46 OBG Management September 2011 Vol. 23 No. 9 obgmanagement.com
|
|
|
- Sherman Dawson
- 5 years ago
- Views:
Transcription
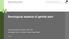
1 The lower vagina and vulva are richly supplied with peripheral nerves and are, therefore, sensitive to pain, particularly the region of the hymeneal ring. Although the pudendal nerve (arrow) courses through the area, it is an uncommon source of vulvar pain. ALEXANDRA BAKER for obg Management 46
2 first of 3 parts Vulvar pain syndromes Your first challenge is making the correct diagnosis Many cases of generalized vulvodynia and localized vulvodynia (vestibulodynia) are mistakenly attributed to yeast infection, pudendal neuralgia, and other entities. Avoid those pitfalls by using a reliable roadmap for evaluation, differentiation, and identification of the various forms of vulvar pain. Neal M. Lonky, MD, MPH, moderator; Libby Edwards, MD, Jennifer Gunter, MD, and Hope K. Haefner, MD, panelists Although the incidence of vulvar pain has increased over the past decade thanks to both greater awareness and increasing numbers of affected women the phenomenon is not a recent development. As early as 1874, T. Galliard Thomas wrote, [T] his disorder, although fortunately not very frequent, is by no means very rare. 1 He went on to express surprise that it had not been more generally and fully described. Despite the focus Thomas directed to the issue, vulvar pain did not get much attention until the 21st century, when a number of studies began to gauge its prevalence. For example, in a study in Boston of about 5,000 women, the lifetime prevalence of chronic vulvar pain was 16%. 2 And in a study in Texas, the prevalence of vulvar pain in an urban, largely minority population was estimated to be 11%. 3 The Boston study also reported that nearly 40% of women chose not to seek treatment, and, of those who did, 60% saw three or more doctors, many of whom could not provide a diagnosis. 2 Clearly, there is a need for comprehensive information on vulvar pain and its causes, symptoms, diagnosis, and treatment. To address the lack of guidance, OBG Management Contributing Editor Neal M. Lonky, MD, assembled a panel of experts on vulvar pain syndromes and invited them to share their considerable knowledge. The ensuing discussion, presented in three parts, offers a gold mine of information. In this opening article, the panel focuses on causes, symptomatology, and diagnosis of this common complaint. In Part 2, which will appear in the October issue of this journal, the focus is the bounty of treatment options. Part 3 follows in November, when the discussion shifts to vestibulodynia. Common diagnoses and misdiagnoses Dr. Lonky: What are the most common diagnoses when vulvar pain is the complaint? Dr. Gunter: The most common cause of chronic vulvar pain is vulvodynia, although lichen simplex chronicus, chronic yeast infections, and non-neoplastic epithelial disorders, such as lichen sclerosus and lichen planus, can also produce irritation and pain. In postmenopausal women, atrophic vaginitis can In this Article What needs to be ruled out for a diagnosis of vulvodynia? page 52 Conditions other than vulvodynia that are associated with vulvar pain page 54 How common is pudendal neuralgia? page 56 Vol. 23 No. 9 September 2011 OBG Management 47
3 The OBG Management expert panel neal M. Lonky, MD, MPH, moderator of this discussion, is Clinical Professor of Obstetrics and Gynecology at the University of California Irvine and a member of the Board of Directors of Southern California Permanente Medical Group. He serves as an OBG Management Contributing Editor. libby Edwards, MD, is Adjunct Clinical Associate Professor of Dermatology at the University of North Carolina in Chapel Hill, NC, and Chief of Dermatology at Carolinas Medical Center in Charlotte, NC. Dr. Edwards is a Past President and Past Secretary General of the International Society for the Study of Vulvovaginal Disease. Jennifer Gunter, MD, is Director of Pelvic Pain and Vulvovaginal Disorders for Kaiser Permanente in San Francisco, Calif. Hope K. Haefner, MD, is Professor of Obstetrics and Gynecology at the University of Michigan Hospitals and Co-Director of the University of Michigan Center for Vulvar Diseases in Ann Arbor, Mich. also cause a burning pain, although symptoms are typically more vaginal than vulvar. Yeast and lichen simplex chronicus typically produce itching, although sometimes they can present with irritation and pain, so they must be considered in the differential diagnosis. It is important to remember that many women with vulvodynia have used multiple topical agents and may have developed complex hygiene rituals in an attempt to treat their symptoms, which can result in a secondary lichen simplex chronicus. That said, there is a high frequency of misdiagnosis with yeast. For example, in a study by Nyirjesy and colleagues, two thirds of women who were referred to a tertiary clinic for chronic vulvovaginal candidiasis were found to have a noninfectious entity instead most commonly lichen simplex chronicus and vulvodynia. 4 Dr. Edwards: The most common diagnosis for vulvar pain is vulvodynia. However, the definition of vulvodynia is pain i.e., burning, rawness, irritation, soreness, aching, or stabbing or stinging sensations in the absence of skin disease, infection, or specific neurologic disease. Therefore, even though the usual cause of vulvar pain is vulvodynia, it is a diagnosis of exclusion, and skin disease, infection, and neurologic disease must be ruled out. In regard to infection, Candida albicans and bacterial vaginosis (BV) are usually the first conditions that are considered when a patient complains of vulvar pain, but they are not common causes of vulvar pain and are never causes of chronic vulvar pain. Very rarely they may cause recurrent pain that clears, at least briefly, with treatment. Candida albicans is usually primarily pruritic, and BV produces discharge and odor, sometimes with minor symptoms. Nonalbicans Candida (e.g., Candida glabrata) is nearly always asymptomatic, but it occasionally causes irritation and burning. Group B streptococcus is another infectious entity that very, very occasionally causes irritation and dyspareunia but is usually only a colonizer. Herpes simplex virus is a cause of recurrent but not chronic pain. Chronic pain is more likely to be caused by skin disease than by infection. Lichen simplex chronicus causes itching; any pain is due to erosions from scratching. Dr. Haefner: Several other infectious conditions or their treatments can cause vulvar pain. For example, herpes (particularly primary herpes infection) is classically associated with vulvar pain. The pain is so great that, at times, the patient requires admission for pain control. Surprisingly, despite the known pain of herpes, approximately 80% of patients who have it are unaware of their diagnosis. Although condyloma is generally a painless condition, many patients complain of pain following treatment for it, whether treatment continued on page 52 48
4 TABLE 1 Terminology and classification of vulvar pain from the International Society for the Study of Vulvovaginal Disease A. Vulvar pain related to a specific disorder 1. Infectious (including candidiasis, herpes) 2. Inflammatory (lichen planus, immunobullous disorders) 3. Neoplastic (Paget s disease, squamous cell carcinoma) 4. Neurologic (herpes neuralgia, spinal nerve compression) B. Vulvodynia 1. Generalized a. Provoked (sexual, nonsexual, or both) b. Unprovoked c. Mixed (provoked and unprovoked) 2. Localized (including vestibulodynia, clitorodynia, hemivulvodynia) a. Provoked (sexual, nonsexual, or both) b. Unprovoked c. Mixed (provoked and unprovoked) SOURCE: Moyal-Barracco and Lynch. 5 Reproduced with permission from the Journal of Reproductive Medicine. Skin diseases that affect the vulva are usually pruritic pain is a later sign. Libby Edwards, MD involves topical medications or laser surgery. Chancroid is a painful vulvar ulcer. Trichomonas can sometimes be associated with vulvar pain. Dr. Lonky: What terminology do we use when we discuss vulvar pain? Dr. Haefner: The current terminology used to describe vulvar pain was published in 2004, after years of debate over nomenclature within the International Society for the Study of Vulvovaginal Disease. 5 The terminology lists two major categories of vulvar pain: pain related to a specific disorder. This category encompasses numerous conditions that feature an abnormal appearance of the vulva (Table 1). vulvodynia, in which the vulva appears normal, other than occasional erythema, which is most prominent at the duct openings (vestibular ducts Bartholin s and Skene s). As for vulvar pain, there are two major forms: hyperalgesia (a low threshold for pain) allodynia (pain in response to light touch). Some diseases that are associated with vulvar pain do not qualify for the diagnosis of vulvodynia (Table 2, page 54) because they are associated with an abnormal appearance of the vulva. What needs to be ruled out for a diagnosis of vulvodynia? Dr. Lonky: What skin diseases need to be ruled out before vulvodynia can be diagnosed? Dr. Edwards: Skin diseases that affect the vulva are usually pruritic pain is a later sign. Lichen simplex chronicus (also known as eczema) is pruritus caused by any irritant; any pain that arises is produced by visible excoriations from scratching. Lichen sclerosus manifests as white epithelium that has a crinkling, shiny, or waxy texture. It can produce pain, especially dyspareunia. The pain is caused by erosions that arise from fragility and introital narrowing and inelasticity. Vulvovaginal lichen planus is usually erosive and preferentially affects mucous membranes, especially the vestibule; it sometimes affects the vagina and mouth, as well. Desquamative inflammatory vaginitis is most likely a skin disease that affects only the vagina. It involves introital redness and a clinically and microscopically purulent vaginal discharge that also reveals parabasal cells and absent lactobacilli. Dr. Lonky: You mentioned that neurologic diseases can sometimes cause vulvar pain. Which ones? Dr. Edwards: Pudendal neuralgia, diabetic neuropathy, and post-herpetic neuralgia are the most common specific neurologic causes of vulvar pain. Multiple sclerosis can also produce pain syndromes. Post-herpetic neuralgia follows herpes zoster not herpes simplex virus infection. Dr. Lonky: Any other conditions that can cause vulvar pain? Dr. Haefner: Aphthous ulcers are common and are often flared by stress. Non-neoplastic epithelial disorders are also seen frequently in health-care providers 52
5 Sixty-five percent to 75% of women referred to my clinic with chronic yeast actually have lichen simplex chronicus or vulvodynia. Jennifer Gunter, MD TABLE 2 Conditions other than vulvodynia that are associated with vulvar pain Acute irritant contact dermatitis (e.g., erosion due to podofilox, imiquimod, cantharidin, fluorouracil, or podophyllin toxin) Aphthous ulcer Atrophy Bartholin s abscess Candidiasis Carcinoma Chronic irritant contact dermatitis Endometriosis Herpes (simplex and zoster) Immunobullous diseases (including cicatricial pemphigoid, pemphigus vulgaris, linear immunoglobulin A disease, etc.) Lichen planus Lichen sclerosus Podophyllin overdose (see above) Prolapsed urethra Sjögren s syndrome Trauma Trichomoniasis Vulvar intraepithelial neoplasia offices; many patients who experience them report pain on the vulva. It is always important to consider cancer when a patient has an abnormal vulvar appearance and pain that has persisted despite treatment. What are the most common vulvar pain syndromes? Dr. Lonky: If you were to rank vulvar pain syndromes according to their prevalence, what would the most common syndromes be? Dr. Gunter: Given the misdiagnosis of many women, who are told they have chronic yeast infection, as I mentioned, it s hard to know which vulvar pain syndromes are most prevalent. I suspect that lichen simplex chronicus is most common, followed by vulvodynia, with chronic yeast infection a distant third. My experience reflects what Nyirjesy and colleagues 4 found: 65% to 75% of women referred to my clinic with chronic yeast actually have lichen simplex chronicus or vulvodynia. In postmenopausal women, atrophic vaginitis is also a consideration; it s becoming more common now that the use of systemic hormone replacement therapy is decreasing. Dr. Lonky: What about subsets of vulvodynia? Which ones are most common? Dr. Edwards: There is good evidence of marked overlap among subsets of vulvodynia. The vast majority of women who have vulvodynia experience primarily provoked vestibular pain, regardless of age. However, I find that almost all patients also report pain that extends beyond the vestibule at times, as well as occasional unprovoked pain. The diagnosis requires the exclusion of other causes of vulvar pain, and the subset is identified by the location of pain (that is, is it strictly localized or generalized or even migratory?) and its provoked or unprovoked nature. Localized clitoral pain and vulvar pain localized to one side of the vulva are extremely uncommon, but they do occur. And although I rarely encounter teenagers and prepubertal children who have vulvodynia, I do have patients in both age groups who have vulvodynia. Dr. Lonky: Are there racial differences in the prevalence of vulvodynia? Dr. Edwards: Although several good studies show that women of African descent and white patients are equally likely to experience vulvodynia, the vast majority (99%) of my patients who have vulvodynia are white. My patients of African descent consult me primarily for itching or discharge. My local demographics prevent me from judging the likelihood of Asians having vulvodynia, and our Hispanic population has limited access to health care. In general, I don t think that demographics are useful in making the diagnosis of vulvodynia. continued on page 56 54
6 Women who have vulvodynia often have other medical problems as well. Hope K. Haefner, MD Do women who have vulvar pain tend to have comorbidities? Dr. Lonky: Do your patients who have vulvodynia or another vulvar pain syndrome tend to have comorbidities? If so, is this information helpful in establishing the diagnosis and planning therapy? Dr. Haefner: Women who have vulvodynia often have other medical problems as well. In my practice, when new patients who have vulvodynia complete their intake survey, they often report a history of headache, irritable bowel syndrome, interstitial cystitis, fibromyalgia, 6 chronic fatigue syndrome, back pain, and temporomandibular joint (TMJ) disorder. These comorbidities are not particularly helpful in establishing the diagnosis of vulvodynia, but they are an important consideration when choosing therapy for the patient. Often, the medications chosen to treat one condition will also benefit another condition. However, it s important to check for potential interactions between drugs before prescribing a new treatment. Dr. Gunter: A significant number of women who have vulvodynia also have other chronic pain syndromes. For example, the incidence of bladder pain syndrome interstitial cystitis is 68% to 82% among women who have vulvodynia, compared with a baseline rate among all women of 6% to 11% The rate of irritable bowel syndrome is more than doubled among women who have vulvodynia, compared with the general population (27% versus 12%). 8 Another common comorbidity, hypertonic somatic dysfunction of the pelvic floor, is identified in 10% to 90% of women who have chronic vulvar pain. 8,11,12 These women also have a higher incidence of nongenital pain syndromes, such as fibromyalgia, migraine, and TMJ dysfunction, than the general population, as Dr. Haefner noted. 8,12,13 Many studies have evaluated psychological and emotional contributions to chronic vulvar pain. Pain and depression are intimately related the incidence of depression among all people who experience chronic pain ranges from 27% to 54%, compared with 5% to 17% among the general population The relationship is complex because chronic illness in general is associated with depression. Nevertheless, several studies have noted an increase in anxiety, stress, and depression among women who have vulvodynia I screen every patient for depression using a Patient Health Questionnaire (PHQ-9); I also screen for anxiety. I find that a significant percentage of patients in my clinic are depressed or have an anxiety disorder. Failure to address these comorbidities makes treatment very difficult. I typically prescribe citalopram (Celexa), although there is some question whether it can safely be combined with a tricyclic antidepressant. We also offer stress-reduction classes, teach every patient the value of diaphragmatic breathing, offer mind-body classes for anxiety and stress, and provide intensive programs where the patient can learn important self-care skills, such as pacing (spacing activities throughout the day in a manner that avoids aggravating the pain), and address her anxiety and stress in a more guided manner. We also have a psychologist who specializes in pain for any patient who may need one-on-one counseling. Dr. Edwards: The presence of comorbidities is somewhat useful in making the diagnosis of vulvodynia. I question my diagnosis, in fact, when a patient who has vulvodynia does not have headaches, low energy, depression, anxiety, irritable bowel syndrome, constipation, fibromyalgia, chronic fatigue, sensitivity to medications, TMJ dysfunction, or urinary symptoms. How common is pudendal neuralgia? Dr. Lonky: How prevalent is a finding of pudendal neuralgia? Dr. Edwards: The prevalence and incidence of pudendal neuralgia are not known. Those who specialize in this condition think it is relatively common. I do not identify or suspect it very often. Its definitive diagnosis and management are outside the purview of the general gynecologist, but the general continued on page 58 56
7 TABLE 3 Nantes Criteria for pudendal neuralgia by pudendal nerve entrapment Essential criteria Pain in the territory of the pudendal nerve: from the anus to the penis or clitoris Pain is predominantly experienced while sitting the pain does not wake the patient at night Pain with no objective sensory impairment Pain relieved by diagnostic pudendal nerve block Complementary diagnostic criteria Burning, shooting, stabbing pain; numbness Allodynia or hyperpathia Rectal or vaginal foreign body sensation (sympathalgia) Worsening of pain during the day Predominantly unilateral pain Pain triggered by defecation Presence of exquisite tenderness on palpation of the ischial spine Clinical neurophysiology findings in men or nulliparous women Exclusion criteria Exclusively coccygeal, gluteal, pubic, or hypogastric pain Pruritus Exclusively paroxysmal pain Imaging abnormalities able to account for the pain Associated signs not excluding the diagnosis Buttock pain on sitting Referred sciatic pain Pain referred to the medial aspect of the thigh Suprapubic pain Urinary frequency or pain on a full bladder, or both Pain occurring after ejaculation Dyspareunia or pain after sexual intercourse, or both Erectile dysfunction Normal clinical neurophysiology SOURCE: Labat et al. 21 Reproduced with permission from Neurology and Urodynamics. gynecologist should recognize the symptoms of pudendal neuralgia and refer the patient for evaluation and therapy. Dr. Lonky: What are those symptoms? Dr. Haefner: Pudendal neuralgia often occurs following trauma to the pudendal nerve. The pudendal nerve arises from sacral nerves, generally sacral nerves 2 to 4. Several tests can be utilized to diagnose this condition, including quantitative sensor tests, pudendal nerve motor latency tests, electromyography (EMG), and pudendal nerve blocks. 20 Nantes Criteria allow for making a diagnosis of pudendal neuralgia (Table 3). 21 Initial treatments for pudendal neuralgia should be conservative. Treatments consist of lifestyle changes to prevent flare of disease. Physical therapy, medical management, nerve blocks, and alternative treatments may be beneficial. Pudendal nerve entrapment is often exacerbated by sitting (not on a toilet seat, however) and is reduced in a standing position. It tends to increase in intensity throughout the day. 22 The final treatment for pudendal nerve entrapment is surgery if the nerve is compressed. By this time, the generalist is not generally the provider who performs the surgery. Dr. Gunter: I believe pudendal neuralgia is sometimes overdiagnosed. EMG studies of the pudendal nerve, often touted as a diagnostic tool, are unreliable (they can be abnormal after vaginal delivery or vaginal hysterectomy, for example). In my experience, bilateral pain is less likely to be pudendal neuralgia; spontaneous bilateral compression neuropathy at exactly the same level is not a common phenomenon in chronic pain. I reserve the diagnosis of pudendal neuralgia for women who have allodynia in the distribution of the pudendal nerve with severe pain on sitting, and who have exquisite tenderness when pressure is applied over the pudendal nerve (at the level of the ischial spine on vaginal examination). Typically, the vaginal sidewall on the affected side is very sensitive to light touch. I do see pudendal nerve pain after vaginal surgery when there has been some compromise of the pudendal nerve or the sacral plexus. This is typically unilateral pain. Dr. Lonky: Thank you all. We ll continue our discussion, with a focus on treatment, in the October 2011 issue. References 1. Thomas TG. Practical Treatise on the Diseases of Women. Philadelphia, Pa: Henry C. Lea; Harlow BL, Stewart EG. A population-based assessment of chronic unexplained vulvar pain: have we underestimated the prevalence of vulvodynia? J Am Med Womens Assoc. 2003;58(2): Lavy RJ, Hynan LS, Haley RW. Prevalence of vulvar 58
8 pain in an urban, minority population. J Reprod Med. 2007;52(1): Nyirjesy P, Peyton C, Weitz MV, Mathew L, Culhane JF. Causes of chronic vaginitis: analysis of a prospective database of affected women. Obstet Gynecol. 2006; 108(5): Moyal-Barracco M, Lynch PJ ISSVD terminology and classification of vulvodynia: a historical perspective. J Reprod Med. 2004;49(10): Yunas MB. Fibromyalgia and overlapping disorders: the unifying concept of central sensitivity syndromes. Semin Arthritis Rheum. 2007;36(6): Kahn BS, Tatro C, Parsons CL, Willems JJ. Prevalence of interstitial cystitis in vulvodynia patients detected by bladder potassium sensitivity. J Sex Med. 2010; 7(2 Pt 2): Arnold JD, Bachman GS, Rosen R, Kelly S, Rhoads GG. Vulvodynia: characteristics and associations with comorbidities and quality of life. Obstet Gynecol. 2006;107(3): Parsons CL, Dell J, Stanford EJ, et al. The prevalence of interstitial cystitis in gynecologic patients with pelvic pain, as detected by intravesical potassium sensitivity. Am J Obstet Gynecol. 2002;187(5): Clemens JQ, Meenan RT, O Keefe Rosetti MC, et al. Prevalence of interstitial cystitis symptoms in a managed care population. J Urol. 2005;174(2): Engman M, Lindehammar H, Wijma B. Surface electromyography diagnostics in women with partial vaginismus with or without vulvar vestibulitis and in asymptomatic women. J Psychosom Obstet Gynecol. 2004;25(3 4): Gunter J. Vulvodynia: new thoughts on a devastating condition. Obstet Gynecol Surv. 2007;62(12): Gordon AS, Panahlan-Jand M, McComb F, Melegari C, Sharp S. Characteristics of women with vulvar pain disorders: a Web-based survey. J Sex Marital Ther. 2003;29(suppl 1): Whitten CE, Cristobal K. Chronic pain is a chronic condition not just a symptom. Permanente J. 2005;9(3): Manchikanti L, Fellows B, Pampati V, et al. Comparison of psychological status of chronic pain patients and the general population. Pain Physician. 2002;5(1): Banks SM, Kerns RD. Explaining the high rates of depression in chronic pain: a diathesis-stress framework. Psychological Bulletin. 1996;119(1): Sadownik LA. Clinical correlates of vulvodynia patients. A prospective study of 300 patients. J Reprod Med. 2000;5: Editor found in PubMed: Sadownik LA. Clinical profile of vulvodynia patients. A prospective study of 300 patients. J Reprod Med. 2000;45(8): Could not find the citation listed. Please confirm. 18. Reed BD, Haefner HK, Punch MR, Roth RS, Gorenflo DW, Gillespie BW. Psychosocial and sexual functioning in women with vulvodynia and chronic pelvic pain. A comparative evaluation. J Reprod Med. 2000;45(8): Landry T, Bergeron S. Biopsychosocial factors associated with dyspareunia in a community sample of adolescent girls. Arch Sex Behav. 2011;June Goldstein A, Pukall C, Goldstein I. When Sex Hurts: A Woman s Guide to Banishing Sexual Pain. Cambridge, Mass: Da Capo Lifelong Books; 2011: Labat JJ, Riant T, Robert R, Amarenco G, Lefaucheur JP, Rigaud J. Diagnostic criteria for pudendal neuralgia by pudendal nerve entrapment (Nantes criteria). Neurol Urodyn. 2008;27(4): Popeney C, Answell V, Renney K. Pudendal entrapment as an etiology of chronic perineal pain: Diagnosis and treatment. Neurol Urodyn. 2007;26(6): continued from page 15 evidence-based medicine undermines the very foundation of scientific investigation. More questions than answers The major conclusion of this study is that EFM protects against early neonatal death. So why is there no information about cause of death? These data should be readily available from a linked birth/death certificate data set. Such information might help to determine whether the excess early neonatal deaths were related to EFM or, more likely, to other variables surrounding or related to the delivery, such as the inability to perform an emergency cesarean, if indicated, or the lack of providers skilled in neonatal resuscitation. References 1. Hon EH, Lee ST. Electronic evaluation of the fetal heart rate. VIII. Patterns preceding fetal death, further observations. Am J Obstet Gynecol. 1963;87: American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 106: Intrapartum fetal heart rate monitoring: nomenclature, interpretation, and general management principles. Obstet Gynecol. 2009;114(1): Alfirevic Z, Devane D, Gyte GM. Continuous cardiotocography (CTG) as a form of electronic fetal monitoring (EFM) for fetal assessment during labour. Cochrane Database Syst Rev. 2006;3:CD Devoe LD. Electronic fetal monitoring: Does it really lead to better outcomes? Am J Obstet Gynecol. 2011;204(6):
Title: Vulvodynia: terminology and clinical features. Authors: Miletta, M.; 1 * Bogliatto, F. 1. Type: Original Article
 Title: Vulvodynia: terminology and clinical features. Authors: Miletta, M.; 1 * Bogliatto, F. 1 Type: Original Article Keywords: vulvodynia; issvd; pain; classification; vulva; 1 AZIENDA SANITARIA LOCALE
Title: Vulvodynia: terminology and clinical features. Authors: Miletta, M.; 1 * Bogliatto, F. 1 Type: Original Article Keywords: vulvodynia; issvd; pain; classification; vulva; 1 AZIENDA SANITARIA LOCALE
Vulvodynia and vestibulectomy
 Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
Vulvodynia and vestibulectomy treatment of an important problem for a gynecologist Dr. Tolga Taşçı Associate Proffessor of Obstetrics and Gynecology Gynecologic Oncologist Okmeydanı Teaching and Research
The Geography Of Vulval Pain. Chronic Vulval Pain. Can you tell if its. Nociceptive, Inflammatory or Pathological?
 The Geography Of Vulval Pain Chronic Vulval Pain Can you tell if its Nociceptive, Inflammatory or Pathological? Dr Micheline Byrne, The Jefferiss Wing, St Mary s Hospital Dominant symptoms in vulval patients
The Geography Of Vulval Pain Chronic Vulval Pain Can you tell if its Nociceptive, Inflammatory or Pathological? Dr Micheline Byrne, The Jefferiss Wing, St Mary s Hospital Dominant symptoms in vulval patients
Vulvovaginal Disease Update 2017 Co-Sponsored by:
 Vulvovaginal Disease Update 2017 Co-Sponsored by: The North American Chapter Of The International Society For The Study Of Vulvovaginal Disease & The Vulvovaginal Health Clinic Baylor College of Medicine
Vulvovaginal Disease Update 2017 Co-Sponsored by: The North American Chapter Of The International Society For The Study Of Vulvovaginal Disease & The Vulvovaginal Health Clinic Baylor College of Medicine
Persistent Genital Arousal Disorder (PGAD) in Women: Mental or Body
 Persistent Genital Arousal Disorder (PGAD) in Women: Mental or Body Irwin Goldstein MD Director, Sexual Medicine, Alvarado Hospital, San Diego, California Clinical Professor of Surgery, University of California,
Persistent Genital Arousal Disorder (PGAD) in Women: Mental or Body Irwin Goldstein MD Director, Sexual Medicine, Alvarado Hospital, San Diego, California Clinical Professor of Surgery, University of California,
Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary vulvar clinic Vestibulectomy
 From Pain to Pleasure Surgical Treatment of Vestibulodynia Päivi Tommola Specialist in Gynecology 13.10.2010 GKS Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary
From Pain to Pleasure Surgical Treatment of Vestibulodynia Päivi Tommola Specialist in Gynecology 13.10.2010 GKS Vestibulodynia Terminology Clinical features of the disease Ethiopatogenesis Treatment Multidisciplinary
Pathogenesis of Chronic Pelvic Pain
 Pathogenesis of Chronic Pelvic Pain Yong-Chul Kim Department of anesthesia and pain medicine, Seoul National University College of Medicine 1 Overview Anatomy Nerve innervation CPP by pathology CPP by
Pathogenesis of Chronic Pelvic Pain Yong-Chul Kim Department of anesthesia and pain medicine, Seoul National University College of Medicine 1 Overview Anatomy Nerve innervation CPP by pathology CPP by
Vulvodynia What a Health Practitioner Should Know
 Vulvodynia What a Health Practitioner Should Know Catherine M. Leclair, MD Associate Professor Director, Program in Vulvar Health Objective: To present a clinically based approach to vulvodynia Identify
Vulvodynia What a Health Practitioner Should Know Catherine M. Leclair, MD Associate Professor Director, Program in Vulvar Health Objective: To present a clinically based approach to vulvodynia Identify
Vulvodynia What s Behind the Name?
 Vulvodynia What s Behind the Name? Vulvodynia is a diagnostic term referring to chronic pain in the vulvar area of at least 3 months duration. Vulvodynia includes and encompasses a number of heterogeneous
Vulvodynia What s Behind the Name? Vulvodynia is a diagnostic term referring to chronic pain in the vulvar area of at least 3 months duration. Vulvodynia includes and encompasses a number of heterogeneous
VULVODYNIA: OVERVIEW AND ASSESSMENT OF PAIN OUTCOMES and IMPLICATIONS FOR INCLUSION CRITERIA
 VULVODYNIA: OVERVIEW AND ASSESSMENT OF PAIN OUTCOMES and IMPLICATIONS FOR INCLUSION CRITERIA ANDREA RAPKIN M.D. PROFESSSOR OF OBSTETRICS AND GYNECOLOGY Vulvodynia Most recent nomenclature was developed
VULVODYNIA: OVERVIEW AND ASSESSMENT OF PAIN OUTCOMES and IMPLICATIONS FOR INCLUSION CRITERIA ANDREA RAPKIN M.D. PROFESSSOR OF OBSTETRICS AND GYNECOLOGY Vulvodynia Most recent nomenclature was developed
How does interstitial cystitis begin?
 Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Original Article How does interstitial cystitis begin? C. Lowell Parsons Division of Urology, Department of Surgery, University of California, San Diego Medical Center, University of California, San Diego,
Disorders of the vulva
 Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Vulval lesions Disorders of the vulva Terminology standardised by the International Society for the Study of Vulvovaginal Disease(ISSVD) Classification 1.Nonneoplastic epithelial disorders of vulva Lichen
Vaginitis. Is vaginal discharge ever normal? Women with vaginal discharge. Vaginal symptoms are very common. Patient with chronic vaginal discharge
 Vaginitis Is the wet prep out of the building? No disclosures related to this topic Images are cited with permissions Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Health
Vaginitis Is the wet prep out of the building? No disclosures related to this topic Images are cited with permissions Barbara S. Apgar, MD, MS Professor of Family Medicine University of Michigan Health
Patients presenting with chronic vulvovaginal. Vulvovaginal pain and dyspareunia. Part 1: An often challenging presentation
 MedicineToday 2014; 15(7): 41-46 PEER REVIEWED FEATURE 2 CPD POINTS Vulvovaginal pain and dyspareunia Key points Patients with vulvovaginal pain, particularly when it is chronic, are often distressed and
MedicineToday 2014; 15(7): 41-46 PEER REVIEWED FEATURE 2 CPD POINTS Vulvovaginal pain and dyspareunia Key points Patients with vulvovaginal pain, particularly when it is chronic, are often distressed and
Vestibulectomy. Hope K. Haefner, MD Michigan Medicine Ann Arbor, MI USA
 Vestibulectomy Hope K. Haefner, MD Michigan Medicine Ann Arbor, MI USA Learning Objectives At the end of this lecture, the participant will: Understand the surgical techniques used to treat localized vulvodynia
Vestibulectomy Hope K. Haefner, MD Michigan Medicine Ann Arbor, MI USA Learning Objectives At the end of this lecture, the participant will: Understand the surgical techniques used to treat localized vulvodynia
Vulvar Disease Clinical Cases
 Vulvar Disease Clinical Cases Hope K. Haefner, MD Professor University of Michigan Health System February 27, 2015 Cartagena Conflicts of Interest Hope Haefner, MD is on the Advisory Board of Merck Co.,
Vulvar Disease Clinical Cases Hope K. Haefner, MD Professor University of Michigan Health System February 27, 2015 Cartagena Conflicts of Interest Hope Haefner, MD is on the Advisory Board of Merck Co.,
PITA Pain In The A** And Other Pains You May Not Have Heard Of. Allan S. Gordon MD Neurologist and Director Wasser PMC/ MSH
 PITA Pain In The A** And Other Pains You May Not Have Heard Of Allan S. Gordon MD Neurologist and Director Wasser PMC/ MSH Wasser Pain Management Centre Clinical care, education and research in chronic
PITA Pain In The A** And Other Pains You May Not Have Heard Of Allan S. Gordon MD Neurologist and Director Wasser PMC/ MSH Wasser Pain Management Centre Clinical care, education and research in chronic
Burdensome Vaginal Infections: Best Diagnostic Practices for Driving Better Patient Outcomes
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Postpartum Complications
 ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
ACOG Postpartum Toolkit Postpartum Complications Introduction The effects of pregnancy on many organ systems begin to resolve spontaneously after birth of the infant and delivery of the placenta. The timeline
Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions
 Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD Professor University of Michigan Health System Ann Arbor, Michigan February, 2017 Industry Support and Financial
Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD Professor University of Michigan Health System Ann Arbor, Michigan February, 2017 Industry Support and Financial
Firefighting: Burning Mouth Syndrome and Burning Vulva (vulvodynia)
 Firefighting: Burning Mouth Syndrome and Burning Vulva (vulvodynia) Rochelle Torgerson, MD, PhD Chair of Education Department of Dermatology Mayo Clinic, Rochester, MN DISCLOSURE OF RELEVANT RELATIONSHIPS
Firefighting: Burning Mouth Syndrome and Burning Vulva (vulvodynia) Rochelle Torgerson, MD, PhD Chair of Education Department of Dermatology Mayo Clinic, Rochester, MN DISCLOSURE OF RELEVANT RELATIONSHIPS
Assistance and Recommendations for GP s: Managing Chronic Vulval Pain
 Assistance and Recommendations for GP s: Managing Chronic Vulval Pain 06.06.18 Chronic pain is a complex disease affecting one in five adult Europeans. The relationship between chronic pain, well-being
Assistance and Recommendations for GP s: Managing Chronic Vulval Pain 06.06.18 Chronic pain is a complex disease affecting one in five adult Europeans. The relationship between chronic pain, well-being
VIN/VAIN O C T O B E R 3 RD J M O R G A N
 VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
VIN/VAIN O C T O B E R 3 RD 2 0 1 8 J M O R G A N Vaginal Intraepithelial Neoplasia VAIN I, II, III Incidence 0.1/100,000 women in US Mean age 50s (J Womens Health (Larchmt) 2009:18:1731) (J Obstet Gynaecol
5/29/2015. Objectives. Functions of the PFM. Various phases of PFM. Evaluation of the PFM
 The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
The Physical Therapist s Approach to the Female Pelvic Floor Musculature Examination and Treatment. Presented By: Evelyne Burtis, DPT Objectives Core and pelvic floor muscles (PFM) Functions of the PFM
WHITE PAPER SmartXide 2 V 2 LR. MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy
 WHITE PAPER SmartXide 2 V 2 LR MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy DEKA White Paper SMARTXIDE 2 V 2 LR November 2015 MonaLisa Touch Dual Probe Therapy
WHITE PAPER SmartXide 2 V 2 LR MonaLisa Touch Dual Probe Therapy for the Treatment of Lichen Sclerosus and Vaginal Atrophy DEKA White Paper SMARTXIDE 2 V 2 LR November 2015 MonaLisa Touch Dual Probe Therapy
Diseases of the vulva
 Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Diseases of the vulva 1. Bartholin Cyst - Infection of the Bartholin gland produces an acute inflammation within the gland (adenitis) and may result in an abscess. Bartholin duct cysts - Are relatively
Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation
 Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation Ashley Christensen, BSN, 1 Michael Haugsdal, MD, 2 and Noelle Bowdler, MD 2 Keywords: Vulvovaginal irritation,
Importance of the physical exam and in-office tests in the evaluation of vulvovaginal irritation Ashley Christensen, BSN, 1 Michael Haugsdal, MD, 2 and Noelle Bowdler, MD 2 Keywords: Vulvovaginal irritation,
** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! **
 ** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! ** WHY AM I FILLING OUT THIS FORM? Your responses will help us to understand your experience. Please take your time and try to answer
** IMPORTANT!! PLEASE READ THIS BEFORE YOU FILL OUT YOUR QUESTIONNAIRE! ** WHY AM I FILLING OUT THIS FORM? Your responses will help us to understand your experience. Please take your time and try to answer
Sexological aspects of genital pain
 Sexological aspects of genital pain Annamaria Giraldi, professor, MD, PHD Sexological Clinic, Psychiatric Centre Copenhagen 1 Disclosures Speaker: Eli Lilly, Pfizer Consultant: Eli Lilly,Palatin 2 Agenda
Sexological aspects of genital pain Annamaria Giraldi, professor, MD, PHD Sexological Clinic, Psychiatric Centre Copenhagen 1 Disclosures Speaker: Eli Lilly, Pfizer Consultant: Eli Lilly,Palatin 2 Agenda
INTERSTITIAL CYSTITIS (IC) MANAGEMENT
 INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
INTERSTITIAL CYSTITIS (IC) MANAGEMENT About Interstitial Cystitis (IC) What is IC? IC is a chronic, yet manageable, bladder condition, characterized by bladder or pelvic pain, pain during or after sexual
Case 1. Case Studies in Vulvovaginal Disease. Disclosures. What is your diagnosis? Case 1. Lichen sclerosus 10/19/2018
 Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
Case 1 Case Studies in Vulvovaginal Disease Leah Moynihan, RNC, MSN Women & Infants Hospital of Rhode Island Division of Urogynecology & Reconstructive Pelvic Surgery Disclosures I have no relevant financial
In evaluating a patient with lower urinary tract symptoms (LUTS), urologists
 CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
CLINICAL MANAGEMENT OF INTERSTITIAL CYSTITIS Interstitial Cystitis and Lower Urinary Tract Symptoms in Males and Females The Combined Role of Potassium and Epithelial Dysfunction C. Lowell Parsons, MD
Vulvar Diseases What Do You Know?
 Vulvar Diseases What Do You Know? Hope K. Haefner, MD Michigan Medicine Ann Arbor, MI ACOG 2018 Course Objectives At the end of this course, the participant should be able to: Identify the clinical features
Vulvar Diseases What Do You Know? Hope K. Haefner, MD Michigan Medicine Ann Arbor, MI ACOG 2018 Course Objectives At the end of this course, the participant should be able to: Identify the clinical features
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE?
 PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
PELVIC HEALTH PHYSICAL THERAPY AND THE NURSE PRACTITIONER: WHAT S GOING ON DOWN THERE? Kathy Curry, PT, DPT Physical Therapy Today Pelvic Health Physical Therapy () Objectives: Discuss components of pelvic
32 OBG Management July 2010 Vol. 22 No. 7 obgmanagement.com
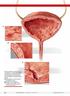 A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
A B C Although interstitial cystitis (IC) occurs in the absence of urinary tract infection or malignancy, some pathology may become apparent during cystoscopy with hydrodistention. Potential findings include:
Vulvar and Vaginal Disorders Questionnaire
 1 Your Name: Vulvar and Vaginal Disorders Questionnaire Referring provider: To whom should we send a report about this visit: My physician: Don t send anyone a report Address/Phone: Ethnicity (circle):
1 Your Name: Vulvar and Vaginal Disorders Questionnaire Referring provider: To whom should we send a report about this visit: My physician: Don t send anyone a report Address/Phone: Ethnicity (circle):
Neuromuscular pain Clinical Assessment and Therapeutic Management. Dr Jean-Jacques LABAT Dr Jérôme RIGAUD
 Neuromuscular pain Clinical Assessment and Therapeutic Management Dr Jean-Jacques LABAT Dr Jérôme RIGAUD Chronic Post-operative operative pelvi-perineal Pain Eliminate Infection Haematoma Mesh erosion
Neuromuscular pain Clinical Assessment and Therapeutic Management Dr Jean-Jacques LABAT Dr Jérôme RIGAUD Chronic Post-operative operative pelvi-perineal Pain Eliminate Infection Haematoma Mesh erosion
Aldo Campana Training Course in Reproductive Health/ Sexual Health Research Geneva 2006
 Female dyspareunia Aldo Campana Training Course in Reproductive Health/ Sexual Health Research Geneva 2006 Female dyspareunia Terms and definitions Prevalence Etiology Evaluation and differential diagnosis
Female dyspareunia Aldo Campana Training Course in Reproductive Health/ Sexual Health Research Geneva 2006 Female dyspareunia Terms and definitions Prevalence Etiology Evaluation and differential diagnosis
4/3/2017 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS BACTERIAL VAGINOSIS EPIDEMIOLOGY OBJECTIVES
 DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
DIAGNOSIS AND THERAPY OF RECURRENT VULVOVAGINAL SYMPTOMS KELLY HODGES, MD (NO DISCLOSURES) OBJECTIVES REVIEW THE TWO MOST COMMON CAUSES OF RECURRENT ABNORMAL DISCHARGE (CANDIDA AND BV) REVIEW THE MOST
Role of Physiotherapy in the Management of Persistent Pelvic Pain. Brigitte Fung Physiotherapist Kwong Wah Hospital
 Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Role of Physiotherapy in the Management of Persistent Pelvic Pain Brigitte Fung Physiotherapist Kwong Wah Hospital What is PPP? Chronic Pelvic Pain Pelvic Pain Pelvic Floor/ Pelvic Pain Syndrome Pelvic
Dear Patient, Sincerely, The Pelvic Health and Rehabilitation Center
 Dear Patient, Welcome to the Pelvic Health and Rehabilitation Center! We specialize in physical therapy management of numerous pelvic pain disorders. We believe in a multidisciplinary collaborative approach
Dear Patient, Welcome to the Pelvic Health and Rehabilitation Center! We specialize in physical therapy management of numerous pelvic pain disorders. We believe in a multidisciplinary collaborative approach
Results of a Sequential Treatment Plan
 Infectious Diseases in Obstetrics and Gynecology 3:193-197 (1995) (C) 1996 Wiley-Liss, Inc. Medical Management of Vulvar Vestibulitis: Results of a Sequential Treatment Plan Paul Nyirjesy and Meredith
Infectious Diseases in Obstetrics and Gynecology 3:193-197 (1995) (C) 1996 Wiley-Liss, Inc. Medical Management of Vulvar Vestibulitis: Results of a Sequential Treatment Plan Paul Nyirjesy and Meredith
OBSTETRICS & GYNECOLOGY
 JANUARY 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Female Sexual Arousal
JANUARY 2012 COMPOUNDING PHARMACY SOLUTIONS PRESCRIPTION COMPOUNDING WWW.CPSRXS. COM We customize individual prescriptions for the specific needs of our patients. INSIDE THIS ISSUE: Female Sexual Arousal
BLADDER HEALTH. Painful Bladder AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION
 BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
BLADDER HEALTH Painful Bladder Interstitial Cystitis AUA FOUNDATION OFFICIAL FOUNDATION OF THE AMERICAN UROLOGICAL ASSOCIATION Don t Let Interstitial Cystitis Keep You from Enjoying Life. many people have
Chronic Pelvic Pain Case Study
 Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
Case Study Chronic Pelvic Pain Case Study Melissa, a 28 year old veteran comes to your office complaining of lower abdominal pain for the past 6 months. She has tried acetaminophen and ibuprofen but they
SEXUAL PAIN Home messages, a summary from Presentations, moderated Posters and Podiums
 SEXUAL PAIN Home messages, a summary from Presentations, moderated Posters and Podiums María Luisa Banfi, MD Gynecologist, Sexologist Montevideo, Uruguay, South America CHICAGO 2012,SMS- ISSM, World Meeting
SEXUAL PAIN Home messages, a summary from Presentations, moderated Posters and Podiums María Luisa Banfi, MD Gynecologist, Sexologist Montevideo, Uruguay, South America CHICAGO 2012,SMS- ISSM, World Meeting
Case L.M. Question 1 4/17/2013. Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin
 Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
Sumana Koduri, MD Associate Professor, Ob/gyn and Urology Medical College of Wisconsin Case L.M. L.M. is a 46 yo G0 woman who presents with a 3 year history of worsening pelvic pain. She has a h/o endometriosis
Vulvodynia. Information for patients Gynaecology
 Vulvodynia Information for patients Gynaecology page 2 of 8 What is vulvodynia? Vulvodynia is a chronic (long term) condition of vulval pain. It is the term used to describe women who experience the sensation
Vulvodynia Information for patients Gynaecology page 2 of 8 What is vulvodynia? Vulvodynia is a chronic (long term) condition of vulval pain. It is the term used to describe women who experience the sensation
Kelly H. Tyler, MD, FACOG, FAAD S052 Gender Dermatology: Diagnosis and Treatment of Genital Skin Disorders Vulvar Dermatitis
 Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
Vulvar Dermatitis Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics and Gynecology Center for
A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia
 Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
Pain Ther (2012) 1:2 DOI 10.1007/s40122-012-0002-7 ORIGINAL RESEARCH A Population-Based Study of Pregnancy and Delivery Characteristics Among Women with Vulvodynia Ruby H. N. Nguyen Elizabeth G. Stewart
Dr. Maliheh Keshvari
 1 Dr. Maliheh Keshvari Assistant professor of Urology Fellowship in Female Urology Mashhad University of Medical Sciences 2 Female Sexual Function and Dysfunction 3 It was not until recently that urologists
1 Dr. Maliheh Keshvari Assistant professor of Urology Fellowship in Female Urology Mashhad University of Medical Sciences 2 Female Sexual Function and Dysfunction 3 It was not until recently that urologists
Conflicts of interest
 Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Vulvar Cases 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology)
Dora Street, Hurstville 160 Belmore Road, Randwick
 www.orthosports.com.au 29 31 Dora Street, Hurstville 160 Belmore Road, Randwick Pudendal Nerve Entrapment Andreas Loefler Hip, Knee, and Spine Surgeon PNE Pudendal Neuralgia Alcock s Syndrome Cyclists
www.orthosports.com.au 29 31 Dora Street, Hurstville 160 Belmore Road, Randwick Pudendal Nerve Entrapment Andreas Loefler Hip, Knee, and Spine Surgeon PNE Pudendal Neuralgia Alcock s Syndrome Cyclists
Chronic pelvic pain. S Afr Fam Pract REVIEW. Abstract. Introduction. P Zinn. Corresponding author: Philip Zinn, e-mai:
 South African Family Practice 2015; 57(4):4-9 Open Access article distributed under the terms of the Creative Commons License [CC BY-NC-ND 4.0] http://creativecommons.org/licenses/by-nc-nd/4.0 S Afr Fam
South African Family Practice 2015; 57(4):4-9 Open Access article distributed under the terms of the Creative Commons License [CC BY-NC-ND 4.0] http://creativecommons.org/licenses/by-nc-nd/4.0 S Afr Fam
Provenance Rehabilitation Pelvic Intake Form
 Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Patient Name: Age: Weight: Gender: Male Female Provenance Rehabilitation Pelvic Intake Form Date: DOB: Occupation: Relationship Status: Hobbies / Leisure Activities: Exercise Routine: Briefly describe
Bacterial Vaginosis & VVC: How Can We Improve Current Diagnosis Methods?
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/womens-health-update/bacterial-vaginosis-vvc-how-can-we-improvecurrent-diagnosis-methods/10413/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/womens-health-update/bacterial-vaginosis-vvc-how-can-we-improvecurrent-diagnosis-methods/10413/
Office of Research on Women s Health National Institutes of Health u.s.department of health & human services Publication No.
 Office of Research on Women s Health National Institutes of Health u.s.department of health & human services Publication No. 07-6293 Resources on Vulvodynia National Institutes of Health (NIH), U.S. Department
Office of Research on Women s Health National Institutes of Health u.s.department of health & human services Publication No. 07-6293 Resources on Vulvodynia National Institutes of Health (NIH), U.S. Department
Vulvodynia / Pain. NVA RESEARCH UPDATE NEWSLETTER September 2005
 NVA RESEARCH UPDATE NEWSLETTER September 2005 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
NVA RESEARCH UPDATE NEWSLETTER September 2005 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
Asymptomatic Undiagnosed Lichen Sclerosus
 Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
Asymptomatic Undiagnosed Lichen Sclerosus Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology and Surgery(Dermatology) Geisel School of Medicine at Dartmouth Lebanon, NH, USA Disclosures
Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California.
 Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California? Disclosures Hope K. Haefner, MD is on the advisory board of Merck Co. Inc. Lynette
Vulvar Diseases: What Do You Know? Hope K. Haefner, MD Lynette J. Margesson, MD ACOG May 5, 2015 San Francisco, California? Disclosures Hope K. Haefner, MD is on the advisory board of Merck Co. Inc. Lynette
Dr Hannah Blakely. Dr Ben Sharp. Ms Julee Binns. Sara Widdowson. 7:15-8:15 Breakfast Session: Oxford Women's Health
 Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
Dr Hannah Blakely Clinical Psychologist Oxford Women's Health Ms Julee Binns Consultant Physiotherapist Oxford Women's Health, Christchurch Sara Widdowson NZ Registered Dietitian Christchurch Public Hospital
The use of CO2 laser for patients with Lichen sclerosus
 The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
The use of CO2 laser for patients with Lichen sclerosus Dr. Christina Kuhler-Obbarius, Elisabeth Kunkel, Dr. Matthias Theden-Schow, Hamburg, Germany Our clinical center located in Hamburg includes eight
Innovations in the Management of Dyspareunia
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Perceived Stereotyping and Seeking Care for Chronic Vulvar Pain
 bs_bs_banner Pain Medicine 2013; 14: 1461 1467 Wiley Periodicals, Inc. Perceived Stereotyping and Seeking Care for Chronic Vulvar Pain Ruby H. N. Nguyen, PhD, Rachael M. Turner, BS, Sarah A. Rydell, MPH,
bs_bs_banner Pain Medicine 2013; 14: 1461 1467 Wiley Periodicals, Inc. Perceived Stereotyping and Seeking Care for Chronic Vulvar Pain Ruby H. N. Nguyen, PhD, Rachael M. Turner, BS, Sarah A. Rydell, MPH,
Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow.
 Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow Objectives& 1) Overview of female sexual dysfunction 2) Explore the relationship
Female&sexual& dysfunction&and& Interstitial&cystitis& Urology Grand Rounds November 14, 2012 Momoe Hyakutake, Urogynecology Fellow Objectives& 1) Overview of female sexual dysfunction 2) Explore the relationship
Evaluation of gabapentin in the treatment of generalized vulvodynia, unprovoked. Harris G, Horowitz B, Borgida A J Reprod Med Feb;52(2):103-6
 NVA RESEARCH UPDATE NEWSLETTER June 2007 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
NVA RESEARCH UPDATE NEWSLETTER June 2007 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
Cases of Non-Infectious Vulvovaginitis
 Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
Cases of Non-Infectious Vulvovaginitis 2 nd PANHELLANIC CONGRESS on Lower Genital Tract Disorders December 14-16 Grand Hyatt Athens Lynette J. Margesson MD FRCPC Assistant Professor of Obstetrics & Gynecology
Meet the ISSVD. President ISSVD. Jacob Bornstein, MD
 Meet the ISSVD Jacob Bornstein, MD President ISSVD Chairman, Department of Obstetrics and Gynecology Western Galilee Hospital Bar-Ilan University Faculty of Medicine Nahariya, Israel ISSVD Symposium: The
Meet the ISSVD Jacob Bornstein, MD President ISSVD Chairman, Department of Obstetrics and Gynecology Western Galilee Hospital Bar-Ilan University Faculty of Medicine Nahariya, Israel ISSVD Symposium: The
A population-based assessment of chronic unexplained vulvar pain: have we underestimated the prevalence of vulvodynia?
 NVA RESEARCH UPDATE NEWSLETTER Volume III, Issue II June 2003 www.nva.org This newsletter has been supported, in part, through an unrestricted educational grant from Personal Products Company, a division
NVA RESEARCH UPDATE NEWSLETTER Volume III, Issue II June 2003 www.nva.org This newsletter has been supported, in part, through an unrestricted educational grant from Personal Products Company, a division
MYTHS OF STIs True or False
 MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
Topics in Women s Health. Ann Laros, MD University of Iowa
 Topics in Women s Health Ann Laros, MD University of Iowa Topics in Women s Health 1. Cervical cancer screening guidelines 2. ACHA Pap and STI data 3. Vulvar pearls 4. Genital HSV 2012 Cervical Cancer
Topics in Women s Health Ann Laros, MD University of Iowa Topics in Women s Health 1. Cervical cancer screening guidelines 2. ACHA Pap and STI data 3. Vulvar pearls 4. Genital HSV 2012 Cervical Cancer
CHRONIC PELVIC PAIN AS WE UNDERSTAND IT TODAY. Dr. Sonia Wartan Consultant in Pain Medicine
 CHRONIC PELVIC PAIN AS WE UNDERSTAND IT TODAY Dr. Sonia Wartan Consultant in Pain Medicine Clinical Lead of Chronic Pain Services Chronic Pelvic MDT Clinic Royal Gwent Hospital Acute Pain Specific disease/injury
CHRONIC PELVIC PAIN AS WE UNDERSTAND IT TODAY Dr. Sonia Wartan Consultant in Pain Medicine Clinical Lead of Chronic Pain Services Chronic Pelvic MDT Clinic Royal Gwent Hospital Acute Pain Specific disease/injury
WOMENCARE. Herpes. Source: PDR.net Page 1 of 8. A Healthy Woman is a Powerful Woman (407)
 WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
Complex Vaginitis Cases: Applying New Diagnostic Methods to Enhance Patient Outcomes ReachMD Page 1 of 5
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Sexually Transmitted Diseases: Overview
 Sexually Transmitted Diseases: Overview Q: What is a sexually transmitted disease (STD)? A: It is an infection or disease passed from person to person through sexual contact. Q: How many people have STDs?
Sexually Transmitted Diseases: Overview Q: What is a sexually transmitted disease (STD)? A: It is an infection or disease passed from person to person through sexual contact. Q: How many people have STDs?
Gynecological Cancers
 Gynecological Cancers Outline Ovarian Cancer Uterine (Endometrial) Cancer Cervical Cancer Vulvar Cancer Vaginal Cancer Overian Cancer Ovarian cancer is cancer that forms in the tissue of the ovary and
Gynecological Cancers Outline Ovarian Cancer Uterine (Endometrial) Cancer Cervical Cancer Vulvar Cancer Vaginal Cancer Overian Cancer Ovarian cancer is cancer that forms in the tissue of the ovary and
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES GYNECOLOGIC CANCER VULVAR Last Revision Date July 2015 1 Site Group: Gynecologic Cancer Vulvar Author: Dr. Stephane Laframboise 1. INTRODUCTION
Vulvodynia / Pain. NVA RESEARCH UPDATE NEWSLETTER December 2004
 NVA RESEARCH UPDATE NEWSLETTER December 2004 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
NVA RESEARCH UPDATE NEWSLETTER December 2004 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
PAINFUL URINATION CAUSES & NATURAL REMEDY. Dr. Bestman Anyatonwu
 LIBRACIN NATURAL MEDICINE IND. LTD PAINFUL URINATION CAUSES & NATURAL REMEDY Dr. Bestman Anyatonwu MEANING Painful urination is a broad term that describes discomfort during urination. This pain may originate
LIBRACIN NATURAL MEDICINE IND. LTD PAINFUL URINATION CAUSES & NATURAL REMEDY Dr. Bestman Anyatonwu MEANING Painful urination is a broad term that describes discomfort during urination. This pain may originate
Core outcome sets for Clinical trials and Observational Studies in Vulvovaginal Disease
 P a g e 1 JLGTD Editorial Core outcome sets for Clinical trials and Observational Studies in Vulvovaginal Disease I. Define the issue general concepts Clinical trials and observational studies in medical
P a g e 1 JLGTD Editorial Core outcome sets for Clinical trials and Observational Studies in Vulvovaginal Disease I. Define the issue general concepts Clinical trials and observational studies in medical
Sexually Transmitted Diseases: Overview
 Sexually Transmitted Diseases: Overview frequent and more serious complications from STDs than men. Q: How do you get an STD? A: You can get and pass STDs through Q: What is a sexually transmitted vaginal,
Sexually Transmitted Diseases: Overview frequent and more serious complications from STDs than men. Q: How do you get an STD? A: You can get and pass STDs through Q: What is a sexually transmitted vaginal,
Differentiation between women with vulvovaginal symptoms who are positive or negative for Candida species by culture
 Infect Dis Obstet Gynecol 2001;9:221 225 Differentiation between women with vulvovaginal symptoms who are positive or negative for species by culture Iara M. Linhares 1,2, Steven S. Witkin 2, Shirlei D.
Infect Dis Obstet Gynecol 2001;9:221 225 Differentiation between women with vulvovaginal symptoms who are positive or negative for species by culture Iara M. Linhares 1,2, Steven S. Witkin 2, Shirlei D.
Provoked vestibulodynia: A qualitative exploration of women s experiences
 Leslie A. Sadownik, MD, MEd, FRCSC, Brooke Nicole Seal, PhD, Lori A. Brotto, PhD, R Psych Provoked vestibulodynia: A qualitative exploration of women s experiences A unique program allows women with vulvovaginal
Leslie A. Sadownik, MD, MEd, FRCSC, Brooke Nicole Seal, PhD, Lori A. Brotto, PhD, R Psych Provoked vestibulodynia: A qualitative exploration of women s experiences A unique program allows women with vulvovaginal
Sexually Transmitted. Diseases
 Sexually Transmitted Diseases How can I get an STD? Many STDs are carried and transmitted through semen and vaginal fluids. Some STDs can be spread through skin to skin contact Mother to child STDs: Signs
Sexually Transmitted Diseases How can I get an STD? Many STDs are carried and transmitted through semen and vaginal fluids. Some STDs can be spread through skin to skin contact Mother to child STDs: Signs
Clinically Microscopically Pathogenesis: autoimmune not lifetime
 Vulvar Diseases: Can be divided to non-neoplastic and neoplastic diseases. The neoplastic diseases are much less common. Of those, squamous cell carcinoma is the most common. most common in postmenopausal
Vulvar Diseases: Can be divided to non-neoplastic and neoplastic diseases. The neoplastic diseases are much less common. Of those, squamous cell carcinoma is the most common. most common in postmenopausal
Vulvar Diseases What Do You Know? AKA Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions
 Vulvar Diseases What Do You Know? AKA Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD San Diego, California Disclosures/Conflicts of Interest Hope K. Haefner,
Vulvar Diseases What Do You Know? AKA Your Diagnosis Is? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD San Diego, California Disclosures/Conflicts of Interest Hope K. Haefner,
Vulvar Diseases What Do You Know? Test Your Knowledge of Various Vulvovaginal Conditions. Hope K. Haefner, MD San Diego, California ACOG 2017
 Vulvar Diseases What Do You Know? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD San Diego, California ACOG 2017 Disclosures/Conflicts of Interest Hope K. Haefner, MD was previously
Vulvar Diseases What Do You Know? Test Your Knowledge of Various Vulvovaginal Conditions Hope K. Haefner, MD San Diego, California ACOG 2017 Disclosures/Conflicts of Interest Hope K. Haefner, MD was previously
The Case of Mrs. Virginia Jones* Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver, Canada
 Case title: Case authors: Case synopsis: The Case of Mrs. Virginia Jones* Dr. Leslie A. Sadownik Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver,
Case title: Case authors: Case synopsis: The Case of Mrs. Virginia Jones* Dr. Leslie A. Sadownik Asst. Professor Division of Gyne-Oncology University of British Columbia, Department of Gynecology Vancouver,
Neuromodulation and the pudendal nerve
 Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Neuromodulation and the pudendal nerve Stefan De Wachter, MD, PhD, FEBU Professor of Urology University of Antwerpen, Belgium Chairman dept of Urology, UZA Disclosures Consultant speaker: Astellas, Medtronic,
Vulvodynia / Pain. NVA RESEARCH UPDATE NEWSLETTER June 2004
 NVA RESEARCH UPDATE NEWSLETTER June 2004 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
NVA RESEARCH UPDATE NEWSLETTER June 2004 www.nva.org This newsletter has been supported, in part, through a grant from the Enterprise Rent-A-Car Foundation. www.enterprise.com This newsletter is quarterly
An All Too Familiar Story
 All that itches is not yeast Michele Ambor Hutz NP An All Too Familiar Story A patient presents to her provider complaining of frequent yeast infections. The provider prescribes treatment without an exam
All that itches is not yeast Michele Ambor Hutz NP An All Too Familiar Story A patient presents to her provider complaining of frequent yeast infections. The provider prescribes treatment without an exam
What are the symptoms of a vulval skin condition?
 Information for you Published in December 2013 Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting the vulva. If you are
Information for you Published in December 2013 Skin conditions of the vulva About this information This information is for you if you want to know about skin conditions affecting the vulva. If you are
Sexually Transmitted Infections. Kim Dawson October 2010
 Sexually Transmitted Infections Kim Dawson October 2010 Objectives: You will learn about: Sexually Transmitted Infections (STI s). How they are transferred. High risk behavior. The most common STI s. How
Sexually Transmitted Infections Kim Dawson October 2010 Objectives: You will learn about: Sexually Transmitted Infections (STI s). How they are transferred. High risk behavior. The most common STI s. How
Other physician #1. #(p) List any allergies to medications. Please list below all other current medical conditions or previous surgeries
 Dept. of Obstetrics and Gynecology Division of Gynecological Pain and Minimally Invasive Surgery Frank Tu, MD, MPH Sangeeta Senapati, MD, MS Howard Topel, MD Name: New Patient Intake Questionnaire Names
Dept. of Obstetrics and Gynecology Division of Gynecological Pain and Minimally Invasive Surgery Frank Tu, MD, MPH Sangeeta Senapati, MD, MS Howard Topel, MD Name: New Patient Intake Questionnaire Names
Interstitial Cystitis
 Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Interstitial Cystitis Interstitial cystitis (IC) is a chronic bladder condition. Its symptoms are urinary urgency (the feeling that you need to urinate), frequent urination and/or pain anywhere between
Diagnosis and Management of Vulvar Disorders
 Diagnosis and Management of Vulvar Disorders Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics
Diagnosis and Management of Vulvar Disorders Kelly H. Tyler, MD, FACOG, FAAD Assistant Professor The Ohio State University Department of Internal Medicine, Division of Dermatology Department of Obstetrics
Disease (diabetic neuropathy, multiple sclerosis, tumors, and, rarely, tertiary syphilis)
 COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Adult Men with Sexual Performance Problems Individual Planning: A Treatment Plan Overview for Adult Men with Sexual
COURSES ARTICLE - THERAPYTOOLS.US Individual Planning: A Treatment Plan Overview for Adult Men with Sexual Performance Problems Individual Planning: A Treatment Plan Overview for Adult Men with Sexual
I dentifying the cause of a patient s dyspareunia
 OBG MANAGEMENT BY ELIZABETH G. STEWART, MD Dyspareunia: 5 overlooked causes Disorders ranging from a simple anatomic problem to a complex psychosocial/ biologic phenomenon can cause difficult or painful
OBG MANAGEMENT BY ELIZABETH G. STEWART, MD Dyspareunia: 5 overlooked causes Disorders ranging from a simple anatomic problem to a complex psychosocial/ biologic phenomenon can cause difficult or painful
WELCOME. Training village
 WELCOME Training village PERFORM EASY AND PAINLESS VAGINAL DRYNESS TREATMENT WITH ELEA Dr Bertrand Durantet Aesthetic Doctor LYON France PART 1 FEATURES ON ELEA THE MAGNETIC SUPPORT THE FOOT PEDAL THE
WELCOME Training village PERFORM EASY AND PAINLESS VAGINAL DRYNESS TREATMENT WITH ELEA Dr Bertrand Durantet Aesthetic Doctor LYON France PART 1 FEATURES ON ELEA THE MAGNETIC SUPPORT THE FOOT PEDAL THE
