Does patient history and physical examination predict MRI proven cauda equina syndrome?
|
|
|
- Paula Marshall
- 5 years ago
- Views:
Transcription
1 Does patient history and physical examination predict MRI proven cauda equina syndrome? Authors Jeremy Fairbank¹, Robin Hashimoto², Andrew Dailey ³, Alpesh A Patel³, Joseph R Dettori² Institutions ¹Nuffield Orthopaedic Centre, Oxford, UK ² Spectrum Research Inc, Tacoma, WA, USA ³ University of Utah, Salt Lake City, UT, USA ABSTRACT Study design: Systematic review. Study rationale: While magnetic resonance imaging (MRI) is used as the gold standard for cauda equina syndrome (CES), many MRI scans obtained from patients presenting with signs and/ or symptoms of CES do not reveal concordant pathology. As a result, the role of the history and physical examination remains unclear when determining which patients require emergent MRI. or clinical question: Are there elements from the history or physical examination that are associated with CES as established by MRI? Methods: A systematic review of the literature was undertaken for articles published through April 13, PubMed, Cochrane, National Guideline Clearinghouse Databases, and bibliographies of key articles were searched. Two independent reviewers reviewed articles. and exclusion criteria were set and each article was subject to a predefined quality-rating scheme. Results: We identified four articles meeting our inclusion criteria. All studies evaluated patients with symptoms suggestive of CES and compared symptoms and/or signs with findings at MRI. The mean prevalence of CES as diagnosed by MRI ranged from 14% 48% of patients. No symptoms or signs reported by more than one showed high sensitivity and specificity, and all likelihood ratios were low. Symptoms included back/low back pain, bilateral sciatica, bladder retention, bladder incontinence, frequent urination, decreased urinary sensation, and bowel incontinence; signs included saddle numbness and reduced anal tone. Conclusions: There is low evidence that individual symptoms or signs from the patient history or clinical examination, respectively, can be used to diagnose CES. Additional prospective studies are needed to evaluate whether any single and/or combination of symptoms are associated with a positive diagnosis of CES. This systematic review was funded by AOSpine.
2 28 Systematic review Does patient history and physical examination predict (...) STUDY RATIONALE AND CONTEXT Cauda equina syndrome (CES) is often defined by a broad range of symptoms and physical examination findings: back pain, leg pain, weakness, numbness, and bowel or urinary changes. However, many of these symptoms may also be caused by medications, nonspinal pathology, or by spine diseases that can be treated nonemergently. Cauda equina syndrome is one of the most commonly litigated diagnoses with medicolegal concerns regarding the impact of a missed or delayed diagnosis. Given the lack of clearly defined symptoms and signs as well as the legal risks associated with perceived delays in diagnosis, magnetic resonance imaging (MRI) is frequently obtained in patients presenting with these symptoms. While MRI, coupled with patient history and examination, remains the gold standard, it comes at a high cost with many patients demonstrating no concordant pathology. Given the need to accurately diagnose CES while balancing the cost of diagnosis, the role of patient history and physical examination needs to be clarified. There is a problem of true diagnosis here in that CES is only really established when treatment has failed. At presentation with symptoms and signs of CES, not all subjects have CES (perhaps 40% in terms of MRI). At investigation (usually MR) a judgment has to be made if there is cauda equina decompression that might be relieved by surgery. Surgical success is if there are no residual symptoms, but there cannot be complete certainty that this would not have happened by natural resolution. Surgical failure is CES. We have chosen to use MR as the gold standard since it is at this stage that a surgical solution has to be planned and executed. CLINICAL QUESTION Are there elements of the patient history or physical examination that are associated with CES as established during imaging? METHODS Study design: Systematic review. Sampling: PubMed, Cochrane Collaboration Database, bibliographies of key articles. Dates searched: through April 13, criteria: (1) adults presenting with clinical features suggestive of CES; (2) studies evaluating elements from patient history (symptoms) and/or from the physical examination (signs); (3) imaging (MRI, CT, or myelography) or findings at surgery as the gold standard. criteria (Fig 1): (1) patients < 18 years old; (2) patients with trauma, inflammatory cause, spondylolisthesis, Paget disease, osteochondrosis, congenital malformation, visceral diseases, or cancer; (3) confirmed CES in all patients; (4) gold standard used is composite of surgery or imaging with index test; and (5) therapeutic studies. Elements from history and physical examination: Symptoms Back pain Leg pain/sciatica Neurological symptoms (weakness; bowel or bladder) Aggravating factors Alleviating factors Signs Neurological examination (motor or sensory) Reflexes Rectal tone Outcomes: Prevalence of CES according to MRI findings Summary of sensitivity, specificity, and likelihood ratios for symptoms and signs reported by more than one Analysis: Prevalence, sensitivities, specificities, and likelihood ratios were recorded or calculated from the available data. Overall strength of the evidence was assessed using GRADE criteria. Additional methodological and technical details are provided in the Web Appendix at
3 29 Fig 1 Results of literature search. RESULTS 1. Total citations (N= 79) 2. Title/abstract exclusion (n = 71) 5. Publications included (n = 4) 3. Retrieved for full-text evaluation (n = 8) 4. Excluded at full text review (n = 4) From 77 citations, 8 underwent full-text review. Four [1 4] met the inclusion criteria (Table 1): 1 prospective (LoE-III) [2] and 3 retrospective (LoE-IV) studies [1, 3, 4]. (See Table 2 of the Web Appendix). Patients with suspected CES underwent MRI (Table 1, Web appendix), mean prevalence CES: 14% 48% (Tables 3 4, Web Appendix) [1 4]. Symptoms (Table 3) Back pain and bowel incontinence [1 4] had high sensitivities, low specificities, and low LRs [1, 3, 4]. Bilateral sciatica had lower sensitivity, higher specificity, and low LRs [1 4] Bladder incontinence, bladder retention, decreased urinary sensation, and frequent urination had varying sensitivities and specificities and low LRs [1 4]. Signs (Table 4) Saddle numbness had varying sensitivities and specificities and low LRs [2, 3]. Reduced anal tone had low sensitivity, high specificity, and low LRs [1 4]. Additional symptoms and signs reported by one each are summarized in Tables 3 and 4 of the Web Appendix. CLINICAL GUIDELINES None found. Table 1 Patient and treatment characteristics of included studies investigating accuracy of elements of patient history or physical examination compared with imaging or findings at surgery. * Author Study design (LoE) Demographics Symptoms/ patient history Signs/physical examination Reference standard; criteria positive CES diagnosis Study objective; inclusion/exclusion Balasubramanian et al [1]; (2010) Domen et al [3], (2009) Retrospective N = 80 Male: NR Mean age: NR (range, y) (57% in 4th and 5th decades) Back pain: 90% (72/80) Unilateral leg pain: 75% (60/80) Bilateral leg pain: 11% (8/80) Bladder incontinence: 48% (33/69) Bladder retention: 18% (14/79) Bowel incontinence: 15% (12/79) Mean duration of symptoms: NR Saddle sensory deficit/ saddle anesthesia: 26% (20/77) Reduced anal tone/ lax anal sphincter: 9% (7/75) MRI Canal compromise > 75% To evaluate efficacy of clinical assessment in diagnosing CES All patients seen by on-call spine surgery team presenting with clinical features of CES (Jan Dec 2010)
4 30 Systematic review Does patient history and physical examination predict (...) Table 1 (cont) Patient and treatment characteristics of included studies investigating accuracy of elements of patient history or physical examination compared with imaging or findings at surgery. * Author Study design (LoE) Demographics Symptoms/ patient history Signs/physical examination Reference standard; criteria positive CES diagnosis Study objective; inclusion/exclusion Bell et al [2] (2007); Balasubramanian et al [1] (2010) Prospective N = 23 Male: 61% Mean age: 39 (range, 17 59) y Back pain: 100% (23/23) Sciatica: 74% (17/23) Unilateral sciatica: 57% (13/23) Bilateral sciatica: 17% (4/23) Urinary symptoms (any): 100% (23/23) Urinary incontinence: 26% (6/23) Painful urinary retention: 30% (7/23) Painless urinary retention: 4% (1/23) Decreased sensation of urination: 30% (7/23) Frequent urination: 30% (7/23) Erectile dysfunction: 0% males (0/14) Mean duration of back pain: 745 (range, ) d Mean duration of urinary symptoms: 4 (range, 1 24) d MRI Disc prolapse causing significant cauda equina/ thecal distortion To determine whether any single symptom can be used to accurately predict presence of CES on subsequent MRI All patients referred to one neurosurgical center from primary care with suspected diagnosis of CES Patients who admitting neurosurgical registrar was confident did not have signs or symptoms of CES; patients who had already received imaging Domen et al [3](2009); Bell et al [2], 2007 Retrospective N = 58 Male: NR Mean age: NR Low back pain <1 mo: 74% (43/58) Bilateral sciatica: 33% (19/58) Bladder incontinence: 40% (23/58) Bladder retention: 64% (37/58) Decreased sensation of urination: 36% (21/58) Frequent urination: 10% (6/58) Bowel incontinence: 16% (9/58) Mean duration of symptoms: NR Urinary retention > 500 ml: 21% (8/39 tested) Saddle anesthesia/ numbness: 36% (21/58) Decreased anal sphincter tone: 16% (9/58) Decreased anal sphincter reflex: 40% (23/58) Lasègé straight leg test positive: 48% (28/58) Loss of motor function in leg: 50% (29/58) Loss of motor function in foot raisers: 33% (19/58) Decreased ankle reflex: 29% (17/58) MRI All scans done on same 1.5-T clinical MRI scanner (Intera; Phillips, Best, the Netherlands) using following sequences (done according to in-house lumbar protocol): sagittal T1-weighted MRI (12 slides; SL 4.00 mm; TR 550 ms; TE 13 ms), sagittal T2-weighted MRI (12 slides; SL 4.0 mm; TR 3191 ms; TE 130 ms), axial driven-equilibrium (T2) MRI (50 slides; SL 2.0 mm; TR 700 ms; TE 1010 ms) and MR cauda equina myelography Presence of cauda equina compression To determine whether the presence or absence of CES can be accurately predicted by certain clinical characteristics in the hopes of avoiding unnecessary urgent MRI scans All patients who underwent urgent MRI imaging for suspected CES at hospital neurology department (Jan 2003 Dec 2007) Patients with pre-medical history of recent or extensive malignant disease; patients with metastatic disease as cause of CES
5 31 Table 1 (cont) Patient and treatment characteristics of included studies investigating accuracy of elements of patient history or physical examination compared with imaging or findings at surgery. * Author Study design (LoE) Demographics Symptoms/ patient history Signs/physical examination Reference standard; criteria positive CES diagnosis Study objective; inclusion/exclusion Rooney et al [4 ] (2009); Domen et al [3] (2009) Retrospective N = 98 Male: 27% (18/66) Mean age: 43 y Low back pain: 94% (58/62) Sciatica: 89% (49/55) Unilateral sciatica: 60% (33/55) Bilateral sciatica: 29% (16/55) Leg numbness: 83% (33/40) Unilateral leg numbness: 53% (21/40) Bilateral leg numbness: 30% (12/40) Bladder incontinence: 56% (27/48) Bladder retention: 43% (17/40) Decreased sensation of urination: 43% (18/42) Bowel incontinence: 8% (4/48) Bowel retention: 13% (5/40) Decreased fecal sensation: 5% (2/42) Mean duration of symptoms: NR Saddle numbness: 55% (34/66) Leg numbness: 80% (49/61) Loss of power (unilateral or bilateral): 59% (38/64) Unilateral loss of power: 33% (21/64) Bilateral loss of power: 19% (12/64) Loss of reflexes (unilateral or bilateral): 41% (26/64) Unilateral loss of reflexes: 22% (14/64) Bilateral loss of reflexes: 19% (12/64) Increase in reflexes (unilateral or bilateral): 14% (9/64) Unilateral increase in reflexes: 2% (1/64) Bilateral increase in reflexes: 13% (8/64) MRI Relevant abnormality on scan (details NR) To assess whether any simple clinical characteristics are able to distinguish patients with CES from those without All patients referred to neurosurgical department at hospital with symptoms suggestive enough of CES to warrant MRI (Mar Dec 2004) Readmissions of same patient; previous MRI scan in different hospital; on clinical reevaluation CES seemed unlikely; incomplete records (32 patients had incomplete records) * CES indicates cauda equina syndrome; NR, not reported; and MRI, magnetic resonance imaging. Complete records available for 66 of 98 patients, the remaining 22 were excluded; all data reported for n = 66 patients with complete records. ILLUSTRATIVE CASE A 37-year-old woman had acute onset of low back pain while lifting at work. During 4 days she experienced pain down her legs, bilateral foot weakness, and perineal numbness. She could no longer sense when her bladder was full and began to wear a diaper. On presentation, strength testing revealed plantar flexion, dorsiflexion, and extensor hallicus longus 0/5 on the right, dorsiflexion and hallucis longus (EHL) 4/5 and plantar flexion 5/5 on the left. She had saddle anesthesia, diminished rectal tone, and more than1000 cc of retained urine upon placing a urinary catheter. Fig 2 a Axial (left); b sagittal (right). T2 magnetic resonance imaging reveals a massive disc extrusion from the L4 5 level associated with signs and symptoms of cauda equina syndrome. a b Emergent MRI revealed a massive L4 5 disc herniation causing cauda equina compression (Fig 2). Despite the delay in referral, she was taken urgently to the operating room for laminectomy and disc excision. She made a full-motor recovery over 2 years but she still has sacral numbness and manually expresses her bladder, although she no longer needed a catheter.
6 32 Systematic review Does patient history and physical examination predict (...) DISCUSSION Limitations Small number of poor studies available (three studies are level IV; one level III). No indication in any whether the reference test (MRI) was interpreted in a manner that was blind to the results of the patient history and physical examination. None of the studies provided sufficient details for replication of both the tests and MRI. None of the symptoms or signs reported had a likelihood ratio with a magnitude that would suggest ruling in or out CES given the pretest probability of disease. The literature did not define objective, reliable clinical criteria for the diagnosis of CES. There are insufficient data in the literature to determine the relationship between signs and symptoms of CES and the timing or severity (ie, complete vs incomplete) of the disease. While MRI is considered the standard in the diagnosis of CES, the literature reveals a lack of an objective, reliable system of classifying MRI findings. Furthermore, the subjective MRI findings reported in the literature may not be specific to CES. Insufficient data is present in the literature to identify signs or symptoms that correlated with either negative or positive MRI studies. Prospective studies evaluating larger cohorts of patients are needed to more definitively determine whether any individual or combination of signs and/ or symptoms is associated with CES. Prospective studies should comprise objective, reliable definitions for CES, including timing and severity of disease, as well as a reliable classification of MRI findings. EVIDENCE SUMMARY Question 1: Are there elements of the patient history that are associated with cauda equina syndrome (CES) as established during imaging? Outcomes Strength of evidence Conclusions/comments Sensitivity, specificity, and likelihood ratio Very low Low Moderate High Further research is likely to have an important impact on our confidence in the estimate of effect and is likely to change the estimate. One prospective and three retrospective cohort studies were identified that compared symptoms as established during patient history taking to MRI findings regarding CES. All symptoms identified had low likelihood ratios. No studies evaluated a combination of symptoms. Question 2: Are there elements of the physical examination that are associated with CES as established during imaging? Outcomes Strength of evidence Conclusions/comments Sensitivity, specificity, and likelihood ratio Very low Low Moderate High One prospective and three retrospective cohort studies were found that compared signs as established during the physical examination to the CES diagnosis according to MRI. All symptoms identified had low likelihood ratios. Further research is likely to have an important impact on our confidence No studies evaluated a combination of signs. in the estimate of effect and is likely to change the estimate.
7 33 REFERENCES 1. Balasubramanian K, Kalsi P, Greenough CG, et al (2010) Reliability of clinical assessment in diagnosing cauda equina syndrome. Br J Neurosurg; 24(4): Bell DA, Collie D, Statham PF (2007) Cauda equina syndrome: what is the correlation between clinical assessment and MRI scanning? Br J Neurosurg; 21(2): Domen PM, Hofman PA, van Santbrink H, et al (2009) Predictive value of clinical characteristics in patients with suspected cauda equina syndrome. Eur J Neurol; 16(3): Rooney A, Statham PF, Stone J (2009) Cauda equina syndrome with normal MR imaging. J Neurol; 256(5): CES is a description of a neural deficit best to be avoided in the first place as it describes an ongoing neurological deficit. CES can be defined as the sudden loss of function of the lumbar and lumbosacral plexus below the conus medullaris due to a number of conditions, such as massive disc herniation, tumor, trauma, and by other forms of neural canal compromise. The traditional findings of acute loss of bowel and bladder control function, sexual dysfunction, lower extremity weakness, and numbness in the perianal region and lower extremities describe an active process of neurological damage underway for which recovery is unpredictable. Recognition of an immanent CES is clearly preferable to waiting for actual manifestations of CES to occur. CES remains a major challenge regarding best pathway to timely diagnosis due to a plethora of presentations and large number of confounding factors. Lumbar MRI remains the preferred modality to identify neural space compromise. In the era of attempting to develop pathways for use of lumbar neural imaging for patients with low back pain based on their clinical presentations, the possibility of missing an evolving CES remains a real challenge. A review of the physical examination findings reported in this systematic review by Fairbanks et al clearly show the main constant of physical findings with patients who ended up experiencing CES was low back pain. A smaller number of patients presented with bilateral leg pain. All other physical examination findings pretty much described an ongoing evolving CES the condition all agreed that should be avoided in the first place. The authors clearly found that there was a dearth of reliable patient complaints or physical examination findings in the literature to use as a red flag in the development of pathways for low back pain. There also appears to be poor correlation of the amount of canal compromise and the evolution as well as severity of neurological deficits. In conclusion, we can all agree on some points: EDITORIAL PERSPECTIVE The subject of cauda equina syndrome (CES) continues to provide ample controversy to all involved in care of spine patients, scientific, and education. This includes the responses of our reviewers who were split about the best way to approach the subject and then interpret the available literature and what conclusions to draw from the findings. All agree on the following: CES as a worst-case scenario for a number of conditions, such as disc herniation, clearly begs for further prospective investigation with quality-data collection and analysis. The neurophysiological basis of CES would benefit from further basic science. Low back pain continues to present a major challenge to simplified and care pathways due to its highly nonspecific nature. EBSJ thanks Fairbank and colleagues for tackling this controversial subject and providing a welcome foundation for further investigation.
Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH
 Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...)
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review (...) 59 59 66 Cervical artificial disc replacement versus fusion in the cervical spine:
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
The ABC s of LUMBAR SPINE DISEASE
 The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
Nursing review section of Surgical Neurology International: Part 1 lumbar disc disease
 SNI: Neurosurgical Nursing OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article Nursing review
SNI: Neurosurgical Nursing OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: Nancy E. Epstein, MD Winthrop Hospital, Mineola, NY, USA Review Article Nursing review
Incomplete cauda equina syndrome in adult monozygotic twins
 Incomplete cauda equina syndrome in adult monozygotic twins J. Mohar, R. Kramar, N. Hero, R. J. Cirman Department of Spine Surgery and Paediatric Orthopaedics, Orthopaedic Hospital Valdoltra, Ankaran,
Incomplete cauda equina syndrome in adult monozygotic twins J. Mohar, R. Kramar, N. Hero, R. J. Cirman Department of Spine Surgery and Paediatric Orthopaedics, Orthopaedic Hospital Valdoltra, Ankaran,
Case Studies, Impairment of the Spine in Washington State
 Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
The ABC s of LUMBAR SPINE DISEASE
 The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery URMC Neurosurgery APP s Objectives Identify the most common pathology that leads to spine
The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery URMC Neurosurgery APP s Objectives Identify the most common pathology that leads to spine
Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center
 Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center 1. The less specific the patient is about symptoms and pain, the less likely a specific diagnosis will be made and the less likely the patient
Gary Rea MD PhD Medical Director OSU Comprehensive Spine Center 1. The less specific the patient is about symptoms and pain, the less likely a specific diagnosis will be made and the less likely the patient
ishing you and your families a safe, peaceful and joyous holiday season From The Editor From The TSG Family In This Issue...
 From The Editor In this issue of the TSG Newsletter, we present Failure to Diagnose Cauda Equina Syndrome. Emergency, urgent care and primary care physicians see so many patients with back pain complaints
From The Editor In this issue of the TSG Newsletter, we present Failure to Diagnose Cauda Equina Syndrome. Emergency, urgent care and primary care physicians see so many patients with back pain complaints
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Predictors of outcome. with cauda equina syndrome
 Eur Spine J (1999) 8 :317 322 Springer-Verlag 1999 ORIGINAL ARTICLE J. G. Kennedy K. E. Soffe A. McGrath M. M. Stephens M. G. Walsh F. McManus Predictors of outcome in cauda equina syndrome Received: 18
Eur Spine J (1999) 8 :317 322 Springer-Verlag 1999 ORIGINAL ARTICLE J. G. Kennedy K. E. Soffe A. McGrath M. M. Stephens M. G. Walsh F. McManus Predictors of outcome in cauda equina syndrome Received: 18
Cauda equina syndrome with normal MR imaging
 J Neurol (2009) 256:721 725 DOI 10.1007/s00415-009-5003-z ORIGINAL COMMUNICATION Cauda equina syndrome with normal MR imaging Alasdair Rooney Æ Patrick F. Statham Æ Jon Stone Received: 1 October 2008 /
J Neurol (2009) 256:721 725 DOI 10.1007/s00415-009-5003-z ORIGINAL COMMUNICATION Cauda equina syndrome with normal MR imaging Alasdair Rooney Æ Patrick F. Statham Æ Jon Stone Received: 1 October 2008 /
Anuj D. Bharuka*, Rajendra Phunde, Hiren B. Patel
 International Journal of Research in Orthopaedics Bharuka AD et al. Int J Res Orthop. 17 Sep;3(5):998-13 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/1.183/issn.55-51.intjresorthop1731
International Journal of Research in Orthopaedics Bharuka AD et al. Int J Res Orthop. 17 Sep;3(5):998-13 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/1.183/issn.55-51.intjresorthop1731
The Beacon. Cauda Equina Syndrome: A Medical/Surgical Emergency. In This Issue. Case #1
 A Medical Mutual Insurance Company of Maine Publication The Beacon Second Quarter 2015 Cauda Equina Syndrome: A Medical/Surgical Emergency Cauda equina syndrome (CES) is a rare syndrome that has been described
A Medical Mutual Insurance Company of Maine Publication The Beacon Second Quarter 2015 Cauda Equina Syndrome: A Medical/Surgical Emergency Cauda equina syndrome (CES) is a rare syndrome that has been described
Wendy Field Advanced Physiotherapy Practitioner June 2018
 Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
LOW BACK PAIN EPIDEMIOLOGY:
 LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
LOW BACK PAIN OBJECTIVES: Discuss epidemiology of low back pain Summarize diagnosis/ special tests Review Red Flags Discuss treatment and referral guidelines Discuss light duty guidelines EPIDEMIOLOGY:
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Objectives. Identify and differentiate appropriate surgical cases. Good Surgical Outcomes
 ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
ECHO February 5 th, 2015 Surgical Selection for Low Back Pain Objectives Identify and differentiate appropriate surgical cases Disclosures Medical director for UHN Rehabilitations Solution Back and Neck
A Syndrome (Pattern) Approach to Low Back Pain. History
 A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
A Syndrome (Pattern) Approach to Low Back Pain Hamilton Hall MD FRCSC Professor, Department of Surgery, University of Toronto Medical Director, CBI Health Group Executive Director, Canadian Spine Society
Spinal Cord Compression Diagnosis and Management. Information for Shared Care Centres and Community Staff
 Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
Reference: CG1412 Written by: Dr Daniel Yeomanson Peer reviewer Dr Jeanette Payne Approved: August 2016 Approved by D&TC: 10 th June 2016 Review Due: August 2019 Intended Audience This document contains
CLINICAL GUIDELINES. Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision
 CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
CLINICAL GUIDELINES Primary Care Guideline Summary Lumbar Spine Thomas J. Gilbert M.D., M.P.P. 3/17/15 revision TRIAGE At the initial visit, a focused history and physical examination is performed to assign
Suspecting Tumors, or Could it be cancer?
 Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
Suspecting Tumors, or Could it be cancer? Donna E. Reece, M.D. Princess Margaret Cancer Centre University Health Network Toronto, ON CANADA 07 February 2018 Background Low back pain is common However,
Cox Technic Case Report #124 published at ( sent October 2013 ) 1
 Cox Technic Case Report #124 published at www.coxtechnic.com ( sent October 2013 ) 1 5 th Lumbar Disc Herniation with Spondylolisthesis Treated with Cox Technic Flexion Distraction by Travis Cross BS,
Cox Technic Case Report #124 published at www.coxtechnic.com ( sent October 2013 ) 1 5 th Lumbar Disc Herniation with Spondylolisthesis Treated with Cox Technic Flexion Distraction by Travis Cross BS,
JOSS ABSTRACT INTRODUCTION /jp-journals
 Giulio Anichini et al ORIGINAL ARTICLE 10.5005/jp-journals-10039-1150 Cauda Equina Syndrome Assessment, Diagnosis, and Management: Results from a Neurosurgical Unit from 1-year Retrospective Series Is
Giulio Anichini et al ORIGINAL ARTICLE 10.5005/jp-journals-10039-1150 Cauda Equina Syndrome Assessment, Diagnosis, and Management: Results from a Neurosurgical Unit from 1-year Retrospective Series Is
Malignant Spinal cord Compression. Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania
 Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
Malignant Spinal cord Compression Dr. Thiru Thirukkumaran Palliative Care Services - Northwest Tasmania Background Statistics of SCC -1 Incidence of SCC Vertebral body metastases 85 % Para-vertebral (Lymphoma)
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Cauda Equina Syndrome; first contact to MRI
 Multi Shades of Grey Cauda Equina Syndrome Authors: Laura Finucane, Sue Greenhalgh, Chris Mercer Cauda Equina Syndrome; first contact to MRI Rare early diagnosis critical Clinical diagnosis confirmed with
Multi Shades of Grey Cauda Equina Syndrome Authors: Laura Finucane, Sue Greenhalgh, Chris Mercer Cauda Equina Syndrome; first contact to MRI Rare early diagnosis critical Clinical diagnosis confirmed with
Back Pain Policies Summary
 Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Cauda equina syndrome: evaluation of the clinical outcome
 European Review for Medical and Pharmacological Sciences Cauda equina syndrome: evaluation of the clinical outcome 2014; 18: 1098-1105 F.C. TAMBURRELLI, M. GENITIEMPO, M. BOCHICCHIO, L. DONISI 1, C. RATTO
European Review for Medical and Pharmacological Sciences Cauda equina syndrome: evaluation of the clinical outcome 2014; 18: 1098-1105 F.C. TAMBURRELLI, M. GENITIEMPO, M. BOCHICCHIO, L. DONISI 1, C. RATTO
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Back pain and bladder problems
 Back pain and bladder problems Search Learn the causes and symptoms of chronic back pain, as well as safe techniques that provide back pain relief better than prescriptions drugs. If back pain is reducing
Back pain and bladder problems Search Learn the causes and symptoms of chronic back pain, as well as safe techniques that provide back pain relief better than prescriptions drugs. If back pain is reducing
Lumbar disc prolapse. Done by : Areej Al-Hadidi
 Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients
 Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Numb bum means cauda equina Per rectal examination is indicated to assess anal tone
 SPINE Age and occupation Pain: Where: Low back or leg Which is worse? Where about in the leg? Describe the radiation How long? More than 6 wks need warrant evaluation How the pain is now compared to the
SPINE Age and occupation Pain: Where: Low back or leg Which is worse? Where about in the leg? Describe the radiation How long? More than 6 wks need warrant evaluation How the pain is now compared to the
Spectrum of magnetic resonance imaging findings in chronic low back pain
 Original article: Spectrum of magnetic resonance imaging findings in chronic low back pain Dr Sanjeev Sharma (1), Dr Monika Sharma (2), DR Bhardwaj (3), MD; Dr Asha Negi, (4) Department of Radiodiagnosis,
Original article: Spectrum of magnetic resonance imaging findings in chronic low back pain Dr Sanjeev Sharma (1), Dr Monika Sharma (2), DR Bhardwaj (3), MD; Dr Asha Negi, (4) Department of Radiodiagnosis,
Speaker: Dr Gautam (Vini) Khurana MBBS (Syd, Hons), BScMed (Syd, Medal), PhD (Mayo Clinic), FRACS
 A Pain in the Back GPCE Workshop Sydney Olympic Park May 22-24, 2015 Speaker: Dr Gautam (Vini) Khurana MBBS (Syd, Hons), BScMed (Syd, Medal), PhD (Mayo Clinic), FRACS www.cnsneurosurgery.com.au VMO Neurosurgeon
A Pain in the Back GPCE Workshop Sydney Olympic Park May 22-24, 2015 Speaker: Dr Gautam (Vini) Khurana MBBS (Syd, Hons), BScMed (Syd, Medal), PhD (Mayo Clinic), FRACS www.cnsneurosurgery.com.au VMO Neurosurgeon
Cauda Equina Syndrome: presentation, outcome, and predictors with focus on micturition, defecation, and sexual dysfunction
 Eur Spine J (2017) 26:894 904 DOI 10.1007/s00586-017-4943-8 ORIGINAL ARTICLE Cauda Equina Syndrome: presentation, outcome, and predictors with focus on micturition, defecation, and sexual dysfunction N.
Eur Spine J (2017) 26:894 904 DOI 10.1007/s00586-017-4943-8 ORIGINAL ARTICLE Cauda Equina Syndrome: presentation, outcome, and predictors with focus on micturition, defecation, and sexual dysfunction N.
Natural Evolution of Lumbar Spinal Stenosis
 Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Primary care referral criteria for musculoskeletal MRI scans
 Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
Appendix 1 Primary care referral criteria for musculoskeletal MRI scans Accepted Criteria for Direct Access MRI Body Part Symptoms Imaging indicated Lumbar Spine Low Back Pain with adverse symptoms or
Posterior decompression via total laminectomy and
 CASE REPORT J Neurosurg Spine 27:352 356, 2017 Anterior lumbar discectomy and fusion for acute cauda equina syndrome caused by recurrent disc prolapse: report of 3 cases Kimberly-Anne Tan, MBBS, 1,2 Mathew
CASE REPORT J Neurosurg Spine 27:352 356, 2017 Anterior lumbar discectomy and fusion for acute cauda equina syndrome caused by recurrent disc prolapse: report of 3 cases Kimberly-Anne Tan, MBBS, 1,2 Mathew
Risk factors for development of cervical spondylotic myelopathy: results of a systematic review
 Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
Systematic review Risk factors for development of cervical spondylotic myelopathy 35 35 42 Risk factors for development of cervical spondylotic myelopathy: results of a systematic review Authors Anoushka
AMA Guides 4 th Edition: Sample Case Review
 AMA Guides 4 th Edition: Sample Case Review CASE #1 Ms. Parker is a 26 year old woman who sustained a fracture of the tuft of the distal phalynx of the right little finger, which was treated with a splint.
AMA Guides 4 th Edition: Sample Case Review CASE #1 Ms. Parker is a 26 year old woman who sustained a fracture of the tuft of the distal phalynx of the right little finger, which was treated with a splint.
Cox Technic Case Report #169 published at (sent 5/9/17) 1
 Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Cox Technic Case Report #169 published at www.coxtechnic.com (sent 5/9/17) 1 Management of Lumbar Radiculopathy Associated with an Extruded L4 L5 disc and concurrent L5 S1 Spondylolytic Spondylolisthesis
Chapter 35 Back Pain. Episode overview: Wisecracks: Crack Cast Show Notes Back Pain July 2016
 Chapter 35 Back Pain Episode overview: 1) List 10 historical red flags for back pain 2) List 6 Emergent Diagnosis for back pain Wisecracks: 1) Describe the most common sites of disc protrusion with their
Chapter 35 Back Pain Episode overview: 1) List 10 historical red flags for back pain 2) List 6 Emergent Diagnosis for back pain Wisecracks: 1) Describe the most common sites of disc protrusion with their
Spinal Trauma. General Rehabilitation of Patient with Spinal Trauma. Common Spinal Injuries. Important Anatomical Structures at each Vertebral Level
 Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Accepted Manuscript. Running title: Prognosis of Cauda Equina Syndrome. Authors:
 Accepted Manuscript Title: Prognosis of Cauda Equina Syndrome Caused by Herniated Disc after Lumbar Disk Surgery in Patients Referring to Al-Zahra Hospital of Isfahan from 2013 to 2015 Running title: Prognosis
Accepted Manuscript Title: Prognosis of Cauda Equina Syndrome Caused by Herniated Disc after Lumbar Disk Surgery in Patients Referring to Al-Zahra Hospital of Isfahan from 2013 to 2015 Running title: Prognosis
Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty
 35 35 43 Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty Authors Josh E Schroeder¹, Erika Ecker², Andrea C Skelly², Leon Kaplan¹ Institutions ¹ Orthopedic
35 35 43 Cement augmentation in spinal tumors: a systematic review comparing vertebroplasty and kyphoplasty Authors Josh E Schroeder¹, Erika Ecker², Andrea C Skelly², Leon Kaplan¹ Institutions ¹ Orthopedic
LOTHIAN LUMBAR SPINE PATHWAYS
 LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
LOTHIAN LUMBAR SPINE PATHWAYS Patient Completes STarT Back form Assess patient and screen for Red Flags. If present refer to Appendix 1 Establish if Neurogenic. If so refer to Appendix 2 Children under
Suspected spinal cord compression form
 Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
Suspected spinal cord compression form Enter this form into the notes at the appropriate date in the Progress / Evaluation sheets. Please copy this form to Lisa Lewis, Medical PA (ext 4551), for audit
Central Cord Syndrome: Does early surgical intervention improve neurological outcome
 Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Herniated Disk in the Lower Back
 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Spinal Stenosis Surgical
 Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery
 The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery SPINE Volume 35, Number 17, pp E849 E854 2010, Lippincott Williams & Wilkins Chun-Hao
The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery SPINE Volume 35, Number 17, pp E849 E854 2010, Lippincott Williams & Wilkins Chun-Hao
Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers
 In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
In Partnership with Regional Back Pain and Radicular Pain Pathway Frequently asked Questions and Answers Moving BACK to health Don t let your back pain get the better of you! The Regional Back Pain and
Changes in a Lumbar Disc Extrusion After Cox Technic Flexion Distraction Therapy in a 44 year old Office Worker. Submitted by
 Changes in a Lumbar Disc Extrusion After Cox Technic Flexion Distraction Therapy in a 44 year old Office Worker History Submitted by Dr Joel Dixon B.App.Sc (Chiropractic) J.P. Melbourne Spine Clinic Melbourne,
Changes in a Lumbar Disc Extrusion After Cox Technic Flexion Distraction Therapy in a 44 year old Office Worker History Submitted by Dr Joel Dixon B.App.Sc (Chiropractic) J.P. Melbourne Spine Clinic Melbourne,
Paul Allan Regional Clinical Lead - South. Lumbar Spine. Assessment & Differential Diagnosis
 Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
A Surgeon s Perspective for the Primary Care Physician Stephen Curtin M.D. Tucson Orthopeadic Institute
 A Surgeon s Perspective for the Primary Care Physician Stephen Curtin M.D. Tucson Orthopeadic Institute 26th Annual Southwestern Conference on Medicine AXIAL MUSCULO- SKELETAL PACK PAIN: Common Self-limited
A Surgeon s Perspective for the Primary Care Physician Stephen Curtin M.D. Tucson Orthopeadic Institute 26th Annual Southwestern Conference on Medicine AXIAL MUSCULO- SKELETAL PACK PAIN: Common Self-limited
Chiropractic Health Plan - Diagnosis of Low Back Pain
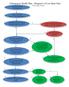 Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Chiropractic Health Plan - Diagnosis of Low Back Pain 1 Adult Patient with ot for major Trauma Low back pain 2 Intake Evaluation (Inset 1) Recommendation 1 3 Potentially Serious Condition Strongly Suspected
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review comparing multilevel versus single-level surgery
 Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
Systematic review Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review ( ) 19 19 30 Cervical artificial disc replacement versus fusion in the cervical spine: a
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society
 Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
Diagnosis and Treatment of Low Back Pain: A Joint Clinical Practice Guideline from the American College of Physicians and the American Pain Society Annals of Internal Medicine October 2007 Volume 147,
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R
 The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R 2011 MFMER slide-1 Disclosures None 2011 MFMER slide-2 Learning Objectives Review indications for obtaining imaging studies
The Complex/Challenging Spine Patient Steve Wisniewski, M.D. Department of PM&R 2011 MFMER slide-1 Disclosures None 2011 MFMER slide-2 Learning Objectives Review indications for obtaining imaging studies
3/3/2016. International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI)
 International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI) American Spinal Injury Association International Spinal Cord Society Presented by Adam Stein, MD Chairman and Professor
International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI) American Spinal Injury Association International Spinal Cord Society Presented by Adam Stein, MD Chairman and Professor
Spine injuries Which cases should have early surgery? And which should NOT?
 Spine injuries Which cases should have early surgery? And which should NOT? Tolga Aydoğ, MD, PhD Acıbadem Fulya Hospital Acıbadem Sports Acıbadem Mehmet Ali Aydınlar University Eczacıbaşı Sports Club Spine
Spine injuries Which cases should have early surgery? And which should NOT? Tolga Aydoğ, MD, PhD Acıbadem Fulya Hospital Acıbadem Sports Acıbadem Mehmet Ali Aydınlar University Eczacıbaşı Sports Club Spine
Acute spinal subdural hematoma complicating lumbar decompressive surgery
 Case report Acute spinal subdural hematoma complicating lumbar decompressive surgery 57 57 62 Acute spinal subdural hematoma complicating lumbar decompressive surgery Authors Institution Kok Chun Chang,
Case report Acute spinal subdural hematoma complicating lumbar decompressive surgery 57 57 62 Acute spinal subdural hematoma complicating lumbar decompressive surgery Authors Institution Kok Chun Chang,
Recognition & Treatment of Malignant Spinal Cord Compression Study Day
 Recognition & Treatment of Malignant Spinal Cord Compression Study Day 16 th October 2014 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk
Recognition & Treatment of Malignant Spinal Cord Compression Study Day 16 th October 2014 Dr Bernie Foran Consultant Clinical Oncologist & Honorary Senior Lecturer Weston Park Hospital Outline of Talk
High Yield Neurological Examination
 High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
High Yield Neurological Examination Vanja Douglas, MD Sara & Evan Williams Foundation Endowed Neurohospitalist Chair Director, Neurohospitalist Division Associate Professor of Clinical Neurology UCSF Department
RED AND AMBER FLAG GUIDANCE ORTHOPAEDIC CONDITIONS
 RED AND AMBER FLAG GUIDANCE ORTHOPAEDIC CONDITIONS Distribution list: Clinical Commissioning Groups / All Worcestershire GP practices; Musculoskeletal Integrated Clinical and Assessment Services; Commissioning
RED AND AMBER FLAG GUIDANCE ORTHOPAEDIC CONDITIONS Distribution list: Clinical Commissioning Groups / All Worcestershire GP practices; Musculoskeletal Integrated Clinical and Assessment Services; Commissioning
Changes in a Lumbar Disc Extrusion After Cox Technic Flexion Distraction Therapy in a 44 year old Office Worker: Pre and Post MRI Images
 Cox Technic Case Report #170 published at www.coxtechnic.com (sent 6/14/17) 1 Changes in a Lumbar Disc Extrusion After Cox Technic Flexion Distraction Therapy in a 44 year old Office Worker: Pre and Post
Cox Technic Case Report #170 published at www.coxtechnic.com (sent 6/14/17) 1 Changes in a Lumbar Disc Extrusion After Cox Technic Flexion Distraction Therapy in a 44 year old Office Worker: Pre and Post
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto
 Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Neck Pain: Help! Eric M. Massicotte, MD, MSc, MBA, FRCSC Associate Professor University of Toronto Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied,
Incidental Findings on Magnetic Resonance Imaging of the Spine in the Asymptomatic Pediatric Population: A Systematic Review
 Systematic Review 95 Incidental Findings on Magnetic Resonance Imaging of the Spine in the Asymptomatic Pediatric Population: A Systematic Review Uma Ramadorai 1 Justin Hire 1 John G. DeVine 2 Erika D.
Systematic Review 95 Incidental Findings on Magnetic Resonance Imaging of the Spine in the Asymptomatic Pediatric Population: A Systematic Review Uma Ramadorai 1 Justin Hire 1 John G. DeVine 2 Erika D.
Acute spinal cord injury
 Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Acute spinal cord injury Thakul Oearsakul Songklanagarind hospital Hat Yai Songkhla Introduction New SCI 10000-12000 cases Approximately 4.0-5.3 per 100000 population Common causes of traumatic SCI :Motor
Objectives. Emergency Department: Rapid Fire Diagnosis 10/4/16. Why emergency medicine is unique. Approach to the emergent patient
 Emergency Department: Rapid Fire Diagnosis Julie Beard DO St. Luke s Hospital Emergency Department October 4 th, 2016 Objectives Why emergency medicine is unique Approach to the emergent patient Discuss
Emergency Department: Rapid Fire Diagnosis Julie Beard DO St. Luke s Hospital Emergency Department October 4 th, 2016 Objectives Why emergency medicine is unique Approach to the emergent patient Discuss
Misdiagnosis in cervical spondylosis myelopathy.
 Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
Journal of the International Society of Head and Neck Trauma (ISHANT) Case report Misdiagnosis in cervical spondylosis myelopathy. Dr. Reinel A. Junco Martin. Neurosurgeon. Assistant professor Miguel Enriquez
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Schwannoma of T12 vertebra: case report and review of literature
 Sarcoma (2000) 4, 185± 190 CASE REPORT Schwannoma of T12 vertebra: case report and review of literature P. RAMASAMY, I. SHACKLEFORD & M. AL JAFARI Warrington General Hospital,WarringtonWA5 1QG, UK Abstract
Sarcoma (2000) 4, 185± 190 CASE REPORT Schwannoma of T12 vertebra: case report and review of literature P. RAMASAMY, I. SHACKLEFORD & M. AL JAFARI Warrington General Hospital,WarringtonWA5 1QG, UK Abstract
Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center
 Oh My Aching Back! Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center Epidemiology 90% of episodes of LBP resolves
Oh My Aching Back! Francine M. Pulver, MD, Clinical Assistant Professor Department of Physical Medicine & Rehabilitation Ohio State University Medical Center Epidemiology 90% of episodes of LBP resolves
Cauda equina syndrome (CES) develops as a result of
 SPINE Volume 39, Number 7, pp 596-602 2014, Lippincott Williams & Wilkins DIAGNOSTICS Assessment of Cauda Equina Syndrome Progression Pattern to Improve Diagnosis Jing-Chuan Sun, PhD, * Tao Xu, PhD, *
SPINE Volume 39, Number 7, pp 596-602 2014, Lippincott Williams & Wilkins DIAGNOSTICS Assessment of Cauda Equina Syndrome Progression Pattern to Improve Diagnosis Jing-Chuan Sun, PhD, * Tao Xu, PhD, *
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 73/09
 WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 73/09 BEFORE: N. Jugnundan: Vice-Chair HEARING: January 12, 2009 at Toronto Oral DATE OF DECISION: January 20, 2009 NEUTRAL CITATION: 2009 ONWSIAT
WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 73/09 BEFORE: N. Jugnundan: Vice-Chair HEARING: January 12, 2009 at Toronto Oral DATE OF DECISION: January 20, 2009 NEUTRAL CITATION: 2009 ONWSIAT
Low Back Pain Optimal Management in General Practice
 Low Back Pain Optimal Management in General Practice Dr Neil Hearnden Musculoskeletal Physician M.B. B.S. FRACGP. Grad Dip Musculoskeletal.Med. (Otago) MAFMM Arana Hills Medical Centre Brisbane Outcome
Low Back Pain Optimal Management in General Practice Dr Neil Hearnden Musculoskeletal Physician M.B. B.S. FRACGP. Grad Dip Musculoskeletal.Med. (Otago) MAFMM Arana Hills Medical Centre Brisbane Outcome
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Peggers Super Summaries: The Aging Spine
 Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
THE COMPRESSED NERVE. Timothy Jones PhD FRCS(SN) Consultant Neurosurgeon
 THE COMPRESSED NERVE Timothy Jones PhD FRCS(SN) Consultant Neurosurgeon MY BACKGROUND Consultant Neurosurgeon at St George s Hospital Trained in the region Subspecialty interest in neuro-oncology & trigeminal
THE COMPRESSED NERVE Timothy Jones PhD FRCS(SN) Consultant Neurosurgeon MY BACKGROUND Consultant Neurosurgeon at St George s Hospital Trained in the region Subspecialty interest in neuro-oncology & trigeminal
Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018
 Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018 Disclosures Neither I nor any family members have financial disclosures Special thanks
Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018 Disclosures Neither I nor any family members have financial disclosures Special thanks
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc. Copyright 2014, 2011, 2006 by Saunders, an imprint of Elsevier, Inc.
 Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
DISORDERS OF THE SPINE TREATING PHYSICIAN DATA SHEET
 DISORDERS OF THE SPINE TREATING PHYSICIAN DATA SHEET Short form FOR REPRESENTATIVE USE ONLY REPRESENTATIVE S NAME AND ADDRESS REPRESENTATIVE S TELEPHONE REPRESENTATIVE S EMAIL PHYSICIAN S NAME AND ADDRESS
DISORDERS OF THE SPINE TREATING PHYSICIAN DATA SHEET Short form FOR REPRESENTATIVE USE ONLY REPRESENTATIVE S NAME AND ADDRESS REPRESENTATIVE S TELEPHONE REPRESENTATIVE S EMAIL PHYSICIAN S NAME AND ADDRESS
Hailee Gibson, CCPA Neurosurgery Physician Assistant. Windsor Neurosurgery & Spine Associates. Windsor Regional Hospital Ouellette Campus
 Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Degenerative Spinal Disorders. Gábor Nagy MD PhD Zoltán Papp MD
 Degenerative Spinal Disorders Gábor Nagy MD PhD Zoltán Papp MD Neurosurgery Surgical treatment of diseases of central and peripheral nervous system Surgery of nerves (brain, spine, peripheral nerves) Surgery
Degenerative Spinal Disorders Gábor Nagy MD PhD Zoltán Papp MD Neurosurgery Surgical treatment of diseases of central and peripheral nervous system Surgery of nerves (brain, spine, peripheral nerves) Surgery
