BACKGROUND. The current study evaluated the effect of bevacizumab added to
|
|
|
- Bartholomew Carr
- 5 years ago
- Views:
Transcription
1 2761 Bevacizumab Improves Pathologic Response and Protects Against Hepatic Injury in Patients Treated With Oxaliplatin-Based Chemotherapy for Colorectal Liver Metastases Dario Ribero, MD 1 Huamin Wang, MD 2 Matteo Donadon, MD 1 Daria Zorzi, MD 1 Melanie B. Thomas, MD 3 Cathy Eng, MD 3 David Z. Chang, MD, PhD 3 Steven A. Curley, MD 1 Eddie K. Abdalla, MD 1 Lee M. Ellis, MD 4 Jean-Nicolas Vauthey, MD 1 1 Department of Surgical Oncology, The University of Texas M. D. Anderson Cancer Center, Houston, Texas. 2 Department of Pathology, The University of Texas M. D. Anderson Cancer Center, Houston, Texas. 3 Department of Gastrointestinal Medical Oncology, The University of Texas M. D. Anderson Cancer Center, Houston, Texas. 4 Department of Cancer Biology, The University of Texas M. D. Anderson Cancer Center, Houston, Texas. Supported in part by a research grant provided by the Cancer Fighters of Houston, Inc. Dr. Ellis has acted as a member of the Speakers Bureau for Genetech and has received research support from Sanofi-Aventis. Drs. Abdalla and Vauthey have received research support from Sanofi-Aventis. We thank Dr. Gregory Y. Lauwers, Chief of the Division of Gastrointestinal Pathology, Massachusetts General Hospital and Harvard Medical School, Boston, for critical review of the article; Ms. Stephanie Deming of the Department of Scientific Publications at the University of Texas M. D. Anderson Cancer Center, who offered editorial suggestions on drafts of this article; and Ms. Ruth J. Haynes for secretarial assistance. BACKGROUND. The current study evaluated the effect of bevacizumab added to fluoropyrimidine-plus-oxaliplatin (5FU/OX) chemotherapy for colorectal liver metastases (CLM) on the pathologic response and nontumorous liver histology. METHODS. A total of 105 consecutive patients treated preoperatively with 5FU/OX chemotherapy with (n 5 62) or without (n 5 43) bevacizumab were analyzed. The response to chemotherapy was evaluated by pathologic analysis of tumor viability (percentage of viable tumor in relation to tumor surface area). The incidence and grade of hepatic sinusoidal dilation were also investigated. RESULTS. Bevacizumab-containing regimens significantly reduced the degree of tumor viability compared with 5FU/OX-only chemotherapy (32.9% vs 45.3%; P 5.02). After stratification according to the magnitude of tumor viability, a higher proportion of patients treated with bevacizumab than without had <25% residual viable tumor cells (45% vs 23%; P 5.02). However, the addition of bevacizumab to 5FU/OX did not appear to increase the incidence of complete pathologic response (11.3% vs 11.6%; P 5.59). The incidence and severity of sinusoidal dilation was lower in patients treated with bevacizumab than in those treated with 5FU/OX only (any grade: 27.4% vs 53.5%; moderate or severe: 8.1% vs 27.9%; both P <.01). CONCLUSIONS. In patients treated with 5FU/OX chemotherapy, bevacizumab improves the pathologic response, as demonstrated by a reduction of the degree of tumor viability, and reduces the incidence and severity of hepatic injury. This retrospective study provides additional evidence supporting the use of bevacizumab in combination with 5FU/OX for CLM. Cancer 2007;110: Ó 2007 American Cancer Society. KEYWORDS: oxaliplatin, bevacizumab, tumor response, colorectal liver metastases, sinusoidal dilatation, hepatotoxicity. In recent years, preoperative systemic chemotherapy has been used in patients with colorectal liver metastases (CLM) to downsize unresectable tumors and make hepatic resection possible, 1 3 and to identify responders so that patients can be spared nonbeneficial surgical treatment and ineffective postoperative chemotherapy. 4 6 The clinical relevance of the radiographic response to chemotherapy, Address for reprints: Jean-Nicolas Vauthey, MD, Department of Surgical Oncology, The University of Texas M. D. Anderson Cancer Center, 1515 Holcombe Blvd., Unit 444, Houston, TX ; Fax: (713) ; jvauthey@mdanderson.org Received April 27, 2006; revision received June 4, 2007; accepted June 26, ª 2007 American Cancer Society DOI /cncr Published online 24 October 2007 in Wiley InterScience (
2 2762 CANCER December 15, 2007 / Volume 110 / Number 12 defined as a reduction of tumor size, is also emphasized by its conventional use for treatment efficacy assessment. 7 However, this simple, macroscopic criterion for tumor response evaluation may not be enough per se to determine the effectiveness of a treatment. 8 Pathologic analysis of tumor viability represents an alternative method to evaluate tumor response after preoperative treatments. Recent data indicate that preoperative chemotherapy results in a reduction or disappearance of viable tumor cells, 9 and assessment of residual viable tumor cells has been used to compare the efficacy of different preoperative treatments. 10 As more patients receive preoperative systemic chemotherapy, clinically significant chemotherapyspecific hepatic injuries are increasingly being reported. 4,11 13 We recently reported a 20% incidence of steatohepatitis in association with irinotecan-based chemotherapy and a 19% incidence of sinusoidal injury after treatment with oxaliplatin. 4 In 2 series reporting on patients who received mostly oxaliplatin-based preoperative chemotherapy, the authors reported a higher rate of sinusoidal injury and an increase in perioperative blood transfusions and surgical complications in patients who received preoperative chemotherapy than in those who did not. 11,12 In patients with advanced metastatic colorectal cancer, targeted biologic therapy with bevacizumab, a recombinant human monoclonal antibody to vascular endothelial growth factor-a (VEGF-A), has recently been used in association with 5-fluorouracil, irinotecan, and oxaliplatin. Preliminary data from these studies indicate an increase in radiologic response rate and survival with the combination of bevacizumab and cytotoxic chemotherapy However, to our knowledge, the efficacy of bevacizumab in combination with chemotherapy in patients undergoing preoperative chemotherapy followed by liver resection has not been published to date, and it is not known whether the combination of bevacizumab and cytotoxic therapy improves pathologic response or affects hepatic injury of the nontumorous liver. 4,11 The objective of the current study was to determine the effect of bevacizumab added to fluoropyrimidine-plus-oxaliplatin chemotherapy administered before hepatic resection for CLM. To achieve this objective, we reviewed a consecutive series of patients who received preoperative fluoropyrimidineplus-oxaliplatin chemotherapy with or without bevacizumab to answer the following questions: Does bevacizumab 1) increase the response of CLM as measured by systematic pathologic analysis of tumor viability? and 2) affect the incidence of sinusoidal dilation? MATERIALS AND METHODS From the hepatobiliary database of the University of Texas M. D. Anderson Cancer Center, we identified 105 consecutive patients who underwent liver resection for CLM after preoperative fluoropyrimidine-plus-oxaliplatin (5FU/OX) chemotherapy with or without bevacizumab between November 2002 and July In the group that received bevacizumab, the last dose was administered 6 or more weeks before surgery. 17 With the aim of maximizing tumor response, 1 additional cycle of 5FU/OX was usually administered after bevacizumab was discontinued. To ensure homogeneity within groups, patients treated at any time before hepatic resection with drugs other than fluoropyrimidines, oxaliplatin, and bevacizumab were excluded. This study was approved by our Institutional Review Board (IRB #RCR ). Demographic and clinical data were obtained by reviewing medical records. A single gastrointestinal pathologist with hepatobiliary expertise (H.W.), blinded to the chemotherapy regimens with which individual patients had been treated, evaluated the resected specimens. Nontumorous liver tissue was reviewedtodefinethepresenceandgradeofsinusoidal dilation according to a previously reported standard 4-point scale on which 0 indicated the absence of sinusoidal dilation, 1 indicated mild sinusoidal dilation (centrilobular involvement limited to approximately one-third of the lobular surface), 2 indicated moderate sinusoidal dilation (centrilobular involvement extending in approximately twothirds of the lobular surface), and 3 indicated severe sinusoidal dilation (complete lobular involvement). 4,18 The tumoricidal effect of chemotherapy was analyzed using a previously defined methodology 19 as follows. On routine hematoxylin & eosin-stained sections the area of residual viable tumor cells within each metastatic nodule was estimated as a percentage of the total tumor surface area that includes areas of coagulative necrosis, calcification, fibrosis, and the associated histiocytes, foreign body giant cells, and inflammatory cells (Fig. 1). All archival slides, for an average of 2 to 3 sections per tumor nodule, were reviewed. When multiple tumors were present, the mean percentage was used. Continuous variables, presented as means with standard error of the mean unless otherwise stated, were compared using the Mann-Whitney U test; discrete variables, expressed as the number and percentage, were compared using the chi-square test or Fisher exact test, when appropriate. Statistical significance was defined as P <.05.
3 Colorectal Liver Metastases and Bevacizumab/Ribero et al TABLE 1 Clinical and Pathologic Features of Patients* Variable 5FU/OX (n = 43) 5FU/OX plus bevacizumab (n = 62) P Median age (range), y 57 (26 80) 53.5 (34 85).61 Gender Male 26 (60) 36 (58).80 Female 17 (40) 26 (42) BMI Median (range), kg/m ( ) 27.5 ( ).89 >25 kg/m 2 31 (72) 37 (60) Coexisting diabetes 4 (9) 8 (13).98 Site of primary tumor Colon 32 (74) 43 (69).57 Rectum 11 (26) 19 (31) Status of primary lymph nodes Positive 32 (74) 44 (71).95 Not available 2 (5) 6 (10) Synchronous hepatic metastases y 32 (74) 34 (55).12 Median no. of cycles of preoperative.46 chemotherapy (range) 6 (2 16) 6 (3 12) Mean (SEM) interval time between completion of chemotherapy and surgery, mo { 1.71 (0.153) 1.99 (0.156).15 Median largest tumor dimension (range), cm 3.5 (1 10) 2 (0.5 12).004 Colorectal liver metastases Median no. (range) 2 (1 8) 2 (1 21).33 Solitary metastasis 16 (37) 22 (35).85 5FU/OX indicates fluoropyrimidines plus oxaliplatin; BMI, body mass index; SEM, standard error of the mean. * Values in the table are shown as the number of patients (percentages) unless otherwise indicated. y Disease-free interval of <1 month. { Data were not available for all patients. Calculated using the size of the largest lesion when multiple colorectal liver metastases were present. FIGURE 1. Representative photomicrographs of metastases demonstrating different percentages of residual viable tumor cells. (A) Approximately 90% residual viable tumor cells. (B) Approximately 50% residual viable tumor cells. (C) Extensive fibrosis, necrosis, calcifications, and the associated collections of histiocytes and inflammatory cells with 1% viable tumor cells (marked with arrows and shown in the inset ) (H & E, original magnification 320; inset: 3200). RESULTS Forty-three patients received 5FU/OX without bevacizumab and 62 received 5FU/OX with bevacizumab. Clinical and pathologic characteristics for the patients in the 2 study groups are shown in Table 1. Pathologic Response A total of 285 tumor nodules were reviewed. Pathologic analysis revealed that treatment with 5FU/OX only was associated with significantly greater percentage of residual viable tumor cells compared with treatment with 5FU/OX plus bevacizumab (45.3% 3.7 vs 32.9% 3.5; P 5.02) (Fig. 2A). When patients were stratified according to the magnitude of tumor viability (<25%, 25 49%, 50 75%, and >75% of total tumor surface area), a significantly higher proportion of patients treated with bevacizumab had <25% residual viable tumor cells compared with patients who were not treated with bevacizumab (45% vs 23%; P 5.02). A complete pathologic response (ie, no identifiable viable tumor cells in any tumor nodules) was observed in 5 patients (11.6%) treated with 5FU/OX only for a median of 12 cycles (range, 4 15 cycles) and 7 patients (11.3%) treated with 5FU/OX plus bevacizumab for a median of 4 cycles (range, 4 12 cycles) (P 5.59). It is
4 2764 CANCER December 15, 2007 / Volume 110 / Number 12 FIGURE 2. Percentage of residual tumor cells after preoperative chemotherapy with fluoropyrimidine plus oxaliplatin only (5FU/OX) and 5FU/OX plus bevacizumab (5FU/OX plus Bev). (A) Overall results. (B) Results for subgroups stratified according to posttreatment tumor dimension as measured on macroscopic pathology. *P <.05. interesting to note that the mean dimension, measured on macroscopic pathology, of the 26 metastases found in these 12 patients was 2 cm 0.5 cm (median, 1.9 cm) despite the absence of viable tumor cells. There were a wide range of tumor sizes resected in both groups (median, 2 cm [range, cm] in the bevacizumab group, and 3.5 cm [range, 1 10 cm] in the 5FU/OX group). To investigate whether resected tumor dimension might be associated with the degree of pathologic response, patients were stratified according to tumor dimension as measured on macroscopic pathology for the following subgroups: 2 cm, 3 cm, 4 cm, and >4 cm (the number of patients compared in each stratum were 40, 47, 54, and 8, respectively, in the bevacizumab group and 16, 21, 28, and 15, respectively, in the 5FU/OX group) (Fig. 2B). Treatment with bevacizumab was associated with significantly reduced percentages of residual viable tumor cells in each subgroup (2 cm: 24.6% 3.7 [median, 20%] vs 45.6% 6.6 [median, 50%] [P 5.01]; 3 cm: 25.9% 3.7 [median, 20%] vs 46.2% 5.2 [median, 50%] [P 5.003]; and 4 cm: 29.5% 3.5 [median, 30%] vs 45.4% 5.1 [median, 50%] [P 5.01]). When considering patients with tumors >4 cm, no difference was found between patients treated with and those treated without bevacizumab with regard to tumor viability (58.5% 10.7 [median, 70%] vs [median, 50%]; P 5.09). Overall, treatment duration was similar between the groups treated with and those treated without bevacizumab. To clarify the effect of the duration of chemotherapy on pathologic response, patients were stratified according to the number of cycles of 5FU/ OX received (2 4 [42 patients], patients]; and >8 [20 patients]). The distribution of patients across FIGURE 3. Incidence of (A) sinusoidal dilation of any grade and (B) moderate or severe (grade 2 or 3) sinusoidal dilation after preoperative chemotherapy with fluoropyrimidines plus oxaliplatin only (5FU/OX) or 5FU/OX plus bevacizumab (5FU/OX plus Bev). *P these subgroups was similar between the 2 treatment groups (5FU/OX with or without bevacizumab). Patients treated without bevacizumab had greater percentages of residual viable tumor cells than those treated with bevacizumab regardless of the duration of treatment (2 4 cycles: 50% 5.3 [median, 50%] vs 35.5% 6.2 [median, 30%]; 5 8 cycles: 46.2% 5.9 [median, 55%] vs 32.7% 4.3 [median, 30%]; and >8 cycles: 32.5% 9.9 [median, 45%] vs 28.18% 9.2 [median, 5%], respectively) (differences did not reach statistical significance in these subgroup analyses). Incidence of Sinusoidal Dilation Pathologic review of the nontumorous liver parenchyma revealed that the incidence of sinusoidal dilation of any grade was significantly higher in patients treated without bevacizumab (23 of 43 patients; 53.5%) than in those treated with bevacizumab (17 of 62 patients; 27.4%) (P 5.006) (Fig. 3A). The incidence of moderate or severe sinusoidal dilation was also significantly higher in patients treated without bevacizumab (12 of 43 patients; 27.9%) than in those treated with bevacizumab (5 of 62 patients; 8.1%) (P 5.006) (Fig. 3B). These differences were independent of the duration of chemotherapy. The median number of cycles of 5FU/OX was similar in patients who developed any grade of sinusoidal dilation (6 cycles; range, 2 16 cycles) and those who did not (6 cycles; range, 2 15 cycles) and in those who developed moderate to severe sinusoidal dilation (6.5 cycles; range, 2 13 cycles) and those who did not (6 cycles; range, 2 16 cycles) (both P >.05).
5 Colorectal Liver Metastases and Bevacizumab/Ribero et al FIGURE 4. Pathologic response to preoperative treatment with fluoropyrimidines plus oxaliplatin (5FU/OX) and bevacizumab in a patient aged 36 years with synchronous bilobar liver metastases from pt3 pn1 sigmoid adenocarcinoma who was a candidate for a 2-stage hepatectomy. (A) Before chemotherapy, the patient had a metastasis measuring 3.4 cm in segment 3 of the liver. (B) Partial radiographic response of the metastasis in segment 3 after 3 cycles of 5FU/OX and bevacizumab (dimension of 1.5 cm). At this time, the patient underwent wedge resection of the metastasis in segment 3 (first-stage surgery). A representative photomicrograph of this metastasis is shown in Figure 1C. DISCUSSION In this study, we found that 5FU/OX plus bevacizumab was oncologically more effective than 5FU/OX alone as demonstrated by the greater pathologic responses assessed in resected tumors. We also found that the incidences and severity of hepatic injury were reduced when bevacizumab was added to 5FU/OX. These findings provide additional evidence supporting the use of bevacizumab for CLM. To our knowledge, this is the first study to analyze the pathologic effect of preoperative chemotherapy with 5FU/OX plus bevacizumab on resected CLM and nontumorous liver. Previous studies have examined the efficacy of bevacizumab added to cytotoxic therapy using clinical outcome measures, 14,15 but analysis of pathologic changes that occur in tumors after treatment with biologic agents is lacking. Our decision to evaluate tumor response pathologically was motivated by recent reports that suggest that radiologic assessment of changes in tumor size may not accurately reflect response to chemotherapy 8 and may either overestimate 20 or underestimate the actual extent of tumor regression. 18 (Fig. 4) Two studies focused on targeted biologic therapies have further emphasized these limitations 21 and demonstrated that in some disease types changes in tumor size in response to biologic therapies underestimate the actual pathologic tumor response. 22 One possible explanation is that radiologic methods cannot fully differentiate between areas of viable tumor and areas of fibrotic replacement induced by effective chemotherapy. (Fig. 4) A recent study by Rubbia-Brandt et al. 9 provides new insights into the pathologic changes induced by oxaliplatin-based chemotherapy and provides a framework within which the findings of the current study can be analyzed. The findings of that study demonstrated that, compared with tumors not treated with preoperative chemotherapy, tumors treated with preoperative oxaliplatin exhibit significant tumor regression with marked reduction or disappearance of viable tumor cells and fibrosis overgrowth. 18 In the current study, we confirmed the finding of Rubbia-Brandt et al. that tumor response to chemotherapy is characterized, in part, by replacement of tumor with fibrosis (Fig. 1C). Furthermore, we found not only that a similar pathologic change occurs in tumors treated with 5FU/OX plus bevacizumab, but the addition of bevacizumab to 5FU/OX yielded an incrementally greater decrease in residual viable cells within the resected tumors over the decrease associated with 5FU/OX alone. It is interesting to note that this differentially greater pathologic response with bevacizumab was significant in tumors measuring 4 cm and was independent of the duration of chemotherapy. The absence of improved response in tumors measuring >4 cm may be related to the inadequate sample size to detect the difference, or to the lesser effectiveness associated with bevacizumab for this subset. These data also suggest that the improved tumor regression with bevacizumab occurs early during treatment and that a fairly stable benefit is sustained with increasing duration of treatment. Increased pathologic response to preoperative treatment is associated with improved long-term outcome in several malignancies, such as esophageal cancer and colorectal cancer. 19,23 A similar survival
6 2766 CANCER December 15, 2007 / Volume 110 / Number 12 advantage has been recently reported in patients with CLM treated with 5-fluorouracil, oxaliplatin, or irinotecan. 9 However, whether the degree of improved pathologic response associated with bevacizumab for CLM translates into improved long-term outcome remains to be evaluated by further study. The second major finding of this study was that bevacizumab reduced the incidence and severity of oxaliplatin-related sinusoidal dilation. Oxaliplatinbased chemotherapy has been shown to cause hepatic sinusoidal dilation, 4,12,18 a vascular injury characteristic of veno-occlusive disease, 24 recently renamed sinusoidal obstruction syndrome (SOS). 25 SOS is a complication of conditioning chemotherapy before bone marrow transplantation in 5% to 54% of patients Although to our knowledge the pathophysiology of drug-induced SOS is not fully understood, in vitro and in vivo models suggest that oxaliplatin induces an overproduction of reactive oxygen species and depletion of glutathione in endothelial cells, 29,30 which plays a pivotal role in SOS development. 31 DeLeve et al. 32 have also demonstrated that sinusoidal endothelial cell release of matrix metalloproteinase (MMP)-2 and MMP-9 precipitates the early steps of SOS by degrading the extracellular matrix in the spaces of Disse and endothelial cell degradation and embolization. VEGF is known to regulate MMP-9 activation by inducing its expression. In patients undergoing bone marrow transplantation, the serum VEGF level is found to be elevated in individuals who develop SOS, and the degree of the increase in VEGF serum level parallels the clinical severity of SOS. 33 Therefore, although the mechanisms that explain a bevacizumab-mediated decrease in the hepatic toxicity of oxaliplatin remain unknown, VEGF blockade may attenuate sinusoidal injury by down-regulating MMP-9 production. The clinical relevance of sinusoidal dilation with respect to outcomes after hepatic resection is increasingly recognized. We reported no increase in morbidity after a median of 12 weeks of treatment with oxaliplatin-based chemotherapy, 4 but 2 recent studies have described an increase in blood transfusions and complications in patients treated preoperatively for >12 weeks. 11,12 In rare cases, prolonged treatment of CLM with oxaliplatin has been associated with SOS and death. 13 Although our study cannot clarify whether bevacizumab protects from long-term exposure to oxaliplatin, the protective effect of bevacizumab observed in the current study is attractive. Although this study is limited by its retrospective nature, the increase in the magnitude of pathologic response after treatment with bevacizumab and the reduction in the incidence and severity of sinusoidal dilation strongly suggest a benefit for the use of bevacizumab-containing regimens over oxaliplatin alone. Further studies are needed to expand on these initial findings and to provide further insight into the role of bevacizumab as a potentially protective agent against the broader spectrum of diseases associated with SOS. REFERENCES 1. Adam R, Delvart V, Pascal G, et al. Rescue surgery for unresectable colorectal liver metastases downstaged by chemotherapy: a model to predict long-term survival. Ann Surg. 2004;240: Alberts SR, Horvath WL, Sternfeld WC, et al. Oxaliplatin, fluorouracil, and leucovorin for patients with unresectable liver-only metastases from colorectal cancer: a North Central Cancer Treatment Group phase II study. J Clin Oncol. 2005;23: Poston G, Adam R, Vauthey JN. Downstaging or downsizing: time for a new staging system in advanced colorectal cancer? J Clin Oncol. 2006;24: Vauthey JN, Pawlik TM, Ribero D, et al. Chemotherapy regimen predicts steatohepatitis and an increase in 90-day mortality after surgery for hepatic colorectal metastases. J Clin Oncol. 2006;24: Adam R, Pascal G, Castaing D, et al. Tumor progression while on chemotherapy: a contraindication to liver resection for multiple colorectal metastases? Ann Surg. 2004; 240: Allen PJ, Kemeny N, Jarnagin W, DeMatteo R, Blumgart L, Fong Y. Importance of response to neoadjuvant chemotherapy in patients undergoing resection of synchronous colorectal liver metastases. J Gastrointest Surg. 2003;7: Therasse P, Arbuck SG, Eisenhauer EA, et al. New guidelines to evaluate the response to treatment in solid tumors. European Organization for Research and Treatment of Cancer, National Cancer Institute of the United States, National Cancer Institute of Canada. J Natl Cancer Inst. 2000;92: Grothey A, Hedrick EE, Mass RD, et al. Response rate using conventional criteria is a poor surrogate for clinical benefit on progression-free (PFS) and overall survival (OS) in metastatic colorectal cancer (mcrc): a comparative analysis of N9741 and AVF2107. Proc Am Soc Clin Oncol. 2006;24:150s. 9. Rubbia-Brandt L, Giostra E, Brezault C, et al. Importance of histological tumor response assessment in predicting the outcome in patients with colorectal liver metastases treated with neoadjuvant chemotherapy followed by liver surgery. Ann Oncol. 2007;18: Malaisrie SC, Hofstetter WL, Correa AM, et al. The addition of induction chemotherapy to preoperative, concurrent chemoradiotherapy improves tumor response in patients with esophageal adenocarcinoma. Cancer. 2006;107: Karoui M, Penna C, Amin-Hashem M, et al. Influence of preoperative chemotherapy on the risk of major hepatectomy for colorectal liver metastases. Ann Surg. 2006;243: Aloia T, Sebagh M, Plasse M, et al. Liver histology and surgical outcomes after preoperative chemotherapy with fluorouracil plus oxaliplatin in colorectal cancer liver metastases. J Clin Oncol. 2006;24: Tisman G, MacDonald D, Shindell N, et al. Oxaliplatin toxicity masquerading as recurrent colon cancer. J Clin Oncol. 2004;22:
7 Colorectal Liver Metastases and Bevacizumab/Ribero et al Hochster HS, Hart LL, Ramanathan RK, Hainsworth JD, Hedrick EE, Childs BH. Safety and efficacy of oxaliplatin/ fluoropyrimidine regimens with or without bevacizumab as first-line treatment of metastatic colorectal cancer (mcrc): final analysis of the TREE-study. Proc Am Soc Clin Oncol. 2006:148s. 15. Hurwitz H, Fehrenbacher L, Novotny W, et al. Bevacizumab plus irinotecan, fluorouracil, and leucovorin for metastatic colorectal cancer. N Engl J Med. 2004;350: Giantonio BJ, Catalano PJ, Meropol NJ, et al. Bevacizumab in combination with oxaliplatin, fluorouracil, and leucovorin (FOLFOX 4) for previously treated metastatic colorectal cancer: results from the Eastern Cooperative Oncology Group Study E3200. J Clin Oncol. 2007;12: Ellis LM, Curley SA, Grothey A. Surgical resection after downsizing of colorectal liver metastasis in the era of bevacizumab. J Clin Oncol. 2005;23: Rubbia-Brandt L, Audard V, Sartoretti P, et al. Severe hepatic sinusoidal obstruction associated with oxaliplatinbased chemotherapy in patients with metastatic colorectal cancer. Ann Oncol. 2004;15: Ajani JA, Mansfield PF, Crane CH, et al. Paclitaxel-based chemoradiotherapy in localized gastric carcinoma: degree of pathologic response and not clinical parameters dictated patient outcome. J Clin Oncol. 2005;23: Benoist S, Brouquet A, Penna C, et al. Complete response of colorectal liver metastases after chemotherapy: does it mean cure? J Clin Oncol. 2006;24: Bechtold RE, Chen MY, Stanton CA, Savage PD, Levine EA. Cystic changes in hepatic and peritoneal metastases from gastrointestinal stromal tumors treated with Gleevec. Abdom Imaging. 2003;28: Goh BK, Chow PK, Chuah KL, Yap WM, Wong WK. Pathologic, radiologic and PET scan response of gastrointestinal stromal tumors after neoadjuvant treatment with imatinib mesylate. Eur J Surg Oncol. 2006;32: Bouzourene H, Bosman FT, Seelentag W, Matter M, Coucke P. Importance of tumor regression assessment in predicting the outcome in patients with locally advanced rectal carcinoma who are treated with preoperative radiotherapy. Cancer. 2002;94: Willmot FC, Robertson GW. Senecio disease, or cirrhosis of the liver due to senecio poisoning. Lancet. 1920;196: DeLeve LD, Shulman HM, McDonald GB. Toxic injury to hepatic sinusoids: sinusoidal obstruction syndrome (venoocclusive disease). Semin Liver Dis. 2002;22: Carreras E, Bertz H, Arcese W, et al. Incidence and outcome of hepatic veno-occlusive disease after blood or marrow transplantation: a prospective cohort study of the European Group for Blood and Marrow Transplantation. European Group for Blood and Marrow Transplantation Chronic Leukemia Working Party. Blood. 1998;92: McDonald GB, Hinds MS, Fisher LD, et al. Veno-occlusive disease of the liver and multiorgan failure after bone marrow transplantation: a cohort study of 355 patients. Ann Intern Med. 1993;118: Hasegawa S, Horibe K, Kawabe T, et al. Veno-occlusive disease of the liver after allogeneic bone marrow transplantation in children with hematologic malignancies: incidence, onset time and risk factors. Bone Marrow Transplant. 1998; 22: Laurent A, Nicco C, Chereau C, et al. Controlling tumor growth by modulating endogenous production of reactive oxygen species. Cancer Res. 2005;65: Alexandre J, Nicco C, Chereau C, et al. Improvement of the therapeutic index of anticancer drugs by the superoxide dismutase mimic mangafodipir. J Natl Cancer Inst. 2006;98: Wang X, Kanel GC, DeLeve LD. Support of sinusoidal endothelial cell glutathione prevents hepatic veno-occlusive disease in the rat. Hepatology. 2000;31: Deleve LD, Wang X, Tsai J, Kanel G, Strasberg S, Tokes ZA. Sinusoidal obstruction syndrome (veno-occlusive disease) in the rat is prevented by matrix metalloproteinase inhibition. Gastroenterology. 2003;125: Iguchi A, Kobayashi R, Yoshida M, et al. Vascular endothelial growth factor (VEGF) is 1 of the cytokines causative and predictive of hepatic veno-occlusive disease (VOD) in stem cell transplantation. Bone Marrow Transplant. 2001; 27:
Treatment of Colorectal Liver Metastases State of the Art
 Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Treatment of Colorectal Liver Metastases State of the Art Eddie K. Abdalla, MD, FACS Professor and Chairman of Surgery Chief of Hepatobiliary Surgery Hilton Metropolitan Palace Hotel Beirut 16 November,
Colon Cancer Liver Metastases: Liver-Directed Therapy
 Colon Cancer Liver Metastases: Liver-Directed Therapy Shishir K. Maithel, MD FACS Assistant Professor of Surgery Division of Surgical Oncology Winship Cancer Institute Emory University August 10, 2014
Colon Cancer Liver Metastases: Liver-Directed Therapy Shishir K. Maithel, MD FACS Assistant Professor of Surgery Division of Surgical Oncology Winship Cancer Institute Emory University August 10, 2014
Resection of liver limited resectable metastases Upfront, neoadjuvant and repeat hepatectomy
 Resection of liver limited resectable metastases Upfront, neoadjuvant and repeat hepatectomy Dr Chan Chung Yip MBBS, M.Med(Surgery), MD, FAMS, FRCSEd Senior Consultant and Head Department of Hepatopancreatobiliary
Resection of liver limited resectable metastases Upfront, neoadjuvant and repeat hepatectomy Dr Chan Chung Yip MBBS, M.Med(Surgery), MD, FAMS, FRCSEd Senior Consultant and Head Department of Hepatopancreatobiliary
Behandeling van colorectale levermetastasen. Rol van beeldvorming van de lever bij colorectaal carcinoom
 Behandeling van colorectale levermetastasen Rol van beeldvorming van de lever bij colorectaal carcinoom B. Op de Beeck Universitair Ziekenhuis Antwerpen bart.op.de.beeck@uza.be 10.12.2016 AZ Turnhout campus
Behandeling van colorectale levermetastasen Rol van beeldvorming van de lever bij colorectaal carcinoom B. Op de Beeck Universitair Ziekenhuis Antwerpen bart.op.de.beeck@uza.be 10.12.2016 AZ Turnhout campus
Predictors of a True Complete Response Among Disappearing Liver Metastases From Colorectal Cancer After Chemotherapy
 Original Article Predictors of a True Complete Response Among Disappearing Liver Metastases From Colorectal Cancer After Chemotherapy Rebecca C. Auer, MD 1 ; Rebekah R. White, MD 2 ; Nancy E. Kemeny, MD
Original Article Predictors of a True Complete Response Among Disappearing Liver Metastases From Colorectal Cancer After Chemotherapy Rebecca C. Auer, MD 1 ; Rebekah R. White, MD 2 ; Nancy E. Kemeny, MD
Introduction. Case Report
 Case Report A patient who showed a pathologically complete response after undergoing treatment with XELOX plus bevacizumab for synchronous liver metastasis of grade H2 from sigmoid colon cancer Yasuhito
Case Report A patient who showed a pathologically complete response after undergoing treatment with XELOX plus bevacizumab for synchronous liver metastasis of grade H2 from sigmoid colon cancer Yasuhito
Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D.
 Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D. Department of Surgery Grand Rounds University of Kentucky January 15, 2014 Metastatic Colorectal Cancer (CRC)
Techniques to Improve Resectability of Colorectal Liver Metastases Ching-Wei D. Tzeng, M.D. Department of Surgery Grand Rounds University of Kentucky January 15, 2014 Metastatic Colorectal Cancer (CRC)
Surgical Management of Advanced Stage Colon Cancer. Nathan Huber, MD 6/11/14
 Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
Surgical Management of Advanced Stage Colon Cancer Nathan Huber, MD 6/11/14 Colon Cancer Overview Approximately 50,000 attributable deaths per year Colorectal cancer is the 3 rd most common cause of cancer-related
BACKGROUND: STUDY DESIGN: RESULTS: CONCLUSIONS:
 Improved Survival after Resection of Liver and Lung Colorectal Metastases Compared with Liver-Only Metastases: A Study of 112 Patients with Limited Lung Metastatic Disease Antoine Brouquet, MD, Jean Nicolas
Improved Survival after Resection of Liver and Lung Colorectal Metastases Compared with Liver-Only Metastases: A Study of 112 Patients with Limited Lung Metastatic Disease Antoine Brouquet, MD, Jean Nicolas
MANAGEMENT OF COLORECTAL METASTASES. Robert Warren, MD. The Postgraduate Course in General Surgery March 22, /22/2011
 MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
MANAGEMENT OF COLORECTAL METASTASES Robert Warren, MD The Postgraduate Course in General Surgery March 22, 2011 Local Systemic LIVER TUMORS:THERAPEUTIC OPTIONS Hepatoma Cholangio. Neuroendo. Colorectal
Effect of age on the development of chemotherapy associated liver injury in colorectal cancer liver metastasis
 200 Effect of age on the development of chemotherapy associated liver injury in colorectal cancer liver metastasis TAIICHI WAKIYA 1, DAISUKE KUDO 1, KEINOSUKE ISHIDO 1, NORIHISA KIMURA 1, YUTA YAKOSHI
200 Effect of age on the development of chemotherapy associated liver injury in colorectal cancer liver metastasis TAIICHI WAKIYA 1, DAISUKE KUDO 1, KEINOSUKE ISHIDO 1, NORIHISA KIMURA 1, YUTA YAKOSHI
Multidisciplinary Treatment Strategies for Primary and Metastatic Liver Cancers
 Multidisciplinary Treatment Strategies for Primary and Metastatic Liver Cancers Ching-Wei D. Tzeng, M.D. Assistant Professor Surgical Oncology University of Kentucky Markey Cancer Center Affiliate Network
Multidisciplinary Treatment Strategies for Primary and Metastatic Liver Cancers Ching-Wei D. Tzeng, M.D. Assistant Professor Surgical Oncology University of Kentucky Markey Cancer Center Affiliate Network
Panel Two: Evidence for Use of Maintenance Therapy
 Panel Two: Evidence for Use of Maintenance Therapy Evidence for Use of Maintenance Therapy Richard L. Schilsky University of Chicago Comprehensive Cancer Center What is maintenance therapy? The continued
Panel Two: Evidence for Use of Maintenance Therapy Evidence for Use of Maintenance Therapy Richard L. Schilsky University of Chicago Comprehensive Cancer Center What is maintenance therapy? The continued
Regenerative Nodular Hyperplasia of the Liver Related to Chemotherapy: Impact on Outcome of Liver Surgery for Colorectal Metastases
 Ann Surg Oncol (2011) 18:659 669 DOI 10.1245/s10434-010-1385-5 ORIGINAL ARTICLE HEPATOBILIARY TUMORS Regenerative Nodular Hyperplasia of the Liver Related to Chemotherapy: Impact on Outcome of Liver Surgery
Ann Surg Oncol (2011) 18:659 669 DOI 10.1245/s10434-010-1385-5 ORIGINAL ARTICLE HEPATOBILIARY TUMORS Regenerative Nodular Hyperplasia of the Liver Related to Chemotherapy: Impact on Outcome of Liver Surgery
Treatment strategy of metastatic rectal cancer
 35.Schweizerische Koloproktologie-Tagung Treatment strategy of metastatic rectal cancer Gilles Mentha University hospital of Geneva Bern, January 18th, 2014 Colorectal cancer is the third most frequent
35.Schweizerische Koloproktologie-Tagung Treatment strategy of metastatic rectal cancer Gilles Mentha University hospital of Geneva Bern, January 18th, 2014 Colorectal cancer is the third most frequent
Is it possible to cure patients with liver metastases? Taghizadeh Ali MD Oncologist, MUMS
 Is it possible to cure patients with liver metastases? Taghizadeh Ali MD Oncologist, MUMS Survival Rates of by Stage of Adenocarcinoma of the Colon Liver Resection New Perspective Colorectal cancer liver
Is it possible to cure patients with liver metastases? Taghizadeh Ali MD Oncologist, MUMS Survival Rates of by Stage of Adenocarcinoma of the Colon Liver Resection New Perspective Colorectal cancer liver
State of the Art: Colorectal Cancer Liver Metastasis Dr. Iain Tan
 State of the Art: Colorectal Cancer Liver Metastasis Dr. Iain Tan Consultant GI Medical Oncologist National Cancer Centre Singapore Clinician Scientist, Genome Institute of Singapore OS (%) Overall survival
State of the Art: Colorectal Cancer Liver Metastasis Dr. Iain Tan Consultant GI Medical Oncologist National Cancer Centre Singapore Clinician Scientist, Genome Institute of Singapore OS (%) Overall survival
The Role of Adjuvant Chemotherapy for Colorectal Liver Metastasectomy after Pre-Operative Chemotherapy: Is the Treatment Worthwhile?
 1179 Ivyspring International Publisher Research Paper Journal of Cancer 2017; 8(7): 1179-1186. doi: 10.7150/jca.18091 The Role of Adjuvant Chemotherapy for Colorectal Liver Metastasectomy after Pre-Operative
1179 Ivyspring International Publisher Research Paper Journal of Cancer 2017; 8(7): 1179-1186. doi: 10.7150/jca.18091 The Role of Adjuvant Chemotherapy for Colorectal Liver Metastasectomy after Pre-Operative
Aintree University Hospital
 Aintree University Hospital Liverpool, UK Evolving role of DEBIRI with DC Bead - TACE in mcrc Hassan Z Malik MD FRCS Consultant Hepatobiliary Surgeon Hassan Z Malik is a consultant to Biocompatibles UK
Aintree University Hospital Liverpool, UK Evolving role of DEBIRI with DC Bead - TACE in mcrc Hassan Z Malik MD FRCS Consultant Hepatobiliary Surgeon Hassan Z Malik is a consultant to Biocompatibles UK
ORIGINAL ARTICLE. Effectiveness of Positron Emission Tomography for Predicting Chemotherapy Response in Colorectal Cancer Liver Metastases
 ORIGINAL ARTICLE Effectiveness of Positron Emission Tomography for Predicting Chemotherapy Response in Colorectal Cancer Liver Metastases Evan S. Glazer, MD; Karen Beaty, PA-C; Eddie K. Abdalla, MD; J.
ORIGINAL ARTICLE Effectiveness of Positron Emission Tomography for Predicting Chemotherapy Response in Colorectal Cancer Liver Metastases Evan S. Glazer, MD; Karen Beaty, PA-C; Eddie K. Abdalla, MD; J.
Targeted Therapies in Metastatic Colorectal Cancer: An Update
 Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
The efficacy of bevacizumab in Chinese patients with metastatic colorectal cancer and its effect in different line setting*
 Chinese-German J Clin Oncol DOI 10.1007/s10330-014-1295-2 April 2014, Vol. 13, No. 4, P169 P173 The efficacy of bevacizumab in Chinese patients with metastatic colorectal cancer and its effect in different
Chinese-German J Clin Oncol DOI 10.1007/s10330-014-1295-2 April 2014, Vol. 13, No. 4, P169 P173 The efficacy of bevacizumab in Chinese patients with metastatic colorectal cancer and its effect in different
Image Guidance Improves Localization of Sonographically Occult Colorectal Liver Metastases
 Image Guidance Improves Localization of Sonographically Occult Colorectal Liver Metastases Universe Leung a, Amber L. Simpson a,b, Lauryn B. Adams a, William R. Jarnagin a, Michael I. Miga b, and T. Peter
Image Guidance Improves Localization of Sonographically Occult Colorectal Liver Metastases Universe Leung a, Amber L. Simpson a,b, Lauryn B. Adams a, William R. Jarnagin a, Michael I. Miga b, and T. Peter
Current Status of Adjuvant Therapy for Colorectal Cancer
 Review Article [1] May 01, 2004 By Michael J. O connell, MD [2] Adjuvant therapy with chemotherapy and/or radiation therapy in addition to surgery improves outcome for patients with high-risk carcinomas
Review Article [1] May 01, 2004 By Michael J. O connell, MD [2] Adjuvant therapy with chemotherapy and/or radiation therapy in addition to surgery improves outcome for patients with high-risk carcinomas
State of the art management of Colorectal Liver Metastasis: an interplay of Chemotherapy and Surgical options
 State of the art management of Colorectal Liver Metastasis: an interplay of Chemotherapy and Surgical options Ioannis S. Hatzaras, MD, MPH, FACS Assistant Professor of Surgery Division of Surgical Oncology
State of the art management of Colorectal Liver Metastasis: an interplay of Chemotherapy and Surgical options Ioannis S. Hatzaras, MD, MPH, FACS Assistant Professor of Surgery Division of Surgical Oncology
Case Report Management of a Patient with Metastatic Colorectal Cancer and Liver Metastases
 Case Reports in Oncological Medicine, Article ID 790192, 4 pages http://dx.doi.org/10.1155/2014/790192 Case Report Management of a Patient with Metastatic Colorectal Cancer and Liver Metastases Muhammad
Case Reports in Oncological Medicine, Article ID 790192, 4 pages http://dx.doi.org/10.1155/2014/790192 Case Report Management of a Patient with Metastatic Colorectal Cancer and Liver Metastases Muhammad
Colon Cancer Molecular Target Agents
 Colon Cancer Molecular Target Agents Ci Caio Max SR S. Rocha Lima, M.D. MD Professor of Medicine CDi CoDiretor Cl Colorectal tlheptobiliary, Pancreatic SDG, and Phase I Unit University of Miami & Silvester
Colon Cancer Molecular Target Agents Ci Caio Max SR S. Rocha Lima, M.D. MD Professor of Medicine CDi CoDiretor Cl Colorectal tlheptobiliary, Pancreatic SDG, and Phase I Unit University of Miami & Silvester
Where Are Anti-Angiogenic Agents Positioned Within Cancer Care Guidelines?
 Introduction Additionally, other anti-angiogenic drugs, including sorafenib, sunitinib, axitinib, pazopanib, vandetanib, The development and subsequent use of drugs for treating cancer cabozantinib, and
Introduction Additionally, other anti-angiogenic drugs, including sorafenib, sunitinib, axitinib, pazopanib, vandetanib, The development and subsequent use of drugs for treating cancer cabozantinib, and
New Options in Metastatic Colorectal Cancer. Jeffrey A. Bubis, DO, FACOI, FACP Fleming Island Baptist South Palatka
 New Options in Metastatic Colorectal Cancer Jeffrey A. Bubis, DO, FACOI, FACP Fleming Island Baptist South Palatka 4 th most frequently diagnosed CA in the US 2 nd leading cause of CA death in the US Incidence
New Options in Metastatic Colorectal Cancer Jeffrey A. Bubis, DO, FACOI, FACP Fleming Island Baptist South Palatka 4 th most frequently diagnosed CA in the US 2 nd leading cause of CA death in the US Incidence
Medicinae Doctoris. One university. Many futures.
 Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Surgical treatment of colorectal liver metastases
 Review Article Page 1 of 9 Surgical treatment of colorectal liver metastases Amanda B. Cooper, Steven A. Curley Department of Surgical Oncology, The University of Texas M.D. Anderson Cancer Center, Houston,
Review Article Page 1 of 9 Surgical treatment of colorectal liver metastases Amanda B. Cooper, Steven A. Curley Department of Surgical Oncology, The University of Texas M.D. Anderson Cancer Center, Houston,
Trattamento chirurgico delle lesioni epatiche secondarie difficili. Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica
 Trattamento chirurgico delle lesioni epatiche secondarie difficili Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica What does it mean difficult lesions? Diagnosis Treatment Small size Unfit
Trattamento chirurgico delle lesioni epatiche secondarie difficili Adelmo Antonucci Chirurgia Oncologica e Epato-bilio-pancreatica What does it mean difficult lesions? Diagnosis Treatment Small size Unfit
Complete pathological response (ypt0n0m0) after preoperative chemotherapy alone for stage IV rectal cancer
 CASE REPORT Open Access Complete pathological response (ypt0n0m0) after preoperative chemotherapy alone for stage IV rectal cancer Surennaidoo P Naiken 1*, Christian Toso 1, Laura Rubbia-Brandt 2, Theodoros
CASE REPORT Open Access Complete pathological response (ypt0n0m0) after preoperative chemotherapy alone for stage IV rectal cancer Surennaidoo P Naiken 1*, Christian Toso 1, Laura Rubbia-Brandt 2, Theodoros
8 Giornata Onco-ematologica Varesina
 Azienda Ospedaliera Sant Antonio Abate di Gallarate 8 Giornata Onco-ematologica Varesina Le esperienze di eccellenza del DIPO di Varese Metastasi epatiche da tumore del colon-retto: terapia medica in funzione
Azienda Ospedaliera Sant Antonio Abate di Gallarate 8 Giornata Onco-ematologica Varesina Le esperienze di eccellenza del DIPO di Varese Metastasi epatiche da tumore del colon-retto: terapia medica in funzione
Oxaliplatin-induced Liver Injury Mimicking Metastatic Tumor on Images: A Case Report
 Jpn J Clin Oncol 2013;43(10)1034 1038 doi:10.1093/jjco/hyt113 Advance Access Publication 19 August 2013 Oxaliplatin-induced Liver Injury Mimicking Metastatic Tumor on Images: A Case Report Kaori Uchino
Jpn J Clin Oncol 2013;43(10)1034 1038 doi:10.1093/jjco/hyt113 Advance Access Publication 19 August 2013 Oxaliplatin-induced Liver Injury Mimicking Metastatic Tumor on Images: A Case Report Kaori Uchino
Management of colorectal cancer liver metastases
 Management of colorectal cancer liver metastases Aliakbarian M. M.D. Assistant professor of surgery Organ Transplant & Hepatopancreatobiliary Surgeon SUBJECTS The importance of surgical resection in colorectal
Management of colorectal cancer liver metastases Aliakbarian M. M.D. Assistant professor of surgery Organ Transplant & Hepatopancreatobiliary Surgeon SUBJECTS The importance of surgical resection in colorectal
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Index Note: Page numbers of article titles are in boldface type. A Abdominal drainage, after hepatic resection, 159 160 Ablation, radiofrequency, for hepatocellular carcinoma, 160 161 Adenocarcinoma, pancreatic.
Colorectal Liver Metastases
 J Gastrointest Surg (2013) 17:195 202 DOI 10.1007/s11605-012-2022-3 EVIDENCE-BASED CURRENT SURGICAL PRACTICE Colorectal Liver Metastases Ching-Wei D. Tzeng & Thomas A. Aloia Received: 22 July 2012 /Accepted:
J Gastrointest Surg (2013) 17:195 202 DOI 10.1007/s11605-012-2022-3 EVIDENCE-BASED CURRENT SURGICAL PRACTICE Colorectal Liver Metastases Ching-Wei D. Tzeng & Thomas A. Aloia Received: 22 July 2012 /Accepted:
Embolotherapy for Cholangiocarcinoma: 2016 Update
 Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Embolotherapy for Cholangiocarcinoma: 2016 Update Igor Lobko,MD Chief, Division Vascular and Interventional Radiology Long Island Jewish Medical Center GEST 2016 Igor Lobko, M.D. No relevant financial
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Kaoru Takeshima, Kazuo Yamafuji, Atsunori Asami, Hideo Baba, Nobuhiko Okamoto, Hidena Takahashi, Chisato Takagi, and Kiyoshi Kubochi
 Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Case Reports in Surgery Volume 2016, Article ID 4548798, 5 pages http://dx.doi.org/10.1155/2016/4548798 Case Report Successful Resection of Isolated Para-Aortic Lymph Node Recurrence from Advanced Sigmoid
Colorectal Liver Metastases Metachronous
 Colorectal Liver Metastases Metachronous Professor Rowan Parks Professor of Surgical Sciences University of Edinburgh No disclosures Natural History of Unresected Untreated Colorectal Metastases Year N
Colorectal Liver Metastases Metachronous Professor Rowan Parks Professor of Surgical Sciences University of Edinburgh No disclosures Natural History of Unresected Untreated Colorectal Metastases Year N
Neoadjuvant and conversion treatment of patients with colorectal liver metastasis: the potential role of bevacizumab and other antiangiogenic agents
 Targ Oncol (2015) 10:453 465 DOI 10.1007/s11523-015-0362-0 REVIEW Neoadjuvant and conversion treatment of patients with colorectal liver metastasis: the potential role of bevacizumab and other antiangiogenic
Targ Oncol (2015) 10:453 465 DOI 10.1007/s11523-015-0362-0 REVIEW Neoadjuvant and conversion treatment of patients with colorectal liver metastasis: the potential role of bevacizumab and other antiangiogenic
Trends and Comparative Effectiveness in Treatment of Stage IV Colorectal Adenocarcinoma
 Trends and Comparative Effectiveness in Treatment of Stage IV Colorectal Adenocarcinoma Taylor S. Riall, MD, PhD CERCIT Workshop October 19, 2012 Department of Surgery Center for Comparative Effectiveness
Trends and Comparative Effectiveness in Treatment of Stage IV Colorectal Adenocarcinoma Taylor S. Riall, MD, PhD CERCIT Workshop October 19, 2012 Department of Surgery Center for Comparative Effectiveness
Are we making progress? Marked reduction in operative morbidity and mortality
 Are we making progress? Surgical Progress Marked reduction in operative morbidity and mortality Introduction of Minimal-Access approaches for complex esophageal cancer resections Significantly better functional
Are we making progress? Surgical Progress Marked reduction in operative morbidity and mortality Introduction of Minimal-Access approaches for complex esophageal cancer resections Significantly better functional
Chemotherapy for resectable liver mets: Options and Issues. Herbert Hurwitz Duke University Medical Center Durham, North Carolina, USA
 Chemotherapy for resectable liver mets: Options and Issues Herbert Hurwitz Duke University Medical Center Durham, North Carolina, USA Chemotherapy regimens in 1 st line mcrc Standard FOLFOX-Bev FOLFIRI-Bev
Chemotherapy for resectable liver mets: Options and Issues Herbert Hurwitz Duke University Medical Center Durham, North Carolina, USA Chemotherapy regimens in 1 st line mcrc Standard FOLFOX-Bev FOLFIRI-Bev
Management of Colorectal Liver Metastases
 Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Management of Colorectal Liver Metastases MM Bernon, JEJ Krige HPB Surgical Unit, Groote Schuur Hospital Department of Surgery, University of Cape Town 50% of patients with colorectal cancer develop liver
Chemotherapy of colon cancers
 Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GASTROINTESTINAL RECTAL CANCER GI Site Group Rectal Cancer Authors: Dr. Jennifer Knox, Dr. Mairead McNamara 1. INTRODUCTION 3 2. SCREENING AND
Risk factors for cancer recurrence or death within 6 months after liver resection in patients with colorectal cancer liver metastasis
 ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.5.257 Annals of Surgical Treatment and Research Risk factors for cancer recurrence or death within 6 months after
ORIGINAL ARTICLE pissn 2288-6575 eissn 2288-6796 http://dx.doi.org/10.4174/astr.2016.90.5.257 Annals of Surgical Treatment and Research Risk factors for cancer recurrence or death within 6 months after
Colorectal cancer is the second leading cause of cancer-related
 ORIGINAL ARTICLES Long-Term Outcome of Initially Unresectable Metastatic Colorectal Cancer Patients Treated with 5-Fluorouracil/Leucovorin, Oxaliplatin, and Irinotecan (FOLFOXIRI) Followed by Radical Surgery
ORIGINAL ARTICLES Long-Term Outcome of Initially Unresectable Metastatic Colorectal Cancer Patients Treated with 5-Fluorouracil/Leucovorin, Oxaliplatin, and Irinotecan (FOLFOXIRI) Followed by Radical Surgery
ADVANCED COLORECTAL CANCER: UNRESECTABLE OR BORDERLINE RESECTABLE (GROUP 1) CHEMOTHERAPY +/- TARGETED AGENTS. Andrés Cervantes. Professor of Medicine
 ADVANCED COLORECTAL CANCER: UNRESECTABLE OR BORDERLINE RESECTABLE (GROUP 1) CHEMOTHERAPY +/- TARGETED AGENTS Andrés Cervantes Professor of Medicine 1995 One option Advances in the treatment of mcrc 2000
ADVANCED COLORECTAL CANCER: UNRESECTABLE OR BORDERLINE RESECTABLE (GROUP 1) CHEMOTHERAPY +/- TARGETED AGENTS Andrés Cervantes Professor of Medicine 1995 One option Advances in the treatment of mcrc 2000
Management of Stage IV Colorectal Cancer: Expanding the Horizon
 Management of Stage IV Colorectal Cancer: Expanding the Horizon May Tee, MD, MPH and Jan Franko, MD, PhD MercyOne Surgical Group (Mercy Surgical Affiliates) GI Oncology Conference 2019 March 1, 2019 Disclosures
Management of Stage IV Colorectal Cancer: Expanding the Horizon May Tee, MD, MPH and Jan Franko, MD, PhD MercyOne Surgical Group (Mercy Surgical Affiliates) GI Oncology Conference 2019 March 1, 2019 Disclosures
Tumor Marker Evolution: Comparison with Imaging for Assessment of Response to Chemotherapy in Patients with Colorectal Liver Metastases
 Ann Surg Oncol DOI 1.1245/s1434-9-887-5 ORIGINAL ARTICLE HEPATOBILIARY TUMORS Tumor Marker Evolution: Comparison with Imaging for Assessment of Response to Chemotherapy in with Colorectal Liver Metastases
Ann Surg Oncol DOI 1.1245/s1434-9-887-5 ORIGINAL ARTICLE HEPATOBILIARY TUMORS Tumor Marker Evolution: Comparison with Imaging for Assessment of Response to Chemotherapy in with Colorectal Liver Metastases
* * * * Supplementary Figure 1. DS Lv CK HSA CK HSA. CK Col-3. CK Col-3. See overleaf for figure legend. Cancer cells
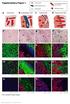 Supplementary Figure 1 Cancer cells Desmoplastic stroma Hepatocytes Pre-existing sinusoidal blood vessel New blood vessel a Normal liver b Desmoplastic HGP c Pushing HGP d Replacement HGP e f g h i DS
Supplementary Figure 1 Cancer cells Desmoplastic stroma Hepatocytes Pre-existing sinusoidal blood vessel New blood vessel a Normal liver b Desmoplastic HGP c Pushing HGP d Replacement HGP e f g h i DS
Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers
 日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
日大医誌 75 (1): 10 15 (2016) 10 Original Article Implications of Progesterone Receptor Status for the Biology and Prognosis of Breast Cancers Naotaka Uchida 1), Yasuki Matsui 1), Takeshi Notsu 1) and Manabu
Evaluating and Reporting Gastrointestinal Stromal Tumors after Imatinib Mesylate Treatment
 The Open Pathology Journal, 2009, 3, 53-57 53 Open Access Evaluating and Reporting Gastrointestinal Stromal Tumors after Imatinib Mesylate Treatment Katie L. Dennis * and Ivan Damjanov Department of Pathology
The Open Pathology Journal, 2009, 3, 53-57 53 Open Access Evaluating and Reporting Gastrointestinal Stromal Tumors after Imatinib Mesylate Treatment Katie L. Dennis * and Ivan Damjanov Department of Pathology
Effective Panitumumab Treatment in Patients with Heavily Pre-treated Metastatic Colorectal Cancer: A Case Series
 Effective Panitumumab Treatment in Patients with Heavily Pre-treated Metastatic Colorectal Cancer: A Case Series ALEXANDROS A. TZOVARAS, ATHANASSIOS KARAGIANNIS, CHARALAMBIA MARGARI, GEORGIA BARLA and
Effective Panitumumab Treatment in Patients with Heavily Pre-treated Metastatic Colorectal Cancer: A Case Series ALEXANDROS A. TZOVARAS, ATHANASSIOS KARAGIANNIS, CHARALAMBIA MARGARI, GEORGIA BARLA and
Current Controversies in the Surgical Management of Colorectal Cancer Metastases to the Liver
 Current Controversies in the Surgical Management of Colorectal Cancer Metastases to the Liver Risa Small BA, Nir Lubezky MD and Menahem Ben-Haim MD Liver Surgery Unit, Department of Surgery B, Tel Aviv
Current Controversies in the Surgical Management of Colorectal Cancer Metastases to the Liver Risa Small BA, Nir Lubezky MD and Menahem Ben-Haim MD Liver Surgery Unit, Department of Surgery B, Tel Aviv
Primary tumor with synchronous metastases
 Metastatic colorectal cancer: special clinical situations Primary tumor with synchronous metastases Stefan Heinrich & Hauke Lang Department of General, Visceral and Transplantation Surgery University Hospital
Metastatic colorectal cancer: special clinical situations Primary tumor with synchronous metastases Stefan Heinrich & Hauke Lang Department of General, Visceral and Transplantation Surgery University Hospital
What s New in Colon Cancer? Therapy over the last decade
 What s New in Colon Cancer? 9/19/2014 Michael McNamara, MD Therapy over the last decade Cytotoxic chemotherapy - 5FU ( Mayo, Roswell, Infusional) - Xeloda (01 ) - Oxaliplatin (02 ) - Irinotecan (96 ) Anti-
What s New in Colon Cancer? 9/19/2014 Michael McNamara, MD Therapy over the last decade Cytotoxic chemotherapy - 5FU ( Mayo, Roswell, Infusional) - Xeloda (01 ) - Oxaliplatin (02 ) - Irinotecan (96 ) Anti-
COMETS: COlorectal MEtastatic Two Sequences
 COMETS: COlorectal MEtastatic Two Sequences A Phase III Multicenter Trial Comparing Two Different Sequences of Second/Third Line Therapy (Irinotecan/Cetuximab Followed By FOLFOX-4 vs. FOLFOX-4 Followed
COMETS: COlorectal MEtastatic Two Sequences A Phase III Multicenter Trial Comparing Two Different Sequences of Second/Third Line Therapy (Irinotecan/Cetuximab Followed By FOLFOX-4 vs. FOLFOX-4 Followed
Unresectable or boarderline resectable disease
 ESMO Preceptorship Colorectal Cancer Nov 2016 Barcelona Unresectable or boarderline resectable disease Claus-Henning Köhne Klinik für Onkologie und Hämatologie North West German Cancer Center (NWTZ) Learning
ESMO Preceptorship Colorectal Cancer Nov 2016 Barcelona Unresectable or boarderline resectable disease Claus-Henning Köhne Klinik für Onkologie und Hämatologie North West German Cancer Center (NWTZ) Learning
FIRST LINE 5-FU-BASED CHEMOTHERAPY WITH/ WITHOUT BEVACIZUMAB FOR METASTATIC COLORECTAL CANCER: ONE CENTER EXPERIENCE RESULTS
 PROCEEDINGS FIRST LINE 5-FU-BASED CHEMOTHERAPY WITH/ WITHOUT BEVACIZUMAB FOR METASTATIC COLORECTAL CANCER: ONE CENTER EXPERIENCE RESULTS Assia Konsoulova, Ivan Donev, Nikolay Conev, Sonya Draganova, Trifon
PROCEEDINGS FIRST LINE 5-FU-BASED CHEMOTHERAPY WITH/ WITHOUT BEVACIZUMAB FOR METASTATIC COLORECTAL CANCER: ONE CENTER EXPERIENCE RESULTS Assia Konsoulova, Ivan Donev, Nikolay Conev, Sonya Draganova, Trifon
SECONDARIES: A PRELIMINARY REPORT
 HPB Surgery, 1990, Vol. 2, pp. 69-72 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORTS
HPB Surgery, 1990, Vol. 2, pp. 69-72 Reprints available directly from the publisher Photocopying permitted by license only 1990 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORTS
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
abcd Clinical Study for Public Disclosure This clinical study synopsis is provided in line with s Policy on Transparency and Publication of Clinical Study Data. The synopsis which is part of the clinical
Clinical Studies. Keywords: metastatic; colorectal cancer; bevacizumab; curative-intent; R0 metastasectomy
 British Journal of Cancer (2009) 101, 1033 1038 All rights reserved 0007 0920/09 $32.00 www.bjcancer.com Surgery with curative-intent in patients treated with first-line chemotherapy plus bevacizumab for
British Journal of Cancer (2009) 101, 1033 1038 All rights reserved 0007 0920/09 $32.00 www.bjcancer.com Surgery with curative-intent in patients treated with first-line chemotherapy plus bevacizumab for
Carcinoma del retto: Highlights
 Carcinoma del retto: Highlights Stefano Cordio Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Roma 17 Febbraio 2018 Disclosures Advisory Committee, research funding and speakers bureau
Carcinoma del retto: Highlights Stefano Cordio Struttura Complessa di Oncologia Medica ARNAS Garibaldi Catania Roma 17 Febbraio 2018 Disclosures Advisory Committee, research funding and speakers bureau
Gastrointestinal Stromal Tumor Case Presentations
 Gastrointestinal Stromal Tumor Case Presentations Ricardo J. Gonzalez, MD Professor of Surgery Chair, Sarcoma Department Chief of Surgery Moffitt Cancer Center Patient number 1 64 yo male with upper abdominal
Gastrointestinal Stromal Tumor Case Presentations Ricardo J. Gonzalez, MD Professor of Surgery Chair, Sarcoma Department Chief of Surgery Moffitt Cancer Center Patient number 1 64 yo male with upper abdominal
Advances in gastric cancer: How to approach localised disease?
 Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Advances in gastric cancer: How to approach localised disease? Andrés Cervantes Professor of Medicine Classical approach to localised gastric cancer Surgical resection Pathology assessment and estimation
Present Status and Perspectives of Colorectal Cancer in Asia: Colorectal Cancer Working Group Report in 30th Asia-Pacific Cancer Conference
 Present Status and Perspectives of Colorectal Cancer in Asia: Colorectal Cancer Working Group Report in 30th Asia-Pacific Cancer Conference Jpn J Clin Oncol 2010;40(Supplement 1)i38 i43 doi:10.1093/jjco/hyq125
Present Status and Perspectives of Colorectal Cancer in Asia: Colorectal Cancer Working Group Report in 30th Asia-Pacific Cancer Conference Jpn J Clin Oncol 2010;40(Supplement 1)i38 i43 doi:10.1093/jjco/hyq125
Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients
 Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients Bradley Carthon, MD, PhD Assistant Professor, Genitourinary Medical Oncology Winship
Winship Cancer Institute of Emory University Neoadjuvant Systemic Therapy in Metastatic Renal Cell Carcinoma Patients Bradley Carthon, MD, PhD Assistant Professor, Genitourinary Medical Oncology Winship
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Nivolumab for previously treated metastatic colorectal cancer with high microsatellite instability or mismatch repair deficiency
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Health Technology Appraisal Nivolumab for previously treated metastatic colorectal cancer with high microsatellite instability or mismatch repair deficiency
Bevacizumab is currently licensed for the following indication relevant for this NICE review:
 Roche Executive Summary Context Bevacizumab (Avastin) is a humanized (93% human) murine monoclonal antibody which binds to and neutralizes VEGF, a powerful pro-angiogenic glycoprotein produced by both
Roche Executive Summary Context Bevacizumab (Avastin) is a humanized (93% human) murine monoclonal antibody which binds to and neutralizes VEGF, a powerful pro-angiogenic glycoprotein produced by both
Ryosuke Arata 1, Toshiyuki Itamoto 1,4*, Satoshi Ikeda 1, Hideki Nakahara 1, Akihiko Oshita 1,4, Katsunori Shinozaki 2 and Takashi Nishisaka 3
 Arata et al. Surgical Case Reports (2016) 2:106 DOI 10.1186/s40792-016-0231-9 CASE REPORT Pathological complete response after neoadjuvant chemotherapy for rectal cancer with synchronous multiple liver
Arata et al. Surgical Case Reports (2016) 2:106 DOI 10.1186/s40792-016-0231-9 CASE REPORT Pathological complete response after neoadjuvant chemotherapy for rectal cancer with synchronous multiple liver
Aggressive surgery in the multimodality treatment of liver metastases from colorectal cancer
 Journal of BUON 12: 209-213, 2007 2007 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Aggressive surgery in the multimodality treatment of liver metastases from colorectal cancer N.
Journal of BUON 12: 209-213, 2007 2007 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Aggressive surgery in the multimodality treatment of liver metastases from colorectal cancer N.
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database
 Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Surgical Management of Metastatic Colon Cancer: analysis of the Surveillance, Epidemiology and End Results (SEER) database Hadi Khan, MD 1, Adam J. Olszewski, MD 2 and Ponnandai S. Somasundar, MD 1 1 Department
Adjuvant therapies for large bowel cancer Wasantha Rathnayake, MD
 LEADING ARTICLE Adjuvant therapies for large bowel cancer Wasantha Rathnayake, MD Consultant Clinical Oncologist, National Cancer Institute, Maharagama, Sri Lanka. Key words: Large bowel; Cancer; Adjuvant
LEADING ARTICLE Adjuvant therapies for large bowel cancer Wasantha Rathnayake, MD Consultant Clinical Oncologist, National Cancer Institute, Maharagama, Sri Lanka. Key words: Large bowel; Cancer; Adjuvant
Perioperative Chemotherapy With or Without Bevacizumab in Patients With Metastatic Colorectal Cancer Undergoing Liver Resection
 Original Study Perioperative With or Without Bevacizumab in Patients With Metastatic Colorectal Cancer Undergoing Liver Resection Anastasia Constantinidou, 1 David Cunningham, 1 Fatima Shurmahi, 1 Uzma
Original Study Perioperative With or Without Bevacizumab in Patients With Metastatic Colorectal Cancer Undergoing Liver Resection Anastasia Constantinidou, 1 David Cunningham, 1 Fatima Shurmahi, 1 Uzma
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain
 Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Adjuvant and neoadjuvant chemotherapy for rectal cancer: Expensive but little gain Outline The problem Adjuvant therapy Neoadjuvant therapy Options Conclusion The problem 30 years ago: Local recurrence
Efficacy of Neoadjuvant Chemotherapy Regimens Prior to Resection of Colorectal Liver Metastases
 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2-11-2008 Efficacy of Neoadjuvant Chemotherapy Regimens Prior to Resection
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2-11-2008 Efficacy of Neoadjuvant Chemotherapy Regimens Prior to Resection
The International Duration Evaluation of Adjuvant Chemotherapy study: implications for clinical practice
 Editorial The International Duration Evaluation of Adjuvant Chemotherapy study: implications for clinical practice Marwan Fakih Department of Medical Oncology and Therapeutics Research, City of Hope Comprehensive
Editorial The International Duration Evaluation of Adjuvant Chemotherapy study: implications for clinical practice Marwan Fakih Department of Medical Oncology and Therapeutics Research, City of Hope Comprehensive
INFLUENCE OF PRE-OPERATIVE CHEMOTHERAPY ON HEPATIC MORPHO-PATHOLOGY
 INFLUENCE OF PRE-OPERATIVE CHEMOTHERAPY ON HEPATIC MORPHO-PATHOLOGY Carolina Negrei 1, George Traian Alexandru Burcea Dragomiroiu 2, Octav Ginghină 3*, Daniel Boda 4, Bianca Galateanu 5, Miriana Stan 1,
INFLUENCE OF PRE-OPERATIVE CHEMOTHERAPY ON HEPATIC MORPHO-PATHOLOGY Carolina Negrei 1, George Traian Alexandru Burcea Dragomiroiu 2, Octav Ginghină 3*, Daniel Boda 4, Bianca Galateanu 5, Miriana Stan 1,
Gastrointestinal Imaging Original Research
 Gastrointestinal Imaging Original Research Chung et al. Response Evaluation in Patients With Colorectal Liver Metastases Gastrointestinal Imaging Original Research Woo-Suk Chung 1 Mi-Suk Park 1 Sang Joon
Gastrointestinal Imaging Original Research Chung et al. Response Evaluation in Patients With Colorectal Liver Metastases Gastrointestinal Imaging Original Research Woo-Suk Chung 1 Mi-Suk Park 1 Sang Joon
Correspondence should be addressed to Roland Andersson,
 Gastroenterology Research and Practice Volume 2012, Article ID 568214, 4 pages doi:10.1155/2012/568214 Research Article Repeated Liver Resection for Colorectal Liver Metastases: A Comparison with Primary
Gastroenterology Research and Practice Volume 2012, Article ID 568214, 4 pages doi:10.1155/2012/568214 Research Article Repeated Liver Resection for Colorectal Liver Metastases: A Comparison with Primary
How to deal with synchronous primary and liver metastases
 How to deal with synchronous primary and liver metastases Luis Sabater Ortí MD, PhD Associate Professor University of Valencia European Board Surgical Qualification HBP (EBSQ-HPB) Department of Surgery.
How to deal with synchronous primary and liver metastases Luis Sabater Ortí MD, PhD Associate Professor University of Valencia European Board Surgical Qualification HBP (EBSQ-HPB) Department of Surgery.
My name is Dr. David Ilson, Professor of Medicine at Memorial Sloan Kettering Cancer Center and Weill Cornell Medical Center in New York, New York.
 Welcome to this CME/CE-certified activity entitled, Integrating the Latest Advances Into Clinical Experience: Data and Expert Insights From the 2016 Meeting on Gastrointestinal Cancers in San Francisco.
Welcome to this CME/CE-certified activity entitled, Integrating the Latest Advances Into Clinical Experience: Data and Expert Insights From the 2016 Meeting on Gastrointestinal Cancers in San Francisco.
Peritoneal Involvement in Stage II Colon Cancer
 Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Anatomic Pathology / PERITONEAL INVOLVEMENT IN STAGE II COLON CANCER Peritoneal Involvement in Stage II Colon Cancer A.M. Lennon, MB, MRCPI, H.E. Mulcahy, MD, MRCPI, J.M.P. Hyland, MCh, FRCS, FRCSI, C.
Title: What is the role of pre-operative PET/PET-CT in the management of patients with
 Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Title: What is the role of pre-operative PET/PET-CT in the management of patients with potentially resectable colorectal cancer liver metastasis? Pablo E. Serrano, Julian F. Daza, Natalie M. Solis June
Department of Surgery, Institute of Health Biosciences, The University of Tokushima Graduate School, Tokushima, Japan
 bs_bs_banner Hepatology Research 2014; 44: 59 69 doi: 10.1111/hepr.12107 Review Article Evaluation and management of hepatic injury induced by oxaliplatin-based chemotherapy in patients with hepatic resection
bs_bs_banner Hepatology Research 2014; 44: 59 69 doi: 10.1111/hepr.12107 Review Article Evaluation and management of hepatic injury induced by oxaliplatin-based chemotherapy in patients with hepatic resection
COLON CANCER PERITONEAL CARCINOMATOSIS TREATMENT Prof. Annibale Donini
 UNIVERSITY OF PERUGIA Department of General and Emergency Surgery Chief: Prof. Annibale Donini COLON CANCER PERITONEAL CARCINOMATOSIS TREATMENT Prof. Annibale Donini COLON CANCER IS A HIGHLY FREQUENT NEOPLASIA
UNIVERSITY OF PERUGIA Department of General and Emergency Surgery Chief: Prof. Annibale Donini COLON CANCER PERITONEAL CARCINOMATOSIS TREATMENT Prof. Annibale Donini COLON CANCER IS A HIGHLY FREQUENT NEOPLASIA
MEETING SUMMARY ESMO 2018, Munich, Germany. Dr. Jenny Seligmann University of Leeds, UK HIGHLIGHTS ON COLORECTAL CANCER
 MEETING SUMMARY ESMO 2018, Munich, Germany Dr. Jenny Seligmann University of Leeds, UK HIGHLIGHTS ON COLORECTAL CANCER DISCLAIMER Please note: The views expressed within this presentation are the personal
MEETING SUMMARY ESMO 2018, Munich, Germany Dr. Jenny Seligmann University of Leeds, UK HIGHLIGHTS ON COLORECTAL CANCER DISCLAIMER Please note: The views expressed within this presentation are the personal
DALLA CAPECITABINA AL TAS 102
 DALLA CAPECITABINA AL TAS 102 Milano 29 settembre 2016 LE PROSPETTIVE NELLA RICERCA Armando Santoro Humanitas Cancer Center THE 1,2.AND 3 LINE CHEMOTHERAPY IN CRC M BEVACIZUMAB AFLIBERCET RAS wt RAS mu
DALLA CAPECITABINA AL TAS 102 Milano 29 settembre 2016 LE PROSPETTIVE NELLA RICERCA Armando Santoro Humanitas Cancer Center THE 1,2.AND 3 LINE CHEMOTHERAPY IN CRC M BEVACIZUMAB AFLIBERCET RAS wt RAS mu
ORIGINAL ARTICLE. A Second Liver Resection Due to Recurrent Colorectal Liver Metastases. accepted as the only curative
 ORIGINAL ARTICLE A Second Liver Resection Due to Recurrent Colorectal Liver Metastases Antonio Sa Cunha, MD; Christophe Laurent, MD; Alexandre Rault, MD; Philippe Couderc, MD; Eric Rullier, MD; Jean Saric,
ORIGINAL ARTICLE A Second Liver Resection Due to Recurrent Colorectal Liver Metastases Antonio Sa Cunha, MD; Christophe Laurent, MD; Alexandre Rault, MD; Philippe Couderc, MD; Eric Rullier, MD; Jean Saric,
Patient Presentation. 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201
 Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Patient Presentation 32 y.o. female complains of lower abdominal mass CEA = 433, CA125 = 201 CT shows: Thickening of the right hemidiaphragm CT shows: Fluid in the right paracolic sulcus CT shows: Large
Case Conference. Craig Morgenthal Department of Surgery Long Island College Hospital
 Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
Case Conference Craig Morgenthal Department of Surgery Long Island College Hospital Neoadjuvant versus Adjuvant Radiation Therapy in Rectal Carcinoma Epidemiology American Cancer Society statistics for
ADJUVANT CHEMOTHERAPY...
 Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Colorectal Pathway Board: Non-Surgical Oncology Guidelines October 2015 Organization» Table of Contents ADJUVANT CHEMOTHERAPY... 2 DUKES C/ TNM STAGE 3... 2 DUKES B/ TNM STAGE 2... 3 LOCALLY ADVANCED
Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study
 Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Original Article Outcome of rectal cancer after radiotherapy with a long or short waiting period before surgery, a descriptive clinical study Elmer E. van Eeghen 1, Frank den Boer 2, Sandra D. Bakker 1,
Hepatic Lesions that Mimic Metastasis on Radiological Imaging during Chemotherapy for Gastrointestinal Malignancy: Recent Updates
 Review Article Gastrointestinal Imaging hepatic nodule could change both the clinical cancer stage and the therapeutic plan. Therefore, if radiologists are aware of a history of underlying gastrointestinal
Review Article Gastrointestinal Imaging hepatic nodule could change both the clinical cancer stage and the therapeutic plan. Therefore, if radiologists are aware of a history of underlying gastrointestinal
Systemic Therapy for Metastatic Colorectal Cancer: Patterns of Chemotherapy and Biologic Therapy Use in US Medical Oncology Practice
 Original Contribution Systemic Therapy for Metastatic Colorectal Cancer: Patterns of Chemotherapy and Biologic Therapy Use in US Medical Oncology Practice By Gregory P. Hess, MD, MSc, Peter Feng Wang,
Original Contribution Systemic Therapy for Metastatic Colorectal Cancer: Patterns of Chemotherapy and Biologic Therapy Use in US Medical Oncology Practice By Gregory P. Hess, MD, MSc, Peter Feng Wang,
