Transfusion Reactions. Megan Rowley and Peter Struik
|
|
|
- Arron Wade
- 5 years ago
- Views:
Transcription
1 Transfusion Reactions Megan Rowley and Peter Struik BMS Education Day 28 th January and 4th February 2013 This presentation provides realistic case studies which have been designed with audience participation in mind and should encourage discussion within the group. The cases are NOT designed for individual learning and if used in this way caution is advised. Each case unfolds as time goes on reflecting a true clinical situation and, as a result, there are no clear-cut correct answers until the case is concluded. Discussion of these case studies should use problem-solving skills, be based on effective communication between the laboratory and the clinicians and take into consideration national and local policies on the management and investigation of transfusion reactions. Note: It will be beneficial for staff to read the BCSH guidelines on the investigation and management of acute transfusion reactions and to review the local transfusion reaction policy. Disclaimer: All of these cases reflect a similar case in clinical practice but they have been modified so that the hospital, the staff and the patient are not identifiable. The information given reflects current clinical and laboratory practice but local variations may be in place. Slides 1-7 Introduction to the subject This presentation is for Biomedical Scientists and assumes a basic knowledge of the adverse effects of transfusion. This brief introduction provides an overview of other support and learning materials.
2 Category of Reaction <24 hours from the transfusion = ACUTE >24 hours from the transfusion = DELAYED Infectious Bacterial contamination Viral HIV, Hepatitis, Parvovirus Protozoal Malaria, Syphilis Prion - vcjd Non-infectious Immune Febrile Non-Haemolytic Allergic Acute Haemolytic Reaction -ABO Anaphylactic -anti-iga Transfusion Related Acute Lung Injury Non-immune TACO/TAD Immune Delayed haemolytic reaction Transfusion Associated-GvHD Post Transfusion Purpura Non-immune Iron overload
3 As you participate in this session please; Understand your role in when a patient has an adverse reaction to blood components At the same time try and understand everyone else s role too DOCTOR, NURSE, BIOMEDICAL SCIENTIST, PORTER Never forget the patient who is having the reaction. That s why we are all here.
4 NURSE DOCTOR CARE OF THE PATIENT DURING TRANSFUSION NURSE DOCTOR There are many links in the chain that delivers the right blood to the right patient DOCTOR ORDERING AND PRESCRIBING THE BLOOD, DOCUMENTING THE TRANSFUSION CHECKING THE BLOOD AND STARTING THE TRANSFUSION PORTER NURSE PHLEBOTOMIST NURSE DOCTOR BIOMEDICAL SCIENTIST TAKING A BLOOD SAMPLE FOR COMPATIBILITY TESTING TESTING THE BLOOD GROUP AND CROSSMATCHING THE BLOOD COLLECTING THE BLOOD AND DELIVERING TO THE CLINICAL AREA
5 How do we know, what we know? FIRSTLY: What can go wrong? We have been reporting Serious Hazards Of Transfusion to SHOT since 1996 MHRA have been collecting Serious Adverse Blood Reactions and Events via the SABRE website since 2005 Look at the SHOT definitions and the annual report on the website
6 SECONDLY: What should we do about it? Transfusion Medicine Handbook (for clinicians) Useful flow chart BCSH guidelines (for laboratory and clinicians) Compatibility guidelines Acute transfusion reaction guidelines Look at websites and
7 THIRDLY: Support from NHSBT at hospital.blood.co.uk Contact numbers Guidance Forms
8 Interactive Session Clinical information The orange boxes represent the clinical picture. There are many things going on and transfusion may only be a small part of the picture. Remember, they know more about the patient than you do Learning Points Laboratory information The blue boxes represent the laboratory situation. This is often the only information you have access to when deciding what is going on. Remember, you know more about transfusion practice than they do To take back and use in everyday practice Slide 8 Introduction to the cases This part of the education session was interactive and examples were used to stimulate conversation and group learning. No answer was deemed incorrect but justification was needed for your answer. Notes have been added after the presentation to help with some guidance when delivering this back in the work place and used for learning. Discussion with your lab manager and/or training manager will aid learning. There are learning points throughout the presentation (highlighted in black) containing knowledge that can be applied in daily practice.
9 Monday 9.30 am Transfusion Dept. 30 year old woman with suspected ectopic pregnancy came into the ED at 8.45 Described as in severe pain but stable FBC, coag. screen, G&S already processed by out of hours BMS. Second G&S sample requested, received and tested All 4 core identifiers present on samples; not previously known to your hospital Hb 90g/L, coag. screen normal, A RhD positive Going to theatre in 10 minutes, request for 4 units of blood immediately 1 Slides 9-18 Case study 1
10 Monday 9.30 am Emergency Dept. 30 year old woman with severe left sided abdominal pain arrived 45 mins ago. Positive pregnancy test Scan suggests ectopic with free-fluid +++ Following morphine is pain-free but very drowsy & clammy, hypotensive (80/? mmhg) and fast pulse (120/min) Decided to operate Urgent transfusion needed because of internal bleeding 1
11 Q1 : What blood would you issue? 1 1. Emergency O RhD negative, no XM 2. Group specific, uncrossmatched 3. Group specific, electronic issue 4. None of these, something else 0% 0% 0% 0% Slide 11 Case study 1, question 1 Option 1: (Emergency O RhD negative) Whilst O RhD negative is a safe option, it is appropriate to conserve O RhD negative blood for those patients where an alternative cannot be used. A group and screen on 2 samples was already available and, providing the samples were labelled according to the sample acceptance policy and had been taken from the right patient, group specific blood could have been given. Options 2 and 3: The patient had a second sample taken which was received and tested so the patient should be eligible for electronic issue if this is the laboratory policy and all the other criteria have been met. As the case is an emergency it would not be inappropriate to release group specific uncrossmatched units as 2 samples have been tested. Discussion point: What processes do you have in the laboratory to issue blood in an emergency? What crossmatching techniques are available in your laboratory? What are the criteria for electronic issue? Option 4: If this option was selected there should be discussion as to what the something else is. Be aware that this is a female of childbearing potential so avoiding sensitisation to the D and K antigens should be considered. In an emergency situation the provision of blood should be a priority. It may be beneficial to find out from the clinical team if other blood components are required.
12 Monday 9.45 am Transfusion Dept. You ask do you want to activate the major haemorrhage protocol? Gynae SpR says no, but please issue 4 units of blood as soon as you can and send it straight to theatres You issue 4 units of A RhD positive red cells by electronic issue by 9.55am 1
13 Monday 10 am Gynae. Theatre 1 2 units of blood are given over 10 minutes Surgery starts at 10.05am The ruptured ectopic in the left fallopian tube is removed and bleeding stops 1 litre of blood is drained and surgery is finished by 10.30am In recovery, patient is cold (35 C) and hypotensive. She is on oxygen and warmed iv fluids. She has produced no urine.
14 Monday am Haematology Dept. Repeat FBC and coagulation screen arrive After 30 minutes you phone the results Hb 50g/L, platelets 45 x10 9 /L, PT 20 seconds, APTT 60 seconds, fibrinogen 1.0 g/l She has moved to intensive care and they request 4 more units of blood, 4 FFP and 1 ATD platelets You issue group A blood, platelets and FFP 1
15 Q2 : What is the most likely explanation for these blood results? 1 1. She has DIC because of the ectopic 2. She has dilutional coagulopathy because of all the blood and iv fluids 3. The surgery has not succeeded in stopping the bleeding 4. She has DIC because of an ABO incompatible red cell transfusion 0% 0% 0% 0% Slide 15 Case study 1, question 2 There may be not enough information at this stage to give a full and complete answer and there should be a discussion with regards to which answers were chosen and why. Option 1: Ectopic pregnancy can cause DIC, this option would not explain the drop in Hb. Option 2: We do not have information on what other IV fluids, or the volume, the patient has received. A review of the patient s treatment may help support or exclude this diagnosis. Option 3: This option may explain the drop in Hb in this case. This is a possibility. Option 4: DIC and drop in Hb with no urine production are symptoms of acute haemolytic transfusion reactions. If a patient has had a blood transfusion this may be an option due to sampling/administration/checking errors. However, in this case there were 2 samples grouped for this patient and a two sample policy reduces the risk of WBIT. Discussion points: How confident are staff with the laboratory testing for ABO? What are the signs and symptoms of an ABO transfusion reaction? What additional samples would you request and what tests would you perform?
16 Monday Intensive Care Unit 1 The lab phone to say the blood components are ready The lab is concerned that the blood is haemolysed You have noticed very poor urine output and very dark urine The patient is very sick and deteriorating rapidly You discuss with the haematology SpR and both of you are worried about an acute haemolytic reaction
17 Q3 : The patient is retested and is group O instead of group A. What is the most likely explanation? 1. The transfusion laboratory tested the wrong patient s sample 2. The clinicians bled the wrong patient 3. The transfusion laboratory made a mistake when testing the sample 4. There were probably two patients with a similar name admitted at the same time 1 0% 0% 0% 0% Slide 17 Case study 1, question 3 The options were given to encourage discussion and learning between the group of delegates. Options 1 & 3: This is a possibility, but this would have meant that the same errors occurred twice on 2 different runs, as the laboratory received and tested 2 separate samples for this patient. Discussion points: How confident are you with regards to your laboratory ABO typing? Could there be a possibility a mistake could be made on 2 separate samples? Option 2: Wrong blood in tube (WBIT) has been reported in all Trusts. The new BSCH Guidelines state that 2 samples, taken at 2 separate times, should be tested prior to a transfusion. There has been reports of 2 samples been taken at the same time and one kept and sent later in order to save time and not bleed the patient twice this practice does not reduce the risk of a wrong blood in tube incident. The Department of Health have listed an ABO incompatible transfusion as a never event. Discussion points: Why might the person taking the blood take 2 samples at the same time? Can you think of any safe guards to prevent an ABO incompatible transfusion? Option 4: Failures in the final administration stage have occurred and have been documented in past SHOT reports. It may be that the wrong patient was bled at the time of admission although 2 samples were received in the laboratory. This is a likely source of error but the patient may have had a dedicated team involved in transfusion and communication with the lab as she was bleeding and in urgent need of treatment.
18 ABO-incompatible transfusions 1 The two-sample rule can prevent ABO incompatible transfusions IF the samples are taken at separate times (but you don t always get this in a massive haemorrhage situation) Shift hand-over times are error-prone; incomplete handovers, hurrying and cutting corners In a complex clinical situation ABO incompatibility (or any transfusion reaction) can be missed because the symptoms are attributed to something else If you have any suspicions or clues in the lab there is a WBIT or that wrong blood has been given, always speak out immediately
19 Thursday 9pm, Care of the Elderly Ward 2 Mrs. P is 75 and has had myelodysplasia for the last 18 months, requiring red cell transfusions every 3 weeks and occasionally requires platelets. She is refractory to random platelets as a result of HLA-antibodies She was admitted 2 days ago with a high fever and is now on iv antibiotics for pneumonia The nurse checks todays blood results and contacts the on-call doctor Hb 75 g/l, platelets 23 x10 9 /L, WBC 27 x10 9 /L The doctor reviews the patient, who is quite breathless, and arranges 3 units of blood Slides Case study 2
20 Thursday 10pm, Haematology Dept. 2 The on-call BMS takes a verbal request for 3 units of red cells The patient is O RhD positive and has anti-fy a The last transfusion was 10 days ago 2 units of O+ Fya- blood have already been crossmatched for tomorrow There is also one unit of HLA-matched platelets for her, which expires at midnight tonight
21 Q4 : What is the most important thing to communicate to the doctor caring for Mrs. P tonight? 1. That blood and platelets are available, but give the platelets before midnight 2. That the patient has RBC and HLA antibodies 3. To discuss the case with the haematology team 4. That it is hospital policy to avoid overnight transfusion, unless the patient is unstable 0% 0% 0% 0% Slide 21 Case study 2, question 4 All the options contain information that would be useful for the Dr. Get the group to vote for the option and have a discussion regarding the choices made. Option 1: This is useful information although the patient may have already been reviewed by the haematologist managing the patients care, hence the 2 units already crossmatched for tomorrow. The platelets have not been requested and by telling the Dr that they are expiring at midnight may mean that they decide to give these. Making sure all requests are appropriate should be the key concern. Option 2: The fact that the patient has antibodies may not be something the Dr knows about his patient and is useful information. Option 3: As the patient has MDS and has been treated for if for the last 18 months they will be under the care of the haematology team. Referral to this team to check the treatment plan would be important as there may be a good reason to wait and transfuse the patient in the morning as originally planned. Option 4: Due to reduced number of staffing and patient safety it is not recommended that patients are routinely transfused at night. If a transfusion is not urgent it should be given during routine hours. In this scenario the patient is breathless and therefore may be deemed symptomatic. Discussion point: If unsure of the appropriateness of a request who do you refer to?
22 Friday 2.30am, Care of the Elderly Ward 2 The doctor prescribes the platelets over 30 minutes and each RBC unit over 2 hours, covered with oral furosemide (diuretic) The baseline pre transfusion obs. at 11pm were BP 130/85, pulse 102, temp 37.5 C, resp. rate 28 The platelets were given uneventfully Within 15 minutes of the first RBC unit the patient becomes more breathless BP 140/90, pulse 110, temp 39.2 C resp. rate 32
23 Q5 : You receive a phone call from the nurse on the ward to say Mrs. P is having a transfusion reaction and they have stopped the blood. What would you say? 2 1. Don t call me, there s nothing I can do 2. Get the doctor looking after the patient to assess the reaction and speak to the on-call haematologist for advice 3. Tell the clinical team to document the reaction and send the implicated RBC unit back to the transfusion department 4. None of these, something else 0% 0% 0% 0% Slide 23 Case study 2, question 5 Patient has an increase in temperature, blood pressure and respiratory rate which are signs of a transfusion reaction. Option 1: The transfusion labs are the experts in the transfusion medicine field and are the point of contact and support for the clinical area. If it is felt that dealing with this is not within your knowledge base you should be able to advise them who to contact. Options 2 and 3: These are both considered correct actions. Reference to local policy should be made. Suspected transfusion reactions should always be referred to the haematologist. Discussion points: If you received the implicated unit in the laboratory what tests would you perform? Would a post transfusion sample be requested? Option 4: Discussion should be held as to what other actions would have been done at this point if this was selected by anyone in the group. It may be that this option has been chosen because both option 2 and 3 would have been selected.
24 Friday 9am, Haematology Dept. 2 The haematology SpR reports that Mrs. P is now ventilated on the Intensive Care Unit She has had blood cultures and a change of iv antibiotics but is still pyrexial She had poor renal function before but this is now much worse At 8am her Hb was 60g/L, platelets 55 x10 9 /L, WBC 12x10 9 /L
25 Q6 : What do you think the likely cause of this transfusion reaction? 2 1. Transfusion Associated Circulatory Overload 2. Transfusion Related Acute Lung Injury 3. Haemolytic Transfusion Reaction 4. Anaphylaxis 5. Bacterial contamination the red cells 0% 0% 0% 0% 0% Slide 25 Case Study 2, question 6 Option 1: The patient has had significant changes in observation without a significant fever and is breathless. These are signs of TACO. The weight of the patient has not been given and it is unclear what other fluids the patient has been given. The patient also has poor renal function. Option 2: The patient has had significant changes in observation without a significant fever and is breathless. These are signs of TRALI. With TACO, the central venous pressure (CVP) will be raised and with TRALI the CVP will be normal. Option 3: The patient has anti-fya but the units transfused were Fya negative and crossmatch compatible. Haemolytic transfusion reactions related to non-abo blood group systems do not tend to be immediate. Option 4: Anaphylaxis causes shock/severe hypotension with a wheeze or stridor. This can be caused by transfusion in patients who are IgA deficient. The patient should be treated with adrenaline. Option 5: The temperature rise was less than 2C but the temperature is above 39 C. Bacterial contamination presents with shock/severe hypotension without clinical sign of anaphylaxis or fluid overload. Discussion points: What would be the most likely diagnosis based on the results and clinical picture presented so far? Could more than one diagnosis be possible?
26 Symptoms/signs of an acute transfusion reaction Stop the transfusion and call a doctor Observations and documentation check Febrile nonhaemolytic transfusion reaction ABO incompatibility Bacterial infection of unit TACO Fluid overload Mild fever Bleeding Dark urine High fever Raised CVP Reaction involves mild fever or urticarial rash only No Significant change in observations with collapse/shock? And Significant fever? No Significant breathlessness? Urticaria Swelling Wheeze Normal CVP Mild allergic reaction Severe allergic reaction TRALI
27 Friday 11.15am, Intensive Care Unit 2 Blood cultures taken the night before grow pseudomonas, the same organism that was detected in the sputum on admission Chest X-ray suggests worsening pneumonia with bilateral infiltrates and a large heart She has clinical signs to suggest heart failure and is in positive fluid balance The haematology SpR reviews the patient and suggests a plan of investigation
28 Q7 : Which set of investigations would be the most useful in this case? 2 1. Repeat blood group, crossmatch and antibody screen. Check bilirubin and look at a blood film 2. Send the remains of the RBC unit to NHSBT for culture and ask them to recall any associated units 3. Discuss the case with the TRALI panel 4. Check an IgA level and anti- IgA antibodies 5. None of these, something else 0% 0% 0% 0% 0% Slide 28 Case Study 2, question 7 Discuss all options bearing in mind the following notes, BCSH guidelines and local policy. Option 1: These tests are useful when looking for a serological transfusion reaction. In this case these are not the most useful set of investigations. Option 2: When bacterial contamination is suspected NHSBT should be informed to quarantine other products made form this donor. In this case the patient s blood cultures have shown no additional bacterial growth and the pseudomonas detected is the same as the organism detected on admission. Therefore it is very unlikely that the reason for the patient s deterioration is due to bacterial contamination of the transfusion. Option 3: If a TRALI is suspected the case should be discussed with the TRALI panel at NHSBT. Samples will be requested and tested for neutrophil antibodies. If a TRALI is suspected treatment should not be delayed until the laboratory results are returned. Option 4: IgA deficient patients may have anaphylactic reactions following a transfusion. This patient however has been transfused many time and therefore would have had a reaction previously. Option 5: TACO. This patient has a positive fluid balance and has clinical signs to support cardiac failure. These are symptoms of TACO. The patient also has impaired renal function
29 Respiratory Complications of Transfusion 2 Breathlessness is a feature of most severe acute reactions After resuscitating the patient, there needs to be a clinical review to guide further investigations It is important to focus investigations on the case don t do every test on every case The pattern of symptoms and the time of onset after the start of transfusion is usually more helpful that laboratory investigations Not all breathlessness is transfusion-related!
30 Friday 4pm, Haematology Day Ward 3 21 year old male with very severe aplastic anaemia diagnosed 2 months ago He requires platelets twice a week and RBC transfusion every 2 weeks He continues to attend his university course and intends to finish his degree. The final exams are in 3 weeks He has not had any recent infections There have been no previous transfusion reactions He is about to go home when he starts to feel itchy and shows you a rash over his arms and body Slides Case study 3
31 Q8 : What should the day-ward staff do? 3 1. Arrange for him to have washed platelets next time 2. Take a set of observations and advise him to wait to be reviewed by the doctor 3. Give him antihistamines and then let him drive home if the rash settles 4. Alert the blood service and send the unit of platelet for culture to exclude bacterial contamination 0% 0% 0% 0% Slide 31 Case Study 3, question 8 Option 1: it is possible he could have developed an allergy to the plasma in platelets although this is the first time the patient has had a reaction. Washed platelets should be considered if severe reactions occur on more than one occasion. Option 2: The patient should wait and be reviewed by the doctor before being allowed to go home. Option 3: Antihistamines can be given to deal with the allergy but this causes drowsiness so he should not be allowed to drive home Option 4: Unlikely, but we do not have all the clinical details on the patient. If there had been a significant rise in temperature there may be reason to suggest bacterial contamination.
32 Category Mild Moderate Severe Febrile reaction Temperature rise up to 2 C No other symptoms/signs Temperature rise of 2 C or more Rigors, chills other inflammatory symptoms Temperature rise of 2 C or more plus symptoms that require urgent medical review or prolong hospital stay Allergic reaction Transient flushing, urticaria or rash Wheeze or angiooedema but no significant breathlessness or hypotension Bronchospasm, stridor, angiooedema, circulatory problems. Anaphylaxis Reaction with both allergic and febrile features Features of mild febrile and mild allergic reactions Features of both allergic and febrile reactions One feature in moderate category Features of both allergic and febrile reactions One feature in severe category Hypotensive reaction Isolated fall in BP of 30mm or more No allergic or inflammatory symptoms Shock without allergic or inflammatory symptoms
33 Reaction by Component Type
34 Allergic Reactions 3 Are quite common Sometimes related to a factor in the donor Occur in patients with other allergies Sometimes mild reactions can get worse and patients should be observed for a period of time
35 Learning Points 1. A multi-professional team approach to transfusion reactions produces the best results 2. Patients present with symptoms of their underlying disease as well as those of transfusion reactions It is GOOD when clinical staff consider the possibility of a reaction, so be encouraging! 3. Symptoms and timing of onset are clues to the cause of the reaction Flowcharts are a useful complement knowledge of the type of reactions 4. Mild reactions should be discussed and documented in the notes But do not require extensive investigations
BMS Education Day 28 th January and 4th February 2013
 BMS Education Day 28 th January and 4th February 2013 Category of Reaction 24 hours from the transfusion = DELAYED Infectious Bacterial contamination Viral HIV,
BMS Education Day 28 th January and 4th February 2013 Category of Reaction 24 hours from the transfusion = DELAYED Infectious Bacterial contamination Viral HIV,
Pulmonary complications in the Elderly. Paula Bolton-Maggs Medical Director
 Pulmonary complications in the Elderly Paula Bolton-Maggs Medical Director What does SHOT do? Serious Hazards of Transfusion Collect data on serious adverse reactions and events related to transfusion
Pulmonary complications in the Elderly Paula Bolton-Maggs Medical Director What does SHOT do? Serious Hazards of Transfusion Collect data on serious adverse reactions and events related to transfusion
Transfusion reactions. Jim Taylor Haematology SpR Sheffield
 Transfusion reactions Jim Taylor Haematology SpR Sheffield Pre questions 1. Platelet transfusions are more prone to bacterial contamination compared to red cells. T/F 2. Common causes of an acute transfusion
Transfusion reactions Jim Taylor Haematology SpR Sheffield Pre questions 1. Platelet transfusions are more prone to bacterial contamination compared to red cells. T/F 2. Common causes of an acute transfusion
Have you ever managed patients who have experienced an adverse reaction to transfusion?
 Have you ever managed patients who have experienced an adverse reaction to transfusion? A. Yes, often B. Yes, occasionally C. No A. 1 in 30 units? B. 1 in 100? C. 1 in 1000? D. 1 in 10,000? SHOT collects
Have you ever managed patients who have experienced an adverse reaction to transfusion? A. Yes, often B. Yes, occasionally C. No A. 1 in 30 units? B. 1 in 100? C. 1 in 1000? D. 1 in 10,000? SHOT collects
Definitions of Current SHOT Categories & What to Report
 Definitions of Current SHOT Categories & What to Report Revised March 2011 1 ADVERSE EVENTS TERM DEFINITION WHAT TO REPORT IBCT - Wrong Blood Transfused (Incorrect Blood Component Transfused) Where a patient
Definitions of Current SHOT Categories & What to Report Revised March 2011 1 ADVERSE EVENTS TERM DEFINITION WHAT TO REPORT IBCT - Wrong Blood Transfused (Incorrect Blood Component Transfused) Where a patient
Boot Camp Transfusion Reactions
 Boot Camp Transfusion Reactions Dr. Kristine Roland Regional Medical Lead for Transfusion Medicine, VCH Objectives By the end of this session, you should be able to: Describe in common language the potential
Boot Camp Transfusion Reactions Dr. Kristine Roland Regional Medical Lead for Transfusion Medicine, VCH Objectives By the end of this session, you should be able to: Describe in common language the potential
Transfusion Challenges. - Transfusion Reactions - Do they need platelets? Dr. Eoghan Molloy Haem SpR 2016
 Transfusion Challenges - Transfusion Reactions - Do they need platelets? Dr. Eoghan Molloy Haem SpR 2016 Guidance on Transfusion Hospital transfusion guidelines and procedures Irish Blood Transfusion Service
Transfusion Challenges - Transfusion Reactions - Do they need platelets? Dr. Eoghan Molloy Haem SpR 2016 Guidance on Transfusion Hospital transfusion guidelines and procedures Irish Blood Transfusion Service
Transfusion Reactions. Directed by M-azad March 2012
 Transfusion Reactions Directed by M-azad March 2012 Transfusion Reactions are Adverse reactions associated with the transfusion of blood and its components Transfusion reactions Non-threatening to fatal
Transfusion Reactions Directed by M-azad March 2012 Transfusion Reactions are Adverse reactions associated with the transfusion of blood and its components Transfusion reactions Non-threatening to fatal
Blood is serious business
 Transfusion at RCH BLOOD TRANSFUSION Anthea Greenway Dept of Clinical Haematology >10000 fresh blood products per year Supports craniofacial and cardiac surgery Support bone marrow, liver transplant and
Transfusion at RCH BLOOD TRANSFUSION Anthea Greenway Dept of Clinical Haematology >10000 fresh blood products per year Supports craniofacial and cardiac surgery Support bone marrow, liver transplant and
Blood Transfusion. Dr William Dooley
 Blood Transfusion Dr William Dooley Plan Cases Blood groups / Indications Procedure Monitoring / Reactions Cases For following cases: - Would you give them a blood transfusion? - How many units you would
Blood Transfusion Dr William Dooley Plan Cases Blood groups / Indications Procedure Monitoring / Reactions Cases For following cases: - Would you give them a blood transfusion? - How many units you would
Blood Transfusion. Dr Will Dooley
 Blood Transfusion Dr Will Dooley Plan Cases OSCE practice scenario Blood groups Monitoring / Reactions Miss Irene Bleede, 23yo Asymptomatic, healthy woman with menorrhagia Hb 78 g/l, MCV 73fl Would you
Blood Transfusion Dr Will Dooley Plan Cases OSCE practice scenario Blood groups Monitoring / Reactions Miss Irene Bleede, 23yo Asymptomatic, healthy woman with menorrhagia Hb 78 g/l, MCV 73fl Would you
Mary Berg, M.D. Medical Director, Transfusion Services Associate Professor of Pathology University of Colorado Hospital
 Transfusion Reactions/Complications Mary Berg, M.D. Medical Director, Transfusion Services Associate Professor of Pathology University of Colorado Hospital Acute Transfusion Reactions Can be seen with
Transfusion Reactions/Complications Mary Berg, M.D. Medical Director, Transfusion Services Associate Professor of Pathology University of Colorado Hospital Acute Transfusion Reactions Can be seen with
Haemovigilance: Acute transfusion reactions. Paula Bolton-Maggs Medical Director Serious Hazards of Transfusion
 Haemovigilance: Acute transfusion reactions Paula Bolton-Maggs Medical Director Serious Hazards of Transfusion SHOT Cumulative data: 18 years n=14822 Deaths related to transfusion reported in 2015 Total
Haemovigilance: Acute transfusion reactions Paula Bolton-Maggs Medical Director Serious Hazards of Transfusion SHOT Cumulative data: 18 years n=14822 Deaths related to transfusion reported in 2015 Total
Crossmatching and Issuing Blood Components; Indications and Effects.
 Crossmatching and Issuing Blood Components; Indications and Effects. Alison Muir Blood Transfusion, Blood Sciences, Newcastle Trust Topics Covered Taking the blood sample ABO Group Antibody Screening Compatibility
Crossmatching and Issuing Blood Components; Indications and Effects. Alison Muir Blood Transfusion, Blood Sciences, Newcastle Trust Topics Covered Taking the blood sample ABO Group Antibody Screening Compatibility
Revised November 2012
 Revised November 2012 1 ADVERSE EVENTS IBCT - Wrong Blood Transfused (Incorrect Blood Component Transfused) IBCT- SRNM (Specific Requirements Not Met) Where a patient was transfused with a blood component
Revised November 2012 1 ADVERSE EVENTS IBCT - Wrong Blood Transfused (Incorrect Blood Component Transfused) IBCT- SRNM (Specific Requirements Not Met) Where a patient was transfused with a blood component
INVESTIGATION OF ADVERSE TRANSFUSION REACTIONS TABLE OF RECOMMENDED TESTS. Type of Reaction Presentation Recommended Tests Follow-up Tests
 Minor Allergic (Urticarial) Urticaria, pruritis, flushing, rash If skin reaction only and mild hives/ rash
Minor Allergic (Urticarial) Urticaria, pruritis, flushing, rash If skin reaction only and mild hives/ rash
TRANSFUSION REACTION EVALUATION
 Lab Dept: Test Name: Transfusion Services TRANSFUSION REACTION EVALUATION General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: TRXR Transfusion Complication Workup; Hemolytic reaction
Lab Dept: Test Name: Transfusion Services TRANSFUSION REACTION EVALUATION General Information Lab Order Codes: Synonyms: CPT Codes: Test Includes: TRXR Transfusion Complication Workup; Hemolytic reaction
2/2/2011. Blood Components and Transfusions. Why Blood Transfusion?
 Blood Components and Transfusions Describe blood components Identify nursing responsibilities r/t blood transfusion Discuss factors r/t blood transfusion including blood typing, Rh factor, and cross matching
Blood Components and Transfusions Describe blood components Identify nursing responsibilities r/t blood transfusion Discuss factors r/t blood transfusion including blood typing, Rh factor, and cross matching
Julie Ball SHOT Clinical Incidents Specialist
 Julie Ball SHOT Clinical Incidents Specialist Surveillance procedures from the collection of blood and its components to the follow up of the recipients To collect and assess information on unexpected
Julie Ball SHOT Clinical Incidents Specialist Surveillance procedures from the collection of blood and its components to the follow up of the recipients To collect and assess information on unexpected
Blood/Blood Component Utilization and Administration Annual Compliance Education
 Blood/Blood Component Utilization and Administration Annual Compliance Education This course contains annual compliance education necessary to meet compliance and regulatory requirements. Instructions:
Blood/Blood Component Utilization and Administration Annual Compliance Education This course contains annual compliance education necessary to meet compliance and regulatory requirements. Instructions:
Fifty ways to fail your patient. Haemolytic transfusion reactions
 Fifty ways to fail your patient Haemolytic transfusion reactions Nearly Fifty ways to fail your patient Haemolytic transfusion reactions Acute haemolytic transfusion reaction (AHTR): definition Fever and
Fifty ways to fail your patient Haemolytic transfusion reactions Nearly Fifty ways to fail your patient Haemolytic transfusion reactions Acute haemolytic transfusion reaction (AHTR): definition Fever and
Acute Transfusion Reactions (Allergic, Hypotensive and Severe Febrile) (ATR) n=296 11
 REACTIONS IN PATIENTS: Serious adverse reactions including EU definition ANNUAL SHOT REPORT 2015 Acute Transfusion Reactions (Allergic, Hypotensive and Severe Febrile) (ATR) n=296 11 Authors: Janet Birchall,
REACTIONS IN PATIENTS: Serious adverse reactions including EU definition ANNUAL SHOT REPORT 2015 Acute Transfusion Reactions (Allergic, Hypotensive and Severe Febrile) (ATR) n=296 11 Authors: Janet Birchall,
Essential Transfusion. Medical Students
 Essential Transfusion Medical Students Aim is to ensure that the student has knowledge of an acceptable and safe level for the authorisation of blood and blood components, and the management of a suspected
Essential Transfusion Medical Students Aim is to ensure that the student has knowledge of an acceptable and safe level for the authorisation of blood and blood components, and the management of a suspected
TACO CASE STUDIES RTC JUNE Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner
 TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
TACO CASE STUDIES RTC JUNE 2017 Kerry Dowling Blood Transfusion Laboratory Manager Jonathan Ricks Blood Transfusion Nurse Practitioner RISK FACTORS - TACO Age over 70 years although also seen in younger
Approach to a patient with suspected blood transfusion reaction. Raju Vaddepally, MD
 Approach to a patient with suspected blood transfusion reaction Raju Vaddepally, MD Goals Detection of Acute Transfusion Reactions (ATR) Clinical and Laboratory Evaluation of ATR Management of individual
Approach to a patient with suspected blood transfusion reaction Raju Vaddepally, MD Goals Detection of Acute Transfusion Reactions (ATR) Clinical and Laboratory Evaluation of ATR Management of individual
Methotrexate for inflammatory bowel disease: what you need to know
 Methotrexate for inflammatory bowel disease: what you need to know This leaflet aims to answer your questions about taking methotrexate for inflammatory bowel disease (IBD). If you have any questions or
Methotrexate for inflammatory bowel disease: what you need to know This leaflet aims to answer your questions about taking methotrexate for inflammatory bowel disease (IBD). If you have any questions or
Thinking Twice About Transfusions: When TACOS and TRALIs Turn Treatment Into Tragedy. Megan Boysen Osborn, MD, MHPE
 Thinking Twice About Transfusions: When TACOS and TRALIs Turn Treatment Into Tragedy Megan Boysen Osborn, MD, MHPE Let s TACO bout Transfusion Reactions Megan Boysen Osborn, MD, MHPE Let s TACO bout Transfusion
Thinking Twice About Transfusions: When TACOS and TRALIs Turn Treatment Into Tragedy Megan Boysen Osborn, MD, MHPE Let s TACO bout Transfusion Reactions Megan Boysen Osborn, MD, MHPE Let s TACO bout Transfusion
Red blood cell transfusion
 Red blood cell transfusion This leaflet explains more about red blood cell transfusion, including the benefits, risks and any alternatives and what you can expect when you come to hospital. If you have
Red blood cell transfusion This leaflet explains more about red blood cell transfusion, including the benefits, risks and any alternatives and what you can expect when you come to hospital. If you have
Paula Bolton-Maggs Medical Director SHOT
 Paula Bolton-Maggs Medical Director SHOT Lancet April 30, 1983 The baby was transfused in March 1981 but there was reluctance by reviewers and publishers to publish rapidly NEJM: Confirmed link between
Paula Bolton-Maggs Medical Director SHOT Lancet April 30, 1983 The baby was transfused in March 1981 but there was reluctance by reviewers and publishers to publish rapidly NEJM: Confirmed link between
Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant. Lab Matters study day Oake Manor, Taunton, 8 th July 2015
 Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant Lab Matters study day Oake Manor, Taunton, 8 th July 2015 NPSA Rapid Response Report 2010 Transfusion of blood and blood components
Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant Lab Matters study day Oake Manor, Taunton, 8 th July 2015 NPSA Rapid Response Report 2010 Transfusion of blood and blood components
Non-Medical Authorisation Course
 Non-Medical Authorisation Course November 2017 Authorising, Prescribing & Sampling Janice Smith Matron Transfusion Specialist Aims of this session To discuss and understand: Authorising blood / blood components
Non-Medical Authorisation Course November 2017 Authorising, Prescribing & Sampling Janice Smith Matron Transfusion Specialist Aims of this session To discuss and understand: Authorising blood / blood components
Transfusion Reactions
 Transfusion Reactions From A to T Provincial Blood Coordinating Program Daphne Osborne MN PANC (C) RN We want you to know Definition Appropriate actions Classification Complete case studies Transfusion
Transfusion Reactions From A to T Provincial Blood Coordinating Program Daphne Osborne MN PANC (C) RN We want you to know Definition Appropriate actions Classification Complete case studies Transfusion
BLOOD TRANSFUSION. Dr Lumka Ntabeni
 BLOOD TRANSFUSION Dr Lumka Ntabeni Blood transfusion definition SAFE transfer of BLOOD COMPONENTS from a DONOR to a RECEPIENT CONTENT Brief history of blood transfusion How is safety guaranteed? How do
BLOOD TRANSFUSION Dr Lumka Ntabeni Blood transfusion definition SAFE transfer of BLOOD COMPONENTS from a DONOR to a RECEPIENT CONTENT Brief history of blood transfusion How is safety guaranteed? How do
Newcastle upon Tyne Blood Transfusion Course
 Newcastle upon Tyne Blood Transfusion Course Susan Whitehead Transfusion Practitioner (Recently Retired and loving it) Newcastle Did we need a Course? Came into post May 2000 Back ground General Surgery/Day
Newcastle upon Tyne Blood Transfusion Course Susan Whitehead Transfusion Practitioner (Recently Retired and loving it) Newcastle Did we need a Course? Came into post May 2000 Back ground General Surgery/Day
Transfusion Reactions. Objectives. 1) Identify a transfusion reaction 25/02/16. Dr Matthew Horan. 1) Identify a transfusion reaction
 Transfusion Reactions 25/02/16 Dr Matthew Horan Objectives 1) Identify a transfusion reaction 2) Treat a transfusion reaction 3) Report a transfusion reaction 1) Identify a transfusion reaction Could this
Transfusion Reactions 25/02/16 Dr Matthew Horan Objectives 1) Identify a transfusion reaction 2) Treat a transfusion reaction 3) Report a transfusion reaction 1) Identify a transfusion reaction Could this
Title: Blood Transfusion Laboratory User Handbook
 Title: Blood Transfusion Laboratory User Handbook No.of copies : 1 Location of copies : 1. Web site 2. Contents Introduction 2 High risk specimens 2 Referred work 2 Location of the laboratory 2 Transportation
Title: Blood Transfusion Laboratory User Handbook No.of copies : 1 Location of copies : 1. Web site 2. Contents Introduction 2 High risk specimens 2 Referred work 2 Location of the laboratory 2 Transportation
TRANSFUSION SAFETY 101 ARE YOU SMARTER THAN A BLOOD BANKER?
 TRANSFUSION SAFETY 101 ARE YOU SMARTER THAN A BLOOD BANKER? 1. Fatal blood transfusion reactions are most likely the result of: a. Circulatory overload b. ABO incompatible blood due to patient identification
TRANSFUSION SAFETY 101 ARE YOU SMARTER THAN A BLOOD BANKER? 1. Fatal blood transfusion reactions are most likely the result of: a. Circulatory overload b. ABO incompatible blood due to patient identification
MASSIVE TRANSFUSION DR.K.HITESH KUMAR FINAL YEAR PG DEPT. OF TRANSFUSION MEDICINE
 MASSIVE TRANSFUSION DR.K.HITESH KUMAR FINAL YEAR PG DEPT. OF TRANSFUSION MEDICINE CONTENTS Definition Indications Transfusion trigger Massive transfusion protocol Complications DEFINITION Massive transfusion:
MASSIVE TRANSFUSION DR.K.HITESH KUMAR FINAL YEAR PG DEPT. OF TRANSFUSION MEDICINE CONTENTS Definition Indications Transfusion trigger Massive transfusion protocol Complications DEFINITION Massive transfusion:
Blood Transfusion Reactions
 Blood Transfusion Reactions Introduction Many individuals require blood components and blood products. As per the BC Transfusion Medicine Advisory Group (BCTMAG), a blood component is at therapeutic component
Blood Transfusion Reactions Introduction Many individuals require blood components and blood products. As per the BC Transfusion Medicine Advisory Group (BCTMAG), a blood component is at therapeutic component
Laboratory Empowerment. Debbie Asher Adrian Ebbs Transfusion Laboratory Managers, Eastern Pathology Alliance
 Laboratory Empowerment Debbie Asher Adrian Ebbs Transfusion Laboratory Managers, Eastern Pathology Alliance Why? Electronic ICE requesting was in use for requesting red cells NBTC Indication Codes were
Laboratory Empowerment Debbie Asher Adrian Ebbs Transfusion Laboratory Managers, Eastern Pathology Alliance Why? Electronic ICE requesting was in use for requesting red cells NBTC Indication Codes were
Transfusion Reactions:
 Transfusion Reactions: Melissa R. George, D.O., F.C.A.P. Medical Director, Transfusion Medicine & Apheresis Penn State Milton S. Hershey Medical Center Office: HG069, Phone: 717-531-4627 E-mail: mgeorge5@hmc.psu.edu
Transfusion Reactions: Melissa R. George, D.O., F.C.A.P. Medical Director, Transfusion Medicine & Apheresis Penn State Milton S. Hershey Medical Center Office: HG069, Phone: 717-531-4627 E-mail: mgeorge5@hmc.psu.edu
Transfusion-Related Acute Lung Injury (TRALI) and Strategies for Prevention. Khalid Abdulla Sharif, MD, MRCP (UK)*
 Bahrain Medical Bulletin, Vol. 29, No.4, December 2007 Transfusion-Related Acute Lung Injury (TRALI) and Strategies for Prevention Khalid Abdulla Sharif, MD, MRCP (UK)* Background: Transfusion-Related
Bahrain Medical Bulletin, Vol. 29, No.4, December 2007 Transfusion-Related Acute Lung Injury (TRALI) and Strategies for Prevention Khalid Abdulla Sharif, MD, MRCP (UK)* Background: Transfusion-Related
Blood transfusion. Dr. J. Potgieter Dept. of Haematology NHLS - TAD
 Blood transfusion Dr. J. Potgieter Dept. of Haematology NHLS - TAD General Blood is collected from volunteer donors >90% is separated into individual components and plasma Donors should be: healthy, have
Blood transfusion Dr. J. Potgieter Dept. of Haematology NHLS - TAD General Blood is collected from volunteer donors >90% is separated into individual components and plasma Donors should be: healthy, have
Administration of blood components. Tina Parker - Transfusion Practitioner
 . Administration of blood components Tina Parker - Transfusion Practitioner Red Cells Each unit contains 250-350mls Preserved with glucose and Mannitol to keep the correct tension Lasts 35 days from midnight
. Administration of blood components Tina Parker - Transfusion Practitioner Red Cells Each unit contains 250-350mls Preserved with glucose and Mannitol to keep the correct tension Lasts 35 days from midnight
TRANSFUSION REACTIONS
 14 TRANSFUSION REACTIONS 14.1 INTRODUCTION Transfusion of blood and blood products are reported to cause reactions during or after procedure specially in patients who receive multiple transfusions. These
14 TRANSFUSION REACTIONS 14.1 INTRODUCTION Transfusion of blood and blood products are reported to cause reactions during or after procedure specially in patients who receive multiple transfusions. These
COMPLICATIONS OF BLOOD TRANSFUSIONS. :Prepared by Dr. Nawal Mogales & Dr. Mohammed Aqlan
 COMPLICATIONS OF BLOOD TRANSFUSIONS :Prepared by Dr. Nawal Mogales & Dr. Mohammed Aqlan COMPLICATIONS OF TRANSFUSIONS Transfusion reaction may result from either : A. Immune transfusion reaction. B. Non
COMPLICATIONS OF BLOOD TRANSFUSIONS :Prepared by Dr. Nawal Mogales & Dr. Mohammed Aqlan COMPLICATIONS OF TRANSFUSIONS Transfusion reaction may result from either : A. Immune transfusion reaction. B. Non
WRHA Blood Conservation Service WRHA Transfusion Practice Committee. TEAM TRANSFUSION Differential Diagnosis of Adverse Events
 WRHA Blood Conservation Service WRHA Transfusion Practice Committee TEAM TRANSFUSION Differential Diagnosis of Adverse Events MANITOBA ADVERSE EVENT REPORTING SYSTEM DATA FLOW REACTION Physician orders
WRHA Blood Conservation Service WRHA Transfusion Practice Committee TEAM TRANSFUSION Differential Diagnosis of Adverse Events MANITOBA ADVERSE EVENT REPORTING SYSTEM DATA FLOW REACTION Physician orders
Information for patients with Sickle Cell Disease who may need a blood transfusion. Patient information
 Information for patients with Sickle Cell Disease who may need a blood transfusion Patient information This information leaflet answers some of the questions you may have about having a blood transfusion
Information for patients with Sickle Cell Disease who may need a blood transfusion Patient information This information leaflet answers some of the questions you may have about having a blood transfusion
Chapter 13 ADVERSE TRANSFUSION EVENTS
 Chapter 13 ADVERSE TRANSFUSION EVENTS PRACTICE POINTS The most common severe reaction is ABO incompatibility caused by mis-identification or mis-labelling of the blood component, patient or pre-transfusion
Chapter 13 ADVERSE TRANSFUSION EVENTS PRACTICE POINTS The most common severe reaction is ABO incompatibility caused by mis-identification or mis-labelling of the blood component, patient or pre-transfusion
CrackCast Episode 7 Blood and Blood Components
 CrackCast Episode 7 Blood and Blood Components Episode Overview: 1) Describe the 3 categories of blood antigens 2) Who is the universal donor and why? 3) Define massive transfusion 4) List 5 physiologic
CrackCast Episode 7 Blood and Blood Components Episode Overview: 1) Describe the 3 categories of blood antigens 2) Who is the universal donor and why? 3) Define massive transfusion 4) List 5 physiologic
ERCP. Patient Information
 ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
ERCP What is an ERCP? ERCP stands for endoscopicretrogradecholangiopancreatography. It is a test where an endoscopist looks into the upper part of your gut (the upper gastrointestinal tract) to see if
MASSIVE HAEMORRHAGE POLICY. ABMU HB Transfusion Team
 MASSIVE HAEMORRHAGE POLICY ABMU HB Transfusion Team Objec@ves To define the responsibili@es and roles of the Clinical team and the Haematology Department in the management of MASSIVE HAEMORRHAGE To describe
MASSIVE HAEMORRHAGE POLICY ABMU HB Transfusion Team Objec@ves To define the responsibili@es and roles of the Clinical team and the Haematology Department in the management of MASSIVE HAEMORRHAGE To describe
CAUTION: Refer to the Document Library for the most recent version of this document. Cryoprecipitate Transfusion Guideline for Practice.
 Directorate Department Year Version Number Central Index Number Endorsing Committee Date Endorsed Approval Committee Date Approved Author Name and Job Title Key Words (for search purposes) Date Published
Directorate Department Year Version Number Central Index Number Endorsing Committee Date Endorsed Approval Committee Date Approved Author Name and Job Title Key Words (for search purposes) Date Published
Transfusion 2004: Current Practice Standards. Kay Elliott, MT (ASCP) SBB SWMC Transfusion Service
 Transfusion 2004: Current Practice Standards Kay Elliott, MT (ASCP) SBB SWMC Transfusion Service Massive Transfusion Protocol (MTP) When should it be activated? Massive bleeding i.e. loss of one blood
Transfusion 2004: Current Practice Standards Kay Elliott, MT (ASCP) SBB SWMC Transfusion Service Massive Transfusion Protocol (MTP) When should it be activated? Massive bleeding i.e. loss of one blood
Immunohaematology: a branch of immunology that deals with the immunologic properties of blood.
 1 Immunohaematology: a branch of immunology that deals with the immunologic properties of blood. The red blood cells have on their surface hundreds of antigens and according to the antigen on their surface
1 Immunohaematology: a branch of immunology that deals with the immunologic properties of blood. The red blood cells have on their surface hundreds of antigens and according to the antigen on their surface
Patient Blood Management. Marisa B. Marques, MD UAB Department of Pathology November 17, 2016
 Patient Blood Management Marisa B. Marques, MD UAB Department of Pathology November 17, 2016 Learning Objectives Upon completion of the session, the participant will: 1) Differentiate between the various
Patient Blood Management Marisa B. Marques, MD UAB Department of Pathology November 17, 2016 Learning Objectives Upon completion of the session, the participant will: 1) Differentiate between the various
Major Blood Loss (MBL) Dicing With Death. Tracey McConnell Senior BMS NNUH
 Major Blood Loss (MBL) Dicing With Death Tracey McConnell Senior BMS NNUH MBL Thanks to Katy Veale who first presented Dicing with Death at NEQAS seminar on which this is based MBL Section 1 1. First Contact
Major Blood Loss (MBL) Dicing With Death Tracey McConnell Senior BMS NNUH MBL Thanks to Katy Veale who first presented Dicing with Death at NEQAS seminar on which this is based MBL Section 1 1. First Contact
Lesson 8 STD & Responsible Actions
 Lesson 8 STD & Responsible Actions Overview This lesson reinforces taking care of sexual health by teaching responsible actions around STD prevention. After discussing the responsibilities of a person
Lesson 8 STD & Responsible Actions Overview This lesson reinforces taking care of sexual health by teaching responsible actions around STD prevention. After discussing the responsibilities of a person
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS
 REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
REPORT OF TRANSFUSION ADVERSE REACTION TO BLOOD CENTERS INSTRUCTIONS: Send the form to ALL blood centers that provided blood components to this patient. Timely reporting is important, so that, if appropriate,
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin
 Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Document Information Version: 2 Date: 28 th December 2013 Authors (incl. job title): Professor David Rees (Consultant
Why the Hospital Transfusion laboratory may challenge the use of O D negative blood in an emergency.
 Why the Hospital Transfusion laboratory may challenge the use of O D negative blood in an emergency. Carly Lattimore Blood Bank Team Manager Chesterfield Royal Hospital Why the laboratory may challenge
Why the Hospital Transfusion laboratory may challenge the use of O D negative blood in an emergency. Carly Lattimore Blood Bank Team Manager Chesterfield Royal Hospital Why the laboratory may challenge
REFERENCE LABORATORY. Regular Hours - Monday through Friday 8:00 AM to 4:00 PM. On-Call Staff - Evenings, Nights, Weekend and Holidays.
 I. REFERENCE LABORATORY HOURS OF OPERATION: Regular Hours - Monday through Friday 8:00 AM to 4:00 PM. On-Call Staff - Evenings, Nights, Weekend and Holidays. All Reference Lab procedures are subject to
I. REFERENCE LABORATORY HOURS OF OPERATION: Regular Hours - Monday through Friday 8:00 AM to 4:00 PM. On-Call Staff - Evenings, Nights, Weekend and Holidays. All Reference Lab procedures are subject to
Sepsis in primary care. what is good care?
 Sepsis in primary care @SepsisUK what is good care? Emmanuel Nsutebu Consultant Infectious Disease Physician & Clinical lead for sepsis Tropical and Infectious Disease Unit Royal Liverpool Hospital Do
Sepsis in primary care @SepsisUK what is good care? Emmanuel Nsutebu Consultant Infectious Disease Physician & Clinical lead for sepsis Tropical and Infectious Disease Unit Royal Liverpool Hospital Do
Components of Blood. N26 Blood Administration 4/24/2012. Cabrillo College ADN/C. Madsen RN, MSN 1. Formed elements Cells. Plasma. What can we give?
 Components of Blood Formed elements Cells Erythrocytes (RBCs) Leukocytes (WBCs) Thrombocytes (platelets) Plasma 90% water 10% solutes Proteins, clotting factors 1 What can we give? Whole blood Packed RBC
Components of Blood Formed elements Cells Erythrocytes (RBCs) Leukocytes (WBCs) Thrombocytes (platelets) Plasma 90% water 10% solutes Proteins, clotting factors 1 What can we give? Whole blood Packed RBC
Pathology Service User Guide Haematology
 Pathology Service User Guide Haematology St Richard s This section of the Pathology Service User Guide includes: Anticoagulant Therapy Information about the Anticoagulant Clinic Low Molecular Weight Heparin
Pathology Service User Guide Haematology St Richard s This section of the Pathology Service User Guide includes: Anticoagulant Therapy Information about the Anticoagulant Clinic Low Molecular Weight Heparin
Having a kidney biopsy. Information for patients Sheffield Kidney Institute (Renal Unit)
 Having a kidney biopsy Information for patients Sheffield Kidney Institute (Renal Unit) This leaflet is designed to answer any questions you may have about having a biopsy of your kidney. We hope that
Having a kidney biopsy Information for patients Sheffield Kidney Institute (Renal Unit) This leaflet is designed to answer any questions you may have about having a biopsy of your kidney. We hope that
Significance of Antibodies and appropriate selection of red cells for transfusion Chris Elliott Haematology Service manager
 Significance of Antibodies and appropriate selection of red cells for transfusion Chris Elliott Haematology Service manager James Cook University Hospital Friarage Hospital Over the next 30 minutes Bit
Significance of Antibodies and appropriate selection of red cells for transfusion Chris Elliott Haematology Service manager James Cook University Hospital Friarage Hospital Over the next 30 minutes Bit
For more information about how to cite these materials visit
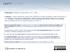 Author(s): Robertson Davenport, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Author(s): Robertson Davenport, M.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Noncommercial Share Alike 3.0 License: http://creativecommons.org/licenses/by-nc-sa/3.0/
Unit 5: Blood Transfusion
 Unit 5: Blood Transfusion Blood transfusion (BT) therapy: Involves transfusing whole blood or blood components (specific portion or fraction of blood lacking in patient). Learn the concepts behind blood
Unit 5: Blood Transfusion Blood transfusion (BT) therapy: Involves transfusing whole blood or blood components (specific portion or fraction of blood lacking in patient). Learn the concepts behind blood
Transfusion reactions illustrated
 Transfusion reactions illustrated Chapter 1 Transfusion practice 1 Procedure of transfusion practice In general, transfusion-associated incidents occur due to multiple errors, most of which occur in the
Transfusion reactions illustrated Chapter 1 Transfusion practice 1 Procedure of transfusion practice In general, transfusion-associated incidents occur due to multiple errors, most of which occur in the
Transfusion Pitfalls. Objectives. Packed Red Blood Cells. TRICC trial (subgroups): Is transfusion always good? Components
 Objectives Transfusion Pitfalls Gregory W. Hendey, MD, FACEP Professor and Chief UCSF Fresno, Emergency Medicine To list risks and benefits of various blood products To discuss controversy over liberal
Objectives Transfusion Pitfalls Gregory W. Hendey, MD, FACEP Professor and Chief UCSF Fresno, Emergency Medicine To list risks and benefits of various blood products To discuss controversy over liberal
PACKAGE LEAFLET: INFORMATION FOR THE USER. octaplaslg mg/ml solution for infusion Human plasma proteins
 PACKAGE LEAFLET: INFORMATION FOR THE USER octaplaslg 45-70 mg/ml solution for infusion Human plasma proteins Read all of this leaflet carefully before you start using this medicine. - Keep this leaflet.
PACKAGE LEAFLET: INFORMATION FOR THE USER octaplaslg 45-70 mg/ml solution for infusion Human plasma proteins Read all of this leaflet carefully before you start using this medicine. - Keep this leaflet.
Your Chemotherapy. The Common side effects are:
 1 10 This information leaflet is designed to help you understand more about the treatment you have opted to undertake. You will be receiving both chemotherapy and radiotherapy that work together to treat
1 10 This information leaflet is designed to help you understand more about the treatment you have opted to undertake. You will be receiving both chemotherapy and radiotherapy that work together to treat
Plasma exchange. Information for patients Sheffield Kidney Institute (Renal Unit)
 Plasma exchange Information for patients Sheffield Kidney Institute (Renal Unit) Plasma exchange This leaflet explains about plasma exchange; the benefits, risks, alternatives and what you can expect when
Plasma exchange Information for patients Sheffield Kidney Institute (Renal Unit) Plasma exchange This leaflet explains about plasma exchange; the benefits, risks, alternatives and what you can expect when
Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant
 Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant All medical RCC transfusions (but only 1 in 3 haematology or oncology cases) in 3 x one week periods Medical specialties include:
Alister Jones Patient Blood Management Practitioner NHS Blood and Transplant All medical RCC transfusions (but only 1 in 3 haematology or oncology cases) in 3 x one week periods Medical specialties include:
All institutions that transfuse blood components and products should implement national and local policies and written procedures for:
 5.0 GENERAL GUIDE TO GOOD TRANSFUSION PRACTICE Blood and the various components prepared or manufactured from it are biologic (in the case of blood cells, living human tissues) products intended for use
5.0 GENERAL GUIDE TO GOOD TRANSFUSION PRACTICE Blood and the various components prepared or manufactured from it are biologic (in the case of blood cells, living human tissues) products intended for use
An Audit of Emergency Group O blood use in Royal Devon and Exeter Hospital
 An Audit of Emergency Group O blood use in Royal Devon and Exeter Hospital Jack Cunningham Keira Soanes Why are we looking at our use of Emergency Group O RhD negative blood? Following the NHSBT National
An Audit of Emergency Group O blood use in Royal Devon and Exeter Hospital Jack Cunningham Keira Soanes Why are we looking at our use of Emergency Group O RhD negative blood? Following the NHSBT National
Case Study: Biomedical Scientist - Caroline
 Case Study: Biomedical Scientist - Caroline What do you do? I'm a biomedical scientist, in haematology. I work in an NHS hospital. We study the morphology of the cells - what they actually look like, such
Case Study: Biomedical Scientist - Caroline What do you do? I'm a biomedical scientist, in haematology. I work in an NHS hospital. We study the morphology of the cells - what they actually look like, such
Specific Requirements
 Specific Requirements AIMS Specific requirements your patients have for transfusion and how this is managed Classify which patients require: Irradiated components CMV negative components Washed components
Specific Requirements AIMS Specific requirements your patients have for transfusion and how this is managed Classify which patients require: Irradiated components CMV negative components Washed components
Plasma-derived products Information for patients
 Plasma-derived products Information for patients page 2 You have been given this leaflet as your doctor has advised you that you may require plasma-derived products as a treatment for your bleeding disorder.
Plasma-derived products Information for patients page 2 You have been given this leaflet as your doctor has advised you that you may require plasma-derived products as a treatment for your bleeding disorder.
Hi doctor, can you come and see my patient, she s just had a coffee ground vomit. Dr Rhona Hurley, FY2
 Hi doctor, can you come and see my patient, she s just had a coffee ground vomit. Dr Rhona Hurley, FY2 Ask for more information What now? o What might you ask? o Do you have enough information about this
Hi doctor, can you come and see my patient, she s just had a coffee ground vomit. Dr Rhona Hurley, FY2 Ask for more information What now? o What might you ask? o Do you have enough information about this
Sofosbuvir, Pegylated Interferon and Ribavirin for the Treatment of Hepatitis C
 Sofosbuvir, Pegylated Interferon and Ribavirin for the Treatment of Hepatitis C Department of Hepatology Digestive Diseases Centre Patient Information This leaflet is designed to give you important information
Sofosbuvir, Pegylated Interferon and Ribavirin for the Treatment of Hepatitis C Department of Hepatology Digestive Diseases Centre Patient Information This leaflet is designed to give you important information
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin
 Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Version: 6 Date: 2 nd March 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/
Guidelines on the Management of a Child with Sickle Cell Disease and low Haemoglobin Version: 6 Date: 2 nd March 2010 Authors: Responsible committee or Director: Review date: Target audience: Stakeholders/
Significance of Antibodies and appropriate selection of red cells for transfusion. Divis ion of Pat hology
 Significance of Antibodies and appropriate selection of red cells for transfusion Bit of basic immunology Serological red cell transfusion reactions Testing and sample timing Problems Coping strategies
Significance of Antibodies and appropriate selection of red cells for transfusion Bit of basic immunology Serological red cell transfusion reactions Testing and sample timing Problems Coping strategies
CAUTION: You must refer to the intranet for the most recent version of this procedural document.
 Procedure for the use of Intravenous Iron Dextran (CosmoFer ) Sharepoint Location Sharepoint Index Directory Clinical Policies and Guidelines General Policies and Guidelines/ Haematology And blood transfusion
Procedure for the use of Intravenous Iron Dextran (CosmoFer ) Sharepoint Location Sharepoint Index Directory Clinical Policies and Guidelines General Policies and Guidelines/ Haematology And blood transfusion
A Patient s Guide to Blood Components and Products
 2014 A Patient s Guide to Blood Components and Products Contents What is a blood transfusion?... 1 Informed consent... 1 Frequently asked questions about blood transfusions... 2 What can I expect during
2014 A Patient s Guide to Blood Components and Products Contents What is a blood transfusion?... 1 Informed consent... 1 Frequently asked questions about blood transfusions... 2 What can I expect during
CT Guided Lung Biopsy. A guide for patients undergoing biopsy
 CT Guided Lung Biopsy A guide for patients undergoing biopsy Introduction The aim of this booklet is to: Answer your questions about CT guided lung biopsy Explain why you need the test Describe what is
CT Guided Lung Biopsy A guide for patients undergoing biopsy Introduction The aim of this booklet is to: Answer your questions about CT guided lung biopsy Explain why you need the test Describe what is
Respiratory Patient Information Leaflet
 Bronchiectasis Self- Management Plan Respiratory Patient Information Leaflet Your Bronchiectasis Management Plan This plan is designed to help you manage your day to day symptoms and assist you in noticing
Bronchiectasis Self- Management Plan Respiratory Patient Information Leaflet Your Bronchiectasis Management Plan This plan is designed to help you manage your day to day symptoms and assist you in noticing
Transfusion Medicine Potpourri. BUMC - Phoenix Internal Medicine Residents September 29, 2015
 Transfusion Medicine Potpourri BUMC - Phoenix Internal Medicine Residents September 29, 2015 Clinical case A 24 year old female with sickle cell anemia has just moved to the area and presents as a new
Transfusion Medicine Potpourri BUMC - Phoenix Internal Medicine Residents September 29, 2015 Clinical case A 24 year old female with sickle cell anemia has just moved to the area and presents as a new
Transarterial Chemoembolization (TACE)
 Transarterial Chemoembolization (TACE) Princess Margaret Know what to expect Read this booklet to learn: What TACE is...1 How TACE works...2 The benefits of TACE...3 The risks and side effects of TACE...3
Transarterial Chemoembolization (TACE) Princess Margaret Know what to expect Read this booklet to learn: What TACE is...1 How TACE works...2 The benefits of TACE...3 The risks and side effects of TACE...3
Learning Objectives: At the end of this exercise, the student will be able to:
 Applications in Transfusion Medicine- A CBL Exercise- Student Guide 1 Title: Applications in Transfusion Medicine A CBL Exercise Purpose: At the conclusion of this exercise, students will be able to apply
Applications in Transfusion Medicine- A CBL Exercise- Student Guide 1 Title: Applications in Transfusion Medicine A CBL Exercise Purpose: At the conclusion of this exercise, students will be able to apply
Reference Guide for Group Education
 A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
A p l a n o f a c t i o n f o r l i f e Reference Guide for Group Education Session 5 Plan of Action: Part I Overview of the Plan of Action and Management of Respiratory Infections Plan of Action: Objectives
Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway
 Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway Dr Alex Williams, Oncology Specialty Doctor. Cheltenham General Hospital Oncology Centre
Reducing the Door to Needle Time for Antibiotics in Suspected Neutropenic Sepsis using a Dedicated Clinical Pathway Dr Alex Williams, Oncology Specialty Doctor. Cheltenham General Hospital Oncology Centre
Flexible Sigmoidoscopy Patient Information
 Flexible Sigmoidoscopy Patient Information Introduction Your doctor has recommended that you have a flexible sigmoidoscopy. However, it is your decision whether or not to go ahead with the test. This leaflet
Flexible Sigmoidoscopy Patient Information Introduction Your doctor has recommended that you have a flexible sigmoidoscopy. However, it is your decision whether or not to go ahead with the test. This leaflet
Sepsis. Patient Information
 Sepsis Patient Information This leaflet aims to answer your questions about what the Sepsis is. It will explain the signs and symptoms of sepsis, treatment of sepsis and information about what Brighton
Sepsis Patient Information This leaflet aims to answer your questions about what the Sepsis is. It will explain the signs and symptoms of sepsis, treatment of sepsis and information about what Brighton
A Patient s guide to. Blood Transfusions and Human Tissue Transplant
 A Patient s guide to Blood Transfusions and Human Tissue Transplant Why might I need a blood transfusion? Blood transfusions are given to replace blood lost in surgery or to treat anaemia (lack of red
A Patient s guide to Blood Transfusions and Human Tissue Transplant Why might I need a blood transfusion? Blood transfusions are given to replace blood lost in surgery or to treat anaemia (lack of red
Significance of Antibodies and appropriate selection of red cells for transfusion
 Significance of Antibodies and appropriate selection of red cells for transfusion James Cook University Hospital Friarage Hospital Bit of basic immunology Serological red cell transfusion reactions Testing
Significance of Antibodies and appropriate selection of red cells for transfusion James Cook University Hospital Friarage Hospital Bit of basic immunology Serological red cell transfusion reactions Testing
Chapter 17: Transfusion-Transmitted Infections (TTI)
 Annual SHOT Report 2014 Supplementary Information Chapter 17: Transfusion-Transmitted s (TTI) The table below is an excerpt from the full Table 17.2 which can be viewed in the main report. Case reports
Annual SHOT Report 2014 Supplementary Information Chapter 17: Transfusion-Transmitted s (TTI) The table below is an excerpt from the full Table 17.2 which can be viewed in the main report. Case reports
Policy for the Treatment of Anaphylaxis in Adults and Children
 Policy for the Treatment of Anaphylaxis in Adults and Children June 2008 Policy Title: Policy for the Treatment of Anaphylaxis in Adults or Children Policy Reference Number: PrimCare08/17 Implementation
Policy for the Treatment of Anaphylaxis in Adults and Children June 2008 Policy Title: Policy for the Treatment of Anaphylaxis in Adults or Children Policy Reference Number: PrimCare08/17 Implementation
