Gene expression profiling of the DNMT3A R882 mutation in acute leukemia
|
|
|
- Julie Stevenson
- 6 years ago
- Views:
Transcription
1 268 Gene expression profiling of the DNMT3A R882 mutation in acute leukemia XIANGNAN HUANG *, DAOXIN MA *, WENHAO DONG, PENG LI, TING LU, NA HE, TIAN TIAN, NA LIU, YAHUI DU and CHUNYAN JI Department of Hematology, Qilu Hospital of Shandong University, Jinan, Shandong , P.R. China Received December 15, 2012; Accepted April 30, 2013 DOI: /ol Abstract. DNA methyltransferase 3A (DNMT3A) is one of two human de novo DNA methyltransferases essential for the regulation of gene expression. DNMT3A mutations and deletions have been previously observed in acute myeloid leukemia (AML), myelodysplastic sydromes and myeloproliferative neoplasms. However, the involvement of DNMT3A in acute lymphoblastic leukemia (ALL) has rarely been reported. In the present study, PCR and direct sequencing was performed to analyze mutations of DNMT3A amino acid residue 882 in 99 acute leukemia patients, including 57 AML patients, 41 ALL patients and a single biphenotypic acute leukemia (BAL) patient. DNMT3A expression was detected in mononuclear cells of the bone marrow in these patients and in normal individuals using real time quantitative polymerase chain reaction, and 17.5% (10/57) of AML patients were found to exhibit DNMT3A mutations. Four missense mutations were observed in the DNMT3A mutated AML patients, including R882 mutations and a novel single nucleotide polymorphism resulting in the M880V amino acid substitution. However, the ALL and BAL patients were not found to exhibit DNMT3A mutations. The DNMT3A expression levels in the AML patients were significantly higher compared with those of the ALL patients or normal controls. The reduced expression levels of DNMT3A were associated with a significantly lower complete remission rate in the AML patients. However, in the ALL patients, no statistical significance was identified. The results of the present study indicate that DNMT3A may play varying roles in the regulation of DNA methylation in AML and ALL. Correspondence to: Professor Chunyan Ji, Department of Hematology, Qilu Hospital of Shandong University, 107 Wenhuaxi Road, Jinan, Shandong , P.R. China jichunyan@sdu.edu.cn * Contributed equally Key words: DNMT3A, R882 mutations, acute myeloid leukemia, acute lymphoblastic leukemia, gene expression Introduction Acute leukemia (AL) consists of a group of heterogeneous malignancies in which immature and dysfunctional hematopoietic progenitors proliferate and accumulate in the bone marrow. DNA methylation plays a key role in the pathophysiology of acute myeloid leukemia (AML) (1) and acute lymphoblastic leukemia (ALL) (2,3). DNA methyltransferase 3A (DNMT3A) is one of two human de novo DNA methyltransferases essential for regulating gene expression during cellular development and differentiation (4). DNMT3A mutations and deletions have been analyzed in AML (5), chronic myeloid leukemia (CML), chronic myelomonocytic leukemia (CMML), myelodysplastic syndrome (MDS), lymphoma and myeloproliferative neoplasms (MPNs) (6 11). The frequency of the mutations in patients with different diseases varies between 0 (0/81, CML patients in blast crisis) and 22.1% (62/281, AML patients). The most common mutation has been identified at the site of amino acid residue R882. DNMT3A mutations have been found to be enriched in the M4 (32.8%) and M5 subtypes (57.1%), according to the French American British (FAB) classification system (12). The DNMT3A expression levels in patients with DNMT3A mutations were observed to be marginally lower than those without mutations. In addition, DNMT3A was also found to be expressed in normal human CD34 + bone marrow cells and its expression decreased with terminal myeloid differentiation (5). However, to date, the differences in the DNMT3A expression levels in various subtypes of AML, according to FAB classification, have not been determined. In a previous study, the results of a multivariate analysis indicated that DNMT3A mutations represented independent predictive factors of poor prognosis, including a reduced overall survival (OS) and complete remission (CR) rate (7). Qiao et al (13) reported that the CR rate in acute leukemia (AL) patients that were identified to positively express all the DNMT genes was significantly higher than that of patients with partially positive or negative expression, indicating that DNMT3A mutations and expression may be associated with the pathogenesis and prognosis of AL. ALL is a heterogeneous malignancy caused by the clonal proliferation of lymphocytes. The pathogenesis and causal cancer genes associated with AML and ALL differ (14). Unlike AML, extremely little is known about the mutation
2 HUANG et al: DNMT3A IN ACUTE LEUKEMIA 269 Table I. Clinical characteristics of 57 patients with AML. No DNMT3A R882 Non-R882 Any DNMT3A Characteristics mutation mutation mutation mutation P value a Patients, n Age at study entry, years 42.4±16.1 b 60.3±16.5 b ±15.7 b c Male gender (%) 26 (55.3) 3 (33.3) 0 (0.0) 3 (30.0) d Bone marrow blasts at diagnosis, % 77.75±20.84 b 84.9±19.7 b ±19.7 b c Normal karyotype, n/total (%) 11/13 (84.6) 4/4 (100) 1/1 (100.0) 5/5 (100.0) White-cell count at diagnosis, x10 3 cells/mm 3 Mean 26.71±45.57 b ±88.34 b ±88.21 b <0.001 b Median Cytogenetic risk, n/total (%) Favorable 18/45 (40.0) 0/7 (0.0) 0/1 (0.0) 0/8 (0.0) Intermediate 19/45 (42.2) 7/7 (100.0) 1/1 (100.0) 8/8 (100.0) Adverse 8/45 (17.8) 0/7 (0.0) 0/1 (0.0) 0/8 (0.0) AML subtype, n (%) M2 6 (12.8) 0 (0.0) 0 (0.0) 0 (0.0) M3 14 (29.8) 0 (0.0) 0 (0.0) 0 (0.0) M4 10 (21.3) 0 (0.0) 0 (0.0) 0 (0.0) M5 17 (36.2) 9 (100.0) 1 (100.0) 10 (100.0) a P values, no DNMT3A mutations vs. any DNMT3A mutation. b Data are presented as mean ± SD. P values were calculated using c Fisher's exact or d Wilcoxon tests. AML, acute myeloid leukemia d frequency of DNMT3A in ALL patients. Therefore, in the present study, 99 Chinese AL patients were screened for DNMT3A R882 mutations, with the aim of uncovering the frequency of the R882 mutations in ALL and the relationship between ALL and AML. In addition, DNMT3A expression levels were determined in these samples and normal controls to determine whether expression levels correlate with poor prognosis. The results demonstrate that the DNMT3A mutation status in AML is an important factor to consider for risk stratification of the disease. Materials and methods Patients, healthy subjects and bone marrow mononuclear cell (BMMC) and peripheral blood mononuclear cell (PBMC) collection. The study recruited 99 consecutive adult patients with AL [AML, ALL and biphenotypic acute leukemia (BAL)] newly diagnosed at Qilu Hospital of Shandong University between August 2011 and November The diagnosis was made according to the FAB classification. For the clinical analysis, CR, partial remission (PR) and non remission (NR) were defined according to the criteria of the International Working Group (15). Cytogenetic risk was determined in the AML patients following a method described previously (16). The characteristics of the patients at the time of sampling are presented in Tables I and II. The patients with AML were treated with standard induction chemotherapy (anthracycline and cytarabine). The patients with ALL were treated with standard induction chemotherapy (vincristine, daunorubicin, L asparaginase and prednisone). In addition, a control group of 16 healthy donors was included. An assessment of the patient history and a physical examination were performed during the initial diagnosis. The corresponding laboratory tests were performed. BMMCs and PBMCs were obtained from 41 ALL patients (bone marrow or whole blood), 57 AML patients, one BAL patient and 16 control individuals (bone marrow) using density gradient centrifugation with the Ficoll Hypaque technique (Ficoll, Pharmacia LKB Biotechnology Inc., Piscataway, NY, USA). The samples were then stored at 80 C. The present study was approved by the ethics committee of Qilu Hospital, Shandong University (Jinan, China). Written informed patient consent was obtained from all participants for the treatment and cryopreservation of BM and peripheral blood according to the Declaration of Helsinki. Genomic DNA isolation, PCR amplification and sequencing. Genomic DNA samples from bone marrow or whole blood of AML and ALL patients were extracted using the TIANamp genomic DNA kit [Tiangen Biotech (Beijing) Co., Ltd., Beijing, China] or the total DNA/RNA/protein extraction kit (Omega Bio Tek, Inc., Norcross, GA, USA). A DNA fragment of 379 bp covering the R882 site in exon 23 of the DNMT3A gene was amplified using the S1000 thermal cycler (Bio Rad, Hercules, CA, USA). Forward primer, 5' TCC TGC TGT GTG GTT AGA CG 3'; and reverse primer: 5' TAT TTC CGC CTC TGT GGT TT 3'. PCR was performed in a 25 µl volume containing 30 ng DNA, 12.5 µl PCR mastermix, 1 µl forward primer, 1 µl reverse primer and ddh 2 O. The PCR conditions
3 270 Table II. Clinical characteristics of 41 ALL patients and one BAL patient. ALL with Characteristics T-cell leukemia B-cell leukemia unknown phenotype BAL Patients, n DNMT3A mutations, n (%) 0 (0.0) 0 (0.0) 0 (0.0) 0 (0.0) Age at study entry, years 28.3±24.7 a 37.4±16.7 a 43.0±24.6 a 60 Male gender, n (%) 4 (66.7) 16 (51.6) 2 (50.0) 1 (100.0) Bone marrow blasts at diagnosis, % 95.0±0.0 a 86.1±13.8 a 83.5±12.0 a 97 Normal karyotype, n/total (%) 4/4 (100.0) 9/23 (39.1) 0/2 (0.0) 0/0 (0.0) White cell count at diagnosis, x10 3 cells/mm 3 Mean 52.1±67.8 a 63.0±98.4 a 2.54±1.94 a 5.08 Median Aberrant karyotype, n/total (%) (9,22)(q34;q11) or BCR/ABL fusion gene 0/4 (0.0) 13/23 (41.9) 0/2 (0.0) 0/0 (0.0) a Data are presented as mean ± SD. ALL, acute lymphoblastic leukemia; BAL, biphenotypic acute leukemia. were as follows: denaturation at 94 C for 5 min, followed by 35 cycles of denaturation at 94 C for 30 sec, annealing at 55 C for 30 sec, extension at 72 C for 30 sec and ending with an extension at 72 C for 10 min. The PCR products were sequenced bidirectionally using the ABI 3730xl DNA analyzer (Applied Biosystems, Bedford, MA, USA). RNA preparation and real time quantitative PCR. The total RNA was extracted using TRIzol (Invitrogen Life Technologies, Carlsbad, CA, USA), and the cdna was prepared using M MLV reverse transcriptase (Promega Corporation, Madison, WI, USA) according to the manufacturer's instructions. Reverse transcription was performed at 37 C for 15 min, followed by 85 C for 5 sec. Real time quantitative PCR (RQ PCR) was performed using the ABI Prism 7500 system (Applied Biosystems) according to the manufacturer's instructions. PCR was performed in a total volume of 10 µl, which included 5 µl 2X SYBR Green real time PCR master mix (Toyobo Co. Ltd., Osaka, Japan), PCR grade water, 1 µl template cdna and 0.5 µl forward and reverse primers. The sequences of the target specific primers were designed from human cdna sequences available in GenBank. DNMT3A forward, 5' GCC ACC TCT TCG CTC CGC TG 3' and reverse, 5' GAT GAT GTC CAA CCC TTT TCG CAA 3'; and β actin forward, 5' TGA CGT GGA CAT CCG CAA AG 3' and reverse, 5' CTG GAA GGT GGA CAG CGA GG 3'. The thermal cycling profile consisted of 95 C denaturation for 5 min, followed by 40 cycles at 95 C for 15 sec, 65 C for 15 sec and 72 C for 45 sec. To exclude non specific amplification and primer dimer formation, a dissociation curve analysis was performed and PCR products were confirmed by agarose gel electrophoresis. PCR grade water was used instead of template cdna for the negative control. The fold change in the gene expression was determined using the 2 ΔCT method with β actin as an endogenous control. All experiments were performed at least twice. Statistical analysis. The Student's t test was used to compare the differences in DNMT3A expression levels between the AML patients with R882 mutations and the normal controls. The difference in the DNMT3A expression levels between M5 subtype AML and the other AML subtypes was also compared by Student's t test. Differences in the DNMT3A expression levels were compared by an analysis of variance in three groups. The clinical characteristics of the AML and ALL patients, including gender, age, white cell count and other factors, are presented in Tables I and II. The AML and ALL patients were categorized into high and low DNMT3A expressing subgroups using the median value as the cut off. Fisher's exact test was used to compare the CR rate in patients with an intermediate risk profile. Pearson's chi square test was used to compare the CR rates between other groups. P<0.05 was considered to indicate a statistically significant difference. Statistical analysis was performed using the SPSS 17.0 statistical software program (SPSS Inc., Chicago, IL, USA). Results DNMT3A mutations. DNMT3A R882 mutational status was determined in a cohort of 57 AML and 41 ALL patients and 1 BAL patient. Of the AML patients, 6 were identified to exhibit the R882H variant, two the R882C variant, one the R882P variant and one the M880V variant, a novel single nucleotide polymorphism that leads to amino acid substitution. The DNMT3A mutation frequency in AML was 17.5% (10/57). Sequencing results of each type of mutation are presented in Fig. 1. None of the DNMT3A mutations were found in the ALL and BAL patients. The AML patients with DNMT3A mutations revealed lower CR rates following induction therapy compared with those with wild type DNMT3A (0 vs. 62.8%; P<0.001). The presence of a DNMT3A mutation was found
4 HUANG et al: DNMT3A IN ACUTE LEUKEMIA 271 Table III. Clinical and genetic characteristics of the ten DNMT3A-mutated AML cases. Nucleotide Aberrant expression or Response or outcome following UPN change Consequence Age, years Gender FAB Karyotype mutation of other genes induction chemotherapy QL-049 c.2645g>c p.r882p 37 Female M5 46, XX None PR QL-053 c.2645g>a p.r882h 79 Male M5 46, XY None Deceased QL-054 c.2644c>t p.r882c 44 Male M5 46, XY None NR QL-055 c.2645g>a p.r882h 41 Female M5 Unknown WT1 (+) NR QL-056 c.2644c>t p.r882c 65 Male M5 46, XY None NR QL-058 c.2645g>a p.r882h 71 Female M5 Unknown None NR QL-062 c.2638a>g p.m880v 55 Female M5 46, XX WT1 (+) NR QL-067 c.2645g>a p.r882h 60 Female M5 46, XX WT1 (+) NR QL-084 c.2645g>a p.r882h 63 Female M5 46, XX NPM1 (+), CEBPA (+) NR QL-092 c.2645g>a p.r882h 83 Female M5 46, XX FLT3 (+) Deceased UPN, unique patient number; FAB, French-American-British; PR, partial remission; NR, non-remission. A B C D E Figure 1. Sequencing of DNMT3A mutations in patients with AML. (A) Wild type and (B E) mutated DNMT3A gene Arrow indicates the mutated site. Three heterozygous mutations were identified at codon 882 in the samples of nine AML patients, and the sequencing figures of three patients are presented. (E) A novel SNP causing amino acid substitution, M880V, was found in a female patient with AML. The unique patient number (UPN) and mutation details of these patients are provided to the right of the peak charts. DNMT3A, DNA methyltransferase 3A; AML, acute myeloid leukemia; SNP, single nucleotide polymorphism. to correlate with a low CR rate in the AML patients with an intermediate risk profile (P=0.061). Clinical features of patients with DNMT3A mutations. The association between the status of DNMT3A mutations and clinical features in AML was investigated. Patients with DNMT3A mutations were classified with M5 subtype AML. The age and white cell count of the AML patients with DNMT3A mutations were higher than those without DNMT3A mutations. Gender and percentage of bone marrow blasts at diagnosis were not found to be significantly different between the two groups. DNMT3A mutations were significantly enriched in 8/26 patients with a cytogenetic profile associated with intermediate risk (30.8%; P=0.004; Table I). The clinical and genetic characteristics of the 10 DNMT3A mutated AML cases are presented in Table III. DNMT3A expression level. The DNMT3A expression levels were measured using RQ PCR. DNMT3A expression in the AML patients was found to be significantly higher than that of the ALL patients or normal controls (P=0.002 or P<0.001). DNMT3A expression was significantly decreased in the AML patients with DNMT3A mutations, including R882 and M880 mutations, compared with individuals without mutations (P<0.001). The AML patients with wild type DNMT3A revealed significantly higher DNMT3A expression levels compared with the normal controls (P<0.001). No statistical difference was identified between the AML patients with DNMT3A mutations and the normal controls (P=0.747). The ALL patients demonstrated higher DNMT3A expression levels compared with the normal controls, however, this difference was not statistically significant (P=0.127). No difference was
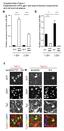
5 272 A B C D E F Figure 2. DNMT3A expression levels. Each dot represents one sample. (A) DNMT3A expression for 41 ALL patients, 57 AML patients, 1 BAL patient and the normal controls (n=16). DNMT3A expression in AML patients with (B) wild type or (C) R882 or other DNMT3A mutations compared with normal controls. (D) 37 ALL patients are divided into 6 T-ALL and 31 B-ALL patients. No difference was identified between DNMT3A expression levels in T-ALL and B-ALL patients. (E) DNMT3A expression levels for various AML subtypes according to FAB classification. (F) DNMT3A expression levels for M5 subtype AML were lower compared with other types of AML. DNMT3A, DNA methyltransferase 3A; ALL, acute lymphoblastic leukemia; AML, acute myeloid leukemia; BAL, biphenotypic acute leukemia; T, T cell; B, B cell; FAB, French American British. found in DNMT3A expression between the T cell ALL and B cell ALL patients (P=0.874). DNMT3A expression between the different AML subtypes (P=0.006) was significantly different. The M5 subtype AML patients were found to exhibit significantly lower DNMT3A expression levels compared with the patients with other subtypes of AML, including the M2, M3 and M4 subtypes (P=0.002; Fig. 2). To determine whether DNMT3A expression levels affect the treatment response of AML patients, the patients were divided into 2 groups; those with low or high DNMT3A expression (below or above the median level, respectively). The CR rate was calculated for each group according to the DNMT3A expression levels. The group with low DNMT3A expression revealed a lower CR rate than that of the high DNMT3A expression group (30.8 vs. 70.4%; P=0.002). The ALL patients were also divided into two groups using the same method. No significant difference was observed in the CR rate (57.9 vs. 60%; P=0.894) between the two groups or between T cell and B cell lymphoblastic leukemia (33.3 vs. 62.1%; P=0.195). Discussion To date, DNMT3A mutations have been detected in AML, CML, CMML, MDS, lymphoma and MPN. The frequency of DNMT3A mutations in AML is the highest when compared with other heterogeneous malignancies. Recently, Ribeiro et al reported that mutant DNMT3A represents an independent prognostic marker in AML. When patients with DNMT3A mutations at position R882 were analyzed, an association with an inferior outcome was also observed (16). In the present study, 10 mutations were identified in DNMT3A in 10/57 (17.5%) de novo AML patients. This high frequency is consistent with results of previous studies on DNMT3A mutations in AML patients (5,17). In addition, the mutation of DNMT3A was found to correlate with a low CR rate in AML patients with an intermediate risk profile, indicating that the mutation of DNMT3A represents a novel prognostic index for intermediate risk AML patients. However, none of the DNMT3A R882 mutations were identified in this consecutive series of ALL cases. Prior to the present study, Kim et al reported that the frequency of DNMT3A mutations in adult ALL was extremely low (0.8%, 1/124) (18). Differences in the frequency of DNMT3A mutations between AML and ALL may be associated with the different pathogenic mechanisms in AML and ALL. This hypothesis must be studied further, using larger cohorts to identify DNMT3A mutations in ALL patients and to evaluate the prognostic impact of the mutations. In the present study, DNMT3A R882 mutations were observed to be recurrent in AML patients and associated with a poor clinical outcome. DNMT3A is markedly overexpressed in the majority of AML patients with wild type DNMT3A when compared with normal controls. However, no difference was identified in DNMT3A expression between the AML patients with DNMT3A mutations and the control
6 HUANG et al: DNMT3A IN ACUTE LEUKEMIA 273 individuals. These results indicate that DNMT3A mutations may reduce the methyltransferase activity. Therefore, we hypothesized that the reduced expression of DNMT3A is indicative of a poor clinical outcome in AML patients due to decreased methyltransferase activity. This hypothesis is consistent with the observations that M880V and all R882 mutations are heterozygous and that this mutation reduces methyltransferase activity in vitro (19). Therefore, DNMT3A expression may represent a potential biomarker for the prediction of prognosis in AML. In the present study, the DNMT3A expression levels in AML patients were compared between various FAB subtypes, and a significant difference was identified. DNMT3A expression in M5 subtype AML was lower than that of other AML subtypes. In addition, the frequency of DNMT3A mutations in the AML patients with the M5 subtype was higher compared with the patients of other subtypes, indicating that decreased DNMT3A expression caused by DNMT3A mutations may be associated with the incidence and progression of AML, particularly in the M5 subtype. The difference in the CR rate between the two groups of AML patients indicated that lower DNMT3A expression correlated with an adverse treatment response. In the ALL patients, no difference was found in the CR rate, which may be explained by the marked difference in the DNMT3A mutation status and expression levels between AML and ALL. These results indicate that the function of DNMT3A in gene methylation in ALL may be distinct from its role in AML. A number of studies have confirmed that the DNA methylation of specific genes is associated with the clinical outcome (3,20,21) and that the activity of DNA methyltransferases may contribute to specific DNA methylation profiles. Previously, Challen et al analyzed the effect of hematopoietic specific conditional Dnmt3a deletion on self renewal in serial transplantation assays (14). Using conditional ablation, the study reported that Dnmt3a loss progressively impaired mouse hematopoietic stem cell (HSC) differentiation. Dnmt3a null HSCs were found to exhibit increased and decreased methylation at distinct loci, including substantial CpG island hyper and hypomethylation. In the Dnmt3a null HSCs, an extremely large number of hypomethylated genes were found that are commonly overexpressed in different types of leukemia, including AML and ALL. These observations are indicative of a crucial role for Dnmt3a in the pathogenesis of malignant neoplasms. However, the Dnmt3a null status in HSCs in mice is distinct from DNMT3A mutations in humans, as all R882 mutations are heterozygous. Whether the same set of genes is subjected to altered epigenetic patterning in DNMT3A mutant AML cells has not been investigated. TET2 and NPM1 mutations are markedly associated with DNMT3A mutations in T cell lymphoma and adult AML, respectively (5,10,17). These studies indicate an oncogenic cooperation between DNMT3A and other gene mutations, resulting in the deregulation of the cytosine methylation and demethylation processes. In the present study, the patients with DNMT3A mutations were older than the patients without DNMT3A mutations in AML, which was consistent with the results obtained by Ley et al (5). Consistent with these observations, a low frequency of DNMT3A mutations in pediatric AML was observed in studies by Ho et al (0/180, 0%) (22) and Hollink et al (3/140, 2.1%) (23). In pediatric AML, there is a 4-5 fold lower frequency of NPM1 mutations compared with adult AML (24). These results may partially explain why the frequency of DNMT3A mutations is low. Therefore, we hypothesized that DNMT3A mutations alone are insufficient to generate AML and other malignancies, and that second hits may be required. The results of the present study, in combination with observations of previous studies, indicate that DNMT3A mutations are associated with adverse outcomes in AML and that they may represent a novel marker for the risk stratification of AML. By contrast, DNMT3A mutations in ALL are rare. At present, the mechanisms by which mutated DNMT3A regulates DNA methylation remain unclear. Additional studies must be performed to identify and understand the regulatory mechanisms of DNMT3A. Screening for DNMT3A mutations may provide a novel tool for the prediction of clinical outcome. Acknowledgements The present study was supported by grants from the National Natural Science Foundation of China (nos , , and ), the Specialized Research Fund for the Doctoral Program of Higher Education of the Ministry of Education (no ) and the Independent Innovation Fund of Shandong University (IIFSDU ). References 1. Alvarez S, Suela J, Valencia A, et al: DNA methylation profiles and their relationship with cytogenetic status in adult acute myeloid leukemia. PLoS One 5: e12197, Roman Gomez J, Jimenez Velasco A, Agirre X, et al: Promoter hypermethylation and global hypomethylation are independent epigenetic events in lymphoid leukemogenesis with opposing effects on clinical outcome. Leukemia 20: , Kraszewska MD, Dawidowska M, Larmonie NSD, et al: DNA methylation pattern is altered in childhood T cell acute lymphoblastic leukemia patients as compared with normal thymic subsets: insights into CpG island methylator phenotype in T ALL. Leukemia 26: , Holz Schietinger C, Matje DM, Harrison MF and Reich NO: Oligomerization of DNMT3A controls the mechanism of de novo DNA methylation. J Biol Chem 286: , Ley TJ, Ding L, Walter MJ, et al: DNMT3A mutations in acute myeloid leukemia. N Engl J Med 363: , Li X, Cen J, Wang Q, et al: Absence of DNMT3A gene mutation in chronic myeloid leukemia patients in blast crisis. Eur J Haematol 88: , Shen Y, Zhu YM, Fan X, et al: Gene mutation patterns and their prognostic impact in a cohort of 1185 patients with acute myeloid leukemia. Blood 118: , Jankowska AM, Makishima H, Tiu RV, et al: Mutational spectrum analysis of chronic myelomonocytic leukemia includes genes associated with epigenetic regulation: UTX, EZH2 and DNMT3A. Blood 118: , Walter MJ, Ding L, Shen D, et al: Recurrent DNMT3A mutations in patients with myelodysplastic syndromes. Leukemia 25: , Couronné L, Bastard C and Bernard OA: TET2 and DNMT3A mutations in human T Cell lymphoma. N Engl J Med 366: 95-96, Stegelmann F, Bullinger L, Schlenk RF, et al: DNMT3A mutations in myeloproliferative neoplasms. Leukemia 25: , Bennett JM, Catovsky D, Daniel MT, et al: Proposals for the classification of the acute leukaemias. French-American-British (FAB) co-operative group. Br J Haematol 33: , 1976.
7 Qiao SK, Xu SR, Guo XN and Wang Y: Clinical significance of the expression of DNA methyltransferase genes (DNMT) in acute leukemia patients. Zhongguo Shi Yan Xue Ye Xue Za Zhi 13: , 2005 (In Chinese). 14. Challen GA, Sun D, Jeong M, et al: Dnmt3a is essential for hematopoietic stem cell differentiation. Nat Genet 44: 23 31, Cheson BD, Bennett JM, Kopecky KJ, et al: Revised recommendations of the International Working Group for diagnosis, standardization of response criteria, treatment outcomes, and reporting standards for therapeutic trials in acute myeloid leukemia. J Clin Oncol 21: , Ribeiro AF, Pratcorona M, Erpelinck Verschueren C, et al: Mutant DNMT3A: a marker of poor prognosis in acute myeloid leukemia. Blood 119: , Yan XJ, Xu J, Gu ZH, et al: Exome sequencing identifies somatic mutations of DNA methyltransferase gene DNMT3A in acute monocytic leukemia. Nat Genet 43: , Kim MS, Kim YR, Yoo NJ and Lee SH: Mutational analysis of DNMT3A gene in acute leukemias and common solid cancers. APMIS 121: 85-94, Yamashita Y, Yuan J, Suetake I, et al: Array based genomic resequencing of human leukemia. Oncogene 29: , Shen L, Kantarjian H, Guo Y, et al: DNA methylation predicts survival and response to therapy in patients with myelodysplastic syndromes. J Clin Oncol 28: , Figueroa ME, Lugthart S, Li Y, et al: DNA methylation signatures identify biologically distinct subtypes in acute myeloid leukemia. Cancer Cell 17: 13 27, Ho PA, Kutny MA, Alonzo TA, et al: Leukemic mutations in the methylation associated genes DNMT3A and IDH2 are rare events in pediatric AML: a report from the Children's Oncology Group. Pediatr Blood Cancer 57: , Hollink IH, Feng Q, Danen van Oorschot AA, et al: Low frequency of DNMT3A mutations in pediatric AML and the identification of the OCI AML3 cell line as an in vitro model. Leukemia 26: , Hollink IH, Zwaan CM, Zimmermann M, et al: Favorable prognostic impact of NPM1 gene mutations in childhood acute myeloid leukemia, with emphasis on cytogenetically normal AML. Leukemia 23: , 2009.
SUPPLEMENTARY INFORMATION
 Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Supplementary Document
 Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
Supplementary Document 1. Supplementary Table legends 2. Supplementary Figure legends 3. Supplementary Tables 4. Supplementary Figures 5. Supplementary References 1. Supplementary Table legends Suppl.
MicroRNA-29a Reveals Oncogenic Role on Myeloid Malignancies by Regulating DNMT3A
 MicroRNA-29a Reveals Oncogenic Role on Myeloid Malignancies by Regulating DNMT3A Heba Alkhatabi, PhD Assistant Professor Department of Medical Laboratory Collage of Applied Medical science King Abdul Aziz
MicroRNA-29a Reveals Oncogenic Role on Myeloid Malignancies by Regulating DNMT3A Heba Alkhatabi, PhD Assistant Professor Department of Medical Laboratory Collage of Applied Medical science King Abdul Aziz
Supplemental material Mutant DNMT3A: A Marker of Poor Prognosis in Acute Myeloid Leukemia Ana Flávia Tibúrcio Ribeiro, Marta Pratcorona, Claudia
 Supplemental material Mutant DNMT3A: A Marker of Poor Prognosis in Acute Myeloid Leukemia Ana Flávia Tibúrcio Ribeiro, Marta Pratcorona, Claudia Erpelinck-Verschueren, Veronika Rockova, Mathijs Sanders,
Supplemental material Mutant DNMT3A: A Marker of Poor Prognosis in Acute Myeloid Leukemia Ana Flávia Tibúrcio Ribeiro, Marta Pratcorona, Claudia Erpelinck-Verschueren, Veronika Rockova, Mathijs Sanders,
New drugs in Acute Leukemia. Cristina Papayannidis, MD, PhD University of Bologna
 New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sherman SI, Wirth LJ, Droz J-P, et al. Motesanib diphosphate
Acute leukemia and myelodysplastic syndromes
 11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schlenk RF, Döhner K, Krauter J, et al. Mutations and treatment
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schlenk RF, Döhner K, Krauter J, et al. Mutations and treatment
Screening for mutation R882 in the DNMT3A gene in Chinese patients with hematological disease
 Int J Hematol (2012) 96:229 233 DOI 10.1007/s12185-012-1104-z ORIGINAL ARTICLE Screening for mutation R882 in the DNMT3A gene in Chinese patients with hematological disease Yunlong Li Deng-Feng Zhang Shi-Wen
Int J Hematol (2012) 96:229 233 DOI 10.1007/s12185-012-1104-z ORIGINAL ARTICLE Screening for mutation R882 in the DNMT3A gene in Chinese patients with hematological disease Yunlong Li Deng-Feng Zhang Shi-Wen
c Tuj1(-) apoptotic live 1 DIV 2 DIV 1 DIV 2 DIV Tuj1(+) Tuj1/GFP/DAPI Tuj1 DAPI GFP
 Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
Supplementary Figure 1 Establishment of the gain- and loss-of-function experiments and cell survival assays. a Relative expression of mature mir-484 30 20 10 0 **** **** NCP mir- 484P NCP mir- 484P b Relative
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
DNMT3A mutations and clinical features in Chinese patients with acute myeloid leukemia
 Lu et al. Cancer Cell International 2013, 13:1 PRIMARY RESEARCH Open Access DNMT3A mutations and clinical features in Chinese patients with acute myeloid leukemia Quanyi Lu 1*, Yamei Chen 1, Hang Wang
Lu et al. Cancer Cell International 2013, 13:1 PRIMARY RESEARCH Open Access DNMT3A mutations and clinical features in Chinese patients with acute myeloid leukemia Quanyi Lu 1*, Yamei Chen 1, Hang Wang
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia
 Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
Corporate Medical Policy. Policy Effective February 23, 2018
 Corporate Medical Policy Genetic Testing for FLT3, NPM1 and CEBPA Mutations in Acute File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_flt3_npm1_and_cebpa_mutations_in_acute_myeloid_leukemia
Corporate Medical Policy Genetic Testing for FLT3, NPM1 and CEBPA Mutations in Acute File Name: Origination: Last CAP Review: Next CAP Review: Last Review: genetic_testing_for_flt3_npm1_and_cebpa_mutations_in_acute_myeloid_leukemia
Supplementary Table 3. 3 UTR primer sequences. Primer sequences used to amplify and clone the 3 UTR of each indicated gene are listed.
 Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
Supplemental Figure 1. DLKI-DIO3 mirna/mrna complementarity. Complementarity between the indicated DLK1-DIO3 cluster mirnas and the UTR of SOX2, SOX9, HIF1A, ZEB1, ZEB2, STAT3 and CDH1with mirsvr and PhastCons
N Engl J Med Volume 373(12): September 17, 2015
 Review Article Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. N Engl J Med Volume 373(12):1136-1152 September 17, 2015 Acute Myeloid Leukemia Most
Review Article Acute Myeloid Leukemia Hartmut Döhner, M.D., Daniel J. Weisdorf, M.D., and Clara D. Bloomfield, M.D. N Engl J Med Volume 373(12):1136-1152 September 17, 2015 Acute Myeloid Leukemia Most
Molecular Markers in Acute Leukemia. Dr Muhd Zanapiah Zakaria Hospital Ampang
 Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
THE USE OF WT1-QPCR TO MEASURE AND DETECT MINIMAL RESIDUAL DISEASE IN ACUTE MYELOID LEUKEMIA. Ava Greco
 THE USE OF WT1-QPCR TO MEASURE AND DETECT MINIMAL RESIDUAL DISEASE IN ACUTE MYELOID LEUKEMIA Ava Greco REVIEW OF LITERATURE What is Leukemia? Abnormal growth of cells in the blood stream Progresses rapidly
THE USE OF WT1-QPCR TO MEASURE AND DETECT MINIMAL RESIDUAL DISEASE IN ACUTE MYELOID LEUKEMIA Ava Greco REVIEW OF LITERATURE What is Leukemia? Abnormal growth of cells in the blood stream Progresses rapidly
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Elisabeth Koller 3rd Medical Dept., Center for Hematology and Oncology, Hanusch Hospital, Vienna, Austria
 Elisabeth Koller 3rd Medical Dept., Center for Hematology and Oncology, Hanusch Hospital, Vienna, Austria Incidence Diagnosis Prognostic factors Treatment Induction therapy - HSCT Indications for HSCT
Elisabeth Koller 3rd Medical Dept., Center for Hematology and Oncology, Hanusch Hospital, Vienna, Austria Incidence Diagnosis Prognostic factors Treatment Induction therapy - HSCT Indications for HSCT
Peking University People's Hospital, Peking University Institute of Hematology
 Qian Jiang, M.D. Peking University People's Hospital, Peking University Institute of Hematology No. 11 Xizhimen South Street, Beijing, 100044, China. Phone number: 86-10-66583802 Mobile: 86-13611115100
Qian Jiang, M.D. Peking University People's Hospital, Peking University Institute of Hematology No. 11 Xizhimen South Street, Beijing, 100044, China. Phone number: 86-10-66583802 Mobile: 86-13611115100
Nature Structural & Molecular Biology: doi: /nsmb Supplementary Figure 1
 Supplementary Figure 1 U1 inhibition causes a shift of RNA-seq reads from exons to introns. (a) Evidence for the high purity of 4-shU-labeled RNAs used for RNA-seq. HeLa cells transfected with control
Supplementary Figure 1 U1 inhibition causes a shift of RNA-seq reads from exons to introns. (a) Evidence for the high purity of 4-shU-labeled RNAs used for RNA-seq. HeLa cells transfected with control
The role of DNMT3A and HOXA9 hypomethylation in acute myeloid leukemia (AML)
 Campbell Drohan BIOL 463 December 2016 The role of DNMT3A and HOXA9 hypomethylation in acute myeloid leukemia (AML) Introduction Epigenetic modifications of DNA and histones are key to gene regulation
Campbell Drohan BIOL 463 December 2016 The role of DNMT3A and HOXA9 hypomethylation in acute myeloid leukemia (AML) Introduction Epigenetic modifications of DNA and histones are key to gene regulation
Supplementary Figure 1 a
 Supplementary Figure a Normalized expression/tbp (A.U.).6... Trip-br transcripts Trans Trans Trans b..5. Trip-br Ctrl LPS Normalized expression/tbp (A.U.) c Trip-br transcripts. adipocytes.... Trans Trans
Supplementary Figure a Normalized expression/tbp (A.U.).6... Trip-br transcripts Trans Trans Trans b..5. Trip-br Ctrl LPS Normalized expression/tbp (A.U.) c Trip-br transcripts. adipocytes.... Trans Trans
Abbreviations: P- paraffin-embedded section; C, cryosection; Bio-SA, biotin-streptavidin-conjugated fluorescein amplification.
 Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
How do novel molecular genetic markers influence treatment decisions in acute myeloid leukemia?
 ACUTE MYELOID LEUKEMIA: NEWLY DISCOVERED GENES, SCREENS (FOR MINIMAL RESIDUAL DISEASE), AND THERAPEUTIC MEANS How do novel molecular genetic markers influence treatment decisions in acute myeloid leukemia?
ACUTE MYELOID LEUKEMIA: NEWLY DISCOVERED GENES, SCREENS (FOR MINIMAL RESIDUAL DISEASE), AND THERAPEUTIC MEANS How do novel molecular genetic markers influence treatment decisions in acute myeloid leukemia?
Personalized Therapy for Acute Myeloid Leukemia. Patrick Stiff MD Loyola University Medical Center
 Personalized Therapy for Acute Myeloid Leukemia Patrick Stiff MD Loyola University Medical Center 708-327-3216 Major groups of Mutations in AML Targets for AML: Is this Achievable? Chronic Myeloid Leukemia:
Personalized Therapy for Acute Myeloid Leukemia Patrick Stiff MD Loyola University Medical Center 708-327-3216 Major groups of Mutations in AML Targets for AML: Is this Achievable? Chronic Myeloid Leukemia:
New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke
 University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
Changing AML Outcomes via Personalized Medicine: Transforming Cancer Management with Genetic Insight
 Changing AML Outcomes via Personalized Medicine: Transforming Cancer Management with Genetic Insight Co-Moderators: Rick Winneker, PhD, Senior Vice President, Research, Leukemia & Lymphoma Society Mike
Changing AML Outcomes via Personalized Medicine: Transforming Cancer Management with Genetic Insight Co-Moderators: Rick Winneker, PhD, Senior Vice President, Research, Leukemia & Lymphoma Society Mike
Supplementary Materials
 Supplementary Materials 1 Supplementary Table 1. List of primers used for quantitative PCR analysis. Gene name Gene symbol Accession IDs Sequence range Product Primer sequences size (bp) β-actin Actb gi
Supplementary Materials 1 Supplementary Table 1. List of primers used for quantitative PCR analysis. Gene name Gene symbol Accession IDs Sequence range Product Primer sequences size (bp) β-actin Actb gi
TET2 mutations were predictive of inferior prognosis in the presence of ASXL1 mutations in patients with chronic myelomonocytic leukemia
 Short Report TET2 mutations were predictive of inferior prognosis in the presence of ASXL1 mutations in patients with chronic myelomonocytic leukemia Yajuan Cui 1,2 *, Hongyan Tong 3 *, Xin Du 4 *, Bing
Short Report TET2 mutations were predictive of inferior prognosis in the presence of ASXL1 mutations in patients with chronic myelomonocytic leukemia Yajuan Cui 1,2 *, Hongyan Tong 3 *, Xin Du 4 *, Bing
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Patel JP, Gönen M, Figueroa ME, et al. Prognostic relevance
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Patel JP, Gönen M, Figueroa ME, et al. Prognostic relevance
Objectives. Morphology and IHC. Flow and Cyto FISH. Testing for Heme Malignancies 3/20/2013
 Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Supplemental Data. Shin et al. Plant Cell. (2012) /tpc YFP N
 MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
MYC YFP N PIF5 YFP C N-TIC TIC Supplemental Data. Shin et al. Plant Cell. ()..5/tpc..95 Supplemental Figure. TIC interacts with MYC in the nucleus. Bimolecular fluorescence complementation assay using
Supplementary Figure 1 MicroRNA expression in human synovial fibroblasts from different locations. MicroRNA, which were identified by RNAseq as most
 Supplementary Figure 1 MicroRNA expression in human synovial fibroblasts from different locations. MicroRNA, which were identified by RNAseq as most differentially expressed between human synovial fibroblasts
Supplementary Figure 1 MicroRNA expression in human synovial fibroblasts from different locations. MicroRNA, which were identified by RNAseq as most differentially expressed between human synovial fibroblasts
a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53
 1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
1 2 3 4 5 6 7 8 9 10 Supplementary Figure 1. Induction of p53 LOH by MADM. a) Primary cultures derived from the pancreas of an 11-week-old Pdx1-Cre; K-MADM-p53 mouse revealed increased p53 KO/KO (green,
Relationship between SPOP mutation and breast cancer in Chinese population
 Relationship between SPOP mutation and breast cancer in Chinese population M.A. Khan 1 *, L. Zhu 1 *, M. Tania 1, X.L. Xiao 2 and J.J. Fu 1 1 Key Laboratory of Epigenetics and Oncology, The Research Center
Relationship between SPOP mutation and breast cancer in Chinese population M.A. Khan 1 *, L. Zhu 1 *, M. Tania 1, X.L. Xiao 2 and J.J. Fu 1 1 Key Laboratory of Epigenetics and Oncology, The Research Center
Beta Thalassemia Case Study Introduction to Bioinformatics
 Beta Thalassemia Case Study Sami Khuri Department of Computer Science San José State University San José, California, USA sami.khuri@sjsu.edu www.cs.sjsu.edu/faculty/khuri Outline v Hemoglobin v Alpha
Beta Thalassemia Case Study Sami Khuri Department of Computer Science San José State University San José, California, USA sami.khuri@sjsu.edu www.cs.sjsu.edu/faculty/khuri Outline v Hemoglobin v Alpha
Welcome and Introductions
 Information for Patients With Acute Myeloid Leukemia (AML) Welcome and Introductions Information for Patients With Acute Myeloid Leukemia (AML) Mark B. Juckett, MD Vice Chair for Clinical Affairs and Quality
Information for Patients With Acute Myeloid Leukemia (AML) Welcome and Introductions Information for Patients With Acute Myeloid Leukemia (AML) Mark B. Juckett, MD Vice Chair for Clinical Affairs and Quality
MicroRNAs: the primary cause or a determinant of progression in leukemia?
 MicroRNAs: the primary cause or a determinant of progression in leukemia? The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters. Citation
MicroRNAs: the primary cause or a determinant of progression in leukemia? The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters. Citation
Recurrent DNMT3A R882 Mutations in Chinese Patients with Acute Myeloid Leukemia and Myelodysplastic Syndrome
 Recurrent DNMT3A R882 Mutations in Chinese Patients with Acute Myeloid Leukemia and Myelodysplastic Syndrome Jiang Lin 1,2, Dong-ming Yao 1, Jun Qian 1 *, Qin Chen 1, Wei Qian 2 *, Yun Li 1, Jing Yang
Recurrent DNMT3A R882 Mutations in Chinese Patients with Acute Myeloid Leukemia and Myelodysplastic Syndrome Jiang Lin 1,2, Dong-ming Yao 1, Jun Qian 1 *, Qin Chen 1, Wei Qian 2 *, Yun Li 1, Jing Yang
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1
 Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards
 Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards incubated in 100 % ethanol overnight at 4 C and embedded in
Toluidin-Staining of mast cells Ear tissue was fixed with Carnoy (60% ethanol, 30% chloroform, 10% acetic acid) overnight at 4 C, afterwards incubated in 100 % ethanol overnight at 4 C and embedded in
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
Evolving Targeted Management of Acute Myeloid Leukemia
 Evolving Targeted Management of Acute Myeloid Leukemia Jessica Altman, MD Robert H. Lurie Comprehensive Cancer Center of Northwestern University Learning Objectives Identify which mutations should be assessed
Evolving Targeted Management of Acute Myeloid Leukemia Jessica Altman, MD Robert H. Lurie Comprehensive Cancer Center of Northwestern University Learning Objectives Identify which mutations should be assessed
SUPPLEMENTARY FIG. S3. Kaplan Meier survival analysis followed with log-rank test of de novo acute myeloid leukemia patients selected by age <60, IA
 Supplementary Data Supplementary Appendix A: Treatment Protocols Treatment protocols of 123 cases patients were treated with the protocols as follows: 110 patients received standard DA (daunorubicin 45
Supplementary Data Supplementary Appendix A: Treatment Protocols Treatment protocols of 123 cases patients were treated with the protocols as follows: 110 patients received standard DA (daunorubicin 45
Molecular Detection of BCR/ABL1 for the Diagnosis and Monitoring of CML
 Molecular Detection of BCR/ABL1 for the Diagnosis and Monitoring of CML Imran Mirza, MD, MS, FRCPC Pathology & Laboratory Medicine Institute Sheikh Khalifa Medical City, Abu Dhabi, UAE. imirza@skmc.ae
Molecular Detection of BCR/ABL1 for the Diagnosis and Monitoring of CML Imran Mirza, MD, MS, FRCPC Pathology & Laboratory Medicine Institute Sheikh Khalifa Medical City, Abu Dhabi, UAE. imirza@skmc.ae
Recommended Timing for Transplant Consultation
 REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
REFERRAL GUIDELINES Recommended Timing for Transplant Consultation Published jointly by the National Marrow Donor Program /Be The Match and the American Society for Blood and Marrow Transplantation BeTheMatchClinical.org
News Release. Title Integrated molecular profiling of juvenile myelomonocytic leukemia
 News Release Title Integrated molecular profiling of juvenile myelomonocytic leukemia Key Points We identified ALK/ROS1 tyrosine kinase fusions (DCTN1-ALK, RANBP2-ALK, and TBL1XR1-ROS1) in patients with
News Release Title Integrated molecular profiling of juvenile myelomonocytic leukemia Key Points We identified ALK/ROS1 tyrosine kinase fusions (DCTN1-ALK, RANBP2-ALK, and TBL1XR1-ROS1) in patients with
Methylation status of SOCS1 and SOCS3 in BCR-ABL negative and. JAK2V617F negative chronic myeloproliferative disorders.
 Methylation status of SOCS1 and SOCS3 in BCR-ABL negative and JAK2V617F negative chronic myeloproliferative disorders. To the Editor BCR-ABL negative Chronic Myeloproliferative Disorders (s) are a heterogeneous
Methylation status of SOCS1 and SOCS3 in BCR-ABL negative and JAK2V617F negative chronic myeloproliferative disorders. To the Editor BCR-ABL negative Chronic Myeloproliferative Disorders (s) are a heterogeneous
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017
 Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Table S1. Oligonucleotides used for the in-house RT-PCR assays targeting the M, H7 or N9. Assay (s) Target Name Sequence (5 3 ) Comments
 SUPPLEMENTAL INFORMATION 2 3 Table S. Oligonucleotides used for the in-house RT-PCR assays targeting the M, H7 or N9 genes. Assay (s) Target Name Sequence (5 3 ) Comments CDC M InfA Forward (NS), CDC M
SUPPLEMENTAL INFORMATION 2 3 Table S. Oligonucleotides used for the in-house RT-PCR assays targeting the M, H7 or N9 genes. Assay (s) Target Name Sequence (5 3 ) Comments CDC M InfA Forward (NS), CDC M
Chronic myelomonocytic leukemia. Lymphoma Tumor Board. May 26, 2017
 Chronic myelomonocytic leukemia Lymphoma Tumor Board May 26, 2017 Myeloproliferative Neoplasms CMML has an estimated incidence of less than 1 per 100,000 persons per year Myeloproliferative neoplasms (MPN)
Chronic myelomonocytic leukemia Lymphoma Tumor Board May 26, 2017 Myeloproliferative Neoplasms CMML has an estimated incidence of less than 1 per 100,000 persons per year Myeloproliferative neoplasms (MPN)
Early Clearance of Peripheral Blood Blasts Predicts Response to Induction Chemotherapy in Acute Myeloid Leukemia
 Early Clearance of Peripheral Blood Blasts Predicts Response to Induction Chemotherapy in Acute Myeloid Leukemia Martha Arellano, MD 1 ; Suchita Pakkala, MD 1 ; Amelia Langston, MD 1 ; Mourad Tighiouart,
Early Clearance of Peripheral Blood Blasts Predicts Response to Induction Chemotherapy in Acute Myeloid Leukemia Martha Arellano, MD 1 ; Suchita Pakkala, MD 1 ; Amelia Langston, MD 1 ; Mourad Tighiouart,
Supplementary Figure 1. ROS induces rapid Sod1 nuclear localization in a dosagedependent manner. WT yeast cells (SZy1051) were treated with 4NQO at
 Supplementary Figure 1. ROS induces rapid Sod1 nuclear localization in a dosagedependent manner. WT yeast cells (SZy1051) were treated with 4NQO at different concentrations for 30 min and analyzed for
Supplementary Figure 1. ROS induces rapid Sod1 nuclear localization in a dosagedependent manner. WT yeast cells (SZy1051) were treated with 4NQO at different concentrations for 30 min and analyzed for
GENETIC TESTING FOR FLT3, NPM1 AND CEBPA VARIANTS IN CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA
 CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
CYTOGENETICALLY NORMAL ACUTE MYELOID LEUKEMIA Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures,
Background CPX-351. Lancet J, et al. J Clin Oncol. 2017;35(suppl): Abstract 7035.
 Overall Survival (OS) With Versus in Older Adults With Newly Diagnosed, Therapy-Related Acute Myeloid Leukemia (taml): Subgroup Analysis of a Phase 3 Study Abstract 7035 Lancet JE, Rizzieri D, Schiller
Overall Survival (OS) With Versus in Older Adults With Newly Diagnosed, Therapy-Related Acute Myeloid Leukemia (taml): Subgroup Analysis of a Phase 3 Study Abstract 7035 Lancet JE, Rizzieri D, Schiller
Supplementary Figures
 Supplementary Figures Supplementary Figure 1. H3F3B expression in lung cancer. a. Comparison of H3F3B expression in relapsed and non-relapsed lung cancer patients. b. Prognosis of two groups of lung cancer
Supplementary Figures Supplementary Figure 1. H3F3B expression in lung cancer. a. Comparison of H3F3B expression in relapsed and non-relapsed lung cancer patients. b. Prognosis of two groups of lung cancer
Johann Hitzler, MD, FRCPC, FAAP Jacqueline Halton, MD, FRCPC Jason D. Pole, PhD
 Photo by Tynan Studio Johann Hitzler, MD, FRCPC, FAAP Jacqueline Halton, MD, FRCPC Jason D. Pole, PhD 96 Atlas of Childhood Cancer in Ontario (1985-2004) Chapter 6: Leukemia 6 Leukemia Atlas of Childhood
Photo by Tynan Studio Johann Hitzler, MD, FRCPC, FAAP Jacqueline Halton, MD, FRCPC Jason D. Pole, PhD 96 Atlas of Childhood Cancer in Ontario (1985-2004) Chapter 6: Leukemia 6 Leukemia Atlas of Childhood
MRD detection in AML. Adriano Venditti Hematology Fondazione Policlinico Tor Vergata Rome
 MRD detection in AML Adriano Venditti Hematology Fondazione Policlinico Tor Vergata Rome Determinants of Treatment Response Leukemia Tumor burden Growth potential Drug resistance Karyotype Genetics Host
MRD detection in AML Adriano Venditti Hematology Fondazione Policlinico Tor Vergata Rome Determinants of Treatment Response Leukemia Tumor burden Growth potential Drug resistance Karyotype Genetics Host
Acute Myeloid Leukemia Progress at last
 Acute Myeloid Leukemia Progress at last Bruno C. Medeiros, MD September 9, 217 Introduction Mechanisms of leukemogenesis Emerging therapies in AML Previously untreated AML Relapsed and refractory patients
Acute Myeloid Leukemia Progress at last Bruno C. Medeiros, MD September 9, 217 Introduction Mechanisms of leukemogenesis Emerging therapies in AML Previously untreated AML Relapsed and refractory patients
Review Article The Epigenetic Landscape of Acute Myeloid Leukemia
 Advances in Hematology, Article ID 103175, 15 pages http://dx.doi.org/10.1155/2014/103175 Review Article The Epigenetic Landscape of Acute Myeloid Leukemia Emma Conway O Brien, Steven Prideaux, and Timothy
Advances in Hematology, Article ID 103175, 15 pages http://dx.doi.org/10.1155/2014/103175 Review Article The Epigenetic Landscape of Acute Myeloid Leukemia Emma Conway O Brien, Steven Prideaux, and Timothy
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation
 a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
a resource for physicians Recommended Referral Timing for Stem Cell Transplant Evaluation This resource has been developed to help guide you regarding the appropriate timing and conditions for a referral
Supplemental Information. Cancer-Associated Fibroblasts Neutralize. the Anti-tumor Effect of CSF1 Receptor Blockade
 Cancer Cell, Volume 32 Supplemental Information Cancer-Associated Fibroblasts Neutralize the Anti-tumor Effect of CSF1 Receptor Blockade by Inducing PMN-MDSC Infiltration of Tumors Vinit Kumar, Laxminarasimha
Cancer Cell, Volume 32 Supplemental Information Cancer-Associated Fibroblasts Neutralize the Anti-tumor Effect of CSF1 Receptor Blockade by Inducing PMN-MDSC Infiltration of Tumors Vinit Kumar, Laxminarasimha
Mixed Phenotype Acute Leukemias
 Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Figure S1. Analysis of genomic and cdna sequences of the targeted regions in WT-KI and
 Figure S1. Analysis of genomic and sequences of the targeted regions in and indicated mutant KI cells, with WT and corresponding mutant sequences underlined. (A) cells; (B) K21E-KI cells; (C) D33A-KI cells;
Figure S1. Analysis of genomic and sequences of the targeted regions in and indicated mutant KI cells, with WT and corresponding mutant sequences underlined. (A) cells; (B) K21E-KI cells; (C) D33A-KI cells;
Future Targets for Acute Myeloid Leukemia
 Future Targets for Acute Myeloid Leukemia E. Anders Kolb, M.D. Director, Nemours Center for Cancer and Blood Disorders Chair, Children s Oncology Group Myeloid Disease Committee Future Targets for Acute
Future Targets for Acute Myeloid Leukemia E. Anders Kolb, M.D. Director, Nemours Center for Cancer and Blood Disorders Chair, Children s Oncology Group Myeloid Disease Committee Future Targets for Acute
September 20, Submitted electronically to: Cc: To Whom It May Concern:
 History Study (NOT-HL-12-147), p. 1 September 20, 2012 Re: Request for Information (RFI): Building a National Resource to Study Myelodysplastic Syndromes (MDS) The MDS Cohort Natural History Study (NOT-HL-12-147).
History Study (NOT-HL-12-147), p. 1 September 20, 2012 Re: Request for Information (RFI): Building a National Resource to Study Myelodysplastic Syndromes (MDS) The MDS Cohort Natural History Study (NOT-HL-12-147).
All patients with FLT3 mutant AML should receive midostaurin-based induction therapy. Not so fast!
 All patients with FLT3 mutant AML should receive midostaurin-based induction therapy Not so fast! Harry P. Erba, M.D., Ph.D. Professor, Internal Medicine Director, Hematologic Malignancy Program University
All patients with FLT3 mutant AML should receive midostaurin-based induction therapy Not so fast! Harry P. Erba, M.D., Ph.D. Professor, Internal Medicine Director, Hematologic Malignancy Program University
ADVANCES IN CHILDHOOD ACUTE LEUKEMIAS : GENERAL OVERVIEW
 ADVANCES IN CHILDHOOD ACUTE LEUKEMIAS : GENERAL OVERVIEW Danièle SOMMELET European Scientific Seminar Luxemburg, 3.11.2009 1 Definition of acute leukemias Malignant process coming from lymphoid (85 %)
ADVANCES IN CHILDHOOD ACUTE LEUKEMIAS : GENERAL OVERVIEW Danièle SOMMELET European Scientific Seminar Luxemburg, 3.11.2009 1 Definition of acute leukemias Malignant process coming from lymphoid (85 %)
Beta Thalassemia Sami Khuri Department of Computer Science San José State University Spring 2015
 Bioinformatics in Medical Product Development SMPD 287 Three Beta Thalassemia Sami Khuri Department of Computer Science San José State University Hemoglobin Outline Anatomy of a gene Hemoglobinopathies
Bioinformatics in Medical Product Development SMPD 287 Three Beta Thalassemia Sami Khuri Department of Computer Science San José State University Hemoglobin Outline Anatomy of a gene Hemoglobinopathies
Expression of Selected Inflammatory Cytokine Genes in Bladder Biopsies
 Borneo Journal of Resource Science and Technology (2013) 3(2): 15-20 Expression of Selected Inflammatory Cytokine Genes in Bladder Biopsies EDMUND UI-HANG SIM *1, NUR DIANA ANUAR 2, TENG-AIK ONG 3, GUAN-
Borneo Journal of Resource Science and Technology (2013) 3(2): 15-20 Expression of Selected Inflammatory Cytokine Genes in Bladder Biopsies EDMUND UI-HANG SIM *1, NUR DIANA ANUAR 2, TENG-AIK ONG 3, GUAN-
Blast transformation in chronic myelomonocytic leukemia: Risk factors, genetic features, survival, and treatment outcome
 RESEARCH ARTICLE Blast transformation in chronic myelomonocytic leukemia: Risk factors, genetic features, survival, and treatment outcome AJH Mrinal M. Patnaik, 1 Emnet A. Wassie, 1 Terra L. Lasho, 2 Curtis
RESEARCH ARTICLE Blast transformation in chronic myelomonocytic leukemia: Risk factors, genetic features, survival, and treatment outcome AJH Mrinal M. Patnaik, 1 Emnet A. Wassie, 1 Terra L. Lasho, 2 Curtis
Baseline clinical characteristics for the 81 CMML patients Routine diagnostic testing and statistical analyses... 3
 Next-Generation Sequencing Technology Reveals a Characteristic Pattern of Molecular Mutations in 72.8% of Chronic Myelomonocytic Leukemia (CMML) by Detecting Frequent Alterations in TET2, CBL, RAS, and
Next-Generation Sequencing Technology Reveals a Characteristic Pattern of Molecular Mutations in 72.8% of Chronic Myelomonocytic Leukemia (CMML) by Detecting Frequent Alterations in TET2, CBL, RAS, and
Variant interpretation exercise. ACGS Somatic Variant Interpretation Workshop Joanne Mason 21/09/18
 Variant interpretation exercise ACGS Somatic Variant Interpretation Workshop Joanne Mason 21/09/18 Format of exercise Compile a list of tricky variants across solid cancer and haematological malignancy.
Variant interpretation exercise ACGS Somatic Variant Interpretation Workshop Joanne Mason 21/09/18 Format of exercise Compile a list of tricky variants across solid cancer and haematological malignancy.
Supplementary Information
 Supplementary Information Detection and differential diagnosis of colon cancer by a cumulative analysis of promoter methylation Qiong Yang 1,3*, Ying Dong 2,3, Wei Wu 1, Chunlei Zhu 1, Hui Chong 1, Jiangyang
Supplementary Information Detection and differential diagnosis of colon cancer by a cumulative analysis of promoter methylation Qiong Yang 1,3*, Ying Dong 2,3, Wei Wu 1, Chunlei Zhu 1, Hui Chong 1, Jiangyang
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH )
 Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia
 Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia Hartmut Döhner Medical Director, Department of Internal Medicine III Director, Comprehensive Cancer Center Ulm Ulm University,
Impact of Biomarkers in the Management of Patients with Acute Myeloid Leukemia Hartmut Döhner Medical Director, Department of Internal Medicine III Director, Comprehensive Cancer Center Ulm Ulm University,
Department of Leukemia, The University of Texas M.D. Anderson Cancer Center, Houston, Texas; 2 Sunesis Pharmaceuticals, Inc, South San Francisco
 Phase I/II Study of Vosaroxin and Decitabine in Newly Diagnosed Older Patients with Acute Myeloid Leukemia (AML) and High Risk Myelodysplastic Syndrome (MDS) Naval Daver 1, Hagop Kantarjian 1, Guillermo
Phase I/II Study of Vosaroxin and Decitabine in Newly Diagnosed Older Patients with Acute Myeloid Leukemia (AML) and High Risk Myelodysplastic Syndrome (MDS) Naval Daver 1, Hagop Kantarjian 1, Guillermo
TCF3 breakpoints of TCF3-PBX1 (patients 1a 5a) and TCF3-HLF (patients 6a 9a and11a) translocations.
 Supplementary Figure 1 TCF3 breakpoints of TCF3-PBX1 (patients 1a 5a) and TCF3-HLF (patients 6a 9a and11a) translocations. The CpG motifs closest to the breakpoints are highlighted in red boxes and the
Supplementary Figure 1 TCF3 breakpoints of TCF3-PBX1 (patients 1a 5a) and TCF3-HLF (patients 6a 9a and11a) translocations. The CpG motifs closest to the breakpoints are highlighted in red boxes and the
AML Genomics 11/27/17. Normal neutrophil maturation. Acute Myeloid Leukemia (AML) = block in differentiation. Myelomonocy9c FAB M5
 AML Genomics 1 Normal neutrophil maturation Acute Myeloid Leukemia (AML) = block in differentiation AML with minimal differen9a9on FAB M1 Promyelocy9c leukemia FAB M3 Myelomonocy9c FAB M5 2 1 Principle
AML Genomics 1 Normal neutrophil maturation Acute Myeloid Leukemia (AML) = block in differentiation AML with minimal differen9a9on FAB M1 Promyelocy9c leukemia FAB M3 Myelomonocy9c FAB M5 2 1 Principle
RUNX1 and FPD/AML Translational Research. The Leukemia and Lymphoma Society / Babich Family Foundation Partnership. September 2016
 www.lls.org www.runx1.com RUNX1 and FPD/AML Translational Research The Leukemia and Lymphoma Society / Babich Family Foundation Partnership September 2016 Prepared by L. Greenberger, PhD Chief Scientific
www.lls.org www.runx1.com RUNX1 and FPD/AML Translational Research The Leukemia and Lymphoma Society / Babich Family Foundation Partnership September 2016 Prepared by L. Greenberger, PhD Chief Scientific
RESEARCH ARTICLE. Firoz Ahmad 1, Rupali Mohota 1, Savita Sanap 1, Swarna Mandava 2, Bibhu Ranjan Das 1 * Abstract. Introduction
 DOI:http://dx.doi.org/10.7314/APJCP.2014.15.3.1247 RESEARCH ARTICLE Molecular Evaluation of DNMT3A and IDH1/2 Gene Mutation: Frequency, Distribution Pattern and Associations with Additional Molecular Markers
DOI:http://dx.doi.org/10.7314/APJCP.2014.15.3.1247 RESEARCH ARTICLE Molecular Evaluation of DNMT3A and IDH1/2 Gene Mutation: Frequency, Distribution Pattern and Associations with Additional Molecular Markers
NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia
 Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Expression of Micro-RNA 128 and Let-7b in Pediatric Acute Lymphoblastic Leukemia Cases
 DOI:10.22034/APJCP.2018.19.8.2263 RESEARCH ARTICLE Editorial Process: Submission:03/05/2018 Acceptance:07/17/2018 Expression of Micro-RNA 128 and Let-7b in Pediatric Acute Lymphoblastic Leukemia Cases
DOI:10.22034/APJCP.2018.19.8.2263 RESEARCH ARTICLE Editorial Process: Submission:03/05/2018 Acceptance:07/17/2018 Expression of Micro-RNA 128 and Let-7b in Pediatric Acute Lymphoblastic Leukemia Cases
Supplementary Figure 1
 Supplementary Figure 1 Supplementary Figure 1: Cryopreservation alters CD62L expression by CD4 T cells. Freshly isolated (left) or cryopreserved PBMCs (right) were stained with the mix of antibodies described
Supplementary Figure 1 Supplementary Figure 1: Cryopreservation alters CD62L expression by CD4 T cells. Freshly isolated (left) or cryopreserved PBMCs (right) were stained with the mix of antibodies described
Treatments and Current Research in Leukemia. Richard A. Larson, MD University of Chicago
 Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Prospective study of MTHFR genetic polymorphisms as a possible etiology of male infertility
 Prospective study of MTHFR genetic polymorphisms as a possible etiology of male infertility S.-S. Li 1, J. Li 1, Z. Xiao 2, A.-G. Ren 3 and L. Jin 3 1 Beijing Obstetrics and Gynecology Hospital, Capital
Prospective study of MTHFR genetic polymorphisms as a possible etiology of male infertility S.-S. Li 1, J. Li 1, Z. Xiao 2, A.-G. Ren 3 and L. Jin 3 1 Beijing Obstetrics and Gynecology Hospital, Capital
Leukemia and subsequent solid tumors among patients with myeloproliferative neoplasms
 Leukemia and subsequent solid tumors among patients with myeloproliferative neoplasms Tiziano Barbui (tbarbui@asst-pg23.it Hematology and Research Foundation,Ospedale Papa Giovanni XXIII, Bergamo Italy
Leukemia and subsequent solid tumors among patients with myeloproliferative neoplasms Tiziano Barbui (tbarbui@asst-pg23.it Hematology and Research Foundation,Ospedale Papa Giovanni XXIII, Bergamo Italy
HTA. Efficacies of HTA regimen for acute myeloid leukemia AML. J of Wannan Medical College HHT THP AML 1 DA AML
 564 1002-0217 2015 06-0564 - 04 HTA 241001 HHT THP Ara-C HTA AML 2006 8 ~ 2013 12 15 AML HTA 1 CR + CRi PR OR CR + PR DA 23 HTA 15 1 CR 11 PR 2 OR 13 DA 23 1 CR 14 PR 3 OR 17 HTA CR DA P > 0. 05 HTA AML
564 1002-0217 2015 06-0564 - 04 HTA 241001 HHT THP Ara-C HTA AML 2006 8 ~ 2013 12 15 AML HTA 1 CR + CRi PR OR CR + PR DA 23 HTA 15 1 CR 11 PR 2 OR 13 DA 23 1 CR 14 PR 3 OR 17 HTA CR DA P > 0. 05 HTA AML
Supplementary Table 2. Conserved regulatory elements in the promoters of CD36.
 Supplementary Table 1. RT-qPCR primers for CD3, PPARg and CEBP. Assay Forward Primer Reverse Primer 1A CAT TTG TGG CCT TGT GCT CTT TGA TGA GTC ACA GAA AGA ATC AAT TC 1B AGG AAA TGA ACT GAT GAG TCA CAG
Supplementary Table 1. RT-qPCR primers for CD3, PPARg and CEBP. Assay Forward Primer Reverse Primer 1A CAT TTG TGG CCT TGT GCT CTT TGA TGA GTC ACA GAA AGA ATC AAT TC 1B AGG AAA TGA ACT GAT GAG TCA CAG
Acute Myeloid Leukemia
 Acute Myeloid Leukemia Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University Outline Molecular biology Chemotherapy and Hypomethylating agent Novel Therapy
Acute Myeloid Leukemia Pimjai Niparuck Division of Hematology, Department of Medicine Ramathibodi Hospital, Mahidol University Outline Molecular biology Chemotherapy and Hypomethylating agent Novel Therapy
Clinical significance of serum mir-21 in breast cancer compared with CA153 and CEA
 Original Article Clinical significance of serum mir-21 in breast cancer compared with CA153 and CEA Jianjian Gao, Qingyun Zhang, Jianjun Xu, Lijuan Guo, Xuefeng Li Key Laboratory of Carcinogenesis and
Original Article Clinical significance of serum mir-21 in breast cancer compared with CA153 and CEA Jianjian Gao, Qingyun Zhang, Jianjun Xu, Lijuan Guo, Xuefeng Li Key Laboratory of Carcinogenesis and
CME/SAM. Mixed Phenotype Acute Leukemia
 AJCP / Original Article Mixed Phenotype Acute Leukemia A Study of 61 Cases Using World Health Organization and European Group for the Immunological Classification of Leukaemias Criteria Olga K. Weinberg,
AJCP / Original Article Mixed Phenotype Acute Leukemia A Study of 61 Cases Using World Health Organization and European Group for the Immunological Classification of Leukaemias Criteria Olga K. Weinberg,
Molecular Pathology of Ovarian Carcinoma with Morphological Correlation
 Molecular athology of Ovarian Carcinoma with Morphological Correlation Kathleen R. Cho, M.D. Comprehensive Cancer Center and Departments of athology and Internal Medicine University of Michigan Medical
Molecular athology of Ovarian Carcinoma with Morphological Correlation Kathleen R. Cho, M.D. Comprehensive Cancer Center and Departments of athology and Internal Medicine University of Michigan Medical
