Medical / Microbiology
|
|
|
- Lenard Hoover
- 6 years ago
- Views:
Transcription
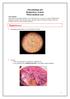
1 Medical / Microbiology Pseudomonas aeruginosa biofilms in the lungs of Cystic Fibrosis Patients Thomas Bjarnsholt, PhD, Associate professor 1,2, Peter Østrup Jensen, PhD 2 and Niels Høiby, MD, Dr. Med, Professor 1,2 The article is written for Cystic Fibrosis Worldwide, based upon our scientific work published together with: Mark J. Fiandaca 3, Jette Pedersen 4, Christine Rønne Hansen 6, Claus Bøgelund Andersen 5, Tacjana Pressler 6 and Michael Givskov 1. ( 1 International Sundhed, Immunologi og Mikrobiologi, Sundhedsvidenskabeligt Fakultet, Københavns Universitet. 2 Klinisk Mikrobiologisk afd. 3 AdvanDx, Inc. Woburn, Massachusetts, USA, 4 Bartholin Institutet, 5 Patologisk afd., Rigshospitalet og 6 CF Centret, Rigshospitalet) Please refer to the original scientific article published by Pediatric Pulmonology for all the results and references included in this present article. Introduction Recent research indicates that chronic bacterial infections are caused by the ability of bacteria to organize themselves in microcolonies also called biofilms. In this state the bacteria are imbedded in a self produced protective matrix, often with surrounding inflammatory cells. Bacteria living in biofilms are very well protected against antibiotics and the host defense. In the past, CF patients suffered from severe lung infections caused by Haemophilus influenzae, Streptococcus pneumonia, and especially Staphylococcus aureus, resulting in high mortality in the early childhood. These bacteria have been treatable the last 30 years, but other bacteria such as Pseudomonas aeruginosa, Burkholderia cepacia complex, Stenotrophomonas maltophilia and Achromobacter xylosoxidans have become a serious problem. Today up to 80% of young adults suffering from CF are chronically infected with P. aeruginosa. P. aeruginosa in general P. aeruginosa is an opportunistic human pathogen. This means that the bacterium only infects individuals with a compromised host defense such as people with CF. The bacterium is a low virulent pathogen because its disease causing properties in the initial infection are few and the infection has a slow progress. In contrast, highly virulent bacteria, such as haemolytic streptococci and pneumococci, cause an acute infection with fever and inflammation. P. aeruginosa can be isolated from most environments: soil, marshes, the sea, plants and mammal tissue. In hospital environments P. aeruginosa grows in moist reservoirs such as food, cut flowers, sinks, toilets, floor mops, dialysis equipment, and even in disinfectants. P. aeruginosa has become synonym with the lung infection of people suffering from CF. In CF lungs, P. aeruginosa exists as free single bacteria (planktonic) or in enclaves of bacteria, in which the bacteria grow as biofilms. P. aeruginosa may become extremely slimy, a form called mucoid P. aeruginosa. This is caused by a genetic change of the bacterium (mutation), resulting in the release of large quantatives of alginate (a kind of sugar). The change to mucoid strengthens its defense capacity against antibiotics and the host defense even further and may provoke inflammation. Why a scientific demonstration of biofilms in CF Since 1976 great success in treating CF patients, suffering from chronic P. aeruginosa lung infection, has been obtained by intensive treatment using high concentrations of antibiotics at the Copenhagen CF center. This was initially done by routinely i.v. anti- P. aeruginosa treatment for 14 days, every third month. Since 1987 daily inhalation of antibiotics was added. Before 1976 only 50% of the CF patients would survive 5 years of chronic P. aeruginosa lung infection. Today most survive for decades with chronic infection.
2 Despite intensive treatment of chronic P. aeruginosa infections the bacteria remain. The intensive treatment postpones and reduces the damage caused by the chronic infection, but can not eradicate it. During the chronic P. aeruginosa infection the CF patients experience a continuous degradation of lung tissue. This is caused in part by the infection and part by the inflammatory processes (the body s reaction to the infection). The consequence is a decline in the lung function, which is the primary cause of death for CF patients. The present study was based on the following assumption (hypothesis): The intensive usage of antibiotics delays the damage of the chronic P. aeruginosa infection, but does not stop the bacteria from forming biofilms in the lungs. To test our hypothesis we have compared the lungs from two different groups of CF patients. Group 1: CF patients suffering from chronic P. aeruginosa infection treated intensively with antibiotics. Group 2: CF patients suffering from chronic P. aeruginosa infection NOT treated intensively with antibiotics. The scientific work material Lungs in group 1 were obtained from 3 CF patients, age range: years, having had lung transplantation due to their chronic P. aeruginosa lung infection. The patients have had chronic P. aeruginosa infections on average for 27 years when transplanted. The lungs were collected with acceptance of the patients as approved by the Danish Scientific Ethical Board. For group 2 we used material from 11 CF patients who died from 1974 to Nine of the CF patients, age range: 3-20 years, died due to chronic P. aeruginosa lung infection. The duration of the chronic lung infection was on average 3.5 years (1 month 8 years). At this time the mortality of CF patients was high at Rigshospitalet (University Hospital of Copenhagen). P. aeruginosa was not yet recognized as an important CF pathogen and the infection was only treated in case of severe clinical conditions. No regular maintanence theraphy was used. Lungs for control were obtained from 2 CF patients who died at 15 and 18 years and did not suffer from P. aeruginosa infection. Lungs belonging to group 2 were collected at Rigshospitalet before the intensive antibiotic treatment regime was initiated in 1976 by one of the authors (NH), who conducted a medical research project involving lung autopsies for immune pathology and bacteriology. Additionally, 77 recent sputum samples from chronically infected, present CF patients, age range: years, was examined and compared to the biofilms produced by P. aeruginosa in the lower part of the lungs. The scientific work method We used a species specific staining of the bacteria to identify and localize the bacteria in the lungs and sputum. In addition, we used a traditional non-specific stain, the Gram stain. In all the lungs, we examined all the relevant areas such as the bronchi, alveoli, inflamed tissue and healthy tissue. The scientific work Results Sputum P. aeruginosa was the only bacteria that could be isolated from the sputum samples. The mucoid P. aeruginosa dominated the samples though the non-mucoid was present as well. P. aeruginosa appeared both as single cells (planktonic) and as aggregates in the sputum (figure 1). The single bacteria were unevenly distributed and separated from the microcolonies. The microcolonies were of different sizes and shapes, and randomly distributed throughout the samples. Most of the microcolonies were surrounded by PMNs (white blood cells), but in a few cases PMNs were detected inside the aggregates (figure 1c). The aggregates bear resemblance to Gram-stained, mucoid P. aeruginosa colonies grown in the laboratory. Lungs from the intensively treated chronically infected CF patients group 1 The lung function of the explanted lungs was reduced to an extent that requires lung transplantation for the patient to survive. The bacteria were mainly localized in the conductive zone (the upper part of the lung with large and small bronchi, which function as pipes transporting air back and forth to the alveoli) (figure 2). All of the bacteria were imbedded in mucus plugs. The mucus plugs containing bacteria varied much in size and spatial orientation. The bacteria within the mucus were dominated by aggregates and only few planktonic bacteria were detected. Vast amount of PMNs surrounded the aggregates. The bacteria were not found adhering to the epithelial wall, demonstrating that the bacteria grew within the mucus and not in the lung
3 tissue. Using specific antibodies against alginate we observed a majority of mucoid P. aeruginosa aggregates intraluminally in the conductive zone together with few possible non-mucoid planktonic bacteria. P. aeruginosa was the only detected bacteria in this study. In the respiratory part of the lungs (the lower part the alveoli where the gas-exchange with the blood occur) we saw both dead alveoli and air filled healthy alveoli (figure 2 G-I). Relatively few bacteria were detected in the respiratory part of the lungs as compared to the conductive part. We found both a few single planktonic cells and small aggregates in the respiratory zone, however the planktonic bacteria were always phagocytosed (eaten) by PMNs and the aggregated bacteria were closely surrounded by PMNs (figure 2 I). Lungs from the non- intensively treated chronically infected CF patients group 2 In group 2, the bacteria in the conductive zone were also found inside the mucus surrounded by an abundance of PMNs, with no bacteria adhering to the airway epithelia (figure 3). In striking contrast to the explanted group 1 lungs, the alveoli of the respiratory zone were filled with aggregating bacteria and PMNs (figure 3 G and H). Most of the lung tissue was extensively destroyed probably caused by the heavy infection and inflammation. Using the specific stain and antibodies against alginate we detected abundance of mucoid P. aeruginosa aggregates in these non-intensively treated chronically infected patients. What can we learn from our work? The present work underlines that the lung infection in CF patients is a biofilm based infection. We found P. aeruginosa as microcolonies embedded in alginate. Since alginate embedded, aggregated bacteria are considered a strong evidence for the presence of bacterial biofilms the aggregates detected in this study should be considered as biofilms. The tissue damage during the chronic infection is due to an extensive, ongoing inflammatory response, which does not eradicate the bacteria, but instead persistently degrades the lung. In addition, though antibiotics fail to clear the bacteria completely, the survival in the Copenhagen CF Centre has significantly increased due to intensive anti- P. aeruginosa therapy. This intensive therapy builds on monthly examination including identification and susceptibility testing to antibiotics of all the isolated bacteria and fungi from sputum or lower respiratory tract secretions obtained by endolaryngeal suction. Until 1975, chronic P. aeruginosa infection was only treated during acute exacerbations (on an average one 2-week course per year). But after 1976 all chronically infected patients received elective 2-week courses of i.v. anti Pseudomonas antibiotics every 3 months. This treatment was supplemented with daily inhaled colistin since 1987 and daily oral azithromyzin since As an example one of the intensively treated patients has been treated with 114 two-week intravenous courses of all together 1 kg tobramycin, 10 kg beta-lactams and 1 kg of nebulized colistin before lung transplantation, but in spite of this, the biofilm growing bacteria survived. This intensive antibiotic treatment at the Copenhagen CF center, may explain the nearly exclusive detection of P. aeruginosa in the samples, from in the conductive airways, investigated in this study. Before the intensive antibiotic therapy, P. aeruginosa infected and destroyed the CF lungs faster. Our demonstration of the many massively infected alveoli of the non-intensively treated CF lungs suggests fast lung deterioration caused by to rapid bacterial spreading into the respiratory zone. Thus, the intensive antibiotic regime may suppress the bacteria, but does not eradicate them in the conductive zone, whereas the remaining respiratory zone is protected from massive biofilm infection for prolonged time. These results suggest that the present intensive maintenance antibiotic therapy offers a better protection of the lungs of the CF patients than could be achieved before the aggressive maintenance therapy was initiated. The daily inhalation of antibiotics may suppress the bacteria in the conductive zone. The remaining relatively healthy respiratory zone may be protected from massive biofilm infection for prolonged time due to the intravenous antibiotics, administered repeatedly every 3 month. We are currently expanding these studies on all the explanted CF patients in Copenhagen. Similar studies in CF centers with less intensive antibiotic protocols would be interesting.
4 Figure 1. The diversity of P. aeruginosa biofilms in sputum. A-E). Visualization of P. aeruginosa biofilms and PMNs in sputum by Gram-staining. Blue arrows point to PMNs and black arrows point to bacteria. F). Specific staining of a P. aeruginosa microcolonies. Figure 2. Microscopic investigation of lungs from group (1) P. aeruginosa biofilms are contained in the conductive zone, only very few bacteria are detected in the respiratory zone and here they are phagocytosed. A). Bacterial biofilm
5 in a bronchia visualized with Gram stain. B, C). HE stain of bacteria filled bronchiole. D, E). Intraluminal P. aeruginosa biofilms surrounded by PMNs. F) Intact bronchi wall. G, H). Increasing consolidation of alveoli. I). Single phagocytosed P. aeruginosa in the respiratory zone. Figure 3. Microscopic investigation of the lungs from group 2. Massive bacterial biofilms detected by Gram stain of the conductive (A) and respiratory zone (B). Intraluminal P. aeruginosa biofilms surrounded by PMNs (D, E) and P. aeruginosa biofilms in the respiratory zone (G, H) visualized by specific P. aeruginosa stain. Most of the tissue in both zones is extensively destroyed.
Eradication regimens for early or recurrent Pseudomonas aeruginosa infection
 Eradication regimens for early or recurrent Pseudomonas aeruginosa infection The Leeds Method of Management. April, 2008. Cystic fibrosis and eradication therapy for early or recurrent Pseudomonas aeruginosa
Eradication regimens for early or recurrent Pseudomonas aeruginosa infection The Leeds Method of Management. April, 2008. Cystic fibrosis and eradication therapy for early or recurrent Pseudomonas aeruginosa
Macrolide therapy in cystic fibrosis: new developments in clinical use
 Macrolide therapy in cystic fibrosis: new developments in clinical use Clin. Invest. (2013) 3(12), 1179 1186 Macrolide therapy, in particular azithromycin, has been shown to improve aspects of lung health
Macrolide therapy in cystic fibrosis: new developments in clinical use Clin. Invest. (2013) 3(12), 1179 1186 Macrolide therapy, in particular azithromycin, has been shown to improve aspects of lung health
NON-CF BRONCHIECTASIS IN ADULTS
 Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
Séminaire de Pathologie Infectieuse Jeudi 25 juin 2008 Cliniques Universitaires UCL de Mont-Godinne, Yvoir NON-CF BRONCHIECTASIS IN ADULTS Dr Robert Wilson Royal Brompton Hospital, London, UK Aetiology
Treatment of lung infection in patients with cystic fibrosis: Current and future strategies,
 Journal of Cystic Fibrosis 11 (2012) 461 479 www.elsevier.com/locate/jcf Review Treatment of lung infection in patients with cystic fibrosis: Current and future strategies, Gerd Döring a,, Patrick Flume
Journal of Cystic Fibrosis 11 (2012) 461 479 www.elsevier.com/locate/jcf Review Treatment of lung infection in patients with cystic fibrosis: Current and future strategies, Gerd Döring a,, Patrick Flume
INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES
 Upper Respiratory Tract Infections Return to Syllabus INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES General Goal: To know the major mechanisms of defense in the URT, the major mechanisms invaders use
Upper Respiratory Tract Infections Return to Syllabus INTRODUCTION TO UPPER RESPIRATORY TRACT DISEASES General Goal: To know the major mechanisms of defense in the URT, the major mechanisms invaders use
Development of novel inhaled antibiotic regimens in patients with cystic fibrosis (CF) and patients with non-cf bronchiectasis (BE)
 Development of novel inhaled antibiotic regimens in patients with cystic fibrosis (CF) and patients with non-cf bronchiectasis (BE) Dr. Juliane Bernholz, Novartis (Coordinator) Dr. Andrea Appenzeller,
Development of novel inhaled antibiotic regimens in patients with cystic fibrosis (CF) and patients with non-cf bronchiectasis (BE) Dr. Juliane Bernholz, Novartis (Coordinator) Dr. Andrea Appenzeller,
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review)
 Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Nebulised anti-pseudomonal antibiotics for cystic fibrosis (Review) Ryan G, Mukhopadhyay S, Singh M This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published
Infection Control: AND DIRTY N A D I N E L E I S E, R R T
 Infection Control: GETTING DOWN AND DIRTY N A D I N E L E I S E, R R T Disclosures: None POLL EVERYWHERE Text gross to 22333 once to join... and then select A, B, C, etc when prompted If on tablet or ipad
Infection Control: GETTING DOWN AND DIRTY N A D I N E L E I S E, R R T Disclosures: None POLL EVERYWHERE Text gross to 22333 once to join... and then select A, B, C, etc when prompted If on tablet or ipad
Preventing & Controlling the Spread of Infection
 Preventing & Controlling the Spread of Infection Contributors: Alice Pong M.D., Hospital Epidemiologist Chris Abe, R.N., Senior Director Ancillary and Support Services Objectives Review the magnitude of
Preventing & Controlling the Spread of Infection Contributors: Alice Pong M.D., Hospital Epidemiologist Chris Abe, R.N., Senior Director Ancillary and Support Services Objectives Review the magnitude of
The Bacteriology of Bronchiectasis in Australian Indigenous children
 The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
The Bacteriology of Bronchiectasis in Australian Indigenous children Kim Hare, Amanda Leach, Peter Morris, Heidi Smith-Vaughan, Anne Chang Presentation outline What is bronchiectasis? Our research at Menzies
Appendix D Clinical specialist statement template
 Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
Appendix D Colistimethate sodium powder and tobramycin powder for inhalation for the treatment of pseudomonas lung infection in cystic fibrosis Thank you for agreeing to give us a statement on your organisation
Staphylococci. Gram stain: gram positive cocci arranged in clusters.
 Microbiology lab Respiratory system Third medical year Lab contents: Gram positive bacteria (Staphylococcus and Streptococcus spp), two types of filamentous fungi (Aspergillus and Penicillium spp), and
Microbiology lab Respiratory system Third medical year Lab contents: Gram positive bacteria (Staphylococcus and Streptococcus spp), two types of filamentous fungi (Aspergillus and Penicillium spp), and
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis
 Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Efficacy of Pseudomonas aeruginosa eradication regimens in bronchiectasis Vallières, E., Tumelty, K., Tunney, M. M., Hannah, R., Hewitt, O., Elborn, J. S., & Downey, D. G. (2017). Efficacy of Pseudomonas
Interim Results of Expanded Access Program of AB-SA01 and AB-PA01 for Treatment of Serious and Life-threatening S. aureus and P. aeruginosa Infections
 Advancing bacteriophage therapeutics for patients with antibioticresistant infections Interim Results of Expanded Access Program of AB-SA01 and AB-PA01 for Treatment of Serious and Life-threatening S.
Advancing bacteriophage therapeutics for patients with antibioticresistant infections Interim Results of Expanded Access Program of AB-SA01 and AB-PA01 for Treatment of Serious and Life-threatening S.
Streptococcus pneumonia
 Streptococcus pneumonia The pneumococci (S. pneumoniae) are gram-positive diplococci. Often lancet shaped or arranged in chains, possessing a capsule of polysaccharide that permits typing with specific
Streptococcus pneumonia The pneumococci (S. pneumoniae) are gram-positive diplococci. Often lancet shaped or arranged in chains, possessing a capsule of polysaccharide that permits typing with specific
an inflammation of the bronchial tubes
 BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
BRONCHITIS DEFINITION Bronchitis is an inflammation of the bronchial tubes (or bronchi), which are the air passages that extend from the trachea into the small airways and alveoli. Triggers may be infectious
PROTEUS-PROVIDENCIA-MORGANELLA GENERA
 Gram-negative rods Proteus & Pseudomonas DR. HUDA ABO-ALEES 2014-2015 Objectives: Describe the morphology & physiology for Proteus & Pseudomonas. Determine the virulence factors of proteus and pseudomonas.
Gram-negative rods Proteus & Pseudomonas DR. HUDA ABO-ALEES 2014-2015 Objectives: Describe the morphology & physiology for Proteus & Pseudomonas. Determine the virulence factors of proteus and pseudomonas.
Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults)
 Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults) Reference: NHS England 1621 First published: Month Year Prepared
Clinical Commissioning Policy Proposition: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (Adults) Reference: NHS England 1621 First published: Month Year Prepared
Chapter 13 Respiration & Excretion
 Chapter 13 Respiration & Excretion Breathing Did you know? Lungs are very spongy and elastic because of the millions of air sacs Lungs exchange about 10,000 L of air a day. Lungs would float like corks
Chapter 13 Respiration & Excretion Breathing Did you know? Lungs are very spongy and elastic because of the millions of air sacs Lungs exchange about 10,000 L of air a day. Lungs would float like corks
Clinical and Microbiological Impact of Inhaled Tobramycin Treatment on Cystic Fibrosis Patients with Pseudomonas aeruginosa
 JMID/ 2017; 7 (4):178-185 Journal of Microbiology and Infectious Diseases doi: 10.5799/jmid.368802 RESEARCH ARTICLE Clinical and Microbiological Impact of Inhaled Tobramycin Treatment on Cystic Fibrosis
JMID/ 2017; 7 (4):178-185 Journal of Microbiology and Infectious Diseases doi: 10.5799/jmid.368802 RESEARCH ARTICLE Clinical and Microbiological Impact of Inhaled Tobramycin Treatment on Cystic Fibrosis
TRANSPARENCY COMMITTEE OPINION. 15 October Date of Marketing Authorisation (national procedure): 16 April 1997, variation of 18 February 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 15 October 2008 MERONEM 1 g, powder for solution for IV Injection Box of 10 vials (CIP: 387 830-6) Applicant: ASTRAZENECA
Germs are everywhere.
 What You Should Know About Germs Germs are everywhere. For people with cystic fibrosis (CF), some germs or pathogens can cause major respiratory or lung infections. This pamphlet explains how germs are
What You Should Know About Germs Germs are everywhere. For people with cystic fibrosis (CF), some germs or pathogens can cause major respiratory or lung infections. This pamphlet explains how germs are
Histopathology: pulmonary pathology
 Histopathology: pulmonary pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
Histopathology: pulmonary pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
Hospital-acquired Pneumonia
 Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Hospital-acquired Pneumonia Hospital-acquired pneumonia (HAP) Pneumonia that occurs at least 2 days after hospital admission. The second most common and the leading cause of death due to hospital-acquired
Medical Bacteriology- lecture 13. Mycobacterium Actinomycetes
 Medical Bacteriology- lecture 13 Mycobacterium Actinomycetes Mycobacterium tuberculosis Large, very weakly gram positive rods, Obligate aerobes, related to Actinomycetes, non spore forming, non motile
Medical Bacteriology- lecture 13 Mycobacterium Actinomycetes Mycobacterium tuberculosis Large, very weakly gram positive rods, Obligate aerobes, related to Actinomycetes, non spore forming, non motile
Babak Valizadeh, DCLS
 Laboratory Diagnosis of Bacterial Infections of the Respiratory Tract Babak Valizadeh, DCLS 1391. 02. 05 2012. 04. 25 Babak_Valizadeh@hotmail.com Biological Safety Cabinet Process specimens in biological
Laboratory Diagnosis of Bacterial Infections of the Respiratory Tract Babak Valizadeh, DCLS 1391. 02. 05 2012. 04. 25 Babak_Valizadeh@hotmail.com Biological Safety Cabinet Process specimens in biological
Pseudomonas aeruginosa eradication guideline
 SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
SCOTTISH PAEDIATRIC CYSTIC FIBROSIS MCN Pseudomonas aeruginosa eradication guideline Date Created: 27 th June 2013 Date Approved by Steering Group: 30 th May 2014 Date of Review: 31 st May 2016 Lead Author:
Pulmonary Exacerbations:
 Pulmonary Exacerbations: Better Understanding Needed Michael Tracy, MD Clinical Assistant Professor Pediatric Pulmonary CF Pulmonary Exacerbations Definition Importance Causes Treatment Research opportunities
Pulmonary Exacerbations: Better Understanding Needed Michael Tracy, MD Clinical Assistant Professor Pediatric Pulmonary CF Pulmonary Exacerbations Definition Importance Causes Treatment Research opportunities
Page 1 of 20. * Sections or subsections omitted from the full prescribing information are not listed. Diluent (0.17% sodium chloride): 1 ml/ampule (3)
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use CAYSTON safely and effectively. See full prescribing information for CAYSTON. CAYSTON (aztreonam
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use CAYSTON safely and effectively. See full prescribing information for CAYSTON. CAYSTON (aztreonam
Multidrug Resistant Pseudomonas aeruginosa. Presenter: Andrew Webb Block Lecturer: George Zhanel Date: 10 January 2019
 Multidrug Resistant Pseudomonas aeruginosa Presenter: Andrew Webb Block Lecturer: George Zhanel Date: 10 January 2019 1 Pseudomonas aeruginosa Not a member of human microbiome Inhabitant of soil and moist
Multidrug Resistant Pseudomonas aeruginosa Presenter: Andrew Webb Block Lecturer: George Zhanel Date: 10 January 2019 1 Pseudomonas aeruginosa Not a member of human microbiome Inhabitant of soil and moist
Foundations in Microbiology
 Foundations in Microbiology Fifth Edition Talaro Chapter 13 Microbe Human Interactions: Infection and Disease Chapter 13 2 3 Infection a condition in which pathogenic microbes penetrate host defenses,
Foundations in Microbiology Fifth Edition Talaro Chapter 13 Microbe Human Interactions: Infection and Disease Chapter 13 2 3 Infection a condition in which pathogenic microbes penetrate host defenses,
Respiratory Pharmacology: Treatment of Cystic Fibrosis
 Respiratory Pharmacology: Treatment of Cystic Fibrosis Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
Respiratory Pharmacology: Treatment of Cystic Fibrosis Dr. Tillie-Louise Hackett Department of Anesthesiology, Pharmacology and Therapeutics University of British Columbia Associate Head, Centre of Heart
Skin reactivity to autologous bacteria isolated from respiratory tract of patients with obstructive pulmonary disease
 Skin reactivity to autologous bacteria 149 Original Article Skin reactivity to autologous bacteria isolated from respiratory tract of patients with obstructive pulmonary disease J. Halasa 1, M. Halasa
Skin reactivity to autologous bacteria 149 Original Article Skin reactivity to autologous bacteria isolated from respiratory tract of patients with obstructive pulmonary disease J. Halasa 1, M. Halasa
CCLI. Bronchiectasis Treatment Antibiotics. Charles Haworth. Physician / Patient Conference, Georgetown University, May 2017
 Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
Physician / Patient Conference, Georgetown University, May 2017 Bronchiectasis Treatment Antibiotics Charles Haworth CCLI Cambridge Centre for Lung Infection Disclosures Educational talks and / or consultancy
Molecular diagnostics in cystic fibrosis microbiology
 Molecular diagnostics in cystic fibrosis microbiology Jane L. Burns, MD Seattle Children s Hospital Center for CF Microbiology University of Washington CF microbiology Key concepts Phenotypic adaptations
Molecular diagnostics in cystic fibrosis microbiology Jane L. Burns, MD Seattle Children s Hospital Center for CF Microbiology University of Washington CF microbiology Key concepts Phenotypic adaptations
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017
 i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
Antibiotic therapy against Pseudomonas aeruginosa in cystic fibrosis: a European consensus
 Eur Respir J 2000; 16: 749±767 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 CONSENSUS STATEMENT Antibiotic therapy against Pseudomonas
Eur Respir J 2000; 16: 749±767 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 CONSENSUS STATEMENT Antibiotic therapy against Pseudomonas
Small living organism Not visible to the naked eye Must be viewed under a microscope Found everywhere in the environment, including on and in the
 Small living organism Not visible to the naked eye Must be viewed under a microscope Found everywhere in the environment, including on and in the human body Many Microorganisms are part of normal flora
Small living organism Not visible to the naked eye Must be viewed under a microscope Found everywhere in the environment, including on and in the human body Many Microorganisms are part of normal flora
The Adult Cystic Fibrosis Airway Microbiota Is Stable over Time and Infection Type, and Highly Resilient to Antibiotic Treatment of Exacerbations
 The Adult Cystic Fibrosis Airway Microbiota Is Stable over Time and Infection Type, and Highly Resilient to Antibiotic Treatment of Exacerbations Anthony A. Fodor 1 *., Erich R. Klem 2, Deirdre F. Gilpin
The Adult Cystic Fibrosis Airway Microbiota Is Stable over Time and Infection Type, and Highly Resilient to Antibiotic Treatment of Exacerbations Anthony A. Fodor 1 *., Erich R. Klem 2, Deirdre F. Gilpin
Burton's Microbiology for the Health Sciences
 Burton's Microbiology for the Health Sciences Section VII. Pathogenesis and Host Defense Mechanisms Burton's Microbiology for the Health Sciences Chapter 14. Pathogenesis of Infectious Diseases 1 Chapter
Burton's Microbiology for the Health Sciences Section VII. Pathogenesis and Host Defense Mechanisms Burton's Microbiology for the Health Sciences Chapter 14. Pathogenesis of Infectious Diseases 1 Chapter
Early Pseudomonas Infection Control (EPIC) Clinical Study. Overview for Families
 Early Pseudomonas Infection Control (EPIC) Clinical Study Overview for Families What is the EPIC Clinical Study? The EPIC Clinical Study Compares different treatments for children with CF who have just
Early Pseudomonas Infection Control (EPIC) Clinical Study Overview for Families What is the EPIC Clinical Study? The EPIC Clinical Study Compares different treatments for children with CF who have just
Inhalational antibacterial regimens in non-cystic fibrosis patients. Jeff Alder Bayer HealthCare
 Inhalational antibacterial regimens in non-cystic fibrosis patients Jeff Alder Bayer HealthCare Alder - Inhaled therapy for non-cf - EMA 25-26 Oct 2012 1 Inhalational antibacterials: two approaches 1.
Inhalational antibacterial regimens in non-cystic fibrosis patients Jeff Alder Bayer HealthCare Alder - Inhaled therapy for non-cf - EMA 25-26 Oct 2012 1 Inhalational antibacterials: two approaches 1.
Chapter 4 Inflammation and Infection
 Chapter 4 Inflammation and Infection Defense Mechanisms Three lines of defense protect the body against foreign invasion: Physical or surface barriers Inflammation Immune response Inflammation Non-specific
Chapter 4 Inflammation and Infection Defense Mechanisms Three lines of defense protect the body against foreign invasion: Physical or surface barriers Inflammation Immune response Inflammation Non-specific
Medical Bacteriology- Lecture 10. Mycobacterium. Actinomycetes. Nocardia
 Medical Bacteriology- Lecture 10 Mycobacterium Actinomycetes Nocardia 1 Mycobacterium Characteristics - Large, very weakly gram positive rods - Obligate aerobes, related to Actinomycetes - Catalase positive
Medical Bacteriology- Lecture 10 Mycobacterium Actinomycetes Nocardia 1 Mycobacterium Characteristics - Large, very weakly gram positive rods - Obligate aerobes, related to Actinomycetes - Catalase positive
Disease-Atlas: Navigating Disease Trajectories with Deep Learning. Bryan Lim & Mihaela van der Schaar University of Oxford
 Disease-Atlas: Navigating Disease Trajectories with Deep Learning Bryan Lim & Mihaela van der Schaar University of Oxford Background: Chronic Disease Management Patients with long-term conditions have
Disease-Atlas: Navigating Disease Trajectories with Deep Learning Bryan Lim & Mihaela van der Schaar University of Oxford Background: Chronic Disease Management Patients with long-term conditions have
PATHOGENICITY OF MICROORGANISMS
 PATHOGENICITY OF MICROORGANISMS Some microorganisms are : 1- Harmless microorganism, as normal flora 2- Harmfull microorganism, as pathogenic. A pathogenic microorganism is defined as one that causes or
PATHOGENICITY OF MICROORGANISMS Some microorganisms are : 1- Harmless microorganism, as normal flora 2- Harmfull microorganism, as pathogenic. A pathogenic microorganism is defined as one that causes or
Topical antimicrobial agents in wound care. Professor Val Edwards-Jones Manchester Metropolitan University UK
 Topical antimicrobial agents in wound care Professor Val Edwards-Jones Manchester Metropolitan University UK Antimicrobial agents Antibacterial agents Antifungal agents Antiviral agents Antiparasitic agents?others
Topical antimicrobial agents in wound care Professor Val Edwards-Jones Manchester Metropolitan University UK Antimicrobial agents Antibacterial agents Antifungal agents Antiviral agents Antiparasitic agents?others
In cystic fibrosis (CF), Pseudomonas aeruginosa. Evaluating the Leeds criteria for Pseudomonas aeruginosa infection in a cystic fibrosis centre
 Eur Respir J 2006; 27: 937 943 DOI: 10.1183/09031936.06.00100805 CopyrightßERS Journals Ltd 2006 Evaluating the Leeds criteria for Pseudomonas aeruginosa infection in a cystic fibrosis centre M. Proesmans*,
Eur Respir J 2006; 27: 937 943 DOI: 10.1183/09031936.06.00100805 CopyrightßERS Journals Ltd 2006 Evaluating the Leeds criteria for Pseudomonas aeruginosa infection in a cystic fibrosis centre M. Proesmans*,
Host Parasite Relationship. Prof. Hanan Habib Department of Pathology, College of Medicine,KSU
 Host Parasite Relationship Prof. Hanan Habib Department of Pathology, College of Medicine,KSU OBJECTIVES Define core terms important in host-parasite relationship. Know host response to parasite invasion
Host Parasite Relationship Prof. Hanan Habib Department of Pathology, College of Medicine,KSU OBJECTIVES Define core terms important in host-parasite relationship. Know host response to parasite invasion
Infection Control in Cystic Fibrosis
 CLINICAL MICROBIOLOGY REVIEWS, Jan. 2004, p. 57 71 Vol. 17, No. 1 0893-8512/04/$08.00 0 DOI: 10.1128/CMR.17.1.57 71.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved. Infection
CLINICAL MICROBIOLOGY REVIEWS, Jan. 2004, p. 57 71 Vol. 17, No. 1 0893-8512/04/$08.00 0 DOI: 10.1128/CMR.17.1.57 71.2004 Copyright 2004, American Society for Microbiology. All Rights Reserved. Infection
Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2
 Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
Miss. kamlah 1 Epiglottitis. Bronchitis. Bronchiolitis. Pneumonia. Croup syndrome. Miss. kamlah 2 Acute Epiglottitis Is an infection of the epiglottis, the long narrow structure that closes off the glottis
10/05/2017. Learning Objectives. Etiology and Prevalence. Diagnosis of Cystic Fibrosis. Disease of Childhood? Survival in Cystic Fibrosis
 Management of the Cystic Fibrosis Patient Jessica Goggin, MAS, RN Nurse Manager UC San Diego Adult Cystic Fibrosis Program Learning Objectives 1. Describe the symptoms associated with Cystic Fibrosis (CF).
Management of the Cystic Fibrosis Patient Jessica Goggin, MAS, RN Nurse Manager UC San Diego Adult Cystic Fibrosis Program Learning Objectives 1. Describe the symptoms associated with Cystic Fibrosis (CF).
PNEUMONIA. I. Background 6 th most common cause of death in U.S. Most common cause of infection related mortality
 Page 1 of 8 September 4, 2001 Donald P. Levine, M.D. University Health Center Suite 5C Office: 577-0348 dlevine@intmed.wayne.edu Assigned reading: pages 153-160; 553-563 PNEUMONIA the most widespread and
Page 1 of 8 September 4, 2001 Donald P. Levine, M.D. University Health Center Suite 5C Office: 577-0348 dlevine@intmed.wayne.edu Assigned reading: pages 153-160; 553-563 PNEUMONIA the most widespread and
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012
 Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Cystic Fibrosis Complications ANDRES ZIRLINGER, MD STANFORD UNIVERSITY MEDICAL CENTER MARCH 3, 2012 INTRODUCTION PNEUMOTHORAX HEMOPTYSIS RESPIRATORY FAILURE Cystic Fibrosis Autosomal Recessive Genetically
Unit II Problem 2 Pathology: Pneumonia
 Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Unit II Problem 2 Pathology: Pneumonia - Definition: pneumonia is the infection of lung parenchyma which occurs especially when normal defenses are impaired such as: Cough reflex. Damage of cilia in respiratory
Pathology of Pneumonia
 Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Pathology of Pneumonia Dr. Atif Ali Bashir Assistant Professor of Pathology College of Medicine Majma ah University Introduction: 5000 sq meters of area.! (olympic track) Filters >10,000 L of air / day!
Upper...and Lower Respiratory Tract Infections
 Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
Upper...and Lower Respiratory Tract Infections Robin Jump, MD, PhD Cleveland Geriatric Research Education and Clinical Center (GRECC) Louis Stokes Cleveland VA Medical Center Case Western Reserve University
Anatomy and Physiology of the Lungs
 The lungs consist of right and left sides. The right lung has three lobes: Upper lobe, Middle lobe, Lower lobe The left lung has two lobes: Upper lobe, Lower lobe Anatomy and Physiology of the Lungs The
The lungs consist of right and left sides. The right lung has three lobes: Upper lobe, Middle lobe, Lower lobe The left lung has two lobes: Upper lobe, Lower lobe Anatomy and Physiology of the Lungs The
Medical Bacteriology- Lecture 13 Gram Negative Coccobacilli Haemophilus Bordetella
 Medical Bacteriology- Lecture 13 Gram Negative Coccobacilli Haemophilus Bordetella 1 Haemophilus "loves heme" Small gram-negative coccobacilli Non-spore forming Non-motile Growth is enhanced in CO2 Present
Medical Bacteriology- Lecture 13 Gram Negative Coccobacilli Haemophilus Bordetella 1 Haemophilus "loves heme" Small gram-negative coccobacilli Non-spore forming Non-motile Growth is enhanced in CO2 Present
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY
 HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
HEALTHCARE-ASSOCIATED PNEUMONIA: EPIDEMIOLOGY, MICROBIOLOGY & PATHOPHYSIOLOGY David Jay Weber, M.D., M.P.H. Professor of Medicine, Pediatrics, & Epidemiology Associate Chief Medical Officer, UNC Health
with cystic fibrosis. All patients with cystic fibrosis attending the cystic the study according to the following criteria: (a)
 Archives of Disease in Childhood, 1989, 64, 122-128 Treatment of Pseudomonas aeruginosa colonisation in cystic fibrosis G STEINKAMP, B TUMMLER, R MALOTTKE,* AND H VON DER HARDT Departments of Paediatric
Archives of Disease in Childhood, 1989, 64, 122-128 Treatment of Pseudomonas aeruginosa colonisation in cystic fibrosis G STEINKAMP, B TUMMLER, R MALOTTKE,* AND H VON DER HARDT Departments of Paediatric
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
The distribution, organization and ecology of bacteria in chronic wounds ACCEPTED
 JCM Accepts, published online ahead of print on May 00 J. Clin. Microbiol. doi:./jcm.0001-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
JCM Accepts, published online ahead of print on May 00 J. Clin. Microbiol. doi:./jcm.0001-0 Copyright 00, American Society for Microbiology and/or the Listed Authors/Institutions. All Rights Reserved.
The ecology of disease interactions in CF
 1/44 The ecology of disease in CF University of Utah Department of Mathematics and Department of Biology September 4, 2014 2/44 The big questions in ecology Why are there so many species? Charley Harper
1/44 The ecology of disease in CF University of Utah Department of Mathematics and Department of Biology September 4, 2014 2/44 The big questions in ecology Why are there so many species? Charley Harper
Pathogenesis of Infectious Diseases. CLS 212: Medical Microbiology
 Pathogenesis of Infectious Diseases CLS 212: Medical Microbiology Definitions Path- means disease. Pathogenesis The steps or mechanisms involved in the development of a disease. Infection The presence
Pathogenesis of Infectious Diseases CLS 212: Medical Microbiology Definitions Path- means disease. Pathogenesis The steps or mechanisms involved in the development of a disease. Infection The presence
Palliative and Supportive Care in Cystic Fibrosis
 Palliative and Supportive Care in Cystic Fibrosis Dr William Flight Consultant in Respiratory Medicine Oxford Adult Cystic Fibrosis Centre 27 th January 2017 Overview 1. Cystic Fibrosis Clinical Aspects
Palliative and Supportive Care in Cystic Fibrosis Dr William Flight Consultant in Respiratory Medicine Oxford Adult Cystic Fibrosis Centre 27 th January 2017 Overview 1. Cystic Fibrosis Clinical Aspects
Changes in the management of children with Cystic Fibrosis. Caroline Murphy & Deirdre O Donovan CF Nurses
 Changes in the management of children with Cystic Fibrosis Caroline Murphy & Deirdre O Donovan CF Nurses What Is Cystic Fibrosis? Cystic fibrosis (CF) is an inherited chronic disease that primarily affects
Changes in the management of children with Cystic Fibrosis Caroline Murphy & Deirdre O Donovan CF Nurses What Is Cystic Fibrosis? Cystic fibrosis (CF) is an inherited chronic disease that primarily affects
Northumbria Healthcare NHS Foundation Trust. Bronchiectasis. Issued by Respiratory Medicine
 Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
Northumbria Healthcare NHS Foundation Trust Bronchiectasis Issued by Respiratory Medicine The aim of this booklet is to help you manage your bronchiectasis. It contains information which you should find
Journal Club The ELITE Trial. Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010
 Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
Journal Club The ELITE Trial Sandra Katalinic, Pharmacy Resident University Hospital of Northern British Columbia April 28, 2010 Overview Journal article Title, journal, authors, funding Abstract Introduction
Principles of Infectious Disease Lecture #13 Dr. Gary Mumaugh
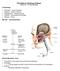 Principles of Infectious Disease Lecture #13 Dr. Gary Mumaugh Terminology Pathology study of disease Etiology cause of disease Pathogenesis disease process Infection colonization by microbes Disease illness
Principles of Infectious Disease Lecture #13 Dr. Gary Mumaugh Terminology Pathology study of disease Etiology cause of disease Pathogenesis disease process Infection colonization by microbes Disease illness
Appendix E1. Epidemiology
 Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Appendix E1 Epidemiology Viruses are the most frequent cause of human infectious diseases and are responsible for a spectrum of illnesses ranging from trivial colds to fatal immunoimpairment caused by
Spread of colistin resistant non-mucoid Pseudomonas aeruginosa among chronically infected Danish cystic fibrosis patients
 Journal of Cystic Fibrosis 7 (2008) 391 397 www.elsevier.com/locate/jcf Spread of colistin resistant non-mucoid Pseudomonas aeruginosa among chronically infected Danish cystic fibrosis patients Helle Krogh
Journal of Cystic Fibrosis 7 (2008) 391 397 www.elsevier.com/locate/jcf Spread of colistin resistant non-mucoid Pseudomonas aeruginosa among chronically infected Danish cystic fibrosis patients Helle Krogh
Microbiological surveillance in lung disease in ataxia telangiectasia
 Microbiological surveillance in lung disease in ataxia telangiectasia To the Editor: Ataxia telangiectasia is a progressive, neurodegenerative disease causing immunodeficiency, an increased risk of malignancy
Microbiological surveillance in lung disease in ataxia telangiectasia To the Editor: Ataxia telangiectasia is a progressive, neurodegenerative disease causing immunodeficiency, an increased risk of malignancy
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Community Acquired Pneumonia. Abdullah Alharbi, MD, FCCP
 Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
Community Acquired Pneumonia Abdullah Alharbi, MD, FCCP A 68 y/ male presented to the ED with SOB and productive coughing for 2 days. Reports poor oral intake since onset due to nausea and intermittent
You Can Observe a Lot By Just Watching. Wayne J. Morgan, MD, CM
 You Can Observe a Lot By Just Watching Wayne J. Morgan, MD, CM Disclosures Genentech Epidemiological Study of Cystic Fibrosis, Scientific Advisory Group CF Foundation Data Safety Monitoring Board Registry/Comparative
You Can Observe a Lot By Just Watching Wayne J. Morgan, MD, CM Disclosures Genentech Epidemiological Study of Cystic Fibrosis, Scientific Advisory Group CF Foundation Data Safety Monitoring Board Registry/Comparative
Acute respiratory illness This is a disease that typically affects the airways in the nose and throat (the upper respiratory tract).
 Influenza glossary Adapted from the Centers for Disease Control and Prevention, US https://www.cdc.gov/flu/glossary/index.htm and the World Health Organization http://www.wpro.who.int/emerging_diseases/glossary_rev_sept28.pdf?ua=1
Influenza glossary Adapted from the Centers for Disease Control and Prevention, US https://www.cdc.gov/flu/glossary/index.htm and the World Health Organization http://www.wpro.who.int/emerging_diseases/glossary_rev_sept28.pdf?ua=1
Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
 Journal of Cystic Fibrosis 12 (2013) 482 486 www.elsevier.com/locate/jcf Original Article Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
Journal of Cystic Fibrosis 12 (2013) 482 486 www.elsevier.com/locate/jcf Original Article Chronic Stenotrophomonas maltophilia infection and mortality or lung transplantation in cystic fibrosis patients
Focus on Cystic Fibrosis. Cystic Fibrosis. Cystic Fibrosis
 Focus on (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Autosomal recessive, multisystem
Focus on (Relates to Chapter 29, Nursing Management: Obstructive Pulmonary Diseases, in the textbook) Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Autosomal recessive, multisystem
Characteristics of Mycobacterium
 Mycobacterium Characteristics of Mycobacterium Very thin, rod shape. Culture: Aerobic, need high levels of oxygen to grow. Very slow in grow compared to other bacteria (colonies may be visible in up to
Mycobacterium Characteristics of Mycobacterium Very thin, rod shape. Culture: Aerobic, need high levels of oxygen to grow. Very slow in grow compared to other bacteria (colonies may be visible in up to
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages)
 Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Clinical Commissioning Policy: Levofloxacin nebuliser solution for chronic Pseudomonas lung infection in cystic fibrosis (all ages) NHS England Reference: 1732P NHS England INFORMATION READER BOX Directorate
Baby bottle steam sterilizers disinfect home nebulizers inoculated with bacterial respiratory pathogens
 Journal of Cystic Fibrosis 12 (2013) 512 516 www.elsevier.com/locate/jcf Original Article Baby bottle steam sterilizers disinfect home nebulizers inoculated with bacterial respiratory pathogens Dana Towle
Journal of Cystic Fibrosis 12 (2013) 512 516 www.elsevier.com/locate/jcf Original Article Baby bottle steam sterilizers disinfect home nebulizers inoculated with bacterial respiratory pathogens Dana Towle
Conference Report: The Wound Infection Summit. Kings College Hospital, London; March 2013
 Conference Report: The Wound Infection Summit Kings College Hospital, London; March 2013 We report on the first Wound Infection Summit, which took place at Kings College Hospital, London, on 20 th March
Conference Report: The Wound Infection Summit Kings College Hospital, London; March 2013 We report on the first Wound Infection Summit, which took place at Kings College Hospital, London, on 20 th March
IMMUNE SYSTEM. Biology 2201
 IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. Two Types of Diseases Non-infectious often called functional
IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. Two Types of Diseases Non-infectious often called functional
IMMUNE SYSTEM. Biology What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body.
 IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. 1 Two Types of Diseases Non-infectious often called functional
IMMUNE SYSTEM Biology 2201 What is a disease? Other than an injury, any change in the body that interferes with the normal functioning of the body. 1 Two Types of Diseases Non-infectious often called functional
Cystic Fibrosis. Cystic Fibrosis. Cystic Fibrosis 5/01/2011 CYSTIC FIBROSIS OF THE PANCREAS AND ITS RELATION TO CELIAC DISEASE. D ANDERSEN.
 1938 OF THE PANCREAS AND ITS RELATION TO CELIAC DISEASE. D ANDERSEN. American Journal Diseases Children. : The beginning May 1938: 49 cases 25 20 15 Nos of cases 10 5 0 0.5 1 1.5 2 2.5 3 3.5 4 4.5 5 Age
1938 OF THE PANCREAS AND ITS RELATION TO CELIAC DISEASE. D ANDERSEN. American Journal Diseases Children. : The beginning May 1938: 49 cases 25 20 15 Nos of cases 10 5 0 0.5 1 1.5 2 2.5 3 3.5 4 4.5 5 Age
California Association for Medical Laboratory Technology
 California Association for Medical Laboratory Technology Distance Learning Program Cystic Fibrosis and Microbial Infections Course # DL-966 by Lucy Treagan, Ph.D., Prof. Biol. Emerita University of San
California Association for Medical Laboratory Technology Distance Learning Program Cystic Fibrosis and Microbial Infections Course # DL-966 by Lucy Treagan, Ph.D., Prof. Biol. Emerita University of San
Bacterial Mechanisms of Pathogenicity. 2 nd Lecture
 Bacterial Mechanisms of Pathogenicity 2 nd Lecture Preferred Portal of Entry Just because a pathogen enters your body it does not mean it s going to cause disease. pathogens - preferred portal of entry
Bacterial Mechanisms of Pathogenicity 2 nd Lecture Preferred Portal of Entry Just because a pathogen enters your body it does not mean it s going to cause disease. pathogens - preferred portal of entry
Microbiology - Problem Drill 21: Microbial Diseases of the Digestive System
 Microbiology - Problem Drill 21: Microbial Diseases of the Digestive System No. 1 of 10 1. Which of the following organs is not part of the gastrointestinal tract (GI)? (A) Esophagus (B) Small intestine
Microbiology - Problem Drill 21: Microbial Diseases of the Digestive System No. 1 of 10 1. Which of the following organs is not part of the gastrointestinal tract (GI)? (A) Esophagus (B) Small intestine
Immune System. Name: Class: Date: Multiple Choice Identify the choice that best completes the statement or answers the question.
 Class: Date: Immune System Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Which of the bacteria is the cause of pneumonia? a. staphylococci c. Treponema
Class: Date: Immune System Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Which of the bacteria is the cause of pneumonia? a. staphylococci c. Treponema
INHALED ANTIBIOTICS THERAPY IN NON-CF LUNG DISEASE
 INHALED ANTIBIOTICS THERAPY IN NON-CF LUNG DISEASE Hannah Blau MBBS Pulmonary Institute and Graub CF Center SCHNEIDER CHILDREN S MEDICAL CENTER OF ISRAEL Chipap 18 th February 2015 Inhaled antibiotic therapy:
INHALED ANTIBIOTICS THERAPY IN NON-CF LUNG DISEASE Hannah Blau MBBS Pulmonary Institute and Graub CF Center SCHNEIDER CHILDREN S MEDICAL CENTER OF ISRAEL Chipap 18 th February 2015 Inhaled antibiotic therapy:
Unit 1: Asepsis and Infection Control
 Unit 1: Asepsis and Infection Control Outlines - Type of microorganism causing infection. - Types of infection. - Nosocomial infection. - Chain of infection. - Body defenses against infection. - Factors
Unit 1: Asepsis and Infection Control Outlines - Type of microorganism causing infection. - Types of infection. - Nosocomial infection. - Chain of infection. - Body defenses against infection. - Factors
320 MBIO Microbial Diagnosis. Aljawharah F. Alabbad Noorah A. Alkubaisi 2017
 320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Pathogens of the Urinary tract The urinary system is composed of organs that regulate the chemical composition and volume of
320 MBIO Microbial Diagnosis Aljawharah F. Alabbad Noorah A. Alkubaisi 2017 Pathogens of the Urinary tract The urinary system is composed of organs that regulate the chemical composition and volume of
Medical Bacteriology Lecture 15
 Medical Bacteriology Lecture 15 Gram Negative Coccobacilli Haemophilus Bordetella pertussis Haemophilus "loves heme" small gram-negative coccobacilli, non-spore forming, non-motile, require enriched media
Medical Bacteriology Lecture 15 Gram Negative Coccobacilli Haemophilus Bordetella pertussis Haemophilus "loves heme" small gram-negative coccobacilli, non-spore forming, non-motile, require enriched media
Secretory IgA as a diagnostic tool for Pseudomonas aeruginosa respiratory colonization
 Journal of Cystic Fibrosis 12 (2013) 81 87 www.elsevier.com/locate/jcf Original Article Secretory as a diagnostic tool for Pseudomonas aeruginosa respiratory colonization Kasper Aanaes a,, Helle Krogh
Journal of Cystic Fibrosis 12 (2013) 81 87 www.elsevier.com/locate/jcf Original Article Secretory as a diagnostic tool for Pseudomonas aeruginosa respiratory colonization Kasper Aanaes a,, Helle Krogh
The RESPIRATORY System. Unit 3 Transportation Systems
 The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
The RESPIRATORY System Unit 3 Transportation Systems The Respiratory System Functions of the Respiratory System Warms, moistens, and filters incoming air Nasal cavity Resonating chambers for speech and
Lecture 10 Immune System
 Lecture 10 Immune System Lecture 10 1. Introduction 2. Nonspecific External Defenses 3. Innate Immune Response 4. Acquired Immune Response 5. Antibiotics and Vaccines 1 The not-so-common cold A cold is
Lecture 10 Immune System Lecture 10 1. Introduction 2. Nonspecific External Defenses 3. Innate Immune Response 4. Acquired Immune Response 5. Antibiotics and Vaccines 1 The not-so-common cold A cold is
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
Slide 120, Lobar Pneumonia. Slide 120, Lobar Pneumonia. Slide 172, Interstitial Pneumonia. Slide 172, Interstitial Pneumonia. 53 Year-Old Smoker
 Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
Slide 120, Lobar Pneumonia Slide 120, Lobar Pneumonia Slide 172, Interstitial Pneumonia Slide 172, Interstitial Pneumonia 53 Year-Old Smoker Emphysema Pink puffer Barrel chest Hyperinflation Trapped air
