Transforaminal Lumbar Interbody Fusion Clinical and Radiologic Results and Complications in 50 Consecutive Patients
|
|
|
- Delphia Logan
- 5 years ago
- Views:
Transcription
1 Med. J. Cairo Univ., Vol. 80, No., March: 5-0, 0 Transforaminal Lumbar Interbody Fusion Clinical and Radiologic Results and Complications in 50 Consecutive Patients MOHAMED Y. EL-QAZAZ, M.D., Ph.D. and TARIQ ELEMAM ELSHAFEY, M.D., Ph.D. The Department of Neurosurgery, Faculty of Medicine, Suez Canal University, Ismailia, Egypt Abstract Objectives: To assess fusion rate and clinical outcomes in patients with degenerative segmental instability who were operated by transforaminal lumbar interbody fusion. Methods: Fifty consecutive adult patients were analyzed. Patient participation was based on the presence of degenerative segmental instability. They were operated for instrumented spinal stabilization with screws and TLIF between February 007 and September 0. Participants were evaluated preoperatively and post-operatively at,6,9, and month intervals. Pain was scored by a VAS for both lower limb and back pain both preoperatively and postoperatively. The clinical outcomes were assessed using the Prolo economic and functional rating scale and the fusion status was assessed using radiological criteria. Results: A total of 50 patients were included. Patients had preoperative symptoms duration for. ±. years. Of the 50 patients, 4 underwent single-level fusion: Seven patients underwent a two-level fusion and one patient underwent a three-level fusion from L-S. The average hospital stay was 4.7±.8 days. By months follow-up period, 74% of the study group expressed clinical success. Seventy percent of patients were considered to have undergone successful fusion. Conclusions: TLIF is safe, fusion rate is high and patient outcome compares favorably to literature series. Proper patient selection remains the key to satisfactory spinal fusion outcome. Key Words: Degenerative disc disease Transforaminal lumbar interbody fusion (TLIF) Spinal stabilization Spinal fusion Segmental instability. Introduction LUMBAR interbody fusion has many advantages over other forms of stabilization and fusion. An interbody graft is better suited to resist axial loads, Abbreviations used in this paper: LBP = Low back pain. TLIF = Transforaminal lumbar interbody fusion. PLIF = Posterior lumbar interbody fusion. VAS = Visual analogue scale. Correspondence to: Dr. Mohamed Youssef El-Qazaz, myalqazaz@hotmail.com prevent movement across a motion segment, and provide structural support because the graft is placed in vicinity of the instantaneous axis of rotation. Despite theoretical advantages of an interbody fusion, whether one type of the interbody graft or implant is superior to the other in terms of fusion rate and, more important, clinical outcome is an area of great debate []. In 98, Harms and Rolinger [] suggested the placement of bone graft, via a transforaminal route, into disc space that previously had been distracted using pedicle screw instrumentation (transforaminal lumbar interbody fusion [TLIF]). Such an approach can be accomplished without exposing more than the ipsilateral foramen, and retraction on the thecal sac is minimal. This approach can be particularly advantageous in the face of scarring after prior surgery. Moreover, the pedicle screw construct can be used dynamically to restore lumbar lordosis, while maintaining disc height with bone graft [- 5]. The ability to achieve a circumferential fusion, without substantial risk to neurological function or the need for sequential operations, would significantly broaden surgical options in the treatment of degenerative disease of the lumbar spine [6,7]. We present our clinical experience using the TLIF procedure, focusing on technique, clinical and radiological outcomes and safety. Material and Methods This study was designed as prospective, clinical study. Patients were selected to receive TLIF in an instrumented lumbar fusion. Between February 007 and September 0, at Suez Canal University Hospital (Ismailia, Egypt) a total of 50 consecutive patients indicated for TLIF with screw fixation were included. 5
2 6 Transforaminal Lumbar Interbody Fusion Clinical & Radiologic Inclusion criteria required all patients to present with degenerative segmental instability on clinical and radiological basis. Patients may have degenerative disc disease, degenerative spondylolisthesis or retrolisthesis (grade or ), previous laminectomy or discectomy, Pseudoarthrosis after other types of lumbar spine fusion. Patients should have been unresponsive to conservative management for a minimum of months. Exclusion criteria ruled out patients with general diseases that preclude surgical management (severe osteoporosis, immune suppression, malignancy and active local and/or systemic infection). Patients with morbid obesity as measured by body mass index >40, with spondylolisthesis of grades higher than grade or with epidural scarring and prior CSF leak were also excluded. Surgical technique: Patients are operated under general anesthesia in the prone position, to maintain the lumbar lordosis. Posterior midline incision is done extending slightly beyond the levels to be approached, followed by subperiostal dissection of the muscles until complete exposure of the transverse processes. Posterior decompression of the canal and vertebral foramen, as far as necessary is done. Unilateral resection of the inferior articular facet of the superior vertebra and the superior articular facet of the inferior vertebra is accomplished exposing unilaterally the intervertebral foramen. Then We Expose the posterolateral portion of the ipsilateral disc space in the topography of the vertebral foramen. Coagulation (with bipolar) of the small epidural vessels, and visualization and protection of the dura medially was followed. Pedicle screws are placed in the standard fashion followed by removal of the disc through the vertebral foramen, and also of the end plates. We distract the involved segment using rod over the screws on the opposite side, then completing the removal of the cartilagenous material inside the disc space. Harvested local bone combined with corticocancellous iliac crest autograft is packed in the disk space transforaminally. Final rods of desired length were contoured to the appropriate lordotic curve and are applied over the pedicle screws in compression. A drainage catheter is inserted. Facial, subcutaneous, and skin layers are closed. Post-operative care: The patients were advised to begin to walk one day after the surgery, wearing vest or elastic belt for comfort for months, and were usually discharged on the third or fourth day after surgery. We prescribed analgesic and muscle relaxant, and we avoided the use of anti inflammatory and tobacco. Perioperative data: Duration of surgery, blood loss, and duration of inpatient treatment were recorded. Intraoperative and perioperative complications were assessed. Clinical follow-up: Patients were followed weeks,,6,9 and months after surgery. During follow-up visit the following data were collected: Location of pain; intensity of leg and back pain according to the VAS; neurological symptoms; pain medication, complications, subsequent spinal surgery and assessment of the patient economic (activity) and functional (pain) statuses were assessed and the clinical outcome was evaluated using the Prolo economic and functional rating scale (Table ), in which there is a maximum score of 0 points. (Poor, -4; fair, 5-6; good, 7-8; and excellent, 9-0 points). Good and excellent results were considered a clinical success [8-0]. Finally patients were asked to rate their condition as improved, unchanged, or worse; they were also questioned as to whether they would undergo the same procedure again under the same circumstances. Radiological follow-up: Radiological fusion was assessed at individual levels as observed on plain radiographs that were obtained postoperatively every months to evaluate fusion. Radiological fusion was assessed according to the criteria approved by the FDA for evaluation of lumbar intervertebral fusions. (Table ) Fusion was defined as a continuous bone bridge between the vertebrae seen in at least one sagittal reconstruction []. Results Preoperative data: A total of 50 patients were included in this study. The demographic data of the study group are presented in (Table ). On average, patients had preoperative symptoms duration for. ±. years (range -0) (Table ). According to indication for surgery, patients may be separated into three subgroups. Group consisted of 4 patients with no history of surgery but with evidence of translational instability on preoperative radiographs. Group contained 7 patients with neither a history of surgery nor the presence of spondylolisthesis but with signs of degenerative disc disease. Group contained 9
3 Mohamed Y. Al-Qazaz & Tariq E. Elshafey 7 patients who had already undergone disc surgery or posterolateral fusion. A total of 58 levels were surgically treated. Of the 50 patients, 4 (84%) underwent singlelevel fusion: L4-5 ( patients), L-4 (8 patients) and L5-S ( patients). Seven (4%) patients underwent a two-level fusion: L-L5 (4 cases) and L4-S ( cases). One patient underwent a threelevel fusion from L-S. The mean values of preoperative back pain as determined by VAS (0-0) were 7.7 ±0.. The mean values of radicular pain were 8. ±.4. The mean values of preoperative economic and functional state as determined by Prolo Scale (-0) were 5. ±0.7. Perioperative data: The average operating time was 75 ±40 minutes. Average blood loss in the study group was 00± 60cm. The average hospital stay was 4.7±.8 days. Clinical outcome: In the study group, at year follow up and in comparison to the preoperative level, the mean back pain on VAS decreased significantly to.6±0.4 (range 0-6) (p<0.0) and the mean lower limb pain on VAS also decreased significantly to.5 ±0.5 (range 0-4) (p<0.0). When the outcome was evaluated by more objective means, such as the Prolo economic and functional scale, 4% ( of 50) of all the patients experienced excellent results, 50% (5 of 50) had good results, 4% ( of 50) had fair results, and 6% ( of 50) had poor results. Clinical success was considered if the patient got good or excellent score on Prolo scale ( 7 points). By months follow up period, 74% of the study group expressed clinical success. In months follow-up visit, when the patients were asked if, under the same circumstances, they would undergo the procedure again, 8% of the patients (4 patients) answered affirmatively and this is reflects their satisfaction with the results of their surgeries. Fusion outcome: Of a total of 58 levels evaluated, 7.4% (4 of 58) of these were radiographically shown to have fused at months follow-up according to the criteria mentioned in Table (). We considered a fusion to be successful in one patient when all the operated levels were fused. Seventy percent of patients were considered to have undergone successful fusion. The distribution of successful fusion was as follows: At L-4, 9 of levels; at L4-5, of 8; and at L5-S, of 7. The distribution of successful fusion for the level of the construct was as follows: One-level construct: of 4; two-level construct: of 7; and three-level construct none of one. Association between the clinical and the fusion outcomes: The fusion status was associated with the clinical outcome in the whole series. This is clear as 5/7 of patients who achieved clinical success showed fusion at months follow-up and all of the patients who achieved clinical failure showed non-fusion at months follow-up. Table (): Prolo functional economic rating scale [,]. Score Economic status: E E E E4 E5 Functional status: F F F F4 F5 Description Complete invalid No gainful occupation (including ability to do housework or continue retirement activities) Able to work but not at previous occupation Working at previous occupation on parttime or limited basis Working at previous occupation w/no restrictions of any kind Total incapacity (or worse than preoperative) Mild to moderate level of LBP &/or sciatica (or pain same as pre-operative but able to perform all daily tasks of living) Low level of pain & able to perform all activities except sports No pain, but has had or more recurrences of LBP or sciatica Complete recovery, no recurrent LBP, & able to perform all previous sports activities Table (): Radiographic observations of fusion [4]. Fusion failure 0 = No fusion done. = Collapse of construct. = Resorption of graft. = Large lucency (> mm) around entire graft. 4 = Small lucency (< mm) partially around graft. Fusion success 5 = Bone bridging fusion area. 6 = Increased density of bone. 7 = Continuous trabecular bone bridging the fusion bed.
4 8 Transforaminal Lumbar Interbody Fusion Clinical & Radiologic Table (): Demographic data, primary indication for surgery and surgically treated disc levels in the operated group of patients. Gender: Male Female Mean age/years Age group: Age 0- Age 40- Age 50- Age 60- Occupation: Light-duty work Heavy-duty work Smoking: Non-smokers Smokers Secondary Gain Issue Body mass index: * Average Non-obese Obese Previous Lumbar Surgery Diagnosis primary indication for surgery ( per patient): Degenerative spondylolisthesis Degenerative retrolisthesis Degenerative disc disease Recurrent disc herniation Pseudoarthrosis after fusion Surgically treated disc levels: One-Level Fusion L-4 L4-5 L5-S Two-Level Fusion: L-5 L4-S Three-Level Fusion: L-S Total Number of Operated levels Mean Preoperative Symptoms Duration/ Years drop postoperatively and was partially improved with physiotherapy. Five misplacement of the traspedicular screws were recorded. (Table 4) This was adjusted by repositioning of the trajectory or insertion of larger size pedicle screw if the pedicle 7 is partially violated. 49.5±9. B- Early postoperative complications: Seven neurological complications were record- 7 9 ed. Five of these were radicular pain and dysthesia 5 that had resolved within - months. Two patients 9 suffered increasing motor deficit. One of them was described before due to root injury and the other 40 one suffered added weakness of the extensor Hal- 0 lucis longus tendon that improved over the follow up. There were five superficial wound infections 4 and deep infection that required culture and 9 treatment with intravenous antibiotics. Also one 5 patient suffered iliac crest wound infection. One patient experienced postoperative DVT and the 8.4± ±. * Obesity is defined as BMI that is higher than 7.5 of the body mass index. Complications: Complications in the study group (Table 4) are divided into: A- Intraoperative complications: Three dural tears were recorded. Dural tears were repaired primarily, not requiring reoperation but prolonged the hospital stay. One patient suffered intraoperative L5 root injury during insertion of the graft. The patient developed added partial foot patient improved with the standard anticoagulation therapy. C- Late postoperative complications during the follow-up period: Three patients suffered continuous low back pain. In addition, patients needed further surgical interventions due to failure of the system of fixation. Collapse of the construct was also noted in patients most probably was caused by small amount of the bone graft in the disc space. Table (4): Complications recorded in the study group. Complications Intraoperative complications: Dural tear Root injury Hard ware related complications: Screws misplacement Early postoperative complications: Neurological complications: Radicular pain and dysthesia Increased Motor weakness Sphincter disturbance Infection: Superficial wound infection Deep wound infection Iliac crest wound infection DVT: Late postoperative complications during the follow-up: Continuous low back pain Hard ware complications: Broken Transpedicular screws Broken rod of fixation Collapse of intervertebral space No
5 Mohamed Y. Al-Qazaz & Tariq E. Elshafey 9 Fig. (): Preoperative radiology of 57-year-old male patient. To the left, MRI lumbosacral spine, T-weighted image with degenerative spondylolisthesis of the L-4 and L4-5 levels. To the right Postoperative months follow-up plain X- ray lumbosacral spine, lateral view, with transpedicular screw fixation L-5 and TLIF in both levels. There is continuous bone bridging the fusion bed. Fig. (): Preoperative radiology of a 45 year old female patient. To the left, MRI lumbosacral spine, T-weighted image with degenerative disc the L4-5 level. In the middle plain X-ray lumbosacral spine, lateral view with anterior sublaxation of the L4 vertebra over the L5. To the right, Postoperative months follow-up plain X-ray lumbosacral spine, lateral view, with transpedicular screw fixation L4-5 and TLIF. Discussion There are several different techniques of lumbar circumferential fusion. Among those, ALIF, PLIF, and more recently TLIF. In these techniques, ALIF is done through anterior approach, while PLIF and TLIF are done posteriorly. The difference is that in PLIF the access to the disc is through the canal, and in TLIF is through the inferior portion of the neurovertebral foramen. The TLIF arose as an improvement of PLIF, access sing the intervertebral disc through the far lateral portion of the vertebral foramen, by avoiding access to the disc through the vertebral canal, close to the dural sac and nerves. Lowe and Tahermia [] evaluated the cases of 40 patients operated by the TLIF technique. Twenty three patients had DDD, had spondylolysis and 4 had recurrent disc herniation. In 4 cases the arthodesis was limited to one level and in 6 it cases was done in levels. Radiological fusion was demonstrated in 95% of the cases. The clinical result was good to excellent in 88% of the patients.
6 0 Transforaminal Lumbar Interbody Fusion Clinical & Radiologic Two patients had pseudo-arthodesis and one had transitory neuropraxia. Humphreys et al. [] made a comparative study of 4 PLIF with 40 TLIF cases. Of the 4 PLIF procedures, were single level, 0 were double level and was triple level. Of the 40 TLIF, 7 were single and were double level. There were no complications with the TLIF patients. However, with the PLIF, there were 4 cases of radiculitis, case of broken hardware, case of screw loosening, cases of screw removal, nonunion requiring additional fusion, and superficial wound infection. The authors concluded that the TLIF showed to be a good alternative to PLIF with relatively less risk of complications, less operating time and hospitalization, as well as significant reduction in blood loss during operation. Hence, TLIF offers the advantage of being an efficient circumferential arthodesis through single access with the minimum risk of neural and dural lesion. At the same time, it allows posterior and foraminal decompression. Therefore, we believe that this technique should be promoted and properly employed in selected cases, especially when posterior decompression and circumferential interbody fusion of the lumbar region are necessary, as well as in many cases of DDD, recurrent disc herniation, spinal stenosis and low grade spondylolisthesis [4]. Our cases show a good experience with TLIF. Evaluation of the patients during the first 8 to 8 months after surgery showed improvement in 70% of the cases. Therefore, we believe that this technique should be promoted and properly employed in selected cases, especially when posterior decompression and circumferential fusion of the lumbar region are necessary. TLIF demonstrated its efficiency in treating cases of chronic lumbar pain with or without radiation to lower limbs, from DDD, recurrent disc herniation, low grade spondylolisthesis and iatrogenic segmental instability, especially when posterior decompression of the canal and vertebral foramen is indicated. The use of this technique should be encouraged to be performed by spine surgeons. References - EGGER E., GOTTSAUNER-WOLF F., PALMER J., et al.: Effects of axial dynamization on bone healing. J. Trauma, 4: 85-9, HARMS J. and ROLINGER H.: A one-stage procedure in operative treatment of spondylolistheses: Dorsal traction-reposition and anterior fusion [in German]. Z. Orthop. Ihre. Grenzgeb., 0: 4-47, AGAZZI S., REVERDIN A., MAY D.: Posterior lumbar interbody fusion with cages: An independent review of 7 cases. J. Neurosurg. (Spine ), 9: 86-9, BAKER J.K., REARDON P.R., REARDON M.J. and HEGGENESS M.H.: Vascular injury in anterior lumbar surgery. Spine, 8: 7-0, BENZEL E.C.: Ventral exposures of the lumbar spine, in Benzel E.C. (ed): Surgical Exposure of the Spine: An Extensile Approach. Park Ridge, AANS, pp 99-6, FRASER R.D.: Interbody, posterior, and combined lumbar fusions. Spine 0 (Suppl 4): 67S-77S, GROB D., SCHEIER H.J., DVORAK J., SIEGRIST H., RUBELI M. and JOLLER R.: Circumferential fusion of the lumbar and lumbosacral spine. Arch. Orthop. Trauma. Surg., : 0-5, CHRISTENSEN F.B. and BUNGER C.E.: Retrograde ejaculation after retroperitoneal lower lumbar interbody fusion. Int. Orthop., : 76-80, HALVORSON T.L., KELLEY L.A., THOMAS K.A., WHITECLOUD T.S. III and COOK S.D.: Effects of bone mineral density on pedicle screw fixation. Spine, 9: 45-40, PROLO D.J., OKLUND S.A. and BUTCHER M.: Toward uniformity in evaluating results of lumbar spine operations. A paradigm applied to posterior lumbar interbody fusions. Spine, : , BRANTIGAN J.W.: Carbon fiber I/F Cage system for interbody vertebral Fusion. In Haid RW, Mclaughlin MR, Fessler RG. Lumbar Interbody Fusion Techniques. Cages, Dowels, and Grafts. Quality Medical publishing, Inc. ST. Louis, Missori. Ch., 9: pp 47-7, LOWE T., TAHERNIA A.D.: Unilateral transforaminal posterior interbody fusion. Scoliosis Research Society Annual Meeting, San. Diego, CA, HUMPHREYS S.C., HODGES S.D., PATWARDHAN A.G., ECK J.C., MURPHY R.B. and COVINGTON L.A.: Comparison of posterior and transforaminal approaches to lumbar interbody fusion. Spine, 6: , TRIBUS C.B.: Circumferential fusion techniques. In Resnick D.K., Haid R.W. (eds). The surgical management of low back pain. American Association of Neurological Surgeon, 7-, 00.
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012
 Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Interspinous Fusion Devices. Midterm results. ROME SPINE 2012, 7th International Meeting Rome, 6-7 December 2012 Posterior distraction and decompression Secure Fixation and Stabilization Integrated Bone
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis
 Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
Acta Orthop. Belg., 2008, 74, 667-671 ORIGINAL STUDY Unilateral transforaminal lumbar interbody fusion (TLIF) using a single cage for treatment of low grade lytic spondylolisthesis Mohamed Adel EL MASRY,
Audat Z 1, MB, CHSM, Moutasem O 1, MB, CHSM, Yousef K 2, MB, ScD, Mohammad B 3, MB, CHSM INTRODUCTION METHODS
 Singapore Med J 212; 53(3) : 183 Comparison of clinical and radiological results of posterolateral fusion, posterior lumbar interbody fusion and transforaminal lumbar interbody fusion techniques in the
Singapore Med J 212; 53(3) : 183 Comparison of clinical and radiological results of posterolateral fusion, posterior lumbar interbody fusion and transforaminal lumbar interbody fusion techniques in the
Spine Tango annual report 2012
 DOI 10.1007/s00586-013-2943-x SPINE TANGO REPORT 2012 Spine Tango annual report 2012 M. Neukamp G. Perler T. Pigott E. Munting M. Aebi C. Röder Received: 31 July 2013 / Published online: 30 August 2013
DOI 10.1007/s00586-013-2943-x SPINE TANGO REPORT 2012 Spine Tango annual report 2012 M. Neukamp G. Perler T. Pigott E. Munting M. Aebi C. Röder Received: 31 July 2013 / Published online: 30 August 2013
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
Posterior lumbar interbody fusion for revision disc surgery: review of 50 cases in which carbon fiber cages were implanted
 J Neurosurg (Spine 2) 95:190 195, 2001 Posterior lumbar interbody fusion for revision disc surgery: review of 50 cases in which carbon fiber cages were implanted BHUPAL CHITNAVIS, F.R.C.S.(SN), GIUSEPPE
J Neurosurg (Spine 2) 95:190 195, 2001 Posterior lumbar interbody fusion for revision disc surgery: review of 50 cases in which carbon fiber cages were implanted BHUPAL CHITNAVIS, F.R.C.S.(SN), GIUSEPPE
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
Int J Clin Exp Med 2018;11(2): /ISSN: /IJCEM Yi Yang, Hao Liu, Yueming Song, Tao Li
 Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Int J Clin Exp Med 2018;11(2):1278-1284 www.ijcem.com /ISSN:1940-5901/IJCEM0063093 Case Report Dislocation and screws pull-out after application of an Isobar TTL dynamic stabilisation system at L2/3 in
Surgical Technique. Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion
 Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
Surgical Technique Apache Posterior Lumbar Interbody Fusion Apache Transforaminal Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 5 Disc Exposure 5 Disc and
DISCLOSURES. Goal of Fusion. Expandable Cages: Do they play a role in lumbar MIS surgery? CON 2/15/2017
 Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Expandable Cages: Do they play a role in lumbar MIS surgery? CON Jean-Jacques Abitbol, M.D., FRCSC San Diego, California DISCLOSURES SAB; K2M, Osprey, Nanovis, Vertera, St Theresa Royalties; Osprey, K2M,
Microendoscope-assisted posterior lumbar interbody fusion: a technical note
 Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
Original Study Microendoscope-assisted posterior lumbar interbody fusion: a technical note Hirohiko Inanami 1, Fumiko Saiki 1, Yasushi Oshima 2 1 Department of Orthopaedic Surgery, Inanami Spine and Joint
T.L.I.F. Surgical Technique. Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System.
 Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Original Article Clinics in Orthopedic Surgery 2015;7:
 Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
Alamo T Transforaminal Lumbar Interbody System Surgical Technique
 Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
nvt Transforaminal Lumbar Interbody Fusion System
 nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
Abstract. Med. J. Cairo Univ., Vol. 80, No. 1, March: ,
 Med. J. Cairo Univ., Vol. 80, No. 1, March: 185-192, 2012 www.medicaljournalofcairouniversity.com Evaluation of Transforaminal Lumbar Interbody Fusion Versus Posterior Lumbar Interbody Fusion in Patients
Med. J. Cairo Univ., Vol. 80, No. 1, March: 185-192, 2012 www.medicaljournalofcairouniversity.com Evaluation of Transforaminal Lumbar Interbody Fusion Versus Posterior Lumbar Interbody Fusion in Patients
5/19/2017. Interspinous Process Fixation with the Minuteman G3. What is the Minuteman G3. How Does it Work?
 Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Interspinous Process Fixation with the Minuteman G3 LLOYDINE J. JACOBS, MD CASTELLVI SPINE MEETING MAY 13, 2017 What is the Minuteman G3 The world s first spinous process plating system that is: Minimally
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
Interbody fusion cage for the transforaminal approach. Travios. Surgical Technique
 Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Interbody fusion cage for the transforaminal approach Travios Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Axial Lumbosacral Interbody Fusion. Description
 Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
Section: Surgery Effective Date: April 15, 2014 Subject: Axial Lumbosacral Interbody Fusion Page: 1 of 6 Last Review Status/Date: March 2014 Axial Lumbosacral Interbody Fusion Description Axial lumbosacral
PARADIGM SPINE. Minimally Invasive Lumbar Fusion. Interlaminar Stabilization
 PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
PARADIGM SPINE Minimally Invasive Lumbar Fusion Interlaminar Stabilization 2 A UNIQUE MIS ALTERNATIVE TO PEDICLE SCREW FIXATION The Gold Standard The combined use of surgical decompression and different
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS
 U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
U.S. MARKET FOR MINIMALLY INVASIVE SPINAL IMPLANTS idata_usmis15_rpt Published in December 2014 By idata Research Inc., 2014 idata Research Inc. Suite 308 4211 Kingsway Burnaby, British Columbia, Canada,
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
nvp Posterior Lumbar Interbody Fusion System
 nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine...2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Surgical Technique. Apache Anterior Lumbar Interbody Fusion
 Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
Surgical Technique Apache Anterior Lumbar Interbody Fusion 2 Table of Contents Page Preoperative Planning 4 Patient Positioning 4 Disc and Endplate Preparation 4 Distraction/Size Selection 5 Implantation
Apache Cervical Interbody Fusion Device. Surgical Technique. Page of 13. LC-005 Rev F
 LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
LC-005 Rev F Apache Cervical Interbody Fusion Device Page of 13 Surgical Technique INDICATIONS: When used as an intervertebral body fusion device, the Genesys Spine Interbody Fusion System is indicated
nva Anterior Lumbar Interbody Fusion System
 nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nva Anterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
SURGICAL TECHNIQUE MANUAL. InterFuse T
 1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
1 CONTENTS InterFuse T Product Description 3 Indications for Use 3 X-Ray Marker Locations 4 Product Specifications 4 Instrument Set 5 Step 1 Preoperative Planning 8 Patient Positioning 8 Step 2 Disc Removal
Original Investigation. Peng Luo 1*, Rong-Xue Shao 2*, Ai-Min Wu 1, Hua-Zi Xu 1, Yong-Long ChI 1, Yan LIn 1 ABSTRACT
 DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
DOI: 10.5137/1019-5149.JTN.12450-14.1 Received: 24.11.2014 / Accepted: 05.01.2015 Published Online: 11.07.2016 Original Investigation Transforaminal Lumbar Interbody Fusion with Unilateral Pedicle Screw
T.L.I.F. Transforaminal Lumbar Interbody Fusion
 T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
T.L.I.F. Transforaminal Lumbar Interbody Fusion Cover Surgical Header Technique Sub Guide header Introduction (T.L.I.F. ) technique has gained wide acceptance Additionally, the T.L.I.F. procedure avoids
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
PROCEDURES WE PERFORM
 PROCEDURES WE PERFORM Decompression, Stabilization, and More North American Spine offers a family of advanced, minimally invasive procedures that are highly effective in treating most forms of chronic
PROCEDURES WE PERFORM Decompression, Stabilization, and More North American Spine offers a family of advanced, minimally invasive procedures that are highly effective in treating most forms of chronic
Original Policy Date
 MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
MP 7.01.110 Axial Lumbosacral Interbody Fusion Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search12/2013 Return to Medical
Transforminal Lumbar Interbody Fusion in Management of Degenerative Disorders of the Lumbar Spine (Tlif)
 Transforminal Lumbar Interbody Fusion in Management of Degenerative Disorders of the Lumbar Spine (Tlif) Salah ElDin Elhefnawy 1*, Mohamed Sawan 2, Hossam Salah 2 1 Department of Neurosurgery, Faculty
Transforminal Lumbar Interbody Fusion in Management of Degenerative Disorders of the Lumbar Spine (Tlif) Salah ElDin Elhefnawy 1*, Mohamed Sawan 2, Hossam Salah 2 1 Department of Neurosurgery, Faculty
Lumbar Spinal Fusion Corporate Medical Policy
 Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
ELY ASHKENAZI Israel Spine Center at Assuta Hospital Tel Aviv, Israel
 nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
nterior cervical decompression using the Hybrid Decompression Fixation technique, a combination of corpectomies and or discectomies, in the management of multilevel cervical myelopathy J ORTHOP TRUM SURG
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Two-year outcomes of transforaminal lumbar interbody fusion
 Journal of Orthopaedic Surgery 2011;19(2):135-40 Two-year outcomes of transforaminal lumbar interbody fusion Seng-Yew Poh, Wai-Mun Yue, Li-Tat John Chen, Chang-Ming Guo, William Yeo, Seang-Beng Tan Department
Journal of Orthopaedic Surgery 2011;19(2):135-40 Two-year outcomes of transforaminal lumbar interbody fusion Seng-Yew Poh, Wai-Mun Yue, Li-Tat John Chen, Chang-Ming Guo, William Yeo, Seang-Beng Tan Department
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
5/27/2016. Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation. Disclosures. LLIF Approach
 Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Stand-Alone Lumbar Lateral Interbody Fusion (LLIF) vs. Supplemental Fixation Joseph M. Zavatsky, M.D. Spine & Scoliosis Specialists Tampa, FL Disclosures Consultant - Zimmer / Biomet, DePuy Synthes Spine,
Interbody fusion is the most reliable fusion technique
 Original Article 170 Clinical Results of a Single Central Interbody Fusion Cage and Transpedicle Screws Fixation for Recurrent Herniated Lumbar Disc and Low-Grade Spondylolisthesis Kuo-Feng Huang, MD;
Original Article 170 Clinical Results of a Single Central Interbody Fusion Cage and Transpedicle Screws Fixation for Recurrent Herniated Lumbar Disc and Low-Grade Spondylolisthesis Kuo-Feng Huang, MD;
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
PARADIGM SPINE. Brochure. coflex-f Minimally Invasive Lumbar Fusion
 PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
PARADIGM SPINE Brochure coflex-f Minimally Invasive Lumbar Fusion coflex-f THE UNIQUE, MINIMALLY INVASIVE FUSION DEVICE The coflex-f implant is designed to deliver surgeon confidence and patient satisfaction.
Departement of Neurosurgery A.O.R.N A. Cardarelli- Naples.
 Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
Percutaneous posterior pedicle screw fixation in the treatment of thoracic, lumbar and thoraco-lumbar junction (T12-L1) traumatic and pathological spine fractures. Report of 45 cases. G. Vitale, A. Punzo,
TRANSLAMINAR FACET SCREW FIXATION
 1. Introduction: Although the new era in spine surgery is highly focused on preserving mobility, fusion is still an accepted way of treatment for a variety of spinal disorders. To stabilize the spine until
1. Introduction: Although the new era in spine surgery is highly focused on preserving mobility, fusion is still an accepted way of treatment for a variety of spinal disorders. To stabilize the spine until
C LINICAL A RTICLE. The sacrifice of motion to achieve spinal stability and pain relief has been practised since the early 20 th
 Page 8 / SA ORTHOPAEDIC JOURNAL Autumn 2008 C LINICAL A RTICLE Lumbar fusion indications and surgical options RN Dunn, MBChB(UCT), MMed(UCT)Orth, FCS(SA)Orth Head of Spinal Services, Division of Orthopaedic
Page 8 / SA ORTHOPAEDIC JOURNAL Autumn 2008 C LINICAL A RTICLE Lumbar fusion indications and surgical options RN Dunn, MBChB(UCT), MMed(UCT)Orth, FCS(SA)Orth Head of Spinal Services, Division of Orthopaedic
EIT TLIF Cage. For Natural Bone Ingrowth with EIT Cellular Titanium
 EIT TLIF Cage For Natural Bone Ingrowth with EIT Cellular Titanium EIT TLIF Cage Surgical Technique EIT Cellular Titanium provides active fusion area» ~ 80% porosity» ~ 650 µm diamond pore size» open interconnected
EIT TLIF Cage For Natural Bone Ingrowth with EIT Cellular Titanium EIT TLIF Cage Surgical Technique EIT Cellular Titanium provides active fusion area» ~ 80% porosity» ~ 650 µm diamond pore size» open interconnected
DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL
 SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
SPINAL CHAPTER, NESON DEGENERATIVE SPINAL DISEASE PRABIN SHRESTHA ANISH M SINGH B&B HOSPITAL INTRODUCTION DEGENERATIVE SPINAL DISEASE Gradual loss of normal structure and function of spine with time Also
Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis
 Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis Issue 6: March 2016 Review date: February 2019 Following your recent investigations and consultation with your spinal surgeon, it
Lumbar Decompression and Stabilisation for Spondylitic Spondylolisthesis Issue 6: March 2016 Review date: February 2019 Following your recent investigations and consultation with your spinal surgeon, it
Posterior lumbar interbody fusion with bioabsorbable spacers and local autograft in a series of 27 patients
 Neurosurg Focus 16 (3):Article 8, 2004, Click here to return to Table of Contents Posterior lumbar interbody fusion with bioabsorbable spacers and local autograft in a series of 27 patients DANIEL E. COUTURE,
Neurosurg Focus 16 (3):Article 8, 2004, Click here to return to Table of Contents Posterior lumbar interbody fusion with bioabsorbable spacers and local autograft in a series of 27 patients DANIEL E. COUTURE,
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft. Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD
 Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Induction and Maintenance of Lordosis in MultiLevel ACDF Using Allograft Saad Khairi, MD Jennifer Murphy Robert S. Pashman, MD Purpose Is lordosis induced by multilevel cortical allograft ACDF placed on
Posterior. Lumbar Fusion. Disclaimer. Integrated web marketing. Multimedia Health Education
 Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Posterior Lumbar Fusion Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
The Fusion of Power and Performance.
 The Fusion of Power and Performance. Leading the Way in Lumbar Interbody Fusion with 1 Years of Clinical Results. The JAGUAR Lumbar I/F CAGE System, approved in the U.S. in February 1999, has revolutionized
The Fusion of Power and Performance. Leading the Way in Lumbar Interbody Fusion with 1 Years of Clinical Results. The JAGUAR Lumbar I/F CAGE System, approved in the U.S. in February 1999, has revolutionized
Fixation of multiple level anterior cervical disc using cages versus cages and plating
 Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
Elsayed and Sakr The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2019) 55:12 https://doi.org/10.1186/s41983-019-0062-2 The Egyptian Journal of Neurology, Psychiatry and Neurosurgery RESEARCH
CERVICAL PROCEDURES PHYSICIAN CODING
 CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
CERVICAL PROCEDURES PHYSICIAN CODING Anterior Cervical Discectomy with Interbody Fusion (ACDF) Anterior interbody fusion, with discectomy and decompression; cervical below C2 22551 first interspace 22552
Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion
 Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Open Access Case Report DOI: 10.7759/cureus.653 Focal Correction of Severe Fixed Kyphosis with Single Level Posterior Ponte Osteotomy and Interbody Fusion Seth S. Molloy 1, Faiz U. Ahmad 2, Griffin R.
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
ProDisc-L Total Disc Replacement. IDE Clinical Study
 Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Total Disc Replacement IDE Clinical Study Study Design TDR vs. circumferential fusion: Multi-center, prospective, randomized trial 17 centers, 292 patients 162 patients 80 fusion patients 50 non-randomized
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Zheng Li, Fubing Liu, Shuhao Liu, Zixian Chen, Chun Jiang, Zhenzhou Feng, and Xiaoxing Jiang
 BioMed Research International Volume 2016, Article ID 7261027, 6 pages http://dx.doi.org/10.1155/2016/7261027 Clinical Study Miniopen Transforaminal Lumbar Interbody Fusion with Unilateral Fixation: A
BioMed Research International Volume 2016, Article ID 7261027, 6 pages http://dx.doi.org/10.1155/2016/7261027 Clinical Study Miniopen Transforaminal Lumbar Interbody Fusion with Unilateral Fixation: A
Contact Fusion Cage. Surgical Technique
 Contact Fusion Cage Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by a surgeon experienced
Contact Fusion Cage Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes products. Instruction by a surgeon experienced
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT
 SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
SUBAXIAL CERVICAL SPINE TRAUMA- DIAGNOSIS AND MANAGEMENT 1 Anatomy 3 columns- Anterior, middle and Posterior Anterior- ALL, Anterior 2/3 rd body & disc. Middle- Posterior 1/3 rd of body & disc, PLL Posterior-
Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September
 Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September 2015 213-220 Original Article Transforaminal Lumbar Interbody Fusion for the Treatment of Spondylolisthesis and Degenerative Segmental
Egyptian Journal of Neurosurgery Volume 30 / No. 3 / July - September 2015 213-220 Original Article Transforaminal Lumbar Interbody Fusion for the Treatment of Spondylolisthesis and Degenerative Segmental
Spondylolytic spondylolisthesis:
 CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Spring 2011 Vol 10 No 3 / Page 85 C L I N I C A L A RT I C L E Spondylolytic spondylolisthesis: Surgical management of adult presentation AJ Vlok MBChB, MMed(Neurosurg),
CLINICAL ARTICLE SA ORTHOPAEDIC JOURNAL Spring 2011 Vol 10 No 3 / Page 85 C L I N I C A L A RT I C L E Spondylolytic spondylolisthesis: Surgical management of adult presentation AJ Vlok MBChB, MMed(Neurosurg),
Transforaminal Lumbar Interbody Fusion
 Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
Transforaminal Lumbar Interbody Fusion Issue 6: March 2016 Review date: February 2019 Following your discography investigation and consultation with your spinal surgeon, the possibility of undergoing lumbar
L-VARLOCK. Posterior Lumbar Cage with adjustable lordosis. S urgical T echnique
 L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
L-VARLOCK Posterior Lumbar Cage with adjustable lordosis S urgical T echnique Introduction Designed and manufactured by KISCO International, L-VARLOCK cages are made of titanium alloy Ti 6AI 4V (standards
DEGENERATIVE SPONDYLOLISTHESIS
 AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
AN INTRODUCTION TO DEGENERATIVE SPONDYLOLISTHESIS This booklet is designed to inform you about lumbar degenerative spondylolisthesis. It is not meant to replace any personal conversations that you might
Spinal Terminology Basics
 Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
Spinal Terminology Basics Anterior The front portion of the body. It is often used to indicate the position of one structure relative to another. Annulus Fibrosus The outer, fibrous, ring like portion
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 29 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Lumbar Spinal Fusion Page 1 of 28 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: See Also: Lumbar Spinal Fusion Interspinous Fixation (Fusion) Devices http://www.bcbsks.com/customerservice/providers/medicalpolicies/policies.shtml
Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report
 Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
You Don t Understand This Stuff???
 SPINE SURGERY You Don t Understand This Stuff??? Welcome to the club Most PCP s don t understand what we do Half of other orthopods don t get it Sometimes we can t even explain it to each other Why would
SPINE SURGERY You Don t Understand This Stuff??? Welcome to the club Most PCP s don t understand what we do Half of other orthopods don t get it Sometimes we can t even explain it to each other Why would
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose
 Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Complications of posterior lumbar interbody fusion when using a titanium threaded cage device
 J Neurosurg (Spine 1) 93:45 52, 2000 Complications of posterior lumbar interbody fusion when using a titanium threaded cage device W. JEFFREY ELIAS, M.D., NATHAN E. SIMMONS, M.D., GEORGE J. KAPTAIN, M.D.,
J Neurosurg (Spine 1) 93:45 52, 2000 Complications of posterior lumbar interbody fusion when using a titanium threaded cage device W. JEFFREY ELIAS, M.D., NATHAN E. SIMMONS, M.D., GEORGE J. KAPTAIN, M.D.,
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions:
 Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Am I eligible for the TOPS study? Possibly, if you suffer from one or more of the following conditions: Radiating leg pain Greater leg / buttock pain than back pain Severe pain sets in when walking as
Advantage ALIF. Keith Shevlin Managing Director
 Advantage ALIF Unit 10, 9-11 Myrtle Street, Crows Nest NSW 2065 Keith Shevlin Managing Director keithshevlin@precisionsurgical.com.au Advantage ALIF Introduction & Indications for Use 1 Surgical Technique
Advantage ALIF Unit 10, 9-11 Myrtle Street, Crows Nest NSW 2065 Keith Shevlin Managing Director keithshevlin@precisionsurgical.com.au Advantage ALIF Introduction & Indications for Use 1 Surgical Technique
Paramedian approach for transforaminal lumbar interbody fusion with unilateral pedicle screw fixation
 Neurosurg Focus 20 (3):E5, 2006 Paramedian approach for transforaminal lumbar interbody fusion with unilateral pedicle screw fixation Technical note and preliminary report on 47 cases JONATHAN TUTTLE,
Neurosurg Focus 20 (3):E5, 2006 Paramedian approach for transforaminal lumbar interbody fusion with unilateral pedicle screw fixation Technical note and preliminary report on 47 cases JONATHAN TUTTLE,
The Spine Journal 6 (2006)
 The Spine Journal 6 (2006) 421 427 Outcomes of L1 L2 posterior lumbar interbody fusion with the Lumbar I/F cage and the variable screw placement system: reporting unexpected poor fusion results at L1 L2
The Spine Journal 6 (2006) 421 427 Outcomes of L1 L2 posterior lumbar interbody fusion with the Lumbar I/F cage and the variable screw placement system: reporting unexpected poor fusion results at L1 L2
TABLE OF CONTENTS. ShurFit Anterior Cervical Interbody Fusion (ACIF) System Overview 2. Implant Specifications 3. Instrument Features 4
 Surgical Technique TABLE OF CONTENTS ShurFit Anterior Cervical Interbody Fusion (ACIF) System Overview 2 Product Highlights 2 Indications 2 Implant Specifications 3 Instrument Features 4 Surgical Technique
Surgical Technique TABLE OF CONTENTS ShurFit Anterior Cervical Interbody Fusion (ACIF) System Overview 2 Product Highlights 2 Indications 2 Implant Specifications 3 Instrument Features 4 Surgical Technique
Disclosures 5/27/2016. Narrowing of the spinal canal or neuroforamina causing a symptomatic compression of the neural element.
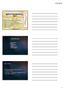 Radiculopathy Saggital MRI view Contained disc extrusion uplifting PLL from bone Terrence Julien, MD, FACS, (blue FAANS arrows) Associate Professor of Neurosurgery System Director, Surgical Neuro-Oncology
Radiculopathy Saggital MRI view Contained disc extrusion uplifting PLL from bone Terrence Julien, MD, FACS, (blue FAANS arrows) Associate Professor of Neurosurgery System Director, Surgical Neuro-Oncology
Patient Information ACDF. Anterior Cervical Discectomy and Fusion
 Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
Patient Information ACDF Anterior Cervical Discectomy and Fusion Table of Contents Anatomy of the Spine...2-3 General Conditions of the Cervical Spine...4 5 What is an ACDF?...6 How is an ACDF performed?...7
ASJ. Radiologic and Clinical Courses of Degenerative Lumbar Scoliosis (10 25 ) after a Short-Segment Fusion. Asian Spine Journal.
 Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Asian Spine Journal 570 Kyu Yeol Clinical Lee et al. Study Asian Spine J 2017;11(4):570-579 https://doi.org/10.4184/asj.2017.11.4.570 Asian Spine J 2017;11(4):570-579 Radiologic and Clinical Courses of
Aesculap CeSpace TM PEEK and CeSpace TM XP Spinal Implant System Instructions for Use
 Aesculap CeSpace TM PEEK and CeSpace TM XP Spinal Implant System Instructions for Use Page 1 of 5 Indications for use: When used as a Vertebral Body Replacement Device: The CeSpace PEEK and CeSpace XP
Aesculap CeSpace TM PEEK and CeSpace TM XP Spinal Implant System Instructions for Use Page 1 of 5 Indications for use: When used as a Vertebral Body Replacement Device: The CeSpace PEEK and CeSpace XP
