Posterior decompression via total laminectomy and
|
|
|
- Jeffery Bridges
- 5 years ago
- Views:
Transcription
1 CASE REPORT J Neurosurg Spine 27: , 2017 Anterior lumbar discectomy and fusion for acute cauda equina syndrome caused by recurrent disc prolapse: report of 3 cases Kimberly-Anne Tan, MBBS, 1,2 Mathew D. Sewell, FRCS, 1 Yma Markmann, MD, 1 Andrew J. Clarke, FRCS, 1 Oliver M. Stokes, FRCS, 1 and Daniel Chan, FRCS 1 1 Exeter Spine Unit, Princess Elizabeth Orthopaedic Centre, Royal Devon and Exeter NHS Foundation Trust, Exeter, United Kingdom; and 2 University of New South Wales, Faculty of Medicine, Sydney, New South Wales, Australia There is a lack of information and consensus regarding the optimal treatment for recurrent disc herniation previously treated by posterior discectomy, and no reports have described an anterior approach for recurrent disc herniation causing cauda equina syndrome (CES). Revision posterior decompression, irrespective of the presence of CES, has been reported to be associated with significantly higher rates of dural tears, hematomas, and iatrogenic nerve root damage. The authors describe treatment and outcomes in 3 consecutive cases of patients who underwent anterior lumbar discectomy and fusion (ALDF) for CES caused by recurrent disc herniations that had been previously treated with posterior discectomy. All 3 patients were operated on within 12 hours of presentation and were treated with an anterior retroperitoneal lumbar approach. Follow-up ranged from 12 to 24 months. Complete retrieval of herniated disc material was achieved without encountering significant epidural scar tissue in all 3 cases. No perioperative infection or neurological injury occurred, and all 3 patients had neurological recovery with restoration of bladder and bowel function and improvement in back and leg pain. ALDF is one option to treat CES caused by recurrent lumbar disc prolapse previously treated with posterior discectomy. The main advantage is that it avoids dissection around epidural scar tissue, but the procedure is associated with other risks and further evaluation of its safety in larger series is required. KEY WORDS anterior lumbar discectomy and fusion; cauda equina syndrome; recurrent disc herniation Posterior decompression via total laminectomy and discectomy is the most commonly performed surgical procedure for the treatment of acute cauda equina syndrome (CES) caused by a canal-filling disc. There is no consensus and a lack of information to advise on the management of acute CES caused by a recurrent disc prolapse as the condition is rare. Irrespective of whether CES is present, the practice for many surgeons is posterior discectomy for the primary disc herniation, revision posterior discectomy for a recurrence, and a subsequent posterior discectomy and fusion if a second recurrence occurs. However, the addition of fusion is controversial and not always necessary. Revision posterior decompression is associated with a significantly higher rate of dural tear, hematoma, and iatrogenic nerve root damage due to the presence of epidural fibrosis. 11 An anterior discectomy, in theory, would lessen these potential risks because it would avoid the epidural scar tissue within the canal; however, it would present the surgeon with a different set of risks, particularly visceral and vascular injury. The rationale for fusion in the revision discectomy setting is to treat postdiscectomy back pain, address segmental instability (which may be caused by extensive posterior bone resection required for safe access to the disc), and enable complete disc removal to eliminate the risk of future ABBREVIATIONS ALDF = anterior lumbar discectomy and fusion; CES = cauda equina syndrome; PLL = posterior longitudinal ligament. ACCOMPANYING EDITORIAL See pp DOI: / SPINE1721. SUBMITTED March 25, ACCEPTED January 5, INCLUDE WHEN CITING Published online July 14, 2017; DOI: / SPINE AANS, 2017
2 Anterior lumbar discectomy and fusion for cauda equina syndrome recurrence. In the presence of a second disc herniation, particularly a large one as in CES, fusion may also prevent sequelae of removal of large fragments of disc from the intervertebral space, such as loss of disc height, back pain, and deformity. Transforaminal and posterior interbody fusions have been performed in this setting with inconsistent results. 3 There are no previous reports describing anterior discectomy and fusion for CES caused by recurrent lumbar disc herniation. We report on 3 cases in which anterior discectomy and fusion were performed for this condition. The rationale for anterior surgery in each of the cases described was as follows: 1) to avoid potential complications related to posterior epidural scarring, 2) to enable a more extensive discectomy to eliminate the risk of recurrence, and 3) to treat postdiscectomy back pain that had complicated the primary posterior lumbar disc surgery in each patient. All 3 patients underwent anterior lumbar discectomy and fusion (ALDF) in which a stand-alone cage was placed at the level of the recurrent pathology. Case Reports Case 1 A 53-year-old man presented to our institution with CES due to a recurrent L5 S1 disc prolapse. He had previously undergone 2 posterior microdiscectomies at L5 S1. The patient s first surgery, 4 years previously, was a posterior L5 S1 microdiscectomy for CES caused by a canal-filling disc. Postoperatively, he recovered full bladder and bowel function and experienced complete resolution of bilateral leg pain. A recurrence of the L5 S1 disc prolapse occurred 2 years later resulting in right S-1 radicular leg pain. Revision right L5 S1 posterior discectomy successfully alleviated the leg pain, but the patient reported ongoing, intermittent low-back pain. Two years later he presented acutely with bilateral radicular leg pain, urinary incontinence, and an abnormal rectal examination with an absent bulbocavernosus reflex. MRI revealed recurrence of a large, right paracentral L5 S1 disc (Fig. 1), and a diagnosis of CES was made in view of the objective evidence of acute sacral nerve root dysfunction. Due to concerns regarding epidural and perineural scarring following the 2 previous L5 S1 discectomies, an anterior approach for discectomy was selected. Fusion was chosen because this was the patient s third presentation for the same-level pathology and the patient had ongoing low-back pain. The patient was operated on immediately via an anterior, left-sided retroperitoneal approach to access the L5 S1 disc, which was excised under direct vision. The posterior annulus fibrosus and posterior longitudinal ligament (PLL) defects were visualized using an operating microscope, and the sequestered fragments were retrieved without difficulty through the defect. The dural tube was found to be mobile and not adherent to the sequestrated fragments. Epidural scarring was seen but not directly encountered during the decompression. A stand-alone constrained anterior cage was filled with femoral head allograft mixed with bone marrow aspirate and placed into the disc space. It was fixed with constrained locking screws to facilitate fusion through the disc space. FIG. 1. Case 1. Preoperative sagittal (left) and axial (right) MR images. On the 1st postoperative day, the patient s bilateral leg pain had resolved and the patient was able to ambulate. The patient s bulbocavernosus reflex had returned, the urinary catheter was removed, and he was able to micturate with voluntary control. Hospital discharge occurred on the 2nd postoperative day. Postoperative MRI (Fig. 2A and B) demonstrated adequate decompression. A radiograph at 8 months demonstrated satisfactory cage positioning (Fig. 2C and D). At 2 years, the patient reported no significant back or leg pain and he no longer required any analgesics. FIG. 2. Case 1. Six-week postoperative sagittal (A) and L5 S1 axial (B) MR images and 8-month postoperative weight-bearing lateral (C) and anteroposterior (D) radiographs. 353
3 K. A. Tan et al. Case 2 A 39-year-old woman presented with acute onset of right leg pain and paresthesia in the S-1 nerve root distribution, perianal numbness, and painless urinary retention. Two years previously, she had undergone posterior discectomy at L5 S1 for right S-1 radicular leg pain. She reported improvement in leg pain following the surgery, but she had intermittent, residual low-back pain. Neurological examination revealed reduced right perineal and leg sensation with no motor deficits. Her bulbocavernosus reflex was absent and her anal tone was reduced. MRI showed a large right paracentral L5 S1 disc (Fig. 3) that was causing cauda equina compression. An ALDF was performed immediately. The anterior approach was chosen due to concerns regarding epidural scarring from the primary surgery. Intraoperatively, under the microscope, a large posterior disc fragment contiguous with the disc was found to be compressing the dural tube. The PLL was taken down to expose the dura, and the disc was removed under direct vision without the need to dissect around epidural scar tissue. The exiting L-5 and traversing S-1 nerve roots were visualized, and a scar could be seen adjacent to the S-1 nerve roots in the lateral recesses on both sides. A stand-alone anterior fusion cage was packed with allograft bone and implanted. Immediately postoperatively, the patient s urinary symptoms improved and her bulbocavernosus reflex returned. Her leg pain improved, but leg and perianal paresthesia remained. She was discharged on Day 3 postoperatively. At her 6-week follow-up, the patient reported continued improvement in back and leg pain and she had ceased taking all neuropathic analgesics. Postoperative MRI demonstrated satisfactory cauda equina decompression (Fig. 4). At 1 year, the patient reported resolution of back and leg pain and normal bladder and bowel function. Neurological examination demonstrated reduced sensation to pinprick and light touch over the right perianal region and in the right S-1 nerve root distribution. Radiography demonstrated signs of bony fusion through the cage. FIG. 4. Case 2. Postoperative sagittal (left) and L5 S1 axial (right) MR images showing adequate cauda equina decompression. Case 3 A 30-year-old woman presented with sciatic pain in her right leg, incomplete urinary voiding, and perianal numbness. Examination demonstrated decreased perineal sensation and reduced anal tone on rectal examination. MRI showed a large right paracentral disc at L4 5 causing cauda equina compression (Fig. 5). Three years previously, the patient had undergone a posterior L4 5 microdiscectomy for right leg pain; the procedure had improved her leg pain but left the patient with residual low-back pain following the surgery. A diagnosis of CES was made, and ALDF (as described in Cases 1 and 2) was performed on the same day as presentation. Intraoperatively, a defect in the posterior annulus fibrosus was identified, and loose disc fragments were seen centrally, extending distally just beyond the superior L-5 endplate, as well as into the axilla of the right L-5 nerve root. Under direct vision with the microscope, these fragments were removed. Epidural scar tissue was not encountered and a posterior lip osteophyte on L-5 was also removed. Immediately postoperatively, the patient s right leg pain improved and her bladder and bowel function returned to normal; however, sensory dysesthesia in the leg and perianal numbness remained. Postoperative MRI demonstrat- FIG. 3. Case 2. Preoperative sagittal (left) and L5 S1 axial (right) MR images. FIG. 5. Case 3. Preoperative sagittal (left) and L4 5 axial (right) MR images. 354
4 Anterior lumbar discectomy and fusion for cauda equina syndrome ed adequate cauda equina decompression at L4 5 (Fig. 6A and B). At 1 year, the patient still complained of sensory dysesthesia in the right leg with persistent perianal numbness. She reported no back or leg pain, and radiography demonstrated radiographic fusion through the cage (Fig. 6C). Discussion The standard surgical treatment for acute disc herniation causing CES is posterior discectomy. 2,9 However, in cases of recurrent disc herniation, a repeat posterior approach poses a higher risk of dural tear, especially during dissection around the nerve roots in the presence of epidural fibrosis. 8 This may necessitate more extensive posterior bone removal for safe access to the disc material that needs retrieval. 3 Avoidance of posterior scar tissue and treatment of residual, postdiscectomy low-back pain FIG. 6. Case 3. Postoperative sagittal (A) and L4 5 axial (B) MR images showing adequate cauda equina decompression. Twelve-month postoperative weight-bearing lateral radiograph (C) showing radiographic evidence of fusion through the cage. were the rationale we used for performing primary ALDF for CES caused by recurrent disc herniation in the patients reported on in this article. The anterior approach obviated the need for dissection around epidural scar tissue, preventing the potential need for excessive posterior bone resection that might have been necessary to achieve safe access to the disc (with inherent risk of postlaminectomy instability), and addressing the residual, postdiscectomy low-back pain in each patient. In cases in which herniated disc material is contiguous with the intervertebral disc, the anterior approach provides an added advantage because the PLL and annular tissue may act as a containing sac within which nuclear material may be more readily extracted via an anterior position. Once this material is removed, any remaining loose material within the canal, external to the herniation sac, may be extracted without the need for placing the dural tube or nerve roots under significant retraction. In our experience, the dural tube and nerve roots are placed under greater retraction when removing these intracanal disc fragments from the posterior position. In all 3 cases, we did not find it necessary to dissect around epidural scar tissue to safely remove compressive disc fragments from the canal. However, we did find that the anterior approach in this revision discectomy setting posed one additional risk. In all cases there was a thin anterior membrane over the anterior annulus of the disc, which is not usually present in a standard anterior approach to a nonoperated disc level. Presumably this was a reactive phenomenon from the previous posterior lumbar disc surgery. This may make vessel mobilization more hazardous when an anterior decompression is performed in the revision setting, which the surgeon should be aware of. There are some disadvantages to and contraindications for the anterior approach for revision lumbar discectomy that the surgeon should be aware of including the requirement for an access surgeon, which can be difficult when the procedure is performed as an emergency procedure as in our 3 cases. In our institution, the senior surgeon carries out all the anterior approaches obviating the need for an access surgeon. This may not be the case in other centers. Additionally, vascular, ureteric, and visceral injuries are all considerable risks that are not present when using the posterior approach. We would urge caution with an anterior approach in the presence of the following factors: increasing age, great-vessel calcification, low bifurcating vasculature, history of abdominal surgery, and presence of anterior osteophytes, which can be adherent to the common iliac veins; all of these can all make the anterior approach more dangerous. When surgery is indicated for a recurrent disc herniation, the most commonly performed revision procedure is a repeat lumbar discectomy alone without fusion. 10 This is the accepted standard of care that most surgeons would follow, and it is the treatment that we advocate in our unit. However, this is a controversial topic, and there remains much debate about the optimal surgical treatment for recurrent lumbar disc herniation. Addition of a fusion to the revision discectomy has been advocated in the presence 1, 4, 6,10 of segmental instability, chronic back pain, and CES. The rationale for fusion in CES caused by recurrent disc 355
5 K. A. Tan et al. herniation is that complete disc material clearance with fusion eliminates the potential for recurrent disc herniation. Furthermore, the disc space is stabilized, removing a further potential pain source should the patient experience ongoing low-back pain. ALDF is one option to achieve fusion with acceptable long-term functional outcomes 1,5, 7,12 and fusion rates for nonrevision discectomy patients. 1,5 However outcomes in the recurrent disc herniation population have not been studied. Alternative methods of fusion, including transforaminal and posterior interbody techniques, are likely to be as equally effective. Comparison studies of techniques are difficult to perform due to the rarity of the condition. The purpose of this case report is to describe a novel technique for the treatment for acute CES caused by recurrent lumbar disc herniation. This is a rare condition, and as such, many different treatment strategies have been proposed. When possible, we would advocate repeat posterior lumbar decompression surgery as the treatment of choice for this clinical scenario, as this procedure has a lower complication rate than a fusion procedure. If the surgeon believes fusion is appropriate because of ongoing low-back pain, the risk of instability, or the wish to remove the entire disc so that recurrence is eliminated, transforaminal and posterior lumbar interbody techniques may be appropriate and effective. These posterior procedures carry different risks and benefits than an anterior fusion procedure. Clearly the effectiveness and safety of this novel technique need further evaluation, but from our limited experience, ALDF has been an effective treatment option in cases of recurrent disc herniation causing CES in patients who have undergone a previous posterior discectomy at the same level and who have had ongoing low-back pain as a sequela of this primary procedure. Our patients reported an improvement in their back and leg pain at 1 year and resolution of their sphincter dysfunction, and we observed no cases of infection, dural tear, or vascular or neurological injury. References 1. Choi JY, Choi YW, Sung KH: Anterior lumbar interbody fusion in patients with a previous discectomy: minimum 2-year follow-up. J Spinal Disord Tech 18: , Gleave JR, Macfarlane R: Cauda equina syndrome: what is the relationship between timing of surgery and outcome? Br J Neurosurg 16: , Glenn JS, Yaker J, Guyer RD, Ohnmeiss DD: Anterior discectomy and total disc replacement for three patients with multiple recurrent lumbar disc herniations. Spine J 11:e1 e6, Greenleaf RM, Harris MB, Bono CM: The role of fusion for recurrent disk herniations. Semin Spine Surg 23: , Inoue S, Watanabe T, Hirose A, Tanaka T, Matsui N, Saegusa O, et al: Anterior discectomy and interbody fusion for lumbar disc herniation. A review of 350 cases. Clin Orthop Relat Res (183):22 31, Li Z, Tang J, Hou S, Ren D, Li L, Lu X, et al: Four-year follow-up results of transforaminal lumbar interbody fusion as revision surgery for recurrent lumbar disc herniation after conventional discectomy. J Clin Neurosci 22: , Miyamoto K: [Long-term follow-up results of anterior discectomy and interbody fusion for lumbar disc herniation.] Nippon Seikeigeka Gakkai Zasshi 65: , 1991 (Jpn) 8. Ozgen S, Naderi S, Ozek MM, Pamir MN: Findings and outcome of revision lumbar disc surgery. J Spinal Disord 12: , Shapiro S: Cauda equina syndrome secondary to lumbar disc herniation. Neurosurgery 32: , Stambough JL: An algorithmic approach to recurrent lumbar disk herniation: evaluation and management. Semin Spine Surg 20:2 13, Stolke D, Sollmann WP, Seifert V: Intra- and postoperative complications in lumbar disc surgery. Spine (Phila Pa 1976) 14:56 59, Vishteh AG, Dickman CA: Anterior lumbar microdiscectomy and interbody fusion for the treatment of recurrent disc herniation. Neurosurgery 48: , 2001 Disclosures Dr. Stokes serves as a consultant for NuVasive. Author Contributions Conception and design: Chan, Markmann. Acquisition of data: Chan, Tan, Markmann. Drafting the article: Tan, Markmann. Critically revising the article: Chan, Tan, Sewell, Clarke, Stokes. Reviewed submitted version of manuscript: Chan, Tan, Clarke, Stokes. Administrative/technical/material support: Chan, Tan, Sewell. Study supervision: Chan, Sewell, Stokes. Correspondence Daniel Chan, Exeter Spine Unit, Princess Elizabeth Orthopaedic Centre, Royal Devon and Exeter NHS Foundation Trust, Barrack Rd., Exeter EX2 5DW, United Kingdom. spineman.yoda@ gmail.com. 356
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion. Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD
 ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
ORIGINAL ARTICLE Recurrent Lumbar Disk Herniation With or Without Posterolateral Fusion Ahmed Zaater, MD, Alaa Azzazi, MD, Sameh Sakr, MD, and Ahmed Elsayed, MD Study Design: A prospective study assessing
Anthem Blue Cross and Blue Shield Central Region Clinical Claim Edit
 Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Subject: Laminotomy (Hemilaminectomy) with Decompression of Nerve Root(s), Including Partial Facetectomy, Foraminotomy and/or Excision of Herniated Intervertebral Disc, Reexploration, Single Interspace-Lumbar
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Disclosures 5/27/2016. Narrowing of the spinal canal or neuroforamina causing a symptomatic compression of the neural element.
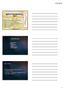 Radiculopathy Saggital MRI view Contained disc extrusion uplifting PLL from bone Terrence Julien, MD, FACS, (blue FAANS arrows) Associate Professor of Neurosurgery System Director, Surgical Neuro-Oncology
Radiculopathy Saggital MRI view Contained disc extrusion uplifting PLL from bone Terrence Julien, MD, FACS, (blue FAANS arrows) Associate Professor of Neurosurgery System Director, Surgical Neuro-Oncology
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
Lumbar disc prolapse. Done by : Areej Al-Hadidi
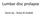 Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
Does patient history and physical examination predict MRI proven cauda equina syndrome?
 27 27 33 Does patient history and physical examination predict MRI proven cauda equina syndrome? Authors Jeremy Fairbank¹, Robin Hashimoto², Andrew Dailey ³, Alpesh A Patel³, Joseph R Dettori² Institutions
27 27 33 Does patient history and physical examination predict MRI proven cauda equina syndrome? Authors Jeremy Fairbank¹, Robin Hashimoto², Andrew Dailey ³, Alpesh A Patel³, Joseph R Dettori² Institutions
Anuj D. Bharuka*, Rajendra Phunde, Hiren B. Patel
 International Journal of Research in Orthopaedics Bharuka AD et al. Int J Res Orthop. 17 Sep;3(5):998-13 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/1.183/issn.55-51.intjresorthop1731
International Journal of Research in Orthopaedics Bharuka AD et al. Int J Res Orthop. 17 Sep;3(5):998-13 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/1.183/issn.55-51.intjresorthop1731
Back Pain Policies Summary
 Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Back Pain Policies Summary These policies are part of the wider project, Reviewing local health policies, which is reviewing and updating more than 100 policies, of which back pain are part of. This review
Surgery. Conus medullaris and Cauda Equina Syndromes. Anatomy. See online here
 Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Surgery Conus medullaris and Cauda Equina Syndromes See online here Conus medullaris and cauda equina syndromes are spinal cord injuries that involve injury to the lumbosacral segment of the spinal cord.
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
REFERENCE DOCTOR Percutaneous Endoscopic Discectomy Transforaminal / Interlaminar. Hyeun Sung Kim, MD, PhD,
 Percutaneous Endoscopic Discectomy Transforaminal / Interlaminar Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean
Percutaneous Endoscopic Discectomy Transforaminal / Interlaminar Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean
Review date: February Lumbar Discectomy
 Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Review date: February 2019 Lumbar Discectomy Following your recent MRI scan and consultation with your spinal surgeon, you have been diagnosed as having a lumbar disc protrusion, resulting in nerve root
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients
 Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Lumbar Disc Prolapse: Management and Outcome Analysis of 96 Surgically treated Patients A. Akbar ( Department of Neurosurgery, Chandka Medical College, Larkana. ) A. Mahar ( Department of Orthopedic Surgery,
Key Primary CPT Codes: Refer to pages: 7-9 Last Review Date: October 2016 Medical Coverage Guideline Number:
 National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
National Imaging Associates, Inc. Clinical guidelines CERVICAL SPINE SURGERY: ANTERI CERVICAL DECOMPRESSION WITH FUSION CERVICAL POSTERI DECOMPRESSION WITH FUSION CERVICAL ARTIFICIAL DISC CERVICAL POSTERI
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH
 Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
Document Control Title Protocol for the management of suspected cauda equine syndrome & decompensating spinal stenosis at NDDH Author Author s job title Consultant T&O Directorate Scheduled Care Department
POSTERIOR CERVICAL FUSION
 AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
AN INTRODUCTION TO PCF POSTERIOR CERVICAL FUSION This booklet provides general information on the Posterior Cervical Fusion (PCF) surgical procedure for you to discuss with your physician. It is not meant
Original Article Clinics in Orthopedic Surgery 2015;7:
 Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
Original Article Clinics in Orthopedic Surgery 2015;7:91-96 http://dx.doi.org/10.4055/cios.2015.7.1.91 Perioperative Surgical Complications and Learning Curve Associated with Minimally Invasive Transforaminal
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage posterior surgery: a case report
 Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Iizuka et al. Journal of Medical Case Reports 2014, 8:421 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Giant schwannoma with extensive scalloping of the lumbar vertebral body treated with one-stage
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Huan-Chieh Chen, 1 Chih-Hsun Lee, 1 Li Wei, 1 Tai-Ngar Lui, 1 and Tien-Jen Lin 1,2. 1. Introduction
 Neurology Research International Volume 2015, Article ID 791943, 5 pages http://dx.doi.org/10.1155/2015/791943 Clinical Study Comparison of Percutaneous Endoscopic Lumbar Discectomy and Open Lumbar Surgery
Neurology Research International Volume 2015, Article ID 791943, 5 pages http://dx.doi.org/10.1155/2015/791943 Clinical Study Comparison of Percutaneous Endoscopic Lumbar Discectomy and Open Lumbar Surgery
Peggers Super Summaries: The Aging Spine
 Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Herniated Disk in the Lower Back
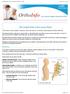 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
HERNIATED DISCS AN INTRODUCTION TO
 AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
AN INTRODUCTION TO HERNIATED S This booklet provides general information on herniated discs. It is not meant to replace any personal conversations that you might wish to have with your physician or other
Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion
 Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Case Reports in Orthopedics, Article ID 456940, 4 pages http://dx.doi.org/10.1155/2014/456940 Case Report Adjacent Lumbar Disc Herniation after Lumbar Short Spinal Fusion Koshi Ninomiya, Koichi Iwatsuki,
Objectives. Comprehension of the common spine disorder
 Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Objectives Comprehension of the common spine disorder Disc degeneration/hernia Spinal stenosis Common spinal deformity (Spondylolisthesis, Scoliosis) Osteoporotic fracture Destructive spinal lesions Anatomy
Insert heading depending. cover options once. other cover options once you have chosen one. 20pt. Ref: N-SC/031
 Insert heading depending Insert Interim Insert heading Clinical Commissioning depending on line on on Policy: line length; length; please please delete delete on line line Spinal length; Surgery please
Insert heading depending Insert Interim Insert heading Clinical Commissioning depending on line on on Policy: line length; length; please please delete delete on line line Spinal length; Surgery please
Case Report A Rare Case of Progressive Palsy of the Lower Leg Caused by a Huge Lumbar Posterior Endplate Lesion after Recurrent Disc Herniation
 Case Reports in Orthopedics Volume 2016, Article ID 5963924, 4 pages http://dx.doi.org/10.1155/2016/5963924 Case Report A Rare Case of Progressive Palsy of the Lower Leg Caused by a Huge Lumbar Posterior
Case Reports in Orthopedics Volume 2016, Article ID 5963924, 4 pages http://dx.doi.org/10.1155/2016/5963924 Case Report A Rare Case of Progressive Palsy of the Lower Leg Caused by a Huge Lumbar Posterior
Zheng Li, Fubing Liu, Shuhao Liu, Zixian Chen, Chun Jiang, Zhenzhou Feng, and Xiaoxing Jiang
 BioMed Research International Volume 2016, Article ID 7261027, 6 pages http://dx.doi.org/10.1155/2016/7261027 Clinical Study Miniopen Transforaminal Lumbar Interbody Fusion with Unilateral Fixation: A
BioMed Research International Volume 2016, Article ID 7261027, 6 pages http://dx.doi.org/10.1155/2016/7261027 Clinical Study Miniopen Transforaminal Lumbar Interbody Fusion with Unilateral Fixation: A
MOHAMED LOTFY, M.D.*; SAMEH A. SAKR, M.D.* and ASHRAF E. ZAGHLOUL, M.D.**
 Med. J. Cairo Univ., Vol. 84, No. 1, December: 1463-1469, 216 www.medicaljournalofcairouniversity.net Extensive Laminectomy for Redo Lumbar Discectomy; Could it Be A Successful Alternative Option in Stable
Med. J. Cairo Univ., Vol. 84, No. 1, December: 1463-1469, 216 www.medicaljournalofcairouniversity.net Extensive Laminectomy for Redo Lumbar Discectomy; Could it Be A Successful Alternative Option in Stable
MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION AN INTRODUCTION TO
 AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
AN INTRODUCTION TO MAS TLIF MAXIMUM ACCESS SURGERY TRANSFORAMINAL LUMBAR INTERBODY FUSION This booklet is designed to inform you about the Maximum Access Surgery (MAS ) Transforaminal Lumbar Interbody
Disclosure. Thoracolumbar Tumors. Intraspinal Tumor Removal Options 6/4/2011. Minimally Invasive Approaches for Spinal Tumors
 Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Approaches for Spinal Tumors Praveen V. Mummaneni, M.D. Disclosure Medtronic (Consultant, Grants) DePuy (Consultant, Other Financial Support) Associate Professor Dept. of Neurosurgery
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy
 Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
Minimally Invasive Spine Surgery Endoscopic Postrior Cervical Foraminotomy Benedikt Burkhardt Department of Neurosurgery, Saarland University Medical Center, Homburg/Saar, Germany Background The managment
Ch ng Hwei Choo, Mun Keong Kwan, Yin Wei Chris Chan. Case presentation. Introduction
 Case Report Page 1 of 5 Surgical reduction technique (transpedicle) for unstable thoracolumbar burst fractures with retropulsion resulting in severe spinal canal stenosis: a preliminary case report Ch
Case Report Page 1 of 5 Surgical reduction technique (transpedicle) for unstable thoracolumbar burst fractures with retropulsion resulting in severe spinal canal stenosis: a preliminary case report Ch
Transdural Discectomy Lumbar Region: A retrospective series of 10 cases
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 16 Number 2 Transdural Discectomy Lumbar Region: A retrospective series of 10 cases M Singh, N Kalsotra, S Sharma, D Singh Citation M Singh,
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 16 Number 2 Transdural Discectomy Lumbar Region: A retrospective series of 10 cases M Singh, N Kalsotra, S Sharma, D Singh Citation M Singh,
Sir William Asher ANATOMY
 SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
SPINAL CORD INJURY BASICS RELATED TO LIFE CARE PLANNING Lesson 1 Sir William Asher Picture the pathetic patient lying long abed, the urine leaking from his distended bladder, the lime draining from his
Anterior cervical diskectomy icd 10 procedure code
 Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
Home Anterior cervical diskectomy icd 10 procedure code Access to discounts at hundreds of restaurants, travel destinations, retail stores, and service providers. AAPC members also have opportunities to
ASJ. A Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia. Asian Spine Journal. Introduction
 sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
sian Spine Journal 126 Dong-Eun Case Shin Report et al. http://dx.doi.org/10.4184/asj.2013.7.2.126 Rare Hyperextension Injury in Thoracic Spine Presenting with Delayed Paraplegia Dong-Eun Shin, Ki-Sik
Physician Reference Manual
 Nucleotome Physician Reference Manual Automated Percutaneous Lumbar Discectomy 900487-001-00, Page 1 Nucleotome Automated Percutaneous Lumbar Discectomy (APLD) Table of Contents Section 1 I. Description
Nucleotome Physician Reference Manual Automated Percutaneous Lumbar Discectomy 900487-001-00, Page 1 Nucleotome Automated Percutaneous Lumbar Discectomy (APLD) Table of Contents Section 1 I. Description
HAMSTRING TIGHTNESS AND SCIATICA IN YOUNG PATIENTS WITH DISC HERNIATION
 HAMSTRNG TGHTNESS AND SATA N YOUNG PATENTS WTH DS HERNATON KEH TAKATA, KAZUHSA TAKAHASH From hiba University, hiba, Japan We evaluated the nerve roots of the cauda equina by T myelography in 36 patients
HAMSTRNG TGHTNESS AND SATA N YOUNG PATENTS WTH DS HERNATON KEH TAKATA, KAZUHSA TAKAHASH From hiba University, hiba, Japan We evaluated the nerve roots of the cauda equina by T myelography in 36 patients
PATIENT: DOB: TODAY S DATE:
 1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
1. I have been strongly advised to carefully read and consider this operative permit. I realize that it is important that I understand this material. I also understand that if certain sections are not
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
REFERENCE DOCTOR Thoracolumbar Trauma MIS Options. Hyeun Sung Kim, MD, PhD,
 Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Thoracolumbar Trauma MIS Options Medical College of Chosun University, Gwangju, South Korea (1994) / Board of Neurosurgery (1999) MEMBERSHIPS & PROFESSIONAL SOCIETIES Korean Neurosurgical Society / Korean
Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture
 779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
779 Spontaneous Resolution of Spinal Canal Deformity After Burst Dispersion Fracture T. M. H. Chakera 1 George Bedbrook C. M. Bradley3 We reviewed the records of 8 patients with 30 burst-dispersion spinal
Patient Information MIS LLIF. Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Patient Information MIS LLIF Lateral Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques Table of Contents Anatomy of Spine....2 General Conditions of the Spine....4 What is Spondylolisthesis....5
Surgical Treatment for Posterior Rim Separation of the Lumbar and Sacral Vertebrae
 177 2013 Chinese Orthopaedic Association and Wiley Publishing Asia Pty Ltd CLINICAL ARTICLE Surgical Treatment for Posterior Rim Separation of the Lumbar and Sacral Vertebrae Jiang-tao He, MD, Jian-wen
177 2013 Chinese Orthopaedic Association and Wiley Publishing Asia Pty Ltd CLINICAL ARTICLE Surgical Treatment for Posterior Rim Separation of the Lumbar and Sacral Vertebrae Jiang-tao He, MD, Jian-wen
Clinical and Radiological Findings of Nerve Root Herniation after Discectomy of Lumbar Disc Herniation
 www.jkns.or.kr J Korean Neurosurg Soc 52 : 62-66, 2012 http://dx.doi.org/10.3340/jkns.2012.52.1.62 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2012 The Korean Neurosurgical Society Case Report
www.jkns.or.kr J Korean Neurosurg Soc 52 : 62-66, 2012 http://dx.doi.org/10.3340/jkns.2012.52.1.62 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2012 The Korean Neurosurgical Society Case Report
Innovative Techniques in Minimally Invasive Cervical Spine Surgery. Bruce McCormack, MD San Francisco California
 Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Innovative Techniques in Minimally Invasive Cervical Spine Surgery Bruce McCormack, MD San Francisco California PCF Posterior Cervical Fusion PCF not currently an ambulatory care procedure Pearl diver
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose
 Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
Anterior and Lateral Lumbar Minimally Invasive Approaches: How to Choose Lukas P. Zebala, MD Assistant Professor Washington University School of Medicine St. Louis, MO Disclosures Consultant: K2M, Inc.
A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
 Pain Physician 2017; 20:E605-E609 ISSN 2150-1149 Case Report A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
Pain Physician 2017; 20:E605-E609 ISSN 2150-1149 Case Report A Novel Combination of Percutaneous Endoscopic Lumbar Discectomy and Epiduroscopic Laser Neural Decompression for Down-migrated Disc Herniation
The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery
 The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery SPINE Volume 35, Number 17, pp E849 E854 2010, Lippincott Williams & Wilkins Chun-Hao
The Evaluation of Bladder Symptoms in Patients With Lumbar Compression Disorders Who Have Undergone Decompressive Surgery SPINE Volume 35, Number 17, pp E849 E854 2010, Lippincott Williams & Wilkins Chun-Hao
Case Report Synovial Cyst Mimicking an Intraspinal Sacral Mass
 , Article ID 953579, 4 pages http://dx.doi.org/10.1155/2014/953579 Case Report Synovial Cyst Mimicking an Intraspinal Sacral Mass Jason Hoover 1,2 and Stephen Pirris 3 1 The Texas Brain and Spine Institute,
, Article ID 953579, 4 pages http://dx.doi.org/10.1155/2014/953579 Case Report Synovial Cyst Mimicking an Intraspinal Sacral Mass Jason Hoover 1,2 and Stephen Pirris 3 1 The Texas Brain and Spine Institute,
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018
 Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018 Disclosures Neither I nor any family members have financial disclosures Special thanks
Gillian Wooldridge, DO Houston Methodist Willowbrook Hospital Primary Care Sports Medicine Fellowship May 3, 2018 Disclosures Neither I nor any family members have financial disclosures Special thanks
LATERAL LUMBAR INTERBODY FUSION
 LATERAL LUMBAR INTERBODY FUSION Dr. Majesh Pratap Malla * and Dr. She Yuan Ju Department of Orthopaedics, Clinical Medical College of Yangtze University, Jingzhou Central Hospital Jingzhou, Hubei Province,
LATERAL LUMBAR INTERBODY FUSION Dr. Majesh Pratap Malla * and Dr. She Yuan Ju Department of Orthopaedics, Clinical Medical College of Yangtze University, Jingzhou Central Hospital Jingzhou, Hubei Province,
paracentral disc herniations, especially disc extrusions and disc sequestrations, remains challenging.
 Orthopaedic Surgery SURGICAL TECHNOLOGY INTERNATIONAL XIX Transforaminal Endoscopic Lumbar Procedure for Disc Herniations: A "Between" Technique KAI-XUAN LIU, M.D, PH.D. ATLANTIC SPINAL CARE EDISON, NEW
Orthopaedic Surgery SURGICAL TECHNOLOGY INTERNATIONAL XIX Transforaminal Endoscopic Lumbar Procedure for Disc Herniations: A "Between" Technique KAI-XUAN LIU, M.D, PH.D. ATLANTIC SPINAL CARE EDISON, NEW
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Chapter 35 Back Pain. Episode overview: Wisecracks: Crack Cast Show Notes Back Pain July 2016
 Chapter 35 Back Pain Episode overview: 1) List 10 historical red flags for back pain 2) List 6 Emergent Diagnosis for back pain Wisecracks: 1) Describe the most common sites of disc protrusion with their
Chapter 35 Back Pain Episode overview: 1) List 10 historical red flags for back pain 2) List 6 Emergent Diagnosis for back pain Wisecracks: 1) Describe the most common sites of disc protrusion with their
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Functional Outcome of Patients with Lumbar Intervertebral Disc Herniation after Minimally Invasive Microdiscectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. II (July. 2017), PP 35-39 www.iosrjournals.org Functional Outcome of Patients with Lumbar
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. II (July. 2017), PP 35-39 www.iosrjournals.org Functional Outcome of Patients with Lumbar
Medical Policy Original Effective Date: Revised Date: Page 1 of 11
 Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Page 1 of 11 Content Disclaimer Description Coverage Determination Clinical Indications Lumbar Spine Surgery Lumbar Spine Surgery Description Indication Coding Lumbar Spinal Fusion (single level)surgery
Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review
 Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
Pain Physician 2017; 20:E445-E449 ISSN 2150-1149 Literature Review Transforaminal Endoscopic Decompression for a Giant Epidural Gas-Containing Pseudocyst: A Case Report and Literature Review Bin Zhu, MD,
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint
 J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
J Orthop Sci (2012) 17:189 193 DOI 10.1007/s00776-011-0082-y CASE REPORT A rare case of spinal injury: bilateral facet dislocation without fracture at the lumbosacral joint Kei Shinohara Shigeru Soshi
Case Studies, Impairment of the Spine in Washington State
 Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
Case Studies, Impairment of the Spine in Washington State NAOEM at Skamania, 2015 25 Sep, 2015 Tim Gilmore, MD Several Slides from this Presentation Borrowed with permission from the Washington State Department
Degenerative L4-5 SPONDYLOLISTHESIS with Stenosis: Laminectomy and Postero-Lateral Fusion. Rick C. Sasso MD
 Degenerative L4-5 SPONDYLOLISTHESIS with Stenosis: Laminectomy and Postero-Lateral Fusion Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure:
Degenerative L4-5 SPONDYLOLISTHESIS with Stenosis: Laminectomy and Postero-Lateral Fusion Rick C. Sasso MD Professor Chief of Surgery Clinical Orthopaedic Surgery University School of Medicine Disclosure:
Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion
 Original Study Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion Tomohide Segawa 1, Hirohiko Inanami 1, Hisashi Koga 2 1 Department of Orthopaedic Surgery, Inanami Spine and
Original Study Clinical evaluation of microendoscopy-assisted extreme lateral interbody fusion Tomohide Segawa 1, Hirohiko Inanami 1, Hisashi Koga 2 1 Department of Orthopaedic Surgery, Inanami Spine and
Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature
 ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 2 Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature I Omeis, A Cutler,
ISPUB.COM The Internet Journal of Neurosurgery Volume 3 Number 2 Sequestered High Lumbar Intradural Disc Herniation Mimicking A Spinal Tumor: Case Report And Review Of The Literature I Omeis, A Cutler,
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Christopher I. Shaffrey, MD
 CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
CSRS 21st Instructional Course Wednesday, November 30, 2016 Laminoplasty/Foraminotomy: Why Fuse the Spine at all? Christopher I. Shaffrey, MD John A. Jane Distinguished Professor Departments of Neurosurgery
AMA Guides 4 th Edition: Sample Case Review
 AMA Guides 4 th Edition: Sample Case Review CASE #1 Ms. Parker is a 26 year old woman who sustained a fracture of the tuft of the distal phalynx of the right little finger, which was treated with a splint.
AMA Guides 4 th Edition: Sample Case Review CASE #1 Ms. Parker is a 26 year old woman who sustained a fracture of the tuft of the distal phalynx of the right little finger, which was treated with a splint.
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion
 Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Romanian Neurosurgery Volume XXXI Number 1 2017 January - March Article Surgery in cervical disc herniation: anterior cervical discectomy without fusion or with fusion Andrei Stefan Iencean ROMANIA DOI:
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF)
 Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Royal Oak IBFD System Surgical Technique Posterior Lumbar Interbody Fusion (PLIF) Preoperative Planning Preoperative planning is necessary for the correct selection of lumbar interbody fusion devices.
Alamo T Transforaminal Lumbar Interbody System Surgical Technique
 Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
Transforaminal Lumbar Interbody System Surgical Technique Table of Contents Indications and Device Description.............. 1 Alamo T Implant Features and Instruments...........2 Surgical Technique......................
nvt Transforaminal Lumbar Interbody Fusion System
 nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
nvt Transforaminal Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine
Commander Cervical Cage - SURGICAL TECHNIQUE
 Commander Cervical Cage - SURGICAL TECHNIQUE D e s i g n e d to c l o s e l y f i t yo u! Commander Cervical Cage - SURGICAL TECHNIQUE Indications Commander cervical cages are designed primarly for restoring
Commander Cervical Cage - SURGICAL TECHNIQUE D e s i g n e d to c l o s e l y f i t yo u! Commander Cervical Cage - SURGICAL TECHNIQUE Indications Commander cervical cages are designed primarly for restoring
nvp Posterior Lumbar Interbody Fusion System
 nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
nvp Posterior Lumbar Interbody Fusion System 1 IMPORTANT INFORMATION FOR PHYSICIANS, SURGEONS, AND/OR STAFF The nv a, nv p, and nv t are an intervertebral body fusion device used in the lumbar spine following
INTERVERTEBRAL BODY FUSION DEVICE. Surgical Technique
 INTERVERTEBRAL BODY FUSION DEVICE Surgical Technique Joint Spine Sports Med MectaLIF Oblique & Posterior Surgical Technique 2 INDEX 1. INTRODUCTION 4 1.1 Materials & Markers 5 2. INDICATIONS 6 3. CONTRAINDICATIONS
INTERVERTEBRAL BODY FUSION DEVICE Surgical Technique Joint Spine Sports Med MectaLIF Oblique & Posterior Surgical Technique 2 INDEX 1. INTRODUCTION 4 1.1 Materials & Markers 5 2. INDICATIONS 6 3. CONTRAINDICATIONS
3D titanium interbody fusion cages sharx. White Paper
 3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
3D titanium interbody fusion cages sharx (SLM selective laser melted) Goal of the study: Does the sharx intervertebral cage due to innovative material, new design, and lordotic shape solve some problems
Posterior Lumbar Decompression for Spinal Stenosis
 Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Posterior Lumbar Decompression for Spinal Stenosis Issue 6: March 2016 Review date: February 2019 Following your recent MRI scan and consultation with your spinal surgeon you have been diagnosed with
Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy
 Case Report Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy Ryutaro Shiboi 1,2, Yasushi Oshima 1,2,3, Takeshi Kaneko
Case Report Different operative findings of cases predicted to be symptomatic discal pseudocysts after percutaneous endoscopic lumbar discectomy Ryutaro Shiboi 1,2, Yasushi Oshima 1,2,3, Takeshi Kaneko
Thoracic and Lumbar Spine Fractures and Dislocations: Assessment and Classification
 Thoracic and Lumbar Spine Fractures and Dislocations: Assessment and Classification Mark L Prasarn MD University of Texas Dept of Orthopaedic Surgery Houston, Texas Updated 7/2016 Anatomy of the Spine
Thoracic and Lumbar Spine Fractures and Dislocations: Assessment and Classification Mark L Prasarn MD University of Texas Dept of Orthopaedic Surgery Houston, Texas Updated 7/2016 Anatomy of the Spine
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report
 Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
Upsala Journal of Medical Sciences. 2012; 117: 72 77 CASE REPORT Bilateral spondylolysis of inferior articular processes of the fourth lumbar vertebra: a case report TOMOAKI KOAKUTSU 1,2, NAOKI MOROZUMI
SpineFAQs. Cervical Disc Replacement
 SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
SpineFAQs Cervical Disc Replacement Artificial disc replacement (ADR) is relatively new. In June 2004, the first ADR for the lumbar spine (low back) was approved by the FDA for use in the US. Replacing
