Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website:
|
|
|
- Rosanna Hood
- 5 years ago
- Views:
Transcription
1 Mrs Ami Shukla Consultant Gynaecologist and Obstetrician Lead Urogynaecologist, Northampton General Hospital Website: What is Painful Bladder (PBS) or Interstitial Cystitis (IC)? Interstitial Cystitis (IC) is a chronic inflammation of the bladder wall, which can also be diagnosed as Painful Bladder Syndrome (PBS) or Bladder Pain Syndrome (BPS). It is a disorder with symptoms of mild to severe bladder pain and an urgent and/or frequent need to urinate. How common is IC/PBS? There is an estimated 400,000 people in UK with IC/PBS, of whom 90% are females and 10% are males. What causes IC? The cause of IC/PBS is not yet known. Research continues to find the cause. Indications suggest the condition could be due to a defective bladder lining, or an autoimmune disorder. Normally, the lining protects the bladder wall from the toxic effects of urine. In about 70% of the people who have interstitial cystitis, the protective layer of the bladder is "leaky." This may let urine irritate the bladder wall, causing interstitial cystitis. Other possible causes may be an increase of histamine-producing cells in the bladder wall or an autoimmune response (when antibodies are made that act against a part of the body).ic/pbs may resemble a bacterial bladder infection, however short term antibiotics are not effective. What are the main symptoms of IC/PBS? People who have interstitial cystitis may have the following symptoms: An urgent need to urinate, (yet you may pass only very small amounts of urine each time) and increased frequency both in the daytime and during the night Pressure, pain and tenderness around the bladder, pelvis and perineum (the area between the anus and vagina). This pain and pressure may increase as the bladder fills and decrease as it empties in urination. A bladder that won't hold as much urine as it used to Pain during sexual intercourse
2 How can IC/PBS affect an individual's life? Many IC/PBS patients find that their life revolves around knowing where the nearest toilet is known as Toilet mapping. This can be very restricting. Going out of the house require thought and planning. Some severe sufferers of IC/PBS can find themselves virtually housebound. This leads to social isolation and depression. Interrupted sleep pattern due to frequency and urgency of urination throughout the night and pain causes tiredness and poor performance. Constant pain especially after sex can affect relationship. These issues are not easy to talk about so patients feel quite helpless about it. How is IC diagnosed? IC is diagnosed by elimination. If the symptoms are suggestive of IC, diagnostic tests such as Urodynamics (bladder pressure studies) or Cystoscopy (looking inside the bladder with telescope) are performed to rule out other similar conditions like overactive bladder. Repeated midstream urine samples might be checked to rule out bacterial cystitis. It can take time to obtain a correct diagnosis as symptoms of IC/PBS can be similar to other conditions. Painful Bladder Flares Patients suffering from IC have periods when symptoms are not bothersome and they can have almost normal life that alternate with periods when symptoms are bothersome or even severe. These periods are called flares. It is not always clear why flares develop. There are triggers that worsen symptoms. The potential triggers are Bladder infections Gastrointestinal problems Activities, such as sex and prolonged sitting Certain Foods and beverages, including alcohol and coffee Aggravating conditions such as bladder infections and yeast infections can worsen IC symptoms. Patients should see a healthcare provider to be evaluated and treated promptly for such conditions to avoid flare ups. Pain in other areas due to conditions like Crohn s disease, Ulcerative Colitis, diverticulitis, irritable bowel syndrome, painful menstrual periods or endometriosis should be treated vigorously as these conditions can increase bladder sensitivity. More than one healthcare provider or specialist is often needed for people who have multiple medical conditions. If you are able to identify foods or drinks that aggravate bladder pain or urinary urgency or frequency, it is reasonable to avoid these items during a symptom flare. However, it is not clear that these items should be avoided at other times. Some practitioners strongly
3 recommend a highly restrictive "interstitial cystitis diet", although its benefit has never been studied. (You can follow diet advice given by interstitial cystitis network, How is IC treated? As yet there is no cure for IC, so treatment approaches are designed to control symptoms. Each patient has his or her own unique subset of bothersome symptoms. Many a times you need specialist team to design therapies to alleviate each of your symptoms. Most people feel better after trying one or more of the following treatments: Diet. Your doctor may tell you to change what you eat. You may need to avoid alcohol, acidic foods and tobacco. Bladder distention. Under anesthesia, a doctor overfills your bladder with gas or fluid. This stretches the walls of the bladder. It is unexplained why distension helps. It may make your bladder be able to hold more urine. It may also interfere with the pain signals sent by nerves in the bladder. Bladder instillation for Interstitial Cystitis (also called a bladder wash or bath), a procedure in which the bladder is filled with a therapeutic solution (usually containing a combination of agents) that is retained in the bladder for varying periods of time, from a few seconds to 15 minutes, before it is released through urination. Doctors use treatments that are thought to either coat and protect the bladder or suppress inflammation. This can be done by a clinician or you can learn to self-administer the treatment at home. The treatment schedule varies but it can be for a single dose every month to up to three times a week or only with flare ups. The medicines used include Cystistat (sodium hyaluronate) and Uracyst (chondroitin). They are believed to replace the deficient GAG layer on the bladder wall. Medications for Interstitial Cystitis such as Elmiron (the first oral medication approved specifically for IC). Elmiron may reduce bladder discomfort and pain in some people with IC and may work by repairing the damaged bladder lining. Another oral medicine used to treat interstitial cystitis is an antihistamine called hydroxyzine. This medicine reduces the amount of histamine that is made in the bladder wall. Another medicine that may help is amitriptyline. It blocks pain and reduces bladder spasms. This medicine can make you sleepy, so it is usually taken at bedtime. Your doctor may also suggest that you take an over-the-counter pain medicine to ease pain. Transcutaneous posterior tibial nerve stimulation for Interstitial Cystitis in which doctors send mild electric pulses to a nerve in the foot through a small acupuncture needle. These pulses may work by increasing blood flow to the bladder, strengthening pelvic muscles that help control the bladder, and triggering the release of hormones that block pain. Bladder training for Interstitial Cystitis is a therapeutic technique where you void at designated times and use relaxation techniques and distractions to help keep to the schedule. Gradually, the patient tries to lengthen the time between the scheduled voids.
4 A typical bladder training protocol involves avoiding an urge and learning to urinate "by the clock". This is used throughout the day, but is not used while sleeping. As an example, if you currently void every 30 minutes, you will first try to urinate only once every 45 minutes during the daytime, whether you feel the need to urinate or not. You should not urinate more frequently than every 45 minutes, if possible. This voiding goal is continued for a full week or until you are comfortable with this interval. Once you are comfortable voiding every 45 minutes, you can increase your time interval by 15 to 30 minutes every week. In this example, you would urinate every 60 minutes for the second week, every 90 minutes for the third week, every 2 hours for the fourth week, and every 2.5 hours for the fifth week. Interstim for Interstitial Cystitis is a small pacemaker that sends impulses to the sacral nerve, which controls the bladder. Some patients with IC find that it helps relieve their frequency, but it is usually reserved for those who have not responded to other treatments. Doctors implant the pacemaker in two stages. During the first stage (an outpatient procedure) they insert a small lead or wire into the tailbone. The lead is connected to an external battery that delivers a small electrical impulse, and is worn for two to four weeks. If the patient improves during this time, urologists insert a small generator for the bladder into the upper buttock region. If the device is not helpful during the first stage, doctors remove the device at the second operation. Diet modification to treat Interstitial Cystitis may help alleviate symptoms because alcohol, tomatoes, spices, chocolate, caffeinated and citrus beverages, and high-acid foods can contribute to bladder inflammation, some physicians and patients believe. Although there is no scientific evidence linking diet to IC, eliminating these substances from the diet helps some people with IC. Smoking cessation to treat for Interstitial Cystitis is important because the chemicals in cigarette smoke can concentrate in the urine and irritate the bladder wall. Exercise to treat Interstitial Cystitis can help relieve IC symptoms in some people or even hasten remission. Alternative therapy can help to cope with chronic pain. Psychosocial support (psychotherapy) can be helpful in dealing with issues like stress, anxiety and depression associated with this long term condition. Relaxation techniques can relieve musculoskeletal tension, and may include meditation, progressive muscle relaxation, self-hypnosis, or biofeedback. Many patients with IC have tight and tender muscles and connective tissue in the pelvis, lower abdomen, thighs, groin, and buttocks. Pelvic floor physical therapy (PT) may be recommended to decrease tightness in these muscles. It can decrease bladder or pelvic pain as well as urinary urgency and frequency. This type of Physiotherapy is specialised requiring therapist specially trained in pelvic soft tissue manipulation and rehabilitation. Several small studies have demonstrated the benefit of PT for tight and tender pelvic muscles associated with IC. It is performed weekly for at least 12 weeks. You will also be given stretching exercises to perform at home. Most people begin to see improvement after six to eight sessions.
5 Treatment of painful bladder often depends upon a clinician's preferences and experience in treating the disorder and availability of different options rather than upon scientific studies because the cause of this condition is not clear. A number of treatments are available for PBS/IC, many of which are effective for at least some patients. Most patients with PBS/IC need to try more than one treatment, sometimes in combination, to find the one(s) that provides the greatest relief.
Interstitial Cystitis - Painful Bladder Syndrome
 Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Interstitial Cystitis - Painful Bladder Syndrome Interstitial cystitis (in-tur-stish-ul sis-tie-tis) also called painful bladder syndrome is a chronic condition in which you experience bladder pressure,
Painful Bladder Syndrome
 Painful Bladder Syndrome Department of Urology Patient Information What What is Painful is Painful Bladder Bladder Syndrome? Syndrome? Painful bladder syndrome also known as Interstitial Cystitis is a
Painful Bladder Syndrome Department of Urology Patient Information What What is Painful is Painful Bladder Bladder Syndrome? Syndrome? Painful bladder syndrome also known as Interstitial Cystitis is a
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
Interstitial Cystitis
 Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Interstitial Cystitis/ Bladder Pain Syndrome
 page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
page 1 Interstitial Cystitis/ Bladder Pain Syndrome Q: What is interstitial cystitis/bladder pain syndrome (IC/BPS)? A: Interstitial cystitis (int-uhr-stishuhl siss-tyt-uhss) (IC), is a chronic pain condition
URINARY INCONTINENCE
 Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
Center for Continence Care and Pelvic Medicine What is urinary incontinence? URINARY INCONTINENCE Urinary incontinence is the uncontrollable loss of urine. The amount of urine leaked can vary from only
WHAT IS INTERSTITIAL CYSTITIS?
 Patient Information WHAT IS INTERSTITIAL CYSTITIS? Interstitial Cystitis (IC) is a condition resulting in recurring discomfort or pain in the bladder and the surrounding pelvic region. Its cause is unknown,
Patient Information WHAT IS INTERSTITIAL CYSTITIS? Interstitial Cystitis (IC) is a condition resulting in recurring discomfort or pain in the bladder and the surrounding pelvic region. Its cause is unknown,
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information
 Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
Interstitial Cystitis (Chronic Pelvic Pain) Consultation Information Round Rock Jollyville Westlake Central office: Phone 512-231-1444 Fax 512-231-1470 www.urologyteam.com Rev June 2017 What is Interstitial
University College Hospital at Westmoreland Street. Percutaneous Tibial Nerve Stimulation (PTNS)
 University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
University College Hospital at Westmoreland Street Percutaneous Tibial Nerve Stimulation (PTNS) Urology Directorate If you need a large print, audio or translated copy of this document, please contact
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre
 PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
PATIENT INFORMATION HANDOUT Dr Joseph K Johnson KG Medical Centre Chronic Pelvic Pain What is Chronic Pelvic Pain? Chronic pelvic pain refers to pain in the lower half of your abdomen, lasting six months,
Advanced Care for Female Overactive Bladder & Urinary Incontinence. Department of Urology Kaiser Permanente Santa Rosa
 Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Advanced Care for Female Overactive Bladder & Urinary Incontinence Department of Urology Kaiser Permanente Santa Rosa Goals Participants will: Review normal urinary tract anatomy and function Understand
Overactive bladder syndrome (OAB)
 Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
Service: Urology Overactive bladder syndrome (OAB) Exceptional healthcare, personally delivered What is OAB? An overactive bladder or OAB is where a person regularly gets a sudden and compelling need or
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
Urogynecology in EDS. Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018
 Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Urogynecology in EDS Joan L. Blomquist, MD Greater Baltimore Medical Center August 2018 One in three like me Voiding Issues Frequency/Urgency Urinary Incontinence neurogenic bladder Neurologic supply
Chronic pelvic pain has many different characteristics. Signs and symptoms may include:
 Pelvic Pain in Women Pelvic pain in women refers to pain in the lowest part of your abdomen and pelvis. If asked to locate your pain, you might sweep your hand over that entire area rather than point to
Pelvic Pain in Women Pelvic pain in women refers to pain in the lowest part of your abdomen and pelvis. If asked to locate your pain, you might sweep your hand over that entire area rather than point to
Painful Bladder Syndrome/Interstitial Cystitis
 n The Leeds Teaching Hospitals NHS Trust Painful Bladder Syndrome/Interstitial Cystitis Information for patients Leeds Centre for Women s Health Welcome to the Department of Urogynaecology Your consultant
n The Leeds Teaching Hospitals NHS Trust Painful Bladder Syndrome/Interstitial Cystitis Information for patients Leeds Centre for Women s Health Welcome to the Department of Urogynaecology Your consultant
Incontinence. Anatomy The human body has two kidneys. The kidneys continuously filter the blood and make urine.
 Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Incontinence Introduction Urinary incontinence occurs when a person cannot control the emptying of his or her urinary bladder. It can happen to anyone, but is very common in older people. Urinary incontinence
Promoting Continence with Physiotherapy
 A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
A Common problem for Men and women Promoting Continence with Physiotherapy This leaflet contains information about physiotherapy advice and treatment for anyone with bladder and bowel problems. This may
Using Physiotherapy to Manage Urinary Incontinence in Women
 Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Using Physiotherapy to Manage Urinary Incontinence in Women Bladder control problems are common, and affect people of all ages, genders and backgrounds. These problems are referred to as urinary incontinence
Percutaneous Tibial Nerve Stimulation for Overactive Bladder Symptoms. Patient Information Leaflet
 Percutaneous Tibial Nerve Stimulation for Overactive Bladder Symptoms Patient Information Leaflet About this leaflet The information provided in this leaflet should be used as a guide. There may be some
Percutaneous Tibial Nerve Stimulation for Overactive Bladder Symptoms Patient Information Leaflet About this leaflet The information provided in this leaflet should be used as a guide. There may be some
THE OVER-ACTIVE BLADDER (OAB)
 THE OVER-ACTIVE BLADDER (OAB) Passage of urine is caused by the bladder muscle contracting coordinated with the relaxation of the sphincter muscles, which is controlled by higher centers in the central
THE OVER-ACTIVE BLADDER (OAB) Passage of urine is caused by the bladder muscle contracting coordinated with the relaxation of the sphincter muscles, which is controlled by higher centers in the central
A Review on Interstitial Cystitis Syndrome (ICS)
 31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
31 Review Article A Review on Interstitial Cystitis Syndrome (ICS) M Sushma*, TVV Vidyadhar, R Mohanraj, M Babu Department of Pharmacy Practice, Raghavendra Institute of Pharmaceutical Education & Research
Female Urinary Incontinence: What It Is and What You Can Do About It
 Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Female Urinary Incontinence: What It Is and What You Can Do About It Urogynecology Patient Information Sheet What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for example,
Uterus (Womb) Rectum. Another problem could be the sensation of something coming down at the birth canal or back passage (prolapse).
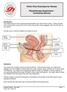 Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
Pelvic Floor Exercises for Women Physiotherapy Department Continence Service Introduction This leaflet tells you how to exercise and strengthen your pelvic floor muscles. These muscles form a broad sling
IMPROVING URINARY INCONTINENCE
 IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
IMPROVING URINARY INCONTINENCE INFORMATION FOR OLDER ADULTS, FAMILIES, AND CAREGIVERS READ THIS PAMPHLET TO LEARN: What Urinary Incontinence is. How to Manage Urinary Incontinence. What Pelvic Floor Exercises
Overactive bladder. Information for patients from Urogynaecology
 Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
Overactive bladder Information for patients from Urogynaecology An overactive bladder (OAB) is a very common problem. It can cause distressing symptoms that are difficult to control. These can include
Y0028_2726_0 File&Use Bladder Control Does Matter
 Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Y0028_2726_0 File&Use 04092012 Bladder Control Does Matter If you suffer from urinary incontinence, you re not alone Don t be afraid to raise your hand if you ve been struggling with the embarrassment
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Urinary Incontinence Q: What is urinary incontinence and what causes it? A: When you are not able to hold your urine until you can get to a bathroom, you have what s called urinary incontinence (also called
Overactive Bladder. When to see a doctor. Normal bladder function
 Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Overactive Bladder Overactive bladder is a problem with bladder-storage function that causes a sudden urge to urinate. The urge may be difficult to stop, and overactive bladder may lead to the involuntary
Patient Information Incontinence & Prolapse Self-help
 Patient Information Incontinence & Prolapse Self-help Urogynaecology Introduction This leaflet is produced as a self-help guide for women of East and North Herts that are experiencing issues with continence.
Patient Information Incontinence & Prolapse Self-help Urogynaecology Introduction This leaflet is produced as a self-help guide for women of East and North Herts that are experiencing issues with continence.
Chronic Pelvic Pain. AP099, December 2010
 AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
Sacral Nerve Stimulation (SNS) System Implantation
 Patient & Family Guide 2016 Sacral Nerve Stimulation (SNS) System Implantation www.nshealth.ca Sacral Nerve Stimulation (SNS) System Implantation SNS system implantation involves placing a lead ( leed,
Patient & Family Guide 2016 Sacral Nerve Stimulation (SNS) System Implantation www.nshealth.ca Sacral Nerve Stimulation (SNS) System Implantation SNS system implantation involves placing a lead ( leed,
Various Types. Ralph Boling, DO, FACOG
 Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Various Types Ralph Boling, DO, FACOG The goal of this lecture is to increase assessment and treatment abilities for physicians managing urinary incontinence (UI) patients. 1. Effectively communicate with
Tension Free vaginal tape. Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD
 Tension Free vaginal tape Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD What is a TVT procedure? A TVT (Tension Free Vaginal Tape) procedure is an operation
Tension Free vaginal tape Mrs Ami Shukla, Consultant Urogynaecologist Northampton General Hospital Northampton NN1 5BD What is a TVT procedure? A TVT (Tension Free Vaginal Tape) procedure is an operation
PELVIC PAIN QUESTIONNAIRE
 PELVIC PAIN QUESTIONNAIRE Name: DOB: / / Are you currently: Single Married Separated Divorced Re-married De-Facto Who do you live with? What type of employment are you currently in? How long? INFORMATION
PELVIC PAIN QUESTIONNAIRE Name: DOB: / / Are you currently: Single Married Separated Divorced Re-married De-Facto Who do you live with? What type of employment are you currently in? How long? INFORMATION
Overactive bladder can result from one or more of the following causes:
 Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
Overactive bladder can affect people of any age; however, it is more common in older people. Effective treatments are available and seeing your doctor for symptoms of overactive bladder often results in
URINARY INCONTINENCE FOR FALLS PREVENTION. by Susan Elms P.T. Elms Physiotherapy
 URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
URINARY INCONTINENCE PHYSIOTHERAPY MANAGEMENT FOR FALLS PREVENTION by Susan Elms P.T. Elms Physiotherapy OR How to avoid the mad dash to the bathroom! INCONTINENCE INFORMATION TALK What is incontinence?
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for women Introduction Many women suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine
Loss of Bladder Control
 BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
BLADDER HEALTH: Surgery for Urinary Incontinence Loss of Bladder Control Surgery for Urinary Incontinence Don t Let Urinary Incontinence Keep You from Enjoying Life. What is Urinary Incontinence? What
INTERSTITIAL CYSTITIS (IC)
 INTERSTITIAL CYSTITIS (IC) Painful Bladder Syndrome (PBS): THE BASIC FACTS ANDREW L. SIEGEL, M.D. Board-Certified Urologist and Urological Surgeon Specialty: Male and Female Incontinence, Voiding Dysfunction,
INTERSTITIAL CYSTITIS (IC) Painful Bladder Syndrome (PBS): THE BASIC FACTS ANDREW L. SIEGEL, M.D. Board-Certified Urologist and Urological Surgeon Specialty: Male and Female Incontinence, Voiding Dysfunction,
Multiple Sclerosis. What is multiple sclerosis? What is the cause? What are the symptoms?
 What is multiple sclerosis? Multiple Sclerosis Multiple sclerosis (MS) is a disease of the central nervous system (the brain and spinal cord). Many people with multiple sclerosis are only mildly affected
What is multiple sclerosis? Multiple Sclerosis Multiple sclerosis (MS) is a disease of the central nervous system (the brain and spinal cord). Many people with multiple sclerosis are only mildly affected
Urinary Incontinence
 Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Urinary Incontinence Q: What is urinary incontinence (UI)? A: UI is also known as loss of bladder control or urinary leakage. UI is when urine leaks out before you can get to a bathroom. If you have UI,
Bladder dysfunction in ALD and AMN
 Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Bladder dysfunction in ALD and AMN Sara Simeoni, MD Department of Uro-Neurology National Hospital for Neurology and Neurosurgery Queen Square, London 10:15 Dr Sara Simeoni- Bladder issues for AMN patients
Prostate surgery. What is the prostate? What is a TURP? Why is a TURP operation necessary? Deciding to have a TURP operation.
 What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
What is the prostate? The prostate is a gland about the size of a walnut that is only present in men. It is located just below the bladder and surrounds the urethra, the tube through which urine flows
Information about your operation: Sacral nerve stimulation (SNS)
 Information about your operation: Sacral nerve stimulation (SNS) Urogynaecology Unit Information for Patients i Important supplementary information What is an overactive bladder? Women with an overactive
Information about your operation: Sacral nerve stimulation (SNS) Urogynaecology Unit Information for Patients i Important supplementary information What is an overactive bladder? Women with an overactive
Interstitial cystitis
 Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
Interstitial cystitis Ilse Truter, PharmITCom Consulting Bladder Normal protective bladder lining Thinning of the protective bladder lining Pinpoint bleeding (glomerulations) on the bladder wall Hunner
INTERSTITIAL CYSTITIS (IC) MANAGEMENT
 INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
The Pelvic Floor Muscles - a Guide for Women
 The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
The Pelvic Floor Muscles - a Guide for Women This booklet is supported by WWWWW Wellbeing of Women Registered Charity No. 239281 www.wellbeingofwomen.org.uk Introduction Up to a third of all women experience
Patient Advice for Third & Fourth Degree Tears
 Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Patient Advice for Third & Fourth Degree Tears Please read this leaflet carefully. It is important that you take note of any instructions or advice given. If you have any questions or problems that are
Intravesical Botox Injections
 Intravesical Botox Injections Department of Urology Patient Information What What is is Botox? Botox? Botox or Botulinum Type-A is toxin produced by bacteria called Clostridium Botulinum. It is given intravesically
Intravesical Botox Injections Department of Urology Patient Information What What is is Botox? Botox? Botox or Botulinum Type-A is toxin produced by bacteria called Clostridium Botulinum. It is given intravesically
Toning your pelvic floor WELCOME
 Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Toning your pelvic floor WELCOME Introductions Amelia Samuels, Physiotherapist, Active Rehabilitation Physiotherapy Supporting the Continence Foundation of Australia Continence Foundation of Australia
Having a Ureteric Stent: What to expect and how to manage
 Having a Ureteric Stent: What to expect and how to manage This leaflet explains: In patients who have, or might have, an obstruction (blockage) of the kidney, an internal drainage tube called a stent is
Having a Ureteric Stent: What to expect and how to manage This leaflet explains: In patients who have, or might have, an obstruction (blockage) of the kidney, an internal drainage tube called a stent is
Stress incontinence -- occurs during certain activities like coughing, sneezing, laughing, or exercise.
 Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Urinary incontinence Definition Incontinence is the inability to control the passage of urine. This can range from an occasional leakage of urine, to a complete inability to hold any urine. The three main
Prostatitis - A straight forward guide to
 Prostatitis - A straight forward guide to inflammation of the prostate and Pelvic Pain Syndrome What is the prostate? Only men have a prostate and it is usually about the size of a walnut. Around the age
Prostatitis - A straight forward guide to inflammation of the prostate and Pelvic Pain Syndrome What is the prostate? Only men have a prostate and it is usually about the size of a walnut. Around the age
Patient Information. Basic Information on Overactive Bladder Symptoms. pubic bone. urethra. scrotum. bladder. vaginal canal
 Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Patient Information English Basic Information on Overactive Bladder Symptoms The underlined terms are listed in the glossary. What is the bladder? pubic bone bladder seminal vesicles prostate rectum The
Urinary Incontinence. a problem for many
 Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
Urinary Incontinence a problem for many This leaflet gives information on urinary incontinence and the problems arising from the various types of urinary incontinence. It also gives advice on how to relieve
PELVIC FLOOR MUSCLE TRAINING FOR WOMEN STRONG PELVIC FLOOR MUSCLES MEAN GOOD BLADDER AND BOWEL CONTROL WHAT ARE THE PELVIC FLOOR MUSCLES?
 06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
06 STRONG S MEAN WHAT ARE THE S? The floor of the pelvis is made up of layers of muscle and other tissues. These layers stretch like a hammock from the tailbone at the back, to the pubic bone at the front.
Loss of Bladder Control
 BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH: Bladder Prolapse Loss of Bladder Control Bladder Prolapse Don t Let Bladder Prolapse Keep You from Enjoying Life. What is the Bladder? The bladder is a hollow, balloon-like organ made mostly
At the outset, we want to clear up some terminology issues. IBS is COPYRIGHTED MATERIAL. What Is IBS?
 1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
1 What Is IBS? At the outset, we want to clear up some terminology issues. IBS is the abbreviation that doctors use for irritable bowel syndrome, often when they are talking about people with IBS. We will
Physiotherapy advice following your third or fourth degree perineal tear
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Provenance Rehabilitation Pelvic Intake Form
 Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Outpatient Rehabilitation Services
 Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
Outpatient Rehabilitation Services Shapiro Building, 2nd Floor 330 Brookline Avenue Boston, MA 02215 (617) 754-9100 bidmc.org/pelvicfloorpt Outpatient Rehabilitation Services ALL ABOUT YOUR Pelvic Floor
Oxford Pelvic Floor Services A guide to the pelvic floor muscles. Information for men
 Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Oxford Pelvic Floor Services A guide to the pelvic floor muscles Information for men Introduction Many men suffer from weakness of their pelvic floor muscles. Common symptoms include: leaking urine with
Pelvic Pain Assessment Form
 Pelvic Pain Assessment Form Physician: Initial History and Physical Examination Date: This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Pelvic Pain Assessment Form Physician: Initial History and Physical Examination Date: This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery
 Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
Loyola University Medical Center Female Pelvic Medicine & Reconstructive Surgery Medical History Questionnaire Name: Date: Age: D.O.B. Race: What is the nature of your current gynecologic or urologic medical
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors
 DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
DIAPPERS: Transient Causes of Urinary Incontinence and other contributing factors D Delirium Acute confusion alters one s ability to anticipate and meet own needs. Delirium may occur from drugs, surgery,
Pelvic Pain Assessment Form
 Pelvic Pain Assessment Form Physician : Date: Initial History and Physical Examination This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Pelvic Pain Assessment Form Physician : Date: Initial History and Physical Examination This assessment form is intended to assist the clinician with the initial patient assessment and is not meant to be
Pelvic organ prolapse
 Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Page 1 of 11 Pelvic organ prolapse Introduction The aim of this leaflet is to give you information about a pelvic organ prolapse, its causes and available treatments but does not replace advice given by
Irritable Bowel. Syndrome. Health Promotion Service
 The information in this leaflet is not intended to replace the knowledge or diagnosis of a qualified health practitioner. We encourage you to consult a health professional and ensure your IBS is properly
The information in this leaflet is not intended to replace the knowledge or diagnosis of a qualified health practitioner. We encourage you to consult a health professional and ensure your IBS is properly
Bladder pain syndrome / Interstitial cystitis
 Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Bladder pain syndrome / Interstitial cystitis Terminology The term bladder pain syndrome/interstitial cystitis (BPS/IC) is defined as the presence of chronic pain, pressure, or pelvic discomfort lasting
Pelvic Floor Muscle exercises and Bladder advice
 n The Leeds Teaching Hospitals NHS Trust Pelvic Floor Muscle exercises and Bladder advice Information for patients Leeds Centre for Women s Health This leaflet aims to explain about your pelvic floor muscles,
n The Leeds Teaching Hospitals NHS Trust Pelvic Floor Muscle exercises and Bladder advice Information for patients Leeds Centre for Women s Health This leaflet aims to explain about your pelvic floor muscles,
Pelvic Floor Exercises
 Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Directorate of Women, Children and Surgical Services Burton and District Urogynaecology Centre A Nationally Accredited Urogynaecology Unit Pelvic Floor Exercises You have been given this leaflet because
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
BLADDER HEALTH Loss of Bladder Control SURGERY TO TREAT URINARY INCONTINENCE AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is Urinary Incontinence? Urinary incontinence
Top 10 Tips Bladder Control
 Top 10 Tips Bladder Control for Your Personal Guide to a Sensitive Bladder Dr. Mache Seibel Leading authority on women s wellness and menopause Message from Dr. Mache Seibel Thank you for downloading this
Top 10 Tips Bladder Control for Your Personal Guide to a Sensitive Bladder Dr. Mache Seibel Leading authority on women s wellness and menopause Message from Dr. Mache Seibel Thank you for downloading this
Physiotherapy advice following your vaginal birth
 Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Further sources of information NHS Choices: www.nhs.uk/conditions Our website: www.sfh-tr.nhs.uk INFORMATION FOR PATIENTS Patient Experience Team (PET) PET is available to help with any of your compliments,
Long-term pelvic pain:
 Long-term pelvic pain: information for you aashara Published November 005 by the RCOG Title amended October 00 Contents Page number Key points 1 About this information What is long-term pelvic pain? What
Long-term pelvic pain: information for you aashara Published November 005 by the RCOG Title amended October 00 Contents Page number Key points 1 About this information What is long-term pelvic pain? What
FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT
 URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
URO-GYNECOLOGY PATIIENT IINFORMATIION SHEET FEMALE URINARY INCONTINENCE: WHAT IT IS AND WHAT YOU CAN DO ABOUT IT What is Urinary Incontinence? Stress Incontinence is a leakage of urine that occurs, for
DELAYED DIAGNOSIS. Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >60%
 DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
DELAYED DIAGNOSIS Mean time to diagnosis = 4-7 years Mean # of physicians = 8 NIDDK criteria underdiagnoses >6% 1 PREVALENCE 1,, 9,, 8,, 7,, 6,, 5,, 4,, 3,, 2,, 1,, NHS "Prostatitis" "Endometriosis" The
Loss of Bladder Control
 BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
BLADDER HEALTH Loss of Bladder Control Bladder Prolapse AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION What Is the Bladder? The bladder is a hollow, balloon-like organ made mostly
Radiotherapy to the pelvis. (bladder, prostate, rectum)
 Radiotherapy to the pelvis (bladder, prostate, rectum) General advice Everyone having radiotherapy is different. Your treatment is specific to you and so is the way you react to treatment. If you are worried
Radiotherapy to the pelvis (bladder, prostate, rectum) General advice Everyone having radiotherapy is different. Your treatment is specific to you and so is the way you react to treatment. If you are worried
ARTIFICIAL MESH REPAIR FOR TREATMENT OF PELVIC ORGAN PROLAPSE
 Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Pelvic Floor Unit / Department of Gynaecology Ward 17, Singleton Hospital, Sketty, Swansea, SA2 8QA 01792 205666 Secretary Direct Line: 01792 285688. Fax: 01792 285874 ARTIFICIAL MESH REPAIR FOR TREATMENT
Women s & Children s Directorate The TVT Operation - a guide for patients
 Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
Women s & Children s Directorate The TVT Operation - a guide for patients This leaflet was written for women who are considering having a TVT operation. If you have any questions that aren't answered by
InterStim CONSULTATION INFORMATION.
 InterStim CONSULTATION INFORMATION www.urologyaustin.com The Urinary System Making An Informed Decision How Does The Urinary System Work? To understand how sacral nerve stimulation works, it is helpful
InterStim CONSULTATION INFORMATION www.urologyaustin.com The Urinary System Making An Informed Decision How Does The Urinary System Work? To understand how sacral nerve stimulation works, it is helpful
Radiotherapy to the male pelvis. Information and advice for patients, relatives and carers
 Radiotherapy to the male pelvis Information and advice for patients, relatives and carers Introduction This leaflet is a guide to radiotherapy treatment to the male pelvis and outlines a range of possible
Radiotherapy to the male pelvis Information and advice for patients, relatives and carers Introduction This leaflet is a guide to radiotherapy treatment to the male pelvis and outlines a range of possible
GI Physiology - Investigating and treating patients with pelvic floor dysfunction. Lynne Smith Department of GI Physiology NGH Sheffield
 GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
GI Physiology - Investigating and treating patients with pelvic floor dysfunction Lynne Smith Department of GI Physiology NGH Sheffield Aims o o o To give an overview of lower GI investigations To demonstrate
TYPES OF PROSTATITIS There are three types of prostatitis-type presentations:
 SPECIALIZED UROLOGIC CONSULTANTS, SC 10400 Southwest Hwy 16632 S. 107 th Ct. Chicago Ridge, IL 60453 Orland Park, IL 60467 Tel (708) 423-8706 Tel (708) 349-6350 PROSTATITIS - REVIEW Prostatitis is an inflammation
SPECIALIZED UROLOGIC CONSULTANTS, SC 10400 Southwest Hwy 16632 S. 107 th Ct. Chicago Ridge, IL 60453 Orland Park, IL 60467 Tel (708) 423-8706 Tel (708) 349-6350 PROSTATITIS - REVIEW Prostatitis is an inflammation
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment
 Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Managing Symptoms after Prostate Cancer Urine Leaks after Prostate Cancer Treatment Urine leaks after surgery or radiation for prostate cancer are common. The medical term for this is incontinence (say:
Pelvic floor weakness
 Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Information leaflet for patients Pelvic floor weakness Physiotherapy department You have been referred to this department for treatment and advice because you have one or more of the following symptoms:
Gynaecology Department Patient Information Leaflet
 Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Vaginal repair Gynaecology Department Patient Information Leaflet Introduction This leaflet gives information about vaginal repair surgery used to treat a vaginal prolapse. The leaflet explains what a
Having a Ureteric Stent What to expect and how to manage
 Service: Urology Having a Ureteric Stent What to expect and how to manage Exceptional healthcare, personally delivered Introduction In patients who have, or might have, an obstruction (blockage) of the
Service: Urology Having a Ureteric Stent What to expect and how to manage Exceptional healthcare, personally delivered Introduction In patients who have, or might have, an obstruction (blockage) of the
Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises
 MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
MALE LUTS/CUP_11_11 Male Lower Urinary Tract Symptoms: Lifestyle Advice, Bladder Training and Pelvic Floor Exercises Lower urinary tract symptoms (LUTS) include the need to pass water very frequently (frequency)
Fibromyalgia summary. Patient leaflets from the BMJ Group. What is fibromyalgia? What are the symptoms?
 Patient leaflets from the BMJ Group Fibromyalgia summary We all get aches and pains from time to time. But if you have long-term widespread pain across your whole body, you may have a condition called
Patient leaflets from the BMJ Group Fibromyalgia summary We all get aches and pains from time to time. But if you have long-term widespread pain across your whole body, you may have a condition called
Insomnia. F r e q u e n t l y A s k e d Q u e s t i o n s
 Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Insomnia Q: What is insomnia? A: Insomnia is a common sleep disorder. If you have insomnia, you may: Lie awake for a long time and have trouble falling asleep Wake up a lot and have trouble returning to
Patient Information. Tension Free Vaginal/ Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust
 Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Tension Free Vaginal/Obturator Tape (TVT) Royal Devon and Exeter NHS Foundation Trust Patient Information Tension Free Vaginal/ Obturator Tape (TVT) Reference Number: CW 08 011 003 (version date: September
Voiding Diary. Begin recording upon rising in the morning and continue for a full 24 hours.
 Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
Urodvnamics Your physician has scheduled you for a test called URODYNAMICS. This test is a series of different measurements of bladder function and can be used to determine the cause of a variety of bladder
1st stage neuromodulation test
 1st stage neuromodulation test Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 12 This leaflet is to give you some background information
1st stage neuromodulation test Information for patients Urology PROUD TO MAKE A DIFFERENCE SHEFFIELD TEACHING HOSPITALS NHS FOUNDATION TRUST page 2 of 12 This leaflet is to give you some background information
Your guidebook for getting results with Medtronic Bladder Control Therapy Delivered by the NURO System TAKE BACK CONTROL.
 Your guidebook for getting results with Medtronic Bladder Control Therapy Delivered by the NURO System TAKE BACK CONTROL. RESET. RESTORE. * REGAIN CONTROL. Congratulations! You ve decided to try a therapy
Your guidebook for getting results with Medtronic Bladder Control Therapy Delivered by the NURO System TAKE BACK CONTROL. RESET. RESTORE. * REGAIN CONTROL. Congratulations! You ve decided to try a therapy
Bladder retraining - treatment for urgency and urge incontinence
 Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Bladder retraining - treatment for urgency and urge incontinence This leaflet explains what urge incontinence is and how we can help to reduce and relieve your symptoms. If you have any questions or concerns,
Considering Your Non-opioid Options for Pain
 YOUR VALUES YOUR PREFERENCES YOUR CHOICE Considering Your Non-opioid Options for Pain Self-Care, Chiropractic, Physical Therapy, Acupuncture and Pain Rehabilitation 2 Managing Your Pain: Options Pain If
YOUR VALUES YOUR PREFERENCES YOUR CHOICE Considering Your Non-opioid Options for Pain Self-Care, Chiropractic, Physical Therapy, Acupuncture and Pain Rehabilitation 2 Managing Your Pain: Options Pain If
ONE IN THREE WOMEN WHO EVER HAD A BABY WET THEMSELVES EVERY WOMAN WHO HAS HAD A BABY SHOULD DO PELVIC FLOOR MUSCLE TRAINING.
 08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
08 EVERY WOMAN WHO HAS HAD A BABY SHOULD Women who have even just one baby are nearly three times more likely to leak urine and wet themselves, than women who have not had a baby. The more babies you have,
