EUROANESTHESIA 2005 PHYSIOLOGICAL ASPECTS OF CENTRAL BLOCKADE MECHANISMS OF SPINAL AND EPIDURAL ANAESTHESIA DIFFERENTIAL BLOCKADE
|
|
|
- Morgan Poole
- 5 years ago
- Views:
Transcription
1 PHYSIOLOGICAL ASPECTS OF CENTRAL BLOCKADE EUROANESTHESIA 2005 Vienna, Austria May RC1 BERNADETTE VEERING Department of Anaesthesiology Leiden University Medical Center Leiden, The Netherlands Saturday May 28, :00-13:45 Room F2 The physiological responses to spinal and epidural anaesthesia have much in common. These responses are mostly due to the fact that the local anaesthetic solution blocks not only somatic, sensory and motor fibres, but also produces pre-ganglionic sympathetic blockade. Postganglionic sympathetic nerves play a role in controlling gastrointestinal tone and motility, cardiac function and vascular tone thereby regulating regional blood flow. Blockade of sympathetic nerve fibres and resulting loss of vasomotor tone causes changes in blood flow to various organs depending on the level of block achieved. The parasympathetic nervous system is also important in regulating cardiovascular and gastrointestinal function. This lecture will focus on comparison of the physiological responses to spinal and epidural anaesthesia. MECHANISMS OF SPINAL AND EPIDURAL ANAESTHESIA SPINAL ANAESTHESIA The primary site of action of local anaesthetics injected into the subarachnoid space is on the spinal rootlets and in the case of afferent sensory fibres, on the dorsal root ganglia. The nerve roots leaving the spinal cord are not covered by epineurium and are readily exposed to local anaesthetics in the cerebrospinal fluid (CSF) [1]. This radicular blockade produces the well known segmental block pattern. EPIDURAL ANAESTHESIA In the epidural space possible sites of action include the spinal nerve trunks in the paravertebral space, the dorsal root ganglia, the dorsal and ventral spinal roots and the spinal cord itself [2]. In the epidural space the myelinated nerve sheath acts as a barrier to local anaesthetic diffusion, as do the meninges. DIFFERENTIAL BLOCKADE Differential sensitivities of nerves to local anaesthetics result in clinically important zones of differential blockade involving somatic motor fibres, somatic sensory fibres and pre-ganglionic sympathetic fibres [3-5]. The sequence of block varies according to the blocking agent, the size of nerve fibre axons, the frequency of nerve impulse transmission and the length of nerve fibre exposed to the local anaesthetic. Fink [4] suggested that fibre size is not as important as the length of exposed nerve fibre, i.e. the number of nodes (three consecutively) exposed. Measurements in isolated nerve fibres and anatomical considerations may explain the persistence of differential block after epidural and subarachnoid injection. According to this theory there may be differences in block following each technique. SPINAL ANAESTHESIA It has been assumed that sympathetic blockade extends two dermatomes beyond somatic blockade. However, discrepancies exist between studies and it has been shown that sympathetic block after spinal anaesthesia may extend up to six dermatomes beyond the sensory block [5]. Different techniques of indirectly measuring sympathetic function (infrared thermography, flowmetry, skin conductance responses) display wide discrepancies after spinal anaesthesia. The concentration of local anaesthetic in the CSF decreases as a function of the distance from the site of injection, and preganglionic nervous system fibres are anaesthetized by concentrations of local anaesthetics that are inadequate to affect sensory or motor fibres [1,5]. EPIDURAL ANAESTHESIA The sensitivity of various nerve fibres to local anaesthetics is related to the size and type of the nerve fibre, the mass of local anaesthetic administered epidurally and the physicochemical properties of the local anaesthetic agent. With epidural anaesthesia there are zones of differential sensory blockade between pinprick and cold discrimination, with an increasing difference between levels of anaesthesia and analgesia in the cephalad direction.[3] 23
2 SYMPATHETIC DENERVATION The sympathectomy that accompanies spinal and epidural anaesthesia is dependent upon height of block. As all sympathetic nerves derive from T1 through to L2, a block into the midthoracic region causes a considerable decrease in sympathetic activity, particularly in vasomotor control of the lower part of the body. It is unknown whether the efferent pre-ganglionic sympathetic nerves are distributed segmentally. Current methods do not show a clearly discernible boundary between blocked and unblocked segments and so the sympathetic block may appear patchy. Despite high levels of epidural blockade (above T5) weak galvanic skin responses to arousal could still be elicited in the foot, indicating incomplete sympathetic blockade.[6] Even with subarachnoid local anaesthetic block to T5 sympathetic block in the foot was still incomplete.[7 ] When comparing the physiological effects of spinal and epidural anaesthesia it is relevant to ask if spinal anaesthesia does result in a more complete sympathetic block than epidural anaesthesia. To answer this question Stevens et al [8] studied healthy volunteers in a cross-over design and used a cold pressor test as a sympathetic stress. Plasma catecholamines and haemodynamic responses were similar following both techniques, indicating that spinal anaesthesia did not result in more profound attenuation of the sympathetic response than epidural anaesthesia. In addition neither technique produced total sympathetic blockade. CARDIOVASCULAR EFFECTS The cardiovascular effects observed with epidural and spinal anaesthesia are complex and are predominantly related to the extent of sympathetic denervation, autonomic balance, baseline blood volume and cardiovascular function. With epidural anaesthesia the pharmacological effect of systemically absorbed local anaesthetic agents and inclusion of adrenaline to the local anaesthetic solution may play a role. Individual cardiovascular response to different levels of sympathetic blockade varies widely, depending on the degree of sympathetic tone prior to the block. The sympathetic trunk receives its preganglionic fibres from T1 to L2-3. The most important of the cardiovascular effects are related to blockade of vasoconstrictor fibres (below T4) with resulting dilatation of resistance and capacitance vessels and/or cardiac sympathetic fibres with loss of chronotropic and inotropic drive to the myocardium (T1-T5) (fig 1) FIGURE1 Figure 1. Sympathetic blockade: central (cardiac) and peripheral components. These consist of T1-T4 cardiac sympathetic fibres and T1-L2 peripheral sympathetic fibres. Note important innervation of veins and venules. Vagal cardiac fibres are also shown. From Cousins MJ, Veering BT. Epidural Neural Blockade in Clinical Anaesthesia and Management of Pain, third Edition. Edited by Cousins MJ, Bridenbaugh PO. Philadelphia, Lippincott-Raven Publishers, 1998, p261 24
3 The haemodynamic changes produced by spinal and epidural anaesthesia are believed to result from venous and arterial dilatation induced by sympathetic blockade. The venodilation effect predominates. A block below L3 does not affect the sympathetic system and the haemodynamic upset is minimal. Haemodynamic changes relate to the extent of involvement of groups of nerves supplying the peripheral vessels, the splanchnic bed (T5-L3) and the heart (T1-4). Compensatory vasoconstriction of capacitance vessels will occur in remaining unblocked areas. In addition circulating catecholamines released from the adrenal medulla due to increased activity in any unblocked fibres in the splanchnic nerves contribute to the increased sympathetic activity below and above level of block. In a block above T5 the cardioaccelerator nerves (T2-4) will be involved, resulting in a decrease in cardiac output, slowing of the heart rate and decreased contractility. THE CARDIOVASCULAR EFFECTS OF SPINAL COMPARED TO EPIDURAL ANAESTHESIA Comparing the cardiovascular effects associated with equal sensory levels of spinal and epidural anaesthesia (T-5) in volunteers who served as their own controls resulted in differential effects.[9] The decrease in mean arterial blood pressure, cardiac output and stroke volume was greater following spinals. This is partly due to the fact that the onset of sympathetic blockade is slower following an epidural, which allows more time for compensation. Relatively large amounts of local anaesthetic solutions are required to achieve satisfactory epidural anaesthesia. Local anaesthetic agents exhibit a direct action on vascular smooth muscle resulting in either vasoconstriction or vasodilatation, depending upon the local anaesthetic agent, its stereo chemical configuration and concentration, the type of blood vessel (capacitance or resistance) and pre-existing vascular tone. Lower doses of lidocaine, producing plasma concentrations up to 4 mg L -1 have been shown to increase cardiac output by causing vasoconstriction. Conversely at higher doses the vasoconstrictor action of lidocaine changes to one of vasodilatation and hypotension may occur.[10] Epinephrine (5 µg.ml -1 ) is commonly added to the local anaesthetic solution to slow systemic absorption and prolong the duration of action. Vascular systemic absorption of epinephrine results in beta-stimulation.[11] In low doses, epinephrine produces β 2 -receptor vasodilatation action leading to a reduction in peripheral resistance. In greater doses adrenaline stimulates the heart by β 1 -receptor stimulation resulting in increased contractility and heart rate. The early cardiovascular changes observed with absorbed adrenaline are transient. Therefore the prolonged cardiovascular changes seen with local anaesthetics containing adrenaline are probably related to sympathetic blockade. BRADYCARDIA Epidural and spinal anaesthesia (with or without involvement of cardiac segments) may be associated with profound bradycardia and, in some patients, with transient cardiac arrest. This appears to be a vagal reflex.[12] The blockade of sympathetic cardiac accelerator fibres and the failure to block the vagus nerve may cause vasovagal episodes. The normal reflex tachycardia through stimulation of baroreceptors in response to a decreased arterial pressure is often absent during epidural and spinal anaesthesia when sympathetic blockade extends to the lower thoracic segments. Factors thought to contribute to the development of bradycardia include: decreased cardiac sympathetic tone, decreased venous tone, reflex decrease in heart rate resulting from decreased degree of pacemaker stretch, and reflex decrease in heart rate mediated via ventricular mechanoreceptors. Bradycardia is probably caused by an enhancement of cardiac vagal activity secondary to decreased venous return. Jacobsen et al. described echocardiographic and circulatory findings, along with changes in vagally mediated plasma hormonal parameters, in volunteers given lumbar epidurals from T8-10 to L3-L4.[13] Hypotension was accompanied by a 30% decrease in heart rate and a decrease in end-diastolic left ventricular cross-sectional diameter, indicating decreased preload. There was a marked increase in plasma pancreatic polypeptide, an index of vagal activation. This increase in pancreatic polypeptide indicated that organs other than the heart are also exposed to increased vagal activity. The results of this study indicate that during lumbar epidural anaesthesia, presyncopal symptoms are preceded by a reduction of central volume and of left ventricular diameters by approximately 13%. The aetiology of profound bradycardia or asystole during epidural anaesthesia remains unknown. The observations support an activation of the Bezold-Jarisch reflex, a cardio-inhibitory vasodepressor reflex elicited during central volume depletion from mechanoreceptors in the inferoposterior wall of the left ventricle.[14] Vagal activation with bradycardia is thus a protective reflex that prevents the heart from contracting when relatively empty. 25
4 RESPIRATORY EFFECTS The lungs are innervated from the sympathetic system from T2 to T7 and from the parasympathetic system via vagal afferent and efferent pathways. Epidural or spinal anaesthesia per se have little effect on respiration in patient without pre-existing lung disease. Most of the respiratory changes associated with spinal and epidural anaesthesia are due to motor block of the muscles of respiration. Healthy unpremedicated patients receiving high-thoracic dermatome neuraxial blocks are able to maintain normal arterial blood gas tensions and the hypercapnic response is unchanged or increased.[15,16] However, preoperative or intra operative sedation during spinal anaesthesia can result in abnormal gas exchange. Thus, oxygenation should be monitored with pulse oximetry whenever sedative drugs are employed. Since epidural anaesthesia induces segmental block of spinal nerves, an adequate extension of the block of motor nerves can selectively affect respiratory muscles in the rib cage. In healthy awake volunteers thoracic epidural anaesthesia (TEA) caused a reduction of ventilatory response to CO 2 during spontaneous respiration principally because of decreased contribution of the rib cage to tidal breathing.[17] This probably reflects blockade of the efferent or afferent pathway (or both) of the intercostal nerve roots. The respiratory effects of TEA are: modest reduction in vital capacity (VC) and forced expiratory volume in 1 second (FEV 1 ), reduction in total lung capacity (TLC) and maximal mid-expiratory flow rate (MMF) with high thoracic epidural block (T1-6). These alterations in expiratory function are probably of minor clinical importance in healthy patients. In severely compromised pulmonary patients however high TEA may impair the ability to cough effectively. The diaphragm is the principle muscle of inspiration. Diaphragmatic dysfunction is a major determinant of the impaired respiratory function observed after upper abdominal and thoracic surgery. Diaphragmatic activity increases following TEA possibly by the interruption of an inhibitory reflex of phrenic nerve motor activity, either related to direct deafferentation of visceral sensory pathways, or by a diaphragmatic load reduction due to increased abdominal compliance.[18] GASTROINTESTINAL EFFECTS Epidural and spinal block extending from T6-L1 effectively denervates the splanchnic sympathetic supply to the abdominal viscera. Spinal and epidural anaesthesia are both capable of blocking all of the sympathetic fibres innervating the bowel and the hypogastric nerves (S2-4). The vagus nerve, of course, will remain unblocked and as a consequence sympathetic blockade results in a small contracted gut owing to parasympathetic dominance by the vagus and hypogastric nerves. In general, parasympathetic outflow increases gut activity, including tonic contraction, sphincter relaxation, peristalsis and secretion. Gut transit time is reduced and gastric emptying is increased. These results suggest that intraoperative and postoperative epidural anaesthesia with local anaesthetic agents may be useful in preventing and relieving postoperative ileus.[19] Blood flow to the gastrointestinal tract is significantly increased, which may benefit anastomotic sites.[20] Nausea and vomiting may be associated with spinal and epidural anaesthesia. The aetiology of nausea during central neural blockade is poorly understood, but an increased incidence of nausea was associated with hypotension, unopposed vagal activity, sensory levels above T5 and a history of motion sickness.[12] ENDOCRINE-METABOLIC PHYSIOLOGY Significant metabolic and endocrine alterations are associated with the trauma of all surgical procedures. These changes are termed the surgical stress response. Spinal and epidural anaesthesia are able to block the sympathetic stimulation caused by surgical stress that leads to catecholamine and hormonal release. The inhibition is related to the level of neural blockade, particularly in operations on the lower abdomen and lower extremities. There is however little inhibition of endocrinemetabolic response by epidural anaesthesia in upper abdominal surgery, probably due to a failure to block the vagus nerve. 26
5 Few studies have been performed comparing endocrine metabolic responses to similar surgical procedures performed either during spinal or epidural anaesthesia, except during hysterectomy, where no additional metabolic effect was seen with the denser block of a spinal.[21] In contrast, studies in major abdominal (colonic) surgery showed continuous spinal (T4-S5) to be more effective in reducing the stress response than epidural anaesthesia (T4-S5).[22] Continuous spinal anaesthesia attenuated, but did not abolish, the increase in plasma cortisol associated with colonic surgery. THERMOREGULATORY RESPONSE Hypothermia (a decrease in core temperature) is common in patients undergoing surgery with epidural and spinal anaesthesia. Three major factors contribute: (1) internal redistribution of body heat from central to peripheral regions, (2) heat loss to the environment, and (3) inhibition of central thermoregulatory control. Shiveringlike tremor during epidural anaesthesia is triggered by core hypothermia and preceded by vasoconstriction above the level of the block. Comparable sweating, vasoconstriction and shivering thresholds during spinal and epidural anaesthesia have been demonstrated, suggesting that thermoregulatory processing is similar during each type of regional anaesthesia, although the amount of local anaesthetic administered usually differs by an order of magnitude.[23] CONCLUSION The physiological responses to spinal and epidural anaesthesia result from three effects (1) autonomic blockade with effects on both the vascular beds and cardiac function; (2) abolition of somatic pain and the reflex responses associated with it, and (3) from the effects of motor block. When comparing the physiological effects of spinal and epidural anaesthesia it is important to understand that epidural anaesthesia is slowed by the dural and epineurial barriers. Therefore the onset of sympathetic blockade with epidural anaesthesia is slower than with spinal anaesthesia. In general the fall in blood pressure will be relatively mild and more gradual with epidural with comparable spread. In addition the spread of epidural anaesthesia can be more carefully controlled and the block can be performed segmentally, restricting the haemodynamic side effects. The question arises as to whether there will exist any difference with regard to differential block between spinal and epidural anaesthesia. Neither technique provides total sympathetic blockade. Further studies are however needed before clinically relevant conclusions can be drawn. This summary has shown that the physiologic effects of spinal are similar to those of epidural anaesthesia, with the exception that local anaesthetic blood levels following epidural anaesthesia may produce systemic effects on their own. 27
6 REFERENCES 1. Greene NM. Uptake and elimination of local anesthetics during spinal anaesthesia. Anesth Analg 1983;62: Bromage PR. Mechanism of action of extradural analgesia. Br J Anaesth 1975;47: Stevens RA, Bray JG, Artuso JD, Kao TC, Spitzer L. Differential epidural block. Reg Anesth 1992;17: Fink BR. Mechanisms of differential axial blockade in epidural and subarachnoid anesthesia. Anesthesiology 1989;70: Chamberlain D, Chamberlain B. Changes in skin temperature of the trunk and their relationship to sympathetic block during spinal anesthesia. Anesthesiology 1986;65: Malmqvist L-A, Tryggvason B, Bengtsson M. Sympathetic blockade during extradural analgesia with mepivacaine or bupivacaine. Acta Anaesthesiol Scand 1989; 33: Bengtsson M. The effect of spinal analgesia on skin blood flow evaluated by laser Doppler flowmetry. Acta Anaesthesiol Scand 1983; 27: Stevens RA, Beardsley D, White JL, Kao TC, Gantt R, Holman S. Does spinal anesthesia result in a more complete sympathetic block than from epidural anesthesia? Anesthesiology 1995;82: Ward RJ, Bonica JJ, Freund FG, Akamatsu T, Dantzinger F, Englesson S. Epidural and subarachnoid anesthesia: cardiovascular and respiratory effects. JAMA 1965;191: Bonica JJ, Berges PU, Morikawa K. Circulatory effects of peridural block: I. Effects of level of anesthesia and dose of lidocaine. Anesthesiology 1970;33: Bonica JJ, Akamatsu TJ, Berges PU, Morikawa K, Kennedy WF. Circulatory effects 12. Carpenter RL, Caplan RA, Brown DL, Stephenson C, Wu R. Incidence and risk factors for side effects of spinal anesthesia. Anesthesiology 1992;76: Jacobsen J, Sófelt S, Brocks V, Fernandes A, Warberg J, Secher NH. Reduced left ventricular diameters at onset of bradycardia during epidural anaesthesia. Acta Anaesthesiol Scand 1992;36: Campagna JA, Carter C. Clinical relevance of the Bezold-Jarisch reflex.anesthesiology 2003; 98: Sakura S, Saito Y, Kosaka Y. Effect of lumbar epidural anesthesia on ventilatory response to hypercapnia in young and elderly patients. J Clin Anesth 1993;5: Steinbrook R, Concepcion M, Topulos. Ventilatory responses to hypercapnia during bupivacaine spinal anesthesia. Anesth Analg 1988;67: Kochi T, Saco S, Nishino T, Mizuguchi T. Effect of high thoracic extradural anaesthesia on ventilatory response to hypercapnia in normal volunteers. Br J Anaesth 1989;62: Pansard JL, Mankikian B, Bertrand M, Kieffer E, Clergue F, Viars P. Effects of thoracic extradural block on diaphragmatic electrical activity and contractility after upper abdominal surgery. Anesthesiology 1993;78: Liu S, Carpenter RL, Neal JM. Epidural anesthesia and analgesia. Their role on postoperative outcome. Anesthesiology 1995;82: Johansson K, Ahn H, Lindhagen J, Tryselius U. Effect of epidural anaesthesia on intestinal blood flow. Br J Surg 1988;75: Kehlet H. Surgical stress: the role of pain and analgesia. Br J Anaesth 1989;63: Webster J, Barnard M, Carli F. Metabolic responses to colonic surgery: extradural vs continuous spinal. Br J Anaesth 1991;67: Ozaki M, Kurz A, Sessler DI, Lenhardt R, Schroeder M, Moayeri A, Noyes KM, Rotheneder E. Thermoregulatory thresholds during epidural and spinal anesthesia. Anesthesiology 1994;81:
T. Laitinen Departments of Physiology and Clinical Physiology, University of Kuopio and Kuopio University Hospital, Kuopio, Finland
 AUTONOMOUS NEURAL REGULATION T. Laitinen Departments of Physiology and Clinical Physiology, University of Kuopio and Kuopio University Hospital, Kuopio, Finland Keywords: Autonomic nervous system, sympathetic
AUTONOMOUS NEURAL REGULATION T. Laitinen Departments of Physiology and Clinical Physiology, University of Kuopio and Kuopio University Hospital, Kuopio, Finland Keywords: Autonomic nervous system, sympathetic
The Autonomic Nervous
 Autonomic Nervous System The Autonomic Nervous Assess Prof. Fawzia Al-Rouq System Department of Physiology College of Medicine King Saud University LECTUR (1) Functional Anatomy & Physiology of Autonomic
Autonomic Nervous System The Autonomic Nervous Assess Prof. Fawzia Al-Rouq System Department of Physiology College of Medicine King Saud University LECTUR (1) Functional Anatomy & Physiology of Autonomic
Neurocardiogenic syncope
 Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Chapters 9 & 10. Cardiorespiratory System. Cardiovascular Adjustments to Exercise. Cardiovascular Adjustments to Exercise. Nervous System Components
 Cardiorespiratory System Chapters 9 & 10 Cardiorespiratory Control Pulmonary ventilation Gas exchange Left heart Arterial system Tissues Right heart Lungs Pulmonary ventilation Cardiovascular Regulation-
Cardiorespiratory System Chapters 9 & 10 Cardiorespiratory Control Pulmonary ventilation Gas exchange Left heart Arterial system Tissues Right heart Lungs Pulmonary ventilation Cardiovascular Regulation-
Autonomic Nervous System Dr. Ali Ebneshahidi
 Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Autonomic Nervous System Dr. Ali Ebneshahidi Nervous System Divisions of the nervous system The human nervous system consists of the central nervous System (CNS) and the Peripheral Nervous System (PNS).
Chapter 14 The Autonomic Nervous System Chapter Outline
 Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Chapter 14 The Autonomic Nervous System Chapter Outline Module 14.1 Overview of the Autonomic Nervous System (Figures 14.1 14.3) A. The autonomic nervous system (ANS) is the involuntary arm of the peripheral
Autonomic Nervous System
 Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Autonomic Nervous System Keri Muma Bio 6 Organization of the Nervous System Efferent Division Somatic Nervous System Voluntary control Effector = skeletal muscles Muscles must be excited by a motor neuron
Neuropsychiatry Block
 Neuropsychiatry Block Physiology of the Autonomic Nervous System By Laiche Djouhri, PhD Dept. of Physiology Email: ldjouhri@ksu.edu.sa Ext:71044 References The Autonomic Nervous System and the Adrenal
Neuropsychiatry Block Physiology of the Autonomic Nervous System By Laiche Djouhri, PhD Dept. of Physiology Email: ldjouhri@ksu.edu.sa Ext:71044 References The Autonomic Nervous System and the Adrenal
Systems Neuroscience November 21, 2017 The autonomic nervous system
 Systems Neuroscience November 21, 2017 The autonomic nervous system Daniel C. Kiper kiper@ini.phys.ethz.ch http: www.ini.unizh.ch/~kiper/system_neurosci.html How is the organization of the autonomic nervous
Systems Neuroscience November 21, 2017 The autonomic nervous system Daniel C. Kiper kiper@ini.phys.ethz.ch http: www.ini.unizh.ch/~kiper/system_neurosci.html How is the organization of the autonomic nervous
Introduction to Autonomic
 Part 2 Autonomic Pharmacology 3 Introduction to Autonomic Pharmacology FUNCTIONS OF THE AUTONOMIC NERVOUS SYSTEM The autonomic nervous system (Figure 3 1) is composed of the sympathetic and parasympathetic
Part 2 Autonomic Pharmacology 3 Introduction to Autonomic Pharmacology FUNCTIONS OF THE AUTONOMIC NERVOUS SYSTEM The autonomic nervous system (Figure 3 1) is composed of the sympathetic and parasympathetic
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Cardiac arrests during spinal anesthesia are described
 MEDICAL INTELLIGENCE Cardiac Arrest During Spinal Anesthesia: Common Mechanisms and Strategies for Prevention John B. Pollard, MD Departments of Anesthesiology, Veterans Affairs Palo Alto Health Care System
MEDICAL INTELLIGENCE Cardiac Arrest During Spinal Anesthesia: Common Mechanisms and Strategies for Prevention John B. Pollard, MD Departments of Anesthesiology, Veterans Affairs Palo Alto Health Care System
Composed by Natalia Leonidovna Svintsitskaya, Associate professor of the Chair of Human Anatomy, Candidate of Medicine
 Theoretical background to the study of the autonomic nervous system. Sympathetic and parasympathetic divisions of the autonomic nervous system. Features of the structure, function Composed by Natalia Leonidovna
Theoretical background to the study of the autonomic nervous system. Sympathetic and parasympathetic divisions of the autonomic nervous system. Features of the structure, function Composed by Natalia Leonidovna
Lujain Hamdan. Ayman Musleh & Yahya Salem. Mohammed khatatbeh
 12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
12 Lujain Hamdan Ayman Musleh & Yahya Salem Mohammed khatatbeh the last lecture, we have studied the differences between the two divisions of the ANS: sympathetic and parasympathetic pathways which work
Drugs Affecting The Autonomic Nervous System(ANS)
 Drugs Affecting The Autonomic Nervous System(ANS) ANS Pharmacology Lecture 1 Dr. Hiwa K. Saaed College of Pharmacy, University of Sulaimani 2018-2019 AUTOMATIC NERVOUS SYSTEM (ANS) The ANS is the major
Drugs Affecting The Autonomic Nervous System(ANS) ANS Pharmacology Lecture 1 Dr. Hiwa K. Saaed College of Pharmacy, University of Sulaimani 2018-2019 AUTOMATIC NERVOUS SYSTEM (ANS) The ANS is the major
ParasymPathetic Nervous system. Done by : Zaid Al-Ghnaneem
 ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
The Nervous System: Autonomic Nervous System Pearson Education, Inc.
 17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
17 The Nervous System: Autonomic Nervous System Introduction The autonomic nervous system: Functions outside of our conscious awareness Makes routine adjustments in our body s systems The autonomic nervous
Autonomic Division of NS
 Autonomic Division of NS Compare and contrast the structures of the sympathetic and the parasympathetic divisions, including functions and neurotransmitters. Show the levels of integration in the ANS,
Autonomic Division of NS Compare and contrast the structures of the sympathetic and the parasympathetic divisions, including functions and neurotransmitters. Show the levels of integration in the ANS,
CHAPTER 15 LECTURE OUTLINE
 CHAPTER 15 LECTURE OUTLINE I. INTRODUCTION A. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. B. Operation of the ANS to maintain homeostasis,
CHAPTER 15 LECTURE OUTLINE I. INTRODUCTION A. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. B. Operation of the ANS to maintain homeostasis,
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD
 AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
AUTONOMIC NERVOUS SYSTEM PART I: SPINAL CORD How is the organization of the autonomic nervous system different from that of the somatic nervous system? Peripheral Nervous System Divisions Somatic Nervous
Department of Neurology/Division of Anatomical Sciences
 Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Spinal Cord I Lecture Outline and Objectives CNS/Head and Neck Sequence TOPIC: FACULTY: THE SPINAL CORD AND SPINAL NERVES, Part I Department of Neurology/Division of Anatomical Sciences LECTURE: Monday,
Do Now pg What is the fight or flight response? 2. Give an example of when this response would kick in.
 Do Now pg 81 1. What is the fight or flight response? 2. Give an example of when this response would kick in. Autonomic Nervous System The portion of the PNS that functions independently (autonomously)
Do Now pg 81 1. What is the fight or flight response? 2. Give an example of when this response would kick in. Autonomic Nervous System The portion of the PNS that functions independently (autonomously)
number Done by Corrected by Doctor
 number 13 Done by Tamara Wahbeh Corrected by Doctor Omar Shaheen In this sheet the following concepts will be covered: 1. Divisions of the nervous system 2. Anatomy of the ANS. 3. ANS innervations. 4.
number 13 Done by Tamara Wahbeh Corrected by Doctor Omar Shaheen In this sheet the following concepts will be covered: 1. Divisions of the nervous system 2. Anatomy of the ANS. 3. ANS innervations. 4.
Pheochromocytoma: Effects of Catecholamines
 36 PHYSIOLOGY CASES AND PROBLEMS Case 8 Pheochromocytoma: Effects of Catecholamines Helen Ames is a 51-year-old homemaker who experienced what she thought were severe menopausal symptoms. These awful "attacks"
36 PHYSIOLOGY CASES AND PROBLEMS Case 8 Pheochromocytoma: Effects of Catecholamines Helen Ames is a 51-year-old homemaker who experienced what she thought were severe menopausal symptoms. These awful "attacks"
Anaesthesia. Update in. An Introduction to Cardiovascular Physiology. James Rogers Correspondence
 Update in Anaesthesia Originally published in Update in Anaesthesia, edition 10 (1999) An Introduction to Cardiovascular Physiology Correspondence Email: James.Rogers@nbt.nhs.uk INTRODUCTION The cardiovascular
Update in Anaesthesia Originally published in Update in Anaesthesia, edition 10 (1999) An Introduction to Cardiovascular Physiology Correspondence Email: James.Rogers@nbt.nhs.uk INTRODUCTION The cardiovascular
The Autonomic Nervous System
 The Autonomic Nervous System Responsible for control of visceral effectors and visceral reflexes: smooth muscle, glands, the heart. e.g. blood pressure, cardiac output, plasma glucose The autonomic system
The Autonomic Nervous System Responsible for control of visceral effectors and visceral reflexes: smooth muscle, glands, the heart. e.g. blood pressure, cardiac output, plasma glucose The autonomic system
Constriction and dilatation of blood vessels. Contraction and relaxation of smooth muscle in various organs. Visual accommodation, pupillary size.
 The Autonomic Nervous System (ANS) Dr. L. Al tmimi Academic year 2011-2012 This text is focused mostly on the anatomy and physiology of the Autonomic Nervous System (ANS), more specifically, about the
The Autonomic Nervous System (ANS) Dr. L. Al tmimi Academic year 2011-2012 This text is focused mostly on the anatomy and physiology of the Autonomic Nervous System (ANS), more specifically, about the
Chapter 16. APR Enhanced Lecture Slides
 Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
Chapter 16 APR Enhanced Lecture Slides See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes and animations. Copyright The McGraw-Hill Companies, Inc. Permission
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
(C) Muscles provide structural support, are involved in thermoregulation, but have no effect on organ function.
 OAT Biology - Problem Drill 13: The Muscular System Question No. 1 of 10 1. Which statement about muscles is correct? Question #01 (A) Muscles have an origin that is usually attached to a movable bone,
OAT Biology - Problem Drill 13: The Muscular System Question No. 1 of 10 1. Which statement about muscles is correct? Question #01 (A) Muscles have an origin that is usually attached to a movable bone,
Sympathetic Nervous System
 Sympathetic Nervous System Lecture Objectives Review the subdivisions of the nervous system. Review the general arrangement and compare the sympathetic and parasympathetic parts. Describe the following
Sympathetic Nervous System Lecture Objectives Review the subdivisions of the nervous system. Review the general arrangement and compare the sympathetic and parasympathetic parts. Describe the following
Autonomic Nervous System
 Autonomic Nervous System Autonomic nervous system organization Sympathetic Nervous System division of the autonomic nervous system that arouses the body, mobilizing its energy in stressful situations
Autonomic Nervous System Autonomic nervous system organization Sympathetic Nervous System division of the autonomic nervous system that arouses the body, mobilizing its energy in stressful situations
The Nervous System: Autonomic Nervous System
 17 The Nervous System: Autonomic Nervous System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The autonomic nervous system functions
17 The Nervous System: Autonomic Nervous System PowerPoint Lecture Presentations prepared by Steven Bassett Southeast Community College Lincoln, Nebraska Introduction The autonomic nervous system functions
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Fig Glossopharyngeal nerve transmits signals to medulla oblongata. Integrating center. Receptor. Baroreceptors sense increased blood pressure
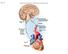 Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
Fig. 5. Integrating center Glossopharyngeal nerve transmits signals to medulla oblongata Receptor 3 Vagus nerve transmits inhibitory signals to cardiac pacemaker Baroreceptors sense increased blood pressure
The Nervous System. Autonomic Division. C h a p t e r. PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas
 C h a p t e r 17 The Nervous System Autonomic Division PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing as Pearson
C h a p t e r 17 The Nervous System Autonomic Division PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing as Pearson
I. Neural Control of Involuntary Effectors. Chapter 9. Autonomic Motor Nerves. Autonomic Neurons. Autonomic Ganglia. Autonomic Neurons 9/19/11
 Chapter 9 I. Neural Control of Involuntary Effectors The Autonomic Nervous System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Autonomic
Chapter 9 I. Neural Control of Involuntary Effectors The Autonomic Nervous System Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Autonomic
Using Figure 14.1, match the following: 1) Myelin sheath. 1) 2) Cell body of ANS preganglionic neuron. 2)
 Practice Exam 1 AP 2 chapters 14 and 18 Name MATCHING: Match labeled areas with the appropriate terminology from the list below. Figure 14.1 Using Figure 14.1, match the following: 1) Myelin sheath. 1)
Practice Exam 1 AP 2 chapters 14 and 18 Name MATCHING: Match labeled areas with the appropriate terminology from the list below. Figure 14.1 Using Figure 14.1, match the following: 1) Myelin sheath. 1)
Biology 218 Human Anatomy
 Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
Chapter 20 Adapted form Tortora 10 th ed. LECTURE OUTLINE A. Introduction (p. 632) 1. The autonomic nervous system (ANS) regulates the activity of smooth muscle, cardiac muscle, and certain glands. 2.
Autonomic Nervous System
 Autonomic Nervous System Touqeer Ahmed PhD 3 rd March, 2017 Atta-ur-Rahman School of Applied Biosciences National University of Sciences and Technology Nervous System Divisions The peripheral nervous system
Autonomic Nervous System Touqeer Ahmed PhD 3 rd March, 2017 Atta-ur-Rahman School of Applied Biosciences National University of Sciences and Technology Nervous System Divisions The peripheral nervous system
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.)
 Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Chp. 16: AUTONOMIC N.S. (In Review: Peripheral N. S.) Peripheral nerves contain both motor and sensory neurons Among the motor neurons, some of these are somatic and innervate skeletal muscles while some
Ganglionic Blockers. Ganglion- blocking agents competitively block the action of
 Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Ganglionic Blockers Ganglion- blocking agents competitively block the action of acetylcholine and similar agonists at nicotinic (Nn) receptors of both parasympathetic and sympathetic autonomic ganglia.
Cardiovascular regulation. Neural and hormonal Regulation Dr Badri Paudel GMC. 1-Local factors (autoregulation) Control of Blood Flow
 Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
Neural and hormonal Regulation Dr Badri Paudel GMC 1 Cardiovascular regulation Fa c t o r s i nvo l v e d i n t h e regulation of cardiovascular function include: 1- Autoregulation 2- Neural regulation
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Ahmad Rabei & Hamad Mrayat. Ahmad Rabei & Hamad Mrayat. Mohd.Khatatbeh
 10 Ahmad Rabei & Hamad Mrayat Ahmad Rabei & Hamad Mrayat Mohd.Khatatbeh Before you start: Important terminology: 1 Ganglion: Nerve cell cluster, where neurons are typically linked by synapses. Also, it`s
10 Ahmad Rabei & Hamad Mrayat Ahmad Rabei & Hamad Mrayat Mohd.Khatatbeh Before you start: Important terminology: 1 Ganglion: Nerve cell cluster, where neurons are typically linked by synapses. Also, it`s
Nervous system. Made up of. Peripheral nervous system. Central nervous system. The central nervous system The peripheral nervous system.
 Made up of The central nervous system The peripheral nervous system Nervous system Central nervous system Peripheral nervous system Brain Spinal Cord Cranial nerve Spinal nerve branch from the brain connect
Made up of The central nervous system The peripheral nervous system Nervous system Central nervous system Peripheral nervous system Brain Spinal Cord Cranial nerve Spinal nerve branch from the brain connect
THE GOOFY ANATOMIST QUIZZES
 THE GOOFY ANATOMIST QUIZZES 5. NERVES Q1. Which of the following classifications of the nervous systems is correct? A. The autonomic nervous system is composed of the brain, cranial nerves and spinal nerves.
THE GOOFY ANATOMIST QUIZZES 5. NERVES Q1. Which of the following classifications of the nervous systems is correct? A. The autonomic nervous system is composed of the brain, cranial nerves and spinal nerves.
COMPARATIVE ANAESTHETIC PROPERTIES OF VARIOUS LOCAL ANAESTHETIC AGENTS IN EXTRADURAL BLOCK FOR LABOUR
 Br.J. Anaesth. (1977), 49, 75 COMPARATIVE ANAESTHETIC PROPERTIES OF VARIOUS LOCAL ANAESTHETIC AGENTS IN EXTRADURAL BLOCK FOR LABOUR D. G. LITTLEWOOD, D. B. SCOTT, J. WILSON AND B. G. COVINO SUMMARY Various
Br.J. Anaesth. (1977), 49, 75 COMPARATIVE ANAESTHETIC PROPERTIES OF VARIOUS LOCAL ANAESTHETIC AGENTS IN EXTRADURAL BLOCK FOR LABOUR D. G. LITTLEWOOD, D. B. SCOTT, J. WILSON AND B. G. COVINO SUMMARY Various
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
INTRODUCTION TO GASTROINTESTINAL FUNCTIONS
 1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
1 INTRODUCTION TO GASTROINTESTINAL FUNCTIONS 2 Learning outcomes List two main components that make up the digestive system Describe the 6 essential functions of the GIT List factors (neurological, hormonal
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Autonomic Nervous System
 Autonomic Nervous System 6 th March, 2015 & 19 th March, 2015 Touqeer Ahmed Ph.D. Atta-ur-Rahman School of Applied Biosciences National University of Sciences and Technology Autonomic Nervous System Role
Autonomic Nervous System 6 th March, 2015 & 19 th March, 2015 Touqeer Ahmed Ph.D. Atta-ur-Rahman School of Applied Biosciences National University of Sciences and Technology Autonomic Nervous System Role
Human Anatomy. Autonomic Nervous System
 Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Human Anatomy Autonomic Nervous System 1 Autonomic Nervous System ANS complex system of nerves controls involuntary actions. Works with the somatic nervous system (SNS) regulates body organs maintains
Properties of Pressure
 OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
OBJECTIVES Overview Relationship between pressure and flow Understand the differences between series and parallel circuits Cardiac output and its distribution Cardiac function Control of blood pressure
2.4 Autonomic Nervous System
 2.4 Autonomic Nervous System The ANS regulates visceral activities normally outside the realm of consciousness and voluntary control: Circulation. Digestion. Sweating. Pupillary size. The ANS consists
2.4 Autonomic Nervous System The ANS regulates visceral activities normally outside the realm of consciousness and voluntary control: Circulation. Digestion. Sweating. Pupillary size. The ANS consists
Autonomic Nervous System DR JAMILA EL MEDANY
 Autonomic Nervous System DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: Define the autonomic nervous system. Describe the structure of autonomic nervous system Trace
Autonomic Nervous System DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: Define the autonomic nervous system. Describe the structure of autonomic nervous system Trace
The Autonomic Nervous System Outline of class lecture for Physiology
 The Autonomic Nervous System Outline of class lecture for Physiology 1 After studying the endocrine system you should be able to: 1. Describe the organization of the nervous system. 2. Compare and contrast
The Autonomic Nervous System Outline of class lecture for Physiology 1 After studying the endocrine system you should be able to: 1. Describe the organization of the nervous system. 2. Compare and contrast
Autonomic Nervous System
 Autonomic Nervous System Autonomic Nervous System Ref: Textbook of Medical Physiology, Guyton, 12th ed: 729-738, 11th ed. P748-760, and 10th ed. p697-708. Fig.17.02 General functions Control and Adaptation
Autonomic Nervous System Autonomic Nervous System Ref: Textbook of Medical Physiology, Guyton, 12th ed: 729-738, 11th ed. P748-760, and 10th ed. p697-708. Fig.17.02 General functions Control and Adaptation
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1)
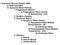 I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
I. Autonomic Nervous System (ANS) A. Dual Innervation B. Autonomic Motor Pathway 1. Preganglionic Neuron a. Preganglionic Fibers (Axons) (1) Acetylcholine - ACh 2. Ganglion (Ganglia) 3. Ganglionic Neuron
Human Anatomy & Physiology
 PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 14 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PowerPoint Lecture Slides prepared by Barbara Heard, Atlantic Cape Community College Ninth Edition Human Anatomy & Physiology C H A P T E R 14 Annie Leibovitz/Contact Press Images 2013 Pearson Education,
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 15 The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems The somatic nervous system includes both sensory and motor
Principles of Anatomy and Physiology 14 th Edition CHAPTER 15 The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems The somatic nervous system includes both sensory and motor
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
MCAT Biology Problem Drill 18: The Muscular System
 MCAT Biology Problem Drill 18: The Muscular System Question No. 1 of 10 Question 1. Which statement about muscles is correct? Question #01 A. Muscles have an origin that is usually attached to a movable
MCAT Biology Problem Drill 18: The Muscular System Question No. 1 of 10 Question 1. Which statement about muscles is correct? Question #01 A. Muscles have an origin that is usually attached to a movable
Autonomic Nervous System (the visceral motor system) Steven McLoon Department of Neuroscience University of Minnesota
 Autonomic Nervous System (the visceral motor system) Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Coffee Hour Monday, Nov 6, 9:00-10:00am Surdyk s Café in Northrop Auditorium
Autonomic Nervous System (the visceral motor system) Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Coffee Hour Monday, Nov 6, 9:00-10:00am Surdyk s Café in Northrop Auditorium
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
The Nervous System An overview
 Nervous System The Nervous System An overview Includes Nerve tissue Sense organs Functions to Sense environment Process information it receives Respond to information 1 Copyright 2009 Pearson Education,
Nervous System The Nervous System An overview Includes Nerve tissue Sense organs Functions to Sense environment Process information it receives Respond to information 1 Copyright 2009 Pearson Education,
nerve blocks in the diagnosis and therapy of visceral disease
 Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
Visceral Pain nerve blocks in the diagnosis and therapy of visceral disease Guy Hans, MD, PhD Dept. of Anesthesiology, Multidisciplinary Pain Center Visceral Pain? Type of nociceptive pain (although often
PNS and ANS Flashcards
 1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
1. Name several SOMATIC SENSES Light touch (being touched by a feather), heat, cold, vibration, pressure, pain are SOMATIC SENSES. 2. What are proprioceptors; and how is proprioception tested? PROPRIOCEPTORS
BIOH111. o Cell Module o Tissue Module o Skeletal system o Muscle system o Nervous system o Endocrine system o Integumentary system
 BIOH111 o Cell Module o Tissue Module o Skeletal system o Muscle system o Nervous system o Endocrine system o Integumentary system Endeavour College of Natural Health endeavour.edu.au 1 Textbook and required/recommended
BIOH111 o Cell Module o Tissue Module o Skeletal system o Muscle system o Nervous system o Endocrine system o Integumentary system Endeavour College of Natural Health endeavour.edu.au 1 Textbook and required/recommended
Cerebral hemisphere. Parietal Frontal Occipital Temporal
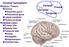 Cerebral hemisphere Sulcus / Fissure Central Precental gyrus Postcentral gyrus Lateral (cerebral) Parieto-occipital Cerebral cortex Frontal lobe Parietal lobe Temporal lobe Insula Amygdala Hippocampus
Cerebral hemisphere Sulcus / Fissure Central Precental gyrus Postcentral gyrus Lateral (cerebral) Parieto-occipital Cerebral cortex Frontal lobe Parietal lobe Temporal lobe Insula Amygdala Hippocampus
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
Spinal anesthesia without hypotension a myth or reality?
 Spinal anesthesia without hypotension a myth or reality? Peter Poredoš, MD, PhD, DESA peter.poredos@kclj.si University Medical Centre Ljubljana, Slovenia Department for Anesthesiology and Intensive Care
Spinal anesthesia without hypotension a myth or reality? Peter Poredoš, MD, PhD, DESA peter.poredos@kclj.si University Medical Centre Ljubljana, Slovenia Department for Anesthesiology and Intensive Care
Drugs Affecting the Autonomic Nervous System-1. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Drugs Affecting the Autonomic Nervous System-1 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia The autonomic nervous system, along with the endocrine system,
Drugs Affecting the Autonomic Nervous System-1 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia The autonomic nervous system, along with the endocrine system,
Spinal nerves. Aygul Shafigullina. Department of Morphology and General Pathology
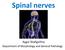 Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
Spinal nerves Aygul Shafigullina Department of Morphology and General Pathology Spinal nerve a mixed nerve, formed in the vicinity of an intervertebral foramen, where fuse a dorsal root and a ventral root,
Chapter 15: The Autonomic Nervous System. Copyright 2009, John Wiley & Sons, Inc.
 Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
Chapter 15: The Autonomic Nervous System Comparison of Somatic and Autonomic Nervous Systems Comparison of Somatic and Autonomic Nervous Systems Anatomy of Autonomic Motor Pathways Preganglionic neuron
The Nervous System. Functions of the Nervous System input gathering To monitor occurring inside and outside the body Changes =
 The Nervous System Functions of the Nervous System input gathering To monitor occurring inside and outside the body Changes = To process and sensory input and decide if is needed output A response to integrated
The Nervous System Functions of the Nervous System input gathering To monitor occurring inside and outside the body Changes = To process and sensory input and decide if is needed output A response to integrated
a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure.
 B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
B. 10 Applied Respiratory Physiology a. Describe the physiological consequences of intermittent positive pressure ventilation and positive end-expiratory pressure. Intermittent positive pressure ventilation
Maternal Physiology and the Anesthetized Pregnant Patient. Kimberly Babiash, MD, MBA Oct 7, 2015
 Maternal Physiology and the Anesthetized Pregnant Patient Kimberly Babiash, MD, MBA Oct 7, 2015 Overview Neuraxial Anesthesia Epidurals vs spinals How they work Physiologic alterations Contraindications
Maternal Physiology and the Anesthetized Pregnant Patient Kimberly Babiash, MD, MBA Oct 7, 2015 Overview Neuraxial Anesthesia Epidurals vs spinals How they work Physiologic alterations Contraindications
The Spinal Cord & Spinal Nerves
 The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
The Spinal Cord & Spinal Nerves Together with brain forms the CNS Functions spinal cord reflexes integration (summation of inhibitory and excitatory) nerve impulses highway for upward and downward travel
Screening and bioassay of Sympatholytics. Dr. Magdy M. Awny Lecture 4
 Screening and bioassay of Sympatholytics by Dr. Magdy M. Awny Lecture 4 1 They are classified into: Sympatholytics = Antagonist of adrenergic activity Drugs that interfere with the activity of the sympathetic
Screening and bioassay of Sympatholytics by Dr. Magdy M. Awny Lecture 4 1 They are classified into: Sympatholytics = Antagonist of adrenergic activity Drugs that interfere with the activity of the sympathetic
Posted: 11/27/2011 on Medscape; Published Br J Anaesth. 2011;107(2): Oxford University Press
 Posted: 11/27/2011 on Medscape; Published Br J Anaesth. 2011;107(2):209-217. 2011 Oxford University Press Effect of Phenylephrine and Ephedrine Bolus Treatment on Cerebral Oxygenation in Anaesthetized
Posted: 11/27/2011 on Medscape; Published Br J Anaesth. 2011;107(2):209-217. 2011 Oxford University Press Effect of Phenylephrine and Ephedrine Bolus Treatment on Cerebral Oxygenation in Anaesthetized
cardiac plexus is continuous with the coronary and no named branches pain from the heart and lungs
 Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Local Anesthetics. Xiaoping Du Room E417 MSB Department of Pharmacology Phone (312) ;
 Local Anesthetics Xiaoping Du Room E417 MSB Department of Pharmacology Phone (312)355 0237; Email: xdu@uic.edu Summary: Local anesthetics are drugs used to prevent or relieve pain in the specific regions
Local Anesthetics Xiaoping Du Room E417 MSB Department of Pharmacology Phone (312)355 0237; Email: xdu@uic.edu Summary: Local anesthetics are drugs used to prevent or relieve pain in the specific regions
ANATOMY & PHYSIOLOGY - CLUTCH CH THE AUTONOMIC NERVOUS SYSTEM.
 !! www.clutchprep.com ANATOMY & PHYSIOLOGY - CLUTCH CONCEPT: THE AUTONOMIC NERVOUS SYSTEM: DIVISIONS AND STRUCTURE The Autonomic Nervous System and its Divisions: Autonomic Nervous System (ANS) controls
!! www.clutchprep.com ANATOMY & PHYSIOLOGY - CLUTCH CONCEPT: THE AUTONOMIC NERVOUS SYSTEM: DIVISIONS AND STRUCTURE The Autonomic Nervous System and its Divisions: Autonomic Nervous System (ANS) controls
ACTIVITY2.15 Text:Campbell,v.8,chapter48 DATE HOUR NERVOUS SYSTEMS NEURON
 AP BIOLOGY ACTIVITY2.15 Text:Campbell,v.8,chapter48 NAME DATE HOUR NERVOUS SYSTEMS NEURON SIMPLE REFLEX RESTING POTENTIAL ACTION POTENTIAL ACTION POTENTIAL GRAPH TRANSMISSION ACROSS A SYNAPSE QUESTIONS:
AP BIOLOGY ACTIVITY2.15 Text:Campbell,v.8,chapter48 NAME DATE HOUR NERVOUS SYSTEMS NEURON SIMPLE REFLEX RESTING POTENTIAL ACTION POTENTIAL ACTION POTENTIAL GRAPH TRANSMISSION ACROSS A SYNAPSE QUESTIONS:
Block of sympathetic innervation accounts
 MINERVA ANESTESIOL 2003;69:433-7 Cardiovascular and pulmonary effects of epidural anaesthesia B.TH. VEERING The cardiovascular effects observed with epidural anaesthesia are complex and are predominantly
MINERVA ANESTESIOL 2003;69:433-7 Cardiovascular and pulmonary effects of epidural anaesthesia B.TH. VEERING The cardiovascular effects observed with epidural anaesthesia are complex and are predominantly
Autonomic nervous system
 Autonomic nervous system Key notes Autonomic: an independent system that runs on its own The ANS is a visceral and involuntary sensory and motor system The visceral motor fibers in the autonomic nerves
Autonomic nervous system Key notes Autonomic: an independent system that runs on its own The ANS is a visceral and involuntary sensory and motor system The visceral motor fibers in the autonomic nerves
Comparison of Bolus Bupivacaine, Fentanyl, and Mixture of Bupivacaine with Fentanyl in Thoracic Epidural Analgesia for Upper Abdominal Surgery
 Original Article DOI: 10.17354/ijss/2016/156 Comparison of Bolus Bupivacaine, Fentanyl, and Mixture of Bupivacaine with Fentanyl in Thoracic Epidural Analgesia for Upper Abdominal Surgery Sachin Gajbhiye
Original Article DOI: 10.17354/ijss/2016/156 Comparison of Bolus Bupivacaine, Fentanyl, and Mixture of Bupivacaine with Fentanyl in Thoracic Epidural Analgesia for Upper Abdominal Surgery Sachin Gajbhiye
The Nervous System PART A
 7 The Nervous System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Structural Classification
7 The Nervous System PART A PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB Structural Classification
Physiologic Anatomy and Nervous Connections of the Bladder
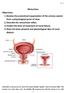 Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Micturition Objectives: 1. Review the anatomical organization of the urinary system from a physiological point of view. 2. Describe the micturition reflex. 3. Predict the lines of treatment of renal failure.
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Autonomic Nervous System. Ms. DS Pillay Room 2P24
 Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Autonomic Nervous System Ms. DS Pillay Room 2P24 OVERVIEW OF THE NERVOUS SYSTEM NERVOUS SYSTEM CNS PNS BRAIN SPINAL CORD SOMATIC ANS SYMPATHEIC PARASYMPATHEIC LOCATION OF GANGLIA IN THE ANS Short post-ganglionic
Ch 9. The Autonomic Nervous System
 Ch 9 The Autonomic Nervous System SLOs Review the organization of the ANS Describe how neural regulation of smooth and cardiac muscles differs from that of skeletal muscles Describe the structure and innervation
Ch 9 The Autonomic Nervous System SLOs Review the organization of the ANS Describe how neural regulation of smooth and cardiac muscles differs from that of skeletal muscles Describe the structure and innervation
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
Autonomic nervous system
 15 Autonomic nervous system The role of nervous system ANTICIPATION Cortex Potential input Potential output Cortex Integration Sensor Input Output Effector REGULATION Feedback regulation http://www.slideshare.net/drpsdeb/presentations
15 Autonomic nervous system The role of nervous system ANTICIPATION Cortex Potential input Potential output Cortex Integration Sensor Input Output Effector REGULATION Feedback regulation http://www.slideshare.net/drpsdeb/presentations
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
