Solifenacin significantly improves all symptoms of overactive bladder syndrome
|
|
|
- Leon Mathews
- 6 years ago
- Views:
Transcription
1 REVIEW doi: /j x Solifenacin significantly improves all symptoms of overactive bladder syndrome C. R. CHAPPLE, 1 L. CARDOZO, 2 W. D. STEERS, 3 F. E. GOVIER 4 1 Department of Urology, The Royal Hallamshire Hospital, Sheffield, 2 Department of Urogynaecology, King s College Hospital, London, UK, 3 Department of Urology, University of Virginia Health System, 4 Department of Urology and Renal Transplantation, Virginia Mason Medical Center, Seattle, WA, USA OnlineOpen: This article is available free online at SUMMARY Overactive bladder syndrome (OAB) is a chronic condition characterised by urgency, with or without associated urge incontinence. Solifenacin succinate is a once daily, bladder selective antimuscarinic available in two doses (5 and 10 mg). The recommended dose is 5 mg once daily and can be increased to 10 mg once daily if 5 mg is well tolerated. This article presents pooled efficacy and safety data from four large, placebo-controlled, multinational phase III trials of solifenacin succinate with a total enrolment of over 2800 patients. Data from these trials show that solifenacin 5 and 10 mg once daily is significantly more effective than placebo at reducing urgency, incontinence, micturition frequency and nocturia and at increasing volume voided per micturition. Adverse events were mainly mild-to-moderate in all treatment groups. The results of these phase III trials support the use of solifenacin in the treatment of OAB. Keywords: Solifenacin; overactive bladder; antimuscarinic ª 2006 Blackwell Publishing Ltd INTRODUCTION Overactive bladder syndrome (OAB) is defined by the International Continence Society (ICS) as urgency, with or without urge incontinence, usually with frequency and nocturia (1). As such, it is a symptomatic diagnosis acknowledging the presence of storage symptoms, based on a patient s history alone, which is suggestive of urodynamically demonstrable detrusor overactivity, in the absence of proven infection or obvious pathology (1). In defining OAB and considering the individual components comprising this symptom complex, the ICS has highlighted the significant role of urgency (1). Urgency is important as it is thought to play a pivotal role in driving the other symptoms of OAB (urinary incontinence, frequency and nocturia) (2). As illustrated in Figure 1, urgency is thought to cause these other OAB symptoms by reducing the time that voiding can be deferred, thereby increasing micturition frequency and reducing the volume voided per micturition. Urgency is also Correspondence to: Christopher R. Chapple, Consultant Urological Surgeon, Department of Urology, The Royal Hallamshire Hospital, and Professor of Urology, Sheffield Hallam University, Sheffield S10 2JF, UK Tel.: þ 44 (114) Fax: þ 44 (114) c.r.chapple@sheffield.ac.uk thought to contribute to incontinence and nocturia, but the relationship is less direct (2). Bladder storage symptoms have a severe impact on all areas of quality of life (QoL) including social, psychological and work function (3,4). Therapy for chronic, non-life threatening conditions, such as OAB, should focus on patient benefit and in doing so must take account of patient perceived outcomes, rather than simple symptom resolution alone. Efficacy of OAB therapy needs to be balanced against tolerability, as a low incidence of adverse events (AEs) improves compliance with treatment. This balance between efficacy and tolerability should provide palpable benefits from a patient s perspective, and promote persistence with a therapy, which is of course an important issue in chronic conditions, such as OAB, that require continued therapy. Unfortunately, many antimuscarinics, especially older agents, have modest clinical efficacy and are associated with unfavourable side effects, leading to poor persistence with therapy (5). Many clinical trials of antimuscarinics have not published efficacy endpoints for all the symptoms contained within the ICS definition for OAB and, further, often overlook patient benefits such as treatment satisfaction and QoL. Antimuscarinic agents are the mainstay of OAB pharmacotherapy, and exert their effects by competitively blocking acetylcholine binding at the muscarinic receptors within the various histological compartments of the bladder. As well as being released from efferent cholinergic nerves innervating
2 960 SOLIFENACIN AND SYMPTOMS OF OAB Figure 1 The role of urgency in initiating overactive bladder syndrome symptoms (reproduced from Chapple et al permission requested (2)) the detrusor, recent experimental work has suggested that acetylcholine can be released by stretch of the urothelium from non-neuronal sources, in addition to being related to leakage from neurones (6). There is also increasing evidence that acetylcholine may act on receptors in the suburothelial plexus, thereby influencing the afferent system and detrusor contraction. Solifenacin succinate is a once-daily, oral antimusarinic agent, which shows in vitro selectivity for bladder tissue over salivary preparations (7,8). Solifenacin has also displayed efficacy in the treatment of OAB, as demonstrated in four large double-blind, placebo-controlled, 12-week, phase III studies assessing over 3000 patients (9 12). As protocols were similar, we are able to present the pooled data from these four studies, allowing an objective evaluation of the efficacy and tolerability of once-daily solifenacin 5 and 10 mg in reducing all symptoms of OAB in one of the largest pooled analyses of an antimuscarinic agent to date. MATERIALS AND METHODS Figure 2 Study design. n ¼ number of patients evaluated for efficacy; od ¼ once daily. The tolterodine treatment arm was included in only one of the four phase III studies Study design and protocol Four multinational, double-blind, randomised, phase III studies were conducted with similar protocols (9 12). A tolterodine 2 mg twice daily active treatment arm was included in one of the four studies, but was not powered for comparison. The methods, design and results of this single study have been previously published (10); the tolterodine data are excluded from the pooled analysis in this current report (Figure 2). Patients completed a 3-day micturition diary before the first visit and before all subsequent monthly visits. All patients underwent a baseline assessment including medication history, physical examination, vital signs, laboratory tests and electrocardiogram. After completing a 2-week placebo run-in or screening/washout period, patients began their treatment regimen on the first day of the study. In two of the studies, patients were randomised to once-daily treatment with solifenacin 10 mg or placebo. In the other two studies, patients were randomised to once-daily treatment with 5 mg solifenacin, 10 mg solifenacin or placebo. These studies were performed in accordance with the International Conference on Harmonisation Good Clinical Practice guidelines, and the principles of the Declaration of Helsinki. The study protocol was approved by the responsible ethical committee at each study site. All patients were informed of the nature and purpose of the study, and written informed consent was obtained before screening. Patients Outpatient men and women, at least 18 years of age, with symptoms of OAB were eligible for enrolment. During a baseline 3-day micturition diary period, patients were required to report a mean of 8 micturitions per 24 h, and either a mean of 1 incontinence episode per 24 h or a mean of 1 urgency episode per 24 h. Efficacy analysis Data on urgency, incontinence, micturition frequency, nocturia episodes and volume voided were collected using a 3-day micturition diary, and reported at baseline and before visits at weeks 4, 8 and 12. For each episode, date and time, whether or not the patient voided, the presence of urgency and incontinence, volume voided (for at least 2 of the 3 days), and whether or not the episode disturbed the patient s sleep (episodes of nocturia) were recorded; the time of rising from and going to bed were also recorded. Efficacy analyses included mean and median changes from baseline to endpoint in the number of each of the following per 24 h: episodes of urgency, incontinence, nocturia and micturitions. The volume voided per micturition was also
3 SOLIFENACIN AND SYMPTOMS OF OAB 961 recorded. Patients without at least one on-treatment efficacy assessment were excluded from the analyses. In line with ICS guidelines for the presentation of data, symptom resolution / normalisation rates were also examined, as well as an assessment of the 50% improvement in the symptoms of urgency, incontinence, number of micturitions and nocturia (13). Symptom resolution was defined as the complete absence of symptoms at the study endpoint that were present at baseline. Symptom normalisation applied only to micturition frequency, and was defined as a reduction to below eight micturitions per 24 h. Two of the four trials described in this analysis measured QoL changes using the King s Health Questionnaire (KHQ) (14). Solifenacin significantly improved KHQ scores from baseline in nine of 10 domains compared with placebo, demonstrating statistically significant improvements in patient QoL (15,16). The clinical relevance of improvements in the KHQ scores was determined using a scale based on a global rating of patient-perceived treatment benefit, and perceived disease impact (25): a minimally important difference (MID) was defined as a 15% point change from baseline, which focussed on the differences between the solifenacin- and placebo-treatment groups for each individual KHQ domain. Safety assessments Treatment emergent adverse events (TEAEs) were evaluated for the safety population. A TEAE was defined as an AE that occurred after the first dose of study medication that was not evident before treatment, or worsening of an AE that was present before start of treatment. Treatment-emergent adverse events were classified into mild/moderate and severe groups, as determined by the investigator. Serious AEs were reported based on the International Conference on Harmonisation of Technical Requirements for Registration of Pharmaceuticals for Human Use (ICH) criteria. Discontinuation rates due to AEs were also evaluated. Statistical methods Mean changes from baseline to endpoint in all symptoms were compared by analysis of covariance (ANCOVA) for each OAB outcome, with treatment and centre as terms and baseline as a covariate. Treatment group comparisons of responder or normalisation rates were based on Fisher s exact test. Actual mean change from baseline to endpoint was normally distributed; therefore, p-values were based on the ANCOVA model. The percent change from baseline to endpoint was not normally distributed; therefore, p-values for the percent change were based on Van Elteren s test stratified by pooled centre. Endpoint was defined as the last available on-treatment assessment. The p-values for the pairwise testing of solifenacin vs. placebo differences in MID for KHQ changes were based on a logistic regression model with treatment and study as terms, and baseline as a covariate. RESULTS Patients Baseline characteristics and OAB symptoms for the pooled study population are summarised in Table 1. From a total of 3032 patients randomised to 5 mg solifenacin, 10 mg solifenacin or placebo, data from 2848 patients were available for the analysis of efficacy and was defined as the full analysis set (Figure 2). Of the patients included in the present analysis, 99% of patients reported an urgency episode, 66% reported an incontinence episode and 89% reported a Table 1 Baseline demographics and efficacy characteristics for the full analysis set Placebo Solifenacin 5 mg od Solifenacin 10 mg od Number of subjects (n) Age (years) Mean years, n (%) 742 (65) 370 (67) 756 (65) 65 years, n (%) 396 (35) 182 (33) 402 (35) Gender Male (%) 219 (19) 121 (22) 242 (21) Female (%) 919 (81) 431 (78) 916 (79) Baseline OAB symptom levels, mean (SE) Urgency episodes per 24 h (n ¼ 2823) 6.3 (0.12) 5.9 (0.20) 6.2 (0.12) Incontinence episodes per 24 h (n ¼ 1873) 2.9 (0.10) 2.6 (0.14) 2.9 (0.10) Micturitions per 24 h (n ¼ 2848) 11.9 (0.11) 12.1 (0.16) 11.9 (0.10) Volume voided per micturition (ml) (n ¼ 2843) (2.24) (2.30) (2.08) Nocturia episodes per 24 h (n ¼ 2534) 1.8 (0.04) 2.0 (0.05) 1.8 (0.04) od, once daily; OAB, overactive bladder syndrome; SE, standard error of mean.
4 962 SOLIFENACIN AND SYMPTOMS OF OAB nocturia episode at baseline, as assessed by a 3-day diary. As part of the inclusion criteria, all patients had a micturition frequency of 8 micturitions per day. Improvements in overactive bladder symptoms Changes from baseline to endpoint in urgency, incontinence, micturition frequency, volume voided and nocturia are summarised in Table 2. Compared with placebo, solifenacin treatment at either the 5 or 10 mg dose resulted in a significant improvement in all of the symptoms measured. This was statistically significant for both 5 and 10 mg solifenacin doses, when comparing mean actual reductions for all of the OAB symptoms and for the mean actual increase in volume voided per micturition (Table 2). When assessing urgency (mean absolute values and median percentage values), treatment with solifenacin 5 and 10 mg resulted in a )2.9 ()66.1%) and )3.4 ()70.0%) baseline to endpoint reduction in urgency episodes, respectively, compared with a )2.0 ()40.0%) episode reduction in patients receiving placebo (p for both solifenacin doses vs. placebo). The reduction in incontinence for 5 and 10 mg solifenacin was )1.5 ()100%) and )1.8 ()100%) baseline to endpoint reduction in episodes compared with a )1.1 ()63.6%) episode reduction for patients receiving placebo (p for both doses vs. placebo). The frequency of micturition was significantly reduced in patients receiving both solifenacin 5 mg ()2.3; )19.4%) and 10 mg ()2.7; )22.5%), compared with placebo ()1.4; )12.0%; p for both doses); this was reflected in the number of nocturia episodes, which were also reduced significantly in solifenacin 5 mg recipients ()0.6; )35.5%) and 10 mg recipients ()0.6; )36.4%), compared with patients receiving placebo ()0.4; )25.0%; p and for solifenacin 5 and 10 mg, respectively). In addition, the volume voided per micturition increased significantly after solifenacin treatment, both with 5 mg (32.3 ml; 19.0%) and 10 mg (42.5 ml; 25.7%), compared with treatment with placebo (8.5 ml; 3.1%; p for both doses) (Figure 3). The greater efficacy seen with solifenacin at both doses, compared with placebo was not affected by either age or gender (Table 2). Resolution / normalisation rates and 50% improvements from baseline In patients treated with solifenacin 5 and 10 mg who had urgency at baseline, 29% and 25%, respectively, had no urgency episodes at endpoint when compared with placebo (15%). This difference was statistically significant for both doses of solifenacin (p ) (Table 3). Furthermore, of those patients who had incontinence at baseline, 51% and 52% of patients receiving 5 and 10 mg solifenacin, respectively, reported no incontinence episodes at the study endpoint, compared with only 34% of patients receiving placebo (p ; Table 3). Patients treated with either solifenacin dose also experienced normalisation of micturition frequency, which was statistically significantly greater than placebo (p for both solifenacin dose groups; Table 3). Similar results were seen with respect to resolution Table 2 Mean actual change in overactive bladder syndrome symptoms from baseline to endpoint Mean baseline to endpoint change per 24 h Number of urgency episodes Number of incontinence episodes Micturition frequency Volume voided per micturition Number of nocturia episodes n Change n Change n Change n Change n Change Placebo (total) 1124 ) ) ) )0.4 Placebo (065 years) 733 ) ) ) )0.5 Placebo (65 years) 391 ) ) ) )0.3 Placebo (males only) 217 ) ) ) ) )0.4 Placebo (females only) 907 ) ) ) )0.4 Solifenacin 5 mg (total) 548 ) ) ) )0.6* Solifenacin 5 mg (065 years) 366 ) ) ) )0.6 Solifenacin 5 mg (65 years) 182 ) )1.5* 182 ) )0.6 Solifenacin 5 mg (males only) 121 )2.7* 43 ) )1.9* )0.5 Solifenacin 5 mg (females only) 427 ) ) ) )0.6* Solifenacin 10 mg (total) 1151 ) ) ) )0.6 Solifenacin 10 mg (065 years) 753 ) ) ) )0.6* Solifenacin 10 mg (65 years) 398 ) ) ) )0.5* Solifenacin 10 mg (males only) 242 ) )1.6* 242 ) )0.4 Solifenacin 10 mg (females only) 909 ) ) ) )0.6 *p vs. placebo; p vs. placebo.
5 SOLIFENACIN AND SYMPTOMS OF OAB 963 Figure 3 Median per cent changes in overactive bladder syndrome symptoms from baseline to endpoint. *p vs. placebo; p vs. placebo. p-values for the per cent change from baseline are based on the Van Elteren s test. od ¼ once daily Table 3 Resolution */ normalisation rates for symptoms of overactive bladder syndrome Patients achieving resolution of urgency Patients achieving continence Patients achieving normalisation of micturition frequency Patients achieving resolution of nocturia % n (N) % n (N) % n (N) % n (N) Placebo (1124) (781) (1138) (1005) Solifenacin 5 mg 28.6à 157 (548) 50.6à 159 (314) 33.0à 182 (552) (494) Solifenacin 10 mg 25.5à 293 (1151) 51.8à 403 (778) 37.3à 432 (1158) (1036) *Resolution is defined as an absence of the symptom at endpoint; p vs. placebo; àp vs. placebo; n, number of patients achieving resolution / normalisation ; N, number of patients with specified overactive bladder syndrome symptom at baseline assessment. of nocturia, with 10 mg solifenacin producing statistically significant resolution of symptoms compared with placebo. In line with ICS guidelines for the presentation of data (1), the 50% improvement rates (i.e. the per cent of patients who achieved 50% improvement in symptoms that were present at baseline) are provided in Table 4. The per cent of solifenacin-treated patients achieving a 50% reduction in symptoms was significantly greater than placebo for urgency, incontinence, frequency and nocturia. Achievement of a minimally important difference in quality of life from baseline In the two studies which examined QoL data, solifenacin significantly improved KHQ scores from baseline in nine of 10 domains compared with placebo, demonstrating statistically significant improvements in patient QoL (15,16). When the MID was examined for each of the individual KHQ domains, it was shown that a significantly greater percentage of patients receiving solifenacin achieved an MID in certain individual domains than those receiving placebo [solifenacin 5 mg: general health perception, incontinence impact, role limitations, social limitations, emotions, sleep/energy, severity measures and symptom severity; p vs. placebo; solifenacin 10 mg: general health perception, incontinence impact, role limitations, physical limitations, social limitations, emotions, sleep/ energy, severity measures and symptom severity; p vs. placebo (Figure 4)].
6 964 SOLIFENACIN AND SYMPTOMS OF OAB Table 4 Patients achieving a 50% reduction in overactive bladder syndrome symptoms Urgency episodes Incontinence episodes Micturitions Nocturia episodes % n (N) % n (N) % n (N) % n (N) Placebo (1124) (781) (1138) (1005) Solifenacin 5 mg (548) (314) (552) 43.3%* 214 (494) Solifenacin 10 mg (1151) (778) (1158) (1036) *p vs. placebo; p vs. placebo. n, number of patients achieving resolution / normalisation ; N, number of patients with specified overactive bladder syndrome symptom at baseline assessment. p-values for between-treatment comparisons of responder and normalisation rates were based on Fisher s exact test. Figure 4 Percentage of subjects achieving a clinically meaningful minimally important difference (MID) (5 points)à in King s Health Questionnaire individual domain scores (mean change from baseline to end of study). *p ; p vs. placebo using a logistic regression model. od ¼ once daily; àmids based on Reese et al. (25) Safety Treatment was well tolerated with both doses of solifenacin, with the majority of AEs being mild-to-moderate in nature. The most common TEAEs were dry mouth, constipation, and blurred vision, all of which are recognised side effects of antimuscarinic therapy (Table 5). Although the incidence of dry mouth was higher in the 10 mg solifenacin treated group compared with patients receiving 5 mg solifenacin, the number of patients discontinuing treatment due to AEs was low and comparable with placebo at both solifenacin doses (4.4% placebo, 2.8% solifenacin 5 mg, 6.8% solifenacin 10 mg). Completion rates in the studies were also high (86.4% placebo, 91.0% solifenacin 5 mg, 86.7% solifenacin 10 mg). DISCUSSION Overactive bladder syndrome is a chronic condition encompassing the bothersome storage symptoms of urgency, with or without urge incontinence, usually with frequency and nocturia. Therefore, effective treatment of OAB must result in a reduction meaningful to the patient in all of these symptoms. This review of the data clearly shows that treatment with once-daily solifenacin 5 and 10 mg is associated with significant improvements in all of the symptoms of OAB. Indeed, 125% of solifenacin-treated patients experienced resolution of urgency, 150% of solifenacin-treated patients achieved continence, and at least one-third of solifenacin-treated patients experienced normalisation of micturition frequency to eight or fewer voids per day by study
7 SOLIFENACIN AND SYMPTOMS OF OAB 965 Table 5 Rates of dry mouth, constipation and blurred vision, and discontinuation rates due to adverse events Treatment emergent adverse events Placebo Solifenacin 5mg Solifenacin 10 mg n % n % n % Dry mouth Mild/moderate Severe Constipation Mild/moderate Severe Blurred vision Mild/moderate Severe Discontinuation due to all adverse events* *Adverse events were given as the primary reason for discontinuation. endpoint. Treatment with both doses of solifenacin was also well tolerated by patients, with a few discontinuations due to AEs. If one acknowledges the importance of urgency as a pivotal symptom in this symptom complex; then clearly the high resolution and improvement rates may well be due to solifenacin s impact on the key symptom of urgency (2). Clearly, pharmacotherapy for OAB should not only improve symptoms, but also be tolerable, both of which will contribute to treatment persistence. One very effective measure of this clinical effectiveness is assessment of QoL. Two of the four trials described in this analysis measured QoL changes (10,12), using the KHQ (14). Solifenacin significantly improved KHQ scores from baseline in nine of 10 domains compared with placebo, demonstrating statistically significant improvements in patient QoL (15,16). The clinical relevance of these improvements to patients was determined using a scale based on a global rating of patientperceived treatment benefit, and perceived disease impact (15,16). When using the following definition of clinical meaning: MID 5 percentage point change from baseline; it was shown that patients who were treated with both 5 and 10 mg solifenacin demonstrated a statistically significant and clinically meaningful MID improvement from baseline in almost all KHQ domains, compared with patients receiving placebo. These improvements in QOL are likely to have contributed to the high persistence rates with solifenacin described in the present analysis (approximately 90% for patients receiving solifenacin). Similarly, high persistence rates have also been observed with longer-term treatment with solifenacin. In a 40-week, open-label extension of two of the studies included in this analysis, 81% of patients remained on solifenacin treatment for the full treatment period (17). Furthermore, patient satisfaction with treatment efficacy and tolerability was high (74% and 85%, respectively) when assessed at the end of the extension study (17). The differences in the methodology used to record efficacy data (e.g. different study populations, different inclusion and exclusion criteria, different ways to measure and define urgency, and varying diary durations) and the selective presentation of data for symptom reduction, make it difficult and indeed academically questionable whether one can compare the results presented here with those of other published clinical trials. However, globally allowing for these misgivings, solifenacin appears to compare favourably to other antimuscarinics with respect to treating urgency and all of the other symptoms of OAB (18 21). This drug is the first antimuscarinic for which there are published reports of improvements in all the key symptoms of OAB frequency, urgency, incontinence and nocturia. Other publications of pivotal trial data for other antimuscarinic agents have reported data for some, but not all, of these symptoms (18 21). When considering the current published literature, there are few data available that report the normalisation rates for OAB symptoms (18 21). Most reports only provide this information for incontinence rates and do not present similar results for the proportion of patients who achieve cessation of urgency and nocturia, or normalisation of micturition frequency (08 micturitions per 24 h). Symptomatic outcome measures such as this should be considered to be an essential facet of the assessment of treatment efficacy and should, therefore, be of keen interest to both clinicians and other healthcare providers in determining the clinical effectiveness and utility of different antimuscarinics. In conclusion, solifenacin s efficacy has clearly been demonstrated in published studies for all symptoms of the OAB complex, with a high degree of tolerability and patient benefit. Whilst it is interesting to speculate that the symptom improvements may be driven by the favourable impact that solifenacin has on urgency, clearly, further studies using more accurate measures of patient perceived outcome are necessary to compare this agent to other antimuscarinics. Recently published results from the STAR study have provided a head-to-head comparison between solifenacin and tolterodine ER (22,23). This study suggested that flexible dosing with both 5 and 10 mg solifenacin is more effective in reducing OAB symptoms such as urgency, incontinence, urge incontinence and improving volume voided, as well as improving patient perception of bladder condition, when compared with the highest (and recommended) dose of tolterodine ER (4 mg). The flexibility associated with solifenacin dosing may further increase its efficacy, as well as allowing treatment regimens to be designed for the needs of the individual patient, thus improving patient compliance and satisfaction (24). Although the occurrence of common antimuscarinic AEs was greater with solifenacin-treated patients than with tolterodine-treated patients, the rate of patient discontinuation was low with solifenacin use, and comparable with tolterodine (23), due to the high rate of
8 966 SOLIFENACIN AND SYMPTOMS OF OAB patient satisfaction. Patient satisfaction is also high with the long-term use of solifenacin (17). Further head-to-head comparison studies with other antimuscarinic OAB therapies are needed before definitive conclusions can be drawn. AUTHOR DISCLOSURE Christopher Chapple, BSc, MD, FRCS (Urol), is an investigator/consultant for Pfizer, Astellas, Schwarz Pharma, Novartis and UCB Pharma. Linda Cardozo, MD, FRCOG, receives money for consultancy and/or advisory work, or research or lecturing from the following companies: Astellas, Lilly/Boehringer Ingelheim, UCB Pharma, Pfizer, Gynecare, Plethora and Cook. William D. Steers, MD, is an investigator/consultant for Sanofi, Pfizer, Lilly and Astellas. Fred E. Govier, MD, has nothing to disclose. ACKNOWLEDGEMENTS The analyses in this paper were funded by an educational grant from Astellas. Editorial assistance was provided by Mark Rose, Medicus International. REFERENCES 1 Abrams P, Cardozo L, Fall M et al. The standardisation of terminology in lower urinary tract function: report from the standardisation sub-committee of the International Continence Society. Urology 2003; 61: Chapple CR, Artibani W, Cardozo LD et al. The role of urinary urgency and its measurement in the overactive bladder symptom syndrome: current concepts and future prospects. BJU Int 2005; 95: Kobelt G. Economic considerations and outcome measurement in urge incontinence. Urology 1997; 50 (6A Suppl.): 100 7; discussion Liberman JN, Hunt TL, Stewart WF et al. Health-related quality of life among adults with symptoms of overactive bladder: results from a U.S. community-based survey. Urology 2001; 57: Wein AJ. Diagnosis and treatment of the overactive bladder. Urology 2003; 62 (5 Suppl. 2): Andersson KE. Antimuscarinics for treatment of overactive bladder. Lancet Neurol 2004; 3: Kobayashi S, Ikeda K, Miyata K. Comparison of in vitro selectivity profiles of solifenacin succinate (YM905) and current antimuscarinic drugs in bladder and salivary glands: a Ca 2þ mobilization study in monkey cells. Life Sci 2004; 74: Ikeda K, Kobayashi S, Suzuki M et al. M(3) receptor antagonism by the novel antimuscarinic agent solifenacin in the urinary bladder and salivary gland. Naunyn Schmiedebergs Arch Pharmacol 2002; 366: Cardozo L. Randomized, double-blind placebo-controlled trial of once-daily antimuscarinic agent solifenacin succinate in patients with overactive bladder. J Urol 2004; 172: Chapple CR, Rechberger T, Al-Shukri S et al. Randomized, double-blind placebo- and tolterodine-controlled trial of the oncedaily antimuscarinic agent solifenacin in patients with symptomatic overactive bladder. BJU Int 2004; 93: Gittelman MC, Kaufman J. Solifenacin succinate 10 mg once daily significantly improves symptoms of overactive bladder. Presented at the 17th International Federation of Gynecology and Obstetrics World Congress, Abstract 111. November 2 7, 2003; Santiago, Chile. 12 Gittelman M. The efficacy and safety of solifenacin in adults with overactive bladder: a multicenter, placebo-controlled study. Int J Gynaecol Obstetr 2003; 83 (Suppl. 3): 94 (abstract TP76). 13 Mattiasson A, Djurhuus JC, Fonda D et al. Standardization of outcome studies in patients with lower urinary tract dysfunction: a report on general principles from the Standardisation Committee of the International Continence Society. Neurourol Urodyn 1998; 17: Kelleher CJ, Cardozo L, Chapple CR et al. Improved quality of life in patients with overactive bladder symptoms treated with solifenacin. BJU Int 2005; 95: Kelleher CJ, Pleil AM, Reese PR et al. How much is enough and who says so? BJOG, 2004; 111: Payne C, Kelleher CJ. Redefining response in overactive bladder syndrome impact on quality of life. Presented at the 36th International Continence Society Congress, August 31 September , Abstract 310. November 2 7, 2003; Montreal, Canada. 17 Haab F, Cardozo L, Chapple C et al. Long-term open-label solifenacin treatment associated with persistence with therapy in patients with overactive bladder syndrome. Eur Urol 2005; 47: Haab FL, Dwyer P. Darifenacin, an M3 selective receptor antagonist, is an effective and well-tolerated once-daily treatment for overactive bladder. Eur Urol 2004; 45: 420 9; discussion Van Kerrebroeck P, Kreder K, Jonas U et al. Tolterodine oncedaily: superior efficacy and tolerability in the treatment of the overactive bladder. Urology 2001; 57: Diokno AC, Appell RA, Sand PK et al. Prospective, randomized, double-blind study of the efficacy and tolerability of the extendedrelease formulations of oxybutynin and tolterodine for overactive bladder: results of the OPERA trial. Mayo Clin Proc 2003; 78: Zinner N, Gittelman M, Harris R et al. Trospium chloride improves overactive bladder symptoms: a multicenter phase III trial. J Urol 2004; 171 (6 Pt 1): Chapple C, Ballanger P, Hatzichristou D et al. Improvements in bladder condition in OAB perceived and experienced by patients in a solifenacin vs. tolterodine multinational trial (STAR study). Neurol Urodyn 2005; 24: (abstract 111). 23 Chapple CR, Martinez-Garcia R, Selvaggi L et al. A comparison of the efficacy and tolerability of solifenacin succinate and extended release tolterodine at treating overactive bladder syndrome: results of the STAR trial. Eur Urol 2005; 48: Reese PR, Pleil AM, Okano GJ et al. The Star study: analysis of symptom severity and treatment response in overactive bladder. Proc Eur Assoc Urol 2005 (abstract 380). 25 Reese PR, Pleil AM, Okano GJ et al. Multinational study of reliability and validity of the King s Health Questionnaire in patients with overactive bladder. Qual Life Res 2003; 12: Paper received November 2005, accepted May 2006
The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence
 european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
european urology supplements 5 (2006) 849 853 available at www.sciencedirect.com journal homepage: www.europeanurology.com The Evidence for Antimuscarinic Agents in Female Mixed Urinary Incontinence Stefano
Comparison of Side Effects of Tolterodine and Solifenacinsucinate in Patients with Urinary Incontinence
 ORIGINAL ARTICLE Comparison of Side Effects of Tolterodine and Solifenacinsucinate in Patients with Urinary Incontinence MARYAM RANA, IRAM MOBUSHER ABSTRACT Background: Overactive bladder syndrome is a
ORIGINAL ARTICLE Comparison of Side Effects of Tolterodine and Solifenacinsucinate in Patients with Urinary Incontinence MARYAM RANA, IRAM MOBUSHER ABSTRACT Background: Overactive bladder syndrome is a
Efficacy and safety of solifenacin succinate in Korean patients with overactive bladder: a randomised, prospective, double-blind, multicentre study
 doi: 10.1111/j.1742-1241.2008.01898.x ORIGINAL PAPER Efficacy and safety of solifenacin succinate in n patients with overactive bladder: a randomised, prospective, double-blind, multicentre study M.-S.
doi: 10.1111/j.1742-1241.2008.01898.x ORIGINAL PAPER Efficacy and safety of solifenacin succinate in n patients with overactive bladder: a randomised, prospective, double-blind, multicentre study M.-S.
Subjective Measures of Efficacy: Quality of Life, Patient Satisfaction and Patient-Oriented Goals the Search for Value
 european urology supplements 6 (2007) 438 443 available at www.sciencedirect.com journal homepage: www.europeanurology.com Subjective Measures of Efficacy: Quality of Life, Patient Satisfaction and Patient-Oriented
european urology supplements 6 (2007) 438 443 available at www.sciencedirect.com journal homepage: www.europeanurology.com Subjective Measures of Efficacy: Quality of Life, Patient Satisfaction and Patient-Oriented
Anticholinergic medication use for female overactive bladder in the ambulatory setting in the United States.
 Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
Página 1 de 6 PubMed darifenacin vs solifenacin Display Settings:, Sorted by Recently Added Results: 5 1. Int Urogynecol J. 2013 Oct 25. [Epub ahead of print] Anticholinergic medication use for female
Study No. 178-CL-008 Report Final Version, 14 Dec 2006 Reissued Version, 18 Jul 2011 Astellas Pharma Europe B.V. Page 13 of 122
 Page 13 of 122 3 SYNOPSIS Title of study: (International) Study No: A randomized, double-blind, parallel group, proof-of-concept study of in comparison with placebo and tolterodine in patients with symptomatic
Page 13 of 122 3 SYNOPSIS Title of study: (International) Study No: A randomized, double-blind, parallel group, proof-of-concept study of in comparison with placebo and tolterodine in patients with symptomatic
Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder
 European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
European Urology European Urology 48 (2005) 110 115 Female UrologyöIncontinence Comparison of Symptom Severity and Treatment Response in Patients with Incontinent and Continent Overactive Bladder Martin
Clinical Medicine Insights: Urology
 Clinical Medicine Insights: Urology original research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Efficacy and Safety of 10 mg Solifenacin Succinate in
Clinical Medicine Insights: Urology original research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Efficacy and Safety of 10 mg Solifenacin Succinate in
Report on New Patented Drugs - Vesicare
 Report on New Patented Drugs - Vesicare Under its transparency initiative, the PMPRB publishes the results of the reviews of new patented drugs by Board Staff, for purposes of applying the Board's Excessive
Report on New Patented Drugs - Vesicare Under its transparency initiative, the PMPRB publishes the results of the reviews of new patented drugs by Board Staff, for purposes of applying the Board's Excessive
BJUI. Validity and reliability of the patient s perception of intensity of urgency scale in overactive bladder
 ; 2010 Lower Urinary Tract PATIENT S PERCEPTION OF INTENSITY OF URGENCY SCALE IN OAB CARTWRIGHT ET AL. BJUI Validity and reliability of the patient s perception of intensity of urgency scale in overactive
; 2010 Lower Urinary Tract PATIENT S PERCEPTION OF INTENSITY OF URGENCY SCALE IN OAB CARTWRIGHT ET AL. BJUI Validity and reliability of the patient s perception of intensity of urgency scale in overactive
Results The Authors. BJU Int 2017; 120:
 Functional Urology Efficacy and safety of combinations of mirabegron and solifenacin compared with monotherapy and placebo in patients with overactive bladder (SYNERGY study) Sender Herschorn*, Christopher
Functional Urology Efficacy and safety of combinations of mirabegron and solifenacin compared with monotherapy and placebo in patients with overactive bladder (SYNERGY study) Sender Herschorn*, Christopher
The International Continence Society
 REPORTS Safety and Tolerability of Tolterodine for the Treatment of Overactive Bladder in Adults Richard G. Roberts, MD, JD; Alan D. Garely, MD; and Tamara Bavendam, MD Abstract This article evaluates
REPORTS Safety and Tolerability of Tolterodine for the Treatment of Overactive Bladder in Adults Richard G. Roberts, MD, JD; Alan D. Garely, MD; and Tamara Bavendam, MD Abstract This article evaluates
Comparative Study of Solifenecin Alone Versus Solifenecin with Duloxetine in Patients of Overactive Bladder
 International Journal of Scientific and Research Publications, Volume 3, Issue 1, January 2013 1 Comparative Study of Solifenecin Alone Versus Solifenecin with Duloxetine in Patients of Overactive Bladder
International Journal of Scientific and Research Publications, Volume 3, Issue 1, January 2013 1 Comparative Study of Solifenecin Alone Versus Solifenecin with Duloxetine in Patients of Overactive Bladder
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging
 Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Urinary Incontinence in Women: Never an Acceptable Consequence of Aging Catherine A. Matthews, MD Associate Professor Chief, Urogynecology and Pelvic Reconstructive Surgery University of North Carolina,
Pharmacologic management of overactive bladder
 REVIEW Pharmacologic management of overactive bladder Sum Lam 1,2 lga Hilas 1,3 1 St. John s University, College of Pharmacy and Allied Health Professions, Department of Clinical Pharmacy Practice, Queens,
REVIEW Pharmacologic management of overactive bladder Sum Lam 1,2 lga Hilas 1,3 1 St. John s University, College of Pharmacy and Allied Health Professions, Department of Clinical Pharmacy Practice, Queens,
Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder
 www.kjurology.org DOI:10.4111/kju.2011.52.6.396 Voiding Dysfunction Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder Young Kook Han, Won Ki Lee, Seong Ho Lee, Dae
www.kjurology.org DOI:10.4111/kju.2011.52.6.396 Voiding Dysfunction Effect of Desmopressin with Anticholinergics in Female Patients with Overactive Bladder Young Kook Han, Won Ki Lee, Seong Ho Lee, Dae
Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study
 LUTS () 3, 36 4 ORIGINAL ARTICLE Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study Naoki WADA, Masaki WATANABE, Masafumi
LUTS () 3, 36 4 ORIGINAL ARTICLE Efficacy and Safety of Propiverine and Solifenacin for the Treatment of Female Patients with Overactive Bladder: A Crossover Study Naoki WADA, Masaki WATANABE, Masafumi
3/20/10. Prevalence of OAB Men: 16.0% Women: 16.9% Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Dry. Population (millions) Wet
 1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
1 Prevalence of OAB Men: 16.0% Women: 16.9% Stewart WF, et al. World J Urol. 2003;20:327-336. Prevalence of OAB with incontinence (OAB wet) Men: 2.6% Women: 9.3% Stewart WF, et al. World J Urol. 2003;20:327-336.
Office based non-oncology urology trials Richard W. Casey, MD, 1 Jack Barkin, MD 2
 Office based non-oncology urology trials Richard W. Casey, MD, 1 Jack Barkin, MD 2 1 The Male Health Centre, Oakville, Ontario, Canada 2 Humber River Regional Hospital, University of Toronto, Toronto,
Office based non-oncology urology trials Richard W. Casey, MD, 1 Jack Barkin, MD 2 1 The Male Health Centre, Oakville, Ontario, Canada 2 Humber River Regional Hospital, University of Toronto, Toronto,
Innovations in Childhood Incontinence: Neurogenic and Functional Bladder Disorders
 TNe 10 Innovations in Childhood Incontinence: Neurogenic and Functional Bladder Disorders Stuart B. Bauer, MD President, ICCS Department of Urology Children s Hospital Boston Professor of Urology Harvard
TNe 10 Innovations in Childhood Incontinence: Neurogenic and Functional Bladder Disorders Stuart B. Bauer, MD President, ICCS Department of Urology Children s Hospital Boston Professor of Urology Harvard
Darifenacin: first M3 receptor antagonist for overactive bladder
 Darifenacin: first M3 receptor antagonist for overactive bladder Steve Chaplin MSc, MRPharmS and Christopher Chapple BSc, MD, FRCS(Urol) PRODUCT PROFILE Proprietary name: Emselex Constituents: darifenacin
Darifenacin: first M3 receptor antagonist for overactive bladder Steve Chaplin MSc, MRPharmS and Christopher Chapple BSc, MD, FRCS(Urol) PRODUCT PROFILE Proprietary name: Emselex Constituents: darifenacin
SELECTED POSTER PRESENTATIONS
 SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
SELECTED POSTER PRESENTATIONS The following summaries are based on posters presented at the American Urogynecological Society 2004 Scientific Meeting, held July 29-31, 2004, in San Diego, California. CENTRAL
Overactive bladder (OAB) affects approximately 15% of the adult population. Diagnosis is based
 Overactive bladder (OAB) affects approximately 15% of the adult population. Diagnosis is based upon a medical history, and includes a focused physical exam (abdominal, neurological, pelvic in females and
Overactive bladder (OAB) affects approximately 15% of the adult population. Diagnosis is based upon a medical history, and includes a focused physical exam (abdominal, neurological, pelvic in females and
Overactive bladder: current understanding and future issues
 DOI: 10.1111/j.1471-0528.2006.01081.x www.blackwellpublishing.com/bjog Review article Overactive bladder: current understanding and future issues I Milsom Department of Obstetrics and Gynecology, Sahlgrenska
DOI: 10.1111/j.1471-0528.2006.01081.x www.blackwellpublishing.com/bjog Review article Overactive bladder: current understanding and future issues I Milsom Department of Obstetrics and Gynecology, Sahlgrenska
Mirabegron 50 mg once-daily for the treatment of symptoms of overactive bladder: An overview of efficacy and tolerability over 12 weeks and 1 year
 bs_bs_banner International Journal of Urology (2014) 21, 960 967 doi: 10.1111/iju.12568 Review Article Mirabegron 50 mg once-daily for the treatment of symptoms of overactive bladder: An overview of efficacy
bs_bs_banner International Journal of Urology (2014) 21, 960 967 doi: 10.1111/iju.12568 Review Article Mirabegron 50 mg once-daily for the treatment of symptoms of overactive bladder: An overview of efficacy
Validation of the bladder control self-assessment questionnaire (B-SAQ) in men
 Functional Urology Validation of the bladder control self-assessment questionnaire (B-SAQ) in men Arun Sahai*, Christopher Dowson*, Eduardo Cortes, Jai Seth*, Jane Watkins*, Muhammed Shamim Khan*, Prokar
Functional Urology Validation of the bladder control self-assessment questionnaire (B-SAQ) in men Arun Sahai*, Christopher Dowson*, Eduardo Cortes, Jai Seth*, Jane Watkins*, Muhammed Shamim Khan*, Prokar
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH
 TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
TREATMENT OF OVERACTIVE BLADDER IN ADULTS FUGA 2016 KGH CONTENTS Overactive bladder (OAB) Treatment of OAB Beta-3 adrenoceptor agonist (Betmiga ) - Panacea? LASER treatment - a flash in the pan or the
Overactive Bladder in Clinical Practice
 Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
Overactive Bladder in Clinical Practice Alan J. Wein Christopher Chapple Overactive Bladder in Clinical Practice Authors Alan J. Wein Division of Urology University of Pennsylvania Health System Philadelphia
CDEC FINAL RECOMMENDATION
 CDEC FINAL RECOMMENDATION MIRABEGRON (Myrbetriq Astellas Pharma Canada Inc.) Indication: Overactive Bladder Recommendation: The Canadian Drug Expert Committee (CDEC) recommends that mirabegron be listed
CDEC FINAL RECOMMENDATION MIRABEGRON (Myrbetriq Astellas Pharma Canada Inc.) Indication: Overactive Bladder Recommendation: The Canadian Drug Expert Committee (CDEC) recommends that mirabegron be listed
Diagnosis and Mangement of Nocturia in Adults
 Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Diagnosis and Mangement of Nocturia in Adults Christopher Chapple Professor of Urology Sheffield Teaching Hospitals University of Sheffield Sheffield Hallam University UK 23 rd October 2015 Terminology
Overactive Bladder beyond antimuscarinics
 Overactive Bladder beyond antimuscarinics Marcus Drake Bristol Urological Institute Conflicts of interest; Allergan, AMS, Astellas, Ferring, Pfizer Getting the diagnosis right Improving treatment Improving
Overactive Bladder beyond antimuscarinics Marcus Drake Bristol Urological Institute Conflicts of interest; Allergan, AMS, Astellas, Ferring, Pfizer Getting the diagnosis right Improving treatment Improving
Solifenacin: a new drug for the treatment of overactive bladder and detrusor overactivity
 DRUG PROFILE Solifenacin: a new drug for the treatment of overactive bladder and detrusor overactivity Jean-Jacques Wyndaele University Hospital Antwerp, Department of Urology, 10 Wilrijkstraat, B 2650
DRUG PROFILE Solifenacin: a new drug for the treatment of overactive bladder and detrusor overactivity Jean-Jacques Wyndaele University Hospital Antwerp, Department of Urology, 10 Wilrijkstraat, B 2650
Alpha antagonists from initial concept to routine clinical practice
 european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
european urology 50 (2006) 635 642 available at www.sciencedirect.com journal homepage: www.europeanurology.com Editorial 50th Anniversary Alpha antagonists from initial concept to routine clinical practice
Treatment of OAB in postmenopause. Držislav Kalafatić Department Obstetrics and Gynecology School of Medicine, University of Zagreb
 Treatment of OAB in postmenopause Držislav Kalafatić Department Obstetrics and Gynecology School of Medicine, University of Zagreb Spectrum of overactive bladder Urinary urgency usually accompanied by
Treatment of OAB in postmenopause Držislav Kalafatić Department Obstetrics and Gynecology School of Medicine, University of Zagreb Spectrum of overactive bladder Urinary urgency usually accompanied by
Overactive bladder affects 33 million adults in the United
 Overactive Bladder: Treatment Options in Primary Care Medicine David O. Sussman, DO Overactive bladder is a highly prevalent condition, affecting approximately 33 million adults in the United States. Despite
Overactive Bladder: Treatment Options in Primary Care Medicine David O. Sussman, DO Overactive bladder is a highly prevalent condition, affecting approximately 33 million adults in the United States. Despite
DRUG FORECAST. Select Conditions of the Lower Urinary Tract
 Transdermal Oxybutynin: Novel Drug Delivery for Overactive Bladder Vitalina Rozenfeld, PharmD, BCPS, Stanley Zaslau, MD, Kathleen New Geissel, PharmD, David Lucas, PhD, and Lili Babazadeh, PharmD INTRODUCTION
Transdermal Oxybutynin: Novel Drug Delivery for Overactive Bladder Vitalina Rozenfeld, PharmD, BCPS, Stanley Zaslau, MD, Kathleen New Geissel, PharmD, David Lucas, PhD, and Lili Babazadeh, PharmD INTRODUCTION
Drugs for the overactive bladder: are there differences in persistence and compliance?
 Editorial Drugs for the overactive bladder: are there differences in persistence and compliance? Karl-Erik Andersson 1,2 1 Institute for Regenerative Medicine, Wake Forest University School of Medicine,
Editorial Drugs for the overactive bladder: are there differences in persistence and compliance? Karl-Erik Andersson 1,2 1 Institute for Regenerative Medicine, Wake Forest University School of Medicine,
The Effects of AntimuscarinicTreatments in Overactive Bladder: A Systematic Review and Meta-Analysis
 European Urology European Urology 48 (2005) 5 26 ReviewöOveractive Bladder The Effects of AntimuscarinicTreatments in Overactive Bladder: A Systematic Review and Meta-Analysis Christopher Chapple a, *,
European Urology European Urology 48 (2005) 5 26 ReviewöOveractive Bladder The Effects of AntimuscarinicTreatments in Overactive Bladder: A Systematic Review and Meta-Analysis Christopher Chapple a, *,
Objectives. Prevalence of Urinary Incontinence URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS
 URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
URINARY INCONTINENCE: EVALUATION AND CURRENT TREATMENT OPTIONS Lisa S Pair, MSN, CRNP Division of Urogynecology and Pelvic Reconstructive Surgery Department of Obstetrics and Gynecology University of Alabama
Long-Term Safety, Tolerability and Ef cacy of Extended-Release Tolterodine in the Treatment of Overactive Bladder
 European Urology European Urology 41 (2002) 588±595 Long-Term Safety, Tolerability and Ef cacy of Extended-Release Tolterodine in the Treatment of Overactive Bladder K. Kreder a,*, C. Mayne b, U. Jonas
European Urology European Urology 41 (2002) 588±595 Long-Term Safety, Tolerability and Ef cacy of Extended-Release Tolterodine in the Treatment of Overactive Bladder K. Kreder a,*, C. Mayne b, U. Jonas
Overactive Bladder (OAB) Step Therapy Program Policy Number: Last Review: Origination: Next Review: Policy When Policy Topic is covered:
 Overactive Bladder (OAB) Step Therapy Program Policy Number: 5.01.556 Origination: 07/2013 Last Review: 11/2014 Next Review: 11/2015 Policy BCBSKC will provide coverage for brand name Overactive Bladder
Overactive Bladder (OAB) Step Therapy Program Policy Number: 5.01.556 Origination: 07/2013 Last Review: 11/2014 Next Review: 11/2015 Policy BCBSKC will provide coverage for brand name Overactive Bladder
Urinary Incontinence and Overactive Bladder Update NICE Guidelines on UI for women - GP Perspectives
 Urinary Incontinence and Overactive Bladder Update NICE Guidelines on UI for women - GP Perspectives Arun Sahai PhD, FRCS (Urol) Consultant Urological Surgeon & Honorary Senior Lecturer Guy s Hospital
Urinary Incontinence and Overactive Bladder Update NICE Guidelines on UI for women - GP Perspectives Arun Sahai PhD, FRCS (Urol) Consultant Urological Surgeon & Honorary Senior Lecturer Guy s Hospital
Possible Effect of Carbamazepine A Sodium Channel Blocker on Urinary Bladder Dysfunction in Type-1 Diabetic Patients
 Med. J. Cairo Univ., Vol. 84, No. 1, March: 85-90, 2016 www.medicaljournalofcairouniversity.net Possible Effect of Carbamazepine A Sodium Channel Blocker on Urinary Bladder Dysfunction in Type-1 Diabetic
Med. J. Cairo Univ., Vol. 84, No. 1, March: 85-90, 2016 www.medicaljournalofcairouniversity.net Possible Effect of Carbamazepine A Sodium Channel Blocker on Urinary Bladder Dysfunction in Type-1 Diabetic
Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder
 Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
Urol Sci 21;21(1):38 43 ORIGINAL ARTICLE Efficacy and Adverse Effects of Solifenacin in the Treatment of Lower Urinary Tract Symptoms in Patients With Overactive Bladder Yih-Chou Chen, Chia-Yen Chen, Hann-Chorng
Overactive Bladder (OAB) Step Therapy Program
 Overactive Bladder (OAB) Step Therapy Program Policy Number: 5.01.556 Last Review: 11/2018 Origination: 7/2013 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Overactive Bladder (OAB) Step Therapy Program Policy Number: 5.01.556 Last Review: 11/2018 Origination: 7/2013 Next Review: 11/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Overactive Bladder (OAB) and Quality of Life
 Overactive Bladder (OAB) and Quality of Life Dr. Byron Wong MBBS (Sydney), FRCSEd, FRCSEd (Urol), FCSHK, FHKAM (Surgery) Specialist in Urology Central Urology Clinic Hong Kong Continence Society Annual
Overactive Bladder (OAB) and Quality of Life Dr. Byron Wong MBBS (Sydney), FRCSEd, FRCSEd (Urol), FCSHK, FHKAM (Surgery) Specialist in Urology Central Urology Clinic Hong Kong Continence Society Annual
Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions?
 Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
Review Article SENSORY ACTIONS OF ANTIMUSCARINICS FINNEY et al. Antimuscarinic drugs in detrusor overactivity and the overactive bladder syndrome: motor or sensory actions? STEVEN M. FINNEY, KARL-ERIK
According to the INDICATIONS AND USAGE section of its FDA-approved product labeling (PI):
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Silver Spring, MD 20993 TRANSMITTED BY FACSIMILE Karen L. Walles, M.S. Assistant Director, Regulatory Affairs 3
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Silver Spring, MD 20993 TRANSMITTED BY FACSIMILE Karen L. Walles, M.S. Assistant Director, Regulatory Affairs 3
Urogynecology Office. Can You Hold? An Update on the Treatment of OAB. Can You Hold? Urogynecology Office
 Urogynecology Office Urogynecology Office Can You Hold? An Update on the Treatment of OAB Can You Hold? Karen Noblett, MD Professor and Chair Department of OB/GYN University of California, Riverside Disclosures
Urogynecology Office Urogynecology Office Can You Hold? An Update on the Treatment of OAB Can You Hold? Karen Noblett, MD Professor and Chair Department of OB/GYN University of California, Riverside Disclosures
Comparison of efficacy and tolerability of pharmacological treatment for the overactive bladder in women: A network meta-analysis
 RESEARCH Comparison of efficacy and tolerability of pharmacological treatment for the overactive bladder in women: A network meta-analysis Sivalingam Nalliah, Pou Wee Gan, Premjit K Masten Singh, Piravin
RESEARCH Comparison of efficacy and tolerability of pharmacological treatment for the overactive bladder in women: A network meta-analysis Sivalingam Nalliah, Pou Wee Gan, Premjit K Masten Singh, Piravin
Current drug treatments for female urinary incontinence Tarang Majmudar MRCOG and Mark Slack MMed, FRCOG, FCOG(SA)
 Drug review Incontinence Current drug treatments for female urinary incontinence Tarang Majmudar MRCOG and Mark Slack MMed, FRCOG, FCOG(SA) Skyline Imaging Ltd Several new drug treatments are now marketed
Drug review Incontinence Current drug treatments for female urinary incontinence Tarang Majmudar MRCOG and Mark Slack MMed, FRCOG, FCOG(SA) Skyline Imaging Ltd Several new drug treatments are now marketed
Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder
 European Urology European Urology 45 (2004) 240 244 Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder A. Raes a,, P. Hoebeke b, I. Segaert a, E. Van
European Urology European Urology 45 (2004) 240 244 Retrospective Analysis of Efficacy and Tolerability of Tolterodine in Children with Overactive Bladder A. Raes a,, P. Hoebeke b, I. Segaert a, E. Van
Report on New Patented Drugs Enablex
 Report on New Patented Drugs Enablex Under its transparency initiative, the PMPRB publishes the results of the reviews of new patented drugs by Board Staff, for purposes of applying the PMPRB s Excessive
Report on New Patented Drugs Enablex Under its transparency initiative, the PMPRB publishes the results of the reviews of new patented drugs by Board Staff, for purposes of applying the PMPRB s Excessive
CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION
 CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION PROPIVERINE HYDROCHLORIDE (Mictoryl/Mictoryl Pediatric Duchesnay Inc.) Indication: Overactive bladder This document was originally issued on April
CADTH CANADIAN DRUG EXPERT COMMITTEE FINAL RECOMMENDATION PROPIVERINE HYDROCHLORIDE (Mictoryl/Mictoryl Pediatric Duchesnay Inc.) Indication: Overactive bladder This document was originally issued on April
Pharmacokinetics, Safety, and Tolerability of Solifenacin in Patients With Renal Insufficiency
 J Pharmacol Sci 103, 67 74 (2007) Journal of Pharmacological Sciences 2007 The Japanese Pharmacological Society Full Paper Pharmacokinetics, Safety, and Tolerability of Solifenacin in Patients With Renal
J Pharmacol Sci 103, 67 74 (2007) Journal of Pharmacological Sciences 2007 The Japanese Pharmacological Society Full Paper Pharmacokinetics, Safety, and Tolerability of Solifenacin in Patients With Renal
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline.
 Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU guideline. TARGET POPULATION Eligibility Decidable (Y or N) Inclusion Criterion non-neurogenic OAB Exclusion Criterion
Urinary Incontinence for the Primary Care Provider
 Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
Urinary Incontinence for the Primary Care Provider Diana J Scott FNP-BC https://youtu.be/gmzaue1ojn4 1 Assessment of Urinary Incontinence Urge Stress Mixed Other overflow, postural, continuous, insensible,
H6D-MC-LVHR Clinical Study Report Synopsis Page LVHR Synopsis (LY450190)
 H6D-MC-LVHR Clinical Study Report Synopsis Page 1 2. LVHR Synopsis H6D-MC-LVHR Clinical Study Report Synopsis Page 2 Clinical Study Report Synopsis: Study H6D-MC-LVHR Title of Study: A Randomized, Double-Blind,
H6D-MC-LVHR Clinical Study Report Synopsis Page 1 2. LVHR Synopsis H6D-MC-LVHR Clinical Study Report Synopsis Page 2 Clinical Study Report Synopsis: Study H6D-MC-LVHR Title of Study: A Randomized, Double-Blind,
Management of OAB. Lynsey McHugh. Consultant Urological Surgeon. Lancashire Teaching Hospitals
 Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Management of OAB Lynsey McHugh Consultant Urological Surgeon Lancashire Teaching Hospitals Summary Physiology Epidemiology Definitions NICE guidelines Evaluation Conservative management Medical management
Efficacy and Safety of Propiverine in Children with Overactive Bladder
 www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.4.275 Pediatric Urology Efficacy and Safety of Propiverine in Children with Overactive Bladder Woo Jung Kim, Dong-Gi Lee 1, Sang Wook Lee 2, Yoon
www.kjurology.org http://dx.doi.org/10.4111/kju.2012.53.4.275 Pediatric Urology Efficacy and Safety of Propiverine in Children with Overactive Bladder Woo Jung Kim, Dong-Gi Lee 1, Sang Wook Lee 2, Yoon
Drug Class Review on Overactive Bladder Drugs
 Drug Class Review on Overactive Bladder Drugs Preliminary Scan Report #1 February 2014 Last Summary Review (June 2013) The Agency for Healthcare Research and Quality has not yet seen or approved this report
Drug Class Review on Overactive Bladder Drugs Preliminary Scan Report #1 February 2014 Last Summary Review (June 2013) The Agency for Healthcare Research and Quality has not yet seen or approved this report
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Urinary incontinence in women: the management of urinary incontinence in women 1.1 Short title Urinary incontinence in women
Overactive Bladder Syndrome
 Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
Overactive Bladder Syndrome behavioural modifications to pharmacological and surgical treatments Dr Jos Jayarajan Urologist Austin Health, Eastern Health Warringal Private, Northpark Private, Epworth Overactive
2/9/2008. Men Women. Prevalence of OAB. Men: 16.0% Women: 16.9% Prevalence (%) < Age (years)
 Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
Definition Botox for Overactive Bladder Donna Y. Deng Assistant Professor UCSF Department of Urology Urinary urgency With or without urge incontinence Usually with frequency & nocturia International Continence
ORIGINAL CLINICAL ARTICLE
 Received: 20 January 2017 Accepted: 25 April 2017 DOI: 10.1002/nau.23315 ORIGINAL CLINICAL ARTICLE Patient-reported outcomes from SYNERGY, a randomized, double-blind, multicenter study evaluating combinations
Received: 20 January 2017 Accepted: 25 April 2017 DOI: 10.1002/nau.23315 ORIGINAL CLINICAL ARTICLE Patient-reported outcomes from SYNERGY, a randomized, double-blind, multicenter study evaluating combinations
Rational Pharmacotherapy for LUTS in Older People. Dr William Gibson MBChB MRCP
 Rational Pharmacotherapy for LUTS in Older People Dr William Gibson MBChB MRCP Frailty Frailty = state of increased vulnerability resulting from agingassociated decline in reserve and function NOT synonymous
Rational Pharmacotherapy for LUTS in Older People Dr William Gibson MBChB MRCP Frailty Frailty = state of increased vulnerability resulting from agingassociated decline in reserve and function NOT synonymous
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA
 Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Kathleen C. Kobashi, MD, FACS Head, Section of Urology and Renal Transplantation Virginia Mason Medical Center, Seattle, WA Disclosures Advisory Board and/or Speaker Allergan Medtronic Astellas AUA Guidelines
Incidence and risk factors of recurrence of overactive bladder symptoms after discontinuation of successful medical treatment
 Original Article - Lower Urinary Tract Dysfunction https://doi.org/10.4111/icu.2017.58.1.42 pissn 2466-0493 eissn 2466-054X Incidence and risk factors of recurrence of overactive bladder symptoms after
Original Article - Lower Urinary Tract Dysfunction https://doi.org/10.4111/icu.2017.58.1.42 pissn 2466-0493 eissn 2466-054X Incidence and risk factors of recurrence of overactive bladder symptoms after
Diagnosis and Treatment of Overactive Bladder
 Diagnosis and Treatment of Overactive Bladder Case study: Mr. Lin I I have started to rush out of meetings to go to the toilet I I need to void every one hour I I used to be quite active. This is becoming
Diagnosis and Treatment of Overactive Bladder Case study: Mr. Lin I I have started to rush out of meetings to go to the toilet I I need to void every one hour I I used to be quite active. This is becoming
Muscarinic receptor antagonists for overactive bladder
 Great drug classes ANTIMUSCARINIC DRUGS FOR OAB From time to time we publish a full review of drugs that are available for the treatment of common conditions. In this issue, the review is written by two
Great drug classes ANTIMUSCARINIC DRUGS FOR OAB From time to time we publish a full review of drugs that are available for the treatment of common conditions. In this issue, the review is written by two
Long-term persistence with mirabegron in a real-world clinical setting
 International Journal of Urology (2018) 25, 501--506 doi: 10.1111/iju.13558 Original Article: Clinical Investigation Long-term persistence with in a real-world clinical setting Naoki Wada, Masaki Watanabe,
International Journal of Urology (2018) 25, 501--506 doi: 10.1111/iju.13558 Original Article: Clinical Investigation Long-term persistence with in a real-world clinical setting Naoki Wada, Masaki Watanabe,
OVERACTIVE BLADDER (OAB)
 OVERACTIVE BLADDER (OAB) Ms Taryn Hallam Alana Health Care for Women Women s Health Training Associates OVERACTIVE BLADDER The most misdiagnosed and misunderstood of all the urinary disorders. Problem???
OVERACTIVE BLADDER (OAB) Ms Taryn Hallam Alana Health Care for Women Women s Health Training Associates OVERACTIVE BLADDER The most misdiagnosed and misunderstood of all the urinary disorders. Problem???
Review Anticholinergic drugs for overactive bladder: a review of the literature and practical guide
 The Obstetrician & Gynaecologist 10.1576/toag.9.1.009.27290 www.rcog.org.uk/togonline 2007;9:9 14 Review Review Anticholinergic drugs for overactive bladder: a review of the literature and practical guide
The Obstetrician & Gynaecologist 10.1576/toag.9.1.009.27290 www.rcog.org.uk/togonline 2007;9:9 14 Review Review Anticholinergic drugs for overactive bladder: a review of the literature and practical guide
Efficacy and safety of daily mirabegron 50 mg in male patients with overactive bladder: a critical analysis of five phase III studies
 702797TAU0010.1177/1756287217702797Therapeutic Advances in UrologyA. Tubaro research-article2017 Therapeutic Advances in Urology Original Research Efficacy and safety of daily mirabegron 50 mg in male
702797TAU0010.1177/1756287217702797Therapeutic Advances in UrologyA. Tubaro research-article2017 Therapeutic Advances in Urology Original Research Efficacy and safety of daily mirabegron 50 mg in male
Duloxetine in women awaiting surgery
 DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
DOI: 1.1111/j.1471-528.6.879.x www.blackwellpublishing.com/bjog Review article H Drutz Ontario Power Generation Building, Toronto, Ontario, Canada Correspondence: Prof. Dr H Drutz, Mount Sinai Hospital,
Management of urinary incontinence in older people Shashi Gadgil BSc, MRCP and Adrian Wagg FRCP
 Management of urinary incontinence in older people Shashi Gadgil BSc, MRCP and Adrian Wagg FRCP Prevalence (%) 40 35 30 25 20 15 10 5 Our series Prescribing in older people gives practical advice for successful
Management of urinary incontinence in older people Shashi Gadgil BSc, MRCP and Adrian Wagg FRCP Prevalence (%) 40 35 30 25 20 15 10 5 Our series Prescribing in older people gives practical advice for successful
Primary Care management of Overactive Bladder (OAB)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Primary Care management of Overactive Bladder (OAB) Prescribing Tips All medicines for OAB have similar dose-related efficacy. More than one agent (up
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Primary Care management of Overactive Bladder (OAB) Prescribing Tips All medicines for OAB have similar dose-related efficacy. More than one agent (up
Reevaluating the Health-Related Quality of Life Impact and the Economic Burden of Urgency Urinary Incontinence
 EUROPEAN UROLOGY SUPPLEMENTS 10 (2011) 3 7 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reevaluating the Health-Related Quality of Life Impact and the Economic Burden of
EUROPEAN UROLOGY SUPPLEMENTS 10 (2011) 3 7 available at www.sciencedirect.com journal homepage: www.europeanurology.com Reevaluating the Health-Related Quality of Life Impact and the Economic Burden of
Supplement. Updated Literature Search for Pharmacologic Treatments for Urgency UI
 Supplement. Updated Literature Search for Pharmacologic Treatments for Urgency UI Authors: Tatyana A. Shamliyan, MD, MS Senior Director, Evidence-Based Medicine Quality Assurance Elsevier 1600 JFK Blvd,
Supplement. Updated Literature Search for Pharmacologic Treatments for Urgency UI Authors: Tatyana A. Shamliyan, MD, MS Senior Director, Evidence-Based Medicine Quality Assurance Elsevier 1600 JFK Blvd,
Additional low-dose antimuscarinics can improve overactive bladder symptoms in patients with suboptimal response to beta 3 agonist monotherapy
 Original Article - Female Urology Investig Clin Urol Posted online 217.6.27 Posted online 217.6.27 pissn 2466-493 eissn 2466-54X Additional low-dose antimuscarinics can improve overactive bladder symptoms
Original Article - Female Urology Investig Clin Urol Posted online 217.6.27 Posted online 217.6.27 pissn 2466-493 eissn 2466-54X Additional low-dose antimuscarinics can improve overactive bladder symptoms
Association of BPH with OAB: The Plumbing or the Pump?
 Association of BPH with OAB: The Plumbing or the Pump? Ryan P. Terlecki, MD FACS Associate Professor of Urology Director, Men s Health Clinic Director, GURS Fellowship in Reconstructive Urology, Prosthetic
Association of BPH with OAB: The Plumbing or the Pump? Ryan P. Terlecki, MD FACS Associate Professor of Urology Director, Men s Health Clinic Director, GURS Fellowship in Reconstructive Urology, Prosthetic
Overactive Bladder: Prevalence and Implications in Brazil
 european urology 49 (2006) 1087 1092 available at www.sciencedirect.com journal homepage: www.europeanurology.com Neuro-Urology Overactive Bladder: Prevalence and Implications in Brazil Claudio Teloken
european urology 49 (2006) 1087 1092 available at www.sciencedirect.com journal homepage: www.europeanurology.com Neuro-Urology Overactive Bladder: Prevalence and Implications in Brazil Claudio Teloken
What is on the Horizon in Drug Therapy for OAB?
 What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
What is on the Horizon in Drug Therapy for OAB? K-E Andersson, MD, PhD Wake Forest Institute for Regenerative Medicine Wake Forest University School of Medicine Winston Salem, North Carolina Disclosures
Hiroshi Yagi, M.D., Gaku Arai, M.D., Shigehiro Soh, M.D., Hiroshi Okada, M.D.
 Dokkyo Journal of Medical Sciences (1)(2017) (1):9 once-daily 15,2017 oxybutynin patch for overactive bladder in patients not tolerating oral antimuscarinic drugs 9 Efficacy and Safety of Once-daily Oxybutynin
Dokkyo Journal of Medical Sciences (1)(2017) (1):9 once-daily 15,2017 oxybutynin patch for overactive bladder in patients not tolerating oral antimuscarinic drugs 9 Efficacy and Safety of Once-daily Oxybutynin
FDA Briefing Document for Nonprescription Drugs Advisory Committee
 FDA Briefing Document for Nonprescription Drugs Advisory Committee Oxybutynin Transdermal System NDA 202211 Proposed Indication: Treats overactive bladder in women Topic: Partial Rx-to-OTC switch for oxybutynin
FDA Briefing Document for Nonprescription Drugs Advisory Committee Oxybutynin Transdermal System NDA 202211 Proposed Indication: Treats overactive bladder in women Topic: Partial Rx-to-OTC switch for oxybutynin
Overactive bladder (OAB) is defined. Treatment of Overactive Bladder: A Model Comparing Extended-release Formulations of Tolterodine and Oxybutynin
 REPORTS Treatment of Overactive Bladder: A Model Comparing Extended-release Formulations of Tolterodine and Oxybutynin Eleanor M. Perfetto, PhD; Prasun Subedi, MS; and Zhanna Jumadilova, MD, MBA Abstract
REPORTS Treatment of Overactive Bladder: A Model Comparing Extended-release Formulations of Tolterodine and Oxybutynin Eleanor M. Perfetto, PhD; Prasun Subedi, MS; and Zhanna Jumadilova, MD, MBA Abstract
Drug Class Review Agents for Overactive Bladder
 Drug Class Review Agents for Overactive Bladder Final Update 4 Report March 2009 The purpose of reports is to make available information regarding the comparative clinical effectiveness and harms of different
Drug Class Review Agents for Overactive Bladder Final Update 4 Report March 2009 The purpose of reports is to make available information regarding the comparative clinical effectiveness and harms of different
Ariana L. Smith and Alan J. Wein Division of Urology, Hospital of University of Pennsylvania, Philadelphia, PA, USA
 ; 2011 Mini Reviews PHARMACOLOGICAL MANAGEMENT OF NOCTURIA SMITH and WEIN BJUI Outcomes of pharmacological management of with non-antidiuretic agents: does statistically significant equal clinically significant?
; 2011 Mini Reviews PHARMACOLOGICAL MANAGEMENT OF NOCTURIA SMITH and WEIN BJUI Outcomes of pharmacological management of with non-antidiuretic agents: does statistically significant equal clinically significant?
The relationship between urinary symptom questionnaires and urodynamic diagnoses: an analysis of two methods of questionnaire administration
 BJOG: an International Journal of Obstetrics and Gynaecology May 2004, Vol. 111, pp. 468 474 DOI: 1 0. 1111/j.1471-0528.2004.00126.x The relationship between urinary symptom questionnaires and urodynamic
BJOG: an International Journal of Obstetrics and Gynaecology May 2004, Vol. 111, pp. 468 474 DOI: 1 0. 1111/j.1471-0528.2004.00126.x The relationship between urinary symptom questionnaires and urodynamic
NICE Pathways bring together all NICE guidance, quality standards and other NICE information on a specific topic.
 bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
bring together all NICE guidance, quality standards and other NICE information on a specific topic. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published.
Content validity and test-retest reliability of patient perception of intensity of urgency scale (PPIUS) for overactive bladder
 Notte et al. BMC Urology 2012, 12:26 RESEARCH ARTICLE Open Access Content validity and test-retest reliability of patient perception of intensity of urgency scale (PPIUS) for overactive bladder Sherilyn
Notte et al. BMC Urology 2012, 12:26 RESEARCH ARTICLE Open Access Content validity and test-retest reliability of patient perception of intensity of urgency scale (PPIUS) for overactive bladder Sherilyn
The patient, your co-pilot in assessing LUTS
 The patient, your co-pilot in assessing LUTS Frank Van der Aa Leuven, Belgium This symposium is supported by Astellas Pharma Europe Ltd., including speaker honoraria and production of materials the slides
The patient, your co-pilot in assessing LUTS Frank Van der Aa Leuven, Belgium This symposium is supported by Astellas Pharma Europe Ltd., including speaker honoraria and production of materials the slides
Treatment of overactive bladder in the aging population: focus on darifenacin
 REVIEW Treatment of overactive bladder in the aging population: focus on darifenacin Swati Jha Matthew Parsons Department of Urogynaecology, Birmingham Women s Hospital, Birmingham. UK Abstract: Anticholinergics
REVIEW Treatment of overactive bladder in the aging population: focus on darifenacin Swati Jha Matthew Parsons Department of Urogynaecology, Birmingham Women s Hospital, Birmingham. UK Abstract: Anticholinergics
HEALTH AND WELLBEING IMPACT AND TREATMENT OF NOCTURIA A REVIEW OF THE LITERATURE
 HEALTH AND WELLBEING IMPACT AND TREATMENT OF NOCTURIA A REVIEW OF THE LITERATURE Nadir I. Osman, 1 Christopher Hillary, 1 *Christopher R. Chapple 2 1. Clinical Research Fellow, Department of Urology, Royal
HEALTH AND WELLBEING IMPACT AND TREATMENT OF NOCTURIA A REVIEW OF THE LITERATURE Nadir I. Osman, 1 Christopher Hillary, 1 *Christopher R. Chapple 2 1. Clinical Research Fellow, Department of Urology, Royal
Technology appraisal guidance Published: 26 June 2013 nice.org.uk/guidance/ta290
 Mirabegron for treating symptoms of overactive bladder Technology appraisal guidance Published: 26 June 2013 nice.org.uk/guidance/ta290 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Mirabegron for treating symptoms of overactive bladder Technology appraisal guidance Published: 26 June 2013 nice.org.uk/guidance/ta290 NICE 2018. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Botulinum Toxin Injection for OAB: Indications & Technique
 Classification of LUTS Botulinum Toxin Injection for OAB: Indications & Technique Sherif Mourad, MD Professor of Urology, Ain Shams University General Secretary of International Continence President of
Classification of LUTS Botulinum Toxin Injection for OAB: Indications & Technique Sherif Mourad, MD Professor of Urology, Ain Shams University General Secretary of International Continence President of
Philadelphia College of Osteopathic Medicine. Victoria J. Kopec Philadelphia College of Osteopathic Medicine,
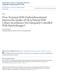 Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Treatment With OnabotulinumtoxinA
Philadelphia College of Osteopathic Medicine DigitalCommons@PCOM PCOM Physician Assistant Studies Student Scholarship Student Dissertations, Theses and Papers 2015 Does Treatment With OnabotulinumtoxinA
Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial
 ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
ORIGINAL ARTICLE Posterior Tibial Nerve Stimulation for Treating Neurologic Bladder in Women: a Randomized Clinical Trial Tahereh Eftekhar 1, Nastaran Teimoory 1, Elahe Miri 1, Abolghasem Nikfallah 2,
Overactive bladder: prevalence, risk factors and relation to stress incontinence in middle-aged women.
 Overactive bladder: prevalence, risk factors and relation to stress incontinence in middle-aged women. Teleman, Pia; Lidfeldt, Jonas; Nerbrand, Christina; Samsioe, Göran; Mattiasson, Anders Published in:
Overactive bladder: prevalence, risk factors and relation to stress incontinence in middle-aged women. Teleman, Pia; Lidfeldt, Jonas; Nerbrand, Christina; Samsioe, Göran; Mattiasson, Anders Published in:
A Comparative Study on the Efficacy of Solifenacin Succinate in Patients with Urinary Frequency with or without Urgency
 A Comparative Study on the Efficacy of Solifenacin Succinate in Patients with Urinary Frequency with or without Urgency Ji-Yeon Han 1, Kyu-Sung Lee 2, Won Hee Park 3, Choal Hee Park 4, Jeong Gu Lee 5,
A Comparative Study on the Efficacy of Solifenacin Succinate in Patients with Urinary Frequency with or without Urgency Ji-Yeon Han 1, Kyu-Sung Lee 2, Won Hee Park 3, Choal Hee Park 4, Jeong Gu Lee 5,
