Conventionally, the role of chemotherapy in
|
|
|
- Sabina Freeman
- 5 years ago
- Views:
Transcription
1 THE ROLE OF CHEMOTHERAPY AND OTHER MODALITIES IN HEAD AND NECK CANCER * Patrick J. Medina, PharmD, BCOP ABSTRACT For patients with head and neck cancer (HNCA), therapy for earlier-stage disease has traditionally involved surgery and radiation, and chemotherapy has been relegated to palliation for metastatic disease. Recently, an increase in the use of antineoplastic agents for earlier stages of HNCA has been seen. The taxanes, 5-fluorouracil, and the platinum analogs cisplatin and carboplatin are the workhorses of HNCA chemotherapy. With increasing frequency, they are being combined with radiotherapy to improve locoregional control and organ preservation and to reduce the formation of distant metastases and the incidence of severe, acute, treatment-related adverse side effects, particularly mucositis. Although neoadjuvant therapy has yet to be conclusively proven to be beneficial, combined chemoradiation has shown some promise in randomized trials. Although the radiosensitizing effects of cisplatin are valuable, cisplatin is not tumor specific, and dose-related toxicities limit its use. Another clinical conundrum is posed by patients with metastatic disease, in whom combination chemotherapy trials consistently show increased response rates but no survival benefit. To boost survival rates, the current focus is on the development of targeted therapies, *Based on a presentation given by Dr Medina at a satellite symposium held in conjunction with the 40th Annual American Society of Health-System Pharmacists Midyear Clinical Meeting on December 5, 2005, in Las Vegas, Nevada. Associate Professor, Department of Pharmacy, Clinical and Administrative Sciences, The University of Oklahoma College of Pharmacy, Oklahoma City, Oklahoma. Address correspondence to: Patrick J. Medina, PharmD, BCOP, Associate Professor, Department of Pharmacy, Clinical and Administrative Sciences, The University of Oklahoma College of Pharmacy, 1110 North Stonewall, Oklahoma City, OK Patrick-Medina@ouhsc.edu. such as the epidermal growth factor receptor (EGFR) inhibitors erlotinib and gefitinib, which are small-molecule tyrosine kinase inhibitors, and cetuximab, a chimeric human-murine monoclonal IgG 1 antibody. Emerging clinical data are demonstrating the value of EGFR inhibitors in HNCA, and additional studies are being planned to assess their value when combined with the traditional treatment modalities. (Adv Stud Pharm. 2006;3(1):12-20) Conventionally, the role of chemotherapy in patients with head and neck cancer (HNCA) has been limited to palliation. However, the role of chemotherapy in the definitive management of these malignancies has evolved tremendously in the past decade. Recent data from randomized trials support a role for chemotherapy as part of combined-modality, curative treatment strategies in the management of patients with unresectable disease or advanced HNCA. In addition, targeted biologic agents, such as epidermal growth factor receptor (EGFR) inhibitors, are being investigated in studies in which they are given with traditional chemotherapeutic agents. APPROACHES TO TREATING HEAD AND NECK CANCER The strategy for treating HNCA depends on the stage of the disease. For example, early-stage disease is treated with surgery alone. However, most patients are diagnosed with locally advanced disease and have historically been treated with curative intent with surgery followed by radiotherapy or radiotherapy alone. Most multi-institutional trials that included patients treated this way have resulted in locoregional recurrence rates 12 Vol. 3, No. 1 April 2006
2 of 30%, rates of distant metastasis formation of 25%, and 5-year survival rates of 40%, in addition to clinically significant sequelae from major surgery. 1 The 5- year mortality rate for HNCA has not changed substantially in the past few decades despite advances in treatment modalities. 2 Thus, the management of late-stage HNCA is relatively unsatisfactory, and optimal therapy remains a matter of debate, especially with regard to treatment intensity and sequencing. To increase cure rates while preserving organ function, chemotherapy is being used in 3 different approaches. One of these is as neoadjuvant chemotherapy, which refers to giving chemotherapy before locoregional therapy consisting of surgery or radiation. This approach attempts to downstage the tumor, which facilitates local therapy, and to eradicate micrometastatic disease. Another approach is concurrent chemoradiation, which is chemotherapy given at the same time as radiation. This approach not only treats local disease but also attempts to eradicate micrometastatic disease. The third approach is adjuvant therapy, which is chemotherapy given after local therapy. Because of the lack of a standard of care, the role of adjuvant therapy in HNCA will not be discussed here. Metastatic disease is treated with palliative chemotherapy. TRADITIONAL CHEMOTHERAPEUTIC AGENTS The primary agents used for treating HNCA are the platinum analogs, 5-fluorouracil (5-FU), and the taxanes, in addition to older agents, such as methotrexate and mitomycin C. Although useful, all of these agents have limited effectiveness and are associated with severe toxicities. PLATINUM ANALOGS The platinum-containing agents cisplatin and carboplatin are DNA cross-linking agents similar to, but not identical to, the alkylating agents. These platinum analogs act by cross-linking DNA in various ways, which prevents rapidly dividing cells from duplicating their DNA for mitosis. The damaged DNA then sets off DNA repair mechanisms, which activate apoptosis when repair proves impossible. Because of the molecular differences between the 2 agents, their dosing also differs. In HNCA, cisplatin is typically given in a single dose of 75 to 100 mg/m2 every 3 to 4 weeks. 3 Prehydration is essential to prevent the renal damage that cisplatin can cause. 4 Prehydration is usually accomplished by intravenously (IV) giving 1 L of normal saline, to which is added 20 meq potassium chloride and 8 meq magnesium sulfate over 1 to 2 hours to obtain a urinary flow rate of at least 100 ml per hour; posthydration consists of giving the same IV fluids. Because renal excretion is the main route of elimination for carboplatin, carboplatin dosing involves using the Calvert method, which is a calibration method based on kidney function. The Calvert method involves calculating the dose in milligrams by multiplying the target area under the concentration time curve (AUC) by the sum of the creatinine clearance (CrCl) plus 25 (ie, dose [mg] = target AUC x [CrCl + 25]). 5 The target AUC can range from 1 to 8 mg/ml per minute, depending on whether radiation is being given concurrently or whether carboplatin treatment is given weekly or every 3 weeks. Whether cisplatin and carboplatin are interchangeable in treating HNCA depends on the role chemotherapy is expected to play. In general, cisplatin appears to be the superior agent, especially if radiotherapy is being used concurrently, because cisplatin is a better radiosensitizer than carboplatin. Two randomized trials have shown that superior disease-free survival and response rates resulted from cisplatin chemotherapy compared to carboplatin chemotherapy. 3,6 No difference between the 2 drugs was observed in overall survival. However, because cisplatin is the better radiosensitizer, it is a better choice than carboplatin, even though its effect on survival has not yet been demonstrated. When palliation is the goal, platinum analogs can be used or therapy can be switched from 1 to the other to enhance tolerability. The use of cisplatin results in more nephrotoxicity, nausea and vomiting, and neurotoxicity than carboplatin. However, unlike cisplatin, carboplatin causes myelosuppression, specifically thrombocytopenia, and, in some cases, carboplatin can cause severe nausea and vomiting. 5-FLUOROURACIL 5-Fluorouracil is a prodrug that is broken down into 2 primary products: 5-fluorouridine-5 -triphosphate (FUTP) and 5-fluorodeoxyuridine-5 -monophosphate (FdUMP). The 5-FU product FUTP is incorporated into RNA, which causes impaired protein synthesis. 7 However, the main mechanism of action occurs through inhibition of DNA; FdUMP forms a tight but reversible covalent bond with thymidylate synthetase, an enzyme needed for the synthesis of thymidine, 1 of the 4 building blocks of DNA. By inhibiting this key enzyme, 5-FU University of Tennessee Advanced Studies in Pharmacy 13
3 reduces the rate of DNA synthesis, replication, and repair. 5-FU is cell-cycle specific for the synthesis phase and tends to produce better response rates when given as an infusion. As in colon cancer, in HNCA infusions of 5-FU appear to result in better response rates for several reasons. For example, compared to bolus delivery, a 24- hour infusion permits delivery of more drug to the site of action and exposes a larger number of tumor cells to 5-FU. In addition, the adverse effect profile of an infusion differs from that of a bolus and is considered more tolerable. The dose-limiting adverse effect of infusional 5-FU tends to be diarrhea, whereas, in bolus administration mucositis is more prevalent. Furthermore, prolonged, continuous IV infusions have yielded higher response rates than IV bolus regimens. In a randomized trial in 44 patients with advanced and recurrent HNCA, cisplatin 100 mg/m2 given on day 1 and a 24-hour infusion of 5-FU 1000 mg/m2 given on days 1 through 4 was compared to cisplatin 100 mg/m2 given on day 1 and bolus 5-FU 600 mg/m2 given on days 1 and 8. 8 The response rate for the infusion arm was 72% (4/18 who had a complete response [CR] + 9/18 who had a partial response [PR]), whereas the response rate for the bolus arm was 20% (2/20 CR + 2/20 PR). The difference in response between treatment arms was statistically significant (P <.01). However, continuous infusion often requires the patient to be admitted to the hospital when the patient does not have access to portable ambulatory care pumps. This requirement entails greater expense and places a larger burden on the healthcare system. 9 In addition, continuous infusion may cause complications arising from the use of indwelling catheters. 10 The major adverse side effects associated with 5-FU are those that are dose limiting and include diarrhea, mucositis, and hand-foot syndrome. Other adverse effects include cardiac toxicity (which may result in angina and myocardial infarction), photosensitivity, skin reactions (eg, hyperpigmentation, nail bed changes, or rashes), gastrointestinal problems (eg, nausea or vomiting), and ocular side effects (eg, burning, tearing, or itching). Another complication involves dihydropyrimidine dehydrogenase (DPD), an enzyme needed in the initial and rate-limiting step in pyrimidine catabolism. The enzyme DPD regulates the amount of 5-FU available for anabolism, which thereby affects its pharmacokinetics, toxicity, and efficacy. Because the catabolic pathway does not function in patients with DPD deficiency, administration of standard doses of 5-FU results in altered 5-FU pharmacokinetics and severe toxicity that may cause mucositis, granulocytopenia, neuropathy, and death. This toxicity appears to result from decreased drug clearance, which markedly prolongs exposure to 5-FU. Recent evidence has shown that African Americans are more prone to DPD deficiency than whites (7.7% vs 2.3%) and therefore, are at greater risk from the toxicities associated with 5-FU administration. 11 TAXANES The taxanes include paclitaxel and docetaxel. These agents work by disrupting the microtubular network in cells that are essential for mitotic and interphase cellular functions, specifically those that occur during the mitosis phase of the cell cycle. The taxanes bind to free tubulin and promote the assembly of tubulin into stable microtubules while inhibiting their disassembly. This effect leads to the production of microtubule bundles without normal function and to the stabilization of microtubules, which results in the inhibition of mitosis in cells. 12,13 Taxanes are specific for the mitosis phase of the cell cycle and also are excellent radiosensitizers. The taxanes mechanism of action through microtubule stabilization is unique among chemotherapeutic agents. Taxanes have shown response rates similar to those of standard, first-line combination regimens. Phase II studies have evaluated the efficacy of docetaxel monotherapy in patients with HNCA. 14,15 Cumulative response rates were approximately 30%, and higher response rates were observed in patients who had not received chemotherapy previously. Docetaxel also has been used with cisplatin and with cisplatin plus 5-FU. 15 Although response rates that resulted from such combination regimens were shown to be superior to those that resulted from the use of docetaxel monotherapy, grade 3 and 4 adverse effects, especially mucositis, nausea, and neutropenia, also were more prevalent. Paclitaxel is administered at a dose of 135 to 175 mg/m2 as an IV infusion every 3 weeks and should be given before a platinum-containing agent when used in combination regimens. 12 Docetaxel is given at a dose of 75 to 100 mg/m2 as an IV infusion over 1 hour every 3 weeks. 13 The main adverse effect associated with paclitaxel and docetaxel is dose-limiting leukopenia. Additional toxicities seen with paclitaxel include hypersensitivity reactions, alopecia, cardiac toxicity, peripheral neuropathies, and mucositis. Additional toxicities seen with docetaxel include peripheral edema and alopecia. 14 Vol. 3, No. 1 April 2006
4 Before receiving docetaxel, all patients should be premedicated with oral corticosteroids, such as dexamethasone 8 mg twice a day for 3 days, starting 1 day before docetaxel is given to reduce the severity of fluid retention. 13 Similarly, all patients receiving paclitaxel should be premedicated with dexamethasone 20 mg taken orally approximately 12 hours and 6 hours before the taxane is given, diphenhydramine 50 mg given IV 30 to 60 minutes before the taxane is given, and cimetidine 300 mg or ranitidine 50 mg given IV 30 to 60 minutes before the taxane is given to reduce hypersensitivity reactions. 14 rate. 17,18 A large meta-analysis, the Meta-analysis of Chemotherapy on Head and Neck Cancer, which looked at the impact on survival of various chemotherapy regimens when added to locoregional treatment, showed an overall 2% survival advantage at 5 years for this approach, which increased to 5% when only cisplatin/5-fu studies were included. 19 Neoadjuvant therapy has been somewhat more successful in preserving organ function in a variety of trials (Table 2) In the Veterans Affairs Laryngeal Cancer Study Group, a land- COMBINATION THERAPY As with most cancers, single-agent chemotherapy is rarely given in HNCA. Combination therapy has been attempted in patients with HNCA with varying degrees of success; the greatest success has been reported for the combination of cisplatin and 5-FU. Response rates for combination therapy are superior to those for monotherapy and are as high as 80%, although a survival benefit for combination therapy has been difficult to prove. Nevertheless, when used as neoadjuvant therapy or for metastatic disease, combination therapy has become the standard of care for most patients with HNCA. Table 1 is a summary of the major neoadjuvant trials that showed some benefit in terms of survival and/or distant failure, which is a marker for lack of eradication of micrometastatic disease Most randomized neoadjuvant trials do not show a survival advantage. For example, The Head and Neck Contracts Program gave 1 cycle of induction cisplatin and bleomycin, then 6 cycles of cisplatin. 16 No survival advantage was evident, but the study did show a reduction in distant metastases as the first site of failure. Two European trials the Groupe d Etude des Tumeurs de la Tete Et du Cou and the Gruppo di Studio sui Tumori della Testa e del Collo (GSTTC) showed a survival benefit with 3 or 4 cycles of induction cisplatin and 5-FU; the GSTTC trial also showed a reduction in the distant failure Table 1. Neoadjuvant Chemotherapy Effects on Survival Distant Future Trial Patients, n Chemotherapy Survival Benefit Benefit HNCP Cisplatin and bleomycin x 1, No Yes Cisplatin x 6 GSTTC Cisplatin and 5-FU x 4 Yes Yes GETTEC Cisplatin and 5-FU x 3 Yes No MACH-NC Various 2% at 5 yr; 5% in Yes cisplatin and 5-FU trials 5-FU = 5-fluorouracil; GETTEC = Groupe d Etude des Tumeurs de la Tete Et du Cou; GSTTC = Gruppo di Studio sui Tumori della Testa e del Collo; HNCP = Head and Neck Contracts Program; MACH-NC = Meta-analysis of Chemotherapy on Head and Neck Cancer. Data from Head and Neck Contracts Program 16 ; Paccagnella et al 17 ; Domenge et al 18 ; and Pignon et al. 19 Table 2. Neoadjuvant Chemotherapy Effects on Organ Preservation Organ Trial Patients, n Chemotherapy Survival Benefit Preservation VA Laryngeal 332 Cisplatin and 5-FU x 3 No Yes Cancer Study RT vs none Group 20 S RT EORTC Cisplatin and 5-FU x 3 No Yes RT vs none S RT Richard et al Cisplatin and 5-FU x 3 In favor of Yes RT vs none surgery arm S RT MACH-NC Various Trend in favor of n/a surgery arm 5-FU = 5-fluorouracil; EORTC = European Organisation for the Research and Treatment of Cancer; MACH-NC = Meta-analysis of Chemotherapy on Head and Neck Cancer; n/a = data not available; RT = radiotherapy; S = surgery; VA = Department of Veterans Affairs. Data from Pignon et al 19 ; Department of Veterans Affairs Laryngeal Cancer Study Group 20 ; Lefebvre et al 21 ; and Richard et al. 22 University of Tennessee Advanced Studies in Pharmacy 15
5 mark study in organ preservation, and the European Organisation for the Research and Treatment of Cancer (EORTC) trial, patients were randomized to receive induction cisplatin/5-fu (at least 2 cycles, and, if a response was seen, a third cycle), then radiation, or to receive surgery, then radiation. 20,21 In these studies, no difference in survival was observed on the basis of treatment strategy, and an improvement in organ preservation was shown by a decrease in need for laryngectomy. 20,21 However, a small trial in 68 patients done by Richard et al found the opposite. 22 In that trial, results of surgery followed by radiation were found to be superior to those of chemotherapy followed by radiation (2-year overall survival: 69% vs 84%; P =.006). 22 Moreover, a large meta-analysis of patients found no difference in survival but a trend toward decreased survival (P =.1) in the nonsurgery arm, which led the investigators to conclude that we cannot exclude the negative impact of this strategy on survival. 19 Neoadjuvant chemotherapy has shown some benefit in treating patients with resectable disease, albeit in terms of organ preservation rather than survival. However, the use of this approach followed by radiotherapy alone or by surgery if the primary tumor becomes resectable has not shown any survival benefit in treating initially unresectable disease; therefore, it is not recommended as a standard approach. 23 Nevertheless, a 2004 randomized EORTC trial in patients with unresectable HNCA showed that the addition of docetaxel to 4 cycles of cisplatin/5-fu significantly improved overall survival (median survival: 14.5 months vs 18.6 months; P =.016), which suggests that neoadjuvant chemotherapy should be reconsidered. 24 However, for the most part, these generally disappointing results have fueled the trend towards replacing neoadjuvant chemotherapy with chemoradiation. In a meta-analysis that examined the various approaches to chemoradiation, the reduction in risk of death was 19% when both therapies were given concomitantly versus 5% for neoadjuvant chemotherapy and 2% for adjuvant chemotherapy. 19 The concomitant approach produced an 8% absolute benefit at 5 years versus a 2% absolute benefit for neoadjuvant chemotherapy and a 1% absolute benefit for adjuvant chemotherapy. In an intergroup, phase III trial, radiation alone was compared to radiation plus cisplatin and radiation plus cisplatin/5-fu given in a split course. 25 Patients received 3 cycles of treatment; radiation was given during the first and third cycles but omitted during the second cycle to decrease toxicity. The results showed that concomitant cisplatin/radiation was the superior regimen; the overall 3-year survival rate that resulted from this regimen was 37% versus 23% for radiation alone (P =.014). TREATMENT OF METASTATIC DISEASE When treating metastatic HNCA, the same drugs are used as when treating the earlier stages of HNCA but are used for palliation rather than survival. The median duration of survival for patients with metastatic disease is a mere 6 months; the 1-year survival rate is 20% and is typically not increased by chemotherapy. Several randomized trials have compared combination chemotherapy with single-agent chemotherapy (Table 3). 3,26,27 These trials consistently have shown Table 3. Combination vs Single-Agent Chemotherapy for Metastatic Disease Response Mean Study Patients, n Agents Rate, % Survival, mo CHEMORADIATION Unlike neoadjuvant chemotherapy, chemoradiation takes advantage of the radiosensitizing effects of chemotherapy. However, the radiosensitizing effects of chemotherapy are not tumor selective, and high rates of toxicity have been seen, especially with combination regimens. Because of its superior radiosensitizing ability, cisplatin is generally the drug of choice for the chemoradiation of HNCA. Jacobs et al Cisplatin and 5-FU 32* 5.5 Cisplatin FU Forastiere et al Cisplatin and 5-FU Carboplatin and 5-FU 21 5 Methotrexate Clavel et al Cisplatin, methotrexate, 34 7 bleomycin, and vincristine Cisplatin and 5-FU 31 7 Cisplatin 15 7 *P =.035; P <.001; P <.001; P = FU = 5-fluorouracil. Data from Forastiere et al 3 ; Jacobs et al 26 ; and Clavel et al Vol. 3, No. 1 April 2006
6 increased response rates for combination regimens but have not shown a survival benefit. 3,26,27 However, on the basis of the increase in response rates and manageable toxicity, combination therapy with a platinum analog plus another drug, such as bleomycin, 5-FU, methotrexate, and/or vincristine in various combinations, has become the standard of care for metastatic disease. In the study by Forastiere et al, carboplatin was found to be comparable to cisplatin in terms of overall survival but resulted in a lower response rate than cisplatin. 3 The trial by Clavel et al showed that giving more than 2 traditional chemotherapeutic agents produced no better results than giving 2 traditional chemotherapeutic agents in terms of overall survival and response rates. 27 EPIDERMAL GROWTH FACTOR RECEPTOR BLOCKADE A newer approach to treating cancer is to block EGFRs. Peptide growth factors activate signaling pathways, which control cell proliferation and death in normal and malignant cells. 28 The epidermal growth factor was one of the first growth factors to be identified and has a pivotal role in the regulation of normal cell growth and differentiation. The EGFR autocrine pathway contributes to several processes that are important in cancer development and progression, including cell proliferation, apoptosis, angiogenesis, and metastatic spread. The key role the EGFR plays in cancer has led to an extensive search for selective inhibitors of the EGFR signaling pathway. A variety of approaches are currently being used to target the EGFR. surgery. Cetuximab also was approved for use in patients with metastatic HNCA that have already failed traditional chemotherapy. 29 In a phase III study of patients with locoregionally advanced squamous cell carcinoma of the head and neck, high-dose radiotherapy was compared to highdose radiotherapy plus cetuximab. 30 After a median follow-up of 45 months, the median durations of locoregional control (LRC) were 24.4 months for radiotherapy plus cetuximab and 14.9 months for radiotherapy only (log-rank P =.005). Adding cetuximab to radiotherapy reduced the risk of locoregional failure by 32% (hazard ratio = 0.68). At 2 years, 50% of the patients in the radiotherapy plus cetuximab arm and 41% of those in the radiotherapy only arm had LRC. The median duration of survival was 49 months for combination therapy and 29 months for radiotherapy only (median follow-up, 45 months). A 26% reduction in the risk of mortality also was noted for combination therapy compared to radiotherapy only (hazard ratio = 0.74, log-rank P =.03). The 3-year survival rates were 56% for combination therapy and 45% for radiotherapy only. Except for acne-like rashes and infusion reactions, the incidence of grade 3 or 4 adverse effects did not differ between the treatment arms. Reports of several phase II trials of cetuximab alone or with chemotherapy in patients with refractory or recurrent HNCA have been published (Table 4) CETUXIMAB The most promising strategies in clinical development include producing monoclonal antibodies to prevent ligand binding and creating small-molecule inhibitors of tyrosine kinase enzymatic activity to inhibit autophosphorylation and downstream intracellular signaling. Cetuximab is a chimeric human-murine monoclonal IgG 1 antibody that has been the first anti- EGFR targeted therapy to receive clinical evaluation in patients with cancer in phase II and III studies when given alone or with conventional therapies, such as radiotherapy and chemotherapy. In March 2006, cetuximab was approved by the US Food and Drug Administration for use in combination with radiation therapy to treat patients with squamous cell HNCA that cannot be removed by Table 4. Cetuximab in Patients with Refractory/Recurrent Head and Neck Cancer Regimens Patients, n Response Rate, % Median Survival, mo Historical controls 30 * Platinum-based chemotherapy + cetuximab Cisplatin + cetuximab SD, 18 SD, 11.7 PD/1, 20 PD/1, 6.1 PD/2, 6 PD/2, 4.3 Cetuximab monotherapy *Historical controls had disease that was refractory to platinum-analog chemotherapy. PD/1 = patients with progressive disease who received cetuximab and cisplatin; PD/2 = patients in whom progressive disease developed within 90 days after platinum-analog therapy and who were then given cetuximab; SD = stable disease. Data from Leon et al 31 ; Baselga et al 32 ; Herbst et al 33 ; and Trigo et al. 34 University of Tennessee Advanced Studies in Pharmacy 17
7 Results of these trials have been compared to those obtained in patients who have not responded to platinum-analog therapy and who therefore serve as historical controls to underscore their dismal prognosis and the need for novel therapies. 31 Baselga et al treated 96 patients with cetuximab followed by platinum-analog chemotherapy at the same dose and schedule, after which progressive disease (PD) was documented before entry into the study. 32 The response rate in the intent-to-treat population was 10%, and the disease control rate, which included CR, PR, and stable disease (SD), was 53%. The median time to progression was 85 days, and the median duration of survival was 183 days. Treatment was well tolerated. The most common cetuximab-related adverse events were skin reactions, particularly an acne-like rash. In a study by Herbst et al, 132 patients with HNCA received 2 3-week cycles of treatment with cisplatin/paclitaxel or cisplatin/5-fu. 33 Patients with a CR or PR continued to receive standard therapy. Seventy-six patients with SD (n = 51) or those with PD in arm 1 (PD/1; n = 25) received combination therapy with cetuximab and cisplatin. The protocol was subsequently amended to enroll patients who had developed PD within 90 days after platinum-analog therapy (PD arm 2 [PD/2]; n = 54). The results showed that 5 patients (20%) in PD/1, 3 patients (6%) in PD/2, and 9 patients (18%) with SD achieved an objective response. Median duration of response was 4.2 months in the PD/1 group, 4.1 months in the PD/2 group, and 7.4 months in the SD group; median duration of overall survival was 6.1 months in the PD/1 group, 4.3 months in the PD/2 group, and 11.7 months in the SD group. The most common adverse effects were anemia, acne-like skin rash, leukopenia, fatigue/malaise, nausea, and vomiting. Cetuximab monotherapy in 103 patients with recurrent/metastatic HNCA whose disease was refractory to platinum-analog therapy resulted in an overall response rate of 16.5% and a median duration of survival of 5.8 months. 34 The median duration of survival of approximately 6 months achieved with cetuximab in platinum-analog refractory HNCA is comparable to the result observed with first-line therapy and represents an increase in survival of 2.5 months compared to that for historical controls with platinum-analog refractory disease. On the basis of these results, cetuximab monotherapy seems to be a useful option in patients with recurrent/metastatic HNCA whose disease has progressed during platinum-analog chemotherapy. In HNCA, cetuximab is given IV at an initial loading dose of 400 mg/m2 over 2 hours, then at weekly maintenance doses of 250 mg/m2 over 60 minutes; both loading and maintenance doses should be infused no faster than 5 ml per minute. Toxicities include an infusion reaction, in addition to an acne-like skin rash, asthenia, nausea, and vomiting. SMALL-MOLECULE EGFR INHIBITORS Several oral small-molecule inhibitors of EGFR tyrosine kinase enzymatic activity also are being assessed for their value in cancer therapy. Erlotinib has been approved for use in non-small cell lung cancer (NSCLC) and pancreatic cancer; gefitinib has been approved for NSCLC. In a study of erlotinib in 115 patients with metastatic HNCA, 5 patients had a PR, which resulted in an overall objective response rate of 4.3%. 35 Disease was stabilized in 44 patients (38.3%) for a median duration of 16.1 weeks. The median duration of progression-free survival was 9.6 weeks, and the median duration of overall survival was 6 months. Rash (in 79%) and diarrhea (in 37%) were the most common drug-related adverse effects, although their severity was mild to moderate in most cases. In a phase II study of 47 patients with advanced HNCA, patients were given gefitinib 500 mg daily in combination with 1 other therapy or as monotherapy. 36 The observed response rate was 10.6%, and the disease control rate was 53%. Median time to progression was 3.4 months, and median duration of survival was 8.1 months. The only grade 3 adverse effect was diarrhea, which occurred in 3 patients. More studies are needed to assess the results of using these agents with traditional therapies in patients with HNCA. CONCLUSIONS Progress has been and continues to be made in the treatment of HNCA. However, current outcomes are unacceptable, particularly in advanced disease, and therefore, a need exists for novel approaches to disease management that combine traditional agents with the newer agents currently being developed. Despite promising results of randomized studies and metaanalyses, optimism must be balanced with realism because survival rates remain low. In early-stage disease, progress in surgical techniques and imaging has enabled more accurate resection. The objective now is to maintain a favorable efficacy-toxicity ratio for treat- 18 Vol. 3, No. 1 April 2006
8 ment and to reduce the incidence of second primary tumors, which are often the major cause of relapse. In patients with advanced HNCA, survival improves when chemotherapy is combined with radiotherapy compared to when radiotherapy is given alone. As in this instance, we continue to hone our therapeutic skills, albeit painstakingly slowly. The immediate aim of treatment for advanced HNCA should be to increase survival, LRC, and organ preservation and to reduce the formation of distant metastases and the incidence of severe, acute, treatment-related adverse side effects, particularly mucositis. In addition, the use of neoadjuvant chemotherapy, which has so far failed to meet expectations, merits further investigation in well-defined, controlled trials. The outlook for patients with recurrent/metastatic disease remains poor, particularly for those patients whose disease progresses when treated with platinumbased therapies. For these patients, the goal is to improve response rates to chemotherapy and, whenever possible, to prolong survival without compromising quality of life. In the search for treatments that improve outcomes in various cancers, targeted molecular therapies, such as cetuximab, erlotinib, and gefitinib, are in the investigational stages. Clinical experience with cetuximab plus radiotherapy for locally advanced disease and cetuximab plus chemotherapy for recurrent/metastatic disease indicates that these combination therapies show promise. Studies in which cisplatin-refractory disease was treated with cetuximab alone or with cisplatin plus cetuximab have produced encouraging results. The ability of targeted therapies to increase the therapeutic index of current conventional therapies without increasing their toxicities indicates that these agents have a key role to play in future practice and merit further investigation when used with other, more established therapies. REFERENCES 1. Laramore GE, Scott CB, al-sarraf M, et al. Adjuvant chemotherapy for resectable squamous cell carcinomas of the head and neck: report on Intergroup Study Int J Radiat Oncol Biol Phys. 1992;23: Kurtulmaz SY, Erkal HS, Serin M, et al. Squamous cell carcinoma of the head and neck: descriptive analysis of 1293 cases. J Laryngol Otol. 1997;111: Forastiere AA, Metch B, Schuller DE, et al. Randomized comparison of cisplatin plus fluorouracil and carboplatin plus fluorouracil versus methotrexate in advanced squamous-cell carcinoma of the head and neck: a Southwest Oncology Group study. J Clin Oncol. 1992;10: Platinol [prescribing information]. Princeton, NJ: Bristol- Myers Squibb; Paraplatin [prescribing information]. Princeton, NJ: Bristol- Myers Squibb; De Andres L, Brunet J, Lopez-Pousa A, et al. Randomized trial of neoadjuvant cisplatin and fluorouracil versus carboplatin and fluorouracil in patients with stage IV-M0 head and neck cancer. J Clin Oncol. 1995;13: Pinedo HM, Peters GF. Fluorouracil: biochemistry and pharmacology. J Clin Oncol. 1988;6: Kish JA, Ensley JF, Jacobs J, et al. A randomized trial of cisplatin (CACP) + 5-fluorouracil (5-FU) infusion and CACP + 5-FU bolus for recurrent and advanced squamous cell carcinoma of the head and neck. Cancer. 1985;56: Van Cutsem E, Cunningham D, Hoff PM, Maroun J. Thymidine phosphorylase (TP) activation: convenience through innovation. Oncologist. 2001;6: Partridge S, Leslie M, Irvine A. Infusional 5-fluorouracil can be a pain in the neck: a case for repositioning displaced Hickman lines. Clin Oncol (R Coll Radiol). 1999;11: Mattison L, Fourie J, Carpenter M, et al. Evidence for increased incidence of dihydropyrimidine dehydrogenase (DPD) deficiency in African Americans compared to Caucasians [abstract 2004]. Presented at: 41st Annual Meeting of the American Society of Clinical Oncology; May 13-17, 2005; Orlando, Fla. 12. Taxol [prescribing information]. Princeton, NJ: Bristol-Myers Squibb; Taxotere [prescribing information]. Bridgewater, NJ: Aventis Pharmaceuticals, Inc.; Schrijvers DL, Vroman P, Dyck J, et al. Weekly docetaxel in patients with recurrent and/ or metastatic head and neck cancer [abstract 2544]. Presented at: 37th Annual Meeting of the American Society of Clinical Oncology; May 12-15, 2001; San Francisco, Calif. 15. Colevas AD, Norris CM, Tishler RB, et al. Phase II trial of Taxotere, Platinol, 5-FU, and leucovorin as induction for squamous cell carcinoma of the head and neck. J Clin Oncol. 1999;17: Head and Neck Contracts Program. Adjuvant chemotherapy for advanced head and neck squamous carcinoma. Final report of the Head and Neck Contracts Program. Cancer. 1987;60: Paccagnella A, Orlando A, Marchiori C, et al. Phase III trial of initial chemotherapy in stage III or IV head and neck cancers: a study by the Gruppo di Studio sui Tumori della Testa e del Collo. J Natl Cancer Inst. 1994;86: Domenge C, Hill C, Lefebvre JL, et al. Randomized trial of neoadjuvant chemotherapy in oropharyngeal carcinoma. Br J Cancer. 2000;83: Pignon JP, Bourhis J, Domenge C, Designe L. Chemotherapy added to locoregional treatment for head and neck squamous-cell carcinoma: three meta-analyses of updated individual data. Lancet. 2000;355: Department of Veterans Affairs Laryngeal Cancer Study Group. Induction chemotherapy plus radiation compared with surgery plus radiation in patients with advanced laryngeal cancer. N Engl J Med. 1991;324: Lefebvre JL, Chevalier D, Luboinski B, et al. Larynx preservation in pyriform sinus cancer: preliminary results of a European Organization for Research and Treatment of Cancer phase III trial. J Natl Cancer Inst. 1996;88: University of Tennessee Advanced Studies in Pharmacy 19
9 22. Richard JM, Sancho-Garnier H, Pessey JJ, et al. Randomized trial of induction chemotherapy in larynx carcinoma. Oral Oncol. 1998;34: Pivot X. ESMO minimum clinical recommendations for diagnosis, treatment and follow-up of squamous cell carcinoma of the head and neck. Ann Oncol. 2003;14: Vermorken JB, Remenar E, Van Herpen C, et al. Standard cisplatin/infusional 5-fluorouracil (PF) vs docetaxel (T) plus PF (TPF) as neoadjuvant chemotherapy for nonresectable locally advanced squamous cell carcinoma of the head and neck (LA-SCCHN): a phase III trial of the EORTC Head and Neck Cancer Group (EORTC #24971) [abstract 5508]. Presented at: 40th Annual Meeting of the American Society of Clinical Oncology; June 5-8, 2004; New Orleans, La. 25. Adelstein DJ, Li Y, Adams GL, et al. An intergroup phase III comparison of standard radiation therapy and two schedules of concurrent chemoradiotherapy in patients with unresectable squamous cell head and neck cancer. J Clin Oncol. 2003;21: Jacobs C, Lyman G, Velez-Garcia E, et al. A phase III randomized study comparing cisplatin and fluorouracil as single agents and in combination for advanced squamous cell carcinoma of the head and neck. J Clin Oncol. 1992;10: Clavel M, Vermorken JB, Cognetti F, et al. Randomized comparison of cisplatin, methotrexate, bleomycin, and vincristine (CABO) versus cisplatin and 5-fluorouracil (CF) versus cisplatin (C) in recurrent or metastatic squamous cell carcinoma of the head and neck. Ann Oncol. 1994;5: Ciardiello F, Tortora G. A novel approach in the treatment of cancer: targeting the epidermal growth factor. Clin Cancer Res. 2001;7: US Food and Drug Administration. FDA approves first head and neck cancer treatment in 45 years, data shows treatment with Erbitux extends survival. Available at: NEW01329.html. Accessed March 26, Bonner JA, Giralt J, Harari PM, et al. Cetuximab prolongs survival in patients with locoregionally advanced squamous cell carcinoma of head and neck: a phase III study of high dose radiation therapy with or without cetuximab [abstract 5507]. Presented at: 40th Annual Meeting of the American Society of Clinical Oncology; June 5-8, 2004; New Orleans, La. 31. Leon X, Hitt R, Constenla M, et al. A retrospective analysis of the outcome of patients (pts) with recurrent or metastatic squamous cell carcinoma of the head and neck (R&M SCCHN) who are progressing while on a platinum-based palliative chemotherapy. Proc Am Soc Clin Oncol. 2003;22:A Baselga J, Trigo JM, Bourhis J, et al. Phase II multicenter study of the antiepidermal growth factor receptor monoclonal antibody cetuximab in combination with platinum-based chemotherapy in patients with platinum-refractory metastatic and/or recurrent squamous cell carcinoma of the head and neck. J Clin Oncol. 2005;23: Herbst RS, Arquette M, Shin DM, et al. Phase II multicenter study of the epidermal growth factor receptor antibody cetuximab and cisplatin for recurrent and refractory squamous cell carcinoma of the head and neck. J Clin Oncol. 2005;23: Trigo J, Hitt R, Koralewski P, et al. Cetuximab monotherapy is active in patients (pts) with platinum-refractory recurrent/metastatic squamous cell carcinoma of the head and neck (SCCHN): results of a phase II study [abstract 5502]. Presented at: 40th Annual Meeting of the American Society of Clinical Oncology; June 5-8, 2004; New Orleans, La. 35. Soulieres D, Senzer NN, Vokes EE, et al. Multicenter phase II study of erlotinib, an oral epidermal growth factor receptor tyrosine kinase inhibitor, in patients with recurrent or metastatic squamous cell cancer of the head and neck. J Clin Oncol. 2004;22: Cohen EE, Rosen F, Stadler WM, et al. Phase II trial of ZD1839 in recurrent or metastatic squamous cell carcinoma of the head and neck. J Clin Oncol. 2003;21: Vol. 3, No. 1 April 2006
Paradigm Shift in the Treatment of Head and Neck Cancer: The Role of Neoadjuvant Chemotherapy
 This material is protected by U.S. Copyright law. Unauthorized reproduction is prohibited. For reprints contact: Reprints@AlphaMedPress.com Paradigm Shift in the Treatment of Head and Neck Cancer: The
This material is protected by U.S. Copyright law. Unauthorized reproduction is prohibited. For reprints contact: Reprints@AlphaMedPress.com Paradigm Shift in the Treatment of Head and Neck Cancer: The
Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice?
 Cent. Eur. J. Med. 9(2) 2014 279-284 DOI: 10.2478/s11536-013-0154-9 Central European Journal of Medicine Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice? Jacopo Giuliani* 1, Marina
Cent. Eur. J. Med. 9(2) 2014 279-284 DOI: 10.2478/s11536-013-0154-9 Central European Journal of Medicine Cetuximab/cisplatin and radiotherapy in HNSCC: is there a favorite choice? Jacopo Giuliani* 1, Marina
Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck. Mei Tang, MD
 Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck Mei Tang, MD Head and Neck Cancer Worldwide New cases : 644,000 Cancer deaths: 350,000 About 5% of all cancers Local Recurrence:
Neoadjuvant Chemotherapy in Locally Advanced Squamous Cell Cancer of Head and Neck Mei Tang, MD Head and Neck Cancer Worldwide New cases : 644,000 Cancer deaths: 350,000 About 5% of all cancers Local Recurrence:
Emerging Role of Immunotherapy in Head and Neck Cancer
 Emerging Role of Immunotherapy in Head and Neck Cancer Jared Weiss, MD Associate Professor of Medicine and Section Chief of Thoracic and Head/Neck Oncology UNC Lineberger Comprehensive Cancer Center Copyright
Emerging Role of Immunotherapy in Head and Neck Cancer Jared Weiss, MD Associate Professor of Medicine and Section Chief of Thoracic and Head/Neck Oncology UNC Lineberger Comprehensive Cancer Center Copyright
Accepted 20 April 2009 Published online 25 June 2009 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.21179
 ORIGINAL ARTICLE DOCETAXEL, CISPLATIN, AND FLUOROURACIL INDUCTION CHEMOTHERAPY FOLLOWED BY ACCELERATED FRACTIONATION/CONCOMITANT BOOST RADIATION AND CONCURRENT CISPLATIN IN PATIENTS WITH ADVANCED SQUAMOUS
ORIGINAL ARTICLE DOCETAXEL, CISPLATIN, AND FLUOROURACIL INDUCTION CHEMOTHERAPY FOLLOWED BY ACCELERATED FRACTIONATION/CONCOMITANT BOOST RADIATION AND CONCURRENT CISPLATIN IN PATIENTS WITH ADVANCED SQUAMOUS
Scottish Medicines Consortium
 Scottish Medicines Consortium cetuximab 2mg/ml intravenous infusion (Erbitux ) (279/06) MerckKGaA No 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
Scottish Medicines Consortium cetuximab 2mg/ml intravenous infusion (Erbitux ) (279/06) MerckKGaA No 9 June 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product
The effect of induction chemotherapy followed by chemoradiotherapy in advanced head and neck cancer: a prospective study
 International Journal of Research in Medical Sciences Nikam BM et al. Int J Res Med Sci. 2014 May;2(2):476-480 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20140519
International Journal of Research in Medical Sciences Nikam BM et al. Int J Res Med Sci. 2014 May;2(2):476-480 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: 10.5455/2320-6012.ijrms20140519
Accepted 12 April 2006 Published online 13 November 2006 in Wiley InterScience ( DOI: /hed.
 ORIGINAL ARTICLE PHASE II ANALYSIS OF PACLITAXEL AND CAPECITABINE IN THE TREATMENT OF RECURRENT OR DISSEMINATED SQUAMOUS CELL CARCINOMA OF THE HEAD AND NECK REGION Jens D Bentzen, MD, 1 Hanne Sand Hansen,
ORIGINAL ARTICLE PHASE II ANALYSIS OF PACLITAXEL AND CAPECITABINE IN THE TREATMENT OF RECURRENT OR DISSEMINATED SQUAMOUS CELL CARCINOMA OF THE HEAD AND NECK REGION Jens D Bentzen, MD, 1 Hanne Sand Hansen,
Erbitux. Erbitux (cetuximab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.84 Subject: Erbitux Page: 1 of 6 Last Review Date: December 2, 2016 Erbitux Description Erbitux (cetuximab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.21.84 Subject: Erbitux Page: 1 of 6 Last Review Date: December 2, 2016 Erbitux Description Erbitux (cetuximab)
HEAD AND NECK CANCER TREATMENT REGIMENS (Part 1 of 5)
 HEAD AND NECK CANCER TREATMENT S (Part 1 of 5) Clinical Trials: The National Comprehensive Cancer Network (NCCN) recommends cancer patient participation in clinical trials as the gold standard for treatment.
HEAD AND NECK CANCER TREATMENT S (Part 1 of 5) Clinical Trials: The National Comprehensive Cancer Network (NCCN) recommends cancer patient participation in clinical trials as the gold standard for treatment.
Laryngeal and hypopharyngeal cancers
 Laryngeal and hypopharyngeal cancers Induction Chemotherapy in combined modality approaches Atenas 16.09.2017 Ana Ferreira Castro, MD Medical Oncology Centro Hospitalar do Porto Instituto de Ciências Biomédicas
Laryngeal and hypopharyngeal cancers Induction Chemotherapy in combined modality approaches Atenas 16.09.2017 Ana Ferreira Castro, MD Medical Oncology Centro Hospitalar do Porto Instituto de Ciências Biomédicas
Practice teaching course on head and neck cancer management
 28-29 October 2016 - Saint-Priest en Jarez, France Practice teaching course on head and neck cancer management IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Nicolas Magné France
28-29 October 2016 - Saint-Priest en Jarez, France Practice teaching course on head and neck cancer management IMPROVING THE PATIENT S LIFE THROUGH MEDICAL EDUCATION www.excemed.org Nicolas Magné France
[ ] (2010) Clinical Guideline
![[ ] (2010) Clinical Guideline [ ] (2010) Clinical Guideline](/thumbs/93/114472514.jpg) 98 2010 3 8 2 China Journal of Oral and Maxillofacial Surgery Vol.8 No.2 March2010 [ ]1672-3244(2010)02-0098-09 Clinical Guideline [ ] 3%~5% 90% 3 5 65% 5 30% 2009 NCCN [ ] ; ; [ ] R739.8 [ ] A The protocol
98 2010 3 8 2 China Journal of Oral and Maxillofacial Surgery Vol.8 No.2 March2010 [ ]1672-3244(2010)02-0098-09 Clinical Guideline [ ] 3%~5% 90% 3 5 65% 5 30% 2009 NCCN [ ] ; ; [ ] R739.8 [ ] A The protocol
Neoplasie del laringe Diagnosi e trattamento
 Neoplasie del laringe Diagnosi e trattamento Venerdì 22 maggio 2015 Alessandria Trattamenti non chirurgici: Preservazione d organo, malattia localmente avanzata Marco C Merlano A.O. S.Croce e Carle, Ospedale
Neoplasie del laringe Diagnosi e trattamento Venerdì 22 maggio 2015 Alessandria Trattamenti non chirurgici: Preservazione d organo, malattia localmente avanzata Marco C Merlano A.O. S.Croce e Carle, Ospedale
Guillaume Janoray, Yoann Pointreau, Pascal Garaud, Sophie Chapet, Marc Alfonsi, Christian Sire, Eric Jadaud, Gilles Calais
 JNCI J Natl Cancer Inst (016) 108(4): djv368 doi:10.1093/jnci/djv368 First published online December 16, 015 Article Long-Term Results of a Multicenter Randomized Phase III Trial of Induction Chemotherapy
JNCI J Natl Cancer Inst (016) 108(4): djv368 doi:10.1093/jnci/djv368 First published online December 16, 015 Article Long-Term Results of a Multicenter Randomized Phase III Trial of Induction Chemotherapy
The Role of Docetaxel in the Treatment of Head and Neck Cancer
 GBMC Head and Neck Conference The Role of Docetaxel in the Treatment of Head and Neck Cancer Simon Best December 7, 2007 Needs assessment: Providers who participate in the care of head and neck cancer
GBMC Head and Neck Conference The Role of Docetaxel in the Treatment of Head and Neck Cancer Simon Best December 7, 2007 Needs assessment: Providers who participate in the care of head and neck cancer
HEAD AND NECK CANCER TREATMENT REGIMENS (Part 1 of 5)
 HEAD AND NECK CANCER TREATMENT S (Part 1 of 5) Clinical Trials: The National Comprehensive Cancer Network (NCCN) recommends cancer patient participation in clinical trials as the gold standard for treatment.
HEAD AND NECK CANCER TREATMENT S (Part 1 of 5) Clinical Trials: The National Comprehensive Cancer Network (NCCN) recommends cancer patient participation in clinical trials as the gold standard for treatment.
Docetaxel. Class: Antineoplastic agent, Antimicrotubular, Taxane derivative.
 Docetaxel Class: Antineoplastic agent, Antimicrotubular, Taxane derivative. Indications: -Breast cancer: -Non small cell lung cancer -Prostate cancer -Gastric adenocarcinoma _Head and neck cancer Unlabeled
Docetaxel Class: Antineoplastic agent, Antimicrotubular, Taxane derivative. Indications: -Breast cancer: -Non small cell lung cancer -Prostate cancer -Gastric adenocarcinoma _Head and neck cancer Unlabeled
Medicinae Doctoris. One university. Many futures.
 Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
Medicinae Doctoris The Before and The After: Can chemotherapy revise the trajectory of gastric and esophageal cancers? Dr. David Dawe MD, FRCPC Medical Oncologist Assistant Professor Disclosures None All
NEWER DRUGS IN HEAD AND NECK CANCER. Prof. Anup Majumdar. HOD, Radiotherapy, IPGMER Kolkata
 NEWER DRUGS IN HEAD AND NECK CANCER Prof. Anup Majumdar HOD, Radiotherapy, IPGMER Kolkata 1 Included Oral cavity Nasal cavity Pharynx Larynx Lymph node in upper part of neck Excluded Brain Eye Cancer arising
NEWER DRUGS IN HEAD AND NECK CANCER Prof. Anup Majumdar HOD, Radiotherapy, IPGMER Kolkata 1 Included Oral cavity Nasal cavity Pharynx Larynx Lymph node in upper part of neck Excluded Brain Eye Cancer arising
Laryngeal Preservation Using Radiation Therapy. Chemotherapy and Organ Preservation
 1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
1 Laryngeal Preservation Using Radiation Therapy 1903: Schepegrell was the first to perform radiation therapy for the treatment of laryngeal cancer Conventional external beam radiation produced disappointing
Adjuvant Therapy in Locally Advanced Head and Neck Cancer. Ezra EW Cohen University of Chicago. Financial Support
 Adjuvant Therapy in Locally Advanced Head and Neck Cancer Ezra EW Cohen University of Chicago Financial Support This program is made possible by an educational grant from Eli Lilly Oncology, who had no
Adjuvant Therapy in Locally Advanced Head and Neck Cancer Ezra EW Cohen University of Chicago Financial Support This program is made possible by an educational grant from Eli Lilly Oncology, who had no
Moving EGFR Targeted Therapy into the Induction Phase of the Management of Squamous Cell Carcinoma of the Head and Neck
 14 Journal of Cancer Research Updates, 2012, 1, 14-21 Moving EGFR Targeted Therapy into the Induction Phase of the Management of Squamous Cell Carcinoma of the Head and Neck Belisario A. Arango 1, Bertha
14 Journal of Cancer Research Updates, 2012, 1, 14-21 Moving EGFR Targeted Therapy into the Induction Phase of the Management of Squamous Cell Carcinoma of the Head and Neck Belisario A. Arango 1, Bertha
Self-Assessment Module 2016 Annual Refresher Course
 LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
LS16031305 The Management of s With r. Lin Learning Objectives: 1. To understand the changing demographics of oropharynx cancer, and the impact of human papillomavirus on overall survival and the patterns
Organ-Preservation Strategies in head and neck cancer. Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari
 Organ-Preservation Strategies in head and neck cancer Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari Larynx Hypopharynx The goal of treatment is to achieve larynx preservation
Organ-Preservation Strategies in head and neck cancer Teresa Bonfill Abella Oncologia Mèdica Parc Taulí Sabadell. Hospital Universitari Larynx Hypopharynx The goal of treatment is to achieve larynx preservation
Nasopharyngeal Cancer:Role of Chemotherapy
 Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer:Role of Chemotherapy PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 16/9/2017 2 nd Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Chemotherapy of colon cancers
 Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
Chemotherapy of colon cancers Stage distribution Stage I : 15% T 1,2 NO Stage IV: 20 25% M+ Stage II : 20 30% T3,4 NO Stage III N+: 30 40% clinical stages I, II, or III colon cancer are at risk for having
STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER
 Contact: Anne Bancillon + 33 (0)6 70 93 75 28 STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER Key results of 42 nd annual meeting of the American Society of Clinical
Contact: Anne Bancillon + 33 (0)6 70 93 75 28 STUDY FINDINGS PRESENTED ON TAXOTERE REGIMENS IN HEAD AND NECK, LUNG AND BREAST CANCER Key results of 42 nd annual meeting of the American Society of Clinical
Treatment of Locally Recurrent and Metastatic Squamous Cell Carcinoma of Head and Neck
 Review Article imedpub Journals http://www.imedpub.com/ Head and Neck Cancer Research ISSN 2572-2107 Treatment of Locally Recurrent and Metastatic Squamous Cell Carcinoma of Head and Neck Chukwuemeka V
Review Article imedpub Journals http://www.imedpub.com/ Head and Neck Cancer Research ISSN 2572-2107 Treatment of Locally Recurrent and Metastatic Squamous Cell Carcinoma of Head and Neck Chukwuemeka V
Predictors of Outcome With Cetuximab and Paclitaxel for Head and Neck Squamous Cell Carcinoma
 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Predictors of Outcome With Cetuximab and Paclitaxel for Head and Neck Squamous Cell Carcinoma Bruna Pellini
The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Predictors of Outcome With Cetuximab and Paclitaxel for Head and Neck Squamous Cell Carcinoma Bruna Pellini
Pharmacy Management Drug Policy
 11/13, 10/12, 11/11, 1, 6/10, Page 1 of 5 DESCRIPTION: Cetuximab is a recombinant humanized monoclonal antibody that binds specifically to the extracellular domain of the human epidermal growth factor
11/13, 10/12, 11/11, 1, 6/10, Page 1 of 5 DESCRIPTION: Cetuximab is a recombinant humanized monoclonal antibody that binds specifically to the extracellular domain of the human epidermal growth factor
Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer. Dr P Vijay Anand Reddy Director Apollo Cancer Hospital
 Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer Dr P Vijay Anand Reddy Director Apollo Cancer Hospital H&N Ca - Disease Burden 15-20% of all cancers in India, 8% worldwide
Sequencing Chemo with Radiation therapy Locally Advanced Head and Neck Cancer Dr P Vijay Anand Reddy Director Apollo Cancer Hospital H&N Ca - Disease Burden 15-20% of all cancers in India, 8% worldwide
Targeted Therapies in Metastatic Colorectal Cancer: An Update
 Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
Targeted Therapies in Metastatic Colorectal Cancer: An Update ASCO 2007: Targeted Therapies in Metastatic Colorectal Cancer: An Update Bevacizumab is effective in combination with XELOX or FOLFOX-4 Bevacizumab
ORIGINAL ARTICLE. Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation
 ORIGINAL ARTICLE Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation Michael E. Poole, PA-C, MPH; Scott L. Sailer, MD; Julian G. Rosenman,
ORIGINAL ARTICLE Chemoradiation for Locally Advanced Squamous Cell Carcinoma of the Head and Neck for Organ Preservation and Palliation Michael E. Poole, PA-C, MPH; Scott L. Sailer, MD; Julian G. Rosenman,
Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer
 Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer Faye Johnson MD, PhD Associate Professor Thoracic/Head and Neck Medical Oncology August 2017 Objectives Review data that support concurrent chemo-
Concurrent Chemo- and Radiotherapy for Ororpharynx Cancer Faye Johnson MD, PhD Associate Professor Thoracic/Head and Neck Medical Oncology August 2017 Objectives Review data that support concurrent chemo-
De-Escalate Trial for the Head and neck NSSG. Dr Eleanor Aynsley Consultant Clinical Oncologist
 De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
De-Escalate Trial for the Head and neck NSSG Dr Eleanor Aynsley Consultant Clinical Oncologist 3 HPV+ H&N A distinct disease entity Leemans et al., Nature Reviews, 2011 4 Good news Improved response to
5/20/ ) Haffty GB: Concurrent chemoradiation in the treatment of head and neck cancer. Hematol. Oncol. Clin: North Am.
 Prague, 24-25 25 April 29 ALTERNATING CHEMORADIATION: FOR WHOM? M. Merlano MD Holy Cross Gen. Hospital Cuneo - Italy ALTERNATING CHEMORADIATION: FOR WHOM? Definition of alternating chemoradiation Targets
Prague, 24-25 25 April 29 ALTERNATING CHEMORADIATION: FOR WHOM? M. Merlano MD Holy Cross Gen. Hospital Cuneo - Italy ALTERNATING CHEMORADIATION: FOR WHOM? Definition of alternating chemoradiation Targets
Nasopharyngeal Cancer/Multimodality Treatment
 Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Nasopharyngeal Cancer/Multimodality Treatment PANAGIOTIS KATSAOUNIS Medical Oncologist IASO GENERAL HOSPITAL Athens, 22/10/2016 1 st Hellenic Multidisciplinary Conference on Head and Neck Cancer INTRODUCTION
Immunotherapy in head and neck cancer and MSI in solid tumors
 Immunotherapy in head and neck cancer and MSI in solid tumors Brian Hunis, MD, MBA Associate Medical Director, Memorial Cancer Institute. Hollywood, FL »No disclosures Objectives»Discuss the role of immunology
Immunotherapy in head and neck cancer and MSI in solid tumors Brian Hunis, MD, MBA Associate Medical Director, Memorial Cancer Institute. Hollywood, FL »No disclosures Objectives»Discuss the role of immunology
GASTRIC & PANCREATIC CANCER
 GASTRIC & PANCREATIC CANCER ASCO HIGHLIGHTS 2005 Fadi Sami Farhat, MD Head of Hematology Oncology Division Hammoud Hospital University Medical Center Saida Lebanon Tel: +961 3 753 155 E-Mail: drfadi@drfadi.org
GASTRIC & PANCREATIC CANCER ASCO HIGHLIGHTS 2005 Fadi Sami Farhat, MD Head of Hematology Oncology Division Hammoud Hospital University Medical Center Saida Lebanon Tel: +961 3 753 155 E-Mail: drfadi@drfadi.org
Clinical Policy: Cetuximab (Erbitux) Reference Number: PA.CP.PHAR.317
 Clinical Policy: (Erbitux) Reference Number: PA.CP.PHAR.317 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that patients
Clinical Policy: (Erbitux) Reference Number: PA.CP.PHAR.317 Effective Date: 01/18 Last Review Date: 11/17 Coding Implications Revision Log Description The intent of the criteria is to ensure that patients
The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review
 The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review M.D. Al-Sarraf 1 1 Williams Beaumont Hospital, Royal Oak, Michigan, USA Introduction In the past, radiotherapy
The Role of Concurrent Chemo-radiotherapy in Patients with Head and Neck Cancers: A Review M.D. Al-Sarraf 1 1 Williams Beaumont Hospital, Royal Oak, Michigan, USA Introduction In the past, radiotherapy
Expanding Role of the Medical Oncologist in the Management of Head and Neck Cancer Nicholas Choong and Everett Vokes DOI: /CA.2007.
 Expanding Role of the Medical Oncologist in the Management of Head and Neck Cancer Nicholas Choong and Everett Vokes CA Cancer J Clin 2008;58;32-53; originally published online Dec 20, 2007; DOI: 10.3322/CA.2007.0004
Expanding Role of the Medical Oncologist in the Management of Head and Neck Cancer Nicholas Choong and Everett Vokes CA Cancer J Clin 2008;58;32-53; originally published online Dec 20, 2007; DOI: 10.3322/CA.2007.0004
trial update clinical
 trial update clinical by John W. Mucenski, BS, PharmD, Director of Pharmacy Operations, UPMC Cancer Centers The treatment outcome for patients with relapsed or refractory cervical carcinoma remains dismal.
trial update clinical by John W. Mucenski, BS, PharmD, Director of Pharmacy Operations, UPMC Cancer Centers The treatment outcome for patients with relapsed or refractory cervical carcinoma remains dismal.
Jonathan Dickinson, LCL Xeloda
 Xeloda A blockbuster in the making Jonathan Dickinson, LCL Xeloda Xeloda unique tumor-activated mechanism Delivering more cancer-killing agent straight into cancer Highly effective comparable efficacy
Xeloda A blockbuster in the making Jonathan Dickinson, LCL Xeloda Xeloda unique tumor-activated mechanism Delivering more cancer-killing agent straight into cancer Highly effective comparable efficacy
The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer
 The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer Robert I. Haddad, Guilherme Rabinowits, Roy B. Tishler,
The PARADIGM Study: A Phase III Study Comparing Sequential Therapy (ST) to Concurrent Chemoradiotherapy (CRT) in Locally Advanced Head and Neck Cancer Robert I. Haddad, Guilherme Rabinowits, Roy B. Tishler,
Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit
 Editorial Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit Hiroto Ishiki, Satoru Iwase Department of Palliative Medicine, The Institute of Medical
Editorial Non-surgical treatment for locally advanced head and neck squamous cell carcinoma: beyond the upper limit Hiroto Ishiki, Satoru Iwase Department of Palliative Medicine, The Institute of Medical
TRANSPARENCY COMMITTEE OPINION. 18 October 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 ERBITUX 2 mg/ml, Solution for infusion 1 bottle of 50 ml (CIP: 565 806 9) Applicant : MERCK LIPHA
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 October 2006 ERBITUX 2 mg/ml, Solution for infusion 1 bottle of 50 ml (CIP: 565 806 9) Applicant : MERCK LIPHA
SAMO MASTERCLASS HEAD & NECK CANCER. Nicolas Mach, PD Geneva University Hospital
 SAMO MASTERCLASS HEAD & NECK CANCER Nicolas Mach, PD Geneva University Hospital Epidemiology Prevention Best treatment for localized disease Best treatment for relapsed or metastatic disease Introduction
SAMO MASTERCLASS HEAD & NECK CANCER Nicolas Mach, PD Geneva University Hospital Epidemiology Prevention Best treatment for localized disease Best treatment for relapsed or metastatic disease Introduction
Heather Wakelee, M.D.
 Heather Wakelee, M.D. Assistant Professor of Medicine, Oncology Stanford University Sponsored by Educational Grant Support from Adjuvant (Post-Operative) Lung Cancer Chemotherapy Heather Wakelee, M.D.
Heather Wakelee, M.D. Assistant Professor of Medicine, Oncology Stanford University Sponsored by Educational Grant Support from Adjuvant (Post-Operative) Lung Cancer Chemotherapy Heather Wakelee, M.D.
Cisplatin and Fluorouracil (head and neck)
 Cisplatin and Fluorouracil (head and neck) Indication Palliative chemotherapy for recurrent or metastatic head and neck squamous cell cancer where combination treatment with cetuximab is not indicated.
Cisplatin and Fluorouracil (head and neck) Indication Palliative chemotherapy for recurrent or metastatic head and neck squamous cell cancer where combination treatment with cetuximab is not indicated.
Update on Chemotherapy for Advanced Colorectal Cancer
 Review Article [1] March 02, 2001 By Daniel G. Haller, MD [2] Efforts to improve the length and quality of life, as well as to expand treatment options, for patients with metastatic colorectal cancer have
Review Article [1] March 02, 2001 By Daniel G. Haller, MD [2] Efforts to improve the length and quality of life, as well as to expand treatment options, for patients with metastatic colorectal cancer have
INAS I. ABDELHALIM, M.D.; NAWAL M. ELSAID, M.D.; ELSAID M. ALI, M.D. and BASHEER S. ATA, M.Sc.
 Med. J. Cairo Univ., Vol. 81, No. 1, December: 887-893, 2013 www.medicaljournalofcairouniversity.net Neoadjuvant Docetaxel (Taxotere) Plus Cisplatin and 5-Flurouracil Followed by Concomitent Chemoradiotherapy
Med. J. Cairo Univ., Vol. 81, No. 1, December: 887-893, 2013 www.medicaljournalofcairouniversity.net Neoadjuvant Docetaxel (Taxotere) Plus Cisplatin and 5-Flurouracil Followed by Concomitent Chemoradiotherapy
Disclosures. Colorectal Cancer Update GAFP November Risk Assessment. Colon and Rectal Cancer The Challenge. Issues in Colon and Rectal Cancer
 Disclosures Colorectal Cancer Update GAFP November 2006 Robert C. Hermann, MD Georgia Center for Oncology Research and Education Northwest Georgia Oncology Centers, PC WellStar Health System Marietta,
Disclosures Colorectal Cancer Update GAFP November 2006 Robert C. Hermann, MD Georgia Center for Oncology Research and Education Northwest Georgia Oncology Centers, PC WellStar Health System Marietta,
The International Federation of Head and Neck Oncologic Societies. Current Concepts in Head and Neck Surgery and Oncology
 The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
The International Federation of Head and Neck Oncologic Societies Current Concepts in Head and Neck Surgery and Oncology www.ifhnos.net The International Federation of Head and Neck Oncologic Societies
Larynx Hypopharynx. Therapy algorithms. Why larynx preservation at all? State of the art Jean Louis Lefebvre,Lille Jan Klozar,Prague
 Larynx Hypopharynx Moderation Rainald Knecht,Hamburg State of the art Jean Louis Lefebvre,Lille Debate pro CRT Jan Klozar,Prague contra CRT Marshall Posner,Boston Clinical cases all Therapy algorithms
Larynx Hypopharynx Moderation Rainald Knecht,Hamburg State of the art Jean Louis Lefebvre,Lille Debate pro CRT Jan Klozar,Prague contra CRT Marshall Posner,Boston Clinical cases all Therapy algorithms
RAMY R. GHALI, M.D.*; EMAN EL-SHARAWY, M.D.*; AZZA M. ADEL, M.D.* and SAMER A. IBRAHIM, M.D.**
 Med. J. Cairo Univ., Vol. 79, No. 2, June: 13-18, 2011 www.medicaljournalofcairouniversity.com Induction Docetaxel, Cisplatin and 5 Fluorouracil (TPF) Followed by Concomitant Chemoradiotherapy Versus Concomitant
Med. J. Cairo Univ., Vol. 79, No. 2, June: 13-18, 2011 www.medicaljournalofcairouniversity.com Induction Docetaxel, Cisplatin and 5 Fluorouracil (TPF) Followed by Concomitant Chemoradiotherapy Versus Concomitant
INTRODUCTION. Cancer Res Treat. 2007;39(3):93-98
 Cancer Res Treat. 2007;39(3):93-98 The Efficacy of an Induction Chemotherapy Combination with Docetaxel, Cisplatin, and 5-FU Followed by Concurrent Chemoradiotherapy in Advanced Head and Neck Cancer Jae-Sook
Cancer Res Treat. 2007;39(3):93-98 The Efficacy of an Induction Chemotherapy Combination with Docetaxel, Cisplatin, and 5-FU Followed by Concurrent Chemoradiotherapy in Advanced Head and Neck Cancer Jae-Sook
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón
 Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Tratamiento Multidisciplinar de Estadios Localmente Avanzados en Cáncer de Pulmón Santiago Ponce Aix Servicio Oncología Médica Hospital Universitario 12 de Octubre Madrid Stage III: heterogenous disease
Cisplatin and Fluorouracil (palliative)
 Cisplatin and Fluorouracil (palliative) Indication Palliative chemotherapy for recurrent or metastatic head and neck squamous cell cancer where combination treatment with cetuximab is not indicated. PS0-1
Cisplatin and Fluorouracil (palliative) Indication Palliative chemotherapy for recurrent or metastatic head and neck squamous cell cancer where combination treatment with cetuximab is not indicated. PS0-1
Management of Advanced Colorectal Cancer in Older Patients
 Review Article [1] April 15, 2005 By Stuart M. Lichtman, MD, FACP [2] Many elderly individuals have substantial life expectancy, even in the setting of significant illness. There is evidence to indicate
Review Article [1] April 15, 2005 By Stuart M. Lichtman, MD, FACP [2] Many elderly individuals have substantial life expectancy, even in the setting of significant illness. There is evidence to indicate
Thoracic and head/neck oncology new developments
 Thoracic and head/neck oncology new developments Goh Boon Cher Department of Hematology-Oncology National University Cancer Institute of Singapore Research Clinical Care Education Scope Lung cancer Screening
Thoracic and head/neck oncology new developments Goh Boon Cher Department of Hematology-Oncology National University Cancer Institute of Singapore Research Clinical Care Education Scope Lung cancer Screening
Drug Comparison: Lartruvo TM (Olaratumab) for Soft Tissue Sarcoma By: Majd Abedrabbo, PharmD Candidate 2018 Fairleigh Dickinson University School of
 Drug Comparison: Lartruvo TM (Olaratumab) for Soft Tissue Sarcoma By: Majd Abedrabbo, PharmD Candidate 2018 Fairleigh Dickinson University School of Pharmacy May 3, 2017 Introduction Soft Tissue Sarcoma
Drug Comparison: Lartruvo TM (Olaratumab) for Soft Tissue Sarcoma By: Majd Abedrabbo, PharmD Candidate 2018 Fairleigh Dickinson University School of Pharmacy May 3, 2017 Introduction Soft Tissue Sarcoma
Maintenance Therapy for Advanced NSCLC: When, What, Why & What s Left After Post-Maintenance Relapse?
 Maintenance Therapy for Advanced NSCLC: When, What, Why & What s Left After Post-Maintenance Relapse? Mark A. Socinski, MD Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive
Maintenance Therapy for Advanced NSCLC: When, What, Why & What s Left After Post-Maintenance Relapse? Mark A. Socinski, MD Professor of Medicine Multidisciplinary Thoracic Oncology Program Lineberger Comprehensive
Vision of the Future: Capecitabine
 Vision of the Future: Capecitabine CHRIS TWELVES Cancer Research Campaign Department of Medical Oncology, University of Glasgow, and Beatson Oncology Centre, Glasgow, United Kingdom Key Words. Capecitabine
Vision of the Future: Capecitabine CHRIS TWELVES Cancer Research Campaign Department of Medical Oncology, University of Glasgow, and Beatson Oncology Centre, Glasgow, United Kingdom Key Words. Capecitabine
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease
 Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
Tristate Lung Meeting 2014 Pro-Con Debate: Surgery has no role in the management of certain subsets of N2 disease Jennifer E. Tseng, MD UFHealth Cancer Center-Orlando Health Sep 12, 2014 Background Approximately
J Clin Oncol 25: by American Society of Clinical Oncology INTRODUCTION
 VOLUME 25 NUMBER 16 JUNE 1 2007 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Open-Label, Uncontrolled, Multicenter Phase II Study to Evaluate the Efficacy and Toxicity of Cetuximab As a Single
VOLUME 25 NUMBER 16 JUNE 1 2007 JOURNAL OF CLINICAL ONCOLOGY O R I G I N A L R E P O R T Open-Label, Uncontrolled, Multicenter Phase II Study to Evaluate the Efficacy and Toxicity of Cetuximab As a Single
MEDICAL PRIOR AUTHORIZATION
 MEDICAL PRIOR AUTHORIZATION TAXOTERE (docetaxel) DOCEFREZ(docetaxel) docetaxel (generic) POLICY I. INDICATIONS The indications below including FDA-approved indications and compendial uses are considered
MEDICAL PRIOR AUTHORIZATION TAXOTERE (docetaxel) DOCEFREZ(docetaxel) docetaxel (generic) POLICY I. INDICATIONS The indications below including FDA-approved indications and compendial uses are considered
Carboplatin and Fluorouracil
 Carboplatin and Fluorouracil Indication Palliative chemotherapy for recurrent or metastatic head and neck squamous cell cancer for patients where cisplatin and / or cetuximab are not appropriate. Performance
Carboplatin and Fluorouracil Indication Palliative chemotherapy for recurrent or metastatic head and neck squamous cell cancer for patients where cisplatin and / or cetuximab are not appropriate. Performance
Cancer Cell Research 14 (2017)
 Available at http:// www.cancercellresearch.org ISSN 2161-2609 Efficacy and safety of bevacizumab for patients with advanced non-small cell lung cancer Ping Xu, Hongmei Li*, Xiaoyan Zhang Department of
Available at http:// www.cancercellresearch.org ISSN 2161-2609 Efficacy and safety of bevacizumab for patients with advanced non-small cell lung cancer Ping Xu, Hongmei Li*, Xiaoyan Zhang Department of
Adjuvant Chemotherapy
 State-of-the-art: standard of care for resectable NSCLC Adjuvant Chemotherapy JY DOUILLARD MD PhD Professor of Medical Oncology Integrated Centers of Oncology R Gauducheau University of Nantes France Adjuvant
State-of-the-art: standard of care for resectable NSCLC Adjuvant Chemotherapy JY DOUILLARD MD PhD Professor of Medical Oncology Integrated Centers of Oncology R Gauducheau University of Nantes France Adjuvant
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist
 Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Non-small Cell Lung Cancer: Multidisciplinary Role: Role of Medical Oncologist Vichien Srimuninnimit, MD. Medical Oncology Division Faculty of Medicine, Siriraj Hospital Outline Resectable NSCLC stage
Accepted 24 October 2007 Published online 22 January 2008 in Wiley InterScience (www.interscience.wiley.com). DOI: /hed.
 ORIGINAL ARTICLE PHASE II STUDY OF GEFITINIB FOR THE TREATMENT OF RECURRENT AND METASTATIC NASOPHARYNGEAL CARCINOMA Daniel T. T. Chua, MD, 1 William I. Wei, MD, 2 Maria P. Wong, MD, 3 Jonathan S. T. Sham,
ORIGINAL ARTICLE PHASE II STUDY OF GEFITINIB FOR THE TREATMENT OF RECURRENT AND METASTATIC NASOPHARYNGEAL CARCINOMA Daniel T. T. Chua, MD, 1 William I. Wei, MD, 2 Maria P. Wong, MD, 3 Jonathan S. T. Sham,
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer
 Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
Update on Neoadjuvant Chemotherapy (NACT) in Cervical Cancer Nicoletta Colombo, MD University of Milan-Bicocca European Institute of Oncology Milan, Italy NACT in Cervical Cancer NACT Stage -IB2 -IIA>4cm
Head and Neck cancer
 Head and Neck cancer Medical Oncologist s Role in Multidisciplinary Teams - Focus on Adjuvant & Neo-adjuvant Therapy - Hye Ryun Kim, M.D. Yonsei Cancer Center, Medical Oncology Contents I. Introduction
Head and Neck cancer Medical Oncologist s Role in Multidisciplinary Teams - Focus on Adjuvant & Neo-adjuvant Therapy - Hye Ryun Kim, M.D. Yonsei Cancer Center, Medical Oncology Contents I. Introduction
BCCA Protocol Summary for Treatment of Advanced Squamous Cell Carcinoma of the Head and Neck Cancer Using Fluorouracil and Platinum
 BCCA Protocol Summary for Treatment of Advanced Squamous Cell Carcinoma of the Head and Neck Cancer Using Fluorouracil and Platinum Protocol Code: Tumour Group: Contact Physician: HNAVFUP Head and Neck
BCCA Protocol Summary for Treatment of Advanced Squamous Cell Carcinoma of the Head and Neck Cancer Using Fluorouracil and Platinum Protocol Code: Tumour Group: Contact Physician: HNAVFUP Head and Neck
Oncologist. The. Taxane-Platinum Combinations in Advanced Non-Small Cell Lung Cancer: A Review JAMES R. RIGAS LEARNING OBJECTIVES ABSTRACT
 The Oncologist Taxane-Platinum Combinations in Advanced Non-Small Cell Lung Cancer: A Review JAMES R. RIGAS Norris Cotton Cancer Center, Dartmouth Medical School, Lebanon, New Hampshire, USA Key Words.
The Oncologist Taxane-Platinum Combinations in Advanced Non-Small Cell Lung Cancer: A Review JAMES R. RIGAS Norris Cotton Cancer Center, Dartmouth Medical School, Lebanon, New Hampshire, USA Key Words.
RT +/- Surgery. Concurrent ChemoRT +/- Surgery
 Molecular targeted approaches to head and neck cancer Lillian L. Siu Department of Medical Oncology & Hematology Princess Margaret Hospital, University of Toronto Locally Advanced HNSCC Locally Advanced
Molecular targeted approaches to head and neck cancer Lillian L. Siu Department of Medical Oncology & Hematology Princess Margaret Hospital, University of Toronto Locally Advanced HNSCC Locally Advanced
Title. CitationInternational Journal of Clinical Oncology, 20(6): 1. Issue Date Doc URL. Rights. Type. File Information
 Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
Title Clinical outcomes of weekly cisplatin chemoradiother Sakashita, Tomohiro; Homma, Akihiro; Hatakeyama, Hir Author(s) Takatsugu; Iizuka, Satoshi; Onimaru, Rikiya; Tsuchiy CitationInternational Journal
Recent Advances in Oral Oncology
 Recent Advances in Oral Oncology Alexander D Rapidis 1 and Crispian Scully 2 1. Chairman, Department of Head and Neck/Maxillofacial Surgery, Greek Anticancer Institute, Saint Savvas Hospital, Athens, and
Recent Advances in Oral Oncology Alexander D Rapidis 1 and Crispian Scully 2 1. Chairman, Department of Head and Neck/Maxillofacial Surgery, Greek Anticancer Institute, Saint Savvas Hospital, Athens, and
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,900 116,000 120M Open access books available International authors and editors Downloads Our
Summary. Primož Strojan. Rep Pract Oncol Radiother, 2007; 12(6): Department of Radiotherapy, Institute of Oncology, Ljubljana, Slovenia
 Original Paper Received: 2007.06.21 Accepted: 2007.09.24 Published: 2007.12.27 Authors Contribution: A Study Design B Data Collection C Statistical Analysis D Data Interpretation E Manuscript Preparation
Original Paper Received: 2007.06.21 Accepted: 2007.09.24 Published: 2007.12.27 Authors Contribution: A Study Design B Data Collection C Statistical Analysis D Data Interpretation E Manuscript Preparation
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective
 Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Management Guidelines and Targeted Therapies in Metastatic Non-Small Cell Lung Cancer: An Oncologist s Perspective Julie R. Brahmer, M.D. Associate Professor of Oncology The Sidney Kimmel Comprehensive
Paclitaxel in Breast Cancer
 Paclitaxel in Breast Cancer EDITH A. PEREZ Mayo Foundation and Mayo Clinic Jacksonville, Jacksonville, Florida, USA Key Words. Paclitaxel Antineoplastic agents Breast neoplasms Clinical trials ABSTRACT
Paclitaxel in Breast Cancer EDITH A. PEREZ Mayo Foundation and Mayo Clinic Jacksonville, Jacksonville, Florida, USA Key Words. Paclitaxel Antineoplastic agents Breast neoplasms Clinical trials ABSTRACT
ROLE OF ALTERED FRACTIONATION & CHEMORADIATION IN HEAD AND NECK CANCER
 ROLE OF ALTERED FRACTIONATION & CHEMORADIATION IN HEAD AND NECK CANCER What is conventional fractionation? Radiation is given at doses of 1.8 to 2.0 Gy delivered once daily, 5 days weekly for 6 to 7 weeks.
ROLE OF ALTERED FRACTIONATION & CHEMORADIATION IN HEAD AND NECK CANCER What is conventional fractionation? Radiation is given at doses of 1.8 to 2.0 Gy delivered once daily, 5 days weekly for 6 to 7 weeks.
through the cell cycle. However, how we administer drugs also depends on the combinations that we give and the doses that we give.
 Hello and welcome to this lecture. My name is Hillary Prescott. I am a Clinical Pharmacy Specialist at The University of Texas MD Anderson Cancer Center. My colleague, Jeff Bryan and I have prepared this
Hello and welcome to this lecture. My name is Hillary Prescott. I am a Clinical Pharmacy Specialist at The University of Texas MD Anderson Cancer Center. My colleague, Jeff Bryan and I have prepared this
Single Technology Appraisal (STA)
 Single Technology Appraisal (STA) Durvalumab for maintenance treatment of locally advanced unresectable non-small cell lung cancer that has not progressed after platinum-based chemoradiation therapy Response
Single Technology Appraisal (STA) Durvalumab for maintenance treatment of locally advanced unresectable non-small cell lung cancer that has not progressed after platinum-based chemoradiation therapy Response
AHFS Final. line. Criteria Used in. combined. cisplatin. Strength. established was. Non-small Cell Lung. Cancer: of carboplatin and
 Drug/Drug Combination: Cetuximab Off-label Use: First-line treatment of advanced non-small Use for Review: cell lung cancer Criteria Used in Selection of Off-labell AHFS Final Determination of Medical
Drug/Drug Combination: Cetuximab Off-label Use: First-line treatment of advanced non-small Use for Review: cell lung cancer Criteria Used in Selection of Off-labell AHFS Final Determination of Medical
Locally advanced head and neck cancer
 Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
Locally advanced head and neck cancer Radiation Oncology Perspective Petek Erpolat, MD Gazi University, Turkey Definition and Management of LAHNC Stage III or IV cancers generally include larger primary
The next wave of successful drug therapy strategies in HER2-positive breast cancer. Hans Wildiers University Hospitals Leuven Belgium
 The next wave of successful drug therapy strategies in HER2-positive breast cancer Hans Wildiers University Hospitals Leuven Belgium Trastuzumab in 1st Line significantly improved the prognosis of HER2-positive
The next wave of successful drug therapy strategies in HER2-positive breast cancer Hans Wildiers University Hospitals Leuven Belgium Trastuzumab in 1st Line significantly improved the prognosis of HER2-positive
Recent advances in the management of metastatic breast cancer in older adults
 Recent advances in the management of metastatic breast cancer in older adults Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Important recent advances in the
Recent advances in the management of metastatic breast cancer in older adults Laura Biganzoli Medical Oncology Dept New Hospital of Prato Istituto Toscano Tumori Italy Important recent advances in the
Policy No: dru281. Medication Policy Manual. Date of Origin: September 24, Topic: Perjeta, pertuzumab. Next Review Date: May 2015
 Medication Policy Manual Topic: Perjeta, pertuzumab Committee Approval Date: May 9, 2014 Policy No: dru281 Date of Origin: September 24, 2012 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Topic: Perjeta, pertuzumab Committee Approval Date: May 9, 2014 Policy No: dru281 Date of Origin: September 24, 2012 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
New Paradigms for Treatment of. Erminia Massarelli, MD, PHD, MS Clinical Associate Professor
 New Paradigms for Treatment of Head and Neck cancers Erminia Massarelli, MD, PHD, MS Clinical Associate Professor City of Hope Disclosure Statement Grant/Research Support frommerck Bristol Grant/Research
New Paradigms for Treatment of Head and Neck cancers Erminia Massarelli, MD, PHD, MS Clinical Associate Professor City of Hope Disclosure Statement Grant/Research Support frommerck Bristol Grant/Research
Cisplatin100 plus Radiotherapy for locally Advanced Squamous Cell Carcinoma Head and Neck
 Cisplatin100 plus Radiotherapy for locally Advanced Squamous Cell Carcinoma Head and Neck Indication: 1) Concomitant chemo-radiotherapy for locally advanced squamous cell carcinoma head and neck 2) Post-operative
Cisplatin100 plus Radiotherapy for locally Advanced Squamous Cell Carcinoma Head and Neck Indication: 1) Concomitant chemo-radiotherapy for locally advanced squamous cell carcinoma head and neck 2) Post-operative
Fluorouracil, Oxaliplatin and Docetaxel (FLOT)
 Fluorouracil, Oxaliplatin and Docetaxel (FLOT) Indication Perioperative chemotherapy for resectable gastric or gastroesophageal junction (GEJ) adenocarcinoma. ICD-10 codes Codes with a prefix C15,C16 Regimen
Fluorouracil, Oxaliplatin and Docetaxel (FLOT) Indication Perioperative chemotherapy for resectable gastric or gastroesophageal junction (GEJ) adenocarcinoma. ICD-10 codes Codes with a prefix C15,C16 Regimen
x Principal Investigator: Muh-Hwa Yang x IRB Approved: Yes
 Clinical Trial Results Cisplatin/Tegafur/Uracil/Irinotecan Triple Combination Therapy for Recurrent/Metastatic Head and Neck Squamous Cell Carcinoma: A Phase I/II Clinical Study SAN-CHI CHEN, a,b,c PETER
Clinical Trial Results Cisplatin/Tegafur/Uracil/Irinotecan Triple Combination Therapy for Recurrent/Metastatic Head and Neck Squamous Cell Carcinoma: A Phase I/II Clinical Study SAN-CHI CHEN, a,b,c PETER
Post-Operative Concurrent Chemoradiation with Mitomycin-C for Advanced Head and Neck Cancer
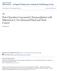 Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2006 Post-Operative Concurrent Chemoradiation with Mitomycin-C for
Yale University EliScholar A Digital Platform for Scholarly Publishing at Yale Yale Medicine Thesis Digital Library School of Medicine 2006 Post-Operative Concurrent Chemoradiation with Mitomycin-C for
Lipoplatin monotherapy for oncologists
 Lipoplatin monotherapy for oncologists Dr. George Stathopoulos demonstrated that Lipoplatin monotherapy against adenocarcinomas of the lung can have very high efficacy (38% partial response, 43% stable
Lipoplatin monotherapy for oncologists Dr. George Stathopoulos demonstrated that Lipoplatin monotherapy against adenocarcinomas of the lung can have very high efficacy (38% partial response, 43% stable
NCCP Chemotherapy Regimen
 QUASAR (Modified) Fluorouracil (370mg/m 2 ) and Folinic Acid (50mg) Weekly INDICATIONS FOR USE: Regimen INDICATION ICD10 Code Treatment of metastatic colorectal cancer C18 00428a Adjuvant treatment of
QUASAR (Modified) Fluorouracil (370mg/m 2 ) and Folinic Acid (50mg) Weekly INDICATIONS FOR USE: Regimen INDICATION ICD10 Code Treatment of metastatic colorectal cancer C18 00428a Adjuvant treatment of
NCCP Chemotherapy Protocol. Cetuximab Therapy - 7 days
 Cetuximab Therapy - 7 days INDICATIONS FOR USE: INDICATION Treatment of patients with epidermal growth factor receptor (EGFR)- expressing RAS wild-type metastatic colorectal cancer (mcrc) Treatment of
Cetuximab Therapy - 7 days INDICATIONS FOR USE: INDICATION Treatment of patients with epidermal growth factor receptor (EGFR)- expressing RAS wild-type metastatic colorectal cancer (mcrc) Treatment of
