Hematolymphoid lesions of the skin Part II Myeloid neoplastic proliferations Houston Society of Clinical Pathologists Symposium April 14, 2018
|
|
|
- Rosemary Henderson
- 5 years ago
- Views:
Transcription
1 Hematolymphoid lesions of the skin Part II Myeloid neoplastic proliferations Houston Society of Clinical Pathologists Symposium April 14, 2018 Carlos A. Torres-Cabala, MD Associate Professor Chief, Dermatopathology Section The University of Texas MD Anderson Cancer Center Houston, Texas
2 No conflicts of interest to disclose
3 Myeloid leukemia cutis Skin involvement in myeloproliferative disorders (CMML) Blastic plasmacytoid dendritic cell neoplasm
4 Myeloid Leukemia Cutis
5 Myeloid Leukemia Cutis Leukemia cutis (LC) by myeloid (granulocytic or monocytic) neoplastic cells occurs in the setting of acute myeloid leukemia (AML), myelodysplastic syndrome (MDS), and myeloproliferative disorders (MPDs) Rare cases of cutaneous involvement without systemic disease are reported as aleukemic LC
6
7 Myeloid Leukemia Cutis
8 Myeloid Leukemia Cutis LC occurs in about 10% of patients with AML, less frequently in chronic myeloproliferative disorders The most common types of AML involving skin are AMML and acute monocytic leukemia (50% of patients present with skin involvement) Patients present with a solitary or multiple erythematous, violaceous, or hemorrhagic papules or nodules The prognosis of LC is usually poor
9
10 Courtesy of Dr. C. Chian
11 Myeloid Leukemia Cutis LC presents as a perivascular and periadnexal or diffuse infiltrate of mononuclear cells involving dermis and subcutis without extension into the epidermis The term myeloid sarcoma applies when the proliferation of immature myeloid (granulocytic) cells completely effaces the skin architecture (and corresponds to extrahematopoietic myeloid leukemia mostly de novo )
12
13
14
15
16
17 Myeloid Leukemia Cutis The cytologic appearance of the tumor cells vary according to the type of leukemia and therefore the infiltrate may show blastic, monocytoid/histiocytic, or pleomorphic features; in some cases it mimics carcinoma Immature eosinophils may be present
18
19 Myeloid Leukemia Cutis Confounding findings: Numerous neutrophils, with or without leukocytoclasia (Sweet syndrome-like) Numerous histiocyte-like cells (Histiocytoid Sweet syndrome-like) Granulomatous changes (and GA-like pattern)
20 Myeloid Leukemia Cutis The AML and MDS cells are commonly positive for CD43 Other markers useful in the diagnosis: lysozyme, myeloperoxidase (at least focally), myeloid nuclear differentiation antigen (MNDA), CD68, and CD45, and may express CD34, CD33, CD4, CD117, CD163, CD56, CD123, HLA-DR In general: lack of expression of T-cell markers, B-cell markers, and CD30
21 Subtil A
22 A B A. CD43 B. CD33 C. Myeloperoxidase C
23
24 Myeloid Leukemia Cutis CD34 and CD117 have been reported to have relatively low sensitivity (10-30%) AMML is most likely to be negative for CD34 and CD117 CD34 is often negative in NPM1-mutated cases
25 Myeloid Leukemia Cutis Some AML may express B cell markers: CD19, PAX5, CD79a (AML with t(8;21) Discrepancies between blood/bone marrow and skin phenotypes are not uncommon (CD34)
26 Myeloid Leukemia Cutis Cytogenetics shows normal karyotype in about 40%, complex abnormalities (20%), aneuploidy of chromosome 8 (15%) (Benet et al. 2011) Complex karyotype seems to be most frequent in secondary (39%) than de novo cases (17%) (Claerhout et al. 2018)
27 Myeloid Leukemia Cutis Demonstration of genetic abnormalities is sometimes necessary for a diagnosis of LC or myeloid sarcoma These findings include abnormalities in chromosome 8 copy numbers, monosomy 7, NPM1 mutations, inv (16), and MLL (11q23) gene rearrangement, among others
28 Myeloid Leukemia Cutis In a recent report (Claerhout et al. 2018), de novo MS demonstrated RUNX1-RUNX1T1 (10%), followed by CBFB-MYH11, KMT2A- MLLT3, and JAK2 V617F mutation
29 Eur J Haematol Mar 12
30 Myeloid Leukemia Cutis Molecular tests may aid may confirm and/or establish the diagnosis of LC in aleukemic patients
31
32 E. CD68, F. CD163, G. CD33, H. CD43, I. CD34, J. MPO
33 K. Molecular analysis. A01: bone marrow; B01: skin
34 Cutaneous Manifestations of Myeloproliferative Neoplasms (Chronic Myelomonocytic Leukemia)
35 CMML CMML is a chronic hematologic disorder that displays features of both a myeloproliferative and a myelodysplastic syndrome
36 CMML Chronic myelomonocytic leukemia (CMML) cells in the skin have been described to variably display a spectrum of molecules of dendritic cell differentiation in addition to the myeloid markers already described, such as CD123, TCL1, CD1a, and S100
37 CMML Vitte et al. studied a large series of CMML cases involving skin and described four patterns: Myelomonocytic cell tumors Mature plasmacytoid dendritic cell neoplasms Blastic plasmacytoid dendritic cell neoplasms Blastic indeterminate dendritic cell tumors
38
39
40
41
42
43
44
45 A clonal relationship between CMML and cutaneous indeterminate dendritic cell neoplasm is supported by the ability of malignant monocytes to differentiate into dendritic cells in vitro IDCN in patients with CMML may be part of the continuum of myeloid, monocytic, and dendritic cell subsets conforming a single hematopoietic neoplasm
46 Blastic Plasmacytoid Dendritic Cell Neoplasm
47 BPDCN Blastic plasmacytoid dendritic cell neoplasm (BPDCN) is a rare tumor thought to derive from precursors of plasmacytoid dendritic cells (pdc, professional type I interferonproducing cells) BPDCN usually affects male adults and presents as asymptomatic nodules or bruiselike lesions, most of the cases without evidence of extracutaneous disease
48 Courtesy of Dr. M. Postigo
49 BPDCN As the disease progresses, it involves peripheral blood and bone marrow At diagnosis most patients present with stage IV disease Cases presenting without skin involvement are extremely rare; most patients eventually develop cutaneous lesions
50 BPDCN Patients develop leukemia in the terminal stage of the disease Median survival is months About a quarter of the cases present with myelodysplasia or other myeloid disorders: 10 to 20% are associated or progress into myeloid processes such as CMML (most frequently), MDS, or AML
51 BPDCN BPDCN is characterized by a dense diffuse infiltrate involving dermis and subcutis, composed by medium-sized cells with blastic appearance Dermal hemorrhage is frequent Less cellular, perivascular infiltrates can be seen in cases undergoing therapy.
52
53
54
55 BPDCN The tumor cells in BPDCN are classically CD4+/CD56+, but occasional cases with negative or only weak expression of one of the two markers can be encountered 8% of cases are negative for CD4 or CD56
56 BPDCN Other more specific markers of plasmacytoid dendritic cells such as CD123, TCL-1, and TCF4 are generally expressed The tumor cells may express CD43, CD45RA, CD45, CD7, CD2, CD33, CD68 (50-80% as dotlike cytoplasmic pattern), and TdT
57 CD4 CD123 CD56 TdT
58
59
60
61 CD123/TCF4
62 BPDCN The tumor cells can express other plasmacytoid dendritic cell-associated markers: BDCA-2/CD303 (blood dendritic cell antigen 2, most sensitive marker?), MxA (interferon alpha-dependent) Other hematopoietic precursor-associated antigens (CD38, HLA-DR) are expressed in most of the cases
63 BPDCN 25-30% positive for S100 (more frequently in children) 30% positive for TdT May express BCL2, BCL6, MUM1
64 BPDCN Usually negative for: myeloblastic markers (CD13, MPO, MNDA) monoblastic markers (CD11c, CD14, lysozyme) B and T lymphoblasts (CD19, PAX5, CD3, LAT, CD5, CD20) CD34, CD117, EBER
65 BPDCN Somatic mutations in NRAS, ATM, TET2 and TP53, among others, have been identified in BPDCN ASXL1, IKZF3, ATM, MET, KRAS, IDH2, KIT, APC, RB1, VHL, BRAF, MLH1, RET Some of these mutations are also seen in myeloid leukemias, underscoring the close relationship between BPDCN and myeloid disorders
66 BPDCN Inactivation of tumor suppressor genes (RB1, TP53, ASXL1, PBRM1, CDKN2A/CDKN2B/CDKN1B), activation of oncogenes (NRAS, KRAS), mutations in epigenetic regulators (TET2, TET1, DNMT3A, IDH1, IDH2), frequently mutated in AML and MDS Mutations in IKAROS family genes (IKZF3/IKZF1) and ATM, also found in lymphoid neoplasms Most frequent: TET2 (36%), ASXL1 (32%), NRAS (20%), NPM1 (20%) Same mutations of TET2 and SRSF2 were detected in both CMML and BPDCN
67 BPDCN Genomic losses are frequent Complex aberrations similar to those seen in MDS/AML Losses in 5q21 or 5q34, 12p13, 13q13-q21, 6q23-qter, 15q, chromosome 9 Deleted regions involve 9p21.3 (CDKN2A/CDKN2B), 13q13.1-q14.3 (RB1), 12p13.2-p13.1 (CDKN1B), 13q11-q12 (LATS2), and 7p12.2 (IKZF1) Biallelic loss of 9p21.3 appears to be associated with bad prognosis
68 BPDCN Shorter survival: extensive marrow or peripheral blood blastosis, low TdT, low CD303, low Ki67, CDKN2A/CDKN2B deletions, mutations in DNA methylation pathway genes Boddu et al (MDACC) reported 10-15% of cases showing 8q24/MYC rearrangement and response to ALL therapies
69 Plasmacytoid dendritic cells (pdc) are not present in normal skin Reactive infiltrates rich in pdc can be seen in skin in: Allergic contact hypersensitivity reactions Lupus erythematosus Psoriasis Positive reactions to tuberculin skin test (PPD) Viral infections (herpes simplex, varicella) Hydroa vacciniforme
70 Aggregates of PDCs can be seen in Kikuchi, Castleman hyaline-vascular disease, among others, but these are not extensive nodules
71 Mature plasmacytoid dendritic cell proliferation associated with myeloid neoplasms Most patients with CMML, rarely MDS, AML with monocytic differentiation, NO CML Lymphadenopathy and skin lesions (multiple erythematous macules or papules) Infiltrates of cells similar to normal PDC, with occasional rims of cells phenotypically corresponding to interdigitating dendritic cells (S100+, CD1a+) IHC: similar to normal PDC with occasional aberrant expression of CD2, CD5, CD7, CD10, CD13, CD14, CD15, CD33, low Ki67, negative TdT, CD34
72
73 Mature plasmacytoid dendritic cell proliferation associated with myeloid neoplasms There is evidence of clonal relationship between these cells and the myeloid tumor Treatment of the myeloid neoplasm may result in regression of the plasmacytoid dendritic cell infiltrates Prognosis is dismal (evolution of the myeloid process)
74
75
76
77
78 Immunology Jan 3
79 Take home messages CD43 is an important marker for the diagnosis of myeloid leukemia cutis Be aware that MPO and lysozyme can be only focally positive in myeloid leukemia cutis CD34 and CD117 may be negative in myeloid leukemia cutis; phenotype discrepancies with bone marrow leukemic cells occur
80 Take home messages Remember that myeloid, monocytoid, and dendritic cells display great plasticity Be aware of histiocytoid or indeterminate dendritic cell proliferations that actually represent involvement by myeloid neoplasms
81 Take home messages Plasmacytoid dendritic cells are not found in normal skin; these cells are usually CD56 negative and Granzyme B positive Tumors derived from plasmacytoid dendritic cells may show a mature phenotype or a blastic phenotype (BPDCN)
82 Acknowledgements Dermatopathology Section Dr. Victor Prieto Dr. Doina Ivan Dr. Jonathan Curry Dr. Michael Tetzlaff Dr. Phyu Aung Dr. Priya Nagarajan
83
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH )
 Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Blastic Plasmacytoid Dendritic Cell Neoplasm with DNMT3A and TET2 mutations (SH2017-0314) Habibe Kurt, Joseph D. Khoury, Carlos E. Bueso-Ramos, Jeffrey L. Jorgensen, Guilin Tang, L. Jeffrey Medeiros, and
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
The spectrum of flow cytometry of the bone marrow
 The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
The spectrum of flow cytometry of the bone marrow Anna Porwit Lund University Faculty of Medicine Dept. of Clinical Sciences Div. Oncology and Pathology anna.porwit@med.lu.se Disclosure of speaker s interests
Molecular Markers in Acute Leukemia. Dr Muhd Zanapiah Zakaria Hospital Ampang
 Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Molecular Markers in Acute Leukemia Dr Muhd Zanapiah Zakaria Hospital Ampang Molecular Markers Useful at diagnosis Classify groups and prognosis Development of more specific therapies Application of risk-adjusted
Session 7 Summary. Magdalena Czader, MD, PhD David Czuchlewski, MD MOLECULAR GENETICS OF HEMATOPOIETIC NEOPLASMS
 Session 7 Summary Magdalena Czader, MD, PhD David Czuchlewski, MD MOLECULAR GENETICS OF HEMATOPOIETIC NEOPLASMS 1 Cases according to 2016 WHO classification Acute myeloid leukemia: 26 AML with recurrent
Session 7 Summary Magdalena Czader, MD, PhD David Czuchlewski, MD MOLECULAR GENETICS OF HEMATOPOIETIC NEOPLASMS 1 Cases according to 2016 WHO classification Acute myeloid leukemia: 26 AML with recurrent
AML: WHO classification, biology and prognosis. Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen
 AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
AML: WHO classification, biology and prognosis Dimitri Breems, MD, PhD Internist-Hematoloog Ziekenhuis Netwerk Antwerpen Acute myeloid leukemia Clonal expansion of undifferentiated myeloid precursors Impaired
Update on the WHO Classification of Acute Myeloid Leukemia. Kaaren K. Reichard, MD Mayo Clinic Rochester
 Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Update on the WHO Classification of Acute Myeloid Leukemia Kaaren K. Reichard, MD Mayo Clinic Rochester reichard.kaaren@mayo.edu Nothing to disclose Conflict of Interest Objectives Present a practical
Mixed Phenotype Acute Leukemias
 Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
Mixed Phenotype Acute Leukemias CHEN GAO; AMY M. SANDS; JIANLAN SUN NORTH AMERICAN JOURNAL OF MEDICINE AND SCIENCE APR 2012 VOL 5 NO.2 INTRODUCTION Most cases of acute leukemia can be classified based
SUPPLEMENTARY INFORMATION
 Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Neoplasias)de)células)dendrí1cas)plasmocitoides)blás1cas.) Dr#San'ago#Montes#Moreno## Servicio#de#Anatomía#Patológica#HUMV.#
 Neoplasias)de)células)dendrí1cas)plasmocitoides)blás1cas.) Dr#San'ago#Montes#Moreno## Servicio#de#Anatomía#Patológica#HUMV.# smontes@humv.es# )Clinical)features:)) ) 61#year#old#male#with#mul'ple#cutaneous#
Neoplasias)de)células)dendrí1cas)plasmocitoides)blás1cas.) Dr#San'ago#Montes#Moreno## Servicio#de#Anatomía#Patológica#HUMV.# smontes@humv.es# )Clinical)features:)) ) 61#year#old#male#with#mul'ple#cutaneous#
3/31/2017. Disclosure of Relevant Financial Relationships
 Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content of CME disclose any relevant financial relationship
Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content of CME disclose any relevant financial relationship
9/25/2017. Disclosure. I have nothing to disclose. Young S. Kim MD Dept. of Pathology
 Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Disclosure MAST CELLNEOPLASM I have nothing to disclose. Young S. Kim MD Dept. of Pathology 1 Objectives What is mast cell lineage? Changes in updated WHO 2016 mastocytosis Issues of Mastocytosis CD30
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Treatments and Current Research in Leukemia. Richard A. Larson, MD University of Chicago
 Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
Treatments and Current Research in Leukemia Richard A. Larson, MD University of Chicago 2 Acute (rapid progression) Myeloid Acute myeloid leukemia (AML) Acute promyelocytic leukemia (APL) Lymphoid Acute
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities
 WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
WHO Classification of Myeloid Neoplasms with Defined Molecular Abnormalities Robert W. McKenna, M.D. 1/2009 WHO Classification of Myeloid Neoplasms (4th Edition)--2008 Incorporates new information that
Acute Myeloid Leukemia with RUNX1 and Several Co-mutations
 Case SH2017-0281 Acute Myeloid Leukemia with RUNX1 and Several Co-mutations James Bauer, MD, PhD David Yang, MD Erik Ranheim, MD, PhD Catherine Leith, MB, Bchir Clinical History Chief Complaint: 72 year
Case SH2017-0281 Acute Myeloid Leukemia with RUNX1 and Several Co-mutations James Bauer, MD, PhD David Yang, MD Erik Ranheim, MD, PhD Catherine Leith, MB, Bchir Clinical History Chief Complaint: 72 year
2010 Hematopoietic and Lymphoid ICD-O Codes - Alphabetical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
Acute basophilic leukemia 9870/3 Acute biphenotypic leukemia [OBS] 9805/3 Acute erythroid leukemia 9840/3 Acute megakaryoblastic leukemia 9910/3 Acute monoblastic and monocytic leukemia 9891/3 Acute myeloid
2012 Hematopoietic and Lymphoid ICD-O Codes - Numerical List THIS TABLE REPLACES ALL ICD-O-3 Codes
 Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Malignant lymphoma, NOS 9590/3 Non-Hodgkin lymphoma, NOS 9591/3 B-cell lymphoma, unclassifiable, with features intermediate between diffuse large B-cell lymphoma and classical Hodgkin lymphoma 9596/3 Primary
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and
 Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
Group of malignant disorders of the hematopoietic tissues characteristically associated with increased numbers of white cells in the bone marrow and / or peripheral blood Classified based on cell type
5/21/2018. Disclosures. Objectives. Normal blood cells production. Bone marrow failure syndromes. Story of DNA
 AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
AML: Understanding your diagnosis and current and emerging treatments Nothing to disclose. Disclosures Mohammad Abu Zaid, MD Assistant Professor of Medicine Indiana University School of Medicine Indiana
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
3/24/2017 DENDRITIC CELL NEOPLASMS: HISTOLOGY, IMMUNOHISTOCHEMISTRY, AND MOLECULAR GENETICS. Disclosure of Relevant Financial Relationships
 DENDRITIC CELL NEOPLASMS: HISTOLOGY, IMMUNOHISTOCHEMISTRY, AND MOLECULAR GENETICS Jason L. Hornick, M.D., Ph.D. Director of Surgical Pathology and Immunohistochemistry Brigham and Women s Hospital Professor
DENDRITIC CELL NEOPLASMS: HISTOLOGY, IMMUNOHISTOCHEMISTRY, AND MOLECULAR GENETICS Jason L. Hornick, M.D., Ph.D. Director of Surgical Pathology and Immunohistochemistry Brigham and Women s Hospital Professor
Corrigenda. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run
 Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation
 Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
Eosinophilia: A Diagnostic Approach and Test Utilization Strategies for Bone Marrow Evaluation American Society for Clinical Pathology 2014 Annual Meeting Presented by: Matthew T. Howard, MD Assistant
CASE REPORT LEUKEMIA CUTIS- A CASE REPORT
 LEUKEMIA CUTIS- A CASE REPORT C. Nirmala 1, Mangal V. Kulkarni 2. 1. Associate Professor, Department Of Pathology, Bangalore Medical College &RI 2. Tutor, Department Of Pathology, Bangalore Medical College
LEUKEMIA CUTIS- A CASE REPORT C. Nirmala 1, Mangal V. Kulkarni 2. 1. Associate Professor, Department Of Pathology, Bangalore Medical College &RI 2. Tutor, Department Of Pathology, Bangalore Medical College
Combinations of morphology codes of haematological malignancies (HM) referring to the same tumour or to a potential transformation
 Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Major subgroups according to the World Health Organisation (WHO) Classification Myeloproliferative neoplasms (MPN) Myeloid and lymphoid neoplasms with eosinophilia and abnormalities of PDGFRA, PDGFRB or
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1
 Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
Juan Ma 1, Jennifer Dunlap 2, Lisong Shen 1, Guang Fan 2 1 Xin Hua Hospital, Shanghai, China 2 Oregon Health & Science University, Portland, OR, United States AML is a hematopoietic neoplasms characterized
Objectives. Morphology and IHC. Flow and Cyto FISH. Testing for Heme Malignancies 3/20/2013
 Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
GENETICS OF HEMATOLOGICAL MALIGNANCIES
 de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
de DUVE INSTITUTE GENETICS OF HEMATOLOGICAL MALIGNANCIES INTERUNIVERSITY CERTIFICATE IN HUMAN GENETICS Université catholique de Louvain Brussels,19/02/2016 Professor Hélène Antoine-Poirel, MD, PhD Center
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Diagnostic Approach for Eosinophilia and Mastocytosis. Curtis A. Hanson, M.D.
 Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Diagnostic Approach for Eosinophilia and Mastocytosis Curtis A. Hanson, M.D. 2014 MFMER slide-1 DISCLOSURES: Relevant Financial Relationship(s) None Off Label Usage None 2014 MFMER slide-2 Molecular Classification
Case year old male with abdominal lymphadenopathy Treated with 8 cycles of R-CHOP One year later B-symptoms and progressive disease
 Codirectors Tsieh Sun, M.D., FASCP Francisco Vega, M.D., Ph.D. Department of Hematopathology UT MD Anderson Cancer Center Houston Texas There is no conflict of interest involved in the content and presentation
Codirectors Tsieh Sun, M.D., FASCP Francisco Vega, M.D., Ph.D. Department of Hematopathology UT MD Anderson Cancer Center Houston Texas There is no conflict of interest involved in the content and presentation
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota
 Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Reporting cytogenetics Can it make sense? Daniel Weisdorf MD University of Minnesota Reporting cytogenetics What is it? Terminology Clinical value What details are important Diagnostic Tools for Leukemia
Update on Spitzoid and Blue nevus-like melanocytic lesions Emphasis on molecular studies informing diagnosis, prognosis and therapy
 Update on Spitzoid and Blue nevus-like melanocytic lesions Emphasis on molecular studies informing diagnosis, prognosis and therapy Michael T. Tetzlaff MD, PhD Associate Professor Department of Pathology,
Update on Spitzoid and Blue nevus-like melanocytic lesions Emphasis on molecular studies informing diagnosis, prognosis and therapy Michael T. Tetzlaff MD, PhD Associate Professor Department of Pathology,
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual
 Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
Changes to the Hematopoietic and Lymphoid Neoplasm Coding Manual KCR 2018 SPRING TRAINING 2018 Hematopoietic Database Updates Updates were done to the Hematopoietic Database based on the WHO Hematopoietic
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
JMSCR Vol 05 Issue 05 Page May 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i5.11 Leukemia Cutis with Acute Myelomonocytic
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i5.11 Leukemia Cutis with Acute Myelomonocytic
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Leukemia (2007) 21, Cytoplasmic mutated nucleophosmin (NPM) defines the molecular status of a significant fraction of myeloid sarcomas
 Leukemia (2007) 21, 1566-1570 Cytoplasmic mutated nucleophosmin (NPM) defines the molecular status of a significant fraction of myeloid sarcomas Clinical presentation Mean age: 55.8 years (range: 16-87).
Leukemia (2007) 21, 1566-1570 Cytoplasmic mutated nucleophosmin (NPM) defines the molecular status of a significant fraction of myeloid sarcomas Clinical presentation Mean age: 55.8 years (range: 16-87).
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD. Part 4 MYELOID NEOPLASMS
 HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
HENATOLYMPHOID SYSTEM THIRD YEAR MEDICAL STUDENTS- UNIVERSITY OF JORDAN AHMAD T. MANSOUR, MD Part 4 MYELOID NEOPLASMS Introduction: o Myeloid neoplasms are divided into three major categories: o Acute
Bone Marrow. Procedures Blood Film Aspirate, Cell Block Trephine Biopsy, Touch Imprint
 Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
Bone Marrow Protocol applies to acute leukemias, myelodysplastic syndromes, myeloproliferative disorders, chronic lymphoproliferative disorders, malignant lymphomas, plasma cell dyscrasias, histiocytic
WHO Classification 7/2/2009
 Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Least Malignant Myeloproliferative Disorders Myelodysplastic Syndromes Most Malignant Acute Leukemia Classifying Hematopoietic Disorders French-American-British (FAB) World Health Organization (WHO) Thanks
Summary. Case report. DOI /j x
 CASE REPORT DOI 10.1111/j.1365-2133.2008.08480.x Acute myeloid dendritic cell leukaemia with specific cutaneous involvement: a diagnostic challenge M. Ferran, F. Gallardo, A.M. Ferrer,* A. Salar, E. Pérez-Vila,*
CASE REPORT DOI 10.1111/j.1365-2133.2008.08480.x Acute myeloid dendritic cell leukaemia with specific cutaneous involvement: a diagnostic challenge M. Ferran, F. Gallardo, A.M. Ferrer,* A. Salar, E. Pérez-Vila,*
Extramedullary precursor T-lymphoblastic transformation of CML at presentation
 Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
Extramedullary precursor T-lymphoblastic transformation of CML at presentation Neerja Vajpayee, Constance Stein, Bernard Poeisz & Robert E. Hutchison Clinical History 30 year old man presented to the emergency
Application of Whole Genome Microarrays in Cancer: You should be doing this test!!
 Application of Whole Genome Microarrays in Cancer: You should be doing this test!! Daynna Wolff, Ph.D. Director, Cytogenetics and Genomics Disclosures Clinical Laboratory Director and Employee, Medical
Application of Whole Genome Microarrays in Cancer: You should be doing this test!! Daynna Wolff, Ph.D. Director, Cytogenetics and Genomics Disclosures Clinical Laboratory Director and Employee, Medical
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
LL - LL-ROHINI (NATIONAL REFERENCE 135091533 Age 28 Years Gender Male 1/9/2017 120000AM 1/9/2017 105415AM 4/9/2017 23858M Ref By Final LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE, ANY 6 MARKERS t (1;19) (q23
The Revised 2016 WHO Classification of Acute Leukemias
 The Revised 2016 WHO Classification of Acute Leukemias Robert P Hasserjian, MD Associate Professor Massachusetts General Hospital and Harvard Medical School Acute leukemias Aggressive hematopoietic neoplasms
The Revised 2016 WHO Classification of Acute Leukemias Robert P Hasserjian, MD Associate Professor Massachusetts General Hospital and Harvard Medical School Acute leukemias Aggressive hematopoietic neoplasms
Out-Patient Billing CPT Codes
 Out-Patient Billing CPT Codes Updated Date: August 3, 08 Client Billed Molecular Tests HPV DNA Tissue Testing 8764 No Medicare Billed - Molecular Tests NeoARRAY NeoARRAY SNP/Cytogenetic No 89 NeoLAB NeoLAB
Out-Patient Billing CPT Codes Updated Date: August 3, 08 Client Billed Molecular Tests HPV DNA Tissue Testing 8764 No Medicare Billed - Molecular Tests NeoARRAY NeoARRAY SNP/Cytogenetic No 89 NeoLAB NeoLAB
CHAPTER:4 LEUKEMIA. BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY 8/12/2009
 LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
LEUKEMIA CHAPTER:4 1 BY Mrs. K.SHAILAJA., M. PHARM., LECTURER DEPT OF PHARMACY PRACTICE, SRM COLLEGE OF PHARMACY Leukemia A group of malignant disorders affecting the blood and blood-forming tissues of
Molecular. Oncology & Pathology. Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine. Liquid Biopsy.
 Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
Molecular Oncology & Pathology Hereditary Cancer Somatic Cancer Liquid Biopsy Next-Gen Sequencing qpcr Sanger Sequencing Diagnostic, Prognostic, Therapeutic, and Predisposition Tests in Precision Medicine
SWOG ONCOLOGY RESEARCH PROFESSIONAL (ORP) MANUAL LEUKEMIA FORMS CHAPTER 16A REVISED: DECEMBER 2017
 LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
LEUKEMIA FORMS The guidelines and figures below are specific to Leukemia studies. The information in this manual does NOT represent a complete set of required forms for any leukemia study. Please refer
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017
 Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Examining Genetics and Genomics of Acute Myeloid Leukemia in 2017 Elli Papaemmanuil, PhD Memorial Sloan Kettering Cancer Center New York, New York, United States Today s Talk Cancer genome introduction
Test Name Results Units Bio. Ref. Interval. Positive
 LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
LL - LL-ROHINI (NATIONAL REFERENCE 135091534 Age 36 Years Gender Female 1/9/2017 120000AM 1/9/2017 105316AM 2/9/2017 104147AM Ref By Final LEUKEMIA GENETIC ROFILE ANY SIX MARKERS, CR QUALITATIVE AML ETO
Update on Merkel cell carcinoma
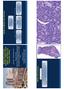 Merkel cell carcinoma: Diagnosis, staging, sentinel lymph node biopsy and prognostic markers Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational
Merkel cell carcinoma: Diagnosis, staging, sentinel lymph node biopsy and prognostic markers Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational
Integrated Hematopathology. Morphology and FCI with IHC
 Integrated Hematopathology Morphology and FCI with IHC FrontMatter.indd i 9/6/2009 9:30:12 PM FrontMatter.indd ii 9/6/2009 9:30:18 PM Integrated Hematopathology Morphology and FCI with IHC Cherie H Dunphy,
Integrated Hematopathology Morphology and FCI with IHC FrontMatter.indd i 9/6/2009 9:30:12 PM FrontMatter.indd ii 9/6/2009 9:30:18 PM Integrated Hematopathology Morphology and FCI with IHC Cherie H Dunphy,
Pathology. #11 Acute Leukemias. Farah Banyhany. Dr. Sohaib Al- Khatib 23/2/16
 35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
35 Pathology #11 Acute Leukemias Farah Banyhany Dr. Sohaib Al- Khatib 23/2/16 1 Salam First of all, this tafreegh is NOT as long as you may think. If you just focus while studying this, everything will
Acute leukemia and myelodysplastic syndromes
 11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
11/01/2012 Post-ASH meeting 1 Acute leukemia and myelodysplastic syndromes Peter Vandenberghe Centrum Menselijke Erfelijkheid & Afdeling Hematologie, UZ Leuven 11/01/2012 Post-ASH meeting 2 1. Acute myeloid
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Therapy-related acute myeloid leukemia with germline TP53 mutation (Li-Fraumeni syndrome) SH Chelsey Deel MD Teresa Scordino MD
 Therapy-related acute myeloid leukemia with germline TP53 mutation (Li-Fraumeni syndrome) SH2017-167 Chelsey Deel MD Teresa Scordino MD Clinical History HPI: 44 year old Caucasian female referred for evaluation
Therapy-related acute myeloid leukemia with germline TP53 mutation (Li-Fraumeni syndrome) SH2017-167 Chelsey Deel MD Teresa Scordino MD Clinical History HPI: 44 year old Caucasian female referred for evaluation
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression
 Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Spectrum of clinical presentations
 Spectrum of clinical presentations Case History A 7-day-old male patient born full-term via uncomplicated vaginal delivery was seen for multiple erythematous red-brown purpuric lesions that were present
Spectrum of clinical presentations Case History A 7-day-old male patient born full-term via uncomplicated vaginal delivery was seen for multiple erythematous red-brown purpuric lesions that were present
Session 4: Summary and Conclusions
 Session 4: Summary and Conclusions Total cases in Session 4 Myeloproliferative neoplasms 16 cases Oral #300 (CEL, NOS) Mastocytosis 2 cases Oral #156 (SM-AHN) Myeloid/lymphoid neoplasms with eosinophilia
Session 4: Summary and Conclusions Total cases in Session 4 Myeloproliferative neoplasms 16 cases Oral #300 (CEL, NOS) Mastocytosis 2 cases Oral #156 (SM-AHN) Myeloid/lymphoid neoplasms with eosinophilia
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Merkel cell carcinoma: Diagnosis, staging, sentinel lymph node biopsy and prognostic markers
 Merkel cell carcinoma: Diagnosis, staging, sentinel lymph node biopsy and prognostic markers Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational
Merkel cell carcinoma: Diagnosis, staging, sentinel lymph node biopsy and prognostic markers Michael T. Tetzlaff MD, PhD Associate Professor Departments of Pathology (Dermatopathology) and Translational
Primer of Immunohistochemistry (Leukocytic)
 Primer of Immunohistochemistry (Leukocytic) Paul K. Shitabata, M.D. Dermatopathology Institute Torrance, CA BENIGN LYMPHOID SKIN LESIONS CAPABLE OF SIMULATING LYMPHOMA -Jessner s lymphoid infiltrate -Dermal-subcutaneous
Primer of Immunohistochemistry (Leukocytic) Paul K. Shitabata, M.D. Dermatopathology Institute Torrance, CA BENIGN LYMPHOID SKIN LESIONS CAPABLE OF SIMULATING LYMPHOMA -Jessner s lymphoid infiltrate -Dermal-subcutaneous
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities
 Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Acute Myeloid Leukemia with Recurrent Cytogenetic Abnormalities Acute Myeloid Leukemia with recurrent cytogenetic Abnormalities -t(8;21)(q22;q22)(aml/eto) -inv(16) or t(16;16) -t(15;17) -11q23 Acute Myeloid
Session 5. Pre-malignant clonal hematopoietic proliferations. Chairs: Frank Kuo and Valentina Nardi
 Session 5 Pre-malignant clonal hematopoietic proliferations Chairs: Frank Kuo and Valentina Nardi Pre-malignant clonal hematopoietic proliferations Clonal LYMPHOID proliferations: - Monoclonal gammopathy
Session 5 Pre-malignant clonal hematopoietic proliferations Chairs: Frank Kuo and Valentina Nardi Pre-malignant clonal hematopoietic proliferations Clonal LYMPHOID proliferations: - Monoclonal gammopathy
SH/EAHP WORKSHOP 2017 CASE 210 PRESENTATION
 SH/EAHP WORKSHOP 2017 CASE 210 PRESENTATION Jonathon H Gralewski DO, MS, Ginell R Post MD, PhD, Youzhong Yuan MD September 9, 2017 Clinical History 60 year old male with history of c-maf high-risk IgG
SH/EAHP WORKSHOP 2017 CASE 210 PRESENTATION Jonathon H Gralewski DO, MS, Ginell R Post MD, PhD, Youzhong Yuan MD September 9, 2017 Clinical History 60 year old male with history of c-maf high-risk IgG
Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party. The European Group for Blood and Marrow Transplantation
 36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
36th EBMT & 9th Data Management Group Annual Meeting Vienna, 23 March 2010 Jordi Esteve Hospital Clínic (Barcelona) Acute Leukemia Working Party The European Group for Blood and Marrow Transplantation
Immunopathology of Lymphoma
 Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Immunopathology of Lymphoma Noraidah Masir MBBCh, M.Med (Pathology), D.Phil. Department of Pathology Faculty of Medicine Universiti Kebangsaan Malaysia Lymphoma classification has been challenging to pathologists.
Introduction: The Revised (4 th Edition) World Health Organization (WHO) Classification of Tumors of Hematopoietic and Lymphoid Tissues
 Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
Society for Hematopathology Scientific Symposium USCAP Companion Meeting, Boston, MA March 8, 2009 Boston, MA Steven H. Swerdlow and James Vardiman, Moderators Introduction: The Revised (4 th Edition)
Cost-Effective Strategies in the Workup of Hematologic Neoplasm. Karl S. Theil, Claudiu V. Cotta Cleveland Clinic
 Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Cost-Effective Strategies in the Workup of Hematologic Neoplasm Karl S. Theil, Claudiu V. Cotta Cleveland Clinic In the past 12 months, we have not had a significant financial interest or other relationship
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia
 Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
Concomitant WT1 mutations predicted poor prognosis in CEBPA double-mutated acute myeloid leukemia Feng-Ming Tien, Hsin-An Hou, Jih-Luh Tang, Yuan-Yeh Kuo, Chien-Yuan Chen, Cheng-Hong Tsai, Ming Yao, Chi-Cheng
New drugs in Acute Leukemia. Cristina Papayannidis, MD, PhD University of Bologna
 New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
Juvenile Myelomonocytic Leukemia (JMML)
 Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Myeloproliferative Disorders - D Savage - 9 Jan 2002
 Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Disease Usual phenotype acute leukemia precursor chronic leukemia low grade lymphoma myeloma differentiated Total WBC > 60 leukemoid reaction acute leukemia Blast Pro Myel Meta Band Seg Lymph 0 0 0 2
Pathology of Hematopoietic and Lymphoid tissue
 Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
Pathology of Hematopoietic and Lymphoid tissue Peerayut Sitthichaiyakul, M.D. Department of Pathology and Forensic Medicine Faculty of Medicine, Naresuan University CONTENTS White blood cells and lymph
74y old Female with chronic elevation of Platelet count. August 18, 2005 Faizi Ali, MD Hematopathology Fellow
 74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
74y old Female with chronic elevation of Platelet count August 18, 2005 Faizi Ali, MD Hematopathology Fellow Clinical History Patient is a 74y old otherwise healthy Caucasian female with no major complaint
Initial Diagnostic Workup of Acute Leukemia
 Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
Initial Diagnostic Workup of Acute Leukemia Guideline from the College of American Pathologists (CAP) and the American Society of Hematology (ASH) Publication: Archives of Pathology and Laboratory Medicine
TEST MENU TEST CPT CODES TAT. Chromosome Analysis Bone Marrow x 2, 88264, x 3, Days
 TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
TEST MENU CANCER/LEUKEMIA CHROMOSOME ANALYSIS Chromosome Analysis Bone Marrow 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome Analysis Bone Marrow Core 88237 x 2, 88264, 88280 x 3, 88291 4 Days Chromosome
Approaching myeloid neoplasms: diagnostic algorithms
 Approaching myeloid neoplasms: diagnostic algorithms Alexandar Tzankov Histopathology Pathology Content Integration of clinical and laboratory data Bone marrow evaluation approaching Myeloproliferative
Approaching myeloid neoplasms: diagnostic algorithms Alexandar Tzankov Histopathology Pathology Content Integration of clinical and laboratory data Bone marrow evaluation approaching Myeloproliferative
Chronic Myelomonocytic Leukemia with molecular abnormalities SH
 Chronic Myelomonocytic Leukemia with molecular abnormalities SH2017-0351 Madhu P. Menon MD,PhD, Juan Gomez MD, Kedar V. Inamdar MD,PhD and Kristin Karner MD Madhu P Menon, MD, PhD Henry Ford Hospital Patient
Chronic Myelomonocytic Leukemia with molecular abnormalities SH2017-0351 Madhu P. Menon MD,PhD, Juan Gomez MD, Kedar V. Inamdar MD,PhD and Kristin Karner MD Madhu P Menon, MD, PhD Henry Ford Hospital Patient
Lymphocytoma Cutis. Cynthia M. Magro MD. Director of Dermatopathology Weill Medical College of Cornell University New York, New York
 Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Lymphocytoma Cutis Cynthia M. Magro MD Professor of Pathology Director of Dermatopathology Weill Medical College of Cornell University New York, New York Lymphocytoma Cutis Falls under other designations
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders
 Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Primary Cutaneous CD30-Positive T-cell Lymphoproliferative Disorders Definition A spectrum of related conditions originating from transformed or activated CD30-positive T-lymphocytes May coexist in individual
Test Name Results Units Bio. Ref. Interval. Positive
 Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
Lab No 135091548 Age 35 Years Gender Female 1/9/2017 120000AM 1/9/2017 103420AM 4/9/2017 23753M Ref By Dr UNKNWON Final Test Results Units Bio Ref Interval LEUKEMIA DIAGNOSTIC COMREHENSIVE ROFILE 3 t (1;19)
Investigation. Li Li 1 Yanan Wang 1 Christine Guo Lian 2 Nina Hu 2 Hongzhong Jin 1 Yuehua Liu 1. DOI:
 Investigation 216 Particular characteristics of atopic eczema in tropical environments. The Tropical Environment... 216 s Clinical and pathological features of myeloid leukemia cutis * Li Li 1 Yanan Wang
Investigation 216 Particular characteristics of atopic eczema in tropical environments. The Tropical Environment... 216 s Clinical and pathological features of myeloid leukemia cutis * Li Li 1 Yanan Wang
Management of Myelodysplastic Syndromes
 Management of Myelodysplastic Syndromes Peter L. Greenberg, MD Stanford Cancer Institute Myelodysplastic Syndromes: Clinical & Molecular Advances for Disease Classification and Prognostication MDSs: A
Management of Myelodysplastic Syndromes Peter L. Greenberg, MD Stanford Cancer Institute Myelodysplastic Syndromes: Clinical & Molecular Advances for Disease Classification and Prognostication MDSs: A
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
CME/SAM. Mixed Phenotype Acute Leukemia
 AJCP / Original Article Mixed Phenotype Acute Leukemia A Study of 61 Cases Using World Health Organization and European Group for the Immunological Classification of Leukaemias Criteria Olga K. Weinberg,
AJCP / Original Article Mixed Phenotype Acute Leukemia A Study of 61 Cases Using World Health Organization and European Group for the Immunological Classification of Leukaemias Criteria Olga K. Weinberg,
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228
 2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
2007 Workshop of Society for Hematopathology & European Association for Hematopathology Indianapolis, IN, USA Case # 228 Vishnu V. B Reddy, MD University of Alabama at Birmingham Birmingham, AL USA 11/03/07
Case Workshop of Society for Hematopathology and European Association for Haematopathology
 Case 24 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Aliyah Rahemtullah 1, Martin K Selig 1, Paola Dal Cin 2 and Robert P Hasserjian 1 Departments of Pathology,
Case 24 2007 Workshop of Society for Hematopathology and European Association for Haematopathology Aliyah Rahemtullah 1, Martin K Selig 1, Paola Dal Cin 2 and Robert P Hasserjian 1 Departments of Pathology,
WHO Update to Myeloproliferative Neoplasms
 WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
WHO Update to Myeloproliferative Neoplasms Archana M Agarwal, MD, Associate Professor of Pathology University of Utah Department of Pathology/ARUP Laboratories Myeloproliferative Neoplasms The categories
Krishna Reddy CH and Ashwin Dalal. Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad
 Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Clinical Cytogenetics in the Diagnosis and Prognosis of Leukemias Krishna Reddy CH and Ashwin Dalal Diagnostics Division, Centre for DNA Fingerprinting and Diagnostics, Hyderabad Email: krishnareddy.chr@gmail.com
Leukemia and subsequent solid tumors among patients with myeloproliferative neoplasms
 Leukemia and subsequent solid tumors among patients with myeloproliferative neoplasms Tiziano Barbui (tbarbui@asst-pg23.it Hematology and Research Foundation,Ospedale Papa Giovanni XXIII, Bergamo Italy
Leukemia and subsequent solid tumors among patients with myeloproliferative neoplasms Tiziano Barbui (tbarbui@asst-pg23.it Hematology and Research Foundation,Ospedale Papa Giovanni XXIII, Bergamo Italy
