specialist Care Centre, 300 Park Avenue, Aztec West Almondsbury, Bristol, BS32 4SY Chairs: Mr Jaspal Phull (JP) & Ms
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Soft Tissue Sarcoma Network Site Specific Group. Constitution.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Soft Tissue Sarcoma Network Site Specific June 2017 Revision due: April 2019 Page 1 of 23 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Soft Tissue Sarcoma Network Site Specific June 2017 Revision due: April 2019 Page 1 of 23 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Transforming Cancer Services for London
 Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
Programme Director Paul Roche Status Draft Owner Laura Boyd Version 0.4 Author Jennifer Layburn Date 15/05/13 Transforming Cancer Services for London Best Practice Commissioning Pathway for the early detection
South West Strategic Clinical Network Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services
 Meeting of the SWAG Network UGI / HPB Site Specific Group (SSG) Friday 15 th May 2015 at The Academy, Holiday Inn, Bristol City Centre, 12:30-16:30 Chair: Mr Richard Krysztopik This meeting was sponsored
Meeting of the SWAG Network UGI / HPB Site Specific Group (SSG) Friday 15 th May 2015 at The Academy, Holiday Inn, Bristol City Centre, 12:30-16:30 Chair: Mr Richard Krysztopik This meeting was sponsored
South West Strategic Clinical Network Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services
 Meeting of the SWAG Network Skin Cancer Site Specific Group (SSG) 17 th May 2016, Jurys Inn, Gloucester Road, Cheltenham, GL51 0TS, 09:30-13:00 This meeting was sponsored by DERMAL, PROSTRAKAN and BRISTOL
Meeting of the SWAG Network Skin Cancer Site Specific Group (SSG) 17 th May 2016, Jurys Inn, Gloucester Road, Cheltenham, GL51 0TS, 09:30-13:00 This meeting was sponsored by DERMAL, PROSTRAKAN and BRISTOL
Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer
 Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer Start date: May 2015 Review date: April 2018 1 Background Mismatch repair (MMR) deficiency is seen in approximately 15%
Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer Start date: May 2015 Review date: April 2018 1 Background Mismatch repair (MMR) deficiency is seen in approximately 15%
South West Strategic Clinical Network Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services
 Meeting of the SWAG Network Haematology Site Specific Group (SSG) Wednesday 2 nd November 2016, 14.00-16.30 Engineers House Conference Centre, Clifton Down, Bristol Chair: Dr Deepak Mannari (DM) This meeting
Meeting of the SWAG Network Haematology Site Specific Group (SSG) Wednesday 2 nd November 2016, 14.00-16.30 Engineers House Conference Centre, Clifton Down, Bristol Chair: Dr Deepak Mannari (DM) This meeting
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER. Guidelines for the assessment of mismatch. Colorectal Cancer
 COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer January 2015 1 Background Mismatch repair (MMR) deficiency is seen in approximately
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer January 2015 1 Background Mismatch repair (MMR) deficiency is seen in approximately
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER. Guidelines for the assessment of mismatch. Colorectal Cancer
 COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer March 2017 1 Background Mismatch repair (MMR) deficiency is seen in approximately
COLORECTAL PATHWAY GROUP, MANCHESTER CANCER Guidelines for the assessment of mismatch repair (MMR) status in Colorectal Cancer March 2017 1 Background Mismatch repair (MMR) deficiency is seen in approximately
Colorectal Cancer Pathway Clinical Subgroup Tuesday 4 th September pm 4 pm CTCCU Seminar Room UHSM
 Manchester Cancer Colorectal Cancer Pathway Clinical Subgroup Tuesday 4 th September2014 2 pm 4 pm CTCCU Seminar Room UHSM Attendance Sarah Duff Michael Braun David Bisset Mohammed Sadat Deborah Hitchen
Manchester Cancer Colorectal Cancer Pathway Clinical Subgroup Tuesday 4 th September2014 2 pm 4 pm CTCCU Seminar Room UHSM Attendance Sarah Duff Michael Braun David Bisset Mohammed Sadat Deborah Hitchen
ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY. Phases One and Two Final Report
 ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY Phases One and Two Final Report July 2017 Introduction This paper presents the learning and actions that have been generated from phase One and Two
ACE Programme SOMERSET INTEGRATED LUNG CANCER PATHWAY Phases One and Two Final Report July 2017 Introduction This paper presents the learning and actions that have been generated from phase One and Two
Northern Ireland Bowel Cancer Screening Programme. Pathways. Version 4 1 st October 2013
 Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
Northern Ireland Bowel Cancer Screening Programme Pathways These changes will be version controlled, led by the Quality Assurance Director for the Programme. Any updated versions will be circulated and
Living With and Beyond Cancer where next?
 Living With and Beyond Cancer where next? Lesley Smith, Senior Programme Manager, LWBC, NHS England National Network of Colorectal Cancer Nurses, Sept 2018 Disclosure Trustee (unpaid) of the Pelvic Radiation
Living With and Beyond Cancer where next? Lesley Smith, Senior Programme Manager, LWBC, NHS England National Network of Colorectal Cancer Nurses, Sept 2018 Disclosure Trustee (unpaid) of the Pelvic Radiation
Resource impact report: Molecular testing strategies for Lynch syndrome in people with colorectal cancer (DG27)
 Putting NICE guidance into practice Resource impact report: Molecular testing strategies for Lynch syndrome in people with colorectal cancer (DG27) Published: February 2017 Summary Molecular testing strategies
Putting NICE guidance into practice Resource impact report: Molecular testing strategies for Lynch syndrome in people with colorectal cancer (DG27) Published: February 2017 Summary Molecular testing strategies
Data briefing: Reflex testing for Lynch syndrome in people diagnosed with bowel cancer under the age of 50
 Data briefing: Reflex testing for Lynch syndrome in people diagnosed with bowel cancer under the age of 50 Introduction Lynch syndrome is an inherited condition that predisposes individuals to bowel and
Data briefing: Reflex testing for Lynch syndrome in people diagnosed with bowel cancer under the age of 50 Introduction Lynch syndrome is an inherited condition that predisposes individuals to bowel and
LCA Lung Clinical Forum. 21 st October 2014
 LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
LCA Lung Clinical Forum 21 st October 2014 Welcome Dr Liz Sawicka Chair - LCA Lung Pathway Group Succession planning Dr Kate Haire Consultant in Public Health Medicine, LCA Commissioning Intentions for
South West Cancer Alliances Rapid Diagnostic Pathway for Lung Cancer Project Evaluation
 Somerset, Wiltshire, Avon and Gloucestershire Cancer Alliance Peninsula Cancer Alliance South West Cancer Alliances Rapid Diagnostic Pathway for Lung Cancer Project Evaluation Peninsula Thoracic-Oncology
Somerset, Wiltshire, Avon and Gloucestershire Cancer Alliance Peninsula Cancer Alliance South West Cancer Alliances Rapid Diagnostic Pathway for Lung Cancer Project Evaluation Peninsula Thoracic-Oncology
Colorectal Pathway Meeting minutes Wednesday 16 th July 2014, 2 pm 4 pm Nightingale Lecture Theatre, UHSM
 Colorectal Pathway Meeting minutes Wednesday 16 th July 2014, 2 pm 4 pm Nightingale Lecture Theatre, UHSM Attendance: Sarah Duff Edwin Clark Sophie Harrison Caroline Whitaker Sarah Taylor Debbie West Mark
Colorectal Pathway Meeting minutes Wednesday 16 th July 2014, 2 pm 4 pm Nightingale Lecture Theatre, UHSM Attendance: Sarah Duff Edwin Clark Sophie Harrison Caroline Whitaker Sarah Taylor Debbie West Mark
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician CSCCN PORTSMOUTH HOSPITALS Portsmouth Colorectal MDT (11-2D-1) - 2011/12 Daniel OLeary Compliance Self Assessment COLORECTAL
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician CSCCN PORTSMOUTH HOSPITALS Portsmouth Colorectal MDT (11-2D-1) - 2011/12 Daniel OLeary Compliance Self Assessment COLORECTAL
MCIP Recruitment Pack
 MCIP Recruitment Pack Page 1 of 13 Welcome Thank you for the interest you have shown in the MCIP Programme. An exciting partnership has been established to redesign cancer care in Manchester. Funded by
MCIP Recruitment Pack Page 1 of 13 Welcome Thank you for the interest you have shown in the MCIP Programme. An exciting partnership has been established to redesign cancer care in Manchester. Funded by
South West Strategic Clinical Network Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services
 SWAG Cancer of Unknown Primary (CUP) Referral Processes The SWAG network site specific groups refer any patient with metastatic carcinoma of unknown origin on for discussion to the specialist carcinoma
SWAG Cancer of Unknown Primary (CUP) Referral Processes The SWAG network site specific groups refer any patient with metastatic carcinoma of unknown origin on for discussion to the specialist carcinoma
National Cancer Registration Service South West Cancer Alliance Manager NHS England South, South West
 Present : Apologies: Meeting of the SWAG Area Cancer Operational Group (formerly ASW) Held on Wednesday 18 th April 2018, 10.00-12.00 Sanford Education Centre, Room 10, 32 Keynsham Road, Cheltenham, GL53
Present : Apologies: Meeting of the SWAG Area Cancer Operational Group (formerly ASW) Held on Wednesday 18 th April 2018, 10.00-12.00 Sanford Education Centre, Room 10, 32 Keynsham Road, Cheltenham, GL53
Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview.
 Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview. Document Title An Overview of Commissioning Living with and Beyond Cancer in Yorkshire and Humber Version number: 1 First
Commissioning Living with and Beyond Cancer in Yorkshire and Humber; an Overview. Document Title An Overview of Commissioning Living with and Beyond Cancer in Yorkshire and Humber Version number: 1 First
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM)
 PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team DCN POOLE Poole THYROID ONLY MDT (11-2I-2) - 2011/12 Peer Review Visit Date 18th August 2011 Compliance THYROID ONLY
PEER REVIEW VISIT REPORT (MULTI-DISCIPLINARY TEAM) Network Organisation (Trust) Team DCN POOLE Poole THYROID ONLY MDT (11-2I-2) - 2011/12 Peer Review Visit Date 18th August 2011 Compliance THYROID ONLY
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Cancer of Unknown Primary (CUP) Network Site Specific Group.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary (CUP) Network Site Specific Group Annual Report 2015 Version 1.0 1 This Annual Report was prepared by: Tania
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Cancer of Unknown Primary (CUP) Network Site Specific Group Annual Report 2015 Version 1.0 1 This Annual Report was prepared by: Tania
National Cancer Peer Review Sarcoma. Julia Hill Acting Deputy National Co-ordinator
 National Cancer Peer Review Sarcoma Julia Hill Acting Deputy National Co-ordinator Improving Outcomes Guidance The Intentions of Improving Outcomes for People with Sarcoma Changes in the provision of care
National Cancer Peer Review Sarcoma Julia Hill Acting Deputy National Co-ordinator Improving Outcomes Guidance The Intentions of Improving Outcomes for People with Sarcoma Changes in the provision of care
Work Programme/Service Delivery Plan 2010/2013
 Essex and East Suffolk Gynaecological Cancer Network Site Specific Group Work Programme/Service Delivery Plan 2010/2013 Version Number 1.2 Author Members of the NSSG Date Written June 2010 Reviewed May
Essex and East Suffolk Gynaecological Cancer Network Site Specific Group Work Programme/Service Delivery Plan 2010/2013 Version Number 1.2 Author Members of the NSSG Date Written June 2010 Reviewed May
DCP Newsletter. Welcome. Issue 1 June Key Dates. National Men s Health Week June 2018
 DCP Newsletter Issue 1 June 2018 Welcome Hello and a warm welcome to all of our readers of this first edition of the Dorset Cancer Partnership (DCP) newsletter. Each edition of this newsletter will provide
DCP Newsletter Issue 1 June 2018 Welcome Hello and a warm welcome to all of our readers of this first edition of the Dorset Cancer Partnership (DCP) newsletter. Each edition of this newsletter will provide
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Breast Cancer Network Site Specific Group. Constitution.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Breast Cancer Network Site Specific Group Constitution June 2015 Revision due: April 2016 Page 1 of 20 VERSION CONTROL THIS IS A CONTROLLED
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Breast Cancer Network Site Specific Group Constitution June 2015 Revision due: April 2016 Page 1 of 20 VERSION CONTROL THIS IS A CONTROLLED
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Head and Neck Cancer Network Site Specific Group. Constitution.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Head and Neck Cancer Network Site Specific Group Constitution June 2017 Revision due: April 2019 Page 1 of 23 VERSION CONTROL THIS IS
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Head and Neck Cancer Network Site Specific Group Constitution June 2017 Revision due: April 2019 Page 1 of 23 VERSION CONTROL THIS IS
SCAN Colorectal Group
 SCAN Colorectal Group Friday 1 st June 2012 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Dumfries Present Alison Allen Angie Balfour Paul Fineron Stephen Glancy Mohammad Hosny Martin Keith
SCAN Colorectal Group Friday 1 st June 2012 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Dumfries Present Alison Allen Angie Balfour Paul Fineron Stephen Glancy Mohammad Hosny Martin Keith
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Colorectal Cancer Network Site Specific Group. Constitution.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Colorectal Cancer Network Site Specific Group June 2015 Page 1 of 37 Revision due: April 2016 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Colorectal Cancer Network Site Specific Group June 2015 Page 1 of 37 Revision due: April 2016 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
CT Colon Service & Radiology Pathways
 CT Colon Service & Radiology Pathways Louisa Edwards CT Colon Advanced Radiography Practitioner ABMU 6 th February 2019 Louisa.Edwards@wales.nhs.uk CT, Radiology Dept, POWH, ABMU Health Board Context and
CT Colon Service & Radiology Pathways Louisa Edwards CT Colon Advanced Radiography Practitioner ABMU 6 th February 2019 Louisa.Edwards@wales.nhs.uk CT, Radiology Dept, POWH, ABMU Health Board Context and
National Group for Volunteering in NHS Scotland
 National Group for Volunteering in NHS Scotland Minutes of the meeting held on Tuesday 23 August 2016 at Delta House, West Nile Street, Glasgow Present Neil Galbraith Rob Coward Sandie Dickson Marion Findlay
National Group for Volunteering in NHS Scotland Minutes of the meeting held on Tuesday 23 August 2016 at Delta House, West Nile Street, Glasgow Present Neil Galbraith Rob Coward Sandie Dickson Marion Findlay
Cancer Improvement Plan Update. September 2014
 Cancer Improvement Plan Update September 2014 1 Contents Page 1. Introduction 3 2. Key Achievements 4-5 3. Update on Independent Review Recommendations 6-13 4. Update on IST Recommendations 14-15 5. Update
Cancer Improvement Plan Update September 2014 1 Contents Page 1. Introduction 3 2. Key Achievements 4-5 3. Update on Independent Review Recommendations 6-13 4. Update on IST Recommendations 14-15 5. Update
Delivering stratified follow-up in primary care for Prostate Cancer Patients - The NCL Approach. Dr Elizabeth Babatunde Macmillan GP
 Delivering stratified follow-up in primary care for Prostate Cancer Patients - The NCL Approach Dr Elizabeth Babatunde Macmillan GP Background 2 Objectives Enhance patient experience and outcomes by providing
Delivering stratified follow-up in primary care for Prostate Cancer Patients - The NCL Approach Dr Elizabeth Babatunde Macmillan GP Background 2 Objectives Enhance patient experience and outcomes by providing
SCAN Colorectal Group
 DRAFT SCAN Colorectal Group Friday 6 th December 2013 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Victoria Hospital, Kirkcaldy. Present Ibrahim Amin Angie Balfour Sarah Buchan Paul Fineron
DRAFT SCAN Colorectal Group Friday 6 th December 2013 14.15 16.15pm Oncology Seminar Room, WGH with videolink to Victoria Hospital, Kirkcaldy. Present Ibrahim Amin Angie Balfour Sarah Buchan Paul Fineron
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM)
 INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT NECN N Tees & Hartlepool North Tees And Hartlepool Date Self Assessment Completed 23rd July 2009 Date of IV Review 19th June 2009
INTERNAL VALIDATION REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT NECN N Tees & Hartlepool North Tees And Hartlepool Date Self Assessment Completed 23rd July 2009 Date of IV Review 19th June 2009
Colorectal Subgroup Minutes Tuesday 22 nd September 2015, 2pm 4pm CTCCU Seminar Room, UHSM
 Colorectal Subgroup Minutes Tuesday 22 nd September 2015, 2pm 4pm CTCCU Seminar Room, UHSM ATTENDANCE Sarah Duff Tom Pharaoh Mike Braun Edwin Clark Dave Smith Vanessa Denvir Hannah Leaton Malcolm Wilson
Colorectal Subgroup Minutes Tuesday 22 nd September 2015, 2pm 4pm CTCCU Seminar Room, UHSM ATTENDANCE Sarah Duff Tom Pharaoh Mike Braun Edwin Clark Dave Smith Vanessa Denvir Hannah Leaton Malcolm Wilson
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs. Gynaecological sarcomas Version 1
 Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Gynaecological sarcomas Version 1 Background This guidance is to provide direction for the management of patients with sarcomas
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Gynaecological sarcomas Version 1 Background This guidance is to provide direction for the management of patients with sarcomas
Information for families with a slightly increased risk of bowel cancer. Family History of Bowel Cancer
 Information for families with a slightly increased risk of bowel cancer Family History of Bowel Cancer How common is bowel cancer? Bowel cancer is the 3rd most common cancer in the UK. 1 in 20 people develop
Information for families with a slightly increased risk of bowel cancer Family History of Bowel Cancer How common is bowel cancer? Bowel cancer is the 3rd most common cancer in the UK. 1 in 20 people develop
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM)
 SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
SELF ASSESSMENT REPORT (MULTI-DISCIPLINARY TEAM) Network Trust MDT MDT Lead Clinician GMCN ROYAL WOLVERHAMPTON HOSPITALS The Royal Wolverhampton Hospitals Trust Lung MDT (11-2C-1) - 2011/12 Dr Angela Morgan
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services. Colorectal Cancer Network Site Specific Group. Constitution.
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Colorectal Cancer Network Site Specific Group June 2017 Revision due: April 2019 Page 1 of 36 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Colorectal Cancer Network Site Specific Group June 2017 Revision due: April 2019 Page 1 of 36 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Richard Watson, Chief Transformation Officer. Dr P Holloway, GP Clinical Lead for Cancer Lisa Parrish, Senior Transformation Lead
 GOVERNING BODY Agenda Item No. 08 Reference No. IESCCG 18-02 Date. 23 January 2018 Title Lead Chief Officer Author(s) Purpose Cancer Services Update Richard Watson, Chief Transformation Officer Dr P Holloway,
GOVERNING BODY Agenda Item No. 08 Reference No. IESCCG 18-02 Date. 23 January 2018 Title Lead Chief Officer Author(s) Purpose Cancer Services Update Richard Watson, Chief Transformation Officer Dr P Holloway,
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Alliance
 Meeting of the SWAG Network Gynae SSG Friday 15 th June 2018, 15:30-18:30, Board Room, Trust Headquarters, Bristol Royal Infirmary, Bristol, BS1 3NU THIS MEETING WAS SUPPORTED BY ASTRAZENECA AND STRYKER
Meeting of the SWAG Network Gynae SSG Friday 15 th June 2018, 15:30-18:30, Board Room, Trust Headquarters, Bristol Royal Infirmary, Bristol, BS1 3NU THIS MEETING WAS SUPPORTED BY ASTRAZENECA AND STRYKER
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Alliance
 Meeting of the SWAG Network Urology SSG Thursday 5 th July 2018, 13:30-17:00 Spire Specialist Care Centre, 300 Park Avenue, Aztec West Almondsbury, Bristol, BS32 4SY Chairs: Mr Jaspal Phull (JP) & Ms Lucinda
Meeting of the SWAG Network Urology SSG Thursday 5 th July 2018, 13:30-17:00 Spire Specialist Care Centre, 300 Park Avenue, Aztec West Almondsbury, Bristol, BS32 4SY Chairs: Mr Jaspal Phull (JP) & Ms Lucinda
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Lung /chest wall sarcomas incl. pulmonary metastatectomy Version 2
 Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Lung /chest wall sarcomas incl. pulmonary metastatectomy Version 2 Background Sarcomas that arise in the lung de novo are
Shared Care Pathway for Soft Tissue Sarcomas Presenting to Site Specialised MDTs Lung /chest wall sarcomas incl. pulmonary metastatectomy Version 2 Background Sarcomas that arise in the lung de novo are
National Breast Cancer Audit next steps. Martin Lee
 National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
National Breast Cancer Audit next steps Martin Lee National Cancer Audits Current Bowel Cancer Head & Neck Cancer Lung cancer Oesophagogastric cancer New Prostate Cancer - undergoing procurement Breast
SWAG Cancer Alliance Programme Manager
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Alliance Minutes of the Somerset, Wiltshire, Avon and Gloucestershire Cancer Alliance Board Meeting held on Friday 9 th June 2017 10:00-12:00
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Alliance Minutes of the Somerset, Wiltshire, Avon and Gloucestershire Cancer Alliance Board Meeting held on Friday 9 th June 2017 10:00-12:00
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Alliance
 Meeting of the SWAG Network Skin Cancer Site Specific Group (SSG) Wednesday 23 rd May 2018, 09:30-13:30 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, Bristol, BS20 0HH This meeting was sponsored by
Meeting of the SWAG Network Skin Cancer Site Specific Group (SSG) Wednesday 23 rd May 2018, 09:30-13:30 Penny Brohn Cancer Care, Chapel Pill Lane, Pill, Bristol, BS20 0HH This meeting was sponsored by
Delivering 62 Day GP Cancer Waits in a Complex Landscape. Hannah Marder Cancer Manager University Hospitals Bristol
 Delivering 62 Day GP Cancer Waits in a Complex Landscape Hannah Marder Cancer Manager University Hospitals Bristol Overview The 62 day GP target Cancer pathways What causes breaches? Good practice and
Delivering 62 Day GP Cancer Waits in a Complex Landscape Hannah Marder Cancer Manager University Hospitals Bristol Overview The 62 day GP target Cancer pathways What causes breaches? Good practice and
National Optimal Lung Cancer Pathways. Dr Sadia Anwar Nottingham University Hospitals NHS Trust Clinical Lead for Lung Cancer
 National Optimal Lung Cancer Pathways Dr Sadia Anwar ttingham University Hospitals NHS Trust Clinical Lead for Lung Cancer Overview How NOLCP evolved How it relates to national guidance Pathways Implementation
National Optimal Lung Cancer Pathways Dr Sadia Anwar ttingham University Hospitals NHS Trust Clinical Lead for Lung Cancer Overview How NOLCP evolved How it relates to national guidance Pathways Implementation
Prevention of Bowel Cancer: which patients do I send for colonoscopy?
 Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
Prevention of Bowel Cancer: which patients do I send for colonoscopy? Dr Chris Groves Consultant Gastroenterologist and Honorary Senior Lecturer St George s Hospital and Medical School Director, SW London
The Urology One-Stop Clinic
 The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
The Urology One-Stop Clinic Exceptional healthcare, personally delivered The aim of this leaflet is to answer any questions you may have about the Urology One-Stop Clinic. What is the Urology One-Stop
Clinical Advice for the Commissioning of the Whole Bowel Cancer Pathway
 Clinical Advice for the Commissioning of the Whole Bowel Cancer Pathway This document was produced by the Colorectal Cancer Clinical Expert Group November 2017 Clinical Advice to Cancer Alliances for the
Clinical Advice for the Commissioning of the Whole Bowel Cancer Pathway This document was produced by the Colorectal Cancer Clinical Expert Group November 2017 Clinical Advice to Cancer Alliances for the
On-going and planned colorectal cancer clinical outcome analyses
 On-going and planned colorectal cancer clinical outcome analyses Eva Morris Cancer Research UK Bobby Moore Career Development Fellow National Cancer Data Repository Numerous routine health data sources
On-going and planned colorectal cancer clinical outcome analyses Eva Morris Cancer Research UK Bobby Moore Career Development Fellow National Cancer Data Repository Numerous routine health data sources
LCA Mental Health & Psychological Support Mapping
 LCA Mental Health & Psychological Support Mapping November 2013 Contents 1 Introduction... 3 2 Method... 3 3 Results... 3 3.1 Information Centres... 3 3.2 Training and Education... 5 3.3 Level Two Supervision...
LCA Mental Health & Psychological Support Mapping November 2013 Contents 1 Introduction... 3 2 Method... 3 3 Results... 3 3.1 Information Centres... 3 3.2 Training and Education... 5 3.3 Level Two Supervision...
Local Healthwatch Quality Statements. February 2016
 Local Healthwatch Quality Statements February 2016 Local Healthwatch Quality Statements Contents 1 About the Quality Statements... 3 1.1 Strategic context and relationships... 5 1.2 Community voice and
Local Healthwatch Quality Statements February 2016 Local Healthwatch Quality Statements Contents 1 About the Quality Statements... 3 1.1 Strategic context and relationships... 5 1.2 Community voice and
West Midlands Sarcoma Advisory Group
 West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
West Midlands Sarcoma Advisory Group Guideline for the Initial Investigation and Referral to Sarcoma Specialist Multi Disciplinary Team for Suspected Sarcoma of Soft Tissue Extremities (limbs and trunk
NCIN Conference Feedback 2015
 NCIN Conference Feedback 2015 Parallel Sessions Treatments (Black type is the topic; blue type are comments) The use of population and research data in the development of guidelines for cancer treatment
NCIN Conference Feedback 2015 Parallel Sessions Treatments (Black type is the topic; blue type are comments) The use of population and research data in the development of guidelines for cancer treatment
Test and Learn Community Frailty Service for frail housebound patients and those living in care homes in South Gloucestershire
 Test and Learn Community Frailty Service for frail housebound patients and those living in care homes in South Gloucestershire Introduction This document introduces South Gloucestershire Clinical Commissioning
Test and Learn Community Frailty Service for frail housebound patients and those living in care homes in South Gloucestershire Introduction This document introduces South Gloucestershire Clinical Commissioning
Streamlining the lung diagnostic pathway (A87)
 Streamlining the lung diagnostic pathway (A87) Crawley CCG with Surrey and Sussex Healthcare NHS Trust Evaluation January 2017 Summary A new Straight-to-CT pathway for patients with an abnormal CXR result
Streamlining the lung diagnostic pathway (A87) Crawley CCG with Surrey and Sussex Healthcare NHS Trust Evaluation January 2017 Summary A new Straight-to-CT pathway for patients with an abnormal CXR result
Quality Standards for Diagnosis and Treatment in Breast Units Across Greater Manchester
 Quality Standards for Diagnosis and Treatment in Breast Units Across Greater Manchester Greater Manchester Cancer Clinical Director: Mr Mohammed Absar Pathway Manager: Rebecca Price Pathway approval: 24
Quality Standards for Diagnosis and Treatment in Breast Units Across Greater Manchester Greater Manchester Cancer Clinical Director: Mr Mohammed Absar Pathway Manager: Rebecca Price Pathway approval: 24
Bowel Cancer Information Leaflet THE DIGESTIVE SYSTEM
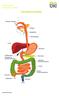 THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
THE DIGESTIVE SYSTEM This factsheet is about bowel cancer Throughout our lives, the lining of the bowel constantly renews itself. This lining contains many millions of tiny cells, which grow, serve their
GREATER MANCHESTER EXPERIENCE
 Greater Manchester Cancer Vanguard Innovation Remote Monitoring / Stratified Pathways GREATER MANCHESTER EXPERIENCE NADEEM AHMED - INFORMATICS ENTERPRISE ARCHITECT, DIGITAL PROJECTS @ The Christie Previously
Greater Manchester Cancer Vanguard Innovation Remote Monitoring / Stratified Pathways GREATER MANCHESTER EXPERIENCE NADEEM AHMED - INFORMATICS ENTERPRISE ARCHITECT, DIGITAL PROJECTS @ The Christie Previously
Cancer and Data in the New NHS May Di Riley, Director Clinical Outcomes
 Cancer and Data in the New NHS May 2011 Di Riley, Director Clinical Outcomes Overarching NHS context Financial constraints White Paper GP Commissioning/Commissioning Board Public Health England National
Cancer and Data in the New NHS May 2011 Di Riley, Director Clinical Outcomes Overarching NHS context Financial constraints White Paper GP Commissioning/Commissioning Board Public Health England National
Streamlining Memory Service Pathways. Guidance from the London Dementia Clinical Network
 Triage Initial Assessment Investigations 2nd Appointment Streamlining Memory Service Pathways Guidance from the London Dementia Clinical Network London Dementia Clinical Network July 2017 1 Contents Introduction...
Triage Initial Assessment Investigations 2nd Appointment Streamlining Memory Service Pathways Guidance from the London Dementia Clinical Network London Dementia Clinical Network July 2017 1 Contents Introduction...
Cancer Transformation Programme
 Cancer Transformation Programme Introduction to and supporting documentation for VALUE BASED TRANSFORMATION FUNDING SITE SELECTION November 2016 1 Introduction and Contents The Planning Guidance for 2017-2019
Cancer Transformation Programme Introduction to and supporting documentation for VALUE BASED TRANSFORMATION FUNDING SITE SELECTION November 2016 1 Introduction and Contents The Planning Guidance for 2017-2019
Developing Services for Teenagers and Young Adults (TYA) with Cancer
 Selena Riggs South West Specialised Commissioning Group Deirdre Brunton- Teenage Cancer Trust, TYA Lead Nurse Developing Services for Teenagers and Young Adults (TYA) with Cancer South West Specialised
Selena Riggs South West Specialised Commissioning Group Deirdre Brunton- Teenage Cancer Trust, TYA Lead Nurse Developing Services for Teenagers and Young Adults (TYA) with Cancer South West Specialised
National Group for Volunteering in NHS Scotland
 National Group for Volunteering in NHS Scotland Minutes of the meeting held on Tuesday 15 November 2016 Crammond Room, Scottish Health Services Centre, Edinburgh. Present Neil Galbraith Alan Bigham Rob
National Group for Volunteering in NHS Scotland Minutes of the meeting held on Tuesday 15 November 2016 Crammond Room, Scottish Health Services Centre, Edinburgh. Present Neil Galbraith Alan Bigham Rob
In this edition: Newsletter Summer How Primary Care can help earlier diagnosis. Improving communication between Primary & Secondary Care
 Newsletter Summer 2016 In this edition: How Primary Care can help earlier diagnosis Improving communication between Primary & Secondary Care A new approach to longer term care How primary care is adapting
Newsletter Summer 2016 In this edition: How Primary Care can help earlier diagnosis Improving communication between Primary & Secondary Care A new approach to longer term care How primary care is adapting
Identifying distinguishing features of the MDC model within the five ACE projects
 Identifying distinguishing features of the MDC model within the five ACE projects Context: The ACE Programme (Wave 2) has been working with five projects across England to trial and evaluate the concept
Identifying distinguishing features of the MDC model within the five ACE projects Context: The ACE Programme (Wave 2) has been working with five projects across England to trial and evaluate the concept
The Colorectal (bowel) Family History Clinic. Information for patients Endoscopy
 The Colorectal (bowel) Family History Clinic Information for patients Endoscopy What does the Colorectal Family History Clinic provide? The Family History Clinic provides a chance for you to talk about
The Colorectal (bowel) Family History Clinic Information for patients Endoscopy What does the Colorectal Family History Clinic provide? The Family History Clinic provides a chance for you to talk about
SCAN Skin Group Friday 1 st November 2013
 SCAN Skin Group Friday 1 st November 2013 Dermatology Seminar Room, Lauriston Buildings with videolinks to Oncology Seminar Room, Western General Hospital and Borders General Hospital. MINUTES Present
SCAN Skin Group Friday 1 st November 2013 Dermatology Seminar Room, Lauriston Buildings with videolinks to Oncology Seminar Room, Western General Hospital and Borders General Hospital. MINUTES Present
NICE Quality Standards and COF
 NICE Quality Standards and COF David Baldwin Consultant Respiratory Physician NUH Hon Senior Lecturer Nottingham University Clinical lead NICE lung cancer GL Chair NICE QS Topic Expert Group Quality Standards
NICE Quality Standards and COF David Baldwin Consultant Respiratory Physician NUH Hon Senior Lecturer Nottingham University Clinical lead NICE lung cancer GL Chair NICE QS Topic Expert Group Quality Standards
The Peninsula Network Site Specific Group for Thoracic Oncology
 The Peninsula Network Site Specific Group for Thoracic Oncology Network Annual Report June 205 Acting Chair: Liz Toy Date Approved: Annual report of the Network Site Specific Group for Thoracic Oncology
The Peninsula Network Site Specific Group for Thoracic Oncology Network Annual Report June 205 Acting Chair: Liz Toy Date Approved: Annual report of the Network Site Specific Group for Thoracic Oncology
Improving diagnostic pathways for patients with suspected lung cancer
 Improving diagnostic pathways for patients with suspected lung cancer Executive summary Accelerate, Coordinate, Evaluate (ACE) Programme An early diagnosis of cancer initiative supported by: NHS England,
Improving diagnostic pathways for patients with suspected lung cancer Executive summary Accelerate, Coordinate, Evaluate (ACE) Programme An early diagnosis of cancer initiative supported by: NHS England,
Haemato-oncology Clinical Forum. 20 th June 2013
 Haemato-oncology Clinical Forum 20 th June 2013 Welcome Dr Majid Kazmi, LCA Haemato-oncology Pathway Group Chair Purpose of today Provide an update on progress of the LCA to date Identify priorities for
Haemato-oncology Clinical Forum 20 th June 2013 Welcome Dr Majid Kazmi, LCA Haemato-oncology Pathway Group Chair Purpose of today Provide an update on progress of the LCA to date Identify priorities for
Patient Survey Report Spring 2013
 Patient Survey Report Spring 2013 We invited the original group of Patients from last year s PPG to become part of a Virtual Forum once again this year and also sent text messages to all out patients inviting
Patient Survey Report Spring 2013 We invited the original group of Patients from last year s PPG to become part of a Virtual Forum once again this year and also sent text messages to all out patients inviting
Supra Network Sarcoma Advisory Group (SAG) Annual Report
 London and South East Sarcoma Network Supra Network Sarcoma Advisory Group (SAG) Annual Report 2011-2012 Hosted by Date: December 2012 Version: 2 Review Date: September 2013 London Cancer Integrated Cancer
London and South East Sarcoma Network Supra Network Sarcoma Advisory Group (SAG) Annual Report 2011-2012 Hosted by Date: December 2012 Version: 2 Review Date: September 2013 London Cancer Integrated Cancer
Patient Information Forum
 Patient Information Forum Nov 2010 - Update Apologies for cancelling our October meeting (due to unforeseen circumstances). Our next meeting is on 14 December, 9:30am-12:30pm, Seminar Room 2, Cancer Centre,
Patient Information Forum Nov 2010 - Update Apologies for cancelling our October meeting (due to unforeseen circumstances). Our next meeting is on 14 December, 9:30am-12:30pm, Seminar Room 2, Cancer Centre,
Follow up The way ahead. John Griffith
 Follow up The way ahead John Griffith Key Emerging Principles Risk stratified pathways of care Personalised care plan and treatment summary with a hand held record Information and education Remote monitoring
Follow up The way ahead John Griffith Key Emerging Principles Risk stratified pathways of care Personalised care plan and treatment summary with a hand held record Information and education Remote monitoring
Fixing footcare in Sheffield: Improving the pathway
 FOOTCARE CASE STUDY 1: FEBRUARY 2015 Fixing footcare in Sheffield: Improving the pathway SUMMARY The Sheffield Teaching Hospitals NHS Foundation Trust diabetes team transformed local footcare services
FOOTCARE CASE STUDY 1: FEBRUARY 2015 Fixing footcare in Sheffield: Improving the pathway SUMMARY The Sheffield Teaching Hospitals NHS Foundation Trust diabetes team transformed local footcare services
Improving services for upper GI (OG) cancer Application template (Version 2)
 Trust Clinical lead Improving services for upper GI (OG) cancer Application template (Version 2) Managerial lead Date completed 14 June 2013 Barnet & Chase Farm Hospitals NHS Trust Dr Marta Carpani Upper
Trust Clinical lead Improving services for upper GI (OG) cancer Application template (Version 2) Managerial lead Date completed 14 June 2013 Barnet & Chase Farm Hospitals NHS Trust Dr Marta Carpani Upper
Cancer Services Position & Recovery Plan June 2015
 Appendix 6 Cancer Services Position & Recovery Plan June 2015 Introduction The Trust is required to achieve 85% compliance for patients on a 62 day pathway from the referral date to the date they receive
Appendix 6 Cancer Services Position & Recovery Plan June 2015 Introduction The Trust is required to achieve 85% compliance for patients on a 62 day pathway from the referral date to the date they receive
Advice Statement. Advice Statement November Advice for NHSScotland. Why is SHTG looking at this topic?
 Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
Advice Statement 014-18 November 2018 Advice Statement Colon capsule endoscopy (CCE-2) for the detection of colorectal polyps and cancer in adults with signs or symptoms of colorectal cancer or at increased
Head & Neck Cancer Network Site Specific Group. Clinical Guidelines. June 2015
 Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Head & Neck Cancer Network Site Specific Group June 2015 Revision due: July 2015 Page 1 of 6 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
Somerset, Wiltshire, Avon and Gloucestershire (SWAG) Cancer Services Head & Neck Cancer Network Site Specific Group June 2015 Revision due: July 2015 Page 1 of 6 VERSION CONTROL THIS IS A CONTROLLED DOCUMENT.
We need to talk about Palliative Care. Pancreatic Cancer UK
 We need to talk about Palliative Care Pancreatic Cancer UK 1. Pancreatic Cancer UK welcomes the opportunity to respond to the Health and Sport Committee s inquiry on palliative care. About Pancreatic Cancer
We need to talk about Palliative Care Pancreatic Cancer UK 1. Pancreatic Cancer UK welcomes the opportunity to respond to the Health and Sport Committee s inquiry on palliative care. About Pancreatic Cancer
Activity Report April 2012 to March 2013
 North, South East and West of Scotland Cancer Networks Brain/Central Nervous System Tumours National Managed Clinical Network Activity Report April 2012 to March 2013 Professor Roy Rampling Emeritus Professor
North, South East and West of Scotland Cancer Networks Brain/Central Nervous System Tumours National Managed Clinical Network Activity Report April 2012 to March 2013 Professor Roy Rampling Emeritus Professor
Greater Manchester Cancer
 Meeting at Manchester Royal Infirmary Date of Meeting: 30 November 2017 Chair: Mr Derek O Reilly Greater Manchester Cancer Attendance Derek O Reilly Rebecca Price Vicki Stephenson Hornby Neil Bibby Saurabh
Meeting at Manchester Royal Infirmary Date of Meeting: 30 November 2017 Chair: Mr Derek O Reilly Greater Manchester Cancer Attendance Derek O Reilly Rebecca Price Vicki Stephenson Hornby Neil Bibby Saurabh
