Endoscopic Ultrasound With Fine-Needle Aspiration in the Diagnosis and Staging of Lung Cancer
|
|
|
- Silas Hunter
- 5 years ago
- Views:
Transcription
1 Endoscopic Ultrasound With Fine-Needle Aspiration in the Diagnosis and Staging of Lung Cancer Gerard A. Silvestri, MD, Brenda J. Hoffman, MD, Manoop S. Bhutani, MD, Robert H. Hawes, MD, Lynn Coppage, MD, Angela Sanders-Cliette, MD, and Carolyn E. Reed, MD Departments of Surgery, Medicine, Radiology, and Pathology, Medical University of South Carolina, Charleston, South Carolina Background. Esophageal endoscopic ultrasonographic (EUS) guidance for fine-needle aspiration (FNA) of mediastinal lymph nodes has been introduced only recently. The utility of EUS/FNA in diagnosing and staging bronchogenic carcinoma is unknown. Methods. After a thoracic computed tomographic scan, 27 patients with known or suspected lung cancer underwent EUS. Accessible abnormal mediastinal lymph nodes were aspirated under EUS guidance. Patients with positive cytologic studies did not undergo further testing, whereas the remaining patients underwent mediastinal exploration. The sensitivity, specificity, accuracy, positive predictive value, and negative predictive value were calculated for both chest computed tomography and EUS/FNA. Results. Twenty-two of 27 patients had mediastinal adenopathy by computed tomography scan. Sixteen patients had positive findings on EUS, 15 with positive FNA (10 non-small cell lung cancer; 5 small cell lung cancer) and 1 with T4 status. Fourteen patients with positive FNA had lymph nodes sampled at level 5, level 7, or both. Of 11 patients with negative EUS/FNA, 2 had positive findings at operation (sensitivity 89%). The diagnosis of lung cancer was established in 7 patients. Conclusions. The results showed that EUS/FNA improves the accuracy of computed tomographic scan in the staging of lung cancer. By accessing lymph nodes at levels 5 and 7, EUS/FNA complements mediastinoscopy and is considered the staging modality of choice in these regions. Positive EUS/FNA can obviate the need for further invasive staging. (Ann Thorac Surg 1996;61:1441-6) A ccurate determination of the extent of disease (ie, staging) is critical in patients with lung cancer, as it has implications for both prognosis and treatment. When the standard roentgenogram or computed tomographic (CT) scan of the chest reveals enlarged mediastinal lymph nodes, further diagnostic testing is warranted. Mediastinoscopy, mediastinotomy, and thoracoscopy are established invasive procedures used to evaluate enlarged mediastinal lymph nodes. Esophageal endoscopic ultrasonography (EUS) is a new modality that can detect mediastinal lymph nodes adjacent to the esophagus. It is now possible to use EUS to visually guide a fine needle into the lymph nodes and perform aspiration. The utility of this procedure for the diagnosis and staging of bronchogenic carcinoma is unknown. We prospectively evaluated EUS with fineneedle aspiration (FNA) in patients with suspected or documented lung cancer. Presented at the Forty-second Annual Meeting of the Southern Thoracic Surgical Association, San Antonio, TX, Nov 9-11, Address correspondence to Dr Silvestri, Medical University of South Carolina, 171 Ashley Ave, Rm 812-CSB, Charleston, SC Material and Methods Twenty-seven patients with known or suspected lung cancer were considered candidates for this study. All patients provided signed informed consent, and the study was approved by the institutional review board. All patients underwent contrast-enhanced CT of the chest; all chest CT scans were reviewed by one chest radiologist (L.C.). The location of all enlarged lymph nodes (greater than 10 mm in short-axis diameter) was defined using American Thoracic Society criteria [1]. Tumor size and the presence or absence of metastases within the thorax or upper abdomen were also recorded. The radiologist was blinded to the results of EUS/FNA and any other diagnostic procedure performed. Lymph nodes considered accessible by EUS were located in the aortopulmonary window (subaortic lymph nodes lateral to the ligamentum arteriosum; level 5), the subcarinal region (level 7), the right tracheobronchial angle nodes (nodes from the cephalic border of the azygos vein to the origin of the right upper lobe bronchus; 10R), the left tracheobronchial angle nodes (nodes medial to the ligamentum arteriosum; 10L), the paraesophageal nodes (level 8), and the inferior pulmonary ligament lymph nodes (level 9) (Figs 1-3). Lymph nodes located anterior and lateral to the trachea (levels 2, 3, and 4) were considered inaccessible by this approach by The Society of Thoracic Surgeons /96/$15.00 Published by Elsevier Science Inc PII S (95)
2 1442 SILVESTRI ET AL Ann Thorac Surg FINE-NEEDLE ASPIRATION FOR LUNG CANCER 1996;61: Fig 1. Computed tomographic scan illustrates level 5 (aortopulmonary) lymph nodes visualized and sampled by esophageal endoscopic ultrasonography/~ne-needle aspiration. Esophageal endoscopic ultrasonography with FNA was performed in an outpatient endoscopy suite by a qualified gastroenterologist (B.J.H., M.S.B., R.H.H.) skilled in this procedure, after obtaining informed consent. The oropharynx was sprayed with 1% xylocaine, and intravenous sedation (midazolam and meperidine) was administered. After the patient was placed in the left lateral decubitus position, a radial scanning echoendoscope (GIF-UM-20; Olympus America, Lake Success, NY) was introduced and a complete endoscopic ultrasound examination was performed. The radial echoendoscope was withdrawn with fixed images obtained at 1-cm increments at both 7.5- and 12-MHz frequencies. Abnormal mediastinal lymph nodes that could be accessed by EUS/FNA were documented and recorded on videotape. The radial scanning echoendoscope was then removed and a linear-array echoendoscope (FG 32-UA; Pentax, Orangeburg, NY) was inserted (Fig 4). This instrument was placed in the lumen opposite the identified biopsy site, and the balloon was filled with water. Pulsed-wave Fig 3. Enlarged level-5 (aortopulmonary) lymph node CLN) visualized by esophageal endoscopic ultrasonography overlying the left pulmonary aorta. Doppler echocardiography was performed to exclude vascular structures. The FNA needle-catheter system, consisting of a 23- gauge needle attached to a 5F aspiration catheter, with a length of 180 cm (Wilson-Cook, Salem, NC), was inserted through the working channel of the endoscope (see Fig 4). When the tip of the catheter was visualized endoscopically, the needle was advanced from the catheter sheath through the wall of the esophagus and guided into the target lesion using real-time ultrasound (Fig 5). The stylet was removed and suction was applied with a 10-mL syringe while manipulating the needle back and forth within the lymph node. After I to 2 minutes, the suction was released and the needle was retracted. The aspirate was placed on glass slides, preserved with Diff-Quik stain (American Scientific Products, McGraw Park, IL), and reviewed immediately by an on-site pathologist (A.S.C.) to ensure adequate specimens (ie, lymphocytes). At least four adequate samples were obtained Fig 2. Computed tomographic scan illustrates level 7 (subcarinal) lymph nodes, Fig 4. Linear-array echoendoscope with fine needle exiting the biopsy channel.
3 Ann Thorac Surg SILVESTRI ET AL ;61: FINE-NEEDLE ASPIRATION FOR LUNG CANCER Twenty-two patients had enlarged lymph nodes by CT scan. Malignant lymph nodes were confirmed in 16 patients: 15 by EUS/FNA and I by operation. One patient with enlarged lymph nodes had aortic invasion by EUS, and FNA was unnecessary. Five patients with enlarged lymph nodes on CT had a negative EUS and negative operative pathologic studies. Five patients did not have enlarged lymph nodes on CT, but two of these had malignant mediastinal lymph nodes at exploration. The diagnosis of lung cancer was established by EUS in 7 patients, of whom 5 had small cell lung cancer. Ten cases of non-smau cell lung cancer were properly staged by this procedure and were deemed unresectable. The sensitivity, specificity, accuracy, positive predictive value, and negative predictive value of EUS/FNA and chest CT were as follows: 89%, 100%, 100%, 89%, and 82%, and 89%, 38%, 74%, 76%, and 60%, respectively. Fig 5. Needle tip is visualized by esophageal endoscopic ultrasonography penetrating an enlarged lymph node. for each lymph node aspirate unless cytology studies confirmed malignant cells. Patients with cytologic evidence of malignancy did not undergo further testing. All other patients underwent mediastinal exploration to evaluate the lymph nodes. Sensitivity, specificity, accuracy, positive predictive value, and negative predictive value were calculated for both chest CT and EUS/FNA. Results All 27 patients underwent chest CT, of whom 22 had enlarged lymph nodes. The patients then underwent EUS in an outpatient endoscopy suite and were discharged the same day, with no complications. Sixteen patients had positive findings on EUS. One patient had evidence of invasion of the aorta, which was not previously appreciated by CT; this patient did not undergo FNA. Fifteen patients with abnormally enlarged lymph nodes underwent FNA and had malignant cells on cytologic examination, 10 with non-small cell lung cancer and 5 with small cell lung cancer. Lymph nodes accessed by FNA were level 5 (5 patients), level 7 (8 patients), both levels 5 and 7 (1 patient), and level 10R (1 patient). Of the 10 patients with non-small cell lung cancer, 3 had positive contralateral nodes, and their disease was therefore deemed unresectable. Six patients had multiple lymph node levels enlarged on CT scan, and after EUS confirmation of mediastinal involvement, they entered neoadjuvant protocols (2 patients) or were offered nonsurgical therapy (4 patients). One patient sustained a stroke before operation and became medically inoperable. Eleven patients had a negative EUS study or negative FNA and proceeded to operation. Two patients had malignant cells identified at exploration. One patient underwent lobectomy and mediastinal node dissection, and had a microscopic focus of tumor in a level-7 lymph node. The other had positive mediastinoscopy findings (Fig 6). Comment The addition of high-frequency ultrasonic transducers built into the tip of a flexible endoscope has allowed the depiction of lesions in and around the gastrointestinal tract, including adjacent lymph nodes. However, the differentiation between benign and malignant lymph nodes has previously been limited to size, contour, and echo characteristics [2, 3]. Esophageal endoscopic ultrasonography-guided aspiration of various lesions within or outside the gastrointestinal wall became feasible with the development of the linear-array echoendoscope. This instrument is a 60- degree oblique-forward-viewing fiberoptic endoscope with a curved-array ultrasonic transducer mounted in front of the optic lens. A biopsy channel ends close to the optic lens (see Fig 4). A needle can be introduced into the sector-shaped sound field and be visualized both through the optics and on the ultrasonographic image. This study demonstrates that EUS offers a modality to identify and biopsy lymph nodes in regions not easily [EUS pos[ ~ (n=27) [EUS neg[ (n= 16) (n= 11) "'~ Tumor Invasion (1) ]FNA pos] [Surgery ] ~ LN pos (2) LN neg (9) SCLC (5) NSCLC (10) Fig 6. Findings at esophageal endoscopic ultrasonography (EUS) in 27 patients with known or suspected lung cancer. (FNA = fine-needle aspiration; LN = lymph node; NSCLC = non-small cell lung cancer; SCLC - small cell lung cancer.)
4 1444 SILVESTRI ET AL Ann Thorac Surg FINE-NEEDLE ASPIRATION FOR LUNG CANCER 1996;61: accessible by cervical mediastinoscopy (ie, levels 5, 7, 8, and 9). It allows examination of the contralateral mediastinum and hilum. The results of our study confirm that EUS/FNA is feasible and safe. It can be performed in the outpatient setting, with the patient discharged the same day. We evaluated the utility of EUS/FNA in the diagnosis and staging of presumed or known lung cancer. We showed that EUS/FNA is useful in the diagnosis of lung cancer, particularly in patients who have bulky mediastinal adenopathy and a nondiagnostic bronchoscopy study. Five patients in this category had small cell lung cancer. In all, EUS/FNA provided the diagnosis in 7 of the 27 patients (26%). In addition, 10 patients (4,5%) with nonsmall cell lung cancer were deemed to have unresectable disease or to be candidates for a neoadjuvant protocol based on EUS/FNA. This compares favorably with a report by Gress and associates [4], which showed that operation was precluded in 59% of patients by EUS/FNA. We compared this modality to chest CT, the primary noninvasive test for evaluation of mediastinal adenopathy in bronchogenic carcinoma. The accuracy of CT in the identification of mediastinal lymph node metastases is variable, with a sensitivity that ranges from 57% to 95% [5-15]. Accuracy varies by nodal station, with the highest sensitivity in the right paratracheal region (4R) and the lowest in level 7 [2]. Eight percent to 15% of patients without mediastinal lymph node enlargement on CT have mediastinal lymph node metastases found at operative exploration [9, 11, 12]. Greater than 30% of patients with enlarged mediastinal lymph nodes detected by CT do not have metastatic disease when explored [16]. Because decisions regarding operative resectability are based upon the presence or absence of tumor in the mediastinum, CT alone cannot be used to stage the mediastinum, and histologic confirmation of enlarged mediastinal lymph nodes is imperative. The 89% accuracy of EUS/FNA in our study is comparable to that in other reports. Giovannini and colleagues [17] performed 50 lymph node aspirations (24 mediastinal and 26 celiac) with an accuracy of 82%. Gress and associates [4] compared EUS alone versus CT scan versus EUS/FNA in predicting mediastinal lymph node involvement. In 22 patients, EUS/FNA had a 95% accuracy, compared with a 43% accuracy of the CT scan. Our study also demonstrated an unacceptably low accuracy of CT, which supports the need for histologic confirmation of enlarged mediastinal lymph nodes detected by CT. The sensitivity of EUS/FNA was limited by microscopic foci of metastatic disease in normal-appearing lymph nodes. This accounted for one of our false-negative results; probable sampling error accounted for the other. Despite these two false-negative results, the sensitivity of EUS/FNA is similar to that of mediastinoscopy [18]. The utility of EUS/FNA must be compared with that of mediastinoscopy, which is the most frequently used invasive staging tool to evaluate the peritracheal and anterior subcarinal lymph nodes. The accuracy of mediastinoscopy ranges from 89% to 95% [18], with the subcarinal region (level 7) the most commonly missed. The aortopulmonary region (level 5) is not accessible unless extended cervical mediastinoscopy is used [19], and the inferior mediastinum cannot be sampled. Anterior mediastinotomy (Chamberlain procedure) has been used on the left to evaluate lymph nodes in the subaortic and lateral aortic regions. More recently, thoracoscopy has been used to access nodes in the posterior mediastinum as well as the paratracheal, subazygos, and aortopulmonary nodal regions. Subcarinal lymph nodes can be sampled, most easily by a right thoracoscopic approach [20]. Transcarinal needle aspiration (Wang needle) performed through a bronchoscope can also access the subcarinal lymph nodes [21]. Unfortunately, the yield of this procedure is highly variable depending on the technician, and is generally lower than that of either mediastinoscopy or EUS/FNA [22]. An important finding in this study was the accessibility of lymph node stations 5 and 7, which are currently difficult to evaluate by mediastinoscopy. In summary, EUS/FNA is useful in the diagnosis and staging of bronchogenic cancer. This modality improves the accuracy of CT and complements mediastinoscopy by readily accessing lymph nodes at levels 5 and 7 and the inferior mediastinum. We consider EUS/FNA the modality of choice for obtaining cytologic confirmation of malignancy in the aortopulmonary window and the subcarinal region. The technique of EUS/FNA in the mediastinal lymph nodes is feasible and safe and can be performed in the outpatient setting. Lung cancer can be diagnosed by EUS/FNA. Documentation of positive mediastinal lymph nodes by EUS/FNA may obviate further operative staging. References 1. Tisi GM, Friedman PH, Peters RM, et al. American Thoracic Society: clinical staging of primary lung cancer. Am Rev Respir Dis 1983;127: Lee N, Inoue K, Yamamoto R, Kinoshita H. Patterns of internal echoes in lymph nodes in the diagnosis of lung cancer metastasis. World J Surg 1992;16: Kondo D, Imaizumi M, Abe T, Naruke T, Suemasu K. Endoscopic ultrasound examination for mediastinal lymph node metastases of lung cancer. Chest 1990;98: Gress FG, Savides TJ, Kesler K, et al. A prospective comparison study of endoscopic ultrasound (EUS), computed tomography, and EUS directed to fine needle aspiration biopsy of the mediastinum in the preoperative evaluation and staging of non-small cell lung cancer [Abstract]. Gastrnintest Endosc 1995;41: McLoud TC, Bourgouin PM, Greenberg RW, et al. Bronchogenic carcinoma: analysis of staging in the mediastinum with CT by correlative lymph node mapping and sampling. Radiology 1992;182: Daly BDT, Faling LJ, Bite G, et al. Mediastinal lymph node evaluation by computed tomography in lung cancer. J Thorac Cardiovasc Surg 1987;94: Dales RE, Stark RM, Raman S. Computed tomography to stage lung cancer. Approaching a controversy using metaanalysis. Am Rev Respir Dis 1990;141: Aronchick JM. CT of mediastinal lymph nodes in patients with non-small cell lung carcinoma. Radiol Clin North Am 1990;28: Izbicki JR, Thetter O, Karg O, et al. Accuracy of computed tomographic scan and surgical assessment for staging of bronchial carcinoma. J Thorac Cardiovasc Surg 1992;104:
5 Ann Thorac Surg SILVESTRI ET AL ;61: FINE-NEEDLE ASPIRATION FOR LUNG CANCER 10. Staples CA, Muller NL, Miller RR, Evans KG, Nelems B. Mediastinal nodes in bronchogenic carcinoma: comparison between CT and mediastinoscopy. Radiology 1988;167: Richey HM, Matthews JI, Helsel RA, Cable H. Thoracic CT scanning in the staging of bronchogenic carcinoma. Chest 1984;85: Lewis JW, Madrazo BL, Gross SC, et al. The value of radiographic and computed tomography in the staging of lung carcinoma. Ann Thorac Surg 1982;34: Glazer GM. Radiologic staging of lung cancer using CT and MRI. Chest 1989;96:44S-7S. 14. Rea HH, Shevland JE, House AJS. Accuracy of computed tomographic scanning in assessment of the mediastinum in bronchial carcinoma. J Thorac Cardiovasc Surg 1981;81: McKenna RJ, Libshitz HI, Mountain CE, McMurtrey MJ. Roentgenographic evaluation of mediastinal nodes for preoperative assessment in lung cancer. Chest 1985;88: Whittiesey D. Prospective computed tomographic scanning in the staging of bronchogenic cancer. J Thorac Cardiovasc Surg 1988;95: Giovannini M, Seitz JF, Monges G, Perrier H, Rabbia I. Fine-needle aspiration cytology guided by endoscopic ultrasonography: results in 141 patients. Endoscopy 1995;27: Funatsu T, Matsubara Y, Hatakenaka R, Kosaba S, Yasuda Y, Ikeda S. The role of mediastinoscopic biopsy in preoperative assessment of lung cancer. J Thorac Cardiovasc Surg 1992; 104: Ginsberg RJ, Rice TW, Goldberg M, Waters PF, Schomocker BJ. Extended cervical mediastinoscopy. A single procedure for bronchogenic carcinoma of the left upper lobe. J Thorac Cardiovasc Surg 1984;94: Krasna MJ, Mack MJ. Lymph node dissection and staging. In: Krasna MJ, Mack MJ, eds. Arias of thoracoscopic surgery. St. Louis: Quality Medical Publishing, 1994: Shure D, Fedullo PF. The role of transcarinal needle aspiration in the staging of bronchogenic carcinoma. Chest 1984; 86: Harrow EM, Oldenburg FA Jr, Lingenfelter MA, Smith AM Jr. Transbronchial needle aspiration in clinical practice. Chest 1989;96: DISCUSSION DR MARK J. KRASNA (Baltimore, MD): I want to compliment Dr Reed on an excellent presentation and thank her and her coauthors for sending me their manuscript. At the University of Maryland, my pulmonary colleague, Dr Jonathan Orens, has just presented data on 80 patients in a prospective, randomized trial with endobronchial ultrasound and transbronchial needle aspiration. Basically we found that this was a very good way of minimizing the number of passes necessary to get a positive transbronchial needle aspiration, and it also allowed biopsy of lesions that were less than 1 cm in size, as opposed to the usual 1.5 cm by transbronchial needle aspiration. As you know, we have described here and elsewhere the use of thoracoscopy in both lung and esophagus cancer for biopsy of mediastinal lymph nodes. I therefore have two questions. First, it seems that in lung cancer, the primary areas that we are concerned with are the level 2 and 4 paratracheal lymph nodes and, as you mentioned, the subcarinal lymph nodes. These lymph nodes historically have been accessible by cervical mediastinoscopy, and I think you adequately showed that this technique, although useful for some lymph node stations, does in fact miss these paratracheal lymph nodes. I therefore wonder if you could put in perspective for us where this technique will fall in the total armamentarium of operative staging for all lung cancer patients, since you imply in your manuscript that this may be used to allocate patients to protocols. Second, I was surprised to see how easily you were able to access level 5, the aortopulmonary window. The inferior pulmonary ligament lymph node often can be seen away from the ligament and the esophagus and actually closer to the lung. I am therefore curious as to how you are able to traverse the pleural cavity so successfully. Obviously you showed us how you were able to avoid the pulmonary artery, but I wonder if you can comment on the yield for level-5 and level-9 lymph nodes. I do think that this is a very interesting technology, and I will look forward to new advances in this field. I guess that this is going to have more of a role in esophageal cancer staging than in lung cancer staging, where we typically are more concerned about the upper paratracheal and subcarinal lymph nodes. DR REED: I thank Dr Krasna for his comments, and we recognize him as a leader in thoracoscopy. I will start by saying that we believe this technique complements mediastinoscopy. As you know, the paratracheal area is the easiest to access by mediastinoscopy and certainly in a variety of series has a high sensitivity. The least sensitive area for mediastinoscopy is level 7, which is easily accessed by this procedure. We have found that this technique is particularly useful for left upper lobe carcinomas, and many of these patients had left upper lobe lesions. But I hasten to reiterate that we currently believe this technique complements mediastinoscopy. We have accessed level 5 many times with no problem. An important point in the manuscript is that when the echoendoscope is placed, especially for level 5, opposite the esophageal wall, first a pulsed-wave Doppler echocardiographic examination is performed to exclude any vascular structures. I should add that only a few of these patients actually had the inferior mediastinum sampled, and I think it is unusual that we sample or are actually concerned about this area. DR WILLIAM A. COOK (North Andover, MA): As a practitioner in smaller hospitals, I am sure I am not the only one who would be interested in what the costs for this procedure might be. I would also like you to reflect on the presence of positive nodes on both sides of the mediastinum and how you would approach that problem. DR REED: We did not say anything about cost in this report because we did not examine this prospectively. However, I did go back and review some cost data, anticipating that this might be a concern. The mediastinoscopy data are for a patient who is admitted the same day and discharged that evening; as you know, a few patients may actually stay overnight, so I think this is a pretty tight cost here. At our institution, hospital and physician charges are about $4,200, whereas for EUS and FNA, it is about $1,800. So actually there is a cost savings with the EUS/FNA procedure. As to the second question, I should note that EUS allows you to look at the contralateral hilum and mediastinum. Again, it complements the other staging procedures. It has been especially useful in those patients who present with bilateral bulky mediastinal adenopathy without a clear nodule in the lung and who have had a nondiagnostic bronchoscopy. In fact, in our
6 1446 SILVESTRI ET AL Ann Thorac Surg FINE-NEEDLE ASPIRATION FOR LUNG CANCER 1996;61: hands, 5 of those patients turned out to have small cell lung cancer. DR FRANCIS ROBICSEK (Charlotte, NC): I have difficulty appreciating how the value of different diagnostic methods are compared in this very interesting lecture. First of all, you compared EUS with CT scan for diagnostic accuracy. I believe it is more appropriate to compare EUS with CT-scan-dlrected needle biopsy, which has a much higher yield than CT scan alone. As presented, the data do not reflect which technique is better. The second question concerns costs. Again, we are comparing EUS to mediastinoscopy. It is established that CT-scan-directed needle biopsy in many respects is comparable in diagnostic yield to mediastinoscopy. If we want to show the economic advantage of EUS, we should compare its cost to that of CT scan and simultaneous needle biopsy. At our institution, when we send the patient for CT scan, we ask the radiologist, in appro- priate situations, to do the needle biopsy at the same time if he identifies suspicious nodes. Therefore, my question is: How does the diagnostic yield of EUS compare with CT-scan-directed needle biopsy, and how does the cost of the procedure compare when it is done at the same sitting? DR REED: I do not have any information on CT needle biopsy. We do that extremely infrequently at my institution. Our CT people are not anxious to perform biopsy of lymph nodes in the level 5 region, and most of the time my patients come to me with a CT scan already performed, so we cannot decide to do the needle biopsy at that time. I think you have a very good point. We are not necessarily comparing EUS as a staging tool with CT scan. I am just pointing out that the CT scan, which is used often as a staging tool, is inaccurate and that we need to have techniques that confirm positivity or negativity. Notice From the American Board of Thoracic Surgery The American Board of Thoracic Surgery began its recertification process in Diplomates interested in participating in this examination should maintain a documented list of the operations they performed during the year prior to application for recerfification. This practice review should consist of I year's consecutive major operative experiences. (If more than 100 cases occur in I year, only 100 need to be listed.) They should also keep a record of their attendance at approved postgraduate medical education activities for the 2 years prior to application. A minimum of 100 hours of approved CME activity is required. In place of a cognitive examination, candidates for recertification will be required to complete both the general thoracic and cardiac portions of the SESATS VI syllabus (Self-Education/Self-Assessment in Thoracic Surgery). It is not necessary for candidates to purchase SESATS VI booklets prior to applying for recertification. SESATS VI booklets will be forwarded to candidates after their applications have been accepted. Diplomates whose 10-year certificates will expire in 1998 may begin the recertification process in This new certificate will be dated 10 years from the time of expiration of the original certificate. Recertification is also open to any diplomate with an unlimited certificate and will in no way affect the validity of the original certificate. The deadline for submission of applications is May 1, A recertification brochure outlining the rules and requirements for recertification in thoracic surgery is available upon request from the American Board of Thoracic Surgery, One Rotary Center, Suite 803, Evanston, IL
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER
 MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
MEDIASTINAL LYMPH NODE METASTASIS IN PATIENTS WITH CLINICAL STAGE I PERIPHERAL NON-SMALL-CELL LUNG CANCER Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Hideki Akamatsu, MD a Yuzo
Endoscopic Ultrasound-Guided Fine Needle Aspiration for Staging Patients With Carcinoma of the Lung
 Endoscopic Ultrasound-Guided Fine Needle Aspiration for Staging Patients With Carcinoma of the Lung Michael B. Wallace, MD, MPH, Gerard A. Silvestri, MD, MS, Anand V. Sahai, MD, MS (Epid), Robert H. Hawes,
Endoscopic Ultrasound-Guided Fine Needle Aspiration for Staging Patients With Carcinoma of the Lung Michael B. Wallace, MD, MPH, Gerard A. Silvestri, MD, MS, Anand V. Sahai, MD, MS (Epid), Robert H. Hawes,
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
The Itracacies of Staging Patients with Suspected Lung Cancer
 The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C.
 Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Research Grants: Disclosures
Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Research Grants: Disclosures
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
Transbronchial fine needle aspiration
 Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer
 Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Role of EBUS in mediastinal staging of lung cancer. -Dr. Nandakishore Baikunje
 Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
Mediastinoscopy is a common procedure used for the GENERAL THORACIC SURGERY THE CURRENT ROLE OF MEDIASTINOSCOPY IN THE EVALUATION OF THORACIC DISEASE
 GENERAL THORACIC SURGERY THE CURRENT ROLE OF MEDIASTINOSCOPY IN THE EVALUATION OF THORACIC DISEASE Zane T. Hammoud, MD Richard C. Anderson, MD Bryan F. Meyers, MD Tracey J. Guthrie, RN, BSN Charles L.
GENERAL THORACIC SURGERY THE CURRENT ROLE OF MEDIASTINOSCOPY IN THE EVALUATION OF THORACIC DISEASE Zane T. Hammoud, MD Richard C. Anderson, MD Bryan F. Meyers, MD Tracey J. Guthrie, RN, BSN Charles L.
UNDERSTANDING SERIES LUNG CANCER BIOPSIES LungCancerAlliance.org
 UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
Preoperative Evaluation of Lymph Node Metastasis in Esophageal Cancer
 Review Preoperative Evaluation of Lymph Node Metastasis in Esophageal Cancer Yoko Murata, Masaho Ohta, Kazuhiko Hayashi, Hiroko Ide, and Ken Takasaki Lymph node metastasis (LMN) in esophageal cancer occurs
Review Preoperative Evaluation of Lymph Node Metastasis in Esophageal Cancer Yoko Murata, Masaho Ohta, Kazuhiko Hayashi, Hiroko Ide, and Ken Takasaki Lymph node metastasis (LMN) in esophageal cancer occurs
The right middle lobe is the smallest lobe in the lung, and
 ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
ORIGINAL ARTICLE The Impact of Superior Mediastinal Lymph Node Metastases on Prognosis in Non-small Cell Lung Cancer Located in the Right Middle Lobe Yukinori Sakao, MD, PhD,* Sakae Okumura, MD,* Mun Mingyon,
Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis
 CHEST Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis Carlos G. Micames, MD; Douglas C. McCrory, MD; Darren A. Pavey, MD;
CHEST Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis Carlos G. Micames, MD; Douglas C. McCrory, MD; Darren A. Pavey, MD;
Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer
 Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer Ryoichi Nakanishi, MD, Toshihiro Osaki, MD, Kozo Nakanishi, MD, Ichiro Yoshino, MD, Takashi Yoshimatsu,
Treatment Strategy for Patients With Surgically Discovered N2 Stage IIIA Non-Small Cell Lung Cancer Ryoichi Nakanishi, MD, Toshihiro Osaki, MD, Kozo Nakanishi, MD, Ichiro Yoshino, MD, Takashi Yoshimatsu,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
Endoscopic ultrasound-guided needle aspiration in lung cancer
 ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial
 Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial Robert James Cerfolio, MD, FACS, Ayesha S. Bryant, MD, MSPH, Buddhiwardhan Ojha, MD, MPH, and Mohammad Eloubeidi,
Improving the Inaccuracies of Clinical Staging of Patients with NSCLC: A Prospective Trial Robert James Cerfolio, MD, FACS, Ayesha S. Bryant, MD, MSPH, Buddhiwardhan Ojha, MD, MPH, and Mohammad Eloubeidi,
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG
 LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
LYMPH NODE METASTASIS IN SMALL PERIPHERAL ADENOCARCINOMA OF THE LUNG Tsuneyo Takizawa, MD a Masanori Terashima, MD a Teruaki Koike, MD a Takehiro Watanabe, MD a Yuzo Kurita, MD b Akira Yokoyama, MD b Keiichi
Endoscopic Ultrasound and Positron Emission Tomography for Lung Cancer Staging
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:846 851 Endoscopic Ultrasound and Positron Emission Tomography for Lung Cancer Staging MANDEEP S. SAWHNEY,*, ROBERT A. KRATZKE, FRANK A. LEDERLE, AMY M.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:846 851 Endoscopic Ultrasound and Positron Emission Tomography for Lung Cancer Staging MANDEEP S. SAWHNEY,*, ROBERT A. KRATZKE, FRANK A. LEDERLE, AMY M.
Mediastinal Spread of Metastatic Lymph Nodes in Bronchogenic Carcinoma*
 Mediastinal Spread of Metastatic Lymph Nodes in Bronchogenic Carcinoma* Mediastinal Nodal Metastases in Lung Cancer Yoh Watanabe, M.D., F.C.C.P.; ]unzo Shimizu, M.D.; Makoto Tsubota, M.D.; and Takashi
Mediastinal Spread of Metastatic Lymph Nodes in Bronchogenic Carcinoma* Mediastinal Nodal Metastases in Lung Cancer Yoh Watanabe, M.D., F.C.C.P.; ]unzo Shimizu, M.D.; Makoto Tsubota, M.D.; and Takashi
Abhishek Biswas 1, John P. Wynne 2, Divya Patel 1, Michelle Weber 3, Shaleen Thakur 4, P. S. Sriram 1
 Letter to the Editor Comparison of the yield of 19-G excelon core needle to a 21-G EUS needle during endobronchial ultrasound guided transbronchial needle aspiration of mediastinal lymph nodes for the
Letter to the Editor Comparison of the yield of 19-G excelon core needle to a 21-G EUS needle during endobronchial ultrasound guided transbronchial needle aspiration of mediastinal lymph nodes for the
Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis
 ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
ORIGINAL ARTICLES: Superior and Basal Segment Lung Cancers in the Lower Lobe Have Different Lymph Node Metastatic Pathways and Prognosis Shun-ichi Watanabe, MD, Kenji Suzuki, MD, and Hisao Asamura, MD
In 1982 Pearson and colleagues [1] from Toronto published
![In 1982 Pearson and colleagues [1] from Toronto published In 1982 Pearson and colleagues [1] from Toronto published](/thumbs/95/124110746.jpg) Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
Transition From Mediastinoscopy to Endoscopic Ultrasound for Lung Cancer Staging Mark I. Block, MD Division of Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. Esophageal endoscopic
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire. V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique
 Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique 1 Invasive Mediastinal Staging Purpose : to exclude Involvement
Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique 1 Invasive Mediastinal Staging Purpose : to exclude Involvement
Editorial. CT of Mediastinal Lymph Nodes in Lung Cancer: Is There a "State of the Art"? Selection of Patients
 1081 Editorial CT of Mediastinal Lymph Nodes in Lung Cancer: Is There a "State of the Art"? As our technology improves, much of what has been done must be reevaluated. Initial reports of new techniques
1081 Editorial CT of Mediastinal Lymph Nodes in Lung Cancer: Is There a "State of the Art"? As our technology improves, much of what has been done must be reevaluated. Initial reports of new techniques
Corporate Medical Policy Electromagnetic Navigation Bronchoscopy
 Corporate Medical Policy Electromagnetic Navigation Bronchoscopy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: electromagnetic_navigation_bronchoscopy 1/2010 3/2017 3/2018 9/2017
Corporate Medical Policy Electromagnetic Navigation Bronchoscopy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: electromagnetic_navigation_bronchoscopy 1/2010 3/2017 3/2018 9/2017
Case Scenario 1. The patient agreed to a CT guided biopsy of the left upper lobe mass. This was performed and confirmed non-small cell carcinoma.
 Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Case Scenario 1 An 89 year old male patient presented with a progressive cough for approximately six weeks for which he received approximately three rounds of antibiotic therapy without response. A chest
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital
 Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
Non-Small Cell Lung Cancer: Disease Spectrum and Management in a Tertiary Care Hospital Muhammad Rizwan Khan,Sulaiman B. Hasan,Shahid A. Sami ( Department of Surgery, The Aga Khan University Hospital,
May 2017 Imaging Case of the Month. Prasad M. Panse, MD and Michael B. Gotway, MD. Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA
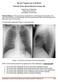 May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
May 2017 Imaging Case of the Month Prasad M. Panse, MD and Michael B. Gotway, MD Department of Radiology Mayo Clinic Arizona Scottsdale, Arizona USA Clinical History: A 32-year-old man presented for routine
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/21364
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/2066/21364
Bronchoscopy and endobronchial ultrasound for diagnosis and staging of lung cancer
 FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
Impact of Radical Systematic Mediastinal Lymphadenectomy on Tumor Staging in Lung Cancer
 Impact of Radical Systematic Mediastinal Lymphadenectomy on Tumor Staging in Lung Cancer Jakob R. Izbicki, MD, Bernward Passlick, MD, Ortrud Karg, MD, Christian Bloechle, MD, Klaus Pantel, MD, Wolfram
Impact of Radical Systematic Mediastinal Lymphadenectomy on Tumor Staging in Lung Cancer Jakob R. Izbicki, MD, Bernward Passlick, MD, Ortrud Karg, MD, Christian Bloechle, MD, Klaus Pantel, MD, Wolfram
Pathologic staging of the mediastinal lymph nodes is
 Mediastinoscopy: Still the Gold Standard Joseph B. Shrager, MD Division of Thoracic Surgery, Department of Cardiothoracic Surgery, Stanford University School of Medicine, Stanford, and Veterans Administration
Mediastinoscopy: Still the Gold Standard Joseph B. Shrager, MD Division of Thoracic Surgery, Department of Cardiothoracic Surgery, Stanford University School of Medicine, Stanford, and Veterans Administration
Exercise 15: CSv2 Data Item Coding Instructions ANSWERS
 Exercise 15: CSv2 Data Item Coding Instructions ANSWERS CS Tumor Size Tumor size is the diameter of the tumor, not the depth or thickness of the tumor. Chest x-ray shows 3.5 cm mass; the pathology report
Exercise 15: CSv2 Data Item Coding Instructions ANSWERS CS Tumor Size Tumor size is the diameter of the tumor, not the depth or thickness of the tumor. Chest x-ray shows 3.5 cm mass; the pathology report
Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping
 GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
GCTAB Column Thoracoscopic left upper lobectomy with systematic lymph nodes dissection under left pulmonary artery clamping Yi-Nan Dong, Nan Sun, Yi Ren, Liang Zhang, Ji-Jia Li, Yong-Yu Liu Department
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases
 Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases Akintayo Sokunbi, M.D MidMichigan Hospital Midland, Michigan Objectives Discuss EBUS guided biopsy principles
Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases Akintayo Sokunbi, M.D MidMichigan Hospital Midland, Michigan Objectives Discuss EBUS guided biopsy principles
Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications
 Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications Poster No.: E-0060 Congress: ESTI 2012 Type: Scientific Exhibit Authors: K. Lee, T. J.
Esophageal Cancer Staging Essentials: The New TNM Staging System (7th edition) and Clinicoradiologic Implications Poster No.: E-0060 Congress: ESTI 2012 Type: Scientific Exhibit Authors: K. Lee, T. J.
Transaortic EUS-guided FNA in the diagnosis of lung tumors and lymph nodes
 CASE STUDIES Transaortic EUS-guided FNA in the diagnosis of lung tumors and lymph nodes Martin B. von Bartheld, BSc, Klaus F. Rabe, MD, PhD, Jouke T. Annema, MD, PhD Leiden, The Netherlands Background:
CASE STUDIES Transaortic EUS-guided FNA in the diagnosis of lung tumors and lymph nodes Martin B. von Bartheld, BSc, Klaus F. Rabe, MD, PhD, Jouke T. Annema, MD, PhD Leiden, The Netherlands Background:
Minimally Invasive Mediastinal Staging of Non Small-Cell Lung Cancer: Emphasis on Ultrasonography-Guided Fine-Needle Aspiration
 Endobronchial ultrasound and endoscopic ultrasound-guided lymph node biopsy may represent an alternative to cervical mediastinoscopy. Dorothy Fox, Rough Seas. Acrylic on canvas, 36ʺ 36ʺ. Minimally Invasive
Endobronchial ultrasound and endoscopic ultrasound-guided lymph node biopsy may represent an alternative to cervical mediastinoscopy. Dorothy Fox, Rough Seas. Acrylic on canvas, 36ʺ 36ʺ. Minimally Invasive
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Collaborative Stage. Site-Specific Instructions - LUNG
 Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Slide 1 Collaborative Stage Site-Specific Instructions - LUNG In this presentation, we are going to review the AJCC Cancer Staging criteria for the lung primary site. Slide 2 Reading Assignments As each
Accurate mediastinal staging is a critical component
 Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Endoscopic Ultrasound Guided Fine Needle Aspiration in the Diagnosis of Mediastinal Masses of Unknown Origin
 THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 10, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(02)04381-2 Endoscopic Ultrasound
THE AMERICAN JOURNAL OF GASTROENTEROLOGY Vol. 97, No. 10, 2002 2002 by Am. Coll. of Gastroenterology ISSN 0002-9270/02/$22.00 Published by Elsevier Science Inc. PII S0002-9270(02)04381-2 Endoscopic Ultrasound
Invasive Mediastinal Staging of Lung Cancer* ACCP Evidence-Based Clinical Practice Guidelines (2nd Edition)
 Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER: ACCP GUIDELINES Invasive Mediastinal Staging of Lung Cancer* ACCP Evidence-Based Clinical Practice Guidelines (2nd Edition) Frank C. Detterbeck, MD,
Supplement DIAGNOSIS AND MANAGEMENT OF LUNG CANCER: ACCP GUIDELINES Invasive Mediastinal Staging of Lung Cancer* ACCP Evidence-Based Clinical Practice Guidelines (2nd Edition) Frank C. Detterbeck, MD,
Skip Metastasis to the Mediastinal Lymph Nodes in Non-Small Cell Lung Cancer
 Skip Metastasis to the Mediastinal Lymph Nodes in Non-Small Cell Lung Cancer Ichiro Yoshino, MD, Hideki Yokoyama, MD, Tokujiro Yano, MD, Takashi Ueda, MD, Eiji Takai, MD, Kazuki Mizutani, MD, Hiroshi Asoh,
Skip Metastasis to the Mediastinal Lymph Nodes in Non-Small Cell Lung Cancer Ichiro Yoshino, MD, Hideki Yokoyama, MD, Tokujiro Yano, MD, Takashi Ueda, MD, Eiji Takai, MD, Kazuki Mizutani, MD, Hiroshi Asoh,
ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM
 ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM This competency-based curriculum has been designed by a task force of interventional pulmonology specialists to underline the learning outcomes
ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM This competency-based curriculum has been designed by a task force of interventional pulmonology specialists to underline the learning outcomes
Endoscopic Ultrasound-Guided Fine-Needle Aspiration in Patients With Non-Small Cell Lung Cancer and Prior Negative Mediastinoscopy
 Endoscopic Ultrasound-Guided Fine-Needle Aspiration in Patients With Non-Small Cell Lung Cancer and Prior Negative Mediastinoscopy Mohamad A. Eloubeidi, MD, MHS, Ashutosh Tamhane, MD, MSPH, Victor K. Chen,
Endoscopic Ultrasound-Guided Fine-Needle Aspiration in Patients With Non-Small Cell Lung Cancer and Prior Negative Mediastinoscopy Mohamad A. Eloubeidi, MD, MHS, Ashutosh Tamhane, MD, MSPH, Victor K. Chen,
Esophageal cancer (EC) is the eighth most common cancer worldwide and the sixth most common cause of cancer-related mortality (Kamangar et al.
 Arch. Biol. Sci., Belgrade, 65 (3), 821-827, 2013 DOI:10.2298/ABS1303821L DETERMINING THE LYMPH NODE CLINICAL TARGET VOLUME OF UPPER ESOPHAGEAL CARCINOMA WITH COMPUTED TOMOGRAPHY MINGHUAN LI 1, YUHUI LIU
Arch. Biol. Sci., Belgrade, 65 (3), 821-827, 2013 DOI:10.2298/ABS1303821L DETERMINING THE LYMPH NODE CLINICAL TARGET VOLUME OF UPPER ESOPHAGEAL CARCINOMA WITH COMPUTED TOMOGRAPHY MINGHUAN LI 1, YUHUI LIU
Original articles. Pathological assessment of mediastinal lymph. nodes in lung cancer: implications for noninvasive mediastinal staging
 Thorax 1992;47:337-341 Original articles 337 Pathology K M Kerr D Lamb Respiratory Medicine C G Wathen N J Douglas Thoracic Surgery W S Walker University of dinburgh, City Hospital and Royal Infirmary,
Thorax 1992;47:337-341 Original articles 337 Pathology K M Kerr D Lamb Respiratory Medicine C G Wathen N J Douglas Thoracic Surgery W S Walker University of dinburgh, City Hospital and Royal Infirmary,
Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy
 Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy Florian Loehe, MD, Sonja Kobinger, MD, Rudolf A. Hatz, MD, Thomas Helmberger, MD, Udo Loehrs, MD, and Heinrich Fuerst,
Value of Systematic Mediastinal Lymph Node Dissection During Pulmonary Metastasectomy Florian Loehe, MD, Sonja Kobinger, MD, Rudolf A. Hatz, MD, Thomas Helmberger, MD, Udo Loehrs, MD, and Heinrich Fuerst,
Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules
 Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
In non small cell lung cancer, metastasis to lymph nodes, the N factor, is
 Okada et al General Thoracic Surgery Border between N1 and N2 stations in lung carcinoma: Lessons from lymph node metastatic patterns of lower lobe tumors Morihito Okada, MD, PhD Toshihiko Sakamoto, MD,
Okada et al General Thoracic Surgery Border between N1 and N2 stations in lung carcinoma: Lessons from lymph node metastatic patterns of lower lobe tumors Morihito Okada, MD, PhD Toshihiko Sakamoto, MD,
Owing to the recent attention given to lung cancer
 Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
A Prospective Study of Indications for Mediastinoscopy in Lung Cancer With CT Findings, Tumor Size, and Tumor Markers
 GENERAL THORACIC A Prospective Study of Indications for Mediastinoscopy in Lung Cancer With CT Findings, Tumor Size, and Tumor Markers Hideki Kimura, MD, PhD, Naomichi Iwai, MD, PhD, Soichiro Ando, MD,
GENERAL THORACIC A Prospective Study of Indications for Mediastinoscopy in Lung Cancer With CT Findings, Tumor Size, and Tumor Markers Hideki Kimura, MD, PhD, Naomichi Iwai, MD, PhD, Soichiro Ando, MD,
VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER
 VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER Christophoros N. Foroulis Associate Professor of Thoracic Surgery Aristotle University of Thessaloniki 1 st International Course on
VIDEO-ASSISTED MEDIASTINOSCOPY FOR MEDIASTINAL STAGING OF LUNG CANCER Christophoros N. Foroulis Associate Professor of Thoracic Surgery Aristotle University of Thessaloniki 1 st International Course on
Significance of Metastatic Disease
 Significance of Metastatic Disease in Subaortic Lymph Nodes G. A. Patterson, M.D., D. Piazza, M.D., F. G. Pearson, M.D., T. R. J. Todd, M.D., R. J. Ginsberg, M.D., M. Goldberg, M.D., P. Waters, M.D., D.
Significance of Metastatic Disease in Subaortic Lymph Nodes G. A. Patterson, M.D., D. Piazza, M.D., F. G. Pearson, M.D., T. R. J. Todd, M.D., R. J. Ginsberg, M.D., M. Goldberg, M.D., P. Waters, M.D., D.
A Standard Endobronchial Ultrasound Image Classification System
 CHEST Original Research INTERVENTIONAL PULMONOLOGY The Utility of Sonographic Features During Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for Lymph Node Staging in Patients With Lung
CHEST Original Research INTERVENTIONAL PULMONOLOGY The Utility of Sonographic Features During Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for Lymph Node Staging in Patients With Lung
Larry Tan, MD Thoracic Surgery, HSC. Community Cancer Care Educational Conference October 27, 2017
 Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
THORACIC MALIGNANCIES
 THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
THORACIC MALIGNANCIES Summary for Malignant Malignancies. Lung Ca 1 Lung Cancer Non-Small Cell Lung Cancer Diagnostic Evaluation for Non-Small Lung Cancer 1. History and Physical examination. 2. CBCDE,
Endoscopic and Endobronchial Ultrasound Staging for Lung Cancer. Michael B. Wallace, MD, MPH Professor of Medicine Mayo Clinic, Jacksonville
 Endoscopic and Endobronchial Ultrasound Staging for Lung Cancer Michael B. Wallace, MD, MPH Professor of Medicine Mayo Clinic, Jacksonville Background: Lung Cancer 170,000 cases/yr in U.S. (# 1 cancer)
Endoscopic and Endobronchial Ultrasound Staging for Lung Cancer Michael B. Wallace, MD, MPH Professor of Medicine Mayo Clinic, Jacksonville Background: Lung Cancer 170,000 cases/yr in U.S. (# 1 cancer)
Lymph node dissection for lung cancer is both an old
 LOBE-SPECIFIC EXTENT OF SYSTEMATIC LYMPH NODE DISSECTION FOR NON SMALL CELL LUNG CARCINOMAS ACCORDING TO A RETROSPECTIVE STUDY OF METASTASIS AND PROGNOSIS Hisao Asamura, MD Haruhiko Nakayama, MD Haruhiko
LOBE-SPECIFIC EXTENT OF SYSTEMATIC LYMPH NODE DISSECTION FOR NON SMALL CELL LUNG CARCINOMAS ACCORDING TO A RETROSPECTIVE STUDY OF METASTASIS AND PROGNOSIS Hisao Asamura, MD Haruhiko Nakayama, MD Haruhiko
Radiological staging of lung cancer. Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh
 Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Radiological staging of lung cancer Shukri Loutfi,MD,FRCR Consultant Thoracic Radiologist KAMC-Riyadh Bronchogenic Carcinoma Accounts for 14% of new cancer diagnoses in 2012. Estimated to kill ~150,000
Mediastinoscopy. EBUS versus Mediastinoscopy?
 Mediastinoscopy M.A. Paul, MD, PhD Dept of Surgery VU University Medical Center Amsterdam Perspectives in Lung Cancer, Amsterdam 9 10 March 2012 1 EBUS versus Mediastinoscopy? I had prepared for a Pro
Mediastinoscopy M.A. Paul, MD, PhD Dept of Surgery VU University Medical Center Amsterdam Perspectives in Lung Cancer, Amsterdam 9 10 March 2012 1 EBUS versus Mediastinoscopy? I had prepared for a Pro
Preoperative Evaluation
 Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Preoperative Evaluation Lateral compartment lymph nodes are easier to detect and are amenable to FNA Central compartment lymph nodes are much more difficult to detect and FNA (Tg washout testing is compromised)
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor
 Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Esophageal seeding after endoscopic ultrasound-guided fine-needle aspiration of a mediastinal tumor Authors Kensuke Yokoyama 1,JunUshio 1,NorikatsuNumao 1, Kiichi Tamada 1, Noriyoshi Fukushima 2, Alan
Innovations in Lung Cancer Diagnosis and Surgical Treatment
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
S promise of long-term survival for patients with nonsmall
 Aggressive Surgical ntervention in N Non-Small Cell Cancer of the Lung Yoh Watanabe, MD, Junzo Shimizu, MD, Makoto Oda, MD, Yoshinobu Hayashi, MD, Shinichiro Watanabe, MD, Yasuhiko Tatsuzawa, MD, Takashi
Aggressive Surgical ntervention in N Non-Small Cell Cancer of the Lung Yoh Watanabe, MD, Junzo Shimizu, MD, Makoto Oda, MD, Yoshinobu Hayashi, MD, Shinichiro Watanabe, MD, Yasuhiko Tatsuzawa, MD, Takashi
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
GROUP 1: Peripheral tumour with normal hilar and mediastinum on staging CT with no disant metastases. Including: Excluding:
 GROUP 1: Including: Excluding: Peripheral tumour with normal hilar and mediastinum on staging CT with no disant metastases Solid pulmonary nodules 8mm diameter / 300mm3 volume and BROCK risk of malignancy
GROUP 1: Including: Excluding: Peripheral tumour with normal hilar and mediastinum on staging CT with no disant metastases Solid pulmonary nodules 8mm diameter / 300mm3 volume and BROCK risk of malignancy
A Guide to Endobronchial and Endoscopic Ultrasound (EBUS and EUS) for Thoracic Radiologists.
 A Guide to Endobronchial and Endoscopic Ultrasound (EBUS and EUS) for Thoracic Radiologists. AP Barker 1, S Karia 1, NR Carroll 1,2, RC Rintoul 2, J Herre 1, EM Godfrey 1, S Ramasundara 1, JL Babar 1 ;
A Guide to Endobronchial and Endoscopic Ultrasound (EBUS and EUS) for Thoracic Radiologists. AP Barker 1, S Karia 1, NR Carroll 1,2, RC Rintoul 2, J Herre 1, EM Godfrey 1, S Ramasundara 1, JL Babar 1 ;
Mediastinal Mysteries: What can be solved with EBUS?
 Mediastinal Mysteries: What can be solved with EBUS? W. Graham Carlos MD Pulmonary & Critical Care Fellow Indiana University School of Medicine Disclosures None Objectives Introduce you to the technique
Mediastinal Mysteries: What can be solved with EBUS? W. Graham Carlos MD Pulmonary & Critical Care Fellow Indiana University School of Medicine Disclosures None Objectives Introduce you to the technique
and Strength of Recommendations
 ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
ASTRO with ASCO Qualifying Statements in Bold Italics s patients with T1-2, N0 non-small cell lung cancer who are medically operable? 1A: Patients with stage I NSCLC should be evaluated by a thoracic surgeon,
Noriaki Kurimoto, MD; Masaki Murayama, MD; Shinkichiro Yoshioka, MD; Takashi Nishisaka, MD; Kouki Inai, MD; and Kiyohiko Dohi, MD
 Assessment of Usefulness of Endobronchial Ultrasonography in Determination of Depth of Tracheobronchial Tumor Invasion* Noriaki Kurimoto, MD; Masaki Murayama, MD; Shinkichiro Yoshioka, MD; Takashi Nishisaka,
Assessment of Usefulness of Endobronchial Ultrasonography in Determination of Depth of Tracheobronchial Tumor Invasion* Noriaki Kurimoto, MD; Masaki Murayama, MD; Shinkichiro Yoshioka, MD; Takashi Nishisaka,
Patients with pathologically diagnosed involved mediastinal
 MINI-SYMPOSIUM ON EMERGING TECHNIQUES FOR LUNG CANCER STAGING European Trends in Preoperative and Intraoperative Nodal Staging: ESTS Guidelines P. De Leyn, MF, PhD,* D. Lardinois, MD, P. Van Schil, MD,
MINI-SYMPOSIUM ON EMERGING TECHNIQUES FOR LUNG CANCER STAGING European Trends in Preoperative and Intraoperative Nodal Staging: ESTS Guidelines P. De Leyn, MF, PhD,* D. Lardinois, MD, P. Van Schil, MD,
Maximum Standard Uptake Value of Mediastinal Lymph Nodes on Integrated FDG-PET-CT Predicts Pathology in Patients with Non-Small Cell Lung Cancer
 Maximum Standard Uptake Value of Mediastinal Lymph odes on Integrated FDG-PET-CT Predicts Pathology in Patients with on-small Cell Lung Cancer Ayesha S. Bryant, MSPH, MD, Robert J. Cerfolio, MD, FACS,
Maximum Standard Uptake Value of Mediastinal Lymph odes on Integrated FDG-PET-CT Predicts Pathology in Patients with on-small Cell Lung Cancer Ayesha S. Bryant, MSPH, MD, Robert J. Cerfolio, MD, FACS,
Predictive risk factors for lymph node metastasis in patients with small size non-small cell lung cancer
 Original Article Predictive risk factors for lymph node metastasis in patients with small size non-small cell lung cancer Feichao Bao, Ping Yuan, Xiaoshuai Yuan, Xiayi Lv, Zhitian Wang, Jian Hu Department
Original Article Predictive risk factors for lymph node metastasis in patients with small size non-small cell lung cancer Feichao Bao, Ping Yuan, Xiaoshuai Yuan, Xiayi Lv, Zhitian Wang, Jian Hu Department
Esophageal Cancer. What is esophageal cancer?
 Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
Scan for mobile link. Esophageal Cancer Esophageal cancer occurs when cancer cells develop in the esophagus. The two main types are squamous cell carcinoma and adenocarcinoma. Esophageal cancer may not
Diagnosis and Preoperative Staging of Esophageal Cancer
 2 Diagnosis and Preoperative Staging of Esophageal Cancer ARNOLD J. MARKOWITZ, MD HANS GERDES, MD The clinical presentation of esophageal cancer in the United States and Europe has been changing, but unfortunately,
2 Diagnosis and Preoperative Staging of Esophageal Cancer ARNOLD J. MARKOWITZ, MD HANS GERDES, MD The clinical presentation of esophageal cancer in the United States and Europe has been changing, but unfortunately,
Parenchyma-sparing lung resections are a potential therapeutic
 Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Lung Segmentectomy for Patients with Peripheral T1 Lesions Bryan A. Whitson, MD, Rafael S. Andrade, MD, and Michael A. Maddaus, MD Parenchyma-sparing lung resections are a potential therapeutic option
Video-Mediastinoscopy Thoracoscopy (VATS)
 Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Cervical Lymph Nodes
 Cervical Lymph Nodes Diana Gaitini, MD Unit of Ultrasound, Department of Medical Imaging Rambam Medical Center and Faculty of Medicine Technion, Israel Institute of Technology Haifa, Israel Learning Targets
Cervical Lymph Nodes Diana Gaitini, MD Unit of Ultrasound, Department of Medical Imaging Rambam Medical Center and Faculty of Medicine Technion, Israel Institute of Technology Haifa, Israel Learning Targets
GUIDELINES FOR CANCER IMAGING Lung Cancer
 GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
GUIDELINES FOR CANCER IMAGING Lung Cancer Greater Manchester and Cheshire Cancer Network Cancer Imaging Cross-Cutting Group April 2010 1 INTRODUCTION This document is intended as a ready reference for
Joseph B. Zwischenberger, MD, FCCP; Clare Savage, MD; Scott K. Alpard, BA; Carryn M. Anderson, BA; Santiago Marroquin, MD; and Brian W.
 Mediastinal Transthoracic Needle and Core Lymph Node Biopsy* Should It Replace Mediastinoscopy? Joseph B. Zwischenberger, MD, FCCP; Clare Savage, MD; Scott K. Alpard, BA; Carryn M. Anderson, BA; Santiago
Mediastinal Transthoracic Needle and Core Lymph Node Biopsy* Should It Replace Mediastinoscopy? Joseph B. Zwischenberger, MD, FCCP; Clare Savage, MD; Scott K. Alpard, BA; Carryn M. Anderson, BA; Santiago
Felix J. F. Herth, MD, FCCP; Ralf Eberhardt, MD; Mark Krasnik, MD; and Armin Ernst, MD, FCCP
 Original Research INTERVENTIONAL PULMONOLOGY Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration of Lymph Nodes in the Radiologically and Positron Emission Tomography-Normal Mediastinum in
Original Research INTERVENTIONAL PULMONOLOGY Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration of Lymph Nodes in the Radiologically and Positron Emission Tomography-Normal Mediastinum in
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions. Alper Toker, MD
 Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery The mediastinum is a complex anatomic
Mediastinoscopy, Mediastinotomy And Thoracoscopy For Mediastinal Lesions Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery The mediastinum is a complex anatomic
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Carcinoma of the Lung
 THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
THE ANNALS OF THORACIC SURGERY Journal of The Society of Thoracic Surgeons and the Southern Thoracic Surgical Association VOLUME 1 I - NUMBER 3 0 MARCH 1971 Carcinoma of the Lung M. L. Dillon, M.D., and
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
International Association for the Study of Lung Cancer lymph node map Lymph node stations Imaging CT
 Review of the International Association for the Study of Lung Cancer Lymph Node Classification System Localization of Lymph Node Stations on CT Imaging Hamza Jawad, MBBS a, Arlene Sirajuddin, MD b, Jonathan
Review of the International Association for the Study of Lung Cancer Lymph Node Classification System Localization of Lymph Node Stations on CT Imaging Hamza Jawad, MBBS a, Arlene Sirajuddin, MD b, Jonathan
SURGICAL TECHNIQUE. Radical treatment for left upper-lobe cancer via complete VATS. Jun Liu, Fei Cui, Shu-Ben Li. Introduction
 SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
SURGICAL TECHNIQUE Radical treatment for left upper-lobe cancer via complete VATS Jun Liu, Fei Cui, Shu-Ben Li The First Affiliated Hospital of Guangzhou Medical College, Guangzhou, China ABSTRACT KEYWORDS
Chapter 8. Other Important Tests and Procedures. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Mediastinoscopy is an exploratory surgical procedure
 Remediastinoscopy After Induction Chemotherapy in Non-Small Cell Lung Cancer Miquel Mateu-Navarro, MD, Ramón Rami-Porta, MD, Romà Bastus-Piulats, MD, Luis Cirera-Nogueras, MD, and Guadalupe González-Pont,
Remediastinoscopy After Induction Chemotherapy in Non-Small Cell Lung Cancer Miquel Mateu-Navarro, MD, Ramón Rami-Porta, MD, Romà Bastus-Piulats, MD, Luis Cirera-Nogueras, MD, and Guadalupe González-Pont,
Lung Surgery: Thoracoscopy
 Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
