Wound bed preparation: TIME in practice
|
|
|
- Martina Barber
- 6 years ago
- Views:
Transcription
1 Wound bed preparation: TIME in practice Wound bed preparation is now a well established concept and the TIME framework has been developed as a practical tool to assist practitioners when assessing and managing patients with wounds. It is important, however, to remember to assess the whole patient; the wound bed preparation care cycle promotes the treatment of the whole patient and not just the hole in the patient. This paper discusses the implementation of the wound bed preparation care cycle and the TIME framework, with a detailed focus on Tissue, Infection, Moisture and wound Edge (TIME). Caroline Dowsett, Heather Newton KEY WORDS Wound bed preparation Tissue Infection Moisture Edge The concept of wound bed preparation has gained international recognition as a framework that can provide a structured approach to wound management. By definition wound bed preparation is the management of a wound in order to accelerate endogenous healing or to facilitate the effectiveness of other therapeutic measures (Falanga, 2000; Schultz et al, 2003). The concept focuses the clinician on optimising conditions at the wound bed so as to encourage normal endogenous healing. It is an approach that should be considered for all wounds that are not progressing to normal wound healing. Wound healing is a complex series of events that are interlinked and Caroline Dowsett is Nurse Consultant in Tissue Viability, Newham Primary Care Trust, London, and Heather Newton is Nurse Consultant in Tissue Viability, Royal Cornwall Hospital Trust, Cornwall dependent on one another. Acute wounds usually follow a well-defined process described as: 8Coagulation 8Inflammation 8Cell proliferation and repair of the matrix 8Epithelialisation and remodelling of scar tissue. In the past this model of healing has been applied to chronic wounds, but it is now known that chronic wound healing is different from acute wound healing. Chronic wounds become stuck in the inflammatory and proliferative stages of healing (Ennis and Menses, 2000) which delays closure. The epidermis fails to migrate at the wound margins, which interferes with normal cellular migration over the wound bed (Schultz et al, 2003). In chronic wounds there appears to be an over production of matrix molecules resulting from underlying cellular dysfunction and disregulation (Falanga, 2000). Fibrinogen and fibrin are also common in chronic wounds and it is thought that these and other macromolecules scavenge growth factors and other molecules involved in promoting wound repair (Falanga, 2000). Chronic wound fluid is also biochemically distinct from acute wound fluid; it slows down, and can block the proliferation of cells, which are essential for the wound healing process (Schultz et al, 2003). Wound bed preparation as a concept allows the clinician to focus systematically on all of the critical components of a non-healing wound to identify the cause of the problem, and implement a care programme so as to achieve a stable wound that has healthy granulation tissue and a well vascularised wound bed. The TIME framework To assist with implementing the concept of wound bed preparation, the TIME acronym was developed in 2002 by a group of wound care experts, as a practical guide for use when managing patients with wounds (Schultz et al, 2003). The TIME table (Table 1) summarises the four main components of wound bed preparation: 8Tissue management 8Control of infection and inflammation 8Moisture imbalance 8Advancement of the epithelial edge of the wound. The TIME framework is a useful practical tool based on identifying the barriers to healing and implementing a plan of care to remove these barriers and promote wound healing. It is important to understand wound bed preparation and TIME within the context of total patient care. If a wound fails to heal there is often a complex mix of local and host factors which 58 Wounds UK
2 Table 1 TIME Principles of wound bed preparation Clinical observations Proposed pathophysiology WBP clinical actions Effect of WBP actions Clinical outcome Tissue non-viable or deficient Defective matrix and cell Viable wound base debris impair healing Infection or Inflammation High bacterial counts or prolonged inflammation Inflammatory cytokines Protease activity Growth factor activity Debridement (episodic or continuous): 8Autolytic, sharp surgical, enzymatic, mechanical or biological 8Biological agents Remove infected foci Topical/systemic: 8Antimicrobials 8Anti-inflammatories 8Protease inhibition Restoration of wound base and functional extracellular matrix proteins Low bacterial counts or controlled inflammation: Inflammatory cytokines Protease activity Growth factor activity Bacterial balance and reduced inflammation Moisture imbalance Desiccation slows epithelial cell migration Apply moisture-balancing dressings Restored epithelial cell migration, desiccation avoided Moisture balance Excessive fluid causes maceration of wound margin Compression, negative pressure or other methods of removing fluid Oedema, excessive fluid controlled, maceration avoided Edge of wound non-advancing or undermining Non-migrating keratinocytes Non-responsive wound cells and abnormalities in extracellular matrix or abnormal protease activity Re-assess cause or consider corrective therapies: 8Debridement 8Skin grafts 8Biological agents 8Adjunctive therapies Migrating keratinocytes and responsive wound cells. Restoration of appropriate protease profile Advancing edge of wound will need to be assessed and treated. A full and detailed patient assessment will highlight the underlying aetiology of the wound and other factors that may impede wound healing such as pain and poor nutrition (Dealey, 2000). With this in mind the wound bed preparation care cycle was developed in 2004 (Dowsett, 2004) to provide a care programme that includes the TIME framework. It focuses both on the patient and on the wound in an attempt to address all factors that influence wound healing. Wound bed preparation care cycle The care cycle (Figure 1) starts with the patient and their environment of care. Individual patient concerns need to be addressed as well as quality of life issues in order to achieve a successful care programme. Patients need to understand the underlying cause of their wound and the rationale for treatments. Assessment and treatment of the underlying condition is essential as the type of wound bed preparation implemented may vary with wound type. For example, sharp debridement is common in the management of patients with diabetic foot ulceration, while compression therapy is the recommended treatment for patients with venous leg ulcers (European Wound Management Association, 2004). The cycle moves from patient assessment and diagnosis to assessing and treating the wound using the TIME framework. The importance of assessment in terms of evaluating the effectiveness of the treatment is highlighted in the cycle. Those patients who have healed come out of the cycle into a prevention programme and patients who have not progressed to healing or who have palliative wounds remain in the cycle and are reassessed, using TIME. The TIME table has been designed to help the clinician make a systematic interpretation of the observable characteristics of a wound and to decide on the most appropriate intervention: T for tissue: non-viable or deficient I for infection/inflammation M for moisture imbalance E for edge, which is not advancing or undermining. T Tissue The specific characteristics of the tissue within a wound bed play a very important role in the wound healing continuum. Accurate description of this tissue is an important feature of wound assessment. Where tissue is non-viable or deficient, wound healing is delayed. It also provides a focus for infection, prolongs the inflammatory response, mechanically obstructs contraction 60 Wounds UK
3 Prevention Yes Healed Figure 1. The wound bed preparation care cycle. Figure 2. Fixed yellow slough on a wound bed. and impedes re-epithelialisation (Baharestani, 1999). Necrosis, eschar, and slough are terms that describe non-viable tissue, however, little is known about their constituents. Work undertaken by Thomas et al (1999) found that devitalised tissue has a defined structure similar to human dermis, however, there are areas of scattered, degraded or disrupted tissue present. For epidermal cells to migrate across a wound surface a well built extracellular matrix is required. Therefore, early interventions to remove devitalised tissue are an essential part of wound management. Necrosis or eschar on a wound is usually identified through its black/ No Treat & evaluate TIME interventions Start with the patient Wound bed preparation Care cycle Perform TIME assessment Agree goals Identifying wound aetiology dark grey appearance and, when dried out, is tough and leathery to touch. Wound eschar is full thickness, dry, devitalised tissue that has arisen through prolonged local ischaemia (Gray et al, 2005). It is derived from granulation tissue after the death of fibroblasts and endothelial cells and may also contain inflammatory cells (Thomas et al, 1999) which increases the risk of chronic inflammation of the wound and delays extracellular matrix formation. Necrotic tissue acts as a physical barrier to epidermal cell migration, and hydration at the wound interface is significantly reduced. Slough is adherent fibrous material derived from proteins, fibrin and fibrinogen (Tong, 1999). It is usually creamy yellow in appearance and can be found dehydrated and adhered to the wound bed (Figure 2) or loose and stringy when associated with increased wound moisture. The presence of devitalised tissue in a wound is often a challenge to health care professionals. It is difficult to accurately assess the depth of a wound that is covered or filled with necrotic or sloughy tissue and, until removed, the true extent of the wound may not be realised. In the majority of clinical cases there is a need to remove the devitalised tissue through a process of debridement, however, it is important to assess the blood flow to the affected area first, particularly if the wound is on the lower leg or foot. In cases where the limb requires revascularisation, it may not be appropriate to undertake tissue debridement until the viability of the limb is determined. Debridement Debridement is the process of removing devitalised tissue and/or foreign material from a wound and it may occur naturally. However, in some cases the patient may have an underlying pathology which affects the ability of the body to naturally debride the wound. In a chronic wound, debridement is often required more than once as the healing process can stop or slow down allowing further devitalised tissue to develop. Where debridement is an option for clinicians the following methods may be used: 8Surgical 8Sharp 8Autolytic 8Enzymatic 8Larval 8Mechanical. Surgical and sharp debridement Surgical and sharp debridement are the fastest methods of removing devitalised tissue and have the benefit of converting a non-healing chronic wound to that of an acute wound within a chronic wound environment (Schultz et al, 2003) Surgical debridement is normally performed where there is a large extent of devitalised tissue present and where there are significant infection risks. Sharp debridement is more conservative, but it still requires the skills of an experienced practitioner. Clinical competencies such as knowledge of anatomy, identification of viable or non-viable tissue, ability and resources to manage complications such as bleeding and the skills to obtain patient consent are all essential before undertaking this procedure. 62 Wounds UK
4 Autolytic debridement Autolytic debridement is a highly selective process involving macrophage and endogenous proteolytic enzymes which liquefy and separate necrotic tissue and eschar from healthy tissue (Schultz et al, 2003) The natural process is further enhanced by the use of occlusive and semi-occlusive dressings and those which interact to create a moist environment. Phagocytic activity is enhanced and increasing the moisture at the wound interface promotes tissue granulation. Table 2. Risk factors for infection in chronic wounds Local factors Large wound area Deep wound High degree of chronicity Anatomic location, e.g. anal region Presence of necrotic tissue High degree of contamination Reduced tissue perfusion Systemic factors Vascular disease Oedema Malnutrition Diabetes mellitus/rheumatoid arthritis Smoking/alcoholism Previous surgery or radiotherapy Use of corticosteroids/immunosuppressants Enzymatic degradation Enzymatic debridement is a less common method of debridement, however, it is effective in the removal of hard necrotic eschar where surgical debridement is not an option. Exogenous enzymes are applied to the wound bed where they combine with the endogenous enzymes in the wound to break down the devitalised tissue. (Schultz et al, 2005). Larval therapy Larval therapy is a quick, efficient method of removing slough and debris from a wound, however, not all patients or staff find this debridement method socially acceptable. Sterile larvae secrete powerful enzymes to break down devitalised tissue without destroying healthy granulation tissue (Thomas et al, 1998). Mechanical debridement Mechanical methods of debridement such as irrigation and wet to dry dressings are rarely used as they can cause increased pain and can damage newly formed granulation tissue (NICE, 2001). If debridement is effective, the T of TIME is removed and wounds can progress through the remaining phases of wound healing. I infection/inflammation Infection in a wound causes pain and discomfort for the patient, delayed wound healing, and can be life threatening. Clinical infections as well as having serious consequences for the patient can add to the overall cost Figure 3. Clinically infected wound. of care. All wounds contain bacteria at levels ranging from contamination, through critical colonisation (also known as increased bacterial burden or occult infection), to infection. The increased bacterial burden may be confined to the superficial wound bed or may be present in the deep compartment and surrounding tissue of the wound margins. Several systemic and local factors increase the risk of infection (Table 2). Emphasis is often placed on the bacterial burden, but in fact host resistance is often the critical factor in determining whether infection will occur. Host resistance is lowered by poor tissue perfusion, poor nutrition, local oedema and other behavioural factors such as smoking and drinking excess alcohol. Other systemic factors that impair healing include co-morbidities and medication such as steroid therapy and immunosuppressive drugs. Local factors at the wound bed, such as necrotic tissue and foreign material such as fragments of gauze and dressings, also affect healing and the risk of infection. When a wound is infected (Figure 3) it contains replicating micro-organisms which elicit a host response and cause injury to the host. In an acute wound, infection is met by a rapid inflammatory response which is initiated by complement fixation and an innate immune response followed by the release of cytokines and growth factors (Dow et al, 1999). The inflammatory cascade produces vasodilation and a significant increase of blood flow to Wounds UK 63
5 Table 3 Differentiating between superficial and deep infection Superficial infection Non-healing Friable granulation tissue Exuberant bright granulation tissue Increased exudate New areas of necrosis in base Wound breakdown the injured area. This also facilitates the removal of micro-organisms, foreign bodies, bacterial toxins and enzymes by phagocytic cells, complements, and antibodies. The coagulation cascade is activated isolating the site of infection in a gel matrix to protect the host (Dow et al,1999). In a chronic wound, however, the continuous presence of virulent micro-organisms leads to a continued inflammatory response which eventually contributes to host injury. There is persistent production of inflammatory mediators and steady migration of neutrophils which release cytolytic enzymes and oxygen-free radicals. There is localised thrombosis and the release of vasoconstricting metabolites which can lead to tissue hypoxia, bringing further bacterial proliferation and tissue destruction (Sibbald et al, 2003). The presence of bacteria in a chronic wound does not necessarily indicate that infection has occurred or that it will lead to impaired wound healing (Cooper and Lawrence, 1996). Micro-organisms are present in all chronic wounds and low levels of certain bacteria can facilitate wound healing as they produce enzymes such as hyaluronidase which contributes to wound debridement and stimulates neutrophils to release proteases (Stone, 1980). Diagnosis of infection is primarily a clinical skill and microbiological data should be used to supplement the Deep infection Pain: other than usually reported Increased size Warmth Erythema > 1 2cm Probes to bone or bone exposed Odour (Sibbald et al, 2000) clinical diagnosis. The classic signs of infection in acute wounds include: 8Pain 8Erythema 8Oedema 8Purulent discharge 8Increased heat. For chronic wounds it has been suggested that other signs should be added: 8Delayed healing 8Increased exudates 8Bright red discolouration of granulation tissue 8Friable and exuberant tissue 8New areas of slough 8Undermining 8Malodour and wound breakdown (Cutting and Harding, 1994). These criteria have now been modified according to wound type (Cutting et al, 2005) and are the subject of a position paper (EWMA, 2005). In this document, Cutting et al describe the results of a Delphi approach as a method of developing consensus on the criteria for identification of wound infection. The results of the study indicated that cellulities, malodour, pain, delayed healing or deterioration in the wound/wound breakdown are criteria common to all wounds, but other changes should be noted in different wound types. The Delphi process identified the criteria for six different wound types and should be used as a guide when diagnosing infection in both acute and chronic wounds. Sibbald et al (2000) suggest that diagnosis should differentiate between superficial and deep infection as outlined in Table 3. Treatment of infection should first of all focus on optimising host resistance by promoting healthy eating, encouraging smoking cessation and addressing underlying medical conditions such as diabetes. Systemic antibiotics are not necessarily the most appropriate way of reducing bacterial burden in wounds, particularly because of the threat of increasing bacterial resistance and should only be used where there is evidence of deep infection or where infection cannot be managed with local therapy (Schultz et al, 2003). Local methods include: debridement to remove devitalised tissue; wound cleansing; and the use of topical antimicrobials such as iodine dressings and silver. There is renewed interest in the selective use of topical antimicrobials as bacteria become more resistant to antibiotics. Studies show that some iodine and silver preparations have bactericidal effects even against multiresistant organisms such as methicillinresistant Staphylococcus aureus (MRSA) (Landsdown, 2002; Romanelli et al, 2003; Sibbald et al, 2003). Where infection in the wound has extended beyond the level that can be managed with local therapy, systemic antibiotics should be used. Systemic signs of infection, such as fever, and cellulities extending at least 1cm beyond the wound margin and underlying deep structures, will require systemic antibiotic therapy (Schultz et al, 2003). M moisture imbalance Creating a moisture balance at the wound interface is essential if wound healing is to be achieved. Exudate is produced as part of the body s response to tissue damage and the amount of exudate produced is dependant upon the pressure gradient within the tissues (Trudgian, 2005). A wound which progresses through the normal wound healing cycle produces enough moisture to promote cell 64 Wounds UK
6 Table 4 Exudate types Description of exudate Serous Fibrinous Purulent Haemopurulent Haemorrhagic proliferation and supports the removal of devitalised tissue through autolysis. If, however, the wound becomes inflamed and/or stuck in the inflammatory phase of healing, exudate production increases as the blood vessels dilate. A description of the types of exudates can be found in Table 4. Evidence suggests that there are significant differences between acute and chronic wound fluid (Park et al,1998). Acute wound fluid supports the stimulation of fibroblasts and the production of endothelial cells as it is rich in leukocytes and essential nutrients. Chronic wound fluid, however, has been found to contain high levels of proteases which have an adverse effect on wound healing by slowing down or blocking cell proliferation (Schultz et al, 2003) in particular keratinocytes, fibroblasts Components of exudate Clear and watery. Bacteria may be present Cloudy. Contains fibrin protein strands Milky. Contains infective bacteria and inflammatory cells As above but dermal capillary damage leads to the presence of red cells Red blood cells are a major component of the exudate (Vowden and Vowden, 2004) Figure 4. Evidence of irritant dermatitis following dressing application. and endothelial cells. Increased levels of proteolytic enzymes and reduced growth factor activity all contribute to a poorly developed extracellular wound matrix. This in turn affects the ability of the epidermal cells to migrate across the surface of the wound to complete the healing process. Factors such as the underlying condition of the patient, the pathology of the wound and the dressing selection all affect the production of exudate (White, 2001). Moisture in a wound enhances the natural autolytic process and also acts as a transport medium for essential growth factors during epithelialisation. If a wound bed becomes too dry, however, a scab will form which then impedes healing and wound contraction. The underlying collagen matrix and the surrounding tissue at the wound edge become desiccated (Dowsett and Ayello, 2004). If a wound produces excessive amounts of exudate the wound bed becomes saturated and moisture leaks out onto the peri-wound skin causing maceration and excoriation. This in turn could lead to an increased risk of infection. Exudate assessment Assessment of the exudate is an important part of wound management. The type, amount and viscosity of the exudate should be recorded and dressings selected based on the exudate s characteristics. If a wound is too dry, rehydration should be the principle of management, unless contraindicated as in the case of ischaemic disease. Occlusive dressing products promote a moist environment at the wound interface. As wounds heal, the level of exudate gradually decreases. The management of excess exudate in chronic wounds, however, presents a challenge to many health care professionals. Vowden and Vowden (2004) suggest that an understanding of the systemic and local conditions influencing exudate production and knowledge of the potential damaging chemical constituents of exudates should inform management strategy. Dressing selection When selecting a dressing, consideration should be given to the volume of exudate and the viscosity as some dressings absorb a higher volume of fluid than others and some are more efficient when dealing with viscous exudate. There are a variety of dressing products available for the management of exudates ranging from foams, hydrocolloids, alginates, hydrofibres, cadexomer iodine to capillary action dressings. All play a role in the removal of fluid away from the wound surface, however, many of the products, through their ability to gel on contact with wound exudates, maintain a moisture balance on the wound surface itself. VAC therapy or total negative pressure is a therapy which draws exudates from the wound bed through application of sub-atmospheric pressure via an electronic pump (Mendez- Eastman, 2001). Compression bandages also play a role in the removal of excess 68 Wounds UK
7 fluid in the lower limbs in patients with venous leg ulcers and lymphoedema. The condition of the surrounding skin is also important as vulnerable skin can react to excess exudate and cause maceration, excoriation, and irritant dermatitis (Figure 4). Early application of a protective skin barrier film can minimise these risks. It is important to remember to treat the underlying clinical condition when addressing moisture imbalance in a wound (Newton and Cameron, 2003). E edge When the epidermal margins of a wound fail to migrate across the wound bed or the wound edges fail to contract and reduce in size, consideration needs to have been given to the T,I, and M first to ensure that all aspects of wound bed preparation have been considered. The final stage of wound healing is epithelialisation, which is the active division, migration, and maturation of epidermal cells from the wound margin across the open wound (Dodds and Haynes, 2004). There are many factors which need to be present in order for epithelialisation to take place. The wound bed must be full of well vascularised granulation tissue in order for the proliferating epidermal cells to migrate. This also ensures that there is adequate oxygen and nutrients to support epidermal regeneration. There needs to be a rich source of viable epidermal cells which can undergo repeated cell division particularly at the edge of the wound. Where cells have become senescent the process slows down or stops completely. Wounds that have a significant number of fibroblasts that are arrested due to senescence, damaged DNA or enduring quiescence do not heal (Vande Berg and Robson, 2003). Other factors, such as bacteria or the presence of devitalised tissue, which interfere with epidermal cell growth, have the potential to influence the rate of wound healing. There are many reasons why the epidermal margin fails to migrate Figure 5. Diabetic foot ulcer. including hypoxia, infection, desiccation, dressing trauma, hyperkeratosis and callus at the wound margin (Moffatt et al, 2004). For wound healing to be effective, there needs to be adequate tissue oxygenation. Decreased oxygen levels impair the ability of the leucocytes to kill bacteria, lower production of collagen and reduce epithelialisation (Schultz et al, 2003). It is important to remember that wounds rely on both macro- and microcirculation particularly in the lower limb. A baseline assessment needs to be undertaken to determine the degree of ischaemic disease and the ability of the wound to heal without vascular intervention. Wound infection as discussed previously is extremely destructive to a healing wound. Inflammation caused by bacteria causes the extracellular matrix to degrade and therefore epidermal cell migration is interrupted. Wounds become chronic and fail to heal. Dressing products, particularly if adhered or made of fibrous materials, also cause trauma and inflammation of the wound bed which in turn delays healing. It is important to select dressing products which are non adherent, and will not dry out or leave fibres in the wound bed. In certain clinical conditions such as in diabetic neuropathy, there is an over production of hyperkeratosis and callus formation (Figure 5). It has also been noted that the epidermis of the skin surrounding venous leg ulcers is thicker than normal skin and highly keratinised (Schultz et al, 2005). If this proliferative, thickened tissue is not removed, wounds will fail to epithelialise. Failure of a wound edge to migrate is also thought to be associated with the inhibition of the process of normal programmed cell death (apoptosis) which particularly affects fibrobasts and keratinocytes. Cells undergo a characteristic series of changes following mechanical damage to the cell and on exposure to toxic chemicals. Cells become unresponsive and die. Undermining or rolling of a wound edge can also influence the ability of the wound to heal. Undermining can be indicative of a chronic wound and in particular, those wounds that are Wounds UK 69
8 also critically colonised with bacteria or infected. Rolled edges can present in wounds that have an inflammatory origin such as pyoderma gangenosum or in malignancy. Early diagnosis is important in these cases as failure to provide the appropriate second-line therapy such as oral steroids or tissue biopsy and excision can result in poor healing outcomes. Measuring a wound at the start of treatment is seen as best practice to enable accurate assessment of the impact of a clinician s intervention. Subsequent measuring can identify whether or not a wound is failing to heal or deteriorating. The edge of the wound will not epithelialise unless the wound bed is well prepared. Always consider the elements of T,I, and M first to ensure that the use of advanced therapies are appropriate and if used are applied to a well prepared wound bed to ensure optimal effect. Summary and conclusion The management of chronic wounds has progressed from merely assessing the status of the wound to understanding the underlying molecular and cellular abnormalities that prevent the wound from healing. The concept of wound bed preparation has simultaneously evolved to provide a systematic approach to removing the barriers to natural healing and enhancing the effects of advanced therapies. Wound bed preparation and the TIME framework are most likely to be successful when used alongside the wound bed preparation care cycle. References Baharestani M (1999) The clinical relevance of debridement. In: Baharestani M et al, eds. The Clinical Relevance of Debridement. Springer- Verlag, Berlin Cooper RA, Lawrence JC (1996) Microorganisms and wounds. J Wound Care 5(5): Cutting KF, Harding KG (1994) Criteria for identifying wound infection. J Wound Care 3: Cutting K, Tong A (2003) Wound Physiology and Moist Wound healing. Medical Communications Ltd, Holsworthy Key Points 8 The TIME framework has been developed as a practical tool for managing patients with wounds. 8 The wound bed preparation care cycle focuses care on the patient and their underlying condition. 8 Patient progress and response to treatment should be regularly evaluated. Dealey C (2000) The Care of Wounds. Blackwell Science, Oxford Dodds S, Haynes S (2004) The wound edge, epithelialisation and monitoring wound healing. A journey through TIME. Wound bed preparation in practice. Br J Nurs Supplement Dow G, Browne A, Sibbald RG (1999) Infection in chronic wounds: controversies in diagnosis and treatment. Ostomy Wound Manag 45: Dowsett C, Ayello E (2004) TIME principles of chronic wound bed preparation and treatment. Br J Nurs 13(Suppl 15): S16 S23 Dowsett C (2004) TIME in Context. The Wound Bed Preparation Care Cycle. Oral presentation at Wounds UK 2004, Harrogate, UK Ennis WJ, Menses P (2000) Wound healing at the local level: the stunned wound. Ostomy Wound Manag 46: 39S 48S European Wound Management Association (2004) Position Document: Wound Bed Preparation in Practice. MEP Ltd, London European Wound Management Association (2005) Position Document: Identifying Criteria for Wound Infection. MEP Ltd, London Falanga V (2000) Classifications for wound bed preparation and stimulation of chronic wounds. Wound Repair Regen 8: Falanga V (2002) Wound bed preparation and the role of enzymes: a case for multiple actions of therapeutic agents. Wounds 4(2): Gray D, White R, Cooper P, Kingsley A (2005) Using the wound healing continuum to identify treatment objectives. Applied Wound Management supplement. Part 2. Wounds UK 1(2): S9 S14 Lansdown AB (2002) Silver: Its antibacterial properties and mechanism of action. J Wound Care 11(4): Mendez-Eastman S (2001) Guidelines for using negative pressure wound therapy. Adv Skin Wound Care 14(6): Moffatt C, Morison MJ, Pina E (2004) Wound bed preparation for Venous Ulcers. In: Wound Bed Preparation in Practice. EWMA Position Document, MEP, London National Institute for Clinical Excellence (2001) Guidance of the Use of Debriding Agents and Specialist Wound Care Clinics for Difficult to Heal Surgical Wounds. NICE, London Newton H, Cameron J (2003) Skin Care in Wound Management. Medical Communications Ltd. Holsworthy, UK Park HY, Shon K, Phillips T (1998) The effect of heat on the inhibitory effects of chronic wound fluid on fibroblasts in vitro. Wounds 10: Romanelli M, Magliaro A, Mastronicola D, Siani S, et al (2003) Systemic antimicrobial therapies for pressure ulcers. Ostomy Wound management 49(5a Suppl): 25 9 Schultz G, Sibbald G, Falanga V, et al (2003) Wound bed preparation: a systematic approach to wound management. Wound Repair Regen 11: 1 28 Schultz G, Ladwig G, Wysocki A (2005) Extracellular matrix: review of its role in acute and chronic wounds. World Wide Wounds. Sibbald RG, Williamson D, Orsted HL, et al (2000) Preparing the wound bed: debridement, bacterial balance and moisture balance. Ostomy Wound Manag 46: Sibbald RG, Orsted HL, Schultz G, Coutts RN, Keast MD (2003) Preparing the wound bed: focus on infection and inflammation. Ostomy Wound Manag 47: Stone LL (1980) Bacterial debridement of the burn eschar: the in vivo activity of selected organisms. J Surg Res 29: Thomas AML, Harding KG, Moore K (1999) The structure and composition of chronic wound eschar. J Wound Care 8(6): Tong A (1999) The identification and treatment of slough. J Wound Care 8(7): Trudgian J (2005) Exudate management and wound bed preparation: taking the moist approach. Wounds UK 1(suppl 2): Vande Berg JS, Robson MC (2003) Arresting cell cycles and the effect on wound healing. Surg Clin North America 83(3): Vowden K, Vowden P (2004) Understanding exudates management and the role of exudates in the healing process. The Exudate Supplement,Part Two. Br J Nurs White R (2001) Managing exudates. Part 1. Nursing Times 97(9): XI XIII 70 Wounds UK
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
The Triangle of Wound Assessment
 The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
The Triangle of Wound Assessment A simple and holistic framework for wound management CPWSC_TOWA_Brochure_210x210_2018.indd 1 10/01/2018 15.13 ? We asked healthcare professionals around the world about
Fundamentals Of Wound Management. Julie Hewish Senior Tissue Viability Nurse
 Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Fundamentals Of Wound Management Julie Hewish Senior Tissue Viability Nurse Wound Management What are we trying to achieve? Maintaining a controlled set of local conditions that is able to sustain the
Wound Care in the Community. Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts
 Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
Wound Care in the Community Lisa Sutherland MSc Tissue Viability Senior Lead Ipswich Hospital & Community NHS Trusts What are the key elements? What is the patient s goal or aim for the wound? What are
RN Cathy Hammond. Specialist Wound Management Service at Nurse Maude Christchurch
 RN Cathy Hammond Specialist Wound Management Service at Nurse Maude Christchurch 14:00-14:55 WS #141: Wound Infection - What You Need to Know 15:05-16:00 WS #153: Wound Infection - What You Need to Know
RN Cathy Hammond Specialist Wound Management Service at Nurse Maude Christchurch 14:00-14:55 WS #141: Wound Infection - What You Need to Know 15:05-16:00 WS #153: Wound Infection - What You Need to Know
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Disclosures for Tarik Alam. Wound Bed Preparation. Wound Prognosis. Session Objectives. Debridement 4/26/2015
 Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Disclosures for Tarik Alam Challenges in Managing Bioburden and Devitalized Tissue Tarik Alam RN, BScN, ET, MClSc(WH) Enterostomal Therapy Nurse tarikalam@hotmail.com Clinical Affairs Manager for Hollister
Foam dressings have frequently
 The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
The practical use of foam dressings Efficient and cost-effective management of excessive exudate continues to challenge clinicians. Foam dressings are commonly used in the management of moderate to heavily
Assessment & Management of Wounds in primary practice.
 Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Assessment & Management of Wounds in primary practice. Nutrition Successful wound management depends on appropriate nutritional support. Poor nutrition is recognised as one of the major causes of poor
Wound debridement: guidelines and practice to remove barriers to healing
 Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
Wound debridement: guidelines and practice to remove barriers to healing Learning objectives 1. The burden of wounds and the impact to the NHS 2. Understand what debridement is and why it is needed 3.
How Wounds Heal: A Guide for the Wound-care Novice
 C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
C L I N I C A L P R A C T I C E How Wounds Heal: A Guide for the Wound-care Novice BY Christine Pearson Christine Pearson, RN, IIWCC, is a wound clinician for Vancouver Coastal Health and has worked in
DEBRIDEMENT. Professor Donald G. MacLellan Executive Director Health Education & Management Innovations
 DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
DEBRIDEMENT Professor Donald G. MacLellan Executive Director Health Education & Management Innovations DEBRIDEMENT Principles - CSD Methods of Debridement Biopsy options PRINCIPLES OF WOUND MANAGEMENT
Advanced Wound Care. Cut Shape Innovate
 Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Advanced Wound Care Cut Shape Innovate Vacutex incorporates a patented three layer construction of poly-cotton elements that promotes an accelerated capillary action on wound interfaces. Effectively lifting,
Resources to Guide the Management of Suspected Infection in Chronic Wounds
 Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Resources to Guide the Management of Suspected Infection in Chronic Wounds Health Improvement Scotland published their 13th Health Technology Assessment (HTA 13) in December 2015 entitled, Antimicrobial
Debridement: treatment, options and selection.
 This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
This document is the Accepted Manuscript version of a Published Work that appeared in final form in Independent Nurse, copyright MA Healthcare, after peer review and technical editing by the publisher.
I ve a drawer full of dressings i don t know how to use!
 I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
I ve a drawer full of dressings i don t know how to use! Introduction: Originating from battlefield medicine much of what we use today is an evolution of material science combined with our understanding
TIME CONCEPT AND LOCAL WOUND MANAGEMENT
 TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
TIME CONCEPT AND LOCAL WOUND MANAGEMENT B. BRAUN WOUND CARE INTRODUCTION: TIME is a global care framework used to implement appropriate care plans and promote wound healing Tissue Management Inflammation
Wound assessment is a
 Wound assessment part 2: exudate Wound exudate provides the moist environment required for cell regeneration. However, in chronic wounds exudate can become excessive and prevent healing. Changes in the
Wound assessment part 2: exudate Wound exudate provides the moist environment required for cell regeneration. However, in chronic wounds exudate can become excessive and prevent healing. Changes in the
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Making the Most of your Dressing Products Catherine Hammond CNS/CNE
 Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Making the Most of your Dressing Products 2013 Catherine Hammond CNS/CNE What do you need in your dressings cupboard? 2 Skin tear 3 4 Lack Confidence in Selecting Dressings? 5 Appropriate Use of Product
Topical antimicrobials (antiseptics) Iodine, Silver, Honey
 Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Topical antimicrobials (antiseptics) Iodine, Silver, Honey Iodine Honey Silver Enzymatic debridement Proteolytic enzyme, also called Proteinase Proteinase breaks the long chainlike molecules of proteins
Diagnosing wound infection - a clinical challenge
 Diagnosing wound infection - a clinical challenge Keith F Cutting Merimbula, 5 th November 2010 Wound infection microbial load immune system microbial load + + + immune system infection host response Diagnosing
Diagnosing wound infection - a clinical challenge Keith F Cutting Merimbula, 5 th November 2010 Wound infection microbial load immune system microbial load + + + immune system infection host response Diagnosing
WHY WOUNDS FAIL TO HEAL SIMPLIFIED
 WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
WHY WOUNDS FAIL TO HEAL SIMPLIFIED 10 Some of the common signs of failure to heal with possible causes and some interventions WHY WOUNDS FAIL TO HEAL There must be adequate supplies of nutrients and oxygen
Hemostasis Inflammatory Phase Proliferative/rebuilding Phase Maturation Phase
 The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
The presenters are staff members of the CHI Health St. Elizabeth Burn and Wound Center. Many of the products discussed are used in our current practice but we have no conflict of interest to disclose.
SAMPLE. HLTEN406A Undertake basic wound care. Learner resource. HLT07 Health Training Package. Version 2
 HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
HLT07 Health Training Package HLTEN406A Undertake basic wound care Learner resource Version 2 Training and Education Support Industry Skills Unit Meadowbank Acknowledgments The TAFE NSW Training and Education
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Understanding the importance of holistic wound assessment
 Understanding the importance of holistic wound assessment It is important to undertake a holistic assessment of the patient who presents with a wound. Karen Ousey and Leanne Cook give an overview of the
Understanding the importance of holistic wound assessment It is important to undertake a holistic assessment of the patient who presents with a wound. Karen Ousey and Leanne Cook give an overview of the
Surgical Wounds & Incisions
 Surgical Wounds & Incisions A Comprehensive Review Assessment & Management Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist www.woundcarenurses.org 1
Surgical Wounds & Incisions A Comprehensive Review Assessment & Management Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist www.woundcarenurses.org 1
Wound bed preparation
 Wound bed preparation Author(s) Kathryn Vowden RGN, DPSN(TV) Clinical Nurse Specialist (Vascular and Wound Healing) Bradford Royal Infirmary Bradford, UK Peter Vowden MD, FRCS Consultant Vascular Surgeon
Wound bed preparation Author(s) Kathryn Vowden RGN, DPSN(TV) Clinical Nurse Specialist (Vascular and Wound Healing) Bradford Royal Infirmary Bradford, UK Peter Vowden MD, FRCS Consultant Vascular Surgeon
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Effective Diagnosis of Local Wound Bed Infection. Julie Hewish Senior Tissue Viability Nurse Oxford Health NHS Foundation Trust
 Effective Diagnosis of Local Wound Bed Infection Julie Hewish Senior Tissue Viability Nurse Oxford Health NHS Foundation Trust Localised Wound Bed Infection is the Result of imbalance between patient s
Effective Diagnosis of Local Wound Bed Infection Julie Hewish Senior Tissue Viability Nurse Oxford Health NHS Foundation Trust Localised Wound Bed Infection is the Result of imbalance between patient s
Currently, the NHS is facing the challenge of
 Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
Evaluation of a superabsorbent dressing in a primary care organization Jackie Stephen-Haynes and Claire Stephens Jackie Stephen-Haynes is Professor and Nurse Consultant, Practice Development Unit, Birmingham
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Essity Internal. Taking the fear out of wound infection: conquering everyday issues
 Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Taking the fear out of wound infection: conquering everyday issues Learning objectives 1. Identifying the cost which wound infection can have on both the patient and healthcare organisations 2. Understanding
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
We will dose your Gentamycin. We will dose your Vancomycin
 We will dose your Gentamycin We will dose your Vancomycin We will dose your Heparin We will dose your Warfarin We will do your wound care Animal models show that wounds, including chronic wounds, heal
We will dose your Gentamycin We will dose your Vancomycin We will dose your Heparin We will dose your Warfarin We will do your wound care Animal models show that wounds, including chronic wounds, heal
DRESSING SELECTION SIMPLIFIED
 10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
10 DRESSING SELECTION SIMPLIFIED It must be recognised that no one dressing provides the optimum environment for the healing of all wounds (Mahoney, 2015) DRESSING SELECTION SIMPLIFIED Selecting the correct
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Wound Assessment & Treatment
 Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
Wound Assessment & Treatment Cathy Lyle Advanced Practice Nurse Providence Care, SMOL site LTC Physicians CME June 2011 Outline l Is it healing? l Will it heal? l What colour is it? l How wet is it? l
The Management of Lower Limb Oedema. Catherine Hammond CNS/CNE 2018
 The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
The Management of Lower Limb Oedema Catherine Hammond CNS/CNE 2018 Causes of oedema Venous stasis Lymphoedema Heart Failure Dependency Liver and kidney failure Medications Cellulitis Low protein Under
Galen ( A.D) Advanced Wound Dressing
 Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Galen (120-201A.D) Advanced Wound Dressing Wounds heal optimally in a moist environment นพ.เก งกาจ ว น ยโกศล Wound assessment Ideal wound dressing Type of wound Clinical appearance Wound location Measurement
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Prontosan. Clean. Easy Wound Healing. Wound Cleansing
 Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Prontosan Clean. Easy Wound Healing. Wound Cleansing CoE Infection Control Prontosan the unique combination of Betaine & Polihexanide reduces healing time removes and prevents biofilm prevents infections
Ray Norris, Rachel Henchy
 Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Use of low frequency ultrasound therapy in the treatment of recalcitrant leg ulcers: case series This series of case reports looks at the efficacy of low frequency ultrasound using the MIST Therapy System
Guide to avoiding complications after Caesarean section
 Guide to avoiding complications after Caesarean section Lindsey Bullough Tissue Viability Nurse, Wrightington, Wigan and Leigh NHS Foundation Trust Reducing Caesarean section complications The proportion
Guide to avoiding complications after Caesarean section Lindsey Bullough Tissue Viability Nurse, Wrightington, Wigan and Leigh NHS Foundation Trust Reducing Caesarean section complications The proportion
Debridement masterclass <KOL>
 Debridement masterclass The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
Debridement masterclass The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE
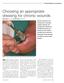 Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
Choosing an appropriate dressing for chronic wounds Denise Bell BSc, RGN and Dot Hyam RGN, DipHE Chronic wounds are nonhealing with a sometimes complex aetiology, and dressing such wounds can be difficult
EWMA Educational Development Programme. Curriculum Development Project. Education Module. Wound Infection
 EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
EWMA Educational Development Programme Curriculum Development Project Education Module Wound Infection Latest revision: February 2014 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME The Programme is designed
DEBRIDEMENT. In This Chapter. Chapter 8. Necrotic Tissue Eschar Slough Types of Debridement When Not to Debride...
 Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Chapter 8 DEBRIDEMENT In This Chapter Necrotic Tissue.............................. 165 Eschar.................................... 165 Slough.................................... 166 Types of........................
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
The Risk. Background / Bias. Integrating Wound Care into a Limb Preservation Initiative 4/24/2009
 Stimulating Wound Granulation: Advances in NPWT and other Measures (Wound Bed Preparation) Charles Andersen MD, FACS, FAPWCA Clinical Prof of Surgery UW, USUHS Chief Vascular/Endovascular/ Limb Preservation
Stimulating Wound Granulation: Advances in NPWT and other Measures (Wound Bed Preparation) Charles Andersen MD, FACS, FAPWCA Clinical Prof of Surgery UW, USUHS Chief Vascular/Endovascular/ Limb Preservation
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Wound Healing Basic Concept
 Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
Department of Orthopaedic & Traumatology The Chinese University of Hong Kong Wound Healing Basic Concept Dr TSE Lung Fung ( 謝龍峰醫生 ) MBChB(CUHK),FRCS(Edin),FRCSEd(Orth),FHKCOS,FHKAM(Ortho) Tissue Damage
The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study
 The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study Woundmanagement Summary In the treatment of patients with chronic
The clinical performance of PermaFoam cavity in the management of chronic wounds: a prospective, non-randomized clinical observation study Woundmanagement Summary In the treatment of patients with chronic
This article is based on a symposium held
 Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Advances in wound cleansing: an integrated approach LIZ OVENS Independent Tissue Viability Specialist Nurse SALLY IRVING Independent Tissue Viability Nurse Consultant This article is based on a symposium
Wound Management Capital Health Network Practice Nurses 20 Feb 2018
 Wound Management Capital Health Network Practice Nurses 20 Feb 2018 ) MNP Judith Barker RN; NP; STN; B Hlth Sc (Nurs); MN (NP) Nurse Practitioner Wound Management Rehabilitation, Aged & Community Care
Wound Management Capital Health Network Practice Nurses 20 Feb 2018 ) MNP Judith Barker RN; NP; STN; B Hlth Sc (Nurs); MN (NP) Nurse Practitioner Wound Management Rehabilitation, Aged & Community Care
WOUND CARE UPDATE. -Commonly Used Skin Substitute Products For Wound. -Total Contact Casting. Jack W. Hutter DPM, FACFAS, C. ped.
 WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
WOUND CARE UPDATE -Commonly Used Skin Substitute Products For Wound Closure -Total Contact Casting Jack W. Hutter DPM, FACFAS, C. ped. Commonly Used Skin Substitute Products for Wound Closure why are they
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Pressure Ulcer Prevention Guidelines
 EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE Debrisoft for the debridement of acute and chronic wounds 1 Technology 1.1 Description of the technology The Debrisoft
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Wound Healing: General Principles. Mansour Dib MD
 Wound Healing: General Principles Mansour Dib MD Normal Wound Healing Chronic Wounds: Stuck Where does it get stuck? Mostly Proliferation Sometimes Remodeling Why? Systemic factors Local factors How do
Wound Healing: General Principles Mansour Dib MD Normal Wound Healing Chronic Wounds: Stuck Where does it get stuck? Mostly Proliferation Sometimes Remodeling Why? Systemic factors Local factors How do
Exudate in the early stages of wound healing
 Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Wound management accounts for
 An audit to determine the clinical effectiveness of a pathway for managing wound infection KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
An audit to determine the clinical effectiveness of a pathway for managing wound infection KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
Wound management accounts for
 An audit to determine the clinical effectiveness of a pathway for managing wound infection. KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
An audit to determine the clinical effectiveness of a pathway for managing wound infection. KEY WORDS Wound management Infection risk Clinical pathway Audit Prevention of wound infection is a key objective
INVESTIGATING: WOUND INFECTION
 INVESTIGATING: WOUND INFECTION Diagnosing infection in surgical and other wounds involves nurses being able to observe the clinical signs in a wound rather than simply obtaining positive microbiology results
INVESTIGATING: WOUND INFECTION Diagnosing infection in surgical and other wounds involves nurses being able to observe the clinical signs in a wound rather than simply obtaining positive microbiology results
Many patients with chronic wounds. Case reports. The use of Prontosan in combination with Askina Calgitrol : an independent case series
 Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Independent evaluation of BEMER physical vascular regulation therapy
 of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
of BEMER Liezl Naudé Advanced nurse specialist: wound management Advanced lower limb and wound management centre, Pretoria Heart 4 the Wounded 5-7 July Pretoria Introduction Lower limb wounds have always
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude
 Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Evaluating the use of a topical haemoglobin spray as adjunctive therapy in non-healing chronic wounds a pilot study Liezl Naude Abstract Wound Management Specialist Eloquent Health & Wellness Centre, Pretoria,
Venous. Arterial. Neuropathic (e.g. diabetic foot ulcer) Describe Wound Types & Stages of. Pressure Ulcers. Identify Phases of Healing & Wound Care
 A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
A dressing the situation at hand Describe Wound Types & Stages of Pressure Ulcers Identify Phases of Healing & Wound Care Goals Clarify Referral Protocol Lacerations- The goal is nearest to complete approximation
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Vacuumed Assisted Closure
 Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
SDMA Categorisation of Wound Care and Associated Products
 Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Larval Debridement Therapy Making healing possible
 Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Larval Debridement Therapy Making healing possible What is Larval Debridement Therapy (LDT)? The term Larval Debridement Therapy describes the use of maggots, precisely the larvae of the green bottle blowfly
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
easy made Triangle of Wound Assessment
 Triangle of Wound made easy Wounds Asia May 2015 www.woundsasia.com Introduction Wound assessment is essential in informing the selection of appropriate therapeutic strategies to achieve clinical goals,
Triangle of Wound made easy Wounds Asia May 2015 www.woundsasia.com Introduction Wound assessment is essential in informing the selection of appropriate therapeutic strategies to achieve clinical goals,
addressed to optimise wound healing.
 HOME CARE UNIT NO. 4 WOUND CARE Dr Low Lian Leng ABSTRACT Common chronic encountered by Family Physicians in the home care setting include pressure ulcers, diabetic foot ulcers, venous ulcers and arterial
HOME CARE UNIT NO. 4 WOUND CARE Dr Low Lian Leng ABSTRACT Common chronic encountered by Family Physicians in the home care setting include pressure ulcers, diabetic foot ulcers, venous ulcers and arterial
3M Tegaderm Matrix Matrix Dressing. Conquer Non-healing. Wounds
 Conquer Non-healing Wounds Chronic wounds Chronic wounds have been defined as those that fail to progress through a normal, orderly and timely sequence of repair. Or, wounds that pass through the repair
Conquer Non-healing Wounds Chronic wounds Chronic wounds have been defined as those that fail to progress through a normal, orderly and timely sequence of repair. Or, wounds that pass through the repair
BIS TIME management by medicinal larvae Dr. Wilhelm Jung
 Infoservice Larval Therapy up-to-date BIS TIME management Dr. Wilhelm Jung Making healing possible BIS TIME management Original publication: TIME management Pritchard D.I., Cerovsky V., Nigam Y., Pickles
Infoservice Larval Therapy up-to-date BIS TIME management Dr. Wilhelm Jung Making healing possible BIS TIME management Original publication: TIME management Pritchard D.I., Cerovsky V., Nigam Y., Pickles
Prevention and Management of Leg Ulcers
 EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
EWMA Educational Development Programme Curriculum Development Project Education Module: Prevention and Management of Leg Ulcers Latest revision: October 2015 ABOUT THE EWMA EDUCATIONAL DEVELOPMENT PROGRAMME
Management of Complex Wounds with Vacuum Assisted Closure
 Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Management of Complex Wounds with Vacuum Assisted Closure Wendy McInnes Vascular / Wound Nurse Practitioner The Queen Elizabeth Hospital, Adelaide, South Australia Treasurer ANZSVN wendy.mcinnes@health.sa.gov.au
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine
 Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
Novel Approaches for Accelerating Wound Healing Negative Pressure Wound Therapy in Accelerating Wound Healing Telemedicine Dr. Julian Vitse, Montellier University Hospital, France Negative Pressure Wound
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL. of the infection risk in chronic wound
 Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Supporting healthcare professionals in taking control of the infection risk with ACTICOAT Flex TAKE CONTROL of the infection risk in chronic wound Introduction The impact of infection on patients is well
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Understanding Debridement
 Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Understanding Debridement Figure 1. Wound Healing Process Wound Blood Clot Blood Blood Vessel Fat Tissue The wound in the skin exposes deep tissue layers to the air. Scab Scab Exudate Granulation Tissue
Education Module. Use of Conservative Sharp Wound Debridement to Debride Necrotic Tissue in Wounds
 British Columbia Provincial Nurses Skin and Wound Committee Education Module: Conservative Sharp Wound Debridement. Developed by the BC Provincial Nursing Skin and Wound Committee in collaboration with
British Columbia Provincial Nurses Skin and Wound Committee Education Module: Conservative Sharp Wound Debridement. Developed by the BC Provincial Nursing Skin and Wound Committee in collaboration with
Embrace the Call to Wound Prevention and Care
 CONCLUSION Embrace the Call to Wound Prevention and Care A challenging career Be part of an interprofessional team Help patients, families, communities Commit to lifelong learning To cure occasionally,
CONCLUSION Embrace the Call to Wound Prevention and Care A challenging career Be part of an interprofessional team Help patients, families, communities Commit to lifelong learning To cure occasionally,
Debridement within the context of the EWMA s debridement guidelines. Emil Schmidt WCNS SDHB - Otago
 Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
Debridement within the context of the EWMA s debridement guidelines Emil Schmidt WCNS SDHB - Otago EWMA Debridement Document Expert consensus document, 2013 Contents Mechanical debridement options Autolytic
Moisture Guide South West Regional Wound Care Program Last Updated March 27,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009)
 Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Guidelines for the Treatment of Pressure Ulcers (Adapted from EPUAP & NPUAP 2009) This guidance should be read in conjunction with your local dressing formulary and anti-biotic prescribing guidelines.
Date Issued Planned Review PGN No: Kevin Chapman Tissue Viability Modern Matron
 Tissue Viability Policy, Practice Guidance Note Wound Assessment V01 Date Issued Planned Review PGN No: Issue 1 July 2016 Issue 2 Sept 2017 July 2019 TV-PGN-04 Part of NTW(C)18 Tissue Viability Policy
Tissue Viability Policy, Practice Guidance Note Wound Assessment V01 Date Issued Planned Review PGN No: Issue 1 July 2016 Issue 2 Sept 2017 July 2019 TV-PGN-04 Part of NTW(C)18 Tissue Viability Policy
MANAGING THE BURN WOUND
 MANAGING THE BURN WOUND Robert H. Demling, M.D. Leslie DeSanti R.N., Brigham and Women s Hospital Burn Center Harvard Medical School Boston, MA TABLE OF CONTENTS Section I: Section II: Section III: Section
MANAGING THE BURN WOUND Robert H. Demling, M.D. Leslie DeSanti R.N., Brigham and Women s Hospital Burn Center Harvard Medical School Boston, MA TABLE OF CONTENTS Section I: Section II: Section III: Section
Workshop on Debridement
 MEDICINSK TEKNIK I SÅRDIAGNOSTIK OCH SÅRBEHANDLING Monday, 20 th of april 2015 Stockholm Sweden Workshop on Debridement Sources for best practice Reference documents available in several languages : WHY
MEDICINSK TEKNIK I SÅRDIAGNOSTIK OCH SÅRBEHANDLING Monday, 20 th of april 2015 Stockholm Sweden Workshop on Debridement Sources for best practice Reference documents available in several languages : WHY
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
ACOFP 55th Annual Convention & Scientific Seminars. New Physicians and Residents: Introduction to Wound Care. Katherine Lincoln, DO, FAAFP
 8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
8 ACOFP 55th Annual Convention & Scientific Seminars New Physicians and Residents: Introduction to Wound Care Katherine Lincoln, DO, FAAFP Introduction to Wound Care KATHERINE LINCOLN, DO, FAAFP ACOFP
